Involvement of the small intestine in systemic mast
|
|
|
- Bonnie Lane
- 5 years ago
- Views:
Transcription
1 Gut, 1975, 16, Involvement of the small intestine in systemic mast cell disease BRIAN B. SCOTT, G. J. HARDY, AND M. S. LOSOWSKY From the University Department of Medicine and Department ofpathology, St James's Hospital, Leeds SUMMARY A patient is reported with mast cell infiltration of the small intestine in the absence of the skin involvement characteristic of mast cell disease. She also had subtotal villous atrophy responsive to a gluten-free diet. Criteria for diagnosing mast cell disease of the small intestine are proposed. The literature of small intestinal mast cell disease is reviewed and the relationship to coeliac disease is discussed. Mast cell disease or mastocytosis has been defined Case Report as '... chronic affections accompanied by specific infiltrations of mast cells into the skin or other The patient, a 47 year old housewife, became ill at tissue' (Sagher and Even-Paz, 1967). Mast cells are the age of 28 years when she began to complain of distinguished histologically by characteristic, metachromatic, cytoplasmic granules and special stains Sigmoidoscopy and radiology of the small and large bouts of colicky abdominal pain and diarrhoea. such as toluidine blue are recommended for their bowel were normal. Symptoms persisted for 10 years detection (Sagher and Even-Paz, 1967). The skin is after which she started to complain of flushing nearly always involved and the characteristic rash is attacks lasting about 20 minutes and mainly affecting the face. known as urticaria pigmentosa. Systemic involvement occurs in 10% of patients with mast cell disease; any organ may be involved, including the small intestinal malabsorption: faecal fat 56 mmol/24 h, Further investigation at a second hospital showed bowel on rare occasions. There are only a very few xylose absorption impaired, lactose tolerance curve well-documented reports of systemicmastcelldisease flat; a barium follow-through examination showed in the absence of skin involvement (Mutter et al., non-specific features of malabsorption. Recurring 1963; Gonnella and Lipsey, 1964). features of intestinal obstruction suggested Crohn's Mast cell infiltrations in the gastrointestinal tract disease and laparotomy was performed which have been demonstrated in a number of cases at showed a thickened, distended jejunum and small necropsy (Sagher and Even-Paz, 1967) but detection glands in the mesentery. Operative jejunal biopsy during life is distinctly rare. One of the problems in showed subtotal villous atrophy. A diagnosis of mast diagnosis is a lack of agreed criteria for recognizing cell disease was considered and, although no skin '... specific infiltrations of mast cells...' changes were present and bone marrow examination The present report describes a patient with typical was normal, confirmatory evidence was provided by symptoms of mast cell disease and mast cell infiltration of the small intestine but no skin involve- 5-HIAA excretion was repeatedly normal. Treatment a raised urinary histamine excretion. Urinary ment. In addition, there was subtotal villous atrophy with antihistamines gave some relief. and a response to a gluten-free diet, features described previously in association with mast cell attacks of abdominal pain, often with flushing, and The patient continued to complain of recurrent disease. Studies are presented in which mast cells in was admitted to a third hospital for investigation. the small bowel mucosa are quantitated in health There was no blood eosinophilia, repeated faecal and disease to enable criteria to be proposed for examinations for protozoa, cysts and acid-fast diagnosing mast cell disease at this site. bacilli were negative, urinary histamine excretion varied from 1190 to 5230,ug/24 h (normal less than 2000), a 15 g histidine load was handled normally Received for publication 9 Jtily with no excess of histamine in the urine, urinary 918
2 Involvement of the small intestine in systemic mast cell disease 5-HIAA excretion was normal both in between (19,mol/24 h) and during (29,umol/24 h) attacks of pain, an oral load of 5-HT was handled normally with an expected increase in urinary 5-HIAA, urinary heparinoids were increased to 36 and 40 units/hour (normal 13-29), skin biopsy showed no excess of mast cells, bone marrow examination showed no mast cells or acid-fast bacilli, a small bowel enema showed fine and coarse nodules in the mucosa. At a further laparotomy the bowel appeared normal but there were five enlarged glands at the root of the jejunal mesentery, one of which, after excision, was found to contain creamy pus. Operative small bowel biopsy showed partial villous atrophy and 30 mast cells/high-power field of the lamina propria (mean of 20 HPF). Liver histology was normal and no mast cells were seen. The lymph nodes showed irregular areas of necrosis containing much leucocyte debris. A zone of macrophages, lymphocytes Fig. 1 Abdominal lymph node showing leucocyte debris (top right) in centre ofgranuloma. No microorganisms were demonstrable either histologically or on culture. x and plasma cells surrounded the necrotic areas, and occasional multinucleate macrophages were seen (Fig. 1).No bacteria were demonstrated inthelesions, either by Gram staining or by the Ziehl-Neelsen technique, and stains for fungi were negative. She was given one year's antituberculous therapy with streptomycin and Pasinah D. Although she gained weight, she continued to complain of recurrent abdominal pain and distension and further investigation was undertaken. Malabsorption persisted: faecal fat 53 mmol/24 h, the glucose tolerance curve was flat, the lactose tolerance curve was flat, xylose absorption was impaired. A 15 % eosinophilia had developed but this disappeared after antituberculous therapy was stopped. A 16-day trial of 40 mg prednisone daily effected no improvement. A gluten-free diet was tried but was found disagreeable and was stopped after three weeks. She was then discharged home taking propantheline, antihistamines and analgesics and she became chronically constipated. Further investigation at a fourth hospital three years after the first laparotomy showed persistent malabsorption (faecal fat 42 mmol/24 h). The Mantoux test was negative at 1/1000 PPD tuberculin. A significant disturbance of colonic motility was found and selfadministered intramuscular hyoscine was advised with good effect. Attacks of abdominal pain continued and nine years after the first laparotomy she developed recurrent severe abdominal pain requiring regular pethidine and was readmitted to a fifth hospital. Steatorrhoea had diminished to 25 mmol/24 h. It was considered that social and emotional problems were largely responsible for her symptoms. FINAL INVESTIGATIONS A few months later she was referred to this department. She was taking the following drugs: diazepam, imipramine, sodium amytal, hyoscine, Dorbanex and Doloxene. She looked well and abdominal examination showed no significant abnormality. The results of investigations were as follows (normal values in parentheses): Haematology Hb 11.5 g/dl, white cell count 8100 per cmm with a normal differential count, a blood film showed mild macrocytosis and slight hypochromia, the ESR was 50 mm in one hour, serum iron 11,gmol/l (11-33), iron-binding capacity 65,umol/l (54-80), serum folate 0.8,ug/l ( ), red cell folate 153,tg/l ( ), serum B ng/l (> 110), prothrombin time 12 s (control 12 s). Biochemistry Serum albumin 44 g/l (37-49), serum calcium 2-31
3 920 mmol/l ( ), serum alkaline phosphatase 8.7 KA units (413), plasma carotene 1-93,umol/l (> 0.74). Tests of Absorption Glucose tolerance test (blood glucese levels before and at 30-min intervals following 50 g oral glucose) 4.4, 4 7, 6.1, 4.4, 5.5 mmol/l; 60% of a 5g dose of xylose was excreted in the urine in five hours (> 23%); Schilling test with intrinsic factor, 5.6% of oral 58Co vitamin B12 appeared in the urine in 24 h (> 12%); urinary indican 0.41 mmol/24 h (< 0.47); two-day faecal fat 25 mmol/24 h (< 18); dietary fat 100 g/24 h. Small bowel biopsy With the peroral hydraulic instrument (Flick et al., 1961) three biopsies each were taken from the second part of the duodenum, 5 cm past the duodenojejunal junction, and 20 cm past the duodenojejunal junction. All showed a flat mucosa on dissecting microscopy and all showed subtotal villous atrophy on histology (Fig. 2). The surface epithelium was cuboidal with haphazardly situated nuclei and increased interepithelial lymphocytes. There were two eosinophils/hpf of the lamina propria (mean of 20 HPF). Toluidine blue staining showed 30mastcells/HPF (mean of 20HPF) (Fig. 3). Brian B. Scott, G. J. Hardy, and M. S. Losowsky Fig. 2 Jejunal biopsy taken just before treatment with a gluten-free diet from 20 cm past the duodenojejunal junction showing subtotal villous atrophy and disorganized surface epithelium. x 30. Immunology HL-A type-hl-al, HL-A8, W18; immunoglobulins IgG g/l ( ), IgA 2-74 g/1 (0.9-45), IgM 1.56 g/l ( ), serum gluten antibodies by tanned red cell test 1/1028, milk antibodies 1/256; no serum autoantibodies were detected by the indirect tissue immunofluorescent technique; the Mantoux test was negative at 1/1000 PPD tuberculin. Radiology A chest radiograph was normal as was a skeletal survey. She was treated only with a gluten-free diet and within two weeks she reported symptomatic improvement. After three months, small bowel biopsies, taken from the same sites as,previously, showed a marked improvement with partial villous atrophy and regular, columnar epithelial cells (Fig. 4), the improvement being most marked in the distal specimens. The mast cell content, however, had not altered, there being 30 per HPF (mean of 90 HPF in nine biopsies). Criteria for Small Intestinal Mast Cell Disease Normal human skin contains 1-2 mast cells per HPF (Kallman, 1960; Lese, 1962) which may be increased up to threefold in chronic inflammatory states (Lese, 1962). The finding of more than 6 mast cells per HPF should strongly suggest mast cell disease at that site (Sagher and Even-Paz, 1967). There is less information about other organs but Norris et al. (1963) in a necropsy study of the
4 Involvement of the small intestine in systemic mast cell disease gastrointestinal tract of a 30 year old negress dying of active rheumatic heart disease showed that mast cell numbers varied both according to the level and the layer. In the jejunum there were Fig. 3 Lamina propria ofjejunal mucosa stained with toluidine blue. Mast cells are indicated by arrows. x mast cells per HPF of the mucosa, 4.5 per HPF of the submucosa, 2.5 per HPF of the muscularis mucosae, and 2 per HPF of serosa. We have studied p_roral biopsies ofjejunum from Jejunal biopsy taken after three months' treatment with a <is~ gluten-free diet from 20 cm past the duodenojejunal junction s*i showing partial villous atrophya definite improvement (cf Fig. 2) x 30. W bfig 921
5 922 Brian B. Scott, G. J. Hardy, and M. S. Losowsky Diagnosis Age Sex Biopsy Appearance' Mast Cells per HPF' No. of HPF Counted Coeliac disease (normal diet) 41 F SVA Coeliac disease (normal diet) 30 F SVA Coeliac disease (normal diet) 39 M PVA Coeliac disease (normal diet) 35 F SVA Coeliac disease (normal diet) 35 F SVA Coeliac disease (normal diet) 39 F SVA Coeliac disease (normal diet) 62 F SVA Coeliac disease (normal diet) 33 M SVA Coeliac disease (normal diet) 19 F SVA Coeliac disease (normal diet) 36 F SVA Coeliac disease (normal diet) 17 F SVA Mean Irritable colon syndrome 32 F N Irritable colon syndrome 46 M N Irritable colon syndrome 41 F N Irritable colon syndrome 38 M N Irritable colon syndrome 49 F N Irritable colon syndrome 52 F N Irritable colon syndrome 52 F N Irritable colon syndrome 50 F N Irritable colon syndrome 15 F N Unexplained anaemia 55 F N Mean Table 1 Numbers of mast cells per HPF of lamina propria in peroraljejunal biopsies 5SVA = subtotal villous atrophy, N = normal, PVA = partial villous atrophy. 'One HPF = approximately 0-2 mn_3. 11 patients with untreated coeliac disease and 10 controls without evidence of small bowel disease. The numbers of mast cells in the lamina propria are shown in Table 1. The average number of mast cells in both groups was 2 per HPF. Thus by analogy with the findings in the skin we would tentatively suggest that the demonstration of more than 6 mast cells per HPF in the lamina propria of jejunal biopsies is suggestive of mast cell disease. Discussion PRESENT CASE The following features all support a diagnosis of mast cell disease in this patient: (1) histaminuria, (2) typical flushing attacks, (3) recurrent gastrointestinal symptoms, (4) typical barium contrast radiological appearance of the small intestine, (5) increased urinary heparinoids, and (6) increased mast cells in the small bowel mucosa. Against this diagnosis is the absence of skin involvement, which, although extremely rare, has been described in mast cell disease. In addition, there was subtotal villous atrophy of the small bowel mucosa and surface epithelial changes typical of coeliac disease with improvement following treatment with a gluten-free diet, thus establishing a diagnosis of coeliac disease. Other features of coeliac disease were raised levels of gluten antibodies (Taylor et al., 1964) and the presence of HL-A8 (Falchuck et al., 1972; Stokes et al., 1973). The nature of the granulomatous condition of the abdominal lymph node is not clear.if this were active tuberculosis, one would expect detection of the tubercle bacillus either on microscopy or culture. A positive Mantoux test would also be expected although intestinal tuberculosis with a negative test has been reported (Fung et al., 1970). Even if it were tuberculosis, it would appear not to have contributed significantly to the clinical picture since symptoms and biochemical abnormalities continued unchanged during and after antituberculous therapy. Furthermore, tuberculosis may have arisen secondary to intestinal disease since similar patients have depressed cell-mediated immunity and negative Mantoux tests (Scott and Losowsky, 1974). REPORTED CASES OF SMALL INTESTINAL MAST CELL DISEASE Jarnum and Zachariae (1967) and Clemett et al. (case III, 1968) each described a single patient with mast cell disease, mast cell infiltration in the lamina propria of the small bowel, and normal villi. Three patients with mast cell disease and partial villous atrophy are described, one had a 'large' increase in mast cells (Clemett et al., 1968, case I), another (Bank and Marks, 1963), in whom mast cells did not appear excessive, had an eosinophilic infiltration which is a feature suggestive of mast cell infiltration (Sagher and Even-Paz, 1967); and the third (Goldgraber, 1963) had an increase of round cells in the lamina propria, which were thought to be mast
6 Involvement of the small intestine in systemic mast cell disease cells. Rubin and Dobbins (1965) reported a patient with subtotal villous atrophy of the small bowel but no increase in mast cells and Broitman et al. (1970) reported a patient (also reported by Fitzpatrick, 1961; Janower, 1962; Clemett et al., 1968) with subtotal villous atrophy but no increase in mast cells although eosinophils were increased and increased mast cells had been previously demonstrated in the submucosa. Interestingly, both patients responded clinically and histologically to a glutenfree diet and must therefore be considered to have coeliac disease. Furthermore, there is another patient who probably also had systemic mast cell disease and coeliac disease (Lees and Stroud, 1959) although histological details were not given. All of the above patients were said to have typical urticaria pigmentosa except the patient of Rubin and Dobbins (1965) in whom this is presumed. RELATIONSHIP TO COELIAC DISEASE The association of coeliac disease with mast cell disease, now reported in four patients, would seem to be more than fortuitous. Moreover it is possible that three additional patients (Bank and Marks, 1963; Goldgraber, 1963; Clemett et al., 1968, case I) also had coeliac disease since they had partial villous atrophy but without demonstrated responses to a gluten-free diet. The possiblity that mast cell infiltration is a result of gluten sensitivity is unlikely in view of (1) the mast cell content not altering after treatment with a gluten-free diet and (2) the absence of mucosal mast cell infiltration in patients with untreated, uncomplicated coeliac disease. The other possibility, that mast cell infiltration predisposes to gluten sensitivity, cannot be refuted in the present state of knowledge, but immunological mechanisms are almost certainly involved in the mucosal damage of coeliac disease and mast cells have a role in some immunological reactions, especially type I reactions involving IgE. It is of interest that Shiner (1973) has demonstrated a 'slight to moderate' infiltration of mast cells after gluten challenge in coeliac children and after milk challenge in a child with cow's milk allergy (Shiner et al., 1975). Other mechanisms must, however, also operate in view of (1) patients with mucosal mast cell infiltration and normal villi (Jarnum and Zachariae, 1967; Clemett et al., 1968, case III) and (2) patients with subtotal villous atrophy but no demonstrated increase in mast cells at that site (Rubin and Dobbins, 1965; Broitman et al., 1970). RADIOLOGY A characteristic barium contrast radiological appearance of the small bowel in systemic mast cell disease has been described (Janower, 1962; Remy, 1962; Clemett et al., 1968; Jarnum and Zachariae, 1967). This consists of diffuse thickening of the bowel wall and multiple nodular filling defects similar to the appearance of nodular lymphoid hyperplasia. It is not clear whether the nodules represent mast cell infiltrates or 'urticaria' of the small bowel mucosa. MALABSORPTION AND MAST CELL DISEASE Malabsorption in mast cell disease might arise from either mucosal infiltration by mast cells, coincidental coeliac disease, or from the disturbance of gastrointestinal motility produced by histamine or other chemicals released from mast cells. Although diarrhoea and other abdominal complaints are common in all forms of mast cell disease, malabsorption has been documented in only seven patients (Table 2). There are other patients described with diarrhoea suggestive of malabsorption (Ellis, 1949; Asboe- Hansen, 1960) but without adequate documentation. PROGNOSIS AND TREATMENT The effect of small intestinal involvement on the prognosis of mast cell disease is not clear in view of the paucity of recorded cases. However, systemic Author Fat Balance (g/24 hr) Xylosel Test GTT' Schilling' Test (%) Pancreatic Function Test Intake Excretion Havard and Scott (1959) Bank and Marks (1963) Goldgraber (1963) Holti (1964) Jamum and Zachariae (1967) Clemett et al. (case III) (1968) Broitman et al. (1970) Table Increased 40 9% N 28 % (N) 6-4% Reported cases of mast cell disease and malabsorption "Percentage of 25 g oral xylose appearing in urine in five hours. 'Glucose tolerance test. 'Percentage of oral labelled B1, appearing in urine in 48 hours. Flat 2 Flat Flat 9.9 (N) 1-4 Normal Normal 923
7 924 Brian B. Scott, G. J. Hardy, and M. S. Losowsky mast cell disease generally may spontaneously improve, although one-third of patients proceed to a fatal termination, commonly from leukaemia but also from the complications of peptic ulcer or liver involvement. Treatment is aimed at reducing the amount of histamine produced by mast cells. Antihistamines (Sagher and Even-Paz, 1967), histidine decarboxylase inhibitors (Levine, 1960), and oral sodium cromoglycate (Dolovich reported by Kingsley, 1974) may all be effective. Steroids are occasionally beneficial but unsatisfactory results have been recorded by a number of authors (Sagher and Even-Paz, 1967). Avoidance of stimuli to mast cell histamine release should be advised-for example, codeine, aspirin, alcohol, allergens, extremes of heat and cold, trauma and radiation. References Asboe-Hansen, G. (1960). Urticaria pigmentosa with generalized tissue mastocytosis and blood basophilia. Archives of Dermatology, 81, Bank, S., and Marks, I. N. (1963). Malabsorption in systemic mast cell disease. Gastroenterology, 45, Broitman, S. A., McCray, R. S., May, J. C., Deren, J. J., Ackroyd, F., Gottlieb, L. S., McDermott, W., and Zamcheck, N. (1970). Mastocytosis and intestinal malabsorption. American Journal of Medicine, 48, Clemett, A. R., Fishbone, G., Levine, R. J., James, A. E., and Janower, M. (1968). Gastrointestinal lesions in mastocytosis. American Journal of Roentgenology, 103, Ellis, J. M. (1949). Urticaria pigmentosa. Archives of Pathology, 48, Fitzpatrick, T. B. (1961). Urticaria pigmentosa with smallbowel involvement. Archives of Dermatology, 83, 515. Falchuck, Z. M., Rogentine, G. N., and Strober, W. (1972). Predominance of histocompatibility antigen HL-A8 in patients with gluten-sensitive enteropathy. Journal of Clinical Investigation, 51, Flick, A. L., Quinton, W. E., and Rubin, C. E. (1961). A peroral hydraulic biopsy tube for multiple sampling at any level of the gastrointestinal tract. Gastroenterology, 40, Fung, W. P., Tan, K. K., Yu, S. F., and Kho, K. M. (1970). Malabsorption and subtotal villous atrophy secondary to pulmonary and intestinal tuberculosis. Gut, 11, Gonnella, J. S., and Lipsey, A. I. (1964). Mastocytosis manifested by hepatosplenomegaly. New England Journal of Medicine,.271, Goldgraber, M. B. (1963). Steatorrhoea: a clinical-pathologic correlation. Israel Medical Journal, 22, Havard, C. W. H., and Scott, R. B. (1959). Urticaria pigmentosa with visceral and skeletal lesions. Quarterly Journal of Medicine, 28, Holti, G. (1964). Reported by Sagher, F., and Even-Paz, Z. (1967). Mastocytosis and the Mast Cell. Karger, Basel. Janower, M. L. (1962). Mastocytosis of the gastrointestinal tract. Acta Radiologica (Stockholm), 57, Jarnum, S., and Zachariae, H. (1967). Mastocytosis (urticaria pigmentosa) of skin, stomach, and gut with malabsorption. Gut, 8, Kallman, S. (1960). In Discussion by J. Meyers. Urticaria pigmentosa. Archives of Dermatology, 81, Kingsley, P. J. (1974). Oral sodium cromoglycate in gastrointestinal allergy. Lancet, 2, Lees, M. H., and Stroud, C. E. (1959). Bone lesions of urticaria pigmentosa in childhood. Archives of Diseases in Childhood, 34, Lese, L. (1962). Urticaria pigmentosa. Archives of Dermatology, 85, Levine, R. J. (1966). Histamine synthesis in man: inhibition by 4-bromo-3-hydroxybenzyloxyamine. Science, 154, Mutter, R. D., Tannenbaum, M., and Ultmann, J. E. (1963). Systemic mast cell disease. Annals of Internal Medicine, 59, Norris, H. T., Zamcheck, N., and Gottlieb, L. S. (1963). The presence and distribution of mast cells in the human gastrointestinal tract at autopsy. Gastroenterology, 44, Remy, D. (1962). Gewebsmastzellen und Mastzellen- Reticulose. Ergebnesse der Innerin Medizin und Kunderheilkunde, 17, Rubin, C. E., and Dobbins, W. 0. (1965). Peroral biopsy of the small intestine-a review of its diagnostic usefulness. Gastroenterology, 49, Sagher, F., and Even-Paz, Z. (1967). Mastocytosis and the Mast Cell. Karger: Basel. Scott, B. B., and Losowsky, M. S. (1974). Evidence suggesting depression of cell mediated immunity in coeliac disease. In Coeliac Disease, pp Edited by W. Th. J. M. Hekkens and A. S. Pefia, Stenfert Kroese: Leiden. Shiner, M. (1973). Ultrastructural changes suggestive of immune reactions in the jejunal, mucosa of coeliac children following gluten challenge. Gut, 14, Shiner, M., Ballard, J., and Smith, M. E. (1975). The smallintestinal mucosa in cow's milk allergy. Lancet, 1, Stokes, P. L., Asquith, P., Holmnes, G. K. T., Mackintosh, P., and Cooke, W. T. (1973). Inheritance and influence of histocompatibility (HL-A) antigen in adult coeliacs disease. Gut, 14, Taylor, K. B., Truelove, S. C., and Wright, R. (1964). Serologic reactions to gluten and cow's milk proteins in gastrointestinal disease. Gastroenterology, 46,
ranged from two months to 21 years (mean 5% years)
 Gut, 1978, 19, 754-758 Response of the skin in dermatitis herpetiformis to a gluten free diet, with reference to jejunal morphology B. T. COOPER, E. MALLAS, M. D. TROTTER, AND W. T. COOKE From the Nutritional
Gut, 1978, 19, 754-758 Response of the skin in dermatitis herpetiformis to a gluten free diet, with reference to jejunal morphology B. T. COOPER, E. MALLAS, M. D. TROTTER, AND W. T. COOKE From the Nutritional
Coeliac disease with mild mucosal abnormalities: a report of four patients
 Postgraduate Medical Journal (March 1977) 53, 134-138. Coeliac disease with mild mucosal abnormalities: a report of four patients BRIAN B. SCOTT M. S. LOSOWSKY M.D., M.R.C.P. M.D., F.R.C.P. University
Postgraduate Medical Journal (March 1977) 53, 134-138. Coeliac disease with mild mucosal abnormalities: a report of four patients BRIAN B. SCOTT M. S. LOSOWSKY M.D., M.R.C.P. M.D., F.R.C.P. University
coeliac syndrome per day. Investigations showed a megaloblastic anaemia showed a flat mucosa. ileum were resected and he made an uninterrupted
 Gut, 1965, 6, 466 Post-mortem examination of a small intestine in the coeliac syndrome B. CREAMER AND P. LEPPARD From the Gastro-Intestinal Laboratory, St Thomas's Hospital, London EDITORIAL SYNOPSIS This
Gut, 1965, 6, 466 Post-mortem examination of a small intestine in the coeliac syndrome B. CREAMER AND P. LEPPARD From the Gastro-Intestinal Laboratory, St Thomas's Hospital, London EDITORIAL SYNOPSIS This
Reintroduction of gluten in adults and children with treated coeliac disease
 Reintroduction of gluten in adults and children with treated coeliac disease PARVEEN J. KUMAR, D. P. O'DONOGHUE, KATHY STENSON, AND A. M. DAWSON From the Department of Gastroenterology, St. Bartholomew's
Reintroduction of gluten in adults and children with treated coeliac disease PARVEEN J. KUMAR, D. P. O'DONOGHUE, KATHY STENSON, AND A. M. DAWSON From the Department of Gastroenterology, St. Bartholomew's
HDF Case Whipple s disease
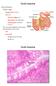
 HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
above 110 g per 100 ml in four patients, but the
 J. clin. Path., 1971, 24, 244-249 Diagnostic value of the serum folate assay J. FORSHAW AND LILIAN HARWOOD From the Haematology Laboratory, Sefton General Hospital, Liverpool SYNOPSIS The diagnostic value
J. clin. Path., 1971, 24, 244-249 Diagnostic value of the serum folate assay J. FORSHAW AND LILIAN HARWOOD From the Haematology Laboratory, Sefton General Hospital, Liverpool SYNOPSIS The diagnostic value
Confirming persistence of gluten intolerance in
 Archives of Disease in Childhood, 1975, 50, 259. Confirming persistence of gluten intolerance in children diagnosed as having coeliac disease in infancy Usefulness of onehour blood xylose test C. J. ROLLES,
Archives of Disease in Childhood, 1975, 50, 259. Confirming persistence of gluten intolerance in children diagnosed as having coeliac disease in infancy Usefulness of onehour blood xylose test C. J. ROLLES,
Adult coeliac disease
 Postgrad. med. J. (August 1968) 44, 632-640. PATENTS with idiopathic steatorrhoea present in many different ways. The dominant feature of the clinical presentation in 100 patients is shown in Table 1.
Postgrad. med. J. (August 1968) 44, 632-640. PATENTS with idiopathic steatorrhoea present in many different ways. The dominant feature of the clinical presentation in 100 patients is shown in Table 1.
Dissecting Microscope Appearance of
 Arch. Dis. Childh., 1967, 42, 626. Dissecting Microscope Appearance of Small Bowel Mucosa in Children JOHN WALKER-SMITH From Professorial Unit, Royal Alexandra Hospital for Children, Camperdown, Sydney,
Arch. Dis. Childh., 1967, 42, 626. Dissecting Microscope Appearance of Small Bowel Mucosa in Children JOHN WALKER-SMITH From Professorial Unit, Royal Alexandra Hospital for Children, Camperdown, Sydney,
The cell population of the upper jejunal mucosa in tropical sprue and postinfective malabsorption
 Gut, 1974, 15, 387-391 The cell population of the upper jejunal mucosa in tropical sprue and postinfective malabsorption R. D. MONTGOMRY AND A. C. I. SHARR From the Metabolic Unit, ast Birmingham Hospital,
Gut, 1974, 15, 387-391 The cell population of the upper jejunal mucosa in tropical sprue and postinfective malabsorption R. D. MONTGOMRY AND A. C. I. SHARR From the Metabolic Unit, ast Birmingham Hospital,
CHRONIC ULCERATIVE JEJUNITIS
 GASTROENTEROLOGY Copyright " 1971 by The Williams & Wilkins Co. Vol. 60, No. 1 Printed in U. S. A. CHRONIC ULCERATIVE JEJUNITIS Report of a case and discussion of classification MORDEKHAI MORITZ, M.D.,
GASTROENTEROLOGY Copyright " 1971 by The Williams & Wilkins Co. Vol. 60, No. 1 Printed in U. S. A. CHRONIC ULCERATIVE JEJUNITIS Report of a case and discussion of classification MORDEKHAI MORITZ, M.D.,
Coeliac disease with severe hypogammaglobulinaemia
 Gut, 1981, 22, 153-157 Case report Coeliac disease with severe hypogammaglobulinaemia A D B WEBSTER, G SLAVIN, M SHINER, T A E PLATTS-MILLS, AND G L ASHERSON From the Divisions of Immunological Medicine
Gut, 1981, 22, 153-157 Case report Coeliac disease with severe hypogammaglobulinaemia A D B WEBSTER, G SLAVIN, M SHINER, T A E PLATTS-MILLS, AND G L ASHERSON From the Divisions of Immunological Medicine
relation to coeliac disease
 Gut, 1983, 24, 565-574 Case reports Small intestinal ulceration: diagnostic difficulties in relation to coeliac disease D A F ROBERTSON, M F DIXON, B B SCOTT, F G SIMPSON, AND M S LOSOWSKY From the Department
Gut, 1983, 24, 565-574 Case reports Small intestinal ulceration: diagnostic difficulties in relation to coeliac disease D A F ROBERTSON, M F DIXON, B B SCOTT, F G SIMPSON, AND M S LOSOWSKY From the Department
Coeliac disease in Sudanese children
 Coeliac disease in Sudanese children G. I. SULIMAN1 Gut, 1978, 19, 121-125 From the Department ofpaediatrics and Child Health, Khartoum Civil Hospital, Khartoum, Sudan SUMMARY Coeliac disease has not hitherto
Coeliac disease in Sudanese children G. I. SULIMAN1 Gut, 1978, 19, 121-125 From the Department ofpaediatrics and Child Health, Khartoum Civil Hospital, Khartoum, Sudan SUMMARY Coeliac disease has not hitherto
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE SCOPE. Coeliac disease: recognition, assessment and management of coeliac disease
 Appendix B: NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Coeliac disease: recognition, assessment and management of coeliac disease 1.1 Short title Coeliac disease 2 The remit
Appendix B: NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Coeliac disease: recognition, assessment and management of coeliac disease 1.1 Short title Coeliac disease 2 The remit
Studies of intestinal fermentation in ulcerative
 Gut, 1968, 9, 51-56 Studies of intestinal fermentation in ulcerative colitis R. D. MONTGOMERY, A. C. FRAZER, CATHRYN HOOD, J. M. GOODHART, M. R. HOLLAND, AND R. SCHNEIDER From the Metabolic Unit, East
Gut, 1968, 9, 51-56 Studies of intestinal fermentation in ulcerative colitis R. D. MONTGOMERY, A. C. FRAZER, CATHRYN HOOD, J. M. GOODHART, M. R. HOLLAND, AND R. SCHNEIDER From the Metabolic Unit, East
Quantitation of intraepithelial lymphocytes
 Gut, 1971, 12, 988-994 Quantitation of intraepithelial lymphocytes inhuman jejunum ANNE FERGUSON AND D. MURRAY From the University Departments ofbacteriology and Immunology (Western Infirmary) and Pathology
Gut, 1971, 12, 988-994 Quantitation of intraepithelial lymphocytes inhuman jejunum ANNE FERGUSON AND D. MURRAY From the University Departments ofbacteriology and Immunology (Western Infirmary) and Pathology
Malignant histiocytosis of the intestine: the early histological lesion
 Gut, 1980, 21, 381-386 Malignant histiocytosis of the intestine: the early histological lesion P ISAACSON From the Department of Pathology, Faculty of Medicine, Southampton University Hospital, Southampton
Gut, 1980, 21, 381-386 Malignant histiocytosis of the intestine: the early histological lesion P ISAACSON From the Department of Pathology, Faculty of Medicine, Southampton University Hospital, Southampton
CLINICAL REVIEW. and small bowel carcinoma SIMON KENWRIGHT* M.R.C.P.
 Postgraduate Medical Journal (November 1972) 48, 673-677. Coeliac disease CLINICAL REVIEW and small bowel carcinoma SIMON KENWRIGHT* M.R.C.P. Department of Gastro-enterology, Frenchay Hospital, Bristol
Postgraduate Medical Journal (November 1972) 48, 673-677. Coeliac disease CLINICAL REVIEW and small bowel carcinoma SIMON KENWRIGHT* M.R.C.P. Department of Gastro-enterology, Frenchay Hospital, Bristol
A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue
 A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue UCSF Liver and Gastrointestinal Pathology Update Sept. 4, 2009 How to Go Wrong When Evaluating Small Bowel Biopsies, Based on
A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue UCSF Liver and Gastrointestinal Pathology Update Sept. 4, 2009 How to Go Wrong When Evaluating Small Bowel Biopsies, Based on
Lactose Intolerance in Childhood Coeliac Disease
 Arch. Dis. Childh., 1968, 43, 433. Lactose Intolerance in Childhood Coeliac Disease Assessment of its Incidence and Importance ALEXANDER S. McNEISH and ELIZABETH M. SWEET From the Royal Hospital for Sick
Arch. Dis. Childh., 1968, 43, 433. Lactose Intolerance in Childhood Coeliac Disease Assessment of its Incidence and Importance ALEXANDER S. McNEISH and ELIZABETH M. SWEET From the Royal Hospital for Sick
DIGESTIVE TRACT ESOPHAGUS
 DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
In-situ and invasive carcinoma of the colon in patients with ulcerative colitis
 Gut, 1972, 13, 566-570 In-situ and invasive carcinoma of the colon in patients with ulcerative colitis D. J. EVANS AND D. J. POLLOCK From the Departments of Pathology, Royal Postgraduate Medical School
Gut, 1972, 13, 566-570 In-situ and invasive carcinoma of the colon in patients with ulcerative colitis D. J. EVANS AND D. J. POLLOCK From the Departments of Pathology, Royal Postgraduate Medical School
Small intestinal mucosal patterns of coeliac disease and idiopathic steatorrhoea seen in other situations
 Gut, 1964, 5, 51 Small intestinal mucosal patterns of coeliac disease and idiopathic steatorrhoea seen in other situations R. R. W. TOWNLEY, M. H. CASS, AND CHARLOTTE M. ANDERSON From the Gastroenterological
Gut, 1964, 5, 51 Small intestinal mucosal patterns of coeliac disease and idiopathic steatorrhoea seen in other situations R. R. W. TOWNLEY, M. H. CASS, AND CHARLOTTE M. ANDERSON From the Gastroenterological
Malignancy in relatives of patients with coeliac disease
 Brit. J. prev. soc. Med. (1976), 30, 17-21 Malignancy in relatives of patients with coeliac disease P. L. STOKES, PATRICIA PRIOR, T. M. SORAHAN, R. J. McWALTER* J. A. H. WATERHOUSE, AND W. T. COOKE The
Brit. J. prev. soc. Med. (1976), 30, 17-21 Malignancy in relatives of patients with coeliac disease P. L. STOKES, PATRICIA PRIOR, T. M. SORAHAN, R. J. McWALTER* J. A. H. WATERHOUSE, AND W. T. COOKE The
These studies were made at a time when it was not. yet fully established that mast cells could react with
 Gut, 1975, 16, 861-866 Mast cells and immunoglobulin E in inflammatory bowel disease G. LLOYD1, F. H. Y. GREEN, H. FOX, V. MANI2, AND L. A. TURNBERG2 From the Department ofpathology, University of Manchester,
Gut, 1975, 16, 861-866 Mast cells and immunoglobulin E in inflammatory bowel disease G. LLOYD1, F. H. Y. GREEN, H. FOX, V. MANI2, AND L. A. TURNBERG2 From the Department ofpathology, University of Manchester,
 SUMMARY Coeliac disease is a common food intolerance in Western populations, in which it has a prevalence of about 1%. In early infancy, when the transition is made to a gluten-containing diet (particularly
SUMMARY Coeliac disease is a common food intolerance in Western populations, in which it has a prevalence of about 1%. In early infancy, when the transition is made to a gluten-containing diet (particularly
General Structure of Digestive Tract
 Dr. Nabil Khouri General Structure of Digestive Tract Common Characteristics: Hollow tube composed of a lumen whose diameter varies. Surrounded by a wall made up of 4 principal layers: Mucosa Epithelial
Dr. Nabil Khouri General Structure of Digestive Tract Common Characteristics: Hollow tube composed of a lumen whose diameter varies. Surrounded by a wall made up of 4 principal layers: Mucosa Epithelial
FBC interpretation. Dr. Gergely Varga
 FBC interpretation Dr. Gergely Varga #1 71 Y/O female, c/o weakness Test Undertaken : FBC (FBC) Sample Type: Whole Blood [ - 26.09.11 14:59] Hb 7.3 g/dl* 12.0-15.5 RBC 3.5 10^12/l * 3.80-5.60 Hct 0.24
FBC interpretation Dr. Gergely Varga #1 71 Y/O female, c/o weakness Test Undertaken : FBC (FBC) Sample Type: Whole Blood [ - 26.09.11 14:59] Hb 7.3 g/dl* 12.0-15.5 RBC 3.5 10^12/l * 3.80-5.60 Hct 0.24
Partial villous atrophy in nutritional megaloblastic
 J. clin Path., 1971, 24, 131-135 Partial villous atrophy in nutritional megaloblastic anaemia corrected by folic acid therapy D. W. DAWSON From Crumpsall Hospital, Manchester SYNOPSIS A patient with megaloblastic
J. clin Path., 1971, 24, 131-135 Partial villous atrophy in nutritional megaloblastic anaemia corrected by folic acid therapy D. W. DAWSON From Crumpsall Hospital, Manchester SYNOPSIS A patient with megaloblastic
MELKERSSON-ROSENTHAL SYNDROME AND CROHN S DISEASE
 British Journal of Oral Surgery (1980) 18, 254-258 @ The British Association of Oral Surgeons OOO7-117X/80/00370254$02.00 MELKERSSON-ROSENTHAL SYNDROME AND CROHN S DISEASE N. WORSAAE,~* K. C. CHRISTENSEN,2
British Journal of Oral Surgery (1980) 18, 254-258 @ The British Association of Oral Surgeons OOO7-117X/80/00370254$02.00 MELKERSSON-ROSENTHAL SYNDROME AND CROHN S DISEASE N. WORSAAE,~* K. C. CHRISTENSEN,2
Prevalence of lactase deficiency in British adults
 Prevalence of lactase deficiency in British adults Gut, 1984, 25, 163-167 ANNE FERGUSON, DOROTHY M MACDONALD, AND W GORDON BRYDON From the Gastro-Intestinal Unit, University of Edinburgh, and Western General
Prevalence of lactase deficiency in British adults Gut, 1984, 25, 163-167 ANNE FERGUSON, DOROTHY M MACDONALD, AND W GORDON BRYDON From the Gastro-Intestinal Unit, University of Edinburgh, and Western General
Anatomy & Histology of The Small intestine
 Anatomy & Histology of The Small intestine Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Jejunum Ileum Histology: Duodenum, jejunum, and ileum
Anatomy & Histology of The Small intestine Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Jejunum Ileum Histology: Duodenum, jejunum, and ileum
Intestinal reticulosis as a complication of idiopathic steatorrhoea
 Gut, 1962, 3, 232 Intestinal reticulosis as a complication of idiopathic steatorrhoea Fronm K. R. GOUGH, A. E. READ, AND J. M. NAISH the Department of Medicine, University of Bristol, and Frenchay Hospital,
Gut, 1962, 3, 232 Intestinal reticulosis as a complication of idiopathic steatorrhoea Fronm K. R. GOUGH, A. E. READ, AND J. M. NAISH the Department of Medicine, University of Bristol, and Frenchay Hospital,
Southern Derbyshire Shared Care Pathology Guidelines. Coeliac Disease
 Southern Derbyshire Shared Care Pathology Guidelines Coeliac Disease Purpose of Guideline When and how to investigate patients for Coeliac Disease What the results mean When and how to refer patients Monitoring
Southern Derbyshire Shared Care Pathology Guidelines Coeliac Disease Purpose of Guideline When and how to investigate patients for Coeliac Disease What the results mean When and how to refer patients Monitoring
Three-dimensional structure of the human small intestinal mucosa in health and disease
 Gut, 1969, 10, 6-12 Three-dimensional structure of the human small intestinal mucosa in health and disease C. A. LOEHRY AND B. CREAMER From the Gastrointestinal Laboratory, St Thomas' Hospital, London
Gut, 1969, 10, 6-12 Three-dimensional structure of the human small intestinal mucosa in health and disease C. A. LOEHRY AND B. CREAMER From the Gastrointestinal Laboratory, St Thomas' Hospital, London
Is a raised intraepithelial lymphocyte count with normal duodenal villous architecture clinically relevant?
 424 ORIGINAL ARTICLE Is a raised intraepithelial lymphocyte count with normal duodenal villous architecture clinically relevant? S Mahadeva, J I Wyatt, P D Howdle... See end of article for authors affiliations...
424 ORIGINAL ARTICLE Is a raised intraepithelial lymphocyte count with normal duodenal villous architecture clinically relevant? S Mahadeva, J I Wyatt, P D Howdle... See end of article for authors affiliations...
Alimentary Canal (I)
 Alimentary Canal (I) Esophagus and Stomach (Objectives) By the end of this lecture, the student should be able to discuss the microscopic structure in correlation with the function of the following organs:
Alimentary Canal (I) Esophagus and Stomach (Objectives) By the end of this lecture, the student should be able to discuss the microscopic structure in correlation with the function of the following organs:
Histopathology: gastritis and peptic ulceration
 Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
Giardiasis and coeliac disease
 Archives of Disease in Childhood, 1973, 48, 414. F. CARSWELL, A. A. M. GIBSON, and T. A. McALLISTER From the Departments of Child Health, Pathology and Bacteriology, Royal Hospital for Sick Children, Yorkhill,
Archives of Disease in Childhood, 1973, 48, 414. F. CARSWELL, A. A. M. GIBSON, and T. A. McALLISTER From the Departments of Child Health, Pathology and Bacteriology, Royal Hospital for Sick Children, Yorkhill,
Fibrin thrombi, a cause of clindamycin-associated
 Gut, 1976, 17, 483487 Fibrin thrombi, a cause of clindamycin-associated colitis? W. V. BOGOMOLETZ From the Department of Pathology, Queen Mary's Hospital, London summary Rectal biopsies from five patients
Gut, 1976, 17, 483487 Fibrin thrombi, a cause of clindamycin-associated colitis? W. V. BOGOMOLETZ From the Department of Pathology, Queen Mary's Hospital, London summary Rectal biopsies from five patients
ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK. Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center
 ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center 1 ST ADMISSION - 2015 38 y/o female Abdominal pain, diarrhea - intermittent
ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center 1 ST ADMISSION - 2015 38 y/o female Abdominal pain, diarrhea - intermittent
Kristin Kenrick, FRNZCGP Department of General Practice and Rural Health Dunedin School of Medicine (Supported by Coeliac New Zealand)
 Kristin Kenrick, FRNZCGP Department of General Practice and Rural Health Dunedin School of Medicine (Supported by Coeliac New Zealand) That you will go away thinking about your practice population, and
Kristin Kenrick, FRNZCGP Department of General Practice and Rural Health Dunedin School of Medicine (Supported by Coeliac New Zealand) That you will go away thinking about your practice population, and
HISTOLOGY. GIT Block 432 Histology Team. Lecture 1: Alimentary Canal (1) (Esophagus & Stomach) Done by: Ethar Alqarni Reviewed by: Ibrahim Alfuraih
 HISTOLOGY Lecture 1: Alimentary Canal (1) (Esophagus & Stomach) Done by: Ethar Alqarni Reviewed by: Ibrahim Alfuraih Color Guide: Black: Slides. Red: Important. Green: Doctor s notes. Blue: Explanation.
HISTOLOGY Lecture 1: Alimentary Canal (1) (Esophagus & Stomach) Done by: Ethar Alqarni Reviewed by: Ibrahim Alfuraih Color Guide: Black: Slides. Red: Important. Green: Doctor s notes. Blue: Explanation.
Chronic immune colitis in rabbits
 Chronic immune colitis in rabbits A. S. MEE, J. E. McLAUGHLIN, H. J. F. HODGSON, AND D. P. JEWELL Gut, 1979, 20, 1-5 From the Academic Department of Medicine and Department of Histopathology, Royal Free
Chronic immune colitis in rabbits A. S. MEE, J. E. McLAUGHLIN, H. J. F. HODGSON, AND D. P. JEWELL Gut, 1979, 20, 1-5 From the Academic Department of Medicine and Department of Histopathology, Royal Free
Malabsorption in rheumatoid disease
 Ann. rheum. Dis. (1971), 3, 626 Malabsorption in rheumatoid disease N. H. DYER, M. J. KENDALL, AND C. F. HAWKINS Queen Elizabeth Hospital, Birmingham 15 Rheumatoid disease is a systemic disorder involving
Ann. rheum. Dis. (1971), 3, 626 Malabsorption in rheumatoid disease N. H. DYER, M. J. KENDALL, AND C. F. HAWKINS Queen Elizabeth Hospital, Birmingham 15 Rheumatoid disease is a systemic disorder involving
Coeliac disease presenting with intestinal pseudoobstruction
 Case reports Coeliac disease presenting with intestinal pseudoobstruction D J DAWSON, C M SCIBERRAS, AND H WHITWELL Gut, 1984, 25, 1003-1008 From the University Departments of Gastroenterology and Histopathology,
Case reports Coeliac disease presenting with intestinal pseudoobstruction D J DAWSON, C M SCIBERRAS, AND H WHITWELL Gut, 1984, 25, 1003-1008 From the University Departments of Gastroenterology and Histopathology,
possible in the present state of our knowledge. history of frequent, loose bowel actions for two relapse on its reintroduction is also necessary for
 Gut, 1970, 11, 743-747 A case of small-intestinal mucosal atrophy R. E. BARRY, JOHN S. MORRIS, AND A. E. A. READ From the Department of Medicine, Bristol Royal Infirmary SUMMARY A patient is described
Gut, 1970, 11, 743-747 A case of small-intestinal mucosal atrophy R. E. BARRY, JOHN S. MORRIS, AND A. E. A. READ From the Department of Medicine, Bristol Royal Infirmary SUMMARY A patient is described
Coeliac disease with histological features of peptic duodenitis: Value of assessment of intraepithelial lymphocytes
 420 4 Clin Pathol 1993;46:420-424 Department of Pathology, St James's Hospital and Trinity College, Dublin Ireland M D Jeffers D O'B Hourihane Correspondence to: Professor D O'B Hourihane Accepted for
420 4 Clin Pathol 1993;46:420-424 Department of Pathology, St James's Hospital and Trinity College, Dublin Ireland M D Jeffers D O'B Hourihane Correspondence to: Professor D O'B Hourihane Accepted for
LYMPHOMA PRESENTING AS MALABSORPTION
 GASTROENTEROLOGY Copyright 1968 by The Williams & Wilkins Co. Vol. 54, No.3 Pnnted in U.S.A. LYMPHOMA PRESENTING AS MALABSORPTION HORACIO JINICH, M.D., EDMUNDO ROJAS, M.D., JOHN A. WEBB, M.D., AND JOHN
GASTROENTEROLOGY Copyright 1968 by The Williams & Wilkins Co. Vol. 54, No.3 Pnnted in U.S.A. LYMPHOMA PRESENTING AS MALABSORPTION HORACIO JINICH, M.D., EDMUNDO ROJAS, M.D., JOHN A. WEBB, M.D., AND JOHN
Coeliac Disease Bible Class Questions and Answers
 Coeliac Disease Bible Class Questions and Answers Jan Hendrik Niess What is the definition of coeliac disease? Coeliac disease is an immune reaction to gluten (wheat, barely, rye) in an genetic predisposed
Coeliac Disease Bible Class Questions and Answers Jan Hendrik Niess What is the definition of coeliac disease? Coeliac disease is an immune reaction to gluten (wheat, barely, rye) in an genetic predisposed
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT.
 PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
What is your diagnosis? a. Lymphocytic colitis. b. Collagenous colitis. c. Common variable immunodeficiency (CVID) associated colitis
 Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
ESIM: Winter School in Riga Case report
 ESIM: Winter School in Riga 2015 Case report Imanta Ozola Zālīte Pauls Stradins Clinical University Hospital Latvia 29.01.2015. January, 2006 32 y., man 2-3 weeks fatigue fluidal stool 2 times per day
ESIM: Winter School in Riga 2015 Case report Imanta Ozola Zālīte Pauls Stradins Clinical University Hospital Latvia 29.01.2015. January, 2006 32 y., man 2-3 weeks fatigue fluidal stool 2 times per day
Lower Gastrointestinal Tract KNH 406
 Lower Gastrointestinal Tract KNH 406 Lower GI Tract A&P Small Intestine Anatomy Duodenum, jejunum, ileum Maximum surface area for digestion and absorption Specialized enterocytes from stem cells of crypts
Lower Gastrointestinal Tract KNH 406 Lower GI Tract A&P Small Intestine Anatomy Duodenum, jejunum, ileum Maximum surface area for digestion and absorption Specialized enterocytes from stem cells of crypts
Nutritional assessments and diagnosis of digestive disorders
 Nutritional assessments and diagnosis of digestive disorders AASER ABDELAZIM Assistant professor of Medical Biochemistry Zagazig University, Egypt University of Bisha, KSA aaserabdelazim@yahoo.com 7 Mal
Nutritional assessments and diagnosis of digestive disorders AASER ABDELAZIM Assistant professor of Medical Biochemistry Zagazig University, Egypt University of Bisha, KSA aaserabdelazim@yahoo.com 7 Mal
THE D-XYLOSE EXCRETION TEST IN COELIAC DISEASE IN CHILDHOOD
 Arch. Dis. Childh., 1963, 38, 476. THE D-XYLOE EXCRETON TET N COELAC DEAE N CHLDHOOD BY DOUGLA HUBBLE and HELA LTTLEJOHN From the Department of Paediatrics and Child Health, the University of Birmingham
Arch. Dis. Childh., 1963, 38, 476. THE D-XYLOE EXCRETON TET N COELAC DEAE N CHLDHOOD BY DOUGLA HUBBLE and HELA LTTLEJOHN From the Department of Paediatrics and Child Health, the University of Birmingham
Case Report Eosinophilic Gastrointestinal Disorder in Coeliac Disease: ACaseReportandReview
 Case Reports in Gastrointestinal Medicine Volume 2012, Article ID 124275, 4 pages doi:10.1155/2012/124275 Case Report Eosinophilic Gastrointestinal Disorder in Coeliac Disease: ACaseReportandReview Dennis
Case Reports in Gastrointestinal Medicine Volume 2012, Article ID 124275, 4 pages doi:10.1155/2012/124275 Case Report Eosinophilic Gastrointestinal Disorder in Coeliac Disease: ACaseReportandReview Dennis
HYPOGAMMAGLOBULlNAEMIA WITH NODULAR LYMPHOID HYPERPLASIA OF THE SMALL INTESTINE
 J. roy. Army med. Cps. 1977. 123,37-41 HYPOGAMMAGLOBULlNAEMIA WITH NODULAR LYMPHOID HYPERPLASIA OF THE SMALL INTESTINE Major W. M. WALLACE, M.B., B.Ch., M.R.C. P., R.A.M.C. Royal Army Medical Col/ege.
J. roy. Army med. Cps. 1977. 123,37-41 HYPOGAMMAGLOBULlNAEMIA WITH NODULAR LYMPHOID HYPERPLASIA OF THE SMALL INTESTINE Major W. M. WALLACE, M.B., B.Ch., M.R.C. P., R.A.M.C. Royal Army Medical Col/ege.
Lymphatic System. Where s your immunity idol?
 Lymphatic System Where s your immunity idol? Functions of the Lymphatic System Fluid Balance Drains excess fluid from tissues Lymph contains solutes from plasma Fat Absorption Lymphatic system absorbs
Lymphatic System Where s your immunity idol? Functions of the Lymphatic System Fluid Balance Drains excess fluid from tissues Lymph contains solutes from plasma Fat Absorption Lymphatic system absorbs
Coeliac disease during the teenage period: The value
 Gut, 1974, 15, 450457 Coeliac disease during the teenage period: The value of serial serum folate estimations D. G. WEIR' AND D. O'B. HOURIHANE From the Departments of Clinical Medicine and Pathology,
Gut, 1974, 15, 450457 Coeliac disease during the teenage period: The value of serial serum folate estimations D. G. WEIR' AND D. O'B. HOURIHANE From the Departments of Clinical Medicine and Pathology,
manifestations are uncommon. Initial descriptions of the disease (Rosai and Dorfman, 1969) specifically
 Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
T of patients with malignant melanoma
 ~~ RADIOGRAPHIC: EVALUATION OF METASTATIC MELANOMA JACK E. MEYER, MD*+$ Malignant melanoma can potentially involve any organ system in the body once it metastasizes beyond the regional lymph nodes. A survey
~~ RADIOGRAPHIC: EVALUATION OF METASTATIC MELANOMA JACK E. MEYER, MD*+$ Malignant melanoma can potentially involve any organ system in the body once it metastasizes beyond the regional lymph nodes. A survey
Plan. Sarcoidosis 21/07/2017. Sarcoidosis Liver involvement. Sarcoidosis GI involvement. Sarcoidosis Diagnosis
 Belfast Pathology 2017 Gastrointestinal tract involvement by systemic disease 21.6.17 Dr Adrian C. Bateman University Hospital Southampton NHS Foundation Trust, UK Plan Dermatological conditions Chronic
Belfast Pathology 2017 Gastrointestinal tract involvement by systemic disease 21.6.17 Dr Adrian C. Bateman University Hospital Southampton NHS Foundation Trust, UK Plan Dermatological conditions Chronic
Splenic atrophy in adult coeliac disease:
 Gut, 1981, 22, 628-632 Splenic atrophy in adult coeliac disease: is it reversible? P N TREWBY, P M CHIPPING, S J PALMER, P D ROBERTS, S M LEWIS, AND J S STEWART From the Departments of Gastroenterology
Gut, 1981, 22, 628-632 Splenic atrophy in adult coeliac disease: is it reversible? P N TREWBY, P M CHIPPING, S J PALMER, P D ROBERTS, S M LEWIS, AND J S STEWART From the Departments of Gastroenterology
Small Intestinal Biopsy in a Patient with Crohn's Disease of the Duodenum
 GASTROENTEROLOGY 76:1009-1014, 1979 Small Intestinal Biopsy in a Patient with Crohn's Disease of the Duodenum The Spectrum of Abnormal Findings in the Absence of Granulomas MICHAEL D. SCHUFFLER and ROBERT
GASTROENTEROLOGY 76:1009-1014, 1979 Small Intestinal Biopsy in a Patient with Crohn's Disease of the Duodenum The Spectrum of Abnormal Findings in the Absence of Granulomas MICHAEL D. SCHUFFLER and ROBERT
Biomarkers of GI tract diseases. By Dr. Gouse Mohiddin Shaik
 By Dr. Gouse Mohiddin Shaik Introduction The gastrointestinal (GI) tract is a complex system performing multiple biological functions which are anatomically distributed Site for food processing and absorption
By Dr. Gouse Mohiddin Shaik Introduction The gastrointestinal (GI) tract is a complex system performing multiple biological functions which are anatomically distributed Site for food processing and absorption
JEJUNAL DISACCHARIDASES IN PROTEIN ENERGY MALNUTRITION AND RECOVERY
 JEJUNAL DISACCHARIDASES IN PROTEIN ENERGY MALNUTRITION AND RECOVERY R. Mehra S.M. Khambadkone M.K. Jain S. Ganapathy ABSTRACT The jejunal disaccharidases, sucrose, maltose and lactose, were determined
JEJUNAL DISACCHARIDASES IN PROTEIN ENERGY MALNUTRITION AND RECOVERY R. Mehra S.M. Khambadkone M.K. Jain S. Ganapathy ABSTRACT The jejunal disaccharidases, sucrose, maltose and lactose, were determined
Clinical presentation of coeliac disease in
 The Ulster Medical Joumal, Volume 54, No. 2, pp. 140-147, October 1985. Clinical presentation of coeliac disease in adult gastroenterological practice S Boyd, B J Collins, P M Bell, A H G Love Accepted
The Ulster Medical Joumal, Volume 54, No. 2, pp. 140-147, October 1985. Clinical presentation of coeliac disease in adult gastroenterological practice S Boyd, B J Collins, P M Bell, A H G Love Accepted
Laboratory Methods for Diagnosing Celiac Disease. Vijay Kumar, PhD, FACB IMMCO Diagnostics, Inc. Buffalo, NY
 Laboratory Methods for Diagnosing Celiac Disease Vijay Kumar, PhD, FACB IMMCO Diagnostics, Inc. Buffalo, NY Prevalence of Celiac Disease Group With Symptoms Adults Children Associated Symptoms Chronic
Laboratory Methods for Diagnosing Celiac Disease Vijay Kumar, PhD, FACB IMMCO Diagnostics, Inc. Buffalo, NY Prevalence of Celiac Disease Group With Symptoms Adults Children Associated Symptoms Chronic
Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding
 Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding Allergic Colitis is an inflammatory disorder of the colon which occurs mainly in preschool children. It is caused by an
Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding Allergic Colitis is an inflammatory disorder of the colon which occurs mainly in preschool children. It is caused by an
Ischaemic strictures of the small intestine in Nigeria
 Gut, 1977, 18, 266-273 Ischaemic strictures of the small intestine in Nigeria S. G. SUBBUSWAMY,1 AND F. I. IWEZE From the Departments ofpathology and Surgery, University of Benin, Benin City, Nigeria SUMMARY
Gut, 1977, 18, 266-273 Ischaemic strictures of the small intestine in Nigeria S. G. SUBBUSWAMY,1 AND F. I. IWEZE From the Departments ofpathology and Surgery, University of Benin, Benin City, Nigeria SUMMARY
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Bowel cancer risk in the under 50s. Greg Rubin Professor of General Practice and Primary Care
 Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
Gastrointestinal involvement in systemic mastocytosis
 Gut, 1976, 17, 107-112 Gastrointestinal involvement in systemic mastocytosis R. W. AMMANN, D. VETTER, P. DEYHLE, H. TSCHEN, H. SULSER, AND M. SCHMID From the Division of Gastroenterology, Department of
Gut, 1976, 17, 107-112 Gastrointestinal involvement in systemic mastocytosis R. W. AMMANN, D. VETTER, P. DEYHLE, H. TSCHEN, H. SULSER, AND M. SCHMID From the Division of Gastroenterology, Department of
(A) Anemia (B) Malaria (C) Dehydration due to excess fluid loss. A. Incorrect! Anemia is symptomatic of sickle cell anemia, but is not the root cause.
 USMLE Step 1- Problem Drill 13: Histology Question No. 1 of 10 1. An 8 year old male complains of fatigue and dactylitis, and has a history of recurrent bacterial infections. Examination of a blood smear
USMLE Step 1- Problem Drill 13: Histology Question No. 1 of 10 1. An 8 year old male complains of fatigue and dactylitis, and has a history of recurrent bacterial infections. Examination of a blood smear
Allergic disorders of the gastrointestinal tract
 Allergic disorders of the gastrointestinal tract Christopher Justinich, MD Introduction The patient with presumed food hypersensitivity continues to present a challenge for the clinician. In certain instances,
Allergic disorders of the gastrointestinal tract Christopher Justinich, MD Introduction The patient with presumed food hypersensitivity continues to present a challenge for the clinician. In certain instances,
Digestive system L 2. Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section
 Digestive system L 2 Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section objectives 1-Describe the general structure of digestive tract: a-mucosa. b-submucosa. c-muscularis externa d-adventitia
Digestive system L 2 Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section objectives 1-Describe the general structure of digestive tract: a-mucosa. b-submucosa. c-muscularis externa d-adventitia
Coeliac Disease: Diagnosis and clinical features
 Coeliac Disease: Diagnosis and clinical features Australasian Gastrointestinal Pathology Society AGM 28 Oct 2016 Dr. Hooi Ee Gastroenterologist, Sir Charles Gairdner Hospital Coeliac disease Greek: koiliakos
Coeliac Disease: Diagnosis and clinical features Australasian Gastrointestinal Pathology Society AGM 28 Oct 2016 Dr. Hooi Ee Gastroenterologist, Sir Charles Gairdner Hospital Coeliac disease Greek: koiliakos
Case discussions. Case 1
 Case discussions Arzu Ensari 12 year old teen Case 1 Progressive cough and dysphagia following flu-like symptoms Family history of asthma Erythema in lower oesophagus 1 40 eos/hpf 2 What is Eosinophilic
Case discussions Arzu Ensari 12 year old teen Case 1 Progressive cough and dysphagia following flu-like symptoms Family history of asthma Erythema in lower oesophagus 1 40 eos/hpf 2 What is Eosinophilic
Lymphocyte subpopulations in adult coeliac disease
 Gut, 1978, 19, 892-897 Lymphocyte subpopulations in adult coeliac disease A. W. BULLEN AND M. S. LOSOWSKY From the Department of Medicine, St James's Hospital, Leeds SUMMARY Rosetting techniques were used
Gut, 1978, 19, 892-897 Lymphocyte subpopulations in adult coeliac disease A. W. BULLEN AND M. S. LOSOWSKY From the Department of Medicine, St James's Hospital, Leeds SUMMARY Rosetting techniques were used
WALSALL COELIAC DISEASE FLOWCHART
 WALSALL COELIAC DISEASE FLOWCHART CLINICAL SUSPICION OF COELIAC DISEASE ( Which can present at any age ) [see Box A or Box B] DO NOT START GLUTEN FREE DIET BEFORE ANY INVESTIGATIONS Test for IgA Tissue
WALSALL COELIAC DISEASE FLOWCHART CLINICAL SUSPICION OF COELIAC DISEASE ( Which can present at any age ) [see Box A or Box B] DO NOT START GLUTEN FREE DIET BEFORE ANY INVESTIGATIONS Test for IgA Tissue
Unit I Problem 9 Histology: Basic Tissues of The Body
 Unit I Problem 9 Histology: Basic Tissues of The Body - What is the difference between cytology and histology? Cytology: it is the study of the structure and functions of cells and their contents. Histology:
Unit I Problem 9 Histology: Basic Tissues of The Body - What is the difference between cytology and histology? Cytology: it is the study of the structure and functions of cells and their contents. Histology:
How I Handle Mast Cells in GI Biopsies
 How I Handle Mast Cells in GI Biopsies Dora Lam-Himlin, MD Mayo Clinic Scottsdale, AZ Rodger C. Haggitt Gastrointestinal Pathology Society Forum United States and Canadian Academy of Pathologists Seattle,
How I Handle Mast Cells in GI Biopsies Dora Lam-Himlin, MD Mayo Clinic Scottsdale, AZ Rodger C. Haggitt Gastrointestinal Pathology Society Forum United States and Canadian Academy of Pathologists Seattle,
Rectal mucosa in cows' milk allergy
 Archives of Disease in Childhood, 1989, 64, 1256-1260 Rectal mucosa in cows' milk allergy N IYNGKARAN,* M YADAVt AND C G BOEYt Departments of *Paediatrics and tpathology, University Hospital, and tdepartment
Archives of Disease in Childhood, 1989, 64, 1256-1260 Rectal mucosa in cows' milk allergy N IYNGKARAN,* M YADAVt AND C G BOEYt Departments of *Paediatrics and tpathology, University Hospital, and tdepartment
This is the second learning component (Learning Component 2) in our first learning module (Learning Module 1). In this component we review a very
 This is the second learning component (Learning Component 2) in our first learning module (Learning Module 1). In this component we review a very basic response to injury inflammation. We ll look at examples
This is the second learning component (Learning Component 2) in our first learning module (Learning Module 1). In this component we review a very basic response to injury inflammation. We ll look at examples
Ileo-caecal tuberculosis
 Gut, 1964, 5, 524 Ileo-caecal tuberculosis J. S. HOWELL1 AND P. J. KNAPTON2 Fr-om the Birmingham United Hospitals and the Department of Pathology, University of Birmingham EDITORIAL SYNOPSIS Seven patients
Gut, 1964, 5, 524 Ileo-caecal tuberculosis J. S. HOWELL1 AND P. J. KNAPTON2 Fr-om the Birmingham United Hospitals and the Department of Pathology, University of Birmingham EDITORIAL SYNOPSIS Seven patients
Chapter 16 Lymphatic System and Immunity. Lymphatic Pathways. Lymphatic Capillaries. network of vessels that assist in circulating fluids
 Chapter 16 Lymphatic System and Immunity network of vessels that assist in circulating fluids closely associated with the cardiovascular system transports excess fluid away from interstitial spaces transports
Chapter 16 Lymphatic System and Immunity network of vessels that assist in circulating fluids closely associated with the cardiovascular system transports excess fluid away from interstitial spaces transports
Guidelines NICE, not NICE and the Daily Mail. Dr Andy Poullis Consultant Gastroenterologist
 Guidelines NICE, not NICE and the Daily Mail 2018 Dr Andy Poullis Consultant Gastroenterologist Coeliac IBS Gall bladder polyps PEI PPI Who to test for Coeliac persistent unexplained abdominal or gastrointestinal
Guidelines NICE, not NICE and the Daily Mail 2018 Dr Andy Poullis Consultant Gastroenterologist Coeliac IBS Gall bladder polyps PEI PPI Who to test for Coeliac persistent unexplained abdominal or gastrointestinal
Human Anatomy and Physiology - Problem Drill 20: Immunity and the Lymphatic System
 Human Anatomy and Physiology - Problem Drill 20: Immunity and the Lymphatic System Question No. 1 of 10 The lymphatic system is formed early during human development. Which of the following statements
Human Anatomy and Physiology - Problem Drill 20: Immunity and the Lymphatic System Question No. 1 of 10 The lymphatic system is formed early during human development. Which of the following statements
ART 50 Capsules. Symptomatic treatment of functional symptoms and signs of osteoarthritis.
 Doctor leaflet Art50-DL-March2012-01 ART 50 Capsules 1. NAME OF THE MEDICINAL PRODUCT Art 50 mg, capsule. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each capsule of ART 50 contains Diacerein 50 mg. For
Doctor leaflet Art50-DL-March2012-01 ART 50 Capsules 1. NAME OF THE MEDICINAL PRODUCT Art 50 mg, capsule. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each capsule of ART 50 contains Diacerein 50 mg. For
DISORDERS OF THE SMALL INTESTINE MALABSORPTION SYNDROMES I.
 DISORDERS OF THE SMALL INTESTINE MALABSORPTION SYNDROMES I. Gyula Mózsik M. D., Sc. D.(med.) University of Pécs 2008 DEFINITIONS: These medical symptomes include all of the clinical pictures in patients
DISORDERS OF THE SMALL INTESTINE MALABSORPTION SYNDROMES I. Gyula Mózsik M. D., Sc. D.(med.) University of Pécs 2008 DEFINITIONS: These medical symptomes include all of the clinical pictures in patients
Small intestine. Small intestine
 General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
REFERRAL GUIDELINES - SUMMARY
 Clinical Immunology & Allergy Unit LEEDS TEACHING HOSPITALS NHS TRUST REFERRAL GUIDELINES - SUMMARY THESE GUIDELINES ARE DESIGNED TO ENSURE THAT PATIENTS REQUIRING SECONDARY CARE ARE SEEN EFFICIENTLY AND
Clinical Immunology & Allergy Unit LEEDS TEACHING HOSPITALS NHS TRUST REFERRAL GUIDELINES - SUMMARY THESE GUIDELINES ARE DESIGNED TO ENSURE THAT PATIENTS REQUIRING SECONDARY CARE ARE SEEN EFFICIENTLY AND
Mesenteric lymph node cavitation in coeliac disease
 Gut, 1986, 27, 728-733 Case report Mesenteric lymph node cavitation in coeliac disease G K T HOLMES From the Department of Gastroenterology, Derbyshire Royal Infirmary, Derby SUMMARY A patient with coeliac
Gut, 1986, 27, 728-733 Case report Mesenteric lymph node cavitation in coeliac disease G K T HOLMES From the Department of Gastroenterology, Derbyshire Royal Infirmary, Derby SUMMARY A patient with coeliac
Collagenous colitis associated with small intestinal villous atrophy
 (Gut, 1986, 27, 1394-1398 Case report Collagenous colitis associated with small intestinal villous atrophy I HAMILTON, S SANDERS, D HOPWOOD, AND I A D BOUCHIER From the University Department of Medicine
(Gut, 1986, 27, 1394-1398 Case report Collagenous colitis associated with small intestinal villous atrophy I HAMILTON, S SANDERS, D HOPWOOD, AND I A D BOUCHIER From the University Department of Medicine
Transient paraproteinaemia in a patient with
 Transient paraproteinaemia in a patient with coeliac disease Gut, 1976,17, 735-739 A. S. PENA, JANNY v. NIEUWKOOP, H. R. E. SCHUIT, W. TH. J. M. HEKKENS, AND A. J. CH. HAEX From the Departments of Gastroenterology
Transient paraproteinaemia in a patient with coeliac disease Gut, 1976,17, 735-739 A. S. PENA, JANNY v. NIEUWKOOP, H. R. E. SCHUIT, W. TH. J. M. HEKKENS, AND A. J. CH. HAEX From the Departments of Gastroenterology
GASTRIC HETEROTOPIA IN THE ILEUM WITH ULCERATION AND CHRONIC BLEEDING
 GASTROENTEROLOGY 66: 113-117, 1974 Copyright 1974 by The Williams & Wilkins Co. Vol. 66, No.1 Printed in U.S.A. CASE REPORTS GASTRIC HETEROTOPIA IN THE ILEUM WITH ULCERATION AND CHRONIC BLEEDING KARIM
GASTROENTEROLOGY 66: 113-117, 1974 Copyright 1974 by The Williams & Wilkins Co. Vol. 66, No.1 Printed in U.S.A. CASE REPORTS GASTRIC HETEROTOPIA IN THE ILEUM WITH ULCERATION AND CHRONIC BLEEDING KARIM
The focus of this week s lab will be pathology of the gastrointestinal and hepatobiliary systems.
 GASTROINTESTINAL AND HEPATOBILIARY SYSTEMS The focus of this week s lab will be pathology of the gastrointestinal and hepatobiliary systems. GASTROINTESTINAL SYSTEM AND HEPATOBILIARY SYSTEM We will examine
GASTROINTESTINAL AND HEPATOBILIARY SYSTEMS The focus of this week s lab will be pathology of the gastrointestinal and hepatobiliary systems. GASTROINTESTINAL SYSTEM AND HEPATOBILIARY SYSTEM We will examine
