Coeliac disease with severe hypogammaglobulinaemia
|
|
|
- Jade Atkinson
- 6 years ago
- Views:
Transcription
1 Gut, 1981, 22, Case report Coeliac disease with severe hypogammaglobulinaemia A D B WEBSTER, G SLAVIN, M SHINER, T A E PLATTS-MILLS, AND G L ASHERSON From the Divisions of Immunological Medicine and Clinical Sciences, Clinical Research Centre, Harrow, and the Histopathology Department, Northwick Park Hospital, Harrow, Middlesex SUMMARY A patient with severe late onset primary hypogammaglobulinaemia developed coeliac disease. The case illustrates that coeliac disease can occur in the virtual absence of local antibody production by plasma cells in the mucosa of the small bowel. Furthermore, our inability to demonstrate specific cellular immunity to a subfraction of gluten raises doubts about the relevance of immunological reactions in the pathogenesis of coeliac disease. There are two main hypotheses to explain the aetiology of coeliac disease. Bronstein et al.' suggested that the disease was caused by enzymatic failure to degrade gluten with a consequent production of peptides which were toxic to the small intestinal epithelial cells. This hypothesis does not exclude a secondary role for immunological reactions in the pathogenesis of the condition. The currently more favoured view2 is that the intestinal lesion is initiated and perpetuated by an immunological reaction. This is supported by the finding of numerous plasma cells in the intestinal lesions of coeliac disease.3 Cellular immune mechanisms may also play a part in causing damage to the mucosa, and it has been suggested that the lymphocytes of coeliac patients may be sensitised to certain subfractions of gluten.465 The strong association with the HLA-DW3 histocompatibility antigen is further evidence that the disease has an immunological basis. The presence of complement and its breakdown products in the mucosal lesions of coeliac patients suggests that the damage is mediated by an Arthus reaction.6 The specificity of the antibody involved is not known but is presumed to be directed against a component of gluten. However, the case described here shows that antibody mediated reactions are not essential in the pathogenesis of coeliac disease. Case report infections. After this he suffered with recurrent episodes of bronchitis and sinusitis. Hypogammaglobulinaemia was diagnosed at 53 years and he was treated with regular weekly injections of gammaglobulin. Thereafter, he did well and only had one or two attacks of bronchitis requiring antibiotics during the subsequent 15 years. For the past 25 years he has suffered with mild recurrent eczematous dermatitis on the fingers and seborrhoeic dermatitis in the groins. At the age of 55 years he developed a small patch of vitiligo over the sternum. During the first few months of 1978 he experienced a number of anaphylactic reactions to his gammaglobulin injections, although he has had no reactions for the past two years. In 1974 (aged 63 years) he began passing three to four steatorrhoeic motions a day, although he was not losing weight. Physical examination at this time showed no abnormality and the following investigations confirmed malabsorption: the five day faecal fat collection on a 100 g fat diet per day was 9.3 g/ day. The red cell folate was 76 ng/ml (normal ng/ml) and the peripheral blood film showed a mild macrocytosis. The serum calcium was 2.2 mmol/l (normal mmol/l). A standard xylose absorption test (25 g oral dose) showed a five hour urinary excretion of 15 mmol (normal > 33 mmol). The serum vitamin B12 was normal at 340 pg/ml and the Schilling test was normal. A pentagastrin stimulation test showed normal gastric LT developed pneumonia when aged 43 years, acid and intrinsic factor production. Barium meal having previously shown no undue susceptibility to showed a malabsorption pattern in the small bowel and a fine nodular pattern in the terminal ileum Received for publication 12 September 1980 characteristic of nodular lymphoid hyperplasia. A 153
2 154 Lundh test showed normal pancreatic function with an intestinal juice trypsin level of 33 IU. A jejunal aspirate contained no giardia parasites and when cultured aerobically and anaerobically for bacteria grew < 104 bacteria/ml (normal < 104). The immunological tests showed a severe hypogammaglobulinaemia and normal cellular immunity Table Immunological tests on patient LT Immunoglobulins Serum IgG IgA IgM IgE Jejunal juice IgG IgA IgM Isohaemagglutinin titre Anti A Anti B E. coli antibody titre Blood lymphocytes T cells (%) B cells (%) IU/mi Delayed hypersensitivity skin tests Candida ) Mumps k Positive PPD J Lymphocyte transformation to PHA 3528 HLA typing < < < :64 >1:32 1:32 >1:16 1:4 >1:64 95 % range of results for normal adults (lu/ml) I,ul /,i Al, W30/B8, 18/CW5/DRW3/DW cpm Webster, Slavin, Shiner, Platts-Mills, and Asherson (Table), and he was classified as having adult onset primary hypogammaglobulinaemia. His lymphocytes carried the HLA Al, B8, DW3 haplotype which is commonly seen in coeliac patients. JEJUNAL HISTOLOGY AND CLINICAL PROGRESS The initial jejunal biopsy (Fig. 1 a) taken in October 1974 shows subtotal villous atrophy with crypt hyperplasia. Inflammatory cells were increased in the lamina propria but only occasional plasma cells were noted. The intraepithelial lymphocyte count was increased (57 lymphocytes/100 epithelial cells; N= <30). Surface enterocytes showed focal flattening and degeneration. The patient was started on a strict gluten free diet in November 1974 and within three weeks he was passing normal motions once a day (Fig. 2). He was still asymptomatic when readmitted in May 1975 for a repeat jejunal biopsy (Fig. Ib). This showed considerable improvement with mild partial villous atrophy. The surface cells were columna and the intraepithelial lymphocyte count was 33 lymphcytes/100 epithelial cells. Plasma cells were not indentified in the lamina propria. He remained on a gluten free diet and was asymptomatic when readmitted in March 1977 for a gluten challenge to confirm the diagnosis. The pre-challenge jejunal biopsy showed partial villous atrophy and no significant change was seen in a biopsy taken 21 hours after gluten. A post-gluten biopsy at 45 hours showed a lymphoid follicle and was inadequate for detailed analysis. When the gluten challenge failed to confirm the diagnosis of gluten enteropathy, he was allowed to Gut: first published as /gut on 1 February Downloaded from Fig. l (a) Initial jejunal biopsy showing subtotal villous atrophy with crypt hyperplasia. H and E, x 95. (b) Jejunal mucosa showing improvenment in appearance of villi after six months on a gluten-free diet. H and E, x 95. (c) Jejunal mucosa showing relapse to subtotal villous atrophy after three months on an unrestricted diet. H and E x 95. (Original magnifications.) on 7 July 2018 by guest. Protected by copyright.
3 Coeliac disease with severe hypogammaglobulinaemia Jan.June Oct Nov Jan May Dec March Nov Feb A Jej biopsy (2a) Subtotal villous atrophy Gluten free diet Jej biopsy (2b) Partial villous atrophy 3 x Jej biopsies during _Partial villous atrophy, gluten challenge Normal diet,a Jej biopsy (2c) Subtotal villous atrophy Gluten free diet Fig. 2 Relationship between diet, symptoms, and.mucosal changes. return to a free diet in November However, within four weeks he developed steatorrhoea with at least four bowel motions a day. He was readmitted for a jejunal biopsy in February 1978, having lost about half a stone in weight. The jejunal biopsy (Fig. lc) was similar to that taken in October 1974 with severe villous atrophy and an increased intraepithelial lymphocyte count (58 lymphocytes/100 epithelial cells). No plasma cells were seen and immunoperoxidase staining for intracellular IgG, IgA, and IgM was negative. Having established a diagnosis of gluten enteropathy, he was again put on a gluten free diet and within a few weeks was passing one normal motion a day. He has since been mainly asymptomatic with occasional bouts of diarrhoea when he relaxes his diet SPECIAL STUDIES Gluteni challenge A gluten challenge test was performed in March 1977, the patient having been on a strict gluten free diet for 16 months. Twenty grams of cooked gluten was taken orally after an initial jejunal biopsy. Additional jejunal biopsies were taken at 21 hours and 45 hours after gluten. Serum was obtained on each occasion to measure total haemolytic complement, IgE and C3, but these showed no significant changes. Immunofluorescence studies on the three jejunal biopsies taken during this study showed no cellular staining for IgA and IgG and only one or two cells in each biopsy stained for IgM. The connective tissue of the lamina propria showed bright staining for IgG, which probably originated from the gammaglobulin injections. Connective tissue staining with 155 antisera to C3 was faint in the pre-challenge mucosa and increased in both of the post-challenge biopsies. Staining for secretory piece was normal. Electronmicroscopy of the pre- and post-challenge biopsies was similar and showed normal enterocytes. No plasma cells were seen, but lymphocytes, macrophages, and eosinophils were plentiful. Mucosal immunoglobulin production in vitro We measured immunoglobulin production in vitro by the patient's jejunal mucosa in order to check that small amounts of immunoglobulin were not being produced by cells that did not have the usual morphological appearances of plasma cells. Using the technique of Oldham et al.'7 the jejunal biopsy taken in February 1978 during relapse was cut into three pieces (weight 1, 3.0, and 2.8 mg) and cultured separately in vitro to assess local immunoglobulin production. No detectable IgA or IgM-that is, <2ng/mg tissue-was produced by the samples at any time over six days. In contrast, normal rectal biopsies continued to produce 30-> 1000 ng/iga per mg of tissue/day on the sixth day of culture (see Oldham et al.7). Some IgG was present in the culture supernatant at 24 hours but rapidly decreased, and was unrecordable on the fifth day. This indicated that the IgG originated from outside the gut and was not synthesised by cells in the mucosa. Specific immunity to gluten Lymphocyte transformation studies to a gluten subfraction were performed in July 1978, when the patient was asymptomatic on a gluten free diet. Peripheral blood lymphocytes obtained from a Ficoll/triosil density gradient were cultured at 1 x 106/ml in Dulbecoo's modified medium and 100% human AB serum with 10, 50, and 100.tg/ml final concentration of the Oxford B2 fraction of gluten. This fraction, which has been previously shown to stimulate lymphocyte transformation in patients with coeliac disease, is a subfraction of Frazer's fraction III.5 3H thymidine (1 uci) was added at 40 hours and the cultures harvested using a Scatron automatic harvester eight hours later. Other cultures were left for five days before 3H thymidine was added and the cultures harvested 16 hours later. The results showed that there was no increased uptake of 3H thymidine in the cultures containing B2 fraction compared with control cultures at either 48 hours or 52 days. However, these data should be interpreted with caution, as no positive controls were used. Skini tests An intradermal skin test with 01 ml of the Oxford B2 fraction, together with an appropriate control, was performed as recommended by Anand et al.10 At
4 156 Webster, Slavin, Shiner, Platts-Mills, and Asherson six hours, the B2 fraction produced an area of erythema of 15 mm diameter which then gradually faded and disappeared by 24 hours. The control test site showed a 3 mm reaction at six hours and then faded rapidly. The skin tests were repeated one month later when the B2 fraction gave a response of 10 mm in diameter, but this time biopsies of the test areas for both the B2 fraction and the control were obtained at six hours. The histology showed an inflammatory reaction, with mononuclear cells and neutrophils in both the control and B2 fraction test site. There was also no significant difference in the number of basophils present in both the control and the test site and immunofluorescent studies showed no accumulation of C3. Discussion Coeliac disease has been previously suspected in a few patients with primary hypogammaglobulinaemia, but has never been satisfactorily confirmed by showing a relapse on a normal diet.8 9 The necessary criteria for the diagnosis of gluten enteropathy have been fulfilled in this patient by demonstrating both histological and clinical improvement after gluten withdrawal, followed by relapse on a normal diet, and then improvement again after gluten withdrawal. Apart from an occasional IgM-containing cell, immunofluorescent and immunoperoxidase staining together with electronmicroscopy failed to demonstrate the presence of immunoglobulin containing plasma cells in jejunal biopsies from this patient. It is difficult to interpret the negative findings after the gluten challenge and we might have seen changes if we had waited longer than 48 hours before repeating the jejunal biopsy. Although Anand et al.10 found a good correlation between coeliac disease and positive skin tests to the B2 fraction of gluten, the interpretation of the skin test in this patient is not straightforward, as positive skin tests are also associated with other inflammatory bowel disorders." Although the timing of the skin reaction in our patient was consistent with an Arthus reaction, this was not confirmed by the histology and immunofluorescent findings. It has been suggested that the increase in epithelial lymphocytes means that the mucosal damage could be mediated by a cellular immune reaction.'2 Intraepithelial lymphocyte counts were raised in our patient during relapse. However, Guix et al.13 suggest that this has little significance in the pathogenesis, as, in absolute terms, the number of intraepithelial lymphocytes does not alter during relapse and remission. Moreover, we found no evidence that peripheral blood lymphocytes from the patient were sensitised to the Oxford B2 fraction. Although the significance of lymphocyte transformation tests in this context remains contentious, Bullen and Losowsky,14 using a macrophage inhibition factor (MIF) test, have demonstrated the presence of lymphocytes sensitised to Frazer's fraction III in the blood of patients with coeliac disease. However, late skin reactions at 48 and 72 hours were not seen when the B2 fraction was used for skin testing. This case demonstrates that the pathogenesis of coeliac disease does not necessarily depend upon the presence of a plasma cell infiltrate into the mucosa. It is also unlikely in this case that an Arthus type reaction is involved in the mucosal lesions. However, we cannot completely exclude a role for antibody as some IgM and IgG was detectable in the jejunal juice and the presence of isohaemagglutinins in the serum indicated some residual capacity to make IgM antibodies. Nevertheless, the IgM in the jejunal juice probably came from the bile and the IgG from the gammaglobulin injections. This patient, like many others with adult onset primary hypogammaglobulinaemia, had a few immunoglobulin-containing cells within the gut mucosa,15 although we were able to demonstrate only one or two IgM-containing cells in some of the biopsies. The apparent accumulation of C3 in the mucosa after gluten challenge is unexplained but could be due to activation of the alternate complement pathway by gluten.16 However, this may only have reflected increased transudation of C3 from serum, as the immunofluorescent studies were done on fixed tissues. We have found no evidence that immunological mechanisms are involved in this patient's coeliac disease. This suggests that the link between the HLA- DW3 histocompatibility marker and coeliac disease may not involve immunological reactions.17 Although immunological reactions may play a part in the pathogenesis of coeliac disease in most patients, this case shows that other non-immunological factors are likely to be of primary importance. We would like to thank Miss S Wilson, Mrs C Newton, and the staff of the Northwick Park Histopathology department for technical assistance. We are also most grateful to Dr P M Rawcliffe and Dr R E Offord for supplying us with the Oxford B2 fraction. We also thank Dr J A Sachs for the HLA typing. References 1Bronstein HD, Haeffner LJ, Kowlessar OD. Enzymatic digestion of gliadin: the effect of the resultant peptides in adult coeliac disease. Clin Chim Acta 1966; 14:
5 Coeliac disease with severe hypogammaglobulinaemia 157 2Booth CC, Peters TJ, Doe WF. Immunopathology of coeliac disease: In Immunology of the gut. Ciba Foundation Symposium 46 (New Series) North Holland: Excerpta Medica, 1977: Shiner M. Ultrastructural changes suggestive of immune reactions in the jejunal mucosa of coeliac children following gluten challenge. Gut 1973; 14: Ferguson A, MacDonald TT, McClure JP, Holden RJ. Cell mediated immunity to gliadin within the small intestinal mucosa in coeliac disease. Lancet 1975; 1: Sikora K, Anand BS, Truelove SC, Ciclitira PJ, Offord RE. Stimulation of lymphocytes from patients with coeliac disease by a subfraction of gluten. Lancet 1976; 2: "Doe WF, Henry K, Booth CC. Complement in coeliac disease. In: Hekkens WTJM, Pena AS, eds. Coeliac disease. Leiden: Stenfert-Kroese, 1974: Oldham G, Platts-Mills TAE, Chalmers DM, Webster ADB. A quantitative method for measuring in vitro synthesis of IgA and IgG by human rectal mucosa; studies on normal controls and patients with hypogammaglobulinaemia. Immunology 1979; 37: Lanning M, Kouvalainen K, Simila S, Raunio V. Agammaglobulinaemia with arthritis and coeliac disease developing after infectious mononucleosis. Scand J Infect Dis 1977; 9: Hughes WS, Cerda JJ, Holtzapple P, Brooks FP. Primary hypogammaglobulinaemia and malabsorption. Ann Intern Med 1971; 74: Anand BS, Truelove SC, Offord RE. Skin test for coeliac disease using a subfraction of gluten. Lancet 1977; 1: "Baker PG, Read AE. Positive skin reactions to gluten in coeliac disease. Q J Med 1976; 45: Ferguson A. Lymphocytes in coeliac disease. In: Hekkens WTJM, Pena AS, eds. Coeliac disease. Leiden: Stenfert-Kroese, 1974: Guix M, Skinner JM, Whitehead R. Measuring intraepithelial lymphocytes, surface area, and volume of lamina propria in the jejunal mucosa of coeliac patients. Gut 1979; 20: Bullen AW, Losowsky MS. Cell mediated immunity to gluten fraction III in adult coeliac disease. Gut 1978; 19: ',Broom BC, de la Concha EG, Webster ADB, Loewi G, Asherson GL. Dichotomy between immunoglobulin synthesis by cells in gut and blood of patients with hypogrammaglobulinaemia. Lancet 1975; 2: Massey A, Capner PM, Mowbray JF. Activation of the alternative pathway by gluten. A possible aetiological factor in dermatitis herpetiformis. Immunology 1977; 33: '7Keuning JJ, Pena AS, Van Leeuwen A, Van Hooff JP, Van Rood JJ. HLA-DW3 association with coeliac disease. Lancet 1976; 1: 506. Gut: first published as /gut on 1 February Downloaded from on 7 July 2018 by guest. Protected by copyright.
ranged from two months to 21 years (mean 5% years)
 Gut, 1978, 19, 754-758 Response of the skin in dermatitis herpetiformis to a gluten free diet, with reference to jejunal morphology B. T. COOPER, E. MALLAS, M. D. TROTTER, AND W. T. COOKE From the Nutritional
Gut, 1978, 19, 754-758 Response of the skin in dermatitis herpetiformis to a gluten free diet, with reference to jejunal morphology B. T. COOPER, E. MALLAS, M. D. TROTTER, AND W. T. COOKE From the Nutritional
Reintroduction of gluten in adults and children with treated coeliac disease
 Reintroduction of gluten in adults and children with treated coeliac disease PARVEEN J. KUMAR, D. P. O'DONOGHUE, KATHY STENSON, AND A. M. DAWSON From the Department of Gastroenterology, St. Bartholomew's
Reintroduction of gluten in adults and children with treated coeliac disease PARVEEN J. KUMAR, D. P. O'DONOGHUE, KATHY STENSON, AND A. M. DAWSON From the Department of Gastroenterology, St. Bartholomew's
Adult coeliac disease
 Postgrad. med. J. (August 1968) 44, 632-640. PATENTS with idiopathic steatorrhoea present in many different ways. The dominant feature of the clinical presentation in 100 patients is shown in Table 1.
Postgrad. med. J. (August 1968) 44, 632-640. PATENTS with idiopathic steatorrhoea present in many different ways. The dominant feature of the clinical presentation in 100 patients is shown in Table 1.
Timing of infiltration of T lymphocytes induced by gluten into the small intestine in coeliac disease
 J Clin Pathol 1987;40:741-745 Timing of infiltration of T lymphocytes induced by gluten into the small intestine in coeliac disease A R FREEDMAN,* J C MACARTNEY,t J M NELUFER,* P J CICLITIRA* From the
J Clin Pathol 1987;40:741-745 Timing of infiltration of T lymphocytes induced by gluten into the small intestine in coeliac disease A R FREEDMAN,* J C MACARTNEY,t J M NELUFER,* P J CICLITIRA* From the
Chronic immune colitis in rabbits
 Chronic immune colitis in rabbits A. S. MEE, J. E. McLAUGHLIN, H. J. F. HODGSON, AND D. P. JEWELL Gut, 1979, 20, 1-5 From the Academic Department of Medicine and Department of Histopathology, Royal Free
Chronic immune colitis in rabbits A. S. MEE, J. E. McLAUGHLIN, H. J. F. HODGSON, AND D. P. JEWELL Gut, 1979, 20, 1-5 From the Academic Department of Medicine and Department of Histopathology, Royal Free
Splenic atrophy in adult coeliac disease:
 Gut, 1981, 22, 628-632 Splenic atrophy in adult coeliac disease: is it reversible? P N TREWBY, P M CHIPPING, S J PALMER, P D ROBERTS, S M LEWIS, AND J S STEWART From the Departments of Gastroenterology
Gut, 1981, 22, 628-632 Splenic atrophy in adult coeliac disease: is it reversible? P N TREWBY, P M CHIPPING, S J PALMER, P D ROBERTS, S M LEWIS, AND J S STEWART From the Departments of Gastroenterology
above 110 g per 100 ml in four patients, but the
 J. clin. Path., 1971, 24, 244-249 Diagnostic value of the serum folate assay J. FORSHAW AND LILIAN HARWOOD From the Haematology Laboratory, Sefton General Hospital, Liverpool SYNOPSIS The diagnostic value
J. clin. Path., 1971, 24, 244-249 Diagnostic value of the serum folate assay J. FORSHAW AND LILIAN HARWOOD From the Haematology Laboratory, Sefton General Hospital, Liverpool SYNOPSIS The diagnostic value
What is your diagnosis? a. Lymphocytic colitis. b. Collagenous colitis. c. Common variable immunodeficiency (CVID) associated colitis
 Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
Coeliac Disease Bible Class Questions and Answers
 Coeliac Disease Bible Class Questions and Answers Jan Hendrik Niess What is the definition of coeliac disease? Coeliac disease is an immune reaction to gluten (wheat, barely, rye) in an genetic predisposed
Coeliac Disease Bible Class Questions and Answers Jan Hendrik Niess What is the definition of coeliac disease? Coeliac disease is an immune reaction to gluten (wheat, barely, rye) in an genetic predisposed
The cell population of the upper jejunal mucosa in tropical sprue and postinfective malabsorption
 Gut, 1974, 15, 387-391 The cell population of the upper jejunal mucosa in tropical sprue and postinfective malabsorption R. D. MONTGOMRY AND A. C. I. SHARR From the Metabolic Unit, ast Birmingham Hospital,
Gut, 1974, 15, 387-391 The cell population of the upper jejunal mucosa in tropical sprue and postinfective malabsorption R. D. MONTGOMRY AND A. C. I. SHARR From the Metabolic Unit, ast Birmingham Hospital,
Confirming persistence of gluten intolerance in
 Archives of Disease in Childhood, 1975, 50, 259. Confirming persistence of gluten intolerance in children diagnosed as having coeliac disease in infancy Usefulness of onehour blood xylose test C. J. ROLLES,
Archives of Disease in Childhood, 1975, 50, 259. Confirming persistence of gluten intolerance in children diagnosed as having coeliac disease in infancy Usefulness of onehour blood xylose test C. J. ROLLES,
Is a raised intraepithelial lymphocyte count with normal duodenal villous architecture clinically relevant?
 424 ORIGINAL ARTICLE Is a raised intraepithelial lymphocyte count with normal duodenal villous architecture clinically relevant? S Mahadeva, J I Wyatt, P D Howdle... See end of article for authors affiliations...
424 ORIGINAL ARTICLE Is a raised intraepithelial lymphocyte count with normal duodenal villous architecture clinically relevant? S Mahadeva, J I Wyatt, P D Howdle... See end of article for authors affiliations...
 SUMMARY Coeliac disease is a common food intolerance in Western populations, in which it has a prevalence of about 1%. In early infancy, when the transition is made to a gluten-containing diet (particularly
SUMMARY Coeliac disease is a common food intolerance in Western populations, in which it has a prevalence of about 1%. In early infancy, when the transition is made to a gluten-containing diet (particularly
Quantitation of intraepithelial lymphocytes
 Gut, 1971, 12, 988-994 Quantitation of intraepithelial lymphocytes inhuman jejunum ANNE FERGUSON AND D. MURRAY From the University Departments ofbacteriology and Immunology (Western Infirmary) and Pathology
Gut, 1971, 12, 988-994 Quantitation of intraepithelial lymphocytes inhuman jejunum ANNE FERGUSON AND D. MURRAY From the University Departments ofbacteriology and Immunology (Western Infirmary) and Pathology
coeliac syndrome per day. Investigations showed a megaloblastic anaemia showed a flat mucosa. ileum were resected and he made an uninterrupted
 Gut, 1965, 6, 466 Post-mortem examination of a small intestine in the coeliac syndrome B. CREAMER AND P. LEPPARD From the Gastro-Intestinal Laboratory, St Thomas's Hospital, London EDITORIAL SYNOPSIS This
Gut, 1965, 6, 466 Post-mortem examination of a small intestine in the coeliac syndrome B. CREAMER AND P. LEPPARD From the Gastro-Intestinal Laboratory, St Thomas's Hospital, London EDITORIAL SYNOPSIS This
Malabsorption is characterized by defective absorption of: Fats fat- and water-soluble vitamins Proteins Carbohydrates Electrolytes Minerals water
 Malabsorption Malabsorption is characterized by defective absorption of: Fats fat- and water-soluble vitamins Proteins Carbohydrates Electrolytes Minerals water presents most commonly as chronic diarrhea
Malabsorption Malabsorption is characterized by defective absorption of: Fats fat- and water-soluble vitamins Proteins Carbohydrates Electrolytes Minerals water presents most commonly as chronic diarrhea
Coeliac disease with histological features of peptic duodenitis: Value of assessment of intraepithelial lymphocytes
 420 4 Clin Pathol 1993;46:420-424 Department of Pathology, St James's Hospital and Trinity College, Dublin Ireland M D Jeffers D O'B Hourihane Correspondence to: Professor D O'B Hourihane Accepted for
420 4 Clin Pathol 1993;46:420-424 Department of Pathology, St James's Hospital and Trinity College, Dublin Ireland M D Jeffers D O'B Hourihane Correspondence to: Professor D O'B Hourihane Accepted for
Kristin Kenrick, FRNZCGP Department of General Practice and Rural Health Dunedin School of Medicine (Supported by Coeliac New Zealand)
 Kristin Kenrick, FRNZCGP Department of General Practice and Rural Health Dunedin School of Medicine (Supported by Coeliac New Zealand) That you will go away thinking about your practice population, and
Kristin Kenrick, FRNZCGP Department of General Practice and Rural Health Dunedin School of Medicine (Supported by Coeliac New Zealand) That you will go away thinking about your practice population, and
Coeliac disease with mild mucosal abnormalities: a report of four patients
 Postgraduate Medical Journal (March 1977) 53, 134-138. Coeliac disease with mild mucosal abnormalities: a report of four patients BRIAN B. SCOTT M. S. LOSOWSKY M.D., M.R.C.P. M.D., F.R.C.P. University
Postgraduate Medical Journal (March 1977) 53, 134-138. Coeliac disease with mild mucosal abnormalities: a report of four patients BRIAN B. SCOTT M. S. LOSOWSKY M.D., M.R.C.P. M.D., F.R.C.P. University
FM CFS leaky gut April pag 1
 FM CFS leaky gut April 21 2018 pag 1 FIBROMYALGIA / CHRONIC FATIGUE SYNDROME AND LEAKY GUT. SUMMARY OF CLINICAL TRIAL DESIGN. Double-blind randomized placebo-controlled challenge with gluten and milk protein
FM CFS leaky gut April 21 2018 pag 1 FIBROMYALGIA / CHRONIC FATIGUE SYNDROME AND LEAKY GUT. SUMMARY OF CLINICAL TRIAL DESIGN. Double-blind randomized placebo-controlled challenge with gluten and milk protein
HDF Case Whipple s disease
 HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
Low gluten diet in the treatment of adult coeliac disease: effect on jejunal morphology and serum anti-gluten antibodies
 Gut, 1988, 29, 1564-1568 Low gluten diet in the treatment of adult coeliac disease: effect on jejunal morphology and serum anti-gluten antibodies A M P MONTGOMERY, A K J GOKA, P J KUMAR, M J G FARTHING,
Gut, 1988, 29, 1564-1568 Low gluten diet in the treatment of adult coeliac disease: effect on jejunal morphology and serum anti-gluten antibodies A M P MONTGOMERY, A K J GOKA, P J KUMAR, M J G FARTHING,
Laboratory Methods for Diagnosing Celiac Disease. Vijay Kumar, PhD, FACB IMMCO Diagnostics, Inc. Buffalo, NY
 Laboratory Methods for Diagnosing Celiac Disease Vijay Kumar, PhD, FACB IMMCO Diagnostics, Inc. Buffalo, NY Prevalence of Celiac Disease Group With Symptoms Adults Children Associated Symptoms Chronic
Laboratory Methods for Diagnosing Celiac Disease Vijay Kumar, PhD, FACB IMMCO Diagnostics, Inc. Buffalo, NY Prevalence of Celiac Disease Group With Symptoms Adults Children Associated Symptoms Chronic
Collagenous colitis associated with small intestinal villous atrophy
 (Gut, 1986, 27, 1394-1398 Case report Collagenous colitis associated with small intestinal villous atrophy I HAMILTON, S SANDERS, D HOPWOOD, AND I A D BOUCHIER From the University Department of Medicine
(Gut, 1986, 27, 1394-1398 Case report Collagenous colitis associated with small intestinal villous atrophy I HAMILTON, S SANDERS, D HOPWOOD, AND I A D BOUCHIER From the University Department of Medicine
A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue
 A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue UCSF Liver and Gastrointestinal Pathology Update Sept. 4, 2009 How to Go Wrong When Evaluating Small Bowel Biopsies, Based on
A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue UCSF Liver and Gastrointestinal Pathology Update Sept. 4, 2009 How to Go Wrong When Evaluating Small Bowel Biopsies, Based on
Histologic Follow-up of People With Celiac Disease on a Gluten-Free Diet Slow and Incomplete Recovery
 Anatomic Pathology / HISTOLOGIC FOLLOW-UP OF PEOPLE WITH CELIAC DISEASE ON A GLUTEN-FREE DIET Histologic Follow-up of People With Celiac Disease on a Gluten-Free Diet Slow and Incomplete Recovery Peter
Anatomic Pathology / HISTOLOGIC FOLLOW-UP OF PEOPLE WITH CELIAC DISEASE ON A GLUTEN-FREE DIET Histologic Follow-up of People With Celiac Disease on a Gluten-Free Diet Slow and Incomplete Recovery Peter
Coeliac Disease: Diagnosis and clinical features
 Coeliac Disease: Diagnosis and clinical features Australasian Gastrointestinal Pathology Society AGM 28 Oct 2016 Dr. Hooi Ee Gastroenterologist, Sir Charles Gairdner Hospital Coeliac disease Greek: koiliakos
Coeliac Disease: Diagnosis and clinical features Australasian Gastrointestinal Pathology Society AGM 28 Oct 2016 Dr. Hooi Ee Gastroenterologist, Sir Charles Gairdner Hospital Coeliac disease Greek: koiliakos
Expression of C-myc oncogene in coeliac disease
 J Clin Pathol 1987;40:307-311 Expression of C-myc oncogene in coeliac disease P J CICLITIRA,* J STEWART,J G EVAN,t D G D WIGHT, K SIKORAt From the *Division of Medicine, The Rayne Institute, The United
J Clin Pathol 1987;40:307-311 Expression of C-myc oncogene in coeliac disease P J CICLITIRA,* J STEWART,J G EVAN,t D G D WIGHT, K SIKORAt From the *Division of Medicine, The Rayne Institute, The United
Dr Kristin Kenrick. Senior Lecturer Dunedin School of Medicine
 Dr Kristin Kenrick Senior Lecturer Dunedin School of Medicine Kristin Kenrick, FRNZCGP Department of General Practice and Rural Health Dunedin School of Medicine (Supported by Coeliac New Zealand) Because
Dr Kristin Kenrick Senior Lecturer Dunedin School of Medicine Kristin Kenrick, FRNZCGP Department of General Practice and Rural Health Dunedin School of Medicine (Supported by Coeliac New Zealand) Because
HDF Case CRYPTOSPORIDIOSE
 HDF Case 986949 CRYPTOSPORIDIOSE 45 yo male with severe diarrhea. Known HIV positive. Endoscopic biopsy of duodenum, the colon and ileum. EXUDATIVE CHANGES GRANULAR BASOPHILIC BODIES Colonic biopsy shows
HDF Case 986949 CRYPTOSPORIDIOSE 45 yo male with severe diarrhea. Known HIV positive. Endoscopic biopsy of duodenum, the colon and ileum. EXUDATIVE CHANGES GRANULAR BASOPHILIC BODIES Colonic biopsy shows
The purpose of this paper is to investigate the. were carried out to determine the immunoglobulin
 Gut, 1974, 15, 284-288 Studies on the nature and significance of connective tissue antibodies in adult coeliac disease and Crohn's disease A. F. N. MAGALHAES, T. J. PETERS, AND WILLIAM F. DOE From the
Gut, 1974, 15, 284-288 Studies on the nature and significance of connective tissue antibodies in adult coeliac disease and Crohn's disease A. F. N. MAGALHAES, T. J. PETERS, AND WILLIAM F. DOE From the
Studies of intestinal fermentation in ulcerative
 Gut, 1968, 9, 51-56 Studies of intestinal fermentation in ulcerative colitis R. D. MONTGOMERY, A. C. FRAZER, CATHRYN HOOD, J. M. GOODHART, M. R. HOLLAND, AND R. SCHNEIDER From the Metabolic Unit, East
Gut, 1968, 9, 51-56 Studies of intestinal fermentation in ulcerative colitis R. D. MONTGOMERY, A. C. FRAZER, CATHRYN HOOD, J. M. GOODHART, M. R. HOLLAND, AND R. SCHNEIDER From the Metabolic Unit, East
Mucosal secretory IgA and secretory piece in adult
 Gut, 1973, 14, 778-783 Mucosal secretory IgA and secretory piece in adult coeliac disease R. J. SHINER AND JANET BALLARD' From the Medical Research Council Gastroenterology Unit, Central Middlesex Hospital,
Gut, 1973, 14, 778-783 Mucosal secretory IgA and secretory piece in adult coeliac disease R. J. SHINER AND JANET BALLARD' From the Medical Research Council Gastroenterology Unit, Central Middlesex Hospital,
Intestinal permeability in patients with coeliac disease and dermatitis herpetiformis
 Gut, 1985, 26, 1214-1219 Intestinal permeability in patients with coeliac disease and dermatitis herpetiformis I BJARNASON, M N MARSH, A PRICE, A J LEVI, AND T J PETERS From the Divisions of Clinical Sciences,
Gut, 1985, 26, 1214-1219 Intestinal permeability in patients with coeliac disease and dermatitis herpetiformis I BJARNASON, M N MARSH, A PRICE, A J LEVI, AND T J PETERS From the Divisions of Clinical Sciences,
Level 2. Non Responsive Celiac Disease KEY POINTS:
 Level 2 Non Responsive Celiac Disease KEY POINTS: Celiac Disease (CD) is an autoimmune condition triggered by ingestion of gluten leading to intestinal damage and a variety of clinical manifestations.
Level 2 Non Responsive Celiac Disease KEY POINTS: Celiac Disease (CD) is an autoimmune condition triggered by ingestion of gluten leading to intestinal damage and a variety of clinical manifestations.
ESIM: Winter School in Riga Case report
 ESIM: Winter School in Riga 2015 Case report Imanta Ozola Zālīte Pauls Stradins Clinical University Hospital Latvia 29.01.2015. January, 2006 32 y., man 2-3 weeks fatigue fluidal stool 2 times per day
ESIM: Winter School in Riga 2015 Case report Imanta Ozola Zālīte Pauls Stradins Clinical University Hospital Latvia 29.01.2015. January, 2006 32 y., man 2-3 weeks fatigue fluidal stool 2 times per day
Definition. Celiac disease is an immune-mediated enteropathy caused by a permanent sensitivity to gluten in genetically susceptible individuals.
 Definition 1 Definition Celiac disease is an immune-mediated enteropathy caused by a permanent sensitivity to gluten in genetically susceptible individuals. It occurs in symptomatic subjects with gastrointestinal
Definition 1 Definition Celiac disease is an immune-mediated enteropathy caused by a permanent sensitivity to gluten in genetically susceptible individuals. It occurs in symptomatic subjects with gastrointestinal
The effect of coeliac disease upon bile salts
 Gut, 1973, 14, 24-2 T. S. LOW-BEER,1 K. W. HEATON, E. W. POMARE, AND A. E. READ From the University Department of Medicine, Bristol Royal Infirmary SUMMARY The size and composition of the bile salt pool
Gut, 1973, 14, 24-2 T. S. LOW-BEER,1 K. W. HEATON, E. W. POMARE, AND A. E. READ From the University Department of Medicine, Bristol Royal Infirmary SUMMARY The size and composition of the bile salt pool
Rectal mucosal plasma cells in inflammatory bowel
 Gut, 1983, 24, 519-524 Rectal mucosal plasma cells in inflammatory bowel disease B B SCOTT, ANNE GOODALL, P STEPHENSON, AND D JENKINS From the Departments of Medicine and Pathology, Lincoln County Hospital,
Gut, 1983, 24, 519-524 Rectal mucosal plasma cells in inflammatory bowel disease B B SCOTT, ANNE GOODALL, P STEPHENSON, AND D JENKINS From the Departments of Medicine and Pathology, Lincoln County Hospital,
Involvement of the small intestine in systemic mast
 Gut, 1975, 16, 918-924 Involvement of the small intestine in systemic mast cell disease BRIAN B. SCOTT, G. J. HARDY, AND M. S. LOSOWSKY From the University Department of Medicine and Department ofpathology,
Gut, 1975, 16, 918-924 Involvement of the small intestine in systemic mast cell disease BRIAN B. SCOTT, G. J. HARDY, AND M. S. LOSOWSKY From the University Department of Medicine and Department ofpathology,
CLINICAL REVIEW. and small bowel carcinoma SIMON KENWRIGHT* M.R.C.P.
 Postgraduate Medical Journal (November 1972) 48, 673-677. Coeliac disease CLINICAL REVIEW and small bowel carcinoma SIMON KENWRIGHT* M.R.C.P. Department of Gastro-enterology, Frenchay Hospital, Bristol
Postgraduate Medical Journal (November 1972) 48, 673-677. Coeliac disease CLINICAL REVIEW and small bowel carcinoma SIMON KENWRIGHT* M.R.C.P. Department of Gastro-enterology, Frenchay Hospital, Bristol
Ultrastructural changes suggestive of immune. following gluten challenge. reactions in the jejunal mucosa of coeliac children
 Gut, 1973, 14, 1-12 Ultrastructural changes suggestive of immune reactions in the jejunal mucosa of coeliac children following gluten challenge MARGOT SHINER' From the Medical Research Council, Gastroenterology
Gut, 1973, 14, 1-12 Ultrastructural changes suggestive of immune reactions in the jejunal mucosa of coeliac children following gluten challenge MARGOT SHINER' From the Medical Research Council, Gastroenterology
Mucosal Immunology Sophomore Dental and Optometry Microbiology Section I: Immunology. Robin Lorenz
 Mucosal Immunology Sophomore Dental and Optometry Microbiology Section I: Immunology Robin Lorenz rlorenz@uab.edu Why do we Need to Understand How the Mucosal Immune System Works? The mucosa is the major
Mucosal Immunology Sophomore Dental and Optometry Microbiology Section I: Immunology Robin Lorenz rlorenz@uab.edu Why do we Need to Understand How the Mucosal Immune System Works? The mucosa is the major
General Structure of Digestive Tract
 Dr. Nabil Khouri General Structure of Digestive Tract Common Characteristics: Hollow tube composed of a lumen whose diameter varies. Surrounded by a wall made up of 4 principal layers: Mucosa Epithelial
Dr. Nabil Khouri General Structure of Digestive Tract Common Characteristics: Hollow tube composed of a lumen whose diameter varies. Surrounded by a wall made up of 4 principal layers: Mucosa Epithelial
A CELL-MEDIATED IMMUNE MODEL OF INFLAMMATORY BOWEL DISEASE IN THE RABBIT
 0016-5085/7501-0029$02.00/0 GASTROENTEROLOGY 75:29-33, 1978 Copyright 1978 by the American Gastroenterological Association Vol. 75, No.1 Printed in U.8A. A CELL-MEDIATED IMMUNE MODEL OF INFLAMMATORY BOWEL
0016-5085/7501-0029$02.00/0 GASTROENTEROLOGY 75:29-33, 1978 Copyright 1978 by the American Gastroenterological Association Vol. 75, No.1 Printed in U.8A. A CELL-MEDIATED IMMUNE MODEL OF INFLAMMATORY BOWEL
Dissecting Microscope Appearance of
 Arch. Dis. Childh., 1967, 42, 626. Dissecting Microscope Appearance of Small Bowel Mucosa in Children JOHN WALKER-SMITH From Professorial Unit, Royal Alexandra Hospital for Children, Camperdown, Sydney,
Arch. Dis. Childh., 1967, 42, 626. Dissecting Microscope Appearance of Small Bowel Mucosa in Children JOHN WALKER-SMITH From Professorial Unit, Royal Alexandra Hospital for Children, Camperdown, Sydney,
Index. in tissue, 87-89
 ANA titers, 79-84 Adult atopic dermatitis, 239 Allergens, contact dermatitis, 253 Allergic contact dermatitis Acontact sensitivity, cellular participants in, 258 factors influencing incidence of, 254 'hardening',
ANA titers, 79-84 Adult atopic dermatitis, 239 Allergens, contact dermatitis, 253 Allergic contact dermatitis Acontact sensitivity, cellular participants in, 258 factors influencing incidence of, 254 'hardening',
HYPOGAMMAGLOBULlNAEMIA WITH NODULAR LYMPHOID HYPERPLASIA OF THE SMALL INTESTINE
 J. roy. Army med. Cps. 1977. 123,37-41 HYPOGAMMAGLOBULlNAEMIA WITH NODULAR LYMPHOID HYPERPLASIA OF THE SMALL INTESTINE Major W. M. WALLACE, M.B., B.Ch., M.R.C. P., R.A.M.C. Royal Army Medical Col/ege.
J. roy. Army med. Cps. 1977. 123,37-41 HYPOGAMMAGLOBULlNAEMIA WITH NODULAR LYMPHOID HYPERPLASIA OF THE SMALL INTESTINE Major W. M. WALLACE, M.B., B.Ch., M.R.C. P., R.A.M.C. Royal Army Medical Col/ege.
Prevalence of lactase deficiency in British adults
 Prevalence of lactase deficiency in British adults Gut, 1984, 25, 163-167 ANNE FERGUSON, DOROTHY M MACDONALD, AND W GORDON BRYDON From the Gastro-Intestinal Unit, University of Edinburgh, and Western General
Prevalence of lactase deficiency in British adults Gut, 1984, 25, 163-167 ANNE FERGUSON, DOROTHY M MACDONALD, AND W GORDON BRYDON From the Gastro-Intestinal Unit, University of Edinburgh, and Western General
Protein synthesis by cultured jejunal mucosa from
 Gut, 1981, 22, 623-627 Protein synthesis by cultured jejunal mucosa from control subjects and patients with coeliac disease P E JONES,* C L L'HIRONDEL,t AND T J PETERS$ From the Department of Medicine,
Gut, 1981, 22, 623-627 Protein synthesis by cultured jejunal mucosa from control subjects and patients with coeliac disease P E JONES,* C L L'HIRONDEL,t AND T J PETERS$ From the Department of Medicine,
Scalloped Valvulae Conniventes: An Endoscopic Marker of Celiac Sprue
 GASTROENTEROLOGY 1988;95:1518-22 Scalloped Valvulae Conniventes: An Endoscopic Marker of Celiac Sprue MANSOUR JABBARI, GARY WILD, CARL A. GORESKY, DONALD S. PAL Y, JOHN O. LOUGH, D. PAUL CLELAND, and DOUGLAS
GASTROENTEROLOGY 1988;95:1518-22 Scalloped Valvulae Conniventes: An Endoscopic Marker of Celiac Sprue MANSOUR JABBARI, GARY WILD, CARL A. GORESKY, DONALD S. PAL Y, JOHN O. LOUGH, D. PAUL CLELAND, and DOUGLAS
A total of 111 subjects admitted consecutively in a. of diseases associated with malabsorption. Informed
 J Clin Pathol 1981;34:174-178 One-hour serum ylose as an absorption test in the tropics PG HILL, IN ROSS,* R JACOB, S JYOTHEESWARAN, AND VI MATHAN From the Wellcome Research Unit and The Gastroenterology
J Clin Pathol 1981;34:174-178 One-hour serum ylose as an absorption test in the tropics PG HILL, IN ROSS,* R JACOB, S JYOTHEESWARAN, AND VI MATHAN From the Wellcome Research Unit and The Gastroenterology
Malignant histiocytosis of the intestine: the early histological lesion
 Gut, 1980, 21, 381-386 Malignant histiocytosis of the intestine: the early histological lesion P ISAACSON From the Department of Pathology, Faculty of Medicine, Southampton University Hospital, Southampton
Gut, 1980, 21, 381-386 Malignant histiocytosis of the intestine: the early histological lesion P ISAACSON From the Department of Pathology, Faculty of Medicine, Southampton University Hospital, Southampton
Dermatitis herpetiformis: jejunal findings and skin response to gluten free diet
 Archives of Disease in Childhood, 1984, 59, 517-522 Dermatitis herpetiformis: jejunal findings and skin response to gluten free diet T REUNALA, I KOSNAI, S KARPATI, P KUITUNEN, E TOROK, AND E SAVILAHTI
Archives of Disease in Childhood, 1984, 59, 517-522 Dermatitis herpetiformis: jejunal findings and skin response to gluten free diet T REUNALA, I KOSNAI, S KARPATI, P KUITUNEN, E TOROK, AND E SAVILAHTI
Coeliac disease during the teenage period: The value
 Gut, 1974, 15, 450457 Coeliac disease during the teenage period: The value of serial serum folate estimations D. G. WEIR' AND D. O'B. HOURIHANE From the Departments of Clinical Medicine and Pathology,
Gut, 1974, 15, 450457 Coeliac disease during the teenage period: The value of serial serum folate estimations D. G. WEIR' AND D. O'B. HOURIHANE From the Departments of Clinical Medicine and Pathology,
Transient paraproteinaemia in a patient with
 Transient paraproteinaemia in a patient with coeliac disease Gut, 1976,17, 735-739 A. S. PENA, JANNY v. NIEUWKOOP, H. R. E. SCHUIT, W. TH. J. M. HEKKENS, AND A. J. CH. HAEX From the Departments of Gastroenterology
Transient paraproteinaemia in a patient with coeliac disease Gut, 1976,17, 735-739 A. S. PENA, JANNY v. NIEUWKOOP, H. R. E. SCHUIT, W. TH. J. M. HEKKENS, AND A. J. CH. HAEX From the Departments of Gastroenterology
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT.
 PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
Southern Derbyshire Shared Care Pathology Guidelines. Coeliac Disease
 Southern Derbyshire Shared Care Pathology Guidelines Coeliac Disease Purpose of Guideline When and how to investigate patients for Coeliac Disease What the results mean When and how to refer patients Monitoring
Southern Derbyshire Shared Care Pathology Guidelines Coeliac Disease Purpose of Guideline When and how to investigate patients for Coeliac Disease What the results mean When and how to refer patients Monitoring
without gut symptoms and in normal adults
 J Clin Pathol 1981;34:386-392 Jejunal mucosal morphometry in children with and without gut symptoms and in normal adults FJ PENNA,* ID HILL,t D KINGSTON,* K ROBERTSON,+ G SLAVIN,+ AND M SHINER* From the
J Clin Pathol 1981;34:386-392 Jejunal mucosal morphometry in children with and without gut symptoms and in normal adults FJ PENNA,* ID HILL,t D KINGSTON,* K ROBERTSON,+ G SLAVIN,+ AND M SHINER* From the
Malabsorption in rheumatoid disease
 Ann. rheum. Dis. (1971), 3, 626 Malabsorption in rheumatoid disease N. H. DYER, M. J. KENDALL, AND C. F. HAWKINS Queen Elizabeth Hospital, Birmingham 15 Rheumatoid disease is a systemic disorder involving
Ann. rheum. Dis. (1971), 3, 626 Malabsorption in rheumatoid disease N. H. DYER, M. J. KENDALL, AND C. F. HAWKINS Queen Elizabeth Hospital, Birmingham 15 Rheumatoid disease is a systemic disorder involving
Hypersensitivity reactions in the small intestine
 Hypersensitivity reactions in the small intestine 2 Effects of allograft rejection on mucosal architecture and lymphoid cell infiltrate T. T. MAcDONALD' AND ANNE FERGUSON Gut, 1976, 17, 81-91 From the
Hypersensitivity reactions in the small intestine 2 Effects of allograft rejection on mucosal architecture and lymphoid cell infiltrate T. T. MAcDONALD' AND ANNE FERGUSON Gut, 1976, 17, 81-91 From the
Done By : shady soghayr
 Done By : shady soghayr Malabsorption Malabsorption is characterized by defective absorption of: Fats fat- and water-soluble vitamins Proteins Carbohydrates Electrolytes Minerals Water presents most commonly
Done By : shady soghayr Malabsorption Malabsorption is characterized by defective absorption of: Fats fat- and water-soluble vitamins Proteins Carbohydrates Electrolytes Minerals Water presents most commonly
Clinical presentation of coeliac disease in
 The Ulster Medical Joumal, Volume 54, No. 2, pp. 140-147, October 1985. Clinical presentation of coeliac disease in adult gastroenterological practice S Boyd, B J Collins, P M Bell, A H G Love Accepted
The Ulster Medical Joumal, Volume 54, No. 2, pp. 140-147, October 1985. Clinical presentation of coeliac disease in adult gastroenterological practice S Boyd, B J Collins, P M Bell, A H G Love Accepted
Lymphocytic Gastritis, Isolated Type Occurring in Family Members. A Case Report.
 Lymphocytic Gastritis, Isolated Type Occurring in Family Members. A Case Report. Alan Shienbaum, DO; AndriyPavlenko, MD; Jun Liu, MD, PhD; Janusz J Godyn, MD. Pathology Department, Kennedy University Hospitals,
Lymphocytic Gastritis, Isolated Type Occurring in Family Members. A Case Report. Alan Shienbaum, DO; AndriyPavlenko, MD; Jun Liu, MD, PhD; Janusz J Godyn, MD. Pathology Department, Kennedy University Hospitals,
Bacteriology. Mycology. Patient: SAMPLE PATIENT DOB: Sex: MRN: Rare. Rare. Positive. Brown. Negative *NG. Negative
 Patient: SAMPLE PATIENT DOB: Sex: MRN: 3.2 0.9-26.8 U/g 1.2 0.2-3.3 mg/g 2.2 1.3-8.6 micromol/g 1.1 1.3-23.7 mg/g 1.1 0.2-3.5 mg/g Rare 1.0 0.2-8.8 mg/g Rare 4.4 2.6-32.4 mg/g 64.6 >= 13.6 micromol/g Bacteriology
Patient: SAMPLE PATIENT DOB: Sex: MRN: 3.2 0.9-26.8 U/g 1.2 0.2-3.3 mg/g 2.2 1.3-8.6 micromol/g 1.1 1.3-23.7 mg/g 1.1 0.2-3.5 mg/g Rare 1.0 0.2-8.8 mg/g Rare 4.4 2.6-32.4 mg/g 64.6 >= 13.6 micromol/g Bacteriology
GPMP and TCA Coeliac disease
 MP and TCA Coeliac disease ITEM: prepares MP (721) REVIEWS MP (732) prepared TCA (723) REVIEW TCA (732) PATIENT DETAILS: DETAILS: DATE PREPARED: Does a current management plan or Team care arrangement
MP and TCA Coeliac disease ITEM: prepares MP (721) REVIEWS MP (732) prepared TCA (723) REVIEW TCA (732) PATIENT DETAILS: DETAILS: DATE PREPARED: Does a current management plan or Team care arrangement
EVIDENCE THAT ACTIVATED MUCOSAL T CELLS PLAY A ROLE IN THE PATHOGENESIS OF ENTEROPATHY IN HUMAN SMALL INTESTINE
 Published Online: 1 April, 1988 Supp Info: http://doi.org/10.1084/jem.167.4.1341 Downloaded from jem.rupress.org on September 23, 2018 EVIDENCE THAT ACTIVATED MUCOSAL T CELLS PLAY A ROLE IN THE PATHOGENESIS
Published Online: 1 April, 1988 Supp Info: http://doi.org/10.1084/jem.167.4.1341 Downloaded from jem.rupress.org on September 23, 2018 EVIDENCE THAT ACTIVATED MUCOSAL T CELLS PLAY A ROLE IN THE PATHOGENESIS
Mucosal immunity Reddy April Deveshni Reddy Allergy Meeting 13 April 2012
 Deveshni Reddy Allergy Meeting 13 April First recorded by Hippocrates over 2000 years ago. 1921: Prausnitz and Kustner demonstrated that substance responsible for Kustner s fish allergy was present in
Deveshni Reddy Allergy Meeting 13 April First recorded by Hippocrates over 2000 years ago. 1921: Prausnitz and Kustner demonstrated that substance responsible for Kustner s fish allergy was present in
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE SCOPE. Coeliac disease: recognition, assessment and management of coeliac disease
 Appendix B: NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Coeliac disease: recognition, assessment and management of coeliac disease 1.1 Short title Coeliac disease 2 The remit
Appendix B: NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Coeliac disease: recognition, assessment and management of coeliac disease 1.1 Short title Coeliac disease 2 The remit
Coeliac disease in Sudanese children
 Coeliac disease in Sudanese children G. I. SULIMAN1 Gut, 1978, 19, 121-125 From the Department ofpaediatrics and Child Health, Khartoum Civil Hospital, Khartoum, Sudan SUMMARY Coeliac disease has not hitherto
Coeliac disease in Sudanese children G. I. SULIMAN1 Gut, 1978, 19, 121-125 From the Department ofpaediatrics and Child Health, Khartoum Civil Hospital, Khartoum, Sudan SUMMARY Coeliac disease has not hitherto
IgA: Biology and deficiency
 Introduction to IgA First described in 1953 IgA: Biology and deficiency Dr Sarah Sasson SydPATH Registrar 14 th July 2014 Most abundant and heterogeneous antibody isotype produced in the body 66mg/kg/day-
Introduction to IgA First described in 1953 IgA: Biology and deficiency Dr Sarah Sasson SydPATH Registrar 14 th July 2014 Most abundant and heterogeneous antibody isotype produced in the body 66mg/kg/day-
Refractory celiac disease (RCD) KASSEM BARADA LEBANESE SOCIETY OF GASTROENTEROLOGY NOVEMBER, 2014
 Refractory celiac disease (RCD) KASSEM BARADA LEBANESE SOCIETY OF GASTROENTEROLOGY NOVEMBER, 2014 Case scenario (1) A 49 year woman presents with intermittent watery diarrhea and bloating of two years
Refractory celiac disease (RCD) KASSEM BARADA LEBANESE SOCIETY OF GASTROENTEROLOGY NOVEMBER, 2014 Case scenario (1) A 49 year woman presents with intermittent watery diarrhea and bloating of two years
Coeliac Disease in Children and Adolescents with Type 1 Diabetes Mellitus
 Clin Pediatr Endocrinol 1998; 7(2), 125-129 Copyright 1998 by The Japanese Society for Pediatric Endocrinology Coeliac Disease in Children and Adolescents with Type 1 Diabetes Mellitus Francesco Chiarelli,
Clin Pediatr Endocrinol 1998; 7(2), 125-129 Copyright 1998 by The Japanese Society for Pediatric Endocrinology Coeliac Disease in Children and Adolescents with Type 1 Diabetes Mellitus Francesco Chiarelli,
Giardiasis and coeliac disease
 Archives of Disease in Childhood, 1973, 48, 414. F. CARSWELL, A. A. M. GIBSON, and T. A. McALLISTER From the Departments of Child Health, Pathology and Bacteriology, Royal Hospital for Sick Children, Yorkhill,
Archives of Disease in Childhood, 1973, 48, 414. F. CARSWELL, A. A. M. GIBSON, and T. A. McALLISTER From the Departments of Child Health, Pathology and Bacteriology, Royal Hospital for Sick Children, Yorkhill,
Invited Re vie W. The nature and implication of intestinal endocrine cell changes in coeliac disease. Histology and Histopathology
 Histol Histopathol (1 998) 13: 1069-1 075 http://www.ehu.es/histol-histopathol Histology and Histopathology Invited Re vie W The nature and implication of intestinal endocrine cell changes in coeliac disease
Histol Histopathol (1 998) 13: 1069-1 075 http://www.ehu.es/histol-histopathol Histology and Histopathology Invited Re vie W The nature and implication of intestinal endocrine cell changes in coeliac disease
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Rectal mucosa in cows' milk allergy
 Archives of Disease in Childhood, 1989, 64, 1256-1260 Rectal mucosa in cows' milk allergy N IYNGKARAN,* M YADAVt AND C G BOEYt Departments of *Paediatrics and tpathology, University Hospital, and tdepartment
Archives of Disease in Childhood, 1989, 64, 1256-1260 Rectal mucosa in cows' milk allergy N IYNGKARAN,* M YADAVt AND C G BOEYt Departments of *Paediatrics and tpathology, University Hospital, and tdepartment
Figure 2: Lymph node Cortical follicular (F) and paracortical (PC) atrophy, with narrowing of the cortex relative to the medulla (M).
 Figure 1: Lymph node Follicular hyperplasia, with expansion of the follicular germinal centres (F) by large blast cells. Paracortical hyperplasia, with expansion of the paracortex (PC) by small lymphocytes.
Figure 1: Lymph node Follicular hyperplasia, with expansion of the follicular germinal centres (F) by large blast cells. Paracortical hyperplasia, with expansion of the paracortex (PC) by small lymphocytes.
Malabsorption: etiology, pathogenesis and evaluation
 Malabsorption: etiology, pathogenesis and evaluation Peter HR Green NORMAL ABSORPTION Coordination of gastric, small intestinal, pancreatic and biliary function Multiple mechanisms Fat protein carbohydrate
Malabsorption: etiology, pathogenesis and evaluation Peter HR Green NORMAL ABSORPTION Coordination of gastric, small intestinal, pancreatic and biliary function Multiple mechanisms Fat protein carbohydrate
Coeliac Disease: Symptoms, Diagnosis, Treatment and Management
 Coeliac Disease: Symptoms, Diagnosis, Treatment and Management Dr Matthew Kurien Senior Clinical Lecturer and Honorary Consultant Gastroenterologist, University of Sheffield Benign Diseases Talk Outline
Coeliac Disease: Symptoms, Diagnosis, Treatment and Management Dr Matthew Kurien Senior Clinical Lecturer and Honorary Consultant Gastroenterologist, University of Sheffield Benign Diseases Talk Outline
COMMON VARIABLE IMMUNODEFICIENCY
 COMMON VARIABLE IMMUNODEFICIENCY This booklet is intended for use by patients and their families and should not replace advice from a clinical immunologist. 1 COMMON VARIABLE IMMUNODEFICIENCY Also available
COMMON VARIABLE IMMUNODEFICIENCY This booklet is intended for use by patients and their families and should not replace advice from a clinical immunologist. 1 COMMON VARIABLE IMMUNODEFICIENCY Also available
Tuesday 10 th April 2018 Dr Rukhsana Hussain. Disclaimers apply:
 Tuesday 10 th April 2018 Dr Rukhsana Hussain What is Non-Coeliac Gluten Sensitivity (NCGS)? Symptoms Pathophysiology Diagnosis Treatment Summary NCGS is a condition in which consumption of gluten leads
Tuesday 10 th April 2018 Dr Rukhsana Hussain What is Non-Coeliac Gluten Sensitivity (NCGS)? Symptoms Pathophysiology Diagnosis Treatment Summary NCGS is a condition in which consumption of gluten leads
Biomarkers of GI tract diseases. By Dr. Gouse Mohiddin Shaik
 By Dr. Gouse Mohiddin Shaik Introduction The gastrointestinal (GI) tract is a complex system performing multiple biological functions which are anatomically distributed Site for food processing and absorption
By Dr. Gouse Mohiddin Shaik Introduction The gastrointestinal (GI) tract is a complex system performing multiple biological functions which are anatomically distributed Site for food processing and absorption
possible in the present state of our knowledge. history of frequent, loose bowel actions for two relapse on its reintroduction is also necessary for
 Gut, 1970, 11, 743-747 A case of small-intestinal mucosal atrophy R. E. BARRY, JOHN S. MORRIS, AND A. E. A. READ From the Department of Medicine, Bristol Royal Infirmary SUMMARY A patient is described
Gut, 1970, 11, 743-747 A case of small-intestinal mucosal atrophy R. E. BARRY, JOHN S. MORRIS, AND A. E. A. READ From the Department of Medicine, Bristol Royal Infirmary SUMMARY A patient is described
Lactose Intolerance in Childhood Coeliac Disease
 Arch. Dis. Childh., 1968, 43, 433. Lactose Intolerance in Childhood Coeliac Disease Assessment of its Incidence and Importance ALEXANDER S. McNEISH and ELIZABETH M. SWEET From the Royal Hospital for Sick
Arch. Dis. Childh., 1968, 43, 433. Lactose Intolerance in Childhood Coeliac Disease Assessment of its Incidence and Importance ALEXANDER S. McNEISH and ELIZABETH M. SWEET From the Royal Hospital for Sick
Quantification of enterochromaffin cells with
 Archives of Disease in Childhood, 1984, 59, 523-527 Quantification of enterochromaffin cells with serotonin immunoreactivity in the duodenal mucosa in coeliac disease E E WHEELER AND D N CHALLACOMBE Somerset
Archives of Disease in Childhood, 1984, 59, 523-527 Quantification of enterochromaffin cells with serotonin immunoreactivity in the duodenal mucosa in coeliac disease E E WHEELER AND D N CHALLACOMBE Somerset
embedded tissue-sections has the advantage of permanence of the sections and is more suitable for
 Gut, 1980, 21, 941-947 Immunoglobulin containing cells in inflammatory bowel disease of the colon: a morphometric and immunohistochemical study P C M ROSEKRANS,* C J L M MEIJER, A M VAN DER WAL, C J CORNELISSE,
Gut, 1980, 21, 941-947 Immunoglobulin containing cells in inflammatory bowel disease of the colon: a morphometric and immunohistochemical study P C M ROSEKRANS,* C J L M MEIJER, A M VAN DER WAL, C J CORNELISSE,
Lower Gastrointestinal Tract KNH 406
 Lower Gastrointestinal Tract KNH 406 Lower GI Tract A&P Small Intestine Anatomy Duodenum, jejunum, ileum Maximum surface area for digestion and absorption Specialized enterocytes from stem cells of crypts
Lower Gastrointestinal Tract KNH 406 Lower GI Tract A&P Small Intestine Anatomy Duodenum, jejunum, ileum Maximum surface area for digestion and absorption Specialized enterocytes from stem cells of crypts
Digestive System 2. Lecture 12. Pathology and Clinical Science 1 (BIOC211) Department of Bioscience. endeavour.edu.au
 Digestive System 2 Lecture 12 Pathology and Clinical Science 1 (BIOC211) Department of Bioscience Text Reference: Grossman, S.C. & Porth, C.M. (2014). Porth s Pathophysiology: concepts of altered health
Digestive System 2 Lecture 12 Pathology and Clinical Science 1 (BIOC211) Department of Bioscience Text Reference: Grossman, S.C. & Porth, C.M. (2014). Porth s Pathophysiology: concepts of altered health
In the name of Allah The most gracious The most merciful
 In the name of Allah The most gracious The most merciful By Dr.Nancy Abd El Fattah Assistant prof. of internal medicine 3-6 m in length 300m2 in surface area Upper 40% duodenum & Jejunum Folds villi micro
In the name of Allah The most gracious The most merciful By Dr.Nancy Abd El Fattah Assistant prof. of internal medicine 3-6 m in length 300m2 in surface area Upper 40% duodenum & Jejunum Folds villi micro
ANTIBODIES Jiri Mestecky, M.D., Ph.D. - Lecturer
 ANTIBODIES Jiri Mestecky, M.D., Ph.D. - Lecturer Distribution in body fluids: secretions plasma (serum), tears, saliva, milk, genitourinary, and intestinal Cells producing antibodies and their tissue distribution:
ANTIBODIES Jiri Mestecky, M.D., Ph.D. - Lecturer Distribution in body fluids: secretions plasma (serum), tears, saliva, milk, genitourinary, and intestinal Cells producing antibodies and their tissue distribution:
partial gastrectomy Western Infirmary, Glasgow ml. water; two hours later 1,000 ptg. vitamin B12 was given to detect any deterioration in vitro.
 Gut, 1963, 4, 32 The reliability and reproducibility of the Schilling test in primary malabsorptive disease and after partial gastrectomy J.. ADAMS AND E. JUNE CARTWRIGHT rom the Western Infirmary, Glasgow
Gut, 1963, 4, 32 The reliability and reproducibility of the Schilling test in primary malabsorptive disease and after partial gastrectomy J.. ADAMS AND E. JUNE CARTWRIGHT rom the Western Infirmary, Glasgow
Lymphocyte subpopulations in adult coeliac disease
 Gut, 1978, 19, 892-897 Lymphocyte subpopulations in adult coeliac disease A. W. BULLEN AND M. S. LOSOWSKY From the Department of Medicine, St James's Hospital, Leeds SUMMARY Rosetting techniques were used
Gut, 1978, 19, 892-897 Lymphocyte subpopulations in adult coeliac disease A. W. BULLEN AND M. S. LOSOWSKY From the Department of Medicine, St James's Hospital, Leeds SUMMARY Rosetting techniques were used
NICE guideline Published: 2 September 2015 nice.org.uk/guidance/ng20
 Coeliac disease: recognition, assessment and management NICE guideline Published: 2 September 2015 nice.org.uk/guidance/ng20 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Coeliac disease: recognition, assessment and management NICE guideline Published: 2 September 2015 nice.org.uk/guidance/ng20 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Small intestine. Small intestine
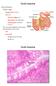 General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
Partial villous atrophy in nutritional megaloblastic
 J. clin Path., 1971, 24, 131-135 Partial villous atrophy in nutritional megaloblastic anaemia corrected by folic acid therapy D. W. DAWSON From Crumpsall Hospital, Manchester SYNOPSIS A patient with megaloblastic
J. clin Path., 1971, 24, 131-135 Partial villous atrophy in nutritional megaloblastic anaemia corrected by folic acid therapy D. W. DAWSON From Crumpsall Hospital, Manchester SYNOPSIS A patient with megaloblastic
Three-dimensional structure of the human small intestinal mucosa in health and disease
 Gut, 1969, 10, 6-12 Three-dimensional structure of the human small intestinal mucosa in health and disease C. A. LOEHRY AND B. CREAMER From the Gastrointestinal Laboratory, St Thomas' Hospital, London
Gut, 1969, 10, 6-12 Three-dimensional structure of the human small intestinal mucosa in health and disease C. A. LOEHRY AND B. CREAMER From the Gastrointestinal Laboratory, St Thomas' Hospital, London
These studies were made at a time when it was not. yet fully established that mast cells could react with
 Gut, 1975, 16, 861-866 Mast cells and immunoglobulin E in inflammatory bowel disease G. LLOYD1, F. H. Y. GREEN, H. FOX, V. MANI2, AND L. A. TURNBERG2 From the Department ofpathology, University of Manchester,
Gut, 1975, 16, 861-866 Mast cells and immunoglobulin E in inflammatory bowel disease G. LLOYD1, F. H. Y. GREEN, H. FOX, V. MANI2, AND L. A. TURNBERG2 From the Department ofpathology, University of Manchester,
Preface and outline of the thesis
 Preface Celiac disease (CD) is characterized by a chronic immune reaction in the small intestine to the gluten proteins that are present in a (Western) daily diet, derived from wheat, barley and rye. It
Preface Celiac disease (CD) is characterized by a chronic immune reaction in the small intestine to the gluten proteins that are present in a (Western) daily diet, derived from wheat, barley and rye. It
