Larry Rosenberger, CNP
|
|
|
- Eugenia Haynes
- 5 years ago
- Views:
Transcription
1 Larry Rosenberger, APRN CNP Julie Melendez, APRN CNP Larry Rosenberger, CNP Northwest Ohio Orthopedics and Sports Medicine Findlay, Ohio Julie Melendez, CNP Northwest Ohio Orthopedics and Sports Medicine Findlay, Ohio 1
2 Objectives Discuss Common Musculoskeletal pathologies and indications for intraarticular and periarticular injections. Explore musculoskeletal anatomy and identify anatomic landmarks necessary to perform successful intraarticular and periarticular injections. Identify common intraarticular and periarticular injection techniques. List important codes for billing and reimbursement. Objectives (RX)Discuss Pharmacological Principles of common injectables including local anesthetics and corticosteroids. Demonstrate proper intraarticular and periarticular injection techiques. Introduction Musculoskeletal disorders are the most debilitating chronic medical conditions Comprise up to 60% of outpatient office visits Studies suggest primary care providers are inadequately prepared to care for musculoskeletal problems (Benham & Geier, 2014, p. 603) 2
3 Intraarticular and Periarticular injections/aspiration Indications Diagnosis Aspiration of synovial fluid Analysis Cell count, crystals, cultures Injection of Lidocaine Differentiate pathology Neers Sign Therapuetic Relieves pain from acute/chronic musculoskeletal conditions. Injection and/or aspiration (Mcnabb, 2015, p. 4) Intraarticular and Periarticular injections/aspiration Contraindications Absolute Uncooperative Patient Allergy to medication or preservative Injecting critical weight bearing tendons Relative Major arteries, veins, pleural surfaces Concurrent Anticoagulation Joint replacement Diabetes and Glaucoma(corticosteroids) (Mcnabb, 2015, p. 5 6) Intraarticular and Periarticular injections/aspiration Synovial Fluid Analysis Usually Clear and transparent Differentiate cause for joint effusion Cell count Crystals Cultures WBC count Noninflammatory <2000 cells/mm² Inflammatory >2000 cells/mm² Infective > 2000 cells/mm² >50 polymorhonucleic cells Hemarthosis Fracture, ligament tear (Mcnabb, 2015, p. 7 9) 3
4 Common Injectables Local Anesthetics Lidocaine Bupivicaine Corticosteroids Soluble Insoluble Viscosupplementation Platelet Rich Plasma Local Anesthetics Lidocaine Mechanism of action Inhibits sodium ion channels, stabilizes neuronal cell membrane, inhibiting nerve impulse Metabolism liver, CYP450 1A2, 3A4 substrate Excretion Urine Onset Rapid Half life hours Local Anesthetics Lidocaine Dosage Max 4.5 mg/kg/dose, up to 300 mg/total Contraindications Hypersensitivity Hepatic impairment Adverse reactions Injection site pain Tinnitus arrhythmia 4
5 Local Anesthetics Marcaine Mechanism of action Inhibits sodium ion channels, stabilizes neuronal cell membrane, inhibiting nerve impulse Metabolism liver, 3A4 substrate Excretion Urine Onset Slow Half life 3.5 hours Local Anesthetics Bupivicaine Dosage Max 2 mg/kg, up to 275 mg/dose Contraindications Hypersensitivity Hepatic impairment Adverse reactions Injection site pain Tinnitus Arrhythmia (Epocrates, 2017) Corticosteroids Mechanism of action Complex Inhibits cytokines and inflammatory mediators Metabolism Liver, CYP 3A4 Excretion Urine Potency Measured against Hydrocortisone Solubility Insoluble Esters, microcrystalline suspensions Soluble Non esters, nonparticulate (Epocrates, 2017, Mcnabb, 2015, p. 13) 5
6 Corticosteroids Caution Hypersensitivity Latent infections HTN DM Glaucoma Adverse reactions Anaphylaxis Hyperglycemia CHF PUD Facial flushing Headache Skin and fatty atrophy (Epocrates, 2017, Mcnabb, 2015, p. 13) Corticosteroids Corticosteroid Relative potency Solubility (%Wt/Vol) Hydrocortisone Acetate (Hydrocortisone) Triamcinolone Acetonide (Kenalog) Methylprednisolo ne (Depo Medrol) Betamethasone and Sodium Phosphate (Celestone) Dexamethasone Acetate (Decadron) 1 High Intermediate Intermediate Low/High High Biological Halflife (hours) (Table adapted Corticosteroids Dosing Equivalency Preparation Trade Name equivalent Dose/Volume (mg/ml) Triamcinolone Kenalog 40 Methylprednisolone Depo medrol 40 Dexamethasone Decadron 8 Betamethasone Acetate and sodiume Phosphate Celestone 6 (Table adapted from Mcnabb, 2015, p.15) 6
7 Corticosteriod Dosing Drug Large Joint (Knee, Hip Shoulder) Medium Sized Joint (Elbow, ankle) Small Joints (Hands, feet) Hydrocortisone mg mg mg Methylprednisolone mg mg 5 10 mg Triamcinolone mg mg 2.5 5mg (Lawery, 2010, p. 130) Corticosteroids Intra articular steroids How often No studies to determine exact interval Currently based on professional opinion General consensus is every 3 months (Mcnabb, 2015, p. 15) Hyaluronic injections/viscosupplementation Hyaluronan (sodium hyaluronate) Natural complex sugar of the glycosamin0glycan family Concentration and size of Endogenous hyaluronate are reduced in Osteoarthritis Viscosupplementation Synthetic hyaluronate supplement Rooter comb Derived from Bacterial fermentation Mechanism of action unknown Lubrication, shock absorption (Mcnabb, 2015, p. 16) 7
8 Platelet Rich Plasma Investigational Injection of centrifuged blood Plasma with concentrated platelets is injected into injured tissue Platelets contain growth factors which is believed to promote/speed healing Intraarticular and Periarticular injections/aspiration Technique/Procedure Prepare injections/gather supplies Identify Landmarks Mark injection site Prep injection site Alcohol, betadine, chlorahexidine Injection Local anesthetic Lidocaine Vapocoolant No touch technique Aseptic technique Intraarticular and Periarticular injections/aspiration Complications Vasovagal reaction Infection Cortisone Flair Crystalline Steroid Preparation Methylparaben preservative Treat with rest, Ice and NSAIDS Headache, flushing, abnormal vaginal bleeding, HPA axis suppression, Osteoporosis Skin/fatty atrophy Skin hypopigmentation Tendon Rupture, ligament rupture (Mcnabb, 2015, p. 23) 8
9 Intraarticular and Periarticular injections/aspiration Aftercare Apply pressure Sterile bandage Ensure Patient is stable Patient instructions Monitor for infection Redness, warmth, proximal red streaking,temp <100 Rest and protect area 1 2 days (Mcnabb, 2015, p. 24) Documentation Diagnosis Risk and benefits Written Consent Post injection instructions Follow up Injection Site Medication Positioning Complications, difficulties Response to injection Post injection condition (Mcnabb, 2015, p. 25) Billing CPT J codes Injection, therapeutic, Carpal Tunnel Injection, single tendon sheath, or ligament, aponeurosis Injection, single tendon origin/insertion Injection single or multiple trigger points Injection, trigger points, three or more muscles Arthocentesis, aspiration and or Injection Small Joint or bursa Arthocentesis, aspiration and or Injection intermediate Joint or bursa Arthocentesis, aspiration and or Injection Large Joint or bursa J3301 Kenalog J1020 Depo medrol 20 mg J1030 Depo medrol 40 mg J1040 Depo medrol 80 mg J0704 Celestone 6 mg J1094 Decadron 1 mg (Mcnabb, 2015, p ) 9
10 Billing Modifiers 25 billing for injection with office visit 51 or 59 injections multiple sites 50 bilateral procedure (Mcnabb, 2015, p. 26) Upper Extremity 1 st Metacarpal Phalangeal Joint Carpal Tunnel Injection Dequervains Tenosynovitis Trigger Finger Medial and Lateral Epicondyle Injections Elbow joint injection/aspiration Subacromial Injection Glenohumeral injection Lower Extremity Greater Trochanter injection Knee joint injection/aspiration Pes Bursa injection Plantar fascia injection Ankle joint injection/aspiration 10
11 1 st Metacarpal Phalangeal Joint Indication First Carpometacarpal Osteoarthritis (CMC (BASAL joint) arthritis, 2014) Supplies Antiseptic Local anesthetic Corticosteroid 3 or 5 ml leur lock syringe 22 or 25 gauge needle Anatomy (Hand anatomy, 2016) 11
12 Landmarks Identify landmarks/joint by having patient adduct the thumb Palpate first metacarpal distal to proximal Tenderness Dip between first metacarpal and Trapezium (Mcnabb, 2015, p. 146) Technique Insert needle perpendicular to skin Inject dorsally to avoid radial artery. Apply traction to thumb to open joint space. (Mcnabb, 2015, p. 147) Demonstration 12
13 1 st Extensor Compartment, Wrist Indications Dequervains Tenosynovitis (Dequervains tenosynovitis, n.d.) Supplies Antiseptic Local anesthetic Corticosteroid 3 or 5 ml leur lock syringe 22 or 25 gauge needle Landmarks Identify tenderness over 1 st dorsal compartment Abductor Pollicis Longus Extensor pollicis brevis Injection site directly between tendons over radial styloid (Mcnabb, 2015, p. 139) 13
14 Landmarks Technique Position needle 45 degree angle directed proximally with bevel up Advance needle to radial styloid, withdraw slightly Slowly inject mixture, should track proximally along tendon sheath, may feel POP with injection (Mcnabb, 2015, p. 140) Demonstration 14
15 Trigger Finger Injection Indications Stenosing Tenosynovitis (Trigger finger, n.d.) Supplies Antiseptic Local anesthetic Corticosteroid 3 or 5 ml leur lock syringe 22 or 25 gauge needle Landmarks Proximal Phalanx Metacarpal Head Flexor Tendons Identify painful palpable nodule A1 pulley Injection site 1 cm distal to palpable nodule (Mcnabb, 2015, p. 153) 15
16 Landmarks Technique Position needle 45 degree angle directed proximally with bevel up Advance needle towards nodule May skewer tendon, withdraw 1 2 ml slowly applying gentle pressure on plunger, once no resistance is felt continue to inject Sausage like mass may form due to distention of tendon sheath. (Mcnabb, 2015, p. 155) Demonstration 16
17 Medial and lateral epicondyle injection Indication Medial Epicondylitis Lateral epicondylitis (Medial and lateral epicondylitis, 2008) Supplies Antiseptic Local anesthetic Corticosteroid 3 or 5 ml leur lock syringe 22 or 25 gauge needle Anatomy Lateral epicondyle Point of Maximal Tenderness adjacent to lateral epicondyle Medial epicondyle Point of maximal tenderness adjacent to medial epicondyle 17
18 Landmarks Lateral epicondyle injection Lateral epicondyle Extensor Carpi Radialis Longus Medial epicondyle Injection Medial epicondyle Olecranon Cubital tunnel (ulnar nerve) (Mcnabb, 2015, p. 115) Landmarks Technique Lateral epicondyle injection Advance needle perpendicular to lateral epicondyle Withdraw needle 1 2 mm and inject Use pinch technique to avoid subcutaneous infiltration Medial epicondyle injection Advance needle to medial epicondyle Withdrawal needle 1 2 mm and inject (Mcnabb, 2015, p. 116 & 120) 18
19 Demonstration Elbow Joint Injection/Aspiration Elbow joint effusion Elbow osteoarthritis Olecranon Bursitis Supplies Injection Antiseptic Local anesthetic Corticosteroid 3 or 5 ml leur lock syringe 22 or 25 gauge needle Aspiration 30 or 60 ml syringe 18 gauge needle 19
20 Landmarks Radial Head Lateral epicondyle Olecranon process Injection site is locate in soft spot between radial head, lateral epicondyle and Olecranon. Landmarks Technique Intraarticular injection Position Lying supine with elbow 45 degrees extension Injection/aspiration Direct needle 90 degrees Insert slowly applying suction Synovial fluid confirms placement Inject if indicated (Mcnabb, 2015, p. 109) 20
21 Technique Olecranon bursa Insert needle away from any open areas and/or cellulitis at the site of maximal fluctuance Insert slowly applying suction Fluid may be thick and not amendable to aspiration Inject following aspiration if indicated (Mcnabb, 2015, p.112) Demonstration Subacromial Injection Indications Rotator Cuff Impingement Partial Rotator Cuff Tear Rotator cuff tendinitis Subacromial Bursitis Proximal Bicep tendinitis (Subacromial impingement, n.d.) 21
22 Supplies Antiseptic 5 or 10 ml leurlock Syringe 1 ½ inch 22 gauge needle 1% lidocaine Corticosteriod of providers choice Anatomy (Shoulder anatomy, n.d.) Landmarks Subacromial injection (Posterior Approach Identify Posterior Lateral Border of Acromion Injection site located in soft spot approximately 2 cm inferior (Lawery, 2010, p. 18) 22
23 Landmarks Technique Positioning Sitting Needle is directed Medially, superior aiming towards acromioclavicular joint (Mcnabb, 2015, p. 84) Demonstration 23
24 Glenohumeral injection Indications Glenohumeral Osteoarthritis (Glenohumeral arthritis, n.d.) Supplies Antiseptic 5 0r 10 ml leurlock Syringe 1 ½ inch 22 gauge needle 1% lidocaine Corticosteriod Landmarks Glenohumeral Injection (Posterior Approach) Identify Posterolateral Margin of Acromion Injection site located 2 finger breadths inferior and medial (Lawery, 2010, p. 18) 24
25 Landmarks Technique Positioning Seated with hands across lap Direct Needle towards Coracoid Once needle reaches posterior humerus Internal/external rotation Demonstration 25
26 Case Study 43 year old male presents for follow up for his right shoulder. He has continued pain despite taking over the counter anti inflammatories, activity modification, and 4 weeks of formal physical therapy. On exam he has positive Neer and Hawkin s signs. What is the next best mode of action? a. Perform Subacromial corticosteroid injection utilizing posterior approach with 160 mg Depo medrol and 8 ml 1% lidocaine. b. Prescribe Norco 5mg/325 mg 1 2 tablets every 4 6 hours as needed for pain. Dispense 240 tablets. No Refills. c. Perform Subacromial corticosteroid Injection utilizing Posterior approach with 80 mg Depo medrol and 8 ml 1% lidocaine. d. Perform Glenohumeral corticosteroid injection utilizing Posterior approach with 80 mg Depo medrol and 8 ml 1 % lidocaine. Case Study Following the injection, what do you anticipate? A. Increased Pain B. Right arm numbness C. Resolution of Neer and Hawkin s Signs D. Reduction in Range of motion Case Study Which reflects the most appropriate Coding for this encounter? A. Level 3, modifier. Large Joint 20610, Depomedrol 80 mg J1040 B. Level 3, modifier. Intermediate Joint 20605, Depo medrol 80 mg J1040 C. Level 3, 99213, 57 modifier, Large Joint 20610, Depomedrol 80 mg J1040 D. Level 3, 99213, 57 modifier, Intermediate joint 20605, Depo medrol 80 mg J
27 Break time Greater trochanteric Bursa injection Indications Greater Trochanteric Bursitis (Greater trochanteric bursitis, 2011) Supplies Antiseptic 5 0r 10 ml leurlock Syringe 1 ½ inch 22 gauge needle 1% lidocaine Corticosteriod 27
28 Landmark Greater trochanter Identify point of maximum tenderness In larger patients can internally and externally rotate hip to identify greater trochanter Technique Positioning Lateral decubitus Affected hip up Insert needle perpendicular to skin Insert needle until contact with femur Withdrawal 1 2 mm and inject Fan injection (Mcnabb, 2015, p. 193) Demonstration 28
29 Knee joint injection/aspiration Indication Knee Arthritis Acute effusion Septic arthritis (Knee effusion, 2013) Supplies Injection Antiseptic 5 0r 10 ml leurlock Syringe 1 ½ inch 22 gauge needle 1% lidocaine Corticosteriod Aspiration 60 ml syringe 18 gauge needle hemostat Landmarks(Lateral suprapatellar Approach) Superior boarder patella Draw line 1 cm superior Posterior edge patella Draw line alone posterior boarder Injection site is where the lines intersect 29
30 Landmarks Technique (Lateral Suprapatellar approach) Position Supine, knee flexed supported by towel or pillow Technique Insert needle perpendicular to skin with needle bevel up Slowly advance with gentle suction between quad and distal femur May feel pop, presence of synovial fluid confirms placement Aspirate fluid as desires, may follow with corticosteriod preparation. (Mcnabb, 2015, p. 204) Landmarks (Anterolateral Approach) Inferior pole patella Lateral femoral condyle Gerdy s Tubercle (proximal tibia) Injection site approximately 1 cm lateral to patellar tendon (soft spot) 30
31 Landmarks Technique Position Sitting on exam table with knee flexed 90 degrees Insert needle degree angle aiming toward condylar notch tibia Apply suction, synovial fluid confirms needle placement Inject slowly (Mcnabb, 2015, p. 214) Demonstration 31
32 Pes Bursa Injection Indication Pes bursitis (Pes bursitis, 2011) Supplies Injection Antiseptic 5 0r 10 ml leurlock Syringe 1 ½ inch 22 gauge needle 1% lidocaine Corticosteriod Landmarks Medial proximal tibia Injection site Point of maximum tenderness 32
33 Technique Position Either supine with knee slightly flexed, or seated with knee flexed 90 degrees Injection Insert needle perpendicular to skin Advance slowly until needle reaches tibia, withdraw 1 2 mm, aspirate and inject. Demonstration Ankle joint injection/aspiration Indications Ankle osteoarthritis Ankle effusion (Ankle, 2014) 33
34 Supplies Injection Antiseptic 5 0r 10 ml leurlock Syringe 1 ½ inch 22 gauge needle 1% lidocaine Corticosteriod Aspiration 10 or 30 ml leurlock Syringe 1 ½ inch 18 gauge needle Hemostat Landmarks Anterolateral Injection Fibula Distal tibia Talus Normal depression, injection site is located in soft spot (Mcnabb, J., p ) Anteromedial Fibula Distal tibia Talus Anterior tibialis tendon Injection site is located 1 cm medial to Tendon (Mcnabb, 2015, p ) Landmarks Anterolateral 34
35 Landmarks Anteromedial Technique Anterolateral Position Supine with ankle at 90 degrees flexion Injection Insert needle directed medially (Mcnabb, J., p ) Anteromedial Position Supine with ankle at 90 degrees flexion Injection Insert needle directed medially (Mcnabb, 2015, p ) Demonstration 35
36 Plantar fascia injection Indications Plantar fasciitis (Plantar fasciitis, 2011) Supplies Antiseptic Local anesthetic Corticosteroid 3 or 5 ml leur lock syringe 22 or 25 gauge needle Landmarks Medial calcaneal tubercle Injection site Draw vertical line alone posterior border or tibia Draw horizontal line one finger breadth above plantar surface Point of intersection correlates with medial calcaneal tubercle (Mcnabb, 2015, p ) 36
37 Landmarks Technique Position Supine Injection Advance needle perpendicular to skin Slowly advance until medial tubercle is reached at plantar facial insertion, slowly inject (Mcnabb, 2015, p ) Demonstration 37
38 Case Study 70 year old Male returns to your clinic for his left knee. He has an established diagnosis of Left knee primary osteoarthritis. He denies new injury. He take Tylenol as needed for the pain, and applies biofreeze with little improvement. He walks daily and wears a knee brace. He is having a hard time with daily tasks. He is having pain at night time that awaken s him. He does not want to have surgery. On exam he exhibits subtle joint effusion. Varus alignment. Medial joint line tenderness. Negative mcmurrays. Patellofemoral crepitance. He has full motion and strength. No instability. Which option is likely to give him the most relief? A. Intramuscular injection 80 mg Depo medrol B. Left knee Pes bursa injection using 80 mg depo medrol 8 ml 1 % lidocaine C. Left knee injection using lateral suprapatellar approach using 8 ml 1 % lidocaine D. Left knee injection using lateral suprapatellar approach using 80 mg Depomedrol and 3 ml 1 % lidocaine. Case Study Which reflects the most appropriate Coding for this encounter? A. Level 3, modifier. Large Joint 20610, Depomedrol 80 mg J1040 B. Level 3, modifier. Intermediate Joint 20605, Depo medrol 80 mg J1040 C. Level 3, 99213, 57 modifier, Large Joint 20610, Depomedrol 80 mg J1040 D. Level 3, 99213, 57 modifier, Intermediate joint 20605, Depo medrol 80 mg J1040 Case Study The previous patient calls your office 24 hours later complaining of severe knee pain. What is the most likely cause? A. Septic arthritis B. Medial Meniscus tear C. Cortisone Flare D. Exacerbation of his arthritis 38
39 Case Study What advice to you give to the patient? A. Go to the emergency room B. Come to the office immediately C. Non weight bearing with axillary crutches D. Provide reassurance. Advise him to apply ice and elevate. Take NSAIDS or Tylenol. Pain should subside in hours. If pain does not improve or if there is redness or warmth, please call the office. Conclusion Musculoskeletal conditions comprise 60 percent of outpatient office visits Intraarticular and periarticular injections offer a safe and valuable adjunct to musculoskeletal care. (Benham & Geier, 2014, p. 603) References Benham, A., & Geier, K. A. (2014). Preparing Nurse Practitioners to Provide Orthopedic Primary Care. The Journal for Nurse Practitioners, 10(8), doi: /j.nurpra Carpal Tunnel [Descriptive image]. (2014, March). Retrieved from content/uploads/2014/03/understanding Carpal Tunnel Syndrome.jpg CMC (BASAL joint) arthritis [Decriptive anatomic image]. (2014, May). Retrieved from Dequervains tenosynovitis [anatomic image]. (n.d.). Retrieved from Glenohumeral arthritis [anatomic image]. (n.d.). Retrieved from Greater trochanteric bursitis [anatomic image]. (2011). Retrieved from joint trochanteric bursitis itband.jpg Hand anatomy [anatomic image]. (2016, December). Retrieved from content/uploads/2016/12/hand Anatomy Bones x1024.jpg Knee effusion [photo]. (2013). Retrieved from content/uploads/2013/07/water on the Knee Knee Effusion.jpg 39
40 References Lawry, G. (2010). Fam's musculoskeletal examination and joint injection techniques. McNabb, J. W. (2015). A practical guide to joint & soft tissue injections. Medial and lateral epicondylitis [anatomic image]. (2008). Retrieved from druvnmcs3c/uluditj58zi/aaaaaaaaama/pietz G3iiQ/s1600/elbow_anatomy07c.jpg Pes bursitis [anatomic image]. (2011). Retrieved from anserine bursitis.jpg Shoulder anatomy [anatomic image]. (n.d.). Retrieved from 8ssoqKo36ew/V67hzndMISI/AAAAAAAAAU0/LPjOAj0TfRkfcddPkL E9miTs6_dCZRzwCLcB/s1600/54513.jpg Subacromial impingement [anatomic image]. (n.d.). Retrieved from Trigger finger [antatomic image]. (n.d.). Retrieved from oe7bifnt_h4/ut FbK8pzI/AAAAAAAAHOI/5ncRCUzHWpo/s1600/tf1.PNG Trigger finger [anatomic image]. (n.d.). Retrieved from Wrist anatomy [anatomic image]. (2012). Retrieved from content/uploads/2012/12/wristanat ex3.jpg 40
Benefits of Aspiration and Injection JOINT INJECTIONS. Injection Indications. Mechanism of Action 1/11/2016
 Benefits of Aspiration and Injection JOINT INJECTIONS Mark Niedfeldt, M.D. Medical College of Wisconsin Decrease or resolution of pain Decrease or resolution of inflammation Decrease or resolution of effusion
Benefits of Aspiration and Injection JOINT INJECTIONS Mark Niedfeldt, M.D. Medical College of Wisconsin Decrease or resolution of pain Decrease or resolution of inflammation Decrease or resolution of effusion
ORTHOPAEDIC INJECTION AND ASPIRATION TECHNIQUES
 ORTHOPAEDIC INJECTION AND ASPIRATION TECHNIQUES OAAPN October 20, 2016 David H. Sohn, JD MD Chief, Shoulder and Sports Medicine University of Toledo Medical Center When to aspirate? To rule out infection
ORTHOPAEDIC INJECTION AND ASPIRATION TECHNIQUES OAAPN October 20, 2016 David H. Sohn, JD MD Chief, Shoulder and Sports Medicine University of Toledo Medical Center When to aspirate? To rule out infection
Injections of the Joints & Soft Tissues. Matthew Kanaan DO, MS
 Injections of the Joints & Soft Tissues Matthew Kanaan DO, MS Outline / Goals! Injection basics (risks, contraindications, supplies )! Upper extremity Injections! HANDS ON - Simulated needle w/ marking
Injections of the Joints & Soft Tissues Matthew Kanaan DO, MS Outline / Goals! Injection basics (risks, contraindications, supplies )! Upper extremity Injections! HANDS ON - Simulated needle w/ marking
Subacromial Bursa Injection
 Subacromial Bursa Injection 5 cc syringe, 21 gauge 1.5 inch needle 1% lidocaine - 4cc 40mg triamcinolone - 1 cc of 40mg/ml identify site-seat the patient with weight of arm hanging down, palpate the lateral
Subacromial Bursa Injection 5 cc syringe, 21 gauge 1.5 inch needle 1% lidocaine - 4cc 40mg triamcinolone - 1 cc of 40mg/ml identify site-seat the patient with weight of arm hanging down, palpate the lateral
Hands on - Steroid Injections. Jan Schulz, MD Associate professor of medicine McGill University
 Hands on - Steroid Injections Jan Schulz, MD Associate professor of medicine McGill University Disclosures Abbott Pharmaceuticals Amgen Roche Bristol-Myers Squibb Janssen Ortho Novartis Adult Rheumatology
Hands on - Steroid Injections Jan Schulz, MD Associate professor of medicine McGill University Disclosures Abbott Pharmaceuticals Amgen Roche Bristol-Myers Squibb Janssen Ortho Novartis Adult Rheumatology
KAPA 2017 Musculoskeletal Aspiration and Injection Workshop. W. Scott Black, MD Physician Assistant Studies Program University of Kentucky
 KAPA 2017 Musculoskeletal Aspiration and Injection Workshop W. Scott Black, MD Physician Assistant Studies Program University of Kentucky Aspiration Relatively quick and inexpensive Can be performed in
KAPA 2017 Musculoskeletal Aspiration and Injection Workshop W. Scott Black, MD Physician Assistant Studies Program University of Kentucky Aspiration Relatively quick and inexpensive Can be performed in
Workshop Hands on - Steroid Injections. Michael Stein MDCM, FRCP(C) Date: Nov
 Workshop Hands on - Steroid Injections Michael Stein MDCM, FRCP(C) Date: Nov 26 2018 Disclosure of Commercial Support This program has received no financial support Faculty/Presenter Disclosures I am a
Workshop Hands on - Steroid Injections Michael Stein MDCM, FRCP(C) Date: Nov 26 2018 Disclosure of Commercial Support This program has received no financial support Faculty/Presenter Disclosures I am a
JOINT INJECTIONS AJ DURFEE PA-C CHRIS MAYBERRY PA-C
 JOINT INJECTIONS AJ DURFEE PA-C Worked with sports group in San Diego for 7 ½ years Worked for Kaiser Orthopedics since 2011 I grew up in San Diego CHRIS MAYBERRY PA-C 1 XAVIER VALDEZ Grew up in Texas
JOINT INJECTIONS AJ DURFEE PA-C Worked with sports group in San Diego for 7 ½ years Worked for Kaiser Orthopedics since 2011 I grew up in San Diego CHRIS MAYBERRY PA-C 1 XAVIER VALDEZ Grew up in Texas
ORTHOPEDIC OFFICE INTERVENTIONS. Objectives of this discussion. Why me? By Steve Benz M.D.
 ORTHOPEDIC OFFICE INTERVENTIONS By Steve Benz M.D. Objectives of this discussion Learn about injections and castings that you can perform in your clinic setting. Learn about the agents that you can inject.
ORTHOPEDIC OFFICE INTERVENTIONS By Steve Benz M.D. Objectives of this discussion Learn about injections and castings that you can perform in your clinic setting. Learn about the agents that you can inject.
Aspiration, Intra-articular and Soft Tissue Injections. MR KEWAL SINGH, MS(orth), FRCS(Eng)
 Aspiration, Intra-articular and Soft Tissue Injections MR KEWAL SINGH, MS(orth), FRCS(Eng) Indications for Aspiration Haemarthrosis Septic arthritis Symptomatic relief of a large effusion Crystal-induced
Aspiration, Intra-articular and Soft Tissue Injections MR KEWAL SINGH, MS(orth), FRCS(Eng) Indications for Aspiration Haemarthrosis Septic arthritis Symptomatic relief of a large effusion Crystal-induced
9/25/2014. Ricki Loar, Ph.D., APN, FNP-BC, GNP-BC. Disclosure: No Disclosures. Strategic Nurse Practitioner Solutions, LLC
 Ricki Loar, Ph.D., APN, FNP-BC, GNP-BC 1 Dr. Ricki S. Loar, Ph.D., FNP-BC, GNP-BC Clinical Director, Be Well Partners in Health Nurse Practitioner, South Naperville Family Practice Faculty, Advanced Practice
Ricki Loar, Ph.D., APN, FNP-BC, GNP-BC 1 Dr. Ricki S. Loar, Ph.D., FNP-BC, GNP-BC Clinical Director, Be Well Partners in Health Nurse Practitioner, South Naperville Family Practice Faculty, Advanced Practice
Introduction to Ultrasound Guided Shoulder Injections. Alison Hall Consultant Sonographer Keele University Cannock Chase Hospital
 Introduction to Ultrasound Guided Shoulder Injections Alison Hall Consultant Sonographer Keele University Cannock Chase Hospital Safe Robust Aim: to provide a service that is Cost effective To enable patients
Introduction to Ultrasound Guided Shoulder Injections Alison Hall Consultant Sonographer Keele University Cannock Chase Hospital Safe Robust Aim: to provide a service that is Cost effective To enable patients
Soft Tissue Rheumatism. Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group
 Soft Tissue Rheumatism Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group Some problems are difficult, but diagnosing and treating most causes of joint pain are not! Common areas of
Soft Tissue Rheumatism Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group Some problems are difficult, but diagnosing and treating most causes of joint pain are not! Common areas of
Musculoskeletal Examination Benchmarks
 Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
GP practical procedures Joint and soft tissue injections. Dr Monica Gupta Dr Hilary Wilson Dr John Hunter
 GP practical procedures Joint and soft tissue injections Dr Monica Gupta Dr Hilary Wilson Dr John Hunter Outline of talk Acute mono arthritis Pros & Cons of injections Regional problems Shoulder Knee Soft
GP practical procedures Joint and soft tissue injections Dr Monica Gupta Dr Hilary Wilson Dr John Hunter Outline of talk Acute mono arthritis Pros & Cons of injections Regional problems Shoulder Knee Soft
Rheumatology & Immunology. Regional pain syndromes to be covered today. Some definitions. Tendinitis. Bursitis. History. History. Exam.
 Rheumatology & Immunology Some problems are difficult, but diagnosing and treating soft tissue syndromes are not! Soft tissue syndromes one of the most common reasons patients present to their doctor.
Rheumatology & Immunology Some problems are difficult, but diagnosing and treating soft tissue syndromes are not! Soft tissue syndromes one of the most common reasons patients present to their doctor.
Joint Injections. AJ Durfee PA-C. Course Objectives. Jerry Hizon,MD, FAAFP,CAQSM
 Jerry Hizon,MD, FAAFP,CAQSM Joint Injections OUCH Sports Med Ctr Team Doctor, SD Chargers (NFL) Temecula Valley High School Assist. Clinical Professor, University of California, San Diego Mayor of Temecula
Jerry Hizon,MD, FAAFP,CAQSM Joint Injections OUCH Sports Med Ctr Team Doctor, SD Chargers (NFL) Temecula Valley High School Assist. Clinical Professor, University of California, San Diego Mayor of Temecula
ORTHOPEDIC PRIMARY CARE Joint Injections in Primary Care. Jackson Orthopaedic Foundation
 ORTHOPEDIC PRIMARY CARE Joint Injections in Primary Care Jackson Orthopaedic Foundation Joint Injections in Primary Care Kathleen A. Geier, DNP, NP, ONC A.J. Benham, DNP, NP, ONC kgeier@jacksonortho.org
ORTHOPEDIC PRIMARY CARE Joint Injections in Primary Care Jackson Orthopaedic Foundation Joint Injections in Primary Care Kathleen A. Geier, DNP, NP, ONC A.J. Benham, DNP, NP, ONC kgeier@jacksonortho.org
Musculoskeletal corticosteroid use:
 Musculoskeletal corticosteroid use: Types, Indications, Contraindications, Equivalent doses, Frequency of use and Adverse effects. Dr Jide Olubaniyi MBBS, FRCR Dr Sean Crowther MB BCh, MRCS, FRCR Dr Sukhvinder
Musculoskeletal corticosteroid use: Types, Indications, Contraindications, Equivalent doses, Frequency of use and Adverse effects. Dr Jide Olubaniyi MBBS, FRCR Dr Sean Crowther MB BCh, MRCS, FRCR Dr Sukhvinder
How to Do a Subacromial Shoulder Injection
 How to Do a Subacromial Shoulder Injection UCSF Primary Care Sports Medicine Conference 2018 Carlin Senter, MD Associate Professor Co-Director UCSF Sports Concussion Program Primary Care Sports Medicine
How to Do a Subacromial Shoulder Injection UCSF Primary Care Sports Medicine Conference 2018 Carlin Senter, MD Associate Professor Co-Director UCSF Sports Concussion Program Primary Care Sports Medicine
Practical 2 Worksheet
 Practical 2 Worksheet Upper Extremity BONES 1. Which end of the clavicle is on the lateral side (acromial or sternal)? 2. Describe the difference in the appearance of the acromial and sternal ends of the
Practical 2 Worksheet Upper Extremity BONES 1. Which end of the clavicle is on the lateral side (acromial or sternal)? 2. Describe the difference in the appearance of the acromial and sternal ends of the
BATES VISUAL GUIDE TO PHYSICAL EXAMINATION. OSCE 4: Knee Pain
 BATES VISUAL GUIDE TO PHYSICAL EXAMINATION OSCE 4: Knee Pain This video format is designed to help you prepare for objective structured clinical examinations, or OSCEs. You are going to observe and participate
BATES VISUAL GUIDE TO PHYSICAL EXAMINATION OSCE 4: Knee Pain This video format is designed to help you prepare for objective structured clinical examinations, or OSCEs. You are going to observe and participate
ARM Brachium Musculature
 ARM Brachium Musculature Coracobrachialis coracoid process of the scapula medial shaft of the humerus at about its middle 1. flexes the humerus 2. assists to adduct the humerus Blood: muscular branches
ARM Brachium Musculature Coracobrachialis coracoid process of the scapula medial shaft of the humerus at about its middle 1. flexes the humerus 2. assists to adduct the humerus Blood: muscular branches
Elbow. Chapter 2 LISTEN. Mechanism of Injury (If Applicable) Pain
 Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
Professor Lisa Stamp
 Professor Lisa Stamp Rheumatologist University of Otago, Christchurch 8:30-9:25 WS #65: Joint Injection Techniques 9:35-10:30 WS #75: Joint Injection Techniques (Repeated) Joint/soft tissue corticosteroid
Professor Lisa Stamp Rheumatologist University of Otago, Christchurch 8:30-9:25 WS #65: Joint Injection Techniques 9:35-10:30 WS #75: Joint Injection Techniques (Repeated) Joint/soft tissue corticosteroid
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A ACJ. See Acromioclavicular joint (ACJ) Acromioclavicular joint (ACJ) procedures of, 557 559 Ankle and foot procedures of, 649 671 (See also
Note: Page numbers of article titles are in boldface type. A ACJ. See Acromioclavicular joint (ACJ) Acromioclavicular joint (ACJ) procedures of, 557 559 Ankle and foot procedures of, 649 671 (See also
Biceps Brachii. Muscles of the Arm and Hand 4/4/2017 MR. S. KELLY
 Muscles of the Arm and Hand PSK 4U MR. S. KELLY NORTH GRENVILLE DHS Biceps Brachii Origin: scapula Insertion: radius, fascia of forearm (bicipital aponeurosis) Action: supination and elbow flexion Innervation:
Muscles of the Arm and Hand PSK 4U MR. S. KELLY NORTH GRENVILLE DHS Biceps Brachii Origin: scapula Insertion: radius, fascia of forearm (bicipital aponeurosis) Action: supination and elbow flexion Innervation:
Evaluation of the Knee and Shoulder
 Evaluation of the Knee and Shoulder Karen J. Boselli, MD Northeast Regional Nurse Practitioner Conference May 2018 Knee Overview History Examination Top 5 diagnoses When to image When to refer Pain most
Evaluation of the Knee and Shoulder Karen J. Boselli, MD Northeast Regional Nurse Practitioner Conference May 2018 Knee Overview History Examination Top 5 diagnoses When to image When to refer Pain most
Lab Activity 11: Group II
 Lab Activity 11: Group II Muscles Martini Chapter 11 Portland Community College BI 231 Origin and Insertion Origin: The place where the fixed end attaches to a bone, cartilage, or connective tissue. Insertion:
Lab Activity 11: Group II Muscles Martini Chapter 11 Portland Community College BI 231 Origin and Insertion Origin: The place where the fixed end attaches to a bone, cartilage, or connective tissue. Insertion:
The Elbow and the cubital fossa. Prof Oluwadiya Kehinde
 The Elbow and the cubital fossa Prof Oluwadiya Kehinde www.oluwadiya.com Elbow and Forearm Anatomy The elbow joint is formed by the humerus, radius, and the ulna Bony anatomy of the elbow Distal Humerus
The Elbow and the cubital fossa Prof Oluwadiya Kehinde www.oluwadiya.com Elbow and Forearm Anatomy The elbow joint is formed by the humerus, radius, and the ulna Bony anatomy of the elbow Distal Humerus
ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW
 PRACTICAL ADVICE ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW Written by Akira M. Murakami, USA Ultrasound is a powerful modality for guiding the intra-articular injection of both therapeutic medication
PRACTICAL ADVICE ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW Written by Akira M. Murakami, USA Ultrasound is a powerful modality for guiding the intra-articular injection of both therapeutic medication
Hand / wrist Injections. MATS. June Condition Symptoms Conservative Treatments Location of injection CBA for surgery
 Hand / wrist Injections. MATS. June 2018. Condition Symptoms Conservative Treatments Location of injection CBA for surgery Carpal Tunnel Tingling / numbness in median nerve distribution (lateral 3 fingers)
Hand / wrist Injections. MATS. June 2018. Condition Symptoms Conservative Treatments Location of injection CBA for surgery Carpal Tunnel Tingling / numbness in median nerve distribution (lateral 3 fingers)
Sustained a sprained ankle
 Student Name : Student s Number : 3. Q 1. 2. Sustained a sprained ankle 1. List at least 3 key items you should ask during the history portion of an examination ( ) Possible Answers and Anything Else you
Student Name : Student s Number : 3. Q 1. 2. Sustained a sprained ankle 1. List at least 3 key items you should ask during the history portion of an examination ( ) Possible Answers and Anything Else you
Live On Screen: Knee Injections ABCs of Musculoskeletal Care. Knee aspiration. Objectives. I have no disclosures.
 I have no disclosures. Live On Screen: Knee Injections ABCs of Musculoskeletal Care Carlin Senter, MD Primary Care Sports Medicine Departments of Medicine and Orthopaedics December 11, 2015 Objectives
I have no disclosures. Live On Screen: Knee Injections ABCs of Musculoskeletal Care Carlin Senter, MD Primary Care Sports Medicine Departments of Medicine and Orthopaedics December 11, 2015 Objectives
Chapter 8. The Pectoral Girdle & Upper Limb
 Chapter 8 The Pectoral Girdle & Upper Limb Pectoral Girdle pectoral girdle (shoulder girdle) supports the arm consists of two on each side of the body // clavicle (collarbone) and scapula (shoulder blade)
Chapter 8 The Pectoral Girdle & Upper Limb Pectoral Girdle pectoral girdle (shoulder girdle) supports the arm consists of two on each side of the body // clavicle (collarbone) and scapula (shoulder blade)
Joint Injection Challenge The art of good injection therapy is to place the appropriate amount of the appropriate medication into the exact site of th
 The Art of the Injection By Jon C. Brillhart PA-C Daivd Lannik MD Portsmouth Orthopedics, Inc Joint Injection Challenge The art of good injection therapy is to place the appropriate amount of the appropriate
The Art of the Injection By Jon C. Brillhart PA-C Daivd Lannik MD Portsmouth Orthopedics, Inc Joint Injection Challenge The art of good injection therapy is to place the appropriate amount of the appropriate
THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER
 THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER Melinda A. Scott, D.O. Orthopedic Associates of Dayton Board Certified in Primary Care Sports Medicine GOALS Identify landmarks necessary for exam of
THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER Melinda A. Scott, D.O. Orthopedic Associates of Dayton Board Certified in Primary Care Sports Medicine GOALS Identify landmarks necessary for exam of
Anatomy and Physiology II. Review Shoulder Girdle New Material Upper Extremities - Bones
 Anatomy and Physiology II Review Shoulder Girdle New Material Upper Extremities - Bones Anatomy and Physiology II Shoulder Girdle Review Questions From Last Lecture Can you identify the following muscles?
Anatomy and Physiology II Review Shoulder Girdle New Material Upper Extremities - Bones Anatomy and Physiology II Shoulder Girdle Review Questions From Last Lecture Can you identify the following muscles?
Main Menu. Wrist and Hand Joints click here. The Power is in Your Hands
 1 The Wrist and Hand Joints click here Main Menu K.5 http://www.handsonlineeducation.com/classes/k5/k5entry.htm[3/23/18, 1:40:40 PM] Bones 29 bones, including radius and ulna 8 carpal bones in 2 rows of
1 The Wrist and Hand Joints click here Main Menu K.5 http://www.handsonlineeducation.com/classes/k5/k5entry.htm[3/23/18, 1:40:40 PM] Bones 29 bones, including radius and ulna 8 carpal bones in 2 rows of
The examination of the painful knee. Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University
 The examination of the painful knee Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University Objectives of the talk By the end of this talk you will know The important anatomy
The examination of the painful knee Maja K Artandi, MD, FACP Clinical Associate Professor of Medicine Stanford University Objectives of the talk By the end of this talk you will know The important anatomy
The Painful Elbow, Wrist, and Hand. Jennifer R Marks, MD
 The Painful Elbow, Wrist, and Hand Jennifer R Marks, MD The Painful Elbow A 44 yo M presents to clinic complaining of a sore elbow What further questions do you have for this patient? What is on your differential
The Painful Elbow, Wrist, and Hand Jennifer R Marks, MD The Painful Elbow A 44 yo M presents to clinic complaining of a sore elbow What further questions do you have for this patient? What is on your differential
MCQWeek2. All arise from the common flexor origin. The posterior aspect of the medial epicondyle is the common flexor origin.
 MCQWeek2. 1. Regarding superficial muscles of anterior compartment of the forearm: All arise from the common flexor origin. The posterior aspect of the medial epicondyle is the common flexor origin. Flexor
MCQWeek2. 1. Regarding superficial muscles of anterior compartment of the forearm: All arise from the common flexor origin. The posterior aspect of the medial epicondyle is the common flexor origin. Flexor
Radiographic Positioning Summary (Basic Projections RAD 222)
 Lower Extremity Radiographic Positioning Summary (Basic Projections RAD 222) AP Pelvis AP Hip (Unilateral) (L or R) AP Femur Mid and distal AP Knee Lateral Knee Pt lies supine on table Align MSP to Center
Lower Extremity Radiographic Positioning Summary (Basic Projections RAD 222) AP Pelvis AP Hip (Unilateral) (L or R) AP Femur Mid and distal AP Knee Lateral Knee Pt lies supine on table Align MSP to Center
Lecture 9: Forearm bones and muscles
 Lecture 9: Forearm bones and muscles Remember, the region between the shoulder and the elbow = brachium/arm, between elbow and wrist = antebrachium/forearm. Forearm bones : Humerus (distal ends) Radius
Lecture 9: Forearm bones and muscles Remember, the region between the shoulder and the elbow = brachium/arm, between elbow and wrist = antebrachium/forearm. Forearm bones : Humerus (distal ends) Radius
Outline. Knee Anatomy. Physical Exam Skills and Office Procedures in Orthopaedics. The quadriceps muscles extend the knee 7/23/2013
 Physical Exam Skills and Office Procedures in Orthopaedics Outline Knee exam Knee aspiration and injection Shoulder exam Subacromial bursa injection UCSF Essentials of Primary Care August 14, 2012 Carlin
Physical Exam Skills and Office Procedures in Orthopaedics Outline Knee exam Knee aspiration and injection Shoulder exam Subacromial bursa injection UCSF Essentials of Primary Care August 14, 2012 Carlin
ARROW EZ-IO Intraosseous Vascular Access System Procedure Template
 ARROW EZ-IO Intraosseous Vascular Access System Procedure Template PURPOSE To provide procedural guidance for establishment of intraosseous vascular access using the ARROW EZ-IO Intraosseous Vascular Access
ARROW EZ-IO Intraosseous Vascular Access System Procedure Template PURPOSE To provide procedural guidance for establishment of intraosseous vascular access using the ARROW EZ-IO Intraosseous Vascular Access
Joint Injection Workshop ACP Scientific Meeting February 28, Andrea M. Barker, MPAS, PA C Michael J. Battistone, MD
 Joint Injection Workshop ACP Scientific Meeting February 28, 2015 Andrea M. Barker, MPAS, PA C Michael J. Battistone, MD Workshop Schedule 1:00 1:15 A Practical Approach to the Shoulder Exam 1:15 1:40
Joint Injection Workshop ACP Scientific Meeting February 28, 2015 Andrea M. Barker, MPAS, PA C Michael J. Battistone, MD Workshop Schedule 1:00 1:15 A Practical Approach to the Shoulder Exam 1:15 1:40
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel!
 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
divided by the bones ( redius and ulna ) and interosseous membrane into :
 fossa Cubital Has: * floor. * roof : - Skin - superficial fasica - deep fascia ( include bicipital aponeurosis ) Structures within the roof : -cephalic and basilic veins -and between them median cubital
fossa Cubital Has: * floor. * roof : - Skin - superficial fasica - deep fascia ( include bicipital aponeurosis ) Structures within the roof : -cephalic and basilic veins -and between them median cubital
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination
 SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
Muscular Nomenclature and Kinesiology - One
 Chapter 16 Muscular Nomenclature and Kinesiology - One Lessons 1-3 (with lesson 4) 1 Introduction 122 major muscles covered in this chapter Chapter divided into nine lessons Kinesiology study of human
Chapter 16 Muscular Nomenclature and Kinesiology - One Lessons 1-3 (with lesson 4) 1 Introduction 122 major muscles covered in this chapter Chapter divided into nine lessons Kinesiology study of human
Sick Call Screener Course
 Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Evidence Based Approach to Shoulder Injections
 Evidence Based Approach to Shoulder Injections Bradley Sandella, DO Christiana Care Sports Medicine Joseph Straight, MD First State Orthopaedics Objectives Relevant Anatomy Indications for injections Injection
Evidence Based Approach to Shoulder Injections Bradley Sandella, DO Christiana Care Sports Medicine Joseph Straight, MD First State Orthopaedics Objectives Relevant Anatomy Indications for injections Injection
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO
 Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
SMF PCP Treatment & Referral Guideline Orthopedics Developed February 1, 2003 Revised: October, 2011
 SUTTER MEDICAL FOUNDATION (SMF) 2800 L Street, 7 th Floor Sacramento, CA 95816 SMF PCP Treatment & Referral Guideline Orthopedics Developed February 1, 2003 Revised: October, 2011 I. Shoulder Pain...Page
SUTTER MEDICAL FOUNDATION (SMF) 2800 L Street, 7 th Floor Sacramento, CA 95816 SMF PCP Treatment & Referral Guideline Orthopedics Developed February 1, 2003 Revised: October, 2011 I. Shoulder Pain...Page
Joel S Sellers, DO, FAOASM CAQSM, RMSK
 Joel S Sellers, DO, FAOASM CAQSM, RMSK This is a sports slide of an Olympic wrestler Chris Taylor 1 This is a Sports Illustrated slide of jockey Johnny Sellers This is a slide of Coach Jim Sellers 2 This
Joel S Sellers, DO, FAOASM CAQSM, RMSK This is a sports slide of an Olympic wrestler Chris Taylor 1 This is a Sports Illustrated slide of jockey Johnny Sellers This is a slide of Coach Jim Sellers 2 This
Musculoskeletal Examination
 Musculoskeletal Examination Statement of Goals Know how to perform a complete musculoskeletal examination. Learning Objectives A. Describe the anatomy of the musculoskeletal system including the bony structures,
Musculoskeletal Examination Statement of Goals Know how to perform a complete musculoskeletal examination. Learning Objectives A. Describe the anatomy of the musculoskeletal system including the bony structures,
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel!
 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders
Mastering the Musculoskeletal Exam UCSF Essentials of Women s Health July 7, 2016 Carlin Senter, M.D. Henry Crevensten, M.D.
 Mastering the Musculoskeletal Exam UCSF Essentials of Women s Health July 7, 2016 Carlin Senter, M.D. Henry Crevensten, M.D. I have nothing to disclose Outline Knee exam Shoulder exam Knee Anatomy The
Mastering the Musculoskeletal Exam UCSF Essentials of Women s Health July 7, 2016 Carlin Senter, M.D. Henry Crevensten, M.D. I have nothing to disclose Outline Knee exam Shoulder exam Knee Anatomy The
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla.
 1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
Netter's Anatomy Flash Cards Section 6 List 4 th Edition
 Netter's Anatomy Flash Cards Section 6 List 4 th Edition https://www.memrise.com/course/1577581/ Section 6 Upper Limb (66 cards) Plate 6-1 Humerus and Scapula: Anterior View 1.1 Acromion 1.2 Greater tubercle
Netter's Anatomy Flash Cards Section 6 List 4 th Edition https://www.memrise.com/course/1577581/ Section 6 Upper Limb (66 cards) Plate 6-1 Humerus and Scapula: Anterior View 1.1 Acromion 1.2 Greater tubercle
MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM. What Are Musculoskeletal Disorders
 MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM What Are Musculoskeletal Disorders Every year more than 1.8 million workers in the United States suffer painful back and repetitive strain injuries,
MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM What Are Musculoskeletal Disorders Every year more than 1.8 million workers in the United States suffer painful back and repetitive strain injuries,
Clinical examination of the wrist, thumb and hand
 Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
2/28/2017. Learning Objectives. Hip Joint: Anatomy and Kinesiology
 Regional Pain Syndromes: Hip and Knee Srinivas Nalamachu, MD Clinical Assistant Professor, KU School of Medicine President and Medical Director, Pain Management Institute Overland Park, KS Learning Objectives
Regional Pain Syndromes: Hip and Knee Srinivas Nalamachu, MD Clinical Assistant Professor, KU School of Medicine President and Medical Director, Pain Management Institute Overland Park, KS Learning Objectives
SMALL GROUP SESSION 16 January 8 th or 10 th. Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination
 SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
The Forearm 2. Extensor & lateral Compartments of the Forearm
 The Forearm 2 Extensor & lateral Compartments of the Forearm 1-Lateral Fascial Compartment (at the lateral side of the forearm ) *Some books mention the lateral compartment contain just the Brachioradialis
The Forearm 2 Extensor & lateral Compartments of the Forearm 1-Lateral Fascial Compartment (at the lateral side of the forearm ) *Some books mention the lateral compartment contain just the Brachioradialis
Gross Anatomy Questions That Should be Answerable After October 27, 2017
 Gross Anatomy Questions That Should be Answerable After October 27, 2017 1. The inferior angle of the scapula of a woman who was recently in an automobile accident seems to protrude making a ridge beneath
Gross Anatomy Questions That Should be Answerable After October 27, 2017 1. The inferior angle of the scapula of a woman who was recently in an automobile accident seems to protrude making a ridge beneath
Copyright 2004, Yoshiyuki Shiratori. All right reserved.
 Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
In which arm muscle are intramuscular injections most often given? (not in text)
 AP1 Lab 9 - Muscles of the Arms and Legs Locate the following muscles on the models and on yourself. Recall anatomical position. Directional terms such as anterior, posterior, lateral, etc. all assume
AP1 Lab 9 - Muscles of the Arms and Legs Locate the following muscles on the models and on yourself. Recall anatomical position. Directional terms such as anterior, posterior, lateral, etc. all assume
Elbow. Chapter 2 LISTEN. Mechanism of Injury (If Applicable) Pain
 Preface The first decade of the twenty-first century has witnessed the continuation of an explosion in our knowledge and understanding of all aspects of disease. Accompanying this has been the increasing
Preface The first decade of the twenty-first century has witnessed the continuation of an explosion in our knowledge and understanding of all aspects of disease. Accompanying this has been the increasing
Kinesiology of The Wrist and Hand. Cuneyt Mirzanli Istanbul Gelisim University
 Kinesiology of The Wrist and Hand Cuneyt Mirzanli Istanbul Gelisim University Bones The wrist and hand contain 29 bones including the radius and ulna. There are eight carpal bones in two rows of four to
Kinesiology of The Wrist and Hand Cuneyt Mirzanli Istanbul Gelisim University Bones The wrist and hand contain 29 bones including the radius and ulna. There are eight carpal bones in two rows of four to
Practical guide to joint and soft tissue injection techniques James Galloway MRCP and Marwan Bukhari PhD, FRCP
 Practical guide to joint and soft tissue injection techniques James Galloway MRCP and Marwan Bukhari PhD, FRCP Figure 1. The authors encourage a medial approach to injection of the knee joint; a combination
Practical guide to joint and soft tissue injection techniques James Galloway MRCP and Marwan Bukhari PhD, FRCP Figure 1. The authors encourage a medial approach to injection of the knee joint; a combination
Muscles of the Upper Limb
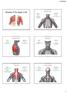 Muscles of the Upper Limb anterior surface of ribs 3 5 coracoid process Pectoralis minor pectoral nerves protracts / depresses scapula Serratus anterior Subclavius ribs 1-8 long thoracic nerve rib 1 ----------------
Muscles of the Upper Limb anterior surface of ribs 3 5 coracoid process Pectoralis minor pectoral nerves protracts / depresses scapula Serratus anterior Subclavius ribs 1-8 long thoracic nerve rib 1 ----------------
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
Wrist & Hand Assessment and General View
 Wrist & Hand Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The hand can be divided
Wrist & Hand Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The hand can be divided
Ultrasound Guided Injections
 Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
WEEKEND 2 Elbow. Elbow Range of Motion Assessment
 Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Elbow Elbow Range of Motion Assessment - Patient Positioning: Sitting or supine towards the edge of the bed - Indications:
Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Elbow Elbow Range of Motion Assessment - Patient Positioning: Sitting or supine towards the edge of the bed - Indications:
HANDS ON: Knee Evaluation J. Scott Delaney MD, FRCPC, FACEP, CSPQ
 HANDS ON: Knee Evaluation J. Scott Delaney MD, FRCPC, FACEP, CSPQ FACULTY DISCLOSURE Dr. Delaney has no affiliation with the manufacturer of any commercial product or provider of any commercial service
HANDS ON: Knee Evaluation J. Scott Delaney MD, FRCPC, FACEP, CSPQ FACULTY DISCLOSURE Dr. Delaney has no affiliation with the manufacturer of any commercial product or provider of any commercial service
Regional Pain. Rheumatologist, Manipal Hospital ChanRe Rheumatology and Immunology Center, Bengaluru
 Regional Pain Dr. B. G. Dharmanand M.D., D.M. (Rheumatology) Rheumatologist, Manipal Hospital ChanRe Rheumatology and Immunology Center, Bengaluru Dharmanand B.G. Regional Pain In Wagh S. (Ed). Rheumatology
Regional Pain Dr. B. G. Dharmanand M.D., D.M. (Rheumatology) Rheumatologist, Manipal Hospital ChanRe Rheumatology and Immunology Center, Bengaluru Dharmanand B.G. Regional Pain In Wagh S. (Ed). Rheumatology
Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader. Lab Leaders: STATION I BRACHIAL PLEXUS
 Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader Lab Leaders: STATION I BRACHIAL PLEXUS A. Posterior cervical triangle and axilla B. Formation of plexus 1. Ventral rami C5-T1 2. Trunks
Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader Lab Leaders: STATION I BRACHIAL PLEXUS A. Posterior cervical triangle and axilla B. Formation of plexus 1. Ventral rami C5-T1 2. Trunks
Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments
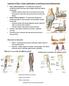 Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments Ulnar Collateral ligament on medial side; arising from medial epicondyle and stops excess valgus movement (lateral movement)
Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments Ulnar Collateral ligament on medial side; arising from medial epicondyle and stops excess valgus movement (lateral movement)
Rance McClain, DO, FACOFP, FAOASM Associate Dean, Clinical Sciences Professor, Clinical Sciences William Carey University College of Osteopathic
 Rance McClain, DO, FACOFP, FAOASM Associate Dean, Clinical Sciences Professor, Clinical Sciences William Carey University College of Osteopathic Medicine Identify common orthopedic conditions presenting
Rance McClain, DO, FACOFP, FAOASM Associate Dean, Clinical Sciences Professor, Clinical Sciences William Carey University College of Osteopathic Medicine Identify common orthopedic conditions presenting
ACPOMIT Conference 2013 Workshop: Hand and Wrist
 ACPOMIT Conference 2013 Workshop: Hand and Wrist Sarah Turner, MCSP, Clinical Specialist in Hand Therapy Grad Dip Injection Therapy Workshop! Trigger Finger! OA 1 st CMC joint! De Quervain s Tenosynovitis!
ACPOMIT Conference 2013 Workshop: Hand and Wrist Sarah Turner, MCSP, Clinical Specialist in Hand Therapy Grad Dip Injection Therapy Workshop! Trigger Finger! OA 1 st CMC joint! De Quervain s Tenosynovitis!
Contents of the Posterior Fascial Compartment of the Thigh
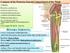 Contents of the Posterior Fascial Compartment of the Thigh 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t
Contents of the Posterior Fascial Compartment of the Thigh 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t
The Muscular System. Chapter 10 Part C. PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College
 Chapter 10 Part C The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.9: Muscles Crossing the Shoulder
Chapter 10 Part C The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.9: Muscles Crossing the Shoulder
Connects arm to thorax 3 joints. Glenohumeral joint Acromioclavicular joint Sternoclavicular joint
 Connects arm to thorax 3 joints Glenohumeral joint Acromioclavicular joint Sternoclavicular joint Scapula Elevation Depression Protraction (abduction) Retraction (adduction) Downward Rotation Upward Rotation
Connects arm to thorax 3 joints Glenohumeral joint Acromioclavicular joint Sternoclavicular joint Scapula Elevation Depression Protraction (abduction) Retraction (adduction) Downward Rotation Upward Rotation
Functional Anatomy of the Elbow
 Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
DART Diagnosis and Related Treatments
 DART Diagnosis and Related Treatments The DART Tool allows a user to obtain Treatment recommendations based on the disorder/condition. These recommendations are provided by ACOEM (American College of Occupational
DART Diagnosis and Related Treatments The DART Tool allows a user to obtain Treatment recommendations based on the disorder/condition. These recommendations are provided by ACOEM (American College of Occupational
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic 2012 MFMER slide MFMER slide-3
 Ultrasound Foot and Ankle Pathology Disclosures None relevant Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012 MFMER slide-2 Foot and Ankle Fundamentals
Ultrasound Foot and Ankle Pathology Disclosures None relevant Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012 MFMER slide-2 Foot and Ankle Fundamentals
Clinical Application of the EMS Swiss DolorClast
 Chapter 12.fm Page 119 Tuesday, November 21, 2006 6:38 PM 12 Clinical Application of the EMS Swiss DolorClast L. Gerdesmeyer, M. Henne, P. Diehl, H. Gollwitzer, M. Göbel In general, the following recommendations
Chapter 12.fm Page 119 Tuesday, November 21, 2006 6:38 PM 12 Clinical Application of the EMS Swiss DolorClast L. Gerdesmeyer, M. Henne, P. Diehl, H. Gollwitzer, M. Göbel In general, the following recommendations
Rotator Cuff Strain and Carpal Tunnel Syndrome
 Rotator Cuff Strain and Carpal Tunnel Syndrome 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem-Solving: SG, Arms, and Hands Punctuality- everybody's time is precious: o o Be ready to learn
Rotator Cuff Strain and Carpal Tunnel Syndrome 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem-Solving: SG, Arms, and Hands Punctuality- everybody's time is precious: o o Be ready to learn
Arthritic history is similar to that of the hip. Add history of give way and locking, swelling
 KNEE VASU PAI Arthritic history is similar to that of the hip. Add history of give way and locking, swelling INJURY MECHANISM When How Sequence Progress Disability IKDC Activity I - Strenuous activity
KNEE VASU PAI Arthritic history is similar to that of the hip. Add history of give way and locking, swelling INJURY MECHANISM When How Sequence Progress Disability IKDC Activity I - Strenuous activity
The Appendicular Skeleton
 8 The Appendicular Skeleton PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris 8-1 The Pectoral Girdle The Pectoral Girdle Also called shoulder girdle Connects the
8 The Appendicular Skeleton PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris 8-1 The Pectoral Girdle The Pectoral Girdle Also called shoulder girdle Connects the
Elbow, Wrist & Hand Evaluation.
 Elbow, Wrist & Hand Evaluation www.fisiokinesiterapia.biz Common Injuries to the Elbow, Wrist, Hand & Fingers Lateral epicondylitis tennis elbow Medial epicondylitis golfer s s elbow, little league elbow
Elbow, Wrist & Hand Evaluation www.fisiokinesiterapia.biz Common Injuries to the Elbow, Wrist, Hand & Fingers Lateral epicondylitis tennis elbow Medial epicondylitis golfer s s elbow, little league elbow
