Development of Partial Thickness Articular Cartilage Injury in an Ovine Model
|
|
|
- Cordelia Goodwin
- 5 years ago
- Views:
Transcription
1 Development of Partial Thickness Articular Cartilage Injury in an Ovine Model Yan Lu, 1 Mark D. Markel, 1 Carol Swain, 2 Lee D. Kaplan 2 1 Comparative Orthopaedic Research Laboratory, School of Veterinary Medicine, University of Wisconsin-Madison, Madison, Wisconsin Division of Sports Medicine, Department of Orthopedics and Rehabilitation, University of Wisconsin-Madison, Madison, Wisconsin Received 15 February 2006; accepted 12 May 2006 Published online 7 August 2006 in Wiley InterScience ( DOI /jor ABSTRACT: The purpose of this study was to create a controlled partial thickness cartilage lesion in a sheep model, and to provide a foundation to study the natural history of the progression of this lesion. Twenty-eight sheep divided into four groups (1, 12, 24, and 52 weeks, n ¼ 7/group) were used in this study. In one stifle, a mechanical tool was used to create a 200 mm partial thickness lesion ( cm 2 ) on the medial femoral condyle via arthroscopy. Joint fluid was drawn presurgery and after euthanasia for analysis of collage II 3/4 C long (C2C). After euthanasia, the condyle was analyzed by gross appearance, confocal laser microscopy (CLM) for cell viability, scanning electronic microscopy (SEM) for surface roughness, Artscan for cartilage stiffness, and histology for cartilage morphology. The gross appearance of the treated area appeared rough, soft, and swollen compared to untreated control over time. CLM demonstrated that the depth of cell death increased to 590 mm at 52 weeks after surgery. SEM demonstrated that the treated area became more irregular over time. Stiffness of the treated area was significantly less than control by 12 weeks after surgery. Histologic analysis demonstrated that the 12, 24, and 52 week groups had significantly poorer histologic scores than the 1 week group. Joint fluid analysis demonstrated that the treatment group at 1 week had significant higher levels of C2C than the pretreatment baseline data. The results of this study demonstrated that partial thickness injury of cartilage continued to propagate and degenerate over time in this sheep model. Options for the prevention or treatment of this lesion may be tested using this model in the future. ß 2006 Orthopaedic Research Society. Published by Wiley Periodicals, Inc. J Orthop Res 24: , 2006 Keywords: articular cartilage; chondrocyte; partial thickness; sheep; confocal laser microscopy INTRODUCTION Partial thickness articular cartilage (PARC) lesions are commonly encountered in orthopedic surgery. 1 These lesions do not have the ability to heal themselves, due to lack of vascular supply and the reliance on synovial nutrition. 2 However, Hunziker and Rosenberg 3 demonstrated that the failure of PARC lesions to heal is not entirely due to the lack of access to mesenchymal cells in perivascular tissue, although their experiments did not result in repaired cartilage. Yoshioka et al. 4 also reported that the repair mechanisms of partial cartilage injury differed according to injury direction using a rat model. Better repair Correspondence to: Lee D. Kaplan (Telephone: ; Fax: ; kaplan@orthorehab.wisc.edu) ß 2006 Orthopaedic Research Society. Published by Wiley Periodicals, Inc. was obtained when the injury was parallel to the direction of joint motion rather than perpendicular to joint motion. The clinical quandary presented by PARC lesions is one with no clear answer. 5 Surgical techniques and options have focused on stabilization of PARC lesions to halt further degeneration. These techniques include mechanical and thermal chondroplasty The use of thermal energy whether laser or radio-frequency generated has been controversial. The primary issue is the viability and denaturation of the remaining articular cartilage after thermal treatment. 7,11 16 Recently, there has been increased focus on the various techniques used to evaluate the cartilage after treatment This has included histological techniques such as hematoxylin and eosin staining and confocal laser microscopy. The utilization of metabolic techniques may add significant information regarding the cellular chondrocyte activity 1974 JOURNAL OF ORTHOPAEDIC RESEARCH OCTOBER 2006
2 PARC INJURY IN AN OVINE MODEL 1975 that occurs following cartilage injury. 14 A combination of all available techniques for cartilage evaluation should provide the most accurate assessment of treatment modalities. The basic science of the natural history of PARC lesions is necessary to fully evaluate current and future treatment techniques. Therefore, an in vivo animal model would provide important information with regard to the clinical applicability of these techniques. To date, the literature on articular cartilage lesions has focused primarily on fulldepth lesions, with only a few studies methodically addressing partial-thickness lesions. 3,20,21 These studies have examined the ability of the lesion to repair itself, or to improve repair through supplemental growth factors in rabbits and miniature swine. 3,20,21 In 2002, Marijnissen et al. 22,23 reported using a Kirschner-wire to make grooves on the weight-bearing area of the femoral condyles in order to induce osteoarthritis (OA) in a canine model. The results of these studies demonstrated that the degenerative joint damage in the canine groove model was slowly progressive over time and showed characteristics identical to those seen in the anterior cruciate ligament (ACL) transaction model. In 2006, Mastbergen et al. 24 further demonstrated that changes observed in the canine groove model were not just the expression of the surgically applied damage but were the result of progressive features of experimental OA. However, the Kirschner-wire used to create damage of the articular cartilage in these studies was not well controlled. The purpose of this study was to create a more precisely controlled PARC lesion that was confined to the cartilage and did not lead to global OA, which would be evaluated by morphology, histology, cell viability, and collagen II destruction over time. This study should serve the orthopedic community by establishing a natural history of PARC lesions and providing a novel, well-characterized model for testing current and future treatment options for these lesions. MATERIALS AND METHODS Twenty-eight mature female sheep, ranging in age from 2 to 5 years and weighing between 60 and 100 kg ( kg: mean SD) were utilized in the study. All experimental protocols were approved by the Institutional Animal Use and Care Committee. Joint fluid was collected from both treatment and contralateral control knee joints in each sheep just before surgery as baseline data for the analysis of collagen II 3/4 C long (C2C) using a technique as previously described. 25 Surgery was carried out under general anesthesia with halothane and oxygen inhalation via endotracheal intubation. Using aseptic techniques, arthroscopy was performed in one randomly selected ovine stifle. Each joint was approached via a stab incision lateral to the distal aspect of the patellar ligament to allow insertion of the arthroscope for the visualization of the medial condyle. A mechanical shaver was used to remove the fat pad for a clearer view if necessary. A second stab incision was made medial to the distal aspect of the patellar ligament to allow insertion of a custom-designed Dremel tool. The Dremel tool with spring-coil controlled pressure tip (depth of tool teeth: 200 mm) was applied to the central surface of the medial condyle to create an approximately cm 2 roughened area (lesion depth of approximately 200 mm) under arthroscopic guidance (Fig. 1A, B). The spring-coil on the tip Figure 1. Image demonstrating the Dremel tool with spring-coil controlled pressure tip (A) roughening the ovine medial condyle (B). After treatment, the condylar surface appeared rough and irregular (C). DOI /jor JOURNAL OF ORTHOPAEDIC RESEARCH OCTOBER 2006
3 1976 LU ET AL. maintained a pressure force of approximately 250 g. If the pressure force applied on the tip was greater than 250 g, the spring-coil would be over-bent to prevent deeper damage on the cartilage surface. The roughened cartilaginous surface approximated grade 2 chondromalacia with protruding fine fronds based on the Outerbridge system (Fig. 1C). The joints were irrigated by lactated Ringer s solution at room temperature during the operation. The contralateral stifle served as an untreated control. After surgery, the operated sheep were allowed to move freely. Sheep were sacrificed at 1, 12, 24, and 52 weeks after surgery (n ¼ 7/time group). After euthanasia, joint fluid was drawn from both treatment and control joints for the analysis of C2C as previously described, 25 then both treatment and control medial condyles were harvested and digitally photographed for evaluation of gross appearance of the cartilaginous surfaces. Following photography, articular cartilage stiffness measurements using the Artscan 2000 TM probe (Artscan Oy., Helsinki, Finland) were taken of the treated area in the treated stifle and the relevant identical area of the control stifle as described by a previous study. 26 The Artscan 2000 TM probe is an electromechanical indentation probe that can be used to measure mechanical stiffness of tissue. It consists of a measurement rod (5 mm in diameter and 150 mm in length), an indenter (300 mm in diameter and 1.3 mm in length) located at the end of the rod and in the center of a 208 inclined reference plate, a bending beam attached to the indenter via two force transducers that measure force applied to the tissue surface, and another pair of transducers that measure force applied on the reference plate against the cartilage surface. Consistent measurements were taken by applying a constant 10 N force to the cartilage surface for 1 s intervals over 60 s, and recording the mean indenter force, which is a measure of stiffness. An average of three mean stiffness values was taken and calculated. After Artscan mechanical testing, harvested medial condyles were cut by band saw with phosphate-buffered saline (PBS) irrigation to prevent frictional heat into small osteochondral blocks including the treatment area with 0.5 cm of its associated subchondral bone. A lowspeed saw equipped with PBS solution flushing (Buehler, Isomet 2000, Lake Bluff, IL) was used to cut the osteochondral block into two slices with a thickness of 1.5 and 2.5 mm, respectively. The 1.5 mm thick slices were analyzed for chondrocyte viability by confocal laser microscopy (CLM) on the same day of the harvest. After taking the CLM image, the same specimen was used for general histologic analysis. The 2.5 mm thick slice was processed for scanning electron microscopy (SEM). The 1.5 mm thick cartilage slices were stained by incubation in a 1.0 ml PBS containing 0.4 ml calcein (acetoxymethylester)/10 ml ethidium homodimer (Molecular Probes, Eugene, OR) for 30 min at room temperature. The method of determining the location of surviving cells was based on the knowledge that viable and nonviable cells differ in their ability to exclude fluorescent dyes. The cell membranes of dead, damaged, or dying cells are penetrated by ethidium homodimer to stain their nuclei red. Living cells with intact plasma membranes and active esterases metabolize calcein (acetoxymethyl ester) and show cytoplasmic green fluorescence. The method of analysis utilized a 1.5 mm thick cartilage slice that was placed on a glass slide and moistened by several drops of PBS. A confocal laser microscope (MRC-1024; Bio-Rad, Hemel Hempsted/ Cambridge, England) equipped with a krypton/argon laser and the necessary filter systems (fluorecein: 522DF32 and rhodamine: 585EFLP) was employed using the triple-labeling technique as previously described. 15,27 All cartilage samples were examined blinded to group assignment. The confocal laser microscope was calibrated using a micrometer measured through the objective lens (2X) used for this project. The pixel length measured on images was converted to micrometers. The mean depth of chondrocyte death (mean depth of three deepest areas of chondrocyte death) was determined in each CLM image of the osteochondral section with Adobe PhotoShop TM (Version 5.0.2; San Jose, CA). After CLM analysis, the same 1.5 mm thick cartilage slice was fixed in 10% neutral buffered formalin, then decalcified and embedded in paraffin. Sections 5 mm thick were cut and stained with hematoxylin-eosin to show general morphology and with Safranin-O to stain proteoglycan in the extracellular matrix. The microscope was calibrated using a micrometer measured through the objective lens (4) used for this project. The pixel length measured on images was converted to micrometers. The mean depth of clefts (mean depth of three deepest clefts on cartilage surface) was determined in each histologic image of the osteochondral section with Adobe Photo- Shop TM The section from each specimen was examined blindly by three senior researchers (Y.L., M.D.M., L.K.), and then the cartilage structure, Safranin-O staining, cell morphology, chondrocyte viability, and tidemark integrity were assessed. Cell viability was evaluated based on the data from CLM. Each of these characteristics was given a score according to a modified Mankin s scoring system described in a previous study. 28 Lower scores indicate better histologic appearance. The 2.5 mm thick cartilage slice cut for SEM was rinsed thoroughly in three changes of normal saline to remove synovial fluid. Then, the cartilage slice was fixed in modified Karnovsky s solution (2% glutaraldehyde in 0.1 mol/l sodium cacodylate buffer, ph 7.4) for 2 h, and then washed in 0.1 mol/l sodium cacodylate buffer twice at room temperature. The samples were stored in 0.1 mol/l sodium phosphate buffer for 8 h at 48C. The samples were dehydrated in a graded series of ethanol (50, 70, 80, 95, 100%), air dried, coated with gold in a Bio-Rad E5000M gold coater, and examined with a Hitachi S570 SEM (Hitachi High Technologies Corp., Tokyo, Japan). Analysis of variance (ANOVA) was used to evaluate the data of mean depth of chondrocyte death, mean depth of clefts on cartilage surface, cartilage stiffness, and C2C levels. When ANOVA revealed significant differences over time, a Duncan s Multiple Range Test was performed to separate these differences. Comparison of JOURNAL OF ORTHOPAEDIC RESEARCH OCTOBER 2006 DOI /jor
4 PARC INJURY IN AN OVINE MODEL 1977 the histologic subjective scores among treatment groups based on the medians was performed by the Kruskal- Wallis test. If the Kruskal-Wallis test demonstrated differences among the groups, the Mann-Whitney U test was used to evaluate these differences. Interobserver precision error was also determined among researchers for histological analysis. Differences were considered to be significant at a probability level of 95% ( p < 0.05). All statistical analyses were performed with a commercially available software program (SAS Version 8e; SAS Institute Inc., Cary, NC). RESULTS Gross appearance of the treated area appeared rough and swollen compared to control over time. Probing of the cartilage surface indicated that the treated area was softer than control beginning at 12 weeks after surgery (Fig. 2). Stiffness of the treated area measured by Artscan was significantly less than control in the 12, 24, and 52 week groups ( p < 0.05). There was no significant difference in the stiffness between treatment and control in the 1 week group (Table 1). CLM demonstrated that the depth of cell death significantly increased over time in the treatment groups, whereas all chondrocytes were viable in the control group for each time interval (Figs. 3 and 4). The depths of chondrocyte death in the 12 (mean SD: mm), 24 ( mm), and 52 week treatment groups ( mm) were significantly greater than that in the 1 week treatment group ( mm) ( p < 0.05). The depths of chondrocyte death in the 24 and 52 week treatment groups were also significantly greater compared to that in the 12 week treatment group ( p < 0.05), whereas there was no significant difference in the depth of chondrocyte death between the 24 and 52 week treatment groups ( p > 0.05). Interobserver precision error for histologic scores was 3.6%. The control in all time groups demonstrated a smooth cartilaginous surface with normal Safranin-O staining (Fig. 5). Histologic images showed that the depth of clefts on the cartilage surface in the 1 week treatment group was significantly less than those in 12, 24, and 52 week treatment groups (Fig. 6) ( p < 0.05). In addition, cloned cells were clearly present in the treated area beginning at 12 weeks. Histologic analysis demonstrated that the 1 week treatment group had a significantly better histologic appearance than the 12, 24, and 52 week treatment groups ( p < 0.05). There were no significant differences in the depths of clefts or histologic scores among the 12, 24, and 52 week treatment groups ( p > 0.05). SEM revealed that the cartilaginous surfaces in all control groups appeared smooth (Fig. 7). SEM demonstrated that the treated area became more irregular over time. The cartilaginous surfaces in the 1 and 12 week treatment groups had fibrillation without clearly detected clefts and fissures. Wider Figure 2. Gross appearance of the medial condylar surface of control (A) and treated specimens at 24 weeks after surgery (arrows) (B). DOI /jor JOURNAL OF ORTHOPAEDIC RESEARCH OCTOBER 2006
5 1978 LU ET AL. Table 1. Artscan Data for Control and Treatment Groups 1 Week 12 Weeks 24 Weeks 52 Weeks Control a a a Treatment b b b Values represent mean standard deviation. Different letters within a column represent differences between control and treatment groups ( p < 0.05). and deeper clefts were easily detected in the 24 and 52 week treatment groups (Fig. 7). For the control knee joints, joint fluid analysis demonstrated that there were no significant differences in the C2C level between any time point and the control baseline data ( p > 0.05). There were also no significant differences in the C2C levels over time ( p > 0.05). For the treatment knee joints, the C2C level in the 1 week treatment group was significantly higher than the pretreatment baseline data ( p < 0.05). There were no significant differences in the C2C level between the treatment and the baseline data at 12 and 52 weeks ( p > 0.05). The C2C level in the 24 week group significantly decreased compared to the baseline data ( p < 0.05). In addition, the C2C levels in the 24 and 52 week treatment groups were significantly less compared to that in the 1 week treatment group ( p < 0.05), whereas there were no significant differences in the C2C levels among the 12, 24, and 52 week treatment groups ( p < 0.05). Figure 3. CLM demonstrating the cartilage surface of a 52 week control specimen (top of the image) and subchondral bone (bottom of the image) (original magnification 20). The green dots indicate viable cells, and the red dots indicate dead cells. In the 52 week control group, all chondrocytes were viable. DISCUSSION The results of this study demonstrated that the development of a PARC lesion in an ovine model was successfully established, and biomechanical, biochemical, and histological characteristics and surface ultrastructural appearance of this PARC lesion continued to progress over time. Although the goat has recently been recommended by ICRS (International Cartilage Research Society) as the animal choice for articular cartilage repair, the reason that we chose the sheep in this study was that the size of the joint in a sheep is larger than in a goat of the same weight, which made it easier to insert the arthroscope and Dremel tool in the joint to roughen the medial condylar cartilage. Importantly, sheep are much easier to obtain in our area than goats. Using arthroscopic techniques to create a PARC lesion may significantly reduce the damage to the surrounding tissue and prevent unnecessary edema and stress on the animal during the perioperative period. The PARC lesion created by the Dremel tool in this study was selected for the weight bearing area of the medial condyle in order to mimic the clinical situation. A recent study performed by Hjelle et al. 29 demonstrated that 58% of articular cartilage lesions in 1,000 knee arthroscopies occurred on the medial femoral condyle. The stiffness analysis by Artscan demonstrated that the treated area was softer compared to contralateral control beginning at 12 weeks after surgery. By 24 weeks after surgery, probing the treated area revealed even more swelling and softening as typically occurs in chondromalacia. We hypothesized that this was caused by the Dremel tool breaking down and rupturing the superficial layers of cartilage during the surgery. The clefts on the cartilaginous surface progressed to deeper levels and the proteoglycan concentration continued to decrease over time as seen in Figures 6 and 7. The indentation response of articular cartilage is dependent upon the high tensile stiffness of the superficial collagen layer, in addition to the JOURNAL OF ORTHOPAEDIC RESEARCH OCTOBER 2006 DOI /jor
6 PARC INJURY IN AN OVINE MODEL 1979 Figure 4. CLM of treated medial femoral condyles. (A) One week group. (B) Twelve week group. (C) Twenty-four week group. (D) Fifty-two week group. The depth of chondrocyte death increased over time (original magnification 20). Figure 5. Safranin-O (S/O) staining of a decalcified section of the medial femoral condyle in the control group at 52 weeks. The morphology of the cartilage appeared normal with smooth surface (S/O staining; original magnification 40). compressive stiffness provided by proteoglycans in the matrix. The superficial collagen layer in the treated area was damaged, which might be partially responsible for the reduced stiffness properties seen in the treated area as previously reported. 30,31 In response to traumatic injury, chondrocytes appear to undergo a response that includes apoptosis with cumulative changes for as long as 1 week after injury. This apoptotic response is thought to be important in the degenerative process. 32,33 This is the reason why we selected 1 week after surgery as the first time point to analyze. The CLM demonstrated that the mean depth of chondrocyte death at 1 week was approximately 250 mm and progressed to 590 mm at 52 weeks after surgery. This result indicated that the chondrocytes in the treated area continued to die over time. Whether this cell death is the result of simple necrosis or apoptosis remains unclear. We hypothesized that the cell death may result from the combination of necrosis and apoptosis. However, there are indications that the apoptosis accounts for the cell death DOI /jor JOURNAL OF ORTHOPAEDIC RESEARCH OCTOBER 2006
7 1980 LU ET AL. Figure 6. S/O staining of the decalcified sections of the medial femoral condyles in the treated groups. (A) Articular surface in the 1 week group appeared fibrillated with fine fronds protruding and clefts were around 250 mm deep. (B) The depth of clefts in the 12 week group increased with S/O staining decreased. Cloned chondrocytes appeared in the treated area (arrows). (C, D) In the 24 and 52 week groups, the clefts were deeper and the S/O staining decreased compared to the 12 week group (S/O staining; original magnification 40). Figure 7. (A D) SEM demonstrating the control at 1, 12, 24, and 52 weeks with smooth cartilage surface. (E, F) In 1 and 12 week groups, the cartilage surface appeared fibrillated with fine fronds. (G, H) In 24 and 52 week groups, the clefts and fissures were wider and deeper (original magnification 120). JOURNAL OF ORTHOPAEDIC RESEARCH OCTOBER 2006 DOI /jor
8 PARC INJURY IN AN OVINE MODEL 1981 after the creation of lesions in cultured fetal sternal cartilage. 34,35 Histologic analysis demonstrated that the fissures or clefts created by the Dremel tool in the treated area continued to progress to deeper levels over time as affirmed by SEM images shown in Figure 6. This finding implies that repetitive loading on the treated area after surgery degraded the articular cartilage matrix and initiated progressive cartilage degeneration and fibrillation as other investigators have reported. 36,37 Histologic scores for the 1 week group were much better than those groups from 12 weeks and greater. This further demonstrated that the degradation of articular cartilage occurred over time in this ovine model. Damage to type II collagen with increased collagenase activity is one fundamental feature in OA. 38,39 Determination of C2C level in the joint fluid has been used as one of the useful indicators to predict OA. 25,40 Compared to pretreatment baseline data, the C2C level of the treated joint in this study increased significantly at 1 week after surgery but then decreased to pretreatment levels over time. We hypothesized that the type II collagen degradation products may correlate with the early inflammatory process, when the collagenase levels are likely to be the highest in the joint fluid. However, the lack of a sham-operated control group in this study may influence the results of C2C analysis when compared to the baseline data in a normal knee. The CLM and histologic analyses demonstrated that the depths of chondrocyte death and clefts on the cartilage surface did not propagate from 24 to 52 weeks after surgery. SEM analysis also revealed that the wider and deeper fissures were present on cartilaginous surface at both 24 and 52 weeks after surgery. These findings may indicate that the process of the PARC lesion did not progress significantly between 24 and 52 weeks after surgery. This may suggest that this PARC lesion model could be produced at 24 weeks after the treatment by the technique used in this ovine model. Several issues of this study deserve discussion. First, an untreated contralateral stifle was used as a control, instead of a sham operated stifle (arthroscopy, irrigation, remove the fat pad if necessary). For this study, we felt it important to compare the lesion to a completely normal joint rather than one where the synovium and fat pad were disrupted. Unfortunately, based on this study design we can not differentiate the effects of the arthroscope approach from the cartilage lesion that was created. Second, no cartilage metabolic analysis such as MTT conversion and proteoglycan 35 S incorporation was performed in this study because the size of the PARC lesion was not large enough for these analyses. Third, this study was designed to evaluate a PARC lesion that did not lead to global OA in the joint; therefore it was different from studies utilizing ACL transaction or thermal treatment to induce joint instability as a trigger for development of OA. 41,42 Fourth, although there were no significant differences in cell viability, depth of clefts, and surface morphology for the PARC lesion between 24 and 52 weeks, the outcome for this PARC lesion at a longer time point than 52 weeks has not been determined. Future studies need to be performed. In summary, this study demonstrated that the PARC lesions created on the weight bearing area of the medial femoral condyle may progress up to and then stabilize at 24 weeks after treatment. Currently, surgical options for this lesion primarily focus on removing fronds and fibrillated cartilage with mechanical debridement and/or thermal modification. This study provided a simple and safe animal model for observing the natural history and propagation of PARC lesions. This study also enabled the study of different treatment options for PARC lesions and early articular lesions. ACKNOWLEDGMENTS The authors thank John Bogdanske, Todd Forsythe, Matt Wisniewski, and Julie Sauer for their assistance with this project. This project was funded by grant support from the Orthopaedic Research and Education Foundation (OREF) and the UW Sports Medicine Fund. REFERENCES 1. Curl WW, Krome J, Gordon ES, et al Cartilage injuries: a review of 31,516 knee arthroscopies. Arthroscopy 13: Buckwalter JA, Mankin HJ Articular cartilage Part II: degeneration and osteoarthrosis, repair, regeneration, and transplantation. J Bone Joint Surg Am 79: Hunziker EB, Rosenberg LC Repair of partialthickness defects in articular cartilage: cell recruitment from the synovial membrane. J Bone Joint Surg Am 78: Yoshioka M, Kubo T, Coutts RD, et al Differences in the repair process of longitudinal and transverse injuries of cartilage in the rat knee. Osteoarthritis Cart 6: Baker CL, Jr., Ferguson CM Future treatment of osteoarthritis. Orthopedics 28:s227 s Edwards RB, Lu Y, Kalscheur VL, et al Thermal chondroplasty of chondromalacic human cartilage: an ex DOI /jor JOURNAL OF ORTHOPAEDIC RESEARCH OCTOBER 2006
9 1982 LU ET AL. vivo comparison of bipolar and monopolar radiofrequency devices. Am J Sports Med 30: Kaab MJ, Bail HJ, Rotter A, et al Monopolar radiofrequency treatment of partial-thickness cartilage defects in the sheep knee joint leads to extended cartilage injury. Am J Sports Med 33: Kaplan LD, Ionescu D, Ernsthausen JM, et al Temperature requirements for altering the morphology of osteoarthritic and nonarthritic articular cartilage: in vitro thermal alteration of articular cartilage. Am J Sports Med 32: Lu Y, Edwards RB, III, Nho S, et al Thermal chondroplasty with bipolar and monopolar radiofrequency energy: effect of treatment time on chondrocyte death and surface contouring. Arthroscopy 18: Owens BD, Stickles BJ, Balikian P, et al Prospective analysis of radiofrequency versus mechanical debridement of isolated patellar chondral lesions. Arthroscopy 18: Caffey S, McPherson E, Moore B, et al Effects of radiofrequency energy on human articular cartilage: an analysis of 5 systems. Am J Sports Med 33: Edwards RB, Lu Y, Rodriguez E, et al Thermometric determination of cartilage matrix temperatures during thermal chondroplasty: comparison of bipolar and monopolar radiofrequency devices. Arthroscopy 18: Kaplan L, Uribe JW, Sasken H, et al The acute effects of radiofrequency energy in articular cartilage: an in vitro study. Arthroscopy 16: Kaplan LD The analysis of articular cartilage after thermal exposure: Is red really dead?. Arthroscopy 19: Lu Y, Edwards RB, Cole BJ, et al Thermal chondroplasty with radiofrequency energy: an in vitro comparison of bipolar and monopolar radiofrequency devices. Am J Sports Med 29: Lu Y, Hayashi K, Hecht P, et al The effect of monopolar radiofrequency energy on partial-thickness defects of articular cartilage. Arthroscopy 16: Kaplan LD, Chu CR, Bradley JP, et al Recovery of chondrocyte metabolic activity after thermal exposure. Am J Sports Med 31: Mainil-Varlet P, Monin D, Weiler C, et al Quantification of laser-induced cartilage injury by confocal microscopy in an ex vivo model. J Bone Joint Surg Am 83: Zuger BJ, Ott B, Mainil-Varlet P, et al Laser solder welding of articular cartilage: tensile strength and chondrocyte viability. Lasers Surg Med 28: Hunziker EB Articular cartilage repair: are the intrinsic biological constraints undermining this process insuperable? [Review] [103 refs]. Osteoarthritis Cart 7: Hunziker EB, Quinn TM Surgical removal of articular cartilage leads to loss of chondrocytes from cartilage bordering the wound edge. J Bone Joint Surg Am 85 Suppl 2: Marijnissen AC, van Roermund PM, Tekoppele JM, et al The canine groove model, compared with the ACLT model of osteoarthritis. Osteoarthritis Cart 10: Marijnissen AC, van Roermund PM, Verzijl N, et al Steady progression of osteoarthritic features in the canine groove model. Osteoarthritis Cart 10: Mastbergen SC, Marijnissen AC, Vianen ME, et al The canine groove model of osteoarthritis is more than simply the expression of surgically applied damage. Osteoarthritis Cart 14: Chu Q, Lopez M, Hayashi K, et al Elevation of a collagenase generated type II collagen neoepitope and proteoglycan epitopes in synovial fluid following induction of joint instability in the dog. Osteoarthritis Cart 10: Cook JL, Kuroki K, Kenter K, et al Bipolar and monopolar radiofrequency treatment of osteoarthritic knee articular cartilage: acute and temporal effects on cartilage compressive stiffness, permeability, cell synthesis, and extracellular matrix composition. J Knee Surg 17: Lu Y, Edwards RB, Kalscheur VL, et al Effect of bipolar radiofrequency energy on human articular cartilage: comparison of confocal laser microscopy and light microscopy. Arthroscopy 17: Kuroki H, Nakagawa Y, Mori K, et al Acoustic stiffness and change in plug cartilage over time after autologous osteochondral grafting: correlation between ultrasound signal intensity and histological score in a rabbit model. Arthritis Res Ther 6:R492 R Hjelle K, Solheim E, Strand T, et al Articular cartilage defects in 1,000 knee arthroscopies. Arthroscopy 18: Jurvelin JS, Arokoski JP, Hunziker EB, et al Topographical variation of the elastic properties of articular cartilage in the canine knee. J Biomech 33: Lyyra T, Arokoski JP, Oksala N, et al Experimental validation of arthroscopic cartilage stiffness measurement using enzymatically degraded cartilage samples. Phys Med Biol 44: Gibson G Active role of chondrocyte apoptosis in endochondral ossification. Microsc Res Tech 43: O Driscoll SW Preclinical cartilage repair: current status and future perspectives. Clin Orthop 391(Suppl): S397 S Tew SR, Kwan AP, Hann A, et al The reactions of articular cartilage to experimental wounding: role of apoptosis. Arthritis Rheum 43: Walker EA, Verner A, Flannery CR, et al Cellular responses of embryonic hyaline cartilage to experimental wounding in vitro. J Orthop Res 18: Buckwalter JA Articular cartilage injuries. Clin Orthop 402: Weightman B Tensile fatigue of human articular cartilage. J Biomech 9: Elsaid KA, Chichester CO Review: Collagen markers in early arthritic diseases. Clin Chim Acta 365: Lohmander LS, Atley LM, Pietka TA, et al The release of crosslinked peptides from type II collagen into human synovial fluid is increased soon after joint injury and in osteoarthritis. Arthritis Rheum 48: Billinghurst RC, Dahlberg L, Ionescu M, et al Enhanced cleavage of type II collagen by collegenases in osteoarthritic articular cartilage. J Clin Invest 99: Batiste DL, Kirkley A, Laverty S, et al Ex vivo characterization of articular cartilage and bone lesions in a rabbit ACL transection model of osteoarthritis using MRI and micro-ct. Osteoarthritis Cart 12: Lopez MJ, Markel MD Anterior cruciate ligament rupture after thermal treatment in a canine model. Am J Sports Med 31: JOURNAL OF ORTHOPAEDIC RESEARCH OCTOBER 2006 DOI /jor
Thermal chondroplasty using the Smith & Nephew DYONICS GLIDER Articular Cartilage Probe
 Knee Series Technique Guide Thermal chondroplasty using the Smith & Nephew DYONICS GLIDER Articular Cartilage Probe Reviewed by: Dr. James H. Lubowitz, MD Director Taos Orthopaedic Institute Taos, New
Knee Series Technique Guide Thermal chondroplasty using the Smith & Nephew DYONICS GLIDER Articular Cartilage Probe Reviewed by: Dr. James H. Lubowitz, MD Director Taos Orthopaedic Institute Taos, New
Thermal Chondroplasty With Bipolar and Monopolar Radiofrequency Energy: Effect of Treatment Time on Chondrocyte Death and Surface Contouring
 Thermal Chondroplasty With Bipolar and Monopolar Radiofrequency Energy: Effect of Treatment Time on Chondrocyte Death and Surface Contouring Yan Lu, M.D., Ryland B. Edwards III, D.V.M., M.S., Shane Nho,
Thermal Chondroplasty With Bipolar and Monopolar Radiofrequency Energy: Effect of Treatment Time on Chondrocyte Death and Surface Contouring Yan Lu, M.D., Ryland B. Edwards III, D.V.M., M.S., Shane Nho,
Chondrocyte Viability and Metabolic Activity After Treatment of Bovine Articular Cartilage With Bipolar Radiofrequency: An In Vitro Study
 Chondrocyte Viability and Metabolic Activity After Treatment of Bovine Articular Cartilage With Bipolar Radiofrequency: An In Vitro Study David Amiel, Ph.D., Scott T. Ball, M.D., and James P. Tasto, M.D.
Chondrocyte Viability and Metabolic Activity After Treatment of Bovine Articular Cartilage With Bipolar Radiofrequency: An In Vitro Study David Amiel, Ph.D., Scott T. Ball, M.D., and James P. Tasto, M.D.
Why the dog? Analogy of the anatomy
 Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Disclosures: C.B. Raub: None. B.C. Hansen: None. T. Yamaguchi: None. M.M. Temple-Wong: None. K. Masuda: None. R.L. Sah: None.
 En Face Microscopy of Rabbit Knee Articular Cartilage Following Anterior Cruciate Ligament Transection Reveals Early Matrix Damage, Chondrocyte Loss and Cloning Christopher B. Raub, PhD, Bradley C. Hansen,
En Face Microscopy of Rabbit Knee Articular Cartilage Following Anterior Cruciate Ligament Transection Reveals Early Matrix Damage, Chondrocyte Loss and Cloning Christopher B. Raub, PhD, Bradley C. Hansen,
Radiofrequency energy (RFE) has gained popularity
 Effect of Bipolar Radiofrequency Energy on Human Articular Cartilage: Comparison of Confocal Laser Microscopy and Light Microscopy Yan Lu, M.D., Ryland B. Edwards III, D.V.M., M.S., Vicki L. Kalscheur,
Effect of Bipolar Radiofrequency Energy on Human Articular Cartilage: Comparison of Confocal Laser Microscopy and Light Microscopy Yan Lu, M.D., Ryland B. Edwards III, D.V.M., M.S., Vicki L. Kalscheur,
Thermal Chondroplasty of Chondromalacic Human Cartilage
 0363-5465/102/3030-0090$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 30, No. 1 2002 American Orthopaedic Society for Sports Medicine Thermal Chondroplasty of Chondromalacic Human Cartilage An
0363-5465/102/3030-0090$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 30, No. 1 2002 American Orthopaedic Society for Sports Medicine Thermal Chondroplasty of Chondromalacic Human Cartilage An
Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice
 Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice Basak Doyran 1, Wei Tong 2, Qing Li 1, Haoruo Jia 2, Xianrong Zhang 3,
Nanomechanical Symptoms in Cartilage Precede Histological Osteoarthritis Signs after the Destabilization of Medial Meniscus in Mice Basak Doyran 1, Wei Tong 2, Qing Li 1, Haoruo Jia 2, Xianrong Zhang 3,
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3
 AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
Arthroscopic Evaluation of Radiofrequency Chondroplasty of the Knee
 Arthroscopic Evaluation of Radiofrequency Chondroplasty of the Knee Ilya Voloshin,* MD, Kenneth R. Morse, MD, C. Dain Allred, MD, Scott A. Bissell, MD, Michael D. Maloney, MD, and Kenneth E. DeHaven, MD
Arthroscopic Evaluation of Radiofrequency Chondroplasty of the Knee Ilya Voloshin,* MD, Kenneth R. Morse, MD, C. Dain Allred, MD, Scott A. Bissell, MD, Michael D. Maloney, MD, and Kenneth E. DeHaven, MD
Bone&JointAppraisal Vol
 Bone&JointAppraisal Vol 01 No 03 December 2016 COBLATION Chondroplasty Versus Mechanical Debridement: Randomized Controlled Trial with 10-Year Outcomes -Year Four-Year Ten-Year Group A COBLATION technology
Bone&JointAppraisal Vol 01 No 03 December 2016 COBLATION Chondroplasty Versus Mechanical Debridement: Randomized Controlled Trial with 10-Year Outcomes -Year Four-Year Ten-Year Group A COBLATION technology
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Osteochondritis Dissecans
 Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Osteochondral Transplant Delivery System
 Osteochondral Transplant Delivery System Team Leader: Alex Teague BPAG: David Fiflis Communicator/BWIG: Alex Babinski BSAC: Zach Wodushek Client: Dr. Brian Walczak, DO Advisor: Dr. Tracy Puccinelli, PhD
Osteochondral Transplant Delivery System Team Leader: Alex Teague BPAG: David Fiflis Communicator/BWIG: Alex Babinski BSAC: Zach Wodushek Client: Dr. Brian Walczak, DO Advisor: Dr. Tracy Puccinelli, PhD
Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee
 1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
Osteochondral regeneration. Getting to the core of the problem.
 Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of the Tibia
 Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Osteoarthritis. Dr Anthony Feher. With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides
 Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
CASE REPORT GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT
 Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
ULTRASONIC DEVICE IN BONE CUTTING
 Acta orthop. scand. 52, 5-10, 1981 ULTRASONIC DEVICE IN BONE CUTTING A Histological and Scanning Electron Microscopical Study H. ARO*, H. KALLIONIEMI**, A. J. AHO* & P. KELLOKUMPU-LEHTINEN*** *Department
Acta orthop. scand. 52, 5-10, 1981 ULTRASONIC DEVICE IN BONE CUTTING A Histological and Scanning Electron Microscopical Study H. ARO*, H. KALLIONIEMI**, A. J. AHO* & P. KELLOKUMPU-LEHTINEN*** *Department
A Patient s Guide to Osteochondritis Dissecans of the Knee
 A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
SUPPLEMENTAL DIGITAL CONTENT (SDC)
 Orozco_Osteoarthritis_MSC_v4.3.doc Mar_1_2013 1 SUPPLEMENTAL DIGITAL CONTENT (SDC) Contents: SUPPLEMENTARY TABLES Supplementary Table S1. Antecedent history of the patients included in this trial. Supplementary
Orozco_Osteoarthritis_MSC_v4.3.doc Mar_1_2013 1 SUPPLEMENTAL DIGITAL CONTENT (SDC) Contents: SUPPLEMENTARY TABLES Supplementary Table S1. Antecedent history of the patients included in this trial. Supplementary
Surgical Removal of Articular Cartilage Leads to Loss of Chondrocytes from Cartilage Bordering the Wound Edge
 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Surgical Removal of Articular Cartilage Leads to Loss of Chondrocytes from
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Surgical Removal of Articular Cartilage Leads to Loss of Chondrocytes from
Osteochondral Transplant Delivery System
 Osteochondral Transplant Delivery System Team Leader: Alex Teague Communicator: Josiah Wolf BWIG: David Fiflis BPAG: Zach Wodushek BSAC: Grace Li Client: Dr. Brian Walczak, DO Advisor: Dr. William Murphy,
Osteochondral Transplant Delivery System Team Leader: Alex Teague Communicator: Josiah Wolf BWIG: David Fiflis BPAG: Zach Wodushek BSAC: Grace Li Client: Dr. Brian Walczak, DO Advisor: Dr. William Murphy,
Introduction to Biomedical Engineering
 Introduction to Biomedical Engineering FW 16/17, AUT Biomechanics of tendons and ligaments G. Rouhi Biomechanics of tendons and ligaments Biomechanics of soft tissues The major soft tissues in musculoskeletal
Introduction to Biomedical Engineering FW 16/17, AUT Biomechanics of tendons and ligaments G. Rouhi Biomechanics of tendons and ligaments Biomechanics of soft tissues The major soft tissues in musculoskeletal
Cruciate Ligament. Summary of the Doctoral Thesis
 Study of the Effect of Excessive Tibial Plateau Angle on Degenerative Changes of Canine Cranial Cruciate Ligament Summary of the Doctoral Thesis Tom Ichinohe Graduate School of Veterinary Medicine and
Study of the Effect of Excessive Tibial Plateau Angle on Degenerative Changes of Canine Cranial Cruciate Ligament Summary of the Doctoral Thesis Tom Ichinohe Graduate School of Veterinary Medicine and
Advanced Hip Arthroscopy
 Advanced Hip Arthroscopy S C OT T D. M A R T I N, M D D I R E C T O R, J O I N T P R E S E R V A T I O N D I R E C T O R, M G H S P O R T S M E D I C I N E F E L L O W S H I P A S S O C I A T E P R O F
Advanced Hip Arthroscopy S C OT T D. M A R T I N, M D D I R E C T O R, J O I N T P R E S E R V A T I O N D I R E C T O R, M G H S P O R T S M E D I C I N E F E L L O W S H I P A S S O C I A T E P R O F
Basics of Cartilage Restoration Introduction of TruFit
 Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary
 SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Effect Of Centralization For Extruded Meniscus Extrusion In A Rat Model
 Effect Of Centralization For Extruded Meniscus Extrusion In A Rat Model Kenichi Kawabata 1, Nobutake Ozeki 1, Hideyuki Koga 1, Yusuke Nakagawa 1, Mio Udo 1, Ryusuke Saito 1, Katsuaki Yanagisawa 1, Toshiyuki
Effect Of Centralization For Extruded Meniscus Extrusion In A Rat Model Kenichi Kawabata 1, Nobutake Ozeki 1, Hideyuki Koga 1, Yusuke Nakagawa 1, Mio Udo 1, Ryusuke Saito 1, Katsuaki Yanagisawa 1, Toshiyuki
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Repair of Articular Cartilage Full Thickness Defects with Cultured Chondrocytes Placed on Polysulphonic Membrane Experimental Studies in Rabbits
 Biocybernetics and Biomedical Engineering 2008, Volume 28, Number 2, pp. 87 93 Repair of Articular Cartilage Full Thickness Defects with Cultured Chondrocytes Placed on Polysulphonic Membrane Experimental
Biocybernetics and Biomedical Engineering 2008, Volume 28, Number 2, pp. 87 93 Repair of Articular Cartilage Full Thickness Defects with Cultured Chondrocytes Placed on Polysulphonic Membrane Experimental
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR FOCAL ARTICULAR CARTILAGE LESIONS
 CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Meniscus Reconstruction: Trough Surgical Technique
 Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Biologics in ACL: What s the Data?
 Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
Case study #11 Rt. knee
 The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
The Efficacy of Intra-Articular Hyaluronan Injection After the Microfracture Technique for the Treatment of Articular Cartilage Lesions
 AJSM PreView, published on February 9, 9 as doi:1.1177/3635465838415 The Efficacy of Intra-Articular Hyaluronan Injection After the Microfracture Technique for the Treatment of Articular Cartilage Lesions
AJSM PreView, published on February 9, 9 as doi:1.1177/3635465838415 The Efficacy of Intra-Articular Hyaluronan Injection After the Microfracture Technique for the Treatment of Articular Cartilage Lesions
Disclosures: A.G. Bajpayee: None. A.M. Scheu: None. R.M. Porter: None. A.J. Grodzinsky: None.
 Avidin as a Carrier for Drug Delivery into Cartilage: Electrostatic Interactions Enable Rapid Penetration, Enhanced Uptake, and Retention in Rat Knee Joints Ambika Goel Bajpayee 1, Alfredo M. Scheu 2,
Avidin as a Carrier for Drug Delivery into Cartilage: Electrostatic Interactions Enable Rapid Penetration, Enhanced Uptake, and Retention in Rat Knee Joints Ambika Goel Bajpayee 1, Alfredo M. Scheu 2,
Comparison and Characterization of In Vitro and In Vivo Treatments of Lubricin-Mimetics on Articular Cartilage
 Comparison and Characterization of In Vitro and In Vivo Treatments of Lubricin-Mimetics on Articular Cartilage Kirk J. Samaroo 1, Mingchee Tan 1, Marco Demange 2, Ashley Titan 3, Camila Carballo 1, Marco
Comparison and Characterization of In Vitro and In Vivo Treatments of Lubricin-Mimetics on Articular Cartilage Kirk J. Samaroo 1, Mingchee Tan 1, Marco Demange 2, Ashley Titan 3, Camila Carballo 1, Marco
Osteoarthritis. RA Hughes
 Osteoarthritis RA Hughes Osteoarthritis (OA) OA is the most common form of arthritis and the most common joint disease Most of the people who have OA are older than age 45, and women are more commonly
Osteoarthritis RA Hughes Osteoarthritis (OA) OA is the most common form of arthritis and the most common joint disease Most of the people who have OA are older than age 45, and women are more commonly
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Evaluation of Bioadhesive Mesh Construct to Augment Achilles Tendon Repair in a Rabbit Model
 Evaluation of Bioadhesive Mesh Construct to Augment Achilles Tendon Repair in a Rabbit Model Yan Lu, MD 1, Brett Nemke 1, Jackie Kondratko 1, Vicki kalscheur 1, Gino Bradica 2, Ray Vanderby 1, Mark D.
Evaluation of Bioadhesive Mesh Construct to Augment Achilles Tendon Repair in a Rabbit Model Yan Lu, MD 1, Brett Nemke 1, Jackie Kondratko 1, Vicki kalscheur 1, Gino Bradica 2, Ray Vanderby 1, Mark D.
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
Evaluation of the wound healing response post deep dermal heating by fractional RF: INTRAcel
 12th symposium of the Association of Korean Dermatologists (2009) 1 Evaluation of the wound healing response post deep dermal heating by fractional RF: INTRAcel Un-Cheol.Yeo, M.D. S&U Dermatologic Clinic,
12th symposium of the Association of Korean Dermatologists (2009) 1 Evaluation of the wound healing response post deep dermal heating by fractional RF: INTRAcel Un-Cheol.Yeo, M.D. S&U Dermatologic Clinic,
Arthroscopy in sports medicine
 Arthroscopy in sports medicine DR PABITRA KUMAR SAHOO, ASSISTANT PROFESSOR (PMR) Sports medicine is a special branch of rehab specialty which deals with training in anatomy, biomechanics, pathophysiology
Arthroscopy in sports medicine DR PABITRA KUMAR SAHOO, ASSISTANT PROFESSOR (PMR) Sports medicine is a special branch of rehab specialty which deals with training in anatomy, biomechanics, pathophysiology
Horizon Scanning Centre November Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects
 Horizon Scanning Centre November 2014 Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects SUMMARY NIHR HSC ID: 8515 This briefing is based on information
Horizon Scanning Centre November 2014 Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects SUMMARY NIHR HSC ID: 8515 This briefing is based on information
Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D.
 Medial Plicae and Degeneration of the Medial Femoral Condyle Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D. Purpose: The purpose of this study was to evaluate and analyze the chronological changes
Medial Plicae and Degeneration of the Medial Femoral Condyle Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D. Purpose: The purpose of this study was to evaluate and analyze the chronological changes
Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation for the Repair of Chondral Defects of the Knee
 International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine Cancun, Mexico MAY 12 16, 2019 Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation
International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine Cancun, Mexico MAY 12 16, 2019 Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation
COR. Precision Targeting Cartilage Repair System. Arthroscopic Technique for Repair of Osteochondral Defects
 COR Precision Targeting Cartilage Repair System Arthroscopic Technique for Repair of Osteochondral Defects Planning the Procedure An 18-gauge spinal needle is initially used to plan a perpendicular approach
COR Precision Targeting Cartilage Repair System Arthroscopic Technique for Repair of Osteochondral Defects Planning the Procedure An 18-gauge spinal needle is initially used to plan a perpendicular approach
Evaluation of the wound healing response post - deep dermal heating by fractional RF: INTRACEL
 12th symposium of the Association of Korean Dermatologists (2009) 1 Evaluation of the wound healing response post - deep dermal heating by fractional RF: INTRACEL Un-Cheol.Yeo, MD S&U Dermatologic Clinic,
12th symposium of the Association of Korean Dermatologists (2009) 1 Evaluation of the wound healing response post - deep dermal heating by fractional RF: INTRACEL Un-Cheol.Yeo, MD S&U Dermatologic Clinic,
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Histopomorphic Evaluation of Radiofrequency Mediated Débridement Chondroplasty
 The Open Orthopaedics Journal, 2010, 4, 211-220 211 Open Access Histopomorphic Evaluation of Radiofrequency Mediated Débridement Chondroplasty Kumkum Ganguly 1, Ian D. McRury 2, Peter M. Goodwin 3, Roy
The Open Orthopaedics Journal, 2010, 4, 211-220 211 Open Access Histopomorphic Evaluation of Radiofrequency Mediated Débridement Chondroplasty Kumkum Ganguly 1, Ian D. McRury 2, Peter M. Goodwin 3, Roy
Osteochondral Transplant System
 Osteochondral Transplant System Rodrigo Umanzor (Team Leader) Nick Zacharias (BWIG & BSAC) Bilin Loi (BPAG) Eduardo Enriquez (Communicator) Client: Dr. Brian Walczak, DO Advisor: Dr. Kris Saha, PhD February
Osteochondral Transplant System Rodrigo Umanzor (Team Leader) Nick Zacharias (BWIG & BSAC) Bilin Loi (BPAG) Eduardo Enriquez (Communicator) Client: Dr. Brian Walczak, DO Advisor: Dr. Kris Saha, PhD February
Non-Invasive Characterization of Cartilage Properties Using MR Imaging
 Non-Invasive Characterization of Cartilage Properties Using MR Imaging by Sophia Natalie Ziemian Department of Biomedical Engineering Duke University Date: Approved: Farshid Guilak, Supervisor Lori A.
Non-Invasive Characterization of Cartilage Properties Using MR Imaging by Sophia Natalie Ziemian Department of Biomedical Engineering Duke University Date: Approved: Farshid Guilak, Supervisor Lori A.
ABNORMAL SOFTENING IN ARTICULAR CARTILAGE
 1209 ABNORMAL SOFTENING IN ARTICULAR CARTILAGE Its Relationship to the Collagen Framework NEIL D. BROOM Abnormal softening in articular cartilage is related to the presence of collagen fibers strongly
1209 ABNORMAL SOFTENING IN ARTICULAR CARTILAGE Its Relationship to the Collagen Framework NEIL D. BROOM Abnormal softening in articular cartilage is related to the presence of collagen fibers strongly
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
o~ r;'c' - OSTEOARTHRITIS
 Osteoarthritis and Cartilage (2001) 9, Supplement A, S102-S108 2001 OsteoArthritis Research Society International doi:10.1053/joca.2001.0451, available online at http://www.idealibrary.com on IDE~l Osteoarthritis
Osteoarthritis and Cartilage (2001) 9, Supplement A, S102-S108 2001 OsteoArthritis Research Society International doi:10.1053/joca.2001.0451, available online at http://www.idealibrary.com on IDE~l Osteoarthritis
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries. Cartilage Surgery. The Knee.
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Determining Collagen Distribution in Articular Cartilage by X-ray Micro-computed Tomography
 Determining Collagen Distribution in Articular Cartilage by X-ray Micro-computed Tomography Heikki J. Nieminen, Ph.D. 1, Mikko A. Finnilä, MHS 2, Sami Kauppinen 2, Tuomo Ylitalo 1,2, Edward Hæggström,
Determining Collagen Distribution in Articular Cartilage by X-ray Micro-computed Tomography Heikki J. Nieminen, Ph.D. 1, Mikko A. Finnilä, MHS 2, Sami Kauppinen 2, Tuomo Ylitalo 1,2, Edward Hæggström,
Disclaimers. Concerns after ACL Tear 3/13/2018. Outcomes after ACLR. Sports, Knee, Shoulder Symposium Snowbird, Utah February 24, 2018
 Outcomes after ACLR Sports, Knee, Shoulder Symposium Snowbird, Utah February 24, 2018 Christopher Kaeding M.D. Judson Wilson Professor of Orthopaedics Executive Director, OSU Sports Medicine Medical Director,
Outcomes after ACLR Sports, Knee, Shoulder Symposium Snowbird, Utah February 24, 2018 Christopher Kaeding M.D. Judson Wilson Professor of Orthopaedics Executive Director, OSU Sports Medicine Medical Director,
Knee Cartilage Transplants
 Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
QUANTIFICATION OF CHONDROCYTE MORPHOLOGY BY CONFOCAL ARTHROSCOPY
 Journal of Musculoskeletal Research, Vol. 8, No. 4 (2004) 145 154 World Scientific Publishing Company ORIGINAL ARTICLES QUANTIFICATION OF CHONDROCYTE MORPHOLOGY BY CONFOCAL ARTHROSCOPY C. W. Jones *, D.
Journal of Musculoskeletal Research, Vol. 8, No. 4 (2004) 145 154 World Scientific Publishing Company ORIGINAL ARTICLES QUANTIFICATION OF CHONDROCYTE MORPHOLOGY BY CONFOCAL ARTHROSCOPY C. W. Jones *, D.
BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS IN TOTAL KNEE REPLACEMENTS
 Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
Testing Micronized Amnion as a Therapeutic for OA in a Rat Model using Contrast Based Micro-CT Imaging
 Testing Micronized Amnion as a Therapeutic for OA in a Rat Model using Contrast Based Micro-CT Imaging Tanushree Thote, B.S 1, Sanjay Sridaran 2, Angela S.P. Lin 3, Nick J. Willett, Ph.D. 2, Robert E.
Testing Micronized Amnion as a Therapeutic for OA in a Rat Model using Contrast Based Micro-CT Imaging Tanushree Thote, B.S 1, Sanjay Sridaran 2, Angela S.P. Lin 3, Nick J. Willett, Ph.D. 2, Robert E.
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING.
 LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
TITLE: Local Blockade of CCL21 and CXCL13 Signaling as a New Strategy to Prevent and Treat Osteoarthritis
 AWARD NUMBER: W1XWH-15-1-31 TITLE: Local Blockade of CCL1 and CXCL13 Signaling as a New Strategy to Prevent and Treat Osteoarthritis PRINCIPAL INVESTIGATOR: Bouchra Edderkaoui., Ph.D. CONTRACTING ORGANIZATION:
AWARD NUMBER: W1XWH-15-1-31 TITLE: Local Blockade of CCL1 and CXCL13 Signaling as a New Strategy to Prevent and Treat Osteoarthritis PRINCIPAL INVESTIGATOR: Bouchra Edderkaoui., Ph.D. CONTRACTING ORGANIZATION:
R. Todd Allen, M.D., Ph.D., James P. Tasto, M.D., Jeffrey Cummings, M.D., Catherine M. Robertson, M.D., and David Amiel, Ph.D.
 Meniscal Debridement With an Arthroscopic Radiofrequency Wand Versus an Arthroscopic Shaver: Comparative Effects on Menisci and Underlying Articular Cartilage R. Todd Allen, M.D., Ph.D., James P. Tasto,
Meniscal Debridement With an Arthroscopic Radiofrequency Wand Versus an Arthroscopic Shaver: Comparative Effects on Menisci and Underlying Articular Cartilage R. Todd Allen, M.D., Ph.D., James P. Tasto,
MRI of Cartilage. D. BENDAHAN (PhD)
 MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
Introduction Knee Anatomy and Function Making the Diagnosis
 Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE?
 HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE? To help horse owners better understand the tools we routinely use at VetweRx to evaluate their horse s soundness, the following section of this website reviews
HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE? To help horse owners better understand the tools we routinely use at VetweRx to evaluate their horse s soundness, the following section of this website reviews
Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model
 Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model Yusuke Hagiwara 1,2, Nathaniel A. Dyment 3, Douglas J. Adams 3, Shinro
Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model Yusuke Hagiwara 1,2, Nathaniel A. Dyment 3, Douglas J. Adams 3, Shinro
Case study #12 Left knee
 The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
Rakesh Patel, MD 4/9/09
 Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Intraosseous Bio Filler. Surgical Technique
 Intraosseous Bio Filler Surgical Technique Intraosseous Bio Filler Surgical Technique Introduction The Intraosseous Bio Filler technique is the treatment of bone pathologies resulting from acute or chronic
Intraosseous Bio Filler Surgical Technique Intraosseous Bio Filler Surgical Technique Introduction The Intraosseous Bio Filler technique is the treatment of bone pathologies resulting from acute or chronic
Surface characteristics of human articular cartilagea scanning electron microscope study
 J. Anat. (1971), 108, 1, pp. 23-30 23 With 16 figures Printed in Great Britain Surface characteristics of human articular cartilagea scanning electron microscope study IAN C. CLARKE BioEngineering Unit,
J. Anat. (1971), 108, 1, pp. 23-30 23 With 16 figures Printed in Great Britain Surface characteristics of human articular cartilagea scanning electron microscope study IAN C. CLARKE BioEngineering Unit,
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
AIMS We will all come across osteo- and rheumatoid arthritis whatever our clinical practice Overview of pathology of osteoarthritis, its assessment an
 Osteoarthritis and Rheumatoid Arthritis Mr. Guy Barham FY1 & FY2 Orthopaedic Curriculum June 2007 AIMS We will all come across osteo- and rheumatoid arthritis whatever our clinical practice Overview of
Osteoarthritis and Rheumatoid Arthritis Mr. Guy Barham FY1 & FY2 Orthopaedic Curriculum June 2007 AIMS We will all come across osteo- and rheumatoid arthritis whatever our clinical practice Overview of
Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status
 # 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
# 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
Latest Treatments for Hip Arthritis. Michael J. Repine MD Boulder Medical Center Orthopedics You re Not Alone
 Latest Treatments for Hip Arthritis Michael J. Repine MD Boulder Medical Center Orthopedics 303-502-9404 You re Not Alone More than 43 million people have some form of arthritis. It is estimated that the
Latest Treatments for Hip Arthritis Michael J. Repine MD Boulder Medical Center Orthopedics 303-502-9404 You re Not Alone More than 43 million people have some form of arthritis. It is estimated that the
RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM
 RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM D R. A M R I S H K R. J H A M S ( O R T H O ) A S S I S T A N T P R O F E S S O R M E D I C A L C O L L E G E, K O L K A T A LABRUM Function as a chock-block,
RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM D R. A M R I S H K R. J H A M S ( O R T H O ) A S S I S T A N T P R O F E S S O R M E D I C A L C O L L E G E, K O L K A T A LABRUM Function as a chock-block,
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Optimal Differentiation of Tissue Types Using Combined Mid and Near Infrared Spectroscopy
 Optimal Differentiation of Tissue Types Using Combined Mid and Near Infrared Spectroscopy Mugdha V. Padalkar, M.S. 1, Cushla M. McGoverin, Ph.D. 1, Uday P. Palukuru, M.S. 1, Nicholas J. Caccese 1, Padraig
Optimal Differentiation of Tissue Types Using Combined Mid and Near Infrared Spectroscopy Mugdha V. Padalkar, M.S. 1, Cushla M. McGoverin, Ph.D. 1, Uday P. Palukuru, M.S. 1, Nicholas J. Caccese 1, Padraig
Anisotropy of Tensile Strengths of Bovine Dentin Regarding Dentinal Tubule Orientation and Location
 Original paper Dental Materials Journal 21 (1): 32-43, 2002 Anisotropy of Tensile Strengths of Bovine Dentin Regarding Dentinal Tubule Orientation and Location Toshiko INOUE, Hidekazu TAKAHASHI and Fumio
Original paper Dental Materials Journal 21 (1): 32-43, 2002 Anisotropy of Tensile Strengths of Bovine Dentin Regarding Dentinal Tubule Orientation and Location Toshiko INOUE, Hidekazu TAKAHASHI and Fumio
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH
 PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
CHONDROTOXICITY OF LOCAL ANESTHETIC
 CHONDROTOXICITY OF LOCAL ANESTHETIC Sport Med 2017 Jas Chahal MD FRCSC MSc MBA University of Toronto NO DISCLOSURES Objectives To understand the clinical presentation and pathogenesis of chondrolysis Differentiate
CHONDROTOXICITY OF LOCAL ANESTHETIC Sport Med 2017 Jas Chahal MD FRCSC MSc MBA University of Toronto NO DISCLOSURES Objectives To understand the clinical presentation and pathogenesis of chondrolysis Differentiate
Evaluation and Treatment of Intra-articular Fractures. Benjamin Maxson, DO Florida Orthopaedic Institute Orthopaedic Trauma Service
 Evaluation and Treatment of Intra-articular Fractures Benjamin Maxson, DO Florida Orthopaedic Institute Orthopaedic Trauma Service Disclosures Nothing to disclose Articular Fractures: Overview Require
Evaluation and Treatment of Intra-articular Fractures Benjamin Maxson, DO Florida Orthopaedic Institute Orthopaedic Trauma Service Disclosures Nothing to disclose Articular Fractures: Overview Require
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System
 Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
Meniscus cartilage replacement with cadaveric
 Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
The Effect of Varus Stress on the Moving Rabbit Knee Joint
 The Effect of Varus Stress on the Moving Rabbit Knee Joint KOSUKE OGATA, M.D., LEO A. WHITESIDE, M.D., PEGGY A. LESKER, B.S. AND DAVID J. SIMMONS, PH.D. Many attempts have been made to induce osteoarthritis
The Effect of Varus Stress on the Moving Rabbit Knee Joint KOSUKE OGATA, M.D., LEO A. WHITESIDE, M.D., PEGGY A. LESKER, B.S. AND DAVID J. SIMMONS, PH.D. Many attempts have been made to induce osteoarthritis
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Changes in the temporomandibular joint after mandibular lengthening with different rates of distraction
 Shujuan Zou, DDS, MS Department of Orthodontics Jing Hu, DDS, MS, PhD Dazhang Wang, DDS, FICD Jihua Li, DDS, MS Zhenglong Tang, DDS, MS Department of Oral and Maxillofacial Surgery Huaxi School of Stomatology
Shujuan Zou, DDS, MS Department of Orthodontics Jing Hu, DDS, MS, PhD Dazhang Wang, DDS, FICD Jihua Li, DDS, MS Zhenglong Tang, DDS, MS Department of Oral and Maxillofacial Surgery Huaxi School of Stomatology
Arthritis of the Shoulder
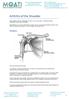 Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
