Eye (2013) 27, & 2013 Macmillan Publishers Limited All rights reserved X/13 S Basu, S Nayak, TR Padhi and T Das
|
|
|
- Brett McKinney
- 5 years ago
- Views:
Transcription
1 (2013) 27, & 2013 Macmillan Publishers Limited All rights reserved X/13 Progressive ocular inflammation following antitubercular therapy for presumed ocular tuberculosis in a high-endemic setting S Basu, S Nayak, TR Padhi and T Das CLINICAL STUDY Abstract Purpose To analyze the incidence and clinical course of patients developing progressive ocular inflammation following anti-tubercular therapy (ATT) for presumed ocular tuberculosis (TB). Methods Retrospective analysis of medical records of patients who received ATT for presumed ocular TB and completed at least 12 months follow-up after initiation of ATT. The diagnosis of presumed ocular TB was based on presence of ocular signs suggestive of TB, evidence of past tubercular infection, and exclusion of mimicking clinical entities. All patients received a combination of ATT and corticosteroid therapy. Primary outcome measure was progression (worsening) of ocular inflammation, defined as a two-step increase in level of inflammation (anterior chamber/ vitreous) or the appearance of new lesions following initiation of ATT. Results A total of 106 patients (64 male, 42 female) received ATT for presumed ocular TB. Twenty-six (24.5%) patients developed progressive intraocular inflammation following ATT. Primary diagnoses in these patients were: anterior uveitis (n ¼ 1), intermediate uveitis (n ¼ 9), retinal vasculitis (n ¼ 3), serpiginous-like choroiditis (n ¼ 7), multifocal choroiditis (n ¼ 2), and pan-uveitis (n ¼ 4). Following progressive inflammation, diagnosis was revised in two patients (7.7%) both responded to alternative therapy. Of the rest, majority (n ¼ 16; 61.5%) resolved with escalation of corticosteroid therapy. Five patients (19.2%) all having intermediate uveitis required therapeutic vitrectomy for resolution. Three patients (11.5%) had persistent inflammation at end of follow-up period. Conclusion Progressive inflammation following ATT for presumed ocular TB is common. It generally resolves on escalation of corticosteroid therapy. Cases not responding to increased immunosuppression need to be re-investigated to rule out a nontubercular cause. (2013) 27, ; doi: /eye ; published online 1 March 2013 Keywords: inflammation; tuberculosis; ocular; anti-tubercular therapy; progressive inflammation Introduction One-third of the world s population is infected with Mycobacterium tuberculosis and can potentially manifest features of ocular tuberculosis (TB). 1 Not surprisingly, TB accounts for large proportion of infectious uveitis cases in endemic countries. 2 The benefits of anti-tubercular therapy (ATT) in treatment of TB-associated uveitis are well documented. 3 Several clinical indicators of ocular TB (applicable in high-endemic settings) have also been identified based on the response to ATT. 4 However, in most cases, the diagnosis of ocular TB remains presumptive because of lack of definitive (microscopy, culture, or PCR) evidence. In such situations, progressive ocular inflammation following ATT can pose a serious diagnostic challenge for the treating physician. It L V Prasad Institute, Bhubaneswar, India Correspondence: S Basu, L V Prasad Institute, Patia, Bhubaneswar , India. Tel: þ ; Fax: þ eyetalk@gmail.com Received: 20 April 2012 Accepted in revised form: 26 December 2012 Published online: 1 March 2013
2 658 Management of TB-associated uveitis can be attributed to missed diagnosis, drug resistance, reinfection, or immunological response to tubercular antigens released during ATT each requiring a different approach to management. Although an alternative diagnosis or drug resistance may need change in specific anti-microbial therapy, immunological reaction to tubercular antigens is usually managed by escalating corticosteroid therapy. Previous studies on role of ATT in ocular TB do not provide detailed analysis of such cases of progressive ocular inflammation. A large study from India (216 patients) mentions that 15.74% (nearly one in six) patients developed recurrent inflammation despite ATT. 3 The anatomic location of uveitis and tuberculin reactivity in these patients has been mentioned. However, the clinical details, time of recurrence, and further course of management have not been described. More recently, continued progression after ATT has been described in patients with tuberculous serpiginous-like choroiditis (SLC). 5 There are no large studies describing such progressive inflammation in other forms of ocular TB. In the present study, we have further analyzed the incidence, clinical presentation, revised diagnoses, and response to treatment in patients who developed progressive ocular inflammation following ATT for presumed ocular TB. Materials and methods We retrospectively analyzed medical records of all patients who were diagnosed as presumed ocular TB and advised ATT between 1 April 2008 and 15 June 2010 at our center, a tertiary care facility in eastern India. All patients were of South Asian ethnicity and were identified by a disease register maintained in the uveitis clinic. We included patients who were initiated on ATT and completed a minimum of 1-year follow-up after initiation of such therapy. All patients had a detailed recording of history including contact with known TB patients. A complete examination was done including visual acuity, applanation tonometry, slit lamp biomicroscopy, and dilated fundus evaluation. Standardization of uveitis nomenclature working group recommendations were used for anatomical classification of uveitis and grading of anterior chamber inflammation. 6 The National Institute system was adopted for grading vitreous haze. Ancillary tests like fluorescein angiography, optical coherence tomography, B-scan ultrasonography, and ultrasound biomicroscopy were done as required. Systemic evaluation and laboratory investigations were guided by the pattern of uveitis identified on historytaking and ocular examination, though baseline investigations like complete blood counts, erythrocyte sedimentation rate, tuberculin test, and chest X-ray were done for all patients. Whenever TB was suspected as a possible etiology, special attention was paid to detection of other foci of extra-pulmonary TB. The diagnosis of presumed ocular TB was based on previously published guidelines. 3 These included the presence of clinical signs consistent with ocular TB, associated with any one or more of the following: (1) positive tuberculin reaction (induration 410 mm, with dosage of five tuberculin units) or interferon-gamma release assay; (2) evidence of active/healed pulmonary/ extra-pulmonary TB; (3) positive therapeutic response to four-drug ATT for 4 6 weeks; and (4) exclusion of other uveitis entities (infectious and noninfectious), which mimic the given clinical presentation of ocular TB. The cut off of 10 mm for the tuberculin test was based on the guidelines from Center of Disease Control, Atlanta, which has recommended this value for high-prevalence countries such as India. 7 In general, these guidelines recommend lower cut off limits for populations with higher pre-test probability of the disease. All patients with a positive tuberculin reaction or interferon-gamma release assay were also reviewed by an internist, before initiation of ATT. We treated all presumed ocular TB patients with a combination of ATT and corticosteroid therapy. ATT consisted of isoniazid 5 mg/kg/day, rifampicin 450 mg/ day if body weight was r50 kg and 600 mg/day if body weight was 450 kg, ethambutol 15 mg/kg/day, and pyrazinamide mg/kg/day for initial 2 months. Thereafter, rifampicin and isoniazid were used for another 4 months. The total duration of therapy was restricted to 6 months, based on the World Health Organization (WHO) recommendations for extra-pulmonary TB. 8 All patients were carefully monitored for compliance to ATT and drug toxicity by the treating internist. The routes of administration of corticosteroid therapy were based on the anatomical location of uveitis, whereas its dosage and duration depended on the degree of intraocular inflammation. In general, topical (±periocular) corticosteroids were preferred for anterior uveitis, periocular (±systemic) corticosteroids for intermediate uveitis, and oral (±intra-venous) corticosteroids for posterior and pan-uveitis. The starting dosage of oral corticosteroids (prednisolone), when required, was 1 mg/ kg body in all patients. Systemic immunosuppressives were used whenever deemed necessary. The primary outcome measure was progression (worsening) of inflammation, defined as a two-step increase in level of inflammation (anterior chamber/ vitreous) or the appearance of new lesions (eg, retinal vasculitis, choroidits, and optic neuritis) following initiation of ATT. Whenever such progression was noted, detailed ocular and systemic evaluation (including a
3 Management of TB-associated uveitis 659 repeat or new laboratory investigations, if required) was done to rule out any alternative diagnosis. If necessary, pulmonologist opinion was sought to rule out drug resistance. Where our working diagnosis remained presumed ocular TB, we escalated corticosteroid dosage (with/without additional systemic immunosuppressives), without discontinuing ATT. If an alternative diagnosis was considered, specific therapy was started for the given uveitis entity (eg, antibiotics for infectious uveitis). The following information was collected from patient records: patient s age, gender, disease laterality, presence of anterior chamber cells, flare, iris nodules, synechiae (anterior and posterior), lens status, vitreous cells, snowballs, pars plana exudates (snow-banking), retinal vasculitis, choroiditis (focal/multifocal/serpiginouslike), sub-retinal abscess, neuro-retinitis, optic neuritis, episcleritis, and scleritis. Because tubercular SLC is often multifocal, we termed superficial lesions with ameboid margins as SLC and deeper choroidal lesions as multifocal choroiditis. Details of treatment including dosage, duration, and routes of administration of corticosteroids and immunosuppressives, and the therapeutic response (quiescence or worsening/ progression of inflammation) were noted. In cases of worsening/progression, the current dose of corticosteroids, any revision in diagnosis, change in treatment plan, and outcome of such treatment were documented. Descriptive statistics like mean, median, SD, and range were used to evaluate the study population. Results In all, 134 out of 147 patients (n ¼ 134; 91.2%) agreed for ATT; 26 patients (19.4%) did not complete 1-year followup. Two patients discontinued treatment because of drug intolerance. Of the remaining 106 patients, 64 were male and 42 were female. The median age of these patients was 33.5 years (range years). The median followup period was 20 months (range months). Fifty-five (51.9%) patients had bilateral disease. Healed or active pulmonary TB (including hilar/mediastinal lymphadenopathy) was noted in 23 (21.7%) patients, and extra-pulmonary TB was seen in 3 (2.8%) patients. Focal lesions (healed or active chorioretinitis/choroiditis) were seen in more than half (33 out of 60, 55%) of the patients with anterior or intermediate uveitis or retinal vasculitis. The demographic details of patients in each clinical category of uveitis are provided in Table 1. In all, progressive intraocular inflammation after initiation of ATT was seen in 26 (24.5%) patients, the largest proportion (37%, 9 out of 27) being in those with intermediate uveitis (Table 2). The median time of onset of inflammation varied from 0.5 months in patients with SLC and multifocal choroiditis to 3.5 months in case of intermediate uveitis. In 22 patients (85.2%), the site of progressive inflammation was the same as presenting site. But in four cases, inflammatory signs were noted at a site different from the original one. This included one patient with unilateral granulomatous anterior uveitis who later developed bilateral multifocal choroiditis, one patient each of intermediate uveitis and SLC, who Table 1 Demographic details of patients with presumed ocular tuberculosis Anterior uveitis Intermediate uveitis Retinal vasculitis Serpiginouslike choroiditis Multifocal/ focal choroiditis Pan-uveitis Total patients Median age and range (in years) 35 (27 42) 39 (16 58) 26 (12 52) 33 (16 60) 27 (22 46) 38 (19 58) Gender Male Female Laterality Bilateral Unilateral Pulmonary TB (healed/active) Extra-pulmonary TB (nonocular) Associated focal chorio-retinal lesions (active/inactive) NA NA NA Initial treatment ATT þ local steroid 2 2 ATT þsystemic Steroid
4 660 Management of TB-associated uveitis Table 2 Clinical details for patients presenting with progressive ocular inflammation in each clinical category of presumed ocular tuberculosis Anterior uveitis (n ¼ 7) Intermediate uveitis (n ¼ 27) Retinal vasculitis (n ¼ 26) Serpiginous-like choroiditis (n ¼ 24) Multifocal/ focal choroiditis (n ¼ 9) Pan-uveitis (n ¼ 13) Number of patients who developed progressive inflammation Median time of onset of progression (in months, range) (1.5 14) 1.0 (0.5 14) 0.5 (0.25 5) ( ) Site of progressive inflammation Same as presenting site Different from presenting site Post-progression diagnosis Same as initial diagnosis (ocular TB) Alternative diagnosis 1 1 Undetermined 6 2 Status at last visit Resolved with increased corticosteroids Resolved with alternative therapy 6 1 Persistent inflammation 1 2 developed episcleritis, and one patient with retinal vasculitis who developed optic neuritis. All the four cases resolved on escalating corticosteroid therapy. Of the remaining 22 patients (progressive inflammation at the same site as at presentation), the original diagnosis was retained in majority (63.6%, n ¼ 16) of patients, all of who responded to escalation in corticosteroid dosage. However, only two out of nine patients with intermediate uveitis who worsened after initiating ATT responded to corticosteroid escalation. The diagnosis remained undetermined in six out of nine patients, five of whom resolved with therapeutic vitrectomy. Notably, none of these six patients had associated focal chorioretinal lesions, healed or active. One patient, who declined surgery, had persistent inflammation till last follow-up. The diagnosis was revised in two patients following onset of progressive inflammation. One patient with intermediate uveitis was diagnosed as Lyme s disease and responded to oral doxycycline therapy. Another patient with retinal vasculitis was later diagnosed as Behcet s uveitis, and required aggressive immunosuppressive therapy. Discussion Our study describes the spectrum of progressive ocular inflammation following initiation of ATT for various clinical manifestations of presumed ocular TB. It highlights the challenges faced by the treating physician in a high-endemic country while managing such cases. The likelihood of TB-associated uveitis is high in these countries, and so is the possibility of falsepositive diagnosis. The problem is compounded further by the variety of factors that can affect the treatment outcome, following ATT. Intermediate uveitis, retinal vasculitis, and SLC (in that order) were the most common clinical manifestations of presumed ocular TB in our study. Significantly, anterior uveitis accounted for only 6.6% cases, as against 31.5% (68 of 216 cases) in an earlier series. 3 Healed or active pulmonary TB (including hilar lymphadenopathy) was detected in only 21.7% patients, whereas extrapulmonary TB was seen in 2.8%. It is possible that more sensitive investigations like high-resolution computed tomography or positron emission tomography would have detected more systemic TB cases. 9 Almost a quarter (24.5%) of our patients developed progressive ocular inflammation following initiation of ATT. This included 16 patients (15.1%) who improved with escalation of corticosteroid therapy and 10 patients (9.4%) in whom the diagnosis was changed or remained undetermined. An earlier study by Bansal et al 3 had reported an overall recurrence rate of 15.7% after initiation of ATT for TB-associated uveitis. However, the cause of these recurrences had not been evaluated in this study. In the present study, progressive inflammation associated with most forms of presumed ocular TB
5 Management of TB-associated uveitis 661 (except intermediate uveitis) appeared to resolve on escalation of corticosteroid therapy. We believe that these cases represent paradoxical worsening (Jarisch Herxheimer reaction), which has been reported following initiation of chemotherapy for TB and several other infections. 5 This phenomenon is thought to result from release of mycobacterial antigens after ATT, strengthening of host immune response, and decrease in immunosuppression mechanisms. 10 Paradoxical worsening in ocular TB has been described both in immunocompromised and immunocompetent patients. 5,11 13 We have earlier described four cases of paradoxical worsening in the eye, two of which occurred following ATT for extra-ocular TB. 13 Gupta et al 5 reported 12 patients with SLC (14% of 84 patients in the study), who developed progressive inflammation following initiation of ATT. This is less than half of the 29.2% (7 out of 24 patients) incidence seen in our patients with SLC. The median time of progression in SLC patients was 0.5 months in our study that is less than the 4 weeks noted in the earlier series. 5 Anecdotal experience suggests that larger SLC lesions (representing a higher antigenic load) are more likely to develop such paradoxical worsening. Inadequate corticosteroid therapy (o1 mg/kg body weight/day) during initiation of ATT may also lead to disease progression. All the SLC patients in our study, as in the earlier series, improved with increased immunosuppression and continued ATT. In addition, the role of rifampicin in reducing the bioavailability of corticosteroids also needs to be considered. Rifampicin has been shown to increase the plasma clearance of prednisolone by 45% and reduce drug bioavailability in tissues by 66%. 14 Because we did not consider this factor in deciding corticosteroid dosage, we may have undertreated the inflammatory component of the disease that led to progressive inflammation. Noncompliance to ATT can also lead to disease progression. In the present study, noncompliance, as well as drug toxicity, was monitored by the treating physician. We also found paradoxical worsening in other forms of presumed ocular TB namely anterior uveitis, retinal vasculitis, multifocal choroiditis, and pan-uveitis. In addition, in four cases, we noted ocular inflammation at anatomical sites other than the presenting site. One patient with unilateral granulomatous anterior uveitis developed bilateral multifocal choroiditis, two developed episcleritis, and one patient developed optic neuritis. We speculate that this may be a result of multiple mycobacterial foci (and thereby antigenic stimulation) at various anatomical locations in the eye. However, in case of intermediate uveitis, majority of patients with progressive inflammation (seven out of nine) did not respond to increase in corticosteroid therapy. In one patient, the diagnosis was revised to Lyme s disease (and the patient responded to specific anti-microbial therapy), but in the remaining six, it remained undetermined. Five of these six patients resolved with therapeutic vitrectomy, whereas one patient had persistent inflammation till last follow-up. In an earlier series on intermediate uveitis from India, 5 out of 42 patients (11.9%) who received ATT for presumed tubercular etiology had recurrent ocular inflammation, though its management was not described. 15 We could not explain the high incidence of disease progression in our intermediate uveitis patients. Significantly, none of the intermediate uveitis patients with disease progression had associated focal chorio-retinal lesions. It is possible that the immunopathogenesis of intermediate uveitis is different from other forms of tubercular uveitis, and requires a different approach to management. The role of 6-month ATT as against longer-duration therapy in causing progressive ocular inflammation is debatable. Although some studies have recommended a longer duration of 9 18 months of therapy, 3,16 others have followed a 6-month ATT schedule. 17 We followed the WHO recommendations for extra-pulmonary TB. 8 Though a longer duration of 9 12 months is recommended for meningeal TB, there is no evidence to suggest that the same should be followed for ocular TB as well. Recently, Ang et al 16 reported that ATT of more than 9-month duration was superior to 6 9-month therapy in treatment of TB-associated uveitis. However, the sample size in this study was relatively small, and larger studies with longer follow-up are required to settle this debate. Importantly, we could not detect drug resistance in our patients with disease progression. However, multi-drug resistance is less frequently seen in extra-pulmonary TB than in pulmonary TB. 18 Also, in the absence of definitive ocular or systemic evidence (M. tuberculosis or its DNA) of TB, it is not possible to diagnose drug resistance. Development of PCR-based diagnostic techniques may resolve this issue in future. Reinfection, though rare, can also cause disease progression, but, like drug resistance, remains difficult to investigate in ocular TB. To summarize, our study provides a guideline to treating physicians to approach progressive ocular inflammation following ATT for presumed ocular TB. Most cases probably represent paradoxical worsening and resolve on escalation of corticosteroid therapy. In cases not responding to increased immunosuppression, targeted reinvestigations to rule out a nontubercular etiology and the possibility of drug interaction between rifampicin and corticosteroids need to be considered. However, the need for correct diagnosis at initial presentation itself, by detailed history and tailored laboratory investigations, remains vital.
6 662 Management of TB-associated uveitis Summary What was known before K Beneficial effect of anti-tubercular therapy in TBassociated uveitis paradoxical worsening of ocular inflammation following anti-tubercular therapy. What this study adds K Incidence and clinical course of progressive ocular inflammation following anti-tubercular therapy in various clinical manifestations of presumed ocular TB Guidelines for identification and management of different forms of progressive ocular inflammation. Conflict of interest The authors declare no conflict of interest. References 1 Bloom BR, Murray CJ. Tuberculosis: commentary on a reemergent killer. Science 1992; 257: Singh R, Gupta V, Gupta A. Pattern of uveitis in a referral eye clinic in north India. Indian J Ophthalmol 2004; 52: Bansal R, Gupta A, Gupta V, Dogra MR, Bambery P, Arora SK. Role of anti-tubercular therapy in uveitis with latent/manifest tuberculosis. Am J Ophthalmol 2008; 146: Gupta A, Bansal R, Gupta V, Sharma A, Bambery P. Ocular signs predictive of tubercular uveitis. Am J Ophthalmol 2010; 149: Gupta V, Bansal R, Gupta A. Continued progression of tubercular serpiginous-like choroiditis after initiating antituberculosis treatment. Am J Ophthalmol 2011; 152: Jabs DA, Nussenblatt RB, Rosenbaum JT. Standardization of Uveitis Nomenclature (SUN) Working Group. Standardization of uveitis nomenclature for reporting clinical data. Results of the first international workshop. Am J Ophthalmol 2005; 140: Centers for Disease Control. Targeted tuberculin testing and treatment of latent tuberculosis infection. MMWR Morb Mortal Wkly Rep 2000; 49: World Health Organization. Treatment of Tuberculosis: Guidelines. 4th edn World Health Organization: Geneva, Switzerland, 2010, pp Ganesh SK, Roopleen, Biswas J, Veena N. Role of highresolution computerized tomography (HRCT) of the chest in granulomatous uveitis: a tertiary uveitis clinic experience from India. Ocul Immunol Inflamm 2011; 19: Afghani B, Lieberman JM. Paradoxical enlargement or development of intracranial tuberculomas during therapy: case report and review. Clin Infect Dis 1994; 19: Rathinam SR, Lalitha P. Paradoxical worsening of ocular tuberculosis in HIV patients after anti-retroviral therapy. 2007; 21: Cheung CM, Chee SP. Jarisch-Herxheimer reaction: paradoxical worsening of tuberculosis chorioretinitis following initiation of antituberculous therapy. 2009; 23: Basu S, Das T. Pitfalls in the management of TB-associated uveitis. 2010; 24: McAllister WA, Thompson PJ, Al-Habet SM, Rogers HJ. Rifampicin reduces effectiveness and bioavailability of prednisolone. Br Med J (Clin Res Ed) 1983; 286: Parchand S, Tandan M, Gupta V, Gupta A. Intermediate uveitis in the Indian population. J Ophthalmic Inflamm Infect 2011; 1: Ang M, Hedayatfar A, Wong W, Chee SP. Duration of antitubercular therapy in uveitis associated with latent tuberculosis: a case-control study. Br J Ophthalmol 2012; 96: Gineys R, Bodaghi B, Carcelain G, Cassoux N, Boutin le TH, Amoura Z et al. QuantiFERON-TB gold cut-off value: implications for the management of tuberculosis related ocular inflammation. Am J Ophthalmol 2011; 152(3): e1. 18 Peto HM, Pratt RH, Harrington TA, LoBue PA, Armstrong LR. Epidemiology of extrapulmonary tuberculosis in the United States, Clin Infect Dis 2009; 49:
Bilateral multiple choroidal granulomas and systemic vasculitis as presenting features of tuberculosis in an immunocompetent patient
 Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
Role of high-resolution computerized tomography chest in identifying tubercular etiology in patients diagnosed as Eales disease
 Kharel (Sitaula) et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:4 DOI 10.1186/s12348-016-0120-1 Journal of Ophthalmic Inflammation and Infection ORIGINAL RESEARCH Open Access Role of
Kharel (Sitaula) et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:4 DOI 10.1186/s12348-016-0120-1 Journal of Ophthalmic Inflammation and Infection ORIGINAL RESEARCH Open Access Role of
Re-emerging infections: Syphilis & Tuberculosis
 Re-emerging infections: Syphilis & Tuberculosis Nicholas Jones Manchester Royal Eye Hospital Syphilis and TB - historical plagues? Syphilis incidence over 40yrs Manchester: Manchester: The Syphilis Capital
Re-emerging infections: Syphilis & Tuberculosis Nicholas Jones Manchester Royal Eye Hospital Syphilis and TB - historical plagues? Syphilis incidence over 40yrs Manchester: Manchester: The Syphilis Capital
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Tuberculous uveitis: association between anti-tuberculous therapy and clinical response in a non-endemic country
 Bajema et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:19 DOI 10.1186/s12348-017-0137-0 Journal of Ophthalmic Inflammation and Infection ORIGINAL RESEARCH Open Access Tuberculous uveitis:
Bajema et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:19 DOI 10.1186/s12348-017-0137-0 Journal of Ophthalmic Inflammation and Infection ORIGINAL RESEARCH Open Access Tuberculous uveitis:
In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between
 In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between the two, we also propose a classification system for
In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between the two, we also propose a classification system for
Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia
 JKAU: Med. Sci., Vol. 19 No. 3, pp: 73-83 (2012 A.D. / 1433 A.H.) DOI: 10.4197/Med. 19-3.6 Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia Nizamuddin Shaik Hakim Mohammad
JKAU: Med. Sci., Vol. 19 No. 3, pp: 73-83 (2012 A.D. / 1433 A.H.) DOI: 10.4197/Med. 19-3.6 Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia Nizamuddin Shaik Hakim Mohammad
Mycobacterial Ocular Inflammation. Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah
 Mycobacterial Ocular Inflammation Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah Financial Disclosure I have no financial interests or relationships to disclose. Applied anatomy What
Mycobacterial Ocular Inflammation Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah Financial Disclosure I have no financial interests or relationships to disclose. Applied anatomy What
Management of uveitis
 Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
Clinical spectrum of tuberculous optic neuropathy
 J Ophthal Inflamm Infect (2012) 2:183 189 DOI 10.1007/s12348-012-0079-5 ORIGINAL RESEARCH Clinical spectrum of tuberculous optic neuropathy Ellen J. Davis & Sivakumar R. Rathinam & Annabelle A. Okada &
J Ophthal Inflamm Infect (2012) 2:183 189 DOI 10.1007/s12348-012-0079-5 ORIGINAL RESEARCH Clinical spectrum of tuberculous optic neuropathy Ellen J. Davis & Sivakumar R. Rathinam & Annabelle A. Okada &
Optical coherence tomography findings in a child with posterior scleritis
 European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
Ocular Tuberculosis- An update
 December 2009 Biswas - Ocular tuberculosis 351 MAJOR REVIEW Ocular Tuberculosis- An update Dr. J. Biswas MS Introduction Tuberculosis (TB) is an air-borne disease that affects one-third of the world s
December 2009 Biswas - Ocular tuberculosis 351 MAJOR REVIEW Ocular Tuberculosis- An update Dr. J. Biswas MS Introduction Tuberculosis (TB) is an air-borne disease that affects one-third of the world s
Update on management of Anterior Uveitis
 Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
o White dot syndromes pattern recognition o Activity and damage o Quality of life o Key points o Idiopathic o Sarcoidosis o Multiple sclerosis
 Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient
 CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
Eye (2009) 23, & 2009 Macmillan Publishers Limited All rights reserved X/09 $32.00
 (2009) 23, 543 548 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye Effects of the duration of initial oral corticosteroid treatment on the recurrence of inflammation
(2009) 23, 543 548 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye Effects of the duration of initial oral corticosteroid treatment on the recurrence of inflammation
Intravitreal Triamcinolone Acetonide for Macular Edema in HLA-B27 Negative Ankylosing Spondylitis
 105 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
105 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
Let s Talk TB A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year
 A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Madhukar Pai, MD, PhD Author and Series Editor Camilla Rodrigues, MD co-author Abstract Most individuals who get exposed
A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Madhukar Pai, MD, PhD Author and Series Editor Camilla Rodrigues, MD co-author Abstract Most individuals who get exposed
A Clinical Study of Anterior Uveitis in a Rural Hospital
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. III. (Mar. 2014), PP 55-59 A Clinical Study of Anterior Uveitis in a Rural Hospital
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. III. (Mar. 2014), PP 55-59 A Clinical Study of Anterior Uveitis in a Rural Hospital
Rare Presentation of Ocular Toxoplasmosis
 Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
 Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
11/3/2009 SECOND EDITION Madhukar Pai McGill University. ISTC Training Modules Introduction
 SECOND EDITION 2009 Madhukar Pai McGill University Introduction 1 Purpose of ISTC ISTC Version 2: Key Points 21 Standards Differ from existing guidelines: standards present what should be done, whereas,
SECOND EDITION 2009 Madhukar Pai McGill University Introduction 1 Purpose of ISTC ISTC Version 2: Key Points 21 Standards Differ from existing guidelines: standards present what should be done, whereas,
Surgery in patients with uveitis. Lyndell Lim and Anthony Hall
 Surgery in patients with uveitis Lyndell Lim and Anthony Hall Disclosures Off label treatments Paid advisory board Bayer Paid research support Allergan (makers of Ozurdex) Paid research support B and L
Surgery in patients with uveitis Lyndell Lim and Anthony Hall Disclosures Off label treatments Paid advisory board Bayer Paid research support Allergan (makers of Ozurdex) Paid research support B and L
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
ISPUB.COM. An Atypical Presentation of Posterior Scleritis. A Ramanathan, A Gaur CASE REPORT
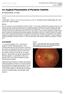 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
UVEITIS. Dr. Yılmaz ÖZYAZGAN
 UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
Patterns of uveitis in a Philippine eye clinic
 VOL. NO. PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE - MARCH 5 Harvey S. Uy, MD Irene W. Tam, OD Asian Eye Institute Makati, Philippines Patterns of uveitis in a Philippine eye clinic
VOL. NO. PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE - MARCH 5 Harvey S. Uy, MD Irene W. Tam, OD Asian Eye Institute Makati, Philippines Patterns of uveitis in a Philippine eye clinic
Tuberculosis Tools: A Clinical Update
 Tuberculosis Tools: A Clinical Update CAPA Conference 2014 JoAnn Deasy, PA-C. MPH, DFAAPA jadeasy@sbcglobal.net Adjunct Faculty Touro PA Program Learning Objectives Outline the pathogenesis of active pulmonary
Tuberculosis Tools: A Clinical Update CAPA Conference 2014 JoAnn Deasy, PA-C. MPH, DFAAPA jadeasy@sbcglobal.net Adjunct Faculty Touro PA Program Learning Objectives Outline the pathogenesis of active pulmonary
Uveitis unplugged: systemic therapy
 Uveitis unplugged: systemic therapy Hobart 2017 Peter McCluskey Save Sight Institute Sydney Eye Hospital Sydney Medical School University of Sydney Sydney Australia No financial or proprietary interest
Uveitis unplugged: systemic therapy Hobart 2017 Peter McCluskey Save Sight Institute Sydney Eye Hospital Sydney Medical School University of Sydney Sydney Australia No financial or proprietary interest
Abbreviated Drug Evaluation: Fluocinolone acetonide intravitreal implant (Retisert )
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Contribution of Dual Fluorescein and Indocyanine Green Angiography to the Appraisal of Presumed Tuberculous Chorioretinitis in a Non-endemic Area
 Original Article Contribution of Dual Fluorescein and Indocyanine Green Angiography to the Appraisal of Presumed Tuberculous Chorioretinitis in a Non-endemic Area Raphael Massy 1,2, MS; Carl P. Herbort
Original Article Contribution of Dual Fluorescein and Indocyanine Green Angiography to the Appraisal of Presumed Tuberculous Chorioretinitis in a Non-endemic Area Raphael Massy 1,2, MS; Carl P. Herbort
CLINICAL SCIENCES. Clinical Features of Tuberculous Serpiginouslike Choroiditis in Contrast to Classic Serpiginous Choroiditis
 CLINICAL SCIENCES Clinical Features of Tuberculous Serpiginouslike Choroiditis in Contrast to Classic Serpiginous Choroiditis Daniel V. Vasconcelos-Santos, MD, PhD; P. Kumar Rao, MD; John B. Davies, MD;
CLINICAL SCIENCES Clinical Features of Tuberculous Serpiginouslike Choroiditis in Contrast to Classic Serpiginous Choroiditis Daniel V. Vasconcelos-Santos, MD, PhD; P. Kumar Rao, MD; John B. Davies, MD;
A case of scleritis associated rheumatoid arthritis accompanying an intraocular elevated lesion
 Kobayashi et al. BMC Ophthalmology (2018) 18:129 https://doi.org/10.1186/s12886-018-0797-z CASE REPORT Open Access A case of scleritis associated rheumatoid arthritis accompanying an intraocular elevated
Kobayashi et al. BMC Ophthalmology (2018) 18:129 https://doi.org/10.1186/s12886-018-0797-z CASE REPORT Open Access A case of scleritis associated rheumatoid arthritis accompanying an intraocular elevated
Study Number CAIN457C2302 (core study) and CAIN457C2302E1 (extension study)
 Clinical Trial Results Database Page 1 Sponsor Novartis Generic Drug Name Secukinumab Therapeutic Area of Trial Uveitis Approved Indication Investigational Study Number CC2302 (core study) and CC2302E1
Clinical Trial Results Database Page 1 Sponsor Novartis Generic Drug Name Secukinumab Therapeutic Area of Trial Uveitis Approved Indication Investigational Study Number CC2302 (core study) and CC2302E1
Differential diagnosis of posterior uveitis
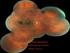 Differential diagnosis of posterior uveitis Diagnostic approach 45-year old male. Floaters and decreased vision since 1 week Fever, lymphadenopathy, myalgias, night sweats, two months ago Oral ulcer sporadically
Differential diagnosis of posterior uveitis Diagnostic approach 45-year old male. Floaters and decreased vision since 1 week Fever, lymphadenopathy, myalgias, night sweats, two months ago Oral ulcer sporadically
Choroidal Neovascularization in Sympathetic Ophthalmia
 Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Bilateral choroidal tuberculoma in miliary tuberculosis - report of a case
 Annamalai and Biswas Journal of Ophthalmic Inflammation and Infection (2015) 5:4 DOI 10.1186/s12348-014-0032-x BRIEF REPORT Open Access Bilateral choroidal tuberculoma in miliary tuberculosis - report
Annamalai and Biswas Journal of Ophthalmic Inflammation and Infection (2015) 5:4 DOI 10.1186/s12348-014-0032-x BRIEF REPORT Open Access Bilateral choroidal tuberculoma in miliary tuberculosis - report
ABSTRACT. KEY WORDS AIDS, cidofovir, complication, drug-induced uveitis, rifabutin, tuberculosis. zzzzzz 1 Dept of Ophthalmology CHU Saint-Pierre and
 DRUG-INDUCED UVEITIS IN AIDS PATIENTS: TWO CASE REPORTS BAZEWICZ M 1, FIKRI J 1, MARTIN CH 2, LIBOIS A 2, MEUNIER A 1, FRIPPIAT F 3, CASPERS L 1, WILLERMAIN F 1 ABSTRACT Patients with acquired immunodeficiency
DRUG-INDUCED UVEITIS IN AIDS PATIENTS: TWO CASE REPORTS BAZEWICZ M 1, FIKRI J 1, MARTIN CH 2, LIBOIS A 2, MEUNIER A 1, FRIPPIAT F 3, CASPERS L 1, WILLERMAIN F 1 ABSTRACT Patients with acquired immunodeficiency
Macular Hole Associated with Vogt-Koyanagi-Harada Disease at the Acute Uveitic Stage
 Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Management of Immune Reconstitution Inflammatory Syndrome (IRIS)
 Management of Immune Reconstitution Inflammatory Syndrome (IRIS) Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the IRIS Guideline
Management of Immune Reconstitution Inflammatory Syndrome (IRIS) Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the IRIS Guideline
What does IGRA testing add to the diagnosis of ocular tuberculosis? A Bayesian latent class analysis
 Agrawal et al. BMC Ophthalmology (2017) 17:245 DOI 10.1186/s12886-017-0597-x RESEARCH ARTICLE Open Access What does IGRA testing add to the diagnosis of ocular tuberculosis? A Bayesian latent class analysis
Agrawal et al. BMC Ophthalmology (2017) 17:245 DOI 10.1186/s12886-017-0597-x RESEARCH ARTICLE Open Access What does IGRA testing add to the diagnosis of ocular tuberculosis? A Bayesian latent class analysis
Novel multi-targeted polymerase chain reaction for diagnosis of presumed tubercular uveitis
 Sharma et al. Journal of Ophthalmic Inflammation and Infection 2013, 3:25 ORIGINAL RESEARCH Open Access Novel multi-targeted polymerase chain reaction for diagnosis of presumed tubercular uveitis Kusum
Sharma et al. Journal of Ophthalmic Inflammation and Infection 2013, 3:25 ORIGINAL RESEARCH Open Access Novel multi-targeted polymerase chain reaction for diagnosis of presumed tubercular uveitis Kusum
Uveitis. Pt Info Brochure. Q: What is Uvea?
 Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age
 Original Article Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age Suma Ganesh 1, Reena Gupta 2, Sumita Sethi 3, Chandra Gurung 4, Raman Mehta 5 1,5 Dr. Shroff s Charitable
Original Article Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age Suma Ganesh 1, Reena Gupta 2, Sumita Sethi 3, Chandra Gurung 4, Raman Mehta 5 1,5 Dr. Shroff s Charitable
Uveitis: Classification, Etiologies and Clinical Signs
 E-ISSN 2454-2784 Recent Advances Uveitis: Classification, Etiologies and Clinical Signs Aditya Shreekant Kelkar 1, Ekta Rakesh Arora 1, B.Sowkath 2, Jyotirmay Biswas 3 1 National Institute of Ophthalmology,Pune
E-ISSN 2454-2784 Recent Advances Uveitis: Classification, Etiologies and Clinical Signs Aditya Shreekant Kelkar 1, Ekta Rakesh Arora 1, B.Sowkath 2, Jyotirmay Biswas 3 1 National Institute of Ophthalmology,Pune
A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D.
 A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D. I. Introduction II. III. IV. A. Why I am giving this talk B. What to take from lecture Diagnosis 1. Better understanding
A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D. I. Introduction II. III. IV. A. Why I am giving this talk B. What to take from lecture Diagnosis 1. Better understanding
Patterns of Uveitis at a Tertiary Referral Center in Southern Iran
 Original Article Patterns of Uveitis at a Tertiary Referral Center in Southern Iran Mansour Rahimi, MD; Ghazaleh Mirmansouri, MD Poustchi Eye Research Center and Ophthalmology Department, Shiraz University
Original Article Patterns of Uveitis at a Tertiary Referral Center in Southern Iran Mansour Rahimi, MD; Ghazaleh Mirmansouri, MD Poustchi Eye Research Center and Ophthalmology Department, Shiraz University
Pan-uveitis - A rare ocular manifestation of dengue
 Case report DOI: http://dx.doi.org/10.18320/jimd/201603.0147 JOURNAL OF INTERNATIONAL MEDICINE AND DENTISTRY To search..to know...to share p-issn: 2454-8847 e-issn: 2350-045X Pan-uveitis - A rare ocular
Case report DOI: http://dx.doi.org/10.18320/jimd/201603.0147 JOURNAL OF INTERNATIONAL MEDICINE AND DENTISTRY To search..to know...to share p-issn: 2454-8847 e-issn: 2350-045X Pan-uveitis - A rare ocular
5. HIV-positive individuals treated with INH should receive Pyridoxine (B6) 25 mg daily or 50 mg twice/thrice weekly on the same schedule as INH
 V. TB and HIV/AIDS A. Standards of Treatment and Management The majority of TB treatment principles apply to persons with HIV/AIDS who require treatment for TB disease. The following points are either
V. TB and HIV/AIDS A. Standards of Treatment and Management The majority of TB treatment principles apply to persons with HIV/AIDS who require treatment for TB disease. The following points are either
High-speed optical coherence tomography as a reliable adjuvant tool to grade ocular anterior chamber inflammation.
 Thomas Jefferson University Jefferson Digital Commons Wills Eye Institute Papers Wills Eye Institute 3-2014 High-speed optical coherence tomography as a reliable adjuvant tool to grade ocular anterior
Thomas Jefferson University Jefferson Digital Commons Wills Eye Institute Papers Wills Eye Institute 3-2014 High-speed optical coherence tomography as a reliable adjuvant tool to grade ocular anterior
Diagnosis Latent Tuberculosis. Disclosures. Case
 Diagnosis Latent Tuberculosis Neha Shah MD MPH Field Medical Officer Tuberculosis Control Branch California Department of Public Health Centers for Disease Control and Prevention September 2016 1 Disclosures
Diagnosis Latent Tuberculosis Neha Shah MD MPH Field Medical Officer Tuberculosis Control Branch California Department of Public Health Centers for Disease Control and Prevention September 2016 1 Disclosures
Sarcoidosis and Uveitis
 Sarcoidosis and Uveitis Nicholas Jones Royal Eye Hospital Manchester, UK Sarcoidosis a multisystem chronic inflammation causing multifocal non-caseating granulomas BUT Diagnosis often made indirectly (without
Sarcoidosis and Uveitis Nicholas Jones Royal Eye Hospital Manchester, UK Sarcoidosis a multisystem chronic inflammation causing multifocal non-caseating granulomas BUT Diagnosis often made indirectly (without
Intraocular Tuberculosis
 Eye (1990) 4, 486-492 Intraocular Tuberculosis P. H. ROSEN*, D. 1. SPALTON and E. M. GRAHAM London Summary 1Welve patients with a diagnosis of intraocular tuberculosis are described. Nine patients presented
Eye (1990) 4, 486-492 Intraocular Tuberculosis P. H. ROSEN*, D. 1. SPALTON and E. M. GRAHAM London Summary 1Welve patients with a diagnosis of intraocular tuberculosis are described. Nine patients presented
Uveitis of spondyloarthritis in Indian subcontinent: a cross sectional study
 International Journal of Advances in Medicine Ninan F et al. Int J Adv Med. 2017 Oct;4(5):1441-1446 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174300
International Journal of Advances in Medicine Ninan F et al. Int J Adv Med. 2017 Oct;4(5):1441-1446 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174300
Why Is Imaging Critical in My Uveitis Practice?
 Why Is Imaging Critical in My Uveitis Practice? Dilraj S. Grewal, MD Developed in collaboration Imaging Is the Backbone of Uveitis Workup and Monitoring Treatment Response FP FAF B- scan Multimodal Imaging
Why Is Imaging Critical in My Uveitis Practice? Dilraj S. Grewal, MD Developed in collaboration Imaging Is the Backbone of Uveitis Workup and Monitoring Treatment Response FP FAF B- scan Multimodal Imaging
Interferon gamma release assays and the NICE 2011 guidelines on the diagnosis of latent tuberculosis
 CLINICAL AUDIT Clinical Medicine 2013, Vol 13, No 4: 362 6 Interferon gamma release assays and the NICE 2011 guidelines on the diagnosis of latent tuberculosis Helen R Mujakperuo, Richard D Thompson and
CLINICAL AUDIT Clinical Medicine 2013, Vol 13, No 4: 362 6 Interferon gamma release assays and the NICE 2011 guidelines on the diagnosis of latent tuberculosis Helen R Mujakperuo, Richard D Thompson and
Ocular mycobacteriosis dual infection of M. tuberculosis complex with M. fortuitum
 Sharma et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:2 DOI 10.1186/s12348-016-0121-0 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Ocular mycobacteriosis
Sharma et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:2 DOI 10.1186/s12348-016-0121-0 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Ocular mycobacteriosis
Interferon Gamma Release Assay Testing for Latent Tuberculosis Infection: Physician Guidelines
 Interferon Gamma Release Assay Testing for Latent Tuberculosis Infection: Physician Guidelines Historically, Latent Tuberculosis Infection (LTBI) diagnosis was based on risk assessment, chest x-ray (CXR)
Interferon Gamma Release Assay Testing for Latent Tuberculosis Infection: Physician Guidelines Historically, Latent Tuberculosis Infection (LTBI) diagnosis was based on risk assessment, chest x-ray (CXR)
Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 743-748 Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 743-748 Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis
 Haddad and Reddy Journal of Ophthalmic Inflammation and Infection 2014, 4:28 BRIEF REPORT Open Access Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis Zeina
Haddad and Reddy Journal of Ophthalmic Inflammation and Infection 2014, 4:28 BRIEF REPORT Open Access Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis Zeina
Patterns of Macular Edema in Uveitis as Diagnosed by Optical Coherence Tomography in Tertiary Eye Center
 Original Article Patterns of Macular Edema in Uveitis as Diagnosed by Optical Coherence Tomography in Tertiary Eye Center Sharad Gupta 1, Dev Narayan Shah 2, Sagun Narayan Joshi 3, Manoj Aryal 4, Lila
Original Article Patterns of Macular Edema in Uveitis as Diagnosed by Optical Coherence Tomography in Tertiary Eye Center Sharad Gupta 1, Dev Narayan Shah 2, Sagun Narayan Joshi 3, Manoj Aryal 4, Lila
UVEITIS IN GENERAL. Information for patients UVEITIS CLINIC WHAT IS UVEITIS? MAIN CATEGORIES OF UVEITIS
 Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Spontaneous Large Serous Retinal Pigment Epithelial Tear
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
TUBERCULOSIS OF THE RIB IN A 20 MONTH S OLD BOY
 CASE REPORT TUBERCULOSIS OF THE RIB IN A 20 MONTH S OLD BOY El Mouhtadi Aghoutane, Tarik Salama, Redouane El Fezzazi Pediatric surgery department, Kadi Ayyad University, Marrakech, Morocco Abstract Primary
CASE REPORT TUBERCULOSIS OF THE RIB IN A 20 MONTH S OLD BOY El Mouhtadi Aghoutane, Tarik Salama, Redouane El Fezzazi Pediatric surgery department, Kadi Ayyad University, Marrakech, Morocco Abstract Primary
Evolving therapies for posterior uveitis. Infliximab (Remicade) Infliximab: pharmacology. FDA-approved monoclonal antibody therapy Target
 Evolving therapies for posterior uveitis Sam Dahr, M.D. September 17, 2005 Midwest Ophthalmology Conference Infliximab (Remicade) FDA approved for Crohn s disease, rheumatoid arthritis, and psoriatic arthritis
Evolving therapies for posterior uveitis Sam Dahr, M.D. September 17, 2005 Midwest Ophthalmology Conference Infliximab (Remicade) FDA approved for Crohn s disease, rheumatoid arthritis, and psoriatic arthritis
Anthony DeWilde, O.D Linwood Blvd. Kansas City, MO x
 Anthony DeWilde, O.D. 4801 Linwood Blvd. Kansas City, MO 64128 816-861-4700 x 57411 anthony.dewilde@va.gov Uveitis and Glaucoma: The Seven Reasons Why IOP Can Increase in Uveitis (and What to do About
Anthony DeWilde, O.D. 4801 Linwood Blvd. Kansas City, MO 64128 816-861-4700 x 57411 anthony.dewilde@va.gov Uveitis and Glaucoma: The Seven Reasons Why IOP Can Increase in Uveitis (and What to do About
Algorithm of Choroiditis
 10.5005/jp-journals-10020-1027 REVIEW ARTICLE Ovi Sofia, Sudharshan Sridharan, Jyotirmay Biswas ABSTRACT Choroiditis may present as focal or multifocal lesions, and could be due to infectious or noninfectious
10.5005/jp-journals-10020-1027 REVIEW ARTICLE Ovi Sofia, Sudharshan Sridharan, Jyotirmay Biswas ABSTRACT Choroiditis may present as focal or multifocal lesions, and could be due to infectious or noninfectious
Uveitis literature 2014: the year in review. Russell N. Van Gelder, MD, PhD Department of Ophthalmology University of Washington Seattle, WA
 Uveitis literature 2014: the year in review Russell N. Van Gelder, MD, PhD Department of Ophthalmology University of Washington Seattle, WA Disclosures RVG serves as Associate Editor of IOVS Editorial
Uveitis literature 2014: the year in review Russell N. Van Gelder, MD, PhD Department of Ophthalmology University of Washington Seattle, WA Disclosures RVG serves as Associate Editor of IOVS Editorial
CASE PRESENTATION. DR.Sravani 1 st yr PG Dept of Ophthalmology
 CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
REFRESHER: ANTERIOR UVEITIS
 REFRESHER: ANTERIOR UVEITIS 2. SAoO Kongress 28.2.2018 Messe Luzern Dr. med. Christian Böni Augenklinik Universitätsspital Zürich Christian Böni Seite 1 Anterior Uveitis: Clinical Issues Diagnostics: yes
REFRESHER: ANTERIOR UVEITIS 2. SAoO Kongress 28.2.2018 Messe Luzern Dr. med. Christian Böni Augenklinik Universitätsspital Zürich Christian Böni Seite 1 Anterior Uveitis: Clinical Issues Diagnostics: yes
Interim Clinical Commissioning Policy Statement: Adalimumab for Severe Refractory Uveitis. Reference: NHS England: /PS
 Interim Clinical Commissioning Policy Statement: Adalimumab for Severe Refractory Uveitis Reference: NHS England: 170010/PS Publications Gateway Reference: Document Purpose Policy 05527s Document Name
Interim Clinical Commissioning Policy Statement: Adalimumab for Severe Refractory Uveitis Reference: NHS England: 170010/PS Publications Gateway Reference: Document Purpose Policy 05527s Document Name
Northwestern Polytechnic University
 Clinical Tuberculosis Assessment by Health Care Provider Clinicians should review and verify the information in the Tuberculosis (TB) Screening Questionnaire (attached). Persons answering YES to any questions
Clinical Tuberculosis Assessment by Health Care Provider Clinicians should review and verify the information in the Tuberculosis (TB) Screening Questionnaire (attached). Persons answering YES to any questions
Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior Uveitis in a Korean Population
 J Korean Med Sci 2009; 24: 722-8 ISSN 1011-8934 DOI: 10.3346/jkms.2009.24.4.722 Copyright The Korean Academy of Medical Sciences Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior
J Korean Med Sci 2009; 24: 722-8 ISSN 1011-8934 DOI: 10.3346/jkms.2009.24.4.722 Copyright The Korean Academy of Medical Sciences Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior
PULMONARY TUBERCULOSIS RADIOLOGY
 PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
Uveitis. What is Uveitis?
 Uveitis What is Uveitis? Uveitis [u-vee-i-tis] is a term for inflammation of the eye. It can occur in one eye or both eyes and affects the layer of the eye called the uvea [u-vee-uh]. It also can be associated
Uveitis What is Uveitis? Uveitis [u-vee-i-tis] is a term for inflammation of the eye. It can occur in one eye or both eyes and affects the layer of the eye called the uvea [u-vee-uh]. It also can be associated
Bilateral acute retinal necrosis in a patient with multiple sclerosis on natalizumab
 Bilateral acute retinal necrosis in a patient with multiple sclerosis on natalizumab Arjun B. Sood, Emory University Gokul Kumar, Emory University Joshua Robinson, Emory University Journal Title: Journal
Bilateral acute retinal necrosis in a patient with multiple sclerosis on natalizumab Arjun B. Sood, Emory University Gokul Kumar, Emory University Joshua Robinson, Emory University Journal Title: Journal
Laboratory Testing and Systemic Investigations in Uveitis
 Laboratory Testing and Systemic Investigations in Uveitis Investigating Uveitis A Tailored Approach Nicholas Jones The Royal Eye Hospital Manchester, UK Nicholas Jones Manchester Uveitis Clinic Manchester
Laboratory Testing and Systemic Investigations in Uveitis Investigating Uveitis A Tailored Approach Nicholas Jones The Royal Eye Hospital Manchester, UK Nicholas Jones Manchester Uveitis Clinic Manchester
Various presentations of herpes simplex retinochoroiditis A case series
 Various presentations of herpes simplex retinochoroidits 47 Various presentations of herpes simplex retinochoroiditis A case series M. T. K. Perera 1, T. S. Keragala 1, M. Gamage 2 The Journal of the College
Various presentations of herpes simplex retinochoroidits 47 Various presentations of herpes simplex retinochoroiditis A case series M. T. K. Perera 1, T. S. Keragala 1, M. Gamage 2 The Journal of the College
Tuberculosis otitis media
 Case Report Brunei Int Med J. 2013; 9 (5): 329-333 Tuberculosis otitis media Poon Seong LIM, Bee See GOH, Lokman SAIM Department of Otorhinolaryngology-Head and Neck Surgery, Faculty of Medicine, Universiti
Case Report Brunei Int Med J. 2013; 9 (5): 329-333 Tuberculosis otitis media Poon Seong LIM, Bee See GOH, Lokman SAIM Department of Otorhinolaryngology-Head and Neck Surgery, Faculty of Medicine, Universiti
Role of RNTCP in the management MDR-TB
 Kamdar DJ, Shah NA, Patel DJ, Parmarr H. Role of RNTCP in the management of MDR-TB. IAIM, 2015; 2(7): 1-5. Original Research Article Role of RNTCP in the management of MDR-TB Deepali J Kamdar 1, Neha A
Kamdar DJ, Shah NA, Patel DJ, Parmarr H. Role of RNTCP in the management of MDR-TB. IAIM, 2015; 2(7): 1-5. Original Research Article Role of RNTCP in the management of MDR-TB Deepali J Kamdar 1, Neha A
Optical Coherence Tomography (OCT) in Uveitis Piergiorgio Neri, BMedSc, MD, PhD Head Ocular Immunology Unit
 The Eye Clinic Polytechnic University of Marche Head: Prof Alfonso Giovannini November, 1991 Optical Coherence Tomography (OCT) in Uveitis Piergiorgio Neri, BMedSc, MD, PhD Head Ocular Immunology Unit
The Eye Clinic Polytechnic University of Marche Head: Prof Alfonso Giovannini November, 1991 Optical Coherence Tomography (OCT) in Uveitis Piergiorgio Neri, BMedSc, MD, PhD Head Ocular Immunology Unit
Pathogenesis and Pathology of Intraocular Tuberculosis
 Ocular Immunology & Inflammation, 2015; 23(4): 353 357 Copyright! Taylor & Francis Group, LLC ISSN: 0927-3948 print / 1744-5078 online DOI: 10.3109/09273948.2015.1056536 REVIEW ARTICLE Pathogenesis and
Ocular Immunology & Inflammation, 2015; 23(4): 353 357 Copyright! Taylor & Francis Group, LLC ISSN: 0927-3948 print / 1744-5078 online DOI: 10.3109/09273948.2015.1056536 REVIEW ARTICLE Pathogenesis and
The Diagnosis of Active TB. Deborah McMahan, MD TB Intensive September 28, 2017
 The Diagnosis of Active TB Deborah McMahan, MD TB Intensive September 28, 2017 Agenda Epidemiology Big picture Conditions that Should Make You Suspicious Which test? Eeenie meenie miny mo Radiographic
The Diagnosis of Active TB Deborah McMahan, MD TB Intensive September 28, 2017 Agenda Epidemiology Big picture Conditions that Should Make You Suspicious Which test? Eeenie meenie miny mo Radiographic
Nausheen Khuddus, MD Melissa Elder, MD, PhD
 Nausheen Khuddus, MD Melissa Elder, MD, PhD Nausheen Khuddus, MD Pediatric Ophthalmologist and Strabismus Specialist Accent Physicians Gainesville, Florida What Is Uveitis? Uveitis is caused by inflammatory
Nausheen Khuddus, MD Melissa Elder, MD, PhD Nausheen Khuddus, MD Pediatric Ophthalmologist and Strabismus Specialist Accent Physicians Gainesville, Florida What Is Uveitis? Uveitis is caused by inflammatory
Objectives. Highlight typical feature of TB pericarditis. How to make a diagnosis. How to treat TB pericarditis
 Dr. Conteh Objectives Highlight typical feature of TB pericarditis How to make a diagnosis How to treat TB pericarditis New evidence for adjunctive corticosteroid Introduction TB pericarditis occurs in
Dr. Conteh Objectives Highlight typical feature of TB pericarditis How to make a diagnosis How to treat TB pericarditis New evidence for adjunctive corticosteroid Introduction TB pericarditis occurs in
Clinical Outcomes of Cyclosporine Treatment for Noninfectious Uveitis
 pissn: 1011-8942 eissn: 2092-9382 Clinical Outcomes of Cyclosporine Treatment for Noninfectious Uveitis Korean J Ophthalmol 2012;26(1):21-25 http://dx.doi.org/10.3341/kjo.2012.26.1.21 Original Article
pissn: 1011-8942 eissn: 2092-9382 Clinical Outcomes of Cyclosporine Treatment for Noninfectious Uveitis Korean J Ophthalmol 2012;26(1):21-25 http://dx.doi.org/10.3341/kjo.2012.26.1.21 Original Article
Diagnosis and Medical Management of Latent TB Infection
 Diagnosis and Medical Management of Latent TB Infection Marsha Majors, RN September 7, 2017 TB Contact Investigation 101 September 6 7, 2017 Little Rock, AR EXCELLENCE EXPERTISE INNOVATION Marsha Majors,
Diagnosis and Medical Management of Latent TB Infection Marsha Majors, RN September 7, 2017 TB Contact Investigation 101 September 6 7, 2017 Little Rock, AR EXCELLENCE EXPERTISE INNOVATION Marsha Majors,
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg
 An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
TB & HIV CO-INFECTION IN CHILDREN. Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012
 TB & HIV CO-INFECTION IN CHILDREN Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012 Introduction TB & HIV are two of the leading causes of morbidity & mortality in children
TB & HIV CO-INFECTION IN CHILDREN Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012 Introduction TB & HIV are two of the leading causes of morbidity & mortality in children
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Pediatric Tuberculosis Lisa Y. Armitige, MD, PhD September 14, 2017
 Pediatric Tuberculosis Lisa Y. Armitige, MD, PhD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following disclosures
Pediatric Tuberculosis Lisa Y. Armitige, MD, PhD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following disclosures
INTENSIFIED TB CASE FINDING
 INTENSIFIED TB CASE FINDING My friends call me Intensified Case Finding (ICF) I undertake regularly screening all people with, or at high risk of HIV, for symptoms of TB in health care facilities, communities
INTENSIFIED TB CASE FINDING My friends call me Intensified Case Finding (ICF) I undertake regularly screening all people with, or at high risk of HIV, for symptoms of TB in health care facilities, communities
Screening and Treatment Recommendations for Persons Exposed to MDR TB
 Screening and Treatment Recommendations for Persons Exposed to MDR TB Although all persons at increased risk of tuberculosis (TB) infection should be screened for TB infection per USPTF/CDC guidelines
Screening and Treatment Recommendations for Persons Exposed to MDR TB Although all persons at increased risk of tuberculosis (TB) infection should be screened for TB infection per USPTF/CDC guidelines
Initial results of QuantiFERON-TB Gold testing in patients with uveitis
 (2009) 23, 904 909 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye CLINICAL STUDY Initial results of QuantiFERON-TB Gold testing in patients with uveitis
(2009) 23, 904 909 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye CLINICAL STUDY Initial results of QuantiFERON-TB Gold testing in patients with uveitis
10. TB and HIV Infection
 10. TB and HIV Infection The management of patients with TB and HIV infection is complex, requiring management by a multidisciplinary team which includes physicians with expertise in the treatment of both
10. TB and HIV Infection The management of patients with TB and HIV infection is complex, requiring management by a multidisciplinary team which includes physicians with expertise in the treatment of both
Evaluation of posterior segment manifestations following typhoid fever-a clinical study
 Original Research Article DOI: 10.18231/2395-1451.2018.0092 Evaluation of posterior segment manifestations following typhoid fever-a clinical study Pavana Acharya 1, Lakshmi Bomalapura Ramamurthy 2,*,
Original Research Article DOI: 10.18231/2395-1451.2018.0092 Evaluation of posterior segment manifestations following typhoid fever-a clinical study Pavana Acharya 1, Lakshmi Bomalapura Ramamurthy 2,*,
Orbital and adnexal tuberculosis: a case series from a South Indian population
 Babu et al. Journal of Ophthalmic Inflammation and Infection 2014, 4:12 ORIGINAL RESEARCH Open Access Orbital and adnexal tuberculosis: a case series from a South Indian population Kalpana Babu 1,2*, Moupia
Babu et al. Journal of Ophthalmic Inflammation and Infection 2014, 4:12 ORIGINAL RESEARCH Open Access Orbital and adnexal tuberculosis: a case series from a South Indian population Kalpana Babu 1,2*, Moupia
Classification Of Uveitis Current Guidelines
 We have made it easy for you to find a PDF Ebooks without any digging. And by having access to our ebooks online or by storing it on your computer, you have convenient answers with classification of uveitis
We have made it easy for you to find a PDF Ebooks without any digging. And by having access to our ebooks online or by storing it on your computer, you have convenient answers with classification of uveitis
HLA-B27-related anterior Uveitis
 HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
