The incidence of bronchiectasis, which is defined as irreversible. Surgical management of childhood bronchiectasis due to infectious disease GTS
|
|
|
- Elizabeth Berry
- 5 years ago
- Views:
Transcription
1 Surgical management of childhood bronchiectasis due to infectious disease Gokhan Haciibrahimoglu, MD Mithat Fazlioglu, MD Aysun Olcmen, MD Atilla Gurses, MD Mehmet Ali Bedirhan, MD Background: The purpose of this study was to estimate operative risk and to identify indicators of adverse prognosis in patients undergoing resection for childhood bronchiectasis. Dr Haciibrahimoglu Methods: From January 1985 to February 2001, patients undergoing resection for bronchiectasis were studied. The indications for operation were failure of medical therapy in 33 patients (94.2%) and hemoptysis in 2 (5.7%). The mean duration of symptoms was 4.2 years (range, 1-9 years). Surgical treatment included lobectomy in 17 patients (48.5%), pneumonectomy in 7 (20%), lobectomy plus segmentectomy in 5 (14.2%), bilobectomy in 2 (5.7%), and segmentectomy in 4 (11.4%). Results: The operative mortality rate was 2.8%, and the morbidity rate was 17.6%. The mean follow-up in 34 patients was 5.4 years (range, 1-12 years). Overall, 22 patients (64.7%) were asymptomatic after surgery. Clinical improvement was noticed in 8 patients (23.5%), and no improvement was noticed in 4 (11.7%). Complete resection resulted in a significantly better clinical outcome than incomplete resection (P.05). Conclusions: Surgery for childhood bronchiectasis can be performed with low mortality and morbidity. Complete resection should be performed when possible. From the Yedikule Hospital for Chest Disease and Thoracic Surgery Center, Department of Thoracic Surgery, Istanbul, Turkey. Received for publication July 25, 2003; revisions requested Oct 24, 2003; revisions received Nov 4, 2003; accepted for publication Nov 20, Address for reprints: Gokhan Haciibrahimoglu, MD, Nispetiye cad. Profesorler sitesi, C3A Blok No. 66/8, Etiler 34337, Istanbul, Turkey ( ghaciibrahim@ yahoo.com). J Thorac Cardiovasc Surg 2004;127: /$30.00 Copyright 2004 by The American Association for Thoracic Surgery doi: /j.jtcvs The incidence of bronchiectasis, which is defined as irreversible dilatation of the bronchial tree, has decreased considerably since the advent of antibiotic therapy. The disease not only affects the structure of the bronchial tree, but also alters pulmonary hemodynamics and causes nonperfused lung fields. Thus, surgical resection is required in some patients despite maximum medical support to control the symptoms and progression of the disease, and it is still an indication for lung resection before puberty. Bronchiectasis occurs for a number of congenital and acquired reasons, and it is predominantly a pediatric disease. 1,2 In postinfectious bronchiectasis, in most cases one can elicit a history of pneumonia developing as a complication of measles, whooping cough, or another contagious disease of childhood; it is thought that the bacterial pneumonia and associated atelectasis are responsible for destruction and dilatation of the bronchial walls. We think that postinfectious bronchiectasis is a different entity. In spite of widely known etiologic factors, the causes could not be determined in 29% to 45% of cases. 3 In our country, pneumonia (30%) and tuberculosis (11%) are the most common causes. 4 The purpose of this study was to evaluate the indications, postoperative complications, and survival with lung resections performed in children because of postinfectious bronchiectasis. The Journal of Thoracic and Cardiovascular Surgery Volume 127, Number
2 TABLE 1. Symptoms Symptom n (%) Recurrence of pulmonary infection 33 (94.2%) Productive cough 32 (91.4%) Fetid sputum 28 (80%) Hemoptysis 4 (11.4%) TABLE 2. Bacteriology Germ n (%) Staphylococcus aureus 17 (48.5%) Pseudomonas aeruginosa 6 (17.1%) Klebsiella pneumoniae 3 (8.5%) Streptococcus pneumoniae 2 (5.7%) Patients and Methods The patient notes of 35 patients who underwent lung resection at our institute from 1985 to 2001 were retrospectively reviewed. The records were analyzed for age, sex, symptoms, type of resection, operative morbidity and mortality, and long-term outcome. Patients older than 14 years of age were excluded. Only patients who had bronchopulmonary infections as an etiologic factor were included in this review. Patients who presented to chest disease clinics with pulmonary infections and excessive amounts of sputum production underwent further evaluation, including pulmonary artery and lateral radiographs and computed tomographic (CT) scan. Preoperative pulmonary function studies were affected by a lack of cooperation with younger patients (5-13 years) and could not be performed completely. Bronchography was used at the beginning of the series. The diagnosis was made on CT scan in all patients. The CT criteria for diagnosing bronchiectasis included a bronchial diameter greater than that of the accompanying pulmonary artery, lack of tapering of the bronchial lumen, and visualization of bronchi in the periphery of the lungs. Ventilation/perfusion (V /Q ) scintigraphy was performed at the end of the series. The congenital origins in childhood bronchiectasis were investigated. Before surgery, a sweat test was performed for cystic fibrosis. Paranasal sinusitis was investigated. Preoperative medical treatment, which included appropriate antibiotic therapy and postural drainage, was supervised by chest physicians. Sputum was cultured for bacterial examination before surgery. Surgical treatment was considered if the medical treatment failed. We considered that the treatment was a failure if sputum production persisted despite several (2 or 3) courses of treatment and if there was a limited extent of disease on CT. As a rule, the extent of diseased lung to justify operation must be localized to achieve complete resection. The decision for the volume of the resected lung was based on radiologic findings rather than on thoracotomy. Detailed investigation was undertaken of the middle lobe in patients having right thoracotomy and of lingular segments in patients having left thoracotomy. All specimens had pathologic confirmation of bronchiectasis. The pulmonary resection was considered complete if the patient was believed to be free of bronchiectasis after thoracotomy. After surgery, patients were observed by a team that included chest physicians and surgeons. They were examined 4 times a year for 3 years and twice thereafter. High-resolution CT (HRCT) examinations were performed once a year. Immunization, including pneumococcus and influenza vaccines, was performed routinely. Clinical improvement can be defined as a decrease in symptoms of infection episodes when compared with the number of episodes preoperatively. This means that symptoms were observed only one time a year, which can be controlled with antibiotics. Operative Technique Rigid bronchoscopy was performed in all patients. We used bronchial blockers for isolation of the airway to prevent spillage of secretions when performing the operation for bronchiectasis in children. All procedures were through a classic posterolateral thoracotomy. Lung resection was performed. Bronchial closure was preferably achieved with manual interrupted semiabsorbable sutures, and the bronchial stump was covered with adjacent tissues in some patients, depending on the surgeons preference. Findings The mean age of the patients at the time of thoracotomy was 10.6 years (range, 5-13 years). There were 18 male and 17 female patients. The most common symptoms were recurrent infections; the average duration of symptoms was 4.2 years (range, 1-9 years; Table 1). In physical examination of these children, according to growth percentiles, musculoskeletal development retardation was noted. These children were the ones who were under the 3rd percentile of the growth percentile curve. Posteroanterior and lateral chest radiographs were first made as preoperative diagnostic studies in all patients. Contrast bronchography was performed in 8 patients (22.8%), and HRCT was performed in 27 patients (77.1%). Bronchography was used mostly in the beginning of the series. V /Q scintigraphy was performed in 10 patients (28%). On V /Q scintigraphy, perfusion and ventilation were both impaired, but ventilation was more affected. Preoperative bronchoscopy was performed routinely in all patients. The cause of secondary bronchiectasis in 5 of the patients was central obstruction or stenosis. We had 5 patients with paranasal sinusitis. These patients had nasal polyps due to chronic sinusitis. Before the operation, these cases were evaluated by a specialist, and 3 of these 5 patients underwent operation. Afterward, they were operated on for bronchiectasis. During their long follow-ups, they had no problems, whereas the other 2 cases had occasional infections. Bacteria were preoperatively proven in 28 patients (80%). These are shown in Table 2. An antibiotic was given to all patients according to the culture antibiogram. A second-generation cephalosporin was administered to patients before surgery (ie, empiric antibiotic treatment). The disease was bilateral in 2 patients (5.7%) and unilateral in 33 (94.2%): right chest in 12 (36.3%) and left chest in 21 (63.6%). Bronchiectasis involvement was predominantly in the basilar segments in 21 patients (60%), lingular segments in 9 (25.7%), and upper lobe segments in 7 (20%). The indication for pulmonary resection was made in 33 patients (94.2%) because of failure in medical therapy and in 2 (5.7%), of 1362 The Journal of Thoracic and Cardiovascular Surgery May 2004
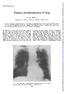
3 TABLE 3. Symptomatic status of 34 patients Symptoms Complete resection Incomplete resection Total Asymptomatic 21 (75%) 1 (16.6%) 22 (64.7%) Clinical improvement 6 (21.4%) 2 (33.3%) 8 (23.5%) No improvement 1 (3.5%) 3 (50%) 4 (11.7%) Total 28 (100%) 6 (100%) 34 (100%) chronic hemoptysis. Seventeen patients (48.5%) underwent lobectomy, and 7 (20%) underwent pneumonectomy. In 5 patients (14.2%) lobectomy plus segmentectomy was performed, in 4 patients (11.4%) segmentectomy was performed, and in 2 others (5.7%) bilobectomy was performed. We performed bilateral resection in 2 patients. The lower lobectomies were performed in 2 stages. In the morphologic classification, 24 cases (68.5%) were cylindrical, 8 cases (22.8%) were saccular, and 3 cases (8.7%) were varicose bronchiectasis. Statistical Analysis Functional results were compared by using a 2 test. Results One patient (2.8%) died the second day after surgery. Right lower bilobectomy had been performed in this patient. The cause of death was unexpected sudden arrhythmia and cardiac arrest. Complications occurred in 6 patients (17.6%). These complications included atelectasis in 3 patients (8.8%), empyema in 2 (5.8%), and prolonged air leak ( 7 days)in1 (2.9%). The follow-up was complete for 34 patients (100%) 28 who had complete resection (82.3%) and 6 who had incomplete resection (17.7%) with a mean time of 5.4 years (range, 1-12 years). We found that there was progressive overinflation of the remaining lung during the first year after pneumonectomy. The overinflation remained stable thereafter. Anterior herniation of the remaining lung with mediastinal shift was seen in long-term follow-up. Anterior herniation crossed the midline anterior to the heart. Cardiac functions of the patients showed no pathologic evidence. After surgery for the patients who underwent pneumonectomy, we observed that the hemithorax at that side became smaller and that slight scoliosis occurred. The growth pattern accelerated but has not yet attained normal percentiles in these patients. The patients underwent direct evaluation. Twenty-two (64.7%) were asymptomatic, and 8 (23.5%) had improved compared with their preoperative symptoms. Only 4 patients (11.7%) showed no improvement (Table 3). The best clinical improvement of this group was observed in patients with complete resection of the disease (27 of 28 patients); only 1 patient did not improve. In contrast, only 1 of 6 patients who had incomplete resection was asymptomatic, and 3 patients (50%) showed no improvement. A case of Figure 1. Preoperative HRCT of the patient in whom left lobectomy was performed. Figure 2. The right middle lobe and lingula show bronchiectatic areas after left lower lobectomy (same patient as in Figure 1; incomplete resection). incomplete resection with HRCT taken before surgery and during the first year after surgery is shown in Figures 1 and 2. Complete resection gave a significantly better result than incomplete resection (P.05). During follow-up of 6 patients who underwent incomplete resection, we observed nonlocalized bronchiectatic areas. In the follow-up, we performed V /Q scans in 10 patients after 1 year. Improvement was especially noted in ventilation. Ventilation scans made before surgery and the first year after surgery, illustrating this situation, are shown in Figures 3 and 4. The Journal of Thoracic and Cardiovascular Surgery Volume 127, Number
4 Figure 3. There is a complete absence of ventilation of the left lower lobe in V /Q scan. Left, Ventilation scan. Right, Perfusion scan. Figure 4. After left lobectomy, the ventilation scan was improved. Discussion Bronchiectasis is a chronic necrotizing condition of the bronchi and bronchioles that leads to irreversible abnormal dilatation of the airways. The morphologic classes of bronchiectasis are cylindrical, varicose, and saccular (cystic). It covers a spectrum from mild (cylindrical) to the most severe form of the disease (cystic). Ashour 5 stated that pulmonary perfusion was retained in the area of cylindrical changes and that, therefore, this type was not a primary indication for surgical management. Two thirds of the patients in our series had cylindrical bronchiectasis and nevertheless had symptoms that were resistant to medical therapy; these were alleviated successfully by surgical management. Furthermore, patients with a cylindrical type acquired a better prognosis after operation than those who had other types. Thus, we recommend surgical resection, even though the diseased lung has cylindrical change. Our experience suggests that patient symptoms indicate surgical resection rather than radiologic findings. In this study, we observed that the basal segments of the lower lobes, especially the posterobasal segments, were the most frequently affected (60%). We had expected this to occur more frequently on the left side, because the retaining of secretions can be thought to more easily occur in the left side (because of its smaller diameter and greater angle and its spatial relationship with the left pulmonary artery). 6,7 Bronchiectasis is usually caused by bronchopulmonary infection or bronchial obstruction; approximately half of patients can trace the onset of symptoms to a childhood infection. Primarily the symptoms are chronic cough and fetid sputum. In our series, Staphylococcus aureus and Pseudomonas aeruginosa were the most common organisms isolated from sputum. The chest radiograph is a poorly sensitive diagnostic instrument, more than 20% of the limited form of which is 1364 The Journal of Thoracic and Cardiovascular Surgery May 2004
5 regarded as normal, and we have used it routinely as a screening tool. Especially when the chest radiograph shows circular or honeycombing appearance, there is a high suspicion of bronchiectasis. The classification of bronchiectasis is less important than determining the extent of disease. The surgeon must identify the segment that is affected, because modern surgical techniques frequently permit preservation of 1 or more healthy pulmonary segments of a lobe in which bronchiectasis is present. Classically, bronchography has been routinely used for confirming the diagnosis and defining the extent of disease. The use of bronchography has been steadily decreasing (it was used in 8 [22.8%] of our patients, mostly in the beginning of the series), and it has been progressively replaced by HRCT. The lack of distal tapering of the bronchial lumen has been considered to be the most sensitive criterion for indicating bronchiectasis. 8 Preoperative bronchoscopy should be routinely performed to rule out foreign body, neoplasm, or stricture. We operated on 5 patients with secondary bronchiectasis caused by central obstruction or stenosis. Preoperative acute suppurative bronchitis was treated aggressively with appropriate antibiotics and postural drainage. A bronchial blocker was used to avoid contralateral contamination of secretions. The bronchial stump was manually sutured by using semiabsorbable materials in all patients, and bronchial reinforcement was performed in some patients, depending on the surgeons preference. The role of pulmonary resection has evolved from early curative resection for all patients 9 to a more palliative approach limited to either those patients with medically resistant disease or those with complications. The occurrence of complications is 9.4% to 24.6% in the current literature 9-11 ; this range is comparable to our rate (17.6%). In our series, complications were seen in 6 patients, and all were treated by a conservative approach. Atelectasis depended on sputum retention. Sputum retention is common because patients with this disease can have problems with ciliary motion and postoperative expectoration, which would easily be disrupted. As others 12 have demonstrated, bilateral bronchiectasis is not a contraindication to operation, and even incomplete resection often results in considerable alleviation. In our series, we performed bilateral resection in only 2 patients, for whom the lower lobectomies were performed in 2 stages. The aims of surgical therapy for bronchiectasis are to improve the quality of life in patients who have debilitating pulmonary symptoms despite medical treatment and to prevent complications such as empyema, recurrent hemoptysis, and lung abscess. Patients with clearly symptomatic, welllocalized childhood bronchiectasis are ideal surgical candidates. 11,13,14 Resection can be performed with almost no risks and a high expectation for cure. In conclusion, surgical treatment for childhood bronchiectasis should be limited to patients with well-localized disease. It can be performed with a definite strategy and strict criteria. Complete resection should be performed whenever possible. Preservation of as much lung parenchyma as possible is important. The basic guidelines for operative therapy of bronchiectasis are infection control, preoperative bronchoscopy, precise anatomic diagnosis, and precise anatomic resection. References 1. Paré JAP, Fraser RG. Synopsis of diseases of the chest. 2nd ed. Philadelphia: Saunders; p Swartz MN. Bronchiectasis. In: Fishman AP, editor. Pulmonary diseases and disorders. New York: McGraw-Hill; p Gracia JD, Rodrigor MJ, Morelle F, et al. Ig G subclass deficiencies associated with bronchiectasis. Am J Respir Crit Care Med. 1996;153: Ilvan A, Bozkanat E, Kartaloglu Z, et al. Son 5 yil icinde bronkografi ile tani konulmus bronsektazi olgularinin degerlendirilmesi. Solunum. 1995;19: Ashour M. Hemodynamic alterations in bronchiectasis: a base for a new classification of the disease. J Thorac Cardiovasc Surg. 1996; 112: Ashour M, Pandya I. Unilateral post-tuberculosis lung destruction: the left bronchus syndrome. Thorax. 1990;45: Ashour M. The anatomy of the bronchus syndrome. Clin Anat. 1995; 8: Lucidorme O, Grenier P, Coche E, Lenoir S, Aubert B, Beigelman C. Bronchiectasis: comparative assessment with thin-section CT and helical CT. Radiology. 1996;200: Ripe E. Bronchiectasis: a follow up study after surgical treatment. Scand J Respir Dis. 1971;52: Annest LS, Kratz JM, Crawford FA. Current results of treatment of bronchiectasis. J Thorac Cardiovasc Surg. 1992;83: Wilson JF, Decker AM. Surgical management of childhood bronchiectasis. Ann Surg. 1982;195: Fujimoto T, Hillejan L, Stamatis G. Current strategy for surgical management of bronchiectasis. Ann Thorac Surg. 2001;72: Agasthian T, Deschamps C, Trastek VF, Allen MS, Pairolero PC. Surgical management of bronchiectasis. Ann Thorac Surg. 1996;62: Prieto D, Bernardo J, Matos MJ, Eugenio L, Antunes M. Surgery for bronchiectasis. Eur J Cardiothorac Surg. 2001;20: The Journal of Thoracic and Cardiovascular Surgery Volume 127, Number
Surgery versus non-surgical treatment for bronchiectasis (Review)
 Surgery versus non-surgical treatment for bronchiectasis (Review) Warburton CJ, Corless JA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in
Surgery versus non-surgical treatment for bronchiectasis (Review) Warburton CJ, Corless JA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in
APICAL SEGMENT OF THE LOWER LOBE IN RESECTIONS FOR BRONCHIECTASIS
 Thorax (1955), 10, 137. THE LATE RESULTS OF THE CONSERVATION OF THE APICAL SEGMENT OF THE LOWER LOBE IN RESECTIONS FOR BRONCHIECTASIS BY E. HOFFMAN From the Regional Thoracic Surgery Centre, Shotley Bridge
Thorax (1955), 10, 137. THE LATE RESULTS OF THE CONSERVATION OF THE APICAL SEGMENT OF THE LOWER LOBE IN RESECTIONS FOR BRONCHIECTASIS BY E. HOFFMAN From the Regional Thoracic Surgery Centre, Shotley Bridge
Surgical Management of Bronchiectasis
 Surgical Management of Bronchiectasis Thirugnanam Agasthian, MD, Claude Deschamps, MD, Victor F. Trastek, MD, Mark S. Allen, MD, and Peter C. Pairolero, MD Section of General Thoracic Surgery, Mayo Clinic
Surgical Management of Bronchiectasis Thirugnanam Agasthian, MD, Claude Deschamps, MD, Victor F. Trastek, MD, Mark S. Allen, MD, and Peter C. Pairolero, MD Section of General Thoracic Surgery, Mayo Clinic
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Bronchial syndrome. Atelectasis Draining bronchus Bronchiectasis
 Bronchial syndrome Atelectasis Draining bronchus Bronchiectasis Etienne Leroy Terquem Pierre L Her SPI / ISP Soutien Pneumologique International / International Support for Pulmonology Atelectasis Consequence
Bronchial syndrome Atelectasis Draining bronchus Bronchiectasis Etienne Leroy Terquem Pierre L Her SPI / ISP Soutien Pneumologique International / International Support for Pulmonology Atelectasis Consequence
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/23566
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/23566
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
tomography Assessment of bronchiectasis by computed Reid' into three types-cystic, varicose, andcylindrical.
 Thorax 1985;40:920-924 Assessment of bronchiectasis by computed tomography IM MOOTOOSAMY, RH REZNEK, J OSMAN, RSO REES, MALCOLM GREEN From the Departments of Diagnostic Radiology and Chest Medicine, St
Thorax 1985;40:920-924 Assessment of bronchiectasis by computed tomography IM MOOTOOSAMY, RH REZNEK, J OSMAN, RSO REES, MALCOLM GREEN From the Departments of Diagnostic Radiology and Chest Medicine, St
FOREIGN BODY ASPIRATION in children. Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital
 FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
CASE REPORTS. Idiopathic Unilateral Hyperlucent Lung
 CASE REPORTS Idiopathic Unilateral Hyperlucent Lung The Swyer-James Syndrome J. Judson McNamara, M.D., Harold C. Urschel, M.D., J. H. Arndt, M.D., Herman Ulevitch, M.D., and W. B. Kingsley, M.D. I diopathic
CASE REPORTS Idiopathic Unilateral Hyperlucent Lung The Swyer-James Syndrome J. Judson McNamara, M.D., Harold C. Urschel, M.D., J. H. Arndt, M.D., Herman Ulevitch, M.D., and W. B. Kingsley, M.D. I diopathic
OSAMA A. ABDULMAJID, ABDELMOMEN M. EBEID, MOHAMED M. MOTAWEH, and IBRAHIM S. KLEIBO
 Aspirated foreign bodies in the tracheobronchial tree: report of 250 cases Thorax (1976), 31, 635. OSAMA A. ABDULMAJID, ABDELMOMEN M. EBEID, MOHAMED M. MOTAWEH, and IBRAHIM S. KLEIBO Thoracic Surgical
Aspirated foreign bodies in the tracheobronchial tree: report of 250 cases Thorax (1976), 31, 635. OSAMA A. ABDULMAJID, ABDELMOMEN M. EBEID, MOHAMED M. MOTAWEH, and IBRAHIM S. KLEIBO Thoracic Surgical
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
A Comparative Study of Video-Assisted Thoracic Surgery with Thoracotomy for Middle Lobe Syndrome
 World J Surg (2017) 41:780 784 DOI 10.1007/s00268-016-3777-6 ORIGINAL SCIENTIFIC REPORT A Comparative Study of Video-Assisted Thoracic Surgery with Thoracotomy for Middle Lobe Syndrome Jian Li 1,2 Chengwu
World J Surg (2017) 41:780 784 DOI 10.1007/s00268-016-3777-6 ORIGINAL SCIENTIFIC REPORT A Comparative Study of Video-Assisted Thoracic Surgery with Thoracotomy for Middle Lobe Syndrome Jian Li 1,2 Chengwu
Postgraduate Course ERS Glasgow 2004 Surgical approach to multiresistant cavitary mycobacteriosis
 REVIEW Postgraduate Course ERS Glasgow 2004 Surgical approach to multiresistant cavitary mycobacteriosis Educational aims To explain the present importance of surgery in TB management. To describe the
REVIEW Postgraduate Course ERS Glasgow 2004 Surgical approach to multiresistant cavitary mycobacteriosis Educational aims To explain the present importance of surgery in TB management. To describe the
Nontuberculous Mycobacteria
 Nontuberculous Mycobacteria When antibiotics are not enough a surgical approach John D. Mitchell, M.D. Davis Endowed Chair in Thoracic Surgery Professor and Chief Section of General Thoracic Surgery University
Nontuberculous Mycobacteria When antibiotics are not enough a surgical approach John D. Mitchell, M.D. Davis Endowed Chair in Thoracic Surgery Professor and Chief Section of General Thoracic Surgery University
squamous-cell carcinoma1
 Thorax (1975), 30, 152. Local ablative procedures designed to destroy squamous-cell carcinoma1 J. M. LEE, FREDERICK P. STITIK, DARRYL CARTER, and R. ROBINSON BAKER Departments of Surgery, Pathology, and
Thorax (1975), 30, 152. Local ablative procedures designed to destroy squamous-cell carcinoma1 J. M. LEE, FREDERICK P. STITIK, DARRYL CARTER, and R. ROBINSON BAKER Departments of Surgery, Pathology, and
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis?
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
NON-CF BRONCHIECTASIS IN ADULTS
 Séminaire de Pathologie Infectieuse Jeudi 25 juin 2008 Cliniques Universitaires UCL de Mont-Godinne, Yvoir NON-CF BRONCHIECTASIS IN ADULTS Dr Robert Wilson Royal Brompton Hospital, London, UK Aetiology
Séminaire de Pathologie Infectieuse Jeudi 25 juin 2008 Cliniques Universitaires UCL de Mont-Godinne, Yvoir NON-CF BRONCHIECTASIS IN ADULTS Dr Robert Wilson Royal Brompton Hospital, London, UK Aetiology
Carcinoma of the Lung
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
ISPUB.COM. Rare Cases: Tracheal/bronchial Obstruction. O Wenker, L Moehn, C Portera, G Walsh HISTORY ADMISSION
 ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
Routine reinforcement of bronchial stump after lobectomy or pneumonectomy with pedicled pericardial flap (PPF)
 Routine reinforcement of bronchial stump after lobectomy or pneumonectomy with pedicled pericardial flap (PPF) Abstract The results of 25 cases underwent a pedicled pericardial flap coverage for the bronchial
Routine reinforcement of bronchial stump after lobectomy or pneumonectomy with pedicled pericardial flap (PPF) Abstract The results of 25 cases underwent a pedicled pericardial flap coverage for the bronchial
Bronchiectasis: An Imaging Approach
 Bronchiectasis: An Imaging Approach Travis S Henry, MD Associate Professor of Clinical Radiology Cardiac and Pulmonary Imaging Section University of California, San Francisco Large Middle Small 1 Bronchiectasis
Bronchiectasis: An Imaging Approach Travis S Henry, MD Associate Professor of Clinical Radiology Cardiac and Pulmonary Imaging Section University of California, San Francisco Large Middle Small 1 Bronchiectasis
Surgical treatment of bullous lung disease
 Surgical treatment of bullous lung disease PD POTGIETER, SR BENATAR, RP HEWITSON, AD FERGUSON Thorax 1981 ;36:885-890 From the Respiratory Clinic, Groote Schuur Hospita', and Departments of Medicine, Anaesthetics,
Surgical treatment of bullous lung disease PD POTGIETER, SR BENATAR, RP HEWITSON, AD FERGUSON Thorax 1981 ;36:885-890 From the Respiratory Clinic, Groote Schuur Hospita', and Departments of Medicine, Anaesthetics,
PULMONARY EMERGENCIES
 EMERGENCIES I. Pneumonia A. Bacterial Pneumonia (most common cause of a focal infiltrate) 1. Epidemiology a. Accounts for up to 10% of hospital admissions in the U.S. b. Most pneumonias are the result
EMERGENCIES I. Pneumonia A. Bacterial Pneumonia (most common cause of a focal infiltrate) 1. Epidemiology a. Accounts for up to 10% of hospital admissions in the U.S. b. Most pneumonias are the result
Chronic lung diseases in children Simple choice 1. Finger clubbing is not characteristic for: a) Diffuse bronchiectasis b) Cystic fibrosis c)
 Chronic lung diseases in children Simple choice 1. Finger clubbing is not characteristic for: a) Diffuse bronchiectasis b) Cystic fibrosis c) Bronchiolitis obliterans d) Complicated acute pneumonia e)
Chronic lung diseases in children Simple choice 1. Finger clubbing is not characteristic for: a) Diffuse bronchiectasis b) Cystic fibrosis c) Bronchiolitis obliterans d) Complicated acute pneumonia e)
Transient pulmonary infiltrations in cystic fibrosis due to allergic aspergillosis
 Thorax (1965), 20, 385 Transient pulmonary infiltrations in cystic fibrosis due to allergic aspergillosis MARGARET MEARNS, WINIFRED YOUNG, AND JOHN BATTEN From the Queen Elizabeth Hospital, Hackney, and
Thorax (1965), 20, 385 Transient pulmonary infiltrations in cystic fibrosis due to allergic aspergillosis MARGARET MEARNS, WINIFRED YOUNG, AND JOHN BATTEN From the Queen Elizabeth Hospital, Hackney, and
Rare Association of Childhood Bronchiectasis with VACTERL Anomalies; a Case Report
 Rare Association of Childhood Bronchiectasis with VACTERL Anomalies; a Case Report Authors Details: Author's Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) R.M.D.H.M.RATHNAYAKE (1)(2)(3)(4)
Rare Association of Childhood Bronchiectasis with VACTERL Anomalies; a Case Report Authors Details: Author's Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) R.M.D.H.M.RATHNAYAKE (1)(2)(3)(4)
Discussing feline tracheal disease
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Unit II Problem 2 Pathology: Pneumonia
 Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Acute pneumonia Simple complement
 Acute pneumonia Simple complement 1. Clinical variants of acute pneumonia in children are, except: A. Bronchopneumonia B. Lobar confluent pneumonia C. Viral pneumonia D. Interstitial pneumonia E. Chronic
Acute pneumonia Simple complement 1. Clinical variants of acute pneumonia in children are, except: A. Bronchopneumonia B. Lobar confluent pneumonia C. Viral pneumonia D. Interstitial pneumonia E. Chronic
Bronchiectasis. from Childhood. patients (Field, 1961) were reduced to 79 of whom. 3 died, and reports on these were included in the
 Arch. Dis. Childh., 1969, 44, 551. Bronchiectasis Third Report on a Follow-up Study of Medical and Surgical Cases from Childhood C. ELAINE FIELD* From University College Hospital; and The Hdspitalfor Sick
Arch. Dis. Childh., 1969, 44, 551. Bronchiectasis Third Report on a Follow-up Study of Medical and Surgical Cases from Childhood C. ELAINE FIELD* From University College Hospital; and The Hdspitalfor Sick
Median Sternotomy for Pneumonectomy in Patients With Pulmonary Complications of Tuberculosis
 Median Sternotomy for Pneumonectomy in Patients With Pulmonary Complications of Tuberculosis Cliff P. Connery, MD, James Knoetgen III, MD, Constantine E. Anagnostopoulos, MD, and Madeline V. Svitak, BS,
Median Sternotomy for Pneumonectomy in Patients With Pulmonary Complications of Tuberculosis Cliff P. Connery, MD, James Knoetgen III, MD, Constantine E. Anagnostopoulos, MD, and Madeline V. Svitak, BS,
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Pathology of Pneumonia
 Pathology of Pneumonia Dr. Atif Ali Bashir Assistant Professor of Pathology College of Medicine Majma ah University Introduction: 5000 sq meters of area.! (olympic track) Filters >10,000 L of air / day!
Pathology of Pneumonia Dr. Atif Ali Bashir Assistant Professor of Pathology College of Medicine Majma ah University Introduction: 5000 sq meters of area.! (olympic track) Filters >10,000 L of air / day!
CONTRIBUTIONS TO THE COMPLEX MEDICO-SURGICAL TREATMENT OF PLEURAL SPACE DISEASES DOCTORAL THESIS
 UNIVERSITY OF MEDICINE AND PHARMACY FROM TÂRGU-MUREŞ DOCTORAL SCHOOL CONTRIBUTIONS TO THE COMPLEX MEDICO-SURGICAL TREATMENT OF PLEURAL SPACE DISEASES DOCTORAL THESIS Scientific Supervisor Prof. Dr. Alexandru-Mihail
UNIVERSITY OF MEDICINE AND PHARMACY FROM TÂRGU-MUREŞ DOCTORAL SCHOOL CONTRIBUTIONS TO THE COMPLEX MEDICO-SURGICAL TREATMENT OF PLEURAL SPACE DISEASES DOCTORAL THESIS Scientific Supervisor Prof. Dr. Alexandru-Mihail
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
An Image Repository for Chest CT
 An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis
 ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
Pneumonectomy in Children for Destroyed Lung: Evaluation of 18 Cases
 Pneumonectomy in Children for Destroyed Lung: Evaluation of 18 Cases Altug Kosar, MD, Alpay Orki, MD, Hakan Kiral, MD, Recep Demirhan, MD, and Bulent Arman, MD Sureyyapasa Chest Disease and Chest Surgery
Pneumonectomy in Children for Destroyed Lung: Evaluation of 18 Cases Altug Kosar, MD, Alpay Orki, MD, Hakan Kiral, MD, Recep Demirhan, MD, and Bulent Arman, MD Sureyyapasa Chest Disease and Chest Surgery
BRONCHOGRAPHY RESIDUAL IODIZED OIL FOLLOWING. bronchiectasis are to be undertaken, a previous inadequate bronchogram which
 Thorax (1946), 1, 93. RESIDUAL IODIZED OIL FOLLOWING BRONCHOGRAPHY BY H. E. COUNIHAN Thoracic Unit, Kewstoke Emergency Hospital Residual oil in the bronchial tree following bronchography is always undesirable;
Thorax (1946), 1, 93. RESIDUAL IODIZED OIL FOLLOWING BRONCHOGRAPHY BY H. E. COUNIHAN Thoracic Unit, Kewstoke Emergency Hospital Residual oil in the bronchial tree following bronchography is always undesirable;
Acute and Chronic Lung Disease
 KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
Diagnostic Evaluation of NTM and Bronchiectasis
 Division of Pulmonary, Critical Care and Sleep Medicine Diagnostic Evaluation of NTM and Bronchiectasis Ashwin Basavaraj, MD, FCCP NTM patient education program November 9, 2016 Involves a combination
Division of Pulmonary, Critical Care and Sleep Medicine Diagnostic Evaluation of NTM and Bronchiectasis Ashwin Basavaraj, MD, FCCP NTM patient education program November 9, 2016 Involves a combination
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
GENERAL THORACIC SURGERY
 GENERAL THORACIC SURGERY ELECTIVE PNEUMONECTOMY FOR BENIGN LUNG DISEASE: MODERN-DAY MORTALITY AND MORBIDITY This retrospective study of elective pneumonectomy for complicated inflammatory lung disease
GENERAL THORACIC SURGERY ELECTIVE PNEUMONECTOMY FOR BENIGN LUNG DISEASE: MODERN-DAY MORTALITY AND MORBIDITY This retrospective study of elective pneumonectomy for complicated inflammatory lung disease
WF RESPIRATORY SYSTEM. RESPIRATORY MEDICINE
 WF RESPIRATORY SYSTEM. RESPIRATORY MEDICINE 1 Societies 11 History 13 Dictionaries. Encyclopaedias. Bibliographies Use for general works only. Classify with specific aspect where possible 15 Classification.
WF RESPIRATORY SYSTEM. RESPIRATORY MEDICINE 1 Societies 11 History 13 Dictionaries. Encyclopaedias. Bibliographies Use for general works only. Classify with specific aspect where possible 15 Classification.
A Place For Airway Clearance Therapy In Today s Healthcare Environment
 A Place For Airway Clearance Therapy In Today s Healthcare Environment Michigan Society for Respiratory Care 2015 Fall Conference K. James Ehlen, MD October 6, 2015 Objectives Describe patients who will
A Place For Airway Clearance Therapy In Today s Healthcare Environment Michigan Society for Respiratory Care 2015 Fall Conference K. James Ehlen, MD October 6, 2015 Objectives Describe patients who will
DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 3: CHRONIC BRNCHITIS AND BRONCHIECTASIS
 DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 3: CHRONIC BRNCHITIS AND BRONCHIECTASIS INTRDUCTION In the last lecture we discussed the difference between restrictive and obstructive lung
DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 3: CHRONIC BRNCHITIS AND BRONCHIECTASIS INTRDUCTION In the last lecture we discussed the difference between restrictive and obstructive lung
PULMONARY TUBERCULOSIS RADIOLOGY
 PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
Pulmonary Agenesis sentations picked up over a period of 4 years. These cases were suspected and then documented during life.
 Pulmonary Agenesis sentations picked up over a period of 4 years. These cases were suspected and then documented during life. B. Rajshekhar Case Reports Sunil Gomber Anurag Krishna* Five cases of pulmonary
Pulmonary Agenesis sentations picked up over a period of 4 years. These cases were suspected and then documented during life. B. Rajshekhar Case Reports Sunil Gomber Anurag Krishna* Five cases of pulmonary
production Comparison of thin section computed tomography with bronchography for identifying bronchiectatic segments in patients with chronic sputum
 Thorax 1990;45:135-139 Host Defence Unit, Department of Thoracic Medicine, National Heart and Lung Institute, London N C Munro D C Currie P J Cole Department of Radiology, Brompton Hospital, London J C
Thorax 1990;45:135-139 Host Defence Unit, Department of Thoracic Medicine, National Heart and Lung Institute, London N C Munro D C Currie P J Cole Department of Radiology, Brompton Hospital, London J C
Imaging of the Lung in Children
 Imaging of the Lung in Children Imaging methods X-Ray of the Lung (Anteroposterior, ) CT, HRCT MRI USG Congenital developmental defects of the lungs Agenesis, aplasia, hypoplasia Tension pulmonary anomalies
Imaging of the Lung in Children Imaging methods X-Ray of the Lung (Anteroposterior, ) CT, HRCT MRI USG Congenital developmental defects of the lungs Agenesis, aplasia, hypoplasia Tension pulmonary anomalies
Chapter 16. Lung Abscess. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Chronic sputum production: correlations between clinical features and findings on high resolution computed tomographic scanning of the chest
 914 Department of Radiology, Addenbrooke's Hospital, Cambridge, UK E Jurriaans S Diedrich C D R Flower Department of Respiratory Medicine, Papworth Hospital, Cambridge CB3 8RE, UK I E Smith N Ali JM Shneerson
914 Department of Radiology, Addenbrooke's Hospital, Cambridge, UK E Jurriaans S Diedrich C D R Flower Department of Respiratory Medicine, Papworth Hospital, Cambridge CB3 8RE, UK I E Smith N Ali JM Shneerson
Destructive pulmonary disease due to mixed anaerobic infection
 Thorax (1970), 25, 41. Destructive pulmonary disease due to mixed anaerobic infection 0. SERIKI, A. ADEYOKUNNU, T. 0. DE LA CRUZ Departments of Paediatrics and Surgery, University College Hospital, Ibadan,
Thorax (1970), 25, 41. Destructive pulmonary disease due to mixed anaerobic infection 0. SERIKI, A. ADEYOKUNNU, T. 0. DE LA CRUZ Departments of Paediatrics and Surgery, University College Hospital, Ibadan,
CASE REPORTS. Inflammatory Polyp of the Bronchus. V. K. Saini, M.S., and P. L. Wahi, M.D.
 CASE REPORTS V. K. Saini, M.S., and P. L. Wahi, M.D. I n 1932 Jackson and Jackson [l] first reported a number of clinical cases under the title Benign Tumors of the Trachea and Bronchi with Especial Reference
CASE REPORTS V. K. Saini, M.S., and P. L. Wahi, M.D. I n 1932 Jackson and Jackson [l] first reported a number of clinical cases under the title Benign Tumors of the Trachea and Bronchi with Especial Reference
PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1
 PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1 Module A1 In-patient management of acute respiratory illness 1. Record of a total of 50 cases in 24 36 months to reflect competencies outlined in curriculum Bronchiolitis
PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1 Module A1 In-patient management of acute respiratory illness 1. Record of a total of 50 cases in 24 36 months to reflect competencies outlined in curriculum Bronchiolitis
Video-assisted thoracic surgery for pulmonary sequestration: a safe alternative procedure
 Original Article Video-assisted thoracic surgery for pulmonary sequestration: a safe alternative procedure Lu-Ming Wang, Jin-Lin Cao, Jian Hu Department of Thoracic Surgery, The First Affiliated Hospital,
Original Article Video-assisted thoracic surgery for pulmonary sequestration: a safe alternative procedure Lu-Ming Wang, Jin-Lin Cao, Jian Hu Department of Thoracic Surgery, The First Affiliated Hospital,
Wedge resection for localized infectious lesions: high margin/ lesion ratio guaranteed operational safety
 Original Article Wedge resection for localized infectious lesions: high margin/ lesion ratio guaranteed operational safety Yifeng Sun 1,2 *, Likun Hou 3 *, Huikang Xie 3, Hui Zheng 1, Gening Jiang 1, Wen
Original Article Wedge resection for localized infectious lesions: high margin/ lesion ratio guaranteed operational safety Yifeng Sun 1,2 *, Likun Hou 3 *, Huikang Xie 3, Hui Zheng 1, Gening Jiang 1, Wen
Bronchiectasis in Adults - Suspected
 Bronchiectasis in Adults - Suspected Clinical symptoms which may indicate bronchiectasis for patients Take full respiratory history including presenting symptoms, past medical & family history Factors
Bronchiectasis in Adults - Suspected Clinical symptoms which may indicate bronchiectasis for patients Take full respiratory history including presenting symptoms, past medical & family history Factors
Thoracic Surgery; An Overview
 Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Despite their reputation of benignity, carcinoid tumors
 Operative Risk and Prognostic Factors of Typical Bronchial Carcinoid Tumors Xavier Ducrocq, MD, Pascal Thomas, MD, Gilbert Massard, MD, Pierre Barsotti, MD, Roger Giudicelli, MD, Pierre Fuentes, MD, and
Operative Risk and Prognostic Factors of Typical Bronchial Carcinoid Tumors Xavier Ducrocq, MD, Pascal Thomas, MD, Gilbert Massard, MD, Pierre Barsotti, MD, Roger Giudicelli, MD, Pierre Fuentes, MD, and
Fariba Rezaeetalab Associate Professor,Pulmonologist
 Fariba Rezaeetalab Associate Professor,Pulmonologist rezaitalabf@mums.ac.ir Patient related risk factors Procedure related risk factors Preoperative risk assessment Risk reduction strategies Age Obesity
Fariba Rezaeetalab Associate Professor,Pulmonologist rezaitalabf@mums.ac.ir Patient related risk factors Procedure related risk factors Preoperative risk assessment Risk reduction strategies Age Obesity
Conventional High-Resolution CT Versus Helical High- Resolution MDCT in the Detection of Bronchiectasis
 High- Resolution CT Versus MDCT in Detecting Bronchiectas is Chest Imaging Original Research A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:414 420 0361 803X/06/1872 414 American Roentgen Ray
High- Resolution CT Versus MDCT in Detecting Bronchiectas is Chest Imaging Original Research A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:414 420 0361 803X/06/1872 414 American Roentgen Ray
Respiratory distress in patients with central airway obstruction
 Indian J Thorac Cardiovasc Surg (2010) 26:151 156 DOI 10.1007/s12055-010-0021-0 ORIGINAL ARTICLE Respiratory distress in patients with central airway obstruction Mohamed Abdel Hamied Regal & Yasser Ahmed
Indian J Thorac Cardiovasc Surg (2010) 26:151 156 DOI 10.1007/s12055-010-0021-0 ORIGINAL ARTICLE Respiratory distress in patients with central airway obstruction Mohamed Abdel Hamied Regal & Yasser Ahmed
High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
 European Review for Medical and Pharmacological Sciences High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
European Review for Medical and Pharmacological Sciences High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
A recurrent empyema with peripheral bronchopleural fistulas treated by retrograde bronchial sealing with Gore Tex plugs: a case report
 Case Report A recurrent empyema with peripheral bronchopleural fistulas treated by retrograde bronchial sealing with Gore Tex plugs: a case report Jin-Young Ahn 1, Dohun Kim 2, Jong-Myeon Hong 2, Si-Wook
Case Report A recurrent empyema with peripheral bronchopleural fistulas treated by retrograde bronchial sealing with Gore Tex plugs: a case report Jin-Young Ahn 1, Dohun Kim 2, Jong-Myeon Hong 2, Si-Wook
Prapaporn Pornsuriyasak, M.D. Pulmonary and Critical Care Medicine Ramathibodi Hospital
 Prapaporn Pornsuriyasak, M.D. Pulmonary and Critical Care Medicine Ramathibodi Hospital Only 20-30% of patients with lung cancer are potential candidates for lung resection Poor lung function alone ruled
Prapaporn Pornsuriyasak, M.D. Pulmonary and Critical Care Medicine Ramathibodi Hospital Only 20-30% of patients with lung cancer are potential candidates for lung resection Poor lung function alone ruled
COUGH Dr. A m A it i e t sh A g A garwa w l Le L ctu t rer Departm t ent t o f f M e M dic i in i e
 COUGH Dr. Amitesh Aggarwal Lecturer Department of Medicine Cough is an explosive expiration that provides a normal protective mechanism for clearing the tracheobronchial tree of secretions and foreign
COUGH Dr. Amitesh Aggarwal Lecturer Department of Medicine Cough is an explosive expiration that provides a normal protective mechanism for clearing the tracheobronchial tree of secretions and foreign
Echinococcus granulosus is frequently encountered in
 Surgical Treatment of Pulmonary Hydatid Cysts: Is Capitonnage Necessary? Akif Turna, MD, Muhammet Ali Yılmaz, MD, Gökhan Hacıibrahimoğlu, MD, Cemal Asım Kutlu, MD, and Mehmet Ali Bedirhan, MD Department
Surgical Treatment of Pulmonary Hydatid Cysts: Is Capitonnage Necessary? Akif Turna, MD, Muhammet Ali Yılmaz, MD, Gökhan Hacıibrahimoğlu, MD, Cemal Asım Kutlu, MD, and Mehmet Ali Bedirhan, MD Department
Bronchography in chronic bronchitis
 Bronchography in chronic bronchitis A. G. OGILVIE Wood Cottage, Thropton, Morpeth, Northumnberland Thorax (1975), 30, 631. Ogilvie, A. G. (1975). Thorax, 30, 631-635. Bronchography in chronic bronchitis.
Bronchography in chronic bronchitis A. G. OGILVIE Wood Cottage, Thropton, Morpeth, Northumnberland Thorax (1975), 30, 631. Ogilvie, A. G. (1975). Thorax, 30, 631-635. Bronchography in chronic bronchitis.
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
4.6 Small airways disease
 4.6 Small airways disease Author: Jean-Marc Fellrath 1. INTRODUCTION Small airways are defined as any non alveolated and noncartilaginous airway that has an internal diameter of 2 mm. Several observations
4.6 Small airways disease Author: Jean-Marc Fellrath 1. INTRODUCTION Small airways are defined as any non alveolated and noncartilaginous airway that has an internal diameter of 2 mm. Several observations
Northumbria Healthcare NHS Foundation Trust. Bronchiectasis. Issued by Respiratory Medicine
 Northumbria Healthcare NHS Foundation Trust Bronchiectasis Issued by Respiratory Medicine The aim of this booklet is to help you manage your bronchiectasis. It contains information which you should find
Northumbria Healthcare NHS Foundation Trust Bronchiectasis Issued by Respiratory Medicine The aim of this booklet is to help you manage your bronchiectasis. It contains information which you should find
141 Ann Thorac Surg , Aug Copyright by The Society of Thoracic Surgeons
 Completion Pneumonectomy: Indications, Complications, and Results Eilis M. McGovern, M.B.B.Ch., Victor F. Trastek, M.D., Peter C. Pairolero, M.D., and W. Spencer Payne, M.D. ABSTRACT From 958 through 985,
Completion Pneumonectomy: Indications, Complications, and Results Eilis M. McGovern, M.B.B.Ch., Victor F. Trastek, M.D., Peter C. Pairolero, M.D., and W. Spencer Payne, M.D. ABSTRACT From 958 through 985,
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax
 Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA
 Thor-ax (1954), 9, 304. PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA W. J. HANBURY, R. J. R. CURETON, AND G. SIMON From St. Bartholomew's Hospital, London BY (RECEIVED FOR PUBLICATION JUNE
Thor-ax (1954), 9, 304. PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA W. J. HANBURY, R. J. R. CURETON, AND G. SIMON From St. Bartholomew's Hospital, London BY (RECEIVED FOR PUBLICATION JUNE
A Case of Pediatric Plasma Cell Granuloma
 August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
Non Cystic Fibrosis Bronchiectasis: How to Proceed?
 Non Cystic Fibrosis Bronchiectasis: How to Proceed? Dr Ankit Parakh MD, DNB, MNAMS, RCPCH Fellow (UK), European Diplomate of Pediatric Respiratory Medicine ERS Fellowship Pediatric Medicine & NIV (GOSH,
Non Cystic Fibrosis Bronchiectasis: How to Proceed? Dr Ankit Parakh MD, DNB, MNAMS, RCPCH Fellow (UK), European Diplomate of Pediatric Respiratory Medicine ERS Fellowship Pediatric Medicine & NIV (GOSH,
Respiratory Pathology. Kristine Krafts, M.D.
 Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Disease spectrum. IPA Invasive pulmonary aspergillosis
 Aspergillus & ABPA Disease spectrum IPA Invasive pulmonary aspergillosis ABPA ABPA pathophysiology conidia of Aspergillus trapped in mucous and narrowed airways of asthmatics/cf germinate to form hyphae
Aspergillus & ABPA Disease spectrum IPA Invasive pulmonary aspergillosis ABPA ABPA pathophysiology conidia of Aspergillus trapped in mucous and narrowed airways of asthmatics/cf germinate to form hyphae
The Bacteriology of Bronchiectasis in Australian Indigenous children
 The Bacteriology of Bronchiectasis in Australian Indigenous children Kim Hare, Amanda Leach, Peter Morris, Heidi Smith-Vaughan, Anne Chang Presentation outline What is bronchiectasis? Our research at Menzies
The Bacteriology of Bronchiectasis in Australian Indigenous children Kim Hare, Amanda Leach, Peter Morris, Heidi Smith-Vaughan, Anne Chang Presentation outline What is bronchiectasis? Our research at Menzies
HEMOPTYSIS. Prof. G. Zuliani
 HEMOPTYSIS Prof. G. Zuliani HEMOPTYSIS Hemoptysis is the expectoration of blood, that can range from blood-streaking of sputum (Hemoptoe) to the presence of gross blood in the absence of any accompanying
HEMOPTYSIS Prof. G. Zuliani HEMOPTYSIS Hemoptysis is the expectoration of blood, that can range from blood-streaking of sputum (Hemoptoe) to the presence of gross blood in the absence of any accompanying
Surgical treatment of synchronous multiple neuroendocrine lung tumours (case series): is more always better?
 Case Report Page 1 of 5 Surgical treatment of synchronous multiple neuroendocrine lung tumours (case series): is more always better? Jury Brandolini, Luca Bertolaccini, Alessandro Pardolesi, Piergiorgio
Case Report Page 1 of 5 Surgical treatment of synchronous multiple neuroendocrine lung tumours (case series): is more always better? Jury Brandolini, Luca Bertolaccini, Alessandro Pardolesi, Piergiorgio
Primary chondrosarcoma of lung
 Thorax,(1970), 25, 366. Primary chondrosarcoma of lung G. M. REES Department of Surgery, Brompton Hospital, Lontdonl, S.W.3 A case of primary chondrosarcoma of the lung is described in a 64-year-old man.
Thorax,(1970), 25, 366. Primary chondrosarcoma of lung G. M. REES Department of Surgery, Brompton Hospital, Lontdonl, S.W.3 A case of primary chondrosarcoma of the lung is described in a 64-year-old man.
PULMONARY RESECTION FOR TUBERCULOSIS
 Thorax (1951), 6, 375. PULMONARY RESECTION FOR TUBERCULOSIS IN CHILDREN BY COLIN A. ROSS From Shotley Bridge Hospital and Poole Sanatorium (RECEIVED FOR PUBLICATION JULY 9, 1951) The literature concerning
Thorax (1951), 6, 375. PULMONARY RESECTION FOR TUBERCULOSIS IN CHILDREN BY COLIN A. ROSS From Shotley Bridge Hospital and Poole Sanatorium (RECEIVED FOR PUBLICATION JULY 9, 1951) The literature concerning
American Journal ofcancer Case Reports
 American Journal ofcancer Case Reports http://ivyunion.org/index.php/ajccr/ Fracasso JI et al. American Journal of Cancer Case Reports 2018, 6:25-30 Page 1 of 6 Case Report Chondrosarcoma of the Sternum
American Journal ofcancer Case Reports http://ivyunion.org/index.php/ajccr/ Fracasso JI et al. American Journal of Cancer Case Reports 2018, 6:25-30 Page 1 of 6 Case Report Chondrosarcoma of the Sternum
Ruijin robotic thoracic surgery: S segmentectomy of the left upper lobe
 Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Case Report Ruptured Hydatid Cyst with an Unusual Presentation
 Case Reports in Surgery Volume 2011, Article ID 730604, 4 pages doi:10.1155/2011/730604 Case Report Ruptured Hydatid Cyst with an Unusual Presentation Deepak Puri, Amit Kumar Mandal, Harinder Pal Kaur,
Case Reports in Surgery Volume 2011, Article ID 730604, 4 pages doi:10.1155/2011/730604 Case Report Ruptured Hydatid Cyst with an Unusual Presentation Deepak Puri, Amit Kumar Mandal, Harinder Pal Kaur,
Bronchiectasis. Examples include: Viral infections (measles, adenovirus, influenza)
 Bronchiectasis What is Bronchiectasis? Bronchiectasis (pronounced bron-kee-ek'-tas-is) is a condition of the airways in the lungs. These airways (bronchial tubes) are tubelike structures that branch from
Bronchiectasis What is Bronchiectasis? Bronchiectasis (pronounced bron-kee-ek'-tas-is) is a condition of the airways in the lungs. These airways (bronchial tubes) are tubelike structures that branch from
The clinical finding, diagnosis and outcome of patients with complicated lung hydatid cysts
 Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 8:293-297 The clinical finding, diagnosis and outcome of patients with complicated
Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 8:293-297 The clinical finding, diagnosis and outcome of patients with complicated
The right middle lobe is the smallest lobe in the lung, and
 ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
How to Analyse Difficult Chest CT
 How to Analyse Difficult Chest CT Complex diseases are:- - Large lesion - Unusual or atypical pattern - Multiple discordant findings Diffuse diseases are:- - Numerous findings in both sides 3 basic steps
How to Analyse Difficult Chest CT Complex diseases are:- - Large lesion - Unusual or atypical pattern - Multiple discordant findings Diffuse diseases are:- - Numerous findings in both sides 3 basic steps
TB Intensive Houston, Texas
 TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
Foreign Body Aspiration in Children - A Persistent Problem
 Foreign Body Aspiration in Children - A Persistent Problem Abstract Parveen Tariq ( Department of Pediatrics, Rawalpindi Medical College, Rawalpindi. ) Pages with reference to book, From 33 To 36 Objective:
Foreign Body Aspiration in Children - A Persistent Problem Abstract Parveen Tariq ( Department of Pediatrics, Rawalpindi Medical College, Rawalpindi. ) Pages with reference to book, From 33 To 36 Objective:
The Surgical Treatment of Tracheobronchial Tuberculosis. The Thoracic Department of Beijing Chest Hospital, Capital Medical University
 The Surgical Treatment of Tracheobronchial Tuberculosis ) The Thoracic Department of Beijing Chest Hospital, Capital Medical University Named also: endobronchial tuberculosis,ebtb defined as tuberculous
The Surgical Treatment of Tracheobronchial Tuberculosis ) The Thoracic Department of Beijing Chest Hospital, Capital Medical University Named also: endobronchial tuberculosis,ebtb defined as tuberculous
