Seattle-King County EMS
|
|
|
- Hilary McGee
- 5 years ago
- Views:
Transcription
1 Seattle-King County EMS Seattle-King County Emergency Medical Services Division Public Health - Seattle/King County th Avenue, Suite 1200 Seattle, WA (206) January 2011 CBT425-EMT11 - Respiratory Emergencies PRINT VERSION FOR A WEB-BASED TRAINING MODULE December 22, Seattle / King County EMS
2 Introduction Patients with lung and heart diseases frequently call because of breathing difficulty. This course reviews common disorders that can cause respiratory emergencies and prehospital management of these conditions. Before You Begin This is a continuing education and recertification course for EMTs. It covers fundamental EMT- Basic concepts and terminology as well as advanced material. We highly recommend completing the practice exam before attempting the exam. We also recommend that you review an EMT textbook chapter covering this topic as a refresher before taking the exam, for example: Chapter 11 - Respiratory Emergencies in Emergency Care and Transportation of the Sick and Injured, 9th edition (AAOS). The elaboration links that appear throughout this course contain supplemental information to aid in your understanding of the topic. The optional external website links are for the purpose of expanding your knowledge; however, the course exams do not cover material from these sources. A PDF/print version of this course is available that contains most of the text content of the online course but does not include the interactive questions or exercises. Practical Skills To receive CBT or OTEP credit for this course a trained skills evaluator must evaluate your ability to perform the following hands-on practical skills including: Airway management (airway maneuvers to include pediatric) Auscultation of breath sounds Assisted ventilation with a BVM Oropharyngeal/nasopharyngeal airway Suction Oxygen administration Course Objectives CBT425 is an EMT continuing education and recertification course. After completing this course you will be able to: 1. Identify the anatomic structures of the respiratory system. 2. Demonstrate an understanding of the physiology of the respiratory system and its relationship to BLS treatment. 3. Identify signs and symptoms of respiratory emergencies. 4. Identify treatment of respiratory emergencies. 5. Distinguish between normal and abnormal breath sounds. 6. Identify correct technique for auscultation of breath sounds. 7. Identify correct BVM technique and suctioning technique. 2
3 Terms Terms You Should Know chronic obstructive pulmonary disease (COPD) - A category of diseases characterized by a slow process of dilation and disruption of pulmonary alveoli. dyspnea - A term for shortness of breath or breathing difficulty. embolus - A blood clot or other substance that has formed in a blood vessel or the heart, that breaks off and travels to another blood vessel, where it may cause blockage. flail chest - A condition in which three or more ribs are fractured in two or more places such that a section of the chest wall is detached from the rest of the chest wall. gag reflex - A protective contraction of the muscles of the throat caused especially by stimulation of the pharynx that prevents food and liquids from entering the airway. hypoxia - A condition in which the body's cells and tissue do not have enough oxygen. pleuritic chest pain - A sharp, stabbing pain in the chest that is worsened by a deep breath; often caused by inflammation or irritation of the pleura. pneumothorax - Condition where air enters the pleural space and is trapped during expiration. It can occur without trauma as in a spontaneous pneumothorax. pulmonary edema - A buildup of fluid in the lungs, usually as a result of congestive heart failure. rales - Crackling, rattling breath sounds signaling fluid in the air spaces of the lungs. rhonchi - Coarse breath sounds heard in patients with mucus in the airways. stridor - A harsh, high-pitched inspiratory sound often heard in acute laryngeal (upper airway) obstruction. tension pneumothorax - A life-threatening condition in which air enters the pleural space and the pressure inside the lung cavity progressively increases and compresses the lung. It may displace the mediastinum and other structures toward the opposite side. traumatic asphyxia - Condition characterized by distended neck veins, cyanosis in face and neck and bleeding in the sclera of the eye that is caused by severe compression of the chest. wheeze - A high-pitched, whistling breath sound, characteristically heard on expiration in patients with asthma or COPD. 3
4 New Terms hypoxic drive - A condition in which the body's stimulus for taking a breath is low oxygen. Occurs in people with COPD. metabolism - The process by which food molecules are broken down to provide material and energy for cellular function. ph (potential of hydrogen) - A measure of the acidity or alkalinity of a solution, numerically equal to 7 for neutral solutions, increasing with increasing alkalinity and decreasing with increasing acidity. The ph scale ranges from 0 to 14. Numbers from 7 and below represent increasing acidity. perfusion - The movement of blood through an organ or tissue in order to supply nutrients and oxygen. tidal volume The volume of gas that is moved with each breath which is normally 500 ml in an adult. ventilation The rate at which gas enters or leaves the lungs. Generally it is described in terms of good or poor ventilation. Bluish or dusky skin can indicate poor ventilation. Respiratory Structures Airway protection and oxygen administration are perhaps the most important BLS skills you have. Therefore it is important to know the structures of the respiratory system understand the basic physiology that is affected by BLS treatment. Functions of the Respiratory Structures Learning Activity located on this page PHYSIOLOGY Metabolism Produces Carbon Dioxide Metabolism is the process by which the body breaks down or "burns" stored fuel to create energy. The cells use oxygen to transform stored glucose into energy. You can think of glucose as "fuel" and oxygen as the "match" that releases the energy. A byproduct of metabolism is carbon dioxide (CO2). Carbon dioxide is produced by the cells and carried by the circulatory system to the lungs where it is expired. If respirations are impaired, carbon dioxide builds up in the blood. This excess carbon dioxide combines with water in the blood to produce an acid. 4
5 ph Acidity in a solution such as blood is measured by what is called potential of hydrogen or ph. The body must maintain a relatively narrow ph range (neither too acidic nor too basic). The respiratory system helps maintain a balanced acid level or ph in the blood. The ph Balancing Act The respiratory system is a mirror for other changes that can happen in the body. If the blood ph becomes too low (acidic), the respiratory system will attempt to fix this by making the lungs breathe more deeply and rapidly, thus excreting more carbon dioxide. The body attempts to maintain a balance or homeostasis. Because the respiratory system helps regulate carbon dioxide excretion or retention, it is an important mechanism for regulating ph. Hypercarbia - Excess Carbon Dioxide Hypercarbia is a state of excessive carbon dioxide in the body. This results in acidosis as the carbon dioxide causes a chemical reaction producing carbonic acid. Hypercarbia can occur through: Metabolic processes that form acids Muscle exertion Shivering Hypercarbia also can occur through decreased elimination of carbon dioxide, for example with: Airway obstruction Inability to exhale fully (e.g., asthma or emphysema) Depressed respiratory drive (e.g., overdose of sedative drugs) When hypercarbia occurs it affects the chemistry of the body causing a ph imbalance. Hypoxic Drive The amount of carbon dioxide in the blood is the primary stimulus for breathing. A secondary stimulus for breathing is hypoxia, a decrease in oxygen. While less important for regulation of breathing in the average person, in some individuals, this so-called hypoxic drive is the primary stimulus for respiration. This occurs in a small percentage of COPD patients whose expirations are so inefficient that their bodies have become accustomed to higher than normal levels of carbon dioxide. A decrease in oxygen, rather than an increase in carbon dioxide, provides the primary stimulus for taking a breath. 5
6 Elaboration - Respiratory Drive Respiratory drive, or the act of breathing, is an autonomic and involuntary function controlled by centers in the brain sensitive to the blood levels of oxygen and carbon dioxide. Specialized brain cells constantly monitor and react to the levels of oxygen and carbon dioxide in the blood. For example, when the body is deprived of oxygen it attempts to compensate by increasing the rate and depth of respirations. The body s response to increased carbon dioxide in the blood is to "blow off carbon dioxide by increasing the rate and depth of respirations. Metabolic Problems Affect Respirations Metabolic imbalances affect the chemistry of the body affecting ph and other measures of body chemistry. While this is not a respiratory problem, the respiratory system often tries to compensate to maintain equilibrium by changing the depth and/or rate of respirations. Elaboration - Metabolic Problems Ketoacidosis is the result of inefficient metabolism of sugars in a diabetic that causes the body to turn to other fuel sources for energy, namely fat and muscle. Byproducts of this inefficient metabolism are acids called ketoacids. The presence of ketoacids and related compounds in the blood will cause a lower ph. The respiratory system responds by increasing the depth and/or rate of respirations. Aspirin overdose can cause metabolic problems. Aspirin is an acid (the chemical name is acetylsalicylic acid). When taken in large quantities, a person with an aspirin overdose can become acidotic. Again, the body compensates by increasing the depth and/or rate of respirations. Fever and sepsis also can cause metabolic problems. Fever increases the metabolic rate, causing the production of more carbon dioxide that can lead to more acid in the blood. When tissue perfusion fails (as it can in sepsis) excess metabolic acids accumulate causing a metabolic acidosis with a low ph. The body in turn responds by increasing the depth and/or rate of respirations. A person who is hyperventilating for psychological reasons is breathing deeply and rapidly. This is a very efficient way of ridding the body of carbon dioxide which in turn may alter the body s equilibrium and cause what is known as alkalosis (meaning very "basic"). Symptoms of respiratory alkalosis may include faintness and tingling in the extremities. CLINICAL SYNDROMES Airway Obstruction EMS providers should intervene if a choking victim has signs of severe airway obstruction such as poor air exchange or increased breathing difficulty as indicated by a silent cough, cyanosis or the inability to speak or breathe. 6
7 If the obstruction is mild and the victim is coughing forcefully, do not interfere with the efforts to relieve the obstruction. Attempt to relieve the obstruction only if it becomes severe. Use a finger sweep only if you can see solid material obstructing the airway of an unresponsive patient. Elaboration Foreign Bodies, Many Ways There are many ways a foreign object can lodge in an airway. For example, a stroke can damage swallowing reflexes, making the person more prone to choking. Consumption of alcohol and some drugs also suppresses the gag reflex. Asthma Asthma is a chronic, inflammatory disease of the airways. Asthma attacks are induced by many different factors including allergens, infections, exercise and smoke. During an asthma attack, the muscles around the bronchioles tighten, the lining of the inside the bronchioles swells and the inside of the bronchioles fills with thick mucous. This severely restricts expiration of air from the lungs. Patients will often describe a history of asthma and have a prescription for a metered-dose inhaler. BLS treatment considerations include: Calming the patient Airway management Oxygen therapy Assisting with a prescribed inhaler Elaboration Asthma Asthma is a disease that affects the bronchi and bronchioles that carry air in and out of the lungs. In persons with asthma, the inside walls of the airways are swollen. They are very sensitive to things such as dust, pollen, drugs, air pollutants and physical stimuli. The airways become narrow and less air flows into the lungs. This causes symptoms like wheezing, coughing, chest tightness and breathing difficulty. In an asthma attack, muscles around the airways tighten, making the airway openings narrower so less air can flow through. Inflammation increases and the airways become more swollen and narrow. Cells in the airways also produce more mucus than normal. This extra mucus also narrows the airways. COPD Chronic obstructive pulmonary disease (COPD) is a category of diseases that includes asthma, emphysema and chronic bronchitis. COPD causes a slow process of dilation and disruption of the airways and alveoli and includes several related irreversible conditions that limit the ability to exhale. 7
8 Persons with COPD can present with shortness of breath, fever and increased sputum production. Their medical history can include upper-respiratory infection, chronic bronchitis, emphysema, a history of smoking or working in a hazardous environment (e.g., coal smoke, asbestos). Common medications for COPD includes: Prednisone Proventil Ventolin Atrovent Azmacort BLS treatment for a COPD patient with respiratory distress should include high flow oxygen. Elaboration Emphysema In emphysema, the very small airways that join the alveoli are damaged and the walls lose elasticity. Chronic irritation of small airways causes inflammation and swelling, reducing the diameter of these air passages. Irritation causes bronchospasms and further decreases the lumen. On inspiration, the expansion of the lungs holds airways open. On exhalation, the lungs relax and the airways narrow, trapping air. Elaboration Chronic Bronchitis Chronic bronchitis is characterized by structural changes in airways of the lungs and enlargement of the mucous glands that cause coughing and production of sputum. Chronic bronchitis also causes shortness of breath and is often accompanied by infection, mucus production and coughing. Congestive Heart Failure Congestive heart failure (CHF) is a result of too much fluid in the lungs making it difficult to get air in as opposed to a COPD patient who has trouble getting air out. CHF Content Player 1. Congestive heart failure occurs when the ventricles are weakened by myocardial infarction, underlying coronary artery disease, hypertension or valve disease. 2. This impairs the heart s ability to contract and empty during systole and blood backs up in the lungs and tissues of the body. 3. Increased pressure in the left ventricle is transmitted to the lung capillaries and fluid is forced into the alveoli. 4. This interrupts gas exchange and results in shortness of breath. 5. Increased pressure in the right ventricle causes fluid to back up into the body s tissues, leading primarily to swelling in the lower extremities. 8
9 6. CHF patients commonly do not suffer from a purely left- or purely right-ventricle heart failure, but rather they present with a combination of symptoms (e.g., fluid in the lungs and swelling in the lower extremities). CHF is usually chronic with acute exacerbations. During an acute exacerbation the patient will present sitting up, short of breath, diaphoretic, and pale, or cyanotic in color. Breath sounds can include rales or wheezes. The medical history can include increased salt ingestion, respiratory infection, non-compliance with medications, angina, or symptoms of acute coronary syndrome. Common medications include: ACE inhibitors Furosemide (Lasix) HCTZ (hydrochlorthiazide) Beta-blockers Angiotensin II receptor blockers Digoxin (Lanoxin) Medications can help differentiate this patient's symptoms from those of someone with COPD. When treating CHF, seat the patient upright and administer high flow oxygen; consider positive pressure ventilation with a BVM if the patient is experiencing severe respiratory difficulty. Inhalation Injuries Inhalation injuries are due to breathing of chemicals, smoke or other substances. Common chief complaints include: shortness of breath, coughing, hoarseness, chest pain due to bronchial irritation and nausea. Individuals with decreased respiratory reserve (e.g., history of COPD or CHF) are likely to experience an exacerbation of the disease. If a patient is in respiratory distress, treat immediately with high flow oxygen. Assist breathing with a BVM if the respiratory effort is insufficient as indicated by a slow rate and poor air exchange. Pneumonia Symptoms of pneumonia include fever, chills, cough (often with yellowish sputum), shortness of breath, general discomfort, fatigue, loss of appetite and headache. There can be chest pain associated with breathing (usually sharp and stabbing in nature) and worsened by coughing or deep inspirations. Other signs that sometimes present are rales, clammy skin, upper abdominal pain and blood-tinged sputum. Emergency care for pneumonia depends on the severity of breathing difficulty but may include oxygen therapy. 9
10 Pneumothorax A pneumothorax is the presence of air in the pleural space. It is caused when an internal or external wound allows air to enter the space between pleural tissues. This causes collapse of the lung. A pneumothorax can cause sharp chest pain and shortness of breath. You may be able to feel subcutaneous air and breath sounds will be diminished. Treatment of a pneumothorax includes high-flow oxygen. Be judicious with use of positivepressure ventilation; it can turn a spontaneous pneumothorax into a life-threatening tension pneumothorax. Elaboration Pneumothorax A pneumothorax is the presence of air between the two layers of the pleura also called the pleural space. Under normal conditions there is no air between these layers because they are sealed together. However, air or blood can enter the space, for example when a hole is punctured in the chest wall by a gunshot or stab wound. A pneumothorax can occur spontaneously (e.g., a rupture due to disease or localized weakness of the lung lining) or as a result of trauma. Forceful coughing can cause a pneumothorax as well. Chest injury and prior history of pneumothorax are possible medical histories. COPD is a risk factor. A pneumothorax can cause collapse of the entire lung. The only symptom may be sudden chest pain. Elaboration Tension Pneumothorax A tension pneumothorax is a progressively worsening pneumothorax that begins to impinge on the function of the lungs and the circulatory system. It is caused when a lung injury acts like a one-way valve that allows free air to move into the pleural space but prevents the free exit of that air. Pressure builds inside the pleural space and compresses the lungs and other organs. The early signs of a tension pneumothorax include: Increased dyspnea Cyanosis Signs of shock Distended neck veins Shift in PMI (Point of maximum intensity, where the heart is the loudest through auscultation) Tracheal displacement Tracheal deviation Pulmonary Embolism A pulmonary embolism (PE) occurs when a particle such as a blood clot, fat embolus, amniotic fluid embolus or air bubble gets loose in the blood stream and travels to the lungs. The embolus lodges in a major branch of the pulmonary artery and circulation through a large portion of the lung is interrupted. Blood is not able to reach the alveoli and it cannot be oxygenated. 10
11 This condition can be caused by immobility of the lower extremities, prolonged bed rest or recent surgery. Signs of PE are a sudden-onset of shortness of breath, tachypnea, chest pain worsened by breathing and coughing up blood. Pulmonary embolism is a life-threatening condition and should be treated with high flow oxygen and rapid transport. Move the patient gently to avoid dislodging additional emboli. Elaboration Volunteer Fire Captain On November 4, 2005, a 38-year-old male volunteer fire Captain was home when the fire department (FD) was dispatched to a medical call. As he began to respond, he collapsed. His wife found him getting up and complaining of breathing difficulty. He asked her to take him to the hospital instead of calling 911. Before he could get dressed, he collapsed again and his wife called 911. FD units and a mutual aid ambulance were dispatched and provided basic life support (BLS). En route to the hospital s emergency department (ED), the Captain became unresponsive, stopped breathing, and was pulseless. Ambulance service emergency medical technicians (EMTs), and FD crew members began cardiopulmonary resuscitation (CPR). Despite CPR and BLS performed by FD crew members and ambulance service EMTs, and advanced life support (ALS) performed by hospital ED personnel, the Captain died. PATIENT CARE Assessment of Respiratory Status Start your evaluation of respiratory status by assessing the rate and depth of respirations. A normal rate is between 12 and 20 respirations per minute for an adult. The depth of respirations is more subjective and varies from shallow, normal, labored or gasping. Together the rate and depth will tell you whether tidal volume is adequate. In addition to rate and depth, your assessment of respiratory status should take into consideration other signs that indicate an adequate oxygen supply to the body s tissues such as: Level of consciousness Breathing effort Ability to speak in complete sentences Use of accessory muscles Skin color Breath sounds Body position Elaboration Irregular Breathing Patterns Irregular breathing patterns are generally caused by specific conditions. For example, Cheyne-Stokes respirations, which may be seen in head injuries and stroke, are characterized by periods of breathing with gradually increasing and decreasing of tidal volume interspersed with periods of no breathing. Irregular, ineffective respirations with no clear pattern are called ataxic respirations. 11
12 Agonal respirations are an abnormal pattern of breathing characterized by ineffective, slow inspirations followed by long pauses. They are often sound like gasps. Agonal respirations are associated with cardiac arrest or severe end-stage shock. Auscultation of Breath Sounds The proper technique for auscultating the chest using a stethoscope includes: Listen at six locations on the back Listen at four locations on the front Instruct the patient to take a deep breath through the mouth then exhale Listen to one or two inspiration/expiration cycles per location Avoid listening through clothing Changing airflow patterns inside the lungs produce normal breath sounds. They make a "swishing" sound as one breathes in or out. Absent breath sounds can indicate apnea, pneumothorax, hemothorax or lung removal. Breath Sounds EMTs must be able to distinguish normal breath sounds from abnormal breath sounds. Airway Management Airway management is one of the most important skills for an EMS provider. You should be well versed in the following airway management techniques: Head tilt/chin lift Jaw thrust Patient positioning Airway adjuncts Suction Oxygen therapy Assisted ventilation Relief of foreign body airway obstruction Suction The purpose of suction is to remove vomit, blood, excretions and other matter from the airway. Here are some guidelines to use for suctioning: Measure the tip from corner of mouth to earlobe Oxygenate the patient well (if the situation permits) Insert the tip into the oral cavity without applying suction Move the suction tip side to-side Oxygenate well after suctioning 12
13 Elaboration - Tips for Effective Suctioning Measure the tip the same as for an oropharyngeal airway from the corner of the mouth to the ear lobe or from the center of the mouth to the angle of the jaw. Insert the tip only to the base of the tongue. If the situation permits (e.g., there is no significant airway threat), give at least 30 seconds of oxygen before suctioning. Administer oxygen after suctioning and consider assisting ventilations with a bag-valve mask to help provide extra oxygen. Do not apply suction while inserting the tip. This can rob the airway of oxygen. Apply suction for no more than 15 seconds at a time. In rare cases, copious vomiting that threatens the airway may require more suctioning. In infants and children, suction for shorter periods of time (e.g., no more than 5 seconds). If there are secretions or emesis that you cannot easily remove with suction, position the patient, (e.g., by using the log roll) so that gravity and a finger sweep can quickly clear the airway. Assisted Ventilation For patients who lack oxygen, for example, someone with a decreased respiratory drive from a narcotic overdose, you must take quick action to improve the depth and rate of respirations. A bag-valve mask (BVM) is a useful tool for improving ventilation and acidbase (ph) balance. The proper technique for assisting ventilation with a BVM is as follows. Unconscious breathing patient: Consider the need for an oropharyngeal airway* Do not over-ventilate Keep the airway open Maintain a good seal Apply the Sellick maneuver which can help reduce airflow into the stomach *Follow local protocols. Non-breathing patient: Deliver a ventilation of 1-second duration Deliver enough volume to make the chest rise 12 ventilations/min 8-10 ventilations/min if an advanced airway is in place Oxygen Delivery The amount of oxygen you administer to a patient and the method of administration depend on many factors including medical history and the cause of respiratory problem. 13
14 Here are delivery rate guidelines for various devices: Rate Volume (liters/min) Device Low flow 2 6 Nasal cannula Low flow 2 6 Blow by High flow Nonrebreathing mask High flow with ventilation 15+ Bag-valve mask with reservoir Summary The main structures of the respiratory system are: Pharynx Trachea Epiglottis Alveoli Bronchi Bronchioles Larynx Pleura Diaphragm The respiratory system is an important mechanism for regulating ph in the body. If respiration is impaired, carbon dioxide builds up in the blood (hypercarbia) and produces an acid. BLS providers can help treat this condition by improving ventilation. Signs of severe airway obstruction include poor air exchange and increased breathing difficulty. Persons with a COPD-related emergency may present with shortness of breath, fever and increased sputum production. Signs of congestive heart failure may include an acute onset of breathing difficulty, diaphoresis and cyanosis. A pneumothorax can cause sharp chest pain and shortness of breath. Signs of pulmonary embolism include a sudden onset of shortness of breath, tachypnea, chest pain worsened by breathing and coughing up of blood. Treatment for a respiratory emergency can include high flow oxygen and, in the case of decreased respiratory drive, assisted ventilations. CHF patients may require positivepressure ventilations. The proper technique for auscultating the chest includes: Listen at six locations on the back Listen at four locations on the front Move from bottom to top in a medical patient Instruct the patient to take a deep breath through the mouth then exhale Listen to one or two inspiration/expiration cycles per location Avoid listening through clothing 14
15 Guidelines for use of suction include: Measure the tip from corner of mouth to earlobe Oxygenate the patient well (if the situation permits) Insert the tip into the oral cavity without applying suction Move the suction tip side to side Oxygenate well after suctioning The key points for ventilating an unconscious breathing patient are: Consider oropharyngeal airway Do not over-ventilate Keep the airway open Maintain a good seal Apply the Sellick maneuver which can help reduce airflow into the stomach 15
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
Anatomy Review. Anatomy Review. Respiratory Emergencies CHAPTER 16
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Firefighter Pre-Hospital Care Program Recruit Presentation. Respiratory Emergencies
 Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Chapter 11: Respiratory Emergencies
 29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
Respiratory Emergencies. Lesson Goal. Lesson Objectives 9/10/2012
 Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
Overview. The Respiratory System. Chapter 18. Respiratory Emergencies 9/11/2012
 Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Respiratory Emergencies
 29698_CH11_Q_p001_012 4/12/05 2:03 PM Page 1 MEDICAL EMERGENCIES S E C T I O N 4 C H A P T E R Respiratory Emergencies 11 Workbook Activities The following activities have been designed to help you. Your
29698_CH11_Q_p001_012 4/12/05 2:03 PM Page 1 MEDICAL EMERGENCIES S E C T I O N 4 C H A P T E R Respiratory Emergencies 11 Workbook Activities The following activities have been designed to help you. Your
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Bronchoconstriction is also treated with medications that inhibit bronchiolar constriction such as: Ipratropium (Atrovent)
 Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Cardiovascular and Respiratory Disorders
 Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 Respiration
 1 Chapter 10 Respiration Introduction/Importance of the Respiratory System All eukaryotic organisms need oxygen to perform cellular respiration (production of ATP), either aerobically or anaerobically.
1 Chapter 10 Respiration Introduction/Importance of the Respiratory System All eukaryotic organisms need oxygen to perform cellular respiration (production of ATP), either aerobically or anaerobically.
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Chapter 16. Objectives. Objectives. Respiratory Emergencies
 Chapter 16 Respiratory Emergencies Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key
Chapter 16 Respiratory Emergencies Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key
Chapter 13. Respiratory Emergencies
 Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
Chapter 15 - Respiratory Emergencies
 1 2 3 4 5 6 7 National EMS Education Standard Competencies (1 of 5) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
1 2 3 4 5 6 7 National EMS Education Standard Competencies (1 of 5) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
Airway Management From Brady s First Responder (8th Edition) 82 Questions
 Airway Management From Brady s First Responder (8th Edition) 82 Questions 1. What color will cyanotic skin be? p. 119 *A.) Blue B.) Red C.) Yellow D.) Green 2. Which is the primary path for air to enter
Airway Management From Brady s First Responder (8th Edition) 82 Questions 1. What color will cyanotic skin be? p. 119 *A.) Blue B.) Red C.) Yellow D.) Green 2. Which is the primary path for air to enter
Appendix (i) The ABCDE approach to the sick patient
 Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Chapter 19 - Respiratory_Emergencies
 Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Respiratory System Anatomy Respiratory system: all the structures that contribute to
 1 2 3 4 5 6 7 8 Chapter 15 Respiratory Emergencies Respiratory Distress Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine.
1 2 3 4 5 6 7 8 Chapter 15 Respiratory Emergencies Respiratory Distress Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine.
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
Tuesday, December 13, 16. Respiratory System
 Respiratory System Trivia Time... What is the fastest sneeze speed? What is the surface area of the lungs? (hint... think of how large the small intestine was) How many breaths does the average person
Respiratory System Trivia Time... What is the fastest sneeze speed? What is the surface area of the lungs? (hint... think of how large the small intestine was) How many breaths does the average person
QI. Read the following questions and choose the most correct answer (20 Marks):
 Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
Chapter 10. The Respiratory System Exchange of Gases. Copyright 2009 Pearson Education, Inc.
 Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery. By: Lillian Han
 Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
About the Respiratory System. Respiratory System. Human Respiratory System. Cellular Respiration. Nostrils. Label diagram
 Respiratory System Human Respiratory System A system to deliver oxygen (O2) to body cells & get rid of carbon dioxide (CO2) as a waste through cellular respiration. Two systems involved: Respiratory &
Respiratory System Human Respiratory System A system to deliver oxygen (O2) to body cells & get rid of carbon dioxide (CO2) as a waste through cellular respiration. Two systems involved: Respiratory &
Respiratory System. Introduction. Atmosphere. Some Properties of Gases. Human Respiratory System. Introduction
 Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 5 Respiratory Disorders. TEXT ASSIGNMENT Paragraphs 5-1 through 5-17. LESSON OBJECTIVES After completing this lesson, you should be able to: 5-1. Identify the characteristics,
LESSON ASSIGNMENT LESSON 5 Respiratory Disorders. TEXT ASSIGNMENT Paragraphs 5-1 through 5-17. LESSON OBJECTIVES After completing this lesson, you should be able to: 5-1. Identify the characteristics,
HASPI Medical Anatomy & Physiology 14b Lab Activity
 HASPI Medical Anatomy & Physiology 14b Lab Activity Name(s): Period: Date: Respiratory Distress Respiratory distress is a broad medical term that applies to any type of breathing difficulty and the associated
HASPI Medical Anatomy & Physiology 14b Lab Activity Name(s): Period: Date: Respiratory Distress Respiratory distress is a broad medical term that applies to any type of breathing difficulty and the associated
Lesson 4-3: Cardiac Emergencies. CARDIAC EMERGENCIES Angina, AMI, CHF and AED
 Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
LUNGS. Requirements of a Respiratory System
 Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
CARDIOVASCULAR AND RESPIRATORY SYSTEMS
 CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
3. Identify the importance in the prehospital setting for the administration of nebulized bronchodilator.
 TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
Chapter 2: Human Body Systems Work Independently and Together
 Chapter 2: Human Body Systems Work Independently and Together 2.1 Body Systems Body systems Are made up of parts that work together as a whole Are connected to one or more other Will not function well
Chapter 2: Human Body Systems Work Independently and Together 2.1 Body Systems Body systems Are made up of parts that work together as a whole Are connected to one or more other Will not function well
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
Anatomy & Physiology 2 Canale. Respiratory System: Exchange of Gases
 Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Why do you breathe? What is oxygen used for? Where does CO2 come from?
 RESPIRATORY SYSTEM How You Breathe Why do you breathe? What is oxygen used for? Where does CO2 come from? Respiration: exchange of gases between air & your body cells 1. Outside air (O2) lungs metabolism
RESPIRATORY SYSTEM How You Breathe Why do you breathe? What is oxygen used for? Where does CO2 come from? Respiration: exchange of gases between air & your body cells 1. Outside air (O2) lungs metabolism
Prior to applying a nonrebreathing mask on a patient with difficulty breathing, you should:!
 An elderly woman with COPD presents with a decreased level of consciousness, cyanosis to her face and neck, and labored respirations. Her pulse is rapid and weak and her oxygen saturation is 76%. You should:
An elderly woman with COPD presents with a decreased level of consciousness, cyanosis to her face and neck, and labored respirations. Her pulse is rapid and weak and her oxygen saturation is 76%. You should:
Respiratory system. Applied Anatomy &Physiology
 Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
CPAP. Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device. Charlottesville Albemarle Rescue Squad - CPAP
 CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Unit 4 Circulatory, Respiratory and Excretory System
 Unit 4 Circulatory, Respiratory and Excretory System Test Date Project Due Lesson 1 The Cardiovascular System Homework: read pages 176-179 and take notes Warm up 1. 2. 3. 4. Finding Target Heart rate (220
Unit 4 Circulatory, Respiratory and Excretory System Test Date Project Due Lesson 1 The Cardiovascular System Homework: read pages 176-179 and take notes Warm up 1. 2. 3. 4. Finding Target Heart rate (220
Phases of Respiration. Chapter 18: The Respiratory System. Structures of the Respiratory System. Structures of the Respiratory System
 Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Chapter 10. Respiratory System and Gas Exchange. Copyright 2005 Pearson Education, Inc. publishing as Benjamin Cummings
 Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
BLS Guideline 1 AIRWAY MANAGEMENT
 Australian Resuscitation Advisory Network BLS Guideline 1 AIRWAY MANAGEMENT Scope Who does this guideline apply to? This guideline applies to all persons who need airway management. Airway management is
Australian Resuscitation Advisory Network BLS Guideline 1 AIRWAY MANAGEMENT Scope Who does this guideline apply to? This guideline applies to all persons who need airway management. Airway management is
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Airway management. Dr. Dóra Ujvárosy Medical Unversity of Debrecen Emergency Department
 Airway management Dr. Dóra Ujvárosy Medical Unversity of Debrecen Emergency Department Airway management Airway management is the medical process of ensuring there is an open pathway between a patient
Airway management Dr. Dóra Ujvárosy Medical Unversity of Debrecen Emergency Department Airway management Airway management is the medical process of ensuring there is an open pathway between a patient
The Respiratory System
 The Respiratory System By Mr. Danilo Villar Rogayan Jr. Instructor I, Department of Natural Sciences RMTU San Marcelino Introduction Function Move air in an out of lungs (ventilation) Delivers oxygen (O
The Respiratory System By Mr. Danilo Villar Rogayan Jr. Instructor I, Department of Natural Sciences RMTU San Marcelino Introduction Function Move air in an out of lungs (ventilation) Delivers oxygen (O
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Unit 14: The Respiratory System
 Unit 14: The Respiratory System See what you already know! 1. Fill in the diagram on your own 2. Collaborate with your partner The Respiratory System The major function of the respiratory system is gas
Unit 14: The Respiratory System See what you already know! 1. Fill in the diagram on your own 2. Collaborate with your partner The Respiratory System The major function of the respiratory system is gas
d) Always ensure patient comfort. Be considerate and warm the diaphragm of your stethoscope with your hand before auscultation.
 Auscultation Auscultation is perhaps the most important and effective clinical technique you will ever learn for evaluating a patient s respiratory function. Before you begin, there are certain things
Auscultation Auscultation is perhaps the most important and effective clinical technique you will ever learn for evaluating a patient s respiratory function. Before you begin, there are certain things
Chapter 29 - Chest_and_Abdominal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
Function: to supply blood with, and to rid the body of
 1 2 3 4 5 Bio 1102 Lec. 7 (guided): Chapter 10 The Respiratory System Respiratory System Function: to supply blood with, and to rid the body of Oxygen: needed by cells to break down food in cellular respiration
1 2 3 4 5 Bio 1102 Lec. 7 (guided): Chapter 10 The Respiratory System Respiratory System Function: to supply blood with, and to rid the body of Oxygen: needed by cells to break down food in cellular respiration
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Cardiovascular Emergencies. Chapter 12
 Cardiovascular Emergencies Chapter 12 Cardiovascular Emergencies Cardiovascular disease (CVD) claimed 931,108 lives in the US during 2001. 2,551 per day Almost two people per minute! CVD accounts for 38.5%
Cardiovascular Emergencies Chapter 12 Cardiovascular Emergencies Cardiovascular disease (CVD) claimed 931,108 lives in the US during 2001. 2,551 per day Almost two people per minute! CVD accounts for 38.5%
The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body.
 Respiratory System The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body. The respiratory system does this
Respiratory System The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body. The respiratory system does this
5/5/2013. The Respiratory System. Chapter 16 Notes. The Respiratory System. Nasal Cavity. Sinuses
 The Respiratory System Chapter 16 Notes The Respiratory System Objectives List the general functions of the respiratory system. Identify the organs of the respiratory system. Describe the functions of
The Respiratory System Chapter 16 Notes The Respiratory System Objectives List the general functions of the respiratory system. Identify the organs of the respiratory system. Describe the functions of
10.1 The Pulmonary-Circulatory System
 pulmonary system breathing lungs pneumonia suffocation asthma circulatory system atrium ventricle artery capillary vein heart attack stroke heart The Pulmonary System Our pulmonary system contains tissues
pulmonary system breathing lungs pneumonia suffocation asthma circulatory system atrium ventricle artery capillary vein heart attack stroke heart The Pulmonary System Our pulmonary system contains tissues
Phases of Respiration
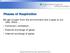 Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
Can be felt where an artery passes near the skin surface and over a
 1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
STS: Circulatory/Pulmonary
 STS: Circulatory/Pulmonary September 27, 2017 You have a 50 y/o male who is complaining of excruciating pain in his chest. You find him sitting down on a bench, arms in a tripod position, breathing heavily.
STS: Circulatory/Pulmonary September 27, 2017 You have a 50 y/o male who is complaining of excruciating pain in his chest. You find him sitting down on a bench, arms in a tripod position, breathing heavily.
ADVANCED ASSESSMENT Respiratory System
 ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
Cardiac Emergencies. A Review of Cardiac Compromise. Lawrence L. Lambert
 Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
Foundation in Critical Care Nursing. Airway / Respiratory / Workbook
 Foundation in Critical Care Nursing Airway / Respiratory / Workbook Airway Anatomy: Please label the following: Tongue Larynx Epiglottis Pharynx Trachea Vertebrae Oesophagus Where is the ET (endotracheal)
Foundation in Critical Care Nursing Airway / Respiratory / Workbook Airway Anatomy: Please label the following: Tongue Larynx Epiglottis Pharynx Trachea Vertebrae Oesophagus Where is the ET (endotracheal)
Circulatory System. and. Respiratory System. Ari Min, Yerim Lee and Min Ji Song THE HEART LUNGS. Monday, May 23, 2011
 Human Anatomy Circulatory System and THE HEART Respiratory System LUNGS Ari Min, Yerim Lee and Min Ji Song Purpose of the Circulatory System Function of circulatory system: exchange gases with cardiovascular
Human Anatomy Circulatory System and THE HEART Respiratory System LUNGS Ari Min, Yerim Lee and Min Ji Song Purpose of the Circulatory System Function of circulatory system: exchange gases with cardiovascular
The Circulatory System
 The Circulatory System Single-celled organisms do not need a circulatory system. They are in direct contact with their environment, so transport of materials occurs by diffusion and osmosis. Larger organisms
The Circulatory System Single-celled organisms do not need a circulatory system. They are in direct contact with their environment, so transport of materials occurs by diffusion and osmosis. Larger organisms
B Unit III Notes 6, 7 and 8
 The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Respiratory System. Chapter 9
 Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Respiratory Distress/Failure - General
 Respiratory Distress/Failure - General Criteria: Dyspnea WITHOUT a clear etiology O 2 V/S and SpO 2 (with and without Oxygen therapy if possible) Blood glucose analysis: if less than 80 mg/dl, refer to
Respiratory Distress/Failure - General Criteria: Dyspnea WITHOUT a clear etiology O 2 V/S and SpO 2 (with and without Oxygen therapy if possible) Blood glucose analysis: if less than 80 mg/dl, refer to
Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since.
 1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
The Respiratory System Structures of the Respiratory System Structures of the Respiratory System Structures of the Respiratory System Nose Sinuses
 CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Pediatric Patients. BCFPD Paramedic Education Program. EMS Education Paramedic Level
 Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Respiratory System. Organization of the Respiratory System
 Respiratory System In addition to the provision of oxygen and elimination of carbon dioxide, the respiratory system serves other functions, as listed in (Table 15 1). Respiration has two quite different
Respiratory System In addition to the provision of oxygen and elimination of carbon dioxide, the respiratory system serves other functions, as listed in (Table 15 1). Respiration has two quite different
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing
 Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Chapter 11. Learning Objectives. Learning Objectives 9/18/2012. Respiratory Emergencies
 Chapter 11 Respiratory Learning Objectives List structures & functions of the respiratory system State signs/symptoms of patient with breathing difficulty Describe emergency medical care of patient with
Chapter 11 Respiratory Learning Objectives List structures & functions of the respiratory system State signs/symptoms of patient with breathing difficulty Describe emergency medical care of patient with
The Respiratory System. Dr. Ali Ebneshahidi
 The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
FIRST AID WRITTEN EXAM. Team Name: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. a. TRUE b. FALSE
 2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
Core Subject Part 4. Identify the principles of approaching the sick patient.
 The Role of The Dental Care Professional During a Medical Emergency: General Dental Council Standards and The Management of The Collapsed Patient Using the ABCDE Approach Aims: Core Subject Part 4 To provide
The Role of The Dental Care Professional During a Medical Emergency: General Dental Council Standards and The Management of The Collapsed Patient Using the ABCDE Approach Aims: Core Subject Part 4 To provide
This activity should be used to motivate students to learn about the significance and concerns associated with patients in respiratory emergencies.
 Pre-Lecture I. You Are the Provider Time: 10 Minutes Small Group Activity/Discussion The You are the Provider case study is discussed within the PowerPoint presentation for this chapter. The instructor
Pre-Lecture I. You Are the Provider Time: 10 Minutes Small Group Activity/Discussion The You are the Provider case study is discussed within the PowerPoint presentation for this chapter. The instructor
MEDICAL KIT - ALGORITHMS
 MEDICAL KIT - ALGORITHMS Page 2 : BRONCHOSPASM / ASTHMA Page 3 : TENSION PNEUMOTHORAX Page 4 : Page 5 : Page 6 : CONGESTIVE HEART FAILURE/ PULMONARY EDEMA ANAPHYLACTIC SHOCK / ALLERGIC REACTION ANGINA
MEDICAL KIT - ALGORITHMS Page 2 : BRONCHOSPASM / ASTHMA Page 3 : TENSION PNEUMOTHORAX Page 4 : Page 5 : Page 6 : CONGESTIVE HEART FAILURE/ PULMONARY EDEMA ANAPHYLACTIC SHOCK / ALLERGIC REACTION ANGINA
Anatomy and Physiology
 Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Oxygenation. Chapter 45. Re'eda Almashagba 1
 Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
