Subject: Pneumonia in Children Section: Pediatrics Hours: 4 hours. Individual preparation for classes: 2 hours.
|
|
|
- Felix Curtis
- 5 years ago
- Views:
Transcription
1 Subject: Pneumonia in Children Section: Pediatrics Hours: 4 hours. Individual preparation for classes: 2 hours. 1. ACTUALITY Pneumonia in children - nonspecific pneumonia based on the infectious toxicosis, respiratory failure, fluid and electrolyte and other metabolic disorders with abnormal changes in all organs and systems of a child's body. Despite the great advances in diagnosis and treatment of respiratory diseases, the condition at the beginning of. Continues grow. Extremely important are pneumonia, which is often noted in the therapeutic practice. Thanks conducted randomized controlled trial (RCT) is review the effectiveness of antibiotic therapy for pneumonia. Every year there improvement of methods and tactics for treatment of pneumonia. 2. THE AIM Learn how to identify the etiologic factors and pathogenic mechanisms of pneumonia children, classify and analyze the typical clinical presentation, diagnose and clinical diagnosis and prescribe appropriate treatment, to forecast and provide preventive recommendations for this disease. 3. EDUCATIONAL OBJECTIVES The student should know: - Pneumonia etiological structure according to age and children pathogenetic factors; - Classification of pneumonia in children; - Clinical signs of respiratory distress in children; - Diagnosis of pneumonia in children, the use of laboratory and instrumental research methods; - The treatment of pneumonia in children; - Prevention and prognosis of pneumonia in children; - Complications of pneumonia in children; - Diagnosis and emergency care for acute respiratory failure in children. The student should be able to: - Collect medical history and physical examination of the patient; - Evaluate the results of paraclinical investigations; - To put and to formulate a diagnosis according to modern classification; - Evaluate the results of X-ray; - Assigned treatment regimen, taking into account the patient's age; - Prescription; - Develop creativity in the laboratory, clinical examination of the child, - Theoretical research on problems of the subject; - Demonstrate the moral and ethical principles of medical specialist and principles of professional subordination;
2 4. INTEGRATION Anatomy Biochemiostry Patholopgic Anatomy Pathoilogic Physiology Microbiology Propedevtics Therapy Radiology Intensive care Anatomical and physiological features of the respiratory system children of different age groups biochemical parameters blood tests. The main pathological changes the respiratory system in children. Mechanisms of inflammation process The methods of sampling and seeding sputum, blood, pleural exudate. Determine microbiological spectrum infectious factors respiratory diseases. Methodology and research semiotics of diseases respiratory system. Methodology of spirometric research. Clinical and medical history laboratory and instrumental complex signs of pneumonia Indications and methods of radiation diagnosis of diseases respiratory tract Signs of respiratory failure varying degrees, causes it development and principles first aid Use knowledge to adequately assess clinical parameters Rate biochemical blood tests Know the stages and dates inflammatory changes for timely and adequate therapy Identify signs of frustration Rate microbiological research To conduct an objective review patient (inspection, palpation, percussion, auscultation) evaluate the results spirometry Identify features pneumonia, forecast further complications Rate radiographs Identify respiratory failure to assess ii the extent to emergency help
3 5. MATERIALS Acute pneumonia - an acute inflammatory disease of the lungs characterized infiltrative changes in lung tissue and respiratory failure. Acute pneumonia is an acute non-specific inflammation of lung tissue, based which is infectious toxicosis, respiratory failure, fluid and electrolyte and other metabolic disorders with abnormal shifts in all organs and systems of children body. According to other views, in pneumonia should be understood as a group of different etiology, pathogenesis and morphological characterization of focal acute infectious and inflammatory lung disease with the obligatory presence of inflammatory vnutrishnoalveolyarnoyi exudation. Over the etiology of acute pneumonia may be bacterial, viral (MS-virus, flu etc.), viral, bacterial, fungal and caused by intracellular pathogens atypical pneumonia (mycoplasma, chlamydia, herpes, cytomegalovirus), protozoa agents. Classification: 1. By location acquired o 1.1 Community-acquired o 1.2 Hospital-acquired 2. By cause o 2.1 Bronchiolitis obliterans organizing pneumonia o 2.2 Chemical pneumonia o 2.3 Aspiration pneumonia o 2.4 Dust pneumonia o 2.5 Necrotizing pneumonia o 2.6 Opportunistic pneumonia o 2.7 Double pneumonia (bilateral pneumonia) o 2.8 Severe acute respiratory syndrome 3. By area of lung affected 4. Clinical Severity - I, II, III, IV, V degree. I level - <50 points, the risk of mortality - 0.1, outpatient treatment; II level points, the risk of mortality - 0.6, outpatient treatment; III level points, the risk of mortality - 2.8, hospitalization; IV degree points, the risk of mortality - 8.2, hospitalization; V level -> 130 points, the risk of mortality , hospitalization; Scores are calculated by the index of severity: Age: <6 months - (25); > 6 months -3 years - (15); 3-15 years - (10). Concomitant diseases: - Congenital heart defects - (+30); - Wasting - (+10); - Immunodeficiency condition - (+10); - Violation of consciousness - (+20); - Shortness of breath - (+20); - Cyanosis - (+15);
4 - Pain in the chest - (+20); - Toxic Encephalopathy - (+30); - Body temperature less than 39 or 36 - (15). Laboratory features: - Leukocytosis - (+20); - Leukopenia - (+10); - Anaemia - (+10); - PH <7,35 - (+30); - BUN> 11 mg / dl - (+20); - Hct <30% - (10); - SaO2 <90% - (20); - Equipment - (20); - Multylobarna infiltration on X-ray - (+15); - Infectious shock -toksychnyy - (40); - Pleural fluid - (+30); - Destruction - (+50). Etiology A specific aetiological agent cannot be identified in 40% to 60% of cases6,7. Viral pneumonia cannot be distinguished from bacterial pneumonia based on a combination of clinical findings. The majority of lower respiratory tract infections that present for medical attention in young children are viral in origin such as respiratory syncytial virus, influenza, adenovirus and parainfluenza virus. Pathogens causing pneumonia Newborns: Group B streptococcus, Escherichia coli, Klebsiella species, Enterobacteriaceae. 1-3 months: Chlamydia trachomatis. Preschool: Streptococcus pneumoniae, Haemophilus influenzae type b, Staphylococcal aureus, Less common: group A streptococcus, Moraxella catarrhalis, Pseudomonas aeruginosa. School: Mycoplasma pneumoniae, Chlamydia pneumoniae. Pathogenesis Pneumonia is characterized by inflammation of the alveoli and terminal airspaces in response to invasion by an infectious agent introduced into the lungs through hematogenous spread or inhalation. The inflammatory cascade triggers the leakage of plasma and the loss of surfactant, resulting in air loss and consolidation. The activated inflammatory response often results in targeted migration of phagocytes, with the release of toxic substances from granules and other microbicidal packages and the initiation of poorly regulated cascades (eg, complement, coagulation, cytokines). These cascades may directly injure host tissues and adversely alter endothelial and epithelial integrity, vasomotor tone, intravascular hemostasis, and the activation state of fixed and migratory phagocytes at the inflammatory focus. The role of apoptosis (noninflammatory programmed cell death) in pneumonia is poorly understood. Pulmonary injuries are caused directly and/or indirectly by invading microorganisms or foreign material and by poorly targeted or inappropriate responses by the host
5 defense system that may damage healthy host tissues as badly as or worse than the invading agent. Direct injury by the invading agent usually results from synthesis and secretion of microbial enzymes, proteins, toxic lipids, and toxins that disrupt host cell membranes, metabolic machinery, and the extracellular matrix that usually inhibits microbial migration. Indirect injury is mediated by structural or secreted molecules, such as endotoxin, leukocidin, and toxic shock syndrome toxin-1 (TSST-1), which may alter local vasomotor tone and integrity, change the characteristics of the tissue perfusate, and generally interfere with the delivery of oxygen and nutrients and removal of waste products from local tissues. On a macroscopic level, the invading agents and the host defenses both tend to increase airway smooth muscle tone and resistance, mucus secretion, and the presence of inflammatory cells and debris in these secretions. These materials may further increase airway resistance and obstruct the airways, partially or totally, causing airtrapping, atelectasis, and ventilatory dead space. In addition, disruption of endothelial and alveolar epithelial integrity may allow surfactant to be inactivated by proteinaceous exudate, a process that may be exacerbated further by the direct effects of meconium or pathogenic microorganisms. In the end, conducting airways offer much more resistance and may become obstructed, alveoli may be atelectatic or hyperexpanded, alveolar perfusion may be markedly altered, and multiple tissues and cell populations in the lung and elsewhere sustain injury that increases the basal requirements for oxygen uptake and excretory gas removal at a time when the lungs are less able to accomplish these tasks. Alveolar diffusion barriers may increase, intrapulmonary shunts may worsen, and ventilation/perfusion (V/Q) mismatch may further impair gas exchange despite endogenous homeostatic attempts to improve matching by regional airway and vascular constriction or dilatation. Because the myocardium has to work harder to overcome the alterations in pulmonary vascular resistance that accompany the above changes of pneumonia, the lungs may be less able to add oxygen and remove carbon dioxide from mixed venous blood for delivery to end organs. The spread of infection or inflammatory response, either systemically or to other focal sites, further exacerbates the situation. Viral infections are characterized by the accumulation of mononuclear cells in the submucosa and perivascular space, resulting in partial obstruction of the airway. Patients with these infections present with wheezing and crackles. Disease progresses when the alveolar type II cells lose their structural integrity and surfactant production is diminished, a hyaline membrane forms, and pulmonary edema develops. In bacterial infections, the alveoli fill with proteinaceous fluid, which triggers a brisk influx of red blood cells (RBCs) and polymorphonuclear (PMN) cells (red hepatization) followed by the deposition of fibrin and the degradation of inflammatory cells (gray hepatization). During resolution, intra-alveolar debris is ingested and removed by the alveolar macrophages. This consolidation leads to decreased air entry and dullness to percussion; inflammation in the small airways leads to crackles. Four stages of lobar pneumonia have been described. In the first stage, which occurs within 24 hours of infection, the lung is characterized microscopically by vascular congestion and alveolar edema. Many bacteria and few neutrophils are present. The
6 stage of red hepatization (2-3 d), so called because of its similarity to the consistency of liver, is characterized by the presence of many erythrocytes, neutrophils, desquamated epithelial cells, and fibrin within the alveoli. In the stage of gray hepatization (2-3 d), the lung is gray-brown to yellow because of fibrinopurulent exudate, disintegration of RBCs, and hemosiderin. The final stage of resolution is characterized by resorption and restoration of the pulmonary architecture. Fibrinous inflammation may lead to resolution or to organization and pleural adhesions. Bronchopneumonia, a patchy consolidation involving one or more lobes, usually involves the dependent lung zones, a pattern attributable to aspiration of oropharyngeal contents. The neutrophilic exudate is centered in bronchi and bronchioles, with centrifugal spread to the adjacent alveoli. In interstitial pneumonia, patchy or diffuse inflammation involving the interstitium is characterized by infiltration of lymphocytes and macrophages. The alveoli do not contain a significant exudate, but protein-rich hyaline membranes similar to those found in adult respiratory distress syndrome (ARDS) may line the alveolar spaces. Bacterial superinfection of viral pneumonia can also produce a mixed pattern of interstitial and alveolar airspace inflammation. Miliary pneumonia is a term applied to multiple, discrete lesions resulting from the spread of the pathogen to the lungs via the bloodstream. The varying degrees of immunocompromise in miliary tuberculosis (TB), histoplasmosis, and coccidioidomycosis may manifest as granulomas with caseous necrosis to foci of necrosis. Miliary herpesvirus, cytomegalovirus (CMV), or varicella-zoster virus infection in severely immunocompromised patients results in numerous acute necrotizing hemorrhagic lesions. Clinical features The clinical diagnosis of pneumonia has traditionally been made using auscultatory findings such as bronchial breath sounds and crepitations in children with cough. However, the sensitivity of auscultation has been shown to be poor and varies between 33 %- 60% with an average of 50 % in children. Tachypnoea is the best single predictor in children of all ages.10 Measurement of tachypnoea is better compared with observations of retractions or auscultatory findings. It is nonetheless important to measure respiratory rate accurately. Respiratory rate should be counted by inspection for 60 seconds. However in the young infants, pneumonia may present with irregular breathing and hypopnea. Investigations Children with bacterial pneumonia cannot be reliably distinguished from those with viral disease on the basis of any single parameter; clinical, laboratory or chest radiograph findings. 1. Chest radiograph Chest radiograph is indicated when clinical criteria suggests pneumonia. It will not identify the aetiological agent. However the chest radiograph is not always necessary if facilities are not available or the pneumonia is mild. 2. Complete white blood cell and differential count This test may be helpful as an increased white blood count with predominance of
7 polymorphonuclear cells may suggest bacterial cause. However, leucopenia can either suggest a viral cause or severe overwhelming infection. 3. Blood culture Blood culture remains the non-invasive gold standard for determining the precise aetiology of pneumonia. However the sensitivity of this test is very low. Positive blood cultures are found only in 10% to 30% of patients with pneumonia15. Even in 44% of patients with radiographic findings consistent with pneumonia, only 2.7% were positive for pathogenic bacteria.16 Blood culture should be performed in severe pneumonia or when there is poor response to the first line antibiotics. 4. Culture from respiratory secretions It should be noted that bacteria isolates from throat swabs and upper respiratory tract secretions are not representative of pathogens present in the lower respiratory tract. Samples from the nasopharynx and throat have no predictive values. This investigation should not be routinely done. 5. Other tests Bronchoalveolar lavage is usually necessary for the diagnosis of Pneumocystis carini infections primarily in immunosuppressed children. It is only to be done when facilities and expertise are available. If there is significant pleural effusion diagnostic, pleural tap will be helpful. Mycoplasma pneumoniae, Chlamydia, Legio nella and Moxarella catarrhalis are difficult organisms to culture, and thus serological studies should be performed in children with suspected atypical pneumonia. An acute phase serum titre of more than 1:160 or paired samples taken 2-4 weeks apart showing four fold rise is a good indicator of Mycoplasma pneumoniae infection. This test should be considered for children aged five years or older with pneumonia. Management I Assessment of severity of pneumonia II Assessment of oxygenation The best objective measurement of hypoxia is by pulse oximetry which avoids the need for arterial blood gases. It is a good indicator of the severity of pneumonia III Criteria for hospitalization Community acquired pneumonia can be treated at home. It is crucial to identify indicators of severity in children who may need admission as failure to do so may result in death. The following indicators can be used as a guide for admission. IV Antibiotic therapy When treating pneumonia clinical, laboratory and radiographic findings should be considered. The age of the child, local epidemiology of respiratory pathogens and sensitivity of these pathogens to particular microbial agents and the emergence of antimicrobial resistance also determine the choice of antibiotic therapy. The severity of the pneumonia and drug costs have also a great impact on the selection of therapy. The majority of childhood infections are caused by viruses and do not require any antibiotic. However, it is also very important to remember that we should be vigilant to choose appropriate antibiotics especially in the initial treatment to reduce further mortality and morbidity. For inpatient management of children with severe pneumonia, the following antibiotic therapy is recommended.
8 1st line drugs: lactams drugs: Benzlypenicillin, Amoxycillin, Ampicillin, Amoxycillin-Clavulanate 2nd line: Cephalosporins : Cefotaxime, Cefuroxime, Ceftazidime, 3rd line: Carbapenem: Imepenam Others Aminoglycosides: Gentamicin, Amikacin If there are no signs of recovery; especially if the patient remains toxic and ill with spiking temperature for hours, a 2nd of 3rd line antibiotic therapy need to be considered. If Mycoplasma or Chlamydia species are the causative agents, a macrolideis the appropriate choice. A child admitted to hospital with severe community acquired pneumonia must receivenparenteral antibiotics. As a rule, in severe cases of pneumonia, combination therapy using a second or third generation cephalasporins and macrolide should be given. Staphylococcal infections and infection caused by Gram negative organisms such as Klebsiella sp are more frequently reported in malnourished children. 8. Respiratory failure Classification of respiratory failure: respiratory failur-1 degree - shortness of breath occurs during usual physical activity; respiratory failur-2 degree -weezing with little physical exertion; respiratory failure-3 level - a significant dyspnea in rest. Acute respiratory failure with pneumonia refers to the diffusion-restrictive type respiratory failure. Classification NAM for young children 1st degree - shortness of breath, tachycardia during exercise (physical Baby load - breastfeeding, scream, excitement) partial pressure of oxygen arterial blood mm Hg. 2nd degree - shortness of breath, tachycardia alone, much of the gain in physical load. Slight cyanosis of the lips, akrotsianoz. Fanning wings of the nose, involvement intercostal spaces during breathing. Lifeless child irritable. The partial pressure of oxygen arterial blood mm 3rd degree - shortness of breath to breaths per minute at rest. Total cyanosis of the skin, mucous. In the act of breathing ancillary muscles involved. Can develop hypoxic encephalopathy (disturbance of consciousness, convulsions). The partial pressure of oxygen - below 50 mmhg General principles of treatment of respiratory failure. Treatment of acute respiratory failure with pneumonia combines the following actions: 1. infants and children with impaired immune status or patients in hospital pneumonia should be prescribed broad-spectrum antibiotics, ampicillin and oxacillin (Kloksatsylin) or cephalosporins. Often shown additional appointment aminoglycosides. In other cases prescribed amoxicillin or erythromycin (for suspected mycoplasma PA etiology of pneumonia). Antibiotics administered parenterally way. 2. Bed rest, nutrition patient through a tube or the PA administration 3. humidified oxygen (40%) when cyanosis, severe respiratory failure or anxiety. 4. Dilution sputum by introducing a sufficient amount of fluid humidifying inhaled air and purpose bromhexine. 5. gammaglobuline for suspected immunodeficiency in a child.
9 6. In the event of severe disease with concomitant acute respiratory failure showing endotracheal intubation and mechanical ventilation. A special place in the restrictive type of acute respiratory failure ranks a condition which can rapidly lead to adverse consequences - a syndrome intrathoracic strain (hard cyst lung pnevmomediastynum, pneumothorax) due to bacterial degradation of lung and diaphragmatic hernia. In a tense pneumothorax occur such paradoxical clinical features: 1. On the inhale lung on the affected side is not increased, but decreased in volume, due to increased intra-pleural pressure and compression of the lungs. 2. inhaling air from damaged lungs due to its compression comes in healthy lung. 3. On the exhale air from the lungs enters the healthy lung damaged, resulting in it increases in volume. The movement of air during inhalation victim with a healthy lung, and under a healthy exhalation of the lung affected is described in the literature as pendulous. 4. The shift of the mediastinum relatively healthy spine toward the lungs, which leads to reduce its surface for gas exchange. Because of the displacement of the mediastinum can happen bend large vessels, leading to cessation of circulation. Treatment involves removal of intrathoracic tension by puncture and (Or) drainage of pleural cavity. Mandatory inhalation of oxygen. Place puncture pleural cavity - the second intercostal gap along the midclavicular line with hydrothorax or hidropnevmotorax - along the middle or posterior axillary at the level of the nipple. Most authors prefer passive pleural decompression oral, citing the fact that the lungs of a child, regardless of the nature of decompression, (Passive or active) finishes for hours, meaning development Board of the normalization of lung ventilation nerfuziynoho ratio. While active thoracostomy has many disadvantages such as the need special adaptations, the relative immobilization of the child, increasing the risk of bleeding in postoperative period. 9. MATERIALS 6.1 Quiz 1. etiological and pathogenetic factors of pneumonia in children. 2. Classification of acute pneumonia in children. 3. Clinical manifestations of respiratory failure in children. 4. Differential diagnosis of pneumonia in children. 5. Clinical management of patients with different clinical variants of pneumonia. 6. Preventing pneumonia complications in her children. 7. Clinical management of patients with different clinical variants of complications of pneumonia in children. 8. Diagnosis of acute pneumonia in children, and use of laboratory instrumental methods; 9. Treatment of acute pneumonia in children. 10. The prevention and prognosis of acute pneumonia in children. 11. Complications of acute pneumonia in children. 12. Diagnostics and emergency treatment of acute respiratory failure in children.
10 6.2 MCQ 6 years old child suffers 2nd week febrilna body temperature, dry cough, there pain in the right side, shortness of breath. An objective examination, obliteration in the lower right chest; percussion - blunting pulmonary tone in the lower case; auscultation - a place blunting breath sharply weakened. Install preliminary diagnosis. A) Pneumothorax B) Bronchitis B) pulmonary atelectasis D) Pleurisy case D) lung tumors 6.3 Case The boy 3 months. there is restlessness, frequent shallow breathing, cough. Objectively: t body - 38,40S, cyanosis nasolabial triangle involving shallow breathing ancillary muscles, BH-60 for 1 min., over lungs- moist rales, heart rate for 1 min., Heart sounds are muffled. Blood: white blood cells g / l; ESR, 22 mm / h. X-ray of the lungs, both lungs focal shadow on the background of intensified bronchopulmonary picture, roots are infiltrated. 1. State the previous diagnosis 2. Plan survey 3. Treatment
Pathology of Pneumonia
 Pathology of Pneumonia Dr. Atif Ali Bashir Assistant Professor of Pathology College of Medicine Majma ah University Introduction: 5000 sq meters of area.! (olympic track) Filters >10,000 L of air / day!
Pathology of Pneumonia Dr. Atif Ali Bashir Assistant Professor of Pathology College of Medicine Majma ah University Introduction: 5000 sq meters of area.! (olympic track) Filters >10,000 L of air / day!
Unit II Problem 2 Pathology: Pneumonia
 Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Acute pneumonia Simple complement
 Acute pneumonia Simple complement 1. Clinical variants of acute pneumonia in children are, except: A. Bronchopneumonia B. Lobar confluent pneumonia C. Viral pneumonia D. Interstitial pneumonia E. Chronic
Acute pneumonia Simple complement 1. Clinical variants of acute pneumonia in children are, except: A. Bronchopneumonia B. Lobar confluent pneumonia C. Viral pneumonia D. Interstitial pneumonia E. Chronic
PNEUMONIA IN CHILDREN. IAP UG Teaching slides
 PNEUMONIA IN CHILDREN 1 INTRODUCTION 156 million new episodes / yr. worldwide 151 million episodes developing world 95% in developing countries 19% of all deaths in children
PNEUMONIA IN CHILDREN 1 INTRODUCTION 156 million new episodes / yr. worldwide 151 million episodes developing world 95% in developing countries 19% of all deaths in children
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2
 Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Key Difference - Pleural Effusion vs Pneumonia
 Difference Between Pleural Effusion and Pneumonia www.differencebetween.com Key Difference - Pleural Effusion vs Pneumonia Pleural effusion and pneumonia are two conditions that affect our respiratory
Difference Between Pleural Effusion and Pneumonia www.differencebetween.com Key Difference - Pleural Effusion vs Pneumonia Pleural effusion and pneumonia are two conditions that affect our respiratory
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I. December 5, 2012
 SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
Chapter 10 Respiratory System J00-J99. Presented by: Jesicca Andrews
 Chapter 10 Respiratory System J00-J99 Presented by: Jesicca Andrews 1 Respiratory System 2 Respiratory Infections A respiratory infection cannot be assumed from a laboratory report alone; physician concurrence
Chapter 10 Respiratory System J00-J99 Presented by: Jesicca Andrews 1 Respiratory System 2 Respiratory Infections A respiratory infection cannot be assumed from a laboratory report alone; physician concurrence
Chapter 22. Pulmonary Infections
 Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
PULMONARY EMERGENCIES
 EMERGENCIES I. Pneumonia A. Bacterial Pneumonia (most common cause of a focal infiltrate) 1. Epidemiology a. Accounts for up to 10% of hospital admissions in the U.S. b. Most pneumonias are the result
EMERGENCIES I. Pneumonia A. Bacterial Pneumonia (most common cause of a focal infiltrate) 1. Epidemiology a. Accounts for up to 10% of hospital admissions in the U.S. b. Most pneumonias are the result
Respiratory Pathology. Kristine Krafts, M.D.
 Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
Bacterial pneumonia with associated pleural empyema pleural effusion
 EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Community Acquired Pneumonia. Abdullah Alharbi, MD, FCCP
 Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
PNEUMONIA. I. Background 6 th most common cause of death in U.S. Most common cause of infection related mortality
 Page 1 of 8 September 4, 2001 Donald P. Levine, M.D. University Health Center Suite 5C Office: 577-0348 dlevine@intmed.wayne.edu Assigned reading: pages 153-160; 553-563 PNEUMONIA the most widespread and
Page 1 of 8 September 4, 2001 Donald P. Levine, M.D. University Health Center Suite 5C Office: 577-0348 dlevine@intmed.wayne.edu Assigned reading: pages 153-160; 553-563 PNEUMONIA the most widespread and
ACUTE COMMUNITY-ACQUIRED PNEUMONIA Simple choice test (CS)
 Cs Cs Cs Cs Cs ACUTE COMMUNITY-ACQUIRED PNEUMONIA Simple choice test () 1. Choose the statement that is not included in the list of clinical and morphological variants of community-acquired pneumonia in
Cs Cs Cs Cs Cs ACUTE COMMUNITY-ACQUIRED PNEUMONIA Simple choice test () 1. Choose the statement that is not included in the list of clinical and morphological variants of community-acquired pneumonia in
The Respiratory System
 The Respiratory System Respiratory Anatomy Upper respiratory tract Nose Nasal passages Pharynx Larynx Respiratory Anatomy Functions of the upper respiratory tract: Provide entry for inhaled air Respiratory
The Respiratory System Respiratory Anatomy Upper respiratory tract Nose Nasal passages Pharynx Larynx Respiratory Anatomy Functions of the upper respiratory tract: Provide entry for inhaled air Respiratory
Pneumonia, Pleurisy, Lung cancer
 Pneumonia, Pleurisy, Lung cancer Pneumonia is an infection of lung parenchyma, which leads to inflammation and exudates filling air spaces with fluid (consolidation). This leads to reduced lung compliance
Pneumonia, Pleurisy, Lung cancer Pneumonia is an infection of lung parenchyma, which leads to inflammation and exudates filling air spaces with fluid (consolidation). This leads to reduced lung compliance
Pneumonia. Dr. Rami M Adil Al-Hayali Assistant professor in medicine
 Pneumonia Dr. Rami M Adil Al-Hayali Assistant professor in medicine Definition Pneumonia is an acute respiratory illness caused by an infection of the lung parenchyma, associated with recently developed
Pneumonia Dr. Rami M Adil Al-Hayali Assistant professor in medicine Definition Pneumonia is an acute respiratory illness caused by an infection of the lung parenchyma, associated with recently developed
Appendix E1. Epidemiology
 Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
Critical Care Nursing Theory. Pneumonia. - Pneumonia is an acute infection of the pulmonary parenchyma
 - is an acute infection of the pulmonary parenchyma - is a common infection encountered by critical care nurses when it complicates the course of a serious illness or leads to acute respiratory distress.
- is an acute infection of the pulmonary parenchyma - is a common infection encountered by critical care nurses when it complicates the course of a serious illness or leads to acute respiratory distress.
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
PBL RESPIRATORY SYSTEM DR. NATHEER OBAIDAT
 PBL RESPIRATORY SYSTEM DR. NATHEER OBAIDAT Dr started to talk about his specialty at the hospital which is (ICU-Pulmonary-Internal Medicine). Pulmonary medical branch is a subspecialty of internal medicine.
PBL RESPIRATORY SYSTEM DR. NATHEER OBAIDAT Dr started to talk about his specialty at the hospital which is (ICU-Pulmonary-Internal Medicine). Pulmonary medical branch is a subspecialty of internal medicine.
Sheet: Patho-Pulmonary infections Done by: Maen Faoury
 Sheet: Patho-Pulmonary infections Done by: Maen Faoury Pneumonitis : might be an infection or not. Chemical Pneumonitis : not an infection. Parenchyma : an infection.( تندرج تحت ال pneumonitis) Lung Parenchyma
Sheet: Patho-Pulmonary infections Done by: Maen Faoury Pneumonitis : might be an infection or not. Chemical Pneumonitis : not an infection. Parenchyma : an infection.( تندرج تحت ال pneumonitis) Lung Parenchyma
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
5/5/2013. The Respiratory System. Chapter 16 Notes. The Respiratory System. Nasal Cavity. Sinuses
 The Respiratory System Chapter 16 Notes The Respiratory System Objectives List the general functions of the respiratory system. Identify the organs of the respiratory system. Describe the functions of
The Respiratory System Chapter 16 Notes The Respiratory System Objectives List the general functions of the respiratory system. Identify the organs of the respiratory system. Describe the functions of
Radiological syndroms. Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome
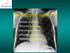 Radiological syndroms Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome Alveolar syndrome Pulmonary architecture : Morphological unit is the lobule 15-25mm
Radiological syndroms Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome Alveolar syndrome Pulmonary architecture : Morphological unit is the lobule 15-25mm
The Respiratory System Structures of the Respiratory System Structures of the Respiratory System Structures of the Respiratory System Nose Sinuses
 CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
09-Mar-15 PNEUMONIA RESPIRATORY SYSTEM L-3
 RESPIRATORY SYSTEM L-3 Professor Department of Pathology, University of Agriculture, Faisalabad. Email: mtjaved@uaf.edu.pk Web: https://sites.geocities.ws/mtjaved PNEUMONIA The pulmonary inflammatory response
RESPIRATORY SYSTEM L-3 Professor Department of Pathology, University of Agriculture, Faisalabad. Email: mtjaved@uaf.edu.pk Web: https://sites.geocities.ws/mtjaved PNEUMONIA The pulmonary inflammatory response
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D.
 Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D. Department of Radiology, Korea University Guro Hospital, College of Medicine, Korea
Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D. Department of Radiology, Korea University Guro Hospital, College of Medicine, Korea
INTRODUCTION TO UPPER RESPIRATORY TRACT DISEASES
 Upper Respiratory Tract Infections Return to Syllabus INTRODUCTION TO UPPER RESPIRATORY TRACT DISEASES General Goal: To know the major mechanisms of defense in the URT, the major mechanisms invaders use
Upper Respiratory Tract Infections Return to Syllabus INTRODUCTION TO UPPER RESPIRATORY TRACT DISEASES General Goal: To know the major mechanisms of defense in the URT, the major mechanisms invaders use
Unit 9. Respiratory System 16-1
 Unit 9 Respiratory System 16-1 Works together with the circulatory system Exchange of gases between atmosphere, blood, and cells If respiratory system and/or circulatory system fails, death will occur
Unit 9 Respiratory System 16-1 Works together with the circulatory system Exchange of gases between atmosphere, blood, and cells If respiratory system and/or circulatory system fails, death will occur
Acute respiratory failure
 Rita Williams, NP-C, PA PeaceHealth Medical Group Pulmonary & Critical Care Acute respiratory failure Ventilation/perfusion mismatching Most common cause of hypoxemia Normal is 1:1 ratio or 1 Ventilation
Rita Williams, NP-C, PA PeaceHealth Medical Group Pulmonary & Critical Care Acute respiratory failure Ventilation/perfusion mismatching Most common cause of hypoxemia Normal is 1:1 ratio or 1 Ventilation
May. Pathology #2. part. Rahaf Al-yousef. Mohammad Al-Qudah
 8 th May Pathology #2 nd Pneumonias 2 part Mohammad Al-Qudah Rahaf Al-yousef In the first part of our lectures today, we will define pneumonia clinically and pathologically(which is an infection of the
8 th May Pathology #2 nd Pneumonias 2 part Mohammad Al-Qudah Rahaf Al-yousef In the first part of our lectures today, we will define pneumonia clinically and pathologically(which is an infection of the
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
Objectives. Pneumonia. Pneumonia. Epidemiology. Prevalence 1/7/2012. Community-Acquired Pneumonia in infants and children
 Objectives Community-Acquired in infants and children Review of Clinical Practice Guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America - 2011 Sabah Charania,
Objectives Community-Acquired in infants and children Review of Clinical Practice Guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America - 2011 Sabah Charania,
Slide 120, Lobar Pneumonia. Slide 120, Lobar Pneumonia. Slide 172, Interstitial Pneumonia. Slide 172, Interstitial Pneumonia. 53 Year-Old Smoker
 Slide 120, Lobar Pneumonia Slide 120, Lobar Pneumonia Slide 172, Interstitial Pneumonia Slide 172, Interstitial Pneumonia 53 Year-Old Smoker Emphysema Pink puffer Barrel chest Hyperinflation Trapped air
Slide 120, Lobar Pneumonia Slide 120, Lobar Pneumonia Slide 172, Interstitial Pneumonia Slide 172, Interstitial Pneumonia 53 Year-Old Smoker Emphysema Pink puffer Barrel chest Hyperinflation Trapped air
People with asthma who smoke. The combination of asthma, a chronic airway disease, and smoking increases the risk of COPD even more.
 COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
Restrictive Pulmonary Diseases
 Restrictive Pulmonary Diseases Causes: Acute alveolo-capillary sysfunction Interstitial disease Pleural disorders Chest wall disorders Neuromuscular disease Resistance Pathophysiology Reduced compliance
Restrictive Pulmonary Diseases Causes: Acute alveolo-capillary sysfunction Interstitial disease Pleural disorders Chest wall disorders Neuromuscular disease Resistance Pathophysiology Reduced compliance
Nosocomial Pneumonia. <5 Days: Non-Multidrug-Resistant Bacteria
 Nosocomial Pneumonia Meredith Deutscher, MD Troy Schaffernocker, MD Ohio State University Burden of Hospital-Acquired Pneumonia Second most common nosocomial infection in the U.S. 5-10 episodes per 1000
Nosocomial Pneumonia Meredith Deutscher, MD Troy Schaffernocker, MD Ohio State University Burden of Hospital-Acquired Pneumonia Second most common nosocomial infection in the U.S. 5-10 episodes per 1000
Turkish Thoracic Society
 Türk Toraks Derneği Turkish Thoracic Society Pocket Books Series Diagnosis and Treatment of Community Acquired Pneumonia in Children Short Version (Handbook) in English www.toraks.org.tr This report was
Türk Toraks Derneği Turkish Thoracic Society Pocket Books Series Diagnosis and Treatment of Community Acquired Pneumonia in Children Short Version (Handbook) in English www.toraks.org.tr This report was
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems The Respiratory System Functions of the Respiratory System Warms, moistens, and filters incoming air Nasal cavity Resonating chambers for speech and
The RESPIRATORY System Unit 3 Transportation Systems The Respiratory System Functions of the Respiratory System Warms, moistens, and filters incoming air Nasal cavity Resonating chambers for speech and
Problem Based Learning Session. Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days.
 Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
Management of URTI s in Children
 Management of URTI s in Children Robin J Green PhD Antibiotics - Dilemmas for General Practitioners Antibiotic overuse = Resistance Delay in antibiotic use = Mortality Patient expectation Employer expectation
Management of URTI s in Children Robin J Green PhD Antibiotics - Dilemmas for General Practitioners Antibiotic overuse = Resistance Delay in antibiotic use = Mortality Patient expectation Employer expectation
Phases of Respiration
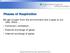 Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days
 Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
Upper Respiratory Tract Infections
 Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Histopathology: pulmonary pathology
 Histopathology: pulmonary pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about these
Histopathology: pulmonary pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about these
Acute Respiratory Disorders. and How to Assess them: Diagnostics
 Acute Respiratory Disorders and How to Assess them: Diagnostics Objectives Discuss 6 diagnostic tests or procedures used to assess lung disorders Name the parts of a focused assessment of a patient with
Acute Respiratory Disorders and How to Assess them: Diagnostics Objectives Discuss 6 diagnostic tests or procedures used to assess lung disorders Name the parts of a focused assessment of a patient with
Exam 1 Review. Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies
 Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Disease causing organisms Resistance Immunity
 Part 1 Disease causing organisms Resistance Immunity Bacteria Most common pathogens Anthrax Cholera Staphylococcus epidermidis bacteria Bacterial diseases Tuberculosis Cholera Bubonic Plague Tetanus Effects
Part 1 Disease causing organisms Resistance Immunity Bacteria Most common pathogens Anthrax Cholera Staphylococcus epidermidis bacteria Bacterial diseases Tuberculosis Cholera Bubonic Plague Tetanus Effects
Respiratory tract infections. Krzysztof Buczkowski
 Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
The Respiratory System. Dr. Ali Ebneshahidi
 The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
Respiratory System. Introduction. Atmosphere. Some Properties of Gases. Human Respiratory System. Introduction
 Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Pulmonary
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Pulmonary 1. GOAL: Diagnose and manage patients with asthma. 2. GOAL: Understand the role of the pediatrician in preventing
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Pulmonary 1. GOAL: Diagnose and manage patients with asthma. 2. GOAL: Understand the role of the pediatrician in preventing
Upper...and Lower Respiratory Tract Infections
 Upper...and Lower Respiratory Tract Infections Robin Jump, MD, PhD Cleveland Geriatric Research Education and Clinical Center (GRECC) Louis Stokes Cleveland VA Medical Center Case Western Reserve University
Upper...and Lower Respiratory Tract Infections Robin Jump, MD, PhD Cleveland Geriatric Research Education and Clinical Center (GRECC) Louis Stokes Cleveland VA Medical Center Case Western Reserve University
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
PULMONARY MEDICINE BOARD REVIEW. Financial Conflicts of Interest. Question #1: Question #1 (Cont.): None. Christopher H. Fanta, M.D.
 PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
Management of Acute Exacerbations
 15 Management of Acute Exacerbations Cenk Kirakli Izmir Dr. Suat Seren Chest Diseases and Surgery Training Hospital Turkey 1. Introduction American Thoracic Society (ATS) and European Respiratory Society
15 Management of Acute Exacerbations Cenk Kirakli Izmir Dr. Suat Seren Chest Diseases and Surgery Training Hospital Turkey 1. Introduction American Thoracic Society (ATS) and European Respiratory Society
Pneumonia Aetiology Why is it so difficult to distinguish pathogens from innocent bystanders?
 Pneumonia Aetiology Why is it so difficult to distinguish pathogens from innocent bystanders? David Murdoch Department of Pathology University of Otago, Christchurch Outline Background Diagnostic challenges
Pneumonia Aetiology Why is it so difficult to distinguish pathogens from innocent bystanders? David Murdoch Department of Pathology University of Otago, Christchurch Outline Background Diagnostic challenges
COPD exacerbation. Dr. med. Frank Rassouli
 Definition according to GOLD report: - «An acute event - characterized by a worsening of the patients respiratory symptoms - that is beyond normal day-to-day variations - and leads to a change in medication»
Definition according to GOLD report: - «An acute event - characterized by a worsening of the patients respiratory symptoms - that is beyond normal day-to-day variations - and leads to a change in medication»
DISEASES OF THE RESPIRATORY SYSTEM 2017 DR HEYAM AWAD LECTURE 1: RESPIRATORY DISTRESS SYNDROMES
 DISEASES OF THE RESPIRATORY SYSTEM 2017 DR HEYAM AWAD LECTURE 1: RESPIRATORY DISTRESS SYNDROMES This lecture covers two topics: neonatal respiratory distress syndrome (neonatal RDS) and adult respiratory
DISEASES OF THE RESPIRATORY SYSTEM 2017 DR HEYAM AWAD LECTURE 1: RESPIRATORY DISTRESS SYNDROMES This lecture covers two topics: neonatal respiratory distress syndrome (neonatal RDS) and adult respiratory
Chapter 16. Lung Abscess. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Respiratory Failure. Causes of Acute Respiratory Failure (ARF): a- Intrapulmonary:
 Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Management of Common Respiratory Disorders in Children. Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016
 Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children. Disclosures. Roadmap 6/10/2016
 Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Pulmonary Problems of the Neonate. Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA
 Pulmonary Problems of the Neonate Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA Lower Respiratory Diseases Ventilation/Perfusion Abnormalities
Pulmonary Problems of the Neonate Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA Lower Respiratory Diseases Ventilation/Perfusion Abnormalities
Chapter 11: Respiratory Emergencies
 29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
The Respiratory System
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Diseases of the Lung and Respiratory Tract, Part I. William Bligh-Glover M.D. Department of Anatomy, CWRU
 Diseases of the Lung and Respiratory Tract, Part I William Bligh-Glover M.D. Department of Anatomy, CWRU Educational objectives: Distinguish the types of atelectasis and their etiologies Distinguish the
Diseases of the Lung and Respiratory Tract, Part I William Bligh-Glover M.D. Department of Anatomy, CWRU Educational objectives: Distinguish the types of atelectasis and their etiologies Distinguish the
2. List seven functions performed by the respiratory system?
 The Respiratory System C23 Study Guide Tortora and Derrickson 1. In physiology we recognize that the word respiration has three meanings. What are the three different meanings of the word respiration as
The Respiratory System C23 Study Guide Tortora and Derrickson 1. In physiology we recognize that the word respiration has three meanings. What are the three different meanings of the word respiration as
There are four general types of congenital lung disorders:
 Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
PATHOGENICITY OF MICROORGANISMS
 PATHOGENICITY OF MICROORGANISMS Some microorganisms are : 1- Harmless microorganism, as normal flora 2- Harmfull microorganism, as pathogenic. A pathogenic microorganism is defined as one that causes or
PATHOGENICITY OF MICROORGANISMS Some microorganisms are : 1- Harmless microorganism, as normal flora 2- Harmfull microorganism, as pathogenic. A pathogenic microorganism is defined as one that causes or
Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease
 Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease Definition Acute chest syndrome (ACS) is defined as an acute illness characterized by fever and/or respiratory
Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease Definition Acute chest syndrome (ACS) is defined as an acute illness characterized by fever and/or respiratory
RESPIRATORY TRACT INFECTIONS. CLS 212: Medical Microbiology
 RESPIRATORY TRACT INFECTIONS CLS 212: Medical Microbiology Anatomy of the Respiratory System Respiratory Infections Respiratory tract can be divided into: Upper Respiratory Tract (URT): Sinuses Nasopharynx,.
RESPIRATORY TRACT INFECTIONS CLS 212: Medical Microbiology Anatomy of the Respiratory System Respiratory Infections Respiratory tract can be divided into: Upper Respiratory Tract (URT): Sinuses Nasopharynx,.
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Questions 1-3 refer to the following diagram. Indicate the plane labeled by the corresponding question number.
 Name: Grade: ANATOMY TEST Questions 1-3 refer to the following diagram. Indicate the plane labeled by the corresponding question number. 1. Plane #1 is the... 2. Plane #2 is the... 3. Plane #3 is the...
Name: Grade: ANATOMY TEST Questions 1-3 refer to the following diagram. Indicate the plane labeled by the corresponding question number. 1. Plane #1 is the... 2. Plane #2 is the... 3. Plane #3 is the...
Exam 2 Respiratory Disorders
 Exam 2 Respiratory Disorders Common Cold Common Cold Pathology Common Cold Consequences Rhinosinusitis Rhinosinusitis Pathology Rhinosinusitis ostia can close due to Influenza (Flu) Influenza Pathology
Exam 2 Respiratory Disorders Common Cold Common Cold Pathology Common Cold Consequences Rhinosinusitis Rhinosinusitis Pathology Rhinosinusitis ostia can close due to Influenza (Flu) Influenza Pathology
Differential diagnosis
 Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
IRIDOLOGY BREATHING. Compiled by. Campbell M Gold (2006) CMG Archives --()--
 IRIDOLOGY BREATHING Compiled by Campbell M Gold (2006) CMG Archives http://campbellmgold.com Introduction The respiratory tract, which is also called respiratory system, is the complex of organs and structures
IRIDOLOGY BREATHING Compiled by Campbell M Gold (2006) CMG Archives http://campbellmgold.com Introduction The respiratory tract, which is also called respiratory system, is the complex of organs and structures
Patient information: Pneumonia in adults (Beyond the Basics)
 Page 1 of 8 Official reprint from UpToDate www.uptodate.com 2014 UpToDate Patient information: Pneumonia in adults (Beyond the Basics) Authors Thomas J Marrie, MD Thomas M File, Jr, MD Section Editor John
Page 1 of 8 Official reprint from UpToDate www.uptodate.com 2014 UpToDate Patient information: Pneumonia in adults (Beyond the Basics) Authors Thomas J Marrie, MD Thomas M File, Jr, MD Section Editor John
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Therapist Written RRT Examination Detailed Content Outline
 I. PATIENT DATA EVALUATION AND RECOMMENDATIONS 4 7 17 28 A. Review Data in the Patient Record 1 4 0 5 1. Patient history e.g., present illness admission notes respiratory care orders medication history
I. PATIENT DATA EVALUATION AND RECOMMENDATIONS 4 7 17 28 A. Review Data in the Patient Record 1 4 0 5 1. Patient history e.g., present illness admission notes respiratory care orders medication history
RESPIRATORY FAILURE. Michael Kelly, MD Division of Pediatric Critical Care Dept. of Pediatrics
 RESPIRATORY FAILURE Michael Kelly, MD Division of Pediatric Critical Care Dept. of Pediatrics What talk is he giving? DO2= CO * CaO2 CO = HR * SV CaO2 = (Hgb* SaO2 * 1.34) + (PaO2 * 0.003) Sound familiar??
RESPIRATORY FAILURE Michael Kelly, MD Division of Pediatric Critical Care Dept. of Pediatrics What talk is he giving? DO2= CO * CaO2 CO = HR * SV CaO2 = (Hgb* SaO2 * 1.34) + (PaO2 * 0.003) Sound familiar??
Pulmonary Pathology II. William Bligh-Glover M.D. Department of Anatomy, CWRU
 Pulmonary Pathology II William Bligh-Glover M.D. Department of Anatomy, CWRU Goals and Objectives Comprehend the etiology, pathogenesis/pathopysiology and consequences of pulmonary hypertension Distinguish
Pulmonary Pathology II William Bligh-Glover M.D. Department of Anatomy, CWRU Goals and Objectives Comprehend the etiology, pathogenesis/pathopysiology and consequences of pulmonary hypertension Distinguish
ADVANCED ASSESSMENT Respiratory System
 ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine
 Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine American Osteopathic Association and American College of Osteopathic Internists BOT Rev. 2/2011 These
Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine American Osteopathic Association and American College of Osteopathic Internists BOT Rev. 2/2011 These
RESPIRATORY TRACT INFECTIONS. CLS 212: Medical Microbiology Zeina Alkudmani
 RESPIRATORY TRACT INFECTIONS CLS 212: Medical Microbiology Zeina Alkudmani Lower Respiratory Tract Upper Respiratory Tract Anatomy of the Respiratory System Nasopharynx Oropharynx Respiratory Tract Infections
RESPIRATORY TRACT INFECTIONS CLS 212: Medical Microbiology Zeina Alkudmani Lower Respiratory Tract Upper Respiratory Tract Anatomy of the Respiratory System Nasopharynx Oropharynx Respiratory Tract Infections
Respiratory Pathophysiology
 Respiratory Pathophysiology Objectives: Respiratory infections and lung cancer. Pleural effusion & edema, pleuritis, pneumothorax and atelectasis. Obstructive airway disease and chronic interstitial lung
Respiratory Pathophysiology Objectives: Respiratory infections and lung cancer. Pleural effusion & edema, pleuritis, pneumothorax and atelectasis. Obstructive airway disease and chronic interstitial lung
