UnitedHealth Premium Program Case-mix Adjusted Benchmarks with Severity or Risk Adjustment
|
|
|
- Amos Reynolds
- 5 years ago
- Views:
Transcription
1 UnitedHealth Premium Program Case-mix Adjusted Benchmarks with Severity or Risk Adjustment Resources u Phone: u u Website: UHCprovider.com/Premium Mail: UnitedHealthcare - UnitedHealth Premium Program MN017-W Health Care Lane Minnetonka, MN This document should be used with the UnitedHealth Premium Program Methodology at UHCprovider.com/Premium. It s important to review the entire document to understand the Premium program methodology. Overview For both the quality and cost efficiency measurements, the Premium program compares the physician s performance to a case-mix adjusted benchmark. Case mix adjustment accounts for variations in the composition of the patients and cases each physician treats. The Premium program also uses severity adjustments for certain quality measures and patient episode cost measurement. The program uses risk adjustment for patient total cost measurement. Quality Case-mix Adjusted Benchmark The benchmark used for quality measure comparison is defined as the case-mix adjusted expected quality measure compliance count. Some recommended interventions may be more or less difficult to accomplish. For example, patients with diabetes are likely to obtain retinal exams at a lower rate than they obtain hemoglobin A1c blood tests because retinal exams take greater effort. Similarly, the rate of adverse reactions to one class of medications might be different from the rate of adverse reactions to another medication. To establish the benchmark for each physician, the Premium program determines the expected compliance count for each measure by unique combinations of: Premium specialty Patient population Condition/procedure Severity level (surgical measures only)
2 The expected compliance count is calculated by multiplying the national compliance rate for each measure by the number of those measures attributed to the physician. Using the expected compliance count for each measure combination takes these patient variations into account. Patient Population A separate benchmark for each measure is established as applicable for the population of patients enrolled in each of the following health plans: UnitedHealthcare Commercial UnitedHealthcare Medicare Solutions UnitedHealthcare Community Plan (Medicaid) Condition/Procedure A separate benchmark for each measure is established as applicable for each condition/procedure. Medical Measures Conditions for medical measures are defined using Symmetry EBM Connect (EBM). Conditions are the medical conditions, disease states, or preventive screening categories for which EBM measures have been created. Patients must satisfy certain criteria to be identified as having particular conditions. These criteria, which vary by condition, include: presence of diagnosis or procedure codes submitted on medical claims, patient demographics, etc. Surgical Measures Procedures for surgical measures are defined using Symmetry Procedure Episode Groups (PEG). Procedures are the major procedure performed, and sub-procedure if applicable. Procedures are further classified into unique APR DRG combinations using 3M APR DRG (APR DRG) (e.g., the Premium program combines some APR DRGs like chest pain and angina). Severity Level For surgical measures, severity level accounts for patient differences that might affect the expected compliance count for the measure independent of the actual treatment given. Surgical measures include outcome measures such as complications and redos and therefore it is necessary to account for patient severity. Medical measures do not require severity adjustment because these measures apply regardless of the severity of a patient s condition. For example, medical evidence indicates that all patients with pharyngitis should be tested for group A streptococcus before antibiotic treatment regardless of the severity of their pharyngitis. In addition, many medical measures account for severity or coexisting conditions through specific clinical exclusions. Refer to Severity Level Surgical Episodes in the Cost Efficiency section below for an explanation of how severity level is determined for surgical procedures. Cost Efficiency Case-mix Adjusted Benchmark The benchmark used for cost efficiency comparison is defined as the case-mix adjusted expected sum of cost percentile ranks. To establish the benchmark for each physician, the Premium program puts patient total costs and patient episode costs into treatment sets by unique combinations of: Premium specialty Geographic area Condition/procedure (patient episode cost only) Inclusion of pharmacy cost Severity level (patient episode cost only) Risk level (patient total cost only) 2
3 Using these comparable treatment sets to establish the benchmark accounts for variations in the composition of the patients and cases each physician treats. The treatment set characteristics vary by cost and/or episode type as shown in the following: Characteristics Premium Specialty Geographic Area Patient Total Cost By specialty (Primary care physicians and non-surgical specialists) By CBSA (Core Based Statistical Area) Medical Episodes By specialty (All Premiumeligible specialties) By CBSA (Core Based Statistical Area) Condition/Procedure NA Condition-based episode: Inclusion of Pharmacy Cost Severity/Risk Level Included or excluded based on availability of patient s pharmacy cost data By patient risk category (based on ERG risk score) Episode Treatment Group (ETG) base class and treatment indicator Included or excluded based on availability of patient s pharmacy cost data Patient Episode Cost Surgical Episodes By specialty (All Premiumeligible specialties) By CBSA (Core Based Statistical Area) Procedure-based episode: Procedure Episode Group anchor/sub-anchor, and APR DRG rollup Excluded By ETG severity level 1-4 By APR DRG severity level 1-4 (inpatient only) Geographic Area A separate benchmark for each measure is established as applicable for each geographic area. Geographic areas are defined using Core Based Statistical Areas (CBSAs) or counties, since not all counties are assigned to a CBSA. In these cases, the county is the geographic area. CBSAs consist of the county or counties associated with at least one core urbanized area or urban cluster of at least 10,000 population, plus adjacent counties having a high degree of social and economic integration with the core as measured through commuting ties with the counties associated with the core. CBSAs are well suited to economic and social analyses because they represent coherent, functional areas. They are typically large enough to capture the complexity and diversity of the relationships among individuals, households, firms and communities, but small enough to be distinct places. Condition/Procedure A separate benchmark for each measure is established as applicable for each condition/procedure. Medical Episodes Medical episodes are defined using Symmetry Episode Treatment Groups (ETG), which accounts for differences in patient severity, including variations in complicating conditions, comorbidities, and major surgeries. Conditions are defined using ETG units which differ from one another with respect to resource use. The ETG units used for patient episode cost measurement are condition (ETG base class) and treatment (ETG treatment indicator code which shows with or without surgery/active treatment). Surgical Episodes Surgical episodes are defined using Symmetry Procedure Episode Groups (PEG) anchor procedure, the major procedure performed, and sub-procedure if applicable. Surgical episodes are further classified using 3M TM APR DRG (APR DRG). The APR DRG Classification System assigns each patient a base class for the underlying condition. The patients grouped into each base class are similar in terms of both clinical characteristics and the hospital resources they use. The PEG units used for patient episode cost measurement are PEG anchor procedure and APR DRG rollup (e.g., the Premium program combines some APR DRGs like chest pain and angina). 3
4 Inclusion of Pharmacy Cost Pharmacy cost is included for patient episode cost (medical episodes only) and patient total cost only when sufficient pharmacy claims information is available. When sufficient pharmacy claims information is not available, those episodes and patients are put into separate without pharmacy treatment sets. Pharmacy cost is only included during the time period that a patient had effective pharmacy and medical coverage. Pharmacy costs are not used for surgical episodes. Severity Level (Patient Episode Cost Only) The healthcare services required to diagnose, manage and treat a clinical condition can vary significantly across episodes. This variation derives from a number of sources, including differences in the practice of medicine across providers, differences in the price paid for medical services and differences in the underlying clinical characteristics of an episode. Severity adjustments account for the aspect of the variation in cost that can be explained by an episode s clinical characteristics. Specifically, the expected cost of an episode is based on clinical factors such as disease progression, comorbidities and other patient attributes that correlate with clinical need. Medical Episodes ETG is used to account for differences in medical episode severity by assigning a severity score to each episode. A higher severity score for an episode means a higher expected cost relative to other episodes of the same type. The severity score takes the following factors involved in the episode and gives them a weight: Patient age and gender (demographic weight) Comorbidities associated with the episode (comorbidity weight) Condition statuses (condition specificity, disease progression, etc.) associated with the episode (condition status weight) These weights are episode-specific. For example, a 50 year old male with asthma and congestive heart failure may receive different demographic weights for those two episodes. The episode of asthma with a comorbidity of diabetes can have a different comorbidity weight than the episode of congestive heart failure that also has a comorbidity of diabetes. ETG has separate condition status and comorbidity weights for age 65 and older. The weights are added to produce the overall severity score for the episode. Based on the severity score, a severity level of 1 to 4 is assigned to each specific episode. The severity level indicates a ranking of the specific episode relative to the population of all episodes of that same type. The value of 1 indicates a less severe episode and the value 4 indicates the most severe episode. The severity levels are determined by analyzing the distribution of episodes using a large nationally representative dataset. Surgical Episodes 3M APR DRG is used to account for differences in inpatient surgical episode severity. There are four severity of illness levels: 1 - minor, 2 - moderate, 3 - major and 4 - extreme. The underlying clinical principle of APR DRGs is that the patient severity of illness is highly dependent on the patient s underlying problem and that patients with high severity of illness are usually characterized by multiple serious diseases or illnesses. The assessment of severity is disease-specific. As a result, the significance attributed to complicating or comorbid conditions is dependent on the underlying problem. For example, certain types of infections are considered a more significant problem in a patient who is immunosuppressed than in a patient with a fractured arm. High severity of illness is primarily determined by the interaction of multiple diseases. To determine the patient severity of illness, APR DRG first determines the severity for each secondary diagnosis. Once the severity of each individual secondary diagnosis is established, APR DRG determines patient severity based on all of the patient s secondary diagnoses. The final patient severity level is determined by incorporating the impact of primary diagnosis, age, operating room procedures, non-operating room procedures, multiple operating room procedures, and combinations of categories of secondary diagnoses. For example, a patient with acute choledocholithiasis (acute gallstone attack) as the highest secondary diagnosis may be considered a major severity of illness (level 3) since there is associated significant organ system dysfunction. If additional, more serious diagnoses are also present, patient severity of illness may increase. For example, if peritonitis is present along with the acute choledocholithiasis, the patient may be considered an extreme severity of illness (level 4). Outpatient surgical episodes are assigned a severity level 1 because they tend to be the lower-severity procedures, or are performed on patients with a lower burden of illness. 4
5 Risk Level (Patient Total Cost Only) The health care services required to diagnose, manage and treat clinical conditions can vary significantly across patients. This variation derives from a number of sources, including differences in the practice of medicine across providers, differences in the price paid for medical services and differences in the underlying clinical characteristics of a patient s episodes. Patient risk defines that aspect of the variation in cost that can be explained by the clinical characteristics of a patient s episodes. In particular, this risk is the expected heath care costs or utilization of a patient. Symmetry Episode Risk Groups (ERG) accounts for differences in patient risk using ETG episodes as markers of risk rather than the diagnoses from individual medical encounters. By using episodes, the focus is placed on the key information describing a patient s underlying medical condition rather than the individual services provided in its treatment. Risk assessment techniques can vary depending on the characteristics of the patient population being measured. For patient total cost measurement, the models incorporated into ERG are designed for the under 65 commercial patient population. Separate models are developed for each Premium specialty for patients with and without pharmacy costs included to allow risk assessment to be performed using a consistent methodology across all similar patients. The fundamental building blocks of ERG are a patient s ETG episodes of care which represent the unique occurrences of a medical condition or disease and the health care services involved in diagnosing and managing their treatment. The nature and mix of the included episodes provide a clinical profile for a patient that serve as a marker of his or her current need for medical care. Once the relevant patient episodes are identified (refer to the Patient Total Cost document for an explanation of which patient episodes are used for patient total cost measurement), the ERG risk score is calculated as follows: 1. Translate ETGs to ERGs: Episodes for each patient are further categorized into one of 189 ERGs. The ERGs are markers of patient risk and represent ETG episodes of similar clinical and risk characteristics. 2. Generate ERG Profile: The mix of ERGs provide a clinical profile for a patient. Patients can be assigned zero, one or more ERGs. Patients with multiple medical conditions would have multiple ERGs. 3. Calculate ERG Risk Score: Using predetermined weights for each Premium specialty category 1 based on the inclusion or exclusion of pharmacy costs, and the patient s ERG profile, a risk score is computed. A patient s risk score is the sum of the weights attached to each ERG observed in the patient s ERG profile. Based on the patient s risk score, a patient s risk level is determined which indicates a ranking of the patient relative to the population of all patients for the Premium specialty category and pharmacy cost status. The number of levels varies by Premium specialty category with a value of 1 indicating a lower risk patient. The risk level values are established by analyzing the distribution of patient risk scores using a large nationally representative dataset. 1 Specialty categories are PCP, OB-GYN, Allergy, Cardiology, Endocrinology, Nephrology, Neurology, Pulmonology and Rheumatology. 5
6 Important notes about the UnitedHealth Premium Physician Program The information from the UnitedHealth Premium program is not an endorsement of a particular physician or health care professional s suitability for the health care needs of any particular member. UnitedHealthcare does not practice medicine nor provide health care services. Physicians are solely responsible for medical judgments and treatments supplied. A Premium Care Physician or Quality Care Physician designation does not guarantee the quality of health care services members will receive from a physician and does not guarantee the outcome of any health care services members will receive. Likewise, the fact that a physician has a Not Evaluated for Premium Care or a Does Not Meet Premium Quality Criteria designation does not mean that the physician does not provide quality health care services. All physicians in the UnitedHealthcare network have met certain minimum credentialing requirements. Regardless of whether a physician has received a Premium Care Physician designation, members have access to all physicians in the UnitedHealthcare network, as further described under the member s benefit plan. The designation of Not Evaluated for Premium Care is given when a physician does not practice in a specialty that is evaluated by the Premium program, or when a physician s evaluation is in process. It is also given when a physician does not have enough health plan claims data to be evaluated, but it is not an indicator of the total number of patients treated by the physician or the number of procedures performed by the physician. Rather, it reflects the statistical requirements of the Premium program, which includes only health plan claims associated with specific Premium program measures and relevant to the physician s specialty. In some cases, there may not be enough data to complete the analytic process from a statistical standpoint. UnitedHealthcare informs members that designations are intended only as a guide when choosing a physician and should not be the sole factor in selecting a physician. As with all programs that evaluate performance based on analysis of a sample, there is a risk of error. There is a risk of error in the claims data used in the evaluation, the calculations used in the evaluation, and the way the Premium program determined that an individual physician was responsible for the treatment of the patient s condition. Physicians have the opportunity to review this data and submit a reconsideration request. UnitedHealthcare uses statistical testing to compare a physician s results to expected or normative results. There is a risk of error in statistical tests when applied to the data and a result based on statistical testing is not a guarantee of correct inference or classification. We inform members that it is important that they consider many factors and information when selecting a physician. We also inform our members that they may wish to discuss designations with a physician before choosing him or her, or confer with their current physician for advice on selecting other physicians. The information contained in this Case-mix Adjusted Benchmarks with Severity or Risk Adjustment document is subject to change. Insurance coverage provided by or through UnitedHealthcare Insurance Company, All Savers Insurance Company, or their affiliates. Health plan coverage provided by UnitedHealthcare of Arizona, Inc., UHC of California DBA UnitedHealthcare of California, UnitedHealthcare Benefits Plan of California, UnitedHealthcare of Colorado, Inc., UnitedHealthcare of Oklahoma, Inc., UnitedHealthcare of Oregon, Inc., UnitedHealthcare of Texas, LLC, UnitedHealthcare Benefits of Texas, Inc., UnitedHealthcare of Utah, Inc. and UnitedHealthcare of Washington, Inc. or other affiliates. Administrative services provided by United HealthCare Services, Inc., OptumRx, OptumHealth Care Solutions, Inc. or its affiliates. Behavioral health products are provided by U.S. Behavioral Health Plan, California (USBHPC), United Behavioral Health (UBH) or its affiliates. D /18 Doc#: PCA _ United HealthCare Services, Inc.
UnitedHealth Premium Designation Program Case-mix Adjusted Benchmarks with Severity or Risk Adjustment
 UnitedHealth Premium Designation Program Case-mix Adjusted Benchmarks with Severity or Risk Adjustment Resources u Phone: 866-270-5588 u u u Website: UnitedHealthcareOnline.com > Quick Links > UnitedHealth
UnitedHealth Premium Designation Program Case-mix Adjusted Benchmarks with Severity or Risk Adjustment Resources u Phone: 866-270-5588 u u u Website: UnitedHealthcareOnline.com > Quick Links > UnitedHealth
UnitedHealth Premium Program Case-mix, Severity and Risk
 UnitedHealth Premium Program Case-mix, Severity and Risk Resources u Phone: 866-270-5588 u u Website: UnitedHealthPremium.UHC.com Mail: UnitedHealthcare - UnitedHealth Premium Program MN017-W700 9700 Health
UnitedHealth Premium Program Case-mix, Severity and Risk Resources u Phone: 866-270-5588 u u Website: UnitedHealthPremium.UHC.com Mail: UnitedHealthcare - UnitedHealth Premium Program MN017-W700 9700 Health
UnitedHealthcare NexusACO Frequently Asked Questions
 UnitedHealthcare NexusACO Frequently Asked Questions Key Points There are two tiered benefit plans in UnitedHealthcare NexusACO UnitedHealthcare NexusACO R (Referrals Required) and UnitedHealthcare Nexus
UnitedHealthcare NexusACO Frequently Asked Questions Key Points There are two tiered benefit plans in UnitedHealthcare NexusACO UnitedHealthcare NexusACO R (Referrals Required) and UnitedHealthcare Nexus
Quick-Start Guide. UnitedHealthcare of Minnesota, North Dakota and South Dakota.
 Quick-Start Guide. UnitedHealthcare of Minnesota, North Dakota and South Dakota. Welcome. Thank you for joining us! As a new payer in Minnesota, North Dakota and South Dakota, we have an extraordinary
Quick-Start Guide. UnitedHealthcare of Minnesota, North Dakota and South Dakota. Welcome. Thank you for joining us! As a new payer in Minnesota, North Dakota and South Dakota, we have an extraordinary
Provider Service Model. Collaborating for Success Jodi Stockslager, Sr. Provider Advocate, Provider Relations
 Provider Service Model Collaborating for Success Jodi Stockslager, Sr. Provider Advocate, Provider Relations Agenda Welcome / Introductions UnitedHealthcare overview Member ID Cards Products and networks
Provider Service Model Collaborating for Success Jodi Stockslager, Sr. Provider Advocate, Provider Relations Agenda Welcome / Introductions UnitedHealthcare overview Member ID Cards Products and networks
UnitedHealth Premium Physician Designation Program Episode Treatment Groups (ETG ) Description and Specialty
 UnitedHealth Premium Physician Designation Program Episode Treatment Groups (ETG ) Description and Specialty 666700 Acne Family Medicine, Internal Medicine, Pediatrics 438300 Acute Bronchitis Allergy,
UnitedHealth Premium Physician Designation Program Episode Treatment Groups (ETG ) Description and Specialty 666700 Acne Family Medicine, Internal Medicine, Pediatrics 438300 Acute Bronchitis Allergy,
ICD-10 Implementation: From ICD-10? to I Can Do-10!
 ICD-10 Implementation: From ICD-10? to I Can Do-10! Prepared For: OH Home and Community Based Service Providers August 12, 2015 Webex Presented By: Aaron R. Sapp, MPS National ICD-10 Program Director Insurance
ICD-10 Implementation: From ICD-10? to I Can Do-10! Prepared For: OH Home and Community Based Service Providers August 12, 2015 Webex Presented By: Aaron R. Sapp, MPS National ICD-10 Program Director Insurance
The BlueCompare SM Physician Designation Program
 The BlueCompare SM Physician Designation Program Continuing escalation of health care costs has driven premiums and medical expenses to higher and higher levels each year, motivating employers and consumers
The BlueCompare SM Physician Designation Program Continuing escalation of health care costs has driven premiums and medical expenses to higher and higher levels each year, motivating employers and consumers
A Prospective Comparison of Two Commercially Available Hospital Admission Risk Scores
 A Prospective Comparison of Two Commercially Available Hospital Admission Risk Scores Dale Eric Green, MD MHA FCCP: Chief Medical Information Officer, Cornerstone Health Care AMGA April, 2014 Disclosure
A Prospective Comparison of Two Commercially Available Hospital Admission Risk Scores Dale Eric Green, MD MHA FCCP: Chief Medical Information Officer, Cornerstone Health Care AMGA April, 2014 Disclosure
Symmetry Episode Treatment Groups
 Symmetry Episode Treatment Groups Measuring health care with meaningful episodes of care Identifying clinical episodes of illness and the services involved in their diagnosis, management, and treatment
Symmetry Episode Treatment Groups Measuring health care with meaningful episodes of care Identifying clinical episodes of illness and the services involved in their diagnosis, management, and treatment
Quality Care Plus 2015 Primary Care Physician Incentive Program. Now includes Medicare patients!
 Quality Care Plus 2015 Primary Care Physician Incentive Program Now includes Medicare patients! Health Partners Plans (HPP) would like to express our appreciation for the invaluable role our primary care
Quality Care Plus 2015 Primary Care Physician Incentive Program Now includes Medicare patients! Health Partners Plans (HPP) would like to express our appreciation for the invaluable role our primary care
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes Respiratory Infection (RI); Pneumonia (PNA); Inpatient Urinary Tract Infection (UTI-I; Outpatient Urinary
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes Respiratory Infection (RI); Pneumonia (PNA); Inpatient Urinary Tract Infection (UTI-I; Outpatient Urinary
Cigna Care Designation and Physician Quality and Cost-Efficiency Displays 2016 Methodologies Whitepaper
 Cigna Care Designation and Physician Quality and Cost-Efficiency Displays 2016 Methodologies Whitepaper For Health Care Professionals February 2016 Introduction... 2 Cigna Physician Quality and Cost-Efficiency
Cigna Care Designation and Physician Quality and Cost-Efficiency Displays 2016 Methodologies Whitepaper For Health Care Professionals February 2016 Introduction... 2 Cigna Physician Quality and Cost-Efficiency
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes Acute COPD exacerbation (COPD); Screening and surveillance colonoscopy (COL); and Outpatient and non-acute
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes Acute COPD exacerbation (COPD); Screening and surveillance colonoscopy (COL); and Outpatient and non-acute
Transparency The Public Reporting of Physician Performance
 (The Evaluation of the Impact of Physician Self-Reporting Administrative Data) Dr. Allen Naidoo PhD Director-Medical Informatics BlueCross and BlueShield of Tennessee Dr. Marc Loizeaux PhD Manager-Provider
(The Evaluation of the Impact of Physician Self-Reporting Administrative Data) Dr. Allen Naidoo PhD Director-Medical Informatics BlueCross and BlueShield of Tennessee Dr. Marc Loizeaux PhD Manager-Provider
Payment Innovation and Health Center Dental Programs: Case Studies from Three States
 Payment Innovation and Health Center Dental Programs: Case Studies from Three States January 2018 CONTENTS California-2 Iowa-3 Implementation-2 Clinical Practice Implications-2 Implementation-4 Clinical
Payment Innovation and Health Center Dental Programs: Case Studies from Three States January 2018 CONTENTS California-2 Iowa-3 Implementation-2 Clinical Practice Implications-2 Implementation-4 Clinical
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes Attention deficit hyperactivity disorder (ADHD); Opposition defiance disorder (ODD); Coronary artery bypass
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes Attention deficit hyperactivity disorder (ADHD); Opposition defiance disorder (ODD); Coronary artery bypass
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments
 Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Trends in Health Plan Design: High Performance Networks. John Bertko, F.S.A., MAAA Vice President and Chief Actuary Humana Inc July 28, 2005
 Trends in Health Plan Design: High Performance Networks John Bertko, F.S.A., MAAA Vice President and Chief Actuary Humana Inc July 28, 2005 1 Overview What is a High Performance Network (HPN) Tighter network
Trends in Health Plan Design: High Performance Networks John Bertko, F.S.A., MAAA Vice President and Chief Actuary Humana Inc July 28, 2005 1 Overview What is a High Performance Network (HPN) Tighter network
extraction can take place. Another problem is that the treatment for chronic diseases is sequential based upon the progression of the disease.
 ix Preface The purpose of this text is to show how the investigation of healthcare databases can be used to examine physician decisions to develop evidence-based treatment guidelines that optimize patient
ix Preface The purpose of this text is to show how the investigation of healthcare databases can be used to examine physician decisions to develop evidence-based treatment guidelines that optimize patient
Quality Corp Measures Description and Methodologies
 Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
Quality Corp Measures Description and Methodologies
 Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
Longitudinal Care Management. September 2016
 Longitudinal Care Management September 2016 Risk Score Assignment of Longitudinal CM Other C M Referral sources Screening: Need CM? Clinical Assessment tools Program Services Integrated Care Management
Longitudinal Care Management September 2016 Risk Score Assignment of Longitudinal CM Other C M Referral sources Screening: Need CM? Clinical Assessment tools Program Services Integrated Care Management
CLINICAL PROCESS IMPROVEMENT INITIATIVE (CPII) EFFICIENCY REPORT EXPLANATION January 4, 2016
 CLINICAL PROCESS IMPROVEMENT INITIATIVE (CPII) EFFICIENCY REPORT EXPLANATION January 4, 2016 WHAT IS AN EPISODE OF CARE? An episode of care is a grouping of a patient s health care claims for a unique
CLINICAL PROCESS IMPROVEMENT INITIATIVE (CPII) EFFICIENCY REPORT EXPLANATION January 4, 2016 WHAT IS AN EPISODE OF CARE? An episode of care is a grouping of a patient s health care claims for a unique
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual
 Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Get the Right Reimbursement for High Risk Patients
 Get the Right Reimbursement for High Risk Patients A Proven Strategy for Managing Hierarchical Condition Categories (HCC) in your EHR 847-272-1242 sales@e-imo.com e-imo.com 1 OVERVIEW Medicare Advantage
Get the Right Reimbursement for High Risk Patients A Proven Strategy for Managing Hierarchical Condition Categories (HCC) in your EHR 847-272-1242 sales@e-imo.com e-imo.com 1 OVERVIEW Medicare Advantage
Efficiency Methodology
 Efficiency Methodology David C. Schutt, MD Bob Kelley Thomson Healthcare October 2007 Overview Definition Clinical Grouping Methods Implementation Considerations Reporting to Physician Organizations Example
Efficiency Methodology David C. Schutt, MD Bob Kelley Thomson Healthcare October 2007 Overview Definition Clinical Grouping Methods Implementation Considerations Reporting to Physician Organizations Example
Symmetry Episode Treatment Groups
 Symmetry Episode Treatment Groups Measuring Health Care with Meaningful Episodes of Care The information in this document is subject to change without notice. This documentation contains proprietary information,
Symmetry Episode Treatment Groups Measuring Health Care with Meaningful Episodes of Care The information in this document is subject to change without notice. This documentation contains proprietary information,
Performance Analysis:
 Performance Analysis: Healthcare Utilization of CCNC- Population 2007-2010 Prepared by Treo Solutions JUNE 2012 Table of Contents SECTION ONE: EXECUTIVE SUMMARY 4-5 SECTION TWO: REPORT DETAILS 6 Inpatient
Performance Analysis: Healthcare Utilization of CCNC- Population 2007-2010 Prepared by Treo Solutions JUNE 2012 Table of Contents SECTION ONE: EXECUTIVE SUMMARY 4-5 SECTION TWO: REPORT DETAILS 6 Inpatient
Medicare Severity-adjusted Diagnosis Related Groups (MS-DRGs) Coding Adjustment
 American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
MEASURING CARE QUALITY
 MEASURING CARE QUALITY Region December 2013 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
MEASURING CARE QUALITY Region December 2013 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
Spending estimates from Cancer Care Spending
 CALIFORNIA HEALTHCARE FOUNDATION August 2015 Estimating Cancer Care Spending in the California Medicare Population: Methodology Detail This paper describes in detail the methods used by Deborah Schrag,
CALIFORNIA HEALTHCARE FOUNDATION August 2015 Estimating Cancer Care Spending in the California Medicare Population: Methodology Detail This paper describes in detail the methods used by Deborah Schrag,
Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach
 Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach Presented by Susan G. Haber, Sc.D 1 ; Boyd H. Gilman, Ph.D. 1 1 RTI International Presented at The 133rd Annual Meeting of
Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach Presented by Susan G. Haber, Sc.D 1 ; Boyd H. Gilman, Ph.D. 1 1 RTI International Presented at The 133rd Annual Meeting of
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes Mastectomy, Breast Cancer Medical Oncology, Breast Biopsy, Tonsillectomy, Otitis media, Anxiety, Non-emergent
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes Mastectomy, Breast Cancer Medical Oncology, Breast Biopsy, Tonsillectomy, Otitis media, Anxiety, Non-emergent
MEASURING CARE QUALITY
 MEASURING CARE QUALITY Region November 2016 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
MEASURING CARE QUALITY Region November 2016 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
NCC Pediatrics Continuity Clinic Curriculum: Medical Home Module 2 Well Visits
 NCC Pediatrics Continuity Clinic Curriculum: Medical Home Module 2 Well Visits Overall Goal: To identify strategies for providing comprehensive care during a well visit. The provision of comprehensive
NCC Pediatrics Continuity Clinic Curriculum: Medical Home Module 2 Well Visits Overall Goal: To identify strategies for providing comprehensive care during a well visit. The provision of comprehensive
Bridges to Excellence Physician Incentive Program. SuperiorHealthPlan.com SHP_
 Bridges to Excellence Physician Incentive Program 2015 SuperiorHealthPlan.com SHP_2014851 Bridges to Excellence (BTE) is a physician recognition program from Health Care Incentives Improvement Institute
Bridges to Excellence Physician Incentive Program 2015 SuperiorHealthPlan.com SHP_2014851 Bridges to Excellence (BTE) is a physician recognition program from Health Care Incentives Improvement Institute
2019 PHARMACY DIRECTORY
 2019 PHARMACY DIRECTORY This is a brief explanation and overview of the pharmacies members can use to get their prescription drugs. In a continued effort to offer our members value, pharmacies may be added
2019 PHARMACY DIRECTORY This is a brief explanation and overview of the pharmacies members can use to get their prescription drugs. In a continued effort to offer our members value, pharmacies may be added
Cost-Motivated Treatment Changes in Commercial Claims:
 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non- Medical Switching August 2017 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non-Medical
Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non- Medical Switching August 2017 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non-Medical
Physical Therapy and Occupational Therapy Initial Evaluation and Reevaluation Reimbursement Policy. Approved By
 Policy Number Physical Therapy and Occupational Therapy Initial Evaluation and Reevaluation Reimbursement Policy 0044 Annual Approval Date 4/2017 Approved By Optum Reimbursement Committee Optum Quality
Policy Number Physical Therapy and Occupational Therapy Initial Evaluation and Reevaluation Reimbursement Policy 0044 Annual Approval Date 4/2017 Approved By Optum Reimbursement Committee Optum Quality
Reference Guide for Adult Health PATH HEDIS, CMS Part D, CAHPS and HOS Measures
 Reference Guide for Adult Health 2018 HEDIS, CMS Part D, CAHPS and HOS Measures HEDIS is a registered trademark of the National Committee for Quality Assurance (NCQA). Information contained in this guide
Reference Guide for Adult Health 2018 HEDIS, CMS Part D, CAHPS and HOS Measures HEDIS is a registered trademark of the National Committee for Quality Assurance (NCQA). Information contained in this guide
Redesign of the National Ambulatory Medical Care Survey to support state estimates
 Redesign of the National Ambulatory Medical Care Survey to support state estimates Esther Hing, M.P.H. 1, Iris Shimizu, Ph.D. 1 1 National Center for Health Statistics, 3311 Toledo Road, Hyattsville, MD
Redesign of the National Ambulatory Medical Care Survey to support state estimates Esther Hing, M.P.H. 1, Iris Shimizu, Ph.D. 1 1 National Center for Health Statistics, 3311 Toledo Road, Hyattsville, MD
Predictive Models: Current and Future. November 9, Steve Wickstrom Vice President, Research and Methods OptumInsight
 Predictive Models: Current and Future November 9, 2011 Steve Wickstrom Vice President, Research and Methods OptumInsight Steven.wickstrom@optum.com OptumInsight Predictive Solutions: Overview OptumInsight
Predictive Models: Current and Future November 9, 2011 Steve Wickstrom Vice President, Research and Methods OptumInsight Steven.wickstrom@optum.com OptumInsight Predictive Solutions: Overview OptumInsight
Based on Medicare FFS Beneficiaries Assigned July 1, 2011 December 31, 2011
 July 2012 Multi-payer Advanced Primary Care Practice (MAPCP) Demonstration Medical Home Feedback Report Based on Medicare FFS Beneficiaries Assigned July 1, 2011 December 31, 2011 Practice Number Practice
July 2012 Multi-payer Advanced Primary Care Practice (MAPCP) Demonstration Medical Home Feedback Report Based on Medicare FFS Beneficiaries Assigned July 1, 2011 December 31, 2011 Practice Number Practice
Table of Contents. Page 2 of 20
 Page 1 of 20 Table of Contents Table of Contents... 2 NMHCTOD Participants... 3 Introduction... 4 Methodology... 5 Types of Data Available... 5 Diabetes in New Mexico... 7 HEDIS Quality Indicators for
Page 1 of 20 Table of Contents Table of Contents... 2 NMHCTOD Participants... 3 Introduction... 4 Methodology... 5 Types of Data Available... 5 Diabetes in New Mexico... 7 HEDIS Quality Indicators for
Precyse University ICD-10 Education Tracks
 Precyse University ICD-10 Education Tracks The following information will help you understand the Precyse University ICD-10 Educational Tracks. Each impacted population requires specific education to prepare
Precyse University ICD-10 Education Tracks The following information will help you understand the Precyse University ICD-10 Educational Tracks. Each impacted population requires specific education to prepare
Lumify. Lumify reimbursement guide {D DOCX / 1
 Lumify Lumify reimbursement guide {D0672917.DOCX / 1 {D0672917.DOCX / 1 } Contents Overview 4 How claims are paid 4 Documentation requirements 5 Billing codes for ultrasound: Non-hospital setting 6 Billing
Lumify Lumify reimbursement guide {D0672917.DOCX / 1 {D0672917.DOCX / 1 } Contents Overview 4 How claims are paid 4 Documentation requirements 5 Billing codes for ultrasound: Non-hospital setting 6 Billing
The Healthy Indiana Plan
 The Healthy Indiana Plan House Enrolled Act 1678 A Pragmatic Approach Governor Mitch Daniels July 16, 2007 Indiana s Fiscal Health is Good First Back-to-Back Balanced Budget in Eight Years $1,000.0 Revenue
The Healthy Indiana Plan House Enrolled Act 1678 A Pragmatic Approach Governor Mitch Daniels July 16, 2007 Indiana s Fiscal Health is Good First Back-to-Back Balanced Budget in Eight Years $1,000.0 Revenue
PCMH 2018 Enrollment and Update August 25, 2017
 PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
Clinical Quality Measures Summary of Upcoming Enhancements
 Upcoming coding enhancements will impact the logic behind the clinical quality indicators applicable to your practice specialty. Please refer to this grid for a summary of the coding enhancements and some
Upcoming coding enhancements will impact the logic behind the clinical quality indicators applicable to your practice specialty. Please refer to this grid for a summary of the coding enhancements and some
Clinical Documentation Improvement: Reporting Opportunities
 Clinical Documentation Improvement: Reporting Opportunities Karee Burns, RN, BSN Midas+ Solutions Consultant Waheed Baqai, MPH, CPH Director Clinical Decision Support Loma Linda University Medical Center
Clinical Documentation Improvement: Reporting Opportunities Karee Burns, RN, BSN Midas+ Solutions Consultant Waheed Baqai, MPH, CPH Director Clinical Decision Support Loma Linda University Medical Center
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Reference Guide for Women s Health
 Reference Guide for Women s Health 2018 HEDIS Measures HEDIS is a registered trademark of the National Committee for Quality Assurance (NCQA). Information contained in this guide is based on NCQA HEDIS
Reference Guide for Women s Health 2018 HEDIS Measures HEDIS is a registered trademark of the National Committee for Quality Assurance (NCQA). Information contained in this guide is based on NCQA HEDIS
NCQA Health Insurance Plan Ratings Methodology October 2014
 NCQA Health Insurance Plan Ratings Methodology October 2014 REVISION CHART Date Published December 2013 April 2014 October 2014 Description Draft version Final version Updated measure list with 50% rule
NCQA Health Insurance Plan Ratings Methodology October 2014 REVISION CHART Date Published December 2013 April 2014 October 2014 Description Draft version Final version Updated measure list with 50% rule
Exhibit 1. Change in State Health System Performance by Indicator
 Exhibit 1. Change in State Health System Performance by Indicator Indicator (arranged by number of states with improvement within dimension) Access and Affordability 0 Children ages 0 18 uninsured At-risk
Exhibit 1. Change in State Health System Performance by Indicator Indicator (arranged by number of states with improvement within dimension) Access and Affordability 0 Children ages 0 18 uninsured At-risk
Rural Training Track Programs: A Guide to the Medicare Requirements
 Rural Training Track Programs: A Guide to the Medicare Requirements Learn Serve Lead Association of American Medical Colleges Introduction Rural Training Track (RTT) programs provide an opportunity for
Rural Training Track Programs: A Guide to the Medicare Requirements Learn Serve Lead Association of American Medical Colleges Introduction Rural Training Track (RTT) programs provide an opportunity for
WATCHMAN. For questions regarding WATCHMAN reimbursement, please contact:
 WATCHMAN IMPORTANCE OF DOCUMENTATION & THE IMPACT ON MS- DRG ASSIGNMENT This guide stresses the importance of documentation in capturing the appropriate acuity level for patients considered WATCHMAN candidates.
WATCHMAN IMPORTANCE OF DOCUMENTATION & THE IMPACT ON MS- DRG ASSIGNMENT This guide stresses the importance of documentation in capturing the appropriate acuity level for patients considered WATCHMAN candidates.
Primary Care Physician (PCP) Election Form for Charter and Navigate. Employer Name: mandatory
 Primary Care Physician (PCP) Election Form for Charter and Navigate mandatory There is no coverage to other physicians or specialists without a referral from the PCP. Employer Name: *Member Name (every
Primary Care Physician (PCP) Election Form for Charter and Navigate mandatory There is no coverage to other physicians or specialists without a referral from the PCP. Employer Name: *Member Name (every
Preferred Care Partners. HEDIS Technical Standards
 Preferred Care Partners HEDIS Technical Standards 1 HEDIS What is HEDIS HEDIS Overview Adults HEDIS Overview Pediatrics HEDIS is a registered trademark of the National Committee for Quality Assurance 2
Preferred Care Partners HEDIS Technical Standards 1 HEDIS What is HEDIS HEDIS Overview Adults HEDIS Overview Pediatrics HEDIS is a registered trademark of the National Committee for Quality Assurance 2
Submitted to: Re: Comments on CMS Proposals for Patient Condition Groups and Care Episode Groups
 April 24, 2017 The Honorable Seema Verma Administrator Centers for Medicare & Medicaid Services Hubert H. Humphrey Building 200 Independence Avenue SW Washington, D.C. 20201 Submitted to: macra-episode-based-cost-measures-info@acumenllc.com
April 24, 2017 The Honorable Seema Verma Administrator Centers for Medicare & Medicaid Services Hubert H. Humphrey Building 200 Independence Avenue SW Washington, D.C. 20201 Submitted to: macra-episode-based-cost-measures-info@acumenllc.com
Data Report 2016 Indiana Physician Licensure Survey
 Data Report 2016 Indiana Physician Licensure Survey May 2016 0 010 0 010 0 0110101010 0110 0 010 011010 010 0 010 0 0110110 0110 0110 0 010 010 0 010 0 01101010 0110 0 010 010 0 010 0 0 PH YS I C IAN 0
Data Report 2016 Indiana Physician Licensure Survey May 2016 0 010 0 010 0 0110101010 0110 0 010 011010 010 0 010 0 0110110 0110 0110 0 010 010 0 010 0 01101010 0110 0 010 010 0 010 0 0 PH YS I C IAN 0
A conversation with Norman Volk, April 1, 2016
 Participants A conversation with Norman Volk, April 1, 2016 Norman Volk Former Chair, The John A. Hartford Foundation Board of Trustees Luke Muehlhauser Research Analyst, Open Philanthropy Project Note:
Participants A conversation with Norman Volk, April 1, 2016 Norman Volk Former Chair, The John A. Hartford Foundation Board of Trustees Luke Muehlhauser Research Analyst, Open Philanthropy Project Note:
Reimbursement Information for Diagnostic Ultrasound and Ultrasound-guided Procedures Commonly Performed by Otolaryngologists
 GE Healthcare Reimbursement Information for Diagnostic Ultrasound and Ultrasound-guided Procedures Commonly Performed by Otolaryngologists 1 January, 2013 www.gehealthcare.com/reimbursement imagination
GE Healthcare Reimbursement Information for Diagnostic Ultrasound and Ultrasound-guided Procedures Commonly Performed by Otolaryngologists 1 January, 2013 www.gehealthcare.com/reimbursement imagination
Population health: Going beyond primary care, making it work in a complex health system. Mary Brainerd, HealthPartners President and CEO
 Population health: Going beyond primary care, making it work in a complex health system Mary Brainerd, HealthPartners President and CEO A little about HealthPartners coverage 1.4 million plan members patients
Population health: Going beyond primary care, making it work in a complex health system Mary Brainerd, HealthPartners President and CEO A little about HealthPartners coverage 1.4 million plan members patients
Chapter 6: Healthcare Expenditures for Persons with CKD
 Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
NATIONAL QUALITY FORUM
 CONFERENCE CALL OF THE RESOURCE USE STEERING COMMITTEE July 15, 2011 Committee Members Participating: Tom Rosenthal, MD (Co-Chair, UCLA School of Medicine); Jeptha Curtis, MD (Yale University School of
CONFERENCE CALL OF THE RESOURCE USE STEERING COMMITTEE July 15, 2011 Committee Members Participating: Tom Rosenthal, MD (Co-Chair, UCLA School of Medicine); Jeptha Curtis, MD (Yale University School of
Aexcel. Specialist Designation in Aetna Performance Network. Methodology Guide
 Aexcel Specialist Designation in Aetna Performance Network Methodology Guide Aexcel 2009 TABLE OF CONTENTS Background on Aexcel Performance Networks... 3 Clinical Performance Evaluation Process... 8 General
Aexcel Specialist Designation in Aetna Performance Network Methodology Guide Aexcel 2009 TABLE OF CONTENTS Background on Aexcel Performance Networks... 3 Clinical Performance Evaluation Process... 8 General
B&T Format. New Measures. Better health care. Better choices. Better health.
 1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February
1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February
The University of Mississippi School of Pharmacy
 LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Reimbursement Information for Automated Breast Ultrasound Screening
 GE Healthcare Reimbursement Information for Automated Breast Ultrasound Screening January 2015 www.gehealthcare.com/reimbursement The Invenia ABUS is indicated as an adjunct to mammography for breast cancer
GE Healthcare Reimbursement Information for Automated Breast Ultrasound Screening January 2015 www.gehealthcare.com/reimbursement The Invenia ABUS is indicated as an adjunct to mammography for breast cancer
Technical Appendix for Outcome Measures
 Study Overview Technical Appendix for Outcome Measures This is a report on data used, and analyses done, by MPA Healthcare Solutions (MPA, formerly Michael Pine and Associates) for Consumers CHECKBOOK/Center
Study Overview Technical Appendix for Outcome Measures This is a report on data used, and analyses done, by MPA Healthcare Solutions (MPA, formerly Michael Pine and Associates) for Consumers CHECKBOOK/Center
Reimbursement Information for Diagnostic Ultrasound and Ultrasound-guided Procedures 1 Performed by Emergency Medicine Physicians
 GE Healthcare Reimbursement Information for Diagnostic Ultrasound and Ultrasound-guided Procedures 1 Performed by Emergency Medicine Physicians January, 2013 www.gehealthcare.com/reimbursement This overview
GE Healthcare Reimbursement Information for Diagnostic Ultrasound and Ultrasound-guided Procedures 1 Performed by Emergency Medicine Physicians January, 2013 www.gehealthcare.com/reimbursement This overview
Policy Brief June 2014
 Policy Brief June 2014 Which Medicare Patients Are Transferred from Rural Emergency Departments? Michelle Casey MS, Jeffrey McCullough PhD, and Robert Kreiger PhD Key Findings Among Medicare beneficiaries
Policy Brief June 2014 Which Medicare Patients Are Transferred from Rural Emergency Departments? Michelle Casey MS, Jeffrey McCullough PhD, and Robert Kreiger PhD Key Findings Among Medicare beneficiaries
2016 Community Service Plan & Community Health Improvement Plan
 2016 Community Service Plan & Community Health Improvement Plan A.O. Fox Memorial Hospital The Mary Imogene Bassett Hospital (dba: Bassett Medical Center) & Otsego County Health Department Service Area:
2016 Community Service Plan & Community Health Improvement Plan A.O. Fox Memorial Hospital The Mary Imogene Bassett Hospital (dba: Bassett Medical Center) & Otsego County Health Department Service Area:
Care Facilitation Quality Improvement Report
 Disease Management Program Clinical Outcomes for Reporting Period: 2006 Diabetes 100.0% 90.0% % of participants with diabetes 80.0% 70.0% 60.0% 50.0% 40.0% 30.0% 20.0% 10.0% 0.0% % participants with at
Disease Management Program Clinical Outcomes for Reporting Period: 2006 Diabetes 100.0% 90.0% % of participants with diabetes 80.0% 70.0% 60.0% 50.0% 40.0% 30.0% 20.0% 10.0% 0.0% % participants with at
Quality measures a for measurement year 2016
 Quality measures a for measurement year 2016 Measure Description Eligible members Childhood immunizations b Adolescent immunizations b Children who turned 2 during the measurement and who were identified
Quality measures a for measurement year 2016 Measure Description Eligible members Childhood immunizations b Adolescent immunizations b Children who turned 2 during the measurement and who were identified
Physician Profile. Revised For January 1, 2005 December 31, 2007
 Physician Profile Revised For January 1, 2005 December 31, 2007 Contents Physician Profile Overview... 3 Sub-specialty Definitions... 4 Cost of Care... 5 Definitions... 5 Notes... 5 Cost Comparison Report
Physician Profile Revised For January 1, 2005 December 31, 2007 Contents Physician Profile Overview... 3 Sub-specialty Definitions... 4 Cost of Care... 5 Definitions... 5 Notes... 5 Cost Comparison Report
Multi-Specialty Quality Measure Information Sheet 2017
 Prevention and Screening Adolescent Preventive Care Measures (APC) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
Prevention and Screening Adolescent Preventive Care Measures (APC) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
Integration of Specialty Care into ACOs: Considering JMAP and Beyond
 Integration of Specialty Care into ACOs: Considering JMAP and Beyond The Seventh National Accountable Care Organization Summit Scott A. Berkowitz MD MBA Senior Medical Director, Accountable Care, Johns
Integration of Specialty Care into ACOs: Considering JMAP and Beyond The Seventh National Accountable Care Organization Summit Scott A. Berkowitz MD MBA Senior Medical Director, Accountable Care, Johns
Target Performance. Category Weight. Available of Incentive Pool Particip ating PCPS & NPs 40+12
 # Measurement Level IHP Performance Measure Set Payment Distribution Formula Earn Condition Measure Data Source Primary Care Physicians Performance Number Available of Particip ating PCPS & NPs 40+12 Peds
# Measurement Level IHP Performance Measure Set Payment Distribution Formula Earn Condition Measure Data Source Primary Care Physicians Performance Number Available of Particip ating PCPS & NPs 40+12 Peds
Quality measures desktop reference for Medicaid providers
 Quality measures desktop reference for Medicaid providers providers.amerigroup.com Please note: The information provided is based on 2016 technical specifications and is subject to change based on guidance
Quality measures desktop reference for Medicaid providers providers.amerigroup.com Please note: The information provided is based on 2016 technical specifications and is subject to change based on guidance
Three Rules for Measuring Physician Market Share
 Crimson Market Advantage RESEARCH BRIEFING Three Rules for Measuring Physician Market Share Research and insights Performance Technologies Consulting and management Talent Development new definition Hospitals
Crimson Market Advantage RESEARCH BRIEFING Three Rules for Measuring Physician Market Share Research and insights Performance Technologies Consulting and management Talent Development new definition Hospitals
Peer Support Services Improve Clinical Outcomes by Fostering Recovery and Promoting Empowerment
 Peer Support Services Improve Clinical Outcomes by Fostering Recovery and Promoting Empowerment Optum has recognized the role of peer support services as an integral part of state Medicaid plans and has
Peer Support Services Improve Clinical Outcomes by Fostering Recovery and Promoting Empowerment Optum has recognized the role of peer support services as an integral part of state Medicaid plans and has
CASE-MIX ANALYSIS ACROSS PATIENT POPULATIONS AND BOUNDARIES: A REFINED CLASSIFICATION SYSTEM DESIGNED SPECIFICALLY FOR INTERNATIONAL USE
 CASE-MIX ANALYSIS ACROSS PATIENT POPULATIONS AND BOUNDARIES: A REFINED CLASSIFICATION SYSTEM DESIGNED SPECIFICALLY FOR INTERNATIONAL USE A WHITE PAPER BY: ROBERT MULLIN, MD JAMES VERTREES, PHD RICHARD
CASE-MIX ANALYSIS ACROSS PATIENT POPULATIONS AND BOUNDARIES: A REFINED CLASSIFICATION SYSTEM DESIGNED SPECIFICALLY FOR INTERNATIONAL USE A WHITE PAPER BY: ROBERT MULLIN, MD JAMES VERTREES, PHD RICHARD
Understanding Your Patient Care Opportunity Report (PCOR)
 Understanding Your Patient Care Opportunity Report (PCOR) Use your January/February 208 PCOR to help improve performance on Medicare Part D Clinical Star Ratings measures. Your January/February 208 Patient
Understanding Your Patient Care Opportunity Report (PCOR) Use your January/February 208 PCOR to help improve performance on Medicare Part D Clinical Star Ratings measures. Your January/February 208 Patient
Trending Determinations by Measure
 1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Parties FROM: Cindy Ottone, Director, Policy DATE: March 2019 RE: HEDIS 1 2019 Measure
1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Parties FROM: Cindy Ottone, Director, Policy DATE: March 2019 RE: HEDIS 1 2019 Measure
Analysis of Low-Value Health Services in the Minnesota All Payer Claims Database
 TECHNICAL SPECIFICATIONS AND METHODS SUPPLEMENT Analysis of Low-Value Health Services in the Minnesota All Payer Claims Database MAY 2017 Minnesota Department of Health Health Economics Program 85 E. 7th
TECHNICAL SPECIFICATIONS AND METHODS SUPPLEMENT Analysis of Low-Value Health Services in the Minnesota All Payer Claims Database MAY 2017 Minnesota Department of Health Health Economics Program 85 E. 7th
DIRECTORY Pharmacy
 2017 Pharmacy DIRECTORY This is a brief explanation and overview of the pharmacies members can use to get their prescription drugs. In a continued effort to offer our members value, pharmacies may be added
2017 Pharmacy DIRECTORY This is a brief explanation and overview of the pharmacies members can use to get their prescription drugs. In a continued effort to offer our members value, pharmacies may be added
2018 PHARMACY DIRECTORY
 2018 PHARMACY DIRECTORY This is a brief explanation and overview of the pharmacies members can use to get their prescription drugs. In a continued effort to offer our members value, pharmacies may be added
2018 PHARMACY DIRECTORY This is a brief explanation and overview of the pharmacies members can use to get their prescription drugs. In a continued effort to offer our members value, pharmacies may be added
Condition/Procedure Measure Compliance Criteria Reference Attribution Method
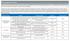 Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Potentially Preventable Hospitalizations in Pennsylvania
 Potentially Preventable Hospitalizations in Pennsylvania Pennsylvania Health Care Cost Containment Council June 2012 About PHC4 The Pennsylvania Health Care Cost Containment Council (PHC4) is an independent
Potentially Preventable Hospitalizations in Pennsylvania Pennsylvania Health Care Cost Containment Council June 2012 About PHC4 The Pennsylvania Health Care Cost Containment Council (PHC4) is an independent
2018 PHARMACY DIRECTORY
 2018 PHARMACY DIRECTORY This is a brief explanation and overview of the pharmacies members can use to get their prescription drugs. In a continued effort to offer our members value, pharmacies may be added
2018 PHARMACY DIRECTORY This is a brief explanation and overview of the pharmacies members can use to get their prescription drugs. In a continued effort to offer our members value, pharmacies may be added
2015 HCPro, a division of BLR. All rights reserved. These materials may not be duplicated without express written permission.
 A Matter of Life or Death: CDI Impact on Mortality Risk Adjustment Allison Clerval, RN, BSN, CCDS Kathleen Shindle, RN, BSN, CCDS Clinical Documentation Supervisors Thomas Jefferson University Hospital
A Matter of Life or Death: CDI Impact on Mortality Risk Adjustment Allison Clerval, RN, BSN, CCDS Kathleen Shindle, RN, BSN, CCDS Clinical Documentation Supervisors Thomas Jefferson University Hospital
Diabetes. Chronic Condition Clinical Advisory Group Value Based Payment Recommendation Report. NYS Medicaid Value Based Payment.
 Diabetes Chronic Condition Clinical Advisory Group Value Based Payment Recommendation Report September 2016 NYS Medicaid Value Based Payment Introduction Delivery System Reform Incentive Payment (DSRIP)
Diabetes Chronic Condition Clinical Advisory Group Value Based Payment Recommendation Report September 2016 NYS Medicaid Value Based Payment Introduction Delivery System Reform Incentive Payment (DSRIP)
Detroit: The Current Status of the Asthma Burden
 Detroit: The Current Status of the Asthma Burden Peter DeGuire, Binxin Cao, Lauren Wisnieski, Doug Strane, Robert Wahl, Sarah Lyon Callo, Erika Garcia, Michigan Department of Health and Human Services
Detroit: The Current Status of the Asthma Burden Peter DeGuire, Binxin Cao, Lauren Wisnieski, Doug Strane, Robert Wahl, Sarah Lyon Callo, Erika Garcia, Michigan Department of Health and Human Services
REIMBURSEMENT GUIDE. Sovereign. Spinal System
 REIMBURSEMENT GUIDE Sovereign Spinal System REIMBURSEMENT GUIDE The Sovereign Spinal System is indicated for use with autogenous bone graft in patients with degenerative disc disease The Sovereign Spinal
REIMBURSEMENT GUIDE Sovereign Spinal System REIMBURSEMENT GUIDE The Sovereign Spinal System is indicated for use with autogenous bone graft in patients with degenerative disc disease The Sovereign Spinal
Risk Adjustment and Hierarchical Condition Category Coding
 Risk Adjustment 101 Agenda Risk Adjustment Model Hierarchical Condition Categories (HCC) Patient Example Documentation MEAT Documentation Guidance Chronic Conditions Risk Score Calculations Steps for Physician
Risk Adjustment 101 Agenda Risk Adjustment Model Hierarchical Condition Categories (HCC) Patient Example Documentation MEAT Documentation Guidance Chronic Conditions Risk Score Calculations Steps for Physician
Care1st Health Plan Taking Quality to the Next Level REPORTING YEAR HEDIS Summary - MPL (Measurement Year 2012)
 Care1st Health Plan s Quality Improvement Department has been diligently working towards improving the Healthcare Effectiveness Data and Information Sets (HEDIS) results across all lines of business. HEDIS
Care1st Health Plan s Quality Improvement Department has been diligently working towards improving the Healthcare Effectiveness Data and Information Sets (HEDIS) results across all lines of business. HEDIS
B&T Format. New Measures. Better health care. Better choices. Better health.
 1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: August 13,
1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: August 13,
