Physician Profile. Revised For January 1, 2005 December 31, 2007
|
|
|
- Phoebe Edwina Carson
- 6 years ago
- Views:
Transcription
1 Physician Profile Revised For January 1, 2005 December 31, 2007
2 Contents Physician Profile Overview... 3 Sub-specialty Definitions... 4 Cost of Care... 5 Definitions... 5 Notes... 5 Cost Comparison Report Descriptions... 6 Generic Cost Comparison Report... 8 Methodology of Cost Comparison Report... 9 Quality of Care Measures...15 General Information...15 Health Conditions for Quality Measures...16 List of Quality Measures by Health Condition...16 Quality Measure Physician Profiles...19 Generic Quality Measure Physician Profile Additional Reporting for Cost Comparison Report...21 Additional Reporting for Quality Measure Report Appendix A...29 Appendix B...31 Appendix C...33
3 Physician Profile Overview Profiles include two components: 1) Cost Comparison Report Cost Comparison Profiles are generated for the following specialties: o Allergy/Immunology o Cardiology Invasive (cardiac catherizations) Interventional (stent and angioplasty) Electrophysiology Non-Invasive o Dermatology o Endocrinology o Family Medicine (Rural and Urban) o Gastroenterology o General Surgery (Rural and Urban) o Internal Medicine (Rural and Urban) o Neurology o Neurosurgery o Obstetrics/Gynecology o Ophthalmology o Otolaryngology o Pediatrics (Rural and Urban) o Pulmonary Medicine o Urology 2) Quality of Care Measures Quality of Care Profiles are generated for the following specialties: o Allergy/Immunology o Cardiology o Endocrinology o Primary Care (includes Family Medicine and Internal Medicine) o Neurology o Obstetrics/Gynecology o Ophthalmology o Otolaryngology o Pediatrics o Pulmonary Medicine o Urology Specialty Cost Comparison and Quality of Care reports contain data for the following product lines: 1) Health Advantage 2) Blue Cross 3) Blue Advantage
4 Subspecialty Definitions Urban/Rural Classification United States Census Bureau data is used to determine the population of each city. Urban: A classification code of U is assigned to the cities where the population is greater than 50,000 persons. Rural: A classification code of R is assigned to the cities where the population is less than 50,000 persons. Using the criteria put forth above these are the areas that are designated urban. All others are rural. City Conway Fayetteville Fort Smith Jonesboro Little Rock North Little Rock Memphis Pine Bluff Rogers Springdale Springfield Texarkana State TN MO /TX Cardiology subspecialties The rationale for splitting cardiology into distinct groups is the result of meetings held with three large central cardiology practices (Arkansas Heart, Little Rock Cardiology and Arkansas Cardiology.) The need to split the cardiologists was identified through the review of the Cost Efficiency Index initiative late 2007/early T-Tests were performed based on the efficiency index of the providers. Methodology: Cardiologists will be separated into the following groups based on the CPT codes in parentheses: Electrophysiology / Ablations ( ) >=1 during the measurement period Interventional ( ) >=5 during the measurement period Invasive ( ) >=5 during the measurement period Non-Invasive (all others) This process will be run every time we update physician Cost of Care information. The providers will be grouped based on the claims contained in the extract BEFORE the group and load process. Once the provider groups have been identified then their specialties must ALSO be changed in the master provider files that we run for CRMS. The process will be run in the order listed above. First, look for all claims specialty 06 (Cardiology) in the extract. If a provider has >=1 claim in the ablation CPT code range, they are included in the EP / ablation group. If not, then run a second pass thru the data to look for the interventional code range. If they have >=5 claims for interventional procedures then they are included in the interventional group. If not, then run a third pass thru the data to look for the invasive CPT code range. If they have >=5 claims in the invasive category then label them invasive. If not, the rest of the providers fall into the noninvasive group. The provider groups are mutually exclusive. A provider can only fall into one category. They are listed from most expensive to least expensive in terms of practice pattern. We want to ensure that we are grouping like providers together in terms of practice pattern cost, so the first category they meet the criteria for is where we will group them.
5 Cost of Care Definitions Episode - A series of health care services provided to a patient over time to treat a specific illness or condition (includes inpatient, outpatient, office, and pharmacy data). Episode Treatment Group (ETG) A classification system used to link a patient s health care services into episodes by categorizing the patient s condition or illness into one of 800+ clinically homogeneous groups. Episode Risk Group (ERG) - Uses episodes of care as markers of risk rather than the diagnoses from individual medical encounters so the focus is placed on the key information describing a patient's underlying condition instead of the individual services. Complete episode An episode not exceeding 365 days that has known start and finish dates. Also, a full year episode that may or may not have known or unknown start and finish dates. An example of a full year episode would be a patient with diabetes. Outlier Episode For a full explanation an outlier episode and how an outlier episode is identified, please see page 10 of this document under 3. Outliers and Exclusions. Notes Based on the Ingenix Episode Treatment Groups (ETGs) and Episode Risk Groups (ERG). For more information visit: ETG assignment is based upon diagnoses, procedures, complications, comorbidities, age and sex of the patient. An episode of care is initiated with an anchor record. An anchor record consists of an evaluation and management service or a defining surgery (can be facility service in absence of one of these two types of service). A patient can have multiple episodes open at the same time. Only complete episodes are included in the profiles. A provider must have at least 30 complete, non-outlier episodes in order for a profile to be generated. The portion of the complete episodes for which the provider was responsible (billed, ordered, or prescribed) is included in this report.
6 Cost Comparison Report Descriptions The Cost Comparison report shows the distribution of the case-mix (complexity of care) and the efficiency index (relative efficiency of managing cost) for a provider and the specialty peer group over a 3-year period. The report also compares the provider's average cost per episode for specific ETGs to that of the peer group. The costs can also be reviewed by type of service: ancillary (x-ray, lab, DME), facility (hospital and ASC charges), management (E&M visits), pharmacy (prescriptions), and surgical (surgery procedures). Report Heading This section of the report provides general information such as the dates of service, product lines included, physician s name, specialty to which the physician is compared, the physician s provider number, the region of the physician and the number of unique patients treated by the provider for the reported episodes. Cost Per Episode ETG Case-mix Index ETG Cost Index Cost Per Patient ERG Case-mix Index ERG Cost Index Provider's ETG case-mix index. The ETG case-mix index is a ratio that shows how complex the medical condition of a provider's patients are in relation to the peer group, based on the provider's mix of patients. (An ETG case-mix index greater than 1.0 indicates that the medical condition of the provider's patients are more complex than average within the peer group. An ETG case-mix index less than 1.0 indicates that the medical condition of the provider's patients are less complex than average within the peer group.) Provider's ETG cost index. The ETG cost index is a ratio that compares a provider's actual costs to expected costs, given the mix of patients. (An ETG cost index greater than 1.0 indicates that the provider's costs are higher than expected, given the case mix. An ETG cost index less than 1.0 indicates that the provider's costs are less than expected, given the case mix. ) Provider's ERG case-mix index. The ERG case-mix index is a ratio that shows how complex the medical condition of a provider's patients are in relation to the peer group, based on the provider's mix of patients. (A case-mix index greater than 1.0 indicates that the medical condition of the provider's patients are more complex than average within the peer group. A case-mix index less than 1.0 indicates that the medical condition of the provider's patients are less complex than average within the peer group.) Provider's ERG cost index. The ERG cost index is a ratio that compares a provider's actual costs to expected costs, given the mix of patients. (An ERG cost index greater than 1.0 indicates that the provider's costs are higher than expected, given the case mix. An ERG cost index less than 1.0 indicates that the provider's costs are less than expected, given the case mix. ) Cost of Care Index and Graph The graph is a symbolic view of the Cost of Care Index and is what is reported on the secured member websites under Physician Connection for this provider (NOTE: provider has the option to suppress his Cost of Care Index graph on the website). Note The statistical results are located under the Cost Index for each category and are based on one-sample, two-sided Z-test. See the Physician Connection Cost Comparison Methodology section for the calculation of the cost and case-mix indexes.
7 Overall Cost Comparison for Provider and Top ETGs by Number of Episodes The information in the header section of the report can be used to determine whether the provider generates higher or lower costs than peers for all of the physician s episodes. The next section provides information on the treatment of conditions within specific ETGs and lists the top six ETGs with non-outlier episodes. Field ETG Description Description Identifying number of the non-outlier Episode Treatment Group. Description of the Episode Treatment Group. # Episodes Number of non-outlier episodes within the ETG in which the provider was involved. Your Excess Costs (Savings) Your cost per episode Spec Avg per episode Difference in cost for the non-outlier episodes as compared to the specialty for the ETG. Provider's average allowed cost per non-outlier episode for all medical and pharmacy claims from all sites of service for the ETG. The average allowed cost for each type of service for the physician is also provided. Specialty's average allowed cost per non-outlier episode for all medical and pharmacy claims from all sites of service for the ETG. The average allowed cost for each type of service for the physician s specialty is also provided.
8 INTERNAL USE ONLY
9 Quality of Care Measures: General Information This initiative has been driven by the federal government s commitment to promote transparent and higher quality health care. Specifically, the Bush administration has mandated that federal health-care agencies must implement programs measuring and comparing quality and cost of physician services. In addition, many employers have requested quality and cost information for the physicians in the networks utilized for their employee health-benefit plans. Consumers also are requesting more cost and quality information, especially with the growth of consumer-directed health plans. Goals and Objectives for Quality Measures Educate members (in lay terms) on quality measures and how Arkansas physicians perform statewide Educate members on individual cost performance of network physicians and identify those physicians who are working to keep medical costs down Through new physician profiles, educate physicians on their specific quality and cost performance compared to peer benchmarks Link quality measures with care reminders for measurement consistency and to add value to the Personal Health Record Selecting Key Performance Indicators Measures drawn from nationally accepted standards Measures with broad clinical acceptance Measures provide stable and reliable information Inform physicians about the development and validation of the measures, and give physicians the opportunity to provide feedback We favored process measures that are under control of the physician and are clearly linked to patient outcomes The measures were derived from claims data and not medical review of patient charts We used a method of generous attribution to all physicians treating the patient if any physician performed the health intervention, then all treating physicians were acknowledged as having performed the intervention Development and Validation Started with 140 MedVantage measures Selected 53 measures (12 specialties) Nationally accepted standards: o AQA (formerly the Ambulatory Care Quality Alliance) o National Quality Forum o National Committee for Quality Assurance o American Medical Association (AMA) o American College of Physicians o Agency for Healthcare Research and Quality o Healthcare Effectiveness Data and Information Set Extensive review of current guidelines of major specialty associations (American College of Cardiology, American College of Radiology, AMA, etc) Available from claims based data Multi-specialty University Medical School Advisory Group (selected by Dean) College of Public Health Arkansas American Academy of Pediatrics Arkansas American Academy of Obstetrics and Gynecology QIO: Arkansas Foundation for Medical Care CMS: Physician Quality Reporting Initiative
10 Health Conditions for Quality Measures The quality of care measures are divided up into the following health conditions. This allows for the member to search for quality measures by health condition as well as by physician specialty. Coronary (Heart) Conditions Diabetes Drug Monitoring Ear, Nose, Throat Conditions Eye Conditions Neurological Conditions Pregnancy Respiratory Conditions Thyroid Condition Urologic Conditions Wellness screening Quality Measures for Physician Connection by Health Condition Coronary (Heart) Conditions Proportion of CAD patients who receive at least one blood glucose test over the 3 year measurement period. Proportion of MI patients who persist in anti-lipidemic agents. Proportion of MI patients who persist in B-blocker use (>135 days of B-blocker use in 180 days following discharge). Exclusions: Hypotension, conduction system disorder, asthma, COPD Proportion of patients who receive a B-blocker after an acute MI. (Exclusions: Hypotension, conduction system disorder, asthma, COPD) Proportion of patients who receive a lipid panel within 12 months of discharge after admit for CAD, MI, CABG, or PTCA. Proportion of patients with LVSD who receive a prescription for a B-blocker. (Exclusions: Hypotension, conduction system disorder, asthma, COPD) Proportion of patients with LVSD who receive a prescription for an ACEI or B. (Exclusions: Hypotension, chronic renal disease) Diabetes Proportion of diabetics age who received at least one eye exam annually. Proportion of diabetics who receive at least one creatinine within 12 months of care. Proportion of diabetics who receive at least one HbA1c during every 12 months of care. Proportion of diabetics who receive at least one lipid measurement. Proportion of diabetics who receive at least one microalbumin (or are already taking ACEI or B) within 12 months of care. Proportion of patients with diabetes and hypertension treated with ACE-I or B. Proportion of patients with diagnosis of impaired glucose or dysmetabolic syndrome who receive follow-up blood sugar.
11 Drug Monitoring Proportion of patients on diuretics who receive at least one K+ during every 12 months following initiation of therapy. Proportion of patients on methotrexate therapy who receive at least one liver function test and CBC annually. Proportion of patients with Rx for ACE-I or B who have K+ and creatinine or BUN annually. Ear, Nose & Throat Conditions Proportion of patients who receive strept test within 3 days (before or after) antibiotics for pharyngitis. Proportion of tonsillectomy patients who had at least 3 scripts for antibiotics in previous 12 months. Eye Conditions Proportion of patients with a diagnosis for open angle glaucoma that have a follow-up visit during measurement period. (Exclusions: Retinal and Ophthalmic Plastic Specialists) Proportion of patients with a diagnosis of diabetic retinopathy that have a follow-up visit at least once during measurement period. (Exclusions: Retinal and Ophthalmic Plastic Specialists) Proportion of patients with glaucoma who have at least one optic nerve exam and visual field during the measurement period. Proportion of patients with no YAG capsulotomy within 3 months after cataract surgery. (Exclusions: Retinal and Ophthalmic Plastic Specialists) Neurological Conditions Percentage of out-patients with TIA or stroke who receive at least one lipid profile. Proportion of headache/migraine patients who do not receive long term narcotics or barbiturates. Proportion of out-patients with new TIA who receive appropriate evaluations. Acceptable evaluations: Transcranial Doppler, Carotid U.S., Carotid Duplex U.S. Pregnancy Proportion of pregnant patients who receive chlamydia screening. Proportion of pregnant women screened for UTI or Asymptomatic bacteriuria. Proportion of pregnant women who are screened for anemia. Proportion of pregnant women who receive Group B strept screening. Proportion of pregnant women who receive Hep B screening. Proportion of pregnant women who receive HIV screening. Proportion of pregnant women who receive pap smear (credit for PAP smear one year prior to or during pregnancy). Respiratory Conditions Proportion of adult out-patients with pneumonia who receive a CXR within 3 days of course of treatment begin date. Proportion of asthma patients who do not overuse short acting B agonists. (Exclusion: COPD) Proportion of asthma patients who receive inhaled steroid before long acting beta agonists. (Exclusion: Exercise induced asthma) Proportion of patients undergoing allergy testing for allergic rhinitis who receive intranasal steroids, or other appropriate medications: cromolyn sulfate, oral anti-histamines, leukotriene modifier
12 Proportion of patients who receive no antibiotics for at least 3 days after initial visit for uncomplicated URI. Proportion of patients with both allergic rhinitis and asthma who receive at least one script for intranasal steroids. (Exclusion: Immunotherapy) Proportion of patients with persistent asthma who are prescribed inhaled steroids or an acceptable alternative for asthma control. (Exclusions: COPD, emphysema) Thyroid Condition Proportion of patients on thyroid replacement medication who receive at least one TSH. Urologic Conditions Proportion of out-patients with pyelonephritis who receive a urine culture within 2 days of diagnosis. Proportion of patients with kidney stone and UTI who receive urine culture. Proportion of patients with kidney stone treated with watchful waiting. No SWL, URS or PNL during the first 7 days. (Exclusions: Stricture or complete obstruction) Proportion of patients with kidney stones who receive U.A. and BUN or creatinine. Proportion of patients with prostate cancer who receive at least one PSA after DX of prostate cancer. Proportion of patients with ureteral stones who do not receive a stent within seven days of diagnosis. (Exclusions: UTI, abscess) Wellness Screening Proportion of high risk patients age 35 or older who receive at least one cholesterol level during the three year measurement period. High Risk = CAD, Family History MI, Hypertension, Diabetes, PVD or AAA. Proportion of patients at high risk for renal failure who receive a creatinine or 24 hour urine study during the three year measurement period. High Risk = CHF, HTN, or Diabetes Proportion of patients who receive colon cancer screening within 12 months of turning 50. Screening Exams: FOBT, Sigmoidoscopy, Colonoscopy, Air Contrast BE. Proportion of women age to receive at least one pap smear over 3 year measurement period. (Exclusion: Hysterectomy) Proportion of women age who receive at least one mammogram every 2 years. (Exclusion: Bilateral Mastectomy) Proportion of women age who receive at least one mammogram annually. (Exclusion: Bilateral Mastectomy)
13 Quality Measure Profiles The Quality Measure report shows the number of treatment opportunities and the number of opportunities that met the measure criteria for the provider and the specialty peer group. The report also shows the physician s adherence compared to the specialty peer group adherence to the measure. Report Heading This section of the report provides general information such as the dates of service, product lines included, physician s name, specialty to which the physician is compared, the physician s provider number, and the region of the physician. The report (example below) shows each of the measure in each of the Health Conditions for that provider. The following information is shown on the individual physician s quality report: Measure Number Measure Description # of Physician s Patients Meeting Criteria o Number of Patients meeting the measure o Total Number of Patients # of Specialty s Patients Meeting Criteria o Number of Patients meeting the measure o Total Number of Patients Physician Compliance Specialty Compliance
14
Clinical Quality Measures Summary of Upcoming Enhancements
 Upcoming coding enhancements will impact the logic behind the clinical quality indicators applicable to your practice specialty. Please refer to this grid for a summary of the coding enhancements and some
Upcoming coding enhancements will impact the logic behind the clinical quality indicators applicable to your practice specialty. Please refer to this grid for a summary of the coding enhancements and some
OCHSNER PHYSICIAN PARTNERS. PQRS Measures by Specialty (FINAL)
 OCHSNER PHYSICIAN PARTNERS PQRS Measures by Specialty (FINAL) Allergy and Immunology 2. Asthma: Pharmacologic Therapy for Persistent Asthma - Ambulatory Care Setting (PQRS 53) 3. Patients aged 18 years
OCHSNER PHYSICIAN PARTNERS PQRS Measures by Specialty (FINAL) Allergy and Immunology 2. Asthma: Pharmacologic Therapy for Persistent Asthma - Ambulatory Care Setting (PQRS 53) 3. Patients aged 18 years
The BlueCompare SM Physician Designation Program
 The BlueCompare SM Physician Designation Program Continuing escalation of health care costs has driven premiums and medical expenses to higher and higher levels each year, motivating employers and consumers
The BlueCompare SM Physician Designation Program Continuing escalation of health care costs has driven premiums and medical expenses to higher and higher levels each year, motivating employers and consumers
CLINICAL PROCESS IMPROVEMENT INITIATIVE (CPII) EFFICIENCY REPORT EXPLANATION January 4, 2016
 CLINICAL PROCESS IMPROVEMENT INITIATIVE (CPII) EFFICIENCY REPORT EXPLANATION January 4, 2016 WHAT IS AN EPISODE OF CARE? An episode of care is a grouping of a patient s health care claims for a unique
CLINICAL PROCESS IMPROVEMENT INITIATIVE (CPII) EFFICIENCY REPORT EXPLANATION January 4, 2016 WHAT IS AN EPISODE OF CARE? An episode of care is a grouping of a patient s health care claims for a unique
proposed set to a required subset of 3 to 5 measures based on the availability of electronic
 CMS-0033-P 143 proposed set to a required subset of 3 to 5 measures based on the availability of electronic measure specifications and comments received. We propose to require for 2011 and 2012 that EP's
CMS-0033-P 143 proposed set to a required subset of 3 to 5 measures based on the availability of electronic measure specifications and comments received. We propose to require for 2011 and 2012 that EP's
Patient-Centered Primary Care Scorecard Measures
 Patient-Centered Primary Care Scorecard Measures Acute and Chronic Care Management Measures Medication Adherence Proportion of Days Covered (PDC): Oral Diabetes Identifies patients with at least two prescriptions
Patient-Centered Primary Care Scorecard Measures Acute and Chronic Care Management Measures Medication Adherence Proportion of Days Covered (PDC): Oral Diabetes Identifies patients with at least two prescriptions
IHA P4P Measure Manual Measure Year Reporting Year 2018
 ADULT PREVENTIVE CARE IHA P4P Measure Manual Measure Year 2017 - Reporting Year 2018 *If line of business not labeled, measure is Commercial only Adult BMI (Medicare) 18-74 Medicare members ages 18-74
ADULT PREVENTIVE CARE IHA P4P Measure Manual Measure Year 2017 - Reporting Year 2018 *If line of business not labeled, measure is Commercial only Adult BMI (Medicare) 18-74 Medicare members ages 18-74
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications
 HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications Fidelis SecureCare strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications Fidelis SecureCare strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
Quality measures a for measurement year 2016
 Quality measures a for measurement year 2016 Measure Description Eligible members Childhood immunizations b Adolescent immunizations b Children who turned 2 during the measurement and who were identified
Quality measures a for measurement year 2016 Measure Description Eligible members Childhood immunizations b Adolescent immunizations b Children who turned 2 during the measurement and who were identified
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual
 Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Total Health Quality Indicators For Providers 2018
 Well Adult Well Visit 20 yrs > Yearly 99385-87, 99395-97, G0402, G0438, G0439, G0463 Total Health Quality Indicators For Providers 2018 Adult- Preventive Z00.00 Report ALL components of an annual visit
Well Adult Well Visit 20 yrs > Yearly 99385-87, 99395-97, G0402, G0438, G0439, G0463 Total Health Quality Indicators For Providers 2018 Adult- Preventive Z00.00 Report ALL components of an annual visit
Key Quality of Care Measures. Blue Cross Blue Shield of Michigan Traditional, PPO and POS Members. Fourth Quarter 2003
 Key Quality of Care Measures Blue Cross Blue Shield of Michigan Traditional, PPO and POS Members Fourth Quarter 2003 Blue Cross Blue Shield of Michigan is a nonprofit corporation and independent licensee
Key Quality of Care Measures Blue Cross Blue Shield of Michigan Traditional, PPO and POS Members Fourth Quarter 2003 Blue Cross Blue Shield of Michigan is a nonprofit corporation and independent licensee
Multi-Specialty Quality Measure Information Sheet 2017
 Prevention and Screening Adolescent Preventive Care Measures (APC) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
Prevention and Screening Adolescent Preventive Care Measures (APC) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
MU - Selection & Configuration of Measures
 MU - Selection & Configuration of Measures Presenter: Christy Erickson October 14, 2011 Objectives Review the 15 Core Measures and highlight some findings from the field Discuss the MU Menu and Clinical
MU - Selection & Configuration of Measures Presenter: Christy Erickson October 14, 2011 Objectives Review the 15 Core Measures and highlight some findings from the field Discuss the MU Menu and Clinical
Impact of WRVU Changes. Allowed Charges (Millions)
 Key Financial and Operational s from the Proposed 2018 PFS Rule: The 2018 Physician Fee Schedule (PFS) proposed rule was made available on July 13, 2018. A detailed summary of the rule will be available
Key Financial and Operational s from the Proposed 2018 PFS Rule: The 2018 Physician Fee Schedule (PFS) proposed rule was made available on July 13, 2018. A detailed summary of the rule will be available
Care1st Health Plan Taking Quality to the Next Level REPORTING YEAR HEDIS Summary - MPL (Measurement Year 2012)
 Care1st Health Plan s Quality Improvement Department has been diligently working towards improving the Healthcare Effectiveness Data and Information Sets (HEDIS) results across all lines of business. HEDIS
Care1st Health Plan s Quality Improvement Department has been diligently working towards improving the Healthcare Effectiveness Data and Information Sets (HEDIS) results across all lines of business. HEDIS
Patient-Centered Primary Care Scorecard Measure Specifications
 Patient-Centered Primary Care Scorecard Measure Specifications Disclaimer of Currency: Material Owner documentation reflects the state of products, software, reports, and procedures as of the publication
Patient-Centered Primary Care Scorecard Measure Specifications Disclaimer of Currency: Material Owner documentation reflects the state of products, software, reports, and procedures as of the publication
Anthem Blue Precision Quality Designation Methodology Summary 2017
 This document outlines Anthem s Blue Precision methodology for measuring Physician Quality. Anthem has physician quality transparency programs for physicians practicing in the following specialties: Allergy/Immunology,
This document outlines Anthem s Blue Precision methodology for measuring Physician Quality. Anthem has physician quality transparency programs for physicians practicing in the following specialties: Allergy/Immunology,
Meaningful Use Overview
 Eligibility Providers may be eligible for incentives from either Medicare or Medicaid, but not both. In addition, providers may not be hospital based. Medicare: A Medicare Eligible Professional (EP) is
Eligibility Providers may be eligible for incentives from either Medicare or Medicaid, but not both. In addition, providers may not be hospital based. Medicare: A Medicare Eligible Professional (EP) is
Commercial Business Measurement Period Handbook For Patient-Centered Primary Care
 Commercial Business Measurement Period Handbook For Patient-Centered Primary Care Measurement Period beginning: 07/01/16 CB Version 070116 V1 Introduction: Welcome to your Commercial Business Measurement
Commercial Business Measurement Period Handbook For Patient-Centered Primary Care Measurement Period beginning: 07/01/16 CB Version 070116 V1 Introduction: Welcome to your Commercial Business Measurement
For Electronic Measure Specification Information go to:
 Diabetes Recognition NQF 0421 PQRI 128 Title: Adult Weight Screening and Follow-Up Description: Percentage of patients aged 18 years and older with a calculated BMI in the past six months or during the
Diabetes Recognition NQF 0421 PQRI 128 Title: Adult Weight Screening and Follow-Up Description: Percentage of patients aged 18 years and older with a calculated BMI in the past six months or during the
NQF Measure Number & PQRI Implementation Number
 Title NQF Steward s Adult Weight Screening and Follow-Up Hypertension: Blood Pressure ment Preventive Care and Screening Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention with a calculated
Title NQF Steward s Adult Weight Screening and Follow-Up Hypertension: Blood Pressure ment Preventive Care and Screening Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention with a calculated
Meaningful Use Clinical Quality Measures for Eligible Professionals
 Meaningful Use Clinical Quality Measures for Eligible Professionals Measure Type NQF ID CMS ID Description Title: Adult Weight Screening and Follow-Up 1 NQF 0421 PQRI 128 calculated BMI in the past six
Meaningful Use Clinical Quality Measures for Eligible Professionals Measure Type NQF ID CMS ID Description Title: Adult Weight Screening and Follow-Up 1 NQF 0421 PQRI 128 calculated BMI in the past six
Trends in Health Plan Design: High Performance Networks. John Bertko, F.S.A., MAAA Vice President and Chief Actuary Humana Inc July 28, 2005
 Trends in Health Plan Design: High Performance Networks John Bertko, F.S.A., MAAA Vice President and Chief Actuary Humana Inc July 28, 2005 1 Overview What is a High Performance Network (HPN) Tighter network
Trends in Health Plan Design: High Performance Networks John Bertko, F.S.A., MAAA Vice President and Chief Actuary Humana Inc July 28, 2005 1 Overview What is a High Performance Network (HPN) Tighter network
Clinical Quality Measures for Submission by Medicare or Medicaid EP/s for the 2011 and 2012 Payment Year
 1 NQF 0059 1 NQF 0064 2 NQF 0061 3 Title: Diabetes: Hemoglobin A1c Poor Control Description: Percentage of patients 18-75 years of age with diabetes (type 1 or type 2) who had hemoglobin A1c > 9.0%. Title:
1 NQF 0059 1 NQF 0064 2 NQF 0061 3 Title: Diabetes: Hemoglobin A1c Poor Control Description: Percentage of patients 18-75 years of age with diabetes (type 1 or type 2) who had hemoglobin A1c > 9.0%. Title:
Clinical Quality Measures
 Core Measures Preventive Care and Screening Measure Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention. Percentage of patients aged 18 years and older who have been seen for at least 2
Core Measures Preventive Care and Screening Measure Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention. Percentage of patients aged 18 years and older who have been seen for at least 2
The clinical quality measures as selected by the Clinical Management subcommittee for 2016 for the adult population are:
 For 2016 the Clinical Integration Program is moving its clinical quality measures from the Verisk Healthcare Quality and Risk Measures to the National Committee for Quality Assurance HEDIS based measures.
For 2016 the Clinical Integration Program is moving its clinical quality measures from the Verisk Healthcare Quality and Risk Measures to the National Committee for Quality Assurance HEDIS based measures.
HEDIS. Quick Reference Guide. For more information, visit
 HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2018 Technical Specifications Michigan Complete Health strives to provide
HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2018 Technical Specifications Michigan Complete Health strives to provide
HEDIS. Quick Reference Guide. For more information, visit
 HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2017 Technical Specifications Michigan Complete Health Medicare-Medicaid Plan
HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2017 Technical Specifications Michigan Complete Health Medicare-Medicaid Plan
Healthcare Effectiveness Data and Information Set Quality Assurance Reporting Requirements
 HEDIS/QARR Healthcare Effectiveness Data and Information Set Quality Assurance Reporting Requirements 2015 Quick Reference Guide ADULTS Avoidance of Antibiotic Treatment in Adults with Acute Bronchitis
HEDIS/QARR Healthcare Effectiveness Data and Information Set Quality Assurance Reporting Requirements 2015 Quick Reference Guide ADULTS Avoidance of Antibiotic Treatment in Adults with Acute Bronchitis
Transparency The Public Reporting of Physician Performance
 (The Evaluation of the Impact of Physician Self-Reporting Administrative Data) Dr. Allen Naidoo PhD Director-Medical Informatics BlueCross and BlueShield of Tennessee Dr. Marc Loizeaux PhD Manager-Provider
(The Evaluation of the Impact of Physician Self-Reporting Administrative Data) Dr. Allen Naidoo PhD Director-Medical Informatics BlueCross and BlueShield of Tennessee Dr. Marc Loizeaux PhD Manager-Provider
MEASURING CARE QUALITY
 MEASURING CARE QUALITY Region December 2013 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
MEASURING CARE QUALITY Region December 2013 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
Quality Corp Measures Description and Methodologies
 Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
Quality Corp Measures Description and Methodologies
 Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
Quality Corp Measures Description and Methodologies Overview: The Oregon Health Care Quality Corporation (Q Corp) is dedicated to improving the quality and affordability of health care in Oregon by leading
Provider Perspective of Quality Measurement
 Provider Perspective of Quality Measurement The American Medical Group Association supports its members in enhancing population health and care for patients through integrated systems of care Improve
Provider Perspective of Quality Measurement The American Medical Group Association supports its members in enhancing population health and care for patients through integrated systems of care Improve
HEDIS Documentation and Coding Adult Guidelines 2017
 HEDIS Documentation and Coding Adult Guidelines 2017 Reproduced with permission from HEDIS 2017, Volume 2: Technical Specifications for Health Plans by the National Committee for Quality Assurance (NCQA).
HEDIS Documentation and Coding Adult Guidelines 2017 Reproduced with permission from HEDIS 2017, Volume 2: Technical Specifications for Health Plans by the National Committee for Quality Assurance (NCQA).
QUALITY IMPROVEMENT Section 9
 Quality Improvement Program The Plan s Quality Improvement Program serves to improve the health of its members through emphasis on health maintenance, education, diagnostic testing and treatment. The Quality
Quality Improvement Program The Plan s Quality Improvement Program serves to improve the health of its members through emphasis on health maintenance, education, diagnostic testing and treatment. The Quality
Cigna Care Designation and Physician Quality and Cost-Efficiency Displays 2016 Methodologies Whitepaper
 Cigna Care Designation and Physician Quality and Cost-Efficiency Displays 2016 Methodologies Whitepaper For Health Care Professionals February 2016 Introduction... 2 Cigna Physician Quality and Cost-Efficiency
Cigna Care Designation and Physician Quality and Cost-Efficiency Displays 2016 Methodologies Whitepaper For Health Care Professionals February 2016 Introduction... 2 Cigna Physician Quality and Cost-Efficiency
ABCBS PCMH Specifications. ARKANSAS BLUE CROSS and BLUE SHIELD An Independent Licensee of the Blue Cross and Blue Shield Association
 ABCBS PCMH 2016 Specifications An Independent Licensee of the Blue Cross and Blue Shield Association Table of Contents I. Terminology 3 II. Transformation Activities 2016 List of Activities 4 3 month 5-9
ABCBS PCMH 2016 Specifications An Independent Licensee of the Blue Cross and Blue Shield Association Table of Contents I. Terminology 3 II. Transformation Activities 2016 List of Activities 4 3 month 5-9
CLINICAL QUALITY MEASURES Stage 1 Meaningful Use
 CLINICAL QUALITY MEASURES Stage 1 Meaningful Use * Eligible professionals (EPs) must report on 3 required core clinical quality measures (CQMs). If the denominator of 1 or more of the required core measures
CLINICAL QUALITY MEASURES Stage 1 Meaningful Use * Eligible professionals (EPs) must report on 3 required core clinical quality measures (CQMs). If the denominator of 1 or more of the required core measures
Family Medicine Clerkship. Learning Prompts
 Family Medicine Clerkship Learning Prompts 9 SYSTEMS & CONDITIONS Respiratory conditions................................. 1 COPD Asthma Infectious diseases.................................... 2 Sore throat
Family Medicine Clerkship Learning Prompts 9 SYSTEMS & CONDITIONS Respiratory conditions................................. 1 COPD Asthma Infectious diseases.................................... 2 Sore throat
HEDIS Adult. Documentation and Coding Guidelines Medical record documentation required. Measure description. Coding ICD-10: Z68.1 Z68.45, Z68.
 HEDIS Adult Documentation and Guidelines 2017 description Adult BMI Assessment (ABI) Members 18 74 years of age who had an outpatient visit and whose body mass index (BMI) was documented during the measurement
HEDIS Adult Documentation and Guidelines 2017 description Adult BMI Assessment (ABI) Members 18 74 years of age who had an outpatient visit and whose body mass index (BMI) was documented during the measurement
Supplementary Online Content
 Supplementary Online Content Friedberg MW, Rosenthal MB, Werner RM, Volpp KG, Schneider EC. Effects of a medical home and shared savings intervention on quality and utilization of care. Published online
Supplementary Online Content Friedberg MW, Rosenthal MB, Werner RM, Volpp KG, Schneider EC. Effects of a medical home and shared savings intervention on quality and utilization of care. Published online
PCMH 2018 Enrollment and Update August 25, 2017
 PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
Letter to the AMGA Board of Directors... 1 Introduction... 3
 Table of Contents Letter to the AMGA Board of Directors... 1 Introduction... 3 Section I: Executive Summary Survey at a Glance... 6 Participant Profile... 10 Survey Methodology... 19 How to Use This Report...
Table of Contents Letter to the AMGA Board of Directors... 1 Introduction... 3 Section I: Executive Summary Survey at a Glance... 6 Participant Profile... 10 Survey Methodology... 19 How to Use This Report...
Letter to the AMGA Board of Directors...1 Introduction...3
 Table of Contents Letter to the AMGA Board of Directors...1 Introduction...3 Section I: Executive Summary Survey at a Glance...6 Participant Profile...10 Survey Methodology...18 How to Use This Report...21
Table of Contents Letter to the AMGA Board of Directors...1 Introduction...3 Section I: Executive Summary Survey at a Glance...6 Participant Profile...10 Survey Methodology...18 How to Use This Report...21
2017 HEDIS Measures. PREVENTIVE SCREENING 2017 Measure Quality Indicator
 PREVENTIVE SCREENING Childhood Immunization Children who turn 2 during the Adolescent Immunization Adolescents who turn 13 during the Lead Screening Children who turn 2 during the Breast Cancer Screening
PREVENTIVE SCREENING Childhood Immunization Children who turn 2 during the Adolescent Immunization Adolescents who turn 13 during the Lead Screening Children who turn 2 during the Breast Cancer Screening
2018 P4P Overview 0518.PR.P.PP.1 6/18
 2018 P4P Overview Agenda MHS Pay For Performance (P4P) Ambetter P4P Program Secure Web Reporting Question and Answer What You Will Learn 1. Measure Overviews & Specifications 2. Documentation Requirements
2018 P4P Overview Agenda MHS Pay For Performance (P4P) Ambetter P4P Program Secure Web Reporting Question and Answer What You Will Learn 1. Measure Overviews & Specifications 2. Documentation Requirements
M4 Coursework Information
 M4 Coursework Information This guide is intended to assist students in selecting and scheduling courses based upon their specialty of interest. Contents ANESTHESIOLOGY... 1 DERMATOLOGY... 2 EMERGENCY MEDICINE...
M4 Coursework Information This guide is intended to assist students in selecting and scheduling courses based upon their specialty of interest. Contents ANESTHESIOLOGY... 1 DERMATOLOGY... 2 EMERGENCY MEDICINE...
Letter to the AMGA Board of Directors... 1 Introduction... 3
 Table of Contents Letter to the AMGA Board of Directors... 1 Introduction... 3 Section I: Executive Summary Survey at a Glance... 6 Participant Profile... 10 Survey Methodology... 19 How to Use This Report...
Table of Contents Letter to the AMGA Board of Directors... 1 Introduction... 3 Section I: Executive Summary Survey at a Glance... 6 Participant Profile... 10 Survey Methodology... 19 How to Use This Report...
Total Health Quality Indicators For Providers 2017
 Well Adult Well Visit 20 yrs > Yearly 99385-87, 99395-97, G0402, G0438, G0439, G0463 Total Health Quality Indicators For Providers 2017 Adult- Preventive Z00.00 Report ALL components of an annual visit
Well Adult Well Visit 20 yrs > Yearly 99385-87, 99395-97, G0402, G0438, G0439, G0463 Total Health Quality Indicators For Providers 2017 Adult- Preventive Z00.00 Report ALL components of an annual visit
Certified Health IT Transparency and Disclosure Information 2014 Edition
 Certified Health IT Transparency and Disclosure Information 2014 Edition 2015 Edition Certified Health IT Transparency and Disclosure Information I. Disclaimer This Complete EHR is 2014 Edition compliant
Certified Health IT Transparency and Disclosure Information 2014 Edition 2015 Edition Certified Health IT Transparency and Disclosure Information I. Disclaimer This Complete EHR is 2014 Edition compliant
HEALTHCARE EFFECTIVENESS DATA AND INFORMATION SET (HEDIS )
 STARS MEASURES 2015 HEALTHCARE EFFECTIVENESS DATA AND INFORMATION SET (HEDIS ) Developed by the National Committee for Quality Assurance (NCQA), HEDIS is the most widely used set of performance measures
STARS MEASURES 2015 HEALTHCARE EFFECTIVENESS DATA AND INFORMATION SET (HEDIS ) Developed by the National Committee for Quality Assurance (NCQA), HEDIS is the most widely used set of performance measures
UnitedHealth Premium Program Case-mix Adjusted Benchmarks with Severity or Risk Adjustment
 UnitedHealth Premium Program Case-mix Adjusted Benchmarks with Severity or Risk Adjustment Resources u Phone: 866-270-5588 u u Website: UHCprovider.com/Premium Mail: UnitedHealthcare - UnitedHealth Premium
UnitedHealth Premium Program Case-mix Adjusted Benchmarks with Severity or Risk Adjustment Resources u Phone: 866-270-5588 u u Website: UHCprovider.com/Premium Mail: UnitedHealthcare - UnitedHealth Premium
SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES
 Summary Table of Measures, Product Lines and Changes 1 SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES General Guidelines for Data Collection and Reporting Guidelines for Calculations and Sampling
Summary Table of Measures, Product Lines and Changes 1 SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES General Guidelines for Data Collection and Reporting Guidelines for Calculations and Sampling
Now iknow SM : Frequently Asked Questions
 Now iknow SM : Frequently Asked Questions Overview Beginning December 2013, Harvard Pilgrim in partnership with Castlight Health, a leader in health care transparency will introduce a new online health
Now iknow SM : Frequently Asked Questions Overview Beginning December 2013, Harvard Pilgrim in partnership with Castlight Health, a leader in health care transparency will introduce a new online health
Arizona Clover Health Choice PPO (040) 2019 Medical Benefits
 Arizona 2019 Medical Benefits Effective Date: 1/1/2019 Version 1.0 Part D Deductible For Part D Copay information, see page 26. /year for Part D prescription drugs /year for Part D prescription drugs Out-of-Pocket
Arizona 2019 Medical Benefits Effective Date: 1/1/2019 Version 1.0 Part D Deductible For Part D Copay information, see page 26. /year for Part D prescription drugs /year for Part D prescription drugs Out-of-Pocket
MEASURING CARE QUALITY
 MEASURING CARE QUALITY Region November 2016 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
MEASURING CARE QUALITY Region November 2016 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
Tusculum College. Benefit Summary Option/Quote: 2. 30% after Deductible. $35 Copay. 30% after Deductible
 Benefit Plan Features: Annual Deductible Effective Date: 4/1/2018 Network: S Benefit Summary Option/Quote: 2 Your Cost In-Network Individual/Family $1250/$2500 Annual Out-of-Pocket Maximum Tusculum College
Benefit Plan Features: Annual Deductible Effective Date: 4/1/2018 Network: S Benefit Summary Option/Quote: 2 Your Cost In-Network Individual/Family $1250/$2500 Annual Out-of-Pocket Maximum Tusculum College
Letter to the AMGA Board of Directors...1 Introduction...3
 Table of Contents Letter to the AMGA Board of Directors...1 Introduction...3 Section I: Executive Summary Survey at a Glance...6 Participant Profile...10 Survey Methodology...18 How to Use This Report...21
Table of Contents Letter to the AMGA Board of Directors...1 Introduction...3 Section I: Executive Summary Survey at a Glance...6 Participant Profile...10 Survey Methodology...18 How to Use This Report...21
SCHEDULE OF BENEFITS PLAN H1
 SCHEDULE OF BENEFITS PLAN H1 Effective June 1, 2018 This Plan is a High Deductible Health Plan (HDHP), designed to qualify for use with a Health Savings Account (HSA). All charges except charges for preventive
SCHEDULE OF BENEFITS PLAN H1 Effective June 1, 2018 This Plan is a High Deductible Health Plan (HDHP), designed to qualify for use with a Health Savings Account (HSA). All charges except charges for preventive
SCHEDULE OF BENEFITS PLAN M7
 SCHEDULE OF BENEFITS PLAN M7 Effective September 1, 2016 All benefits, unless otherwise specified, are based on Usual, Customary and Reasonable (UCR) charges, or the network contracted amounts, and are
SCHEDULE OF BENEFITS PLAN M7 Effective September 1, 2016 All benefits, unless otherwise specified, are based on Usual, Customary and Reasonable (UCR) charges, or the network contracted amounts, and are
Standing Order Policy
 * All CMA s, MA s, LPN s, and RN s are authorized by this practice to complete each standing order listed below. It is policy of this practice to only complete the standing order for patients who have
* All CMA s, MA s, LPN s, and RN s are authorized by this practice to complete each standing order listed below. It is policy of this practice to only complete the standing order for patients who have
Adult-Peds Quality Measure Information Sheet 2018
 Prevention and Screening Adolescent Preventive Care Measures (ADL) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
Prevention and Screening Adolescent Preventive Care Measures (ADL) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
UnitedHealth Premium Designation Program Case-mix Adjusted Benchmarks with Severity or Risk Adjustment
 UnitedHealth Premium Designation Program Case-mix Adjusted Benchmarks with Severity or Risk Adjustment Resources u Phone: 866-270-5588 u u u Website: UnitedHealthcareOnline.com > Quick Links > UnitedHealth
UnitedHealth Premium Designation Program Case-mix Adjusted Benchmarks with Severity or Risk Adjustment Resources u Phone: 866-270-5588 u u u Website: UnitedHealthcareOnline.com > Quick Links > UnitedHealth
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications
 HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications MHS Health Wisconsin strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications MHS Health Wisconsin strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes Respiratory Infection (RI); Pneumonia (PNA); Inpatient Urinary Tract Infection (UTI-I; Outpatient Urinary
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes Respiratory Infection (RI); Pneumonia (PNA); Inpatient Urinary Tract Infection (UTI-I; Outpatient Urinary
STARS SYSTEM 5 CATEGORIES
 TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
Condition/Procedure Measure Compliance Criteria Reference Attribution Method
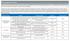 Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Accompanied by Relationship MEDICAL BACKGROUND INFORMATION. Please name the professionals that you have seen for this condition:
 Name: Age: Date: Accompanied by Relationship E-mail: @ MEDICAL BACKGROUND INFORMATION Please name the professionals that you have seen for this condition: Name Specialty Town Phone Who is your primary
Name: Age: Date: Accompanied by Relationship E-mail: @ MEDICAL BACKGROUND INFORMATION Please name the professionals that you have seen for this condition: Name Specialty Town Phone Who is your primary
Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015
 Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015 Amerivantage is an HMO plan with a contract with the New Mexico Medicare program.
Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015 Amerivantage is an HMO plan with a contract with the New Mexico Medicare program.
Georgia Green (Plan 026) 2018 Medical Benefits
 Georgia Green (Plan 026) 2018 Medical Benefits Effective Date: 1/1/2018 Version 1.0 Part D Deductible For Part D Copay information, see page 26. Out-of-Pocket Max $100/year for Part D prescription drugs
Georgia Green (Plan 026) 2018 Medical Benefits Effective Date: 1/1/2018 Version 1.0 Part D Deductible For Part D Copay information, see page 26. Out-of-Pocket Max $100/year for Part D prescription drugs
SCHEDULE OF BENEFITS PLAN M7
 SCHEDULE OF BENEFITS PLAN M7 Effective September 1, 2017 When you need to see a physician, a physician network, PHCS, is utilized for all physician services (primary care and specialists) and ancillary
SCHEDULE OF BENEFITS PLAN M7 Effective September 1, 2017 When you need to see a physician, a physician network, PHCS, is utilized for all physician services (primary care and specialists) and ancillary
HEDIS QUICK REFERENCE GUIDE: DOCUMENTATION TIPS FOR ADULT MEASURES
 HEDIS QUICK REFERENCE GUIDE: DOCUMENTATION TIPS FOR ADULT MEASURES For Health Care Providers January 2018 Helping you improve your scores, as you improve the health of your patients. Healthcare Effectiveness
HEDIS QUICK REFERENCE GUIDE: DOCUMENTATION TIPS FOR ADULT MEASURES For Health Care Providers January 2018 Helping you improve your scores, as you improve the health of your patients. Healthcare Effectiveness
Aexcel. Specialist Designation in Aetna Performance Network. Methodology Guide
 Aexcel Specialist Designation in Aetna Performance Network Methodology Guide Aexcel 2009 TABLE OF CONTENTS Background on Aexcel Performance Networks... 3 Clinical Performance Evaluation Process... 8 General
Aexcel Specialist Designation in Aetna Performance Network Methodology Guide Aexcel 2009 TABLE OF CONTENTS Background on Aexcel Performance Networks... 3 Clinical Performance Evaluation Process... 8 General
Blue represents coding updates. G0389 with diagnosis V81.2, V15.82, or with diagnosis V79.1, or
 An Independent Licensee of the Blue Cross and Blue Shield Association Preventive Care Services The following is a list of preventive services (HCP rider) along with the diagnoses and procedure codes that
An Independent Licensee of the Blue Cross and Blue Shield Association Preventive Care Services The following is a list of preventive services (HCP rider) along with the diagnoses and procedure codes that
STI Presents MIPS: SETTING UP QUALITY MEASURES THIS PRESENTATION WILL BEGIN AT IT S SCHEDULED TIME: 9AM
 STI Presents MIPS: SETTING UP QUALITY MEASURES THIS PRESENTATION WILL BEGIN AT IT S SCHEDULED TIME: 9AM Today we will cover: 2 2017 Quality Category Requirements Selecting Quality Measures Setting up Quality
STI Presents MIPS: SETTING UP QUALITY MEASURES THIS PRESENTATION WILL BEGIN AT IT S SCHEDULED TIME: 9AM Today we will cover: 2 2017 Quality Category Requirements Selecting Quality Measures Setting up Quality
Capitol Hill / Main Building
 Capitol Hill / Urgent Care Department Floor Anesthesia Advisory Clinic 2 2A Business Floor 1 West Volunteer Gift Shop Urgent Care 1A 1C 1C Occupational Therapy Physical Therapy Security 1A Urgent Care
Capitol Hill / Urgent Care Department Floor Anesthesia Advisory Clinic 2 2A Business Floor 1 West Volunteer Gift Shop Urgent Care 1A 1C 1C Occupational Therapy Physical Therapy Security 1A Urgent Care
Meaningful Use Simple Guide
 Meaningful Use Simple Guide 2011-2012 CORE Measures 1. CPOE for Medication Orders 2. Drug Interaction Checks * 3. Maintain Problem & Diagnosis List 4. eprescribing (erx) escripts 5. Active Medication List
Meaningful Use Simple Guide 2011-2012 CORE Measures 1. CPOE for Medication Orders 2. Drug Interaction Checks * 3. Maintain Problem & Diagnosis List 4. eprescribing (erx) escripts 5. Active Medication List
Adult HEDIS & STARs Measures
 HEDIS AND MEDICARE STAR DOCUMENTATION & CODING GUIDE Adult HEDIS & STARs Measures Adult BMI Assessment (ABA) 18 74-year-old Antidepressant Medication Management (AMM) Breast Cancer Screening (BCS) Cervical
HEDIS AND MEDICARE STAR DOCUMENTATION & CODING GUIDE Adult HEDIS & STARs Measures Adult BMI Assessment (ABA) 18 74-year-old Antidepressant Medication Management (AMM) Breast Cancer Screening (BCS) Cervical
EHR SOFTWARE COMPARISON
 EHR SOFTWARE COMPARISON C M CONVERTED MEDIA WHY NOT CREATE YOUR OWN COMPARISON? With our free comparison engine you can build your own side-by-side comparison of leading EHR solutions. Narrow down your
EHR SOFTWARE COMPARISON C M CONVERTED MEDIA WHY NOT CREATE YOUR OWN COMPARISON? With our free comparison engine you can build your own side-by-side comparison of leading EHR solutions. Narrow down your
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes Mastectomy, Breast Cancer Medical Oncology, Breast Biopsy, Tonsillectomy, Otitis media, Anxiety, Non-emergent
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes Mastectomy, Breast Cancer Medical Oncology, Breast Biopsy, Tonsillectomy, Otitis media, Anxiety, Non-emergent
Consultant Services to Kansas Family Physicians
 Consultant Services to Kansas Family Physicians The purpose of this study is to track the use of consultants. An e-mail survey was sent to 114 Kansas family physicians The survey was launched on 11/25/2009
Consultant Services to Kansas Family Physicians The purpose of this study is to track the use of consultants. An e-mail survey was sent to 114 Kansas family physicians The survey was launched on 11/25/2009
SCHEDULE OF BENEFITS PLAN C
 SCHEDULE OF BENEFITS PLAN C Effective September 1, 2016 All benefits, unless otherwise specified, are based on Usual, Customary and Reasonable (UCR) charges, or the network contracted amounts, and are
SCHEDULE OF BENEFITS PLAN C Effective September 1, 2016 All benefits, unless otherwise specified, are based on Usual, Customary and Reasonable (UCR) charges, or the network contracted amounts, and are
Tusculum College. Benefit Summary. $25 Copay. $25 Copay. after Deductible. 20% after Deductible 20% after Deductible
 Benefit Plan Features: Annual Deductible Benefit Summary Your Cost In-Network Individual/Family $750/$1500 Annual Out-of-Pocket Maximum Individual/Family $3500/$7000 4th Quarter Carry-over Covered Services
Benefit Plan Features: Annual Deductible Benefit Summary Your Cost In-Network Individual/Family $750/$1500 Annual Out-of-Pocket Maximum Individual/Family $3500/$7000 4th Quarter Carry-over Covered Services
Evidence-Based Measure (EBMs) Definitions
 Evidence-Based (EBMs) s This guide is a brief summary of the most commonly-used EBMs. All information is based on the MedInsight Evidence Based s (EBMs) User Guide (October 2015), compiled in a way most
Evidence-Based (EBMs) s This guide is a brief summary of the most commonly-used EBMs. All information is based on the MedInsight Evidence Based s (EBMs) User Guide (October 2015), compiled in a way most
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications
 HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications IlliniCare Health strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications IlliniCare Health strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
Target Performance. Category Weight. Available of Incentive Pool Particip ating PCPS & NPs 40+12
 # Measurement Level IHP Performance Measure Set Payment Distribution Formula Earn Condition Measure Data Source Primary Care Physicians Performance Number Available of Particip ating PCPS & NPs 40+12 Peds
# Measurement Level IHP Performance Measure Set Payment Distribution Formula Earn Condition Measure Data Source Primary Care Physicians Performance Number Available of Particip ating PCPS & NPs 40+12 Peds
IN-NETWORK MEMBER PAYS. Out-of-Pocket Maximum (Includes a combination of deductible, copayments and coinsurance for health and pharmacy services)
 HMO-OA-CAL-15-15-0-0-03 HMO Open Access Calendar Year Plan Benefit Summary This is a brief summary of benefits. Refer to your Membership Agreement for complete details on benefits, conditions, limitations
HMO-OA-CAL-15-15-0-0-03 HMO Open Access Calendar Year Plan Benefit Summary This is a brief summary of benefits. Refer to your Membership Agreement for complete details on benefits, conditions, limitations
Pennslyvania Green (Plan 028) 2018 Medical Benefits
 Pennslyvania Green (Plan 028) 2018 Medical Benefits Effective Date: 1/1/2018 Version 1.0 Part D Deductible For Part D Copay information, see page 25. $150/year for Part D prescription drugs Tiers 1 and
Pennslyvania Green (Plan 028) 2018 Medical Benefits Effective Date: 1/1/2018 Version 1.0 Part D Deductible For Part D Copay information, see page 25. $150/year for Part D prescription drugs Tiers 1 and
A1/B1: Complete Care Model: Transforming Chronic and Preventive Care
 A1/B1: Complete Care Model: Transforming Chronic and Preventive Care Michael Kanter, MD, Medical Director, Quality & Clinical Analysis, Kaiser Permanente Regional Quality and Risk Management Gail Lindsay,
A1/B1: Complete Care Model: Transforming Chronic and Preventive Care Michael Kanter, MD, Medical Director, Quality & Clinical Analysis, Kaiser Permanente Regional Quality and Risk Management Gail Lindsay,
Dr Doris M. W Kinuthia
 Dr Doris M. W Kinuthia Objectives Normal blood pressures in children Measurement of blood pressure in children Aetiology of Hypertension in children Evaluation of children with hypertension Treatment of
Dr Doris M. W Kinuthia Objectives Normal blood pressures in children Measurement of blood pressure in children Aetiology of Hypertension in children Evaluation of children with hypertension Treatment of
YOUR GROUP S PRIVATE & PUBLIC REPORT ENCLOSED
 YOUR GROUP S PRIVATE & PUBLIC REPORT ENCLOSED Please read the enclosed documents for important information regarding your group s public report of quality data. Responses must be received by April 4th,
YOUR GROUP S PRIVATE & PUBLIC REPORT ENCLOSED Please read the enclosed documents for important information regarding your group s public report of quality data. Responses must be received by April 4th,
Provider STAR Ratings Quick Reference Guide 2016 Dates of Service. Updated January 20, 2016
 Provider STAR Ratings Quick Reference Guide 2016 Dates of Service Updated January 20, 2016 Adult BMI (Body Mass Index) Assessment (ABA) EXCLUSIONS: Members who have a diagnosis of pregnancy during the
Provider STAR Ratings Quick Reference Guide 2016 Dates of Service Updated January 20, 2016 Adult BMI (Body Mass Index) Assessment (ABA) EXCLUSIONS: Members who have a diagnosis of pregnancy during the
Measure Owner Designation. AMA-PCPI is the measure owner. NCQA is the measure owner. QIP/CMS is the measure owner. AMA-NCQA is the measure owner
 2011 EHR Measure Specifications The specifications listed in this document have been updated to reflect clinical practice guidelines and applicable health informatics standards that are the most current
2011 EHR Measure Specifications The specifications listed in this document have been updated to reflect clinical practice guidelines and applicable health informatics standards that are the most current
Modified Stage 2 Meaningful Use: Clinical Quality Measures (CQMs) Massachusetts Medicaid EHR Incentive Payment Program
 Modified Stage 2 Meaningful Use: Clinical Quality Measures (CQMs) Massachusetts Medicaid EHR Incentive Payment Program July 21, 2016 Today s presenter: Al Wroblewski, PCMH CCE, Client Services Relationship
Modified Stage 2 Meaningful Use: Clinical Quality Measures (CQMs) Massachusetts Medicaid EHR Incentive Payment Program July 21, 2016 Today s presenter: Al Wroblewski, PCMH CCE, Client Services Relationship
Meaningful Use for Eligible Providers
 Meaningful Use for Eligible Providers Summary of Core and Menu objectives and Clinical Quality s Healthcare Technical Assistance Program, March 11, 2011 V.1.0Copyright 2011, Purdue Research Foundation
Meaningful Use for Eligible Providers Summary of Core and Menu objectives and Clinical Quality s Healthcare Technical Assistance Program, March 11, 2011 V.1.0Copyright 2011, Purdue Research Foundation
NORTH CAROLINA STATE HEALTH PLAN FOR TEACHERS AND STATE EMPLOYEES
 NORTH CAROLINA STATE HEALTH PLAN FOR TEACHERS AND STATE EMPLOYEES Using Clinical Risk Groups to Focus Board Strategic Initiatives July 26, 2013 Copyright 2013 by The Segal Group, Inc., parent of The Segal
NORTH CAROLINA STATE HEALTH PLAN FOR TEACHERS AND STATE EMPLOYEES Using Clinical Risk Groups to Focus Board Strategic Initiatives July 26, 2013 Copyright 2013 by The Segal Group, Inc., parent of The Segal
