Clinical Characteristics of Optic Neuritis in Koreans Greater than 50 Years of Age
|
|
|
- Abigail Walsh
- 5 years ago
- Views:
Transcription
1 pissn: eissn: Korean J Ophthalmol 2012;26(2): Original Article Clinical Characteristics of Optic Neuritis in Koreans Greater than 50 Years of Age Jin Choi 1, Seong-Joon Kim 2,3, Ji Woong Chang 4, Jeong Hun Kim 2,3, Young Suk Yu 2,3 1 Department of Ophthalmology, Inje University Sanggye Paik Hospital, Seoul, Korea 2 Department of Ophthalmology, Seoul National University College of Medicine, Seoul, Korea 3 Seoul Artificial Eye Center, Seoul National University Hospital Clinical Research Institute, Seoul, Korea 4 Department of Ophthalmology, Inje University Ilsan Paik Hospital, Ilsan, Korea Purpose: To report clinical characteristics of optic neuritis (ON) in Koreans >50 years of age. Methods: A retrospective chart review was performed on patients with ON between January 2000 and December We obtained the best-corrected visual acuity (BCVA), Goldmann perimetry, relative afferent pupillary (RAPD), and color function tests as well as brain magnetic resonance imaging (MRI) findings in patients who were in the acute stage of the disorder. Results: Nine eyes in eight patients were included. The mean age of patients at presentation was 60.5 years (range, 53 to 71 years). Six patients were female, and two were male. There was one patient with bilateral ON. The mean BCVA at presentation was 20 / 400 (no light perception-20 / 70). Eight eyes (89%) complained of pain with eye movement. Six eyes (66%) had disc edema. Central was the most common field. All eyes had color abnormalities. Five eyes in four patients showed abnormalities of the involved optic nerves on MRI. The patients were followed for a mean of 11.3 months (range, 2 to 34 months). All of the patients recovered to a BCVA of 20 / 40 or better within 2 months. On the last follow-up, the mean BCVA was 20 / 20 (20 / 40 to 20 / 16). Four eyes showed remnant central. One eye had remnant RAPD, and two eyes had mild color abnormalities. Conclusions: Although ON is uncommon in elderly patients, it can develop in patients >50 years of age, and clinical features of optic neuritis in elderly patients are similar to those of younger patients. Key Words: Acute optic neuropathy, Elderly patients, Non-arteritic anterior ischemic optic neuropathy, Optic neuritis, Visual recovery Optic neuritis (ON) is an acute inflammatory condition affecting the optic nerve. The most common cause of ON is demyelination of the optic nerve (either idiopathic or due to multiple sclerosis), although there are other possible etiologies, including para-infectious responses, infections and vasculitides. ON typically affects young adults between 18 and 45 years of age, with a mean age of 30 to 35 years; Received: October 16, 2010 Accepted: May 6, 2011 Corresponding Author: Seong-Joon Kim, MD. Department of Ophthalmology, Seoul National University College of Medicine, 103 Daehakro, Jongno-gu, Seoul , Korea. Tel: , Fax: , ophjun@snu.ac.kr there is a strong female predominance [1]. In the Optic Neuritis Treatment Trial (ONTT), the mean patient age was 31.8 years, and 77% of participants were female [2]. Idiopathic ON and non-arteritic anterior ischemic optic neuropathy (NAION) are acute optic neuropathies with overlapping clinical profiles. ON typically presents as painful loss of vision in younger patients and has good potential for improvement, whereas NAION typically presents as painless loss of vision in the middle-aged or elderly with usually less complete recovery. Although there has been some effort to differentiate ON and NAION using visual field testing [3], magnetic resonance imaging (MRI) [4], pattern electroretinography [5], or optic disc morphology [6], there is no gold standard for distinguishing ON from 2012 The Korean Ophthalmological Society This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( /by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. 111
2 Korean J Ophthalmol Vol.26, No.2, 2012 NAION. Especially in the elderly, ON is uncommon and is often misdiagnosed as NAION. Although we occasionally encounter elderly patients with ON in the clinic, few reports that document ON in elderly patients have been published. Therefore, in this report, we described the clinical course and characteristics of ON in elderly patients. Materials and Methods This study was a retrospective case series. We reviewed the medical records of patients who attended the Neuroophthalmic Clinic in the Department of Ophthalmology at Seoul National University Hospital and were diagnosed with ON between January 2000 and December The study protocol followed the tenets of the Declaration of Helsinki. Informed consent was obtained, and the Institutional Review Board of Seoul National University Hospital Clinical Research Institute approved the study. We searched for patients who were diagnosed with ON or NAION and who were also >50 years of age at the time of initial presentation. Patients who were finally diagnosed with ON by an experienced neuro-ophthalmologist (SJK) were included in this study. The patient age at onset, gender, medical history, duration from the onset of visual symptoms, and presence of ocular pain on eye movement were noted. Determination of the best-corrected visual acuity (BCVA) and the presence of a relative afferent pupillary (RAPD), and visual field testing, color function testing, and fundoscopy were performed at the initial presentation and on each follow-up visit. Patients who underwent any treatment before the visit to our clinic and who had a previous visual loss history or other ocular abnormalities causing visual loss were excluded. Whether or not the patients received treatment for ON was also ascertained. The diagnosis of ON was made on the basis of clinical symptoms, such as ocular pain or gradual visual loss over several days, signs of abnormal optic nerve thickening or on MRI with contrast, and the clinical course of subsequent visual recovery. To distinguish ON from NAION, fluorescene angiography (FAG) was also performed, and disc non-perfusion was ruled out. We examined RAPD by performing the swinging flashlight test and identified color abnormalities by testing participants using the Hardy-Rand-Rittler (HRR) color plate. Color abnormalities were graded as normal color function, and mild, moderate or severe s. Visual fields were examined with the Goldmann perimeter (GVF) by experienced technicians. The mean BCVAs were calculated after conversion to a logarithm of the minimal angle of resolution (logmar). Visual acuity of the counting fingers was converted to 2 in logmar, and hand movement to 3 in logmar. However, light perception or no light perception were not actually visual measurements, so therefore these parameters were excluded from our calculations [7]. Results Nine eyes of eight patients were included in our study. Patient demographics and initial examination results are listed in Table 1. The mean age of the patients was 60.5 years (range, 53 to 71 years). Six patients were female, and two patients were male. One patient had bilateral ON. Five Table 1. Patient demographics and results of examination at initial presentation Patient Gender / Pain on eye Disc Eye BCVA RAPD age movement swelling GVF HRR color test MRI 1 F / 71 R Y 20 / 100 Present Y Central Fail Optic nerve swelling 2 F / 67 R N HM Present N Impossible Fail Normal 3 M / 64 L Y 20 / 1000 Present Y Inferior altitudinal Severe RG-BY Optic nerve 4 F / 60 L Y 20 / 100 Present N Generalized Not performed Not performed decrease 5 F / 58 L Y 20 / 200 Present N Central Severe RG-BY Not performed 6 F / 56 R Y CF Present Y Central Fail Optic nerve 7 M / 55 R Y 20 / 70 Present Y Central Not performed Not performed 8 F / 53 R Y 20 / 100 Absent Y Superior altitudinal Severe RG-BY Optic nerve L Y NLP Present Y Impossible Fail Optic nerve BCVA = best-corrected visual acuity; RAPD = relative afferent papillary ; GVF = Goldmann visual field; HRR = Hardy-Rand-Rittler; MRI = magnetic resonance imaging; HM = hand movement; CF = counting fingers; NLP = no light perception; RG = red-green; BY = blue-yellow. 112
3 J Choi, et al. Optic Neuritis in Elderly Koreans right eyes and four left eyes were involved. One patient had diabetes, and another patient had hyperthyroidism. At the time of the initial examination, eight eyes (89%) were accompanied by pain on eye movement. The mean BCVA was 20 / 400 (range, no light perception-20 / 70). Six eyes (66%) had disc swelling, whereas three eyes had a normal disc appearance. Unaffected fellow eyes had normal disc appearances with normal cup-disc ratios. In patients with unilateral ON, all affected eyes had RAPD, and in the patient with bilateral ON, the more severely affected eye had RAPD. GVF revealed four eyes with central s, two eyes with altitudinal s, and one eye with generalized decrease of perception. Two eyes could not perform the field test due to poor vision. Four eyes failed to distinguish figures on all the plates during the HRR color function test, and three eyes had severe color function s. Two eyes did not undergo the color test at the time of the initial examination. Five patients had MRI, and five eyes of four patients had abnormalities (such as optic nerve swelling or of the involved optic nerve) noted on MRI, but no participants showed abnormal brain (Table 1). The duration from the onset of decreased vision to the time of lowest visual acuity was 9.3 days (range, 5 to 14 days). Among eight patients, three were treated with intravenous, high-dose corticosteroid therapy and three received oral corticosteroid therapy. Two of the three patients who received oral steroids were misdiagnosed with NAION initially, and the other patient was treated at a primary ophthalmic clinic before referral to our clinic. Oral steroids were tapered in our clinic, and intravenous, high-dose corticosteroid therapy was not administered due to the request of the patient. The other two patients refused to receive intravenous high-dose corticosteroid therapy. Three patients who received intravenous steroids showed no side effects. Two patients (cases 3 and 7) was misdiagnosed as NAION initially because they were elderly, had systemic illness such as diabetes mellitus or hypertension, and had disc swelling with relatively abrupt visual impairment, which are all more common in NAION. They also complained of less specific eye pain on eye movement. One patient (case 3) had an altitudinal on GVF. However, no participants showed abnormal disc perfusion on FAG. One participant (case 3) demonstrated optic nerve on MRI, and both showed visual improvement during follow-up, which led to a final diagnosis of optic neuritis. The patients were followed for a mean of 11.3 months (range, 2 to 34 months), and all recovered to a BCVA of 20 / 40 or better within 2 months. Eight eyes gained complete visual recovery, and one eye achieved partial recovery. At the last follow-up, the mean BCVA was 20 / 20 (20 / 40 to 20 / 16). Three eyes had remnant, small central s, and one eye had a small paracentral. RAPD remained in one eye, and mild color abnormalities were present in two eyes. Disc pallor was observed in five eyes (Table 2). Discussion This is the first report involving ON in patients >50 years of age. Based on our results, ON in elderly patients is uncommon; there were only eight patients who visited our clinic between January 2000 and December 2009 who were diagnosed with ON. The diagnosis of ON was based strictly on clinical judgment considering the neuroophthalmic history and examination (fundoscopy, visual field testing, color testing, and MRI). The clinical course Table 2. Patient data at final examination Patient Eye Treatment FU (mon) BCVA RAPD Disc HRR color Time to visual GVF appearance test recovery 20 / 40 1 R Oral steroid / 40 Absent Normal Not performed Mild RG-BY 2 mon 2 R IV steroid / 40 Absent Normal Small central Mild RG-BY 3 L Oral steroid / 16 Absent Normal Normal Normal 4 L No treatment / 16 Absent Normal Normal Normal 3 wk 5 L No treatment / 20 Absent Mild pallor Small paracentral Normal 6 R IV steroid / 16 Absent Mild pallor Normal Normal 7 R Oral steroid / 20 Present Mild pallor Small central Normal 8 R IV steroid / 16 Absent Pallor Normal Normal 1 wk L IV steroid / 20 Absent Pallor Small central Normal FU = follow-up period; BCVA = best-corrected visual acuity; RAPD = relative afferent papillary ; GVF = Goldmann visual field; IV = intravenous; HRR = Hardy-Rand-Rittler; RG = red-green; BY = blue-yellow. 113
4 Korean J Ophthalmol Vol.26, No.2, 2012 of visual impairment was also considered in the final diagnosis of ON because ON (but not NAION) is typically associated with substantial visual recovery [8]. In this study, all affected eyes recovered visual acuity better than 20 / 40 within two months. This clearly demonstrates that ON had a good visual prognosis, even in patients >50 years of age. Nevertheless, there is no gold standard for the diagnosis of ON. Rizzo and Lessell [9] reported that ON and NAION have many overlapping clinical profiles, and it may be difficult to differentiate between ON and NAION solely on nosologic grounds in some instances of acute, unilateral optic neuropathies. From previous reports [1,3-6], some distinguishing characteristics between ON and NAION are known, as follows: ON occurs in young patients, whereas NAION occurs in elderly patients; ON has a normal-color disc edema without hemorrhage in the acute stage and culminates with temporal pallor, whereas NAION has altitudinal or pale disc edema with hemorrhage and retinal arterial attenuation in the acute stage and persistent segmental or altitudinal optic atrophy [6]; most ON patients who receive gadolinium have abnormal signal intensity on MRI, whereas few NAION patients show abnormalities [4]; and ON has characteristic central on the fixation point with a sloping border, whereas NAION has an inferior altitudinal with a sharp border along the horizontal meridian [3]. Despite all of these differences, the diagnosis of ON in some instances is still a matter of debate. In our study, the two patients who received oral steroids were initially misdiagnosed with NAION and prescribed oral steroids. After obtaining a detailed history and undergoing GVF, MRI and follow-up examinations, they were re-diagnosed with ON. The diagnosis of ON in our cases was made according to the initial presenting features, including pain on eye movement, gradual visual impairment over several days, optic nerve abnormalities on MRI during the acute stage, the pattern of visual field on initial examination and follow-up, and visual recovery. Eight of nine eyes experienced pain on eye movement preceding visual impairment in our study, whereas 92% of patients enrolled in the ONTT reported pain [2]. With respect to disc swelling, greater than one-half of the eyes had disc swelling, and one-third of ONTT patients had disc swelling [2]. The discrepancy in the percentages of pain and disc swelling between our study and the ONTT may be attributed to the small number of cases or the different age distribution; further evaluation is necessary. MRI was performed in only five patients, including one patient with bilateral ON; abnormal findings, such as swelling or of the optic nerve, were demonstrated on MRI in five eyes of four patients. No patient had abnormal brain lesions on MRI. Considering the relationship between ON and multiple sclerosis, the small number of cases in our study made it difficult to evaluate the prevalence of multiple sclerosis in elderly patients. However, the high incidence of optic nerve abnormalities on MRI in this study suggested that MRI was important in the diagnosis of ON, which is in agreement with the findings of Rizzo et al. [4]. Central is the characteristic feature of the visual field in ON [3]. In this study, four eyes had central at the time of the initial examination, and two eyes showed central during follow-up. The latter two eyes had very poor visual detection of hand movements and failed to perform GVF initially. Two eyes that showed initial altitudinal s, which is more common in NAION [3] but also can be seen in ON [1-3,10], recovered completely at the time of final examination, whereas visual field s in NAION rarely recover. Therefore, follow-up visual field tests may aid in the diagnosis of ON. Elderly patients are prone to decline intravenous, highdose corticosteroid therapy when offered due to the known side effects, such as sleep disturbances, mood changes, gastric disturbances, facial flushing, weight gain during the treatment period, and infections [11]. Subsequently, the overall treatment rate appears to be lower than that occurring in pediatric or young adult patients. There is also a substantial tendency for multiple sclerosis to develop in patients with ON [12,13], and the intravenous administration of high-dose corticosteroids may lessen the risk of progression to multiple sclerosis within two years of an acute attack of ON [14]. The low rate of intravenous high-dose corticosteroid treatment and age >50 years in this study might have influenced the later development of multiple sclerosis. However, the mean follow-up period for our patients was only 11.3 months, and the prevalence of multiple sclerosis is also much lower in Asian countries compared with the Western population [15]. Therefore, we could not further evaluate this hypothesis regarding ON and multiple sclerosis. The three patients who received intravenous, high-dose corticosteroid therapy initially had more severely impaired visual acuity than counting fingers. Despite steroid therapy, which is known to induce early visual recovery [16], it took >th to acquire a visual acuity of 20 / 40 or better, and remnant, tiny central s existed on the final examination in two of these patients. Based on these findings, the effect of intravenous steroid therapy in elderly patients must be further evaluated. This study had some limitations. First, this was a retrospective study; the number of patients was small because ON is uncommon in elderly patients. Second, the follow-up period of patients was too short to evaluate their long-term prognosis. The favorable visual outcome of ON prohibits patients from returning to the clinic. The two patients who were followed for only two months did not visit our clinic after their visual acuity recovered. A comparison of clinical characteristics with ON in young adults or in patients 114
5 J Choi, et al. Optic Neuritis in Elderly Koreans with NAION may be necessary. Some patients in this study were diagnosed with ON because they showed substantial visual recovery during follow-up, so the conclusion that elderly patients with ON have a good prognosis may be biased. Moreover, visual function testing (including contrast sensitivity or Humprey visual field testing) or evaluation of the fellow eye may help to understand ON in elderly patients. However, we believe that this study is worthy to report because this is the first trial to investigate ON in patients >50 years of age, which is contrary to the general perception that ON occurs between the ages of 20 and 50 years, with a peak between 30 and 35 years of age. In summary, we have shown that ON can develop in elderly patients, and the clinical features of ON in elderly patients do not differ from the clinical features in young patients. Careful diagnostic approaches are essential for the differential diagnosis of acute optic neuropathies in elderly patients. Further evaluations regarding treatment modalities for ON and their effect in elderly patients will be necessary. Although the pathogenesis of ON in elderly patients may differ from ON in young patients, we could not identify any basis by which to determine the differences. Conflict of Interest No potential conflict of interest relevant to this article was reported. References 1. Walsh FB, Hoyt WF, Miller NR. Walsh and Hoyt s clinical neuro-ophthalmology. Vol. 1. 4th ed. Baltimore: Williams & Wilkins; The clinical profile of optic neuritis. Experience of the optic neuritis treatment trial. Optic Neuritis Study Group. Arch Ophthalmol 1991;109: Gerling J, Meyer JH, Kommerell G. Visual field s in optic neuritis and anterior ischemic optic neuropathy: distinctive features. Graefes Arch Clin Exp Ophthalmol 1998;236: Rizzo JF 3rd, Andreoli CM, Rabinov JD. Use of magnetic resonance imaging to differentiate optic neuritis and nonarteritic anterior ischemic optic neuropathy. Ophthalmology 2002;109: Froehlich J, Kaufman DI. Use of pattern electroretinography to differentiate acute optic neuritis from acute anterior ischemic optic neuropathy. Electroencephalogr Clin Neurophysiol 1994;92: Rath EZ, Rehany U, Linn S, Rumelt S. Correlation between optic disc atrophy and aetiology: anterior ischaemic optic neuropathy vs optic neuritis. Eye (Lond) 2003;17: Holladay JT. Proper method for calculating average visual acuity. J Refract Surg 1997;13: Beck RW, Cleary PA, Backlund JC. The course of visual recovery after optic neuritis. Experience of the optic neuritis treatment trial. Ophthalmology 1994;101: Rizzo JF 3rd, Lessell S. Optic neuritis and ischemic optic neuropathy. Overlapping clinical profiles. Arch Ophthalmol 1991;109: Nevalainen J, Krapp E, Paetzold J, et al. Visual field s in acute optic neuritis: distribution of different types of pattern, assessed with threshold-related supraliminal perimetry, ensuring high spatial resolution. Graefes Arch Clin Exp Ophthalmol 2008;246: Chrousos GA, Kattah JC, Beck RW, Cleary PA. Side effects of glucocorticoid treatment. Experience of the optic neuritis treatment trial. JAMA 1993;269: Rizzo JF 3rd, Lessell S. Risk of developing multiple sclerosis after uncomplicated optic neuritis: a long-term prospective study. Neurology 1988;38: Beck RW, Cleary PA, Anderson MM Jr, et al. A randomized, controlled trial of corticosteroids in the treatment of acute optic neuritis. The Optic Neuritis Study Group. N Engl J Med 1992;326: Beck RW, Cleary PA, Trobe JD, et al. The effect of corticosteroids for acute optic neuritis on the subsequent development of multiple sclerosis. The Optic Neuritis Study Group. N Engl J Med 1993;329: Alter M, Good J, Okihiro M. Optic neuritis in Orientals and Caucasians. Neurology 1973;23: Beck RW, Trobe JD. What we have learned from the Optic Neuritis Treatment Trial. Ophthalmology 1995;102:
Analysis of Fundus Photography and Fluorescein Angiography in Nonarteritic Anterior Ischemic Optic Neuropathy and Optic Neuritis
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):289-294 http://dx.doi.org/10.3341/kjo.2016.30.4.289 Original Article Analysis of Fundus Photography and Fluorescein Angiography in Nonarteritic
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):289-294 http://dx.doi.org/10.3341/kjo.2016.30.4.289 Original Article Analysis of Fundus Photography and Fluorescein Angiography in Nonarteritic
Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD
 Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD A 68 year old white woman had a new onset of floaters in her right eye and was found to have
Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD A 68 year old white woman had a new onset of floaters in her right eye and was found to have
Differences between Non-arteritic Anterior Ischemic Optic Neuropathy and Open Angle Glaucoma with Altitudinal Visual Field Defect
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
Optic neuritis in Singapore
 667 Original Article Optic neuritis in Singapore Lim S A, Goh K Y, Tow S, Fu E, Wong T Y, Seah A, Tan C, Cullen J F ABSTRACT Introduction: Optic neuritis (ON) is the commonest optic neuropathy encountered
667 Original Article Optic neuritis in Singapore Lim S A, Goh K Y, Tow S, Fu E, Wong T Y, Seah A, Tan C, Cullen J F ABSTRACT Introduction: Optic neuritis (ON) is the commonest optic neuropathy encountered
Neuro-Ocular Grand Rounds
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Ischaemic optic neuropathy: the Singapore scene
 O r i g i n a l A r t i c l e Singapore Med J 2007; 48 (4) : 281 Ischaemic optic neuropathy: the Singapore scene Cullen J F, Por Y M Abstract The commonest cause of an optic neuropathy in Singapore is
O r i g i n a l A r t i c l e Singapore Med J 2007; 48 (4) : 281 Ischaemic optic neuropathy: the Singapore scene Cullen J F, Por Y M Abstract The commonest cause of an optic neuropathy in Singapore is
Clinical prospective study of visual function in patients with acute optic neuritis
 Journal of the Formosan Medical Association (2013) 112, 87e92 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical prospective study of visual function
Journal of the Formosan Medical Association (2013) 112, 87e92 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical prospective study of visual function
Role Of Various Factors In The Treatment Of Optic Neuritis----A Study Abstract Aim: Materials & Methods Discussion: Conclusion: Key words
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 51-57 www.iosrjournals.org Role Of Various Factors In The Treatment
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 51-57 www.iosrjournals.org Role Of Various Factors In The Treatment
Neuropathy (NAION) and Avastin. Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013
 Non Arteritic Ischemic Optic Neuropathy (NAION) and Avastin Shalom Kelman, MD Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013 Anterior Ischemic Optic Neuropathy Acute, painless, visual loss,
Non Arteritic Ischemic Optic Neuropathy (NAION) and Avastin Shalom Kelman, MD Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013 Anterior Ischemic Optic Neuropathy Acute, painless, visual loss,
Clinical differences between young and older patients with optic neuritis
 Original Article Page 1 of 5 Clinical differences between young and older patients with optic neuritis Wenjing Luo 1 *, Qiu-Shui Huang 2 *, Jian-Feng He 2, Min Han 1, Bo Liu 1, Yi Du 2 1 The Cadre Ward
Original Article Page 1 of 5 Clinical differences between young and older patients with optic neuritis Wenjing Luo 1 *, Qiu-Shui Huang 2 *, Jian-Feng He 2, Min Han 1, Bo Liu 1, Yi Du 2 1 The Cadre Ward
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema. Jonathan A. Micieli, MD Valérie Biousse, MD
 Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Supplementary Online Content
 Supplementary Online Content Park KH, Kim YK, Woo SJ, et al. Iatrogenic occlusion of the ophthalmic artery after cosmetic facial filler injections: a national survey by the Korean Retina Society. JAMA
Supplementary Online Content Park KH, Kim YK, Woo SJ, et al. Iatrogenic occlusion of the ophthalmic artery after cosmetic facial filler injections: a national survey by the Korean Retina Society. JAMA
Factors Influencing the Prevalence of Amblyopia in Children with Anisometropia
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(4):225-229 DOI: 10.3341/kjo.2010.24.4.225 Factors Influencing the Prevalence of Amblyopia in Children with Anisometropia Original Article Chong
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(4):225-229 DOI: 10.3341/kjo.2010.24.4.225 Factors Influencing the Prevalence of Amblyopia in Children with Anisometropia Original Article Chong
ORIGINAL RESEARCH ARTICLE
 Journal of Chitwan Medical College 2015; 5(14): 49-54 Available online at: www.jcmc.cmc.edu.np ISSN 2091-2889 (Online) ISSN 2091-2412 (Print) JOURNAL OF CHITWAN MEDICAL COLLEGE JCMC ESTD 2010 ORIGINAL
Journal of Chitwan Medical College 2015; 5(14): 49-54 Available online at: www.jcmc.cmc.edu.np ISSN 2091-2889 (Online) ISSN 2091-2412 (Print) JOURNAL OF CHITWAN MEDICAL COLLEGE JCMC ESTD 2010 ORIGINAL
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-ophthalmologyophthalmology. Marek Michalec, MD.
 Neuro-ophthalmologyophthalmology Marek Michalec, MD. Neuro-ophthalmology Study integrating ophthalmology and neurology Disorders affecting parts of CNS devoted to vision or eye: Afferent system (visual
Neuro-ophthalmologyophthalmology Marek Michalec, MD. Neuro-ophthalmology Study integrating ophthalmology and neurology Disorders affecting parts of CNS devoted to vision or eye: Afferent system (visual
The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus
 The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus Received: 25/4/2016 Accepted: 8/12/2016 Introduction Diabetic papillopathy is an atypical form of non-arteritic anterior ischemic
The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus Received: 25/4/2016 Accepted: 8/12/2016 Introduction Diabetic papillopathy is an atypical form of non-arteritic anterior ischemic
Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in a Young Patient
 Case Reports in Ophthalmological Medicine Volume 2016, Article ID 6741925, 4 pages http://dx.doi.org/10.1155/2016/6741925 Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in
Case Reports in Ophthalmological Medicine Volume 2016, Article ID 6741925, 4 pages http://dx.doi.org/10.1155/2016/6741925 Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in
I have nothing to disclose but I
 OPTIC NEUROPATHIES Robert L. Tomsak MD PhD Professor of Ophthalmology and Neurology Wayne State t University it Sh School of Mdii Medicine I have nothing to disclose but I wish I did. dd Road map for this
OPTIC NEUROPATHIES Robert L. Tomsak MD PhD Professor of Ophthalmology and Neurology Wayne State t University it Sh School of Mdii Medicine I have nothing to disclose but I wish I did. dd Road map for this
Pearls, Pitfalls and Advances in Neuro-Ophthalmology
 Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Superior Rectus Muscle Recession for Residual Head Tilt after Inferior Oblique Muscle Weakening in Superior Oblique Palsy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(4):285-289 http://dx.doi.org/10.3341/kjo.2012.26.4.285 Original Article Superior Rectus Muscle Recession for Residual Head Tilt after Inferior
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(4):285-289 http://dx.doi.org/10.3341/kjo.2012.26.4.285 Original Article Superior Rectus Muscle Recession for Residual Head Tilt after Inferior
New Insights on Optic Neuritis in Young People
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
Incidence and Clinical Features of Neovascularization of the Iris following Acute Central Retinal Artery Occlusion
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(5):352-359 http://dx.doi.org/10.3341/kjo.2016.30.5.352 Original Article Incidence and Clinical Features of Neovascularization of the Iris following
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(5):352-359 http://dx.doi.org/10.3341/kjo.2016.30.5.352 Original Article Incidence and Clinical Features of Neovascularization of the Iris following
THE OPTIC CHIASM MAY BE DAMAGED BY A VARIETY
 Clinical Features Associated With Lesions Other Than Pituitary Adenoma in Patients With an Optic Chiasmal Syndrome LUIS J. MEJICO, MD, NEIL R. MILLER, MD, AND LI MING DONG, PHD PURPOSE: Pituitary adenomas
Clinical Features Associated With Lesions Other Than Pituitary Adenoma in Patients With an Optic Chiasmal Syndrome LUIS J. MEJICO, MD, NEIL R. MILLER, MD, AND LI MING DONG, PHD PURPOSE: Pituitary adenomas
Criteria for early CLINICAL STUDY. N Fujimoto 1, N Saeki 2, O Miyauchi 1
 (2002) 16, 731 738 2002 Nature Publishing Group All rights reserved 0950-222X/02 $25.00 www.nature.com/eye N Fujimoto 1, N Saeki 2, O Miyauchi 1 Criteria for early and E Adachi-Usami 1 detection of temporal
(2002) 16, 731 738 2002 Nature Publishing Group All rights reserved 0950-222X/02 $25.00 www.nature.com/eye N Fujimoto 1, N Saeki 2, O Miyauchi 1 Criteria for early and E Adachi-Usami 1 detection of temporal
Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results of Cerebral Perfusion MR Imaging
 pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
Five steps: Overview
 Optic atrophy is not a diagnosis Andrew G. Lee, MD Professor of Ophthalmology, Neurology and Neurosurgery, Weill Cornell Medical College Chair, Department of Ophthalmology, Houston Methodist Hospital,
Optic atrophy is not a diagnosis Andrew G. Lee, MD Professor of Ophthalmology, Neurology and Neurosurgery, Weill Cornell Medical College Chair, Department of Ophthalmology, Houston Methodist Hospital,
Intrapapillary hemorrhage with concurrent peripapillary and vitreous hemorrhage in two healthy young patients
 Moon et al. BMC Ophthalmology (2018) 18:172 https://doi.org/10.1186/s12886-018-0833-z CASE REPORT Open Access Intrapapillary hemorrhage with concurrent peripapillary and vitreous hemorrhage in two healthy
Moon et al. BMC Ophthalmology (2018) 18:172 https://doi.org/10.1186/s12886-018-0833-z CASE REPORT Open Access Intrapapillary hemorrhage with concurrent peripapillary and vitreous hemorrhage in two healthy
Research Paper: Tapering Oral Steroid Treatment After IV Methylprednisolone Pulse Therapy in Demyelinating Optic Neuritis
 Caspian Journal of Neurological Sciences "Caspian J Neurol Sci" Journal Homepage: http://cjns.gums.ac.ir Research Paper: Tapering Oral Steroid Treatment After IV Methylprednisolone Pulse Therapy in Demyelinating
Caspian Journal of Neurological Sciences "Caspian J Neurol Sci" Journal Homepage: http://cjns.gums.ac.ir Research Paper: Tapering Oral Steroid Treatment After IV Methylprednisolone Pulse Therapy in Demyelinating
Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic Syndrome
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Ethambutol (EMB), the first-line drug used to treat mycobacterium
 Eye Movements, Strabismus, Amblyopia and Neuro-Ophthalmology Ganglion Cell Layer and Inner Plexiform Layer as Predictors of Vision Recovery in Ethambutol-Induced Optic Neuropathy: A Longitudinal OCT Analysis
Eye Movements, Strabismus, Amblyopia and Neuro-Ophthalmology Ganglion Cell Layer and Inner Plexiform Layer as Predictors of Vision Recovery in Ethambutol-Induced Optic Neuropathy: A Longitudinal OCT Analysis
The Parameters of Pattern Visual Evoked Potential in the Severe Visual Loss Patients in Korean
 pissn: 0894 eissn: 09938 Korean J Ophthalmol 05;9(3):8589 http://dx.doi.org/0.334/kjo.05.9.3.85 Original Article The Parameters of Pattern Visual Evoked Potential in the Severe Visual Loss Patients in
pissn: 0894 eissn: 09938 Korean J Ophthalmol 05;9(3):8589 http://dx.doi.org/0.334/kjo.05.9.3.85 Original Article The Parameters of Pattern Visual Evoked Potential in the Severe Visual Loss Patients in
HOMONYMOUS VISUAL FIELD DEFECTS Perimetric findings and corresponding neuro-imaging results
 Homonymous visual field defects 511 HOMONYMOUS VISUAL FIELD DEFECTS Perimetric findings and corresponding neuro-imaging results JAN SCHILLER 1, TRAUGOTT J. DIETRICH 1, LIESE LORCH 1, MARTIN SKALEJ 2, CHRISTOPH
Homonymous visual field defects 511 HOMONYMOUS VISUAL FIELD DEFECTS Perimetric findings and corresponding neuro-imaging results JAN SCHILLER 1, TRAUGOTT J. DIETRICH 1, LIESE LORCH 1, MARTIN SKALEJ 2, CHRISTOPH
T he extent of damage to the optic nerve caused by nonarteritic
 1274 EXTENDED REPORT Frequency doubling technology perimetry in non-arteritic ischaemic optic neuropathy with altitudinal defects C A Girkin, G McGwin Jr, J DeLeon-Ortega... See end of article for authors
1274 EXTENDED REPORT Frequency doubling technology perimetry in non-arteritic ischaemic optic neuropathy with altitudinal defects C A Girkin, G McGwin Jr, J DeLeon-Ortega... See end of article for authors
Case Report A Case of Recurrent Transient Monocular Visual Loss after Receiving Sildenafil
 Case Reports in Ophthalmological Medicine Volume 2011, Article ID 645089, 4 pages doi:10.1155/2011/645089 Case Report A Case of Recurrent Transient Monocular Visual Loss after Receiving Sildenafil Asaad
Case Reports in Ophthalmological Medicine Volume 2011, Article ID 645089, 4 pages doi:10.1155/2011/645089 Case Report A Case of Recurrent Transient Monocular Visual Loss after Receiving Sildenafil Asaad
OPTIC NEUROPATHIES Optic Neuritis vs AION. Jacqueline M.S. Winterkorn, Ph.D., M.D.
 OPTIC NEUROPATHIES Optic Neuritis vs AION Jacqueline M.S. Winterkorn, Ph.D., M.D. OPTIC NEUROPATHIES Inflammatory Optic Neuritis Ischemic Optic Neuropathy Compressive Optic Neuropathy Traumatic Optic
OPTIC NEUROPATHIES Optic Neuritis vs AION Jacqueline M.S. Winterkorn, Ph.D., M.D. OPTIC NEUROPATHIES Inflammatory Optic Neuritis Ischemic Optic Neuropathy Compressive Optic Neuropathy Traumatic Optic
Evaluation of ONH Pallor in Glaucoma Patients and Suspects. Leticia Rousso, O.D. Joseph Sowka, O.D
 Evaluation of ONH Pallor in Glaucoma Patients and Suspects Leticia Rousso, O.D Joseph Sowka, O.D I. Abstract This case report will evaluate a young glaucoma suspect with unilateral sectoral optic nerve
Evaluation of ONH Pallor in Glaucoma Patients and Suspects Leticia Rousso, O.D Joseph Sowka, O.D I. Abstract This case report will evaluate a young glaucoma suspect with unilateral sectoral optic nerve
Anterior Ischemic Optic Neuropathy (AION)
 Anterior Ischemic Optic Neuropathy (AION) Your doctor thinks you have suffered an episode of anterior ischemic optic neuropathy (AION). This is the most common cause of sudden decreased vision in patients
Anterior Ischemic Optic Neuropathy (AION) Your doctor thinks you have suffered an episode of anterior ischemic optic neuropathy (AION). This is the most common cause of sudden decreased vision in patients
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion
 Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
ORIGINAL CONTRIBUTION. The Natural History of Recurrent Optic Neuritis
 ORIGINAL CONTRIBUTION The Natural History of Recurrent Optic Neuritis Istvan Pirko, MD; Lori K. Blauwet, MD; Timothy G. Lesnick, MSc; Brian G. Weinshenker, MD, FRCP(C) Background: Optic neuritis (ON) may
ORIGINAL CONTRIBUTION The Natural History of Recurrent Optic Neuritis Istvan Pirko, MD; Lori K. Blauwet, MD; Timothy G. Lesnick, MSc; Brian G. Weinshenker, MD, FRCP(C) Background: Optic neuritis (ON) may
S uperior segmental optic hypoplasia (SSOH), also termed
 910 CLINICAL SCIENCE Optical coherence tomography of superior segmental optic hypoplasia K Unoki, N Ohba, W F Hoyt... See end of article for authors affiliations... Correspondence to: Kazuhiko Unoki, MD,
910 CLINICAL SCIENCE Optical coherence tomography of superior segmental optic hypoplasia K Unoki, N Ohba, W F Hoyt... See end of article for authors affiliations... Correspondence to: Kazuhiko Unoki, MD,
Relationship of Hypertropia and Excyclotorsion in Superior Oblique Palsy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(1):39-43 http://dx.doi.org/10.3341/kjo.2013.27.1.39 Relationship of Hypertropia and Excyclotorsion in Superior Oblique Palsy Original Article
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(1):39-43 http://dx.doi.org/10.3341/kjo.2013.27.1.39 Relationship of Hypertropia and Excyclotorsion in Superior Oblique Palsy Original Article
Changes in Peripapillary Retinal Nerve Fiber Layer Thickness after Pattern Scanning Laser Photocoagulation in Patients with Diabetic Retinopathy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(3):220-225 http://dx.doi.org/10.3341/kjo.2014.28.3.220 Original Article Changes in Peripapillary Retinal Nerve Fiber Layer Thickness after
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(3):220-225 http://dx.doi.org/10.3341/kjo.2014.28.3.220 Original Article Changes in Peripapillary Retinal Nerve Fiber Layer Thickness after
Delayed Choroidal Perfusion in Giant Cell Arteritis
 Tournai of Clinical Neuro-ophthalmology 11(4): 221-227,1991. 1991 Raven Press, Ltd., New York Delayed Choroidal Perfusion in Giant Cell Arteritis H. G. Mack, B. Me SC., M.B.B.S., J. O'Day, F.R.A.C.P.,
Tournai of Clinical Neuro-ophthalmology 11(4): 221-227,1991. 1991 Raven Press, Ltd., New York Delayed Choroidal Perfusion in Giant Cell Arteritis H. G. Mack, B. Me SC., M.B.B.S., J. O'Day, F.R.A.C.P.,
Factors Influencing Visual Field Recovery after Transsphenoidal Resection of a Pituitary Adenoma
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(6):488-496 https://doi.org/10.3341/kjo.2017.0094 Original Article Factors Influencing Visual Field Recovery after Transsphenoidal Resection
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(6):488-496 https://doi.org/10.3341/kjo.2017.0094 Original Article Factors Influencing Visual Field Recovery after Transsphenoidal Resection
10/27/2013. Optic Red Herrings
 Optic Red Herrings 1 Optic neuropathy Compressive Inflammatory Toxic Glaucomatous Ischemic Post traumatic GLAUCOMATOUS OPTIC NEUROPATHY Glaucoma: Traditionally defined as a progressive optic neuropathy
Optic Red Herrings 1 Optic neuropathy Compressive Inflammatory Toxic Glaucomatous Ischemic Post traumatic GLAUCOMATOUS OPTIC NEUROPATHY Glaucoma: Traditionally defined as a progressive optic neuropathy
Congenital Aniridia: Long-term Clinical Course, Visual Outcome, and Prognostic Factors
 pissn: 111-894 eissn: 9-938 Korean J Ophthalmol 14;8(6):479-485 http://dx.doi.org/1.3341/kjo.14.8.6.479 Original Article Congenital Aniridia: Long-term Clinical Course, Visual Outcome, and Prognostic Factors
pissn: 111-894 eissn: 9-938 Korean J Ophthalmol 14;8(6):479-485 http://dx.doi.org/1.3341/kjo.14.8.6.479 Original Article Congenital Aniridia: Long-term Clinical Course, Visual Outcome, and Prognostic Factors
Christopher Kin Ming Orr, M.D. Clinical Assistant Instructor, College of Medicine SUNY Downstate Medical Center
 Christopher Kin Ming Orr, M.D. Clinical Assistant Instructor, College of Medicine SUNY Downstate Medical Center Presentation 52 y/o Caucasian woman presents with painless decreased vision in left eye x
Christopher Kin Ming Orr, M.D. Clinical Assistant Instructor, College of Medicine SUNY Downstate Medical Center Presentation 52 y/o Caucasian woman presents with painless decreased vision in left eye x
Speaker Disclosure Statement. " Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose.
 Speaker Disclosure Statement Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose. Diabetes Morbidity Diabetes doubles the risk of stroke. Diabetes quadruples the risk of
Speaker Disclosure Statement Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose. Diabetes Morbidity Diabetes doubles the risk of stroke. Diabetes quadruples the risk of
A Valid Indication and the Effect of Bilateral Inferior Oblique Transposition on Recurrent or Consecutive Horizontal Deviation in Infantile Strabismus
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):138-142 https://doi.org/10.3341/kjo.2017.31.2.138 Original Article A Valid Indication and the Effect of Bilateral Inferior Oblique Transposition
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):138-142 https://doi.org/10.3341/kjo.2017.31.2.138 Original Article A Valid Indication and the Effect of Bilateral Inferior Oblique Transposition
Purtscher s retinopathy: A case of severe bilateral visual loss due to chest compression
 O P E N A C C E S S Case study Purtscher s retinopathy: A case of severe bilateral visual loss due to chest compression Shakeel P Hashim, Maha M El Shafei, Zakia M Al Ansari Hamad Medical Corporation,
O P E N A C C E S S Case study Purtscher s retinopathy: A case of severe bilateral visual loss due to chest compression Shakeel P Hashim, Maha M El Shafei, Zakia M Al Ansari Hamad Medical Corporation,
Pattern Visual Evoked Cortical Potentials in Patients With Toxic Optic Neuropathy Caused by Toluene Abuse
 Pattern Visual Evoked Cortical Potentials in Patients With Toxic Optic Neuropathy Caused by Toluene Abuse Masahiro Kiyokawa, Atsushi Mizota, Michihiko Takasoh and Emiko Adachi-Usami Department of Ophthalmology,
Pattern Visual Evoked Cortical Potentials in Patients With Toxic Optic Neuropathy Caused by Toluene Abuse Masahiro Kiyokawa, Atsushi Mizota, Michihiko Takasoh and Emiko Adachi-Usami Department of Ophthalmology,
Patterns of Subsequent Progression of Localized Retinal Nerve Fiber Layer Defects on Red-free Fundus Photographs in Normal-tension Glaucoma
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):330-336 http://dx.doi.org/10.3341/kjo.2014.28.4.330 Original Article Patterns of Subsequent Progression of Localized Retinal Nerve Fiber
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):330-336 http://dx.doi.org/10.3341/kjo.2014.28.4.330 Original Article Patterns of Subsequent Progression of Localized Retinal Nerve Fiber
EXPERIMENTAL AND THERAPEUTIC MEDICINE 6: , 2013
 268 Comparison of optic nerve morphology in eyes with glaucoma and eyes with non-arteritic anterior ischemic optic neuropathy by Fourier domain optical coherence tomography YUXIN YANG 1, HAITAO ZHANG 1,
268 Comparison of optic nerve morphology in eyes with glaucoma and eyes with non-arteritic anterior ischemic optic neuropathy by Fourier domain optical coherence tomography YUXIN YANG 1, HAITAO ZHANG 1,
Acute inflammatory demyelinating optic. optic neuritis: current concepts in diagnosis and
 Acute inflammatory demyelinating optic neuritis: current concepts in diagnosis and management M. Tariq Bhatti, M.D., a Nicholas J. Schmitt, M.D., b and Randall L. Beatty, M.D., O.D. b a Departments of
Acute inflammatory demyelinating optic neuritis: current concepts in diagnosis and management M. Tariq Bhatti, M.D., a Nicholas J. Schmitt, M.D., b and Randall L. Beatty, M.D., O.D. b a Departments of
Clinically isolated syndromes (CIS) may
 RECOGNIZING AND MANAGING THE CLINICALLY ISOLATED SYNDROME* Steven L. Galetta, MD ABSTRACT Clinically isolated demyelinating syndromes, such as optic neuritis, transverse myelitis, and brain-stem disorders,
RECOGNIZING AND MANAGING THE CLINICALLY ISOLATED SYNDROME* Steven L. Galetta, MD ABSTRACT Clinically isolated demyelinating syndromes, such as optic neuritis, transverse myelitis, and brain-stem disorders,
Research Article Optic Neuritis in the Older Chinese Population: A 5-Year Follow-Up Study
 Hindawi Ophthalmology Volume 217, Article ID 3458356, 7 pages https://doi.org/1.1155/217/3458356 Research Article Optic Neuritis in the Older Chinese Population: A 5-Year Follow-Up Study Junqing Wang,
Hindawi Ophthalmology Volume 217, Article ID 3458356, 7 pages https://doi.org/1.1155/217/3458356 Research Article Optic Neuritis in the Older Chinese Population: A 5-Year Follow-Up Study Junqing Wang,
ISCHEMIC OPTIC neuropathy (ION)
 OBSERVATION Ischemic Optic Neuropathy Associated With Internal Carotid Artery Dissection Valérie Biousse, MD; Monique Schaison, MD; Pierre-Jean Touboul, MD; Jacques D Anglejan-Chatillon, MD; Marie-Germaine
OBSERVATION Ischemic Optic Neuropathy Associated With Internal Carotid Artery Dissection Valérie Biousse, MD; Monique Schaison, MD; Pierre-Jean Touboul, MD; Jacques D Anglejan-Chatillon, MD; Marie-Germaine
A trial of corticotrophin gelatin injection in
 Journal of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 869-873 A trial of corticotrophin gelatin injection in acute optic neuritis A. N. BOWDEN, P. M. A. BOWDEN, A. I. FRIEDMANN, G. D. PERKIN, AND
Journal of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 869-873 A trial of corticotrophin gelatin injection in acute optic neuritis A. N. BOWDEN, P. M. A. BOWDEN, A. I. FRIEDMANN, G. D. PERKIN, AND
CHAPTER 13 CLINICAL CASES INTRODUCTION
 2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
3/16/2018. Optic Nerve Examination. Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital
 Optic Nerve Examination Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Examination Structure ( optic disc) Function Examination of the optic disc The only cranial nerve (brain tract) which
Optic Nerve Examination Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Examination Structure ( optic disc) Function Examination of the optic disc The only cranial nerve (brain tract) which
MOVE IT OR LOSE IT: THE ROLE OF KINETIC VISUAL FIELDS
 MOVE IT OR LOSE IT: THE ROLE OF KINETIC VISUAL FIELDS Course Objectives Review the visual field Review types of perimetry Discuss advantages and disadvantages of different types of visual field testing
MOVE IT OR LOSE IT: THE ROLE OF KINETIC VISUAL FIELDS Course Objectives Review the visual field Review types of perimetry Discuss advantages and disadvantages of different types of visual field testing
No Financial Interest
 Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
PDE-5 Inhibitors and the Increase Risk of Nonarteritic Anterior Ischemic Optic Neuropathy in Males with Erectile Dysfunction
 Pacific University CommonKnowledge School of Physician Assistant Studies College of Health Professions Summer 8-12-2017 PDE-5 Inhibitors and the Increase Risk of Nonarteritic Anterior Ischemic Optic Neuropathy
Pacific University CommonKnowledge School of Physician Assistant Studies College of Health Professions Summer 8-12-2017 PDE-5 Inhibitors and the Increase Risk of Nonarteritic Anterior Ischemic Optic Neuropathy
Professor Helen Danesh-Meyer. Eye Institute Auckland
 Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Neutrophil to Lymphocyte Ratio in Patients with Nonarteritic Anterior Ischemic Optic Neuropathy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):159-164 https://doi.org/10.3341/kjo.2017.31.2.159 Original Article Neutrophil to Lymphocyte Ratio in Patients with Nonarteritic Anterior
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):159-164 https://doi.org/10.3341/kjo.2017.31.2.159 Original Article Neutrophil to Lymphocyte Ratio in Patients with Nonarteritic Anterior
Clinical Profile and Aetiology of Optic Neuritis in Hospital Universiti Sains Malaysia 5 Years Review
 ORIGINAL ARTICLE Clinical Profile and Aetiology of Optic Neuritis in Hospital Universiti Sains Malaysia 5 Years Review Ismail Shatriah, MMed (Ophthal), Wan Hazabbah Wan Hitam, MSurg (Ophthal), Muhd-Nor
ORIGINAL ARTICLE Clinical Profile and Aetiology of Optic Neuritis in Hospital Universiti Sains Malaysia 5 Years Review Ismail Shatriah, MMed (Ophthal), Wan Hazabbah Wan Hitam, MSurg (Ophthal), Muhd-Nor
Case Report Optic Disk Pit with Sudden Central Visual Field Scotoma
 Case Reports in Ophthalmological Medicine Volume 2016, Article ID 1423481, 4 pages http://dx.doi.org/10.1155/2016/1423481 Case Report Optic Disk Pit with Sudden Central Visual Field Scotoma Nikol Panou
Case Reports in Ophthalmological Medicine Volume 2016, Article ID 1423481, 4 pages http://dx.doi.org/10.1155/2016/1423481 Case Report Optic Disk Pit with Sudden Central Visual Field Scotoma Nikol Panou
Long-term Surgical Outcomes of Initial Postoperative Overcorrection in Adults with Intermittent Exotropia
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(3):228-233 https://doi.org/10.3341/kjo.2017.0064 Original Article Long-term Surgical Outcomes of Initial Postoperative Overcorrection in Adults
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(3):228-233 https://doi.org/10.3341/kjo.2017.0064 Original Article Long-term Surgical Outcomes of Initial Postoperative Overcorrection in Adults
NEURO-OPHTHALMIC ASSESSMENT DR. B. C. UGWU
 CLINICAL VIGNETTE 2019; 5:1 NEURO-OPHTHALMIC ASSESSMENT DR. B. C. UGWU Editor-in-Chief: Prof Olufemi Idowu Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria. Copyright-
CLINICAL VIGNETTE 2019; 5:1 NEURO-OPHTHALMIC ASSESSMENT DR. B. C. UGWU Editor-in-Chief: Prof Olufemi Idowu Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria. Copyright-
The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery
 The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery The Case: Upon awakening from anesthesia, he is blind in both eyes After Non-Ocular Surgeries Nancy J. Newman,
The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery The Case: Upon awakening from anesthesia, he is blind in both eyes After Non-Ocular Surgeries Nancy J. Newman,
Evaluation of optic disc blood flow of intraconal orbital tumors using laser speckle flowgraphy.
 Research Article http://www.alliedacademies.org/ophthalmic-and-eye-research/ Evaluation of optic disc blood flow of intraconal orbital tumors using laser speckle flowgraphy. Hideki Chuman*, Takako Hidaka,
Research Article http://www.alliedacademies.org/ophthalmic-and-eye-research/ Evaluation of optic disc blood flow of intraconal orbital tumors using laser speckle flowgraphy. Hideki Chuman*, Takako Hidaka,
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
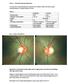 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
The optic disc in glaucoma, III: diffuse optic disc pallor with raised intraocular pressure
 British Journal of Ophthalmology, 1978, 62, 670-675 The optic disc in glaucoma, III: diffuse optic disc pallor with raised intraocular pressure R. A. HITCHINGS From the Institute of Ophthalmology, Moorfields
British Journal of Ophthalmology, 1978, 62, 670-675 The optic disc in glaucoma, III: diffuse optic disc pallor with raised intraocular pressure R. A. HITCHINGS From the Institute of Ophthalmology, Moorfields
Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient
 CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
Hyperbaric Oxygen Therapy in two patients with Non-arteritic Anterior Optic Neuropathy who did not respond to Prednisone
 Case Report Hyperbaric Oxygen Therapy in two patients with Non-arteritic Anterior Optic Neuropathy who did not respond to Prednisone L BOJIĆ, M. IVANIŠEVIĆ, G.GOŠOVIĆ Eye Clinic, Clinical Hospital Split
Case Report Hyperbaric Oxygen Therapy in two patients with Non-arteritic Anterior Optic Neuropathy who did not respond to Prednisone L BOJIĆ, M. IVANIŠEVIĆ, G.GOŠOVIĆ Eye Clinic, Clinical Hospital Split
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
University Hospital Basel. Optical Coherence Tomography Emerging Role in the Assessment of MS PD Dr. Konstantin Gugleta
 University Hospital Basel Optical Coherence Tomography Emerging Role in the Assessment of MS PD Dr. Konstantin Gugleta 15th State of the Art SMSS, Lucerne January 2013 Retinal Nerve Fiber Layer 1.200.000
University Hospital Basel Optical Coherence Tomography Emerging Role in the Assessment of MS PD Dr. Konstantin Gugleta 15th State of the Art SMSS, Lucerne January 2013 Retinal Nerve Fiber Layer 1.200.000
Optic neuritis More than a loss of vision
 clinical practice Edward R Chu MBBS, is resident medical officer, Department of Ophthalmology, Flinders Medical Centre and Flinders University, South Australia. Celia S Chen MBBS, MPHC, FRANZCO, is a consultant
clinical practice Edward R Chu MBBS, is resident medical officer, Department of Ophthalmology, Flinders Medical Centre and Flinders University, South Australia. Celia S Chen MBBS, MPHC, FRANZCO, is a consultant
Radiation Chiasma Neuropathy after Radiotherapy for Treatment of Paranasal Sinus lymphoma
 Radiation Chiasma Neuropathy after Radiotherapy for Treatment of Paranasal Sinus lymphoma Mohammad Pakravan, MD 1 Bagher Hosseiny, MD 2 Mostafa Soltan-Sanjari, MD 3 Abstract Purpose: To present a patient
Radiation Chiasma Neuropathy after Radiotherapy for Treatment of Paranasal Sinus lymphoma Mohammad Pakravan, MD 1 Bagher Hosseiny, MD 2 Mostafa Soltan-Sanjari, MD 3 Abstract Purpose: To present a patient
MRI Imaging of Neuromyelitis Optica
 July 2009 MRI Imaging of Neuromyelitis Optica Jenna Nolan, Harvard Medical School Year III Gillian Lieberman, MD Our Patient: Initial Presentation J.H. is a 29 year-old woman who presents with acute vision
July 2009 MRI Imaging of Neuromyelitis Optica Jenna Nolan, Harvard Medical School Year III Gillian Lieberman, MD Our Patient: Initial Presentation J.H. is a 29 year-old woman who presents with acute vision
Local Intra-arterial Fibrinolysis in Treatment of Incomplete Ophthalmic Artery Occlusion A Case Report
 CASE REPORT Local Intra-arterial Fibrinolysis in Treatment of Incomplete Ophthalmic Artery Occlusion A Case Report Shih-Ting Fang, Pao-Sheng Yen 1, Chien-Chung Chen, Yuan-Chieh Lee Department of Ophthalmology,
CASE REPORT Local Intra-arterial Fibrinolysis in Treatment of Incomplete Ophthalmic Artery Occlusion A Case Report Shih-Ting Fang, Pao-Sheng Yen 1, Chien-Chung Chen, Yuan-Chieh Lee Department of Ophthalmology,
Microscopic Characteristics of Lower Eyelid Retractors in Koreans
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(5):344-348 http://dx.doi.org/10.3341/kjo.2011.25.5.344 Original Article Microscopic Characteristics of Lower Eyelid Retractors in Koreans Won-Kyung
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(5):344-348 http://dx.doi.org/10.3341/kjo.2011.25.5.344 Original Article Microscopic Characteristics of Lower Eyelid Retractors in Koreans Won-Kyung
Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(4):238-242 DOI: 10.3341/kjo.2011.25.4.238 Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery Original
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(4):238-242 DOI: 10.3341/kjo.2011.25.4.238 Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery Original
Time Series Changes in Cataract Surgery in Korea
 pissn: 111-8942 eissn: 292-9382 Korean J Ophthalmol 218;32(3):182-189 https://doi.org/1.3341/kjo.217.72 Time Series Changes in Cataract Surgery in Korea Original Article Ju Hwan Song 1*, Jung Youb Kang
pissn: 111-8942 eissn: 292-9382 Korean J Ophthalmol 218;32(3):182-189 https://doi.org/1.3341/kjo.217.72 Time Series Changes in Cataract Surgery in Korea Original Article Ju Hwan Song 1*, Jung Youb Kang
The Comparison of the Result of Epiduroscopic Laser Neural Decompression between FBSS or Not
 Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Systemic lupus erythematosusassociated optic neuritis: clinical experience and literature review
 Systemic lupus erythematosusassociated optic neuritis: clinical experience and literature review Yen-Ching Lin, 1,2,3 An-Guor Wang 2,3 and May-Yung Yen 2,3 1 Department of Ophthalmology, Suao Veterans
Systemic lupus erythematosusassociated optic neuritis: clinical experience and literature review Yen-Ching Lin, 1,2,3 An-Guor Wang 2,3 and May-Yung Yen 2,3 1 Department of Ophthalmology, Suao Veterans
Research Article Clinical Efficacy Observation of Acupuncture Treatment for Nonarteritic Anterior Ischemic Optic Neuropathy
 Evidence-Based Complementary and Alternative Medicine Volume 2015, Article ID 713218, 6 pages http://dx.doi.org/10.1155/2015/713218 Research Article Clinical Efficacy Observation of Acupuncture Treatment
Evidence-Based Complementary and Alternative Medicine Volume 2015, Article ID 713218, 6 pages http://dx.doi.org/10.1155/2015/713218 Research Article Clinical Efficacy Observation of Acupuncture Treatment
Optic Disk Pit with Sudden Central Visual Field Scotoma
 Optic Disk Pit with Sudden Central Visual Field Scotoma The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version
Optic Disk Pit with Sudden Central Visual Field Scotoma The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version
Minami-Hori M, Tsuji H, Takahashi H, Hanada K, Iizuka H
 The Journal of Dermatology (2013.Jan) :. Optic neuritis in a psoriatic arthritis patient treated by infliximab Minami-Hori M, Tsuji H, Takahashi H, Hanada K, Iizuka H 1 Optic neuritis in a psoriatic arthritis
The Journal of Dermatology (2013.Jan) :. Optic neuritis in a psoriatic arthritis patient treated by infliximab Minami-Hori M, Tsuji H, Takahashi H, Hanada K, Iizuka H 1 Optic neuritis in a psoriatic arthritis
Bilateral Posterior Ischemic Optic Neuropathy in a Patient with Severe Diabetic Ketoacidosis
 Bilateral Posterior Ischemic Optic Neuropathy in a Patient with Severe Diabetic Ketoacidosis The Harvard community has made this article openly available. Please share how this access benefits you. Your
Bilateral Posterior Ischemic Optic Neuropathy in a Patient with Severe Diabetic Ketoacidosis The Harvard community has made this article openly available. Please share how this access benefits you. Your
Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
 Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Unexplained visual loss in seven easy steps
 Unexplained visual loss in seven easy steps Andrew G. Lee, MD Chair Ophthalmology, Houston Methodist Hospital, Professor, Weill Cornell MC; Adjunct Professor, Baylor COM, U Iowa, UTMB Galveston, UT MD
Unexplained visual loss in seven easy steps Andrew G. Lee, MD Chair Ophthalmology, Houston Methodist Hospital, Professor, Weill Cornell MC; Adjunct Professor, Baylor COM, U Iowa, UTMB Galveston, UT MD
Objectives. Unexplained Vision Loss: Where Do I Go From Here. History. History. Drug Induced Vision Loss
 Objectives Unexplained Vision Loss: Where Do I Go From Here Denise Goodwin, OD, FAAO Coordinator, Neuro-ophthalmic Disease Clinic Pacific University College of Optometry goodwin@pacificu.edu Know the importance
Objectives Unexplained Vision Loss: Where Do I Go From Here Denise Goodwin, OD, FAAO Coordinator, Neuro-ophthalmic Disease Clinic Pacific University College of Optometry goodwin@pacificu.edu Know the importance
12/2/16. Ways to differentiate:
 Nate Lighthizer, O.D., F.A.A.O. Assistant Dean for Clinical Care Services Director of CE Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Oklahoma College of Optometry lighthiz@nsuok.edu
Nate Lighthizer, O.D., F.A.A.O. Assistant Dean for Clinical Care Services Director of CE Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Oklahoma College of Optometry lighthiz@nsuok.edu
Clinical Features of Ocular Ischemic Syndrome and Risk Factors for Neovascular Glaucoma
 pissn: 1011-8942 eissn: 2092-9382 2017 Jun 26. [Epub ahead of print] https://doi.org/10.3341/kjo.2016.0067 Original Article Clinical Features of Ocular Ischemic Syndrome and Risk Factors for Neovascular
pissn: 1011-8942 eissn: 2092-9382 2017 Jun 26. [Epub ahead of print] https://doi.org/10.3341/kjo.2016.0067 Original Article Clinical Features of Ocular Ischemic Syndrome and Risk Factors for Neovascular
