Role of Radiation Therapy in Benign Brain Tumors
|
|
|
- Bruce Powers
- 5 years ago
- Views:
Transcription
1 Role of Radiation Therapy in Benign Brain Tumors Dr. Vivek Kaushal MD DNB Sr. Professor and Head Department of Radiotherapy, Regional Cancer Centre Pt. B. D. Sharma Post Graduate Institute of Medical Sciences, Rohtak, Haryana. 1
2 Brain Tumors Worldwide, approximately 238,000 new cases of brain and other CNS tumors with an estimated 175,000 deaths Estimated new cases and deaths from brain and other nervous system tumors in the United States in 2015 New cases: 22,850. Deaths: 15,320. NCI Database
3 Principles of Radiation Treatment in Benign Diseases 1. Estimate the natural course of disease without therapy. 2. Consider potential consequences of non treatment of the patient. 3. Review data about alternative therapies and their therapeutic results. 4. Conduct a risk-benefit analysis compared with other possible measures. 3
4 Principles of Radiation Treatment in Benign Diseases 5. Proof that the indication is justified Conventional therapies have failed Risks of other therapies are greater Non treatment has unacceptable consequences. 6. Consider the individual potential long-term radiogenic risks. 7. Inform patient about all details of radiotherapy 4
5 Principles of Radiation Treatment in Benign Diseases 8. Written consent of the patient following thorough patient education. 9. Assurance of long-term aftercare in order to document result. 10. Second opinion in case of doubts and if the provided patient data or treatment decision are uncertain. 5
6 Benign Brain Tumors Clinical Tip Whether primary, metastatic, malignant, or benign, brain tumors must be differentiated from other space-occupying lesions such as abscesses, arteriovenous malformations, and infarction, which can have a similar clinical presentation. Seizures are a presenting symptom in approximately 20% of patients with supratentorial brain tumors and may antedate the clinical diagnosis by months to years in patients with slowgrowing tumors. 6
7 Benign Brain Tumors & Diseases treated by RT Meningioma Pituitary tumors Craniopharyngioma Hemangioblastoma and Hemaniopericytoma Glomus Jugulare Tumor Pineocytoma Chordoma Vestibular Schwannoma Ganglioglioma Central Neurocytoma Arteriovenous Malformations 7
8 What are the Radiation Techniques available for treatment of benign brain Tumors? Conventional Two Dimensional Planning Conventionally fractionated three dimensional conformal radiotherapy (3DCRT) Conventionally fractionated intensity-modulated radiation therapy (IMRT) Stereotactic radiosurgery (SRS) Fractionatied Stereotactic radiosurgery (FRS) 2-5 F Frame-based or linear accelerator based fractionated stereotactic radiotherapy SRT Protons and heavy ions. 8
9 Stereotactic RadioSurgery (SRS) and Radiotherapy (SRT) Stereotactic refers to using a precise three-dimensional mapping technique to guide a procedure Stereotactic radiosurgery and radiotherapy are techniques to administer precisely directed, high-dose irradiation that tightly conforms to target to create a desired radiobiologic response while minimizing radiation dose to surrounding normal tissue 9
10 Fractionated Stereotactic RadioSurgery (FSR) The term fractionated stereotactic radiosurgery (FSR) is limited to stereotactically guided high-dose conformal radiation administered to a precisely defined target volume in two to five sessions. Although it would have been less confusing to refer to this as hypofractionated SRT and reserve the term radiosurgery for single-fraction irradiation, the terminology is already in use. 10
11 Stereotactic RadioSurgery (SRS) and Radiotherapy (SRT) Techniques Gamma Knife Radiosurgery usually 201 Cobalt sources Rotating Gamma System 30 Cobalt sources China Proton Radiosurgery LINAC Radiosurgery Many LINAC-based systems such as CyberKnife (Accuray Inc XKnife (Radionics Inc.), Novalis (BrainLAB), Peacock System (NOMOS Corp) are commercially available. Tomotherapy Slice Therapy, Add 6MV linac Beam to Diagnostic CT Scan LINAC Image-Guided Radiotherapy Add Diagnostic CT Scan technology to a Linear accelerator 11
12 Stereotactic Radiosurgery Radiation Therapy Oncology Group (RTOG) study established the maximum tolerated dose of single faction SRS to be 24 Gy for 20 mm 18 Gy for 21 to 30 mm 15 Gy for tumors 31 to 40 mm in size 12
13 Fractionated Stereotactic Radiotherapy For lesions larger than 4 cm and/or located in critical regions, the delivery of a single large-fraction treatment as in SRS is not desirable because of a high risk of CNS toxicity. Fractionated stereotactic radiotherapy (FSRT) is a hybrid between conventionally fractionated radiotherapy and SRS that combines fractionation with stereotactic localization and targeting techniques. Various systems for FSRT have been developed, with a reported accuracy of 1 to 3 mm. As for SRS, the use of multiple arcs and circular collimators for irregularly shaped lesions leads to the inclusion of a large amount of normal tissue. The use of multiple noncoplanar fixed fields each having a unique entrance and exit pathway is preferable because of better conformality because multileaf collimators are almost always used. With the Perfexion device, the use of the Extend frame permits FSRT, as well as targeting of lower cranial lesions. 13
14 Meningeal Tumors Meningiomas are the most common benign tumors of the CNS. The incidence peaks in the seventh decade of life 2 to 1 female-to-male predominance Meningiomas are extraaxial tumors that arise from dura; common locations are cerebral convexity, parasagittal falx, and sphenoid ridge. The majority (>90%) of meningiomas are benign and classified by the World Health Organization (WHO) as grade I tumors WHO grade II meningiomas (atypical, clear cell, or chordoid) have a higher tendency for local recurrence WHO grade III malignant meningiomas (anaplastic, rhabdoid, papillary) are exceedingly rare 14
15 Meningioma A very long natural history is characteristic, mandating prolonged follow-up. More than 90% of these tumors are benign; the remainder exhibit atypical histologic features or frank invasion of brain parenchyma. Primary treatment is surgical, if feasible. Radiation therapy is reserved for tumors that are incompletely resected, recur after surgery, are inaccessible to surgical resection, or have atypical or invasive features. The standard radiation dose has been approximately 54 Gy for benign meningiomas and up to 60 Gy for tumors with atypical or invasive features. Stereotactic radiation therapy techniques have been used; however, followup is still short in these studies. Anecdotal reports exist of responses to medical therapy (hydroxyurea and antiestrogen and antiprogesterone agents 15
16 Meningeal Tumors Grade I meningiomas Active surveillance with deferred treatment, especially for incidentally discovered asymptomatic tumors. Surgery. Stereotactic radiosurgery for tumors less than 3 cm. Surgery plus radiation therapy is used in selected cases, such as for patients with known or suspected residual disease or with recurrence after previous surgery. Fractionated radiation therapy for patients with unresectable tumors. WHO grade I meningiomas are usually curable when the mengiomas are resectable. With the increasing use of sensitive neuroimaging tools, there has been greater detection of asymptomatic low-grade meningiomas. The majority appear to show minimal growth and can often be safely observed while therapy is deferred until growth or the development of symptoms. 16
17 Meningeal Tumors Surgical Resection Maximal safe resection Relapse rate is as low as 10% Local recurrence rates are as high as 40% for patients with incomplete resection, although these rates can be substantially reduced with the use of adjuvant radiotherapy. Meningiomas tend to be highly vascularized tumors. In select patients, preoperative embolization is used to decrease blood loss and improve the extent of resection. 17
18 Meningeal Tumors Radiotherapy Primary radiotherapy (RT) is indicated for tumors in locations in which complete resection is not feasible (i.e., optic nerve, cavernous sinus, major venous sinus) or for patients who are poor surgical candidates. Adjuvant RT is indicated for patients with subtotal resection (STR), Recurrent disease, or for WHO grade II or III tumors. RT techniques include conventionally fractionated threedimensional conformal radiotherapy (3D-CRT), conventionally fractionated intensity-modulated radiation therapy (IMRT), frame-based or linear accelerator based fractionated stereotactic radiotherapy (FSRT), stereotactic radiosurgery (SRS), or protons and heavy ions. 18
19 Meningeal Tumors Radiotherapy For 3D-CRT or IMRT treatments, the clinical target volume (CTV) is constructed by adding a 1- or 2-cm symmetric margin around the GTV 54 Gy/30F/6weeks given in 1.8 daily fractions. For patients with more aggressive histology (WHO grade II or III tumors), the GTV is expanded by at least 2 cm, with a higher dose prescription in the range of 60 Gy. Several modern series of radiotherapy show 5-year local control rates >95% 19
20 Radiosurgery and SRS Meningeal Tumors Radiosurgery and SRS are both excellent management options for most small benign meningiomas, with in-field tumor control rates well above 90%, as has been seen with most other benign tumors. Marginal recurrence rates as high as 25% may develop because of the tight margins used for radiosurgery or SRT treatment volumes limited to small recurrences or residual tumor after resection of large parasagittal meningiomas. Marginal recurrences are far less of a problem with unresected (and usually unbiopsied) meningiomas. 20
21 Radiosurgery and FSRS Meningeal Tumors 16 Gy to 80% isodose line (IDL) 1 or 2 fractions. FSRT dose 30 Gy in 5 fractions near optic nerve (to the 80% IDL) with high rates of tumor control and visual preservation Reported results with SRS are excellent, with 5-year local control rates as high as 98% to 100% Male gender, conformality index <1.4, and size >10 ml predict for worse outcome after SRS. 21
22 Radiosurgery and SRS Unbiopsied Meningeal Tumors A University of Pittsburgh study, analyzed 219 imaging-diagnosed meningiomas (unbiopsied) managed with gamma knife radiosurgery to a prescription dose of 8.9 to 20 Gy (median, 14 Gy) The actuarial tumor control rate was 93.2% at 10 years. The actuarial rate for developing any postradiosurgical injury reaction was 8.8% The risk of postradiosurgery sequelae was lower (5.3%) after
23 Meningeal Tumors Grade II meningiomas Surgery plus radiation therapy. The prognoses for patients with meningiomas (WHO grade II) (i.e., atypical, clear cell, and chordoid), meningiomas (WHO grade III) (i.e., anaplastic/malignant, rhabdoid, and papillary), and hemangiopericytomas are worse than are those for patients with lowgrade meningiomas because complete resections are less commonly feasible, and the proliferative capacity is greater. 23
24 Meningioma Evidence- Based Treatment Summary 1. Small asymptomatic meningiomas in noncritical locations, especially in the elderly or in patients with other comorbidities, can be observed. 2. The goal of surgery is to completely resect the meningioma with negative margins, as patients with WHO grade I completely resected meningiomas have low rates of relapse and can be observed postoperatively. 3. For subtotally resected or unresectable progressive meningioma radiotherapy is frequently used but has not been tested in a prospective clinical trial. Local control appears to be improved with postoperative radiotherapy. Both radiosurgery and radiotherapy have been used in this context but have not been directly compared. 4. For grades II and III meningioma, postoperative radiotherapy is routinely recommended. 5. Primary radiotherapy or radiosurgery could be used for unresectable, progressive meningiomas. 6. Systemic therapy does not have a defined role in meningioma. 24
25 Pineal Parenchymal Tumors Standard treatment options: Surgery plus radiation therapy for pineocytoma. Surgery plus radiation therapy and chemotherapy for pineoblastoma. Pineocytoma (WHO grade II), pineoblastoma (WHO grade IV), and pineal parenchymal tumors of intermediate differentiation are diverse tumors that require special consideration. Pineocytomas are slow-growing tumors, and patients with them carry variable prognoses for cure. Pineoblastomas are more rapidly growing tumors, and patients with them have worse prognoses. Pineal parenchymal tumors of intermediate differentiation have unpredictable growth and clinical behavior. 25
26 Craniopharyngiomas They are thought to be vestigial remnants of the Rathke s pouch, representing about 2% of intracranial tumors, occurring about half the time in children and young adults. Craniopharyngiomas are frequently calcified and can be visualized radiographically. They are usually about 3.5 cm in diameter, encapsulated, and solid but can be cystic or multilobulated. They can displace cranial nerves and the optic chiasm and protrude into the floor of the third ventricle. In children, they can cause growth retardation. Adults usually present with visual disturbances. Both can demonstrate hormonal disturbances and diabetes insipidus. Histologically there can be two forms. The adamantinomatous form and papillary craniopharyngioma. Perez
27 Craniopharyngiomas Standard treatment options: Surgery alone if the tumor is totally resectable. Debulking surgery plus radiation therapy if the tumor is unresectable. Craniopharyngiomas (WHO grade I) are often curable. 27
28 Craniopharyngiomas Axial, coronal, and sagittal magnetic resonance imaging of a patient with multicystic (yellow arrows) craniopharyngioma prior to treatment 28
29 Craniopharyngiomas 1.Surgical resection is recommended, when feasible. 2. The use of postoperative radiotherapy has not been tested in prospective trials but reduces the risk of recurrence and improves survival in incompletely resected tumors. Cyst decompression and biopsy followed by radiotherapy may be an acceptable treatment for patients for whom resection is not considered feasible. 3. Intracavitary bleomycin or radiocolloids may be useful in cystic tumors. Perez
30 RT in Craniopharyngioma Radiation therapy is often used in the adjuvant setting. In select patients (i.e., <3 years old), observation following STR may be an option as local control rates are similar with RT at the time of relapse ( salvage RT) compared with adjuvant RT with no compromise in overall survival. RT techniques include 3D-CRT, IMRT, FSRT, proton therapy, and intralesional RT with β-emitting isotopes (yttrium-90, phosphorous-32). The GTV is the postoperative residual tumor volume, including the cyst wall, if present. A margin of 1 to 1.5 cm is added to the GTV to create the PTV. Dose prescriptions for 3D-CRT and IMRT are typically 54 Gy given in 1.8-Gy daily fractions. Perez
31 SRS and FRST in Craniopharyngioma SRS and FSRT have been used with success in the treatment of craniopharyngioma. In one series from Stanford University using a frameless robotic platform, 16 patients were treated postoperatively with doses of 18 to 38 Gy given over 3 to 10 fractions prescribed to mean IDL of 75%. Local control was 91% in this cohort of patients with no visual or neuroendocrine complications. Cystic craniopharyngiomas may also be managed by the use of intralesional radioactive isotope injection using a β-emitter. Typical prescriptions range from 200 to 250 Gy prescribed to the cyst wall. Optimal results are seen in patients whose tumors have one cyst and lack a large solid component. Perez
32 Arteriovenous malformations AVM AVMs arise in the brain, spine, lungs, kidneys and skin. Brain AVMs are the most common. AVMs are an abnormal connection between the arteries and veins. Arteriovenous malformations are most commonly of prenatal origin. The overall ratio of AVMs to aneurysms is probably in the range of 1:10. Most patients present between the ages of 20 and 60 years of age. The mean age is about AVMs are equally distributed between male/female. 32
33 Arteriovenous malformations AVM It is estimated that 1 in have an AVM in the brain. When an AVM bleeds, there is a 10-15% risk of death related to each bleed and a 20-30% chance of permanent brain damage. The risk of bleeding is higher in the first years after the first bleed. In about 50% of patients the presentation is a sudden hemorrhage, or bleeding into the brain, a form of stroke. Other potential complications include seizures, headaches, and stroke-like symptoms (difficulty with movement, speech, and vision). These complications may occur in conjunction with, or independently of, hemorrhage. About 5-10% of AVMs are discovered by accident while the individual is being tested for other unrelated medical problems. 33
34 Arteriovenous malformations AVM before and after Radiosurgery Upper row (before radiosurgery), Lateral right carotid digital subtraction angiogram shows a parietal AVM with arteriovenous shunts and early venous drainage (black arrow); collapsed-view 3D time-of-flight MR angiogram and T1- and T2-wighted transaxial MR images show the AVM (yellow arrows). Lower row (13 months after radiosurgery), MR images show the partially regressed AVM nidus and mild 34 radiation-induced edema (red arrow). AJNR :
35 Arteriovenous malformations AVM AVM size Adjacent eloquent cortex Draining veins Under 3 cm = 1 Non-eloquent = 0 Superficial only = cm = 2 Eloquent* = 1 Deep veins = 1 Over 6 cm = 3 A common method of grading cerebral AVMs is the Spetzler-Martin grade. [5] This system was designed to assess the patient's risk of neurological deficit after open surgical resection (surgical morbidity), based on characteristics of the AVM itself. Based on this system, AVMs may be classified as grades 1-5. This system was not intended to characterize risk of hemorrhage. "Eloquent cortex" is a name used by neurologists for areas of cortex that, if removed will result in loss of sensory processing or linguistic ability, minor paralysis, or paralysis. The risk of post-surgical neurological deficit (difficulty with language, motor weakness, vision loss) increases with increasing Spetzler-Martin grade. 35
36 Stereotactic RadioSurgery Effect of location on the risk of developing permanent symptomatic neurologic injury following arteriovenous malformation (AVM) radiosurgery 36
37 Stereotactic RadioSurgery Phase I Radiation Therapy Oncology Group (RTOG) dose-escalation data for radiosurgery of recurrent brain metastases and glioblastoma fit to logistic dose response curves. The numbers at each data point indicate the number of patients in each dose/diameter group 37
38 Stereotactic RadioSurgery for Arteriovenous Malformation AVM Untreated intracranial AVMs have a bleeding risk of approximately 3% per year, or higher if prior bleeds have occurred. This results in an average of 1% of untreated AVM patients dying each year from hemorrhage. Management options include observation, surgical resection, embolization, and radiosurgery. Radiosurgery can dramatically reduce the risk of hemorrhage. Radiosurgery obliterates the AVM nidus in approximately 75% of patients within 3 years of the procedure. Individual obliteration rates vary from 50% to 88% Although AVM obliteration rates appear to be optimized with marginal doses of approximately 23 Gy, lower doses are selected for most patients to minimize complications. The risk of neurologic sequelae from radiosurgery averages approximately 3% but varies with treatment volume, dose, and location. The risk of hemorrhage while waiting for complete obliteration to develop seems unaltered 38
39 Fractionated Stereotactic RadioSurgery for Arteriovenous Malformation AVM SRS is the radiation modality of choice for the treatment of AVMs. SRS is indicated mostly for lesions in deep or eloquent regions of the brain and is particularly safe and successful for lesions that are <3 cm. Unlike surgery, the time to obliteration ranges from 1 to 4 years after SRS, so the patient remains at a continued bleeding risk. Even with time, Maruyama et al demonstrated that the bleeding risk is not completely eliminated but reduced by approximately 88%. Based on the Flickinger et al dose response data, typical prescriptions for treatment of AVM are 21 to 22 Gy prescribed to the 50% IDL for frame-based radiosurgery. The prescription should be lowered for AVMs near the brainstem or larger lesions (>3 cm). For linac-based SRS, prescriptions generally range from 16 to 24 Gy in a single fraction to 20 to 22 Gy in 2 fractions for spinal AVMs 39
40 Stereotactic RadioSurgery for Arteriovenous Malformation AVM When an AVM nidus fails to completely obliterate by 3 years after radiosurgery, irradiation can be repeated with acceptable morbidity. Although some residual radiation injury effect would be expected within the previously irradiated, unobliterated AVM nidus vasculature, retreatment appears to require similar, if not higher, doses to achieve similar rates of complete obliteration as initial radiosurgery. 40
41 Stereotactic RadioSurgery for Large Arteriovenous Malformation AVM Management of large AVMs is presently difficult because radiosurgery may be associated with high complication risks and low obliteration rates. Recent improvements in embolization with liquid glue (ev3, Inc.) or polymer can sometimes help reduce the target volume but adds to the total risks of the overall management. Another promising approach is staged radiosurgery, in which large AVMs are treated in two or three sections separated by 4- to 6-month intervals to reduce acute toxicity. Whether there is any benefit to fractionating stereotactic irradiation of AVMs is presently unclear 41
42 Stereotactic RadioSurgery for Cavernous Arteriovenous Malformation AVM Cavernous malformations do not show detectable flow on angiography but nevertheless are vascular lesions with annual hemorrhage risks of 0.5% per year with no prior bleed, 4.5% with one prior hemorrhage, and approximately 32% per year after a history of two or more hemorrhages. Lower pressures in these lesions lead to smaller bleeds than are typically seen with AVM. Repeated bleeds from brainstem cavernous malformations can cause considerable neurologic morbidity. Symptomatic, surgically accessible lesions should be resected. Radiosurgery of brainstem cavernous malformations with a history of two or more prior hemorrhages appears to reduce the risk of subsequent bleeds to approximately 1% per year with acceptable morbidity 42
43 Fractionated Stereotactic RadioSurgery for Arteriovenous Malformation AVM FLICKINGER S PREDICTED RATES OF IN-FIELD ARTERIOVENOUS MALFORMATIONS OBLITERATION BASED ON THE MINIMUM DOSE WITHIN THE TARGET VOLUME 43
44 Vestibular Schwannoma and Neurofibroma Vestibular schwannomas, also known as acoustic neuromas, are benign tumors arising from Schwann cells. Acoustic neuromas (AN) represent 5% to 8% of primary CNS brain tumors. They are associated with loss of genetic information on chromosome 22. Vestibular schwannomas either occur on one side as spontaneous mutations or bilaterally as the hallmark of type 2 neurofibromatosis (NF-2). Vestibular schwannomas usually arise within the internal auditory canal and later extend intracranially into the cerebellar pontine angle. Symptoms include sensorineural hearing loss, tinnitus, and vertigo. The differential diagnosis of a cerebellar pontine angle tumor includes vestibular schwannoma (90%), meningioma (close to 10%), cholesteatomas, facial or trigeminal schwannoma, and rare primary or metastatic malignant tumors. 44
45 Vestibular Schwannoma and Neurofibroma Evidence-Based Treatment Summary 1. Small nonprogressive tumors can be observed. 2. Surgical resection is generally considered the standard of care for symptomatic lesions. 3. Radiosurgery produces outcomes equivalent to surgery, although these modalities have not been prospectively compared. 4. Fractionated stereotactic radiotherapy is being increasingly employed, with institutional reports suggesting a lower incidence of cranial neuropathies than radiosurgery, but this has not been prospectively validated. 5. The role of bevacizumab in NF-2-associated progressive bilateral vestibular schwannomas is being explored. 45
46 Stereotactic RadioSurgery for Vestibular Schwannoma The University of Pittsburgh 313 acoustic schwannoma patients who underwent gamma knife radiosurgery SRS Dose of 12 to 13 Gy Tumor control rate, free of surgical intervention, was 98.6% at 7 years. 46
47 Stereotactic Radiation Therapy for Vestibular Schwannoma Various fractionation schemes FSR 18 Gy/3, 20 Gy/4 to 5, 25 Gy/5 SRT 45 to 50 Gy/25, and 54 Gy/30 have been used with vestibular schwannoma with minor differences in results As compared to SRT better hearing preservation ( upto 98% actuarial hearing preservation) similar facial and trigeminal neuropathy rates for the radiosurgery and fractionated radiotherapy groups Perez
48 Chordoma Chordomas are rare, slowly growing midline tumors originating from the embryonal notochord rests in the skull base (35%), vertebral column (15%), or sacral regions (50%). The most common sites of skull-based tumors include the clivus, dorsum sella, and nasopharynx Complete surgical resection is the mainstay of treatment. However, due to location, GTR is often not possible. Relapse rates are as high as 50% even after surgical resection with negative margins 48
49 Chordoma Adjuvant radiation therapy is indicated to reduce recurrence rates for skull-based chordomas. Retrospective data suggest that salvage RT is inferior to adjuvant RT RT techniques for treatment of skull-based chordomas include conventionally fractionated 3D-CRT or IMRT, fractionated charged particle therapy (protons, carbon ions), and FSRT. Determination of the GTV should be made by coregistration of the preoperative and/or postoperative MRI to the treatment planning CT scan. Margins for CTV should be 1 to 2 cm with an additional 3 to 5 mm for the PTV. Dose prescriptions to the PTV for patients receiving photonbased treatment should be at least 60 Gy given in 1.8- to 2.0-Gy daily fractions 49
50 Glomus Jugulare Tumors RT is indicated for patients with tumors in unsuitable locations (i.e., skull base), as adjuvant therapy after STR, or as salvage therapy at the time of relapse after surgery. RT techniques include conventionally fractionated 3D-CRT or IMRT, SRS, and FSRT. The diagnostic MRI should be coregistered with the treatment planning CT scan. The GTV is delineated and 1 to 1.5 cm is added for clinical and setup margin. With conventional techniques, doses are often 45 to 55 Gy given in 1.8- to 2.0-Gy daily fractions with local control rates near or >90% in several series. Results with SRS have been comparable to that of conventionally fractionated RT. Using a frame-based platform, reported tumor margin doses range from 12.5 to 20 Gy prescribed to the 50% IDL Tumor control more than 90% 50
51 Hemangioblastoma Hemangioblastomas are benign vascular tumors that present during the third and fourth decades of life. They account for 1% to 2% of primary CNS tumors in adults. Most arise in the cerebellum, constituting the most common primary cerebellar tumors in adults. An association with von Hippel-Lindau disease is noted in 10% of patients. Histologically, the tumor consists of closely packed, thin-walled blood vessels in a stroma of large, oval foamy cells. The lesions are intensely enhancing on CT and MRI, and angiography confirms the vascular nature of the lesion. Imaging of the craniospinal axis often documents multiple lesions in patients with von Hippel-Lindau disease. Treatment is surgical, and complete resection is curative. Radiosurgery has also been shown to be useful in patients with unresectable disease but is associated with higher rates of recurrence 51
52 Hemangiopericytoma Hemangiopericytoma is a sarcomatous lesion developing from smooth muscle in blood vessels usually along the base of the skull, although intraparenchymal lesions may be seen. In contrast to other primary CNS tumors, hemangiopericytomas commonly develop systemic metastases. There is a 90% 9-year actuarial risk for local failure following surgical resection only. Postoperative radiotherapy to total doses of 50 to 60 Gy reduces the risk of recurrence rate and improves overall survival. Tumor control is dose dependent, with doses >50 Gy associated with superior outcomes. Radiographic response is slow. Radiosurgery has been used for recurrent hemangiopericytomas, with reported local control rates of approximately 80% following treatment. 52
53 Hemangioblastoma and Hemangiopericytoma Evidence-Based Treatment Summary 1. Surgical resection is recommended, when feasible, for both of these diseases. 2. Radiotherapy is generally reserved for subtotally resected progressive hemangioblastoma, but there are no prospective data. 3. Postoperative radiotherapy is recommended for subtotally resected hemangiopericytoma, but there are no prospective data. 4. Radiotherapy or radiosurgery may be considered for unresectable tumors. 53
54 NEURONAL AND MIXED NEURONAL-GLIAL TUMORS These are uncommon tumors that are characterized by the presence of both neuronal and glial elements in variable amounts. They include entities such as desmoplastic infantile astrocytoma and dysembryoplastic neuroepithelial tumor. Most will be cured by surgery, but radiotherapy may be indicated in two tumor types: Ganglioglioma and anaplastic ganglioglioma Central neurocytoma 54
55 Ganglioglioma and Anaplastic Ganglioglioma Gangliogliomas are well-differentiated slowly growing tumors composed of mature ganglion cells in combination with neoplastic glial cells (WHO grade I or II). Tumors in which the glial component shows anaplastic features (WHO grade III) are called anaplastic gangliogliomas. Although these tumors can arise anywhere within the CNS, most in children arise in the temporal region and typically present with seizures. Surgery is the treatment of choice. When resection is complete, the probability of longterm tumor control in patients with ganglioglioma is excellent. The indications for radiotherapy are as for patients with LGAs, that is, for patients with progressive or recurrent disease that is not resectable, and the radiotherapy target volume and dose likewise. The indications for postoperative radiotherapy remain undefined except for patients with anaplastic gangliogliomas who have undergone less than complete resection in whom the use of radiotherapy has been shown to result in improved progression-free survival. 55
56 Central Neurocytoma This is a neoplasm composed of uniform round cells with neuronal differentiation that arises in the lateral or third ventricles, typically the former, that is seen predominantly in adolescents and young adults. Patients usually present with symptoms and signs of raised intracranial pressure. Surgery is the treatment of choice, and when complete resection is achieved long-term tumor control is excellent without adjuvant treatment. Patients in whom complete resection cannot be achieved as well as those with tumors with atypical histology or a high mitotic rate fare less well, and postoperative radiotherapy should be considered in these situations. While a dose of 50 Gy appears adequate for patients with typical neurocytomas, there is evidence of improved tumor control at doses of at least 54 Gy in patients with atypical neurocytoma. 56
57 Pituitary Adenoma Perez
58 Pituitary Adenoma Functional Adenoma Patients with functional adenomas present with signs and symptoms that correspond to the excess hormone: galactorrhea, amenorrhea, diminished libido, and infertility in patients with prolactinomas; acromegaly or gigantism in patients with GHsecreting adenomas; Cushing disease in adrenocorticotropic hormone (ACTH) secreting adenomas; hyperthyroidism in patients with thyroid-stimulating hormone (TSH) secreting adenomas. In patients who have had bilateral adrenalectomy, up to 40% will develop Nelson syndrome, which is characterized by an ACTHsecreting adenoma and increased skin pigmentation secondary to increased release of α-melanocyte stimulating hormone. 58 Perez 2013
59 Pituitary Adenoma workup History and detailed physical examination (H&P) Laboratory analysis of pituitary hormone levels Contrast enhanced MRI with thin slices through the pituitary Tissue diagnosis to rule out other causes of pituitary masses, including craniopharyngioma, meningioma, suprasellar germ cell tumor, metastatic disease, or a benign lesion (i.e., cyst). 59 Perez 2013
60 Pituitary Adenoma Symptomatic adenomas present for medical attention as a result of hormone secretions, compression of nearby normal structures with neurologic symptoms, or compression of the pituitary stalk causing hypopituitarism. An initial therapy for most prolactinomas is with a dopamine agonist such as bromocriptine, lysuride, or pergolide. Medical intervention usually decreases adenoma function and size. Initial therapy for other pituitary adenomas is transsphenoidal surgical resection. Surgery is generally safe and reverses neurologic symptoms, with most patients normalizing hormone levels. It is mostly useful to cure microadenomas. Radiation therapy is often reserved for patients with residual disease after surgery, such as after a debulking surgery. It is also considered for recurrence after definitive surgery or for medically inoperable patients. Typically, conventional radiation delivers a dose of 45 Gy at 1.8 Gy daily fractions. At this dose, good control can usually be achieved with a very low risk of optic neuropathy. Normalization of hormone levels, however, can take months to years to achieve. 60 Perez 2013
61 Pituitary Adenoma Management Management of pituitary adenomas requires a multidisciplinary approach to properly select which patients are suitable for different approaches with Medical therapy Surgery Fractionated radiotherapy Radiosurgery, or combinations of these. Most patients with visual compromise, particularly with a hemianopia or greater, will do better with initial surgical decompression. Prolactinomas are usually initially managed with medical therapy. 61
62 Pituitary Adenoma Management Management of pituitary adenomas requires a multidisciplinary approach to properly select which patients are suitable for different approaches with Medical therapy Surgery Fractionated radiotherapy Radiosurgery, or combinations of these. Most patients with visual compromise, particularly with a hemianopia or greater, will do better with initial surgical decompression. Prolactinomas are usually initially managed with medical therapy. 62
63 Surgery for Pituitary Adenoma Surgery is generally the treatment of choice for pituitary adenomas. Surgery provides immediate relief of compressive symptoms and helps to decrease hormone secretion. The most common surgical technique is through a transsphenoidal approach. In some cases, a more aggressive surgery (i.e., frontal craniotomy) may be indicated for patients with extensive intracranial and skull-based involvement. Overall, local control rates range from 50% to 80% after surgery alone for both functioning and nonfunctioning adenomas. In patients who continue to have abnormally elevated hormones after surgical resection, adjuvant treatment with pharmacotherapy or radiation therapy is pursued. 63
64 RT for Pituitary Adenoma Except for medically inoperable patients in which RT is used in the primary setting, the role of RT is generally in the adjuvant setting with the following indications: recurrent tumor after surgery; persistence of hormone elevation after surgery; residual disease after STR or debulking procedure. Tumor growth control is excellent, particularly for patients with nonfunctioning adenomas. Endocrine control after treatment of functioning adenomas, as demonstrated by normalization of pituitary hormone levels, takes years to develop. At a median of 2 years after RT, growth hormone levels stabilize quickest; normalization is slowest for TSH-secreting adenomas. Pharmacologic therapy should be discontinued 1 to 2 months prior to the initiation of RT based on evidence demonstrating lower RT sensitivity with concurrent medical treatment. 64
65 RT for Pituitary Adenoma A recurrent nonfunctioning pituitary adenoma 7 years after surgical resection in the axial (A) and coronal (B) planes. The yellow arrows denote invasion into the left cavernous sinus. Rapid arc intensity-modulated radiotherapy treatment plan for the same patient in the axial (C), coronal (D), and sagittal (E) planes. The planning target volume (purple shaded area) was prescribed at 50.4 Gy in fractions.
66 RT for Pituitary Adenoma RT techniques include 3D-CRT, IMRT, single-fraction SRS, and FSRT. Delineation of the GTV (or preoperative GTV in the case of GTR) should be performed by coregistration of the postoperative MRI to the treatment planning CT scan. For 3D-CRT and IMRT, the CTV is constructed by adding 1 to 1.5 cm to the GTV; an additional 3 to 5 mm is added to the CTV to create the PTV. These margins may be modified based on institutional policy and other considerations, such as the availability of daily image guidance. Nonfunctional adenomas are typically prescribed a dose of 45/25F to 50.4 Gy/28F given in 1.8Gy daily fractions. Higher doses in the range of 54 Gy /30F/6wks are recommended for secretory adenomas. 66
67 Radiosurgery and FRS for Pituitary Adenoma Small pituitary adenomas, where the target volume can be separated from the optic nerves, are reasonable candidates for radiosurgery. 67
68 Radiosurgery and FSRS for Pituitary Adenoma SRS remains an attractive option for the treatment of pituitary adenomas. General principles apply in that FSRT is used over SRS for large lesions (>3 cm) or lesions near critical structures (<1 or 2 mm from the chiasm). Similar to 3D-CRT or IMRT, higher doses are needed for functional adenomas compared with nonfunctional adenomas. Commonly used prescriptions are 16 to 20 Gy in a single fraction for nonfunctional adenomas and 20 to 25 Gy in a single fraction for functional adenomas using a frameless robotic radiosurgery Sheehan et al performed a review of 35 peer-reviewed reports of radiosurgery for pituitary adenoma that included 1,621 patients. Most studies reported >90% control of tumor size (range, 68% to 100%). The weighted average tumor control rate for all published series (encompassing 1,283 patients) was 96%. In eight published series with mean or median patient follow-up periods of 4 years, tumor growth control rates varied from 83% to 100%. Perez
69 Radiosurgery and SRS for Pituitary Adenoma Cushing s disease Twenty-two series have published radiosurgery results for 314 Cushing s disease patients. The mean radiosurgical prescription (margin) doses for these series varied from 15 to 32 Gy. In those series with at least 10 patients and a median follow-up of 2 years, endocrinologic remission rates range from 17% to 83%. Many of the patients in older series were treated in the pre-ct and MR imaging era of radiosurgery, sometimes as many as four times before their Cushing s disease went into remission. 69
70 Gamma knife Planning for Pituitary Adenoma 70
71 Cyberknife Planning for Pituitary Adenoma 71
72 Proton Therapy planning for Pituitary Adenoma 72
73 Stereotactic RadioSurgery for Benign Intracranial Tummors Most small benign intracranial tumors are well managed with radiosurgery, FSR, or SRT. Radiosurgery control rates are high with radiosurgery, with prescription doses on the order of 12 to 14 Gy Kondziolka et al. evaluated long-term tumor control in 285 patients who underwent radiosurgery for benign intracranial tumors with a median follow-up period of 10 years. These included 157 patients with vestibular schwannomas, 10 with other cranial nerve schwannomas, 85 with meningiomas, 28 with pituitary adenomas 5 with craniopharyngiomas. Forty-four percent of the patients had prior surgical resection and 5% had prior fractionated radiotherapy. They found that 95% of the 285 patients had imaging-defined local tumor control (63% had tumor regression and 32% had no further tumor growth). The crude tumor control was 95% with a 15-year actuarial tumor control rate of 93.7%. In 5% of the patients, delayed tumor growth was identified. Resection was performed after radiosurgery in 13 patients (5%) for tumor growth. 73
Otolaryngologist s Perspective of Stereotactic Radiosurgery
 Otolaryngologist s Perspective of Stereotactic Radiosurgery Douglas E. Mattox, M.D. 25 th Alexandria International Combined ORL Conference April 18-20, 2007 Acoustic Neuroma Benign tumor of the schwann
Otolaryngologist s Perspective of Stereotactic Radiosurgery Douglas E. Mattox, M.D. 25 th Alexandria International Combined ORL Conference April 18-20, 2007 Acoustic Neuroma Benign tumor of the schwann
Chapter 5 Section 3.1
 Radiology Chapter 5 Section 3.1 Issue Date: March 27, 1991 Authority: 32 CFR 199.4(b)(2), (b)(2)(x), (c)(2)(viii), and (g)(15) 1.0 CPT 1 PROCEDURE CODES 37243, 61793, 61795, 77261-77421, 77427-77799, 0073T
Radiology Chapter 5 Section 3.1 Issue Date: March 27, 1991 Authority: 32 CFR 199.4(b)(2), (b)(2)(x), (c)(2)(viii), and (g)(15) 1.0 CPT 1 PROCEDURE CODES 37243, 61793, 61795, 77261-77421, 77427-77799, 0073T
Dosimetry, see MAGIC; Polymer gel dosimetry. Fiducial tracking, see CyberKnife radiosurgery
 Subject Index Acoustic neuroma, neurofibromatosis type 2 complications 103, 105 hearing outcomes 103, 105 outcome measures 101 patient selection 105 study design 101 tumor control 101 105 treatment options
Subject Index Acoustic neuroma, neurofibromatosis type 2 complications 103, 105 hearing outcomes 103, 105 outcome measures 101 patient selection 105 study design 101 tumor control 101 105 treatment options
Meningioma tumor. Meningiomas are named according to their location (Fig. 1) and cause various symptoms: > 1
 Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Original Date: April 2016 Page 1 of 7 FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
Paraganglioma of the Skull Base. Ross Zeitlin, MD Medical College of Wisconsin Milwaukee, WI
 Paraganglioma of the Skull Base Ross Zeitlin, MD Medical College of Wisconsin Milwaukee, WI Case Presentation 63-year-old female presents with right-sided progressive conductive hearing loss for several
Paraganglioma of the Skull Base Ross Zeitlin, MD Medical College of Wisconsin Milwaukee, WI Case Presentation 63-year-old female presents with right-sided progressive conductive hearing loss for several
STEREOTACTIC RADIATION THERAPY. Monique Blanchard ANUM Radiation Oncology Epworth HealthCare
 STEREOTACTIC RADIATION THERAPY Monique Blanchard ANUM Radiation Oncology Epworth HealthCare Overview Stereotactic radiation therapy at Epworth Healthcare What is stereotactic radiation therapy? Delivery
STEREOTACTIC RADIATION THERAPY Monique Blanchard ANUM Radiation Oncology Epworth HealthCare Overview Stereotactic radiation therapy at Epworth Healthcare What is stereotactic radiation therapy? Delivery
Background Principles and Technical Development
 Contents Part I Background Principles and Technical Development 1 Introduction and the Nature of Radiosurgery... 3 Definitions of Radiosurgery... 5 Consequences of Changing Definitions of Radiosurgery...
Contents Part I Background Principles and Technical Development 1 Introduction and the Nature of Radiosurgery... 3 Definitions of Radiosurgery... 5 Consequences of Changing Definitions of Radiosurgery...
Brain tumors: tumor types
 Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
NON MALIGNANT BRAIN TUMOURS Facilitator. Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol
 NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS
 ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS Dr. Maitri P Gandhi 1, Dr. Chandni P Shah 2 1 Junior resident, Gujarat Cancer & Research
ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS Dr. Maitri P Gandhi 1, Dr. Chandni P Shah 2 1 Junior resident, Gujarat Cancer & Research
Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary
 Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary László Bognár M.D., Ph.D., József G. Dobai M.D., Gábor Csiky and Imre Fedorcsák M.D., Ph.D. Department of Neurosurgery, Medical
Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary László Bognár M.D., Ph.D., József G. Dobai M.D., Gábor Csiky and Imre Fedorcsák M.D., Ph.D. Department of Neurosurgery, Medical
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Stereotactic Radiosurgery/Fractionated Stereotactic Radiotherapy for Acoustic Neuroma (Vestibular Schwannomas)
 Strategic Commissioning Group West Midlands Commissioning Policy (WM/38) Stereotactic Radiosurgery/Fractionated Stereotactic Radiotherapy for Acoustic Neuroma (Vestibular Schwannomas) Version 1 July 2010
Strategic Commissioning Group West Midlands Commissioning Policy (WM/38) Stereotactic Radiosurgery/Fractionated Stereotactic Radiotherapy for Acoustic Neuroma (Vestibular Schwannomas) Version 1 July 2010
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2015
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2015
NANOS Patient Brochure
 NANOS Patient Brochure Pituitary Tumor Copyright 2015. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for informational
NANOS Patient Brochure Pituitary Tumor Copyright 2015. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for informational
Imaging The Turkish Saddle. Russell Goodman, HMS III Dr. Gillian Lieberman
 Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Overview of radiosurgery for benign brain tumors
 Overview of radiosurgery for benign brain tumors Anuj V. Peddada, M.D. Department of Radiation Oncology Penrose Cancer Center Colorado Springs, CO Objectives Provide overview of benign brain tumors meningiomas
Overview of radiosurgery for benign brain tumors Anuj V. Peddada, M.D. Department of Radiation Oncology Penrose Cancer Center Colorado Springs, CO Objectives Provide overview of benign brain tumors meningiomas
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2017
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2017
Stereotactic Radiosurgery. Extracranial Stereotactic Radiosurgery. Linear accelerators. Basic technique. Indications of SRS
 Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/20/2015
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/20/2015
TABLES. Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging. Conclusions. Author (Year) Classification Process/Evid ence Class
 TABLES Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging Author Clark (1986) 9 Reformatted sagittal images in the differential diagnosis meningiomas and adenomas with suprasellar
TABLES Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging Author Clark (1986) 9 Reformatted sagittal images in the differential diagnosis meningiomas and adenomas with suprasellar
This LCD recognizes these two distinct treatment approaches and is specific to treatment delivery:
 National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: 77371, 77372, 77373 LCD ID Number: L33410 J-N FL Responsible
National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: 77371, 77372, 77373 LCD ID Number: L33410 J-N FL Responsible
NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) BONE (Version , 03/28/18)
 BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
Year 2003 Paper two: Questions supplied by Tricia
 question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 03/01/2013 Section:
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 03/01/2013 Section:
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Specialised Services Policy: CP22. Stereotactic Radiosurgery
 Specialised Services Policy: CP22 Document Author: Assistant Director of Planning Executive Lead: Director of Planning ad Performance Approved by: Management Group Issue Date: 01 July 2015 Review Date:
Specialised Services Policy: CP22 Document Author: Assistant Director of Planning Executive Lead: Director of Planning ad Performance Approved by: Management Group Issue Date: 01 July 2015 Review Date:
Skullbase Lesions. Skullbase Surgery Open vs endoscopic. Choice Of Surgical Approaches 12/28/2015. Skullbase Surgery: Evolution
 Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Imaging pituitary gland tumors
 November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
Patients Treated with Leksell Gamma Knife
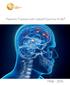 Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined Approach
 Radiosurgery as part of the neurosurgical armamentarium: Educational Symposium November 24 th 2011 Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined
Radiosurgery as part of the neurosurgical armamentarium: Educational Symposium November 24 th 2011 Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined
IMAGE-GUIDED RADIOSURGERY USING THE GAMMA KNIFE
 IMAGE-GUIDED RADIOSURGERY USING THE GAMMA KNIFE L. D. LUNSFORD INTRODUCTION Image guided brain surgery became a reality in the mid-1970s after the introduction of the first methods to obtain axial imaging
IMAGE-GUIDED RADIOSURGERY USING THE GAMMA KNIFE L. D. LUNSFORD INTRODUCTION Image guided brain surgery became a reality in the mid-1970s after the introduction of the first methods to obtain axial imaging
Update on IGKRF Activities
 Stereotactic radiosurgery research, education and publishing for the purpose of improving public health Fall 2016 In this issue: Update on IGKRF Activities The IGKRF Recently Published Articles Topics
Stereotactic radiosurgery research, education and publishing for the purpose of improving public health Fall 2016 In this issue: Update on IGKRF Activities The IGKRF Recently Published Articles Topics
Brain Tumors. What is a brain tumor?
 Scan for mobile link. Brain Tumors A brain tumor is a collection of abnormal cells that grows in or around the brain. It poses a risk to the healthy brain by either invading or destroying normal brain
Scan for mobile link. Brain Tumors A brain tumor is a collection of abnormal cells that grows in or around the brain. It poses a risk to the healthy brain by either invading or destroying normal brain
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Leksell Gamma Knife Icon. Treatment information
 Leksell Gamma Knife Icon Treatment information You may be feeling frightened or overwhelmed by your recent diagnosis. It can be confusing trying to process a diagnosis, understand a new and challenging
Leksell Gamma Knife Icon Treatment information You may be feeling frightened or overwhelmed by your recent diagnosis. It can be confusing trying to process a diagnosis, understand a new and challenging
Sacral Chordoma: The Loma Linda University Radiation Medicine Experience. Kevin Yiee MD, MPH Resident Physician
 Sacral Chordoma: The Loma Linda University Radiation Medicine Experience Kevin Yiee MD, MPH Resident Physician What is a chordoma? 1 st chordoma discovered in clivus by Virchow and Luschka 1856 Rare tumor
Sacral Chordoma: The Loma Linda University Radiation Medicine Experience Kevin Yiee MD, MPH Resident Physician What is a chordoma? 1 st chordoma discovered in clivus by Virchow and Luschka 1856 Rare tumor
Staged-Volume Radiosurgery of Large AVMs
 Case Study Staged-Volume Radiosurgery of Large AVMs Using Gamma Knife Technology Institution New York University Langone Medical Center Location New York City, NY Patient 18 patients Diagnosis Each patient
Case Study Staged-Volume Radiosurgery of Large AVMs Using Gamma Knife Technology Institution New York University Langone Medical Center Location New York City, NY Patient 18 patients Diagnosis Each patient
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
TABLES. Table 1: Imaging. Congress of Neurological Surgeons Author (Year) Description of Study Classification Process / Evidence Class
 TABLES Table 1: Imaging Kremer et al (2002) 2 Study Design: Prospective followed case series. Patient Population: Fifty adult patients with NFPA Study Description: Patients underwent MRI before surgery,
TABLES Table 1: Imaging Kremer et al (2002) 2 Study Design: Prospective followed case series. Patient Population: Fifty adult patients with NFPA Study Description: Patients underwent MRI before surgery,
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis
 Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
Fractionated Stereotactic Radiotherapy. Rationale, indications, & treatment techniques
 Fractionated Stereotactic Radiotherapy Rationale, indications, & treatment techniques Radiobiological principles The BED (Gy) = D(1 + d/α/β) Assume BED 1 = BED 2 for tissue of an unknown α/β: Optic
Fractionated Stereotactic Radiotherapy Rationale, indications, & treatment techniques Radiobiological principles The BED (Gy) = D(1 + d/α/β) Assume BED 1 = BED 2 for tissue of an unknown α/β: Optic
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Radioterapia degli adenomi ipofisari
 Radioterapia degli adenomi ipofisari G Minniti Radiation Oncology, Sant Andrea Hospital, University of Rome Sapienza, and IRCCS Neuromed, Pozzilli (IS) Roma 6-9 Novembre 14 ! Outline " Radiation techniques
Radioterapia degli adenomi ipofisari G Minniti Radiation Oncology, Sant Andrea Hospital, University of Rome Sapienza, and IRCCS Neuromed, Pozzilli (IS) Roma 6-9 Novembre 14 ! Outline " Radiation techniques
PITUITARY PARASELLAR LESIONS. Kim Learned, MD
 PITUITARY PARASELLAR LESIONS Kim Learned, MD DIFFERENTIALS Pituitary Sella Clivus, Sphenoid Sinus Suprasellar Optic chiasm, Hypothalamus, Circle of Willis Parasellar Cavernous Sinus Case 1 17 YEAR-OLD
PITUITARY PARASELLAR LESIONS Kim Learned, MD DIFFERENTIALS Pituitary Sella Clivus, Sphenoid Sinus Suprasellar Optic chiasm, Hypothalamus, Circle of Willis Parasellar Cavernous Sinus Case 1 17 YEAR-OLD
Stereotactic Radiosurgery
 27 th ICRO-AROI 2017 Stereotactic Radiosurgery Dr Sajal Kakkar MD, FUICC (USA), FAROI (Fr) Consultant Radiation Oncologist Max Super Speciality Hospital, Mohali SRS Introduction Stereotactic techniques
27 th ICRO-AROI 2017 Stereotactic Radiosurgery Dr Sajal Kakkar MD, FUICC (USA), FAROI (Fr) Consultant Radiation Oncologist Max Super Speciality Hospital, Mohali SRS Introduction Stereotactic techniques
Adult Brain and Spinal Cord Tumors
 Adult Brain and Spinal Cord Tumors An adult central nervous system (CNS) tumor is a disease in which abnormal cells form in the tissues of the brain and or the spinal cord. Major Parts of the Brain Anatomy
Adult Brain and Spinal Cord Tumors An adult central nervous system (CNS) tumor is a disease in which abnormal cells form in the tissues of the brain and or the spinal cord. Major Parts of the Brain Anatomy
Collection of Recorded Radiotherapy Seminars
 IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org The Role of Radiosurgery in the Treatment of Gliomas Luis Souhami, MD Professor Department of Radiation
IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org The Role of Radiosurgery in the Treatment of Gliomas Luis Souhami, MD Professor Department of Radiation
Extracranial doses in stereotactic and conventional radiotherapy for pituitary adenomas
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 7, NUMBER 2, SPRING 2006 Extracranial doses in stereotactic and conventional radiotherapy for pituitary adenomas Thomas Samuel Ram, a Paul B. Ravindran,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 7, NUMBER 2, SPRING 2006 Extracranial doses in stereotactic and conventional radiotherapy for pituitary adenomas Thomas Samuel Ram, a Paul B. Ravindran,
Update on Pediatric Brain Tumors
 Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Radiosurgery. Most Important! 8/2/2012. Stereotactic Radiosurgery: State of the Art Technology and Implementation Linear Accelerator Radiosurgery
 Therapy SAM Symposium: WE-A-BRCD-1 Stereotactic Radiosurgery: State of the Art Technology and Implementation Linear Accelerator Radiosurgery Kamil M. Yenice, PhD Associate Professor Chief of Clinical Physics
Therapy SAM Symposium: WE-A-BRCD-1 Stereotactic Radiosurgery: State of the Art Technology and Implementation Linear Accelerator Radiosurgery Kamil M. Yenice, PhD Associate Professor Chief of Clinical Physics
Brain Tumor Treatment
 Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Brain and Spine Tumors
 Brain and Spine Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases
Brain and Spine Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: 6.01.10 Last Review: 11/2013 Origination: 1/1989 Next Review: 11/2014 Policy Blue Cross and Blue Shield of Kansas City (Blue
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: 6.01.10 Last Review: 11/2013 Origination: 1/1989 Next Review: 11/2014 Policy Blue Cross and Blue Shield of Kansas City (Blue
Alessandra Gorgulho, MD, MSc
 Manejo do Meningioma que compromete o seio cavernoso: quando eu irradio Alessandra Gorgulho, MD, MSc Chefe Clínico-Científica Centro HCor de Neurociências Professora Visitante, Departamento de Neurocirurgia,
Manejo do Meningioma que compromete o seio cavernoso: quando eu irradio Alessandra Gorgulho, MD, MSc Chefe Clínico-Científica Centro HCor de Neurociências Professora Visitante, Departamento de Neurocirurgia,
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR EPENDYMOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR EPENDYMOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR EPENDYMOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
Current Concepts and Trends in Spinal Radiosurgery. Edward M. Marchan
 Current Concepts and Trends in Spinal Radiosurgery Edward M. Marchan Spinal Neoplasia The spine is the most common site of skeletal metastatic disease. (70%) 40% of bony metastases involve the vertebrae
Current Concepts and Trends in Spinal Radiosurgery Edward M. Marchan Spinal Neoplasia The spine is the most common site of skeletal metastatic disease. (70%) 40% of bony metastases involve the vertebrae
Stereotactic Radiosurgery and Proton Beam Therapy
 Last Review Date: January 12, 2018 Number: MG.MM.RA.13i Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: January 12, 2018 Number: MG.MM.RA.13i Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
AMERICAN BRAIN TUMOR ASSOCIATION. Proton Therapy
 AMERICAN BRAIN TUMOR ASSOCIATION Proton Therapy ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit
AMERICAN BRAIN TUMOR ASSOCIATION Proton Therapy ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Proton Stereotactic Radiotherapy: Clinical Overview. Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS
 Proton Stereotactic Radiotherapy: Clinical Overview Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS Acknowledgements Radiation Oncologists and Physicists at various institutions (MGH, MDACC,
Proton Stereotactic Radiotherapy: Clinical Overview Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS Acknowledgements Radiation Oncologists and Physicists at various institutions (MGH, MDACC,
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT
 SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR
 Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR PhD, FAAPM, FACR, FASTRO Department of Radiation Oncology Indiana University School of Medicine Indianapolis, IN, USA Indra J. Das,
Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR PhD, FAAPM, FACR, FASTRO Department of Radiation Oncology Indiana University School of Medicine Indianapolis, IN, USA Indra J. Das,
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM EPENDYMOMA Last Revision Date July 2015 1 CNS Site Group Ependymoma Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM EPENDYMOMA Last Revision Date July 2015 1 CNS Site Group Ependymoma Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2.
Clinical Commissioning Policy: Arteriovenous Malformations. December Reference : NHSCB/D5/4
 Clinical Commissioning Policy: Arteriovenous Malformations December 2012 Reference : NHSCB/D5/4 NHS Commissioning Board Clinical Commissioning Policy: Arteriovenous Malformations First published: December
Clinical Commissioning Policy: Arteriovenous Malformations December 2012 Reference : NHSCB/D5/4 NHS Commissioning Board Clinical Commissioning Policy: Arteriovenous Malformations First published: December
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: charged_particle_radiotherapy 3/12/96 5/2017 5/2018 5/2017 Description of Procedure or Service Charged-particle
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: charged_particle_radiotherapy 3/12/96 5/2017 5/2018 5/2017 Description of Procedure or Service Charged-particle
Brain Tumors. Andrew J. Fabiano, MD FAANS. Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine
 Brain Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases Brain
Brain Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases Brain
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
Refresher Course EAR TUMOR. Sasikarn Chamchod, MD Chulabhorn Hospital
 Refresher Course EAR TUMOR Sasikarn Chamchod, MD Chulabhorn Hospital Reference: Perez and Brady s Principles and Practice of radiation oncology sixth edition Outlines Anatomy Epidemiology Clinical presentations
Refresher Course EAR TUMOR Sasikarn Chamchod, MD Chulabhorn Hospital Reference: Perez and Brady s Principles and Practice of radiation oncology sixth edition Outlines Anatomy Epidemiology Clinical presentations
Case Studies in Sella/Parasellar Region. Child thirsty, increased urination. Imaging. Suprasellar Germ Cell Tumor (Germinoma) No Disclosures
 Case Studies in Sella/Parasellar Region No Disclosures 2018 Head and Neck Imaging Conference Child thirsty, increased urination Suprasellar Germ Cell Tumor (Germinoma) Midline Pineal >> Suprasellar > Other
Case Studies in Sella/Parasellar Region No Disclosures 2018 Head and Neck Imaging Conference Child thirsty, increased urination Suprasellar Germ Cell Tumor (Germinoma) Midline Pineal >> Suprasellar > Other
Adult Central Nervous System Tumors Treatment (PDQ )
 1 di 20 28/06/2016 11.18 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
1 di 20 28/06/2016 11.18 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
Neuro-oncology Update Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013
 Neuro-oncology Update 2013 Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013 Case 1 58 year old man with recent facial droop and HA s Thin, cachectic
Neuro-oncology Update 2013 Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013 Case 1 58 year old man with recent facial droop and HA s Thin, cachectic
Evaluation of Three-dimensional Conformal Radiotherapy and Intensity Modulated Radiotherapy Techniques in High-Grade Gliomas
 1 Carol Boyd Comprehensive Case Study July 11, 2013 Evaluation of Three-dimensional Conformal Radiotherapy and Intensity Modulated Radiotherapy Techniques in High-Grade Gliomas Abstract: Introduction:
1 Carol Boyd Comprehensive Case Study July 11, 2013 Evaluation of Three-dimensional Conformal Radiotherapy and Intensity Modulated Radiotherapy Techniques in High-Grade Gliomas Abstract: Introduction:
Imaging for suspected glioma
 Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
SCIENTIFIC PROGRAMME SNOLA UPDATE ON NEURO- ONCOLOGY th March
 SCIENTIFIC PROGRAMME SNOLA UPDATE ON NEURO- ONCOLOGY 2016 24th March 13h 13h45 pathology case case parasellar meningeoma case : posterior fossa pediatric tumor 13h45 16h Imaging for CNS lymphomas Parasellar
SCIENTIFIC PROGRAMME SNOLA UPDATE ON NEURO- ONCOLOGY 2016 24th March 13h 13h45 pathology case case parasellar meningeoma case : posterior fossa pediatric tumor 13h45 16h Imaging for CNS lymphomas Parasellar
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 04/01/2014 Section:
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 04/01/2014 Section:
Stereotactic Radiosurgery and Stereotactic Body Radiotherapy
 Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Policy Number: 6.01.10 Last Review: 11/2018 Origination: 1/1989 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Policy Number: 6.01.10 Last Review: 11/2018 Origination: 1/1989 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Intensity modulated radiotherapy (IMRT) for treatment of post-operative high grade glioma in the right parietal region of brain
 1 Carol Boyd March Case Study March 11, 2013 Intensity modulated radiotherapy (IMRT) for treatment of post-operative high grade glioma in the right parietal region of brain History of Present Illness:
1 Carol Boyd March Case Study March 11, 2013 Intensity modulated radiotherapy (IMRT) for treatment of post-operative high grade glioma in the right parietal region of brain History of Present Illness:
Childhood Craniopharyngioma Treatment (PDQ )
 1 di 12 27/06/2016 09.45 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
1 di 12 27/06/2016 09.45 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
Radiosurgery by Leksell gamma knife. Josef Novotny, Na Homolce Hospital, Prague
 Radiosurgery by Leksell gamma knife Josef Novotny, Na Homolce Hospital, Prague Radiosurgery - Definition Professor Lars Leksell The tools used by the surgeon must be adapted to the task and where the human
Radiosurgery by Leksell gamma knife Josef Novotny, Na Homolce Hospital, Prague Radiosurgery - Definition Professor Lars Leksell The tools used by the surgeon must be adapted to the task and where the human
Description. Section: Therapy Effective Date: January 15, 2015 Subsection: Therapy Original Policy Date: September 13, 2012 Subject:
 Last Review Status/Date: December 2014 Page: 1 of 51 Description Stereotactic radiosurgery (SRS) and stereotactic body radiotherapy (SBRT) are radiotherapy methods that entail delivering highly focused,
Last Review Status/Date: December 2014 Page: 1 of 51 Description Stereotactic radiosurgery (SRS) and stereotactic body radiotherapy (SBRT) are radiotherapy methods that entail delivering highly focused,
(3) Pituitary tumours
 Hypopituitarism Diabetes Insipidus Pituitary tumours (2) Dr T Kemp - Endocrinology and Metabolism Unit - Steve Biko Academic Hospital (3) Pituitary tumours Pituitary microadenoma - intrasellar adenoma
Hypopituitarism Diabetes Insipidus Pituitary tumours (2) Dr T Kemp - Endocrinology and Metabolism Unit - Steve Biko Academic Hospital (3) Pituitary tumours Pituitary microadenoma - intrasellar adenoma
Dr Eddie Mee. Neurosurgeon Auckland City Hospital, Ascot Integrated Hospital, MercyAscot Hospitals, Auckland
 Dr Eddie Mee Neurosurgeon Auckland City Hospital, Ascot Integrated Hospital, MercyAscot Hospitals, Auckland 16:30-17:25 WS #48: Current Management of Brain Bleeds and Tumours 17:35-18:30 WS #58: Current
Dr Eddie Mee Neurosurgeon Auckland City Hospital, Ascot Integrated Hospital, MercyAscot Hospitals, Auckland 16:30-17:25 WS #48: Current Management of Brain Bleeds and Tumours 17:35-18:30 WS #58: Current
AbstractID: 8073 Title: Quality Assurance, Planning and Clinical Results for Gamma Knife Radiosurgery S. Goetsch, Ph.D. Page 1 Seattle, WA May 2008
 Knife Radiosurgery S. Goetsch, Ph.D. Page 1 Quality Assurance, Planning and Clinical Results for Gamma Knife Radiosurgery Steven J. Goetsch, Ph.D., FAAPM ACMP 25 th Annual Meeting Seattle, WA May 2008
Knife Radiosurgery S. Goetsch, Ph.D. Page 1 Quality Assurance, Planning and Clinical Results for Gamma Knife Radiosurgery Steven J. Goetsch, Ph.D., FAAPM ACMP 25 th Annual Meeting Seattle, WA May 2008
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Stereotactic Diffusion Tensor Tractography For Gamma Knife Stereotactic Radiosurgery
 Disclosures The authors of this study declare that they have no commercial or other interests in the presentation of this study. This study does not contain any use of offlabel devices or treatments. Stereotactic
Disclosures The authors of this study declare that they have no commercial or other interests in the presentation of this study. This study does not contain any use of offlabel devices or treatments. Stereotactic
Neuroimaging Core Curriculum
 Neuroimaging Core Curriculum Program Content The purpose of the training program is to prepare the physician for the independent practice of neuroimaging. Neuroimaging is the subspecialty of Neurology
Neuroimaging Core Curriculum Program Content The purpose of the training program is to prepare the physician for the independent practice of neuroimaging. Neuroimaging is the subspecialty of Neurology
Endocrinological Outcome Among Treated Craniopharyngioma Patients
 Endocrinological Outcome Among Treated Craniopharyngioma Patients Afaf Al Sagheir, MD Head & Consultant, Section of Endocrinology/Diabetes Department of Pediatrics KFSH&RC Introduction Craniopharyngiomas
Endocrinological Outcome Among Treated Craniopharyngioma Patients Afaf Al Sagheir, MD Head & Consultant, Section of Endocrinology/Diabetes Department of Pediatrics KFSH&RC Introduction Craniopharyngiomas
Clinician s Guide To Ordering NeuroImaging Studies
 Clinician s Guide To Ordering NeuroImaging Studies MRI CT South Jersey Radiology Associates The purpose of this general guide is to assist you in choosing the appropriate imaging test to best help your
Clinician s Guide To Ordering NeuroImaging Studies MRI CT South Jersey Radiology Associates The purpose of this general guide is to assist you in choosing the appropriate imaging test to best help your
Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234)
 Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland. In patients
Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland. In patients
Radiographic and statistical analysis of Brain Arteriovenous Malformations.
 Radiographic and statistical analysis of Brain Arteriovenous Malformations. Poster No.: C-0996 Congress: ECR 2017 Type: Educational Exhibit Authors: C. E. Rodriguez 1, A. Lopez Moreno 1, D. Sánchez Paré
Radiographic and statistical analysis of Brain Arteriovenous Malformations. Poster No.: C-0996 Congress: ECR 2017 Type: Educational Exhibit Authors: C. E. Rodriguez 1, A. Lopez Moreno 1, D. Sánchez Paré
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM BRAIN METASTASES CNS Site Group Brain Metastases Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM BRAIN METASTASES CNS Site Group Brain Metastases Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
Neurosurgical Management of Brain Tumours. Nicholas Little Neurosurgeon RNSH
 Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Page 1 of 74 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Stereotactic Radiosurgery and Stereotactic
Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Page 1 of 74 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Stereotactic Radiosurgery and Stereotactic
