An update on congenital melanocytic naevi in children
|
|
|
- Lindsay Moore
- 5 years ago
- Views:
Transcription
1 NEDERLANDS TIJDSCHRIFT VOOR DERMATOLOGIE EN VENEREOLOGIE VOLUME 25 NUMMER 02 februari An update on congenital melanocytic naevi in children V.A. Kinsler Academic Lead Clinician and Consultant Paediatric Dermatologist, Paediatric Dermatology department, Great Ormond Street Hospital for Children NHS Foundation Trust, London Wellcome Trust Fellow, Genetics and Genomic Medicine, UCL Institute of Child Health, London Correspondence: Veronica A. Kinsler MA MB BChir MRCPCH PhD CLASSIFICATION OF CMN The classification of CMN has recently been unified with that of other congenital naevi (epidermal, connective tissue). 1 This is based on clinical phenotype, histology (undifferentiable currently for CMN) and genotype: Clinical phenotype: 1. Cutaneous only single, or multiple (more than one lesion at birth) 2. With extracutaneous features then termed CMN syndrome Genotype: 1. NRAS mutation positive 2. Other causative mutation (would need to be shown in more than one lesion from the same patient, no other causative mutations yet published) To further refine the clinical phenotypic groups the most recent classification proposed to define the severity of the cutaneous phenotype is as follows:2 CMN projected adult size categories: small (<1.5 cm); medium (M1: cm, M2: >10-20 cm); large (L1: >20-30 cm, L2: >30-40 cm); and giant (G1: >40-60 cm, G2: >60 cm) Total number of naevi in the first year of life: 0, 1 to 20, 21 to 50, 51 or more Additional descriptors of CMN: localization, colour heterogeneity, surface rugosity, hypertrichosis (all none, moderate, marked), presence of nodules (none, scattered, extensive) In the author s own practice however the terms relating to size are not used (only measurement), and in particular giant is avoided as it is often disliked by families, and nor is the term satellite naevi as these are true congenital naevi in their own right, not an offshoot of the largest lesion. 3 Also in the author s practice the total number of naevi is categorized as 0-10, 11-20, 21-50, , , and >200, because many severely affected children are seen. Lastly the author also registers whether the lesions are clinically stable or not (ie producing new nodules), and whether the patient is developing new naevi. GENETICS OF CMN In 1987 Happle predicted that CMN syndrome (under the term neurocutaneous melanosis) would be one of various dermatological conditions caused by a lethal mutation surviving by mosaicism. 4 The first contributions to the molecular genetics of CMN were descriptions of mutations in single CMN, or in single lesions from any one patient. These studies described mutations in BRAF 5-11, NRAS 5,10,12-14, MC1R 5,15, TP53 5 and GNAQ. 13 As with all single lesions and indeed with the study of genetics of tumours the difficult lies in assigning their order in the pathogenesis of that lesion. As a result a study was performed to look at more than one lesion from the skin, and from neurological tissue from the same patients. This found that in 80% of cases tested there was conservation of codon 61 mutations in NRAS in different lesions from the same patient, which implies that this mutation is causative. 16 The mutations were absent from blood, proving Happle s original theory. This condition is therefore a mosaic RASopathy in at least 80% of cases. SINGLE CMN A distinction is made between single CMN of any size and multiple CMN (more than one at birth) because extracutaneous abnormalities have not so far been shown in any patient with a single lesion, independent of size or site. While this could still be reported, the risk of extracutaneous problems is clearly low. There is also a good genetic correlate for this observation, as a single CMN suggests a mutation in the embryo affecting only one area of skin, and therefore presumably at a time where the naevus cell lineage was already fate restricted to that one area.
2 78 NEDERLANDS TIJDSCHRIFT VOOR DERMATOLOGIE EN VENEREOLOGIE VOLUME 25 NUMMER 02 februari 2015 Single CMN are still on the basis of pathogenesis likely to carry an increased risk of melanoma compared to normal skin, but this appears to be very low These lesions are therefore not routinely excised for reasons of malignancy risk in the author s practice. 21 They can however be excised for cosmetic lesions if wished by the patient and if technically feasible. Management of single CMN in the author s practice therefore is detailed examination of the patient to check there are no other CMN no matter how small, full physical examination and neurodevelopmental assessment, photography of the lesion, contact made with the patient support group, contact with the plastic surgery team if wished, and then discharge from the Dermatology clinic unless the single lesion is of more than 20cm projected adult size (rare). If the clinical assessment was normal no routine MRI of the CNS is performed independent of the size or site of the lesion. The patient knows they can be referred back to our clinic at short notice if they have any concerns. The one caveat to this is in the case where the single CMN is associated with other types of pigmentary lesion, or with other physical problems. CMN are sometimes the presenting feature of other conditions, most commonly in the author s practice neurofibromatosis type 1. These patients should therefore be kept under review until the situation becomes clearer. MULTIPLE CMN (MORE THAN ONE LESION AT BIRTH) Individuals with multiple CMN carry a risk of extracutaneous abnormalities. In 2008 we published guidelines suggesting that all children more than one CMN at birth should have a routine screening MRI in the first 6 months of life, but single lesions even large or overlying the CNS should not. These guidelines have recently been reviewed and we have found that although the percentage of scans performed has dropped significantly, the percentage of abnormalities detected has not (remains around 20%). 22 Therefore we can assume that these guidelines have not led us to miss any or certainly not a large number of abnormalities. On the basis of clinical phenotype however we are not currently able to refine these guidelines further. Although there is a general association between the severity of the cutaneous phenotype and the chance of neurological abnormalities 17-19,23,24, this is far from perfect, and individuals with two CMN can still be found to have important lesions on scan. 19,22 CMN SYNDROME This term describes the association of CMN and extracutaneous features. These include neurological abnormalities, characteristic facial features, and more recently discovered rarely a hypophospha- taemic. The latter is more usually found in other mosaic RASopathies (HRAS mosaicism, which encompasses Schimmelpenning syndrome and Phakomatosis pigmentokeratotica), but has recently been described in one published case of CMN syndrome. 25 Other bony abnormalities have been described in CMN patients, particularly scoliosis, however it is not clear yet if these are also due to bony involvement by the mosaic mutation. CONGENITAL NEUROLOGICAL ABNORMALITIES WHY DO AN MRI SCAN? This area has been a contentious one, primarily because there is confusion over neurological findings and outcomes. This has stemmed from three problems: firstly this is a rare disease and until recently no group has had sufficient data to produce statistically relevant guidelines, secondly there are two conditions which can afflict the CNS congenital neurological abnormalities, and primary melanoma of the CNS, and thirdly there has been significant publishing bias towards adverse outcome cases, particularly seen in small studies. 17 These problems are largely now overcome by the publication of larger prospective studies. Importantly to note before beginning any discussion on neurological investigation, any child with CMN independent of phenotype with a change in neurological or neurodevelopmental status at any stage should have an MRI of the CNS to look for CNS melanoma. This is different from screening MRI for congenital neurological abnormalities. For screening for congenital neurological abnormalities, the reasons for performing an MRI in individuals with two or more CMN at birth are now known to be the following: 1. Melanin has a characteristic signal on MRI, and certain areas are well-described to show predilection for lesions in CMN patients 26,27 2. MRI is a better predictor of clinical neurological outcome than clinical phenotype Clinical management is altered based on the radiological findings Clinical management in the author s practice based on radiological findings: Normal scan, in 80% of patients with two or more CMN no repeat MRI required at any stage, no special neurodevelopmental follow up 2. Intraparenchymal melanosis alone, in approximately 10% this is the most characteristic radiological finding, most commonly in the amygdala, and can be diagnosed confidently by expert neuroradiologists. These lesions do not require neurosurgery. The children are at increased risk of neurodevelopmental abnormalities and seizures, and therefore require annual neurodevelopmental assessment up to school age.
3 NEDERLANDS TIJDSCHRIFT VOOR DERMATOLOGIE EN VENEREOLOGIE VOLUME 25 NUMMER 02 februari The scan does not need to be repeated routinely, and these lesions are not malignant so do not lead of themselves to a fatal outcome even if symptomatic. 3. All other findings on MRI have to be treated on an individual basis approximately 10%. These findings include benign brain tumours, congenital malformations such as Dandy-Walker, leptomeningeal disease either focal or diffuse, and mostly these are also associated with intraparenchymal melanosis as described above. This group as a whole have a much more guarded prognosis, as many require neurosurgery, many lesions are unique to that patient, and many (but not all) children are neurologically abnormal. These patients require referral to the paediatric neurology and neurosurgery teams, for assessment and follow up, and repeat scanning is the norm until the behaviour of individual lesions is clear. Diffuse leptomeningeal disease requires a particular mention as this frequently behaves as melanoma, and repeat scans are required at short intervals (weeks or months) until stability is established or malignancy is diagnosed. CHARACTERISTIC FACIAL FEATURES IN ASSOCIATION WITH CMN Children with CMN have been found in one cohort to have characteristic facial features. Their faces are not strikingly dysmorphic, however they do have a common face shared with other children with the same condition. The facial phenotype does not so far appear to be connected to the severity of the cutaneous phenotype, or to the presence of the neurological phenotype, but larger studies are underway to examine these questions. At least three characteristic facial features were seen in 70% of the children studied, and the possible facial features are as follows: a wide or prominent forehead, hypertelorism, eyebrow variants, periorbital fullness, small/ short nose, narrow nasal bridge, anteverted nares, broad nasal tip, broad or round face, full cheeks, prominent pre-maxilla, open mouth appearance, prominent everted lower lip, and prominent or long philtrum. 28 Characteristic facial features are seen in a variety of genetic disorders where the underlying abnormality is mosaic, for example Pallister-Killian syndrome, and mosaic Cornelia de Lange syndrome. 29 The RAS pathway germline conditions all also have characteristic facial features, and genes on this pathway (including NRAS) are therefore known to influence facial development. MELANOMA IN CMN PATIENTS For single CMN and melanoma see above. Individuals with CMN have a risk of developing melanoma, which is thought to peak in childhood 17, and although it is not inconceivable that this is due to publishing bias, the author s impression is that there is a peak in childhood due to the complex neurological phenotypes carrying a significant risk of malignant transformation. 22 For individuals with multiple CMN or CMN syndrome the risk of melanoma is a genetic risk to that individual, and there is no evidence thus far that UV exposure has anything to do with the risk of melanoma development. Sensible UV protection precautions are therefore a good idea as for all children, but over-zealous UV protection is not advised. Melanoma arising in the skin of children with CMN, particularly those with severe cutaneous phenotypes, is difficult to detect. This is partly because CMN are often highly heterogeneous making detection physically difficult, and partly because of the confounding problem of benign proliferative nodules. Proliferative nodules are common in severe phenotypes, and come in many phenotypic guises. As a general rule, the author deals with new nodules by having open access to clinics at short notice for a new lump in a CMN (patient usually seen within two weeks of reporting the issue), a photograph is taken with a scale, the patient is examined thoroughly, and if everything else is normal the nodule is reviewed within four weeks. If the nodule has grown or changed markedly within that time it will be resected. The vast majority however do not change, but stabilize. This avoids continuous resections in patients who produce many nodules, but judgement obviously has to be exerted for individual cases. At least half the cases of melanoma in children with CMN arise as a primary in the CNS 17,19, and in the author s experience it is much more common in the CNS than in the skin. Melanoma in the CNS usually presents with hydrocephalus before the fontanelles have closed, or raised intracranial pressure if afterwards. It can either appear as a solid intraparenchymal tumour, sometimes but not necessarily connected to the leptomeninges, or as leptomeningeal disease. While the solid intraparenchymal tumour will look different from congenital neurological disease in this condition, with malignant radiological features, the leptomeningeal disease does not necessarily look different initially. Indeed, often very early in the process no leptomeningeal disease is detectable on MRI, due to the limits of resolution of scanning, and only becomes apparent after some weeks. In the situation of acute onset of hydrocephalus or raised intracranial pressure with no other apparent cause therefore it is reasonable to assume that leptomeningeal disease is leading to obstruction of circulation of cerebrospinal fluid. The treatment for this in the short-term is ventriculo-peritoneal shunting, which improves the situation symptomatically. However, follow up scanning within a month is advocated to look for radiological progression, as this is an important sign of malignant disease. If progression is shown a leptomeningeal biopsy (or biopsy of a solid tumour) is the next step.
4 80 NEDERLANDS TIJDSCHRIFT VOOR DERMATOLOGIE EN VENEREOLOGIE VOLUME 25 NUMMER 02 februari 2015 Biopsy of CNS tissue for melanoma is fraught with the same problems as cutaneous melanoma in CMN tissue. Histology is notoriously difficult, and should be reviewed by at least two individuals with experience in the field. More recently, published and unpublished data from our lab on NRAS mutation testing has been shown to be useful, in that loss of the normal allele of NRAS (ie a progression from heterozygous NRAS mutation to homozygous mutation) can occur in melanoma. 16 The reverse however is not true, as melanoma can be present with only a heterozygous NRAS mutation, although other mutations are usually seen. Groundbreaking research on the utility of array comparative genomic hybridization in differentiating melanoma in CMN from benign proliferative nodules 30 has been confirmed in our laboratory in CNS malignancy as well as in the skin (unpublished data). Our current practice therefore is to do NRAS sequencing and array CGH on any tissue suspected of malignant transformation. In the author s opinion there is no place for lumbar puncture and histology of melanocytic cells in the cerebrospinal fluid, as these results are very difficult to interpret, and cells will be present in anyone with leptomeningeal disease, benign or malignant. Melanoma can also rarely arise within other tissues 18, and other non-melanoma tumours (in particular rhabdomyosarcoma) have also been rarely described in individuals with CMN Any unusual mass lesion in children with CMN should therefore be taken seriously and investigated thoroughly. As a general principal, although rare, where melanoma does arise in CMN patients it is extremely difficult or impossible to treat, with almost every proven case being fatal within 6-12 months from diagnosis. This is almost certainly due to the genetic drivers involved in this disease, but will also be confounded by difficulty of detection. New trials of new drug therapies are being trialled in the author s institution for melanoma in these patients. Prophylactic surgical resection of large areas of multiple CMN has not been shown to reduce the malignancy risk in this condition, probably for the genetic reasons given above, and because the majority of cases arise in the CNS. This does not preclude the judicious use of surgery for cosmetic reasons where deemed appropriate by the family and clinicians. 21 References 1. Kinsler VA, Sebire SN. Rook s Textbook of Dermatology: Wiley-Blackwell; Krengel S, Scope A, Dusza SW, Vonthein R, Marghoob AA. New recommendations for the categorization of cutaneous features of congenital melanocytic nevi. J Am Acad Dermatol 2013;68: Epub 2012/09/ Kinsler V. Satellite lesions in congenital melanocytic nevi-- time for a change of name. Pediatr Dermatol 2011;28: Epub 2011/03/ Happle R. Lethal genes surviving by mosaicism: a possible explanation for sporadic birth defects involving the skin. J Am Acad Dermatol 1987;16: Papp T, Pemsel H, Zimmermann R, Bastrop R, Weiss DG, Schiffmann D. Mutational analysis of the N-ras, p53, p16ink4a, CDK4, and MC1R genes in human congenital melanocytic naevi. J Med Genet 1999;36: Papp T, Schipper H, Kumar K, Schiffmann D, Zimmermann R. Mutational analysis of the BRAF gene in human congenital and dysplastic melanocytic naevi. Melanoma Res 2005;15: Pollock PM, Harper UL, Hansen KS, Yudt LM, Stark M, Robbins CM, et al. High frequency of BRAF mutations in nevi. Nat Genet 2003;33: Kumar R, Angelini S, Snellman E, Hemminki K. BRAF mutations are common somatic events in melanocytic nevi. J Invest Dermatol 2004;122: Ichii-Nakato N, Takata M, Takayanagi S, Takashima S, Lin J, Murata H, et al. High frequency of BRAFV600E mutation in acquired nevi and small congenital nevi, but low frequency of mutation in medium-sized congenital nevi. J Invest Dermatol 2006;126: Dessars B, De Raeve LE, El HH, Debouck CJ, Sidon PJ, Morandini R, et al. Chromosomal translocations as a mechanism of BRAF activation in two cases of large congenital melanocytic nevi. J Invest Dermatol 2007;127: Adjei AA, Cohen RB, Franklin W, Morris C, Wilson D, Molina JR, et al. Phase I pharmacokinetic and pharmacodynamic study of the oral, small-molecule mitogen-activated protein kinase kinase 1/2 inhibitor AZD6244 (ARRY ) in patients with advanced cancers. J Clin Oncol 2008;26: Bauer J, Curtin JA, Pinkel D, Bastian BC. Congenital melanocytic nevi frequently harbor NRAS mutations but no BRAF mutations. J nvest Dermatol 2007;127: Phadke PA, Rakheja D, Le LP, Selim MA, Kapur P, Davis A, et al. Proliferative nodules arising within congenital melanocytic nevi: a histologic, immunohistochemical, and molecular analyses of 43 cases. Am J Surg Pathol 2011;35: Wu D, Wang M, Wang X, Yin N, Song T, Li H, et al. Lack of BRAF(V600E) mutations in giant congenital melanocytic nevi in a Chinese population. Am J Dermatopathol 2011;33: Kinsler VA, Abu-Amero S, Budd P, Jackson IJ, Ring SM, Northstone K, et al. Germline Melanocortin-1-Receptor Genotype Is Associated with Severity of Cutaneous Phenotype in Congenital Melanocytic Nevi: A Role for MC1R in Human Fetal Development. J Invest Dermatol Epub 2012/05/11. De complete literatuurlijst is, vanaf drie weken na publicatie in dit tijdschrift, te vinden op
5 NEDERLANDS TIJDSCHRIFT VOOR DERMATOLOGIE EN VENEREOLOGIE VOLUME 25 NUMMER 02 februari Summary The classification of congenital melanocytic naevi (CMN) mirrors that of other congenital naevi. Hence CMN can be single or multiple, defined as two or more lesions at birth, whereas CMN syndrome is the association of CMN with extracutaneous features. Extracutaneous features described are characteristic facies, congenital neurological abnormalities, and very rarely abnormal bony metabolism. The term CMN syndrome has replaced the term neurocutaneous melanosis, due to the broad spectrum of neurological features described. A screening MRI scan of the CNS in the first year of life (ideally under 6 months), looking for congenital neurological abnormalities, has been shown to be the best predictor of clinical outcome in infants born with multiple CMN, independent of size or site. These results therefore dictate clinical management. This should be differentiated from MRI in any CMN patient with new neurological symptoms, to look for primary CNS melanoma, at least as common as cutaneous melanoma. Overall rates of malignancy are low (approximately 2%), however the most severely affected children have a substantial risk (approximately 10% in those with CMN greater than 40cm projected adult size). The genetic basis of multiple CMN and CMN syndrome has been established in the majority of cases (approximately 80%). This condition is a mosaic RASopathy, due to post-zygotic mutations in the gene NRAS. NRAS controls many important inter-cellular signalling pathways, and is already known to be involved in the pathogenesis of melanoma in the normal population. This explains the predisposition to melanoma in individuals with CMN, however further mutations are required to progress from the naevus to malignancy.
Approach to the Genetic Diagnosis of Neurological Disorders
 Approach to the Genetic Diagnosis of Neurological Disorders Dr Wendy Jones MBBS MRCP Great Ormond Street Hospital for Children National Hospital for Neurology and Neurosurgery What is a genetic diagnosis?
Approach to the Genetic Diagnosis of Neurological Disorders Dr Wendy Jones MBBS MRCP Great Ormond Street Hospital for Children National Hospital for Neurology and Neurosurgery What is a genetic diagnosis?
What Syndrome s That? Syndromes Associated with Vascular Anomalies
 What Syndrome s That? Syndromes Associated with Vascular Anomalies Dawn Siegel, MD Medical College of Wisconsin American Academy of Dermatology Meeting San Diego, CA Sat. February 17 th, 2018 Learning
What Syndrome s That? Syndromes Associated with Vascular Anomalies Dawn Siegel, MD Medical College of Wisconsin American Academy of Dermatology Meeting San Diego, CA Sat. February 17 th, 2018 Learning
Vernon K. Sondak. Department of Cutaneous Oncology Moffitt Cancer Center Tampa, Florida
 Vernon K. Sondak Department of Cutaneous Oncology Moffitt Cancer Center Tampa, Florida Australasian Melanoma Conference 2016 Sydney, NSW, Australia October 29, 2016 Disclosures Dr. Sondak is a compensated
Vernon K. Sondak Department of Cutaneous Oncology Moffitt Cancer Center Tampa, Florida Australasian Melanoma Conference 2016 Sydney, NSW, Australia October 29, 2016 Disclosures Dr. Sondak is a compensated
21/07/2017. The «gray zone» of diagnosis is visible. Nevus Atypical nevus Melanoma. Melanoma ex-blue nevus
 Update on the Clinico- Pathological and Molecular Diagnosis of Melanocytic Lesions None to declare Conflicts of interest Belfast pathology Arnaud de la Fouchardière MD, PhD Lyon, France What is new? Today
Update on the Clinico- Pathological and Molecular Diagnosis of Melanocytic Lesions None to declare Conflicts of interest Belfast pathology Arnaud de la Fouchardière MD, PhD Lyon, France What is new? Today
Birthmarks: When to worry, when to reassure
 Birthmarks: When to worry, when to reassure Aimee Smidt, MD, FAAD, FAAP Associate Professor, Depts of Dermatology and Pediatrics University of New Mexico School of Medicine November 2016 Goals and Objectives
Birthmarks: When to worry, when to reassure Aimee Smidt, MD, FAAD, FAAP Associate Professor, Depts of Dermatology and Pediatrics University of New Mexico School of Medicine November 2016 Goals and Objectives
Neurofibromatosis type 1 and RASopathies
 Neurofibromatosis type 1 and RASopathies Dawn Siegel, MD Medical College of Wisconsin American Academy of Dermatology San Diego, CA February 19 th, 2018 Neurofibromatosis Type 1 NF1- diagnostic criteria
Neurofibromatosis type 1 and RASopathies Dawn Siegel, MD Medical College of Wisconsin American Academy of Dermatology San Diego, CA February 19 th, 2018 Neurofibromatosis Type 1 NF1- diagnostic criteria
LENTIGO SIMPLEX. Epidemiology
 LENTIGO SIMPLEX Epidemiology The frequency of lentigo simplex in children and adults has not been determined. There does not appear to be a racial or gender predilection. Lentigo simplex is the most common
LENTIGO SIMPLEX Epidemiology The frequency of lentigo simplex in children and adults has not been determined. There does not appear to be a racial or gender predilection. Lentigo simplex is the most common
Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology
 Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology Outline Germline testing CDKN2A BRCA2 BAP1 Somatic testing Gene expression profiling (GEP) BRAF Germline vs Somatic testing
Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology Outline Germline testing CDKN2A BRCA2 BAP1 Somatic testing Gene expression profiling (GEP) BRAF Germline vs Somatic testing
Melanoma. Consultation on draft guideline - stakeholder comments. Comments to be submitted before 5pm on Friday 13 March 2015
 Please note: Please fill in both the stakeholder organisation and name of commentator fields. We cannot accept forms with attachments such as research articles, letters or leaflets. Stakeholder organisation(s)
Please note: Please fill in both the stakeholder organisation and name of commentator fields. We cannot accept forms with attachments such as research articles, letters or leaflets. Stakeholder organisation(s)
Malignant Melanoma of The Skin - Still A Medical Conundrum?
 SCENIHR Public hearing on the Preliminary Opinion: 'Biological effects of ultraviolet radiation relevant to health with particular reference to sunbeds for cosmetic purposes. Luxembourg, April 12 th, 2016
SCENIHR Public hearing on the Preliminary Opinion: 'Biological effects of ultraviolet radiation relevant to health with particular reference to sunbeds for cosmetic purposes. Luxembourg, April 12 th, 2016
Corporate Medical Policy Genetic Testing for Cutaneous Malignant Melanoma
 Corporate Medical Policy Genetic Testing for Cutaneous Malignant Melanoma File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_cutaneous_malignant_melanoma 8/2011
Corporate Medical Policy Genetic Testing for Cutaneous Malignant Melanoma File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_cutaneous_malignant_melanoma 8/2011
Early detection of Retinoblastoma in children. Max Mantik
 Early detection of Retinoblastoma in children Max Mantik Introduction The most common primary intraocular malignancy of childhood 10 to 15 % of cancers that occur within the first year of life Typical
Early detection of Retinoblastoma in children Max Mantik Introduction The most common primary intraocular malignancy of childhood 10 to 15 % of cancers that occur within the first year of life Typical
Reviewers' comments: Reviewer #1 (Remarks to the Author):
 Reviewers' comments: Reviewer #1 (Remarks to the Author): In this study the authors analysed 18 deep penetrating nevi for oncogenic genomic changes (single nucleotide variations, insertions/deletions,
Reviewers' comments: Reviewer #1 (Remarks to the Author): In this study the authors analysed 18 deep penetrating nevi for oncogenic genomic changes (single nucleotide variations, insertions/deletions,
MELANOMA. 4 Fitzroy Square, London W1T 5HQ Tel: Fax: Registered Charity No.
 MELANOMA This leaflet had been written to help you understand more about melanoma. It tells you what it is, what causes it, what can be done about it, how it can be prevented, and where you can find out
MELANOMA This leaflet had been written to help you understand more about melanoma. It tells you what it is, what causes it, what can be done about it, how it can be prevented, and where you can find out
Psychosocial sequelae in 29 children with giant congenital melanocytic naevi
 Clinical dermatology X Original article Psychosocial sequelae in 29 children with giant congenital melanocytic naevi H. M. Koot, F. de Waard-van der Spek,* C. D. Peer,* P. G. H. Mulder ² and A. P. Oranje*
Clinical dermatology X Original article Psychosocial sequelae in 29 children with giant congenital melanocytic naevi H. M. Koot, F. de Waard-van der Spek,* C. D. Peer,* P. G. H. Mulder ² and A. P. Oranje*
Clinical Commissioning Policy Proposition: Everolimus for subependymal giant cell astrocytoma (SEGA) associated with tuberous sclerosis complex
 Clinical Commissioning Policy Proposition: Everolimus for subependymal giant cell astrocytoma (SEGA) associated with tuberous sclerosis complex Reference: NHS England E09X04/01 Information Reader Box (IRB)
Clinical Commissioning Policy Proposition: Everolimus for subependymal giant cell astrocytoma (SEGA) associated with tuberous sclerosis complex Reference: NHS England E09X04/01 Information Reader Box (IRB)
CHROMOSOMAL MICROARRAY (CGH+SNP)
 Chromosome imbalances are a significant cause of developmental delay, mental retardation, autism spectrum disorders, dysmorphic features and/or birth defects. The imbalance of genetic material may be due
Chromosome imbalances are a significant cause of developmental delay, mental retardation, autism spectrum disorders, dysmorphic features and/or birth defects. The imbalance of genetic material may be due
22q11.2 DELETION SYNDROME. Anna Mª Cueto González Clinical Geneticist Programa de Medicina Molecular y Genética Hospital Vall d Hebrón (Barcelona)
 22q11.2 DELETION SYNDROME Anna Mª Cueto González Clinical Geneticist Programa de Medicina Molecular y Genética Hospital Vall d Hebrón (Barcelona) Genomic disorders GENOMICS DISORDERS refers to those diseases
22q11.2 DELETION SYNDROME Anna Mª Cueto González Clinical Geneticist Programa de Medicina Molecular y Genética Hospital Vall d Hebrón (Barcelona) Genomic disorders GENOMICS DISORDERS refers to those diseases
Germline mutation analysis in the CYLD gene in Chinese patients with multiple trichoepitheliomas
 Germline mutation analysis in the CYLD gene in Chinese patients with multiple trichoepitheliomas Z.L. Li 1,2, H.H. Guan 3, X.M. Xiao 1,2, Y. Hui 3, W.X. Jia 1,2, R.X. Yu 1,2, H. Chen 1,2 and C.R. Li 1,2
Germline mutation analysis in the CYLD gene in Chinese patients with multiple trichoepitheliomas Z.L. Li 1,2, H.H. Guan 3, X.M. Xiao 1,2, Y. Hui 3, W.X. Jia 1,2, R.X. Yu 1,2, H. Chen 1,2 and C.R. Li 1,2
NRAS Mutation Is the Sole Recurrent Somatic Mutation in Large Congenital Melanocytic Nevi
 See related commentary on pg 879 ORIGINAL ARTICLE NRAS Mutation Is the Sole Recurrent Somatic Mutation in Large Congenital Melanocytic Nevi Christelle Charbel 1,2, Romain H. Fontaine 1,2,13, Gabriel G.
See related commentary on pg 879 ORIGINAL ARTICLE NRAS Mutation Is the Sole Recurrent Somatic Mutation in Large Congenital Melanocytic Nevi Christelle Charbel 1,2, Romain H. Fontaine 1,2,13, Gabriel G.
Melanocytic proliferations in sundamaged
 Atypical Spitzoid Tumor: What Does It Mean And How Should It Be Managed? Melanocytic proliferations in sundamaged skin Jane L. Messina, Jane L. Messina MD International Melanoma Pathology Working Group
Atypical Spitzoid Tumor: What Does It Mean And How Should It Be Managed? Melanocytic proliferations in sundamaged skin Jane L. Messina, Jane L. Messina MD International Melanoma Pathology Working Group
Molecular Aspects of Melanocytic Neoplasia. Iwei Yeh MD, PhD University of California, San Francisco
 Molecular Aspects of Melanocytic Neoplasia Iwei Yeh MD, PhD University of California, San Francisco Thanks to: Boris Bastian Timothy McCalmont Philip LeBoit Beth Ruben Jeff North Laura Pincus Thaddeus
Molecular Aspects of Melanocytic Neoplasia Iwei Yeh MD, PhD University of California, San Francisco Thanks to: Boris Bastian Timothy McCalmont Philip LeBoit Beth Ruben Jeff North Laura Pincus Thaddeus
Mole mapping and monitoring. Dr Stephen Hayes. Associate Specialist in Dermatology, University Hospital Southampton
 Mole mapping and monitoring Dr Stephen Hayes Associate Specialist in Dermatology, University Hospital Southampton Outline of presentation The melanoma epidemic Benefits of early detection Risks of the
Mole mapping and monitoring Dr Stephen Hayes Associate Specialist in Dermatology, University Hospital Southampton Outline of presentation The melanoma epidemic Benefits of early detection Risks of the
Melanocytic nevi, commonly referred to as
 Evaluation and Management of Melanocytic Nevi in Children Children with melanocytic nevi require proper counseling to discuss the risk for melanoma. Kara N. Shah, MD, PhD Melanocytic nevi, commonly referred
Evaluation and Management of Melanocytic Nevi in Children Children with melanocytic nevi require proper counseling to discuss the risk for melanoma. Kara N. Shah, MD, PhD Melanocytic nevi, commonly referred
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name OMIM number for disease 147920 Disease alternative names Please provide any alternative
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name OMIM number for disease 147920 Disease alternative names Please provide any alternative
MELANOMA IN ADOLESCENTS AND YOUNG ADULTS
 Cancer in Adolescents and Young Adults (AYA) Working Group MELANOMA IN ADOLESCENTS AND YOUNG ADULTS Emmanouil Saloustros MD, DSc General Hospital of Heraklion Venizelio Heraklion, Crete, Greece ESMO Preceptorship
Cancer in Adolescents and Young Adults (AYA) Working Group MELANOMA IN ADOLESCENTS AND YOUNG ADULTS Emmanouil Saloustros MD, DSc General Hospital of Heraklion Venizelio Heraklion, Crete, Greece ESMO Preceptorship
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Multiple Copy Number Variations in a Patient with Developmental Delay ASCLS- March 31, 2016
 Multiple Copy Number Variations in a Patient with Developmental Delay ASCLS- March 31, 2016 Marwan Tayeh, PhD, FACMG Director, MMGL Molecular Genetics Assistant Professor of Pediatrics Department of Pediatrics
Multiple Copy Number Variations in a Patient with Developmental Delay ASCLS- March 31, 2016 Marwan Tayeh, PhD, FACMG Director, MMGL Molecular Genetics Assistant Professor of Pediatrics Department of Pediatrics
Klippel Trenaunay and Proteus Syndrome overlap--a diagnostic dilemma
 Klippel Trenaunay and Proteus Syndrome overlap--a diagnostic dilemma Puri K.J.P.S. (MD)*, Malhotra S.K. (MD)**, Akanksha Jain (MBBS)*** Professor& Head* Professor& Head** Resident*** Department of Dermatology,
Klippel Trenaunay and Proteus Syndrome overlap--a diagnostic dilemma Puri K.J.P.S. (MD)*, Malhotra S.K. (MD)**, Akanksha Jain (MBBS)*** Professor& Head* Professor& Head** Resident*** Department of Dermatology,
PORT WINE STAINS AND STURGE-WEBER SYNDROME
 PORT WINE STAINS AND STURGE-WEBER SYNDROME Ong Hian Tat It is important for general practitioners to recognize cutaneous port-wine stains as these could signify important association with Sturge Weber
PORT WINE STAINS AND STURGE-WEBER SYNDROME Ong Hian Tat It is important for general practitioners to recognize cutaneous port-wine stains as these could signify important association with Sturge Weber
CEWT (Children s Epilepsy Workstream in Trent) Guidelines process.
 ttingham Children s Hospital ttingham University Hospitals Seizure with Fever Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author)
ttingham Children s Hospital ttingham University Hospitals Seizure with Fever Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author)
Assisting diagnosis of melanoma through the noninvasive biopsy of skin lesions
 Assisting diagnosis of melanoma through the noninvasive biopsy of skin lesions Symon D Oyly Cotton Ela Claridge School of Computer Science, The University of Birmingham Birmingham B15 2TT, UK Per Hall
Assisting diagnosis of melanoma through the noninvasive biopsy of skin lesions Symon D Oyly Cotton Ela Claridge School of Computer Science, The University of Birmingham Birmingham B15 2TT, UK Per Hall
Systemic epidermal nevus with involvement of the oral mucosa due to FGFR3 mutation
 Systemic epidermal nevus with involvement of the oral mucosa due to FGFR3 mutation Bygum et al. Bygum et al. BMC Medical Genetics 2011, 12:79 (5 June 2011) CASE REPORT Open Access Systemic epidermal nevus
Systemic epidermal nevus with involvement of the oral mucosa due to FGFR3 mutation Bygum et al. Bygum et al. BMC Medical Genetics 2011, 12:79 (5 June 2011) CASE REPORT Open Access Systemic epidermal nevus
The Enigmatic Spitz Lesion
 The Enigmatic Spitz Lesion The Dawn of Spitz S Spitz Sophie Spitz Melanomas of Childhood ; Am J Pathol 1948 1910-1956 13 children (18 mo - 12 yrs) 12/13 had a benign clinical course Sophie Spitz Born 1910
The Enigmatic Spitz Lesion The Dawn of Spitz S Spitz Sophie Spitz Melanomas of Childhood ; Am J Pathol 1948 1910-1956 13 children (18 mo - 12 yrs) 12/13 had a benign clinical course Sophie Spitz Born 1910
Codominance. P: H R H R (Red) x H W H W (White) H W H R H W H R H W. F1: All Roan (H R H W x H R H W ) Name: Date: Class:
 Name: Date: Class: (Exceptions to Mendelian Genetics Continued) Codominance Firstly, it is important to understand that the meaning of the prefix "co is "together" (i.e. cooperate = work together, coexist
Name: Date: Class: (Exceptions to Mendelian Genetics Continued) Codominance Firstly, it is important to understand that the meaning of the prefix "co is "together" (i.e. cooperate = work together, coexist
Quantification of early stage lesions for loss of p53 should be shown in the main figures.
 Reviewer #1 (Remarks to the Author): Expert in prostate cancer The manuscript "Clonal dynamics following p53 loss of heterozygosity in Kras-driven cancers" uses a number of novel genetically engineered
Reviewer #1 (Remarks to the Author): Expert in prostate cancer The manuscript "Clonal dynamics following p53 loss of heterozygosity in Kras-driven cancers" uses a number of novel genetically engineered
المركب النموذج--- سبيتز وحمة = Type Spitz's Nevus, Compound SPITZ NEVUS 1 / 7
 SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
Update on Spitzoid and Blue nevus-like melanocytic lesions Emphasis on molecular studies informing diagnosis, prognosis and therapy
 Update on Spitzoid and Blue nevus-like melanocytic lesions Emphasis on molecular studies informing diagnosis, prognosis and therapy Michael T. Tetzlaff MD, PhD Associate Professor Department of Pathology,
Update on Spitzoid and Blue nevus-like melanocytic lesions Emphasis on molecular studies informing diagnosis, prognosis and therapy Michael T. Tetzlaff MD, PhD Associate Professor Department of Pathology,
Inflammatory Pseudotumor of the Skin: A Case Report And Review Of The Literature
 ISPUB.COM The Internet Journal of Dermatology Volume 6 Number 1 Inflammatory Pseudotumor of the Skin: A Case Report And Review Of The Literature J Frey, C Huerter, J Shehan Citation J Frey, C Huerter,
ISPUB.COM The Internet Journal of Dermatology Volume 6 Number 1 Inflammatory Pseudotumor of the Skin: A Case Report And Review Of The Literature J Frey, C Huerter, J Shehan Citation J Frey, C Huerter,
Morphologic characteristics of nevi associated with melanoma: a clinical, dermatoscopic and histopathologic analysis
 DERMATOLOGY PRACTICAL & CONCEPTUAL www.derm101.com Morphologic characteristics of nevi associated with melanoma: a clinical, dermatoscopic and histopathologic analysis Temeida Alendar 1, Harald Kittler
DERMATOLOGY PRACTICAL & CONCEPTUAL www.derm101.com Morphologic characteristics of nevi associated with melanoma: a clinical, dermatoscopic and histopathologic analysis Temeida Alendar 1, Harald Kittler
A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL
 A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL OBJECTIVES Discuss current trends and changing concepts in our understanding of
A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL OBJECTIVES Discuss current trends and changing concepts in our understanding of
MELANOMA. Some people are more likely to get a m Melanoma than others:
 MELANOMA This leaflet has been written to help you understand more about Melanoma. It tells you what is it, what causes it, what can be done about it, how it can be prevented, and where you can find out
MELANOMA This leaflet has been written to help you understand more about Melanoma. It tells you what is it, what causes it, what can be done about it, how it can be prevented, and where you can find out
Female 18. Deeply pigmented lesion on trunk.?warty naevus?seborrhoeic keratosis?malignant melanoma. The best diagnosis is:
 Female 18. Deeply pigmented lesion on trunk.?warty naevus?seborrhoeic keratosis?malignant melanoma. The best diagnosis is: A. deep penetrating naevus B. naevoid malignant melanoma C. pigment synthesising
Female 18. Deeply pigmented lesion on trunk.?warty naevus?seborrhoeic keratosis?malignant melanoma. The best diagnosis is: A. deep penetrating naevus B. naevoid malignant melanoma C. pigment synthesising
Lab Activity Report: Mendelian Genetics - Genetic Disorders
 Name Date Period Lab Activity Report: Mendelian Genetics - Genetic Disorders Background: Sometimes genetic disorders are caused by mutations to normal genes. When the mutation has been in the population
Name Date Period Lab Activity Report: Mendelian Genetics - Genetic Disorders Background: Sometimes genetic disorders are caused by mutations to normal genes. When the mutation has been in the population
Bone, soft tissue and skin tumors. By: Shefaa qa qa
 Bone, soft tissue and skin tumors By: Shefaa qa qa Bone tumors Most bone neoplasms develop during the first several decades of life and have a propensity for the long bones of the extremities. The occurrence
Bone, soft tissue and skin tumors By: Shefaa qa qa Bone tumors Most bone neoplasms develop during the first several decades of life and have a propensity for the long bones of the extremities. The occurrence
FAQ-Protocol 3. BRCA mutation carrier guidelines Frequently asked questions
 ULast updated: 09/02/2015 Protocol 3 BRCA mutation carrier guidelines Frequently asked questions UQ: How accurate are the remaining lifetime and 5 year breast cancer risks in the table? These figures are
ULast updated: 09/02/2015 Protocol 3 BRCA mutation carrier guidelines Frequently asked questions UQ: How accurate are the remaining lifetime and 5 year breast cancer risks in the table? These figures are
Update on Genetic Testing for Melanoma
 Update on Genetic Testing for Melanoma Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania February 18, 2018 AAD
Update on Genetic Testing for Melanoma Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania February 18, 2018 AAD
Melanocytic Tumors
 Melanocytic Tumors 803-808-7387 www.gracepets.com These notes are provided to help you understand the diagnosis or possible diagnosis of cancer in your pet. For general information on cancer in pets ask
Melanocytic Tumors 803-808-7387 www.gracepets.com These notes are provided to help you understand the diagnosis or possible diagnosis of cancer in your pet. For general information on cancer in pets ask
Multicompartmental congenital intracranial immature teratoma
 Neurology Asia 2013; 18(1) : 117 121 Multicompartmental congenital intracranial immature teratoma 1 Dharmendra Ganesan MS FRCS(SN), 1 Sheau Fung Sia MS MRCS, 1 Vairavan Narayanan MS, 2 Gnana Kumar FRCR,
Neurology Asia 2013; 18(1) : 117 121 Multicompartmental congenital intracranial immature teratoma 1 Dharmendra Ganesan MS FRCS(SN), 1 Sheau Fung Sia MS MRCS, 1 Vairavan Narayanan MS, 2 Gnana Kumar FRCR,
Springer Healthcare. Staging and Diagnosing Cutaneous Melanoma. Concise Reference. Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone
 Concise Reference Staging and Diagnosing Cutaneous Melanoma Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone Extracted from Handbook of Cutaneous Melanoma: A Guide to Diagnosis and Treatment Published
Concise Reference Staging and Diagnosing Cutaneous Melanoma Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone Extracted from Handbook of Cutaneous Melanoma: A Guide to Diagnosis and Treatment Published
Molecular Methods in the Diagnosis and Prognostication of Melanoma: Pros & Cons
 Molecular Methods in the Diagnosis and Prognostication of Melanoma: Pros & Cons Ben J. Friedman, MD Senior Staff Physician Department of Dermatology Department of Pathology and Laboratory Medicine Henry
Molecular Methods in the Diagnosis and Prognostication of Melanoma: Pros & Cons Ben J. Friedman, MD Senior Staff Physician Department of Dermatology Department of Pathology and Laboratory Medicine Henry
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB. Friday, February 13, :30 am 11:00 am
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 13, 2009 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 13, 2009 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
Cowden Syndrome PTEN Hamartoma Tumor Syndrome. ACCME/Disclosure. 1. Background. Outline
 MASSACHUSETTS GENERAL HOSPITAL HARVARD MEDICAL SCHOOL PATHOLOGY Cowden Syndrome PTEN Hamartoma Tumor Syndrome ACCME/Disclosure Vania Nosé, MD, PhD Professor of Pathology Director of Anatomic Pathology
MASSACHUSETTS GENERAL HOSPITAL HARVARD MEDICAL SCHOOL PATHOLOGY Cowden Syndrome PTEN Hamartoma Tumor Syndrome ACCME/Disclosure Vania Nosé, MD, PhD Professor of Pathology Director of Anatomic Pathology
Integrating Fluorescence in situ Hybridization and Genomic Array Results into the Diagnostic Workup of Melanoma
 Integrating Fluorescence in situ Hybridization and Genomic Array Results into the Diagnostic Workup of Melanoma Association for Molecular Pathology United States and Canadian Academy of Pathology Companion
Integrating Fluorescence in situ Hybridization and Genomic Array Results into the Diagnostic Workup of Melanoma Association for Molecular Pathology United States and Canadian Academy of Pathology Companion
SKIN LESIONS. On behalf of Airedale, Wharfedale and Craven CCG, Bradford City CCG and Bradford Districts CCG. Bradford and Airedale CCGs.
 Bradford and Airedale CCGs SKIN LESIONS Version: 2 Ratified by: Date ratified: Author(s): Responsible Committee: Consultant in Public Health Individual Funding Request Panel Date issue: September 2013
Bradford and Airedale CCGs SKIN LESIONS Version: 2 Ratified by: Date ratified: Author(s): Responsible Committee: Consultant in Public Health Individual Funding Request Panel Date issue: September 2013
Professor Peter Soyer. Academic Dermatologist Brisbane, Australia
 Professor Peter Soyer Academic Dermatologist Brisbane, Australia What s New in Melanoma Dermatology Research Centre, The University of Queensland, School of Medicine, Translational Research Institute &
Professor Peter Soyer Academic Dermatologist Brisbane, Australia What s New in Melanoma Dermatology Research Centre, The University of Queensland, School of Medicine, Translational Research Institute &
Modalities of Radiation
 Modalities of Radiation Superficial radiotherapy Orthovoltage Megavoltage Photons Electrons Brachytherapy Interstitial Moulds When to refer? The vast majority of skin cancers will be managed without any
Modalities of Radiation Superficial radiotherapy Orthovoltage Megavoltage Photons Electrons Brachytherapy Interstitial Moulds When to refer? The vast majority of skin cancers will be managed without any
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names Osteogenesis Imperfecta
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names Osteogenesis Imperfecta
MAPK Pathway. CGH Next Generation Sequencing. Molecular Tools in Care of Patients with Pigmented Lesions 7/20/2017
 Molecular Tools in Care of Patients with Pigmented Lesions Tammie Ferringer, MD Geisinger Medical Center, Danville, PA tferringer@geisinger.edu DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Tammie Ferringer,
Molecular Tools in Care of Patients with Pigmented Lesions Tammie Ferringer, MD Geisinger Medical Center, Danville, PA tferringer@geisinger.edu DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Tammie Ferringer,
Update on Cutaneous Mesenchymal Tumors. Thomas Brenn
 Update on Cutaneous Mesenchymal Tumors Thomas Brenn Cutaneous Mesenchymal Tumours Wide morphological and biological spectrum Myofibroblastic, smooth muscle, neural, vascular, apidocytic, undifferentiated;
Update on Cutaneous Mesenchymal Tumors Thomas Brenn Cutaneous Mesenchymal Tumours Wide morphological and biological spectrum Myofibroblastic, smooth muscle, neural, vascular, apidocytic, undifferentiated;
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT
 Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
MEDICAL GENOMICS LABORATORY. Non-NF1 RASopathy panel by Next-Gen Sequencing and Deletion/Duplication Analysis of SPRED1 (NNP-NG)
 Non-NF1 RASopathy panel by Next-Gen Sequencing and Deletion/Duplication Analysis of SPRED1 (NNP-NG) Ordering Information Acceptable specimen types: Blood (3-6ml EDTA; no time limitations associated with
Non-NF1 RASopathy panel by Next-Gen Sequencing and Deletion/Duplication Analysis of SPRED1 (NNP-NG) Ordering Information Acceptable specimen types: Blood (3-6ml EDTA; no time limitations associated with
Section 2 Original Policy Date 2013 Last Review Status/Date September 1, 2014
 Policy Number 2.04.82 Molecular Markers in Fine Needle Aspirates of the Thyroid Medical Policy Section 2 Original Policy Date 2013 Last Review Status/Date September 1, 2014 Disclaimer Our medical policies
Policy Number 2.04.82 Molecular Markers in Fine Needle Aspirates of the Thyroid Medical Policy Section 2 Original Policy Date 2013 Last Review Status/Date September 1, 2014 Disclaimer Our medical policies
variant led to a premature stop codon p.k316* which resulted in nonsense-mediated mrna decay. Although the exact function of the C19L1 is still
 157 Neurological disorders primarily affect and impair the functioning of the brain and/or neurological system. Structural, electrical or metabolic abnormalities in the brain or neurological system can
157 Neurological disorders primarily affect and impair the functioning of the brain and/or neurological system. Structural, electrical or metabolic abnormalities in the brain or neurological system can
Apps and Telemedicine H. Peter Soyer Dermatology Research Centre
 Apps and Telemedicine H. Peter Soyer Dermatology Research Centre p.soyer@uq.edu.au https://twitter.com/hpsoyer William Gibson The future is already here it's just not very evenly distributed Vision 3D
Apps and Telemedicine H. Peter Soyer Dermatology Research Centre p.soyer@uq.edu.au https://twitter.com/hpsoyer William Gibson The future is already here it's just not very evenly distributed Vision 3D
Infantile Hemangiomas: Not Just Strawberries
 Infantile Hemangiomas: Not Just Strawberries Ilona J. Frieden M.D. Professor of Dermatology & Pediatrics UC San Francisco Conflict of Interests: Consultant: Pierre Fabre Off-label discussion: I do intend
Infantile Hemangiomas: Not Just Strawberries Ilona J. Frieden M.D. Professor of Dermatology & Pediatrics UC San Francisco Conflict of Interests: Consultant: Pierre Fabre Off-label discussion: I do intend
Associate Clinical Professor of Dermatology MUSC
 Re-excision of Moderately Dysplastic Nevi: Should we or shouldn t we? John C. Maize, Jr, M.D. Dermatologist and Dermatopathologist Trident Dermatology, Charleston SC Associate Clinical Professor of Dermatology
Re-excision of Moderately Dysplastic Nevi: Should we or shouldn t we? John C. Maize, Jr, M.D. Dermatologist and Dermatopathologist Trident Dermatology, Charleston SC Associate Clinical Professor of Dermatology
Department of Neurosurgery. Differentiating Craniosynostosis from Positional Plagiocephaly
 Department of Neurosurgery Differentiating Craniosynostosis from Positional Plagiocephaly The number of infants with head shape deformities has risen over the past several years, likely due to increased
Department of Neurosurgery Differentiating Craniosynostosis from Positional Plagiocephaly The number of infants with head shape deformities has risen over the past several years, likely due to increased
Elements of Dysmorphology I. Krzysztof Szczałuba
 Elements of Dysmorphology I Krzysztof Szczałuba 9.05.2016 Common definitions (1) Dysmorphology: recognition and study of birth defects (congenital malformations) and syndromes [David Smith, 1960] Malformation:
Elements of Dysmorphology I Krzysztof Szczałuba 9.05.2016 Common definitions (1) Dysmorphology: recognition and study of birth defects (congenital malformations) and syndromes [David Smith, 1960] Malformation:
Provide specific counseling to parents and patients with neurological disorders, addressing:
 Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Understanding the Human Karyotype Colleen Jackson Cook, Ph.D.
 Understanding the Human Karyotype Colleen Jackson Cook, Ph.D. SUPPLEMENTAL READING Nussbaum, RL, McInnes, RR, and Willard HF (2007) Thompson and Thompson Genetics in Medicine, 7th edition. Saunders: Philadelphia.
Understanding the Human Karyotype Colleen Jackson Cook, Ph.D. SUPPLEMENTAL READING Nussbaum, RL, McInnes, RR, and Willard HF (2007) Thompson and Thompson Genetics in Medicine, 7th edition. Saunders: Philadelphia.
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names you wish listed) (A)-Testing
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names you wish listed) (A)-Testing
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Malignant melanoma: assessment and management of malignant melanoma 1.1 Short title Malignant Melanoma 2 The remit The Department
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Malignant melanoma: assessment and management of malignant melanoma 1.1 Short title Malignant Melanoma 2 The remit The Department
Child Neurology Elective PL1 Rotation
 PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
There is NO single Melanoma Stain. > 6000 Mutations in Melanoma. What else can be done to discriminate atypical nevi from melanoma?
 Las Vegas Fall Clinical 2016: The Assessment and Diagnosis of Melanoma Whitney A. High, MD, JD, MEng Associate Professor, Dermatology & Pathology Director of Dermatopathology (Dermatology) University of
Las Vegas Fall Clinical 2016: The Assessment and Diagnosis of Melanoma Whitney A. High, MD, JD, MEng Associate Professor, Dermatology & Pathology Director of Dermatopathology (Dermatology) University of
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Neurology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
Checklists for Pigmented Lesions and Hamartomas. Barrett Zlotoff, MD Associate Professor University of Virginia
 Checklists for Pigmented Lesions and Hamartomas Barrett Zlotoff, MD Associate Professor University of Virginia Disclosure of Relationships with Industry Barrett Zlotoff, MD F043 - Is it Only Skin Deep?
Checklists for Pigmented Lesions and Hamartomas Barrett Zlotoff, MD Associate Professor University of Virginia Disclosure of Relationships with Industry Barrett Zlotoff, MD F043 - Is it Only Skin Deep?
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
Proposal for a 2-stage RCT in high risk primary SCC: COMMISSAR Catherine Harwood Barts Health NHS Trust / QMUL
 Proposal for a 2-stage RCT in high risk primary SCC: COMMISSAR Catherine Harwood Barts Health NHS Trust / QMUL on behalf of Dr Louise Lansbury, Prof Fiona Bath-Hextall Nottingham Centre for Evidence Based
Proposal for a 2-stage RCT in high risk primary SCC: COMMISSAR Catherine Harwood Barts Health NHS Trust / QMUL on behalf of Dr Louise Lansbury, Prof Fiona Bath-Hextall Nottingham Centre for Evidence Based
BAP-oma & BEYOND MICHAEL A NOWAK, MD
 BAP-oma & BEYOND MICHAEL A NOWAK, MD CONFLICTS No conflicts with the content of this lecture BAP-oma Wiesner 2011: Families with multiple tan dome-shaped papules of head, neck, trunk, and extremities.
BAP-oma & BEYOND MICHAEL A NOWAK, MD CONFLICTS No conflicts with the content of this lecture BAP-oma Wiesner 2011: Families with multiple tan dome-shaped papules of head, neck, trunk, and extremities.
Case Report Giant Verrucous Haemangioma with Linear Features A Rare Entity and Successful Treatment with Complete Excision and Grafting
 IBIMA Publishing JMED Research http://www.ibimapublishing.com/journals/jmed/jmed.html Vol. 2016 (2016), Article ID 952849, 5 pages DOI: 10.5171/2016.952849 Case Report Giant Verrucous Haemangioma with
IBIMA Publishing JMED Research http://www.ibimapublishing.com/journals/jmed/jmed.html Vol. 2016 (2016), Article ID 952849, 5 pages DOI: 10.5171/2016.952849 Case Report Giant Verrucous Haemangioma with
SETPEG GENETIC TESTING GUIDELINES Version 1.0, 5 th October 2017
 SETPEG GENETIC TESTING GUIDELINES Version 1.0, 5 th October 2017 1. The Epilepsy Genetic Diagnostic & Counselling Service at King s Health Partners Professor Deb Pal PhD MRCP (Consultant) deb.pal@nhs.net
SETPEG GENETIC TESTING GUIDELINES Version 1.0, 5 th October 2017 1. The Epilepsy Genetic Diagnostic & Counselling Service at King s Health Partners Professor Deb Pal PhD MRCP (Consultant) deb.pal@nhs.net
The Adult Exceptional Aesthetic Referral Protocol (AEARP) September 2011
 Aesthetic surgery is not routinely offered by the NHS and can only be provided on an exceptional case basis in line with the Please Note Patients should only be referred following a clinical assessment
Aesthetic surgery is not routinely offered by the NHS and can only be provided on an exceptional case basis in line with the Please Note Patients should only be referred following a clinical assessment
Insights from Sequencing the Melanoma Exome
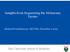 Insights from Sequencing the Melanoma Exome Michael Krauthammer, MD PhD, December 2 2015 Yale University School Yof Medicine 1 2012 Exome Screens and Results Exome Sequencing of 108 sun-exposed melanomas
Insights from Sequencing the Melanoma Exome Michael Krauthammer, MD PhD, December 2 2015 Yale University School Yof Medicine 1 2012 Exome Screens and Results Exome Sequencing of 108 sun-exposed melanomas
Enterprise Interest Nothing to declare
 Enterprise Interest Nothing to declare Diagnoses one would not like to miss in soft tissue pathology early in your career Marta Sbaraglia, MD Department of Pathology Hospital of Treviso University of Padua
Enterprise Interest Nothing to declare Diagnoses one would not like to miss in soft tissue pathology early in your career Marta Sbaraglia, MD Department of Pathology Hospital of Treviso University of Padua
Clinical Interpretation of Cancer Genomes
 IGENZ Ltd, Auckland, New Zealand Clinical Interpretation of Cancer Genomes Dr Amanda Dixon-McIver www.igenz.co.nz 1992 Slovenia and Croatia gain independence USA and Russia declare the Cold War over Steffi
IGENZ Ltd, Auckland, New Zealand Clinical Interpretation of Cancer Genomes Dr Amanda Dixon-McIver www.igenz.co.nz 1992 Slovenia and Croatia gain independence USA and Russia declare the Cold War over Steffi
Phoebe Rich MD Adjunct Professor OHSU Portland, Oregon
 Nail Tips for Diagnosis and Management of Nail Disorders Winter Clinical Dermatology Conference 2017 Hawaii Phoebe Rich MD Adjunct Professor OHSU Portland, Oregon Objectives diagnostic clues for benign
Nail Tips for Diagnosis and Management of Nail Disorders Winter Clinical Dermatology Conference 2017 Hawaii Phoebe Rich MD Adjunct Professor OHSU Portland, Oregon Objectives diagnostic clues for benign
p16 Genetic Test Reporting Counseling Protocol Flip Chart
 p16 Genetic Test Reporting Counseling Protocol Flip Chart Chromosomes, Gene, & Protein Cell Nucleus Chromosomes Gene Protein Adapted from Understanding Gene Testing,, NIH, 1995 Cancer Normal cell Disease
p16 Genetic Test Reporting Counseling Protocol Flip Chart Chromosomes, Gene, & Protein Cell Nucleus Chromosomes Gene Protein Adapted from Understanding Gene Testing,, NIH, 1995 Cancer Normal cell Disease
PanMidlands Ocular Cancer Pathway March 2008 Approved by The Midland Oculoplastic Surgery Society
 PanMidlands Ocular Cancer Pathway March 2008 Approved by The Midland Oculoplastic Surgery Society Periocular Skin Pathway Referrals to Oculoplastics Strong Indication: Lesion within orbital rim Medial
PanMidlands Ocular Cancer Pathway March 2008 Approved by The Midland Oculoplastic Surgery Society Periocular Skin Pathway Referrals to Oculoplastics Strong Indication: Lesion within orbital rim Medial
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names you wish listed) (A)-Testing
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names you wish listed) (A)-Testing
Management of pediatric melanocytic lesions
 Open Journal of Clinical & Medical Case Reports Management of pediatric melanocytic lesions Volume 3 (2017) Issue 8 ISSN 2379-1039 Jin Kim, BS; Emmanuel Gabriel MD, PhD; Weiguo Liu MD, PhD; Lin Lin MD,
Open Journal of Clinical & Medical Case Reports Management of pediatric melanocytic lesions Volume 3 (2017) Issue 8 ISSN 2379-1039 Jin Kim, BS; Emmanuel Gabriel MD, PhD; Weiguo Liu MD, PhD; Lin Lin MD,
Which melanoma patients benefit from genetic testing?
 Which melanoma patients benefit from genetic testing? Michael A. Marchetti, MD Assistant Attending, Dermatology Service Memorial Sloan Kettering Cancer Center American Academy of Dermatology Annual Meeting
Which melanoma patients benefit from genetic testing? Michael A. Marchetti, MD Assistant Attending, Dermatology Service Memorial Sloan Kettering Cancer Center American Academy of Dermatology Annual Meeting
Complex Hydrocephalus
 2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
Introduction to Evaluating Hereditary Risk. Mollie Hutton, MS, CGC Certified Genetic Counselor Roswell Park Comprehensive Cancer Center
 Introduction to Evaluating Hereditary Risk Mollie Hutton, MS, CGC Certified Genetic Counselor Roswell Park Comprehensive Cancer Center Objectives Describe genetic counseling and risk assessment Understand
Introduction to Evaluating Hereditary Risk Mollie Hutton, MS, CGC Certified Genetic Counselor Roswell Park Comprehensive Cancer Center Objectives Describe genetic counseling and risk assessment Understand
THE CHILD WITH NEUROFIBROMATOSIS TYPE 1 (NF1) A GUIDE FOR
 THE CHILD WITH NEUROFIBROMATOSIS TYPE 1 (NF1) A GUIDE FOR HEALTH CARE PROFESSIONALS Neurofibromatosis is actually a term that encompasses at least two distinct disorders, Neurofibromatosis Type 1 (NF1)
THE CHILD WITH NEUROFIBROMATOSIS TYPE 1 (NF1) A GUIDE FOR HEALTH CARE PROFESSIONALS Neurofibromatosis is actually a term that encompasses at least two distinct disorders, Neurofibromatosis Type 1 (NF1)
Histopathology: skin pathology
 Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
THE SPITZ NEVUS OFTEN POSES
 OBSERVATION ONLINE FIRST Melanoma Mimic A Case of Multiple Pagetoid Spitz Nevi KaLynne Harris, MD; Scott R. Florell, MD; Jason Papenfuss, MD; Wendy Kohlmann, MS, CGC; Mona Jahromi, BS; Joshua D. Schiffman,
OBSERVATION ONLINE FIRST Melanoma Mimic A Case of Multiple Pagetoid Spitz Nevi KaLynne Harris, MD; Scott R. Florell, MD; Jason Papenfuss, MD; Wendy Kohlmann, MS, CGC; Mona Jahromi, BS; Joshua D. Schiffman,
An Overview of Melanoma. Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center
 An Overview of Melanoma Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center Melanoma Statistics Median age at presentation 45-55 55 years Incidence: 2003 54,200 cases
An Overview of Melanoma Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center Melanoma Statistics Median age at presentation 45-55 55 years Incidence: 2003 54,200 cases
INTRATHECAL APPLICATION OF MONOCLONAL ANTIBODIES. Samo Rožman Institute of Oncology Ljubljana Slovenia
 INTRATHECAL APPLICATION OF MONOCLONAL ANTIBODIES Samo Rožman Institute of Oncology Ljubljana Slovenia AGENDA 1. INTRATHECAL APPLICATION 2. MONOCLONAL ANTIBODIES 3. MALIGNANT CARCINOMATOSIS 4. INTRATHECAL
INTRATHECAL APPLICATION OF MONOCLONAL ANTIBODIES Samo Rožman Institute of Oncology Ljubljana Slovenia AGENDA 1. INTRATHECAL APPLICATION 2. MONOCLONAL ANTIBODIES 3. MALIGNANT CARCINOMATOSIS 4. INTRATHECAL
