COLORECTAL CANCER COMPARATIVE REPORT
|
|
|
- Miles Warren
- 5 years ago
- Views:
Transcription
1 SA C07/11 W SE Scotland Cancer etwork Prospective Cancer Audit in South East Scotland COLORECTAL CACER COMPARATIVE REPORT Report on Patients Diagnosed January - December 2009 at Borders General Hospital Dumfries and Galloway Royal Infirmary Queen Margaret Hospital, Dunfermline Victoria Hospital, Kirkcaldy Western General Hospital, Edinburgh St John's Hospital at Howden, Livingston Lead Clinicians: Mr M Hosny Mr S Whitelaw Mr T Daniel Mr R G Wilson/Mr BJ Mander Report prepared by: Peigi Muir, SCA Cancer Audit Facilitator Chair of SCA Colorectal Group Mr B.J. Mander Scan Audit Office, c/o Clinical Oncology, Western General Hospital, Crewe Road, Edinburgh EH4 2XU T: W: F Alison Allen@luht.scot.nhs.uk South East Scotland Cancer etwork (SCA) - Working regionally to improve cancer services
2 South East Scotland Cancer etwork Report on Colorectal Cancer Patients Diagnosed 1st January - 31st December 2009 COTETS Page umber DOCUMET HISTORY...3 COLORECTAL SCA GROUP CHAIR COMMET...4 ACTIO POITS Background to this report Datasets, definitions and measures Audit Processes and data recording Data Quality Clinical Sign-Off External QA Estimated Case Ascertainment...7 SUMMARY OF ACHIEVEMET AGAIST ATIOAL STADARDS: HEALTH BOARDS...8 SUMMARY OF ACHIEVEMET AGAIST ATIOAL STADARDS: SCA...9 SUMMARY OF ACHIEVEMET AGAIST ATIOAL STADARDS OT PREVIOUSLY REPORTED...10 OTES O SUMMARY OF STADARDS...11 SUMMARY OF PATIETS BY KEY CATEGORIES...12 STADARD 2: MULTIDISCIPLIARY WORKIG...17 STADARD 3: AUDIT...18 STADARD 4: WAITIG TIMES...19 STADARD 5: PREOPERATIVE PREPARATIOS/IVESTIGATIOS...21 STADARD 6: THERAPEUTIC MAAGEMET...25 STADARD 7: POSTOPERATIVE MAAGEMET...27 STADARD 8: OUTCOMES...28 GLOSSARY...30 SA C07/11 W 09/06/2011 2
3 SCA Comparative Colorectal Cancer Audit Report DOCUMET HISTORY Version Date Issued Description Distribution 1 st Draft of SCA Colorectal Cancer Comparative Report for sensechecking 11/10/2010 SCA Group /10/ nd Draft of SCA Colorectal Cancer Comparative Report incorporating comments received from sensechecking for discussion at Lead Clinicians Meeting on 5/11/10 SCA Clinicians Lead /12/2010 Inclusion of revised figures for Standard 5a1 Mr BJ Mander /01/2011 Inclusion of Chairman s comments and circulation to SCA Group for final comments SCA Group /01/2011 o further comments received therefore finally signed off. Report o. SA C07/11 allocated and lodged on SCA Audit Report Index 4W June 2011 Report o. SA C07/11 W Circulation to: Health board Clinical Governance Groups Regional Cancer Planning Group (for meeting on 23/02/2011) Published on SCA Website SA C07/11 W 09/06/2011 3
4 COLORECTAL SCA GROUP CHAIR COMMET SCA Comparative Colorectal Cancer Audit Report 2009 This report provides comprehensive data on the management of Colorectal Cancer in the South East of Scotland during Enormous credit should be given to the SCA audit team, and Peigi Muir in particular, for the quality of the data. This has been facilitated by local data collection teams. During 2009 in SCA 890 patients were diagnosed with colorectal cancer, 750 (84%) of whom underwent surgery, which was performed with curative intent in 88% of cases. The exceptional standard of surgical care across the region should be highlighted. Perioperative mortality for all patients undergoing surgery was less than1% and has fallen steadily over the last 5 years from 5.3% in These are World-class results. Complications caused by Anastomotic Dehiscence (leakage at the site of the surgical join) are very low (1.5% for colonic anastomosis, 5.6% for rectal anastomosis, and 9.4% for patients undergoing anastomosis following Total Mesorectal Excision). They fall well within the required national HSQIS standards of 5%, 10% and 20% respectively. One or two areas of the report are affected by difficulties in collecting appropriate data. This is particularly an issue within Lothian relating to data on DVT and Antibiotic prophylaxis. This is being resolved through coordination with the process for implementing the Scottish Patient Safety Programme. In Lothian and Dumfries & Galloway processes for recording of access to stoma therapists need to be improved. Other Action Points highlighted which we will be looking into further are: A similar number of patients received radiotherapy and chemotherapy across the network. It was noted however that patients from the Borders General Hospital appear to wait longer for the chemotherapy which may relate to the lack of cross cover for this service when the designated consultant is on leave. We will look into ways of addressing these issues. The report has also highlighted a large number of early stage cancers in Dumfries and Galloway and we will be looking into the reasons for this. The appropriate protocol for access to Clinical urse Specialists for patients with polyp cancers. This report focuses on reporting the existing HSQIS standards. We believe there are a number of areas we should focus on in the coming year. These include auditing the availability of laparoscopic colorectal surgery across the network, reviewing our morbidity rates in patients undergoing chemotherapy, and looking at our long-term outcome data. We hope that there will be opportunities to compare the results of the three Scottish cancer networks, as occurred at the national meeting of In order to compare our results more widely, we have also taken the first steps in 2010 in entering our data into the UK ational Bowel Cancer Audit. Mr B.J. Mander Chair SCA Colorectal Group SA C07/11 W 09/06/2011 4
5 ACTIO POITS Listed below are some possible areas for improvement identified through the report with proposed action outlined against each: Report Section Standard 2 Multidisciplinary Working Standard 4 Waiting Times Summary of Patients by Key Categories Table 10 Possible area for improvement Ensure that appropriate patients have access to a Clinical urse Specialist There is currently no protocol for care of early stage polyp cancer patients, so that it is unclear in what circumstances access to the CS is required. umbers of early-stage cancers are increasing because of screening Aim to ensure that wait for adjuvant chemotherapy is equitable for Borders i.e. for 95% of patients is not greater than 56 days from surgery Ensure comparability of staging across SCA review reasons for larger proportion of Dukes A patients in Dumfries & Galloway Proposed action Develop a protocol for care of patients with polyp cancer including a review of the appropriate circumstances for them to be referred to a CS may not be necessary in all cases Review service issues about availability of oncology cover Compare numbers of Dukes A cancers detected in other SCA areas paying particular attention to the numbers of lymph nodes harvested. Which clinical standard will this meet? QIS Standard 2a1 QIS Standard 4b1 o specific standard but comparability of staging required as essential component of ensuring equity of treatment SA C07/11 W 09/06/2011 5
6 1 Background to this report 1.1 This report is the eighth to present comparative data on patients newly diagnosed with colorectal cancer in South East Scotland Cancer etwork (SCA) at the following hospitals- Borders General Hospital, Dumfries and Galloway Royal Infirmary, Queen Margaret Hospital, Dunfermline, Victoria Hospital, Kirkcaldy, St John's Hospital at Howden, Livingston, and Western General Hospital, Edinburgh. 1.2 The report covers data on patients newly-diagnosed in the twelve months from 1 January to 31 December Lead Clinicians and staff involved in audit were as follows Borders General Hospital (BGH) Mr M Hosny Lynn Smith/Alistair Meikle Dumfries & Galloway Royal Infirmary (DGRI) Mr S Whitelaw Martin Keith Queen Margaret Hospital (Fife) Mr T Daniel Maureen Lamb Western General Hospital, Edinburgh (WGH) Mr RG Wilson Peigi Muir SCA Mr BJ Mander Peigi Muir 2 Datasets, definitions and measures 2.1 The dataset collected is the nationally-agreed core minimum dataset (as revised in 2009), with definitions published by ISD Scotland ( For further information contact Peigi Muir, SCA Audit Facilitator, Western General Hospital, Edinburgh. (peigi.muir@luht.scot.nhs.uk) 2.2 Data has been analysed against national Bowel Cancer HS Quality Improvement Scotland Clinical Standards (revised March 2008), published by the Clinical Standards Board for Scotland, now HS Quality Improvement Scotland (HS QIS), and the 2001 Cancer Strategy: Our ational Health. 2.3 Measurability criteria have been prepared by the SCA Cancer Audit Facilitator who co-ordinates this across the network to ensure consistency of analysis. 2.4 From this report focused on a subset of measures which previously had shown variable results or were key indicators of surgical quality. However from 2009 onwards a more comprehensive review of certain HS QIS Standards which were agreed by the SCA Colorectal Group has been undertaken. 3 Audit Processes and data recording 3.1 Collection of the nationally-agreed core minimum dataset continues in all hospitals in South East Scotland. Data capture is focused round the process for the weekly multidisciplinary meetings i.e. ensuring that data covering patient referral, investigation, and diagnosis is being picked up through the routine process. SA C07/11 W 09/06/2011 6
7 3.2 Surgical and Oncology data is obtained either from the clinical records (electronic systems and case notes) or by download from the Department of Clinical Oncology database within the Edinburgh Cancer Centre (ECC) 3.3 The process remains dependent on audit staff for capture and entry of data, and for data quality checking 3.4 Data is recorded on local Access databases, apart from in the Fife region where data is collected using E-case. 4. Data Quality 4.1 Clinical Sign-Off: This report compares data from reports prepared for individual hospitals and signed off as accurate following review by the lead clinicians from each service. Additionally, the collated SCA results are reviewed by lead clinicians, including the lead Oncologist, to assess variances and provide comments on results. 4.2 External QA: SCA Audit participates in external quality assurance (QA) of data by ISD Scotland, (i.e. when a sample of data is compared with the data definitions). There has not been an external QA of the whole Colorectal Dataset since Estimated Case Ascertainment: Case ascertainment has been estimated using Scottish Cancer Registration data for 2008 for comparison purposes (with exclusions of patients only certified on death certificates and fully private patients). Tables on case ascertainment and five year averages are contained in the relevant section: Standard 3 Audit (QIS Standard 3a3). Most patients are identified through weekly multidisciplinary meetings. The following sources are used to check for missing patients: 1. Pathology records 2. Death lists 3. Dept of Clinical Oncology retrospective database 4. Clinical urse Specialist database 5. Provisional Cancer Registration lists Peigi Muir SCA Audit Facilitator SA C07/11 W 09/06/2011 7
8 SUMMARY OF ACHIEVEMET AGAIST ATIOAL STADARDS: HEALTH BOARDS BGH DGRI FIFE LOTHIA ational Standard CSBS 8b: 100% of Patients to Start XRT within 4 wks of seeing an Oncologist 50.0% 46.2% 72.7% 66.7% 87.5% 85.7% 71.4% 85.7% 100.0% 86.7% 100.0% 100.0% 52.9% 45.8% 78.9% 89.5% 76.5% 77.8% 60.0% 60.0% 78.1% 92.3% 85.2% 83.0% QIS 5b1: The rectum and whole colon is visualised by Colonoscopy or CT Colonography preoperatively (or when this is not possible because of the nature of the tumour, within 12 months of resection) in 95% of patients undergoing treatment with curative intent. 39.7% 59.3% 58.3% 57.9% 83.3% 76.8% 33.6% 57.1% 49.3% 75.0% 65.6% 73.3% 56.1% 69.2% 77.1% 82.1% 88.3% 95.3% 42.1% 55.4% 56.3% 48.5% 91.1% 75.4% QIS Standard 5c1: A CT Scan of the chest, abdomen & pelvis is performed preoperatively (or postoperatively where preoperative scanning is not possible because of emergency presentation) in 90% of patients undergoing surgery for bowel cancer 86.3% 94.9% 95.8% 98.2% 100.0% 96.8% 86.0% 94.0% 95.7% 90.7% 94.5% 95.6% 88.5% 98.6% 97.9% 97.2% 98.6% 98.7% 86.6% 92.6% 82.0% 85.5% 88.3% 92.9% QIS 7c1: Anastomotic Dehiscence is not more than 5% after surgery resulting in colonic anastomosis /R /R 5.9% 5.3% 10.5% 0.0% /R /R 5.6% 4.8% 8.0% 3.4% /R /r 1.5% 3.6% 1.6% 0.0% /R /R 0.0% 1.5% 0.0% 2.4% QIS 7c2: Anastomotic Dehiscence is not more than 10% after surgery resulting in rectal anastomosis /R 5.0% 10.0% 0.0% 8.0% 0.0% /R 10.5% 0.0% 0.0% 4.8% 3.6% /R 8.7% 0.0% 0.0% 2.4% 4.5% /R 7.9% 13.5% 8.9% 3.8% 7.0% QIS 7c3: Anastomotic Dehiscence is not more than 20% after Anterior Resection with Total Mesorectal Excision for rectal cancer 0.0% 0.0% 10.0% 0.0% 20.0% 12.5% 10.5% 0.0% 0.0% 0.0% 18.8% 0.0% 0.0% 8.3% 0.0% 0.0% 3.8% 0.0% 14.3% 7.9% 14.7% 13.3% 5.6% 13.2% QIS 8a1: Treatment Related Mortality is less then 5% after elective surgery 9.8% 8.0% 0.0% 5.4% 2.4% 0.0% 7.5% 7.6% 0.0% 1,4% 0.0% 0.0% 4.5% 4.9% 1.7% 2.4% 0.8% 0.7% 2.9% 2.8% 2.4% 2.9% 2.1% 1.2% QIS 8b1: Permanent Stoma rate is not more than 40% in patients with rectal cancer 21.7% 31.6% 8.7% 21.4% 7.7% 23.8% 9.3% 19.0% 15.0% 15.4% 14.3% 27.6% 31.8% 25.6% 22.6% 14.0% 11.1% 9.5% 15.0% 16.0% 12.4% 6.3% 11.8% 9.5% SA C07/11 W 09/06/2011 8
9 SUMMARY OF ACHIEVEMET AGAIST ATIOAL STADARDS: SCA (See notes overleaf) ational Standard SCA CSBS 8b: 100% of Patients to Start XRT within 4 wks of seeing an Oncologist 56.3% 56.5% 80.0% 88.3% 88.3% 84.5% QIS 5b1: The rectum and whole colon is visualised by Colonoscopy or CT Colonography preoperatively (or when this is not possible because of the nature of the tumour, within 12 months of resection) in 95% of patients undergoing treatment with curative intent. 56.3% 59.0% 59.5% 59.5% 87.2% 79.3% QIS Standard 5c1: A CT Scan of the chest, abdomen & pelvis is performed preoperatively (or postoperatively where preoperative scanning is not possible because of emergency presentation) in 90% of patients undergoing surgery for bowel cancer 87.4% 94.3% 88.7% 89.7% 91.9% 94.9% QIS 7c1: Anastomotic Dehiscence is not more than 5% after surgery resulting in colonic anastomosis /R /R 1.3% 2.6% 1.8% 1.5% QIS 7c2: Anastomotic Dehiscence is not more than 10% after surgery resulting in rectal anastomosis /R 8.0% 7.7% 3.8% 4.1% 5.6% QIS 7c3: Anastomotic Dehiscence is not more than 20% after Anterior Resection with Total Mesorectal Excision for rectal cancer 9.2% 7.1% 10.3% 6.3% 8.4% 9.4% QIS 8a1: Treatment Related Mortality is less then 5% after elective surgery 5.3% 4.8% 1.7% 2.8% 1.6% 0.8% QIS 8b1: Permanent Stoma rate is not more than 40% in patients with rectal cancer 20.0% 20.3% 11.6% 11.4% 11.7% 13.7% SA C07/11 W 09/06/2011 9
10 SUMMARY OF ACHIEVEMET AGAIST ATIOAL STADARDS OT PREVIOUSLY REPORTED HS QIS Standard BGH DGRI FIFE LOTHIA SCA QIS Standard 2a1: All patients have access to a Clinical urse Specialist (CS) 97.5% 95.6% 97.6% 87.8% 91.9% QIS Standard 2b4: There is a weekly Multidisciplinary Team Meeting (MDT) at which all patients are discussed 97.4% 98.2% 99.5% 97.7% 98.2% QIS Standard 2b5: All patients for rectal cancer resection are reviewed at the MDT Meeting preoperatively, unless clinical circumstances dictate otherwise 100.0% 100.0% 100.0% 95.1% 97.5% QIS Standard 4b1: In a minimum of 95% of patients who receive adjuvant chemotherapy, the time between surgery and start of adjuvant chemotherapy is not more than 56 days 50.0% 94.1% 81.1% 79.5% 78.8% QIS Standard 5a1: Patients considered for elective treatment are assessed by digital rectal examination (DRE) and either computed tomography (CT) scanning or magnetic resonance imaging (MRI) scanning of the primary tumour 100.0% 100.0% 98.3% 99.3% 99.2% QIS Standard 5d1: All elective patients who require a stoma are assessed preoperatively by a CS with expertise in stoma care 100.0% 42.9% 100.0% 86.3% 88.2% QIS Standard 5e1: All patients receive DVT prophylaxis preoperatively 96.8% 96.7% 100.0% 59.1% 76.4% QIS Standard 5e2: All patients receive Antibiotic prophylaxis preoperatively 96.8% 92.3% 100.0% 58.9% 75.6% QIS Standard 6a2: All patients with histologically involved Circumferential Margin (CRM) after resection for rectal cancer, receive postoperative radiotherapy (with or without concurrent chemotherapy) unless there is a documented contraindication 0.0% 0.0% 100.0% 0.0% 8.3% QIS Standard 6b1: All distal resection margins are free of tumour 95.2% 98.9% 98.1% 94.7% 96.0% QIS Standard 6b2: In patients undergoing primary resection (i.e. without preoperative radiotherapy or chemoradiotherapy) for rectal cancer, a minimum of 90% of circumferential margins (CRM) are free of tumour 100.0% 94.7% 97.7% 94.9% 96.2% SA C07/11 W 09/06/
11 OTES O SUMMARY OF STADARDS From 2005 Treatment Related Mortality and Permanent Stoma Rate measures will be presented against Health Board of Surgery rather than Health Board of Diagnosis From 2007 Preoperative visualisation of the whole colon Anastomotic Dehiscence after colonic anastomosis Anastomotic Dehiscence after rectal anastomosis Anastomotic Dehiscence after anterior resection with TME Treatment Related Mortality Permanent Stoma Rate are measured against Bowel Cancer HS Quality Improvement Scotland Clinical Standards (revised March 2008) In order to bring data in line with national analysis, from 2008: Standard 5b1 has been measured excluding non definitive surgery Standard 7c2 has not been restricted to patients with rectal cancer only and TME has been excluded Standard 8a1 has been measured excluding non definitive surgery Performance against Standards, for patients diagnosed in 2008, is highlighted by a system of Colour-coding as follows: Green indicates 95.0% - 100% achievement against target Amber indicates 75% % achievement against target Red <75% target not achieved From 2009 CSBS Standard 9c: 100% of patients to have Chest X-Ray or CT Chest performed preoperatively will now be measured against QIS Standard 5c1: A CT Scan of the chest, abdomen and pelvis is performed preoperatively (or postoperatively where preoperative scanning is not possible because of emergency presentation) in 90% of patients undergoing surgery for bowel cancer SA C07/11 W 09/06/
12 SUMMARY OF PATIETS BY KEY CATEGORIES Table 1: Rectal v Other Colorectal patients, percentage of Patients undergoing Surgery o of Patients Diagnosed umber of patients diagnosed with rectal cancer umber of patients diagnosed with rectal cancer who had surgery All patients who had surgery BGH % % % DGRI % % % FIFE % % % WGH % % % SCA % % % Table 2: Rectal v Other Colorectal patients, percentage of patients undergoing definitive surgery (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) o of Patients Diagnosed umber of patients diagnosed with rectal cancer umber of patients diagnosed with rectal cancer who had definitive surgery All patients who had definitive surgery BGH % % % DGRI % % % FIFE % % % WGH % % % SCA % % % Table 3: Emergency v. Elective Surgery (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) All Patients who had Definitive surgery Emergency Elective ot Recorded Missing Data BGH % % 0 0.0% 0 0.0% DGRI % % 0 0.0% 0 0.0% FIFE % % 0 0.0% 0 0.0% WGH % % 0 0.0% 0 0.0% SCA % % 0 0.0% 0 0.0% Clinical Comment by Mr T Daniel, Consultant Surgeon, Fife: The Central Referral Unit in Fife has been running for the past 5 years and allows for GPs to send all suspicion of cancer referrals to this unit where they should be reviewed and appointed within 14 days. As a result of this, particularly in the last 2-3 years, this appears to have been responsible for a downward trend in emergency admissions to hospitals in Fife. SA C07/11 W 09/06/
13 Table 4: Rectal Cancer Patients Emergency v. Elective Surgery (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) All Rectal Patients who had Definitive Surgery Emergency Elective ot Recorded Missing Data BGH % % 0 0.0% 0 0.0% DGRI % % 0 0.0% 0 0.0% FIFE % % 0 0.0% 0 0.0% WGH % % 0 0.0% 0 0.0% SCA % % 0 0.0% 0 0.0% Table 5: Intent of Surgery (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) All Patients who had Definitive Surgery Curative Palliative ot Recorded Missing Data BGH % 6 9.7% 0 0.0% 0 0.0% DGRI % 2 2.2% 3 3.3% 0 0.0% FIFE % % 0 0.0% 0 0.0% WGH % % 0 0.0% 0 0.0% SCA % % 3 0.4% 0 0.0% Clinical Comment: Colonic stenting facilities are available within Lothian and Fife, with interventional radiology available every 2 3 weeks within DGRI and only 1 Gastroenterologist available to Borders. Borders patients can be sent to the Western General Hospital, Edinburgh for stenting purposes. Table 6: Intent of Surgery (All Patients with Rectal Cancer who had surgery (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc)) All Patients with Rectal Cancer who had Definitive Surgery Curative Palliative ot Recorded Missing Data BGH % 2 9.5% 0 0.0% 0 0.0% DGRI % 0 0.0% 1 3.3% 0 0.0% FIFE % 4 9.1% 0 0.0% 0 0.0% WGH % % 0 0.0% 0 0.0% SCA % % 1 0.5% 0 0.0% SA C07/11 W 09/06/
14 Table 7: Sex Total Patients Diagnosed Male Female BGH % % DGRI % % FIFE % % WGH % % SCA % % Table 8: Age at Diagnosis BGH DGRI FIFE WGH SCA < % 0 0.0% 2 1.0% 6 1.2% 9 1.0% % 3 2.7% % % % % % % % % % % % % % % % % % % % % % % % % 4 3.5% 8 3.9% 9 1.8% % Total % % % % % Table 9: Tumour Site Site of Tumour BGH % DGRI % Fife % WGH % SCA % Appendix Ascending Colon Caecum Colon Unspecified Descending Colon Hepatic Flexure Rectum Sigmoid Colon Splenic Flexure Transverse Colon Overlapping Lesion ot Recorded Missing Data Total SA C07/11 W 09/06/
15 Table 10: Dukes Stage BGH % DGRI % Fife % WGH % SCA % Dukes A Dukes B Dukes C Dukes C Dukes D Inapplicable ot Recorded Missing Data Total Clinical Comment: Mr S. Whitelaw, Lead Clinician, DGRI, noted the high percentage of Dukes A cancers within Dumfries & Galloway and felt that this was due to under staging i.e. numbers of lymph nodes harvested. Mr Mander, SCA Group Chair, offered to conduct a comparative study of the other SCA Health Boards. 1 umbers showing an inapplicable Dukes Staging include patients who had no surgery, or patients who had polypectomies, stents, or defunctioning stomas, for whom Dukes Stage would not be assessable. SA C07/11 W 09/06/
16 Table 11: Radiotherapy All Patients diagnosed with Rectal Cancer who received Radiotherapy or Chemoradiotherapy eoadjuvant Single Therapy eoadjuvant Combined Therapy Primary Radical Adjuvant Postoperative Palliative ot Recorded BGH % % 0 0.0% 0 0.0% % 0 0.0% DGRI % % 0 0.0% 0 0.0% 1 6.3% 0 0.0% FIFE % % 0 0.0% 2 7.4% 1 3.7% 0 0.0% WGH % % 2 3.8% 0 0.0% % 0 0.0% SCA % % 2 1.8% 2 1.8% % 0 0.0% Clinical Comment by Mr T Daniel, Consultant Surgeon, Fife: Mr Daniel noted that all rectal patients in Fife were seen by Oncologist who then decided whether neoadjuvant treatment was appropriate. Mr BJ Mander noted that the practice within Lothian was to discuss these patients at the MDM where a joint surgical/oncology decision was made as to the appropriateness of neoadjuvant treatment. Table 12: Chemotherapy All patients who received Chemotherapy or Chemoradiotherapy eoadjuvant Primary Chemotherapy Palliative Chemotherapy Adjuvant Chemotherapy ot Recorded BGH % 0 0.0% % % 1 3.6% DGRI % 0 0.0% % % 1 3.2% FIFE % 0 0.0% % % 0 0.0% WGH % 3 2.1% % % 0 0.0% SCA % 3 1.1% % % 2 0.8% SA C07/11 W 09/06/
17 STADARD 2: MULTIDISCIPLIARY WORKIG QIS Standard 2a1: All patients have access to a Clinical urse Specialist (CS) = All Colorectal Cancer Patients All patients who were seen by a Clinical urse Specialist (CS) All patients who were not seen by a Clinical urse Specialist (CS) ot Patient Recorded Refused Missing Data BGH % 2 2.5% 0 0.0% 0 0.0% 0 0.0% D&G % 5 4.4% 0 0.0% 0 0.0% 0 0.0% FIFE % 5 2.4% 0 0.0% 0 0.0% 0 0.0% WGH % % 0 0.0% 2 0.4% 0 0.0% SCA % % 0 0.0% 2 0.2% 0 0.0% Clinical Comment: Within Lothian, the high percentage of patients not seen by CS is attributable to the fact that there is no policy/protocol for polyp cancer patients to be referred to the CS Service. QIS Standard 2b4: There is a weekly Multidisciplinary Meeting (MDT) at which all patients are discussed = All Colorectal Cancer Patients (exc patients who died before treatment) All patients discussed at MDT All patients not discussed at MDT ot Recorded Missing Data BGH % 1 1.3% 1 1.3% 0 0.0% D&G % 2 1.8% 0 0.0% 0 0.0% FIFE % 1 0.5% 0 0.0% 0 0.0% WGH % % 0 0.0% 0 0.0% SCA % % 1 0.1% 0 0.0% QIS Standard 2b5: All patients for rectal cancer resection are reviewed at the Multidisciplinary Team Meeting (MDT) preoperatively, unless clinical circumstances dictate otherwise. = All rectal cancer patients undergoing resection (exc patients who died before treatment and emergency presentations) All patients diagnosed with rectal cancer - discussed preoperatively at MDT All patients diagnosed with rectal cancer - not discussed preoperatively at MDT ot Recorded Missing Data BGH % 0 0.0% 0 0.0% 0 0.0% D&G % 0 0.0% 0 0.0% 0 0.0% FIFE % 0 0.0% 0 0.0% 0 0.0% WGH % 5 4.9% 0 0.0% 0 0.0% SCA % 5 2.5% 0 0.0% 0 0.0% SA C07/11 W 09/06/
18 STADARD 3: AUDIT QIS Standard 3a.3: There is a minimum of 90% case ascertainment against cancer registry data Registration Registered in Audit Jan - Dec 2009 % Estimated Case Ascertainment 2009 BGH % DGRI % FIFE % LOTHIA % SCA % SCA umbers recorded in audit and 5 Year Averages Cancer Year Averages Registration 5 Year Average BGH DGRI FIFE LOTHIA SCA In Dumfries and Galloway, Cancer Registration includes all patients resident within this area. Some patients, however, choose to attend hospital in Carlisle and therefore diagnosis and treatment occur in England. While these patients are included in Cancer Registry figures they are not included in Dumfries & Galloway data which excludes patients diagnosed outwith Scotland, as per the national dataset. From 2009 onwards private patients and patients whose normal residence is outwith Scotland but who have any part of their treatment within the HS are included in the audit. For the purposes of data continuity and quality, these patients have been noted separately as follows: HS Lothian: 6 private patients who had part of their treatment within the HS HS Fife: 1 patient whose normal residence was outwith Scotland HS DGRI: 2 patients whose normal residence was outwith Scotland 2 Source: Scottish Cancer Registry SA C07/11 W 09/06/
19 STADARD 4: WAITIG TIMES QIS Standard 4b1: In a minimum of 95% of patients who receive adjuvant chemotherapy, the time between surgery and start of adjuvant chemotherapy is not more than 56 days = All patients receiving adjuvant chemotherapy All patients commencing adjuvant Chemotherapy <56 days from Surgery All patients commencing adjuvant chemotherapy >56 days from Surgery ot Recorded Missing Data BGH % % 0 0.0% 0 0.0% D&G % 1 5.9% 0 0.0% 0 0.0% FIFE % % 0 0.0% 0 0.0% WGH % % 0 0.0% 0 0.0% SCA % % 0 0.0% 0 0.0% Clinical Comment: Only 1 Oncologist is available to BGH and therefore during holiday periods etc the waiting time from surgery to commencement of adjuvant chemotherapy can be increased. CSBS Standard 8b: Time from 1st seeing an Oncologist to the start of radiotherapy is not more than 4 weeks 3 = All rectal cancer patients receiving radiotherapy Within 4 weeks Over 4 weeks ot Recorded Missing Data BGH % % 0 0.0% 0 0.0% D&G % 0 0.0% 0 0.0% % FIFE % % 0 0.0% 0 0.0% WGH % % 0 0.0% 0 0.0% SCA % % 0 0.0% 2 1.8% % of Patients receiving Radiotherapy within 4 weeks of seeing an Oncologist Over 6 years across SCA BGH 50.0% 46.2% 72.7% 66.7% 87.5% 85.7% DGRI 71.4% 85.7% 100.0% 86.7% 100.0% 100.0% FIFE 52.9% 45.8% 78.9% 89.5% 76.5% 77.8% WGH 60.0% 60.0% 78.1% 92.3% 85.2% 83.0% SCA 56.3% 56.5% 80.0% 88.3% 88.3% 84.5% 3 This measurement is no longer included within the Bowel Cancer HS Quality Improvement Scotland Clinical Standards (revised March 2008), it was however felt important to continue to monitor this within the SCA region. SA C07/11 W 09/06/
20 SCA % of patients receiving radiotherapy within 4 weeks of seeing an Oncologist 100.0% 80.0% 80.0% 88.3% 88.3% 84.5% 60.0% 40.0% 56.3% 56.5% SCA 20.0% 0.0% SA C07/11 W 09/06/
21 STADARD 5: PREOPERATIVE PREPARATIOS/IVESTIGATIOS QIS Standard 5a1: Patients being considered for elective treatment are assessed by digital rectal examination (DRE) and either computed tomography (CT) scanning or magnetic resonance imaging (MRI) scanning of the primary tumour = All rectal cancer patients (exc emergency presentations) Performed ot Performed Result ot Recorded Missing Data BGH % 0 0.0% 0 0.0% 0 0.0% D&G % 0 0.0% 0 0.0% 0 0.0% FIFE % 1 1.7% 0 0.0% 0 0.0% WGH % 1 0.7% 0 0.0% 0 0.0% SCA % 2 0.8% 0 0.0% 0 0.0% QIS Standard 5b.1: The rectum and whole colon is visualised by Colonoscopy or CT Colonography preoperatively (or when this is not possible because of the nature of the tumour, within 12 months of resection) in 95% of patients undergoing treatment with curative intent. = All colorectal cancer patients undergoing curative resection by hospital of diagnosis (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) Visualised 1 ot Visualised Results /R Missing Data BGH % % 0 0.0% 0 0.0% D&G % % 0 0.0% 0 0.0% FIFE % 6 4.7% 0 0.0% 0 0.0% WGH % % 2 0.6% 0 0.0% SCA % % 2 0.3% 0 0.0% For DGRI: 1 = 23 14/23 not visualised 3/23 patients deceased prior to completion colonoscopy 3/23 patients attempted completion colonoscopy but investigation failed 1/23 patient refused all follow up 1/23 patient not fit for colonoscopy 1/23 patient now resident in orthern Ireland For Lothian: 1 = 42 Colonoscopies/CT Colon not performed + 42 incomplete colonoscopies 30/42 colonoscopies/ct Colon which were not performed were emergency presentations 12/42 colonoscopies/ct Colon which were not performed were elective presentations 28/42 colonoscopies which were incomplete are within 1 year post surgery 14/42 colonoscopies which were incomplete are over 1 year post surgery Clinical Comment: It was noted that the percentage attainment of this standard had improved generally but that there was still room for improvement. Preoperative Visualisation of the whole Colon throughout SCA Region and over 3 years BGH 57.9% 83.3% 76.8% DGRI 75.0% 65.6% 73.3% FIFE 82.1% 88.3% 95.3% WGH 48.5% 91.1% 75.4% SCA 59.5% 87.2% 79.3% SA C07/11 W 09/06/
22 QIS Standard 5c1: A CT Scan of the chest, abdomen and pelvis is performed preoperatively (or postoperatively where preoperative scanning is not possible because of emergency presentation) in 90% of patients undergoing surgery for bowel cancer Elective surgery patients having preoperative CT Chest Scan = All colorectal cancer patients undergoing elective resection by hospital of diagnosis (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) CT Chest Performed CT Chest ot Performed Result ot Recorded Missing Data BGH % 0 0.0% 0 0.0% 0 0.0% D&G % 0 0.0% 0 0.0% 0 0.0% FIFE % 2 1.4% 0 0.0% 0 0.0% WGH % % 0 0.0% 0 0.0% SCA % % 0 0.0% 0 0.0% Emergency surgery patients having preoperative CT Chest Scan = All colorectal cancer patients undergoing emergency resection by hospital of diagnosis (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) CT Chest Performed CT Chest ot Performed Result ot Recorded Missing Data BGH % 0 0.0% 0 0.0% 0 0.0% D&G % % 0 0.0% 0 0.0% FIFE % 0 0.0% 0 0.0% 0 0.0% WGH % % 0 0.0% 0 0.0% SCA % % 0 0.0% 0 0.0% All surgical patients who had CT Chest Scan = All colorectal cancer patients undergoing resection by hospital of diagnosis (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) CT Chest Performed CT Chest ot Performed Result ot Recorded Missing Data BGH % 2 3.2% 0 0.0% 0 0.0% D&G % 4 4.4% 0 0.0% 0 0.0% FIFE % 2 1.3% 0 0.0% 0 0.0% WGH % % 0 0.0% 0 0.0% SCA % % 0 0.0% 0 0.0% SA C07/11 W 09/06/
23 QIS Standard 5c1: A CT Scan of the chest, abdomen and pelvis is performed preoperatively (or postoperatively where preoperative scanning is not possible because of emergency presentation) in 90% of patients undergoing surgery for bowel cancer Elective surgery patients having preoperative CT Abdomen & Pelvis = All colorectal cancer patients undergoing elective resection by hospital of diagnosis (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) Liver Imaging Performed Liver Imaging ot Performed Result ot Recorded Missing Data BGH % 0 0.0% 0 0.0% 0 0.0% D&G % 0 0.0% 0 0.0% 0 0.0% FIFE % 2 1.4% 0 0.0% 0 0.0% WGH % 8 2.4% 0 0.0% 0 0.0% SCA % % 0 0.0% 0 0.0% Emergency surgery patients having preoperative CT Abdomen & Pelvis = All colorectal cancer patients undergoing emergency resection by hospital of diagnosis (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) Liver Imaging Performed Liver Imaging ot Performed Result ot Recorded Missing Data BGH % 0 0.0% 0 0.0% 0 0.0% D&G % 1 5.9% 0 0.0% 0 0.0% FIFE % 0 0.0% 0 0.0% 0 0.0% WGH % 1 1.6% 0 0.0% 0 0.0% SCA % 2 2.0% 0 0.0% 0 0.0% All surgical patients having CT Abdomen & Pelvis = All colorectal cancer patients undergoing resection by hospital of diagnosis (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) Liver Imaging Performed Liver Imaging ot Performed Result ot Recorded Missing Data BGH % 1 1.6% 0 0.0% 0 0.0% D&G % 1 1.1% 0 0.0% 0 0.0% FIFE % 2 1.3% 0 0.0% 0 0.0% WGH % 9 2.3% 0 0.0% 0 0.0% SCA % % 0 0.0% 0 0.0% SA C07/11 W 09/06/
24 QIS Standard 5d1: All elective patients who require a stoma are assessed preoperatively by a Clinical urse Specialist (CS) with expertise in stoma care = All patients presenting electively for surgery and having an operation involving stoma creation Patients seen preoperatively by CS with expertise in Stoma Care Patients ot seen preoperatively by CS with expertise in Stoma Care ot Recorded Missing Data BGH D&G FIFE WGH SCA % 8 6.7% 2 1.7% 4 3.4% The above table has been amended to avoid disclosure of potentially patient identifiable information QIS Standard 5e1: All patients receive DVT prophylaxis preoperatively = All colorectal cancer patients undergoing surgery by hospital of diagnosis (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) Patients receiving DVT Prophylaxis Patients not receiving DVT Prophylaxis ot Missing Recorded Data BGH % 0 0.0% 2 3.2% 0 0.0% D&G % 0 0.0% 0 0.0% 3 3.3% FIFE % 0 0.0% 0 0.0% 0 0.0% WGH % 2 0.5% 7 1.8% % SCA % 2 0.3% 9 1.3% % QIS Standard: 5e2: All patients receive Antibiotic prophylaxis preoperatively = All colorectal cancer patients undergoing surgery by hospital of diagnosis (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) Patients receiving Antibiotic Prophylaxis Patients not receiving Antibiotic Prophylaxis ot Missing Recorded Data BGH % 0 0.0% 2 3.2% 0 0.0% D&G % 3 3.3% 2 2.2% 2 2.2% FIFE % 0 0.0% 0 0.0% 0 0.0% WGH % 2 0.5% % % SCA % 5 0.7% % % For Lothian: The high percentage of missing data is directly attributable to the fact that this data item is only available within the casenotes, and is not recorded on any electronic system. However, from 2010 this information is recorded on the paper Surgical Safety Checklist forms completed under the Scottish Patient Safety Programme (SPSP). These have been made available to the audit facilitator making data capture more efficient. For DGRI: Due to data collection error 2 patients are missing data. These patients are now deceased and it has not been possible to gain access to casenotes. SA C07/11 W 09/06/
25 STADARD 6: THERAPEUTIC MAAGEMET QIS Standard 6a2: All patients with histologically involved Circumferential Margin (CRM) after resection for rectal cancer, receive postoperative radiotherapy (with or without concurrent chemotherapy) unless there is a documented contraindication = Rectal cancer patients undergoing a surgical procedure and having histologically involved Circumferential Margin (CRM) after surgery (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) Patients receiving postoperative Radiotherapy for involved CRM Postoperative radiotherapy contra-indicated in patients with involved CRM ot Missing Recorded Data BGH % 0 0.0% 0 0.0% 0 0.0% D&G % % 0 0.0% 0 0.0% FIFE % 0 0.0% 0 0.0% 0 0.0% WGH % % 0 0.0% 0 0.0% SCA % % 0 0.0% 0 0.0% For Lothian 7/10 patients had preoperative radiotherapy/chemoradiotherapy 3/10 patients had contraindications to postoperative radiotherapy as indicated by Dr HA Phillips QIS Standard 6b1: All distal resection margins are free of tumour = All colorectal cancer patients undergoing surgery (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) Surgical patients with clear distal resection margins Surgical patients with involved distal resection margins ot Recorded Inapplicable BGH % 1 1.6% 0 0.0% 2 3.2% D&G % 0 0.0% 1 1.1% 0 0.0% FIFE % 2 1.3% 1 0.6% 0 0.0% WGH % 0 0.0% 0 0.0% % SCA % 3 0.4% 2 0.3% % For Lothian 12/21 marked as inapplicable = no residual tumour post polypectomy 3/21 marked as inapplicable = no residual tumour post chemotherapy/chemoradiotherapy 2/21 marked as inapplicable = polypoidal tumours 4/21 marked as inapplicable = appendicele tumours SA C07/11 W 09/06/
26 QIS Standard 6b2: In patients undergoing primary resection (i.e. without preoperative radiotherapy or chemoradiotherapy) for rectal cancer, a minimum of 90% of Circumferential Margins (CRM) are free of tumour = All rectal cancer patients undergoing primary resection (exc patients having non definitive surgery i.e. Endoscopic treatment/stents/defunctioning Stomas/Bypass surgery etc) Surgical patients with clear CRM resection margins Surgical patients with involved CRM resection margins ot Recorded Inapplicable BGH % 0 0.0% 0 0.0% 0 0.0% D&G % 1 5.3% 0 0.0% 0 0.0% FIFE % 1 2.3% 0 0.0% 0 0.0% WGH % 3 5.1% 0 0.0% 0 0.0% SCA % 5 3.8% 0 0.0% 0 0.0% For Lothian: 3/59 patients had contraindications to preoperative radiotherapy as indicated by Dr HA Phillips SA C07/11 W 09/06/
27 STADARD 7: POSTOPERATIVE MAAGEMET QIS Standard 7c1: Anastomotic dehiscence is not more than 5% after colonic anastomosis = All colorectal cancer patients undergoing a surgical procedure involving anastomosis of the colon Anastomotic Dehiscence o Anastomotic Dehiscence ot Recorded Missing Data BGH % % 0 0.0% 0 0.0% DGRI % % 0 0.0% 0 0.0% FIFE % % 0 0.0% 0 0.0% WGH % % 5 3.0% 0 0.0% SCA % % 5 1.5% 0 0.0% For Lothian: Discharge summaries were not written in 5 cases and therefore postoperative complications have been marked as not recorded QIS Standard 7c2: Anastomotic dehiscence is not more than 10% after rectal anastomosis = All colorectal cancer patients undergoing a surgical procedure involving anastomosis of the rectum (excluding patients who had a total mesorectal excision (TME)) Anastomotic Dehiscence o Anastomotic Dehiscence ot Recorded Missing Data BGH % % 0 0.0% 0 0.0% DGRI % % 0 0.0% % FIFE % % 0 0.0% 0 0.0% WGH % % 4 3.1% 0 0.0% SCA % % 4 2.0% 3 1.5% For Lothian: Discharge summaries were not written in 4 cases and therefore postoperative complications have been marked as not recorded. QIS Standard 7c3: Anastomotic dehiscence is not more than 20% after anterior resection with total mesorectal excision for rectal cancer = All rectal cancer patients undergoing a surgical anterior resection and total mesorectal excision (TME) Anastomotic Dehiscence Rate after Anterior Resection with Total Mesorectal Excision (TME) BGH % DGRI % FIFE % WGH % SCA % Anastomotic Dehiscence Rate after Anterior Resection with TME (Total Mesorectal Excision) throughout SCA Region and over 6 years BGH 0.0% 0.0% 10.0% 0.0% 20.0% 12.5% DGRI 10.5% 0.0% 0.0% 0.0% 18.8% 0.0% FIFE 0.0% 8.3% 0.0% 0.0% 3.8% 0.0% WGH 14.3% 7.9% 14.7% 13.3% 5.6% 13.2% SCA 9.2% 7.1% 10.3% 6.3% 8.4% 9.4% SA C07/11 W 09/06/
28 STADARD 8: OUTCOMES QIS Standard 8a1: Treatment related mortality (defined as death occurring within 30 days of treatment (i.e. <=30)) is not >5% Treatment related mortality (defined as death occurring within 30 days of treatment (i.e. <=30)) by Health Board Area and Hospital of Surgery. = 1 All patients undergoing elective surgery by Health Board of diagnosis = 2 All patients undergoing elective surgery by Health Board of surgery ( 1 and 2 exclude patients having non-definitive surgery i.e. polypectomies, stents and defunctioning stomas) Health Board of Died <31 Days Diagnosis 1 following Surgery 2 Fife patients had surgery at the Western General Hospital, Edinburgh 4 BGH patients had surgery at the Western General Hospital, Edinburgh Comparative Table showing Treatment Related Mortality Rate by Health Board of Diagnosis and Health Board of Surgery Died <31 Days following Surgery Health Board of Surgery 2 BGH % Borders % DGRI % D&GRI % FIFE % QMH % LOTHIA % Lothian % SCA % SCA % Treatment Related Mortality throughout SCA Region and over 6 years SCA 5.3% 4.8% 1.7% 2.8% 1.6% 0.8% Treatment Related Mortality throughout SCA Region and over 6 years 8.0% 7.0% 6.0% 5.0% 4.0% 3.0% 2.0% 1.0% 0.0% 5.3% 4.8% 2.8% 1.6% 1.7% 0.8% SA C07/11 W 09/06/
29 QIS Standard 8b1: Permanent stoma rate is not more than 40% in patients with rectal tumours In many cases it is not possible to tell if a stoma is permanent until a number of years have passed. For the purposes of this report, a stoma will be defined as permanent only for those procedures (abdominoperineal resection and colostomy and panproctocolectomy and ileostomy) where the stoma was fashioned with the intention of being permanent. Patients left with permanent stoma after rectal cancer surgery by Hospital Board area and Hospital of Surgery = 1 All rectal cancer patients undergoing elective surgery by Health Board of diagnosis = 2 All rectal cancer patients undergoing elective surgery by Health Board of surgery Patients left with Permanent Stoma, by Heallth Board of Diagnosis % Permanent Stoma Rate Patients left with permanent Stoma, by Health Board of surgery % Permanent Stoma Rate Health Board of Diagnosis 1 Health Board of Surgery 2 Borders BGH D&G DGRI Fife QMH/VHK Lothian Lothian SCA % SCA % The above table has been amended to avoid disclosure of potentially patient identifiable information 2 Fife patients had surgery at Western General Hospital, Edinburgh. SA C07/11 W 09/06/
30 GLOSSARY (Edited selection based on HS QIS Bowel Cancer Standards, published 2008) Adjuvant Therapy Anastomosis Anastomotic dehiscence Antibiotic prophylaxis Audit BGH Bowel Cancer Cancer centre Clinical Governance Clinical urse Specialist (CS) The Clinical Standards Board for Scotland/HS QIS From 1 st April 2011 the body encompassing these roles is Healthcare Improvement Scotland (HIS) Colon Colonic anastomosis The use of chemotherapy and/or radiotherapy in addition to surgery. The aim of adjuvant therapy is to destroy any cancer that has spread. An artificial connection, created by surgery, between two tubular organs or parts, especially between two parts of the intestine. For example, a junction created by a surgeon between two pieces of bowel which have been cut to remove the intervening section. Bursting open or splitting of the surgical connection between two sections of intestine The administration of antibiotics to reduce the risk of infection. The measuring and evaluation of care against best practice with a view to improving current practice and care delivery. Borders General Hospital A tube-like structure which runs from the stomach to the anus. It allows digestion of food and the discharge of waste products. The name given to a group of diseases that can occur in any organ of the body, and in blood, and which involve abnormal uncontrolled growth of cells. Cancer services are based in cancer centres. Such centres provide the entire spectrum of cancer care - both on-site and to associated cancer units. Ensures that patients receive the highest quality of care possible, putting each patient at the centre of his or her care. This is achieved by making certain that those providing services work in an environment that supports them and places the safety and quality of care at the top of the organisation's agenda. A clinical nurse specialist is a registered nursing professional who has acquired additional knowledge, skills and experience, together with a professionally and/or academically accredited post-registration qualification (if available) in a clinical speciality. They practice at an advanced level and may have sole responsibility for a care episode or defined client/group. The Clinical Standards Board for Scotland was a statutory body, established as a Special Health Board in April Its role was to develop and run a system of quality control for clinical services designed to promote public confidence that the services provided by the HS met nationally agreed standards, and to demonstrate that, within the resources available, the HS was delivering the highest possible standards of care. On January 2003, CSBS was merged, along with four other clinical effectiveness bodies, to form HS Quality Improvement Scotland (HS QIS) Part of the bowel. Also called the large intestine or large bowel. This structure has five major divisions: caecum, ascending colon, transverse colon, descending colon, and sigmoid colon. The colon is responsible for forming, storing and expelling waste matter into the rectum. A procedure in which a part of the colon is removed and the two remaining ends are rejoined. SA C07/11 W 09/06/
COLORECTAL CANCER COMPARATIVE AUDIT REPORT SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT. Mr B.J. Mander SCAN Group Chair
 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT COLORECTAL CANCER 2013-2014 COMPARATIVE AUDIT REPORT Mr B.J. Mander SCAN Group Chair Mr K Pal, NHS Borders Mr S Whitelaw, NHS Dumfries & Galloway
SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT COLORECTAL CANCER 2013-2014 COMPARATIVE AUDIT REPORT Mr B.J. Mander SCAN Group Chair Mr K Pal, NHS Borders Mr S Whitelaw, NHS Dumfries & Galloway
Colorectal Cancer Comparative Audit Report
 SOUTH EAST SCOTLAND CANCER NETWORK (SCAN) PROSPECTIVE CANCER AUDIT Colorectal Cancer 2014 2015 Comparative Audit Report Mr B.J. Mander, NHS Lothian, Lead Colorectal Cancer Clinician, SCAN Group Chair Mr
SOUTH EAST SCOTLAND CANCER NETWORK (SCAN) PROSPECTIVE CANCER AUDIT Colorectal Cancer 2014 2015 Comparative Audit Report Mr B.J. Mander, NHS Lothian, Lead Colorectal Cancer Clinician, SCAN Group Chair Mr
COLORECTAL CANCER Quality Performance Indicators (QPI) Comparative Report
 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT COLORECTAL CANCER 2016 2017 Quality Performance Indicators (QPI) Comparative Report Mr S Yalamarthi, NHS Fife, Lead Colorectal Cancer Clinician,
SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT COLORECTAL CANCER 2016 2017 Quality Performance Indicators (QPI) Comparative Report Mr S Yalamarthi, NHS Fife, Lead Colorectal Cancer Clinician,
Colorectal Cancer Quality Performance Indicators
 Publication Report Colorectal Cancer Quality Performance Indicators Patients diagnosed between April 2013 and March 2016 Publication date 27th June 2017 An Official Statistics Publication for Scotland
Publication Report Colorectal Cancer Quality Performance Indicators Patients diagnosed between April 2013 and March 2016 Publication date 27th June 2017 An Official Statistics Publication for Scotland
HEAD AND NECK CANCERS
 SE Scotland Cancer Network HEAD AND NECK CANCERS COMPARATIVE ANNUAL REPORT PATIENTS DIAGNOSED 1 January 31 December 2008 Final Report Sign off 31 st August 2010 Chair of Head & Neck Group: - Dr EJ Junor
SE Scotland Cancer Network HEAD AND NECK CANCERS COMPARATIVE ANNUAL REPORT PATIENTS DIAGNOSED 1 January 31 December 2008 Final Report Sign off 31 st August 2010 Chair of Head & Neck Group: - Dr EJ Junor
Head and Neck Cancer 2012 COMPARATIVE AUDIT REPORT
 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT Head and Neck Cancer 2012 COMPARATIVE AUDIT REPORT Mr Guy Vernham, NHS Lothian SCAN Lead Clinician Head & Neck Cancer Mr J Morrison, Fife Mr
SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT Head and Neck Cancer 2012 COMPARATIVE AUDIT REPORT Mr Guy Vernham, NHS Lothian SCAN Lead Clinician Head & Neck Cancer Mr J Morrison, Fife Mr
Audit Report. Colorectal Cancer Quality Performance Indicators. Patients diagnosed April 2016 March Published: March 2018
 Colorectal Cancer Managed Clinical Network Audit Report Colorectal Cancer Quality Performance Indicators Patients diagnosed April 2016 March 2017 Published: March 2018 Mr Michael Walker NOSCAN MCN Clinical
Colorectal Cancer Managed Clinical Network Audit Report Colorectal Cancer Quality Performance Indicators Patients diagnosed April 2016 March 2017 Published: March 2018 Mr Michael Walker NOSCAN MCN Clinical
Head and Neck Cancer 2010 COMPARATIVE AUDIT REPORT
 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT Head and Neck Cancer 2010 COMPARATIVE AUDIT REPORT Mr Guy Vernham, NHS Lothian SCAN Lead Clinician Head & Neck Cancer Mr B Joshi, NHS Dumfries
SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT Head and Neck Cancer 2010 COMPARATIVE AUDIT REPORT Mr Guy Vernham, NHS Lothian SCAN Lead Clinician Head & Neck Cancer Mr B Joshi, NHS Dumfries
HEAD AND NECK CANCERS
 SE Scotland Cancer Network HEAD AND NECK CANCERS SCAN COMPARATIVE ANNUAL AUDIT REPORT PATIENTS DIAGNOSED 1 January 31 December 2009 REPORT NUMBER: SA HN01/11 W Chair of SCAN Head & Neck Group: - Mr Guy
SE Scotland Cancer Network HEAD AND NECK CANCERS SCAN COMPARATIVE ANNUAL AUDIT REPORT PATIENTS DIAGNOSED 1 January 31 December 2009 REPORT NUMBER: SA HN01/11 W Chair of SCAN Head & Neck Group: - Mr Guy
OESOPHAGO-GASTRIC CANCER 2016
 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT OESOPHAGO-GASTRIC CANCER 2016 COMPARATIVE AUDIT REPORT Mr Peter Lamb SCAN Lead Upper GI Cancer Clinician Dr Jonathan Fletcher, Consultant Physician,
SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT OESOPHAGO-GASTRIC CANCER 2016 COMPARATIVE AUDIT REPORT Mr Peter Lamb SCAN Lead Upper GI Cancer Clinician Dr Jonathan Fletcher, Consultant Physician,
SCAN Colorectal Group
 SCAN Colorectal Group Friday 1 st June 2012 14.15 16.15pm Oncology Seminar Room, WGH with videolink to Dumfries Present Alison Allen Angie Balfour Paul Fineron Stephen Glancy Mohammad Hosny Martin Keith
SCAN Colorectal Group Friday 1 st June 2012 14.15 16.15pm Oncology Seminar Room, WGH with videolink to Dumfries Present Alison Allen Angie Balfour Paul Fineron Stephen Glancy Mohammad Hosny Martin Keith
Audit Report. Colorectal Cancer Quality Performance Indicators. Patients diagnosed April 2014 March Published: July 2016
 NORTH OF SCOTLAND PLANNING GROUP Colorectal Cancer Managed Clinical Network Audit Report Colorectal Cancer Quality Performance Indicators Patients diagnosed April 2014 March 2015 Published: July 2016 Mr
NORTH OF SCOTLAND PLANNING GROUP Colorectal Cancer Managed Clinical Network Audit Report Colorectal Cancer Quality Performance Indicators Patients diagnosed April 2014 March 2015 Published: July 2016 Mr
Upper GI Cancer Quality Performance Indicators
 Publication Report Upper GI Cancer Quality Performance Indicators Patients diagnosed during January 2013 to December 2015 Publication date 28 th March 2017 An Official Statistics Publication for Scotland
Publication Report Upper GI Cancer Quality Performance Indicators Patients diagnosed during January 2013 to December 2015 Publication date 28 th March 2017 An Official Statistics Publication for Scotland
REPORT ON PROSPECTIVE AUDIT OF LYMPHOMA PATIENTS BORDERS, FIFE, AND LOTHIAN DIAGNOSED IN 2008
 SE Scotland Cancer Network SCAN AUDIT REPORT ON PROSPECTIVE AUDIT OF LYMPHOMA PATIENTS BORDERS, FIFE, AND LOTHIAN DIAGNOSED IN 2008 Reports prepared by: Christine Maguire SCAN Cancer Audit Facilitator
SE Scotland Cancer Network SCAN AUDIT REPORT ON PROSPECTIVE AUDIT OF LYMPHOMA PATIENTS BORDERS, FIFE, AND LOTHIAN DIAGNOSED IN 2008 Reports prepared by: Christine Maguire SCAN Cancer Audit Facilitator
SE SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT LUNG CANCER REPORT ON PATIENTS DIAGNOSED 1 JANUARY 31 DECEMBER 2009
 SE SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT LUNG CANCER REPORT ON PATIENTS DIAGNOSED 1 JANUARY 31 DECEMBER 2009 Dr Ron Fergusson SCAN Lead Lung Cancer Clinician Dr Colin Selby Dr Jakki Faccenda
SE SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT LUNG CANCER REPORT ON PATIENTS DIAGNOSED 1 JANUARY 31 DECEMBER 2009 Dr Ron Fergusson SCAN Lead Lung Cancer Clinician Dr Colin Selby Dr Jakki Faccenda
S E SCOTLAND CANCER NETWORK REPORT ON PROSPECTIVE AUDIT OF LYMPHOMA PATIENTS BORDERS, FIFE, AND LOTHIAN DIAGNOSED IN 2009
 SE Scotland Cancer Network SCAN AUDIT S E SCOTLAND CANCER NETWORK REPORT ON PROSPECTIVE AUDIT OF LYMPHOMA PATIENTS BORDERS, FIFE, AND LOTHIAN DIAGNOSED IN 2009 Dr John M Davies SCAN and NHS Lothian Dr
SE Scotland Cancer Network SCAN AUDIT S E SCOTLAND CANCER NETWORK REPORT ON PROSPECTIVE AUDIT OF LYMPHOMA PATIENTS BORDERS, FIFE, AND LOTHIAN DIAGNOSED IN 2009 Dr John M Davies SCAN and NHS Lothian Dr
BREAST CANCER 2010 COMPARATIVE AUDIT REPORT
 SOUTH EAST SCOTLAND CANCER PROSPECTIVE CANCER AUDIT BREAST CANCER 2010 COMPARATIVE AUDIT REPORT Dr Jeremy Thomas, NHS Lothian Chair, Breast Group Miss Fawzia Ashkanani, NHS Dumfries and Galloway Mr Matthew
SOUTH EAST SCOTLAND CANCER PROSPECTIVE CANCER AUDIT BREAST CANCER 2010 COMPARATIVE AUDIT REPORT Dr Jeremy Thomas, NHS Lothian Chair, Breast Group Miss Fawzia Ashkanani, NHS Dumfries and Galloway Mr Matthew
Colorectal Cancer Clinical Quality Performance Indicators
 Scottish Cancer Taskforce National Cancer Quality Steering Group Colorectal Cancer Clinical Quality Performance Indicators Published: December 2012 Updated: March 2015 (v2.1) May 2017 (v3.0) Published
Scottish Cancer Taskforce National Cancer Quality Steering Group Colorectal Cancer Clinical Quality Performance Indicators Published: December 2012 Updated: March 2015 (v2.1) May 2017 (v3.0) Published
Ovarian Cancer Quality Performance Indicators
 Ovarian Cancer Quality Performance Indicators Patients diagnosed between October 2013 and September 2016 Publication date 20 February 2018 An Official Statistics publication for Scotland This is an Official
Ovarian Cancer Quality Performance Indicators Patients diagnosed between October 2013 and September 2016 Publication date 20 February 2018 An Official Statistics publication for Scotland This is an Official
SCAN Colorectal Group
 SCAN Colorectal Group Friday 9 th August 2013 14.15 16.15pm Oncology Seminar Room, WGH with videolink to Dumfries Present Lorna Bruce Sarah Buchan Paul Fineron Martin Keith Christina Lilley Joyce Livingston
SCAN Colorectal Group Friday 9 th August 2013 14.15 16.15pm Oncology Seminar Room, WGH with videolink to Dumfries Present Lorna Bruce Sarah Buchan Paul Fineron Martin Keith Christina Lilley Joyce Livingston
LUNG CANCER 2010 COMPARATIVE AUDIT REPORT
 SOUTHEAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT LUNG CANCER 2010 COMPARATIVE AUDIT REPORT Dr Ron Fergusson, NHS Lothian SCAN Lead Lung Cancer Clinician Dr Jakki Faccenda, NHS Borders Dr Paul
SOUTHEAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT LUNG CANCER 2010 COMPARATIVE AUDIT REPORT Dr Ron Fergusson, NHS Lothian SCAN Lead Lung Cancer Clinician Dr Jakki Faccenda, NHS Borders Dr Paul
Bowel Cancer in England and Wales A summary report about the management and outcomes of people with bowel cancer
 Bowel Cancer in England and Wales A summary report about the management and outcomes of people with bowel cancer Based on findings from the National Bowel Cancer Audit Background How are patients diagnosed?
Bowel Cancer in England and Wales A summary report about the management and outcomes of people with bowel cancer Based on findings from the National Bowel Cancer Audit Background How are patients diagnosed?
OVARIAN CANCER 2011 COMPARATIVE AUDIT REPORT
 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT OVARIAN CANCER 2011 COMPARATIVE AUDIT REPORT Dr Melanie Mackean, NHS Lothian SCAN Lead Ovarian Cancer Clinician Dr Jane Macnab, NHS Fife Dr Scott
SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT OVARIAN CANCER 2011 COMPARATIVE AUDIT REPORT Dr Melanie Mackean, NHS Lothian SCAN Lead Ovarian Cancer Clinician Dr Jane Macnab, NHS Fife Dr Scott
SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT
 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT BREAST CANCER 2013 COMPARATIVE AUDIT REPORT Mr Glyn Neades Chair Breast Group and Consultant Surgeon, NHS Fife Mr Matthew Barber, Consultant
SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT BREAST CANCER 2013 COMPARATIVE AUDIT REPORT Mr Glyn Neades Chair Breast Group and Consultant Surgeon, NHS Fife Mr Matthew Barber, Consultant
SCAN Colorectal Group
 DRAFT SCAN Colorectal Group Friday 6 th December 2013 14.15 16.15pm Oncology Seminar Room, WGH with videolink to Victoria Hospital, Kirkcaldy. Present Ibrahim Amin Angie Balfour Sarah Buchan Paul Fineron
DRAFT SCAN Colorectal Group Friday 6 th December 2013 14.15 16.15pm Oncology Seminar Room, WGH with videolink to Victoria Hospital, Kirkcaldy. Present Ibrahim Amin Angie Balfour Sarah Buchan Paul Fineron
UROLOGICAL CANCER 2010 COMPARATIVE AUDIT REPORT
 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT UROLOGICAL CANCER 2010 COMPARATIVE AUDIT REPORT Dr Prasad Bollina, NHS Lothian SCAN Lead Urology Cancer Clinician Dr Prasad Bollina, NHS Lothian
SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT UROLOGICAL CANCER 2010 COMPARATIVE AUDIT REPORT Dr Prasad Bollina, NHS Lothian SCAN Lead Urology Cancer Clinician Dr Prasad Bollina, NHS Lothian
SOUTH EAST SCOTLAND CANCER NETWORK (SCAN) PROSPECTIVE CANCER AUDIT
 SOUTH EAST SCOTLAND CANCER NETWORK (SCAN) PROSPECTIVE CANCER AUDIT BREAST CANCER 2016 COMPARATIVE AUDIT REPORT Mr Glyn Neades Chair SCAN Breast Group and Consultant Surgeon, NHS Fife & NHS Lothian Mr Ahmed
SOUTH EAST SCOTLAND CANCER NETWORK (SCAN) PROSPECTIVE CANCER AUDIT BREAST CANCER 2016 COMPARATIVE AUDIT REPORT Mr Glyn Neades Chair SCAN Breast Group and Consultant Surgeon, NHS Fife & NHS Lothian Mr Ahmed
Audit Report. Report of the 2014 Clinical Audit Data. North, South East and West of Scotland Cancer Networks
 North, South East and West of Scotland Cancer Networks HepatoPancreatoBiliary Cancers National Managed Clinical Network Audit Report Report of the 2014 Clinical Audit Data Professor Stephen Wigmore Consultant
North, South East and West of Scotland Cancer Networks HepatoPancreatoBiliary Cancers National Managed Clinical Network Audit Report Report of the 2014 Clinical Audit Data Professor Stephen Wigmore Consultant
Activity Report April 2012 March 2013
 North, South East and West of Scotland Cancer Networks HepatoPancreatoBiliary Cancers National Managed Clinical Network Activity Report April 2012 March 2013 Mr Colin McKay Consultant Surgeon NMCN Clinical
North, South East and West of Scotland Cancer Networks HepatoPancreatoBiliary Cancers National Managed Clinical Network Activity Report April 2012 March 2013 Mr Colin McKay Consultant Surgeon NMCN Clinical
Ovarian Cancer Audit Comparative Annual Report 01/01/ /12/2009
 SE Scotland Cancer Network SCAN AUDIT Ovarian Cancer Audit Comparative Annual Report 01/01/2009 31/12/2009 S E Scotland Cancer Network (SCAN) (Excluding Dumfries and Galloway) NHS Borders NHS Fife NHS
SE Scotland Cancer Network SCAN AUDIT Ovarian Cancer Audit Comparative Annual Report 01/01/2009 31/12/2009 S E Scotland Cancer Network (SCAN) (Excluding Dumfries and Galloway) NHS Borders NHS Fife NHS
Activity Report April 2013 March 2014
 North, South East and West of Scotland Cancer Networks HepatoPancreatoBiliary Cancers National Managed Clinical Network Activity Report April 2013 March 2014 Mr Colin McKay Consultant Surgeon NMCN Clinical
North, South East and West of Scotland Cancer Networks HepatoPancreatoBiliary Cancers National Managed Clinical Network Activity Report April 2013 March 2014 Mr Colin McKay Consultant Surgeon NMCN Clinical
COLORECTAL CARCINOMA
 QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
Ovarian Cancer Quality Performance Indicators (QPI) Comparative Report
 SOUTH EAST SCOTLAND CANCER NETWORK (SCAN) PROSPECTIVE CANCER AUDIT Ovarian Cancer Quality Performance Indicators (QPI) Comparative Report Dr Cameron Martin, SCAN Lead Ovarian Cancer Clinician Dr Scott
SOUTH EAST SCOTLAND CANCER NETWORK (SCAN) PROSPECTIVE CANCER AUDIT Ovarian Cancer Quality Performance Indicators (QPI) Comparative Report Dr Cameron Martin, SCAN Lead Ovarian Cancer Clinician Dr Scott
UROLOGY CANCER 2009 COMPARATIVE AUDIT REPORT
 Urological Cancer Audit 2009 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT UROLOGY CANCER 2009 COMPARATIVE AUDIT REPORT Dr Prasad Bollina, NHS Lothian SCAN Lead Urology Cancer Clinician Dr
Urological Cancer Audit 2009 SOUTH EAST SCOTLAND CANCER NETWORK PROSPECTIVE CANCER AUDIT UROLOGY CANCER 2009 COMPARATIVE AUDIT REPORT Dr Prasad Bollina, NHS Lothian SCAN Lead Urology Cancer Clinician Dr
Activity Report April 2012 to March 2013
 North, South East and West of Scotland Cancer Networks Brain/Central Nervous System Tumours National Managed Clinical Network Activity Report April 2012 to March 2013 Professor Roy Rampling Emeritus Professor
North, South East and West of Scotland Cancer Networks Brain/Central Nervous System Tumours National Managed Clinical Network Activity Report April 2012 to March 2013 Professor Roy Rampling Emeritus Professor
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE
 COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
BOWEL CANCER. Causes of bowel cancer
 A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
RECTAL CANCER CLINICAL CASE PRESENTATION
 RECTAL CANCER CLINICAL CASE PRESENTATION Francesco Sclafani Medical Oncologist, Clinical Research Fellow The Royal Marsden NHS Foundation Trust, London, UK esmo.org Disclosure I have nothing to declare
RECTAL CANCER CLINICAL CASE PRESENTATION Francesco Sclafani Medical Oncologist, Clinical Research Fellow The Royal Marsden NHS Foundation Trust, London, UK esmo.org Disclosure I have nothing to declare
Audit Report Report of the 2015 Clinical Audit Data
 North, South East and West of Scotland Cancer Networks HepatoPancreatoBiliary Cancers National Managed Clinical Network Audit Report Report of the 2015 Clinical Audit Data Professor Stephen Wigmore Consultant
North, South East and West of Scotland Cancer Networks HepatoPancreatoBiliary Cancers National Managed Clinical Network Audit Report Report of the 2015 Clinical Audit Data Professor Stephen Wigmore Consultant
Lung Cancer Quality Performance Indicators
 Publication Report Lung Cancer Quality Performance Indicators Patients diagnosed during April 2013 to December 2015 Publication date 28 th February 2017 RESTRICTED STATISTICS Release embargoed until Tuesday
Publication Report Lung Cancer Quality Performance Indicators Patients diagnosed during April 2013 to December 2015 Publication date 28 th February 2017 RESTRICTED STATISTICS Release embargoed until Tuesday
Data Definitions for the National Minimum Core Dataset to support the Introduction of Colorectal Quality Performance Indicators
 Colorectal Cancer Data Definitions for the National Minimum Core Dataset to support the Introduction of Colorectal Quality Performance Indicators Definitions developed by ISD Scotland in collaboration
Colorectal Cancer Data Definitions for the National Minimum Core Dataset to support the Introduction of Colorectal Quality Performance Indicators Definitions developed by ISD Scotland in collaboration
SCAN Skin Group Friday 1 st November 2013
 SCAN Skin Group Friday 1 st November 2013 Dermatology Seminar Room, Lauriston Buildings with videolinks to Oncology Seminar Room, Western General Hospital and Borders General Hospital. MINUTES Present
SCAN Skin Group Friday 1 st November 2013 Dermatology Seminar Room, Lauriston Buildings with videolinks to Oncology Seminar Room, Western General Hospital and Borders General Hospital. MINUTES Present
Bowel Cancer Information Leaflet THE DIGESTIVE SYSTEM
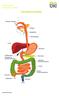 THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
SCAN Lung Group Wednesday 25 th September pm
 DRAFT SCAN Lung Group Wednesday 25 th September 2013 14.15 16.15pm Telepresence Suite, Western General Hospital, Edinburgh with videolinks to Borders and Dumfries Present Sandra Bagnall Mimica Bjelogrlic
DRAFT SCAN Lung Group Wednesday 25 th September 2013 14.15 16.15pm Telepresence Suite, Western General Hospital, Edinburgh with videolinks to Borders and Dumfries Present Sandra Bagnall Mimica Bjelogrlic
8. The polyp in the illustration can be described as (circle all that apply) a. Exophytic b. Pedunculated c. Sessile d. Frank
 Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
Testicular Cancer Quality Performance Indicators
 Testicular Cancer Quality Performance Indicators Patients diagnosed between October 2014 and September 2017 Publication date 28 August 2018 An Official Statistics publication for Scotland This is an Official
Testicular Cancer Quality Performance Indicators Patients diagnosed between October 2014 and September 2017 Publication date 28 August 2018 An Official Statistics publication for Scotland This is an Official
National Bowel Cancer Audit. Detection and management of outliers: Clinical Outcomes Publication
 National Bowel Cancer Audit Detection and management of outliers: Clinical Outcomes Publication November 2017 1 National Bowel Cancer Audit (NBOCA) Detection and management of outliers Clinical Outcomes
National Bowel Cancer Audit Detection and management of outliers: Clinical Outcomes Publication November 2017 1 National Bowel Cancer Audit (NBOCA) Detection and management of outliers Clinical Outcomes
Activity Report April 2012 March 2013
 Colorectal Cancer Managed Clinical Network Activity Report April 2012 March 2013 Paul Horgan Professor of Surgery MCN Clinical Lead Kevin Campbell Network Manager 1 CONTENTS EXECUTIVE SUMMARY 3 1. INTRODUCTION
Colorectal Cancer Managed Clinical Network Activity Report April 2012 March 2013 Paul Horgan Professor of Surgery MCN Clinical Lead Kevin Campbell Network Manager 1 CONTENTS EXECUTIVE SUMMARY 3 1. INTRODUCTION
ADJUVANT CHEMOTHERAPY...
 Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
Report prepared on behalf of the Scottish Head and Neck Cancer Networks by the WoSCAN Information Team
 Scottish Head and Neck Cancer Networks Report of the 2011 Clinical Audit Data Presented at the National Head and Neck Cancer Education Day 26th October 2012 Report prepared on behalf of the Scottish Head
Scottish Head and Neck Cancer Networks Report of the 2011 Clinical Audit Data Presented at the National Head and Neck Cancer Education Day 26th October 2012 Report prepared on behalf of the Scottish Head
Activity Report April 2013 March 2014
 North, South East and West of Scotland Cancer Networks Sarcoma National Managed Clinical Network Activity Report April 2013 March 2014 Dr Jeff White Consultant Oncologist NMCN Clinical Lead Lindsay Campbell
North, South East and West of Scotland Cancer Networks Sarcoma National Managed Clinical Network Activity Report April 2013 March 2014 Dr Jeff White Consultant Oncologist NMCN Clinical Lead Lindsay Campbell
RECTAL CANCER APPARENT COMPLETE RESPONSE (acr) AFTER LONG COURSE CHEMORADIOTHERAPY
 COLORECTAL CLINICAL SUBGROUP RECTAL CANCER APPARENT COMPLETE RESPONSE (acr) AFTER LONG COURSE CHEMORADIOTHERAPY Finalised by: Dr Simon Gollins Mr Andrew Renehan Dr Mark Saunders Mr Nigel Scott Dr Shabbir
COLORECTAL CLINICAL SUBGROUP RECTAL CANCER APPARENT COMPLETE RESPONSE (acr) AFTER LONG COURSE CHEMORADIOTHERAPY Finalised by: Dr Simon Gollins Mr Andrew Renehan Dr Mark Saunders Mr Nigel Scott Dr Shabbir
Advice Statement. Advice Statement November Advice for NHSScotland. Why is SHTG looking at this topic?
 Advice Statement 014-18 November 2018 Advice Statement Colon capsule endoscopy (CCE-2) for the detection of colorectal polyps and cancer in adults with signs or symptoms of colorectal cancer or at increased
Advice Statement 014-18 November 2018 Advice Statement Colon capsule endoscopy (CCE-2) for the detection of colorectal polyps and cancer in adults with signs or symptoms of colorectal cancer or at increased
Audit Report. Breast Cancer Quality Performance Indicators. Patients diagnosed during Published: February 2018
 Breast Cancer Managed Clinical Network Audit Report Breast Cancer Quality Performance Indicators Patients diagnosed during 2016 Published: February 2018 Mr Douglas Brown NOSCAN Breast Cancer MCN Clinical
Breast Cancer Managed Clinical Network Audit Report Breast Cancer Quality Performance Indicators Patients diagnosed during 2016 Published: February 2018 Mr Douglas Brown NOSCAN Breast Cancer MCN Clinical
Annual Report. Public Health Screening Programmes TO 31 MARCH Extract: Chapter 3 : Planning for Bowel Screening Programme
 Public Health Screening Programmes Annual Report TO 31 MARCH 2007 Extract: Chapter 3 : Planning for Bowel Screening Programme Version 1.0 Published: 18 December 2007 1 Contents INTRODUCTION...3 SUMMARY...5
Public Health Screening Programmes Annual Report TO 31 MARCH 2007 Extract: Chapter 3 : Planning for Bowel Screening Programme Version 1.0 Published: 18 December 2007 1 Contents INTRODUCTION...3 SUMMARY...5
Audit Report. Cervical Cancer Quality Performance Indicators. Patients diagnosed October 2014 September Published: September 2016
 Gynaecology Managed Clinical Network NORTH OF SCOTLAND PLANNING GROUP Audit Report Cervical Cancer Quality Performance Indicators Patients diagnosed October 2014 September 2015 Published: September 2016
Gynaecology Managed Clinical Network NORTH OF SCOTLAND PLANNING GROUP Audit Report Cervical Cancer Quality Performance Indicators Patients diagnosed October 2014 September 2015 Published: September 2016
Clinical guideline Published: 1 November 2011 nice.org.uk/guidance/cg131
 Colorectal cancer: diagnosis and management Clinical guideline Published: 1 November 2011 nice.org.uk/guidance/cg131 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Colorectal cancer: diagnosis and management Clinical guideline Published: 1 November 2011 nice.org.uk/guidance/cg131 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Audit Report. Lung Cancer Quality Performance Indicators. Patients diagnosed January December Published: November 2017
 Lung Cancer Managed Clinical Network Audit Report Lung Cancer Quality Performance Indicators Patients diagnosed January December 2016 Published: November 2017 Hardy Remmen NOSCAN Lung Cancer MCN Clinical
Lung Cancer Managed Clinical Network Audit Report Lung Cancer Quality Performance Indicators Patients diagnosed January December 2016 Published: November 2017 Hardy Remmen NOSCAN Lung Cancer MCN Clinical
This is the portion of the intestine which lies between the small intestine and the outlet (Anus).
 THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
abcdefghijklmnopqrstu
 CMO and Public Health Directorate Health Improvement Strategy Division Dear Colleague Scottish Abdominal Aortic Aneurysm Screening Programme This CEL outlines the plan for the implementation of the AAA
CMO and Public Health Directorate Health Improvement Strategy Division Dear Colleague Scottish Abdominal Aortic Aneurysm Screening Programme This CEL outlines the plan for the implementation of the AAA
SCAN Haematology Group Wednesday 23 rd May 2012 Telepresence Room, Western General Hospital, Edinburgh with videolinks to Borders, VHK and St John s
 DRAFT SCAN Haematology Group Wednesday 23 rd May 2012 Telepresence Room, Western General Hospital, Edinburgh with videolinks to Borders, VHK and St John s MINUTES Present Sandra Bagnall Liz Brown Mira
DRAFT SCAN Haematology Group Wednesday 23 rd May 2012 Telepresence Room, Western General Hospital, Edinburgh with videolinks to Borders, VHK and St John s MINUTES Present Sandra Bagnall Liz Brown Mira
National Breast Cancer Audit next steps. Martin Lee
 National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
Bowel cancer. In this fact sheet: Page 1 of 13 Macmillan fact sheet 2017: Bowel cancer. Bowel Cancer: English
 Bowel Cancer: English Bowel cancer This information is about bowel cancer and treatments for bowel cancer. Any words that are underlined are explained in the word list at the end. If you have any questions,
Bowel Cancer: English Bowel cancer This information is about bowel cancer and treatments for bowel cancer. Any words that are underlined are explained in the word list at the end. If you have any questions,
Audit Report Lymphoma Quality Performance Indicators
 West of Scotland Cancer Network Haemato-oncology Managed Clinical Network Audit Report Lymphoma Quality Performance Indicators Clinical Audit Data: 01 October 2016 to 30 September 2017 Dr Grant McQuaker
West of Scotland Cancer Network Haemato-oncology Managed Clinical Network Audit Report Lymphoma Quality Performance Indicators Clinical Audit Data: 01 October 2016 to 30 September 2017 Dr Grant McQuaker
NOVA SCOTIA RECTAL CANCER PROJECT: A POPULATION-BASED ASSESSMENT OF RECTAL CANCER CARE AND OUTCOMES. Devon Paula Richardson
 NOVA SCOTIA RECTAL CANCER PROJECT: A POPULATION-BASED ASSESSMENT OF RECTAL CANCER CARE AND OUTCOMES by Devon Paula Richardson Submitted in partial fulfilment of the requirements for the degree of Master
NOVA SCOTIA RECTAL CANCER PROJECT: A POPULATION-BASED ASSESSMENT OF RECTAL CANCER CARE AND OUTCOMES by Devon Paula Richardson Submitted in partial fulfilment of the requirements for the degree of Master
Faster Cancer Treatment Indicators: Use cases
 Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
Colorectal Pathway Board (Clinical Subgroup): Imaging Guidelines September 2015
 Colorectal Pathway Board (Clinical Subgroup): Imaging Guidelines September 2015 1 Contents Page No. 1. Objective 3 2. Imaging Techniques 3 3. Staging of Colorectal Cancer 5 4. Radiological Reporting 6
Colorectal Pathway Board (Clinical Subgroup): Imaging Guidelines September 2015 1 Contents Page No. 1. Objective 3 2. Imaging Techniques 3 3. Staging of Colorectal Cancer 5 4. Radiological Reporting 6
National Bowel Cancer Audit Supplementary Report 2011
 National Bowel Cancer Audit Supplementary Report 2011 This Supplementary Report contains data from the 2009/2010 reporting period which covers patients in England with a diagnosis date from 1 August 2009
National Bowel Cancer Audit Supplementary Report 2011 This Supplementary Report contains data from the 2009/2010 reporting period which covers patients in England with a diagnosis date from 1 August 2009
SCAN Skin Group Friday 24 th February 2012
 DRAFT SCAN Skin Group Friday 24 th February 2012 Dermatology Seminar Room, Lauriston Building with videolink to Borders General Hospital MINUTES Present Alex Holme Daniel Kemmett Chair Simone Laube Kate
DRAFT SCAN Skin Group Friday 24 th February 2012 Dermatology Seminar Room, Lauriston Building with videolink to Borders General Hospital MINUTES Present Alex Holme Daniel Kemmett Chair Simone Laube Kate
Audit Report. Lung Cancer Quality Performance Indicators. Patients diagnosed April 2014 March Published: May 2016
 NORTH OF SCOTLAND PLANNING GROUP Lung Cancer Managed Clinical Network Audit Report Lung Cancer Quality Performance Indicators Patients diagnosed April 2014 March 2015 Published: May 2016 Mr Hardy Remmen
NORTH OF SCOTLAND PLANNING GROUP Lung Cancer Managed Clinical Network Audit Report Lung Cancer Quality Performance Indicators Patients diagnosed April 2014 March 2015 Published: May 2016 Mr Hardy Remmen
Audit Report. Brain and CNS Cancer Quality Performance Indicators. Report of the 2014 Clinical Audit Data
 North, South East and West of Scotland Cancer Networks Neuro-Oncology Cancers Audit Report Brain and CNS Cancer Quality Performance Indicators Report of the 2014 Clinical Audit Data Dr Avinash Kanodia
North, South East and West of Scotland Cancer Networks Neuro-Oncology Cancers Audit Report Brain and CNS Cancer Quality Performance Indicators Report of the 2014 Clinical Audit Data Dr Avinash Kanodia
SCAN Lung Group Friday 16 th November pm
 SCAN Lung Group Friday 16 th November 2012 14.15 16.15pm Oncology Seminar Room, Western General Hospital, Edinburgh with videolink to Dumfries MINUTES Present Diana Borthwick Martin Keith Kate Macdonald
SCAN Lung Group Friday 16 th November 2012 14.15 16.15pm Oncology Seminar Room, Western General Hospital, Edinburgh with videolink to Dumfries MINUTES Present Diana Borthwick Martin Keith Kate Macdonald
Clinical Advice for the Commissioning of the Whole Bowel Cancer Pathway
 Clinical Advice for the Commissioning of the Whole Bowel Cancer Pathway This document was produced by the Colorectal Cancer Clinical Expert Group November 2017 Clinical Advice to Cancer Alliances for the
Clinical Advice for the Commissioning of the Whole Bowel Cancer Pathway This document was produced by the Colorectal Cancer Clinical Expert Group November 2017 Clinical Advice to Cancer Alliances for the
Audit Report. Upper GI Cancer Quality Performance Indicators. Report of the 2016 Clinical Audit Data. West of Scotland Cancer Network
 Upper Gastro-intestinal Cancer Managed Clinical Network Audit Report Upper GI Cancer Quality Performance Indicators Report of the 216 Clinical Audit Data Mr Matthew Forshaw MCN Clinical Lead Tracey Cole
Upper Gastro-intestinal Cancer Managed Clinical Network Audit Report Upper GI Cancer Quality Performance Indicators Report of the 216 Clinical Audit Data Mr Matthew Forshaw MCN Clinical Lead Tracey Cole
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician ASWCN TAUNTON AND SOMERSET Taunton Lung MDT (11-2C-1) - 2011/12 Dr Sarah Foster Compliance Self Assessment LUNG MDT
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician ASWCN TAUNTON AND SOMERSET Taunton Lung MDT (11-2C-1) - 2011/12 Dr Sarah Foster Compliance Self Assessment LUNG MDT
Bladder Cancer Guidelines
 Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
SCAN Head & Neck Group Friday 18 th January 2013 Oncology Seminar Room, Western General Hospital, Edinburgh
 SCAN Head & Neck Group Friday 18 th January 2013 Oncology Seminar Room, Western General Hospital, Edinburgh Present Sandra Bagnall Marlene Brown Karen Gordon Clare Gorman Nadine Hare Fiona Haston Lesley
SCAN Head & Neck Group Friday 18 th January 2013 Oncology Seminar Room, Western General Hospital, Edinburgh Present Sandra Bagnall Marlene Brown Karen Gordon Clare Gorman Nadine Hare Fiona Haston Lesley
IMAGING GUIDELINES - COLORECTAL CANCER
 IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
Audit Report Report of the 2010 Clinical Audit Data
 Gynaecological Cancer Managed Clinical Network Audit Report Report of the Clinical Audit Data Nick Reed Consultant Clinical Oncologist MCN Clinical Lead (Joint) Nadeem Siddiqui Consultant Gynaecological
Gynaecological Cancer Managed Clinical Network Audit Report Report of the Clinical Audit Data Nick Reed Consultant Clinical Oncologist MCN Clinical Lead (Joint) Nadeem Siddiqui Consultant Gynaecological
Annual Report April 2016 March 2017
 North, South East and West of Scotland Cancer Networks HepatoPancreatoBiliary Cancers National Managed Clinical Network Annual Report April 2016 March 2017 Professor Stephen Wigmore Consultant Surgeon
North, South East and West of Scotland Cancer Networks HepatoPancreatoBiliary Cancers National Managed Clinical Network Annual Report April 2016 March 2017 Professor Stephen Wigmore Consultant Surgeon
Rectal Cancer. GI Practice Guideline
 Rectal Cancer GI Practice Guideline Dr. Brian Dingle MSc, MD, FRCPC Dr. Francisco Perera MD, FRCPC (Radiation Oncologist) Dr. Jay Engel MD, FRCPC (Surgical Oncologist) Approval Date: 2006 This guideline
Rectal Cancer GI Practice Guideline Dr. Brian Dingle MSc, MD, FRCPC Dr. Francisco Perera MD, FRCPC (Radiation Oncologist) Dr. Jay Engel MD, FRCPC (Surgical Oncologist) Approval Date: 2006 This guideline
Bowel Cancer Quality Improvement Report
 Bowel Cancer Quality Improvement Report 2019 Released 2019 health.govt.nz This report publishes quality performance indicator data from patients diagnosed with colorectal cancer in New Zealand between
Bowel Cancer Quality Improvement Report 2019 Released 2019 health.govt.nz This report publishes quality performance indicator data from patients diagnosed with colorectal cancer in New Zealand between
COLON AND RECTAL CANCER
 COLON AND RECTAL CANCER Mark Sun, MD Clinical Associate Professor of Surgery University of Minnesota No disclosures Objectives 1) Understand the epidemiology, management, and prognosis of colon and rectal
COLON AND RECTAL CANCER Mark Sun, MD Clinical Associate Professor of Surgery University of Minnesota No disclosures Objectives 1) Understand the epidemiology, management, and prognosis of colon and rectal
Colorectal Pathway Meeting minutes Wednesday 16 th July 2014, 2 pm 4 pm Nightingale Lecture Theatre, UHSM
 Colorectal Pathway Meeting minutes Wednesday 16 th July 2014, 2 pm 4 pm Nightingale Lecture Theatre, UHSM Attendance: Sarah Duff Edwin Clark Sophie Harrison Caroline Whitaker Sarah Taylor Debbie West Mark
Colorectal Pathway Meeting minutes Wednesday 16 th July 2014, 2 pm 4 pm Nightingale Lecture Theatre, UHSM Attendance: Sarah Duff Edwin Clark Sophie Harrison Caroline Whitaker Sarah Taylor Debbie West Mark
LCA Lung Clinical Forum. 21 st October 2014
 LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
WELSH INFORMATION GOVERNANCE & STANDARDS BOARD
 WELSH INFORMATION GOVERNANCE & STANDARDS BOARD CDSC Notice: CDSCN 2011 / 02 Date of Issue: 31 st March 2011 Ministerial / Official Letter: EH/ML/015/11 Sponsor: Head of Major Health Conditions and Clinical
WELSH INFORMATION GOVERNANCE & STANDARDS BOARD CDSC Notice: CDSCN 2011 / 02 Date of Issue: 31 st March 2011 Ministerial / Official Letter: EH/ML/015/11 Sponsor: Head of Major Health Conditions and Clinical
OFCCR CLINICAL DIAGNOSIS AND TREATMENT FORM
 OFCCR CLINICAL DIAGNOSIS AND TREATMENT FORM Name: _, OFCCR # _ OCGN # _ OCR Group # _ HIN# Sex: MALE FEMALE UNKNOWN Date of Birth: DD MMM YYYY BASELINE DIAGNOSIS & TREATMENT 1. Place of Diagnosis: Name
OFCCR CLINICAL DIAGNOSIS AND TREATMENT FORM Name: _, OFCCR # _ OCGN # _ OCR Group # _ HIN# Sex: MALE FEMALE UNKNOWN Date of Birth: DD MMM YYYY BASELINE DIAGNOSIS & TREATMENT 1. Place of Diagnosis: Name
OVARIAN CANCER ANNUAL REPORT
 ITEM 6.2 South East Scotland Cancer Network OVARIAN CANCER ANNUAL REPORT Data collected: 1 ST JANUARY TO 31 ST DECEMBER 2011 Dr K S Fegan Consultant Gynaecological Oncologist Victoria Hospital Kirkcaldy
ITEM 6.2 South East Scotland Cancer Network OVARIAN CANCER ANNUAL REPORT Data collected: 1 ST JANUARY TO 31 ST DECEMBER 2011 Dr K S Fegan Consultant Gynaecological Oncologist Victoria Hospital Kirkcaldy
National Cancer Peer Review Sarcoma. Julia Hill Acting Deputy National Co-ordinator
 National Cancer Peer Review Sarcoma Julia Hill Acting Deputy National Co-ordinator Improving Outcomes Guidance The Intentions of Improving Outcomes for People with Sarcoma Changes in the provision of care
National Cancer Peer Review Sarcoma Julia Hill Acting Deputy National Co-ordinator Improving Outcomes Guidance The Intentions of Improving Outcomes for People with Sarcoma Changes in the provision of care
A Best Practice Clinical Care Pathway for Major Amputation Surgery
 A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
Yorkshire Cancer Research Yorkshire Bowel Cancer initiative
 Yorkshire Cancer Research Yorkshire Bowel Cancer initiative Phil Quirke, Eva Morris, Paul Finan, Nick West, Penny Wright, David Sebag- Montefiore, Matt Seymour University of Leeds What s the problem? %
Yorkshire Cancer Research Yorkshire Bowel Cancer initiative Phil Quirke, Eva Morris, Paul Finan, Nick West, Penny Wright, David Sebag- Montefiore, Matt Seymour University of Leeds What s the problem? %
COLON AND RECTAL CANCER
 No disclosures COLON AND RECTAL CANCER Mark Sun, MD Clinical Assistant Professor of Surgery University of Minnesota Colon and Rectal Cancer Statistics Overall Incidence 2016 134,490 new cases 8.0% of all
No disclosures COLON AND RECTAL CANCER Mark Sun, MD Clinical Assistant Professor of Surgery University of Minnesota Colon and Rectal Cancer Statistics Overall Incidence 2016 134,490 new cases 8.0% of all
Follow up The way ahead. John Griffith
 Follow up The way ahead John Griffith Key Emerging Principles Risk stratified pathways of care Personalised care plan and treatment summary with a hand held record Information and education Remote monitoring
Follow up The way ahead John Griffith Key Emerging Principles Risk stratified pathways of care Personalised care plan and treatment summary with a hand held record Information and education Remote monitoring
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels.
 Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Audit Report Report of the 2012 Clinical Audit Data
 Gynaecological Cancer Managed Clinical Network Audit Report Report of the 2012 Clinical Audit Data Nadeem Siddiqui Consultant Gynaecological Oncologist MCN Clinical Lead Kevin Campbell MCN Manager Julie
Gynaecological Cancer Managed Clinical Network Audit Report Report of the 2012 Clinical Audit Data Nadeem Siddiqui Consultant Gynaecological Oncologist MCN Clinical Lead Kevin Campbell MCN Manager Julie
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL RECTAL CANCER GI Site Group Rectal Cancer Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION 3 2. SCREENING AND
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL RECTAL CANCER GI Site Group Rectal Cancer Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION 3 2. SCREENING AND
Large bowel cancer. Large bowel cancer: English
 Large bowel cancer: English Large bowel cancer This fact sheet is about how cancer of the large bowel is diagnosed and treated. We also have fact sheets in your language about chemotherapy, radiotherapy,
Large bowel cancer: English Large bowel cancer This fact sheet is about how cancer of the large bowel is diagnosed and treated. We also have fact sheets in your language about chemotherapy, radiotherapy,
Colorectal Cancer Care
 Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. ROUND2.3_CRCa_20pages_5.5x8.5_FINAL.indd
Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. ROUND2.3_CRCa_20pages_5.5x8.5_FINAL.indd
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012
 Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
