Frequency of additional clonal populations detected by high sensitivity flow cytometry in patients with hairy cell leukemia
|
|
|
- Philippa Ray
- 5 years ago
- Views:
Transcription
1 J Hematopathol (2012) 5: DOI /s ORIGINAL ARTICLE Frequency of additional clonal populations detected by high sensitivity flow cytometry in patients with hairy cell leukemia Mikhail Roshal & Sindhu Cherian Received: 9 September 2011 / Accepted: 17 January 2012 / Published online: 16 February 2012 # Springer-Verlag 2012 Abstract Samples from 115 patients with hairy cell leukemia (HCL) were analyzed by high sensitivity flow cytometry for evidence of an additional B cell or plasma cell clone. We found that 10.4% of HCL patients harbored an additional clonal population in either peripheral blood or bone marrow. Among the patients with additional clones, 58% had the second population present at the time of HCL diagnosis and 42% developed the second clone in a subsequent sample. Half of the clonal populations identified represented true disease entities rather than a monoclonal B lymphocytosis (MBL) or monoclonal gammopathy of undetermined significance (MGUS). The frequency of MBL and MGUS was similar to that reported in the general population, but the frequency of B cell-derived malignancies appears increased in the HCL cohort. Compared to patients without additional clones, the patients with second clones were older (median age 66 vs. 55 years old). Patients over age 60 were at higher risk for a second clone (18.2% vs. 5.6%, OR 3.7, P<0.05). Among the patients with a second clone, 75% had second B cell clone, 42% had a plasma cell clone, and 17% had both. We have also identified a clear case of bi-clonal HCL; a finding not previously M. Roshal Department of Pathology and Laboratory Medicine, Weill Cornell Medical College, New York, NY, USA S. Cherian Department of Laboratory Medicine, University of Washington, Seattle, WA, USA S. Cherian (*) Seattle Cancer Care Alliance Mail Stop G7-800, 825 Eastlake Ave. E, Seattle, WA 98109, USA cherians@uw.edu reported using contemporary diagnostic criteria. We conclude that second clonal expansions are relatively common in patients with HCL, in particular in older patients, and may represent clinically significant neoplasms. Keywords Hairy cell leukemia. Flow cytometry. B cell lymphoma. Plasma cell neoplasm Introduction Hairy cell leukemia (HCL) is a rare blood-, bone marrow-, and spleen-based lymphoproliferative disorder of mature B cells. The neoplastic population can be readily identified immunophenotypically by the expression of CD11c, CD25, and CD103 [1, 2]. Detection of the expression of these antigens on an expanded, clonal B cell population is diagnostic for this disorder. Additionally, the IL3 receptor (CD123) has been proposed as a useful marker for HCL [3]. The origin of the neoplastic cell in hairy cell leukemia is not entirely clear, but the near universal absence of expression of the activation marker CD38, germinal center marker Bcl- 6, and germinal center-derived memory cell marker CD27 [4] argue against a germinal center derivation of these cells, despite a not-infrequent expression of CD10 [5, 6]. Patients with HCL are at increased risk for subsequent non-hematopoietic and hematopoietic neoplasms [7 12]. Reasons for the increase are not entirely clear. Immunosuppressive therapy for treatment of HCL, immunosuppressive effect of HCL itself, and/or intrinsic cancer susceptibility of patients with HCL may all play a role. Aside from the aforementioned epidemiologic studies, reports of second hematologic malignancies in patients with HCL are mostly contained in case reports and series containing very few HCL patients [13 16]. Thus, the true
2 124 J Hematopathol (2012) 5: incidence of second clonal expansions in HCL is not established. The largest study to date contained 13 HCL and HCL variant (HCL-v) cases from both unselected patient samples and selected patient samples referred to the reference flow cytometry laboratory for confirmation of a second clone. That study demonstrated a second clonal expansion in 4 out the 13 patients. This finding suggested a possible increased incidence of second clones in HCL, although the study design precluded a definite conclusion [17]. We build on these observations in a much larger study specifically focused on an unselected cohort of HCL patients. In a retrospective analysis, we have identified 115 individual patients with HCL that had definitive immunophenotypic findings characteristic of HCL (positivity for CD25, CD11c, and CD103 on a clonal mature B cell population) over a 5-year period in a single large academic institution. The frequency of additional clonal hematopoietic proliferations and their immunophenotypic and clinical characteristics are described. In addition, we detected an unequivocal case of bi-clonal HCL that was confirmed by molecular studies. This, to our knowledge, is the second report of such a case and the first that uses modern diagnostic criteria of HCL. A prior case report of a single patient was published in 1986, and it is not entirely clear whether the patient s diagnosis in that report would meet the modern diagnostic criteria for HCL as it was based on a relatively limited immunophenotyping that would not distinguish HCL from HCL-v [18]. Finally, we took advantage of the large number of cases to further characterize additional immunophenotypic characteristics of HCL. Materials and methods Cases selection criteria This study was approved by the institutional review board at the University of Washington. All immunophenotyping studies were performed at the University of Washington flow cytometry laboratory in the course of routine clinical work. Cases were selected based on the flow cytometric detection of HCL between January 2004 and December In order to qualify for the study, HCL populations needed to demonstrate monoclonal expression of light chains with bright or moderate co-expression of CD11c, CD25, and CD103. Whenever indicated, clinical and morphologic correlation was performed to confirm the diagnosis. Cases that lacked expression of any of the antigens classically associated with HCL were excluded from further analysis to avoid contamination of the data set with HCL-v and other B cell lymphoproliferative disorders. The cases with a second clone were re-reviewed by two hematopathologists (SC and MR) in order to assure uniform flow cytometric detection of bi-clonal populations and second B cell or plasma cell clones. Only cases where both reviewers agreed about the unequivocal presence of the second clonal population were included. Clinical and pathologic data for cases with a second clone were then reviewed to determine if the second clone met the 2008 WHO criteria [1] foratrue distinct disease entity (B cell lymphoma or plasma cell myeloma) as opposed to monoclonal B lymphocytosis (MBL) or monoclonal gammopathy of undetermined significance (MGUS). Immunophenotyping Blood and bone marrow samples were processed using a standard NH 4 Cl whole blood lysing technique. Briefly, μl of whole blood or bone marrow containing up to 10 6 cells were incubated with 100 μl of a titered reagent cocktail (see below) and incubated at room temperature in the dark for 15 min. About 1.5 ml of buffered NH 4 Cl containing 0.25% ultrapure formaldehyde (Polysciences) was added and incubated in the dark at room temperature for 15 min followed by a single wash with phosphate-buffered saline containing 0.3% bovine serum albumin. Cells (100, ,000) were analyzed using two to four 8 10 color diagnostic panels followed by a confirmatory five-color HCL panel. Initial diagnostic workup of bone marrow and peripheral blood samples included a B cell tube, and in some cases, T cell and myeloid tubes. Confirmation of the HCL population was performed using the described HCL tube. A plasma cell tube was added if there was an indication of an abnormal plasma cell population in the initial workup or if there was a clinical suspicion of a monoclonal plasma cell disorder. All antibody reagents were obtained from either Beckman Coulter (Fullerton, CA) or Becton Dickinson (BD) (San Jose, CA). Antibody combinations used for flow cytometric detection of abnormal populations are listed in Table 1. Cell sorting Cell sorting was used to separate kappa- and lambda-restricted hairy cell populations in the bi-clonal HCL case. Cells were processed as described under immunophenotyping.kappaand lambda-restricted populations were individually sorted using flow cytometric sorting on a FACS-ARIA instrument from BD. Cell sorting was performed using the same staining and fixation method as for flow cytometric analysis using kappa-fitc, lambda-pe, and CD19-ECD. Molecular analysis Molecular analysis on the individually sorted kappa- and lambda-expressing populations as well as unsorted peripheral
3 J Hematopathol (2012) 5: Table 1 Antibody combinations Panel/fluorochrome Pacific blue FITC PE ECD PC5 PC7 A594 APC APC-A700 APC-CY7 B cells CD45 Kappa Lambda CD19 CD20 CD38 CD10 CD5 T cells CD45 CD2 CD7 CD34 CD8 CD3 CD4 CD56 CD5 Myeloid 1 HLA-DR CD15 CD33 CD19 CD117 CD13 CD38 CD34 CD71 CD45 Myeloid 2 HLA-DR CD64 CD123 CD4 CD14 CD13 CD38 CD34 CD16 CD45 HCL CD103 CD25 CD19 CD11c Plasma cells DAPI ckappa clambda CD19 CD45 CD38 CD56 blood from the patient with bi-clonal HCL was performed as described below. DNA was prepared using the Puregene kit (Gentra Systems) according to the method of the manufacturer. The DNA segment of interest was amplified by PCR using Biomed-2 framework one to three fluorescently labeled primer sets [19]. The products were then size-fractionated by capillary electrophoresis using Applied Biosystems 3130 Sequence Analyzer. Negative and positive controls were included in each assay. Results Characteristics of the study group and HCL immunophenotype We identified 115 patient samples with a first time flow cytometric diagnosis of HCL at the University of Washington Hematopathology Flow Cytometry Laboratory. Some patients had been diagnosed with HCL prior to presentation at our institution. HCL diagnosis was based on the identification of a clonal B cell population with bright or moderate expression of CD11c, CD25, and CD103. Overall patient characteristics are summarized in Table 2. As expected from previously published reports [20, 21], the disease demonstrated a marked male predominance (M/F ratio >4) and affected mostly middle age to older individuals (median age 56). Approximately 20% of HCL cases demonstrated Table 2 Demographic and immunophenotypic characteristics of patients with HCL Without additional clones With additional clones Male Female 21 1 M/F ratio 4.3:1 11:1 Mean age 55 (27 95) 66 (47 85) %CD (22/103) 8.3 (1/12) %CD (27/27) 100 (2/2) aberrant expression of CD10 on at least 10% of abnormal population (expression ranged from uniform to variable). All 29 cases in which CD123 expression was analyzed demonstrated uniform expression of CD123 on the abnormal HCL population. Immunophenotypic and clinical characterization of second clonal expansions Twelve of the 115 cases showed flow cytometric evidence of a second clonal population. Compared to patients with HCL alone, the group with a second clone was significantly older [median age 66 (47 85) vs. 55 (27 95), p<0.05]. Overall, patients 60 years and older demonstrated a significantly increased risk for a second clone [18.2% vs. 5.6%, odds ratio 3.7 ( ), p<0.05]. No significant differences were found in sex or immunophenotype (specifically the likelihood of expression of CD10 or CD123) when comparing HCL cases with and without a second clonal population. These finding are summarized in Table 2. The second clone detected by flow cytometry in this study represented either a second B cell clone or a plasma cell population. The majority of patients with a second clone (8 of 12) had a second clonal B cell population while the remainder had evidence of a plasma cell clone. Of note, two patients had a second B cell clone and second plasma cell clone detected. Notably, half of the second clonal expansions identified represented a true disease entity rather than an MBL or MGUS. A summary of the flow cytometric data is presented in Table 3. Two patients had multiple myeloma. In patient 1, myeloma was detected at the time of HCL diagnosis with morphology showing greater than 30% plasma cells in the marrow, and in patient 8, plasma cell leukemia was diagnosed post-hcl therapy with greater than 20% plasma cells noted in the peripheral blood. Patient 10 developed chronic lymphocytic leukemia (CLL) and patient 9 developed mantle cell lymphoma. Patient 4 had an abnormal population with a CLL-like immunophenotype representing 18.5% of the white blood cells in the marrow and had a concurrent FISH studies demonstrating trisomy 12. Although this
4 126 J Hematopathol (2012) 5: Table 3 Immunophenotype and clinical characterization of additional clones in HCL patients Age HCL light chain/ clone size by FC Additional B cell clone Site Immunophenotype of additional population/% of WBC Second clone detected at presentation 1 47/M Kappa/4.9% MM BM CD19 (absent), CD45 (absent), CD56 (subset), and cytoplasmic kappa light chain restriction with normal expression of CD38/3.0% 2 52/M Kappa/1.3% MGUS BM CD19 (absent), monoclonal kappa cytoplasmic light chain restriction with variable CD45, low CD20, and absent CD56/0.3% 3 79/F Lambda/3.3% MZL/LPL, MBL, possible MGUS BM (1) CD25 and kappa light chain restriction with normal expression of CD45, CD19, and CD20 without CD5, CD10, CD11c, CD103, or FMC-7 (MZL/LPL)/10%; (2) CD5, CD20 (low), CD23, and absent to low level lambda light chain expression with normal expression of CD45 and CD19 without FMC7 or CD10 (MBL) /0.3%; (3) CD19 (variable, subset absent), CD45 (subset decreased), CD56 (subset), and monoclonal kappa cytoplasmic light chain restriction with normal expression of CD38 and CD138 (MGUS)/0.65% 4 75/M Lambda/11.7% MBL BM CD45, CD19, and CD20, co-expression of CD5, CD38, low FMC7, and low CD25 with dim kappa light chain restriction without CD10, CD103, or CD23 (FISH demonstrated trisomy 12)/18.5% 5 57/M Kappa/28.6% MBL BM CD5, CD20 (low), CD23 (low to absent), and kappa surface light chain restriction (low) and normal expression of CD45 and CD19 without FMC7/0.7% 6 67/M Lambda/15.3% MBL BM CD5, CD20, and absent to low kappa surface light chain restriction with normal expression of CD45 and CD19 without significant CD10 or CD38/5.3% 7 76/M Kappa/76.0% MBL PB CD5, CD20 (low), CD23, and bi-clonal surface light chain restriction (low kappa predominant) and normal expression of CD45 and CD19 without FMC7 or CD10/0.5% Second clone detected at follow-up 8 71/M Lambda/0.005% MM/plasma cell leukemia 9 85/M Kappa/0.3% Mantle cell lymphoma PB BM CD19 (absent), CD38 (low), CD45 (variable low), CD56, and monoclonal kappa cytoplasmic light chain restriction/20% CD45, CD5, CD19, CD20, low CD38, and lambda light chain restriction without CD10 or CD23 (FISH demonstrated a CCND1 translocation)/25.3% 10 68/M Lambda/0.2% CLL PB CD5, CD20 (low), CD23, and kappa surface light chain restriction (low) and normal expression of CD45 and CD19 without FMC7 or CD10/60% 11 62/M Lambda/10.5% Initially thought to represent a plasma cell neoplasm not further classified; subsequent LN biopsy showed DLBCL with plasmacytic differentiation BM Abnormal monoclonal kappa cytoplasmic light chain restriction with normal expression of CD19, CD45, and CD38 without CD56/5.4%. This was initially thought to represent a PCN; however, a subsequent lymph node biopsy demonstrated both an abnormal B cell population with CD20 (variably decreased), CD38 (variably increased), and kappa light chain restriction with normal expression of CD45 and CD19 without CD5 or CD10/6.2% and an abnormal plasma cell population expressing CD45 (increased) and cytoplasmic kappa light chain restriction with normal expression of CD19 and CD38 without CD56/16.7%. The findings in the lymph node were felt to represent DLBCL with plasmacytic differentiation 12 57/M Kappa/0.005% MBL BM CD5, CD20 (low), CD23, FMC7, and absent surface light chain expression with normal expression of CD45 and CD19 without CD10/0.02% Abbreviations: FC flow cytometry; HCL hairy cell leukemia; PB peripheral blood; BM bone marrow; MM multiple myeloma; MGUS monoclonal gammopathy of undetermined significance; LN lymph node; MZL marginal zone lymphoma; MBL monoclonal B cell lymphocytosis; LPL lymphoplasmacytic lymphoma; CLL chronic lymphocytic leukemia; DLBCL diffuse large B cell lymphoma patient was considered to have CLL at the time of the initial flow cytometric study, this patient had a white blood cell count of 3.9 thousand cells/μl with no lymphadenopathy and would therefore not meet WHO 2008 criteria for a
5 J Hematopathol (2012) 5: diagnosis of CLL and is classified as an MBL. Patient 3 had three additional clonal populations that included a clonal B cell population negative for CD5, CD10, CD11c, or CD103, a small clonal plasma cell population co-expressing CD56 without CD19, and a small MBL population with a CLLlike immunophenotype. The first population in this patient comprised 10% of the white blood cells by flow cytometry and this patient had an IgM kappa monoclonal spike of 1.2 g/dl on serum protein electrophoresis with immunofixation, findings consistent with a low-grade B cell lymphoma with the immunophenotype and laboratory data suggesting lymphoplasmacytic lymphoma or marginal zone lymphoma (LPL/MZL). The significance of the plasma cell population in this patient is unclear. Although the plasma cell population shared similar light chain expression with the LPL/MZL population, raising the possibility that it represented a component of the B cell neoplasm with plasmacytoid differentiation, a major subset of the plasma cells expressed CD56 without CD19, a phenotype more characteristic of a primary plasma cell neoplasm. The abnormal plasma cell population in this case is therefore classified as possible MGUS. Patient 11 had an abnormal plasma cell population identified in the marrow and was subsequently determined to have a diffuse large B cell lymphoma with plasmacytoid differentiation identified in a lymph node biopsy. In addition, four patients had MBL with CLL-like immunophenotype only and one patient had MGUS only. Most (seven) of the cases demonstrated flow cytometric evidence of the second clone at presentation, while the remaining five cases showed a second clone during follow-up (see Table 3 for details). Of note, two of seven (29%) of the second clones identified at presentation were clinically significant while four of five (80%) of the clones detected at follow-up represented true disease entities. Examples of additional clonal populations are shown in Fig. 1. The prevalence of MBL, MGUS, and of a true B cell or plasma cell neoplasm in this cohort was 5.2% (6/115), 1.7% (2/115), and 5.2% (6/115), respectively. Bi-clonal hairy cell leukemia While bi-clonal cases of other B cell neoplasms, most notably CLL/SLL, are encountered with some frequency, to our knowledge only a single case of bi-clonal HCL was reported in the literature over 20 years ago [18]. We have identified an additional case that demonstrated clear bi-clonality based on both alternate light chain expression by two separate HCL populations as well as different immunoglobulin heavy chain receptor gene rearrangements as assessed by polymerase chain reaction. The patient was a 34-year-old male who presented for bone marrow evaluation for investigation of pancytopenia and fever. Flow cytometry demonstrated two immunophenotypically distinct abnormal B cell populations, each with an immunophenotype diagnostic for Fig. 1 Examples of CLL and MM in combination with HCL, flow dot plots. Additional clonal expansions of either B cells (a) or plasma cells (b) were frequently seen in patients with HCL. An example of CLL in combination with HCL (patient 10 from table 3) is shown in (a). In addition to HCL population (red) showing increased side scatter with abnormal expression of CD45 (increased), CD11c, CD25 and CD103 with lambda light chain restriction and expression of FMC-7, there is also an expanded CLL (magenta) population showing abnormal expression of CD5 and CD23 without FMC-7, significant CD25 or CD103. The CLL clone demonstrated low-level kappa light chain restriction. An example of plasma cell neoplasm in combination with HCL (patient 1 from table 3) is shown in (b). In addition to a HCL population (blue) that showed increased side scatter and kappa light chain restriction with CD25, CD11c and CD103 expression (not shown), there was an abnormal plasma cell population (magenta) with abnormal expression of CD45 (absent), CD19 (absent) and CD56 (subset positive), with cytoplasmic kappa light chain restriction HCL. The first abnormal B cell population comprised 51.7% of the white blood cells and expressed CD11c, CD19, CD20, CD25, CD103 (variable), and CD123 with kappa light chain restriction without significant CD5, CD10, or CD43. The second abnormal B cell population comprised 13.3% of the white blood cells and expressed CD10, CD11c, CD19, CD20, CD25, CD103 (variable), and CD123 with lambda light chain restriction without significant CD5 or CD43. The immunophenotype of the abnormal B cell populations was consistent with a diagnosis of HCL with two clones one clone expressing CD10 and lambda light chain and one clone expressing kappa light chain without CD10. Morphologic examination of the bone marrow demonstrated extensive effacement of the normal marrow architecture by abnormal B cells with clumped chromatin and abundant pale cytoplasm on H&E stain. Concurrent peripheral blood demonstrated circulating atypical cells demonstrating distinctive cytoplasmic projections characteristic of HCL. Kappa- and lambda-expressing B cells were separated using flow cytometric sorting and analyzed for a clonal immunoglobulin heavy chain gene receptor rearrangement by polymerase chain reaction followed by capillary electrophoresis. Post-sorting samples clearly demonstrated different clonal immunoglobulin heavy chain gene rearrangements in the two populations. These findings are illustrated in Fig. 2. Discussion To our knowledge, this investigation is the first large systematic study analyzing data from unselected cases of HCL that explores the frequency of bi-clonal HCL proliferations or the coexistence of a second B cell or plasma cell clone in patients with HCL by flow cytometry. We documented that more than one in ten patients with HCL harbor one or more additional clonal B cell or plasma cell populations. Moreover, nearly one in five older patients with HCL harbors an additional detectable clone. The frequency of incidental
6 128 J Hematopathol (2012) 5:
7 J Hematopathol (2012) 5: Fig. 2 Morphologic examination of the bone marrow demonstrated extensive effacement of the normal marrow architecture by abnormal B cells with clumped chromatin and abundant pale cytoplasm on H&E stain and Wright-Giemsa stains (a). Flow cytometry (b) demonstrated two immunophenotypically distinct abnormal B cell populations with immunophenotypes diagnostic for HCL. The first abnormal B cell population expressed kappa light chain restriction (blue) without significant CD10. The second abnormal B cell population expressed lambda light chain restriction (red) and CD10. Both populations expressed CD11c, CD25, and CD103. Kappa and lambda expressing B cells were separated using flow cytometric sorting and analyzed for a clonal immunoglobulin heavy chain receptor rearrangement by polymerase chain reaction followed by capillary electrophoresis. Post sorting samples clearly demonstrated distinct clonal immunoglobulin heavy chain rearrangements in each population (c) second clones representing MBL or MGUS (5.2% and 1.7%, respectively) was similar in this cohort of patients with HCL as compared to that previously reported in the literature for healthy adults [22 26]. However, half of the second clones detected (6 of 12) represented true disease entities corresponding to an overall frequency of 5.2% of patients in this cohort. Although it is difficult to find comparable data for the general population, for non-hodgkin s lymphoma, the reported lifetime risk is 2.13% and the ageadjusted incidence is 19.8 per 100,000 per year, while for myeloma, the reported lifetime risk is 0.65% and the ageadjusted incidence is 5.7 per 100,000 per year as determined by data from the SEER database (calculations based on cases from 2004 to 2008 from 17 SEER geographic regions, see These data suggest that the frequency of B cell lymphoma and/or myeloma may be higher in patients with HCL than in the general population. More than half (7 of 12) of second clonal populations were detected at presentation and the remaining five at follow up for HCL. From this limited sample, it appears that HCL itself or a predisposition to developing a neoplasm of B cell or plasma cell origin, rather than HCL treatment, may be a primary factor in the development of second clone. This conclusion is supported by prior studies demonstrating lack of association of the presence of a second neoplasm in HCL and a specific therapeutic regimen [7, 12]. However, it is interesting to note that while the majority of second clones detected at presentation were clinically insignificant, the majority detected at follow-up were clinically significant. Although it is tempting to speculate that HCL or HCL treatment may contribute to the progression of indolent clonal expansions to true neoplasms, follow-up longitudinal studies would be needed to test this hypothesis. The clonal relationship between the HCL clone and additional clone is not entirely clear on the basis of the data available for review. Because this study was retrospective,
8 130 J Hematopathol (2012) 5: we were unable to analyze the populations by molecular methods. The clones were clearly immunophenotypically distinct and there was no significant association between the light chain restriction in HCL and additional clonal population. Whether the two clones shared a more distant precursor is a question that requires further study. In light of recent data suggesting that CLL may represent a stem cell disorder rather than a neoplasm originating in a disordered mature B cell [27] it would be interesting to investigate whether a similar phenomenon may be occurring in HCL. Our study may not be entirely reflective of a true frequency of second clones in HCL. Observation bias, particularly in patients presenting with symptomatic neoplasms other than HCL and in whom HCL may have been an incidental diagnosis may certainly cause the study to overstate the true prevalence of second clones in HCL. Additionally, as only blood or bone marrow was evaluated in all but one case in this study, we may have missed nodal or extranodal lymphomas. Finally, longer follow-up times may reveal a greater number of cases with a second clone. Nonetheless, our experience is likely to be typical for samples seen in pathology laboratories performing flow cytometric and morphologic evaluation in patients with HCL. References 1. Swerdlow S, Harris NL et al (eds.) World Health Organization Classification of Tumors: WHO classification of tumors of haematopoietic and lymphoid tissues, 4th edition., IARC Press. 2. Goodman GR, Bethel KJ, Saven A (2003) Hairy cell leukemia: an update. Curr Opin Hematol 10: Del Giudice I, Matutes E, Morilla R et al (2004) The diagnostic value of CD123 in B-cell disorders with hairy or villous lymphocytes. Haematologica 89: Forconi F, Sahota SS, Raspadori D et al (2004) Hairy cell leukemia: at the crossroad of somatic mutation and isotype switch. Blood 104: Chen YH, Tallman MS, Goolsby C et al (2006) Immunophenotypic variations in hairy cell leukemia. Am J Clin Pathol 125: Jasionowski TM, Hartung L, Greenwood JH et al (2003) Analysis of CD10+ hairy cell leukemia. Am J Clin Pathol 120: Dasanu CA, Alexandrescu DT (2010) Risk of additional cancers in untreated and treated hairy cell leukemia patients. Expert Opin Pharmacother 11: Hisada M, Chen BE, Jaffe ES et al (2007) Second cancer incidence and cause-specific mortality among 3104 patients with hairy cell leukemia: a population-based study. J Natl Cancer Inst 99: Paltiel O, Adler B, Barchana M et al (2006) A population-based study of hairy cell leukemia in Israel. Eur J Haematol 77: Federico M, Zinzani PL, Frassoldati A et al (2002) Risk of second cancer in patients with hairy cell leukemia: long-term follow-up. J Clin Oncol 20: Au WY, Klasa RJ, Gallagher R et al (1998) Second malignancies in patients with hairy cell leukemia in british columbia: a 20-year experience. Blood 92: Kurzrock R, Strom SS, Estey E et al (1997) Second cancer risk in hairy cell leukemia: analysis of 350 patients. J Clin Oncol 15: Sokol L, Agosti SJ (2004) Simultaneous manifestation of chronic lymphocytic leukemia (CLL) and hairy cell leukemia (HCL). Am J Hematol 75: Gine E, Bosch F, Villamor N et al (2002) Simultaneous diagnosis of hairy cell leukemia and chronic lymphocytic leukemia/small lymphocytic lymphoma: a frequent association? Leukemia 16: Saif MW, Greenberg BR (2001) Multiple myeloma and hairy cell leukemia: a rare association or coincidence? Leuk Lymphoma 42: Resegotti L, Pistone M, Testa D et al (1985) Simultaneous occurrence of hairy cell leukemia and Hodgkin s disease in the same patient. Haematologica 70: Sanchez ML, Almeida J, Gonzalez D et al (2003) Incidence and clinicobiologic characteristics of leukemic B-cell chronic lymphoproliferative disorders with more than one B-cell clone. Blood 102: Raghavachar A, Bartram CR, Porzsolt F (1986) Eradication by alpha-interferon of one clone in biclonal hairy cell leukaemia. Lancet 2: Evans PA, Pott C, Groenen PJ et al (2007) Significantly improved PCR-based clonality testing in B-cell malignancies by use of multiple immunoglobulin gene targets. Report of the BIOMED-2 Concerted Action BHM4-CT Leukemia 21: Staines A, Cartwright RA (1993) Hairy cell leukaemia: descriptive epidemiology and a case control study. Br J Haematol 85: Kristinsson SY, Vidarsson B, Agnarsson BA et al (2002) Epidemiology of hairy cell leukemia in Iceland. Hematol J 3: Nieto WG, Teodosio C, Lopez A et al (2010) Non-CLL-like monoclonal B-cell lymphocytosis in the general population: prevalence and phenotypic/genetic characteristics. Cytometry B Clin Cytom 78(Suppl 1):S24 S Shim YK, Middleton DC, Caporaso NE et al (2010) Prevalence of monoclonal B-cell lymphocytosis: a systematic review. Cytometry B Clin Cytom 78(Suppl 1):S10 S Nieto WG, Almeida J, Romero A et al (2009) Increased frequency (12%) of circulating chronic lymphocytic leukemia-like B-cell clones in healthy subjects using a highly sensitive multicolor flow cytometry approach. Blood 114: Rawstron AC, Green MJ, Kuzmicki A et al (2002) Monoclonal B lymphocytes with the characteristics of indolent chronic lymphocytic leukemia are present in 3.5% of adults with normal blood counts. Blood 100: Kyle RA, Therneau TM, Rajkumar SV et al (2006) Prevalence of monoclonal gammopathy of undetermined significance. N Engl J Med 354: Kikushige Y, Ishikawa F, Miyamoto T et al (2011) Selfrenewing hematopoietic stem cell is the primary target in pathogenesis of human chronic lymphocytic leukemia. Cancer Cell 20:
Lymphoid Neoplasms Associated With IgM Paraprotein A Study of 382 Patients
 Hematopathology / LYMPHOMAS WITH IGM PARAPROTEIN Lymphoid Neoplasms Associated With IgM Paraprotein A Study of 382 Patients Pei Lin, MD, 1 Suyang Hao, MD, 1* Beverly C. Handy, MD, 2 Carlos E. Bueso-Ramos,
Hematopathology / LYMPHOMAS WITH IGM PARAPROTEIN Lymphoid Neoplasms Associated With IgM Paraprotein A Study of 382 Patients Pei Lin, MD, 1 Suyang Hao, MD, 1* Beverly C. Handy, MD, 2 Carlos E. Bueso-Ramos,
V. Acute leukemia. Flow cytometry in evaluation of hematopoietic neoplasms: A case-based approach
 V. Acute leukemia Evaluating a sample for an acute leukemia Acute leukemia is a neoplasm of immature myeloid or lymphoid cells characterized by a block in maturation, usually at the stage of an early progenitor
V. Acute leukemia Evaluating a sample for an acute leukemia Acute leukemia is a neoplasm of immature myeloid or lymphoid cells characterized by a block in maturation, usually at the stage of an early progenitor
The spectrum of flow cytometry of the bone marrow
 The spectrum of flow cytometry of the bone marrow Anna Porwit Lund University Faculty of Medicine Dept. of Clinical Sciences Div. Oncology and Pathology anna.porwit@med.lu.se Disclosure of speaker s interests
The spectrum of flow cytometry of the bone marrow Anna Porwit Lund University Faculty of Medicine Dept. of Clinical Sciences Div. Oncology and Pathology anna.porwit@med.lu.se Disclosure of speaker s interests
Patterns of Lymphoid Neoplasia in Peripheral Blood. Leon F. Baltrucki, M.D. Leon F. Baltrucki, M.D. Disclosure
 Patterns of Lymphoid Neoplasia in Peripheral Blood Leon F. Baltrucki, M.D. Leon F. Baltrucki, M.D. Disclosure Dr Baltrucki has received an honorarium for his participation as a faculty presenter in this
Patterns of Lymphoid Neoplasia in Peripheral Blood Leon F. Baltrucki, M.D. Leon F. Baltrucki, M.D. Disclosure Dr Baltrucki has received an honorarium for his participation as a faculty presenter in this
Flow cytometric analysis of B-cell lymphoproliferative disorders
 Flow cytometric analysis of B-cell lymphoproliferative disorders David M. Dorfman, M.D., Ph.D. Department of Pathology Brigham and Women s Hospital and Harvard Medical School Boston, MA Objectives Review
Flow cytometric analysis of B-cell lymphoproliferative disorders David M. Dorfman, M.D., Ph.D. Department of Pathology Brigham and Women s Hospital and Harvard Medical School Boston, MA Objectives Review
7 Omar Abu Reesh. Dr. Ahmad Mansour Dr. Ahmad Mansour
 7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
Case 3. Ann T. Moriarty,MD
 Case 3 Ann T. Moriarty,MD Case 3 59 year old male with asymptomatic cervical lymphadenopathy. These images are from a fine needle biopsy of a left cervical lymph node. Image 1 Papanicolaou Stained smear,100x.
Case 3 Ann T. Moriarty,MD Case 3 59 year old male with asymptomatic cervical lymphadenopathy. These images are from a fine needle biopsy of a left cervical lymph node. Image 1 Papanicolaou Stained smear,100x.
WHO Classification. B-cell chronic lymphocytic leukemia/small T-cell granular lymphocytic leukemia
 Blood Malignancies-II Prof. Dr. Herman Hariman, a Ph.D, SpPK (KH). Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. of Clinical Pathology, School of Medicine, University of North Sumatra WHO classification
Blood Malignancies-II Prof. Dr. Herman Hariman, a Ph.D, SpPK (KH). Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. of Clinical Pathology, School of Medicine, University of North Sumatra WHO classification
Flow Cytometric Analysis of Surface Light Chain Expression Patterns in B-Cell Lymphomas Using Monoclonal and Polyclonal Antibodies
 Hematopathology / Light Chain Expression in B-NHLs Flow Cytometric Analysis of Surface Light Chain Expression Patterns in B-Cell Lymphomas Using Monoclonal and Polyclonal Antibodies Pedro Horna, MD, Horatiu
Hematopathology / Light Chain Expression in B-NHLs Flow Cytometric Analysis of Surface Light Chain Expression Patterns in B-Cell Lymphomas Using Monoclonal and Polyclonal Antibodies Pedro Horna, MD, Horatiu
The patient had a mild splenomegaly but no obvious lymph node enlargement. The consensus phenotype obtained from part one of the exercise was:
 Case History An 86 year old male was admitted to hospital with chest infection. Haematological examination subsequently revealed the following: Hb- 11.0 g/dl; WBC- 67.1 x 10^9/l; PLT- 99 x10^9/l; RBC-
Case History An 86 year old male was admitted to hospital with chest infection. Haematological examination subsequently revealed the following: Hb- 11.0 g/dl; WBC- 67.1 x 10^9/l; PLT- 99 x10^9/l; RBC-
Session 5. Pre-malignant clonal hematopoietic proliferations. Chairs: Frank Kuo and Valentina Nardi
 Session 5 Pre-malignant clonal hematopoietic proliferations Chairs: Frank Kuo and Valentina Nardi Pre-malignant clonal hematopoietic proliferations Clonal LYMPHOID proliferations: - Monoclonal gammopathy
Session 5 Pre-malignant clonal hematopoietic proliferations Chairs: Frank Kuo and Valentina Nardi Pre-malignant clonal hematopoietic proliferations Clonal LYMPHOID proliferations: - Monoclonal gammopathy
CME/SAM. Abstract. Hematopathology / CD103 and CD123 in B-Cell Neoplasia
 Hematopathology / CD103 and CD123 in B-Cell Neoplasia Characteristic CD103 and CD123 Expression Pattern Defines Hairy Cell Leukemia Usefulness of CD123 and CD103 in the Diagnosis of Mature B-Cell Lymphoproliferative
Hematopathology / CD103 and CD123 in B-Cell Neoplasia Characteristic CD103 and CD123 Expression Pattern Defines Hairy Cell Leukemia Usefulness of CD123 and CD103 in the Diagnosis of Mature B-Cell Lymphoproliferative
Successful flow cytometric immunophenotyping of body fluid specimens
 Successful flow cytometric immunophenotyping of body fluid specimens Fiona E. Craig, MD Division of Hematopathology Mayo Clinic Arizona 2017 MFMER slide-1 Financial disclosure No conflicts 2017 MFMER slide-2
Successful flow cytometric immunophenotyping of body fluid specimens Fiona E. Craig, MD Division of Hematopathology Mayo Clinic Arizona 2017 MFMER slide-1 Financial disclosure No conflicts 2017 MFMER slide-2
Pathology #07. Hussein Al-Sa di. Dr. Sohaib Al-Khatib. Mature B-Cell Neoplasm. 0 P a g e
 Pathology #07 Mature B-Cell Neoplasm Hussein Al-Sa di Dr. Sohaib Al-Khatib 0 P a g e Thursday 18/2/2016 Our lecture today (with the next 2 lectures) will be about lymphoid tumors This is a little bit long
Pathology #07 Mature B-Cell Neoplasm Hussein Al-Sa di Dr. Sohaib Al-Khatib 0 P a g e Thursday 18/2/2016 Our lecture today (with the next 2 lectures) will be about lymphoid tumors This is a little bit long
Immunophenotypic Variations in Hairy Cell Leukemia
 Hematopathology / IMMUNOPHENOTYPIC VARIATIONS IN HCL Immunophenotypic Variations in Hairy Cell Leukemia Yi-Hua Chen, MD, 1* Martin S. Tallman, MD, 2 Charles Goolsby, PhD, 1 and LoAnn Peterson, MD 1 Key
Hematopathology / IMMUNOPHENOTYPIC VARIATIONS IN HCL Immunophenotypic Variations in Hairy Cell Leukemia Yi-Hua Chen, MD, 1* Martin S. Tallman, MD, 2 Charles Goolsby, PhD, 1 and LoAnn Peterson, MD 1 Key
FLOW CYTOMETRY PRINCIPLES AND PRACTICE. Toby Eyre Consultant Haematologist Oxford University Hospitals NHS Foundation Trust June 2018
 FLOW CYTOMETRY PRINCIPLES AND PRACTICE Toby Eyre Consultant Haematologist Oxford University Hospitals NHS Foundation Trust June 2018 Aims and Objectives Principles of flow cytometry Preparation Steps involved
FLOW CYTOMETRY PRINCIPLES AND PRACTICE Toby Eyre Consultant Haematologist Oxford University Hospitals NHS Foundation Trust June 2018 Aims and Objectives Principles of flow cytometry Preparation Steps involved
Pathology of the indolent B-cell lymphomas Elias Campo
 Pathology of the indolent B-cell lymphomas Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas Antigen selection NAIVE -B LYMPHOCYTE MEMORY B-CELL MCL FL LPL MZL CLL Small cell
Pathology of the indolent B-cell lymphomas Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas Antigen selection NAIVE -B LYMPHOCYTE MEMORY B-CELL MCL FL LPL MZL CLL Small cell
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Classification of Hematologic Malignancies. Patricia Aoun MD MPH
 Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
CME/SAM. Olga Pozdnyakova, MD, PhD, 1 Svetlana Kondtratiev, MD, 1,2 Betty Li, MS, 1 Karry Charest, 1 and David M. Dorfman, MD, PhD 1.
 Hematopathology / New Mastocytosis Flow Cytometry Approach High-Sensitivity Flow Cytometric Analysis for the Evaluation of Systemic Mastocytosis Including the Identification of a New Flow Cytometric Criterion
Hematopathology / New Mastocytosis Flow Cytometry Approach High-Sensitivity Flow Cytometric Analysis for the Evaluation of Systemic Mastocytosis Including the Identification of a New Flow Cytometric Criterion
Critical Analysis and Diagnostic Usefulness of Limited Immunophenotyping of B-Cell Non-Hodgkin Lymphomas by Flow Cytometry
 Hematopathology / FLOW CYTOMETRIC IMMUNOPHENOTYPING IN B-CELL NON-HODGKIN LYMPHOMA Critical Analysis and Diagnostic Usefulness of Limited Immunophenotyping of B-Cell Non-Hodgkin Lymphomas by Flow Cytometry
Hematopathology / FLOW CYTOMETRIC IMMUNOPHENOTYPING IN B-CELL NON-HODGKIN LYMPHOMA Critical Analysis and Diagnostic Usefulness of Limited Immunophenotyping of B-Cell Non-Hodgkin Lymphomas by Flow Cytometry
Immunophenotypic Profile of Lymphoplasmacytic Lymphoma/Waldenström Macroglobulinemia
 Hematopathology / IMMUNOPHENOTYPE OF LPL/WM Immunophenotypic Profile of Lymphoplasmacytic Lymphoma/Waldenström Macroglobulinemia Sergej Konoplev, MD, PhD, L. Jeffrey Medeiros, MD, Carlos E. Bueso-Ramos,
Hematopathology / IMMUNOPHENOTYPE OF LPL/WM Immunophenotypic Profile of Lymphoplasmacytic Lymphoma/Waldenström Macroglobulinemia Sergej Konoplev, MD, PhD, L. Jeffrey Medeiros, MD, Carlos E. Bueso-Ramos,
Test Utilization: Chronic Lymphocytic Leukemia
 Test Utilization: Chronic Lymphocytic Leukemia Initial Evaluation Diagnostic Criteria Selection of Tests for Prognosis Response to Therapy Challenges Assessment for persistent disease Paul J. Kurtin, M.D.
Test Utilization: Chronic Lymphocytic Leukemia Initial Evaluation Diagnostic Criteria Selection of Tests for Prognosis Response to Therapy Challenges Assessment for persistent disease Paul J. Kurtin, M.D.
Corrigenda. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run
 Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent
 Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
Hematology 101. Rachid Baz, M.D. 5/16/2014
 Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
Molecular Pathology of Lymphoma (Part 1) Rex K.H. Au-Yeung Department of Pathology, HKU
 Molecular Pathology of Lymphoma (Part 1) Rex K.H. Au-Yeung Department of Pathology, HKU Lecture outline Time 10:00 11:00 11:15 12:10 12:20 13:15 Content Introduction to lymphoma Review of lymphocyte biology
Molecular Pathology of Lymphoma (Part 1) Rex K.H. Au-Yeung Department of Pathology, HKU Lecture outline Time 10:00 11:00 11:15 12:10 12:20 13:15 Content Introduction to lymphoma Review of lymphocyte biology
Do Your Flow Cytometric LDTs. Validation Guidelines? Fiona E. Craig, MD University of Pittsburgh School of Medicine
 Do Your Flow Cytometric LDTs Conform to the ICSH ICCS Validation Guidelines? Fiona E. Craig, MD University of Pittsburgh School of Medicine How should LDTs be validated? Accuracy Specificity Sensitivity
Do Your Flow Cytometric LDTs Conform to the ICSH ICCS Validation Guidelines? Fiona E. Craig, MD University of Pittsburgh School of Medicine How should LDTs be validated? Accuracy Specificity Sensitivity
Dr Prashant Tembhare
 Dr Prashant Tembhare docprt@gmail.com FCM very powerful technology in Identification and characterization of neoplastic plasma cells as it allows - simultaneous assessment of multiple antigens large numbers
Dr Prashant Tembhare docprt@gmail.com FCM very powerful technology in Identification and characterization of neoplastic plasma cells as it allows - simultaneous assessment of multiple antigens large numbers
Clinical question. Screening tube. Diagnostic panel MRD. Clinical question
 OW CYTOMETRY UPDATES IN LYMPHOPROLIFERATIVE DISORDERS CANCER RESEARCH CENTER IBSAL UNIVERSITY & UNIVERSITY HOSPITAL, SALAMANCA (SPAIN) DISCLOSURES The EuroFlow Scientific Consortium Iamco-chairof receives
OW CYTOMETRY UPDATES IN LYMPHOPROLIFERATIVE DISORDERS CANCER RESEARCH CENTER IBSAL UNIVERSITY & UNIVERSITY HOSPITAL, SALAMANCA (SPAIN) DISCLOSURES The EuroFlow Scientific Consortium Iamco-chairof receives
2013 AAIM Pathology Workshop
 2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
Outlines. Disclosures. Updates on B-cell Chronic Lymphoproliferative Disorders of the Blood and Bone Marrow
 Updates on B-cell Chronic Lymphoproliferative Disorders of the Blood and Bone Marrow Sa A, Wang MD Jeffrey L. Jorgensen, MD, PhD Department of Hematopathology, UT M.D. Anderson Cancer Center, Houston,
Updates on B-cell Chronic Lymphoproliferative Disorders of the Blood and Bone Marrow Sa A, Wang MD Jeffrey L. Jorgensen, MD, PhD Department of Hematopathology, UT M.D. Anderson Cancer Center, Houston,
Welcome. Welcome. Emerging Technologies in Flow Cytometry
 Emerging Technologies in Flow Cytometry Dr. William Dittman December 11, 2012 You may download a copy of the handout by clicking on the handout icon, located in the upper right hand corner of your screen
Emerging Technologies in Flow Cytometry Dr. William Dittman December 11, 2012 You may download a copy of the handout by clicking on the handout icon, located in the upper right hand corner of your screen
Commentary on the WHO Classification of Tumors of Lymphoid Tissues (2008): Indolent B Cell Lymphomas
 Commentary on the WHO Classification of Tumors of Lymphoid Tissues (2008): Indolent B Cell Lymphomas The Harvard community has made this article openly available. Please share how this access benefits
Commentary on the WHO Classification of Tumors of Lymphoid Tissues (2008): Indolent B Cell Lymphomas The Harvard community has made this article openly available. Please share how this access benefits
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
88-year-old Female with Lymphadenopathy. Faizi Ali, MD
 88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
Immunopathology of Lymphoma
 Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology. Songlin Zhang, MD, PhD LSUHSC-Shreveport
 From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology Songlin Zhang, MD, PhD LSUHSC-Shreveport I have no Conflict of Interest. FNA on Lymphoproliferative
From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology Songlin Zhang, MD, PhD LSUHSC-Shreveport I have no Conflict of Interest. FNA on Lymphoproliferative
Lack of Surface Immunoglobulin Light Chain Expression by Flow Cytometric Immunophenotyping Can Help Diagnose Peripheral B-Cell Lymphoma
 Hematopathology / SURFACE IMMUNOGLOBULIN LIGHT CHAIN NEGATIVE PERIPHERAL B-CELL LYMPHOMA Lack of Surface Immunoglobulin Light Chain Expression by Flow Cytometric Immunophenotyping Can Help Diagnose Peripheral
Hematopathology / SURFACE IMMUNOGLOBULIN LIGHT CHAIN NEGATIVE PERIPHERAL B-CELL LYMPHOMA Lack of Surface Immunoglobulin Light Chain Expression by Flow Cytometric Immunophenotyping Can Help Diagnose Peripheral
WBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
Case #1. Robert J. Glinert, M.D. David C. Fisher, M.D. Dana Farber Cancer Institute
 Case #1 Robert J. Glinert, M.D. David C. Fisher, M.D. Dana Farber Cancer Institute Patient History Part I 76 year-old man 1997 diagnosed with MGUS (biclonal) during evaluation of (self-limited) anemia.
Case #1 Robert J. Glinert, M.D. David C. Fisher, M.D. Dana Farber Cancer Institute Patient History Part I 76 year-old man 1997 diagnosed with MGUS (biclonal) during evaluation of (self-limited) anemia.
Serum free light chain (SFLC) assays. Dr Sarah Sasson SydPath Registrar
 Serum free light chain (SFLC) assays Dr Sarah Sasson SydPath Registrar Introduction to SFLC Plasma cell dyscrasias such as monoclonal gammopathy of uncertain significance (MGUS) smouldering/asymptomatic
Serum free light chain (SFLC) assays Dr Sarah Sasson SydPath Registrar Introduction to SFLC Plasma cell dyscrasias such as monoclonal gammopathy of uncertain significance (MGUS) smouldering/asymptomatic
B-cell Chronic Lymphoproliferative Disorders of the Blood and Bone Marrow
 B-cell Chronic Lymphoproliferative Disorders of the Blood and Bone Marrow Sanam Loghavi, MD Department of Hematopathology University of Texas MD Anderson Cancer Center Houston, TX Disclosures I have no
B-cell Chronic Lymphoproliferative Disorders of the Blood and Bone Marrow Sanam Loghavi, MD Department of Hematopathology University of Texas MD Anderson Cancer Center Houston, TX Disclosures I have no
Participants Identification No. % Evaluation
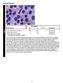 BMD-02 Cell Identification Participants Identification No. % Evaluation Erythrocyte precursor, normal 228 95.8 Educational Erythrocyte, normal 7 3.0 Educational Erythrocyte precursor with megaloblastic
BMD-02 Cell Identification Participants Identification No. % Evaluation Erythrocyte precursor, normal 228 95.8 Educational Erythrocyte, normal 7 3.0 Educational Erythrocyte precursor with megaloblastic
The development of clonality testing for lymphomas in the Bristol Genetics Laboratory. Dr Paula Waits Bristol Genetics Laboratory
 The development of clonality testing for lymphomas in the Bristol Genetics Laboratory Dr Paula Waits Bristol Genetics Laboratory Introduction The majority of lymphoid malignancies belong to the B cell
The development of clonality testing for lymphomas in the Bristol Genetics Laboratory Dr Paula Waits Bristol Genetics Laboratory Introduction The majority of lymphoid malignancies belong to the B cell
MBL in Blood Donors: An Extended Immunophenotypic Analysis of CLL-like, CD5+ MBL.
 1 th Canadian CLL Meeting Winnipeg, Manitoba Inn at the Forks September 18-19, 214 MBL in Blood Donors: An Extended Immunophenotypic Analysis of CLL-like, CD5+ MBL. Fatima Abbasi 1, Justin Meskas 2, Ryan
1 th Canadian CLL Meeting Winnipeg, Manitoba Inn at the Forks September 18-19, 214 MBL in Blood Donors: An Extended Immunophenotypic Analysis of CLL-like, CD5+ MBL. Fatima Abbasi 1, Justin Meskas 2, Ryan
PhenoPath. Diagnoses you can count on B CELL NON-HODGKIN LYMPHOMA
 PhenoPath Diagnoses you can count on B CELL NON-HODGKIN LYMPHOMA C urrent diagnosis of B cell non-hodgkin lymphoma (B-NHL) is based on the 2008 WHO Classification of Tumours of Haematopoietic and Lymphoid
PhenoPath Diagnoses you can count on B CELL NON-HODGKIN LYMPHOMA C urrent diagnosis of B cell non-hodgkin lymphoma (B-NHL) is based on the 2008 WHO Classification of Tumours of Haematopoietic and Lymphoid
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells. Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital
 Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Low-grade B-cell lymphoma
 Low-grade B-cell lymphoma Patho-Basic 11. September 2018 Stephan Dirnhofer Pathology Outline Definition LPL, MBL/CLL/SLL, MCL FL Subtypes & variants Diagnosis including Grading Transformation Summary Be
Low-grade B-cell lymphoma Patho-Basic 11. September 2018 Stephan Dirnhofer Pathology Outline Definition LPL, MBL/CLL/SLL, MCL FL Subtypes & variants Diagnosis including Grading Transformation Summary Be
HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor
 HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor I. Description of the rotation: During this rotation, the resident will gain
HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor I. Description of the rotation: During this rotation, the resident will gain
CD5~ Small B-Cell Leukemias Are Rarely Classifiable as Chronic Lymphocytic Leukemia
 Hematopathology / CD5- LYMPHOPROLIFERATIVE DISORDERS CD5~ Small B-Cell Leukemias Are Rarely Classifiable as Chronic Lymphocytic Leukemia Jane C. Huang, M D, William G. Finn, M D, Charles L. Goolsby, PhD,
Hematopathology / CD5- LYMPHOPROLIFERATIVE DISORDERS CD5~ Small B-Cell Leukemias Are Rarely Classifiable as Chronic Lymphocytic Leukemia Jane C. Huang, M D, William G. Finn, M D, Charles L. Goolsby, PhD,
CME/SAM. Flow Cytometric Immunophenotyping of Cerebrospinal Fluid Specimens
 Hematopathology / Flow Cytometric Immunophenotyping of CSF Specimens Flow Cytometric Immunophenotyping of Cerebrospinal Fluid Specimens Fiona E. Craig, MD, 1 N. Paul Ohori, MD, 2 Timothy S. Gorrill, MD,
Hematopathology / Flow Cytometric Immunophenotyping of CSF Specimens Flow Cytometric Immunophenotyping of Cerebrospinal Fluid Specimens Fiona E. Craig, MD, 1 N. Paul Ohori, MD, 2 Timothy S. Gorrill, MD,
ADx Bone Marrow Report. Patient Information Referring Physician Specimen Information
 ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
Clinical Policy: Bendamustine (Bendeka, Treanda) Reference Number: PA.CP.PHAR.307
 Clinical Policy: (Bendeka, Treanda) Reference Number: PA.CP.PHAR.307 Effective Date: 01/18 Last Review Date: 11/17 Coding Implications Revision Log Description The intent of the criteria is to ensure that
Clinical Policy: (Bendeka, Treanda) Reference Number: PA.CP.PHAR.307 Effective Date: 01/18 Last Review Date: 11/17 Coding Implications Revision Log Description The intent of the criteria is to ensure that
Small, mature-appearing appearing
 B-cell Chronic Lymphoproliferative Disorders of the Blood and Bone Marrow Disclosures I have nothing to disclose. Jeffrey L. Jorgensen, MD, PhD Department of Hematopathology, UT M.D. Anderson Cancer Center,
B-cell Chronic Lymphoproliferative Disorders of the Blood and Bone Marrow Disclosures I have nothing to disclose. Jeffrey L. Jorgensen, MD, PhD Department of Hematopathology, UT M.D. Anderson Cancer Center,
VUmc Basispresentatie
 Clinical diagnostic cytometry Gerrit J Schuurhuis Dept of Hematology VU University Medical Center Amsterdam, Netherlands Use of immunophenotyping at diagnosis to trace residual disease after therapy 1.
Clinical diagnostic cytometry Gerrit J Schuurhuis Dept of Hematology VU University Medical Center Amsterdam, Netherlands Use of immunophenotyping at diagnosis to trace residual disease after therapy 1.
Significant CD5 Expression on Normal Stage 3 Hematogones and Mature B Lymphocytes in Bone Marrow
 Hematopathology / CD5 Expression on Normal B Cells Significant CD5 Expression on Normal Stage 3 Hematogones and Mature B Lymphocytes in Bone Marrow Franklin S. Fuda, DO, Nitin J. Karandikar, MD, PhD, and
Hematopathology / CD5 Expression on Normal B Cells Significant CD5 Expression on Normal Stage 3 Hematogones and Mature B Lymphocytes in Bone Marrow Franklin S. Fuda, DO, Nitin J. Karandikar, MD, PhD, and
5000 International Clinical Cytometry Society: Practical Flow Cytometry in Hematopathology A Case-Based Approach
 5000 International Clinical Cytometry Society: Practical Flow Cytometry in Hematopathology A Case-Based Approach Joseph A DiGiuseppe, MD, PhD Hartford Hospital Disclosures In the past 12 months, I have
5000 International Clinical Cytometry Society: Practical Flow Cytometry in Hematopathology A Case-Based Approach Joseph A DiGiuseppe, MD, PhD Hartford Hospital Disclosures In the past 12 months, I have
Many of the hematolymphoid disorders are derived
 REVIEW ARTICLE Practical Immunohistochemistry in Hematopathology: A Review of Useful Antibodies for Diagnosis Ji Lu, MD and Karen L. Chang, MD Abstract: This review article offers some useful panels of
REVIEW ARTICLE Practical Immunohistochemistry in Hematopathology: A Review of Useful Antibodies for Diagnosis Ji Lu, MD and Karen L. Chang, MD Abstract: This review article offers some useful panels of
JMSCR Vol. 03 Issue 06 Page June 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x An Indolent Natural Killer Cell Leukemia Presenting with Bilateral Ankle Arthritis and Low Grade Fever Abstract Author Subhash Chandra
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x An Indolent Natural Killer Cell Leukemia Presenting with Bilateral Ankle Arthritis and Low Grade Fever Abstract Author Subhash Chandra
CCND1-IGH Fusion-Amplification and MYC Copy Number Gain in a Case of Pleomorphic Variant Mantle Cell Lymphoma
 AJCP /CASE REPORT CCND1-IGH Fusion-Amplification and MYC Copy Number Gain in a Case of Pleomorphic Variant Mantle Cell Lymphoma Yuan Miao, MD, 1,2 Pei Lin, MD, 1 Wei Wang, MD, 1 L. Jeffrey Medeiros, MD,
AJCP /CASE REPORT CCND1-IGH Fusion-Amplification and MYC Copy Number Gain in a Case of Pleomorphic Variant Mantle Cell Lymphoma Yuan Miao, MD, 1,2 Pei Lin, MD, 1 Wei Wang, MD, 1 L. Jeffrey Medeiros, MD,
Plasma cell myeloma (multiple myeloma)
 Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Prepared by: Dr.Mansour Al-Yazji
 C L L CLL Prepared by: Abd El-Hakeem Abd El-Rahman Abu Naser Ahmed Khamis Abu Warda Ahmed Mohammed Abu Ghaben Bassel Ziad Abu Warda Nedal Mostafa El-Nahhal Dr.Mansour Al-Yazji LEUKEMIA Leukemia is a form
C L L CLL Prepared by: Abd El-Hakeem Abd El-Rahman Abu Naser Ahmed Khamis Abu Warda Ahmed Mohammed Abu Ghaben Bassel Ziad Abu Warda Nedal Mostafa El-Nahhal Dr.Mansour Al-Yazji LEUKEMIA Leukemia is a form
Lymphoma Update: Lymphoma Update: What s Likely to be New in the New WHO. Patrick Treseler, MD, PhD University of California San Francisco
 Lymphoma Update: What s Likely to be New in the New WHO Blood 127:2375; 2016 Patrick Treseler, MD, PhD University of California San Francisco Lymphoma Update: What IS New in the New WHO! Patrick Treseler,
Lymphoma Update: What s Likely to be New in the New WHO Blood 127:2375; 2016 Patrick Treseler, MD, PhD University of California San Francisco Lymphoma Update: What IS New in the New WHO! Patrick Treseler,
Multiple myeloma Biological & Clinical Aspects Isabelle Vande Broek, MD, PhD
 Multiple myeloma Biological & Clinical Aspects Isabelle Vande Broek, MD, PhD Department of Oncology & Hematology AZ Nikolaas Iridium Kanker Netwerk Introduction Multiple myeloma = Kahler s disease Dr.
Multiple myeloma Biological & Clinical Aspects Isabelle Vande Broek, MD, PhD Department of Oncology & Hematology AZ Nikolaas Iridium Kanker Netwerk Introduction Multiple myeloma = Kahler s disease Dr.
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113)
 Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Hematology Case Conference 8/5/03
 Hematology Case Conference 8/5/03 Bone Marrow Case Patient: Emmxxx Lylexxx 74 year old AA female S/P craniotomy for SDH. Pt has Hx of HTN, DM, Crohn s disease, (R) nephrectomy. Bone marrow for abnormal
Hematology Case Conference 8/5/03 Bone Marrow Case Patient: Emmxxx Lylexxx 74 year old AA female S/P craniotomy for SDH. Pt has Hx of HTN, DM, Crohn s disease, (R) nephrectomy. Bone marrow for abnormal
ABERRANT EXPRESSION OF CD19 AND CD43
 ABERRANT EXPRESSION OF CD19 AND CD43 IN A PATIENT WITH THERAPY-RELATED ACUTE MYELOID LEUKEMIA AND A HISTORY OF MANTLE CELL LYMPHOMA Yen-Chuan Hsieh, 1 Chien-Liang Lin, 2 Chao-Jung Tsao, 2 Pin-Pen Hsieh,
ABERRANT EXPRESSION OF CD19 AND CD43 IN A PATIENT WITH THERAPY-RELATED ACUTE MYELOID LEUKEMIA AND A HISTORY OF MANTLE CELL LYMPHOMA Yen-Chuan Hsieh, 1 Chien-Liang Lin, 2 Chao-Jung Tsao, 2 Pin-Pen Hsieh,
Bone Marrow. Procedures Blood Film Aspirate, Cell Block Trephine Biopsy, Touch Imprint
 Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD. Parts 2 and 3
 HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Parts 2 and 3 NEOPLASTIC LYMPHOID DISEASES Introduction o The bone marrow is the source of all cells in the
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Parts 2 and 3 NEOPLASTIC LYMPHOID DISEASES Introduction o The bone marrow is the source of all cells in the
DETERMINATION OF A LYMPHOID PROCESS
 Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
9/28/2017. Follicular Lymphoma and Nodal Marginal Zone Lymphoma. Follicular Lymphoma Definition. Low-Grade B-Cell Lymphomas in WHO Classification
 and L. Jeffrey Medeiros, MD DISCLOSURES I do not have anything to disclose Low-Grade B-Cell Lymphomas in WHO Classification Lymphoma Type Frequency Follicular lymphoma 22.1 % Extranodal MALT-lymphoma 7.6
and L. Jeffrey Medeiros, MD DISCLOSURES I do not have anything to disclose Low-Grade B-Cell Lymphomas in WHO Classification Lymphoma Type Frequency Follicular lymphoma 22.1 % Extranodal MALT-lymphoma 7.6
Diagnostic challenge: Acute leukemia with biphenotypic blasts and BCR-ABL1 translocation
 Case Study Diagnostic challenge: Acute leukemia with biphenotypic blasts and BCR-ABL1 translocation Ling Wang 1 and Xiangdong Xu 1,2,* 1 Department of Pathology, University of California, San Diego; 2
Case Study Diagnostic challenge: Acute leukemia with biphenotypic blasts and BCR-ABL1 translocation Ling Wang 1 and Xiangdong Xu 1,2,* 1 Department of Pathology, University of California, San Diego; 2
ACCME/Disclosures 4/13/2016. Clinical History
 ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
Chronic Lymphocytic Leukemia Mantle Cell Lymphoma Elias Campo
 Chronic Lymphocytic Leukemia Mantle Cell Lymphoma Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas NAIVE -B LYMPHOCYTE MEMORY CELL CLL MCL FL MZL Small cell size Low proliferation
Chronic Lymphocytic Leukemia Mantle Cell Lymphoma Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas NAIVE -B LYMPHOCYTE MEMORY CELL CLL MCL FL MZL Small cell size Low proliferation
A.M.W. van Marion. H.M. Lokhorst. N.W.C.J. van de Donk. J.G. van den Tweel. Histopathology 2002, 41 (suppl 2):77-92 (modified)
 chapter 4 The significance of monoclonal plasma cells in the bone marrow biopsies of patients with multiple myeloma following allogeneic or autologous stem cell transplantation A.M.W. van Marion H.M. Lokhorst
chapter 4 The significance of monoclonal plasma cells in the bone marrow biopsies of patients with multiple myeloma following allogeneic or autologous stem cell transplantation A.M.W. van Marion H.M. Lokhorst
Case Report Primary Hairy Cell Leukemia/Lymphoma of the Breast: A Case Report and Review of the Literature
 Hindawi Publishing Corporation Volume 2014, Article ID 497027, 5 pages http://dx.doi.org/10.1155/2014/497027 Case Report Primary Hairy Cell Leukemia/Lymphoma of the Breast: A Case Report and Review of
Hindawi Publishing Corporation Volume 2014, Article ID 497027, 5 pages http://dx.doi.org/10.1155/2014/497027 Case Report Primary Hairy Cell Leukemia/Lymphoma of the Breast: A Case Report and Review of
Osteosclerotic Myeloma (POEMS Syndrome)
 Osteosclerotic Myeloma (POEMS Syndrome) Osteosclerotic Myeloma (POEMS Syndrome) Synonyms Crow-Fukase syndrome Multicentric Castleman disease Takatsuki syndrome Acronym coined by Bardwick POEMS Scheinker,
Osteosclerotic Myeloma (POEMS Syndrome) Osteosclerotic Myeloma (POEMS Syndrome) Synonyms Crow-Fukase syndrome Multicentric Castleman disease Takatsuki syndrome Acronym coined by Bardwick POEMS Scheinker,
A Practical Guide To Diagnose B-Cell Lymphomas on FNAs. Nancy P. Caraway, M.D.
 A Practical Guide To Diagnose B-Cell Lymphomas on FNAs Nancy P. Caraway, M.D. Major Factors Impacting Dx Lymphomas on Small Bxs Classification systems Immunophenotyping by multiprobe flow cytometry and
A Practical Guide To Diagnose B-Cell Lymphomas on FNAs Nancy P. Caraway, M.D. Major Factors Impacting Dx Lymphomas on Small Bxs Classification systems Immunophenotyping by multiprobe flow cytometry and
Small B-cell (Histologically Low Grade) Lymphoma
 Frequency of Lymphoid Neoplasms Small B-cell (Histologically Low Grade) Lymphoma Stephen Hamilton-Dutoit Institute of Pathology Aarhus University Hospital B-cell neoplasms 88% Diffuse large B-cell lymphoma
Frequency of Lymphoid Neoplasms Small B-cell (Histologically Low Grade) Lymphoma Stephen Hamilton-Dutoit Institute of Pathology Aarhus University Hospital B-cell neoplasms 88% Diffuse large B-cell lymphoma
Smouldering Myeloma: to treat or not to treat?
 Smouldering Myeloma: to treat or not to treat? Massimo Offidani Clinica di Ematologia Azienda Ospedaliero-Universitaria Ospedali Riuniti di Ancona Definitions and epidemiology 3000-5000 new SMM/year in
Smouldering Myeloma: to treat or not to treat? Massimo Offidani Clinica di Ematologia Azienda Ospedaliero-Universitaria Ospedali Riuniti di Ancona Definitions and epidemiology 3000-5000 new SMM/year in
Flow Cytometric Analysis of CD5+ B Cells A Frame of Reference for Minimal Residual Disease Analysis in Chronic Lymphocytic Leukemia
 Hematopathology / CD5+ -CELL NLYSIS Y FLOW CYTOMETRY Flow Cytometric nalysis of CD5+ Cells Frame of Reference for Minimal Residual Disease nalysis in Chronic Lymphocytic Leukemia Ritu Gupta, MD, 1 Paresh
Hematopathology / CD5+ -CELL NLYSIS Y FLOW CYTOMETRY Flow Cytometric nalysis of CD5+ Cells Frame of Reference for Minimal Residual Disease nalysis in Chronic Lymphocytic Leukemia Ritu Gupta, MD, 1 Paresh
CHAPTER:4 LEUKEMIA. BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY 8/12/2009
 LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
Molecular Advances in Hematopathology
 Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
Mast Cell Disease Case 054 Session 7
 Mast Cell Disease Case 054 Session 7 Rodney R. Miles, M.D., Ph.D. Lauren B. Smith, M.D. Cem Akin, M.D. Diane Roulston,, Ph.D. Charles W. Ross, M.D. Departments of Pathology and Internal Medicine University
Mast Cell Disease Case 054 Session 7 Rodney R. Miles, M.D., Ph.D. Lauren B. Smith, M.D. Cem Akin, M.D. Diane Roulston,, Ph.D. Charles W. Ross, M.D. Departments of Pathology and Internal Medicine University
Case Report Parotid gland follicular lymphoma lacking both cytoplasmic and surface light chains: a rare case
 Int J Clin Exp Pathol 2014;7(10):7100-7104 www.ijcep.com /ISSN:1936-2625/IJCEP0001717 Case Report Parotid gland follicular lymphoma lacking both cytoplasmic and surface light chains: a rare case Jenny
Int J Clin Exp Pathol 2014;7(10):7100-7104 www.ijcep.com /ISSN:1936-2625/IJCEP0001717 Case Report Parotid gland follicular lymphoma lacking both cytoplasmic and surface light chains: a rare case Jenny
Mantle Cell Lymphoma
 HEMATOPATHOLOGY Original Article Mantle Cell Lymphoma Morphologic Findings in Bone Marrow Involvement JAY WASMAN, MD, 1 NANCY S. ROSENTHAL, MD,' AND DIANE C. FARHI, MD 2 Although mantle cell lymphoma (MCL),
HEMATOPATHOLOGY Original Article Mantle Cell Lymphoma Morphologic Findings in Bone Marrow Involvement JAY WASMAN, MD, 1 NANCY S. ROSENTHAL, MD,' AND DIANE C. FARHI, MD 2 Although mantle cell lymphoma (MCL),
CD5 Positive Follicular Lymphomas- A Diagnostic Dilemma in a Resource Restricted Laboratory Setting
 Original Article DOI: 10.21276/APALM.1364 CD5 Positive Follicular Lymphomas- A Diagnostic Dilemma in a Resource Restricted Laboratory Setting Sakthi Sankari S 1 *, Arjunan A 2, Bhuvaneswari M.G. 2, Sindhuja
Original Article DOI: 10.21276/APALM.1364 CD5 Positive Follicular Lymphomas- A Diagnostic Dilemma in a Resource Restricted Laboratory Setting Sakthi Sankari S 1 *, Arjunan A 2, Bhuvaneswari M.G. 2, Sindhuja
Gray Zones and Double Hits Distinguishing True Burkitt Lymphoma from Other High-Grade B-NHLs Burkitt Lymphoma Burkitt-Like Lymphoma DLBCL Patrick Tres
 Gray Zones and Double Hits Distinguishing True Burkitt Lymphoma from Other High-Grade B-NHLs Burkitt Lymphoma Burkitt-Like Lymphoma DLBCL Patrick Treseler, MD, PhD University of California San Francisco
Gray Zones and Double Hits Distinguishing True Burkitt Lymphoma from Other High-Grade B-NHLs Burkitt Lymphoma Burkitt-Like Lymphoma DLBCL Patrick Treseler, MD, PhD University of California San Francisco
During past decades, because of the lack of knowledge
 Staging and Classification of Lymphoma Ping Lu, MD In 2004, new cases of non-hodgkin s in the United States were estimated at 54,370, representing 4% of all cancers and resulting 4% of all cancer deaths,
Staging and Classification of Lymphoma Ping Lu, MD In 2004, new cases of non-hodgkin s in the United States were estimated at 54,370, representing 4% of all cancers and resulting 4% of all cancer deaths,
Reac%ve and Benign Flow Cytometry findings
 Reac%ve and Benign Flow Cytometry findings Lymph nodes and other /ssues Sindhu Cherian, MD University of Washington, Sea
Reac%ve and Benign Flow Cytometry findings Lymph nodes and other /ssues Sindhu Cherian, MD University of Washington, Sea
NORTH CAROLINA SOCIETY OF PATHOLOGISTS
 NORTH CAROLINA SOCIETY OF PATHOLOGISTS 2018 Annual Meeting and Shelley Lecture April 13-14, 2018 The Ballantyne Hotel Charlotte, NC FOCUS ON HEMATOPATHOLOGY SATURDAY HANDOUTS This continuing medical education
NORTH CAROLINA SOCIETY OF PATHOLOGISTS 2018 Annual Meeting and Shelley Lecture April 13-14, 2018 The Ballantyne Hotel Charlotte, NC FOCUS ON HEMATOPATHOLOGY SATURDAY HANDOUTS This continuing medical education
Contents. vii. Preface... Acknowledgments... v xiii
 Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
FLOCK Cluster Analysis of Mast Cell Event Clustering by High-Sensitivity Flow Cytometry Predicts Systemic Mastocytosis
 FLOCK Cluster Analysis of Mast Cell Event Clustering by High-Sensitivity Flow Cytometry Predicts Systemic Mastocytosis David M. Dorfman, MD, PhD, Charlotte D. LaPlante, Olga Pozdnyakova, MD, PhD, and Betty
FLOCK Cluster Analysis of Mast Cell Event Clustering by High-Sensitivity Flow Cytometry Predicts Systemic Mastocytosis David M. Dorfman, MD, PhD, Charlotte D. LaPlante, Olga Pozdnyakova, MD, PhD, and Betty
Diagnosis of lymphoid neoplasms has been
 Iranian Journal of Pathology (2007)2 (1), 1-61 Review Article Mehdi Nassiri Dep. of Pathology, University of Miami Miller School of Medicine, Miami, USA Abstract Correct diagnosis and classification of
Iranian Journal of Pathology (2007)2 (1), 1-61 Review Article Mehdi Nassiri Dep. of Pathology, University of Miami Miller School of Medicine, Miami, USA Abstract Correct diagnosis and classification of
Flow cytometric evaluation of endoscopic biopsy specimens from patients with gastrointestinal tract B-cell lymphoma: a preliminary report
 Jichi Medical University Journal Flow cytometric evaluation of endoscopic biopsy specimens from patients with gastrointestinal tract B-cell lymphoma: a preliminary report Satoko Oka,, Kazuo Muroi,, Kazuya
Jichi Medical University Journal Flow cytometric evaluation of endoscopic biopsy specimens from patients with gastrointestinal tract B-cell lymphoma: a preliminary report Satoko Oka,, Kazuo Muroi,, Kazuya
Diagnostic Usefulness of CD23 and FMC-7 Antigen Expression Patterns in B-Cell Lymphoma Classification
 Hematopathology / AND ANTIGEN EXPRESSION IN B-CELL LYMPHOMA CLASSIFICATION Diagnostic Usefulness of and Antigen Expression Patterns in B-Cell Lymphoma Classification Diana P. Garcia, MD, 1* Michele T.
Hematopathology / AND ANTIGEN EXPRESSION IN B-CELL LYMPHOMA CLASSIFICATION Diagnostic Usefulness of and Antigen Expression Patterns in B-Cell Lymphoma Classification Diana P. Garcia, MD, 1* Michele T.
FOLLICULARITY in LYMPHOMA
 FOLLICULARITY in LYMPHOMA Reactive Follicular Hyperplasia Follicular Hyperplasia irregular follicles Follicular Hyperplasia dark and light zones Light Zone Dark Zone Follicular hyperplasia MIB1 Follicular
FOLLICULARITY in LYMPHOMA Reactive Follicular Hyperplasia Follicular Hyperplasia irregular follicles Follicular Hyperplasia dark and light zones Light Zone Dark Zone Follicular hyperplasia MIB1 Follicular
Immunophenotypic Differentiation Between Neoplastic Plasma Cells in Mature B-Cell Lymphoma vs Plasma Cell Myeloma
 Hematopathology / PLASMA CELLS IN LYMPHOMA VS MYELOMA Immunophenotypic Differentiation Between Neoplastic Plasma Cells in Mature B-Cell Lymphoma vs Plasma Cell Myeloma Adam C. Seegmiller, MD, PhD, Yin
Hematopathology / PLASMA CELLS IN LYMPHOMA VS MYELOMA Immunophenotypic Differentiation Between Neoplastic Plasma Cells in Mature B-Cell Lymphoma vs Plasma Cell Myeloma Adam C. Seegmiller, MD, PhD, Yin
