Role of Video-Assisted Thoracic Surgery in the Treatment of Pulmonary Metastases: Results of a Prospective Trial
|
|
|
- Augustine Collins
- 5 years ago
- Views:
Transcription
1 Role of Video-Assisted Thoracic Surgery in the Treatment of Pulmonary Metastases: Results of a Prospective Trial Patricia M. McCormacl MD, Manjit S. Bains, MD, Colin B. Begg, PhD, Michael E. Burt, MD, PhD, Robert J. Downey, MD, David M. Panicek, MD, Valerie W. Rusch, MD, Maureen Zakowski, MD, and Robert J. Ginsberg, MD Departments of Diagnostic Radiology, Pathology, Epidemiology & Biostatistics, and Thoracic Surgery, Memorial Sloan-Kettering Cancer Center, New York New York Background. A retrospective review revealed a 42% error rate between computed tomographic scan reports and thoracotomy findings; therefore, a prospective study was designed to compare the value of computed tomographic scans, video-assisted thoracoscopic exploration, and open thoracotomy in the management of pulmonary metastases. Methods. Eligibility included any patient with only one or two ipsilateral pulmonary metastases identified on computed tomographic scan who was being considered for surgical resection. InitiaLly video-assisted thoracic surgery was performed and all lesions identified were resected. A thoracotomy adequate for complete lung palpation was then carried out and any additional lesions found were removed. Results. Eighteen patients of a planned 50 were treated before closure of the study. Four patients (22%) had no additional lesions found at thoracotomy. The primary sites of tumor were colon (10), breast (3), and one patient each skin (squamous), cervix, kidney, melanoma, and sarcoma. Four patients (22%) did have additional lesions at thoracotomy, which were benign. In the remaining 10 patients (56%) additional malignant lesions were found at thoracotomy after video-assisted thoracoscopic exploration. After 18 patients were entered, analysis of the early results disclosed a 56% failure rate of a computed tomographic scan and video-assisted thoracic surgery to detect all lesions. Being within the 95% confidence interval (32% to 78%), the study was abandoned. Conclusions. We conclude that video-assisted thoracic surgery should be used only as a diagnostic tool in managing lung metastasis. A thoracotomy is required to achieve complete resection, which is the major survival prognosticator for satisfactory long-term results. (Ann Thorac Surg 1996;62:213-7) p ulmonary metastases, when found as the only site of metastatic disease in patients where the primary tumor has been controlled, are often best treated by metastasectomy. The most consistent prognostic factor predicting survival has been complete surgical removal of all metastatic foci. When video-assisted thoracic surgery (VATS) was introduced, it was quickly adapted to metastasectomy. Concern was expressed by us that identification of all metastatic tumors to the lung might not be possible when the VATS technique is used, as manual palpation of the entire collapsed lung has been deemed essential. The use of a probe, or single digit might not su~ce as a substitute for the surgeon's hand [1]. Because the estimation of the number and location of metastases and planned operation is based on computed tomographic (CT) scan images, initially we retrospectively compared the radiologic findings with the surgical findings of 72 patients with primary colon cancer meta- Presented at the Thirty-second Annual Meeting of The Society of Thoracic Surgeons, Orlando, FL, January 29-31, Address reprint requests to Dr McCormack, 1275 York Ave, New York, NY static to lung [1]. Computed tomographic scans underestimated surgical findings in 42% (30 of 72 patients). In those with one or two lesions on the CT scan the "missed lesion rate" was 28%. To validate this retrospective review a prospective study was initiated to determine the accuracy of CT scan and video-assisted surgery as compared to open thoracotomy in identifying metastatic lesions in patients with no more than two presumed pulmonary metastases, believing that these would be the patients eligible for a VATS approach. Material and Methods Any patient who fit the general eligibility criteria for operation for lung metastases, and whose CT scan showed no more than two lesions in one lung was eligible. The selection criteria for metastasectomy are primary tumor under control; no tumor sites outside the lungs; CT scan demonstrates complete resectability; no better proven method of treatment is available; and medical condition allows planned resection. The prospective study was approved by the IRB (93-42) and informed consent was obtained from every patient. Operative decisions made by each surgeon were based 1996 by The Society of Thoracic Surgeons /96/$15.00 Published by Elsevier Science Inc PII S (96)
2 214 McCORMACK ET AL Ann Thorac Surg VATS VS THORACOTOMY IN METASTASECTOMY 1996;62: on scans carried out no more than 3 weeks before the planned operation. The o~icial radiologic report, consultation with radiology staff, and personal review of all imaging material by the surgeon were used for preoperative planning. All CT scans were performed with current generation scanners. Only two scans were obtained helically. Computed tomographic scans more than 3 weeks old or judged unreadable were repeated. The scans were reviewed subsequently by a single member of the Radiology Sta~ (D.M.P.). A data form was used to record the number and locations of all suspected lung nodules seen on lung windows. The degree of confidence in findings was graded on a 5-point scale (0 = normal; 1 = probably normal; 2 = indeterminate; 3 = probably abnormal; 4 = abnormal). Initially thoracoscopy was performed. Any lesion identiffed was resected using standard VATS techniques and instrumentation. Finger palpation and solid probes attempted to identify other nodules. Ultrasonography was not used. Under the same anesthetic a formal thoracotomy was then carried out to allow the surgeon to palpate the entire lung and resect any additional lesions found. All resected specimens were reviewed by one pathologist (M.Z.) and were confirmed to have been completely resected before closure. Results There was no mortality or morbidity in this group of patients and the average postoperative stay was 4.5 days. This was before "same-day admission" policy was in use. Eighteen patients were treated in this fashion before concluding the study. The primary sites were colon in 10 patients, breast in 3, squamous carcinoma of skin, leiomyosarcoma of uterus, cervix, kidney and melanoma were one patient each. In 14 patients, one lesion was noted on CT scan, and in 4 others, two lesions. In 15 patients, all nodules noted on preoperative scans were located at thoracoscopy. In 2 patients with a single lesion on the CT scan, no lesions were identified at the video-assisted procedure. In a third patient only one of two lesions was found and removed at thoracoscopy. All three "missing" lesions were ultimately found and removed at thoracotomy. They were not detectable at VATS because of their deep location and technical problems related to pleural adhesions. Only 22% of patients (4 of 18) had no new lesions found. In 22% (4 of 18) additional benign lesions were found at thoracotomy. In 56% of patients (10 of 18) additional malignant tumors were identified at thoracotomy (Fig 1). In only 1 patient was an additional lesion found at VATS. Of the 14 patients with solitary lesions on CT scan, 7 had additional malignant lesions found (14 nodules). In 3 additional patients five nodules were identified that were benign. In only 8 of 18 patients identified preoperatively as having no more than two ipsilateral lesions was the CT scan correct and confirmed by VATS. Benig 1o New 22.2'~ 22.2% Cancer 55.6% Fig 1. Results of pilot study in 18 patients. In two of the four "two-lesion" patients, only one lesion was found at thoracoscopy. The second malignancy was located at thoracotomy in both patients, one of which had three additional benign lesions discovered. In the other 2 patients both lesions were removed at VATS, but in both additional malignancies were identified and removed at thoracotomy (Table 1). In the single cases with skin, cervix, sarcoma and melanoma primaries, no additional malignant lesions were found at thoracotomy. Twelve of the CT scans were available for retrospective review (Table 2). In 7 of these (58%) our results show a misread, 3 overread, and 4 underread. Comment Pulmonary metastasectomy was first reported in the Scandinavian literature by Divis in 1927 [2] and subse- Table 1. Results of Study Primary Site Method of Discovery Pathology/ Thoracotomy CT scan VATS Thorascopy Cancer Benign Colon Colon Colon Rectal Colon Colon Colon Colon Colon Colon Breast Breast Breast Skin (squamous) Sarcoma (LMS) Cervix Renal Melanoma CT = computed tomography; LMS = leiomyosarcoma; VATS = video-assisted thoracic surgery.
3 Ann Thorac SLrrg McCORMACK ET AL ;62:213-7 VATS VS THORACOTOMY IN METASTASECTOMY Table 2. Retrospective Analysis of Computed Tomographic Scans (12 Scans) Total No. Total No. Primary Site at Operation by Radiologist Breast 3 3 Breast 2 2 Breast 1 1 Colon 8 2" Colon 3 7 b Colon 1 3 b Colon 1 1 Colon 3 2 a Colon 5 2 a Colon 2 I a Skin (squamous) 2 5 b Sarcoma 1 1 Underread; t, Overread. quently in North America by Barney and Churchill in 1939 [3]. However, by 1960, 264 cases of successful resection with long-term survival were reported [4]. In 1971 Martini and colleagues reported 29% 5-year survival rates in osteogenic sarcoma patients where none had survived 3 years before metastasectomy was begun [5, 6]. Multiple nodules were resected and multiple thoracotomies were required to achieve these results. Resection of pulmonary metastases is now the recognized standard of care for selected patients who meet specific criteria. Thoracotomy has been proven to be exceedingly safe with minimal morbidity and mortality [7]. Advanced surgical techniques, first median sternotomy [8] and later the clamshell incision [9] have also made bilateral resections at one operation a safe and efficient approach. This study was designed to compare VATS versus thoracotomy, which is best done with the lateral incision. Therefore, all these patients had thoracotomies. It is our practice to use the median sternotomy and clamshell approach when we are concerned about bilaterality. In sarcoma, with a solitary lesion, we do not explore both lungs. Video-assisted thoracic surgery was introduced as an approach offering a less painful incision, and a shorter hospital stay. It was quickly applied to the treatment of lung metastases [10]. Our initial retrospective study identiffed the potential problems of missing small metastatic lesions, resulting in the institution of this present prospective study. The prognostic significance of several variables in the presentation of these patients has been analyzed to improve the selection of potentially curable patients and avoid operation when it would not help the patient. These variables include length of tumor doubling time and disease-free interval, number of metastases, site of the primary tumor, and completeness of the pulmonary resection. All variables have had inconsistent prognostic significance except one: complete resection of all metastatic lesions [7]. After analyzing the results of the first 18 of a proposed 50-patient study, this protocol was closed to accrual because the estimated probability that cancer will be missed if VATS alone is used is 56% (95% confidence interval, 27% to 75%), and was sufficiently high to warrant termination of the study. Even for patients with only one lesion detected on CT the error rate is estimated to be 50% (95% confidence interval, 23% to 77%). The results of this prospective study are somewhat surprising but do confirm our retrospective analysis-- that in patients with solitary metastases and even more with two metastases--thoracotomy will frequently identify more malignant lesions. Our ability to identify these lesions with a VATS approach alone was less than satisfactory. It is unlikely that the higher accuracy found in the sites other than colorectal, breast, and kidney reflect anything but a sampling error. In this study CT scans were used from a wide variety of referring facilities and represents current clinical practice. It was not practical, due to cost and scheduling, to re-scan each patient with our own helical scanner. We acknowledge that this approach may underestimate the accuracy of CT that can be achieved by consistent, optimized CT technique and a dedicated radiologist comparing old films. It was the only pragmatic solution in our practice climate. In a prospective study of 39 patients, Remy-Jardin and colleagues [11] found 42% more nodules on helical CT scans as compared to conventional scanners. Increased identification of smaller nodules, however, lessens their specificity for being cancers [12]. Retrospective analysis as part of a study favors overreading and our results show a misread in the 7 of 12 patients we analyzed (58%) (Table 2). In conclusion, we firmly believe that metastasectomy has a proven efficacy in treating these stage IV patients with 5-year survival rates in our hands shown to be 80% in testicular primary, 50% in colon or breast, 60% in renal, 40% in osteosarcoma, 25% in soft tissue sarcoma and melanoma primary sites. Patients should be offered operation as an option when they fit the selection criteria. Therefore, we have concluded that the CT scan is not accurate in detecting all pulmonary metastases. The VATS technique as now practiced will fail to detect and remove all pulmonary metastases. Manual palpation of the lung is still required to locate all metastatic foci. Video-assisted thoracic surgery should be used for diagnosis only in metastasectomy. Until newer imaging and localization techniques allow a greater accuracy for the VATS approach, thoracotomy and manual palpation must remain the gold standard in treating even solitary pulmonary metastases. References 1. McCormack PM, Ginsberg KB, Bains MS, et al. Accuracy of lung imaging in metastases with implications for the role of thoracoscopy. Ann Thorac Surg 1993;56: Divis G. Einbertrag zur operativen, behandlung der lungengschuuilste. Acta Chit Scand 1927;62: Barney JD, Churchill ET. Adenocarcinoma of the kidney with metastasis to the lung cured by nephrectomy and lobectomy. J Urol 1939;42:
4 216 McCORMACK ET AL Ann Thorac Surg VATS VS THORACOTOMY IN METASTASECTOMY 1996;62: Gliedman M, Horowitz S, Lewis FJ. Lung resection for metastatic cancer. Surgery 1957;42: Marcove RC, Mike V, Hajek JV, et al. Osteogenic sarcoma under the age of 21: a review of 145 operative cases. J Bone Joint Surg (Am) 1970;51: Martini N, Huvos AG, Mike V, et al. Multiple pulmonary resections in the treatment of osteogenic sarcoma. Ann Thorac Surg 1971;12: McCormack PM, Martini N. A current view of surgical management of pulmonary metastases. In: Economou S, eel Adjuncts to cancer therapy. Philadelphia: Lea & Febiger, 1991: Johnston MR. Median sternotomy for resection of pulmonary metastases. J Thorac Cardiovasc Surg 1983;85: Bains MS, Ginsberg RJ, Jones WG III, et al. The clamshell incision: an improved approach to bilateral pulmonary and mediastinal tumor. Ann Thorac Surg 1994;58: Landreneau RJ, Hazelrigg SR, Ferson PF, et ai. Thoracoscopic resection of 85 pulmonary lesions. Ann Thorac Surg 1992;54: Remy-Jardin M, Remy J, Giraud F, Marquette C-H. Pulmonary nodules: detection with thick-section spiral CT versus conventional CT. Radiology 1993;187: Chang AE, Schaner EG, Conkle DM, Flye MW, Dappman JL, Rosenberg SA. Evaluation of computed tomography in the detection of pulmonary metastases: a prospective study. Cancer 1994;43: DISCUSSION DR MICHAEL J. MACK (Dallas, TX): I congratulate Dr McCormack on conducting this pilot study. I also congratulate her on the occasion of her retirement and acknowledge the valuable contributions she has made to the field of thoracic oncology throughout her career. This specialty is more enlightened because of her contributions. I also appreciate her providing me with a manuscript for review before this meeting. My discussion will focus on two aspects of the presentation: (1) the incisions used and (2) the accuracy of computed tomographic (CT) scanning. As Dr McCormack has alluded to, completeness of resection of all metastatic disease has been said to have positive prognostic significance. Because it is known that up to 45% of patients thought to have unilateral disease by CT scan will in fact have bilateral disease, why then did you not take this concept of complete resection to its logical conclusion and perform a sternotomy or clamshell incision rather than a thora -~ cotomy after video-assisted thoracic surgery (VATS) so that the contralateral lung could also be examined by palpation? The second point is regarding the sensitivity of CT scanning for detecting metastatic lesions. I agree that because surgeons using VATS for resection lose the ability to palpate manually the lung, one is totally dependent on the accuracy of the preoperative CT scan to detect occult nodules. In Dr McCormack's series 78% of patients had additional lesions detected at thoracotomy not imaged on the preoperative CT scan. Unfortunately, 16 of the 18 patients had CT scans performed on old generation scanners rather than on spiral or ultrafast CT scans. In our experience with the newer scans, the problem is not a lack of sensitivity but rather too much sensitivity resulting in detection of nodules as small as 2 mm. A 2-mm nodule on an ultrafast CT scan in a patient with a history of bronchoalveolar carcinoma proved to be a metastatic lesion. However, in a spiral CT scan, in a patient with a history of breast cancer, we saw a 6-mm subpleural nodule. This patient underwent a VATS resection after needle localization. The nodule could not be palpated even in the resected specimen but was found to be a caseous granuloma by frozen section. The results of nodules detected by spiral or ultrafast CT scans and resected by VATS in our institution in 1995 in patients with a recent history of cancer showed that one-third of patients had benign disease, including subpleural lymph nodes, hamartomas, and granulomas. Therefore, I would argue that because of the oversensitivity of the new generation scanners in detecting 2- to 3-mm nodules that cannot be palpated even when the specimen is in the surgeon's hand and because of the higher incidence of benign disease in these small lesions, VATS should have an enhanced rather than a diminished role. My questions for Dr McCormack, therefore, are: (1) Why did you choose a thoracotomy rather than a sternotomy or clamshell incision as a follow-up to VATS? (2) Has there been any evidence of recurrence especially in the contralateral lung in these patients? (3) Do you believe that the study should now be repeated with newer, more sensitive spiral and ultrafast CT scans? DR RODNEY J. LANDRENEAU (Pittsburgh, PA): I also enjoyed Dr McCormack's presentation and congratulate her for her contributions during her career. My comments regarding this presentation are both conceptual and technical. With regard to the concept of complete resection as being a primary prognostic factor with metastasectomy, I believe this is quite a sticky issue and it is vital that we all review the literature carefully when looking at the role of metastasectomy of metastatic lesions to the lung. Many earlier reports mix wedge resection of peripheral solitary metastases with cases of exploratory thoracotomy and aborted resection of bulky disease. Certainly the biology of the metastatic disease in these scenarios is quite different, yet broad statements regarding survival after metastasectomy are frequently made. The accuracy of both VATS and thoracotomy approaches to metastasectomy is limited in that we know that 75% to 80% of all patients will die of their systemic process. But we also know that the use of thoracotomy and aggressive resection commonly results in unnecessary resection of benign lesions and the loss of pulmonary parenchyma. I believe that this is a lot to ask of a patient who is likely to manifest later pulmonary lesions and possible pulmonary compromise from the recurrent malignant process. The indication for VATS wedge resection of pulmonary parenchymal lesions is quite specific. It should be directed toward small peripheral lesions that can be encompassed by complete resection of the lesion. There should be no endobr0nchial extension of the disease, and finally, we must always remember that conversion of thoracotomy is necessary when the lesions identified by CT scan cannot be found. I end by saying that metastasectomy done by thoracotomy or VATS is in almost all circumstances diagnostic only. We must remember that our first duty to our patients suffering from the spread of their primary malignancy is to do no harm. In the case of metastasectomy, we must be careful to avoid chasing the tail of their systemic disease. DR RALPH J. LEWIS (New Brunswick, NJ): I too congratulate Dr McCormack on her retirement and, actually, a very fine and interesting presentation that was almost convincing. The literature is very confusing, contradictory, and, at best, anecdotal for curative, surgical resection of multiple, epithelial, pulmonary metastases, and I emphasize epithelial metastases.
5 Ann Thorac Surg McCORMACK ET AL ;62.'213-7 VATS VS THORACOTOMY IN METASTASECTOMY We have never had such enthusiasm for this procedure because of consistent and even predictable poor outcomes, but for those surgeons persuaded that this can be a curative operation, VATS could still be beneficial. It can be used bilaterally at the same sitting, and it even mandates a no-touch, oncologic technique, avoiding the implied release of showers of malignant cells into the bloodstream from extensive palpation. I would just like to say a word or two about the CT scan. It can diagnose very, very small parenchymal lesions, 2 to 3 mm in size. Maybe some lesions so small that they cannot be delineated by palpation alone. As we know, many metastases occur in the periphery of the lung and even on the visceral pleural surface. My radiologists have informed me that these small surface lesions are not detected accurately by the CT scan, and they can be easily missed. Therefore the CT scan, by itself, can only be expected to visualize a portion of the true number of metastases present. This might explain the disparity in trying to count lesions preoperatively, and the number that is actually removed at operation. If we use the magnification of the VATS endoscope, possibly, some very small surface lesions, that could not be seen by the naked eye alone might be detected. Therefore by combining these two technologies, magnification of VATS with the CT scan, probably, we could get a more realistic evaluation. I would like to ask two or three questions. First, are you really repudiating the no-touch, oncologic technique for neoplasms and instead advocating an extensive, compressive, palpation method that could cause the release of malignant cells into the bloodstream? And second, we have all been told that wedge resection is really not an oncologic operation, at least for that very small peripheral, primary, T1 NO lesion, and yet, you seem to be sanctioning wedge resection for bilateral, multiple, large lesions of varying sizes. Also, I am confused because you are performing only unilateral thoracotomies. Why are you accepting the CT scan as being accurate and reliable for metastasis to the contralateral lung? In the literature, some patients have had two, three, and four separate thoracotomies for newly appearing metastases. For these particular patients, would not VATS be more appropriate, kinder, gentler and even more humane? Finally, once again, I congratulate you on your many contributions and wish you a long and very happy retirement. DR McCORMACK: I thank all of the discussers for their kind remarks, especially Michael Mack. And as everything seems to be focused around the same points, let me just say I think Ralph Lewis summed it up probably best: Those who are enthusiastic for this approach to treat metastatic cancer should do so. Those who are not enthusiastic about this approach for metastatic cancer should not do this type of operation. As for incisions, we selected a thoracotomy because it was part of the methodology of this study. Practically speaking, most of us now are much more liberal with the use of a median sternotomy or a clamshell incision to get all of the lesions out bilaterally at the first operation. Recurrences have been found in either lung, the operated lung or the opposite lung. I cannot report on this particular study, it is too short, but our experience over 40 years has been that recurrence is unpredictable. Surface lesions are those that would be picked up, Dr Lewis, by the video, the VATS technique, very nicely. What we have found in this study is that most of the additional lesions are deeply situated in the lung and are not on the surface. The proper selection of patients is used in the criteria selection for each patient. This would weed out those patients who would not profit by another surgical procedure to extend their life. In most of our metastasectomy selections, we have discovered that nothing else works for these patients. Just as an example, in colon metastases, nobody survives beyond 24 months with chemotherapy, and we have a 5-year survival of 50%. This is indeed a technique worth doing, and I think for the sake of the patients it should be offered to them. Cancers that are metastatic to the lung we found grow differently from primary lung cancers; therefore, a wedge resection is an adequate surgical technique. We have not found that by carefully palpating a collapsed lung we have spread cancer cells. Bound volumes available to subscribers Bound volumes of the 1995 issues of The Annals of Thoracic Surgery are available only to subscribers from the Publisher. The cost is $99.00 (outside US add $25.00 for postage) for volumes 59 and 60. Each bound volume contains a subject and author index, and all advertising is removed. The binding is durable buckram with the name of the journal volume number, and year stamped on the spine. Payment must accompany all orders. Contact Elsevier Science Inc, 655 Avenue of the Americas, New York, NY 10010; or telephone (212) (facsimile: (212) ).
Surgical Approaches to Pulmonary Metastases
 Surgical Approaches to Pulmonary Metastases Raja M Flores MD Professor and Chief Thoracic Surgery Mount Sinai School of Medicine New York, New York History of Lung Metastasectomy 1882 Weinlechner +CW 1926
Surgical Approaches to Pulmonary Metastases Raja M Flores MD Professor and Chief Thoracic Surgery Mount Sinai School of Medicine New York, New York History of Lung Metastasectomy 1882 Weinlechner +CW 1926
VATS Metastasectomy. Inderpal (Netu) S. Sarkaria, MD, FACS
 VATS Metastasectomy Inderpal (Netu) S. Sarkaria, MD, FACS Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Disclosures Speaking & Education:
VATS Metastasectomy Inderpal (Netu) S. Sarkaria, MD, FACS Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Disclosures Speaking & Education:
Surgical Management of Pulmonary Metastases. Dr AG Jacobs Principal Specialist Dept Cardiothoracic Surgery Steve Biko Academic Hospital
 Surgical Management of Pulmonary Metastases Dr AG Jacobs Principal Specialist Dept Cardiothoracic Surgery Steve Biko Academic Hospital Introduction Lungs 2 nd most common site of metastatic deposition
Surgical Management of Pulmonary Metastases Dr AG Jacobs Principal Specialist Dept Cardiothoracic Surgery Steve Biko Academic Hospital Introduction Lungs 2 nd most common site of metastatic deposition
Value of Systematic Mediastinal Lymph Node Dissection During Pulmonary Metastasectomy
 Value of Systematic Mediastinal Lymph Node Dissection During Pulmonary Metastasectomy Florian Loehe, MD, Sonja Kobinger, MD, Rudolf A. Hatz, MD, Thomas Helmberger, MD, Udo Loehrs, MD, and Heinrich Fuerst,
Value of Systematic Mediastinal Lymph Node Dissection During Pulmonary Metastasectomy Florian Loehe, MD, Sonja Kobinger, MD, Rudolf A. Hatz, MD, Thomas Helmberger, MD, Udo Loehrs, MD, and Heinrich Fuerst,
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER
 MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
CASE REPORT. Introduction. Case series reports. J Thorac Dis 2012;4(S1): DOI: /j.issn s003
 CASE REPORT Lost in time pulmonary metastases of renal cell carcinoma: complete surgical resection of metachronous metastases, 18 and 15 years after nephrectomy Kosmas Tsakiridis 1, Aikaterini N Visouli
CASE REPORT Lost in time pulmonary metastases of renal cell carcinoma: complete surgical resection of metachronous metastases, 18 and 15 years after nephrectomy Kosmas Tsakiridis 1, Aikaterini N Visouli
After primary tumor treatment, 30% of patients with malignant
 ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
Accepted Manuscript. Preoperative CEA in Patients with Colorectal Metastases Matters. Benny Weksler, MBA, MD
 Accepted Manuscript Preoperative CEA in Patients with Colorectal Metastases Matters Benny Weksler, MBA, MD PII: S0022-5223(19)30068-6 DOI: https://doi.org/10.1016/j.jtcvs.2019.01.016 Reference: YMTC 14019
Accepted Manuscript Preoperative CEA in Patients with Colorectal Metastases Matters Benny Weksler, MBA, MD PII: S0022-5223(19)30068-6 DOI: https://doi.org/10.1016/j.jtcvs.2019.01.016 Reference: YMTC 14019
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Surgical Treatment for Pulmonary Me. Tsunehisa; Kugimiya, Toshiyasu. Citation Acta medica Nagasakiensia. 1983, 28
 NAOSITE: Nagasaki University's Ac Title Author(s) Surgical Treatment for Pulmonary Me Ayabe, Hiroyoshi; Tomita, Masao; Na Katsunobu; Nakao, Susumu; Eguchi, M Tsunehisa; Kugimiya, Toshiyasu Citation Acta
NAOSITE: Nagasaki University's Ac Title Author(s) Surgical Treatment for Pulmonary Me Ayabe, Hiroyoshi; Tomita, Masao; Na Katsunobu; Nakao, Susumu; Eguchi, M Tsunehisa; Kugimiya, Toshiyasu Citation Acta
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
May-Lin Wilgus. A. Study Purpose and Rationale
 Utility of a Computer-Aided Diagnosis Program in the Evaluation of Solitary Pulmonary Nodules Detected on Computed Tomography Scans: A Prospective Observational Study May-Lin Wilgus A. Study Purpose and
Utility of a Computer-Aided Diagnosis Program in the Evaluation of Solitary Pulmonary Nodules Detected on Computed Tomography Scans: A Prospective Observational Study May-Lin Wilgus A. Study Purpose and
Carcinoma of the Lung
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
Results of thoracotomy in osteogenic sarcoma
 Thorax 1991;46:727-731 Bone Tumour Treatment Service, Royal Orthopaedic Hospital, Birmingham B31 2AP S R Carter R J Grimer R S Sneath Thoracic Surgery Unit, East Birmingham Hospital, Birmingham B9 SST
Thorax 1991;46:727-731 Bone Tumour Treatment Service, Royal Orthopaedic Hospital, Birmingham B31 2AP S R Carter R J Grimer R S Sneath Thoracic Surgery Unit, East Birmingham Hospital, Birmingham B9 SST
PET IMAGING (POSITRON EMISSION TOMOGRAPY) FACT SHEET
 Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Pulmonary resection for metastatic colorectal carcinoma was first performed
 General Thoracic Surgery Pulmonary metastasectomy for 165 patients with colorectal carcinoma: A prognostic assessment Yukihito Saito, MD, a Hideyasu Omiya, MD, a Keijiro Kohno, MD, b Takanobu Kobayashi,
General Thoracic Surgery Pulmonary metastasectomy for 165 patients with colorectal carcinoma: A prognostic assessment Yukihito Saito, MD, a Hideyasu Omiya, MD, a Keijiro Kohno, MD, b Takanobu Kobayashi,
Germ cell tumors (GCT) are uncommon neoplasms
 ORIGINAL ARTICLES: GENERAL THORACIC Pulmonary Metastasectomy for Testicular Germ Cell Tumors: A 28-Year Experience David Liu, MD, Amir Abolhoda, MD, Michael E. Burt, MD, PhD, Nael Martini, MD, Manjit S.
ORIGINAL ARTICLES: GENERAL THORACIC Pulmonary Metastasectomy for Testicular Germ Cell Tumors: A 28-Year Experience David Liu, MD, Amir Abolhoda, MD, Michael E. Burt, MD, PhD, Nael Martini, MD, Manjit S.
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer
 Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
sarcoma Reprint requests: Dr M H Robinson, YCRC Senior Lecturer Clinical Oncology, Weston Park Hospital, Whitham Road, Sheffield S10 2SJ.
 1994, The British Journal of Radiology, 67, 129-135 Lung metastasectomy sarcoma in patients with soft tissue 1 M H ROBINSON, MD, MRCP, FRCR, 2 M SHEPPARD, FRCPATH, 3 E MOSKOVIC, MRCP, FRCR and 4 C FISHER,
1994, The British Journal of Radiology, 67, 129-135 Lung metastasectomy sarcoma in patients with soft tissue 1 M H ROBINSON, MD, MRCP, FRCR, 2 M SHEPPARD, FRCPATH, 3 E MOSKOVIC, MRCP, FRCR and 4 C FISHER,
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule
 Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
came from a carcinoma and in 12 from a sarcoma. Ninety lesions were intrapulmonary and the as the chest wall and pleura. Details of the primary
 Thorax 1982;37:366-370 Thoracic metastases MARY P SHEPHERD From the Thoracic Surgical Unit, Harefield Hospital, Harefield ABSTRACI One hundred and four patients are reviewed who were found to have thoracic
Thorax 1982;37:366-370 Thoracic metastases MARY P SHEPHERD From the Thoracic Surgical Unit, Harefield Hospital, Harefield ABSTRACI One hundred and four patients are reviewed who were found to have thoracic
Lung Cancer. Current Therapy JEREMIAH MARTIN MBBCh FRCSI MSCRD
 Lung Cancer Current Therapy JEREMIAH MARTIN MBBCh FRCSI MSCRD Objectives Describe risk factors, early detection & work-up of lung cancer. Define the role of modern treatment options, minimally invasive
Lung Cancer Current Therapy JEREMIAH MARTIN MBBCh FRCSI MSCRD Objectives Describe risk factors, early detection & work-up of lung cancer. Define the role of modern treatment options, minimally invasive
Accuracy of Helical CT in the Detection of Pulmonary Metastases: Is Intraoperative Palpation Still Necessary?
 Accuracy of Helical CT in the Detection of Pulmonary Metastases: Is Intraoperative Palpation Still Necessary? Alden M. Parsons, MD, Frank C. Detterbeck, MD, and Leonard A. Parker, MD Department of Surgery,
Accuracy of Helical CT in the Detection of Pulmonary Metastases: Is Intraoperative Palpation Still Necessary? Alden M. Parsons, MD, Frank C. Detterbeck, MD, and Leonard A. Parker, MD Department of Surgery,
MEDIASTINAL STAGING surgical pro
 MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
Pulmonary Resection for Metastases from Colorectal Cancer
 ORIGINAL ARTICLE Pulmonary Resection for Metastases from Colorectal Cancer Paul M. van Schaik, MD,* Ewout A. Kouwenhoven, MD, PhD,* Robert J. Bolhuis, MD,* Bonne Biesma, MD, PhD, and Koop Bosscha, MD,
ORIGINAL ARTICLE Pulmonary Resection for Metastases from Colorectal Cancer Paul M. van Schaik, MD,* Ewout A. Kouwenhoven, MD, PhD,* Robert J. Bolhuis, MD,* Bonne Biesma, MD, PhD, and Koop Bosscha, MD,
Treatment of oligometastatic NSCLC
 Treatment of oligometastatic NSCLC Jarosław Kużdżał Department of Thoracic Surgery Jagiellonian University Collegium Medicum, John Paul II Hospital, Cracow New idea? 14 NSCLC patients with solitary extrathoracic
Treatment of oligometastatic NSCLC Jarosław Kużdżał Department of Thoracic Surgery Jagiellonian University Collegium Medicum, John Paul II Hospital, Cracow New idea? 14 NSCLC patients with solitary extrathoracic
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Ablative therapy, nonsurgical, for pulmonary metastases of soft tissue sarcoma, 279 280 Adipocytic tumors, atypical lipomatous tumor vs. well-differentiated
Note: Page numbers of article titles are in boldface type. A Ablative therapy, nonsurgical, for pulmonary metastases of soft tissue sarcoma, 279 280 Adipocytic tumors, atypical lipomatous tumor vs. well-differentiated
OBJECTIVES. Solitary Solid Spiculated Nodule. What would you do next? Case Based Discussion: State of the Art Management of Lung Nodules.
 Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
ORIGINAL ARTICLE. Transxiphoid Bilateral Palpation in Video-Assisted Thoracoscopic Lung Metastasectomy
 ORIGINAL ARTICLE Transxiphoid Bilateral Palpation in Video-Assisted Thoracoscopic Lung Metastasectomy Tommaso Claudio Mineo, MD; Vincenzo Ambrogi, MD; Marcello Paci, MD; Nicola Iavicoli, MD; Eugenio Pompeo,
ORIGINAL ARTICLE Transxiphoid Bilateral Palpation in Video-Assisted Thoracoscopic Lung Metastasectomy Tommaso Claudio Mineo, MD; Vincenzo Ambrogi, MD; Marcello Paci, MD; Nicola Iavicoli, MD; Eugenio Pompeo,
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
GENERAL THORACIC SURGERY
 GENERAL THORACIC SURGERY VIDEO-ASSISTED THORACIC SURGICAL RESECTION WITH THE NEODYMIUM:YTTRIUM- ALUMINUM-GARNET LASER Since January 1991, we have performed 79 video-assisted neodymium: yttrium-aluminum-garnet
GENERAL THORACIC SURGERY VIDEO-ASSISTED THORACIC SURGICAL RESECTION WITH THE NEODYMIUM:YTTRIUM- ALUMINUM-GARNET LASER Since January 1991, we have performed 79 video-assisted neodymium: yttrium-aluminum-garnet
Video-assisted thoracic surgery (VATS) for resection of metastatic adenocarcinoma as an acceptable alternative
 Surg Endosc (2009) 23:1947 1954 DOI 10.1007/s00464-008-0243-z Video-assisted thoracic surgery (VATS) for resection of metastatic adenocarcinoma as an acceptable alternative Marilee Carballo Æ Mary S. Maish
Surg Endosc (2009) 23:1947 1954 DOI 10.1007/s00464-008-0243-z Video-assisted thoracic surgery (VATS) for resection of metastatic adenocarcinoma as an acceptable alternative Marilee Carballo Æ Mary S. Maish
Thoracic Surgery; An Overview
 Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
In the past, pulmonary metastases (PM) were considered
 Original Article The Role of Extended Pulmonary Metastasectomy Monica Casiraghi, MD,* Patrick Maisonneuve, Eng, Daniela Brambilla, Msc,* Francesco Petrella, MD,* Piergiorgio Solli, MD,* Juliana Guarize,
Original Article The Role of Extended Pulmonary Metastasectomy Monica Casiraghi, MD,* Patrick Maisonneuve, Eng, Daniela Brambilla, Msc,* Francesco Petrella, MD,* Piergiorgio Solli, MD,* Juliana Guarize,
Pulmonary laser resections: Technical aspects and results in colorectal cancer
 Pulmonary laser resections: Technical aspects and results in colorectal cancer Bernward Passlick Professor of Thoracic Surgery Dept. of Thoracic Surgery University of Freiburg Germany Pulmonary laser resections
Pulmonary laser resections: Technical aspects and results in colorectal cancer Bernward Passlick Professor of Thoracic Surgery Dept. of Thoracic Surgery University of Freiburg Germany Pulmonary laser resections
Prognostic value of visceral pleura invasion in non-small cell lung cancer q
 European Journal of Cardio-thoracic Surgery 23 (2003) 865 869 www.elsevier.com/locate/ejcts Prognostic value of visceral pleura invasion in non-small cell lung cancer q Jeong-Han Kang, Kil Dong Kim, Kyung
European Journal of Cardio-thoracic Surgery 23 (2003) 865 869 www.elsevier.com/locate/ejcts Prognostic value of visceral pleura invasion in non-small cell lung cancer q Jeong-Han Kang, Kil Dong Kim, Kyung
Vienna General Hospital, 1090 Wien, Austria. Key words: Radiology; Computed tomography; Pulmonary nodules; Pediatric; Cancer; Osteosarcoma; Chest
 Journal of Pediatric Surgery (2011) 46, 729 735 www.elsevier.com/locate/jpedsurg Do characteristics of pulmonary nodules on computed tomography in children with known osteosarcoma help distinguish whether
Journal of Pediatric Surgery (2011) 46, 729 735 www.elsevier.com/locate/jpedsurg Do characteristics of pulmonary nodules on computed tomography in children with known osteosarcoma help distinguish whether
Management of Lung Metastases from Colorectal Cancer: Video-Assisted Thoracoscopic Surgery versus Thoracotomy A Case-Matched Study
 98 Original Thoracic Management of Lung Metastases from Colorectal Cancer: Video-Assisted Thoracoscopic Surgery versus Thoracotomy A Case-Matched Study Yin-Kai Chao 1 Hao-Cheng Chang 2 Yi-Cheng Wu 1 Yun-hen
98 Original Thoracic Management of Lung Metastases from Colorectal Cancer: Video-Assisted Thoracoscopic Surgery versus Thoracotomy A Case-Matched Study Yin-Kai Chao 1 Hao-Cheng Chang 2 Yi-Cheng Wu 1 Yun-hen
LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG
 LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Takehiro Watanabe, MD a Yuzo Kurita, MD b Akira Yokoyama, MD b Keiichi
LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Takehiro Watanabe, MD a Yuzo Kurita, MD b Akira Yokoyama, MD b Keiichi
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
The pathophysiology of pulmonary metastases is initiated
 Surgical Management of Pulmonary Metastases Loretta Erhunmwunsee, MD, and Thomas A. D Amico, MD Department of Surgery, Duke University Medical Center, Durham, North Carolina Metastasectomy is the only
Surgical Management of Pulmonary Metastases Loretta Erhunmwunsee, MD, and Thomas A. D Amico, MD Department of Surgery, Duke University Medical Center, Durham, North Carolina Metastasectomy is the only
The lungs are the second most frequent site for metastases
 Prognostic Factors for Survival After Pulmonary Resection of Metastatic Renal Cell Carcinoma Joachim Pfannschmidt, MD, Hans Hoffmann, MD, PhD, Thomas Muley, PhD, Sabine Krysa, MD, Christine Trainer, MD,
Prognostic Factors for Survival After Pulmonary Resection of Metastatic Renal Cell Carcinoma Joachim Pfannschmidt, MD, Hans Hoffmann, MD, PhD, Thomas Muley, PhD, Sabine Krysa, MD, Christine Trainer, MD,
When a solitary pulmonary lesion (SPL) is found in
 GENERAL THORACIC Resection of Solitary Pulmonary Lesion Is Beneficial to Patients With a History of Malignancy Miki Sakamoto, MD, Tomohiro Murakawa, MD, Kentaro Kitano, MD, Tomonori Murayama, MD, Takehiro
GENERAL THORACIC Resection of Solitary Pulmonary Lesion Is Beneficial to Patients With a History of Malignancy Miki Sakamoto, MD, Tomohiro Murakawa, MD, Kentaro Kitano, MD, Tomonori Murayama, MD, Takehiro
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Site of Recurrence in Patients. of the Lung Resected for Cure. with Stages I and I1 Carcinoma
 Site of Recurrence in Patients with Stages I and I1 Carcinoma of the Lung Resected for Cure Steven C. Immerman, M.D., Robert M. Vanecko, M.D., Willard A. Fry, M.D., Louis R. Head, M.D., and Thomas W. Shields,
Site of Recurrence in Patients with Stages I and I1 Carcinoma of the Lung Resected for Cure Steven C. Immerman, M.D., Robert M. Vanecko, M.D., Willard A. Fry, M.D., Louis R. Head, M.D., and Thomas W. Shields,
The Importance of One-Stage Median Stemotomy and Retroperitoneal Node Dissection in Disseminated Testicular Cancer
 The Importance of One-Stage Median Stemotomy and Retroperitoneal Node Dissection in Disseminated Testicular Cancer Isidore Mandelbaum, M.D., Peter B. Yaw, M.D., Lawrence H. Einhorn, M.D., Stephen D. Williams,
The Importance of One-Stage Median Stemotomy and Retroperitoneal Node Dissection in Disseminated Testicular Cancer Isidore Mandelbaum, M.D., Peter B. Yaw, M.D., Lawrence H. Einhorn, M.D., Stephen D. Williams,
Treatment of Clinical Stage I Lung Cancer: Thoracoscopic Lobectomy is the Standard
 Treatment of Clinical Stage I Lung Cancer: Thoracoscopic Lobectomy is the Standard AATS General Thoracic Surgery Symposium May 5, 2010 Thomas A. D Amico MD Professor of Surgery, Duke University Medical
Treatment of Clinical Stage I Lung Cancer: Thoracoscopic Lobectomy is the Standard AATS General Thoracic Surgery Symposium May 5, 2010 Thomas A. D Amico MD Professor of Surgery, Duke University Medical
Guide to Understanding Lung Cancer
 Guide to Understanding Lung Cancer Lung cancer is the second most common cancer overall for men and women in the U.S., with an estimated 222,500 new cases in 2017. However, lung cancer is the most common
Guide to Understanding Lung Cancer Lung cancer is the second most common cancer overall for men and women in the U.S., with an estimated 222,500 new cases in 2017. However, lung cancer is the most common
The Spectrum of Management of Pulmonary Ground Glass Nodules
 The Spectrum of Management of Pulmonary Ground Glass Nodules Stanley S Siegelman CT Society 10/26/2011 No financial disclosures. Noguchi M et al. Cancer 75: 2844-2852, 1995. 236 surgically resected peripheral
The Spectrum of Management of Pulmonary Ground Glass Nodules Stanley S Siegelman CT Society 10/26/2011 No financial disclosures. Noguchi M et al. Cancer 75: 2844-2852, 1995. 236 surgically resected peripheral
Charles Mulligan, MD, FACS, FCCP 26 March 2015
 Charles Mulligan, MD, FACS, FCCP 26 March 2015 Review lung cancer statistics Review the risk factors Discuss presentation and staging Discuss treatment options and outcomes Discuss the status of screening
Charles Mulligan, MD, FACS, FCCP 26 March 2015 Review lung cancer statistics Review the risk factors Discuss presentation and staging Discuss treatment options and outcomes Discuss the status of screening
Surgical Management of Advanced Stage Colon Cancer. Nathan Huber, MD 6/11/14
 Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Surgical resection of pulmonary metastases is an established
 Long-Term Results After Pulmonary Resection of Renal Cell Carcinoma Metastases Stefan Piltz, MD, Georgios Meimarakis, MD, Matthias W. Wichmann, MD, Rudolf Hatz, MD, Friedrich Wilhelm Schildberg, MD, and
Long-Term Results After Pulmonary Resection of Renal Cell Carcinoma Metastases Stefan Piltz, MD, Georgios Meimarakis, MD, Matthias W. Wichmann, MD, Rudolf Hatz, MD, Friedrich Wilhelm Schildberg, MD, and
Mediastinal Staging. Samer Kanaan, M.D.
 Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Cytologically Malignant Margins of Wedge Resected Stage I Non-Small Cell Lung Cancer
 Cytologically Malignant Margins of Wedge Resected Stage I Non-Small Cell Lung Cancer Noriyoshi Sawabata, MD, Akihide Matsumura, MD, Mitsunori Ohota, MD, Hajime Maeda, MD, Hiroshi Hirano, MD, Katsuhiro
Cytologically Malignant Margins of Wedge Resected Stage I Non-Small Cell Lung Cancer Noriyoshi Sawabata, MD, Akihide Matsumura, MD, Mitsunori Ohota, MD, Hajime Maeda, MD, Hiroshi Hirano, MD, Katsuhiro
Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication for Repeat Metastasectomy
 Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
Aggressive Slurgical Management of Testicular Carcinoma Metastatic to Lungs and Mediastinurn
 Aggressive Slurgical Management of Testicular Carcinoma Metastatic to Lungs and Mediastinurn Isadore Mandelbaum, M.D., Stephen D. Williams, M.D., and Lawrence H. Einhorn, M.D. ABSTRACT During the past
Aggressive Slurgical Management of Testicular Carcinoma Metastatic to Lungs and Mediastinurn Isadore Mandelbaum, M.D., Stephen D. Williams, M.D., and Lawrence H. Einhorn, M.D. ABSTRACT During the past
Metachronic solitary breast metastasis from renal cell carcinoma: case report
 Metachronic solitary breast metastasis from renal cell carcinoma: case report Abstract We describe the case of a patient with solitary and metachronic breast metastasis, 3 years after nephrectomy for renal
Metachronic solitary breast metastasis from renal cell carcinoma: case report Abstract We describe the case of a patient with solitary and metachronic breast metastasis, 3 years after nephrectomy for renal
Lung. 10/24/13 Chest X-ray: 2.9 cm mass like density in the inferior lingular segment worrisome for neoplasm. Malignancy cannot be excluded.
 Lung Case Scenario 1 A 54 year white male presents with a recent abnormal CT of the chest. The patient has a history of melanoma, kidney, and prostate cancers. 10/24/13 Chest X-ray: 2.9 cm mass like density
Lung Case Scenario 1 A 54 year white male presents with a recent abnormal CT of the chest. The patient has a history of melanoma, kidney, and prostate cancers. 10/24/13 Chest X-ray: 2.9 cm mass like density
Treatment Strategy for Patients With Surgically Discovered N2 Stage IIIA Non-Small Cell Lung Cancer
 Treatment Strategy for Patients With Surgically Discovered N2 Stage IIIA Non-Small Cell Lung Cancer Ryoichi Nakanishi, MD, Toshihiro Osaki, MD, Kozo Nakanishi, MD, Ichiro Yoshino, MD, Takashi Yoshimatsu,
Treatment Strategy for Patients With Surgically Discovered N2 Stage IIIA Non-Small Cell Lung Cancer Ryoichi Nakanishi, MD, Toshihiro Osaki, MD, Kozo Nakanishi, MD, Ichiro Yoshino, MD, Takashi Yoshimatsu,
Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis
 ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
P sumed to have early lung disease with a favorable
 Survival After Resection of Stage I1 Non-Small Cell Lung Cancer Nael Martini, MD, Michael E. Burt, MD, PhD, Manjit S. Bains, MD, Patricia M. McCormack, MD, Valerie W. Rusch, MD, and Robert J. Ginsberg,
Survival After Resection of Stage I1 Non-Small Cell Lung Cancer Nael Martini, MD, Michael E. Burt, MD, PhD, Manjit S. Bains, MD, Patricia M. McCormack, MD, Valerie W. Rusch, MD, and Robert J. Ginsberg,
4/22/2010. Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey.
 Management of Differentiated Thyroid Cancer: Head Neck Surgeon Perspective Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey Thyroid gland Small endocrine gland:
Management of Differentiated Thyroid Cancer: Head Neck Surgeon Perspective Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey Thyroid gland Small endocrine gland:
Surgical resection is the first treatment of choice for
 Predictors of Lymph Node and Intrapulmonary Metastasis in Clinical Stage IA Non Small Cell Lung Carcinoma Kenji Suzuki, MD, Kanji Nagai, MD, Junji Yoshida, MD, Mitsuyo Nishimura, MD, and Yutaka Nishiwaki,
Predictors of Lymph Node and Intrapulmonary Metastasis in Clinical Stage IA Non Small Cell Lung Carcinoma Kenji Suzuki, MD, Kanji Nagai, MD, Junji Yoshida, MD, Mitsuyo Nishimura, MD, and Yutaka Nishiwaki,
Although the international TNM classification system
 Prognostic Significance of Perioperative Serum Carcinoembryonic Antigen in Non-Small Cell Lung Cancer: Analysis of 1,000 Consecutive Resections for Clinical Stage I Disease Morihito Okada, MD, PhD, Wataru
Prognostic Significance of Perioperative Serum Carcinoembryonic Antigen in Non-Small Cell Lung Cancer: Analysis of 1,000 Consecutive Resections for Clinical Stage I Disease Morihito Okada, MD, PhD, Wataru
Lung Cancer-a primer. Sai Yendamuri, MD Professor and Chair, Dept of Thoracic Surgery,RPCI,Buffalo
 Lung Cancer-a primer Sai Yendamuri, MD Professor and Chair, Dept of Thoracic Surgery,RPCI,Buffalo CLINICAL CATEGORIES THE SOLITARY PULMONARY NODULE MULTIPLE PULMONARY NODULES Differential Diagnosis Malignant
Lung Cancer-a primer Sai Yendamuri, MD Professor and Chair, Dept of Thoracic Surgery,RPCI,Buffalo CLINICAL CATEGORIES THE SOLITARY PULMONARY NODULE MULTIPLE PULMONARY NODULES Differential Diagnosis Malignant
The Frequency and Significance of Small (15 mm) Hepatic Lesions Detected by CT
 535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
Lung Cancer Resection
 Lung Cancer Resection Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your health care provider may have recommended an operation to remove your lung cancer.
Lung Cancer Resection Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your health care provider may have recommended an operation to remove your lung cancer.
Slide 1. Slide 2. Slide 3. Investigation and management of lung cancer Robert Rintoul. Epidemiology. Risk factors/aetiology
 Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
Master Class: Fundamentals of Lung Cancer
 This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule
 Original Article Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule Xuan Zhang*, Hong-Hong Yan, Jun-Tao Lin, Ze-Hua Wu, Jia Liu, Xu-Wei Cao, Xue-Ning Yang From
Original Article Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule Xuan Zhang*, Hong-Hong Yan, Jun-Tao Lin, Ze-Hua Wu, Jia Liu, Xu-Wei Cao, Xue-Ning Yang From
Uniportal video-assisted thoracoscopic surgery segmentectomy
 Case Report on Thoracic Surgery Page 1 of 5 Uniportal video-assisted thoracoscopic surgery segmentectomy John K. C. Tam 1,2 1 Division of Thoracic Surgery, National University Heart Centre, Singapore;
Case Report on Thoracic Surgery Page 1 of 5 Uniportal video-assisted thoracoscopic surgery segmentectomy John K. C. Tam 1,2 1 Division of Thoracic Surgery, National University Heart Centre, Singapore;
minimally invasive techniques
 minimally invasive techniques VATS (Video-Assisted Thoracic Surgery) of Undefined Pulmonary Nodules* Preoperative Evaluation of Videoendoscopic Resectability Christian D. Schwarz, MD; Franz Lenglinger,
minimally invasive techniques VATS (Video-Assisted Thoracic Surgery) of Undefined Pulmonary Nodules* Preoperative Evaluation of Videoendoscopic Resectability Christian D. Schwarz, MD; Franz Lenglinger,
FDG PET/CT STAGING OF LUNG CANCER. Dr Shakher Ramdave
 FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
Significance of Metastatic Disease
 Significance of Metastatic Disease in Subaortic Lymph Nodes G. A. Patterson, M.D., D. Piazza, M.D., F. G. Pearson, M.D., T. R. J. Todd, M.D., R. J. Ginsberg, M.D., M. Goldberg, M.D., P. Waters, M.D., D.
Significance of Metastatic Disease in Subaortic Lymph Nodes G. A. Patterson, M.D., D. Piazza, M.D., F. G. Pearson, M.D., T. R. J. Todd, M.D., R. J. Ginsberg, M.D., M. Goldberg, M.D., P. Waters, M.D., D.
Clinically Resectable Lung Tumors
 Diagnostic and Therapeutic Endoscopy, 1996, Vol. 2, pp. 151-155 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam
Diagnostic and Therapeutic Endoscopy, 1996, Vol. 2, pp. 151-155 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam
Lung Cancer Awareness Month Update 2008
 Lung Cancer Awareness Month Update 2008 Guest Expert: Frank, MD Professor of Thoracic Surgery Lynn, MD Professor of Pulmonary Medicine www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center
Lung Cancer Awareness Month Update 2008 Guest Expert: Frank, MD Professor of Thoracic Surgery Lynn, MD Professor of Pulmonary Medicine www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center
Thoracoscopic Lobectomy for Locally Advanced Lung Cancer. Masters of Minimally Invasive Thoracic Surgery Orlando September 19, 2014
 for Locally Advanced Lung Cancer Masters of Minimally Invasive Thoracic Surgery Orlando September 19, 2014 Thomas A. D Amico MD Gary Hock Endowed Professor and Vice Chair of Surgery Chief Thoracic Surgery
for Locally Advanced Lung Cancer Masters of Minimally Invasive Thoracic Surgery Orlando September 19, 2014 Thomas A. D Amico MD Gary Hock Endowed Professor and Vice Chair of Surgery Chief Thoracic Surgery
More than half of the patients undergoing resection for colorectal
 General Thoracic Surgery Pfannschmidt et al Prognostic factors and survival after complete resection of pulmonary metastases from colorectal carcinoma: Experiences in 167 patients Joachim Pfannschmidt,
General Thoracic Surgery Pfannschmidt et al Prognostic factors and survival after complete resection of pulmonary metastases from colorectal carcinoma: Experiences in 167 patients Joachim Pfannschmidt,
BJUI. Solitary, isolated metastatic disease to the kidney: Memorial Sloan-Kettering Cancer Center experience
 ; 2010 Urological Oncology SOLITARY, ISOLATED METASTATIC DISEASE TO THE KIDNEY ADAMY ET AL. BJUI Solitary, isolated metastatic disease to the kidney: Memorial Sloan-Kettering Cancer Center experience Ari
; 2010 Urological Oncology SOLITARY, ISOLATED METASTATIC DISEASE TO THE KIDNEY ADAMY ET AL. BJUI Solitary, isolated metastatic disease to the kidney: Memorial Sloan-Kettering Cancer Center experience Ari
Thoracoscopy for Lung Cancer
 Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
The Itracacies of Staging Patients with Suspected Lung Cancer
 The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
Mediastinal Spread of Metastatic Lymph Nodes in Bronchogenic Carcinoma*
 Mediastinal Spread of Metastatic Lymph Nodes in Bronchogenic Carcinoma* Mediastinal Nodal Metastases in Lung Cancer Yoh Watanabe, M.D., F.C.C.P.; ]unzo Shimizu, M.D.; Makoto Tsubota, M.D.; and Takashi
Mediastinal Spread of Metastatic Lymph Nodes in Bronchogenic Carcinoma* Mediastinal Nodal Metastases in Lung Cancer Yoh Watanabe, M.D., F.C.C.P.; ]unzo Shimizu, M.D.; Makoto Tsubota, M.D.; and Takashi
Benign Intraparenchymal Scarring in the DBT Era
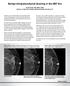 Benign Intraparenchymal Scarring in the DBT Era David Gruen, MD, MBA, FACR Director of Women s Imaging, Stamford Health, Stamford, CT With the advent of Digital Breast Tomosynthesis (DBT or 3D mammography),
Benign Intraparenchymal Scarring in the DBT Era David Gruen, MD, MBA, FACR Director of Women s Imaging, Stamford Health, Stamford, CT With the advent of Digital Breast Tomosynthesis (DBT or 3D mammography),
Lymph node dissection for lung cancer is both an old
 LOBE-SPECIFIC EXTENT OF SYSTEMATIC LYMPH NODE DISSECTION FOR NON SMALL CELL LUNG CARCINOMAS ACCORDING TO A RETROSPECTIVE STUDY OF METASTASIS AND PROGNOSIS Hisao Asamura, MD Haruhiko Nakayama, MD Haruhiko
LOBE-SPECIFIC EXTENT OF SYSTEMATIC LYMPH NODE DISSECTION FOR NON SMALL CELL LUNG CARCINOMAS ACCORDING TO A RETROSPECTIVE STUDY OF METASTASIS AND PROGNOSIS Hisao Asamura, MD Haruhiko Nakayama, MD Haruhiko
Management guideline for patients with differentiated thyroid cancer. Teeraporn Ratanaanekchai ENT, KKU 17 October 2007
 Management guideline for patients with differentiated thyroid Teeraporn Ratanaanekchai ENT, KKU 17 October 2007 Incidence (Srinagarind Hospital, 2005, both sex) Site (all) cases % 1. Liver 1178 27 2. Lung
Management guideline for patients with differentiated thyroid Teeraporn Ratanaanekchai ENT, KKU 17 October 2007 Incidence (Srinagarind Hospital, 2005, both sex) Site (all) cases % 1. Liver 1178 27 2. Lung
T3 NSCLC: Chest Wall, Diaphragm, Mediastinum
 for T3 NSCLC: Chest Wall, Diaphragm, Mediastinum AATS Postgraduate Course April 29, 2012 Thomas A. D Amico MD Professor of Surgery, Chief of Thoracic Surgery Duke University Health System Disclosure No
for T3 NSCLC: Chest Wall, Diaphragm, Mediastinum AATS Postgraduate Course April 29, 2012 Thomas A. D Amico MD Professor of Surgery, Chief of Thoracic Surgery Duke University Health System Disclosure No
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
N.E. Verstegen A.P.W.M. Maat F.J. Lagerwaard M.A. Paul M.I. Versteegh J.J. Joosten. W. Lastdrager E.F. Smit B.J. Slotman J.J.M.E. Nuyttens S.
 N.E. Verstegen A.P.W.M. Maat F.J. Lagerwaard M.A. Paul M.I. Versteegh J.J. Joosten W. Lastdrager E.F. Smit B.J. Slotman J.J.M.E. Nuyttens S.Senan Submitted 10 Salvage surgery for local failures after stereotactic
N.E. Verstegen A.P.W.M. Maat F.J. Lagerwaard M.A. Paul M.I. Versteegh J.J. Joosten W. Lastdrager E.F. Smit B.J. Slotman J.J.M.E. Nuyttens S.Senan Submitted 10 Salvage surgery for local failures after stereotactic
Lung Cancer Screening
 Scan for mobile link. Lung Cancer Screening What is lung cancer screening? Screening examinations are tests performed to find disease before symptoms begin. The goal of screening is to detect disease at
Scan for mobile link. Lung Cancer Screening What is lung cancer screening? Screening examinations are tests performed to find disease before symptoms begin. The goal of screening is to detect disease at
Dr. Andres Wiernik. Lung Cancer
 Dr. Andres Wiernik Lung Cancer Lung Cancer Facts - Demographics World Incidence: 1 8 million / year World Mortality: 1 6 million / year 5-year survival rates vary from 4 17% depending on stage and regional
Dr. Andres Wiernik Lung Cancer Lung Cancer Facts - Demographics World Incidence: 1 8 million / year World Mortality: 1 6 million / year 5-year survival rates vary from 4 17% depending on stage and regional
SECONDARIES: A PRELIMINARY REPORT
 HPB Surgery, 1990, Vol. 2, pp. 69-72 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORTS
HPB Surgery, 1990, Vol. 2, pp. 69-72 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORTS
Post-Induction PET Does Not Correlate with Persistent Nodal Disease or Overall Survival in Surgically Treated Stage IIIA Non-Small Cell Lung Cancer
 Post-Induction PET Does Not Correlate with Persistent Nodal Disease or Overall Survival in Surgically Treated Stage IIIA Non-Small Cell Lung Cancer R. Taylor Ripley, Kei Suzuki, Kay See Tan, Manjit Bains,
Post-Induction PET Does Not Correlate with Persistent Nodal Disease or Overall Survival in Surgically Treated Stage IIIA Non-Small Cell Lung Cancer R. Taylor Ripley, Kei Suzuki, Kay See Tan, Manjit Bains,
Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms
 Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
INTERACTIVE SESSION 2
 INTERACTIVE SESSION 2 2 patients with lung metastases, with complete response after oncologic treatment - Clinical Case Presentation: Dr. Esther Casado Dr. Sergi Call - Expert Opinion: Dr. Raúl Embún Dr.
INTERACTIVE SESSION 2 2 patients with lung metastases, with complete response after oncologic treatment - Clinical Case Presentation: Dr. Esther Casado Dr. Sergi Call - Expert Opinion: Dr. Raúl Embún Dr.
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Radiologic assessment of response of tumors to treatment. Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1
 Radiologic assessment of response of tumors to treatment Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1 Objective response assessment is important to describe the treatment effect of
Radiologic assessment of response of tumors to treatment Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1 Objective response assessment is important to describe the treatment effect of
An Introduction to PET Imaging in Oncology
 January 2002 An Introduction to PET Imaging in Oncology Janet McLaren, Harvard Medical School Year III Basics of PET Principle of Physiologic Imaging: Allows in vivo visualization of structures by their
January 2002 An Introduction to PET Imaging in Oncology Janet McLaren, Harvard Medical School Year III Basics of PET Principle of Physiologic Imaging: Allows in vivo visualization of structures by their
