An update of the WCRF/AICR systematic literature review and meta-analysis on dietary and anthropometric factors and esophageal cancer risk
|
|
|
- Brenda Wilkinson
- 6 years ago
- Views:
Transcription
1 Annals of Oncology 0: 1 11, 2017 doi: /annonc/mdx338 Published online 29 June 2017 REVIEW An update of the WCRF/AICR systematic literature review and meta-analysis on dietary and anthropometric factors and esophageal cancer risk S. Vingeliene 1,2 *, D. S. M. Chan 1, A. R. Vieira 1, E. Polemiti 1, C. Stevens 1, L. Abar 1, D. Navarro Rosenblatt 1, D. C. Greenwood 3 & T. Norat 1 1 Department of Epidemiology and Biostatistics, School of Public Health, Imperial College London, London, UK; 2 Clinical Epidemiology and Biostatistics, School of Medical Sciences, Orebro University, Orebro, Sweden; 3 Division of Biostatistics, University of Leeds, Leeds, UK *Correspondence to: Mrs. Snieguole Vingeliene, Department of Epidemiology and Biostatistics, School of Public Health, Imperial College London, St. Mary s Campus, Norfolk Place, London W2 1PG, UK. Tel: þ ; s.vingeliene@imperial.ac.uk Background: In the 2007 World Cancer Research Fund/American Institute for Cancer Research Second Expert Report, the expert panel judged that there was strong evidence that alcoholic drinks and body fatness increased esophageal cancer risk, whereas fruits and vegetables probably decreased its risk. The judgments were mainly based on case control studies. As part of the Continuous Update Project, we updated the scientific evidence accumulated from cohort studies in this topic. Methods: We updated the Continuous Update Project database up to 10 January 2017 by searching in PubMed and conducted dose response meta-analyses to estimate summary relative risks (RRs) and 95% confidence intervals (CIs) using random effects model. Results: A total of 57 cohort studies were included in 13 meta-analyses. Esophageal adenocarcinoma risk was inversely related to vegetable intake (RR per : 0.89, 95% CI: , n ¼ 3) and directly associated with body mass index (RR per 5 kg/ m 2 : 1.47, 95% CI: , n ¼ 9). For esophageal squamous cell carcinoma, inverse associations were observed with fruit intake (RR for increment: 0.84, 95% CI: , n ¼ 3) and body mass index (RR for 5 kg/m 2 increment: 0.64, 95% CI: , n ¼ 8), and direct associations with intakes of processed meats (RR for increment: 1.59, 95% CI: , n ¼ 3), processed and red meats (RR for increment: 1.37, 95% CI: , n ¼ 3) and alcohol (RR for 10 g/day increment: 1.25, 95% CI: , n ¼ 6). Conclusions: Evidence from cohort studies suggested a protective role of vegetables and body weight control in esophageal adenocarcinomas development. For squamous cell carcinomas, higher intakes of red and processed meats and alcohol may increase the risk, whereas fruits intake may play a protective role. Key words: esophageal cancer, diet, anthropometry, dose response, meta-analysis Introduction Esophageal cancer is the eighth most common cancer and the eighth leading cause of cancer death in the world, with new cases and deaths in 2012, respectively [1]. At the time of diagnosis, only 25% have a localized disease [2]. The 5- year survival rate is only 15% 20% in western countries [3]. Globally, there is a significant variation in esophageal cancer incidence. Esophageal squamous cell carcinoma (SCC) remains the most prevalent histologic type, particularly in esophageal belt countries (e.g. Kazakhstan, Mongolia, Northern parts of China, Iran) [4]. In developed countries (e.g. UK [2], United States, Australia [5]), the incidence of esophageal adenocarcinoma (AC) has been increasing rapidly, exceeding the incidence of SCC. Smoking and alcohol are the major risk factors for esophageal SCC [6]. In 2007, the World Cancer Research Fund/American Institute for Cancer Research (WCRF/AIRC) Second Expert Report [7] concluded that there was strong evidence that alcohol intake is a cause of esophageal cancer, and intake of vegetables, fruits, and foods containing b-carotene and vitamin C probably VC The Author Published by Oxford University Press on behalf of the European Society for Medical Oncology. This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits non-commercial re-use, distribution, and reproduction in any medium, provided the original work is properly cited. For commercial re-use, please contact journals.permissions@oup.com
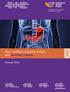
2 Review reduce its risk; body fatness is a cause of esophageal AC, and maté probably increases the risk of esophageal SCC. For other foods and dietary components, the association with esophageal cancer was judged as limited. The majority of evidence was from case control studies and not many studies reported results specifically on esophageal SCC and AC. Since the 2007 WCRF/AICR report, at least 70 relevant publications from prospective studies have been identified. Many of which investigated the associations by histologic types of esophageal cancer, as the etiology of the diseases is different. Modifiable risk factors are important because there are potential public health implications. We conducted an updated systematic review and meta-analysis of dietary and anthropometric factors and the risk of esophageal cancer, SCC and AC, as part of the work for the WCRF CUP [8]. Methods Search strategy This is an update of the 2007 WCRF/AICR report for which the search was conducted through December 2005 in eight electronic databases [7]. All cohort studies included in the report were indexed in PubMed, therefore, we updated the search in PubMed up to 10 January In addition, reference lists of relevant publications were screened for any further publications. The protocol of the CUP including the search strategy can be accessed at oesophageal_cancer.pdf [9]. Study selection Included studies met the following criteria: (i) were designed as cohort, nested case control or case cohort study; (ii) reported relative risk (RR) estimates (hazard ratio, odds ratio, or risk ratio) with confidence intervals (CIs); (iii) reported quantifiable measures of dietary intakes or anthropometric factors. When several publications from the same study were identified, the most recent publication with the largest number of cases was selected for the review. According to the protocol, the dose response meta-analysis is updated in the CUP when at least two new studies had been published after the 2007 WCRF/AICR report and the total number of studies with sufficient data for meta-analysis is five or more. Additional analyses of related exposures were conducted even though the numbers did not meet the criteria. Annals of Oncology Statistical analysis We combined the dose response RR estimates in the studies using a random-effects model, which considers both withinstudy and between-study variation [10]. When the dose response RR estimates were not available in the studies, we used Greenland and Longnecker method to derive the linear dose response trend from the natural logarithm of the risk estimates across the exposure categories [11]. For this method, at least three categories are required, each presenting the number of person-years, cases, RRs and CIs for that category. Where this information was not provided explicitly, it was derived as specified in the protocol [9]. In brief, the following rules were applied: person-years or cases per quantile were estimated by dividing the total number of cases or person-years by the number of quantiles; missing person-years per category were estimated proportionally if the number of cases per category, RRs, and total person-years were available. When food or drinks consumption was reported in servings or times, these were converted to grams/day using standard serving sizes as stated in the protocol [9]. Where intakes were reported per 1000 kcal/day, the mean energy intake of the study population was used to estimate total intake per day. Summary RRs were estimated for men, women, and both combined. When reported separately, the RRs for men and women were first combined using a fixed effect meta-analysis before pooling with other studies. Summary RRs were calculated for any type of esophageal cancer and for SCC and AC separately. When the RRs were available by cancer types only, the combined RR for esophageal cancer was estimated using Hamling s method [12]. Hamling s method was also used to change the reference category if it did not correspond to the lowest exposure category. Floating CIs were converted to conventional 95% CIs using the method described by Orsini et al. [13]. When the study reported observed and calibrated risk estimates, the calibrated one was used for the dose response metaanalysis. Heterogeneity was evaluated by Cochran Q test and I 2 statistics [14]. The sources of heterogeneity were explored in stratified analysis by sex, cancer type (AC, SCC), geographic location, exposure assessment method, length of follow-up, number of cases, year of publication, and adjustment factors when possible. Sensitivity of the summary risk estimate was investigated in influence-analyses by excluding each study in turn. Publication or small study bias was assessed by Egger s test and visual inspection of the funnel plot when at least five studies were included in the analysis [15]. Statistical tests with a P value of <0.05 were considered significant. Analyses were conducted using Stata version 12 software (Stata Corp, College Station, TX). Data extraction The following data were extracted from each study: study characteristics (first author, publication year, country, study name, follow-up period, and losses); study sample characteristics (sex, ethnicity, number of cases and non-cases, study size); exposure details (assessment method, exposure level); outcome details (type of esophageal cancer, case ascertainment method); RR estimates and corresponding 95% CIs; and adjustment variables. Results The study search flowchart is available in Figure 1. Of the 109 publications, 57 publications from 34 different cohort studies were included in the dose response meta-analyses of dietary and anthropometric factors and the risk of esophageal cancer, and SCC and AC. Fifteen studies were conducted in Asia, 11 in Europe, and 8 in the USA. Cases were ascertained through cancer, death or health registries, medical records, death certificates, active follow-up, or a combination of the methods. No studies were 2 Vingeliene et al.
3 Annals of Oncology Review 8577 publications identified in PubMed from January 1 st 2006 to January 10 th 2017 in the CUP update 8193 publications excluded on the basis of title and abstract 384 publications retrieved and assessed for inclusion 81 publications with cohort, casecohort or nested case-control design 303 publications excluded: 61 meta-analyses 11 pooled analyses 45 reviews/no original data 2 randomised controlled trials 4 letters/editorials/comments/magazine articles 3 no measure of the association 38 out of research topic 6 ecological studies 1 cross-sectional study 132case-control studies 28 publications with cohort, casecohort or nested case-control design identified in the SLR for the WCRF/AICR second expert report (published up to 31 st December 2005) 52 publications excluded from the dose-response meta-analyses because superseded by other publications or for missing data 57 publications included in the dose-response meta-analyses of the CUP update Figure 1. Flow chart of the study selection. based on self-reported, unverified cases. Validated dietary questionnaire was used in all but one Chinese study [16 18]. and height data were measured in eight studies [16, 17, 19 26], self-reported in eight [27 34] and taken from medical records in one [35]. Most studies adjusted for multiple main confounding factors such as alcohol, smoking, education, and body mass index (BMI). Main characteristics of each included publication are provided in supplementary Table S1, available at Annals of Oncology online. The excluded publications and reasons for exclusions are in supplementary Table S2, available at Annals of Oncology online. A summary of the dose response relationships examined in the present study is shown in Figure 2. Fruits and vegetables Meta-analyses were conducted for vegetables, green leafy vegetables, fruits and citrus fruits. Only two studies reported on total fruit and vegetable intake [36, 37], and found significant inverse associations with SCC [36, 37] and no association with AC [36]. There was not enough information for other vegetables or fruits [17, 38 40] (results not tabulated). Vegetable intake was not related to the risk of esophageal cancer (all types combined) (RR per ¼ 0.98, 95% CI: , I 2 ¼ 31%, 5 studies) [16, 37, 38, 40, 41]andSCC(RR¼ 0.91, 95% CI: , I 2 ¼ 49%, 4 studies) [16, 36, 37, 40], but was statistically significantly inversely associated with AC (RR ¼ 0.89, 95% CI: , I 2 ¼ 0%, 3 studies) [36, 38, 40], with one study contributing 82% weight in the analysis [36] (supplementary Figure S1, available at Annals of Oncology online). All three studies reported non-significant inverse associations in the analyses adjusted for multiple main confounders; of which two additionally adjusted for fruit intake [36, 40]. Green leafy vegetable intake was significantly inversely associated with the risk of esophageal cancer (RR per ¼ 0.87, 95% CI: , I 2 ¼ 0%, 6 studies) [17, 36 40] and AC (RR ¼ 0.85, 95% CI: , I 2 ¼ 0%, 3 studies) [36, 38, 40], but not SCC (RR ¼ 0.89, 95% CI: , I 2 ¼ 0%, 4 studies)[17, 36, 37, 40] (supplementary Figure S2, available at Annals of Oncology online). Only one study additionally adjusted for intake of fruits and other vegetables [40]. Fruit intake was not related to all esophageal cancer (RR per ¼ 0.94, 95% CI: , I 2 ¼ 0%, 4 studies) [37, 38, doi: /annonc/mdx338 3
4 Review Exposure EC Vegetables Green leafy vegetables Fruits Citrus fruit Processed meat Red/processed meat Coffee Alcohol (as ethanol) BMI Height RR (95% CI) % Increment dose Annals of Oncology I 2 (P) 0.98 (0.90, 1.06) 0.87 (0.77, 0.98) 0.94 (0.89, 1.00) 0.86 (0.74, 1.00) 1.44 (1.08, 1.92) (0.22) 0 (0.86) 0 (0.83) 0 (0.83) 27 (0.25) 1.21 (0.95, 1.54) 0.95 (0.88, 1.03) 1.23 (1.16, 1.30) 0.95 (0.85, 1.06) 1.00 (0.95, 1.06) 0.94 (0.83, 1.07) cup/day 10 g/day 5 kg/m 2 5 cm 5 kg 0 (0.83) 47 (0.10) 95 (<0.001) 85 (<0.001) 72 (<0.001) 90 (<0.001) AC Vegetables Green leafy vegetables Fruits Citrus fruit Processed meat Red/processed meat Coffee Alcohol (as ethanol) BMI Height Waist circumference Waist to hip ratio 0.89 (0.80, 0.99) 0.85 (0.74, 0.96) 1.03 (0.95, 1.11) 0.93 (0.78, 1.11) 1.19 (0.85, 1.68) 0.97 (0.79, 1.20) 0.96 (0.90, 1.04) 1.00 (0.98, 1.02) 1.47 (1.34, 1.61) 0.95 (0.88, 1.02) 1.16 (1.09, 1.22) 1.36 (1.17, 1.57) 1.58 (0.99, 2.50) cup/day 10 g/day 5 kg/m 2 5 cm 5 kg 10 cm 0.1 unit 0 (0.67) 0 (0.89) 0 (0.42) 0 (0.58) 63 (0.07) 6 (0.34) 4 (0.31) 1 (0.41) 36 (0.13) 0 (0.37) 0 (0.40) 32 (0.23) 80 (0.006) SCC Vegetables Green leafy vegetables Fruits Citrus fruit Processed meat Red/processed meat Coffee Alcohol (as ethanol) BMI Height 0.91 (0.81, 1.03) 0.89 (0.75, 1.06) 0.84 (0.75, 0.94) 0.87 (0.69, 1.08) 1.59 (1.11, 2.28) 1.37 (1.04, 1.82) 1.02 (0.89, 1.15) 1.25 (1.12, 1.41) 0.64 (0.56, 0.73) 1.01 (0.91, 1.12) 0.87 (0.72, 1.06) cup/day 10 g/day 5 kg/m 2 5 cm 5 kg 49 (0.12) 0 (0.50) 0 (0.58) 23 (0.27) 41 (0.18) 0 (0.91) 50 (0.14) 95 (<0.001) 71 (0.001) 42 (0.18) 92 (<0.001) Figure 2. Summary of the dose response relationships for the dietary and anthropometric factors and risk of esophageal cancer, adenocarcinoma and squamous cell carcinoma. EC, esophageal cancer; AC, adenocarcinoma; SCC, squamous cell carcinoma. 40, 41] and AC (RR ¼ 1.03, 95% CI: , I 2 ¼ 0%, 3 studies) [36, 38, 40], but was inversely associated with SCC (RR ¼ 0.84, 95% CI: , I 2 ¼ 0%, 3 studies) [36, 37, 40] (supplementary Figure S3, available at Annals of Oncology online). Studies on SCC adjusted for all major confounders and two studies additionally adjusted for vegetable intake [36, 40]. For citrus fruits, no significant associations were observed (supplementary Figure S4, available at Annals of Oncology online). The summary RRs per 100 g/ day were 0.86 (95% CI: , I 2 ¼ 0%) for all esophageal cancer (6 studies) [36 40, 42], 0.93 (95% CI: , I 2 ¼ 0%) for AC (3 studies) [36, 38, 40], and 0.87 (95% CI: , I 2 ¼ 23%) for SCC (3 studies) [36, 37, 40]. In influence analyses, the results remained the same except when the only study on mortality was excluded [39], citrus fruit became significantly inversely associated with all esophageal cancer risk (RR ¼ 0.85, 95% CI: ). Red and processed meats Meta-analyses were conducted for intakes of processed meat as well as processed and red meat combined. Meta-analyses were not conducted for total meat [38, 43 45], specific red meats [39, 46, 47], poultry [38, 39, 48, 49], and fish [39, 43, 45, 48, 50, 51] because of insufficient information. Reported results were mostly non-significant (results not tabulated). Processed meat intake was associated with increased risk of all esophageal cancer (RR per ¼ 1.44, 95% CI: , I 2 ¼ 27%, 4 studies) [39, 49, 52 54] (supplementaryfigures5, 4 Vingeliene et al.
5 Annals of Oncology Author Year AC Per 10 g/day intake RR (95% CI) % Review Yates (0.59, 1.04) 0.43 Hardikar (0.89, 1.27) 1.13 Steevens (0.90, 1.14) 2.55 Allen (0.72, 1.07) 0.92 Freedman (0.93, 1.11) 4.40 Lindblad (0.98, 1.02) Subtotal (I squared = 0.7%, p = 0.411) 1.00 (0.98, 1.02) SCC Steevens (1.19, 1.45) Allen (1.25, 1.55) Ishiguro (1.25, 1.44) Weikert (1.17, 1.30) Freedman (1.12, 1.41) Lindblad (1.02, 1.07) Subtotal (I squared = 95.0%, p = 0.000) 1.25 (1.12, 1.41) NOTE: weights are from random effects analysis Figure 3. Alcohol intake and esophageal cancer risk by histologic type, dose response meta-analysis. AC, adenocarcinoma; SCC, squamous cell carcinoma. available at Annals of Oncology online). No significant association was observed for AC (RR ¼ 1.19, 95% CI: , I 2 ¼ 63%, 3 studies) [49, 52, 53] but a direct association was observed for SCC (RR ¼ 1.59, 95% CI: , I 2 ¼ 41%, 3 studies) [52 54]. For processed and red meat intake combined, the associations were not significant for all esophageal cancer (RR per - ¼ 1.21, 95% CI: , I 2 ¼ 0%, 3 studies) [49, 52 54] and AC (RR ¼ 0.97, 95% CI: , I 2 ¼ 6%, 3 studies) [49, 52, 53], but was significant with SCC (RR ¼ 1.37, 95% CI: , I 2 ¼ 0%, 3 studies) [52 54] (supplementary Figure S6, available at Annals of Oncology online). Hot drinks Six [39, 55 59], two [57, 59], and three studies [57 59] were included in the meta-analyses of coffee and all esophageal cancer, AC and SCC risk, respectively. There were no significant associations (supplementary Figure S7, available at Annals of Oncology online). The summary RRs per 1 cup/day were 0.95 (95% CI: , I 2 ¼ 47%) for all esophageal cancer, 0.96 (95% CI: , I 2 ¼ 4%) for AC, and 1.02 (95% CI: , I 2 ¼ 50%) for SCC. Meta-analysis was not conducted for high-temperature drinks [16, 50, 57], tea [39, 50, 57, 59], green tea [39, 60], and black tea [39] due to low number of studies with sufficient data (results not tabulated). Drinking hot liquid and hot tea were non-significantly inversely associated with SCC [16, 57] and AC [57] risk in two studies and significantly directly associated with esophageal cancer mortality in one study [50], comparing drinking hot versus not hot tea. Alcoholic drinks Alcohol intake, as measured in grams of ethanol, was significantly directly associated with all esophageal cancer risk (RR per 10 g/ day ¼ 1.23, 95% CI: , I 2 ¼ 95%, 18 studies) [21, 35, 43, 50, 61 74] (supplementary Figure S8, available at Annals of Oncology online). The association was restricted to SCC (RR ¼ 1.25, 95% CI: , I 2 ¼ 95%, 6 studies) [35, 61, 63, 64, 69, 70] and not observed with AC (RR ¼ 1.00, 95% CI: , I 2 ¼ 1%, 6 studies) [21, 35, 61, 63, 69, 75] (Figure 3). The substantial proportion of between-study heterogeneity in the analysis on SCC was largely due to one study [35]; when omitted in sensitivity analysis, the relationship remained similar (RR ¼ 1.30, 95% CI: ) but heterogeneity dropped from 95% to 39%. In this study, the reference category of alcohol consumption was relatively high (2 units per day), most of the study participants were in the lowest two categories, and 42% was of unknown alcohol consumption [35]. doi: /annonc/mdx338 5
6 Review Annals of Oncology per 5 % Author Year kg/m 2 RR (95% CI) AC Steffen 2015 Hardikar 2013 Abnet 2008 Corley 2008 Reeves 2007 Merry 2007 Samanic 2006 Lindblad 2005 Engeland 2004 Subtotal (I squared = 36.3%, p = 0.128) 1.43 (1.10, 1.87) 1.05 (0.73, 1.61) 1.28 (1.13, 1.45) 1.61 (1.22, 2.19) 1.54 (1.26, 1.89) 1.93 (1.47, 2.59) 1.56 (1.15, 2.10) 1.41 (1.13, 1.76) 1.56 (1.39, 1.75) 1.47 (1.34, 1.61) SCC Steffen 2009 Corley 2008 Reeves 2007 Merry 2007 Samanic 2006 Lindblad 2005 Tran 2005 Engeland 2004 Subtotal (I squared = 71.4%, p = 0.001) 0.46 (0.35, 0.62) 0.56 (0.42, 0.73) 0.51 (0.42, 0.62) 0.59 (0.37, 0.90) 0.71 (0.58, 0.87) 0.81 (0.55, 1.20) 0.76 (0.67, 0.87) 0.72 (0.67, 0.78) 0.64 (0.56, 0.73) NOTE: s are from random effects analysis Figure 4. BMI and esophageal cancer risk by histologic type, dose response meta-analysis. AC, adenocarcinoma; SCC, squamous cell carcinoma. Anthropometric measurements For BMI, 17 studies were included in the meta-analyses of esophageal cancer [16, 19 24, 26 35], nine in AC [19 21, 23, 25, 27, 33 35] and eight in SCC [16, 19, 20, 23, 26, 33 35]. BMI was not associated with all esophageal cancer risk (RR per 5 kg/m 2 ¼ 0.95, 95% CI: , I 2 ¼ 85%) (supplementary Figure S9, available at Annals of Oncology online). Significant associations, that were directly related to AC (RR ¼ 1.47, 95% CI: ) and inversely to SCC (RR ¼ 0.64, 95% CI: ) were observed (Figure 4). The moderate (I 2 ¼ 36%) and high (I 2 ¼ 71%) proportions of between-study heterogeneity in the respective analyses on AC and SCC were not explained by the exposure assessment method, adjustment for smoking, geographic location, and sex; where the associations remained significant in the subgroup analyses (supplementary Table S3, available at Annals of Oncology online). Meta-analyses were also conducted for weight and height; and for waist circumference and waist-to-hip ratio, where only two [25, 76] and three studies [21, 25, 76] had reported results on the risk of AC, respectively. The associations of weight with all esophageal cancer [16, 26, 30, 76, 77], AC [25, 76] and SCC risk [16, 26] followed those observed for BMI (supplementary Figure S10, available at Annals of Oncology online). Waist circumference and waist-to-hip ratio were directly associated with AC risk (supplementary Figure S11, available at Annals of Oncology online). The summary RRs were 1.36 (95% CI: , I 2 ¼ 32%) for each 10 cm increase of waist circumference and 1.58 (95% CI: , I 2 ¼ 80%) for each 0.1 unit increase of waist-to-hip ratio. Height was not associated with esophageal cancer (RR per 5cm¼ 1.00, 95% CI: , I 2 ¼ 72%, 9 studies) [16, 20, 26, 30, 33, 76, 78 80], AC (RR ¼ 0.95, 95% CI: , I 2 ¼ 0%, 3 studies) [25, 33, 76] or SCC (RR ¼ 1.01, 95% CI: , I 2 ¼ 42%, 3 studies) [16, 26, 33] (supplementary Figure S12, available at Annals of Oncology online). Test of publication or small study bias Egger s test indicated significant evidence of small study bias for alcohol and esophageal cancer (all) (P < 0.01) and SCC (P ¼ 0.01). The asymmetry in the funnel plot of SCC was driven by a study that reported a weaker association [35]. Visual inspection of the funnel plot suggested small studies reported stronger inverse associations between vegetable intake 6 Vingeliene et al.
7 Annals of Oncology and esophageal cancer (all) risk than expected, but the Egger s test was not statistically significant (P ¼ 0.15). All other P-values for Egger s test >0.18. Interactions with smoking: fruits and vegetables, processed and red meat, alcohol, and BMI Studies did not observe statistically significant interactions between smoking and intakes of fruit and vegetable [36, 40], processed and red meat [52], and alcohol [44, 64, 66, 69] in relation to esophageal cancer [36, 44, 66], AC [40, 52], or SCC [37, 40, 52, 64] risks and mortality [66]. One exception was for the inverse associations of BMI with SCC risk that was only significant among smokers and not among non-smokers in the European Prospective Investigation into Cancer and Nutrition study (EPIC) (P interaction <0.01) [26]. The pooled study, Me-Can, reported similar findings but the P- values for interaction were 0.41 for current smokers and 0.59 for former smokers versus never smokers [81]. Discussion The summary data from cohort studies indicate that esophageal AC risk is inversely associated with vegetable intake and directly associated with higher body adiposity (as assessed by BMI and waist circumference), and that the risk of esophageal SCC is inversely related to fruit intake and directly associated with intakes of red and processed meats and alcohol. Fruits and vegetables The estimated risk reductions were 11% for AC per increment of vegetable and 16% for SCC per increment of fruit intake. Whether vegetables and fruits have an independent role in esophageal cancer risk awaits further confirmation as not all studies included in the analyses provided mutually adjusted results. Our findings are in agreement with another metaanalysis on fruit intake [82] and SCC risk but not with a published meta-analysis that reported no association between vegetable intake and risk of AC [83]. The latter included the same prospective studies as in our meta-analysis but compared highest versus lowest intakes and did not conduct dose response metaanalysis. Fruits and vegetables are good sources of vitamin C and phytochemicals such as b-carotene that are tumor inhibiting, as shown in recent experimental studies [84, 85]. Risk reductions of esophageal and gastric cancers were reported in the Shandong Intervention Trial of vitamin C, E and selenium supplementation [86]; and in observational studies, inverse associations between esophageal cancer risk and dietary vitamin C intake [87], and carotenoids [88]. Red and processed meats The summary results of cohort studies show that SCC risk increases 59% for an increment of of processed meats and 37% for an increment of of processed and red meats. A direct but not significant association of processed meat with AC was observed. Review Previously published meta-analyses reported direct but not significant associations between processed meat intake and all types of esophageal cancer [89, 90] and SCC [91] risk. The present meta-analysis includes more recent publications [49, 54] with more cases. A published meta-analysis [92] reported a significant direct association with AC that was mainly influenced by case control studies. Plausible mechanisms explaining the associations include heme iron, polycyclic aromatic hydrocarbons, dietary N- nitroso compounds (NOC) and endogenous nitrosation, that are potentially carcinogenic to humans [49, 53, 92, 93]. Direct associations between heme iron intake and risk of AC [49, 52], and SCC [93]; heterocyclic amines formed in high temperature cooked meat and AC risk [52]; dietary nitrite and risk of esophageal cancer [94] and SCC [93]; endogenous NOC index and esophageal cancer risk [94]; and intake of N-nitrosodimethylamine (NDMA) and risk of esophageal cancer [94], and SCC [93] were observed. Hot drinks Coffee intake was not associated with esophageal cancer risk which is in agreement with a previous meta-analysis of prospective cohort studies that compared the highest versus the lowest intakes [95]. Our meta-analysis has one additional cohort [55]. Drinking very hot beverages, traditionally at 70 C in some areas of China, Iran, Turkey, and South America, was recently classified as probably carcinogenic to humans by the World Health Organization [96]. The epidemiologic evidence comes mainly from case control studies, in which the direct associations were stronger than those observed in the few cohort studies that had reported results [16, 39, 50, 57, 59]. The weaker association could partly be due to the fact that these cohort studies were mostly from geographical areas where hot beverages are not normally consumed at very high temperatures. Further confirmation from prospective studies is needed. Alcohol Our meta-analysis showed that alcohol intake increased the risk of SCC. The results are in concordance with published metaanalyses [97, 98]. The main mechanisms implicated in the carcinogenesis are related to alcohol metabolite acetaldehyde [97] and chronic alcohol consumption induced enzymes generating reactive oxygen species [99]. The specific mechanism of SCC carcinogenesis is related to alcohol metabolism in saliva where acetaldehyde concentration is times higher than in the blood [99]. In smokers, the conversion of acetaldehyde to non-toxic acetate in saliva is inhibited. Anthropometry An increment of 5 kg/m 2 of BMI was associated with 47% increased risk of AC. and waist circumference were also associated with increased risk of esophageal AC. In contrast, BMI increment of 5 kg/m 2 was associated with 36% reduced risk of SCC. Our results are consistent with previously published metaanalyses on AC [100, 101] and SCC [101]. The between-study heterogeneity observed in BMI and SCC remained unexplained, but the heterogeneity was due to the magnitude rather than the direction of the associations in the studies. doi: /annonc/mdx338 7
8 Review The observed inverse association of BMI with SCC risk is similar to what is observed in other smoking-related cancers, as smokers have higher risk of SCC and tend to be slimmer. However, this is not supported by all studies [26]. Increased levels of estrogens associated with higher BMI may have a protective role in SCC development [26]. On the contrary, the EPIC study reported direct associations between waist circumference, and waist-to-hip ratio and the risks of SCC in smokers and non-smokers [26]. The analyses were adjusted for BMI. In agreement with this study, Lin, 2015 reported direct but not significant association for waist circumference in a multivariate-adjusted model including BMI and smoking [79]. Whether waist circumference and waist-to-hip ratio are less confounded by smoking than BMI in the association with SCC risk, independent or not of BMI, needs to be investigated further as current evidence is lacking. Major proposed mechanisms to explain the association between body fatness and risk of cancer involve insulin, insulin-like growth factor, adipokines, inflammation, and immune responses [102]. Pressure from excess body fat in abdominal area may cause gastroesophageal reflux disease (GERD) which in turn may lead to premalignant condition of Barrett s esophagus, a precursor of esophageal AC [24]. Strengths and limitations This meta-analysis has several strengths. In the previous WCRF/ IARC systematic literature review, the evidence was mainly from case control studies [7]. In this review, we included studies of a prospective design, preventing recall bias and providing stronger level of evidence. We reviewed all dietary and anthropometric exposures on esophageal cancer for which dose response meta-analyses were conducted during the Continuous Update Project (CUP), presenting an overview of available evidence on thirteen exposures. When the number of studies was sufficient, sensitivity, and stratified analyses were conducted to test the robustness of findings and explore possible sources of heterogeneity. Evidence of heterogeneity was not detected or was low for many analyses. This review particularly focuses on esophageal AC and SCC, which are more frequent in Western and Asian countries, respectively. Publications from studies based in these areas allow the examination of the differences in cancer etiology by histologic type. In terms of study quality, most studies in our review assessed dietary intake using validated food frequency questionnaires and the esophageal cancer diagnosis was documented. The main limitation of this meta-analysis is the small number of studies on some exposures. For fruits, vegetables and red and processed meats, the small numbers in the stratified analyses reduced the possibility to detect a source of heterogeneity. Those results should be interpreted cautiously as replication is needed. For waist-to-hip ratio in relation to AC risk, sources of the significant between-study heterogeneity could not be explored as only three studies reported results; however, the direct association supported that of BMI and AC. For hot drinks, a meta-analysis was not possible as current data from prospective studies were limited. The small number of studies reporting associations by smoking status limited a possibility to investigate confounding by smoking. Most studies included in this review were controlled for smoking, but residual confounding cannot be ruled out. For instance, no interaction with smoking was observed in North American [36] and European [40] studies on fruits and vegetables and esophageal cancers, but in a Japanese study [37], intake of fruits and vegetables was inversely related to SCC only in current smokers and consumers of >150 g/week of alcohol. It is also possible that the association is mainly observed in smokers because smokers have lower levels of serum vitamin C [103] and may benefit more from higher intakes. Another limitation of this meta-analysis is the lack of information in individual studies on GERD symptoms which increase the risk of Barrett s esophagus that may subsequently lead to AC. However, only 6% 12% of those with prolonged GERD symptoms will develop premalignant lesion of Barrett s esophagus and only 0.5% 1% of these patients will be diagnosed with AC [6]. Therefore, adjusting for GERD symptoms is unlikely to significantly influence results, if not over adjusting the associations of interest for these intermediate factors. Primary prevention of esophageal cancers may be a preferred option due to the aggressive nature of this disease and the lack of cost-effective screening. Body fatness, high alcohol and red and processed meat intakes are risk factors for other diseases and dietary patterns rich in plant foods may reduce the risk of other diseases including type 2 diabetes and CVD [104]. Therefore, existing primary prevention strategies for chronic diseases could also be used to reduce the burden of esophageal cancers. Acknowledgements TN is the principal investigator of the CUP at Imperial College London. CS managed the database for the CUP. SV and EP did the literature search and study selection. SV, DSMC, ARV, EP, LA, and DNR extracted the data. DSMC and SV carried out the statistical analyses. SV wrote the first draft of the original manuscript. SV and DSMC take responsibility for the integrity of the data and the accuracy of the data analysis. We thank the systematic literature review team at the Pennsylvania State University for their contributions to the esophageal cancer database. Funding This work was supported by the World Cancer Research Fund International as part of the CUP (grant number: 2007/SP01) ( The funder of this study had no role in the decisions about the design and conduct of the study; collection, management, analysis, or interpretation of the data; or the preparation, review, or approval of the manuscript. The views expressed in this review are the opinions of the authors. They may not represent the views of WCRF International/AICR and may differ from those in future updates of the evidence related to food, nutrition, physical activity, and cancer risk. Disclosure The authors have declared no conflicts of interest. Annals of Oncology 8 Vingeliene et al.
9 Annals of Oncology References 1. Ferlay J, Soerjomataram I, Dikshit R et al. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN Int J Cancer 2015; 136(5): E359 E Rubenstein JH, Shaheen NJ. Epidemiology, diagnosis, and management of esophageal adenocarcinoma. Gastroenterology 2015; 149(2): e Napier KJ, Scheerer M, Misra S. Esophageal cancer: a review of epidemiology, pathogenesis, staging workup and treatment modalities. World J Gastrointest Oncol 2014; 6(5): Eslick GD. Epidemiology of esophageal cancer. Gastroenterol Clin North Am 2009; 38(1): 17 25, vii. 5. Thrift AP, Whiteman DC. The incidence of esophageal adenocarcinoma continues to rise: analysis of period and birth cohort effects on recent trends. Ann Oncol 2012; 23(12): Domper Arnal MJ, Ferrandez Arenas A, Lanas Arbeloa A. Esophageal cancer: risk factors, screening and endoscopic treatment in Western and Eastern countries. World J Gastroenterol 2015; 21(26): WCRF/AICR: Nutrition, physical activity, and the prevention of cancer: a global perspective. Washington, DC: AICR, WCRF International: Continuous Update Project (CUP), (2 February 2017, date last accessed). 9. CUP Team, Imperial College London: Protocol Version 2: Continuous Update and Systematic Literature Review of Randomised Controlled Trials and Prospective Studies on Food, Nutrition, Physical Activity and the Risk of Oesophageal Cancer. files/protocol_oesophageal_cancer.pdf (10 April 2017, date last accessed). 10. DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials 1986; 7(3): Greenland S, Longnecker MP. Methods for trend estimation from summarized dose response data, with applications to meta-analysis. Am J Epidemiol 1992; 135(11): Hamling J, Lee P, Weitkunat R, Ambuhl M. Facilitating meta-analyses by deriving relative effect and precision estimates for alternative comparisons from a set of estimates presented by exposure level or disease category. Stat Med 2008; 27(7): Orsini N. From floated to conventional confidence intervals for the relative risks based on published dose response data. Comput Methods Programs Biomed 2010; 98(1): Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med 2002; 21(11): Egger M, Davey Smith G, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. Br Med J 1997; 315(7109): Tran GD, Sun XD, Abnet CC et al. Prospective study of risk factors for esophageal and gastric cancers in the Linxian general population trial cohort in China. Int J Cancer 2005; 113(3): Wang JB, Fan JH, Dawsey SM et al. Dietary components and risk of total, cancer and cardiovascular disease mortality in the Linxian Nutrition Intervention Trials cohort in China. Sci Rep 2016; 6: Wang SM, Fan JH, Jia MM et al. Body mass index and long-term risk of death from esophageal squamous cell carcinoma in a Chinese population. Thoracic Cancer 2016; 7(4): Corley DA, Kubo A, Zhao W. Abdominal obesity and the risk of esophageal and gastric cardia carcinomas. Cancer Epidemiol Biomarkers Prev 2008; 17(2): Engeland A, Tretli S, Bjorge T. Height and body mass index in relation to esophageal cancer; 23-year follow-up of two million Norwegian men and women. Cancer Causes Control 2004; 15(8): Hardikar S, Onstad L, Blount PL et al. The role of tobacco, alcohol, and obesity in neoplastic progression to esophageal adenocarcinoma: a prospective study of Barrett s esophagus. PLoS ONE 2013; 8(1): e Jee SH, Yun JE, Park EJ et al. Body mass index and cancer risk in Korean men and women. Int J Cancer 2008; 123(8): Review 23. Samanic C, Chow WH, Gridley G et al. Relation of body mass index to cancer risk in 362,552 Swedish men. Cancer Causes Control 2006; 17(7): Smith M, Zhou M, Whitlock G et al. Esophageal cancer and body mass index: results from a prospective study of 220,000 men in China and a meta-analysis of published studies. Int J Cancer 2008; 122(7): Steffen A, Huerta JM, Weiderpass E et al. General and abdominal obesity and risk of esophageal and gastric adenocarcinoma in the European Prospective Investigation into Cancer and Nutrition. Int J Cancer 2015; 137(3): Steffen A, Schulze MB, Pischon T et al. Anthropometry and esophageal cancer risk in the European prospective investigation into cancer and nutrition. Cancer Epidemiol Biomarkers Prev 2009; 18(7): Abnet CC, Freedman ND, Hollenbeck AR et al. A prospective study of BMI and risk of oesophageal and gastric adenocarcinoma. Eur J Cancer 2008; 44(3): Andreotti G, Hou L, Beane Freeman LE et al. Body mass index, agricultural pesticide use, and cancer incidence in the Agricultural Health Study cohort. Cancer Causes Control 2010; 21(11): Calle EE, Rodriguez C, Walker-Thurmond K, Thun MJ. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med 2003; 348(17): Fujino Y. Anthropometry, development history and mortality in the Japan Collaborative Cohort Study for Evaluation of Cancer (JACC). Asian Pac J Cancer Prev 2007; 8(Suppl): Hong JS, Yi SW, Yi JJ et al. Body mass index and cancer mortality among Korean older middle-aged men: a prospective cohort study. Medicine (Baltimore) 2016; 95(21): e Kuriyama S, Tsubono Y, Hozawa A et al. Obesity and risk of cancer in Japan. Int J Cancer 2005; 113(1): Merry AH, Schouten LJ, Goldbohm RA, van den Brandt PA. Body mass index, height and risk of adenocarcinoma of the oesophagus and gastric cardia: a prospective cohort study. Gut 2007; 56(11): Reeves GK, Pirie K, Beral V et al. Cancer incidence and mortality in relation to body mass index in the Million Women Study: cohort study. Br Med J (Clin Res Ed) 2007; 335(7630): Lindblad M, Rodriguez LA, Lagergren J. Body mass, tobacco and alcohol and risk of esophageal, gastric cardia, and gastric non-cardia adenocarcinoma among men and women in a nested case control study. Cancer Causes Control 2005; 16(3): Freedman ND, Park Y, Subar AF et al. Fruit and vegetable intake and esophageal cancer in a large prospective cohort study. Int J Cancer 2007; 121(12): Yamaji T, Inoue M, Sasazuki S et al. Fruit and vegetable consumption and squamous cell carcinoma of the esophagus in Japan: the JPHC study. Int J Cancer 2008; 123(8): Gonzalez CA, Pera G, Agudo A et al. Fruit and vegetable intake and the risk of stomach and oesophagus adenocarcinoma in the European Prospective Investigation into Cancer and Nutrition (EPIC- EURGAST). Int J Cancer 2006; 118(10): Iso H, Kubota Y. Nutrition and disease in the Japan Collaborative Cohort Study for Evaluation of Cancer (JACC). Asian Pac J Cancer Prev 2007; 8(Suppl): Steevens J, Schouten LJ, Goldbohm RA, van den Brandt PA. Vegetables and fruits consumption and risk of esophageal and gastric cancer subtypes in the Netherlands Cohort Study. Int J Cancer 2011; 129(11): George SM, Park Y, Leitzmann MF et al. Fruit and vegetable intake and risk of cancer: a prospective cohort study. Am J Clin Nutr 2009; 89(1): Li WQ, Kuriyama S, Li Q et al. Citrus consumption and cancer incidence: the Ohsaki cohort study. Int J Cancer 2010; 127(8): Fan Y, Yuan JM, Wang R et al. Alcohol, tobacco, and diet in relation to esophageal cancer: the Shanghai Cohort Study. Nutr Cancer 2008; 60(3): doi: /annonc/mdx338 9
10 Review 44. Guo W, Blot WJ, Li JY et al. A nested case control study of oesophageal and stomach cancers in the Linxian nutrition intervention trial. Int J Epidemiol 1994; 23(3): Hirayama T. [A large scale cohort study on the effect of life styles on the risk of cancer by each site]. Gan No Rinsho 1990; Spec No: Kjaerheim K, Gaard M, Andersen A. The role of alcohol, tobacco, and dietary factors in upper aerogastric tract cancers: a prospective study of 10,900 Norwegian men. Cancer Causes Control 1998; 9(1): Yu Y, Taylor PR, Li JY et al. Retrospective cohort study of risk-factors for esophageal cancer in Linxian, People s Republic of China. Cancer Causes Control 1993; 4(3): Daniel CR, Cross AJ, Graubard BI et al. Prospective investigation of poultry and fish intake in relation to cancer risk. Cancer Prev Res (Philadelphia, Pa) 2011; 4(11): Jakszyn P, Lujan-Barroso L, Agudo A et al. Meat and heme iron intake and esophageal adenocarcinoma in the European Prospective Investigation into Cancer and Nutrition study. Int J Cancer 2013; 133(11): Kinjo Y, Cui Y, Akiba S et al. Mortality risks of oesophageal cancer associated with hot tea, alcohol, tobacco and diet in Japan. J Epidemiol 1998; 8(4): Li WQ, Park Y, Wu JW et al. Index-based dietary patterns and risk of esophageal and gastric cancer in a large cohort study. Clin Gastroenterol Hepatol 2013; 11(9): e Cross AJ, Freedman ND, Ren J et al. Meat consumption and risk of esophageal and gastric cancer in a large prospective study. Am J Gastroenterol 2011; 106(3): Keszei AP, Schouten LJ, Goldbohm RA, van den Brandt PA. Red and processed meat consumption and the risk of esophageal and gastric cancer subtypes in The Netherlands Cohort Study. Ann Oncol 2012; 23(9): Steffen A, Bergmann MM, Sanchez MJ et al. Meat and heme iron intake and risk of squamous cell carcinoma of the upper aero-digestive tract in the European Prospective Investigation into Cancer and Nutrition (EPIC). Cancer Epidemiol Biomarkers Prev 2012; 21(12): Hashibe M, Galeone C, Buys SS et al. Coffee, tea, caffeine intake, and the risk of cancer in the PLCO cohort. Br J Cancer 2015; 113(5): Naganuma T, Kuriyama S, Kakizaki M et al. Coffee consumption and the risk of oral, pharyngeal, and esophageal cancers in Japan: the Miyagi Cohort Study. Am J Epidemiol 2008; 168(12): Ren JS, Freedman ND, Kamangar F et al. Tea, coffee, carbonated soft drinks and upper gastrointestinal tract cancer risk in a large United States prospective cohort study. Eur J Cancer 2010; 46(10): Tverdal A, Hjellvik V, Selmer R. Coffee intake and oral-oesophageal cancer: follow-up of 389,624 Norwegian men and women years. Br J Cancer 2011; 105(1): Zamora-Ros R, Lujan-Barroso L, Bueno-de-Mesquita HB et al. Tea and coffee consumption and risk of esophageal cancer: the European prospective investigation into cancer and nutrition study. Int J Cancer 2014; 135(6): Ishikawa A, Kuriyama S, Tsubono Y et al. Smoking, alcohol drinking, green tea consumption and the risk of esophageal cancer in Japanese men. J Epidemiol 2006; 16(5): Allen NE, Beral V, Casabonne D et al. Moderate alcohol intake and cancer incidence in women. J Natl Cancer Inst 2009; 101(5): Boffetta P, Garfinkel L. Alcohol drinking and mortality among men enrolled in an American Cancer Society prospective study. Epidemiology (Cambridge, Mass) 1990; 1(5): Freedman ND, Abnet CC, Leitzmann MF et al. A prospective study of tobacco, alcohol, and the risk of esophageal and gastric cancer subtypes. Am J Epidemiol 2007; 165(12): Ishiguro S, Sasazuki S, Inoue M et al. Effect of alcohol consumption, cigarette smoking and flushing response on esophageal cancer risk: a population-based cohort study (JPHC study). Cancer Lett 2009; 275(2): Annals of Oncology 65. Kasum CM, Jacobs DR Jr, Nicodemus K, Folsom AR. Dietary risk factors for upper aerodigestive tract cancers. Int J Cancer 2002; 99(2): Kimm H, Kim S, Jee SH. The independent effects of cigarette smoking, alcohol consumption, and serum aspartate aminotransferase on the alanine aminotransferase ratio in Korean men for the risk for esophageal cancer. Yonsei Med J. 2010; 51(3): Nakaya N, Tsubono Y, Kuriyama S et al. Alcohol consumption and the risk of cancer in Japanese men: the Miyagi cohort study. Eur J Cancer Prev 2005; 14(2): Shen C, Schooling CM, Chan WM et al. Alcohol intake and death from cancer in a prospective Chinese elderly cohort study in Hong Kong. J Epidemiol Community Health 2013; 67(10): Steevens J, Schouten LJ, Goldbohm RA, van den Brandt PA. Alcohol consumption, cigarette smoking and risk of subtypes of oesophageal and gastric cancer: a prospective cohort study. Gut 2010; 59(1): Weikert C, Dietrich T, Boeing H et al. Lifetime and baseline alcohol intake and risk of cancer of the upper aero-digestive tract in the European Prospective Investigation into Cancer and Nutrition (EPIC) study. Int J Cancer 2009; 125(2): Yaegashi Y, Onoda T, Morioka S et al. Joint effects of smoking and alcohol drinking on esophageal cancer mortality in Japanese men: findings from the Japan collaborative cohort study. Asian Pac J Cancer Prev 2014; 15(2): Yang L, Zhou M, Sherliker P et al. Alcohol drinking and overall and cause-specific mortality in China: nationally representative prospective study of 220,000 men with 15 years of follow-up. Int J Epidemiol 2012; 41(4): Yi SW, Hong JS, Yi JJ, Ohrr H. Impact of alcohol consumption and body mass index on mortality from nonneoplastic liver diseases, upper aerodigestive tract cancers, and alcohol use disorders in Korean older middle-aged men: prospective cohort study. Medicine (Baltimore). 2016; 95(39): e Yi SW, Sull JW, Linton JA et al. Alcohol consumption and digestive cancer mortality in Koreans: the Kangwha Cohort Study. J Epidemiol 2010; 20(3): Yates M, Cheong E, Luben R et al. Body mass index, smoking, and alcohol and risks of Barrett s esophagus and esophageal adenocarcinoma: a UK prospective cohort study. Dig Dis Sci 2014; 59(7): O Doherty MG, Freedman ND, Hollenbeck AR et al. A prospective cohort study of obesity and risk of oesophageal and gastric adenocarcinoma in the NIH-AARP Diet and Health Study. Gut 2012; 61(9): Tulinius H, Sigfusson N, Sigvaldason H et al. Risk factors for malignant diseases: a cohort study on a population of 22,946 Icelanders. Cancer Epidemiol Biomarkers Prev 1997; 6(11): Batty GD, Shipley MJ, Langenberg C et al. Adult height in relation to mortality from 14 cancer sites in men in London (UK): evidence from the original Whitehall study. Ann Oncol 2006; 17(1): Green J, Cairns BJ, Casabonne D et al. Height and cancer incidence in the Million Women Study: prospective cohort, and meta-analysis of prospective studies of height and total cancer risk. Lancet Oncol 2011; 12(8): Sung J, Song YM, Lawlor DA et al. Height and site-specific cancer risk: a cohort study of a Korean adult population. Am J Epidemiol 2009; 170(1): Lindkvist B, Johansen D, Stocks T et al. Metabolic risk factors for esophageal squamous cell carcinoma and adenocarcinoma: a prospective study of 580,000 subjects within the Me-Can project. BMC Cancer 2014; 14: Liu J, Wang J, Leng Y, Lv C. Intake of fruit and vegetables and risk of esophageal squamous cell carcinoma: a meta-analysis of observational studies. Int J Cancer 2013; 133(2): Li B, Jiang G, Zhang G et al. Intake of vegetables and fruit and risk of esophageal adenocarcinoma: a meta-analysis of observational studies. Eur J Nutr 2014; 53(7): Vingeliene et al.
An update of the WCRF/AICR systematic literature review and meta-analysis on dietary and anthropometric factors and esophageal cancer risk
 Annals of Oncology 28: 2409 2419, 2017 doi:10.1093/annonc/mdx338 Published online 29 June 2017 REVIEW An update of the WCRF/AICR systematic literature review and meta-analysis on dietary and anthropometric
Annals of Oncology 28: 2409 2419, 2017 doi:10.1093/annonc/mdx338 Published online 29 June 2017 REVIEW An update of the WCRF/AICR systematic literature review and meta-analysis on dietary and anthropometric
The WCRF/AICR Third Expert Report Diet, Nutrition, Physical Activity and Cancer: a Global Perspective Methods, Approaches and Lessons Learned
 The WCRF/AICR Third Expert Report Diet, Nutrition, Physical Activity and Cancer: a Global Perspective Methods, Approaches and Lessons Learned Teresa Norat, PhD Principal Research Fellow Imperial College
The WCRF/AICR Third Expert Report Diet, Nutrition, Physical Activity and Cancer: a Global Perspective Methods, Approaches and Lessons Learned Teresa Norat, PhD Principal Research Fellow Imperial College
Body mass index and long-term risk of death from esophageal squamous cell carcinoma in a Chinese population
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Body mass index and long-term risk of death from esophageal squamous cell carcinoma in a Chinese population Shao-Ming Wang 1, Jin-Hu Fan 1, Meng-Meng Jia
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Body mass index and long-term risk of death from esophageal squamous cell carcinoma in a Chinese population Shao-Ming Wang 1, Jin-Hu Fan 1, Meng-Meng Jia
World Cancer Research Fund International Systematic Literature Review
 World Cancer Research und International Systematic Literature Review The Associations between ood, Nutrition and Physical Activity and the Risk of Gallbladder Cancer Imperial College London Continuous
World Cancer Research und International Systematic Literature Review The Associations between ood, Nutrition and Physical Activity and the Risk of Gallbladder Cancer Imperial College London Continuous
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and oesophageal cancer. Revised 2018
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and oesophageal cancer 2016 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and oesophageal cancer 2016 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
RESEARCH. Dagfinn Aune, 1,2 Abhijit Sen, 1 Manya Prasad, 3 Teresa Norat, 2 Imre Janszky, 1 Serena Tonstad, 3 Pål Romundstad, 1 Lars J Vatten 1
 open access BMI and all cause mortality: systematic review and non-linear dose-response meta-analysis of 230 cohort studies with 3.74 million deaths among 30.3 million participants Dagfinn Aune, 1,2 Abhijit
open access BMI and all cause mortality: systematic review and non-linear dose-response meta-analysis of 230 cohort studies with 3.74 million deaths among 30.3 million participants Dagfinn Aune, 1,2 Abhijit
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and oesophageal cancer. Managed and produced by:
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and oesophageal cancer 2016 Managed and produced by: Contents World Cancer Research Fund International 1 Executive
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and oesophageal cancer 2016 Managed and produced by: Contents World Cancer Research Fund International 1 Executive
4.3 Meat, poultry, fish, and eggs
 P ART 2 EVIDENCE AND JUDGEMENTS 4.3 Meat, poultry, fish, and eggs MEAT, POULTRY, FISH, EGGS, AND THE RISK OF CANCER In the judgement of the Panel, the factors listed below modify the risk of cancer. Judgements
P ART 2 EVIDENCE AND JUDGEMENTS 4.3 Meat, poultry, fish, and eggs MEAT, POULTRY, FISH, EGGS, AND THE RISK OF CANCER In the judgement of the Panel, the factors listed below modify the risk of cancer. Judgements
Body mass index and risk of gastric cancer: A 30-year follow-up study in the Linxian general population trial cohort
 Body mass index and risk of gastric cancer: A 30-year follow-up study in the Linxian general population trial cohort Jin-hu Fan, 1,5 Jian-bing Wang, 2,5 Shao-ming Wang, 1 Christian C. Abnet, 3 You-lin
Body mass index and risk of gastric cancer: A 30-year follow-up study in the Linxian general population trial cohort Jin-hu Fan, 1,5 Jian-bing Wang, 2,5 Shao-ming Wang, 1 Christian C. Abnet, 3 You-lin
Height and body fatness and colorectal cancer risk: an update of the WCRF AICR systematic review of published prospective studies
 DOI 10.1007/s00394-017-1557-1 REVIEW Height and body fatness and colorectal cancer risk: an update of the WCRF AICR systematic review of published prospective studies Leila Abar 1 Ana Rita Vieira 1 Dagfinn
DOI 10.1007/s00394-017-1557-1 REVIEW Height and body fatness and colorectal cancer risk: an update of the WCRF AICR systematic review of published prospective studies Leila Abar 1 Ana Rita Vieira 1 Dagfinn
Study on meat intake and mortality
 Study on meat intake and mortality BfR Opinion No. 023/2009, 29 May 2009 In March of this year the daily press discussed an American study on the relationship between the consumption of red meat and an
Study on meat intake and mortality BfR Opinion No. 023/2009, 29 May 2009 In March of this year the daily press discussed an American study on the relationship between the consumption of red meat and an
This is a repository copy of Fruits, vegetables, and bladder cancer risk: a systematic review and meta-analysis.
 This is a repository copy of Fruits, vegetables, and bladder cancer risk: a systematic review and meta-analysis. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/82408/ Version:
This is a repository copy of Fruits, vegetables, and bladder cancer risk: a systematic review and meta-analysis. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/82408/ Version:
S e c t i o n 4 S e c t i o n4
 Section 4 Diet and breast cancer has been investigated extensively, although the overall evidence surrounding the potential relation between dietary factors and breast cancer carcinogenesis has resulted
Section 4 Diet and breast cancer has been investigated extensively, although the overall evidence surrounding the potential relation between dietary factors and breast cancer carcinogenesis has resulted
Nutrition and gastrointestinal cancer: An update of the epidemiological evidence
 Nutrition and gastrointestinal cancer: An update of the epidemiological evidence Krasimira Aleksandrova, PhD MPH Nutrition, Immunity and Metabolsim Start-up Lab Department of Epidemiology German Institute
Nutrition and gastrointestinal cancer: An update of the epidemiological evidence Krasimira Aleksandrova, PhD MPH Nutrition, Immunity and Metabolsim Start-up Lab Department of Epidemiology German Institute
Pancreatic Cancer 2012 Report. Keeping the science current. programmes. cancer research and education. World Cancer Research Fund s
 World Cancer Research Fund American Institute for Cancer Research Continuous Update Project Keeping the science current Join a sponsored walk in your community to raise funds for World Cancer Research
World Cancer Research Fund American Institute for Cancer Research Continuous Update Project Keeping the science current Join a sponsored walk in your community to raise funds for World Cancer Research
Continuous update of the WCRF-AICR report on diet and cancer. Protocol: Breast Cancer. Prepared by: Imperial College Team
 Continuous update of the WCRF-AICR report on diet and cancer Protocol: Breast Cancer Prepared by: Imperial College Team The current protocol for the continuous update should ensure consistency of approach
Continuous update of the WCRF-AICR report on diet and cancer Protocol: Breast Cancer Prepared by: Imperial College Team The current protocol for the continuous update should ensure consistency of approach
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and breast cancer. Revised 2018
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and breast cancer 2017 Revised 2018 Contents World Cancer Research Fund Network 3 Executive Summary 5 1. Summary
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and breast cancer 2017 Revised 2018 Contents World Cancer Research Fund Network 3 Executive Summary 5 1. Summary
Diet, weight, physical activity and cancer. Dr Rachel Thompson, Head of Research Interpretation
 Diet, weight, physical activity and cancer Dr Rachel Thompson, Head of Research Interpretation Outline World Cancer Research Fund network Continuous Update Project Recommendations for cancer prevention
Diet, weight, physical activity and cancer Dr Rachel Thompson, Head of Research Interpretation Outline World Cancer Research Fund network Continuous Update Project Recommendations for cancer prevention
RESEARCH ARTICLE. Sang Hyuk Jung 1, Bayasgalan Gombojav 2, Eun-Cheol Park 3,5, Chung Mo Nam 3, Heechoul Ohrr 2,3, Jong Uk Won 3,4 * Abstract
 RESEARCH ARTICLE Population Based Study of the Association Between Binge Drinking and Mortality from Cancer of Oropharynx and Esophagus in Korean Men: the Kangwha Cohort Study Sang Hyuk Jung 1, Bayasgalan
RESEARCH ARTICLE Population Based Study of the Association Between Binge Drinking and Mortality from Cancer of Oropharynx and Esophagus in Korean Men: the Kangwha Cohort Study Sang Hyuk Jung 1, Bayasgalan
Citation for the published paper: Epidemiology May;24(3): Abdominal fat and male excess of esophageal adenocarcinoma
 This is an author produced version of a paper published in Epidemiology. This paper has been peer-reviewed but does not include the final publisher proof-corrections or journal pagination. Citation for
This is an author produced version of a paper published in Epidemiology. This paper has been peer-reviewed but does not include the final publisher proof-corrections or journal pagination. Citation for
Weight Change and Risk of Colorectal Cancer: A Systematic Review and Meta-Analysis
 American Journal of Epidemiology The Author 2015. Published by Oxford University Press on behalf of the Johns Hopkins Bloomberg School of Public Health. All rights reserved. For permissions, please e-mail:
American Journal of Epidemiology The Author 2015. Published by Oxford University Press on behalf of the Johns Hopkins Bloomberg School of Public Health. All rights reserved. For permissions, please e-mail:
Epidemiological evidence linking food, nutrition, physical activity and prostate cancer risk: results from the Continuous Update Project
 Epidemiological evidence linking food, nutrition, physical activity and prostate cancer risk: results from the Continuous Update Project World Cancer Congress, Saturday 6 December 2014 Michael Leitzmann
Epidemiological evidence linking food, nutrition, physical activity and prostate cancer risk: results from the Continuous Update Project World Cancer Congress, Saturday 6 December 2014 Michael Leitzmann
ESPEN Congress Florence 2008
 ESPEN Congress Florence 2008 Severe obesity - Session organised in conjunction with ASPEN Long term mortality in cohorts of severely obese subjects D. Mirabelli (Italy) Long-term mortality in cohorts of
ESPEN Congress Florence 2008 Severe obesity - Session organised in conjunction with ASPEN Long term mortality in cohorts of severely obese subjects D. Mirabelli (Italy) Long-term mortality in cohorts of
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and cancers of the mouth, pharynx and larynx
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and cancers of the mouth, pharynx and larynx 2018 Contents World Cancer Research Fund Network 3 Executive Summary
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and cancers of the mouth, pharynx and larynx 2018 Contents World Cancer Research Fund Network 3 Executive Summary
World Cancer Research Fund International Systematic Literature Review
 World Cancer Research Fund International Systematic Literature Review The Associations between Food, Nutrition and Physical Activity and the Risk of Cervical Cancer Imperial College London Continuous Update
World Cancer Research Fund International Systematic Literature Review The Associations between Food, Nutrition and Physical Activity and the Risk of Cervical Cancer Imperial College London Continuous Update
Cancers attributable to excess body weight in Canada in D Zakaria, A Shaw Public Health Agency of Canada
 Cancers attributable to excess body weight in Canada in 2010 D Zakaria, A Shaw Public Health Agency of Canada Introduction Cancer is a huge burden in Canada: Nearly 50% of Canadians are expected to be
Cancers attributable to excess body weight in Canada in 2010 D Zakaria, A Shaw Public Health Agency of Canada Introduction Cancer is a huge burden in Canada: Nearly 50% of Canadians are expected to be
Body Mass Index, Smoking, and Alcohol and Risks of Barrett s Esophagus and Esophageal Adenocarcinoma: A UK Prospective Cohort Study
 Dig Dis Sci (2014) 59:1552 1559 DOI 10.1007/s10620-013-3024-z ORIGINAL ARTICLE Body Mass Index, Smoking, and Alcohol and Risks of Barrett s Esophagus and Esophageal Adenocarcinoma: A UK Prospective Cohort
Dig Dis Sci (2014) 59:1552 1559 DOI 10.1007/s10620-013-3024-z ORIGINAL ARTICLE Body Mass Index, Smoking, and Alcohol and Risks of Barrett s Esophagus and Esophageal Adenocarcinoma: A UK Prospective Cohort
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and breast cancer survivors. Revised 2018
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and breast cancer survivors 2014 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and breast cancer survivors 2014 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
Cancer Survivors: - Asian Perspective
 Cancer Survivors: What we Know, What we Need to Know - Asian Perspective Prof. Josette Sin-yee Chor School of Public Health and Primary Care The Chinese University of Hong Kong Asia Varying incidence of
Cancer Survivors: What we Know, What we Need to Know - Asian Perspective Prof. Josette Sin-yee Chor School of Public Health and Primary Care The Chinese University of Hong Kong Asia Varying incidence of
Processed meats and cancer Mariana C. Stern, PhD Associate Professor of Preventive Medicine & Urology USC Norris Comprehensive Cancer Center
 Processed meats and cancer Mariana C. Stern, PhD Associate Professor of Preventive Medicine & Urology USC Norris Comprehensive Cancer Center July 29, 2016 International Conference on Nutrition in Medicine
Processed meats and cancer Mariana C. Stern, PhD Associate Professor of Preventive Medicine & Urology USC Norris Comprehensive Cancer Center July 29, 2016 International Conference on Nutrition in Medicine
Original Article Dietary nitrite and nitrate is not associated with adult glioma risk: a meta-analysis
 Int J Clin Exp Med 2016;9(5):8334-8340 www.ijcem.com /ISSN:1940-5901/IJCEM0021458 Original Article Dietary nitrite and nitrate is not associated with adult glioma risk: a meta-analysis Peng Wang 2*, Chong-Xian
Int J Clin Exp Med 2016;9(5):8334-8340 www.ijcem.com /ISSN:1940-5901/IJCEM0021458 Original Article Dietary nitrite and nitrate is not associated with adult glioma risk: a meta-analysis Peng Wang 2*, Chong-Xian
IJC International Journal of Cancer
 IJC International Journal of Cancer Association between height and thyroid cancer risk: A meta-analysis of prospective studies Zhaohai Jing 1 *, Xu Hou 1 *, Ying Liu 1, Shengli Yan 1, Robin Wang 1,2, Shihua
IJC International Journal of Cancer Association between height and thyroid cancer risk: A meta-analysis of prospective studies Zhaohai Jing 1 *, Xu Hou 1 *, Ying Liu 1, Shengli Yan 1, Robin Wang 1,2, Shihua
/Webpages/zhang/chinese-full full- program.htm
 http://www.ph.ucla.edu/epi/faculty/zhang /Webpages/zhang/chinese-full full- program.htm Cancer Incidence and Mortality and Risk Factors in the World Zuo-Feng Zhang, M.D., Ph.D. Fogarty International Training
http://www.ph.ucla.edu/epi/faculty/zhang /Webpages/zhang/chinese-full full- program.htm Cancer Incidence and Mortality and Risk Factors in the World Zuo-Feng Zhang, M.D., Ph.D. Fogarty International Training
Table Cohort studies of consumption of alcoholic beverages and cancer of the colorectum
 Akhter et al. (2007), Japan, Miyagi Study [data also included in the pooled analysis, Mizoue et al. (2008)] of 21 199 men living in the Miyagi region recruited in 1990; aged 40 64 years; followed-up until
Akhter et al. (2007), Japan, Miyagi Study [data also included in the pooled analysis, Mizoue et al. (2008)] of 21 199 men living in the Miyagi region recruited in 1990; aged 40 64 years; followed-up until
Cancer outcomes associated with food, food contaminants, obesity and dietary patterns: from science to policy
 Cancer outcomes associated with food, food contaminants, obesity and dietary patterns: from science to policy Operationalising the WCRF/AICR cancer prevention recommendations using an index score: recent
Cancer outcomes associated with food, food contaminants, obesity and dietary patterns: from science to policy Operationalising the WCRF/AICR cancer prevention recommendations using an index score: recent
Does Being Overweight Really Reduce Mortality?
 Does Being Overweight Really Reduce Mortality? The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version Accessed
Does Being Overweight Really Reduce Mortality? The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version Accessed
Body Iron Stores and Heme-Iron Intake in Relation to Risk of Type 2 Diabetes: A Systematic Review and Meta- Analysis
 Body Iron Stores and Heme-Iron Intake in Relation to Risk of Type 2 Diabetes: A Systematic Review and Meta- Analysis Zhuoxian Zhao 1, Sheyu Li 1, Guanjian Liu 2, Fangfang Yan 1, Xuelei Ma 3, Zeyu Huang
Body Iron Stores and Heme-Iron Intake in Relation to Risk of Type 2 Diabetes: A Systematic Review and Meta- Analysis Zhuoxian Zhao 1, Sheyu Li 1, Guanjian Liu 2, Fangfang Yan 1, Xuelei Ma 3, Zeyu Huang
Dairy products and the risk of type 2 diabetes: a systematic review and dose-response meta-analysis of cohort studies 1 3
 Dairy products and the risk of type 2 diabetes: a systematic review and dose-response meta-analysis of cohort studies 1 3 Dagfinn Aune, Teresa Norat, Pål Romundstad, and Lars J Vatten ABSTRACT Background:
Dairy products and the risk of type 2 diabetes: a systematic review and dose-response meta-analysis of cohort studies 1 3 Dagfinn Aune, Teresa Norat, Pål Romundstad, and Lars J Vatten ABSTRACT Background:
Relation of Height and Body Mass Index to Renal Cell Carcinoma in Two Million Norwegian Men and Women
 American Journal of Epidemiology Copyright 2004 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 160, No. 12 Printed in U.S.A. DOI: 10.1093/aje/kwh345 Relation of Height
American Journal of Epidemiology Copyright 2004 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 160, No. 12 Printed in U.S.A. DOI: 10.1093/aje/kwh345 Relation of Height
Epidemiology 101. Nutritional Epidemiology Methods and Interpretation Criteria
 Slide 1 Epidemiology 101 Nutritional Epidemiology Methods and Interpretation Criteria Andrew Milkowski PhD Adjunct Professor University of Wisconsin Muscle Biology Laboratory amilkowski@ansci.wisc.edu
Slide 1 Epidemiology 101 Nutritional Epidemiology Methods and Interpretation Criteria Andrew Milkowski PhD Adjunct Professor University of Wisconsin Muscle Biology Laboratory amilkowski@ansci.wisc.edu
Obesity and Breast Cancer in a Multiethnic Population. Gertraud Maskarinec, MD, PhD University of Hawaii Cancer Center, Honolulu, HI
 Obesity and Breast Cancer in a Multiethnic Population Gertraud Maskarinec, MD, PhD University of Hawaii Cancer Center, Honolulu, HI Background Breast cancer incidence remains lower in many Asian than Western
Obesity and Breast Cancer in a Multiethnic Population Gertraud Maskarinec, MD, PhD University of Hawaii Cancer Center, Honolulu, HI Background Breast cancer incidence remains lower in many Asian than Western
Consideration of Anthropometric Measures in Cancer. S. Lani Park April 24, 2009
 Consideration of Anthropometric Measures in Cancer S. Lani Park April 24, 2009 Presentation outline Background in anthropometric measures in cancer Examples of anthropometric measures and investigating
Consideration of Anthropometric Measures in Cancer S. Lani Park April 24, 2009 Presentation outline Background in anthropometric measures in cancer Examples of anthropometric measures and investigating
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and breast cancer survivors. In partnership with
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and breast cancer survivors 2014 In partnership with Contents About World Cancer Research Fund International 1 Our
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and breast cancer survivors 2014 In partnership with Contents About World Cancer Research Fund International 1 Our
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and colorectal cancer. Managed and produced by:
 Analysing research on prevention and survival Diet, nutrition, physical activity and colorectal 2017 Managed and produced by: Contents World Cancer Research Fund network 3 Executive summary 5 1. Summary
Analysing research on prevention and survival Diet, nutrition, physical activity and colorectal 2017 Managed and produced by: Contents World Cancer Research Fund network 3 Executive summary 5 1. Summary
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and stomach cancer. Revised 2018
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and stomach cancer 2016 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and stomach cancer 2016 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
Biomarkers: examples from cancer epidemiology
 Biomarkers: examples from cancer epidemiology In memory of Sheila Bingham Tim Key Cancer Epidemiology Unit Nuffield Department of Clinical Medicine University of Oxford Sheila Bingham (Rodwell) 1947-2009
Biomarkers: examples from cancer epidemiology In memory of Sheila Bingham Tim Key Cancer Epidemiology Unit Nuffield Department of Clinical Medicine University of Oxford Sheila Bingham (Rodwell) 1947-2009
Outline. Background on the American Institute for Cancer Research (AICR) and Continuous Update Project (CUP)
 Alcohol and Cancer: State of the Science Christine L. Sardo Molmenti PhD, MPH, RD AICR Science Analyst Assistant Professor Hofstra-Northwell School of Medicine Northwell Health April 25, 2017 Outline Background
Alcohol and Cancer: State of the Science Christine L. Sardo Molmenti PhD, MPH, RD AICR Science Analyst Assistant Professor Hofstra-Northwell School of Medicine Northwell Health April 25, 2017 Outline Background
Table Case-control studies on consumption of alcoholic beverages and cancer of the oesophagus
 Vioque et al. (2008), Spain, 1995 99 Oesophagus 202 (187 men, 15 women), histologically confirmed; 160 (79.2%) squamous-cell carcinomas, 42 adenocarcinoma; Participation rate, 95.8%. Face-to-face interview
Vioque et al. (2008), Spain, 1995 99 Oesophagus 202 (187 men, 15 women), histologically confirmed; 160 (79.2%) squamous-cell carcinomas, 42 adenocarcinoma; Participation rate, 95.8%. Face-to-face interview
The international health care burden of cancers of the gastrointestinal tract and liver
 The international health care burden of cancers of the gastrointestinal tract and liver William R. Brown 1*, Dennis J. Ahnen 2 1 Department of Medicine, University of Colorado School of Medicine, Denver,
The international health care burden of cancers of the gastrointestinal tract and liver William R. Brown 1*, Dennis J. Ahnen 2 1 Department of Medicine, University of Colorado School of Medicine, Denver,
Diabetes mellitus and incidence of kidney cancer: a meta-analysis of cohort studies
 Diabetologia (2011) 54:1013 1018 DOI 10.1007/s00125-011-2051-6 ARTICLE Diabetes mellitus and incidence of kidney cancer: a meta-analysis of cohort studies S. C. Larsson & A. Wolk Received: 26 October 2010
Diabetologia (2011) 54:1013 1018 DOI 10.1007/s00125-011-2051-6 ARTICLE Diabetes mellitus and incidence of kidney cancer: a meta-analysis of cohort studies S. C. Larsson & A. Wolk Received: 26 October 2010
Continuous Update Project Keeping the science current d n u h F c r a e s e r R e c d C l r o Breast Cancer 2010 Report
 World Cancer Research Fund American Institute for Cancer Research Continuous Update Project Keeping the science current Join a sponsored walk in your community to raise funds for World Cancer Research
World Cancer Research Fund American Institute for Cancer Research Continuous Update Project Keeping the science current Join a sponsored walk in your community to raise funds for World Cancer Research
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and prostate cancer. Revised 2018
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and prostate cancer 2014 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and prostate cancer 2014 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
Protocol Version 2. Prepared by: CUP Team, Imperial College London, May 2013 Reviewed in August 2013
 Protocol Version 2 Continuous Update and Systematic Literature Review of Randomised Controlled Trials, Prospective Studies and Case-control Studies on Food, Nutrition, Physical Activity and Cancers of
Protocol Version 2 Continuous Update and Systematic Literature Review of Randomised Controlled Trials, Prospective Studies and Case-control Studies on Food, Nutrition, Physical Activity and Cancers of
The Role of Observational Studies. Edward Giovannucci, MD, ScD Departments of Nutrition and Epidemiology
 The Role of Observational Studies Edward Giovannucci, MD, ScD Departments of Nutrition and Epidemiology Disclosure Information As required, I would like to report that I have no financial relationships
The Role of Observational Studies Edward Giovannucci, MD, ScD Departments of Nutrition and Epidemiology Disclosure Information As required, I would like to report that I have no financial relationships
7.10 Breast FOOD, NUTRITION, PHYSICAL ACTIVITY, AND CANCER OF THE BREAST (POSTMENOPAUSE)
 7.10 Breast FOOD, NUTRITION, PHYSICAL ACTIVITY, AND CANCER OF THE BREAST (PREMENOPAUSE) In the judgement of the Panel, the factors listed below modify the risk of cancer of the breast (premenopause). Judgements
7.10 Breast FOOD, NUTRITION, PHYSICAL ACTIVITY, AND CANCER OF THE BREAST (PREMENOPAUSE) In the judgement of the Panel, the factors listed below modify the risk of cancer of the breast (premenopause). Judgements
Green Tea and Cancer. Alison Chiang EPI295 October 30,2009
 Green Tea and Cancer Alison Chiang EPI295 October 30,2009 Overview Pathways to cancer Green tea Chemical composition Potential mechanisms General study findings Study 1 Study 2 How does cancer develop?
Green Tea and Cancer Alison Chiang EPI295 October 30,2009 Overview Pathways to cancer Green tea Chemical composition Potential mechanisms General study findings Study 1 Study 2 How does cancer develop?
RESEARCH COMMUNICATION
 RESEARCH COMMUNICATION Comparison of Lifestyle and Living Environment Among High Risk Immigrant and Low Risk Host Residents: Implications for Esophageal Cancer Etiology Xiang Yu 1, Tao Zhang 1, Hexi Zhang
RESEARCH COMMUNICATION Comparison of Lifestyle and Living Environment Among High Risk Immigrant and Low Risk Host Residents: Implications for Esophageal Cancer Etiology Xiang Yu 1, Tao Zhang 1, Hexi Zhang
Index-based Dietary Patterns and Risk of Esophageal and Gastric Cancer in a Large Cohort Study
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:1130 1136 Index-based Dietary Patterns and Risk of Esophageal and Gastric Cancer in a Large Cohort Study WEN QING LI,* YIKYUNG PARK, JENNIFER W. WU, JIAN
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:1130 1136 Index-based Dietary Patterns and Risk of Esophageal and Gastric Cancer in a Large Cohort Study WEN QING LI,* YIKYUNG PARK, JENNIFER W. WU, JIAN
Classifying Foods as Carcinogenic? A Case Study of Red and Processed Meats.
 Classifying Foods as Carcinogenic? A Case Study of Red and Processed Meats. Andrew Milkowski Feb 23, 2016 Outline What is IARC? How are Carcinogen Classifications Determined 2015 IARC Evaluation of Red
Classifying Foods as Carcinogenic? A Case Study of Red and Processed Meats. Andrew Milkowski Feb 23, 2016 Outline What is IARC? How are Carcinogen Classifications Determined 2015 IARC Evaluation of Red
Olio di oliva nella prevenzione. Carlo La Vecchia Università degli Studi di Milano Enrico Pira Università degli Studi di Torino
 Olio di oliva nella prevenzione della patologia cronicodegenerativa, con focus sul cancro Carlo La Vecchia Università degli Studi di Milano Enrico Pira Università degli Studi di Torino Olive oil and cancer:
Olio di oliva nella prevenzione della patologia cronicodegenerativa, con focus sul cancro Carlo La Vecchia Università degli Studi di Milano Enrico Pira Università degli Studi di Torino Olive oil and cancer:
IJC International Journal of Cancer
 IJC International Journal of Cancer Consumption of salted meat and its interactions with alcohol drinking and tobacco smoking on esophageal squamous-cell carcinoma Sihao Lin 1, Xiaorong Wang 1, Chengyu
IJC International Journal of Cancer Consumption of salted meat and its interactions with alcohol drinking and tobacco smoking on esophageal squamous-cell carcinoma Sihao Lin 1, Xiaorong Wang 1, Chengyu
Intake of fruit and vegetables has been hypothesized to
 GASTROENTEROLOGY 2011;141:106 118 Nonlinear Reduction in Risk for Colorectal Cancer by and Vegetable Intake Based on Meta-analysis of Prospective Studies DAGFINN AUNE,* ROSA LAU,* DORIS S. M. CHAN,* RUI
GASTROENTEROLOGY 2011;141:106 118 Nonlinear Reduction in Risk for Colorectal Cancer by and Vegetable Intake Based on Meta-analysis of Prospective Studies DAGFINN AUNE,* ROSA LAU,* DORIS S. M. CHAN,* RUI
Ecologic Study of Serum Selenium and Upper Gastrointestinal Cancers in Iran
 Serum Selenium and Upper GI Cancers Nouraie M Pourshams A Kamangar F Mir-Nasseri MM Sotoudeh M Derakhshan MH Akbari MR Fakheri H Mazandaran University of Medical Zahedi MJ Kerman University of Medical
Serum Selenium and Upper GI Cancers Nouraie M Pourshams A Kamangar F Mir-Nasseri MM Sotoudeh M Derakhshan MH Akbari MR Fakheri H Mazandaran University of Medical Zahedi MJ Kerman University of Medical
Dietary soy intake and changes of mammographic density in premenopausal Chinese women
 Dietary soy intake and changes of mammographic density in premenopausal Chinese women 2010 WCRF International Conference, Nutrition, Physical Activity and Cancer Prevention: Current Challenges, New Horizons
Dietary soy intake and changes of mammographic density in premenopausal Chinese women 2010 WCRF International Conference, Nutrition, Physical Activity and Cancer Prevention: Current Challenges, New Horizons
Analyses on Cancer Incidence and Mortality in Huai an Area, China, 2010
 Open Journal of Preventive Medicine, 2014, 4, 504-512 Published Online June 2014 in SciRes. http://www.scirp.org/journal/ojpm http://dx.doi.org/10.4236/ojpm.2014.46059 Analyses on Cancer Incidence and
Open Journal of Preventive Medicine, 2014, 4, 504-512 Published Online June 2014 in SciRes. http://www.scirp.org/journal/ojpm http://dx.doi.org/10.4236/ojpm.2014.46059 Analyses on Cancer Incidence and
Dietary intake in male and female smokers, ex-smokers, and never smokers: The INTERMAP Study
 (2003) 17, 641 654 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Dietary intake in male and female smokers, ex-smokers, and never smokers: The
(2003) 17, 641 654 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Dietary intake in male and female smokers, ex-smokers, and never smokers: The
Meat Consumption and Risk of Esophageal and Gastric Cancer in a Large Prospective Study
 nature publishing group ORIGINAL CONTRIBUTIONS 1 Meat Consumption and Risk of Esophageal and Gastric Cancer in a Large Prospective Study Amanda J. Cross, PhD 1, Neal D. Freedman, PhD 1, Jiansong Ren, PhD
nature publishing group ORIGINAL CONTRIBUTIONS 1 Meat Consumption and Risk of Esophageal and Gastric Cancer in a Large Prospective Study Amanda J. Cross, PhD 1, Neal D. Freedman, PhD 1, Jiansong Ren, PhD
Association of mir-21 with esophageal cancer prognosis: a meta-analysis
 Association of mir-21 with esophageal cancer prognosis: a meta-analysis S.-W. Wen 1, Y.-F. Zhang 1, Y. Li 1, Z.-X. Liu 2, H.-L. Lv 1, Z.-H. Li 1, Y.-Z. Xu 1, Y.-G. Zhu 1 and Z.-Q. Tian 1 1 Department of
Association of mir-21 with esophageal cancer prognosis: a meta-analysis S.-W. Wen 1, Y.-F. Zhang 1, Y. Li 1, Z.-X. Liu 2, H.-L. Lv 1, Z.-H. Li 1, Y.-Z. Xu 1, Y.-G. Zhu 1 and Z.-Q. Tian 1 1 Department of
Exposed cases/deaths. or level. Lung All coffee (cups/day) Sex, smoking history, β-carotene intake Coffee intake Never 133 1
 Vol 6 Monograph 0 Drinking coffee Section 2 Table 2.4 Table 2.4 Case control studies (hospitalbased) on cancer of the lung and coffee drinking (web only) Mettlin (989) Baffalo, US 982 987 569; histologically
Vol 6 Monograph 0 Drinking coffee Section 2 Table 2.4 Table 2.4 Case control studies (hospitalbased) on cancer of the lung and coffee drinking (web only) Mettlin (989) Baffalo, US 982 987 569; histologically
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and endometrial cancer. Revised 2018
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and endometrial cancer 2013 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and endometrial cancer 2013 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
Tea and Cancer Introduction What is cancer? Causes of cancer Diet and cancer
 Tea and Cancer Introduction Cancer is a major cause of morbidity in the UK with over 200,000 newly diagnosed cases, and around 120,000 deaths from cancer each year. It is expected that more than one in
Tea and Cancer Introduction Cancer is a major cause of morbidity in the UK with over 200,000 newly diagnosed cases, and around 120,000 deaths from cancer each year. It is expected that more than one in
Impact of individual risk factors on German life expectancy
 Impact of individual risk factors on German life expectancy Wilma J. Nusselder and Jose Rubio Valverde Erasmus MC, Rotterdam June 2018 1 Contents Introduction... 3 Part 1 Relative risks of mortality associated
Impact of individual risk factors on German life expectancy Wilma J. Nusselder and Jose Rubio Valverde Erasmus MC, Rotterdam June 2018 1 Contents Introduction... 3 Part 1 Relative risks of mortality associated
Incidence and mortality of laryngeal cancer in China, 2011
 Original Article Incidence and mortality of laryngeal cancer in China, 2011 Lingbin Du 1, Huizhang Li 1, Chen Zhu 1, Rongshou Zheng 2, Siwei Zhang 2, Wanqing Chen 2 1 Zhejiang Provincial Office for Cancer
Original Article Incidence and mortality of laryngeal cancer in China, 2011 Lingbin Du 1, Huizhang Li 1, Chen Zhu 1, Rongshou Zheng 2, Siwei Zhang 2, Wanqing Chen 2 1 Zhejiang Provincial Office for Cancer
The Impact of Body Mass Index on Esophageal Cancer
 Obesity does not appear to affect the morbidity of treatments for esophageal cancer. Samuel Bak. BK1464 Added Perspective I. Oil on canvas, 12ʺ 16ʺ. The Impact of Body Mass Index on Esophageal Cancer Joyce
Obesity does not appear to affect the morbidity of treatments for esophageal cancer. Samuel Bak. BK1464 Added Perspective I. Oil on canvas, 12ʺ 16ʺ. The Impact of Body Mass Index on Esophageal Cancer Joyce
what s new? CONFERENCE ALCOHOL AND HEALTH Amsterdam, 23 September 2010
 CONFERENCE ALCOHOL AND HEALTH Amsterdam, 23 September 2010 Alcohol drinking and cancer risk: what s new? Dr Paule LATINO-MARTEL UMR U 557 Inserm, U 1125 Inra, Cnam, Université Paris 13; CRNH-IdF, France
CONFERENCE ALCOHOL AND HEALTH Amsterdam, 23 September 2010 Alcohol drinking and cancer risk: what s new? Dr Paule LATINO-MARTEL UMR U 557 Inserm, U 1125 Inra, Cnam, Université Paris 13; CRNH-IdF, France
Pattern of esophageal cancer in tertiary care hospital in North India: a clinicopathological study
 International Journal of Research in Medical Sciences Gupta V et al. Int J Res Med Sci. 2017 Apr;5(4):1405-1409 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20171235
International Journal of Research in Medical Sciences Gupta V et al. Int J Res Med Sci. 2017 Apr;5(4):1405-1409 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20171235
Consuming a Varied Diet can Prevent Diabetes But Can You Afford the Added Cost? Annalijn Conklin 18 January 2017, Vancouver, Canada
 1 Consuming a Varied Diet can Prevent Diabetes But Can You Afford the Added Cost? Annalijn Conklin 18 January 2017, Vancouver, Canada 2 Overview The problem of type 2 diabetes What is diet diversity /
1 Consuming a Varied Diet can Prevent Diabetes But Can You Afford the Added Cost? Annalijn Conklin 18 January 2017, Vancouver, Canada 2 Overview The problem of type 2 diabetes What is diet diversity /
Attributable Causes of Cancer in China: Fruit and Vegetable
 www.springerlink.com Chin J Cancer Res 23(3):171-176, 2011 171 Original Article Attributable Causes of Cancer in China: Fruit and Vegetable Hui-juan Xiao 1, 2, 6, Hao Liang 2, Jian-bing Wang 2, 3, Cheng-Yu
www.springerlink.com Chin J Cancer Res 23(3):171-176, 2011 171 Original Article Attributable Causes of Cancer in China: Fruit and Vegetable Hui-juan Xiao 1, 2, 6, Hao Liang 2, Jian-bing Wang 2, 3, Cheng-Yu
Body-mass index and cause-specific mortality in adults: collaborative analyses of 57 prospective studies
 Body-mass index and cause-specific mortality in 900 000 adults: collaborative analyses of 57 prospective studies Prospective Studies Collaboration* Summary Background The main associations of body-mass
Body-mass index and cause-specific mortality in 900 000 adults: collaborative analyses of 57 prospective studies Prospective Studies Collaboration* Summary Background The main associations of body-mass
Alcol e tumori con focus sulle basse dosi
 Alcol e tumori con focus sulle basse dosi Carlo La Vecchia Department of Epidemiology, Istituto Mario Negri Department of Clinical Sciences and Community Health, Università degli Studi di Milano 1 Cancers
Alcol e tumori con focus sulle basse dosi Carlo La Vecchia Department of Epidemiology, Istituto Mario Negri Department of Clinical Sciences and Community Health, Università degli Studi di Milano 1 Cancers
RESEARCH. open access ABSTRACT
 open access Whole grain consumption and risk of cardiovascular disease, cancer, and all cause and cause specific mortality: systematic review and dose-response meta-analysis of prospective studies Dagfinn
open access Whole grain consumption and risk of cardiovascular disease, cancer, and all cause and cause specific mortality: systematic review and dose-response meta-analysis of prospective studies Dagfinn
Epidemiology of weak associations The case of nutrition and cancer. Paolo Boffetta Icahn School of Medicine at Mount Sinai New York NY
 Epidemiology of weak associations The case of nutrition and cancer Paolo Boffetta Icahn School of Medicine at Mount Sinai New York NY Causality in epidemiology Epidemiology can lead to the identification
Epidemiology of weak associations The case of nutrition and cancer Paolo Boffetta Icahn School of Medicine at Mount Sinai New York NY Causality in epidemiology Epidemiology can lead to the identification
Nitrate in drinking water and cancer risk
 Nitrate in drinking water and cancer risk Mary H. Ward, M.S., Ph.D. Occupational and Environmental Epidemiology Branch Division of Cancer Epidemiology & Genetics NCI, NIH Challenges to Providing Safe Drinking
Nitrate in drinking water and cancer risk Mary H. Ward, M.S., Ph.D. Occupational and Environmental Epidemiology Branch Division of Cancer Epidemiology & Genetics NCI, NIH Challenges to Providing Safe Drinking
Tobacco Smoking Increases the Risk of High-Grade Dysplasia and Cancer Among Patients With Barrett s Esophagus
 GASTROENTEROLOGY 2012;142:233 240 CLINCAL ALIMENTARY TRACT Tobacco Smoking Increases the Risk of High-Grade Dysplasia and Cancer Among Patients With Barrett s Esophagus HELEN G. COLEMAN,* SHIVARAM BHAT,*
GASTROENTEROLOGY 2012;142:233 240 CLINCAL ALIMENTARY TRACT Tobacco Smoking Increases the Risk of High-Grade Dysplasia and Cancer Among Patients With Barrett s Esophagus HELEN G. COLEMAN,* SHIVARAM BHAT,*
Biomed Environ Sci, 2015; 28(7):
 Biomed Environ Sci, 2015; 28(7): 527-534 527 Letter to the Editor Nonlinear Reduction in Risk for Type 2 Diabetes by Magnesium Intake: An Updated Meta-Analysis of Prospective Cohort Studies* XU Tian1,^,
Biomed Environ Sci, 2015; 28(7): 527-534 527 Letter to the Editor Nonlinear Reduction in Risk for Type 2 Diabetes by Magnesium Intake: An Updated Meta-Analysis of Prospective Cohort Studies* XU Tian1,^,
Lack of association between IL-6-174G>C polymorphism and lung cancer: a metaanalysis
 Lack of association between IL-6-174G>C polymorphism and lung cancer: a metaanalysis Y. Liu, X.L. Song, G.L. Zhang, A.M. Peng, P.F. Fu, P. Li, M. Tan, X. Li, M. Li and C.H. Wang Department of Respiratory
Lack of association between IL-6-174G>C polymorphism and lung cancer: a metaanalysis Y. Liu, X.L. Song, G.L. Zhang, A.M. Peng, P.F. Fu, P. Li, M. Tan, X. Li, M. Li and C.H. Wang Department of Respiratory
Inverse Association Between Gluteofemoral Obesity and Risk of Barrett s Esophagus in a Pooled Analysis
 Accepted Manuscript Inverse Association Between Gluteofemoral Obesity and Risk of Barrett s Esophagus in a Pooled Analysis Bradley J. Kendall, Joel H. Rubenstein, Michael B. Cook, Thomas L. Vaughan, Lesley
Accepted Manuscript Inverse Association Between Gluteofemoral Obesity and Risk of Barrett s Esophagus in a Pooled Analysis Bradley J. Kendall, Joel H. Rubenstein, Michael B. Cook, Thomas L. Vaughan, Lesley
Esophageal Squamous Cell Carcinoma Presenting as Two Simultaneous Adjacent Masses Confirmed by Pathologic Findings: Report of a Rare Case
 Case Reports in Clinical Practice VOL 3, NO 1, 2018 Case Report Esophageal Squamous Cell Carcinoma Presenting as Two Simultaneous Adjacent Masses Confirmed by Pathologic Findings: Report of a Rare Case
Case Reports in Clinical Practice VOL 3, NO 1, 2018 Case Report Esophageal Squamous Cell Carcinoma Presenting as Two Simultaneous Adjacent Masses Confirmed by Pathologic Findings: Report of a Rare Case
Diet, obesity, lifestyle and cancer prevention:
 Diet, obesity, lifestyle and cancer prevention: Epidemiologic perspectives Graham A Colditz, MD DrPH Niess-Gain Professor Chief, November, 2017 Outline Review evidence on contribution of diet, obesity,
Diet, obesity, lifestyle and cancer prevention: Epidemiologic perspectives Graham A Colditz, MD DrPH Niess-Gain Professor Chief, November, 2017 Outline Review evidence on contribution of diet, obesity,
Esophageal cancer Study: China Story
 NCI-IARC Tumor workshop: Esophageal Squamous Cell Carcinoma Esophageal cancer Study: China Story Youlin Qiao, Shaoming Wang Dept. of Cancer Epidemiology Cancer Institute/Hospital Chinese Academy of Medical
NCI-IARC Tumor workshop: Esophageal Squamous Cell Carcinoma Esophageal cancer Study: China Story Youlin Qiao, Shaoming Wang Dept. of Cancer Epidemiology Cancer Institute/Hospital Chinese Academy of Medical
DIABETES, PHYSICAL ACTIVITY AND ENDOMETRIAL CANCER. Emilie Friberg
 Division of Nutritional Epidemiology, Institute of Environmental Medicine, Karolinska Institutet, Stockholm, Sweden, 2006 DIABETES, PHYSICAL ACTIVITY AND ENDOMETRIAL CANCER Emilie Friberg Stockholm 2006
Division of Nutritional Epidemiology, Institute of Environmental Medicine, Karolinska Institutet, Stockholm, Sweden, 2006 DIABETES, PHYSICAL ACTIVITY AND ENDOMETRIAL CANCER Emilie Friberg Stockholm 2006
Table Case-control studies on tobacco smoking and oesophageal cancer (unspecified) or squamous cell carcinoma of the oesophagus DRAFT
 Table 2.21. Case-control studies on tobacco smoking and oesophageal cancer (unspecified) or squamous cell of Brown et al. (2001) USA 1986-1989 Sharp et al. (2001) UK 1993-1996 Gallus et al. (2001) Italy
Table 2.21. Case-control studies on tobacco smoking and oesophageal cancer (unspecified) or squamous cell of Brown et al. (2001) USA 1986-1989 Sharp et al. (2001) UK 1993-1996 Gallus et al. (2001) Italy
The Associations between Food, Nutrition and Physical Activity and the Risk of Skin Cancer
 The Associations between Food, Nutrition and Physical Activity and the Risk of Skin Cancer Imperial College London Continuous Update Project Team Members Teresa Norat Snieguole Vingeliene Elli Polemiti
The Associations between Food, Nutrition and Physical Activity and the Risk of Skin Cancer Imperial College London Continuous Update Project Team Members Teresa Norat Snieguole Vingeliene Elli Polemiti
Genome-wide association study of esophageal squamous cell carcinoma in Chinese subjects identifies susceptibility loci at PLCE1 and C20orf54
 CORRECTION NOTICE Nat. Genet. 42, 759 763 (2010); published online 22 August 2010; corrected online 27 August 2014 Genome-wide association study of esophageal squamous cell carcinoma in Chinese subjects
CORRECTION NOTICE Nat. Genet. 42, 759 763 (2010); published online 22 August 2010; corrected online 27 August 2014 Genome-wide association study of esophageal squamous cell carcinoma in Chinese subjects
Association between the -77T>C polymorphism in the DNA repair gene XRCC1 and lung cancer risk
 Association between the -77T>C polymorphism in the DNA repair gene XRCC1 and lung cancer risk B.B. Sun, J.Z. Wu, Y.G. Li and L.J. Ma Department of Respiratory Medicine, People s Hospital Affiliated to
Association between the -77T>C polymorphism in the DNA repair gene XRCC1 and lung cancer risk B.B. Sun, J.Z. Wu, Y.G. Li and L.J. Ma Department of Respiratory Medicine, People s Hospital Affiliated to
Risk Factors for Breast Cancer
 Lifestyle Factors The variations seen both regionally and internationally in breast cancer incidence have heightened interest in the medical community in the role of lifestyle-related influences. In general,
Lifestyle Factors The variations seen both regionally and internationally in breast cancer incidence have heightened interest in the medical community in the role of lifestyle-related influences. In general,
1 From the Cancer Epidemiology Unit, Nuffield Department of Population. 4 Address correspondence to KE Bradbury, Cancer Epidemiology Unit,
 Fruit, vegetable, and fiber intake in relation to cancer risk: findings from the European Prospective Investigation into Cancer and Nutrition (EPIC) 1 4 Kathryn E Bradbury, Paul N Appleby, and Timothy
Fruit, vegetable, and fiber intake in relation to cancer risk: findings from the European Prospective Investigation into Cancer and Nutrition (EPIC) 1 4 Kathryn E Bradbury, Paul N Appleby, and Timothy
Fruit & Vegetable Consumption and Mental Health
 Fruit & Vegetable Consumption and Mental Health Saverio Stranges, MD, PhD, FAHA Department of Epidemiology & Biostatistics, Western University Department of Family Medicine, Western University Department
Fruit & Vegetable Consumption and Mental Health Saverio Stranges, MD, PhD, FAHA Department of Epidemiology & Biostatistics, Western University Department of Family Medicine, Western University Department
Multivariate dose-response meta-analysis: an update on glst
 Multivariate dose-response meta-analysis: an update on glst Nicola Orsini Unit of Biostatistics Unit of Nutritional Epidemiology Institute of Environmental Medicine Karolinska Institutet http://www.imm.ki.se/biostatistics/
Multivariate dose-response meta-analysis: an update on glst Nicola Orsini Unit of Biostatistics Unit of Nutritional Epidemiology Institute of Environmental Medicine Karolinska Institutet http://www.imm.ki.se/biostatistics/
Pre-diagnostic cruciferous vegetables intake and lung cancer survival among Chinese women
 Pre-diagnostic cruciferous vegetables intake and lung cancer survival among Chinese women Qi-Jun Wu, Gong Yang, Wei Zheng, Hong-Lan Li, Jing Gao, Jing Wang, Yu-Tang Gao, Xiao-Ou Shu, Yong-Bing Xiang Supplementary
Pre-diagnostic cruciferous vegetables intake and lung cancer survival among Chinese women Qi-Jun Wu, Gong Yang, Wei Zheng, Hong-Lan Li, Jing Gao, Jing Wang, Yu-Tang Gao, Xiao-Ou Shu, Yong-Bing Xiang Supplementary
