SCAN Gynaecological Group. Clinical Management Protocols vulval cancer
|
|
|
- Pierce Wilkinson
- 6 years ago
- Views:
Transcription
1 SE Scotland Cancer Network SCAN Gynaecological Group Clinical Management Protocols vulval cancer August 2001 updated annually, most recently
2 INTRODUCTION The South East Scotland Cancer Network (SCAN) for Gynaecological Cancer was formally established over 10 years ago. Our first task was to develop a consensus document on management protocols. This year we have reviewed our protocols taking into account the Royal College of Gynaecologists report on vulval cancer published in CT and MRI scanning are also becoming increasingly important in the management of patients with gynaecological malignancy and the update reflects this. Patient pathways help patients, doctors, nurses and other members of the team to ensure that patients found to have gynaecological malignancy receive treatment in an appropriate and timely fashion. The clinical management protocols provide the evidence base on which to build these pathways. We are grateful for all the help that has been given by the members of SCAN in reviewing this document. David Farquharson and Melanie Mackean Previous and current chair of SCAN Gynaecological Group December 2009 Membership SCAN Gynae Group See i SCAN Gynae Group Clinical Management Protocol, August 2001/updated September 2009
3 THE MANAGEMENT OF CANCER OF THE VULVA Squamous cell carcinoma of the vulva is the most common malignant tumour, and accounts for approximately 4% of all gynaecological cancers. 80% occur after the menopause, especially in the 7th decade. Incidence approximate 2/100,000 women per year. Rarer malignancies include malignant melanoma, basal cell carcinoma, verrucous squamous carcinoma, Bartholin s gland carcinoma and adenocarcinoma. All patients, following a diagnosis of invasive carcinoma of the vulva, should be referred to the Edinburgh Combined Gynaecological Oncology Multidisciplinary Meeting for discussion regarding their further management. Patients with advanced disease will be seen by both the gynaecological oncologist and the clinical oncologist to discuss possible treatment options. It is well recognised that women with vulval cancer have a variety of psychosocial, psychosexual and informational needs. Patients will be provided with the opportunity to discuss their concerns and questions confidentially in a private area at all stages of the disease process. Written literature will be available to support verbal information. Referral to a Clinical Nurse Specialist will ensure continued support throughout the cancer journey. 1. DIAGNOSIS 1.1 Asymptomatic patients who may be at risk Vulval Intra-epithelial Neoplasia Grade III (VIN III) is the main potentially premalignant condition of the vulva. Adequate conservative therapy (by local excision and/or laser or hyfrecator treatment) can reduce the individual risks of developing carcinoma. Topical treatment with Imiquimod and be useful in conservative management of VIN. In women over the age of 35 the risk of malignant progression is thought to be higher than in younger age groups but at any age the decision to treat depends upon the vulvoscopic appearances, particularly with regard to the possibility of microinvasive disease, and symptomatology (pruritis or pain). Wart virus infection (especially HPV types 16 &18) in immunosuppressed patients can lead to potentially pre-malignant conditions of the vulva. Adequate local treatment with long-term follow up is necessary. Lichen Sclerosus of the vulva is found in association with squamous carcinoma in 3-6% of cases, but its true malignant potential is not known. Patients should be offered support to stop smoking, including referral to smoking cessation clinics, as this is a well recognised risk factor. Women with high grade VIN should be followed up in specialist multidisciplinary clinics or by gynaecology oncologists (RCOG recommendation) 1.2 Symptomatic patients Patients with vulval symptoms such as pruritus vulvae, pain, 2
4 discomfort, bleeding, discharge, nodularity, or ulceration must be closely examined for lesions such as an ulcer, a suspicious warty growth, a fungating growth or a pigmented lesion. Patients with suspicious vulval lesions should be referred to a gynaecologist with a view to biopsy and treatment. The biopsy, which should preferably be incisional rather than excisional, can often be done at the first clinic visit under local anaesthesia, On examination, the lesion is characterised by colour, site, size and laterality, and it is assessed for evidence of spread to the urethra, vagina, anus and/ or inguinal lymph nodes. Following biopsy to establish definitive diagnosis, the lesion is staged according to the FIGO classification (1988 Old; 2008 New). 1.3 Advanced disease Patients with advanced disease may present with a fungating lesion which may cause pain, urinary retention or rectal bleeding and faecal incontinence, depending on its site. Joint consultation with a gynaecological oncologist, urologist, colorectal surgeon and plastic surgeon may be appropriate. Following biopsy to establish definitive diagnosis, the lesion is staged according to the FIGO classification. 2. STAGING AND SPREAD OF DISEASE 2.1a Staging (FIGO ) FIGO updated vulval staging in Both are represented here as previous patients will be staged in the older system FIGO (Old) Stage 0 Carcinoma in situ (VIN3) Stage I Stage IA Microinvasive Carcinoma Tumour 2 cm in diameter confined to the vulva and/or perineum with no nodal metastasis A histological diagnosis in which the depth of stromal invasion is 1mm (measured from the basement membrane of the nearest dermal papilla) Stage IB Stage II IA but < or = 2cm diameter and confirmed to vulva/perineum with no nodal metastasis Tumour >2 cm in diameter confined to the vulva and/or perineum with no nodal metastasis Stage III Tumour of any diameter invading the lower urethra, vagina, or anus, and/or the presence of unilateral groin lymph node metastasis. 3
5 Stage IVa Tumour invasion of upper urethra, bladder or rectal mucosa, pelvic bone and/or bilateral regional lymph node metastases. Stage IVb Any distant metastasis including pelvic lymph nodes 2.1b 2008 FIGO (New) Stage I Tumour Confined to the Vulva IA Microinvasive Carcinoma IB Stage II Lesions 2cm, confined to vulva or perineum and in which the depth of stromal invasion is 1mm (measured from the basement membrane of the nearest dermal papilla). No nodal metastases Tumour >2 cm in diameter or with stromal invasion > 1.0mm, confined to the vulva and/or perineum with no nodal metastasis Tumour of any size with extension to adjacent perineal structures (1/3 lower urethra, 1/3 lower vagina, anus) with negative nodes Stage III IIIA (i) IIIA (ii) IIIB (i) IIIB (ii) IIIC Stage IV Stage IVa Tumour of any size with extension to adjacent perineal structures (1/3 lower urethra, 1/3 lower vagina, anus) with positive inguinofemoral lymph nodes With 1 lymph node metastasis ( 5 mm) or 1-2 lymph node metastasis(es) (< 5mm) With 2 or more lymph node metastases ( 5 mm), or 3 or more lymph node metastases (<5mm) With positive nodes with extracapsular spread Tumour invades other regional (2/3 upper urethra, 2/3 upper vagina) or distant structures Tumour invades any of the following: (i) (ii) Upper urethral and/or vaginal mucosa, bladder mucosa, rectal mucosa, or fixed to pelvic bone, or Fixed or ulcerated inguino-femoral lymph nodes Stage IVb Any distant metastasis including pelvic lymph nodes 2.2 Spread of disease i) Direct: vagina urethra anus bladder, rectum 4
6 pubic bone ii) Lymphatic: inguinal (embolic) femoral pelvic iii) Dissemination:usually late 3. STAGING INVESTIGATIONS i) Examination with or without anaesthetic and vulval biopsies ii) Rectovaginal examination (site dependent) iii) CXR iv) FBC, U&E, Creatinine, LFTs (In advanced disease) v) In advanced disease an MRI scan of the abdomen and pelvis may be helpful for assessment of local spread and measurement of tumour volume. MRI is probably more helpful than CT for the demonstration of lymph node enlargement, but is not always reliable. Any patient being considered for primary chemoradiotherapy should have pretreatment pelvic MRI and CTscan Chest/Abdomen. vi) PET-CT is useful in assessing advanced or recurrent disease and is mandatory prior to exenterative surgery. vii) Consider HIV testing if clinically indicated 4. HISTOPATHOLOGY see Appendix 2 5. TREATMENT All patients will have an opportunity to discuss their condition and will be given a full explanation of the aims and possible side effects of treatment, before giving their written informed consent to treatment. The aim of treatment is to excise disease with a 1cm margin of clearance on all sides. 5.1 Primary Lesions Confined to Vulva and/or Perineum Surgery is the treatment of choice. The aim of treatment is to excise disease with 1cm margin of clearance on all sides Micro-invasive carcinoma Lesions <2 cm in surface extent and 1 mm in depth of invasion should be treated by wide local excision. Groin node dissection is not required 5
7 Stage I Lesions 2 cm in surface extent and >1 mm in depth of invasion should be treated by radical vulvectomy and unilateral or bilateral groin lymphadenectomy through separate incisions. Unilateral, ipsilateral groin node dissection should be reserved for well lateralised lesions 2 cm in diameter, which do not involve the labia minora a lesion is well lateralised if the 1cm medial margin of clearance does not cross the midline. Large, anterior (clitoral/ labia minora) lesions, and those which cross the midline, tend to metastasise bilaterally. Stage II Lesions 2 cm in surface extent and >1 mm depth of invasion should be treated by radical vulvectomy and bilateral groin lymphadenectomy. The role of sentinel node biopsy is to guide selection of patients requiring full groin node dissection or post operative radiotherapy. This may limit post-operative morbidity where it is not indicated. Sentinel node biopsy is being undertaken in some trained centres and being evaluated through prospective multicentre trials. This may become standard management in the future. (In medically unfit elderly patients these guidelines may have to be modified.) Indications for post-operative radiotherapy A) Indications (Depending upon patient fitness and wishes): 1. Positive or close surgical margins (0.8cm) 2. 2 nodes (either or both sides) with microscopic disease 3. single macroscopically involved node 4. extra-nodal spread Consider whole pelvic radiotherapy if 1. 3 or more unilateral nodes involved 2. Bilateral nodal involvement Radiotherapy is usually 4500 cgy in 25 fractions given over a 5 week period. Full radiotherapy protocols are found on the Edinburgh Cancer Centre Quality Assurance Documents (OOQS). 5.2 Locally advanced disease Treatment should be individualised Surgery Ano-vulvectomy or exenterative surgery, with reconstruction should be considered for lesions involving the rectum, vagina or 6
8 Chemo-irradiation bladder, together with groin and/or pelvic lymphadenectomy. Myocutaneous flaps may be required to cover the surgical defect. Surgery is likely to involve a multidisciplinary team of gynaecology oncology specialists with input from urologist, coloproctologist surgeon, and plastic surgeon as required. Radiotherapy +/- chemotherapy should be considered. Primary radical radiotherapy A) Indications (depending upon patient wishes and fitness): Locally advanced squamous cell carcinoma of the vulva where exenterative surgery is being considered. B) Technique Radiotherapy is given in 2 phases over a possible 7 weeks according to the Edinburgh Cancer Centre protocol on OOQS. Phase I : 4500 cgy is given in 25 fractions over 5 weeks. Radiosensitizing chemotherapy is given as weekly cisplatin in selected patients. Phase 2: Response is first assess (4 weeks after starting radiotherapy) and should be rediscussed at the MDM. o 50% response proceed to Phase 2 o <50% response to consider surgical resection In phase two 2000cGy is given in 10 fractions over 2 weeks with no chemotherapy 6. FOLLOW-UP POLICY 6.1 After surgery 3-monthly for 1 year, 6-monthly for 1 year, then yearly to 5 years. Discharge at 5 years if well. 6.2 After chemo irradiation Patients will be reassessed 6-8 weeks post chemo-irradiation, and if there has been an unsatisfactory response will be re-evaluated regarding surgical options. Follow up as clinically indicated - usually 3 monthly for first 18 months, 6 monthly up to 3 years, then yearly to 5 years. Discharge at 5 years if well. Vaginal dilators will be offered to all patients. 6.3 Emotional support Vulval cancer is particularly distressing and patients may often feel lonely and isolated. Contact with Gynaecological oncology nurse specialist and/or pelvic dysfunction clinic is available where necessary at follow-up clinic. 7
9 7.. TREATMENT OF RECURRENT / METASTATIC DISEASE Palliative radiotherapy may be helpful to control bleeding and/ or ulceration from vulval recurrence and should be tailored to patient fitness, symptoms and wishes. Maximum dose of 3000 cgy in 10 fractions. Palliative chemotherapy may be considered with cisplatin according to patient wishes and fitness. 8. OTHER RARER MALIGNANCIES Basal cell carcinoma and verrucous squamous carcinoma these tumours metastasise only very rarely. Wide local excision is usually adequate. Malignant melanoma wide local excision is usually performed aiming for 1 cm clearance at all margins. Palpable groin nodes may be excised but in the absence of signs of clinical involvement groin lymph nodes are not routinely removed. CT scans are performed for staging disease. Bartholin s gland and adenocarcinoma treatment is similar to that for invasive squamous carcinoma of the vulva. Adenoid cystic carcinoma of Bartholin s gland is prone to perineural invasion and a much wider area than macroscopically involved will require treatment. 8
10 References Management of Vulval Cancer. RCOG Guidelines Jan 2006 Online Oncology Quality System (OOQS) - Edinburgh Cancer Protocol for vulval cancer, Edinburgh Cancer Centre Benedet JL, Bender H, Jones III H, Ngan HYS, Pecorelli S. Int J Gynecol Obstet 2000;70: Heaps JM. Gynecol Oncol, 38, , Katz A. Int J Radiat Oncol Biol Phys, 57, , McCall AR. Cancer, 75, , Gilroy JS. Med Dosim, 29, , Cunningham MJ. Gynecol Oncol, 66, , Homesley HD. Gynecol Oncol, 49, , Homesley HD, Am J Obstet Gynecol, 164, , Blake P. Best Practice & Research Clinical Obstetrics & Gynaecology; Vol. 17, No. 4, pp , 2003 Barnes EA, Thomas G, Semin Radiat Oncol 16:
11 Appendix 1 Summary of recommendations (RCOG 2006) Women with high grade VIN, Paget s disease and melanoma in situ should be followed up in specialist multidisciplinary clinics or by gynae oncologists (C) Women with an unexplained vulval lump should be referred urgently (C) Women with pain bleeding pruritis and ulceration should be referred routinely if symptoms persist (C) Vulval cancer should be managed in cancer centres/networks by multidisciplinary teams (B/C) Women should be seen and managed according to national directives on waiting times and time from diagnosis to treatment Radical treatment should not be undertaken without biopsy to confirm malignancy (C) Wide local excision of the primary with a minimum margin of 15mm is often sufficient (C) Groin node dissection should be omitted in stage 1a, melanoma, basal cell, verrucous tumours (B) Surgery is the treatment of choice for groin nodes, in women unfit for surgery XRT may be used (A/B) Groin node surgery can often be carried out through separate incisions in early disease skin bridge recurrence is rare (B) Superficial groin node dissection alone should not be performed (B) In lateral tumours, ipsilateral groin node dissection should be performed, if nodes are positive, contralateral is required (B) Preservation of long saphenous vein reduces groin wound and lower limb problems (C) Grade of recommendations: Grade A: Based on randomised controlled trials (RCTs). Grade B: Based on other robust experimental or good observational studies. Grade C: More limited evidence but the advice relies on expert opinion and has endorsement of respected authorities. 10
12 Appendix 2 - Histopathology Introduction All tissue specimens removed surgically are submitted for histopathological examination. Specimens are handled according to Standard Operating Procedures (SOPs) of the Department of Pathology, which cover fixation, dissection, block taking and reporting, and confirm to national guidelines and minimum data sets (where available). All cases are reviewed by consultant pathologists with a special interest in gynaecological pathology, and presented at the Combined Gynaecological Oncology Multidisciplinary Meeting prior to decision making about post-surgical management. Vulval cancer Vulvectomy specimens should be submitted to pathology pinned to cork (provided by Pathology Department, preferably with coloured pins to aid orientation. ) The histopathological report will include the following: Summary of clinical information provided, including indications for biopsy Specimen type Macroscopic description, including accurate measurement of specimen, tumour and distance from resection margins Macroscopic photographs are helpful in many cases and will be taken as appropriate. Microscopic report including: - Histological tumour type - Grade of tumour - Accurate measurement (optical micrometer) of depth and lateral extent of early invasive tumours - Proximity to nearest vaginal, vulval and deep resection margins - Presence or absence of lymphatic/vascular space invasion - Description of adjacent vulval skin - Total number of lymph nodes in each submitted group - Total number of involved lymph nodes in each submitted group 11
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
Guideline for the Management of Vulval Cancer
 Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Proposed All Wales Vulval Cancer Guidelines. Dr Amanda Tristram
 Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
3/25/2019. J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse
 J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse 1 4 th most common GYN cancer 5% of malignancies of GYN type. 4850 new cases annually 1030 deaths Cigarette smoking Vulvar dystrophy (Lichen
J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse 1 4 th most common GYN cancer 5% of malignancies of GYN type. 4850 new cases annually 1030 deaths Cigarette smoking Vulvar dystrophy (Lichen
Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva Malignant melanoma sho
 Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
Staging and Treatment Update for Gynecologic Malignancies
 Staging and Treatment Update for Gynecologic Malignancies Bunja Rungruang, MD Medical College of Georgia No disclosures 4 th most common new cases of cancer in women 5 th and 6 th leading cancer deaths
Staging and Treatment Update for Gynecologic Malignancies Bunja Rungruang, MD Medical College of Georgia No disclosures 4 th most common new cases of cancer in women 5 th and 6 th leading cancer deaths
Cervical cancer presentation
 Carcinoma of the cervix: Carcinoma of the cervix is the second commonest cancer among women worldwide, with only breast cancer occurring more commonly. Worldwide, cervical cancer accounts for about 500,000
Carcinoma of the cervix: Carcinoma of the cervix is the second commonest cancer among women worldwide, with only breast cancer occurring more commonly. Worldwide, cervical cancer accounts for about 500,000
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX Site Group: Gynecology Cervix Author: Dr. Stephane Laframboise 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING AND
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX Site Group: Gynecology Cervix Author: Dr. Stephane Laframboise 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING AND
Vulva Cancer Histopathology Reporting Proforma
 Vulva Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Ethnicity Unknown AboriginalTorres
Vulva Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Ethnicity Unknown AboriginalTorres
Clinical Pathological Conference. Malignant Melanoma of the Vulva
 Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
North of Scotland Cancer Network Clinical Management Guideline for Carcinoma of the Uterine Cervix
 THIS DOCUMENT North of Scotland Cancer Network Carcinoma of the Uterine Cervix UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Prepared by A Kennedy/AG Macdonald/Others Approved by NOT APPROVED Issue date April
THIS DOCUMENT North of Scotland Cancer Network Carcinoma of the Uterine Cervix UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Prepared by A Kennedy/AG Macdonald/Others Approved by NOT APPROVED Issue date April
Vaginal intraepithelial neoplasia
 Vaginal intraepithelial neoplasia The terminology and pathology of VAIN are analogous to those of CIN (VAIN I-III). The main difference is that vaginal epithelium does not normally have crypts, so the
Vaginal intraepithelial neoplasia The terminology and pathology of VAIN are analogous to those of CIN (VAIN I-III). The main difference is that vaginal epithelium does not normally have crypts, so the
Review Article Selective Inguinal Lymphadenectomy in the Treatment of Invasive Squamous Cell Carcinoma of the Vulva
 Hindawi Publishing Corporation International Journal of Surgical Oncology Volume 2011, Article ID 284374, 6 pages doi:10.1155/2011/284374 Review Article Selective Inguinal Lymphadenectomy in the Treatment
Hindawi Publishing Corporation International Journal of Surgical Oncology Volume 2011, Article ID 284374, 6 pages doi:10.1155/2011/284374 Review Article Selective Inguinal Lymphadenectomy in the Treatment
Coversheet for Network Site Specific Group Agreed Documentation
 Coversheet for Network Site Specific Group Agreed Documentation This sheet is to accompany all documentation agreed by Pan Birmingham Cancer Network Site Specific Groups. This will assist the Network Governance
Coversheet for Network Site Specific Group Agreed Documentation This sheet is to accompany all documentation agreed by Pan Birmingham Cancer Network Site Specific Groups. This will assist the Network Governance
Sarah Burton. Lead Gynae Oncology Nurse Specialist Cancer Care Cymru
 Sarah Burton Lead Gynae Oncology Nurse Specialist Cancer Care Cymru Gynaecological Cancers Cervical Cancers Risk factors Presentation Early sexual activity Multiple sexual partners Smoking Human Papiloma
Sarah Burton Lead Gynae Oncology Nurse Specialist Cancer Care Cymru Gynaecological Cancers Cervical Cancers Risk factors Presentation Early sexual activity Multiple sexual partners Smoking Human Papiloma
Type I. Type II. Excess estrogen Lynch Endometrioid adenocarcinoma PTEN. High grade More aggressive Serous, Clear Cell p53
 Type I Excess estrogen Lynch Endometrioid adenocarcinoma PTEN Type II High grade More aggressive Serous, Clear Cell p53 Stage I IA IB Stage II Stage III IIIA IIIB IIIC IIIC1 IIIC2 Stage IV IVA IVB nodes
Type I Excess estrogen Lynch Endometrioid adenocarcinoma PTEN Type II High grade More aggressive Serous, Clear Cell p53 Stage I IA IB Stage II Stage III IIIA IIIB IIIC IIIC1 IIIC2 Stage IV IVA IVB nodes
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
VULVAR CARCINOMA. Page 1 of 5
 VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
North of Scotland Cancer Network Clinical Management Guideline for Endometrial Cancer
 THIS DOCUMENT North of Scotland Cancer Network Clinical Management Guideline for Endometrial Cancer Based on WOSCAN CMG with further extensive consultation within NOSCAN UNCONTROLLED WHEN PRINTED DOCUMENT
THIS DOCUMENT North of Scotland Cancer Network Clinical Management Guideline for Endometrial Cancer Based on WOSCAN CMG with further extensive consultation within NOSCAN UNCONTROLLED WHEN PRINTED DOCUMENT
1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter.
 Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Squamous vulval cancer an update
 DOI: 10.1111/tog.12059 The Obstetrician & Gynaecologist http://onlinetog.org 2013;15:227 31 Review Squamous vulval cancer an update Claire Bailey MRCOG, 1, * David Luesley MA MD FRCOG 2 1 Specialist Trainee,
DOI: 10.1111/tog.12059 The Obstetrician & Gynaecologist http://onlinetog.org 2013;15:227 31 Review Squamous vulval cancer an update Claire Bailey MRCOG, 1, * David Luesley MA MD FRCOG 2 1 Specialist Trainee,
Cervical Cancer: 2018 FIGO Staging
 Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
The International Federation of Gynecology and Obstetrics (FIGO) updated the staging
 Continuing Education Column Revised FIGO Staging System Hee Sug Ryu, MD Department of Obstetrics and Gynecology, Ajou University School of Medicine E - mail : hsryu@ajou.ac.kr J Korean Med Assoc 2010;
Continuing Education Column Revised FIGO Staging System Hee Sug Ryu, MD Department of Obstetrics and Gynecology, Ajou University School of Medicine E - mail : hsryu@ajou.ac.kr J Korean Med Assoc 2010;
Vagina. 1. Introduction. 1.1 General Information and Aetiology
 Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
Cervical Cancer 3/25/2019. Abnormal vaginal bleeding
 Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
GUIDELINES ON PENILE CANCER
 46 E. Solsona (chairman), F. Algaba, S. Horenblas, G. Pizzocaro, T. Windahl Eur Urol 2002;42(3):199-203 Introduction Penile carcinoma is an uncommon malignant disease with an incidence ranging from 0.1
46 E. Solsona (chairman), F. Algaba, S. Horenblas, G. Pizzocaro, T. Windahl Eur Urol 2002;42(3):199-203 Introduction Penile carcinoma is an uncommon malignant disease with an incidence ranging from 0.1
Invasive Cervical Cancer: Squamous Cell, Adenocarcinoma, Adenosquamous
 Note: If available, clinical trials should be considered as preferred treatment options for eligible patients (www.mdanderson.org/gynonctrials). Other co-morbidities are taken into consideration prior
Note: If available, clinical trials should be considered as preferred treatment options for eligible patients (www.mdanderson.org/gynonctrials). Other co-morbidities are taken into consideration prior
Diseases of the vulva
 Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Chapter 8 Adenocarcinoma
 Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
Staging Classifications and Clinical Practice Guidelines for Gynaecological Cancers
 Pages 10/10/06 10:29 Page i Staging Classifications and Clinical Practice Guidelines for Gynaecological Cancers Emeritus Editor: JL Benedet Editors: Sergio Pecorelli, Hextan YS Ngan and Neville F Hacker
Pages 10/10/06 10:29 Page i Staging Classifications and Clinical Practice Guidelines for Gynaecological Cancers Emeritus Editor: JL Benedet Editors: Sergio Pecorelli, Hextan YS Ngan and Neville F Hacker
SENTINEL NODES FOR EARLY VULVAL CANCER:
 SENTINEL NODES FOR EARLY VULVAL CANCER: FEASIBILITY AND SAFETY IN A LOW RESOURCE SETTING LINDA ROGERS RCOG Congress 2017 None Declaration of Interests Vulval Cancer Rare 4% of all gynaecological malignancies
SENTINEL NODES FOR EARLY VULVAL CANCER: FEASIBILITY AND SAFETY IN A LOW RESOURCE SETTING LINDA ROGERS RCOG Congress 2017 None Declaration of Interests Vulval Cancer Rare 4% of all gynaecological malignancies
Case Scenario 1 Worksheet. Primary Site C44.4 Morphology 8743/3 Laterality 0 Stage/ Prognostic Factors
 CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
Prognostic factors associated with local recurrence in squamous cell carcinoma of the vulva
 Original Article J Gynecol Oncol Vol. 24, No. 3:242-248 pissn 2005-0380 eissn 2005-0399 Prognostic factors associated with local recurrence in squamous cell carcinoma of the vulva Sara Iacoponi, Ignacio
Original Article J Gynecol Oncol Vol. 24, No. 3:242-248 pissn 2005-0380 eissn 2005-0399 Prognostic factors associated with local recurrence in squamous cell carcinoma of the vulva Sara Iacoponi, Ignacio
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
Gynecological Cancers in Primary Care
 Gynecological Cancers in Primary Care Nora M. Lersch MSN CRNP AOCNP Division of Gynecological Oncology Objectives Identify the incidence of ovarian, cervical, vulvar and endometrial cancer Identify common
Gynecological Cancers in Primary Care Nora M. Lersch MSN CRNP AOCNP Division of Gynecological Oncology Objectives Identify the incidence of ovarian, cervical, vulvar and endometrial cancer Identify common
CPC on Cervical Pathology
 CPC on Cervical Pathology Dr. W.K. Ng Senior Medical Officer Department of Clinical Pathology Pamela Youde Nethersole Eastern Hospital Cervical Smear: High Grade SIL (CIN III) Cervical Smear: High Grade
CPC on Cervical Pathology Dr. W.K. Ng Senior Medical Officer Department of Clinical Pathology Pamela Youde Nethersole Eastern Hospital Cervical Smear: High Grade SIL (CIN III) Cervical Smear: High Grade
COLORECTAL CARCINOMA
 QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
New Cancer Cases By Site Breast 28% Lung 14% Colo-Rectal 10% Uterus 6% Thyroid 5% Lymphoma 4% Ovary 3%
 Uterine Malignancy New Cancer Cases By Site 2010 Breast 28% Lung 14% Colo-Rectal 10% Uterus 6% Thyroid 5% Lymphoma 4% Ovary 3% Cancer Deaths By Site 2010 Lung 26% Breast 15% Colo-Rectal 9% Pancreas 7%
Uterine Malignancy New Cancer Cases By Site 2010 Breast 28% Lung 14% Colo-Rectal 10% Uterus 6% Thyroid 5% Lymphoma 4% Ovary 3% Cancer Deaths By Site 2010 Lung 26% Breast 15% Colo-Rectal 9% Pancreas 7%
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
University of Kentucky. Markey Cancer Center
 University of Kentucky Markey Cancer Center Invasive Cancer of the Vagina and Urethra Fred Ueland, MD No matter what you accomplish in your life, the size of your funeral will still be determined by the
University of Kentucky Markey Cancer Center Invasive Cancer of the Vagina and Urethra Fred Ueland, MD No matter what you accomplish in your life, the size of your funeral will still be determined by the
Vulvar cancer: Know what to expect
 Vulvar cancer: Know what to expect For women with vulvar cancer What is the vulva? The vulva is the external (outside) part of the female genitals. The vulva includes the outer and inner lip, the clitoris,
Vulvar cancer: Know what to expect For women with vulvar cancer What is the vulva? The vulva is the external (outside) part of the female genitals. The vulva includes the outer and inner lip, the clitoris,
Staging. Carcinoma confined to the corpus. Carcinoma confined to the endometrium. Less than ½ myometrial invasion. Greater than ½ myometrial invasion
 5 th of June 2009 Background Most common gynaecological carcinoma in developed countries Most cases are post-menopausal Increasing incidence in certain age groups Increasing death rates in the USA 5-year
5 th of June 2009 Background Most common gynaecological carcinoma in developed countries Most cases are post-menopausal Increasing incidence in certain age groups Increasing death rates in the USA 5-year
Glossary of Terms Primary Urethral Cancer
 Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Referral and Management Guidelines for Gynaecological Cancers within North Trent
 North Trent Cancer Network Referral and Management Guidelines for Gynaecological Cancers within North Trent Final Version 3.0 August 2011 Review date : June 2013 Produced by the North Trent Cancer Network
North Trent Cancer Network Referral and Management Guidelines for Gynaecological Cancers within North Trent Final Version 3.0 August 2011 Review date : June 2013 Produced by the North Trent Cancer Network
Most common cancer Africans & Asians more prone because of poor socioeconomic condition Drastic decline in west as more detection of preinvasive
 CANCER CERVIX Most common cancer Africans & Asians more prone because of poor socioeconomic condition Drastic decline in west as more detection of preinvasive leison by PAP Smears. Etiology: Age - 2 peaks
CANCER CERVIX Most common cancer Africans & Asians more prone because of poor socioeconomic condition Drastic decline in west as more detection of preinvasive leison by PAP Smears. Etiology: Age - 2 peaks
North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO)
 North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO) UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Original Prepared by NMcL April 2016
North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO) UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Original Prepared by NMcL April 2016
Protocol for the Examination of Specimens from Patients with Carcinoma of the Vulva
 Protocol for the Examination of Specimens from Patients with Carcinoma of the Vulva Protocol applies to all invasive carcinomas of the vulva. Based on AJCC/UICC TNM, 7th edition, and FIGO 2008 Annual Report
Protocol for the Examination of Specimens from Patients with Carcinoma of the Vulva Protocol applies to all invasive carcinomas of the vulva. Based on AJCC/UICC TNM, 7th edition, and FIGO 2008 Annual Report
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
Bladder Cancer Guidelines
 Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
Information for Patients. Primary urethral cancer. English
 Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
GYNAECOLOGICAL CANCER CLINICAL GUIDELINES
 GYNAECOLOGICAL CANCER CLINICAL GUIDELINES Gynae-Oncology Expert Advisory Group Document Information Title: Cancer Alliance Gynae Cancer Clinical Guidelines Author: Gynae EAG Members Circulation List: See
GYNAECOLOGICAL CANCER CLINICAL GUIDELINES Gynae-Oncology Expert Advisory Group Document Information Title: Cancer Alliance Gynae Cancer Clinical Guidelines Author: Gynae EAG Members Circulation List: See
Gynecologic Oncologist. Surgery Chemotherapy Radiation Therapy Hormonal Therapy Immunotherapy. Cervical cancer
 Gynecologic Oncology Pre invasive vulvar, vaginal, & cervical disease Vulvar Cervical Endometrial Uterine Sarcoma Fallopian Tube Ovarian GTD Gynecologic Oncologist Surgery Chemotherapy Radiation Therapy
Gynecologic Oncology Pre invasive vulvar, vaginal, & cervical disease Vulvar Cervical Endometrial Uterine Sarcoma Fallopian Tube Ovarian GTD Gynecologic Oncologist Surgery Chemotherapy Radiation Therapy
GYNAECOLOGICAL CANCER CLINICAL GUIDELINES
 Northern England Strategic Clinical Networks GYNAECOLOGICAL CANCER CLINICAL GUIDELINES Gynae-Oncology NSSG on behalf of NECN Document Information Title: NECN Gynae Cancer Clinical Guidelines Author: Gynae
Northern England Strategic Clinical Networks GYNAECOLOGICAL CANCER CLINICAL GUIDELINES Gynae-Oncology NSSG on behalf of NECN Document Information Title: NECN Gynae Cancer Clinical Guidelines Author: Gynae
The Role of Radiation in the Management of Gynecologic Cancers. Scott Glaser, MD
 The Role of Radiation in the Management of Gynecologic Cancers Scott Glaser, MD Nothing to disclose DISCLOSURE Outline The role of radiation in: Endometrial Cancer Adjuvant Medically inoperable Cervical
The Role of Radiation in the Management of Gynecologic Cancers Scott Glaser, MD Nothing to disclose DISCLOSURE Outline The role of radiation in: Endometrial Cancer Adjuvant Medically inoperable Cervical
Protocol for the Examination of Specimens From Patients With Primary Carcinoma of the Vulva
 Protocol for the Examination of Specimens From Patients With Primary Carcinoma of the Vulva Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual,
Protocol for the Examination of Specimens From Patients With Primary Carcinoma of the Vulva Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual,
CARCINOMA CERVIX. Dr. PREETHI REDDY. B. M S OBG II yr POST GRADUATE.
 CARCINOMA CERVIX Dr. PREETHI REDDY. B M S OBG II yr POST GRADUATE. Introduction Cervical cancer is the second most common female malignancy worldwide. It is responsible for 4,66,000 deaths annually worldwide
CARCINOMA CERVIX Dr. PREETHI REDDY. B M S OBG II yr POST GRADUATE. Introduction Cervical cancer is the second most common female malignancy worldwide. It is responsible for 4,66,000 deaths annually worldwide
Da Costa was the first to coin the term. Marjolin s Ulcer: A Case Report and Literature Review. Case Report. Introduction
 E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
What is endometrial cancer?
 Uterine cancer What is endometrial cancer? Endometrial cancer is the growth of abnormal cells in the lining of the uterus. The lining is called the endometrium. Endometrial cancer usually occurs in women
Uterine cancer What is endometrial cancer? Endometrial cancer is the growth of abnormal cells in the lining of the uterus. The lining is called the endometrium. Endometrial cancer usually occurs in women
OCCG SERVICE SPECIFICATION (2017/18)
 OCCG SERVICE SPECIFICATION (2017/18) Primary Care Service for Skin Cancers: Dermatology Shared Care Monitoring for Melanoma, Lichen Sclerosus and Squamos Cell Carcinoma 1. Background For patients who have
OCCG SERVICE SPECIFICATION (2017/18) Primary Care Service for Skin Cancers: Dermatology Shared Care Monitoring for Melanoma, Lichen Sclerosus and Squamos Cell Carcinoma 1. Background For patients who have
Japan Society of Gynecologic Oncology guidelines 2015 for the treatment of vulvar cancer and vaginal cancer
 Int J Clin Oncol (2018) 23:201 234 https://doi.org/10.1007/s10147-017-1193-z SPECIAL ARTICLE Japan Society of Gynecologic Oncology guidelines 2015 for the treatment of vulvar cancer and vaginal cancer
Int J Clin Oncol (2018) 23:201 234 https://doi.org/10.1007/s10147-017-1193-z SPECIAL ARTICLE Japan Society of Gynecologic Oncology guidelines 2015 for the treatment of vulvar cancer and vaginal cancer
Head and Neck Cancer Service
 Dr Hoda Al Booz. MMedSci, MD, FFRRCSI, FRCR. Head and Neck Cancer Service Dr Hoda Al Booz Consultant in Clinical Oncology Bristol Cancer Institute Dr Hoda Al Booz. MMedSci, MD, FFRRCSI, FRCR. documents/
Dr Hoda Al Booz. MMedSci, MD, FFRRCSI, FRCR. Head and Neck Cancer Service Dr Hoda Al Booz Consultant in Clinical Oncology Bristol Cancer Institute Dr Hoda Al Booz. MMedSci, MD, FFRRCSI, FRCR. documents/
Navigators Lead the Way
 RN Navigators Their Role in patients with Cancers of the GI tract Navigators Lead the Way Nurse Navigator Defined Nurse Navigator A clinically trained individual responsible for the identification and
RN Navigators Their Role in patients with Cancers of the GI tract Navigators Lead the Way Nurse Navigator Defined Nurse Navigator A clinically trained individual responsible for the identification and
Uterine Cervix. Protocol applies to all invasive carcinomas of the cervix.
 Uterine Cervix Protocol applies to all invasive carcinomas of the cervix. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition and FIGO 2001 Annual Report Procedures Cytology (No Accompanying
Uterine Cervix Protocol applies to all invasive carcinomas of the cervix. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition and FIGO 2001 Annual Report Procedures Cytology (No Accompanying
Cancer of the Oral Cavity
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
Guidelines for Management of Penile Cancer
 Guidelines for Management of Penile Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Sections 3, 5, 6 and 16 updated. Page 1 of 10 1. Scope
Guidelines for Management of Penile Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Sections 3, 5, 6 and 16 updated. Page 1 of 10 1. Scope
North of Scotland Cancer Network Clinical Management Guideline for Malignant Melanoma
 Nth of Scotland Cancer Netwk Clinical Management Guideline f Malignant Melanoma Based on WOSCAN CMG with further consultation within NOSCAN UNCONTROLLED WHEN PRINTED Prepared by Approved by Issue date
Nth of Scotland Cancer Netwk Clinical Management Guideline f Malignant Melanoma Based on WOSCAN CMG with further consultation within NOSCAN UNCONTROLLED WHEN PRINTED Prepared by Approved by Issue date
Janjira Petsuksiri, M.D
 GYN malignancies Janjira Petsuksiri, M.D Outlines Cervical cancer Endometrial cancer Ovarian cancer Vaginal cancer Vulva cancer 2 CA Cervix Epidemiology - Second most common female cancer Risk factors
GYN malignancies Janjira Petsuksiri, M.D Outlines Cervical cancer Endometrial cancer Ovarian cancer Vaginal cancer Vulva cancer 2 CA Cervix Epidemiology - Second most common female cancer Risk factors
Algorithms for management of Cervical cancer
 Algithms f management of Cervical cancer Algithms f management of cervical cancer are based on existing protocols and guidelines within the ESGO comunity and prepared by ESGO Educational Committe as a
Algithms f management of Cervical cancer Algithms f management of cervical cancer are based on existing protocols and guidelines within the ESGO comunity and prepared by ESGO Educational Committe as a
C ORPUS UTERI C ARCINOMA STAGING FORM (Carcinosarcomas should be staged as carcinomas)
 CLINICAL C ORPUS UTERI C ARCINOMA STAGING FORM PATHOLOGIC Extent of disease before S TAGE C ATEGORY D EFINITIONS Extent of disease through any treatment completion of definitive surgery y clinical staging
CLINICAL C ORPUS UTERI C ARCINOMA STAGING FORM PATHOLOGIC Extent of disease before S TAGE C ATEGORY D EFINITIONS Extent of disease through any treatment completion of definitive surgery y clinical staging
Cancer of Unknown Primary (CUP) Protocol
 1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
8. The polyp in the illustration can be described as (circle all that apply) a. Exophytic b. Pedunculated c. Sessile d. Frank
 Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
Estimated New Cancers Cases 2003
 Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz Estimated New Cancers Cases 2003 Images removed due to copyright reasons.
Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz Estimated New Cancers Cases 2003 Images removed due to copyright reasons.
Disclosures. I have no conflicts of interest to disclose. Vulvar Disease. Precancer and Cancerous Vulvar Disease
 Precancer and Cancerous Vulvar Disease Stefanie M. Ueda, M.D. Disclosures I have no conflicts of interest to disclose. Assistant Clinical Professor Division of Gynecologic Oncology University of California,
Precancer and Cancerous Vulvar Disease Stefanie M. Ueda, M.D. Disclosures I have no conflicts of interest to disclose. Assistant Clinical Professor Division of Gynecologic Oncology University of California,
Melanoma Quality Reporting
 Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122
 Ovarian cancer: recognition and initial management Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Ovarian cancer: recognition and initial management Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Guideline for the Follow-up of Patients with Gynaecological Malignancies
 Guideline for the Follow-up of Patients with Gynaecological Malignancies Version History Version Date Summary of Change/Process 2.0 20.02.08 Endorsed by the Governance Committee 2.1 18.11.10 Circulated
Guideline for the Follow-up of Patients with Gynaecological Malignancies Version History Version Date Summary of Change/Process 2.0 20.02.08 Endorsed by the Governance Committee 2.1 18.11.10 Circulated
2009 USCAP Gyn Pathology Evening Session Case #3. Richard J. Zaino, MD Hershey Medical Center Penn State University Hershey, PA
 2009 USCAP Gyn Pathology Evening Session Case #3 Richard J. Zaino, MD Hershey Medical Center Penn State University Hershey, PA rzaino@psu.edu Clinical history Middle aged woman with an exophytic mass of
2009 USCAP Gyn Pathology Evening Session Case #3 Richard J. Zaino, MD Hershey Medical Center Penn State University Hershey, PA rzaino@psu.edu Clinical history Middle aged woman with an exophytic mass of
Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
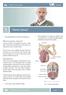 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Cervical cancer is a disease in which malignant (cancer) cells form in the tissues of the cervix.
 Cervical Cancer Cervical cancer is a disease in which malignant (cancer) cells form in the tissues of the cervix. The cervix is the lower, narrow end of the uterus (the hollow, pear-shaped organ where
Cervical Cancer Cervical cancer is a disease in which malignant (cancer) cells form in the tissues of the cervix. The cervix is the lower, narrow end of the uterus (the hollow, pear-shaped organ where
Oral cancer: Prognosis & Treatment. Dr. Hani Al Sheikh Radhi
 Oral cancer: Prognosis & Treatment Dr. Hani Al Sheikh Radhi Prognostic factors in Oral caner TNM staging T stage N stage M stage Site Histological Factors Vascular & Perineural Invasion Surgical Margins
Oral cancer: Prognosis & Treatment Dr. Hani Al Sheikh Radhi Prognostic factors in Oral caner TNM staging T stage N stage M stage Site Histological Factors Vascular & Perineural Invasion Surgical Margins
Pathway Gynaecology Cancer & Diagnostic Protocol for Inter Trust transfer
 NICaN Pathway Gynaecology Cancer & Diagnostic Protocol for Inter Trust transfer Timed schedules to enable the proactive management of the patient from point of receipt of referral to first definitive treatment
NICaN Pathway Gynaecology Cancer & Diagnostic Protocol for Inter Trust transfer Timed schedules to enable the proactive management of the patient from point of receipt of referral to first definitive treatment
ECC or Margins Positive?
 CLINICAL PRESENTATION This practice algorithm has been specifically developed for M. D. Anderson using a multidisciplinary approach and taking into consideration circumstances particular to M. D. Anderson,
CLINICAL PRESENTATION This practice algorithm has been specifically developed for M. D. Anderson using a multidisciplinary approach and taking into consideration circumstances particular to M. D. Anderson,
CLINICAL PRACTICE GUID ELINES
 t SOGC CLINICAL PRACTICE GUID ELINES No. 2, May 1993 This has been provided by the Oncology Committee, Socieq of Obstetricians and Gynaecologists of Canada CURRENT CONCEPTS IN MANAGEMENT OF VULVAR CANCER
t SOGC CLINICAL PRACTICE GUID ELINES No. 2, May 1993 This has been provided by the Oncology Committee, Socieq of Obstetricians and Gynaecologists of Canada CURRENT CONCEPTS IN MANAGEMENT OF VULVAR CANCER
Cervical Cancer Guidelines L and SC Network July Introduction:
 Cervical Cancer Guidelines L and SC Network July 2018 Introduction: There was a total number of 442 cases of cervix cancer diagnosed in Lancashire and South Cumbria Cancer Network in the period 2005 2009
Cervical Cancer Guidelines L and SC Network July 2018 Introduction: There was a total number of 442 cases of cervix cancer diagnosed in Lancashire and South Cumbria Cancer Network in the period 2005 2009
MRI in Cervix and Endometrial Cancer
 28th Congress of the Hungarian Society of Radiologists RCR Session Budapest June 2016 MRI in Cervix and Endometrial Cancer DrSarah Swift St James s University Hospital Leeds, UK Objectives Cervix and endometrial
28th Congress of the Hungarian Society of Radiologists RCR Session Budapest June 2016 MRI in Cervix and Endometrial Cancer DrSarah Swift St James s University Hospital Leeds, UK Objectives Cervix and endometrial
Gynaecology NSSG (Lancs & South Cumbria) Vulval Cancer Guidelines V3.0
 Gynaecology NSSG (Lancs & South Cumbria) Vulval Cancer Guidelines V3.0 ** VALID ON DATE OF PRINTING ONLY all guidelines available on the Strategic Clinical Network website : GMLSC SCN Date First Published
Gynaecology NSSG (Lancs & South Cumbria) Vulval Cancer Guidelines V3.0 ** VALID ON DATE OF PRINTING ONLY all guidelines available on the Strategic Clinical Network website : GMLSC SCN Date First Published
GUIDELINES ON PROSTATE CANCER
 10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
VULVAR CANCER GUIDELINES
 VULVAR ANER GUIDELINES www.esgo.org Broz_210x297_9_16_b.indd 1 13.09.16 21:48 The European Society of Gynaecological Oncology (ESGO) developed guidelines covering diagnosis and referral, preoperative investigations,
VULVAR ANER GUIDELINES www.esgo.org Broz_210x297_9_16_b.indd 1 13.09.16 21:48 The European Society of Gynaecological Oncology (ESGO) developed guidelines covering diagnosis and referral, preoperative investigations,
receive adjuvant chemotherapy
 Women with high h risk early stage endometrial cancer should receive adjuvant chemotherapy Michael Friedlander The Prince of Wales Cancer Centre and Royal Hospital for Women The Prince of Wales Cancer
Women with high h risk early stage endometrial cancer should receive adjuvant chemotherapy Michael Friedlander The Prince of Wales Cancer Centre and Royal Hospital for Women The Prince of Wales Cancer
Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma
 Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given
Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
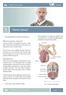 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: SURGICAL ONCOLOGY 5-May-2013 DEVELOPED BY: Bruce
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: SURGICAL ONCOLOGY 5-May-2013 DEVELOPED BY: Bruce
UICC TNM 8 th Edition Errata
 UICC TNM 8 th Edition Errata ions are in italics Head and Neck Tumours Pages 20, p27, p34, p38, p41, and p49 ly pn2a Metastasis in a single ipsilateral lymph node, less than 3cm in greatest dimension with
UICC TNM 8 th Edition Errata ions are in italics Head and Neck Tumours Pages 20, p27, p34, p38, p41, and p49 ly pn2a Metastasis in a single ipsilateral lymph node, less than 3cm in greatest dimension with
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
ARROCase: Locally Advanced Endometrial Cancer
 ARROCase: Locally Advanced Endometrial Cancer Charles Vu, MD (PGY-3) Faculty Advisor: Peter Y. Chen, MD, FACR Beaumont Health (Royal Oak, MI) November 2016 Case 62yo female with a 3yr history of vaginal
ARROCase: Locally Advanced Endometrial Cancer Charles Vu, MD (PGY-3) Faculty Advisor: Peter Y. Chen, MD, FACR Beaumont Health (Royal Oak, MI) November 2016 Case 62yo female with a 3yr history of vaginal
