Esophageal adenocarcinoma is rapidly increasing in. Barrett s Esophagus: Diagnosis, Surveillance, and Endoscopic Management CASE-BASED REVIEW
|
|
|
- Esmond Gilbert Nichols
- 5 years ago
- Views:
Transcription
1 Barrett s Esophagus: Diagnosis, Surveillance, and Endoscopic Management Case Study and Commentary, Michelle H. Lee, MD, and Sharmila Anandasabapathy, MD ABSTRACT Objective: To discuss diagnosis, surveillance, and management strategies for Barrett s esophagus. Methods: Literature review. Results: Barrett s esophagus has gained recognition as the premalignant precursor for esophageal adenocarcinoma. The progression of Barrett s esophagus may involve the development of low-grade dysplasia and high-grade dysplasia before the eventual development of a neoplasm. The challenges to screening include the inability to predict who has Barrett s esophagus prior to endoscopy, the lack of evidence demonstrating improved mortality and the cost-effectiveness of endoscopic screening. The recommendation for endoscopic surveillance of Barrett s esophagus is based on the poor overall survival rate for esophageal adenocarcinoma when it is diagnosed at a late stage. Current treatment options for Barrett s esophagus include surveillance, endoscopic resection, endoscopic ablation therapy and surgical resection. Conclusion: Esophageal adenocarcinoma has been rapidly increasing in incidence in the United States and other countries over the last 30 to 40 years. Controversy still surrounds the screening and surveillance guidelines, but given the poor survival rate for esophageal adenocarcinoma, surveillance endoscopy is endorsed by all major professional gastrointestinal societies. At the current time, patients who are found to have Barrett s esophagus with high-grade dysplasia or intramucosal esophageal neoplasia have the option of choosing minimally invasive endoscopic procedures, which appear to have comparable efficacy to surgery. Esophageal adenocarcinoma is rapidly increasing in incidence in the United States and other countries. Population-based cohort studies examining the incidence of esophageal adenocarcinoma report a 300% to 500% increase throughout the last 30 to 40 years [1]. Barrett s esophagus has gained recognition as the premalignant lesion for adenocarcinoma and is believed to be the major risk factor, with a 20-fold increased risk in the development of esophageal adenocarcinoma when compared to patients without the condition [2-4]. The reported rate of progression of Barrett s esophagus to esophageal adenocarcinoma range from 0.12% to 0.5% per year [3,5 7]. Barrett s esophagus is diagnosed in approximately 10% to 15% of patients with reflux symptoms who are undergoing endoscopy [1]. Barrett s esophagus is defined as a change in the distal esophageal epithelium of any length that can be recognized as columnar type mucosa at endoscopy (Figure 1) and is confirmed to have intestinal metaplasia by biopsy of the esophagus (Figure 2). If the characteristic salmon-colored tongues of Barrett s esophagus are observed on standard light endoscopy, 4-quadrant biopsies should be taken every 1 to 2 cm throughout the Barrett s segment [8]. The progression of Barrett s esophagus may involve the development of low-grade dysplasia and high-grade dysplasia before the eventual development of a neoplasm. Because the average age at diagnosis of esophageal adenocarcinoma is in the sixth and seventh decades of life [9], a clear understanding of the diagnosis and treatment options of Barrett s esophagus is essential in the care of the aging population. CASE STUDY Initial Presentation A 68-year-old man with a body mass index of 33 is referred to a gastroenterologist for evaluation of gastroesophageal reflux disease. He endorses a history of intermittent substernal burning sensation for the last 6 years. From the Division of Gastroenterology, The Mount Sinai Medical Center, New York, NY. Vol. 19, No. 12 December 2012 JCOM 563
2 BARRETT S ESOPHAGUS Figure 1. Barrett s esophagus on endoscopy. What are indications for screening for Barrett s esophagus? Screening A screening test should have the ability to detect a premalignant or early malignant lesion, thereby offering the opportunity for intervention and reduced morbidity and mortality. While screening for Barrett s esophagus in selected patients has been endorsed by certain gastrointestinal societies [10], the challenges to screening include the inability to predict who has Barrett s esophagus prior to endoscopy, the lack of evidence demonstrating improved mortality and the cost-effectiveness of endoscopic screening. The rationale supporting screening for Barrett s esophagus has been based on decision- and cost-analysis studies [11,12] but is limited by the absence of controlled, supportive data. Although attempts have been made to identify the appropriate screening population for Barrett s esophagus, no guidelines have been established. Studies have attempted to predict Barrett s esophagus with clinical and demographic features comparing patients with the disease to controls with gastroesophageal reflux disease (GERD) [13]. Age greater than 50 [14], GERD [8], longer duration of GERD symptoms [15 19], male gender [20], and white race [21] have been associated with Barrett s esophagus, although recently, rates of Barrett s esophagus have been rising in females [22]. While the only consistent predictor across various studies was the presence of heartburn, the sensitivity remains poor [13]. Furthermore, studies demonstrate that up to 40% of patients with esophageal adenocarcinoma do not experience reflux symptoms and therefore would not be included in the targeted screening population [23 25]. Moreover, a Veterans Administration study noted that older patients with Barrett s esophagus had significantly lower symptom severity scores when compared with younger patients with similar pathology, with scores similar to those of asymptomatic controls [26]. This atypical clinical presentation further complicates the determination of appropriate screening groups. Additionally, there is conflicting evidence supporting a mortality benefit from screening and surveillance of Barrett s esophagus [8]. Some retrospective studies have suggested a survival benefit in patients undergoing endoscopy prior to diagnosis of adenocarcinoma [27 34], while other studies have failed to demonstrate an overall mortality benefit in patients undergoing Barrett s surveillance [35 39]. Given the inability to identify high-risk groups, as well as the lack of proven benefit of endoscopic surveillance in patients in whom Barrett s esophagus is identified, screening for Barrett s esophagus in the general population is not recommended at this time (Table 1). The American Gastroenterological Association (AGA) recommends tailoring screening for Barrett s esophagus to patients based on risk factors rather than reflux symptoms alone [8]. On the other hand, the American Society for Gastrointestinal Endoscopy recommends that screening esophagogastroduodenoscopy should be considered in patients with chronic, longstanding GERD (> 5 years) [10]. The American College of Gastroenterology guidelines state that the use of screening in selective populations at higher risk remains to be established and should therefore be individualized [13]. However, alarm symptoms such as dysphagia, weight loss and anemia should prompt primary care physicians to refer patients to a gastroenterologist for an endoscopic evaluation. How should endoscopic surveillance be conducted? 564 JCOM December 2012 Vol. 19, No. 12
3 Figure 2. Histologic appearance of Barrett s epithelium. Normal squamous epithelium (L) and Barrett s glandular mucosa (R). L R Surveillance Although there is a lack of randomized trials supporting the value of surveillance endoscopy in patients with Barrett s esophagus, it is still practiced by the vast majority of endoscopists and endorsed by all major professional gastrointestinal societies [13]. The recommendation for endoscopic surveillance is based on the poor overall survival rate for esophageal adenocarcinoma when it is diagnosed at a late stage [40]. Moreover, multiple cohort studies have demonstrated that esophageal cancers detected in patients in surveillance protocol are associated with longer survival than those diagnosed on an initial endoscopy for alarm symptoms [8]. Patients undergoing surveillance endoscopy should be maintained on proton pump inhibitors, with the goal of decreasing esophageal inflammation and enabling better endoscopic and pathological examination of Barrett s esophagus [41]. If initial pathologic examination demonstrates Barrett s esophagus without dysplasia, a second endoscopy should be performed within 2 years. Subsequent surveillance can be performed at 3- to 5-year intervals (Table 2) [42]. Patients are maintained on proton pump inhibitors based on the hypothesis that neutralization of esophageal acid exposure would remove mucosal irritation, and subsequently reduce the risk of progression to high-grade dysplasia or adenocarcinoma [39]. In addition, some studies have demonstrated that antireflux surgery can provide control over GERD symptoms in Barrett s esophagus [43,44]. Studies have demonstrated that more than 20% of cancers reported in prospective surveillance studies arose in patients lacking dysplasia on initial endoscopy; thus, continued surveillance is recommended even in the absence of dysplasia on both baseline endoscopies [45]. When biopsies demonstrate low-grade dysplasia, repeat endoscopy should be done within 6 months, with biopsies taken every 1 cm to ensure that a higher grade of dysplasia is not present. Low-grade dysplasia warrants annual endoscopies. If no dysplasia is noted on 2 consecutive studies, then a 3-year interval can be followed [13]. Low-grade dysplasia should be confirmed by an expert gastrointestinal pathologist, secondary to the high degree of inter-observer variation [46]. The endoscopic treatment of non-dysplastic Barrett s esophagus is not generally recommended. Low-grade dysplasia is a more controversial area. While some studies have demonstrated eradication of low-grade dysplasia with ablative therapy [47], the long-term efficacy and benefits have not been demonstrated [8]. High-grade dysplasia in flat mucosa should be confirmed by an expert gastrointestinal pathologist and a repeat endoscopy should be performed within 3 months, with biopsies taken every 1 cm. However, high-grade dysplasia with mucosal irregularity should undergo endoscopic mucosal resection due to the increased likelihood of cancer existing in nodularity. In high-grade dysplasia, the 5-year risk of progression to esophageal adenocarcinoma has been shown to range from 16% to 56%; hence, intervention (endoscopic or surgical) is usually recommended for subjects with high-grade dysplasia [13]. Patients with high-grade dysplasia should be advised on various therapeutic options including intensive surveillance, esophagectomy or abla- Vol. 19, No. 12 December 2012 JCOM 565
4 BARRETT S ESOPHAGUS Table 1. Screening Recommendations American College of Gastroenterology [13] Screening for Barrett's esophagus remains controversial. The highest yield is in older ( 50 yr) Caucasian males with longstanding heartburn. American Gastroenterological Association [8,42] Recommends tailoring screening based on multiple risk factors, not just on reflux symptoms alone American Society for Gastrointestinal Endoscopy [10] Recommends screening EGD be considered in patients with chronic, longstanding GERD Table 2. Dysplasia Grade and Surveillance Interval of Barrett s Esophagus Dysplasia Grade First Year Follow-up None Low grade High grade Two endoscopies with biopsies within 1st year Repeat endoscopy with biopsies within 6 12 months Repeat endoscopy with biopsies within 3 months Endoscopy every 3 5 years One-year intervals until no dysplasia on 2 endoscopies Endoscopic resection or ablation Continued 3-month surveillance or intervention Esophagectomy tive therapies. Recent guidelines support the endoscopic eradication of high-grade dysplasia with radiofrequency ablation, photodynamic therapy or endoscopic mucosal resection preferentially over surveillance of high-grade dysplasia [8,48]. In patients without dysplasia on surveillance studies, the recommended follow up should be based upon the highest grade of dysplasia previously confirmed. Patients who have undergone ablative treatment should have biopsies over the entire area of ablation, in time intervals indicated for their prior grade of dysplasia until there are 3 negative consecutive studies [13]. Additionally, continued surveillance is still recommended, as Barrett s esophagus is known to reoccur. Currently there are studies underway evaluating the impact of surveillance endoscopy, with results that should be available in the next few years. There are some caveats to surveillance protocols. While cost-utility studies have demonstrated that screening may have some benefits, continued surveillance in patients with Barrett s esophagus is an expensive practice [11]. Additionally, these patients appear to greatly overestimate their risk of develop adenocarcinoma [49], which can be a source of anxiety and decrease overall quality of life. Advanced Surveillance Technology The current practice of endoscopic surveillance for Barrett s esophagus has limitations in that biopsies are performed randomly and samples may miss metaplasia, dysplasia and esophageal adenocarcinoma because of the patchy distribution of a Barrett s segment [50,51]. Advanced endoscopic optical imaging techniques have been developed with the objective of improving the overall accuracy of endoscopic biopsies of Barrett s epithelium. Narrow-band imaging (electronic chromoendoscopy) uses spectral narrow-band optical filters with a predominance of blue light that highlights mucosal and vascular patterns characteristic of neoplastic tissue [52]. Studies by Kara and Sharma suggest that narrow-band imaging (NBI) has a high sensitivity and specificity for the detection of Barrett s associated neoplasia: 94% and 75%, and 100% and 99%, respectively [53,54]. However, studies by Curvers and by Herrero have shown that NBI does not improve inter-observer agreement or accuracy over high-definition white light endoscopy, independent of expertise [55, 56]. Confocal laser endomicroscopy integrates a confocal laser microscope into the tip of a standard videoendoscope, allowing for real-time histology during the procedure [57]. In a prospective study by Kiesslich et al, patients with Barrett s esophagus underwent endoscope-based confocal laser endomicroscopy (ecle) examination [57]. Barrett s associated neoplasia could be predicted with a sensitivity of 92.9% and a specificity of 98.4%. Sharma et al published results of a multicenter, 568 JCOM December 2012 Vol. 19, No. 12
5 prospective, randomized controlled study in patients with Barrett s esophagus and associated high-grade dysplasia and adenocarcinoma designed to determine the accuracy of probe-based confocal laser endomicroscopy (pcle) [58]. The sensitivity and specificity for highdefinition white light endoscopy with pcle was 68.3% and 87.8%, respectively [58]. Multimodality imaging involves the use of more than one advanced imaging modality simultaneously, with the purpose of improving the detection of high-grade dysplasia and esophageal adenocarcinoma. The techniques that have been used in combination are NBI, autofluorescence imaging and high-resolution endoscopy. However the use of these imaging modalities has not been recommended in current guidelines [8]. Patient Workup The patient undergoes an endoscopic evaluation that demonstrates 4 cm of salmon-colored mucosa with no ulcerations or nodules. Random biopsies confirm the diagnosis of Barrett s esophagus with lowgrade dysplasia and multifocal high-grade dysplasia. How is Barrett s esophagus managed? In the past, esophagectomy was the standard treatment for Barrett s esophagus with high-grade dysplasia. Various minimally invasive techniques have been developed, but esophageal resection may still carry a high risk of complications. Esophagectomy has been correlated with a mortality rate which may be as high as 20% in centers with low-frequency esophagectomies [59,60]. However, the mortality rate may be significantly reduced to less than 2% in experienced, high-volume medical centers [61,62]. Various endoscopic therapies have evolved (Table 3), and subsequently, patients now have alternatives to surgical resection for the treatment of high-grade dysplasia or early intramucosal cancers. Furthermore, the efficacy of endoscopic ablation has been demonstrated in multicenter, randomized controlled trials [63 65]. Endoscopic mucosal resection (EMR) involves the removal of the mucosa and typically partial excision of the submucosa [66]. The most commonly used technique is the ER-cap method. The targeted mucosal tissue is elevated by submucosal injection of fluid and the lesion is sucked into the tip of the endoscope, and then resected with a snare. Another option is the ligate-and-cut technique, which does not require submucosal injection and uses a band-ligating device, similar to variceal ligation device. The ER-cap technique allows for large tissue samples, while the band ligation method is faster and less expensive for multiple resections [67]. EMR can be performed to remove focal visible areas of high-grade dysplasia within a Barrett s segment. It carries the advantage of being both a diagnostic tool, as well as a treatment modality for both high-grade dysplasia and early esophageal adenocarcinoma. Compared to standard endoscopic biopsy methods, EMR enables more precise characterization of neoplasia, less inter-observer variation among pathologists, and more precise evaluation of dysplasia grades and the depths of invasion [48,68,69]. Additionally, EMR can provide more precise staging of submucosal invasion when compared to endoscopic ultrasound [70,71]. Ell et al conducted a single-center prospective study evaluating the efficacy and safety of EMR in patients with low-risk adenocarcinoma of the esophagus arising from Barrett s epithelium. The primary outcome was complete local remission in a mean follow-up period of 36.7 months. Complete local remission was achieved in 99 of the 100 patients. The study also demonstrated that endoscopic therapy appeared to be superior to surgery with regard to mortality and morbidity, as there were no major complications among the 100 patients. The calculated 5-year survival rate was 98% [72]. Before endoscopic therapy can be considered a curative treatment, the extent of the neoplastic involvement must be determined. Esophageal resections performed on intramucosal carcinomas that do not invade the muscularis mucosae have revealed a less than 5% rate of metastases to lymph nodes [73 76]. Therefore, when neoplastic tissue is confined to the mucosa, endoscopic therapy may be a definitive treatment. Thus, EMR has not only a key role in staging early esophageal neoplasms, but also has a role in determining whether endoscopic therapy is appropriate. Prior to undergoing endoscopic therapy, patients should be made aware of complications such as bleeding, perforation, stricture formation and the possibility of residual metaplasia. Moreover, given reported recurrence rates of adenocarcinoma in 10% to 30% [72,77 83], patients should be informed of the necessity of surveillance after endoscopic therapy. Radiofrequency ablation (RFA) uses radiofrequency energy emitted from an endoscopic balloon catheter or Vol. 19, No. 12 December 2012 JCOM 569
6 BARRETT S ESOPHAGUS Table 3. Endoscopic Management of Barrett s Esophagus Treatment Description Benefits Limitations Endoscopic mucosal resection [72,82,83,87] Resection of mucosal and submucosal tissue, allowing for histological evaluation Spares normal tissue Allows for precise cancer staging May require repeat treatment Risk of perforation, bleeding and stricture formation Used on visible lesions Radiofrequency ablation [64,86,87] Radiofrequency energy emitted from endoscopic balloon catheter or focal ablation device Low side-effect profile Requires multiple sessions Requires flat surface for successful ablation Lack of long-term remission data Photodynamic therapy [63,89] Photochemical energy generated with laser light and photosensitizer Treatment in single session Significant post procedure morbidity Multipolar electrocoagulation [90,91] Thermal energy applied to mucosa Well tolerated Easy to use Not used in treatment of highgrade dysplasia and difficult to use in longer segments Argon plasma coagulation [92] Ionized argon gas delivers monopolar energy Easy to use Limited evidence in highgrade dysplasia Risk of residual metaplasia Cryotherapy [94] Endoscopically delivered cryogen (liquid nitrogen or carbon dioxide) Well tolerated Only limited, early clinical trial data available a focal ablation device to destroy Barrett s epithelium. First, the endoscopist determines the diameter of the esophagus with a balloon-measuring device, then an ablation balloon, which is covered with electrodes, is positioned over the esophageal segment to be ablated. Radiofrequency energy is released through the electrodes, producing heat that destroys metaplastic tissue in the muscularis mucosa and superficial submucosa. RFA also has the ability to treat long segments of Barrett s esophagus [66]. Patients typically return 2 to 3 months after the initial RFA treatment for endoscopic assessment, and any remaining metaplastic tissue is removed using the focal ablation device [66]. There have been an increasing number of studies aimed at evaluating the efficacy and safety of RFA in both dysplastic and nondysplastic Barrett s epithelium [64,84,85]. A study by Shaheen et al was the first randomized controlled trial to assess the effectiveness of RFA in eradication of dysplastic Barrett s esophagus [86]. In this multicenter, sham-controlled trial, 127 patients with Barrett s esophagus with low- or high-grade dysplasia were randomly assigned in a 2:1 ratio to receive either RFA or a sham procedure and were surveyed with interval endoscopies for a total of 12 months. Primary outcome was complete eradication of dysplasia and intestinal metaplasia at 12 months. Complete eradication of intestinal metaplasia was found in 77.4% of patients in the RFA group, as compared with 2.3% in the control group (P < 0.001). Among patients with low-grade dysplasia, complete eradication of dysplasia was observed in 90.5% of patients in the treatment group versus 22.7% of those in the control group (P < 0.001). Among patients with high-grade dysplasia, there was complete eradication of dysplasia in 81% in the ablation group compared with 19% in the control group (P < 0.001). The study was not designed to detect a difference in disease progression, yet progression was observed in 16.3% of patients in the control group, as compared with 3.6% of patients in the ablation group (P = 0.03). Esophageal neoplasia developed in significantly more patients in the control group (9.3%) when compared to patients in the ablation group (1.2%, P = 0.045). The investigators extended their initial findings by following this cohort for a mean 3.05 years in a subsequent study [87]. Patients 570 JCOM December 2012 Vol. 19, No. 12
7 were followed for as long as 5 years, depending on their eradication status at 2 years post-ablation. Crossover was permitted between the control and RFA treatment group. After 2 years, 101 of 106 subjects had complete eradication of all dysplasia (95%). Among subjects with initial low-grade dysplasia, dysplasia was eradicated in 51 of 52 (98%) and in those with initial high-grade dysplasia, dysplasia was eradicated in 50 of 54 (93%). After 3 years, dysplasia was eradicated in 55 of 56 of subjects (98%). Kaplan Meier analysis demonstrated that eradication persists in greater than 85% of patients, without maintenance RFA. Serious adverse events were reported in 4 of 119 subjects (3.4%) with a rate of stricture of 7.6%. This study, as well as others [63,86,88], demonstrates comparable efficacy of RFA compared to other modalities. Additionally, the low complication rate and side effect profile make RFA an appealing treatment option for high-grade dysplasia, especially in elderly patients with multiple comorbidities for whom the risk of surgery may be too high. Furthermore, if ablation does not eradicate high-grade dysplasia, surgery and EMR remain an option. Consensus statement by the AGA recommends that RFA, with or without EMR, should be considered as a therapeutic option in select patients with non-dysplastic Barrett s esophagus who are at increased risk for progression of disease [8,42]. However, specific criteria defining that population have not yet been defined. Other ablative techniques include photodynamic therapy (PDT), cryotherapy, multipolar electrocoagulation (MPEC) and argon plasma coagulation (APC). PDT is an ablation technique that uses photochemical energy generated through the interaction of laser light and an intravenously-administered photosensitizer. This interaction leads to the formation of toxic, singlet oxygen molecules that destroy neoplastic tissue. Common side effects of PDT include photosensitivity reactions in > 60%, and stricture formation in up to 36% [63,89]. Because of this side effect profile, PDT is less frequently used as first line treatment for high-grade dysplasia. MPEC involves the application of thermal energy to the mucosa using an electrode-tipped catheter that is advanced through the working channel of the endoscope [90, 91]. MPEC is not practical for ablating large areas of mucosa. Additionally, there is a lack of data establishing the efficacy of MPEC on the treatment of neoplasia in Barrett s esophagus. Likewise, APC is a non-contact technique that delivers monopolar energy to the tissue by using ionized argon gas [66]. However, the recurrence rate of Barrett s esophagus after APC has been reported to be as high as 66% [92]. Given the newer ablation techniques such as RFA and PDT, both APC and MPEC have fallen out of favor for the eradication of Barrett s esophagus [66]. The newest technology available is cryotherapy, which involves the use of an endoscopically delivered cryogen to inflict tissue injury [92]. Two systems exist utilizing either liquid nitrogen or carbon dioxide. Tissue destruction occurs in 2 phases: an immediate phase, caused by freezing of the cells, followed by a delayed phase where cells undergo apoptosis [93]. Cryotherapy can be sprayed without direct contact to mucosal surfaces and therefore may be beneficial for application to uneven surfaces. While data on cryotherapy is still limited, long-term clinical trials are underway. Patient Treatment and Follow-up The patient is started on a proton pump inhibitor and undergoes RFA for the treatment of high-grade dysplasia. Follow-up endoscopy demonstrates eradication of high-grade dysplasia. CONCLUSION While the survival rate from esophageal adenocarcinoma has improved in recent years, the 5-year survival rate is still only 15% to 20% [45]. Physicians caring for the aging population must maintain a high index of suspicion for Barrett s esophagus in patients experiencing longstanding symptoms of reflux, and it is crucial for the physician to refer any patient in whom they suspect Barrett s esophagus or a possible gastrointestinal malignancy to a gastroenterologist. The benefits of screening remain controversial despite continued widespread clinical practice, given the inability to identify high-risk groups, as well as the lack of proven benefit of endoscopic surveillance in patients in whom Barrett s esophagus is identified. Further studies are needed to clearly define the populations that would benefit from screening protocols. Patients with dysplasia or cancer should be seen in a center with expertise in the disease. Current treatment options for Barrett s esophagus include surveillance, endoscopic resection, endoscopic ablation therapy and surgical resection. The treatment needs to be individualized and patient factors such as age, coexisting medical conditions and personal preference, as well as the expertise available in the patient s community must be taken into consideration. Esophageal characteristics such Vol. 19, No. 12 December 2012 JCOM 571
8 BARRETT S ESOPHAGUS as the length of Barrett s segment, presence of visible lesions and the presence of multifocal lesions will also guide treatment options [66]. At the current time, patients who are found to have Barrett s esophagus with high-grade dysplasia or intramucosal esophageal neoplasia have the option of choosing minimally invasive procedures, which appear to have comparable efficacy to surgery, with the benefits of lower morbidity and mortality. Corresponding author: Sharmila Anandasabapathy, MD, Div. of Gastroenterology, The Mount Sinai Medical Center, One Gustave Levy Place, Unit 1069, New York, NY 10029, sharmila.anandasabapathy@mountsinai.org. Financial disclosures: None. REFERENCES 1. Shaheen N, Ransohoff DF. Gastroesophageal reflux, Barrett s esophagus, and esophageal cancer: scientific review. JAMA 2002;287: Jung KW, Talley NJ, Romero Y, et al. Epidemiology and natural history of intestinal metaplasia of the gastroesophageal junction and Barrett s esophagus: a population-based study. Am J Gastroenterol 2011;106: Hvid-Jensen F, Pedersen L, Drewes AM, et al. Incidence of adenocarcinoma among patients with Barrett s esophagus. N Engl J Med 2011;365: Solaymani-Dodaran M, Logan RF, West J, et al. Risk of oesophageal cancer in Barrett s oesophagus and gastrooesophageal reflux. Gut 2004;53: Bhat S, Coleman HG, Yousef F, et al. Risk of malignant progression in Barrett s esophagus patients: results from a large population-based study. J Natl Cancer Inst 2011;103: Desai TK, Krishnan K, Samala N, et al. The incidence of oesophageal adenocarcinoma in non-dysplastic Barrett s oesophagus: a meta-analysis. Gut 2012;61: Alcedo J, Ferrandez A, Arenas J, et al. Trends in Barrett s esophagus diagnosis in Southern Europe: implications for surveillance. Dis Esophagus 2009;22: Spechler SJ, Sharma P, Souza RF, et al. American Gastroenterological Association technical review on the management of Barrett s esophagus. Gastroenterology 2011;140:e Crane SJ, Richard Locke G 3rd, Harmsen WS, et al. The changing incidence of oesophageal and gastric adenocarcinoma by anatomic sub-site. Aliment Pharmacol Ther 2007;25: Hirota WK, Zuckerman MJ, Adler DG, et al. ASGE guideline: the role of endoscopy in the surveillance of premalignant conditions of the upper GI tract. Gastrointest Endosc 2006;63: Inadomi JM, Sampliner R, Lagergren J, et al. Screening and surveillance for Barrett esophagus in high-risk groups: a cost-utility analysis. Ann Intern Med 2003;138: Eloubeidi MA, Homan RK, Martz MD, et al. A cost analysis of outpatient care for patients with Barrett s esophagus in a managed care setting. Am J Gastroenterol 1999;94: Wang KK, Sampliner RE. Updated guidelines 2008 for the diagnosis, surveillance and therapy of Barrett s esophagus. Am J Gastroenterol 2008;103: Rubenstein JH, Scheiman JM, Sadeghi S, et al. Esophageal adenocarcinoma incidence in individuals with gastroesophageal reflux: synthesis and estimates from population studies. Am J Gastroenterol 2011;106: Eloubeidi MA, Provenzale D. Clinical and demographic predictors of Barrett s esophagus among patients with gastroesophageal reflux disease: a multivariable analysis in veterans. J Clin Gastroenterol 2001;33: Eisen GM, Sandler RS, Murray S, Gottfried M. The relationship between gastroesophageal reflux disease and its complications with Barrett s esophagus. Am J Gastroenterol 1997;92: Avidan B, Sonnenberg A, Schnell TG, Sontag SJ. Hiatal hernia and acid reflux frequency predict presence and length of Barrett s esophagus. Dig Dis Sci 2002;47: Smith KJ, O Brien SM, Smithers BM, et al. Interactions among smoking, obesity, and symptoms of acid reflux in Barrett s esophagus. Cancer Epidemiol Biomarkers Prev 2005;14: Lieberman DA, Oehlke M, Helfand M. Risk factors for Barrett s esophagus in community-based practice. GORGE consortium. Gastroenterol Outcomes Res Group Endoscopy. Am J Gastroenterol 1997;92: Gerson LB, Edson R, Lavori PW, Triadafilopoulos G. Use of a simple symptom questionnaire to predict Barrett s esophagus in patients with symptoms of gastroesophageal reflux. Am J Gastroenterol 2001;96: Corley DA, Kubo A, Levin TR, et al. Race, ethnicity, sex and temporal differences in Barrett s oesophagus diagnosis: a large community-based study, Gut 2009;58: Anandasabapathy S, Jhamb J, Davila M, et al. Clinical and endoscopic factors predict higher pathologic grades of Barrett dysplasia. Cancer 2007;109: Lagergren J, Bergstrom R, Lindgren A, Nyren O. Symptomatic gastroesophageal reflux as a risk factor for esophageal adenocarcinoma. N Engl J Med 1999;340: Farrow DC, Vaughan TL, Sweeney C, et al. Gastroesophageal reflux disease, use of H2 receptor antagonists, and risk of esophageal and gastric cancer. Cancer Causes Control 2000;11: Chow WH, Finkle WD, McLaughlin JK, et al. The relation of gastroesophageal reflux disease and its treatment to adenocarcinomas of the esophagus and gastric cardia. JAMA 1995;274: Triadafilopoulos G, Sharma R. Features of symptomatic gastroesophageal reflux disease in elderly patients. Am J Gastroenterol 1997;92: Corley DA, Levin TR, Habel LA, et al. Surveillance and survival in Barrett s adenocarcinomas: a population-based study. Gastroenterology 2002;122: JCOM December 2012 Vol. 19, No. 12
9 28. van Sandick JW, van Lanschot JJ, Kuiken BW, et al. Impact of endoscopic biopsy surveillance of Barrett s oesophagus on pathological stage and clinical outcome of Barrett s carcinoma. Gut 1998;43: Fitzgerald RC, Saeed IT, Khoo D, et al. Rigorous surveillance protocol increases detection of curable cancers associated with Barrett s esophagus. Dig Dis Sci 2001;46: Streitz JM Jr, Andrews CW Jr, Ellis FH Jr. Endoscopic surveillance of Barrett s esophagus. Does it help? J Thorac Cardiovasc Surg 1993;105: Peters JH, Clark GW, Ireland AP, et al. Outcome of adenocarcinoma arising in Barrett s esophagus in endoscopically surveyed and nonsurveyed patients. J Thorac Cardiovasc Surg 1994;108: Fountoulakis A, Zafirellis KD, Dolan K, et al. Effect of surveillance of Barrett s oesophagus on the clinical outcome of oesophageal cancer. Br J Surg 2004;91: Cooper GS, Yuan Z, Chak A, Rimm AA. Association of prediagnosis endoscopy with stage and survival in adenocarcinoma of the esophagus and gastric cardia. Cancer 2002;95: Cooper GS, Kou TD, Chak A. Receipt of previous diagnoses and endoscopy and outcome from esophageal adenocarcinoma: a population-based study with temporal trends. Am J Gastroenterol 2009;104: Rubenstein JH, Sonnenberg A, Davis J, et al. Effect of a prior endoscopy on outcomes of esophageal adenocarcinoma among United States veterans. Gastrointest Endosc 2008;68: Anderson LA, Murray LJ, Murphy SJ, et al. Mortality in Barrett s oesophagus: results from a population based study. Gut 2003;52: Rana PS, Johnston DA. Incidence of adenocarcinoma and mortality in patients with Barrett s oesophagus diagnosed between 1976 and 1986: implications for endoscopic surveillance. Dis Esoph 2000;13: Macdonald CE, Wicks AC, Playford RJ. Final results from 10 year cohort of patients undergoing surveillance for Barrett s oesophagus: observational study. BMJ 2000;321: Conio M, Blanchi S, Lapertosa G, et al. Long-term endoscopic surveillance of patients with Barrett s esophagus. Incidence of dysplasia and adenocarcinoma: a prospective study. Am J Gastroenterol 2003;98: Eloubeidi MA, Mason AC, Desmond RA, El-Serag HB. Temporal trends ( ) in survival of patients with esophageal adenocarcinoma in the United States: a glimmer of hope? Am J Gastroenterol 2003;98: Gilani N, Gerkin RD, Ramirez FC, et al. Prevalence of Barrett s esophagus in patients with moderate to severe erosive esophagitis. World J Gastroenterol 2008;14: Spechler SJ, Sharma P, Souza RF, et al. American Gastroenterological Association medical position statement on the management of Barrett s esophagus. Gastroenterology 2011;140: Lundell L, Miettinen P, Myrvold HE, et al. Continued (5-year) followup of a randomized clinical study comparing antireflux surgery and omeprazole in gastroesophageal reflux disease. J Am Coll Surg 2001;192: Yau P, Watson DI, Devitt PG, et al. Laparoscopic antireflux surgery in the treatment of gastroesophageal reflux in patients with Barrett esophagus. Arch Surg 2000;135: Sharma P, McQuaid K, Dent J, et al. A critical review of the diagnosis and management of Barrett s esophagus: the AGA Chicago Workshop. Gastroenterology 2004;127: Gross CP, Canto MI, Hixson J, Powe NR. Management of Barrett s esophagus: a national study of practice patterns and their cost implications. Am J Gastroenterol 1999;94: Shaheen NJ, Sharma P, Overholt BF, et al. Radiofrequency ablation in Barrett s esophagus with dysplasia. N Engl J Med 2009;360: Bennett C, Vakil N, Bergman J, et al. Consensus statements for management of barrett s dysplasia and early-stage esophageal adenocarcinoma, based on a delphi process. Gastroenterology 2012;143: Shaheen NJ, Green B, Medapalli RK, et al. The perception of cancer risk in patients with prevalent Barrett s esophagus enrolled in an endoscopic surveillance program. Gastroenterology 2005;129: Vieth M, Ell C, Gossner L, et al. Histological analysis of endoscopic resection specimens from 326 patients with Barrett s esophagus and early neoplasia. Endoscopy 2004;36: Tschanz ER. Do 40% of patients resected for barrett esophagus with high-grade dysplasia have unsuspected adenocarcinoma? Arch Pathol Lab Med 2005;129: Gono K, Obi T, Yamaguchi M, et al. Appearance of enhanced tissue features in narrow-band endoscopic imaging. J Biomed Optics 2004;9: Sharma P, Bansal A, Mathur S, et al. The utility of a novel narrow band imaging endoscopy system in patients with Barrett s esophagus. Gastrointest Endosc 2006;64: Kara MA, Peters FP, Fockens P, et al. Endoscopic videoautofluorescence imaging followed by narrow band imaging for detecting early neoplasia in Barrett s esophagus. Gastrointest Endosc 2006;64: Kwon RS, Wong Kee Song LM, Adler DG, et al. Endocytoscopy. Gastrointest Endosc 2009;70: Kodashima S, Fujishiro M, Takubo K, et al. Ex-vivo study of high-magnification chromoendoscopy in the gastrointestinal tract to determine the optimal staining conditions for endocytoscopy. Endoscopy 2006;38: Kiesslich R, Gossner L, Goetz M, et al. In vivo histology of Barrett s esophagus and associated neoplasia by confocal laser endomicroscopy. Clin Gastroenterol Hepatol 2006;4: Sharma P, Meining AR, Coron E, et al. Real-time increased detection of neoplastic tissue in Barrett s esophagus with probe-based confocal laser endomicroscopy: final results of an international multicenter, prospective, randomized, controlled trial. Gastrointest Endosc 2011;74: Birkmeyer JD, Siewers AE, Finlayson EV, et al. Hospital volume and surgical mortality in the United States. N Engl Vol. 19, No. 12 December 2012 JCOM 573
10 BARRETT S ESOPHAGUS J Med 2002;346: Birkmeyer, JD, Stukel TA, Siewers AE, et al. Surgeon volume and operative mortality in the United States. N Engl J Med 2003;349: Smith JW, Shiu MH, Kelsey L, Brennan MF. Morbidity of radical lymphadenectomy in the curative resection of gastric carcinoma. Arch Surg 1991;126: Sano T, Sasako M, Yamamoto S, et al. Gastric cancer surgery: morbidity and mortality results from a prospective randomized controlled trial comparing D2 and extended para-aortic lymphadenectomy--japan Clinical Oncology Group study J Clin Oncol 2004;22: Overholt BF, Lightdale CJ, Wang KK, et al. Photodynamic therapy with porfimer sodium for ablation of high-grade dysplasia in Barrett s esophagus: international, partially blinded, randomized phase III trial. Gastrointest Endosc 2005;62: Fleischer DE, Overholt BF, Sharma VK, et al. Endoscopic ablation of Barrett s esophagus: a multicenter study with 2.5-year follow-up. Gastrointest Endosc 2008;68: Inadomi JM, Somsouk M, Madanick RD, et al. A costutility analysis of ablative therapy for Barrett s esophagus. Gastroenterology 2009;136: Spechler SJ, Fitzgerald RC, Prasad GA, Wang KK. History, molecular mechanisms, and endoscopic treatment of Barrett s esophagus. Gastroenterology 2010;138: Peters FP, Kara MA, Curvers WL, et al. Multiband mucosectomy for endoscopic resection of Barrett s esophagus: feasibility study with matched historical controls. Eur J Gastroenterol Hepatol 2007;19: Peters FP, Brakenhoff KP, Curvers WL, et al. Histologic evaluation of resection specimens obtained at 293 endoscopic resections in Barrett s esophagus. Gastrointest Endosc 2008;67: Mino-Kenudson M, Hull MJ, Brown I, et al. EMR for Barrett s esophagus-related superficial neoplasms offers better diagnostic reproducibility than mucosal biopsy. Gastrointest Endosc 2007;66: Prasad GA, Buttar NS, Wongkeesong LM, et al. Significance of neoplastic involvement of margins obtained by endoscopic mucosal resection in Barrett s esophagus. Am J Gastroenterol 2007;102: Larghi A, Lightdale CJ, Memeo L, et al. EUS followed by EMR for staging of high-grade dysplasia and early cancer in Barrett s esophagus. Gastrointest Endosc 2005;62: Ell C, May A, Pech O, et al. Curative endoscopic resection of early esophageal adenocarcinomas (Barrett s cancer). Gastrointest Endosc 2007;65: Montgomery E, Bronner MP, Goldblum JR, et al. Reproducibility of the diagnosis of dysplasia in Barrett esophagus: a reaffirmation. Hum Pathol 2001;32: Montgomery E, Goldblum JR, Greenson JK, et al. Dysplasia as a predictive marker for invasive carcinoma in Barrett esophagus: a follow-up study based on 138 cases from a diagnostic variability study. Hum Pathol 2001;32: Lewis JT, Wang KK, Abraham SC. Muscularis mucosae duplication and the musculo-fibrous anomaly in endoscopic mucosal resections for barrett esophagus: implications for staging of adenocarcinoma. Am J Surg Pathol 2008;32: Stein HJ, Feith M, Bruecher BL, et al. Early esophageal cancer: pattern of lymphatic spread and prognostic factors for long-term survival after surgical resection. Ann Surg 2005;242: Moss A, Bourke MJ, Hourigan LF, et al. Endoscopic resection for Barrett s high-grade dysplasia and early esophageal adenocarcinoma: an essential staging procedure with long-term therapeutic benefit. Am J Gastroenterol 2010;105: Ell C, May A, Gossner L, et al. Endoscopic mucosal resection of early cancer and high-grade dysplasia in Barrett s esophagus. Gastroenterology 2000;118: Ciocirlan M, Lapalus MG, Hervieu V, et al. Endoscopic mucosal resection for squamous premalignant and early malignant lesions of the esophagus. Endoscopy 2007;39: Esaki M, Matsumoto T, Hirakawa K, et al. Risk factors for local recurrence of superficial esophageal cancer after treatment by endoscopic mucosal resection. Endoscopy 2007;39: May A, Gossner L, Pech O, et al. Local endoscopic therapy for intraepithelial high-grade neoplasia and early adenocarcinoma in Barrett s oesophagus: acute-phase and intermediate results of a new treatment approach. Eur J Gastroenterol Hepatol 2002;14: Pech O, Behrens A, May A, et al. Long-term results and risk factor analysis for recurrence after curative endoscopic therapy in 349 patients with high-grade intraepithelial neoplasia and mucosal adenocarcinoma in Barrett s oesophagus. Gut 2008;57: Prasad GA, Wu TT, Wigle DA, et al. Endoscopic and surgical treatment of mucosal (T1a) esophageal adenocarcinoma in Barrett s esophagus. Gastroenterology 2009;137: Ganz RA, Overholt BF, Sharma VK, et al. Circumferential ablation of Barrett s esophagus that contains high-grade dysplasia: a U.S. Multicenter Registry. Gastrointest Endosc 2008;68: Sharma VK, Jae Kim H, Das A, et al. Circumferential and focal ablation of Barrett s esophagus containing dysplasia. Am J Gastroenterol 2009;104: Shaheen NJ, Sharma P, Overholt BF, et al. Radiofrequency ablation in Barrett s esophagus with dysplasia. N Engl J Med 2009;360: Shaheen NJ, Overholt BF, Sampliner RE, et al. Durability of radiofrequency ablation in Barrett s esophagus with dysplasia. Gastroenterology 2011;141: Gondrie JJ, Pouw RE, Sondermeijer CM, et al. Stepwise circumferential and focal ablation of Barrett s esophagus with high-grade dysplasia: results of the first prospective series of 11 patients. Endoscopy 2008;40: Prasad GA, Wang KK, Buttar NS, et al. Predictors of stricture formation after photodynamic therapy for highgrade dysplasia in Barrett s esophagus. Gastrointest Endosc 2007;65: JCOM December 2012 Vol. 19, No. 12
11 90. Sampliner RE, Faigel D, Fennerty MB, et al. Effective and safe endoscopic reversal of nondysplastic Barrett s esophagus with thermal electrocoagulation combined with high-dose acid inhibition: a multicenter study. Gastrointest Endosc 2001;53: Dulai GS, Jensen DM, Cortina G, et al. Randomized trial of argon plasma coagulation vs. multipolar electrocoagulation for ablation of Barrett s esophagus. Gastrointest Endosc 2005;61: Mork H, Al-Taie O, Berlin F, et al. High recurrence rate of Barrett s epithelium during long-term follow-up after argon plasma coagulation. Scand J Gastroenterol 2007;42: Gage AA, Baust J. Mechanisms of tissue injury in cryosurgery. Cryobiology 1998;37: Greenwald BD, Dumot JA, Horwhat JD, et al. Safety, tolerability, and efficacy of endoscopic low-pressure liquid nitrogen spray cryotherapy in the esophagus. Dis Esoph 2010;23:13 9. Copyright 2012 by Turner White Communications Inc., Wayne, PA. All rights reserved. Vol. 19, No. 12 December 2012 JCOM 575
Current Management: Role of Radiofrequency Ablation
 Esophageal Adenocarcinoma And Barrett s Esophagus: Current Management: Role of Radiofrequency Ablation Ketan Kulkarni, MD Regional Gastroenterology Associates of Lancaster INTRODUCTION The prognosis of
Esophageal Adenocarcinoma And Barrett s Esophagus: Current Management: Role of Radiofrequency Ablation Ketan Kulkarni, MD Regional Gastroenterology Associates of Lancaster INTRODUCTION The prognosis of
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus
 New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus: Old Dog, New Tricks
 Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic management of Barrett s esophagus with dysplasia
 UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
Endoscopic Management of Barrett s Esophagus
 Endoscopic Management of Barrett s Esophagus Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Barrett s Esophagus Consequence of chronic GERD Mean
Endoscopic Management of Barrett s Esophagus Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Barrett s Esophagus Consequence of chronic GERD Mean
Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery
 Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery Norman Barrett (1950) described the esophagus as: that part of the foregut, distal to the cricopharyngeal sphincter, which is lined
Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery Norman Barrett (1950) described the esophagus as: that part of the foregut, distal to the cricopharyngeal sphincter, which is lined
Ablation for Barrett s Esophagus: Burn or Freeze
 Ablation for Barrett s Esophagus: Burn or Freeze John R. Saltzman MD Director of Endoscopy Brigham and Women s Hospital Professor of Medicine Harvard Medical School Disclosures No relevant disclosures
Ablation for Barrett s Esophagus: Burn or Freeze John R. Saltzman MD Director of Endoscopy Brigham and Women s Hospital Professor of Medicine Harvard Medical School Disclosures No relevant disclosures
Barrett s esophagus. Barrett s neoplasia treatment trends
 Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
Definition of GERD American College of Gastroenterology
 Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Present Day Management of Barrett s Esophagus
 Slide 1 Present Day Management of Barrett s Esophagus Kinnari R. Kher, M.D. Slide 2 Goals Risk factors for development of Barrett s esophagus Risks for progression to Esophageal Adenocarcinoma Current
Slide 1 Present Day Management of Barrett s Esophagus Kinnari R. Kher, M.D. Slide 2 Goals Risk factors for development of Barrett s esophagus Risks for progression to Esophageal Adenocarcinoma Current
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus. Original Policy Date
 MP 2.01.52 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature
MP 2.01.52 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature
Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD?
 Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD? Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina 1 Outline What are the risks of progression
Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD? Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina 1 Outline What are the risks of progression
Gregory G. Ginsberg, M.D.
 Radiofrequency Ablation for Barrett s Esophagus with HGD Gregory G. Ginsberg, M.D. Professor of Medicine University of Pennsylvania School of Medicine Abramson Cancer Center Gastroenterology Division Executive
Radiofrequency Ablation for Barrett s Esophagus with HGD Gregory G. Ginsberg, M.D. Professor of Medicine University of Pennsylvania School of Medicine Abramson Cancer Center Gastroenterology Division Executive
Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell
 Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell Department of Internal Medicine 2, HSK Wiesbaden, Wiesbaden, Germany Correspondence to Oliver Pech, MD, PhD, Department of Gastroenterology,
Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell Department of Internal Medicine 2, HSK Wiesbaden, Wiesbaden, Germany Correspondence to Oliver Pech, MD, PhD, Department of Gastroenterology,
Management of Barrett s: From Imaging to Resection
 Management of Barrett s: From Imaging to Resection Michael Wallace, MD, MPH, FACG Professor of Medicine Mayo Clinic Florida Goals of Endoscopic Evaluation in Barrett s Detect Barrett s and dysplasia Reduce/eliminate
Management of Barrett s: From Imaging to Resection Michael Wallace, MD, MPH, FACG Professor of Medicine Mayo Clinic Florida Goals of Endoscopic Evaluation in Barrett s Detect Barrett s and dysplasia Reduce/eliminate
Current Management of Low-Grade Dysplasia in Barrett Esophagus
 Current Management of Low-Grade Dysplasia in Barrett Esophagus Gary W. Falk, MD, MS Dr Falk is a professor of medicine in the Division of Gastroenterology at the University of Pennsylvania Perelman School
Current Management of Low-Grade Dysplasia in Barrett Esophagus Gary W. Falk, MD, MS Dr Falk is a professor of medicine in the Division of Gastroenterology at the University of Pennsylvania Perelman School
Barrett s Esophagus. Radiofrequency Ablation with the HALO Technology A Reference Book
 Radiofrequency Ablation with the HALO Technology A Reference Book 540 Oakmead Parkway, Sunnyvale, CA 94085 What is Barrett s esophagus? Barrett s esophagus is a change that occurs within the cellular lining
Radiofrequency Ablation with the HALO Technology A Reference Book 540 Oakmead Parkway, Sunnyvale, CA 94085 What is Barrett s esophagus? Barrett s esophagus is a change that occurs within the cellular lining
Is Radiofrequency Ablation Effective In Treating Barrett s Esophagus Patients with High-Grade Dysplasia?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2016 Is Radiofrequency Ablation Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2016 Is Radiofrequency Ablation Effective
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus
 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus Policy Number: 2.01.80 Last Review: 6/2018 Origination: 6/2012 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus Policy Number: 2.01.80 Last Review: 6/2018 Origination: 6/2012 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas
Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia
 ...PRESENTATIONS... Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia Based on a presentation by Bergein F. Overholt, MD Presentation Summary Thermal ablation and surgery are
...PRESENTATIONS... Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia Based on a presentation by Bergein F. Overholt, MD Presentation Summary Thermal ablation and surgery are
Section: Medicine Effective Date: July 15, 2015 Subsection: Original Policy Date: December 7, 2011 Subject:
 Last Review Status/Date: June 2015 Page: 1 of 16 Cryoablation for Barrett s Esophagus Description Barrett s esophagus (BE) is a condition in which the normal squamous epithelium is replaced by specialized
Last Review Status/Date: June 2015 Page: 1 of 16 Cryoablation for Barrett s Esophagus Description Barrett s esophagus (BE) is a condition in which the normal squamous epithelium is replaced by specialized
MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018
 MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018 Sachin Wani Medical Director Esophageal and Gastric Center Division of Gastroenterology and Hepatology University of Colorado Anschutz Medical Campus DISCLOSURES
MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018 Sachin Wani Medical Director Esophageal and Gastric Center Division of Gastroenterology and Hepatology University of Colorado Anschutz Medical Campus DISCLOSURES
Medicare Advantage Medical Policy
 Medicare Advantage Medical Policy Current Policy Effective Date: 1/1/18 Title: Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Description/Background Barrett Esophagus and the
Medicare Advantage Medical Policy Current Policy Effective Date: 1/1/18 Title: Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Description/Background Barrett Esophagus and the
ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus
 ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G. Iyer, MD, MSc, FACG 3 and Lauren Gerson, MD, MSc, FACG
ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G. Iyer, MD, MSc, FACG 3 and Lauren Gerson, MD, MSc, FACG
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus
 Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Populations Interventions Comparators Outcomes Individuals: With Barrett esophagus with high-grade dysplasia
 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett (20180) Medical Benefit Effective Date: 01/01/16 Next Review Date: 09/19 Preauthorization No Review Dates: 05/09, 03/10, 03/11, 03/12, 07/12,
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett (20180) Medical Benefit Effective Date: 01/01/16 Next Review Date: 09/19 Preauthorization No Review Dates: 05/09, 03/10, 03/11, 03/12, 07/12,
History. Prevalence at Endoscopy. Prevalence and Reflux Sx. Prevalence at Endoscopy. Barrett s Esophagus: Controversy and Management
 Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus
 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Policy Number: Original Effective Date: MM.02.005 09/01/2010 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Policy Number: Original Effective Date: MM.02.005 09/01/2010 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration
RFA and Cyrotherapy for Esophageal Disease
 RFA and Cyrotherapy for Esophageal Disease Daniel L. Miller MD Chief, General Thoracic Surgery WellStar Healthcare System/ Mayo Clinic Care Network Clinical Professor of Surgery Medical College of Georgia/
RFA and Cyrotherapy for Esophageal Disease Daniel L. Miller MD Chief, General Thoracic Surgery WellStar Healthcare System/ Mayo Clinic Care Network Clinical Professor of Surgery Medical College of Georgia/
Faculty Disclosure. Objectives. State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) 24/11/2014
 State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
Barrett s Esophagus: Ablate Everyone?
 Nicholas J. Shaheen, MD, MPH, FACG Barrett s Esophagus: Ablate Everyone? Nicholas J. Shaheen, MD, MPH, FACG Center for Esophageal Diseases and Swallowing University of North Carolina Greetings from UNC,
Nicholas J. Shaheen, MD, MPH, FACG Barrett s Esophagus: Ablate Everyone? Nicholas J. Shaheen, MD, MPH, FACG Center for Esophageal Diseases and Swallowing University of North Carolina Greetings from UNC,
Learning Objectives:
 Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Editorial: Advanced endoscopic therapeutics in Barrett s neoplasia; where are we now and where are we heading?
 Editorial: Advanced endoscopic therapeutics in Barrett s neoplasia; where are we now and where are we heading? Dr. Gaius Longcroft-Wheaton MB,BS, MD, MRCP(UK), MRCP(Gastro) Consultant gastroenterologist
Editorial: Advanced endoscopic therapeutics in Barrett s neoplasia; where are we now and where are we heading? Dr. Gaius Longcroft-Wheaton MB,BS, MD, MRCP(UK), MRCP(Gastro) Consultant gastroenterologist
Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment Barrett s esophagus
 E318 Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment esophagus Authors Institution Arvind J. Trindade, Benley J. George, Joshua Berkowitz,
E318 Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment esophagus Authors Institution Arvind J. Trindade, Benley J. George, Joshua Berkowitz,
Barrett's Esophagus: Sorting Out the Controversy
 Barrett's Esophagus: Sorting Out the Controversy Learning Objectives 1. Identify the challenges in screening for Barrett s esophagus 2. Demonstrate comprehension of the risk of progression of Barrett s
Barrett's Esophagus: Sorting Out the Controversy Learning Objectives 1. Identify the challenges in screening for Barrett s esophagus 2. Demonstrate comprehension of the risk of progression of Barrett s
Management of Barrett s Esophagus. Case Presentation
 Management of Barrett s Esophagus Lauren B. Gerson MD, MSc Associate Clinical Professor, UCSF Director of Clinical Research Gastroenterology Fellowship Program California Pacific Medical Center San Francisco,
Management of Barrett s Esophagus Lauren B. Gerson MD, MSc Associate Clinical Professor, UCSF Director of Clinical Research Gastroenterology Fellowship Program California Pacific Medical Center San Francisco,
Accepted Manuscript. CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D
 Accepted Manuscript CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D PII: S1542-3565(18)31093-0 DOI: 10.1016/j.cgh.2018.10.010 Reference: YJCGH 56132
Accepted Manuscript CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D PII: S1542-3565(18)31093-0 DOI: 10.1016/j.cgh.2018.10.010 Reference: YJCGH 56132
Sixteen-year follow-up of Barrett s esophagus, endoscopically treated with argon plasma coagulation
 Original Article Sixteen-year of Barrett s esophagus, endoscopically treated with argon plasma coagulation United European Gastroenterology Journal 2014, Vol. 2(5) 367 373! Author(s) 2014 Reprints and
Original Article Sixteen-year of Barrett s esophagus, endoscopically treated with argon plasma coagulation United European Gastroenterology Journal 2014, Vol. 2(5) 367 373! Author(s) 2014 Reprints and
Changes to the diagnosis and management of Barrett s Oesophagus
 Changes to the diagnosis and management of Barrett s Oesophagus A review of the new BSG and NICE guidelines and best practice Anjan Dhar DM, MD, FRCPE, AGAF, MBBS (Hons.), Cert. Med. Ed Senior Lecturer
Changes to the diagnosis and management of Barrett s Oesophagus A review of the new BSG and NICE guidelines and best practice Anjan Dhar DM, MD, FRCPE, AGAF, MBBS (Hons.), Cert. Med. Ed Senior Lecturer
In 1998, the American College of Gastroenterology issued ALIMENTARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
Cryospray ablation using pressurized CO 2 for ablation of Barrett s esophagus with early neoplasia: early termination of a prospective series
 E17 Cryospray ablation using pressurized CO 2 for ablation of Barrett s esophagus with early neoplasia: early termination of a prospective series Authors Romy E. Verbeek 1, Frank P. Vleggaar 1, Fiebo J.
E17 Cryospray ablation using pressurized CO 2 for ablation of Barrett s esophagus with early neoplasia: early termination of a prospective series Authors Romy E. Verbeek 1, Frank P. Vleggaar 1, Fiebo J.
DISCLOSURES. This program meets the requirements for GI specific Category 1 contact hours. M
 DISCLOSURES Educational Dimensions is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center s Commission on Accreditation. Successful completion: Participants
DISCLOSURES Educational Dimensions is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center s Commission on Accreditation. Successful completion: Participants
AGA SECTION. Gastroenterology 2016;150:
 Gastroenterology 2016;150:1026 1030 April 2016 AGA Section 1027 Procedural intervention (3) Upper endoscopy indications 3 6 Non-response of symptoms to a 4 8 week empiric trial of twice-daily PPI Troublesome
Gastroenterology 2016;150:1026 1030 April 2016 AGA Section 1027 Procedural intervention (3) Upper endoscopy indications 3 6 Non-response of symptoms to a 4 8 week empiric trial of twice-daily PPI Troublesome
This medical position statement considers a series of
 GASTROENTEROLOGY 2011;140:1084 1091 American Gastroenterological Association Medical Position Statement on the Management of Barrett s Esophagus The Institute Medical Position Panel consisted of the authors
GASTROENTEROLOGY 2011;140:1084 1091 American Gastroenterological Association Medical Position Statement on the Management of Barrett s Esophagus The Institute Medical Position Panel consisted of the authors
How to remove BE cancer: EMR or ESD? Expected outcome
 How to remove BE cancer: EMR or ESD? Expected outcome Presented by Horst Neuhaus Institution Dpt. of Gastroenterology Evangelisches Krankenhaus Düsseldorf, Germany Indications for endoscopic resection
How to remove BE cancer: EMR or ESD? Expected outcome Presented by Horst Neuhaus Institution Dpt. of Gastroenterology Evangelisches Krankenhaus Düsseldorf, Germany Indications for endoscopic resection
Slide 1. Slide 2. Slide 3 DISCLOSURES EXPECTED OUTCOMES DIAGNOSIS AND TREATMENT
 Slide 1 DIAGNOSIS AND TREATMENT 1 Slide 2 DISCLOSURES Successful completion: Participants must attend the entire program, including any resulting Q & A, and submit required documentation. Conflict of interest:
Slide 1 DIAGNOSIS AND TREATMENT 1 Slide 2 DISCLOSURES Successful completion: Participants must attend the entire program, including any resulting Q & A, and submit required documentation. Conflict of interest:
American Journal of Gastroenterology. Volumetric Laser Endomicroscopy Detects Subsquamous Barrett s Adenocarcinoma
 Volumetric Laser Endomicroscopy Detects Subsquamous Barrett s Adenocarcinoma Journal: Manuscript ID: AJG-13-1412.R1 Manuscript Type: Letter to the Editor Keywords: Barrett-s esophagus, Esophagus, Endoscopy
Volumetric Laser Endomicroscopy Detects Subsquamous Barrett s Adenocarcinoma Journal: Manuscript ID: AJG-13-1412.R1 Manuscript Type: Letter to the Editor Keywords: Barrett-s esophagus, Esophagus, Endoscopy
Barrett esophagus. Bible class Inselspital
 Barrett esophagus Bible class Inselspital 2015.08.10 Guidelines Definition? BSG: ACG: Definition? BSG: ACG: What are the arguments for and against IM as prerequisite for the Dg? What are the arguments
Barrett esophagus Bible class Inselspital 2015.08.10 Guidelines Definition? BSG: ACG: Definition? BSG: ACG: What are the arguments for and against IM as prerequisite for the Dg? What are the arguments
Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic management of Barrett s esophagus with dysplasia
 UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions
 Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
Barrett s esophagus (BE), the premalignant condition
 GASTROENTEROLOGY 2009;136:2101 2114 A Cost-Utility Analysis of Ablative Therapy for Barrett s Esophagus JOHN M. INADOMI,*, MA SOMSOUK,*, RYAN D. MADANICK, JENNIFER P. THOMAS, and NICHOLAS J. SHAHEEN *Division
GASTROENTEROLOGY 2009;136:2101 2114 A Cost-Utility Analysis of Ablative Therapy for Barrett s Esophagus JOHN M. INADOMI,*, MA SOMSOUK,*, RYAN D. MADANICK, JENNIFER P. THOMAS, and NICHOLAS J. SHAHEEN *Division
Everything Esophagus: Barrett s Esophagus. Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina
 Everything Esophagus: Barrett s Esophagus Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina The Most Important Thing Stayed the Same Adenocarcinoma A
Everything Esophagus: Barrett s Esophagus Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina The Most Important Thing Stayed the Same Adenocarcinoma A
RADIOFREQUENCY ABLATION OR CRYOABLATION FOR ESOPHAGEAL DISORDERS
 DISORDERS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
DISORDERS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ
 Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ Table of contents 1 General project information...3 1.1 Inclusion criteria...3 1.2 Registration time points...3 1.3 Project variable
Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ Table of contents 1 General project information...3 1.1 Inclusion criteria...3 1.2 Registration time points...3 1.3 Project variable
Speaker disclosure. Objectives. GERD: Who and When to Treat 7/21/2015
 GERD: Who and When to Treat Eugenio J Hernandez, MD Gastrohealth, PL Assistant Professor of Clinical Medicine, FIU Herbert Wertheim School of Medicine Speaker disclosure I do not have any relevant commercial
GERD: Who and When to Treat Eugenio J Hernandez, MD Gastrohealth, PL Assistant Professor of Clinical Medicine, FIU Herbert Wertheim School of Medicine Speaker disclosure I do not have any relevant commercial
Efficacy of Radiofrequency Ablation Combined With Endoscopic Resection for Barrett s Esophagus With Early Neoplasia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:23 29 ENDOSCOPY CORNER Efficacy of Radiofrequency Ablation Combined With Endoscopic Resection for Barrett s Esophagus With Early Neoplasia ROOS E. POUW,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:23 29 ENDOSCOPY CORNER Efficacy of Radiofrequency Ablation Combined With Endoscopic Resection for Barrett s Esophagus With Early Neoplasia ROOS E. POUW,*
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia
 Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of the distal esophagus, gastroesophageal junction and gastric cardia?
 Diseases of the Esophagus (2007) 20, 36 41 DOI: 10.1111/j.1442-2050.2007.00638.x Blackwell Publishing Asia Original article Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of
Diseases of the Esophagus (2007) 20, 36 41 DOI: 10.1111/j.1442-2050.2007.00638.x Blackwell Publishing Asia Original article Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of
Esophageal cancer: Biology, natural history, staging and therapeutic options
 EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
Current challenges in Barrett s esophagus
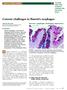 MEDICAL GRAND ROUNDS TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY Current challenges in Barrett s esophagus GARY W. FALK, MD * Director, Center for Swallowing and Esophageal
MEDICAL GRAND ROUNDS TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY Current challenges in Barrett s esophagus GARY W. FALK, MD * Director, Center for Swallowing and Esophageal
Frozen Section Analysis of Esophageal Endoscopic Mucosal Resection Specimens in the Real-Time Management of Barrett s Esophagus
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:173 178 Frozen Section Analysis of Esophageal Endoscopic Mucosal Resection Specimens in the Real-Time Management of Barrett s Esophagus GANAPATHY A. PRASAD,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:173 178 Frozen Section Analysis of Esophageal Endoscopic Mucosal Resection Specimens in the Real-Time Management of Barrett s Esophagus GANAPATHY A. PRASAD,*
Treatment of High-Grade Dysplasia and Early Stage Esophageal Adenocarcinoma with an Endoscope: The Ultimate in Minimally Invasive, Curative Therapy
 Curr Surg Rep (2014) 2:66 DOI 10.1007/s40137-014-0066-x ESOPHAGEAL/REFLUX SURGERY (SR DEMEESTER, SECTION EDITOR) Treatment of High-Grade Dysplasia and Early Stage Esophageal Adenocarcinoma with an Endoscope:
Curr Surg Rep (2014) 2:66 DOI 10.1007/s40137-014-0066-x ESOPHAGEAL/REFLUX SURGERY (SR DEMEESTER, SECTION EDITOR) Treatment of High-Grade Dysplasia and Early Stage Esophageal Adenocarcinoma with an Endoscope:
Barrett s Esophagus in Women: Demographic Features and Progression to High-Grade Dysplasia and Cancer
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1089 1094 Barrett s Esophagus in Women: Demographic Features and Progression to High-Grade Dysplasia and Cancer GARY W. FALK,* PRASHANTHI N. THOTA,* JOEL
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1089 1094 Barrett s Esophagus in Women: Demographic Features and Progression to High-Grade Dysplasia and Cancer GARY W. FALK,* PRASHANTHI N. THOTA,* JOEL
Recurrent intestinal metaplasia at the gastroesophageal junction following endoscopic eradication of dysplastic Barrett s esophagus may not be benign
 THIEME E849 Recurrent intestinal metaplasia at the gastroesophageal junction following endoscopic eradication of dysplastic Barrett s esophagus may not be benign Authors Georgina R. Cameron 1, 3, Paul
THIEME E849 Recurrent intestinal metaplasia at the gastroesophageal junction following endoscopic eradication of dysplastic Barrett s esophagus may not be benign Authors Georgina R. Cameron 1, 3, Paul
Disclosures. Gastroesophageal Reflux Disease. Gastroesophageal Reflux Disease
 Kunal Jajoo, MD Brigham and Women s Hospital July 2012 Disclosures Spouse is a physician employed by Boston Scientific Corporation The content of this lecture equitably discusses products of multiple companies
Kunal Jajoo, MD Brigham and Women s Hospital July 2012 Disclosures Spouse is a physician employed by Boston Scientific Corporation The content of this lecture equitably discusses products of multiple companies
Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus
 Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus Robert J. Korst, MD, a,b Sobeida Santana-Joseph, MSN, a,b John R. Rutledge, MAS,
Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus Robert J. Korst, MD, a,b Sobeida Santana-Joseph, MSN, a,b John R. Rutledge, MAS,
The incidence of esophageal adenocarcinoma (EAC) CLINICAL ALIMENTARY TRACT
 GASTROENTEROLOGY 2009;137:815 823 CLINICAL Endoscopic and Surgical Treatment of Mucosal (T1a) Esophageal Adenocarcinoma in Barrett s Esophagus GANAPATHY A. PRASAD,* TSUNG TEH WU, DENNIS A. WIGLE, NAVTEJ
GASTROENTEROLOGY 2009;137:815 823 CLINICAL Endoscopic and Surgical Treatment of Mucosal (T1a) Esophageal Adenocarcinoma in Barrett s Esophagus GANAPATHY A. PRASAD,* TSUNG TEH WU, DENNIS A. WIGLE, NAVTEJ
Relative risk of dysplasia for patients with intestinal metaplasia in the distal oesophagus and in the gastric cardia
 Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Treat Barrett s, Remove the Risk. HALO System
 Treat Barrett s, Remove the Risk HALO System The HALO 360 System Advanced Ablation Technology for Barrett s Esophagus The HALO 360 System is designed to remove the Barrett s epithelium in a short, well-tolerated
Treat Barrett s, Remove the Risk HALO System The HALO 360 System Advanced Ablation Technology for Barrett s Esophagus The HALO 360 System is designed to remove the Barrett s epithelium in a short, well-tolerated
Endoscopic Therapy of Barrett s Esophagus and Esophageal Adenocarcinoma
 Clinical imaging / therapy Endoscopic Therapy of Barrett s Esophagus and Esophageal Adenocarcinoma Marcel Tantau, Ofelia Mosteanu, Teodora Pop, Alina Tantau, Gabriela Mester University of Medicine and
Clinical imaging / therapy Endoscopic Therapy of Barrett s Esophagus and Esophageal Adenocarcinoma Marcel Tantau, Ofelia Mosteanu, Teodora Pop, Alina Tantau, Gabriela Mester University of Medicine and
Meta-analysis: the association of oesophageal adenocarcinoma with symptoms of gastro-oesophageal reflux
 Alimentary Pharmacology and Therapeutics Meta-analysis: the association of oesophageal adenocarcinoma with symptoms of gastro-oesophageal reflux J. H. Rubenstein*, & J. B. Taylor à *Veterans Affairs Center
Alimentary Pharmacology and Therapeutics Meta-analysis: the association of oesophageal adenocarcinoma with symptoms of gastro-oesophageal reflux J. H. Rubenstein*, & J. B. Taylor à *Veterans Affairs Center
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, by Am. Coll. of Gastroenterology ISSN /02/$22.00
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, 2002 2002 by Am. Coll. of Gastroenterology ISSN 0002-9270/02/$22.00 Published by Elsevier Science Inc. PII S0002-9270(01)03982-X ORIGINAL CONTRIBUTIONS
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, 2002 2002 by Am. Coll. of Gastroenterology ISSN 0002-9270/02/$22.00 Published by Elsevier Science Inc. PII S0002-9270(01)03982-X ORIGINAL CONTRIBUTIONS
University Mainz. Early Gastric Cancer. Ralf Kiesslich. Johannes Gutenberg University Mainz, Germany. Early Gastric Cancer 15.6.
 Ralf Kiesslich Johannes Gutenberg University Mainz, Germany DIAGNOSIS Unmask lesions - Chromoendoscopy -NBI Red flag technology - Autofluorescence Surface and detail analysis - Magnifying endoscopy - High
Ralf Kiesslich Johannes Gutenberg University Mainz, Germany DIAGNOSIS Unmask lesions - Chromoendoscopy -NBI Red flag technology - Autofluorescence Surface and detail analysis - Magnifying endoscopy - High
A bs tr ac t. n engl j med 365;15 nejm.org october 13,
 The new england journal of medicine established in 1812 october 13, 2011 vol. 365 no. 15 Incidence of Adenocarcinoma among Patients with Barrett s Esophagus Frederik Hvid-Jensen, M.D., Lars Pedersen, Ph.D.,
The new england journal of medicine established in 1812 october 13, 2011 vol. 365 no. 15 Incidence of Adenocarcinoma among Patients with Barrett s Esophagus Frederik Hvid-Jensen, M.D., Lars Pedersen, Ph.D.,
Opinion Statement. Esophagus (E Dellon, Section Editor)
 Curr Treat Options Gastro (2016) 14:1 18 DOI 10.1007/s11938-016-0080-4 Esophagus (E Dellon, Section Editor) Current Controversies in Radiofrequency Ablation Therapy for Barrett s Esophagus Kamar Belghazi,
Curr Treat Options Gastro (2016) 14:1 18 DOI 10.1007/s11938-016-0080-4 Esophagus (E Dellon, Section Editor) Current Controversies in Radiofrequency Ablation Therapy for Barrett s Esophagus Kamar Belghazi,
Barrett s Esophagus: State of the Art. Food Getting Stuck
 Barrett s Esophagus: State of the Art Nicholas J. Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina SOM Food Getting Stuck 73-year-old retired Wilmington police
Barrett s Esophagus: State of the Art Nicholas J. Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina SOM Food Getting Stuck 73-year-old retired Wilmington police
ESOPHAGEAL CANCER. Epidemiology 3/22/2017. Esophageal Carcinoma: subtypes. Esophageal Adenocarcinoma (EAC) Epidemiology.
 ESOPHAGEAL CANCER Disclosures Sushil Ahlawat, MD, FACP, FASGE, AGAF Associate Professor of Medicine Director of Endoscopy RUTGERS NJMS Nothing to disclose. Esophageal Carcinoma: subtypes Subtype Squamous
ESOPHAGEAL CANCER Disclosures Sushil Ahlawat, MD, FACP, FASGE, AGAF Associate Professor of Medicine Director of Endoscopy RUTGERS NJMS Nothing to disclose. Esophageal Carcinoma: subtypes Subtype Squamous
Long-term recurrence of neoplasia and Barrett s epithelium after complete endoscopic resection
 Editor s choice Scan to access more free content For numbered affiliations see end of article. Correspondence to Professor Thomas Rösch, Department of Interdisciplinary Endoscopy, University Hospital Hamburg-Eppendorf,
Editor s choice Scan to access more free content For numbered affiliations see end of article. Correspondence to Professor Thomas Rösch, Department of Interdisciplinary Endoscopy, University Hospital Hamburg-Eppendorf,
Frequency of Barrett Esophagus in Patients with Symptoms of Gastroesophageal Reflux Disease
 Original Article Frequency of Barrett Esophagus in Patients with Symptoms of Gastroesophageal Reflux Disease From Military Hospital, Rawalpindi Obaid Ullah Khan, Abdul Rasheed Correspondence: Dr. Abdul
Original Article Frequency of Barrett Esophagus in Patients with Symptoms of Gastroesophageal Reflux Disease From Military Hospital, Rawalpindi Obaid Ullah Khan, Abdul Rasheed Correspondence: Dr. Abdul
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong
 Application of Chromoendoscopy, NBI and AFI in Esophagus why, who, and how? Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong Cancer of
Application of Chromoendoscopy, NBI and AFI in Esophagus why, who, and how? Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong Cancer of
Long-term recurrence of neoplasia and Barrett s epithelium after complete endoscopic resection
 Editor s choice Scan to access more free content ORIGINAL ARTICLE Long-term recurrence of neoplasia and Barrett s epithelium after complete endoscopic resection Mario Anders, 1 Christina Bähr, 1 Muhammad
Editor s choice Scan to access more free content ORIGINAL ARTICLE Long-term recurrence of neoplasia and Barrett s epithelium after complete endoscopic resection Mario Anders, 1 Christina Bähr, 1 Muhammad
Radiofrequency Ablation: Stepwise circumferential and focal RFA of Barrett s s esophagus using the HALO System
 Radiofrequency Ablation: Stepwise circumferential and focal RFA of Barrett s s esophagus using the HALO System Used abbreviations BE: Barrett s esophagus EC: Early cancer ER: Endoscopic resection HGD:
Radiofrequency Ablation: Stepwise circumferential and focal RFA of Barrett s s esophagus using the HALO System Used abbreviations BE: Barrett s esophagus EC: Early cancer ER: Endoscopic resection HGD:
What Is Barrett s Esophagus?
 What Is Barrett s Esophagus? Having Barrett s esophagus means the cells lining the esophagus (the tube that links the mouth and the stomach) have changed into types of intestinal cells that are not normal
What Is Barrett s Esophagus? Having Barrett s esophagus means the cells lining the esophagus (the tube that links the mouth and the stomach) have changed into types of intestinal cells that are not normal
Hiatal Hernias and Barrett s esophagus. Dr Sajida Ahad Mercy General Surgery
 Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Endoscopic resection (ER) is becoming increasingly established ALIMENTARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:630 635 ALIMENTARY TRACT Efficacy, Safety, and Long-term Results of Endoscopic Treatment for Early Stage Adenocarcinoma of the Esophagus With Low-risk sm1
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:630 635 ALIMENTARY TRACT Efficacy, Safety, and Long-term Results of Endoscopic Treatment for Early Stage Adenocarcinoma of the Esophagus With Low-risk sm1
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia
 National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
Vital staining and Barrett s esophagus
 Marcia Irene Canto, MD, MHS Baltimore, Maryland Vital staining or chromoendoscopy refers to staining of endoscopic tissue or topical application of chemical stains or pigments to alter tissue appearances
Marcia Irene Canto, MD, MHS Baltimore, Maryland Vital staining or chromoendoscopy refers to staining of endoscopic tissue or topical application of chemical stains or pigments to alter tissue appearances
Nonsurgical Management of Esophageal Cancer
 8 Nonsurgical Management of Esophageal Cancer Malek M. Safa and Hassan K. Reda Dayton Cancer Center, Dayton, Ohio and University of Kentucky, Lexington, Kentucky, USA 1. Introduction In the recent past,
8 Nonsurgical Management of Esophageal Cancer Malek M. Safa and Hassan K. Reda Dayton Cancer Center, Dayton, Ohio and University of Kentucky, Lexington, Kentucky, USA 1. Introduction In the recent past,
Proton Pump Inhibitors Are Associated with Reduced Incidence of Dysplasia in Barrett s Esophagus
 American Journal of Gastroenterology ISSN 0002-9270 C 2004 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2004.30228.x Published by Blackwell Publishing ORIGINAL CONTRIBUTIONS Proton Pump Inhibitors
American Journal of Gastroenterology ISSN 0002-9270 C 2004 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2004.30228.x Published by Blackwell Publishing ORIGINAL CONTRIBUTIONS Proton Pump Inhibitors
Advances in endoscopic resection and radiofrequency ablation of early esophageal neoplasia van Vilsteren, F.G.I.
 UvA-DARE (Digital Academic Repository) Advances in endoscopic resection and radiofrequency ablation of early esophageal neoplasia van Vilsteren, F.G.I. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Advances in endoscopic resection and radiofrequency ablation of early esophageal neoplasia van Vilsteren, F.G.I. Link to publication Citation for published version
Extensive (8 to 12 cm 2 ) Noncircumferential Endoscopic Mucosal Resection for Early Esophageal Cancer
 SECTION V: ESOPHAGUS MALIGNANT Extensive (8 to 12 cm 2 ) Noncircumferential Endoscopic Mucosal Resection for Early Esophageal Cancer Philippe Monnier, MD, Yves Jaquet, MD, Alexandre Radu, MD, Raphaelle
SECTION V: ESOPHAGUS MALIGNANT Extensive (8 to 12 cm 2 ) Noncircumferential Endoscopic Mucosal Resection for Early Esophageal Cancer Philippe Monnier, MD, Yves Jaquet, MD, Alexandre Radu, MD, Raphaelle
Gastrointestinal Imaging
 Endoscopic Imaging of Gastroesophageal Reflux Disease Kerry B Dunbar, MD Assistant Professor of Medicine, Division of Gastroenterology and Hepatology, Johns Hopkins University School of Medicine Abstract
Endoscopic Imaging of Gastroesophageal Reflux Disease Kerry B Dunbar, MD Assistant Professor of Medicine, Division of Gastroenterology and Hepatology, Johns Hopkins University School of Medicine Abstract
Barrett s esophagus (BE), a known complication of chronic
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:220 227 Patients With Nondysplastic Barrett s Esophagus Have Low Risks for Developing Dysplasia or Esophageal Adenocarcinoma SACHIN WANI,* GARY FALK, MATTHEW
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:220 227 Patients With Nondysplastic Barrett s Esophagus Have Low Risks for Developing Dysplasia or Esophageal Adenocarcinoma SACHIN WANI,* GARY FALK, MATTHEW
How to characterize dysplastic lesions in IBD?
 How to characterize dysplastic lesions in IBD? Name: Institution: Helmut Neumann, MD, PhD, FASGE University Medical Center Mainz What do we know? Patients with IBD carry an increased risk of developing
How to characterize dysplastic lesions in IBD? Name: Institution: Helmut Neumann, MD, PhD, FASGE University Medical Center Mainz What do we know? Patients with IBD carry an increased risk of developing
The incidence of esophageal adenocarcinoma is rising in the ENDOSCOPY CORNER
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:843 847 ENDOSCOPY CORNER Acetic Acid Spray Is an Effective Tool for the Endoscopic Detection of Neoplasia in Patients With Barrett s Esophagus GAIUS LONGCROFT
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:843 847 ENDOSCOPY CORNER Acetic Acid Spray Is an Effective Tool for the Endoscopic Detection of Neoplasia in Patients With Barrett s Esophagus GAIUS LONGCROFT
Quiz Adenocarcinoma of the distal stomach has been increasing in the last 20 years. a. True b. False
 Quiz 1 1. Which of the following are risk factors for esophagus cancer. a. Obesity b. Gastroesophageal reflux c. Smoking and Alcohol d. All of the above 2. Adenocarcinoma of the distal stomach has been
Quiz 1 1. Which of the following are risk factors for esophagus cancer. a. Obesity b. Gastroesophageal reflux c. Smoking and Alcohol d. All of the above 2. Adenocarcinoma of the distal stomach has been
EMR is not inferior to ESD for early Barrett s and EGJ neoplasia: An extensive review on outcome, recurrence and complication rates
 E58 EMR is not inferior to ESD for early Barrett s and EGJ neoplasia: An extensive review on outcome, recurrence and complication rates Authors Institution Yoriaki Komeda, Marco Bruno, Arjun Koch Department
E58 EMR is not inferior to ESD for early Barrett s and EGJ neoplasia: An extensive review on outcome, recurrence and complication rates Authors Institution Yoriaki Komeda, Marco Bruno, Arjun Koch Department
Endoscopic Submucosal Dissection ESD
 Endoscopic Submucosal Dissection ESD Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated
Endoscopic Submucosal Dissection ESD Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated
