The New England Journal of Medicine
|
|
|
- Beverly Gardner
- 5 years ago
- Views:
Transcription
1 The New England Journal of Medicine Copyright 2001 by the Massachusetts Medical Society VOLUME 345 D ECEMBER 6, 2001 NUMBER 23 NEPHRECTOMY FOLLOWED BY ALFA-2b COMPARED WITH ALFA-2b FOR METASTATIC RENAL-CELL CANCER ROBERT C. FLANIGAN, M.D., SYDNEY E. SALMON, M.D., BRENT A. BLUMENSTEIN, PH.D., SCOTT I. BEARMAN, M.D., VIVEK ROY, M.D., PATRICK C. MCGRATH, M.D., JOHN R. CATON, JR., M.D., NIKHIL MUNSHI, M.D., AND E. DAVID CRAWFORD, M.D. ABSTRACT Background The value of nephrectomy in metastatic renal-cell cancer has long been debated. Several nonrandomized studies suggest a higher rate of response to systemic therapy and longer survival in patients who have undergone nephrectomy. Methods We randomly assigned patients with metastatic renal-cell cancer who were acceptable candidates for nephrectomy to undergo radical nephrectomy followed by therapy with interferon alfa-2b or to receive interferon alfa-2b therapy alone. The primary end point was survival, and the secondary end point was a response of the tumor to treatment. Results The median survival of 120 eligible patients assigned to surgery followed by interferon was 11.1 months, and among the 121 eligible patients assigned to interferon alone it was 8.1 months (P=0.05). The difference in median survival between the two groups was independent of performance status, metastatic site, and the presence or absence of a measurable metastatic lesion. Conclusions Nephrectomy followed by interferon therapy results in longer survival among patients with metastatic renal-cell cancer than does interferon therapy alone. (N Engl J Med 2001;345: ) Copyright 2001 Massachusetts Medical Society. IT is unknown whether removal of the primary tumor (cytoreductive surgery) is beneficial in metastatic renal-cell cancer. 1-6 The disease has a poor prognosis and resists conventional chemotherapy, but spontaneous regression occasionally occurs. 7 For these reasons, aggressive surgery has been advocated, especially when solitary or resectable metastatic lesions are present or in patients with a primary tumor in situ whose metastases have responded to interleukin-2. 8,9 Nevertheless, no study has clearly demonstrated that nephrectomy is advantageous in metastatic renal-cell cancer. 5,6 There are indications that patients with metastatic renal-cell cancer who are treated with interferon alfa or other cytokines have improved outcomes if they first undergo nephrectomy. 10,11 Patients who undergo nephrectomy followed by immunotherapy with interleukin-2, with or without tumor-infiltrating lymphocytes, also survive longer than historical controls However, none of the reports were studies based on prospective, controlled trials. In 1989, the Southwest Oncology Group (SWOG) initiated a study to determine whether nephrectomy affects survival in metastatic renal-cell cancer. We report the results of this randomized trial. Study Patients METHODS Eligible patients had a histologically confirmed diagnosis of metastatic renal-cell carcinoma in tissue obtained by needle biopsy or needle aspiration of at least one measurable lesion or the primary tumor and had metastases beyond the regional lymphatics; that is, metastatic disease involving a tumor of any size and any nodal status. The primary tumor was considered amenable to surgical extirpation by the attending surgeon. Patients with thrombosis of the inferior vena cava below the hepatic veins were not excluded. A performance status of 0 or 1 according to the SWOG criteria was required, and patients were excluded if they had received prior treatment with chemotherapy, hormonal therapy, interferon, interleukin-2, lymphocyte-activated killer cells, or other biologic-response modifiers. In addition, prior or concomitant radiation therapy to the primary tumor or to metastatic sites was not allowed. A serum bilirubin level no higher than three times the upper limit of the normal value at the institution and a serum creatinine level of no more From the Loyola University Stritch School of Medicine, Maywood, Ill. (R.C.F.); the University of Arizona Cancer Center, Tucson (S.E.S.); the Southwest Oncology Group Statistical Center, Seattle (B.A.B.); the University of Colorado, Denver (S.I.B., E.D.C.); the University of Oklahoma Health Science Center, Oklahoma City (V.R.); the University of Kentucky Medical Center, Lexington (P.C.M.); Brook Army Medical Center Wilford Hall Medical Center, San Antonio, Tex. (J.R.C.); and the University of Arkansas for Medical Sciences, Little Rock (N.M.). Address reprint requests to the Southwest Oncology Group (SWOG-8949), Operations Office, Omicron Dr., San Antonio, TX , or at rflanig@luc.edu. N Engl J Med, Vol. 345, No. 23 December 6,
2 than 3.0 mg per deciliter (265 µmol per liter) were required. Patients with uncontrolled cardiac arrhythmias were not eligible. Patients who had previously had cancer were also excluded unless they had been free of cancer for at least five years or unless their cancer was adequately treated basal-cell skin cancer, squamous-cell skin cancer, or in situ cervical cancer. All patients provided written informed consent, and the trial was approved by the institutional review board at each institution. Assessment and Treatment Before randomization, patients were stratified according to SWOG performance status (0 vs. 1), the presence or absence of lung metastases only, and the presence or absence of at least one measurable metastatic lesion in the region not to be resected. The patients were randomly assigned by a central computer to one of the two groups with dynamic balancing based on the stratification factors. 16 The patients either underwent immediate radical nephrectomy followed by therapy with interferon alfa-2b (Intron-A, Schering- Plough, Kenilworth, N.J.) (surgery-plus-interferon group) or were given immediate interferon alfa-2b therapy without surgery (interferon-only group). The dosages of subcutaneous interferon alfa-2b were as follows. Induction therapy was begun at 1.25 million IU per square meter of body-surface area, with escalation to a starting dose of 5 million IU per square meter on the first day of treatment (1.25 million IU per square meter three days before, 2.5 million IU per square meter two days before, and 3.75 million IU per square meter the day before treatment). Interferon was to be continued at a dose of 5 million IU per square meter each Monday, Wednesday, and Friday until progression of the tumor was detected. On each day of treatment, the dosage was modified if any toxic effects were observed, and the modified dosage was continued until resolution of the toxic effects. In the case of two or more toxic effects in the same category, dosage modification was based on the highest-grade toxic effect observed. The toxic effects specifically monitored included hematologic, hepatic, and gastrointestinal effects (e.g., diarrhea and anorexia) and hypotension. Radical nephrectomy was performed through a transabdominal, flank, or thoracoabdominal approach. It was defined as the excision of the tumor outside Gerota s fascia, with early ligation of the renal artery and vein. The surgery was performed within four weeks of enrollment. The limits of lymphadenectomy were not defined. The surgeon noted whether grossly involved lymph nodes were left unresected at the time of nephrectomy. Responses to treatment (a complete response, a partial response, a stable condition, progression, and an unconfirmed response) were defined according to the criteria of the SWOG. 17 Statistical Analysis The trial was planned with survival as the primary end point, a one-sided probability of a type I error of 0.05, and a power of 0.85, and it was based on the assumptions that the median survival would be one year in the interferon-only group and that survival in the surgery-plus-interferon group would be 33 percent lower (hazard ratio for survival, 0.67). A one-sided null hypothesis was used to plan the study, because an additional clinical question was addressed: Is there a benefit to nephrectomy before systemic therapy? We calculated that the trial would require 244 patients enrolled over a period of three years, with one year of follow-up. Two formal interim analyses were planned and were performed without interruption of the trial. This article reports the final analysis of the trial. The criterion we used for significance with respect to the primary end point was P= 0.04 (one-sided, with adjustment for the interim analyses). Although the design and monitoring of this trial were based on a one-sided null hypothesis, two-sided P values are reported throughout so as to conform to the Journal s policy of reporting only twosided P values. The primary analysis concerns survival among eligible patients in the two groups. Eligibility was based only on data collected before randomization. The planned primary analysis was performed with the stratified log-rank test (one-sided), with use of the stratification factors identified above. 18 The analyses in this article are based on data obtained through March RESULTS Between June 1991 and October 1998, 246 patients from 80 participating institutions were randomly assigned to two groups of 123 each. Five patients were found to be ineligible because the pathological diagnosis had been incorrect (three in the surgeryplus-interferon group and two in the interferon-only group). For an additional 16 patients (8 in the surgeryplus-interferon group and 8 in the interferon-only group), the data were insufficient for the determination of eligibility; data from these 16 patients were included in the analysis, but the data on the 5 patients who did not have renal-cell cancer were excluded. Table 1 shows relevant characteristics of the patients at the time of enrollment. There were no significant imbalances except with respect to performance status (P=0.04). Of the 120 patients in the surgery-plus-interferon group, 17 did not undergo the planned surgery: 7 refused, 5 were found to be medically ineligible for surgery, 3 had unresectable primary tumors, and 2 died before surgery could be performed. Ninety-eight patients were evaluated for complications of nephrectomy. One patient with an unresectable tumor died of wound dehiscence and intraabdominal abscess with peritonitis; two patients had cardiac ischemia or infarction, two had postoperative infections, and one had hypotension. Sixteen patients had only mild-to-moderate complications. No surgical complications were reported in 76 of the 98 patients. The mean duration of hospitalization for nephrectomy was 8.2 days (range, 3 to 22). The mean time to the initiation of interferon alfa-2b therapy in patients who underwent nephrectomy was 19.9 days. Two eligible patients, one in each group, declined interferon therapy. Two hundred ten patients were evaluated for toxic effects of interferon. One patient in the interferon-only group died of myocardial infarction attributed to interferon. Twenty-three patients (10 in the surgery-plus-interferon group and 13 in the interferon-only group) had severe complications due to interferon. Among the 92 patients in the surgery-plus-interferon group whose responses could be evaluated and who had a measurable lesion at base line, three partial responses were reported (3.3 percent; 95 percent confidence interval, 1 to 9 percent), and among the 83 comparable patients in the interferon-only group, three responses were reported (one complete, one partial, and one unconfirmed; 3.6 percent; 95 percent confidence interval, 1 to 10 percent). Of the 175 patients with a measurable lesion at base line, 65 (37 percent) had inadequate data for assessment of the response, 1656 N Engl J Med, Vol. 345, No. 23 December 6,
3 NEPHREC ALFA-2b VERSUS ALFA-2b FOR RENAL-CELL CANCER TABLE 1. CHARACTERISTICS OF THE 241 ELIGIBLE PATIENTS. CHARACTERISTIC (N=121) (N=120) Age (yr) Mean Range Male sex (%) Measurable metastatic lesion (%) Performance status 1 (%)* Only lung metastases (%) *Performance was scored as 0 or 1, with 1 indicating decreased activity. P=0.04 for the comparison with the interferononly group. and they were assumed not to have had a response. There were no differences between the two groups with respect to the proportion with a response to interferon alfa-2b. The response rates in both groups in this study were lower than those generally reported. 19,20 The most likely explanation for this difference is that the SWOG criteria for a response are more rigorous than the criteria generally used. 17 At the time of our analysis of the study data, only 20 of the 241 eligible patients were alive, with a median follow-up of 368 days. Table 2 shows the estimated median survival times, the Kaplan Meier estimates of survival at one year, and the one-sided P values (derived by the log-rank test) according to group and stratification factors. Figure 1 shows actuarial survival in the two groups. The primary analysis, based on the stratified logrank test, found a significant advantage associated with nephrectomy (P=0.05) (Table 2), with two-sided P values. The median overall survival was 8.1 months in the interferon-only group (95 percent confidence interval, 5.4 to 9.5) and 11.1 months in the surgeryplus-interferon group (95 percent confidence interval, 9.2 to 16.5). The survival advantage associated with nephrectomy was evident in subgroups defined according to all three stratification factors (Table 2). The imbalance with respect to performance status at randomization (Table 1) could explain the overall difference in survival, since patients with a performance status of 1 (those with a worse prognosis) were overrepresented in the interferon-only group. However, the differences in median survival favor the surgery-plus-interferon group among patients with each performance status: 17.4 and 11.7 months for performance status 0 in the surgery-plusinterferon and interferon-only groups, respectively, and 6.9 and 4.8 months for performance status 1. In a proportional-hazards regression model that included treatment group, performance status, and the interaction between treatment group and performance status, the interaction term was not significant an indication that the imbalance did not explain the primary result. DISCUSSION This study provides evidence that nephrectomy before interferon alfa-2b therapy for metastatic renal-cell cancer confers a survival benefit. Metastatic renal-cell cancer is very difficult to treat effectively, because of its unpredictable behavior and resistance to chemotherapy. Yagoda et al. reviewed a large series of trials of chemotherapeutic regimens and found a 5.6 percent TABLE 2. SURVIVAL IN SUBGROUPS DEFINED ACCORDING TO STRATIFICATION FACTORS. CATEGORY MEDIAN SURVIVAL 1-YR SURVIVAL P VALUE* mo % Not stratified Stratification factor Measurable disease Yes No Performance status Type of metastases Lung only Other *P values for the comparison of median survival between groups were derived with the log-rank test. Performance was scored as 0 or 1, with 1 indicating decreased activity. N Engl J Med, Vol. 345, No. 23 December 6,
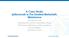
4 Survival (%) Nephrectomy plus interferon 20 Interferon alone Months NO. AT RISK Interferon alone Nephrectomy plus interferon Figure 1. Actuarial Survival among All Eligible Patients, According to Treatment-Group Assignment. In the interferon-only group, there were 115 deaths and median survival was 8.1 months. In the surgeryplus-interferon group, there were 106 deaths and median survival was 11.1 months. rate of objective response to cytotoxic agents in 3502 adequately treated patients. 21 There are, however, indications of improved survival with chemotherapy after nephrectomy. 22 Moreover, previous trials of biologic-response modifiers in metastatic renal-cell cancer have consistently shown an improved response rate or improved survival after removal of the primary tumor. 2,12,23,24 The interval from nephrectomy to the systemic treatment of the renal-cell cancer was not controlled in these series, thus raising the question whether nephrectomy had a biologic effect or whether patients selected for nephrectomy had tumors that would probably respond to systemic treatment. The effect of nephrectomy may, however, be real. Several reports of immunotherapy for renal-cell cancer, with or without concomitant chemotherapy, have supported the idea that patients who undergo nephrectomy before systemic treatment have a survival advantage. 14,25,26 Recently, the combination of nephrectomy, tumorinfiltrating lymphocytes, and cytokine therapy in metastatic renal-cell cancer has yielded a response rate of 33.9 percent (12.5 percent complete responses and 21.4 percent partial responses) 11 and two-year and three-year survival rates of 40 percent and 31 percent, respectively, among patients treated in this aggressive manner. 15 Why nephrectomy before systemic therapy might be effective is unknown. A recent study by Fujikawa et al. suggests that only patients with elevated serum C-reactive protein levels may benefit from cytoreduction by nephrectomy. 13 One argument against the use of nephrectomy before therapy with a biologic-response modifier has been the high operative morbidity and mortality rate. Although earlier series reported mortality rates of 6 to 11 percent, 27,28 there was only one operative death in our study (less than 1.0 percent), and the rate of severe complications with surgery in our trial (4.9 percent; five patients) compares favorably with rates in other studies. 11 Furthermore, there is no evidence that nephrectomy delayed systemic treatment in a way that would offset the survival benefit associated with the surgery (mean hospitalization time, 8.2 days; mean time to initiation of interferon alfa-2b therapy, 19.9 days). We believe that nephrectomy in suitable patients should be an eligibility criterion in trials of new systemic agents for the treatment of metastatic renal-cell cancer. We also believe that nephrectomy followed by therapy with interferon alfa-2b (with or without other cytokines) should be considered the standard of care (i.e., should be used in the control group) in future phase 3 trials. Supported in part by Public Health Service Cooperative Agreements from the National Cancer Institute (CA38926, CA32102, CA46282, CA13612, CA42777, CA58686, CA04920, CA46136, CA76447, CA37981, CA46113, CA16385, CA58416, CA22433, CA35128, CA14028, CA35261, CA12644, CA74647, CA04919, CA35090, CA27057, CA58882, CA35431, 1658 N Engl J Med, Vol. 345, No. 23 December 6,
5 NEPHREC ALFA-2b VERSUS ALFA-2b FOR RENAL-CELL CANCER CA35176, CA35281, CA35119, CA58861, CA45450, CA45461, CA52654, CA76132, CA76448, CA46441, CA45560, CA20319, CA63850, CA76462, CA35192, and CA63845). REFERENCES 1. Flanigan RC. The failure of infarction and/or nephrectomy in stage IV renal cell cancer to influence survival or metastatic regression. Urol Clin North Am 1987;14: DeKernion JB. Treatment of advanced renal cell carcinoma traditional methods and innovative approaches. J Urol 1983;130: Garfield DH, Kennedy BJ. Regression of metastatic renal cell carcinoma following nephrectomy. Cancer 1972;30: Johnson DE, Kaesler KE, Samuels ML. Is nephrectomy justified in patients with metastatic renal cell carcinoma? J Urol 1975;114: Fuselier HA Jr, Guice SL III, Brannan W, et al. Renal cell carcinoma: the Ochsner Medical Institution experience ( ). J Urol 1983; 130: Middleton RG. Surgery for metastatic renal cell carcinoma. J Urol 1967; 97: Nishiyama K, Shirahama T, Yoshimura A, et al. Expression of the multidrug transporter, P-glycoprotein, in renal and transitional cell carcinomas. Cancer 1993;71: Tykka H. Active specific immunotherapy with supportive measures in the treatment of advanced palliatively nephrectomised renal adenocarcinoma: a controlled clinical study. Scand J Urol Nephrol Suppl 1981;63: Tanguay S, Swanson DA, Putnam JB Jr. Renal cell carcinoma metastatic to the lung: potential benefit in the combination of biological therapy and surgery. J Urol 1996;156: Walther MM, Yang JC, Pass HI, Linehan WM, Rosenberg SA. Cytoreductive surgery before high dose interleukin-2 based therapy in patients with metastatic renal cell carcinoma. J Urol 1997;158: Franklin JR, Figlin R, Rauch J, Gitlitz B, Belldegrun A. Cytoreductive surgery in the management of metastatic renal cell carcinoma: the UCLA experience. Semin Urol Oncol 1996;14: Mani S, Todd MB, Katz K, Poo WJ. Prognostic factors for survival in patients with metastatic renal cancer treated with biological response modifiers. J Urol 1995;154: Fujikawa K, Matsui Y, Miura K, et al. Serum immunosuppressive acidic protein and natural killer cell activity in patients with metastatic renal cell carcinoma before and after nephrectomy. J Urol 2000;164: Robertson CN, Linehan WM, Pass HI, et al. Preparative cytoreductive surgery in patients with metastatic renal cell carcinoma treated with adoptive immunotherapy with interleukin-2 or interleukin-2 plus lymphokine activated killer cells. J Urol 1990;144: Figlin RA, Thompson JA, Bukowski RM, et al. Multicenter, randomized, phase III trial of CD8(+) tumor-infiltrating lymphocytes in combination with recombinant interleukin-2 in metastatic renal cell carcinoma. J Clin Oncol 1999;17: Pocock SJ, Simon R. Sequential treatment assignment with balancing for prognostic factors in the controlled clinical trial. Biometrics 1975;31: Green S, Weiss GR. Southwest Oncology Group standard response criteria, endpoint definitions and toxicity criteria. Invest New Drugs 1992; 10: Cox DR, Oakes D. Analysis of survival data. London: Chapman & Hall, Flanigan RC. Advances in immunotherapy and chemotherapy for renal cell carcinoma. In: Rous SN, ed. Urology annual. Vol. 11. Malden, Mass.: Blackwell Science, 1997: Krown SE. Interferon treatment of renal cell carcinoma: current status and future prospects. Cancer 1987;59:Suppl: Yagoda A, Petrylak D, Thompson S. Cytotoxic chemotherapy for advanced renal cell carcinoma. Urol Clin North Am 1993;20: Marshall ME, Goodman P, Kuebler P, Flanigan R, Crawford D. Prognostic factors in patients with advanced renal cell carcinoma (RCC): the Southwest Oncology Group experience. Prog Proc Am Soc Clin Oncol 1992;11:206. abstract. 23. Flanigan RC. Role of surgery in patients with metastatic renal cell carcinoma. Semin Urol Oncol 1996;14: Muss HB, Costanzi JJ, Leavitt R, et al. Recombinant alfa interferon in renal cell carcinoma: a randomized trial of two routes of administration. J Clin Oncol 1987;5: Fisher RI, Coltman CA Jr, Doroshow JH, et al. Metastatic renal cancer treated with interleukin-2 and lymphokine-activated killer cells: a phase II clinical trial. Ann Intern Med 1988;108: Franklin JR, Figlin R, Ranch J, Gitlitz B, Belldegrun A. Cytoreductive surgery in the management of metastatic renal cell carcinoma: the UCLA experience. Semin Urol Oncol 1996;14: Neidhart JA, Murphy SG, Hennick LA, Wise HA. Active specific immunotherapy of stage IV renal carcinoma with aggregated tumor antigen adjuvant. Cancer 1980;46: Fowler JE Jr. Failure of immunotherapy for metastatic renal cell carcinoma. J Urol 1986;135:22-5. Copyright 2001 Massachusetts Medical Society. N Engl J Med, Vol. 345, No. 23 December 6,
Neoadjuvant Chemotherapy plus Cystectomy Compared with Cystectomy Alone for Locally Advanced Bladder Cancer
 The new england journal of medicine original article Neoadjuvant Chemotherapy plus Cystectomy Compared with Cystectomy Alone for Locally Advanced Bladder Cancer H. Barton Grossman, M.D., Ronald B. Natale,
The new england journal of medicine original article Neoadjuvant Chemotherapy plus Cystectomy Compared with Cystectomy Alone for Locally Advanced Bladder Cancer H. Barton Grossman, M.D., Ronald B. Natale,
The role of cytoreductive. nephrectomy in elderly patients. with metastatic renal cell. carcinoma in an era of targeted. therapy
 The role of cytoreductive nephrectomy in elderly patients with metastatic renal cell carcinoma in an era of targeted therapy Dipesh Uprety, MD Amir Bista, MD Yazhini Vallatharasu, MD Angela Smith, MA David
The role of cytoreductive nephrectomy in elderly patients with metastatic renal cell carcinoma in an era of targeted therapy Dipesh Uprety, MD Amir Bista, MD Yazhini Vallatharasu, MD Angela Smith, MA David
CLINICAL INVESTIGATION of new agents and combination
 Interferon-Alfa as a Comparative Treatment for Clinical Trials of New Therapies Against Advanced Renal Cell Carcinoma By Robert J. Motzer, Jennifer Bacik, Barbara A. Murphy, Paul Russo, and Madhu Mazumdar
Interferon-Alfa as a Comparative Treatment for Clinical Trials of New Therapies Against Advanced Renal Cell Carcinoma By Robert J. Motzer, Jennifer Bacik, Barbara A. Murphy, Paul Russo, and Madhu Mazumdar
The New England Journal of Medicine COMPARISON OF FOUR CHEMOTHERAPY REGIMENS FOR ADVANCED NON SMALL-CELL LUNG CANCER
 COMPARISON OF FOUR CHEMOTHERAPY REGIMENS FOR ADVANCED NON SMALL-CELL LUNG CANCER JOAN H. SCHILLER, M.D., DAVID HARRINGTON, PH.D., CHANDRA P. BELANI, M.D., COREY LANGER, M.D., ALAN SANDLER, M.D., JAMES
COMPARISON OF FOUR CHEMOTHERAPY REGIMENS FOR ADVANCED NON SMALL-CELL LUNG CANCER JOAN H. SCHILLER, M.D., DAVID HARRINGTON, PH.D., CHANDRA P. BELANI, M.D., COREY LANGER, M.D., ALAN SANDLER, M.D., JAMES
After primary tumor treatment, 30% of patients with malignant
 ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
Marshall T Bell Research Resident University of Colorado Grand Rounds Nov. 21, 2011
 Marshall T Bell Research Resident University of Colorado Grand Rounds Nov. 21, 2011 Most common form of cancer in adults ages 25-29 3-5% of skin cancers but 65-75% of deaths Most common metastasis to small
Marshall T Bell Research Resident University of Colorado Grand Rounds Nov. 21, 2011 Most common form of cancer in adults ages 25-29 3-5% of skin cancers but 65-75% of deaths Most common metastasis to small
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches
 Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
A Case Study: Ipilimumab in Pre-treated Metastatic Melanoma
 A Case Study: Ipilimumab in Pre-treated Metastatic Melanoma Tai-Tsang Chen, PhD Global Biometric Sciences, Bristol-Myers Squibb EFSPI Statistical Meeting on Evidence Synthesis Brussels, Belgium November
A Case Study: Ipilimumab in Pre-treated Metastatic Melanoma Tai-Tsang Chen, PhD Global Biometric Sciences, Bristol-Myers Squibb EFSPI Statistical Meeting on Evidence Synthesis Brussels, Belgium November
trial update clinical
 trial update clinical by John W. Mucenski, BS, PharmD, Director of Pharmacy Operations, UPMC Cancer Centers The treatment outcome for patients with relapsed or refractory cervical carcinoma remains dismal.
trial update clinical by John W. Mucenski, BS, PharmD, Director of Pharmacy Operations, UPMC Cancer Centers The treatment outcome for patients with relapsed or refractory cervical carcinoma remains dismal.
Copyright, 1995, by the Massachusetts Medical Society
 Copyright, 99, by the Massachusetts Medical Society Volume 332 APRIL 6, 99 Number ADJUVANT CYCLOPHOSPHAMIDE, METHOTREXATE, AND FLUOROURACIL IN NODE- POSITIVE BREAST CANCER The Results of Years of Follow-up
Copyright, 99, by the Massachusetts Medical Society Volume 332 APRIL 6, 99 Number ADJUVANT CYCLOPHOSPHAMIDE, METHOTREXATE, AND FLUOROURACIL IN NODE- POSITIVE BREAST CANCER The Results of Years of Follow-up
Multidisciplinary approach for renal cell carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute
 Multidisciplinary approach for renal cell carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute 20 April, Antalya, Turkey RCC European Union 60.000 new diagnoses/year 26.000 Cancer related deaths
Multidisciplinary approach for renal cell carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute 20 April, Antalya, Turkey RCC European Union 60.000 new diagnoses/year 26.000 Cancer related deaths
Winship Cancer Institute of Emory University Neoadjuvant Systemic Therapy in Metastatic Renal Cell Carcinoma Patients
 Winship Cancer Institute of Emory University Neoadjuvant Systemic Therapy in Metastatic Renal Cell Carcinoma Patients Bradley Carthon, MD, PhD Assistant Professor, Genitourinary Medical Oncology Winship
Winship Cancer Institute of Emory University Neoadjuvant Systemic Therapy in Metastatic Renal Cell Carcinoma Patients Bradley Carthon, MD, PhD Assistant Professor, Genitourinary Medical Oncology Winship
E2804 The BeST Trial
 E2804 The BeST Trial A randomized Phase II Study of VEGF, RAF Kinase and MTOR Combination Targeted Therapy with Bevacizumab, Sorafenib and Temsirolimus in Advanced Renal Cell Carcinoma Investigators Keith
E2804 The BeST Trial A randomized Phase II Study of VEGF, RAF Kinase and MTOR Combination Targeted Therapy with Bevacizumab, Sorafenib and Temsirolimus in Advanced Renal Cell Carcinoma Investigators Keith
DISCLOSURE SLIDE. ARGOS: research funding, scientific advisory board
 INTERIM ANALYSIS OF THE PHASE 3 ADAPT TRIAL EVALUATING ROCAPULDENCEL-T (AGS-003), AN INDIVIDUALIZED IMMUNOTHERAPY FOR THE TREATMENT OF NEWLY-DIAGNOSED PATIENTS WITH METASTATIC RENAL CELL CARCINOMA (MRCC)
INTERIM ANALYSIS OF THE PHASE 3 ADAPT TRIAL EVALUATING ROCAPULDENCEL-T (AGS-003), AN INDIVIDUALIZED IMMUNOTHERAPY FOR THE TREATMENT OF NEWLY-DIAGNOSED PATIENTS WITH METASTATIC RENAL CELL CARCINOMA (MRCC)
ORIGINAL ARTICLE. Clinical Node-Negative Thick Melanoma
 ORIGINAL ARTICLE Clinical Node-Negative Thick Melanoma George I. Salti, MD; Ashwin Kansagra, MD; Michael A. Warso, MD; Salve G. Ronan, MD ; Tapas K. Das Gupta, MD, PhD, DSc Background: Patients with T4
ORIGINAL ARTICLE Clinical Node-Negative Thick Melanoma George I. Salti, MD; Ashwin Kansagra, MD; Michael A. Warso, MD; Salve G. Ronan, MD ; Tapas K. Das Gupta, MD, PhD, DSc Background: Patients with T4
Solitary Contralateral Adrenal Metastases after Nephrectomy for Renal Cell Carcinoma
 Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
Product: Darbepoetin alfa Clinical Study Report: Date: 22 August 2007 Page 2 of 14145
 Date: 22 ugust 2007 Page 2 of 14145 2. SYNOPSIS Name of Sponsor: mgen Inc., Thousand Oaks, C, US Name of Finished Product: ranesp Name of ctive Ingredient: Darbepoetin alfa Title of Study: Randomized,
Date: 22 ugust 2007 Page 2 of 14145 2. SYNOPSIS Name of Sponsor: mgen Inc., Thousand Oaks, C, US Name of Finished Product: ranesp Name of ctive Ingredient: Darbepoetin alfa Title of Study: Randomized,
The right middle lobe is the smallest lobe in the lung, and
 ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
Patient Selection for Surgery in RCC with Thrombus. E. Jason Abel, M.D.
 Patient Selection for Surgery in RCC with Thrombus E. Jason Abel, M.D. RCC with venous invasion Venous invasion occurs in ~10% of RCC Surgery more complex Increased risk for morbidity Thrombus may be confined
Patient Selection for Surgery in RCC with Thrombus E. Jason Abel, M.D. RCC with venous invasion Venous invasion occurs in ~10% of RCC Surgery more complex Increased risk for morbidity Thrombus may be confined
The New England Journal of Medicine BILATERAL ORCHIECTOMY WITH OR WITHOUT FLUTAMIDE FOR METASTATIC PROSTATE CANCER
 BILATERAL ORCHIECTOMY WITH OR WITHOUT FLUTAMIDE FOR METASTATIC PROSTATE CANCER MARIO A. EISENBERGER, M.D., BRENT A. BLUMENSTEIN, PH.D., E. DAVID CRAWFORD, M.D., GARY MILLER, M.D., PH.D., DAVID G. MCLEOD,
BILATERAL ORCHIECTOMY WITH OR WITHOUT FLUTAMIDE FOR METASTATIC PROSTATE CANCER MARIO A. EISENBERGER, M.D., BRENT A. BLUMENSTEIN, PH.D., E. DAVID CRAWFORD, M.D., GARY MILLER, M.D., PH.D., DAVID G. MCLEOD,
Prognostic Factors and Survival after Pulmonary Resection ofmetastaticrenalcellcarcinoma
 European Urology European Urology 48 (2005) 77 82 Kidney Cancer Prognostic Factors and Survival after Pulmonary Resection ofmetastaticrenalcellcarcinoma Hans-Stefan Hofmann*, Heinz Neef, Katharina Krohe,
European Urology European Urology 48 (2005) 77 82 Kidney Cancer Prognostic Factors and Survival after Pulmonary Resection ofmetastaticrenalcellcarcinoma Hans-Stefan Hofmann*, Heinz Neef, Katharina Krohe,
Plattenepithelkarzinom des Ösophagus, 1 st -line
 Plattenepithelkarzinom des Ösophagus, 1 st -line AIO-STO-0309 An open-label, randomized phase III trial of cisplatin and 5-fluorouracil with or without panitumumab for patients with nonresectable, advanced
Plattenepithelkarzinom des Ösophagus, 1 st -line AIO-STO-0309 An open-label, randomized phase III trial of cisplatin and 5-fluorouracil with or without panitumumab for patients with nonresectable, advanced
Lara Kujtan, MD; Abdulraheem Qasem, MD
 The Treatment of Lung Cancer Between 2013-2014 at Truman Medical Center: A Retrospective Review in Fulfillment of the Requirements of Standard 4.6 (Monitoring Compliance with Evidence- Based Guidelines)
The Treatment of Lung Cancer Between 2013-2014 at Truman Medical Center: A Retrospective Review in Fulfillment of the Requirements of Standard 4.6 (Monitoring Compliance with Evidence- Based Guidelines)
When to Integrate Surgery for Metatstatic Urothelial Cancers
 When to Integrate Surgery for Metatstatic Urothelial Cancers Wade J. Sexton, M.D. Senior Member and Professor Department of Genitourinary Oncology Moffitt Cancer Center Case Presentation #1 67 yo male
When to Integrate Surgery for Metatstatic Urothelial Cancers Wade J. Sexton, M.D. Senior Member and Professor Department of Genitourinary Oncology Moffitt Cancer Center Case Presentation #1 67 yo male
Oncologic Applications of Interleukin-2 (Aldesleukin) When Used as Monotherapy. Original Policy Date
 MP 8.01.03 Oncologic Applications of Interleukin-2 (Aldesleukin) When Used as Monotherapy Medical Policy Section Therapy Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with
MP 8.01.03 Oncologic Applications of Interleukin-2 (Aldesleukin) When Used as Monotherapy Medical Policy Section Therapy Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease
 Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Surgery of Renal Cell Carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute
 Surgery of Renal Cell Carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute 23 March 2012, Sao Paulo, Brazil Surgery of RCC Locally confined (small) renal tumours Locally advanced disease Metastatic
Surgery of Renal Cell Carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute 23 March 2012, Sao Paulo, Brazil Surgery of RCC Locally confined (small) renal tumours Locally advanced disease Metastatic
Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis
 ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008
 Special Report Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008 Matthew B. Schabath, PhD, Zachary J. Thompson, PhD,
Special Report Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008 Matthew B. Schabath, PhD, Zachary J. Thompson, PhD,
CANCER UROLOGY VOL. 12. P. S. Borisov 1, M. I. Shkol nik 2, R. V. Orlova 3, P. A. Karlov 1 DOI: /
 CANCER UROLOGY 3 6 VOL. The use of targeted therapies and selection of the optimal treatment sequence in heterogeneous population of patients with metastatic kidney cancer. Results of retrospective study
CANCER UROLOGY 3 6 VOL. The use of targeted therapies and selection of the optimal treatment sequence in heterogeneous population of patients with metastatic kidney cancer. Results of retrospective study
Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer
 - Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
- Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
Cancer Research Group Version Date: November 5, 2015 NCI Update Date: January 15, Schema. L O Step 1 1,2
 Cancer esearch roup ev. 6/14, 2/15, 1/16 Step 2 Schema 5 Arm A: (7 weeks) Step 1 1,2 N Accrual: 515 S Arm S ransoral esection dissections S A N D M Z 4 ntermediate isk 7 Stratify: = 10 pk-yr vs. > 10 pk-yr
Cancer esearch roup ev. 6/14, 2/15, 1/16 Step 2 Schema 5 Arm A: (7 weeks) Step 1 1,2 N Accrual: 515 S Arm S ransoral esection dissections S A N D M Z 4 ntermediate isk 7 Stratify: = 10 pk-yr vs. > 10 pk-yr
Adjuvant Chemotherapy in High Risk Patients after Wertheim Hysterectomy 10-year Survivals
 6 Adjuvant Chemotherapy in High Risk Patients after Wertheim Hysterectomy 0-year Survivals V Sivanesaratnam,*FAMM, FRCOG, FACS Abstract Although the primary operative mortality following radical hysterectomy
6 Adjuvant Chemotherapy in High Risk Patients after Wertheim Hysterectomy 0-year Survivals V Sivanesaratnam,*FAMM, FRCOG, FACS Abstract Although the primary operative mortality following radical hysterectomy
Renal cell cancer: overview and immunochemotherapy
 1 Renal cell cancer: overview and immunochemotherapy Vincent Khoo Introduction and epidemiology Kidney cancer is a relatively common urological cancer, accounting for approximately 2% of all adult cancers.
1 Renal cell cancer: overview and immunochemotherapy Vincent Khoo Introduction and epidemiology Kidney cancer is a relatively common urological cancer, accounting for approximately 2% of all adult cancers.
symposium article introduction symposium article
 Annals of Oncology 17 (Supplement 5): v118 v122, 2006 doi:10.1093/annonc/mdj965 Long-term survival results of a randomized trial comparing gemcitabine/cisplatin and methotrexate/ vinblastine/doxorubicin/cisplatin
Annals of Oncology 17 (Supplement 5): v118 v122, 2006 doi:10.1093/annonc/mdj965 Long-term survival results of a randomized trial comparing gemcitabine/cisplatin and methotrexate/ vinblastine/doxorubicin/cisplatin
Successful Treatment of Renal Cell Carcinoma With Mediastinal Lymph Node Metastasis by Interleukin-2: A case report
 Tokai J Exp Clin Med., Vol. 30, No. 2, pp. 111-115, 2005 Successful Treatment of Renal Cell Carcinoma With Mediastinal Lymph Node Metastasis by Interleukin-2: A case report Masatoshi TOKUNAGA, Aiichiro
Tokai J Exp Clin Med., Vol. 30, No. 2, pp. 111-115, 2005 Successful Treatment of Renal Cell Carcinoma With Mediastinal Lymph Node Metastasis by Interleukin-2: A case report Masatoshi TOKUNAGA, Aiichiro
Early Chemotherapy for Metastatic Prostate Cancer
 Early Chemotherapy for Metastatic Prostate Cancer Daniel P. Petrylak, MD Professor of Medicine and Urology Smilow Cancer Center Yale University Medical Center Disclosure Consultant: Sanofi Aventis, Celgene,
Early Chemotherapy for Metastatic Prostate Cancer Daniel P. Petrylak, MD Professor of Medicine and Urology Smilow Cancer Center Yale University Medical Center Disclosure Consultant: Sanofi Aventis, Celgene,
Long-term safety and efficacy of vismodegib in patients with advanced basal cell carcinoma (BCC): 24-month update of the pivotal ERIVANCE BCC study
 Long-term safety and efficacy of vismodegib in patients with advanced basal cell carcinoma (BCC): 24-month update of the pivotal ERIVANCE BCC study A Sekulic, 1 MR Migden, 2 AE Oro, 3 L Dirix, 4 K Lewis,
Long-term safety and efficacy of vismodegib in patients with advanced basal cell carcinoma (BCC): 24-month update of the pivotal ERIVANCE BCC study A Sekulic, 1 MR Migden, 2 AE Oro, 3 L Dirix, 4 K Lewis,
Bone Metastases in Muscle-Invasive Bladder Cancer
 Journal of the Egyptian Nat. Cancer Inst., Vol. 18, No. 3, September: 03-08, 006 AZZA N. TAHER, M.D.* and MAGDY H. KOTB, M.D.** The Departments of Radiation Oncology* and Nuclear Medicine**, National Cancer
Journal of the Egyptian Nat. Cancer Inst., Vol. 18, No. 3, September: 03-08, 006 AZZA N. TAHER, M.D.* and MAGDY H. KOTB, M.D.** The Departments of Radiation Oncology* and Nuclear Medicine**, National Cancer
Renal Parenchymal Neoplasms
 Renal Parenchymal Neoplasms د. BENIGN TUMORS : Benign renal tumors include adenoma, oncocytoma, angiomyolipoma, leiomyoma, lipoma, hemangioma, and juxtaglomerular tumors. Renal Adenomas : The adenoma is
Renal Parenchymal Neoplasms د. BENIGN TUMORS : Benign renal tumors include adenoma, oncocytoma, angiomyolipoma, leiomyoma, lipoma, hemangioma, and juxtaglomerular tumors. Renal Adenomas : The adenoma is
Primary Endpoint The primary endpoint is overall survival, measured as the time in weeks from randomization to date of death due to any cause.
 CASE STUDY Randomized, Double-Blind, Phase III Trial of NES-822 plus AMO-1002 vs. AMO-1002 alone as first-line therapy in patients with advanced pancreatic cancer This is a multicenter, randomized Phase
CASE STUDY Randomized, Double-Blind, Phase III Trial of NES-822 plus AMO-1002 vs. AMO-1002 alone as first-line therapy in patients with advanced pancreatic cancer This is a multicenter, randomized Phase
GUIDELINES ON RENAL CELL CARCINOMA
 GUIDELINES ON RENAL CELL CARCINOMA B. Ljungberg (chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction This EAU guideline was prepared to help urologists
GUIDELINES ON RENAL CELL CARCINOMA B. Ljungberg (chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction This EAU guideline was prepared to help urologists
Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense?
 Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense? Philippe E. Spiess, MD, FACS Associate Member Department of GU Oncology Department of Tumor Biology Moffitt Cancer
Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense? Philippe E. Spiess, MD, FACS Associate Member Department of GU Oncology Department of Tumor Biology Moffitt Cancer
Melanoma: Therapeutic Progress and the Improvements Continue
 Melanoma: Therapeutic Progress and the Improvements Continue David W. Ollila, MD Professor of Surgery Jesse and James Millis Professor of Melanoma Research May 20, 2016 Disclosures: NONE Outline 2016 Therapeutic
Melanoma: Therapeutic Progress and the Improvements Continue David W. Ollila, MD Professor of Surgery Jesse and James Millis Professor of Melanoma Research May 20, 2016 Disclosures: NONE Outline 2016 Therapeutic
Lower Baseline PSA Predicts Greater Benefit From Sipuleucel-T
 Lower Baseline PSA Predicts Greater Benefit From Sipuleucel-T Schelhammer PF, Chodak G, Whitmore JB, Sims R, Frohlich MW, Kantoff PW. Lower baseline prostate-specific antigen is associated with a greater
Lower Baseline PSA Predicts Greater Benefit From Sipuleucel-T Schelhammer PF, Chodak G, Whitmore JB, Sims R, Frohlich MW, Kantoff PW. Lower baseline prostate-specific antigen is associated with a greater
Synopsis. Study Phase and Title: Study Objectives: Overall Study Design
 Synopsis Study Phase and Title: Study Objectives: Overall Study Design Phase III randomized sequential open-label study to evaluate the efficacy and safety of sorafenib followed by pazopanib versus pazopanib
Synopsis Study Phase and Title: Study Objectives: Overall Study Design Phase III randomized sequential open-label study to evaluate the efficacy and safety of sorafenib followed by pazopanib versus pazopanib
Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival
 MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
Carcinoma of the Lung
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
GUIDELINES ON RENAL CELL CANCER
 20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
Oncotype DX testing in node-positive disease
 Should gene array assays be routinely used in node positive disease? Yes Christy A. Russell, MD University of Southern California Oncotype DX testing in node-positive disease 1 Validity of the Oncotype
Should gene array assays be routinely used in node positive disease? Yes Christy A. Russell, MD University of Southern California Oncotype DX testing in node-positive disease 1 Validity of the Oncotype
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal drainage, after hepatic resection, 159 160 Ablation, radiofrequency, for hepatocellular carcinoma, 160 161 Adenocarcinoma, pancreatic.
Index Note: Page numbers of article titles are in boldface type. A Abdominal drainage, after hepatic resection, 159 160 Ablation, radiofrequency, for hepatocellular carcinoma, 160 161 Adenocarcinoma, pancreatic.
CONTEMPORARY UPDATE OF PROSTATE CANCER STAGING NOMOGRAMS (PARTIN TABLES) FOR THE NEW MILLENNIUM
 RAPID COMMUNICATION CME ARTICLE CONTEMPORARY UPDATE OF PROSTATE CANCER STAGING NOMOGRAMS (PARTIN TABLES) FOR THE NEW MILLENNIUM ALAN W. PARTIN, LESLIE A. MANGOLD, DANA M. LAMM, PATRICK C. WALSH, JONATHAN
RAPID COMMUNICATION CME ARTICLE CONTEMPORARY UPDATE OF PROSTATE CANCER STAGING NOMOGRAMS (PARTIN TABLES) FOR THE NEW MILLENNIUM ALAN W. PARTIN, LESLIE A. MANGOLD, DANA M. LAMM, PATRICK C. WALSH, JONATHAN
CHEMOTHERAPY FOLLOWED BY SURGERY VS. SURGERY ALONE FOR LOCALIZED ESOPHAGEAL CANCER
 CHEMOTHERAPY FOLLOWED BY VS. ALONE FOR LOCALIZED ESOPHAGEAL CANCER CHEMOTHERAPY FOLLOWED BY COMPARED WITH ALONE FOR LOCALIZED ESOPHAGEAL CANCER DAVID P. KELSEN, M.D., ROBERT GINSBERG, M.D., THOMAS F. PAJAK,
CHEMOTHERAPY FOLLOWED BY VS. ALONE FOR LOCALIZED ESOPHAGEAL CANCER CHEMOTHERAPY FOLLOWED BY COMPARED WITH ALONE FOR LOCALIZED ESOPHAGEAL CANCER DAVID P. KELSEN, M.D., ROBERT GINSBERG, M.D., THOMAS F. PAJAK,
Renal Cell Carcinoma: An Overview. Douglas S. Scherr, M.D. Clinical Director, Urologic Oncology Assistant Professor of Urology
 Renal Cell Carcinoma: An Overview Douglas S. Scherr, M.D. Clinical Director, Urologic Oncology Assistant Professor of Urology Background Renal Cell Carcinoma 2% of all malignancies Heterogeneous disease:
Renal Cell Carcinoma: An Overview Douglas S. Scherr, M.D. Clinical Director, Urologic Oncology Assistant Professor of Urology Background Renal Cell Carcinoma 2% of all malignancies Heterogeneous disease:
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Ablative therapy, nonsurgical, for pulmonary metastases of soft tissue sarcoma, 279 280 Adipocytic tumors, atypical lipomatous tumor vs. well-differentiated
Note: Page numbers of article titles are in boldface type. A Ablative therapy, nonsurgical, for pulmonary metastases of soft tissue sarcoma, 279 280 Adipocytic tumors, atypical lipomatous tumor vs. well-differentiated
Salvage Surgery for Advanced Renal Cell Carcinoma
 European Urology Supplements European Urology Supplements 3 (2004) 2 8 Salvage Surgery for Advanced Renal Cell Carcinoma Gerald H. Mickisch * Center of Operative Urology Bremen, Robert-Koch-Str. 34a, D-28277
European Urology Supplements European Urology Supplements 3 (2004) 2 8 Salvage Surgery for Advanced Renal Cell Carcinoma Gerald H. Mickisch * Center of Operative Urology Bremen, Robert-Koch-Str. 34a, D-28277
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
journal of medicine The new england Preoperative PSA Velocity and the Risk of Death from Prostate Cancer after Radical Prostatectomy abstract
 The new england journal of medicine established in 1812 july 8, 4 vol. 31 no. 2 Preoperative PSA Velocity and the Risk of Death from Prostate Cancer after Radical Prostatectomy Anthony V. D Amico, M.D.,
The new england journal of medicine established in 1812 july 8, 4 vol. 31 no. 2 Preoperative PSA Velocity and the Risk of Death from Prostate Cancer after Radical Prostatectomy Anthony V. D Amico, M.D.,
Medical Management of Renal Cell Carcinoma
 Medical Management of Renal Cell Carcinoma Lin Mei, MD Hematology-Oncology Fellow Hematology, Oncology and Palliative Care Virginia Commonwealth University Educational Objectives Background of RCC (epidemiology,
Medical Management of Renal Cell Carcinoma Lin Mei, MD Hematology-Oncology Fellow Hematology, Oncology and Palliative Care Virginia Commonwealth University Educational Objectives Background of RCC (epidemiology,
Summary of the study protocol of the FLOT3-Study
 Summary of the study protocol of the FLOT3-Study EudraCT no. 2007-005143-17 Protocol Code: S396 Title A Prospective Multicenter Study With 5-FU, Leucovorin, Oxaliplatin and Docetaxel (FLOT) in Patients
Summary of the study protocol of the FLOT3-Study EudraCT no. 2007-005143-17 Protocol Code: S396 Title A Prospective Multicenter Study With 5-FU, Leucovorin, Oxaliplatin and Docetaxel (FLOT) in Patients
BACKGROUND. Many patients with invasive urothelial cell cancer are poor candidates
 2181 Treatment Options for Muscle-invasive Urothelial Cancer for Patients Who Were Not Eligible for Cystectomy or Neoadjuvant Chemotherapy With Methotrexate, Vinblastine, Doxorubicin, and Cisplatin Report
2181 Treatment Options for Muscle-invasive Urothelial Cancer for Patients Who Were Not Eligible for Cystectomy or Neoadjuvant Chemotherapy With Methotrexate, Vinblastine, Doxorubicin, and Cisplatin Report
Introduction ORIGINAL RESEARCH
 Cancer Medicine ORIGINAL RESEARCH Open Access The effect of radiation therapy in the treatment of adult soft tissue sarcomas of the extremities: a long- term community- based cancer center experience Jeffrey
Cancer Medicine ORIGINAL RESEARCH Open Access The effect of radiation therapy in the treatment of adult soft tissue sarcomas of the extremities: a long- term community- based cancer center experience Jeffrey
The Predictors of Local Recurrence after Radical Cystectomy in Patients with Invasive Bladder Cancer
 The Predictors of Local Recurrence after Radical Cystectomy in Patients with Invasive Bladder Cancer Hiroki Ide, Eiji Kikuchi, Akira Miyajima, Ken Nakagawa, Takashi Ohigashi, Jun Nakashima and Mototsugu
The Predictors of Local Recurrence after Radical Cystectomy in Patients with Invasive Bladder Cancer Hiroki Ide, Eiji Kikuchi, Akira Miyajima, Ken Nakagawa, Takashi Ohigashi, Jun Nakashima and Mototsugu
Radical Prostatectomy: Management of the Primary From Localized to Oligometasta:c Disease
 Radical Prostatectomy: Management of the Primary From Localized to Oligometasta:c Disease Disclosures I do not have anything to disclose Sexual function causes moderate to severe distress 2 years after
Radical Prostatectomy: Management of the Primary From Localized to Oligometasta:c Disease Disclosures I do not have anything to disclose Sexual function causes moderate to severe distress 2 years after
Characteristics and prognostic factors of synchronous multiple primary esophageal carcinoma: A report of 52 cases
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Characteristics and prognostic factors of synchronous multiple primary esophageal carcinoma: A report of 52 cases Mei Li & Zhi-xiong Lin Department of Radiation
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Characteristics and prognostic factors of synchronous multiple primary esophageal carcinoma: A report of 52 cases Mei Li & Zhi-xiong Lin Department of Radiation
Pulmonary Resection for Metastases from Colorectal Cancer
 ORIGINAL ARTICLE Pulmonary Resection for Metastases from Colorectal Cancer Paul M. van Schaik, MD,* Ewout A. Kouwenhoven, MD, PhD,* Robert J. Bolhuis, MD,* Bonne Biesma, MD, PhD, and Koop Bosscha, MD,
ORIGINAL ARTICLE Pulmonary Resection for Metastases from Colorectal Cancer Paul M. van Schaik, MD,* Ewout A. Kouwenhoven, MD, PhD,* Robert J. Bolhuis, MD,* Bonne Biesma, MD, PhD, and Koop Bosscha, MD,
Who is the Ideal Candidate for PEG Intron?
 Who is the Ideal Candidate for PEG Intron? Sanjiv S. Agarwala, MD Chief, Oncology & Hematology St. Luke s Cancer Center Professor, Temple University School of Medicine Philadelphia, PA, USA Overview Introduction
Who is the Ideal Candidate for PEG Intron? Sanjiv S. Agarwala, MD Chief, Oncology & Hematology St. Luke s Cancer Center Professor, Temple University School of Medicine Philadelphia, PA, USA Overview Introduction
Surgical Management of Renal Cancer. David Nicol Consultant Urologist
 Surgical Management of Renal Cancer David Nicol Consultant Urologist Roles of Surgery 1. Curative intervention localised disease 2. Symptomatic control advanced disease 3. Augmentation of efficacy of systemic
Surgical Management of Renal Cancer David Nicol Consultant Urologist Roles of Surgery 1. Curative intervention localised disease 2. Symptomatic control advanced disease 3. Augmentation of efficacy of systemic
Radical Cystectomy Often Too Late? Yes, But...
 european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
Lymphadenectomy in RCC: Yes, No, Clinical Trial?
 Lymphadenectomy in RCC: Yes, No, Clinical Trial? Viraj Master MD PhD FACS Professor Associate Chair for Clinical Affairs and Quality Director of Clinical Research Unit Department of Urology Emory University
Lymphadenectomy in RCC: Yes, No, Clinical Trial? Viraj Master MD PhD FACS Professor Associate Chair for Clinical Affairs and Quality Director of Clinical Research Unit Department of Urology Emory University
SYNOPSIS PROTOCOL AFU-GETUG 20/0310
 SYNOPSIS PROTOCOL AFU-GETUG 20/0310 A) IDENTIFICATION OF THE CLINICAL TRIAL SPONSOR CODE NUMBER: AFU-GETUG 20/0310 VERSION AND DATE: VERSION DATED MAY, 05 TH 2011 TITLE OF TRIAL: Phase III randomised trial
SYNOPSIS PROTOCOL AFU-GETUG 20/0310 A) IDENTIFICATION OF THE CLINICAL TRIAL SPONSOR CODE NUMBER: AFU-GETUG 20/0310 VERSION AND DATE: VERSION DATED MAY, 05 TH 2011 TITLE OF TRIAL: Phase III randomised trial
Peritoneal Involvement in Stage II Colon Cancer
 Anatomic Pathology / PERITONEAL INVOLVEMENT IN STAGE II COLON CANCER Peritoneal Involvement in Stage II Colon Cancer A.M. Lennon, MB, MRCPI, H.E. Mulcahy, MD, MRCPI, J.M.P. Hyland, MCh, FRCS, FRCSI, C.
Anatomic Pathology / PERITONEAL INVOLVEMENT IN STAGE II COLON CANCER Peritoneal Involvement in Stage II Colon Cancer A.M. Lennon, MB, MRCPI, H.E. Mulcahy, MD, MRCPI, J.M.P. Hyland, MCh, FRCS, FRCSI, C.
Session 4 Chemotherapy for castration refractory prostate cancer First and second- line chemotherapy
 Session 4 Chemotherapy for castration refractory prostate cancer First and second- line chemotherapy October- 2015 ESMO 2004 October- 2015 Fyraftensmøde 2 2010 October- 2015 Fyraftensmøde 3 SWOG 9916 OS
Session 4 Chemotherapy for castration refractory prostate cancer First and second- line chemotherapy October- 2015 ESMO 2004 October- 2015 Fyraftensmøde 2 2010 October- 2015 Fyraftensmøde 3 SWOG 9916 OS
better time to first recurrence compared to no adjuvant treatment. 1 3 Previous large randomized clinical trials performed
 0022-5347/00/1634-1124/0 THE JOURNAL OF UROLOGY Vol. 163, 1124 1129, April 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. MAINTENANCE BACILLUS CALMETTE-GUERIN IMMUNOTHERAPY
0022-5347/00/1634-1124/0 THE JOURNAL OF UROLOGY Vol. 163, 1124 1129, April 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. MAINTENANCE BACILLUS CALMETTE-GUERIN IMMUNOTHERAPY
ABSTRACT Background Patients with clinically localized, intermediate-
 CHEMOTHERAPY ALONE VS. CHEMOTHERAPY PLUS RADIOTHERAPY FOR NON-HODGKIN S LYMPHOMA CHEMOTHERAPY ALONE COMPARED WITH CHEMOTHERAPY PLUS RADIOTHERAPY FOR LOCALIZED INTERMEDIATE- AND HIGH-GRADE NON-HODGKIN S
CHEMOTHERAPY ALONE VS. CHEMOTHERAPY PLUS RADIOTHERAPY FOR NON-HODGKIN S LYMPHOMA CHEMOTHERAPY ALONE COMPARED WITH CHEMOTHERAPY PLUS RADIOTHERAPY FOR LOCALIZED INTERMEDIATE- AND HIGH-GRADE NON-HODGKIN S
Immunotherapy, an exciting era!!
 Immunotherapy, an exciting era!! Yousef Zakharia MD University of Iowa and Holden Comprehensive Cancer Center Alliance Meeting, Chicago November 2016 Presentation Objectives l General approach to immunotherapy
Immunotherapy, an exciting era!! Yousef Zakharia MD University of Iowa and Holden Comprehensive Cancer Center Alliance Meeting, Chicago November 2016 Presentation Objectives l General approach to immunotherapy
Summary of Phase 3 IMPACT Trial Results Presented at AUA Meeting Webcast Conference Call April 28, Nasdaq: DNDN
 Summary of Phase 3 IMPACT Trial Results Presented at AUA Meeting Webcast Conference Call April 28, 2009 Nasdaq: DNDN PROVENGE sipuleucel-t is an autologous active cellular immunotherapy that activates
Summary of Phase 3 IMPACT Trial Results Presented at AUA Meeting Webcast Conference Call April 28, 2009 Nasdaq: DNDN PROVENGE sipuleucel-t is an autologous active cellular immunotherapy that activates
Guidelines on Renal Cell
 Guidelines on Renal Cell Carcinoma (Text update March 2009) B. Ljungberg (Chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction Renal cell carcinoma
Guidelines on Renal Cell Carcinoma (Text update March 2009) B. Ljungberg (Chairman), D.C. Hanbury, M.A. Kuczyk, A.S. Merseburger, P.F.A. Mulders, J-J. Patard, I.C. Sinescu Introduction Renal cell carcinoma
RCC in Adolescents and Young Adults (AYAs): Diagnosis and Management
 RCC in Adolescents and Young Adults (AYAs): Diagnosis and Management Nicholas G. Cost, M.D. Assistant Professor, Department of Surgery, Division of Urology University of Colorado Cancer Center Fifteenth
RCC in Adolescents and Young Adults (AYAs): Diagnosis and Management Nicholas G. Cost, M.D. Assistant Professor, Department of Surgery, Division of Urology University of Colorado Cancer Center Fifteenth
Cytoreductive Nephrectomy
 Cytoreductive Nephrectomy Stephen H. Culp, M.D., Ph.D. Assistant Professor, Department of Urology Outline The Historics of CN The current status of CN The importance of patient selection Cytoreductive
Cytoreductive Nephrectomy Stephen H. Culp, M.D., Ph.D. Assistant Professor, Department of Urology Outline The Historics of CN The current status of CN The importance of patient selection Cytoreductive
Rare Small Cell Carcinoma in Genitourinary Tract: Experience from E-Da Hospital
 E-Da Medical Journal 20;():-5 Original Article Rare Small Cell Carcinoma in Genitourinary Tract: Experience from E-Da Hospital Wei-Ting Kuo, I-Wei Chang2, Kevin Lu, Hua-Pin Wang, Tsan-Jung u, Victor C.
E-Da Medical Journal 20;():-5 Original Article Rare Small Cell Carcinoma in Genitourinary Tract: Experience from E-Da Hospital Wei-Ting Kuo, I-Wei Chang2, Kevin Lu, Hua-Pin Wang, Tsan-Jung u, Victor C.
Surgical Management of Pulmonary Metastases. Dr AG Jacobs Principal Specialist Dept Cardiothoracic Surgery Steve Biko Academic Hospital
 Surgical Management of Pulmonary Metastases Dr AG Jacobs Principal Specialist Dept Cardiothoracic Surgery Steve Biko Academic Hospital Introduction Lungs 2 nd most common site of metastatic deposition
Surgical Management of Pulmonary Metastases Dr AG Jacobs Principal Specialist Dept Cardiothoracic Surgery Steve Biko Academic Hospital Introduction Lungs 2 nd most common site of metastatic deposition
PROCARBAZINE, lomustine, and vincristine (PCV) is
 RAPID PUBLICATION Procarbazine, Lomustine, and Vincristine () Chemotherapy for Anaplastic Astrocytoma: A Retrospective Review of Radiation Therapy Oncology Group Protocols Comparing Survival With Carmustine
RAPID PUBLICATION Procarbazine, Lomustine, and Vincristine () Chemotherapy for Anaplastic Astrocytoma: A Retrospective Review of Radiation Therapy Oncology Group Protocols Comparing Survival With Carmustine
Stage III Colon Cancer Susquehanna Cancer Center Warren L Robinson, MD, FACP May 9, 2007
 Stage III Colon Cancer Susquehanna Cancer Center 1997-21 Warren L Robinson, MD, FACP May 9, 27 Stage III Colon Cancer Susquehanna Cancer Center 1997-21 Colorectal cancer is the third most common cancer
Stage III Colon Cancer Susquehanna Cancer Center 1997-21 Warren L Robinson, MD, FACP May 9, 27 Stage III Colon Cancer Susquehanna Cancer Center 1997-21 Colorectal cancer is the third most common cancer
Surgical Management of Advanced Stage Colon Cancer. Nathan Huber, MD 6/11/14
 Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
MHRA Public Assessment Report. Epoetins for the management of anaemia associated with cancer: risk of tumour progression and mortality.
 MHRA Public Assessment Report Epoetins for the management of anaemia associated with cancer: risk of tumour progression and mortality November 2007 Executive summary 2 Introduction 5 Epoetins for treatment
MHRA Public Assessment Report Epoetins for the management of anaemia associated with cancer: risk of tumour progression and mortality November 2007 Executive summary 2 Introduction 5 Epoetins for treatment
Brain Metastasis From Renal Cell Carcinoma. BACKGROUND. Patients with renal cell carcinoma brain metastases (RCCBM) are
 1641 Brain Metastasis From Renal Cell Carcinoma Presentation, Recurrence, and Survival Brian Shuch, MD 1 Jeff C. La Rochelle, MD 1 Tobias Klatte, MD 1 Stephen B. Riggs, MD 1 Weiqing Liu, MS 2 Fairooz F.
1641 Brain Metastasis From Renal Cell Carcinoma Presentation, Recurrence, and Survival Brian Shuch, MD 1 Jeff C. La Rochelle, MD 1 Tobias Klatte, MD 1 Stephen B. Riggs, MD 1 Weiqing Liu, MS 2 Fairooz F.
Management of High Risk Renal Cell Carcinoma
 Management of High Risk Renal Cell Carcinoma Peter E. Clark, MD Professor and Chair, Department of Urology Carolinas HealthCare System Chair, Urologic Oncology Levine Cancer Institute October 14, 2017
Management of High Risk Renal Cell Carcinoma Peter E. Clark, MD Professor and Chair, Department of Urology Carolinas HealthCare System Chair, Urologic Oncology Levine Cancer Institute October 14, 2017
Metastasectomy for Melanoma What s the Evidence and When Do We Stop?
 Metastasectomy for Melanoma What s the Evidence and When Do We Stop? Vernon K. Sondak, M D Chair, Moffitt Cancer Center Tampa, Florida Focus on Melanoma London, UK October 15, 2013 Disclosures Dr. Sondak
Metastasectomy for Melanoma What s the Evidence and When Do We Stop? Vernon K. Sondak, M D Chair, Moffitt Cancer Center Tampa, Florida Focus on Melanoma London, UK October 15, 2013 Disclosures Dr. Sondak
Renal Cell Cancer. Clinical case study 1 & 2. Petri Bono MD PhD Helsinki University Hospital Helsinki, Finland
 Renal Cell Cancer Clinical case study 1 & 2 Petri Bono MD PhD Helsinki University Hospital Helsinki, Finland 1 Case study 1 - RCC and Lung Metastases Case study 1: Patient History Male, 63 years old Mild
Renal Cell Cancer Clinical case study 1 & 2 Petri Bono MD PhD Helsinki University Hospital Helsinki, Finland 1 Case study 1 - RCC and Lung Metastases Case study 1: Patient History Male, 63 years old Mild
Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis
 Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
RESEARCH ARTICLE. Kuanoon Boupaijit, Prapaporn Suprasert* Abstract. Introduction. Materials and Methods
 RESEARCH ARTICLE Survival Outcomes of Advanced and Recurrent Cervical Cancer Patients Treated with Chemotherapy: Experience of Northern Tertiary Care Hospital in Thailand Kuanoon Boupaijit, Prapaporn Suprasert*
RESEARCH ARTICLE Survival Outcomes of Advanced and Recurrent Cervical Cancer Patients Treated with Chemotherapy: Experience of Northern Tertiary Care Hospital in Thailand Kuanoon Boupaijit, Prapaporn Suprasert*
Scottish Medicines Consortium
 Scottish Medicines Consortium sorafenib 200mg tablets (Nexavar ) (No. 321/06) Bayer Plc 6 October 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
Scottish Medicines Consortium sorafenib 200mg tablets (Nexavar ) (No. 321/06) Bayer Plc 6 October 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
Setting The setting was secondary care. The economic study was carried out in the UK.
 Cost-utility analysis of the GC versus MVAC regimens for the treatment of locally advanced or metastatic bladder cancer Robinson P, von der Masse H, Bhalla S, Kielhorn A, Aristides M, Brown A, Tilden D
Cost-utility analysis of the GC versus MVAC regimens for the treatment of locally advanced or metastatic bladder cancer Robinson P, von der Masse H, Bhalla S, Kielhorn A, Aristides M, Brown A, Tilden D
Open clinical uro-oncology trials in Canada
 CLINICAL TRIALS Open clinical uro-oncology trials in Canada Eric Winquist, MD, Mary J. Mackenzie, MD, George Rodrigues, MD London Health Sciences Centre, London, Ontario, Canada ADRENOCORTICAL MALIGNANCIES
CLINICAL TRIALS Open clinical uro-oncology trials in Canada Eric Winquist, MD, Mary J. Mackenzie, MD, George Rodrigues, MD London Health Sciences Centre, London, Ontario, Canada ADRENOCORTICAL MALIGNANCIES
Impact of lymphadenectomy in management of renal cell carcinoma
 Journal of the Egyptian National Cancer Institute (2012) 24, 57 61 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com ORIGINAL ARTICLE Impact of
Journal of the Egyptian National Cancer Institute (2012) 24, 57 61 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com ORIGINAL ARTICLE Impact of
Clinical Pathological Conference. Malignant Melanoma of the Vulva
 Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
David N. Robinson, MD
 David N. Robinson, MD Background and Treatment of mrcc Background ~ 64,770 new cases of kidney/renal pelvis cancers will be diagnosed in the US in 2012 with an estimated 13,570 deaths [1] ~ 75% are clear-cell
David N. Robinson, MD Background and Treatment of mrcc Background ~ 64,770 new cases of kidney/renal pelvis cancers will be diagnosed in the US in 2012 with an estimated 13,570 deaths [1] ~ 75% are clear-cell
NIH Public Access Author Manuscript J Surg Oncol. Author manuscript; available in PMC 2012 August 1.
 NIH Public Access Author Manuscript Published in final edited form as: J Surg Oncol. 2011 August 1; 104(2): 111 115. doi:10.1002/jso.21903. Does metastasectomy improve survival in patients with Stage IV
NIH Public Access Author Manuscript Published in final edited form as: J Surg Oncol. 2011 August 1; 104(2): 111 115. doi:10.1002/jso.21903. Does metastasectomy improve survival in patients with Stage IV
Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer. Cheol Min Kang 2018/04/05
 Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
