This case involved a 30-year-old married woman with levator ani muscle overactivity and dyspareunia that was 1 year in duration.
|
|
|
- Mariah Boone
- 5 years ago
- Views:
Transcription
1 Case Report Management of Dyspareunia and Associated Levator Ani Muscle Overactivity Kimberly A Fisher Background and Purpose Musculoskeletal dysfunction is a known cause of dyspareunia and a reason for referral for physical therapist management. The purpose of this case report is to describe the physical therapist management of a patient with dyspareunia and overactivity of the pelvic-floor muscles with a limited number of visits and a focus on self-management strategies. Case Description This case involved a 30-year-old married woman with levator ani muscle overactivity and dyspareunia that was 1 year in duration. Intervention The therapist explained the anatomy and function of the pelvic-floor muscles during intercourse, instructed the patient on how to control the levator ani muscles, and instructed her on vaginal self-dilation techniques. Outcomes The patient attended 3 physical therapy sessions over a period of 9 weeks. She performed vaginal self-dilation at home. She rated pain during intercourse as 0/10 on a verbal rating scale and had no remaining tenderness in the levator ani muscles at discharge. KA Fisher, PT, MPT, is Director, Pelvic Floor Rehabilitation Unit, OU Pelvic and Bladder Health Clinic, 825 NE 10th, Ste 3400, Oklahoma City, OK (USA); Clinical Instructor, Section of Female Pelvic Medicine and Reconstructive Surgery/Urogynecology, Department of Obstetrics and Gynecology; and Clinical Instructor, Department of Rehabilitation Sciences, University of Oklahoma Health Science Center, Oklahoma City, Okla. Address all correspondence to Ms Fisher at: Kimberly-A- Fisher@ouhsc.edu. [Fisher KA. Management of dyspareunia and associated levator ani muscle overactivity. Phys Ther. 2007;87: ] 2007 American Physical Therapy Association Discussion Some women with dyspareunia may improve with an intervention that emphasizes education and vaginal self-dilation techniques. Future research should compare home-based and clinic-based treatments. Post a Rapid Response or find The Bottom Line: July 2007 Volume 87 Number 7 Physical Therapy f 935
2 Dyspareunia is pain before, during, or after intercourse. 1 Dyspareunia in women can have a significant negative effect on quality of life and may affect between 20% and 50% of all women. 2 Mathias et al 3 reported that 88% of women surveyed who had pelvic pain and were sexually active stated that they had pain during intercourse in the previous month. These reports likely underestimate the true prevalence of dyspareunia, because many women with dyspareunia do not seek medical treatment. 4 Possible causes of dyspareunia include injury to the pelvic area during childbirth, vulvar atrophy, endometriosis, pelvic inflammatory disease, infection, adhesions, and interstitial cystitis. 4 Psychosocial factors such as depression, physical or sexual abuse, and anxiety also are possible causes of dyspareunia. 5 Women with dyspareunia, however, are less likely to report a history of physical or sexual abuse compared with women diagnosed with pelvic pain. 4 Musculoskeletal dysfunction, specifically muscle pain and overactivity of the levator ani muscles, is another cause of dyspareunia documented in the literature. 1,2,6 9 Overactivity of the levator ani muscles is a condition in which these muscles do not relax completely, or contract when they should relax. 1 Overactive, nonrelaxing muscles are painful to touch, and pain itself may cause spasms of the levator ani muscles, preventing intercourse entirely. 1,7 Dyspareunia, vaginismus (muscle spasm in the outer third of the vagina that interferes with intercourse), 2,10 and vulvar vestibulitis (severe pain in the vestibule) 4,11 are all associated with pain and overactivity of the levator ani muscles. Women diagnosed with dyspareunia are sometimes referred for physical therapist intervention to address any musculoskeletal component of their pain. 12 The goal of physical therapist intervention for dyspareunia is to reduce vaginal pain by reducing overactivity of the pelvic-floor muscles, improving the patient s ability to control these muscles, and increasing the ability of the vaginal tissue to tolerate a stretch. 10,12 Physical therapist interventions for musculoskeletal dysfunction related to dyspareunia include the use of manual therapy, biofeedback, exercise, and vaginal dilators. 9,13 17 As reported in the literature, these interventions are time intensive, requiring several visits over a long period Vaginal self-dilation is a technique that uses vaginal dilators to desensitize the vaginal tissue, promote muscle relaxation, and relieve symptoms of dyspareunia. 18 Successful use of this technique in combination with psychotherapy interventions has been described in the literature. 18,19 In a randomized clinical trial by Schnyder et al, % of patients who performed vaginal dilation, either with verbal instruction on how to perform the dilation at home or with actual insertion of the dilator by the health care provider, reported pain-free intercourse after an average of 6.3 sessions. This study, however, did not evaluate the success of vaginal dilation in conjunction with physical therapy treatment, and this study still required an average of 6.3 visits with the health care provider over approximately 12 weeks. 18 The effectiveness of home-based vaginal dilation rather than clinic-based treatment is not known. It may be possible for patients to succeed with fewer clinic visits than the range of 8 to 31 visits previously described in physical therapy literature. 13,14 If this is true, it is important to identify characteristics of patients likely to respond to minimal intervention. The purpose of this case report is to describe the management of a patient with levator ani muscle overactivity and dyspareunia with an emphasis on home-based treatment. This report meets the University of Oklahoma s Institutional Review Board requirements for the privacy of patient information. Case Description History A 30-year-old, married woman was referred by her urogynecologist for treatment of pelvic-floor spasm and pelvic pain. Her husband attended the examination. Her chief complaint was pain during intercourse, which began as lower abdominal pain during intercourse years previously. Over time, the pain developed at the entrance of the vagina and then throughout the vagina during intercourse. On a verbal rating scale, she rated her pain as 10/10 during intercourse and 0/10 immediately afterward. 20 On a pain drawing, she mapped her pain to the lower abdominal area, inferior to the umbilicus. She described her pain as moderate-to-severe shooting, stabbing, and sharp pain. She reported no pain at rest, during physical activity, or during urination and defecation. She reported having no symptoms of voiding or bowel dysfunction. She could not correlate the onset of her pain with any specific event. Intercourse with her husband was pain-free before this time. She was not sexually active due to her pain. She completed the 6-item Urinary Distress Inventory Short Form (UDI-6) questionnaire and the Incontinence Impact Questionnaire Short Form (IIQ-7). The UDI-6 and IIQ-7 measure symptom distress and life impact of urinary incontinence and related conditions for women, and they correlate well with the long forms of the questionnaires. 21 These questionnaires are a routine part of the examination of any patients with a pelvic-floor dysfunction who have been referred to my clinic. Although the patient was not referred to my 936 f Physical Therapy Volume 87 Number 7 July 2007
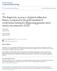
3 clinic because of incontinence, incontinence is often associated with other diagnoses; therefore, it was important to find out whether this is the case for this patient. The patient s responses on the UDI-6 indicated that she was bothered moderately by pain or discomfort in the lower abdominal or genital area, and she indicated in writing that this pain occurred during intercourse. 21 She reported being bothered not at all by frequent urination, urine leakage, or difficulty emptying her bladder. On the IIQ-7, she scored 0 on all 7 items for a total score of 0, indicating that she was not at all affected by urine leakage or prolapse. 21 Her significant medical history included uterine rupture, pelvic fracture, internal bleeding, hepatic laceration, and collapsed lung with subsequent laparotomy and hysterectomy following a motor vehicle accident 11 years before the onset of her pain. She denied any history of physical or sexual abuse. Her primary goal was to eliminate pain during intercourse. Examination and Evaluation A lower-quarter screen was performed to rule out neurological or musculoskeletal dysfunction. This screen included examination of the range of motion of the hips and back; myotome testing of L2 S1; palpation of bony landmarks of the lumbar spine, sacrum, and pelvis for symmetry and pain; motion testing of the sacroiliac joint; palpation of the musculature of the abdominal wall and buttock; and reflex testing. 22 The lower-quarter screen was negative for lumbar and sacroiliac joint dysfunction, pain, weakness, neurological dysfunction, and reproduction of symptoms. After obtaining appropriate verbal consent, an internal pelvic-floor muscle examination was performed due to the patient s chief complaint of dyspareunia and the physician s diagnosis of pelvic-floor spasm. The examination was performed in the dorsal lithotomy position. Sensation in the S2 4 dermatomes, tested with a cotton-tipped swab, was normal. 23 Cotton-swab testing of the vestibule as described by Bergeron et al 11 was negative for tenderness. To examine for pain, pressure was applied to the pelvic-floor muscles externally, 7 and internally through vaginal palpation using one digit. 24 Although less accurate as a measurement of strength (force-producing capacity of muscle), vaginal palpation is the preferred method to determine qualitatively whether the patient can correctly contract and relax the pelvic-floor muscles. 1,24,25 Vaginal palpation also is used to test for pain. 1,17,24,25 The patient denied any pain with external palpation. Any pressure or stretch internally to the vaginal sidewalls caused immediate tenderness and pain that reproduced her pain during intercourse. Internal tenderness to palpation in the muscle bulk of the levator ani and obturator internus muscles bilaterally also reproduced her pain during intercourse. The Figure depicts internal palpation of the obturator internus muscle and the 3 components of the levator ani muscles: the puborectalis, pubovisceral, and iliococcygeus muscles. The location of tenderness in the levator ani muscle group was confirmed by asking the patient to contract her pelvic-floor muscles. 25 The palpable increase in muscle tension at the location of tenderness confirmed that the site of pain was in the levator ani muscle bulk. 25 The procedure was repeated for the obturator internus muscle bilaterally by resisting hip external rotation on each side. 25 She generated a weak levator ani muscle contraction; however, this did not increase her pain. 1 The International Continence Society (ICS) recommends that therapists grade a pelvic-floor muscle contraction as absent, weak, normal, or strong. 1 The patient was then asked to relax her pelvic-floor muscles voluntarily. The patient s voluntary relaxation of the pelvic floor was partial, meaning the pelvic floor returned to its precontraction state, according to the ICS recommended terminology. 1 Diagnosis The patient s primary complaint was superficial and deep dyspareunia. My diagnosis included pain and overactivity of the levator ani and obturator internus muscles. Palpation of these muscles reproduced the patient s pain during intercourse, which indicated that pain and overactivity of these muscles likely contributed to her complaint of dyspareunia. Based on the physical examination, it did not appear that her symptoms arose from any abnormality of the lumbar spine, sacroiliac joint, abdominal wall, or other lower-extremity muscle system. The UDI-6 and IIQ-7 questionnaires ruled out the presence of incontinence and voiding dysfunction. The patient was classified into Preferred Physical Therapist Practice Pattern 4C (Impaired Muscle Performance) in the Guide to Physical Therapist Practice. 26 Prognosis The patient was able to achieve partial muscle relaxation using the cues that I gave to her, and she and her husband expressed a willingness to perform a home program of vaginal dilation independently for a few weeks. Her primary goal was to achieve pain-free intercourse. Based on the results of the study by Schnyder et al, 18 previous clinical experience in similar cases, and the patient s motivation to succeed independently, I expected the patient to achieve her goal of pain-free intercourse over the next 12 weeks. July 2007 Volume 87 Number 7 Physical Therapy f 937
4 Figure. Internal palpation of the obturator internus muscle and the 3 components of the levator ani muscles: the puborectalis, pubovisceral, and iliococcygeus muscles. I anticipated seeing the patient 3 to 6 times, once every 2 to 3 weeks, depending on her level of independence with the home program. 18 The patient made a return appointment for 2 weeks later. Intervention I explained that previous painful attempts at intercourse can cause the pelvic-floor muscles to contract to close the vagina and prevent intercourse. 1 I further explained pelvicfloor anatomy and emphasized that the pelvic-floor muscles should relax sufficiently to allow intercourse to occur. 27 It is important to understand this before attempting vaginal self-dilation. 10 After completing the examination, the patient was cued to contract her pelvic-floor muscles, and the gloved examination finger was inserted or a stretch applied during the relaxation phase after the contraction. Fitz- Gerald and Kotarinos 9 and Weiss 16 described this contract/relax technique as promoting muscle relaxation by applying a stretch immediately after an isometric muscle contraction and maintaining the stretch pressure as the patient contracts again. I cued the patient to relax her muscles using this technique and using deep breathing. The patient s level of discomfort was used as a guide, and the patient could stop the session at any time. Repeated stretches were applied to the posterior and side walls of the vagina. Her pain during the stretches decreased when she could achieve muscle relaxation below the normal resting state of the muscle. The ICS has defined this state as complete relaxation. 1 Because the patient was able to achieve muscle relaxation that improved with verbal and tactile cues and because of a lack of time, a biofeedback examination was not performed at the initial visit. I instructed the patient and her husband to begin using a slender taper candle as a dilator at home in conjunction with contraction and relaxation exercises for the levator ani muscles. The patient chose to begin dilation with a taper candle rather than a commercially available dilator because of convenience. Evidence for the use of vaginal dilators to desensitize and stretch the vaginal tissue is limited, although dilators have been used for some time for this purpose. 19,28 A taper candle or a dilator may allow the patient to desensitize the vaginal tissue to stretch and may 938 f Physical Therapy Volume 87 Number 7 July 2007
5 provide tactile feedback on muscle relaxation and contraction. This technique allows the patient to stretch and perform muscular reeducation at home, pace the progression of the stretches, and exhibit control over the therapy. 10 It is theorized that this patient control is important for women with symptoms of dyspareunia. 10 I instructed her to apply a stretch to the posterior vaginal wall (downward) and the vaginal sidewalls (to the sides) as she could tolerate this. The patient was taught to contract her muscles, and then insert the candle further or apply a stretch during the relaxation phase. This was an adaptation of the contract/relax technique described above. She was advised to perform deep breathing during stretching, perform all stretching in a pain-free way, and to stretch most days of the week for 5 to 10 minutes. Similarly, Schnyder et al 18 recommended using dilators for 10 to 15 minutes, 5 times per week. * Milex Vaginal Silicone Dilators, 4311 N Normandy Ave, Chicago, IL The patient returned for her followup appointment 3 weeks later. She was unable to return at 2 weeks due to an unrelated illness. She reported using the candle dilator without pain with her husband s assistance. Because there was no tenderness to palpation during a one-digit examination of the pelvic floor, I attempted to insert a dilator* (28 mm 140 mm). The patient tolerated the insertion of the dilator approximately half way (6.5 cm) without pain. Progression of the dilator past this point caused pain. Her husband had questions about stretching techniques, and he observed the therapist insert the dilator and apply a stretch to the posterior and side walls of the vagina. He acknowledged that he understood this technique, and the patient took home the larger dilator to use in place of the taper candle. I chose not to use other intervention techniques at that time because the patient was doing well with her home program. The patient scheduled her follow-up appointment for 3 weeks later and was instructed to progress to a larger dilator as soon as she was able to do so. One week later, the patient obtained a larger dilator (32 mm 146 mm) from the physical therapy clinic. Her stretches continued to be pain free. Two-and-a-half weeks later, the patient obtained the largest dilator (38 mm 157 mm). Outcome The patient returned for her third and final appointment 6 weeks after her second appointment, a total of 9 weeks since her first physical therapy session. The primary outcome measure assessed was pain during intercourse, which was rated using a verbal rating scale. At this third and final appointment, she rated pain during intercourse as 0/10. Reexamination of her pelvic-floor muscles was negative for any muscle tenderness or overactivity. The patient met her goal of pain-free intercourse and was discharged from physical therapy. The patient was contacted by telephone for follow-up 2 months later. She reported that intercourse was still pain-free. Discussion and Conclusion The purpose of this case report was to describe the management of a patient with dyspareunia and levator ani muscle pain and overactivity over a minimal number of visits, with an emphasis on home-based treatment. The etiology of dyspareunia and levator ani muscle overactivity in this case was unknown, but this is often difficult to determine. 4 In this case, the patient self-paced her home program by performing stretching, muscle contraction and relaxation, and desensitization exercises using progressively larger dilators. Other reports of physical therapist interventions for dyspareunia include a more clinic-based program involving manual therapy, biofeedback sessions, or a therapist-directed vaginal stretching program. 13,14,18 The use of progressive vaginal dilation to reduce muscle pain and overactivity and to desensitize the vaginal tissue is not a new concept, and was described more than 30 years ago by physicians, psychotherapists, and sex therapists. 19 A review by Reissing et al 19 examined 22 different studies of treatments for dyspareunia and vaginismus. These studies were uncontrolled clinical studies or quasi-experimental studies. Eighteen studies involved the use of vaginal dilators, but only 3 studies mentioned in the review described the combination of mechanical vaginal dilation and instruction in pelvicfloor muscle control and relaxation: Barnes et al, 29 Dawkins and Taylor, 30 and Lamont. 31 These studies reported success rates of 66% to 100%, with success defined as successful intercourse; however, these studies also used a combination of sex therapy, couples therapy, and communication exercises in addition to vaginal dilation and pelvic-floor muscle control exercises. These studies reported that these interventions occurred over an average of 3.4 to 11 treatment sessions. These studies did not involve treatment by a physical therapist. None of the remaining studies in the review involved the use of mechanical dilation and pelvic-floor muscle control together or any mention of the use of physical therapy interventions, but emphasized psychotherapy interventions. The reviewers highlighted the poor methodological qualities of these studies. 19 Further research of higher methodological July 2007 Volume 87 Number 7 Physical Therapy f 939
6 quality is needed to define treatment protocols for dyspareunia and to clarify the role of physical therapy intervention in the management of this condition. Electromyographic (EMG) biofeedback was not used in this case because of the patient s success with verbal and tactile feedback. There is some evidence that EMG biofeedback is helpful for muscle reeducation in patients with overactivity of the levator ani muscles. 15 Glazer et al 15 reported success with biofeedback-assisted pelvic-floor muscle exercises for patients with vulvar vestibulitis and dyspareunia; 26 of 28 patients resumed intercourse after 6 visits and an average of 16 weeks of at-home practice. In the study by Glazer et al, the patients used biofeedback at home to assist in pelvic-floor muscle contraction and relaxation. Although the patient in this case report did not use EMG feedback at home, she did use a vaginal dilator, a form of tactile feedback that may have served the same purpose as the biofeedback described in the study by Glazer et al. 15 In addition, patients in the study by Glazer et al had dyspareunia attributed to vulvar vestibulitis, which the patient in this case report did not have. Downey and Frederick 14 also reported successful use of EMG biofeedback in the treatment of a patient with vulvar vestibulitis and dyspareunia related to a gynecological examination in 8 treatment sessions. Insurance plans may not cover EMG biofeedback, and the equipment is expensive for clinicians to purchase. The purpose of EMG biofeedback is to provide feedback on the patient s ability to contract and relax a muscle. Biofeedback is appropriate if the patient lacks this ability, or if the physical therapist uses the biofeedback to document muscle performance. 24 I could not find a comparison of verbal and tactile feedback to EMG feedback documented in the literature. Future studies should compare these forms of feedback. Various case reports and case series in the literature mention the use of manual therapy and myofascial techniques to decrease levator ani muscle overactivity and pain. 13,14,16,32 Downey and Frederick 14 and Weiss 16 described manual therapy techniques in detail; however, both articles described a program of clinicbased rather than home-based treatment. Weiss 16 recommended 1 to 2 visits per week for 8 to 12 weeks for patients with myofascial trigger points in the pelvic floor. However, the patients in the study by Weiss 16 had interstitial cystitis and urgency frequency syndrome, which differed from the patient in this case report. Downey and Frederick 14 described the use of manual stretching performed by the therapist, biofeedback, and a home exercise program for the pelvic-floor muscles for a patient with vulvar vestibulitis over the course of 8 visits. The patient described in their case report was unwilling to perform self-stretching techniques at home, and the patient tolerated the therapy with minimal pain. 14 In such cases, clinic-based intervention may be an acceptable alternative to a more patient-directed program. Holland 13 described physical therapist management of dyspareunia in 31 visits that included myofascial release techniques, moist heat, biofeedback, exercise, and vaginal dilation using a taper candle at home. The case report by Holland did not specifically describe the manual therapy techniques used and required 28 additional visits over a much longer time period (1 year) compared with the patient described in this case report. FitzGerald and Kotarinos 9 recommended ten 1-hour sessions of manual therapy to treat patients with pelvic-floor dysfunction; however, this recommendation was based on expert opinion. The patient described in the present case report received manual therapy on the first visit and was instructed to perform manual techniques with her dilator at home. Such a home program may achieve results equivalent to manual therapy sessions performed by a physical therapist in some patients. Future studies should compare clinic-based manual therapy and vaginal self-dilation. Case reports are not capable of demonstrating cause and effect, so it is not possible to conclude that the interventions described in this case report caused the positive outcomes. Another potential limitation of this case report is the lack of a quality-oflife scale or a validated sexual function questionnaire as an outcome measure. This report uses a verbal rating scale of pain during intercourse as the primary outcome measure, as is used in other case reports. 8,14,32 The patient s primary complaint was pain, and although there are validated questionnaires related to sexual function, women may find these questionnaires embarrassing. The detail required by these questionnaires may not be necessary. Other limitations of this case report include the terminology used to describe pelvic-floor muscle contraction and relaxation. The ICS does not provide clear distinctions among the terms used to grade pelvic-floor muscle function (ie, absent, weak, normal, and strong). 1 Although overactivity is the recommended term to describe a muscle that will not relax voluntarily, the reliability of this assessment method is not known. 1 Other terms in the literature that are associated with dyspareunia include muscle spasm and hypertonus. There are no clear definitions of 940 f Physical Therapy Volume 87 Number 7 July 2007
7 spasm and hypertonus as they relate to the pelvic-floor muscles in the literature. Another potential limitation is that muscle palpation was the only method used to measure muscle activity in this case report, and additional assessment with EMG was not performed. Future studies should document patient pain levels when comparing interventions, because many manual techniques can be painful. This patient achieved her goal without extensive clinic-based interventions. Future research should compare clinic- and home-based interventions in patients with varying levels of dyspareunia. The patient in this case report was motivated to perform the prescribed muscle relaxation and re-education techniques at home and had at least a partial ability to relax her levator ani muscles during the initial examination. Research is needed to establish a clinical prediction rule to help determine whether these or other patient characteristics are necessary to succeed with minimal clinic-based intervention. The author acknowledges S Abbas Shobeiri, MD, for review of a previous draft of the manuscript and for his illustration in the Figure. This article was submitted June 16, 2006, and was accepted March 1, DOI: /ptj References 1 Messelink B, Benson T, Berghmans B, et al. Standardization of terminology of pelvic floor muscle function and dysfunction: report from the pelvic floor clinical assessment group of the International Continence Society. Neurourol Urodyn. 2005; 24: Basson R, Berman J, Burnett A, et al. Report of the international consensus development conference on female sexual dysfunction: definitions and classifications. J Urol. 2000;163: Mathias SD, Kuppermann M, Lieberman RF, et al. Chronic pelvic pain: prevalence, health-related quality of life, and economic correlates. Obstet Gynecol. 1996;87: Heim LJ. Evaluation and differential diagnosis of dyspareunia. Am Fam Physician. 2001;63: Latthe P, Mignini L, Gray R, et al. Factors presdisposing women to chronic pelvic pain: systematic review. BMJ. 2006;332: American College of Obstetricians and Gynecologists. ACOG Practice Bulletin No. 51: chronic pelvic pain. Obstet Gynecol. 2004;103: Prendergast SA, Weiss JM. Screening for musculoskeletal causes of pelvic pain. Clin Obstet Gynecol. 2003;46: Monif GR, Belatti RG Jr. Intercourserelated vaginal pain syndrome: a variant of vulvar vestibulitis syndrome? Am J Obstet Gynecol. 1993;169: FitzGerald MP, Kotarinos R. Rehabilitation of the short pelvic floor, II: treatment of the patient with the short pelvic floor. Intl Urogynecol J Pelvic Floor Dysfunct. 2003; 14: Crowley T, Richardson D, Goldmeier D. Recommendations for the management of vaginismus: BASHH Special Interest Group for Sexual Dysfunction. Int J STD AIDS. 2006;17: Bergeron S, Binik YM, Khalife S, et al. Vulvar vestibulitis syndrome: reliability of diagnosis and evaluation of current diagnostic criteria. Obstet Gynecol. 2001;98: Rosenbaum TY. Physiotherapy treatment of sexual pain disorders. J Sex Marital Ther. 2005;31: Holland A. Case report: physical therapy intervention for dyspareunia. Journal of the Section on Women s Health. 2003;27(1): Downey P, Frederick I. Physical therapy treatment for vulvar vestibulitis: a case report. Journal of Women s Health Physical Therapy. 2006;30(1): Glazer HI, Rodke G, Swencionis C, et al. Treatment of vulvar vestibulitis syndrome with electromyographic biofeedback of pelvic floor musculature. J Reprod Med. 1995;40: Weiss JM. Pelvic floor myofascial trigger points: manual therapy for interstitial cystitis and the urgency-frequency syndrome. J Urol. 2001;166: FitzGerald MP, Kotarinos R. Rehabilitation of the short pelvic floor, I: background and patient evaluation. Intl Urogynecol J Pelvic Floor Dysfunct. 2003;14: Schnyder U, Schnyder-Luthi C, Ballinari P, Blaser A. Therapy for vaginismus: in vivo versus in vitro desensitization. Can J Psychiatry. 1998;43: Reissing ED, Binik YM, Khalife S. Does vaginismus exist? A critical review of the literature. J Nerv Ment Dis. 1999;187: Ohnhaus EE, Adler R. Methodological problems in the measurement of pain: a comparison between the verbal rating scale and the visual analogue scale. Pain. 1975;1: Uebersax JS, Wyman JF, Shumaker SA, et al. Short forms to assess life quality and symptom distress for urinary incontinence in women: the Incontinence Impact Questionnaire and the Urogenital Distress Inventory. Neurourol Urodyn. 1995;14: Kleeman S. Clinical evaluation and diagnostic tests for urinary incontinence. Journal of Pelvic Medicine and Surgery. 2004; 10: Bourcier A, Juras J, Villet R. Office evaluation and physical examination. In: Bourcier A, McGuire E, Abrams P, eds. Pelvic Floor Disorders. Philadelphia, Pa: Elsevier Saunders; 2004: Bø K, Sherburn M. Evaluation of female pelvic-floor muscle function and strength. Phys Ther. 2005;85: Shelley B, Dunbar A. Clinical commentary: palpation and assessment of the pelvic floor muscles using depth and positional measurements. Journal of the Section on Women s Health. 2004;28(1): Guide to Physical Therapist Practice. 2nd ed. Alexandria, Va: American Physical Therapy Association; Wallace K. Female pelvic floor functions, dysfunctions and behavioral approaches to treatment. In: Agostini R, ed. Clinics in Sports Medicine: The Athletic Woman. Vol 13. Philadelphia, Pa: WB Saunders Co; 1994: McGuire H, Hawton K. Interventions for vaginismus. Cochrane Database Syst Rev. 2003;(1):CD Barnes J, Bowman EP, Cullen J. Biofeedback as an adjunct to psychotherapy in the treatment of vaginismus [abstract]. Biofeedback Self Regul. 1985;9: Dawkins S, Taylor R. Non-consummation of marriage. Lancet. 1961;2: Lamont JA. Vaginismus. Am J Obstet Gynecol. 1978;131: Kalina CW. Manual therapy intervention for dyspareunia of musculoskeletal origin: A case report [abstract]. Journal of the Section on Women s Health. 2004;28(2): July 2007 Volume 87 Number 7 Physical Therapy f 941
10/15/2012. Pelvic Pain and Dysfunction
 Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
Role of Physiotherapy in the Management of Persistent Pelvic Pain. Brigitte Fung Physiotherapist Kwong Wah Hospital
 Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Keywords: Female runner, Pelvic floor dysfunction, PT Management spectrum
 Management of Pelvic floor dysfunction in Female runners Combined Sections Meeting 2017 New Orleans, LA February 23, 2018 10:00 am 12:00 pm We have no relevant financial disclosures or conflicts of interest
Management of Pelvic floor dysfunction in Female runners Combined Sections Meeting 2017 New Orleans, LA February 23, 2018 10:00 am 12:00 pm We have no relevant financial disclosures or conflicts of interest
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE
 PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
5/29/2015. Objectives. Functions of the PFM. Various phases of PFM. Evaluation of the PFM
 The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
IUGA Brisbane, Australia 4 September Workshop: MULTIDISCIPLINARY APPROACH TO FEMALE SEXUALITY BASED ON O PRACTICAL CONCEPTS
 IUGA 2012 Brisbane, Australia 4 September 2012 Workshop: MULTIDISCIPLINARY APPROACH TO FEMALE SEXUALITY BASED ON O PRACTICAL CONCEPTS Current physical therapy for sexual dysfunctions, what is the evidence?
IUGA 2012 Brisbane, Australia 4 September 2012 Workshop: MULTIDISCIPLINARY APPROACH TO FEMALE SEXUALITY BASED ON O PRACTICAL CONCEPTS Current physical therapy for sexual dysfunctions, what is the evidence?
Pelvic Physio 101. OMA Sports Med 2019 Conference. Nelly Faghani PT. January 25,
 Pelvic Physio 101 OMA Sports Med 2019 Conference January 25, 2019 Nelly Faghani PT www.pelvichealthsolutions.ca CFPC CoI Templates: Slide 1 used in Faculty presentation only. Faculty/Presenter Disclosure
Pelvic Physio 101 OMA Sports Med 2019 Conference January 25, 2019 Nelly Faghani PT www.pelvichealthsolutions.ca CFPC CoI Templates: Slide 1 used in Faculty presentation only. Faculty/Presenter Disclosure
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Title: Role of the Physical Therapy in the Multidisciplinary Approach to Vulvodynia: preliminary results
 Title: Role of the Physical Therapy in the Multidisciplinary Approach to Vulvodynia: preliminary results Authors: Miletta, M.; 1 * Bogliatto, F. 1 Type: Original Article Keywords: midwife; multidisciplinary,
Title: Role of the Physical Therapy in the Multidisciplinary Approach to Vulvodynia: preliminary results Authors: Miletta, M.; 1 * Bogliatto, F. 1 Type: Original Article Keywords: midwife; multidisciplinary,
Dear Patient, Sincerely, The Pelvic Health and Rehabilitation Center
 Dear Patient, Welcome to the Pelvic Health and Rehabilitation Center! We specialize in physical therapy management of numerous pelvic pain disorders. We believe in a multidisciplinary collaborative approach
Dear Patient, Welcome to the Pelvic Health and Rehabilitation Center! We specialize in physical therapy management of numerous pelvic pain disorders. We believe in a multidisciplinary collaborative approach
CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER
 CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER What is it? Where is it? Breathing Graded relaxation Incontinence Stress Incontinence
CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER What is it? Where is it? Breathing Graded relaxation Incontinence Stress Incontinence
Over Active Pelvic Floor
 Over Active Pelvic Floor Maeve Whelan SMISCP Specialist Chartered Physiotherapist, Women s Health Background The concept of an overactive pelvic floor (OAPF) is relatively new in pelvic floor rehabilitation.
Over Active Pelvic Floor Maeve Whelan SMISCP Specialist Chartered Physiotherapist, Women s Health Background The concept of an overactive pelvic floor (OAPF) is relatively new in pelvic floor rehabilitation.
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE?
 PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
Dr Hannah Blakely. Dr Ben Sharp. Ms Julee Binns. Sara Widdowson. 7:15-8:15 Breakfast Session: Oxford Women's Health
 Dr Hannah Blakely Clinical Psychologist Oxford Women's Health Ms Julee Binns Consultant Physiotherapist Oxford Women's Health, Christchurch Sara Widdowson NZ Registered Dietitian Christchurch Public Hospital
Dr Hannah Blakely Clinical Psychologist Oxford Women's Health Ms Julee Binns Consultant Physiotherapist Oxford Women's Health, Christchurch Sara Widdowson NZ Registered Dietitian Christchurch Public Hospital
Female&sexual& dysfunction&and& Interstitial&cystitis& Urology Grand Rounds November 14, 2012 Momoe Hyakutake, Urogynecology Fellow.
 Female&sexual& dysfunction&and& Interstitial&cystitis& Urology Grand Rounds November 14, 2012 Momoe Hyakutake, Urogynecology Fellow Objectives& 1) Overview of female sexual dysfunction 2) Explore the relationship
Female&sexual& dysfunction&and& Interstitial&cystitis& Urology Grand Rounds November 14, 2012 Momoe Hyakutake, Urogynecology Fellow Objectives& 1) Overview of female sexual dysfunction 2) Explore the relationship
Case Study: Abdominal & Pelvic Pain
 WRHA: Less Pain, More Gain! Case Study: Abdominal & Pelvic Pain Presented November 4, 2013 Dr. Kelli Berzuk Pelvic Floor Physiotherapist WRHA: Less Pain, More Gain! Case Study To respect patient privacy
WRHA: Less Pain, More Gain! Case Study: Abdominal & Pelvic Pain Presented November 4, 2013 Dr. Kelli Berzuk Pelvic Floor Physiotherapist WRHA: Less Pain, More Gain! Case Study To respect patient privacy
Chronic Pelvic Pain. AP099, December 2010
 AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
AN EXPLORATION OF PELVIC FLOOR DYSFUNCTION: CAUSES, REVIEW OF RESEARCH AND TREATMENT. Karoline Kaminski
 AN EXPLORATION OF PELVIC FLOOR DYSFUNCTION: CAUSES, REVIEW OF RESEARCH AND TREATMENT. Karoline Kaminski Research Project Diploma in Osteopathic Manual Practice Fall 2014 National Academy of Osteopathy
AN EXPLORATION OF PELVIC FLOOR DYSFUNCTION: CAUSES, REVIEW OF RESEARCH AND TREATMENT. Karoline Kaminski Research Project Diploma in Osteopathic Manual Practice Fall 2014 National Academy of Osteopathy
Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website:
 Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website: www.female-gynecologist.com What is Painful Bladder (PBS) or Interstitial Cystitis
Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website: www.female-gynecologist.com What is Painful Bladder (PBS) or Interstitial Cystitis
Pelvic Floor Dysfunction (PFD) Interdisciplinary Treatment and Referral Consideration for Physician Assistants
 Pelvic Floor Dysfunction (PFD) Interdisciplinary Treatment and Referral Consideration for Physician Assistants Gerry Keenan, MMS, PA C Tammy Roehling, PT, DPT Learner Objectives 1. Recreate the pelvic
Pelvic Floor Dysfunction (PFD) Interdisciplinary Treatment and Referral Consideration for Physician Assistants Gerry Keenan, MMS, PA C Tammy Roehling, PT, DPT Learner Objectives 1. Recreate the pelvic
Pelvic Floor Overactivity: Definition and Pathophysiology
 + Pelvic Floor Overactivity: Definition and Pathophysiology WS # 24 The Overactive Pelvic Floor Anna Padoa, MD Urogynecology and Pelvic Floor Service Assaf Harofeh Medical Center + Definition of overactive
+ Pelvic Floor Overactivity: Definition and Pathophysiology WS # 24 The Overactive Pelvic Floor Anna Padoa, MD Urogynecology and Pelvic Floor Service Assaf Harofeh Medical Center + Definition of overactive
Chronic pelvic pain has many different characteristics. Signs and symptoms may include:
 Pelvic Pain in Women Pelvic pain in women refers to pain in the lowest part of your abdomen and pelvis. If asked to locate your pain, you might sweep your hand over that entire area rather than point to
Pelvic Pain in Women Pelvic pain in women refers to pain in the lowest part of your abdomen and pelvis. If asked to locate your pain, you might sweep your hand over that entire area rather than point to
The Female Sexual Pain Disorders: Genital Pain or Sexual Dysfunction?
 Archives of Sexual Behavior, Vol. 31, No. 5, October 2002, pp. 425 429 ( C 2002) The Female Sexual Pain Disorders: Genital Pain or Sexual Dysfunction? Yitzchak M. Binik, Ph.D., 1,5 Elke Reissing, Ph.D.,
Archives of Sexual Behavior, Vol. 31, No. 5, October 2002, pp. 425 429 ( C 2002) The Female Sexual Pain Disorders: Genital Pain or Sexual Dysfunction? Yitzchak M. Binik, Ph.D., 1,5 Elke Reissing, Ph.D.,
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Social History/Employment/Work:
 Case Rationale: Rather than choosing a case study that is seen on a regular basis in my women s health practice and well supported with research such as urinary incontinence, I chose vaginismus specifically
Case Rationale: Rather than choosing a case study that is seen on a regular basis in my women s health practice and well supported with research such as urinary incontinence, I chose vaginismus specifically
Central Texas Myofascial Release New Patient Information Sheet P a g e 1
 P a g e 1 Welcome to our practice! Please help us serve you better by taking a few minutes to provide the following information. If a section does not apply please mark N/A. Name: Last Name First Name
P a g e 1 Welcome to our practice! Please help us serve you better by taking a few minutes to provide the following information. If a section does not apply please mark N/A. Name: Last Name First Name
Inner Stability, Ltd., Bet Shemesh, Israel. Online publication date: 10 March 2011
 This article was downloaded by: [Rosenbaum, Talli] On: 11 March 2011 Access details: Access Details: [subscription number 934772913] Publisher Routledge Informa Ltd Registered in England and Wales Registered
This article was downloaded by: [Rosenbaum, Talli] On: 11 March 2011 Access details: Access Details: [subscription number 934772913] Publisher Routledge Informa Ltd Registered in England and Wales Registered
17 th European congress of Physical Rehabilitation Medicine. 38th SIMFER congress
 17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Female Pelvic Medicine & Reconstructive Surgery Beth Israel Deaconess Medical Center (BIDMC)
 Female Pelvic Medicine & Reconstructive Surgery Beth Israel Deaconess Medical Center (BIDMC) Name: Age: Reason for visit/referral: Are you referred for or interested in surgery? Yes No Maybe Referring
Female Pelvic Medicine & Reconstructive Surgery Beth Israel Deaconess Medical Center (BIDMC) Name: Age: Reason for visit/referral: Are you referred for or interested in surgery? Yes No Maybe Referring
Vague symptoms. Unexpected flares.
 PELVIC FLOOR DYSFUNCTION We need to expand the differential diagnosis for chronic pelvic pain to include pelvic myofascial pain Amie Kawasaki, MD Dr. Kawasaki is Fellow in the Division of Female Pelvic
PELVIC FLOOR DYSFUNCTION We need to expand the differential diagnosis for chronic pelvic pain to include pelvic myofascial pain Amie Kawasaki, MD Dr. Kawasaki is Fellow in the Division of Female Pelvic
Women s & Children s Directorate The TVT Operation - a guide for patients
 Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Dynamic rehabilitative ultrasound for pelvic floor disorders Introduction in techniques and hands-on-workshop
 Dynamic rehabilitative ultrasound for pelvic floor disorders Introduction in techniques and hands-on-workshop Bärbel Junginger, B.Sc. /physiotherapist, manualtherapist (IFOMPT) Kaven Baessler, MD, PhD
Dynamic rehabilitative ultrasound for pelvic floor disorders Introduction in techniques and hands-on-workshop Bärbel Junginger, B.Sc. /physiotherapist, manualtherapist (IFOMPT) Kaven Baessler, MD, PhD
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Chronic Pelvic Pain. Bridget Kamen, MD Obstetrics and Gynecology, Confluence Health. I have no disclosures
 Chronic Pelvic Pain Bridget Kamen, MD Obstetrics and Gynecology, Confluence Health I have no disclosures Objectives A little epidemiology Understand there are both gynecologic and non-gynecologic causes
Chronic Pelvic Pain Bridget Kamen, MD Obstetrics and Gynecology, Confluence Health I have no disclosures Objectives A little epidemiology Understand there are both gynecologic and non-gynecologic causes
Personal Background. Brenau Graduate. Practicing OT for five years Specializing in pelvic floor for three years
 Personal Background Brenau Graduate Practicing OT for five years Specializing in pelvic floor for three years Learning Objectives Identify male and female pelvic floor and pelvic girdle structures List
Personal Background Brenau Graduate Practicing OT for five years Specializing in pelvic floor for three years Learning Objectives Identify male and female pelvic floor and pelvic girdle structures List
Physical Therapy Treatment for Pelvic Floor Disorders: Interventions and Home Programs
 Physical Therapy Treatment for Pelvic Floor Disorders: Interventions and Home Programs T INA M A LLEN, PT PRPC BCB - PMD U N I V E R S I T Y O F W A S H I N G T O N M E D I C A L C E N T E R H E R M A
Physical Therapy Treatment for Pelvic Floor Disorders: Interventions and Home Programs T INA M A LLEN, PT PRPC BCB - PMD U N I V E R S I T Y O F W A S H I N G T O N M E D I C A L C E N T E R H E R M A
PELVIC FLOOR WORKSHOP- LEARN AND GET TO KNOW YOUR FLOOR
 PELVIC FLOOR WORKSHOP- LEARN AND GET TO KNOW YOUR FLOOR LIFE FIT CENTER 2.22.18 DR. SHERINE AUBERT, PT, DPT, PRPC OVERVIEW What What are the functions of the pelvic floor muscles? Who Who goes to pelvic
PELVIC FLOOR WORKSHOP- LEARN AND GET TO KNOW YOUR FLOOR LIFE FIT CENTER 2.22.18 DR. SHERINE AUBERT, PT, DPT, PRPC OVERVIEW What What are the functions of the pelvic floor muscles? Who Who goes to pelvic
Intravaginal Surface Electromyography in the Diagnosis and Treatment of Vulvovaginal Pain Disorders
 FEATURE Intravaginal Surface Electromyography in the Diagnosis and Treatment of Vulvovaginal Pain Disorders Howard I. Glazer, PhD Clinical Associate Professor of Psychology in Psychiatry, Weill College
FEATURE Intravaginal Surface Electromyography in the Diagnosis and Treatment of Vulvovaginal Pain Disorders Howard I. Glazer, PhD Clinical Associate Professor of Psychology in Psychiatry, Weill College
1995 Otterbein College BS Sports Medicine 1997 Mayo Clinic Masters of Physical Therapy
 Kendra Foley, MPT Pelvic Floor Physical Therapy 1995 Otterbein College BS Sports Medicine 1997 Mayo Clinic Masters of Physical Therapy The Foley Family 2015 Pelvic Floor Physical Therapy A Highly Specialized
Kendra Foley, MPT Pelvic Floor Physical Therapy 1995 Otterbein College BS Sports Medicine 1997 Mayo Clinic Masters of Physical Therapy The Foley Family 2015 Pelvic Floor Physical Therapy A Highly Specialized
CommonKnowledge. Pacific University. Gina Clark Pacific University. Lauren Murphy Pacific University. Recommended Citation.
 Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2012 The diagnostic accuracy of patient subjective history compared to the gold standard of urodynamic testing
Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2012 The diagnostic accuracy of patient subjective history compared to the gold standard of urodynamic testing
The role of physiotherapy in sexual health: Is it evidence-based?
 JOBNAME: jacpog PAGE: 1 SESS: 4 OUTPUT: Tue May 23 15:15:05 2006 Journal of the Association of Chartered Physiotherapists in Women s Health, Autumn 2006, 99, 000 000 LITERATURE REVIEW The role of physiotherapy
JOBNAME: jacpog PAGE: 1 SESS: 4 OUTPUT: Tue May 23 15:15:05 2006 Journal of the Association of Chartered Physiotherapists in Women s Health, Autumn 2006, 99, 000 000 LITERATURE REVIEW The role of physiotherapy
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Vulvodynia / Pain. NVA RESEARCH UPDATE NEWSLETTER September 2005
 NVA RESEARCH UPDATE NEWSLETTER September 2005 www.nva.org This newsletter has been supported, in part, through a grant from the Enterprise Rent-A-Car Foundation. www.enterprise.com This newsletter is quarterly
NVA RESEARCH UPDATE NEWSLETTER September 2005 www.nva.org This newsletter has been supported, in part, through a grant from the Enterprise Rent-A-Car Foundation. www.enterprise.com This newsletter is quarterly
Sexuality and Sexual Dysfunction in Women
 Sexuality and Sexual Dysfunction in Women Denise M.S. Willers, MD Associate Professor of Obstetrics and Gynecology Washington University School of Medicine Disclosures No financial disclosures to make
Sexuality and Sexual Dysfunction in Women Denise M.S. Willers, MD Associate Professor of Obstetrics and Gynecology Washington University School of Medicine Disclosures No financial disclosures to make
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Cormie P, et al. Exercise therapy for sexual dysfunction after prostate cancer. Nat Rev Urol 2013;10(12):
 Physical Therapy and Sexual Health Care Before and After Cancer Dr Beth Shelly PT, DPT, WCS, BCB PMD All of Me Iowa Conference: Sexual Health Care in Oncology January 31, 2018 University of Iowa, Iowa
Physical Therapy and Sexual Health Care Before and After Cancer Dr Beth Shelly PT, DPT, WCS, BCB PMD All of Me Iowa Conference: Sexual Health Care in Oncology January 31, 2018 University of Iowa, Iowa
History of Present Illness Please answer the following questions
 Last Name First Name Date of Birth: / / What is the main reason for your visit today? Social Security Number: History of Present Illness Please answer the following questions Bladder Cancer Urinary Tract
Last Name First Name Date of Birth: / / What is the main reason for your visit today? Social Security Number: History of Present Illness Please answer the following questions Bladder Cancer Urinary Tract
Original article J Bas Res Med Sci 2015; 2(2): The incidence of recurrent pelvic organ prolapse: A cross sectional study
 The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
Women s and Men s Health Intake Form Comprehensive Physical Therapy Center
 Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Women's physiotherapy
 The women s health physiotherapy outpatient team treats a variety of conditions affecting women: chronic pelvic pain urinary incontinence birth-related perineal trauma antenatal and postnatal musculoskeletal
The women s health physiotherapy outpatient team treats a variety of conditions affecting women: chronic pelvic pain urinary incontinence birth-related perineal trauma antenatal and postnatal musculoskeletal
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery
 Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery Medical History Questionnaire Name: Date: Age: D.O.B. Race: What is the nature of your current gynecologic or urologic medical
Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery Medical History Questionnaire Name: Date: Age: D.O.B. Race: What is the nature of your current gynecologic or urologic medical
WELCOME TO COMPLETE WELLNESS CLINIC Take the first step to wellness!
 WELCOME TO COMPLETE WELLNESS CLINIC Take the first step to wellness! Your first appointment involves an assessment by a Registered Physiotherapist. Please read our website for more information. You may
WELCOME TO COMPLETE WELLNESS CLINIC Take the first step to wellness! Your first appointment involves an assessment by a Registered Physiotherapist. Please read our website for more information. You may
Todd Martin, PT Jared Bailey, PT Samantha Stollberg, PT, PRPC Karen Bailey, PT John Hollinshead, PT Sarada Bird, DPT Adrian Asencio, OTR/L, CHT
 Adrian Asencio, OTR/L, CHT Please fill out the enclosed forms and bring them with you to your first appointment. At that time, we will do a brief examination of your pelvic floor muscles, and you are welcome
Adrian Asencio, OTR/L, CHT Please fill out the enclosed forms and bring them with you to your first appointment. At that time, we will do a brief examination of your pelvic floor muscles, and you are welcome
Surgical treatment of urinary stress incontinence with tension free vaginal tape
 Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Pelvic floor weakness
 Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
How cancer treatments may affect your vagina How a vaginal dilator may help you How to use vaginal dilators Where to buy vaginal dilators
 SYMPTOM MANAGEMENT Vaginal Dilators Information for Patients In this document you will learn about: How cancer treatments may affect your vagina How a vaginal dilator may help you How to use vaginal dilators
SYMPTOM MANAGEMENT Vaginal Dilators Information for Patients In this document you will learn about: How cancer treatments may affect your vagina How a vaginal dilator may help you How to use vaginal dilators
Chronic Pelvic Pain Case Study
 Case Study Chronic Pelvic Pain Case Study Melissa, a 28 year old veteran comes to your office complaining of lower abdominal pain for the past 6 months. She has tried acetaminophen and ibuprofen but they
Case Study Chronic Pelvic Pain Case Study Melissa, a 28 year old veteran comes to your office complaining of lower abdominal pain for the past 6 months. She has tried acetaminophen and ibuprofen but they
The pelvic floor muscles (PFM) form
 Correlation of Digital Palpation and Transabdominal Ultrasound for Assessment of Pelvic Floor Muscle Contraction Amir Massoud Arab, PT, PhD 1 ; Roxana Bazaz Behbahani, PT, BSc 2 ; Leila Lorestani, PT,
Correlation of Digital Palpation and Transabdominal Ultrasound for Assessment of Pelvic Floor Muscle Contraction Amir Massoud Arab, PT, PhD 1 ; Roxana Bazaz Behbahani, PT, BSc 2 ; Leila Lorestani, PT,
Case L.M. Question 1 4/17/2013. Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin
 Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin Case L.M. L.M. is a 46 yo G0 woman who presents with a 3 year history of worsening pelvic pain. She has a h/o endometriosis
Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin Case L.M. L.M. is a 46 yo G0 woman who presents with a 3 year history of worsening pelvic pain. She has a h/o endometriosis
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Prolapse & Urogynaecology. Hester Mannion and Fabi Sica
 Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
FEMALE INTAKE INFORMED CONSENT FOR ASSESSMENT OF PELVIC FLOOR DYSFUNCTIONS
 Date: FEMALE INTAKE INFORMED CONSENT FOR ASSESSMENT OF PELVIC FLOOR DYSFUNCTIONS Pelvic floor dysfunctions include pelvic pain syndromes, urinary incontinence, fecal incontinence, dyspareunia or pain with
Date: FEMALE INTAKE INFORMED CONSENT FOR ASSESSMENT OF PELVIC FLOOR DYSFUNCTIONS Pelvic floor dysfunctions include pelvic pain syndromes, urinary incontinence, fecal incontinence, dyspareunia or pain with
Dr. Maliheh Keshvari
 1 Dr. Maliheh Keshvari Assistant professor of Urology Fellowship in Female Urology Mashhad University of Medical Sciences 2 Female Sexual Function and Dysfunction 3 It was not until recently that urologists
1 Dr. Maliheh Keshvari Assistant professor of Urology Fellowship in Female Urology Mashhad University of Medical Sciences 2 Female Sexual Function and Dysfunction 3 It was not until recently that urologists
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre
 PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre Chronic Pelvic Pain What is Chronic Pelvic Pain? Chronic pelvic pain refers to pain in the lower half of your abdomen, lasting six months,
PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre Chronic Pelvic Pain What is Chronic Pelvic Pain? Chronic pelvic pain refers to pain in the lower half of your abdomen, lasting six months,
Vestibulodynia Terminology Clinical features of the disease Ethiopatogenesis Treatment Multidisciplinary vulvar clinic Vestibulectomy
 From Pain to Pleasure Surgical Treatment of Vestibulodynia Päivi Tommola Specialist in Gynecology 13.10.2010 GKS Vestibulodynia Terminology Clinical features of the disease Ethiopatogenesis Treatment Multidisciplinary
From Pain to Pleasure Surgical Treatment of Vestibulodynia Päivi Tommola Specialist in Gynecology 13.10.2010 GKS Vestibulodynia Terminology Clinical features of the disease Ethiopatogenesis Treatment Multidisciplinary
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Tips & Tricks for Usage
 Life. Not leaks. BLADDER SUPPORT FOR WOMEN Tips & Tricks for Usage Based on feedback from users and clinicians, here are some questions and answers that might help with using your uresta bladder support
Life. Not leaks. BLADDER SUPPORT FOR WOMEN Tips & Tricks for Usage Based on feedback from users and clinicians, here are some questions and answers that might help with using your uresta bladder support
Provenance Rehabilitation Pelvic Intake Form
 Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
Pelvic floor muscle pain: Outcome Measures, Tues 4th Sep 2012
 Pelvic floor muscle pain: Outcome Measures, Tues 4th Sep 2012 Helena Frawley, PhD, FACP Senior Lecturer, NH&MRC Research Fellow, The University of Melbourne Study / treatment end-points (Turk et al 2006)
Pelvic floor muscle pain: Outcome Measures, Tues 4th Sep 2012 Helena Frawley, PhD, FACP Senior Lecturer, NH&MRC Research Fellow, The University of Melbourne Study / treatment end-points (Turk et al 2006)
Compassionate and effective management
 IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
Pelvic Dysfunction: The Missing Link. Raza Awan, MD
 Pelvic Dysfunction: The Missing Link Raza Awan, MD Disclosures None Housekeeping Thank You Objectives By the end of this session participants will be able to: Identify the link between non-resolving low
Pelvic Dysfunction: The Missing Link Raza Awan, MD Disclosures None Housekeeping Thank You Objectives By the end of this session participants will be able to: Identify the link between non-resolving low
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
ICD-10 Common Codes for Pelvic Rehab Providers
 ICD-10 Common Codes for Pelvic Rehab Providers With ICD-10 changes taking place in 2015, we thought it would be helpful to put together a bit of a cheat sheet for our pelvic health providers. Keep in mind
ICD-10 Common Codes for Pelvic Rehab Providers With ICD-10 changes taking place in 2015, we thought it would be helpful to put together a bit of a cheat sheet for our pelvic health providers. Keep in mind
Prevalence and risk factors for pelvic floor symptoms in women in rural El Salvador
 Int Urogynecol J (2007) 18:1065 1069 DOI 10.1007/s00192-006-0292-6 ORIGINAL ARTICLE Prevalence and risk factors for pelvic floor symptoms in women in rural El Salvador Begüm Özel & Anne Marie Borchelt
Int Urogynecol J (2007) 18:1065 1069 DOI 10.1007/s00192-006-0292-6 ORIGINAL ARTICLE Prevalence and risk factors for pelvic floor symptoms in women in rural El Salvador Begüm Özel & Anne Marie Borchelt
Pelvic Floor Muscle Exercises
 INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
Inside: Incontinence, Chronic Pelvic Pain, & Physical Therapy
 Health & Physical Therapy The Newsletter About Your Health And Caring For Your Body Don t Suffer From Pain Incontinence, Chronic Pelvic Pain, & Physical Therapy Inside: Incontinence, Chronic Pelvic Pain
Health & Physical Therapy The Newsletter About Your Health And Caring For Your Body Don t Suffer From Pain Incontinence, Chronic Pelvic Pain, & Physical Therapy Inside: Incontinence, Chronic Pelvic Pain
By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT, DPT, LAT, CSCS
 The Outcomes Following the Implementation of a Pelvic Floor Contraction with Lumbar Stabilization Exercises for a Patient with Low Back Pain: A Case Report By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT,
The Outcomes Following the Implementation of a Pelvic Floor Contraction with Lumbar Stabilization Exercises for a Patient with Low Back Pain: A Case Report By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT,
Sexual Function in Women with Urinary Incontinence Treated by Pelvic Floor Transvaginal Electrical Stimulation
 Blackwell Publishing IncMalden, USAJSMJournal of Sexual Medicine1743-6095 2006 International Society for Sexual Medicine200743702707Original ArticleWomen Affected by UI and WSD Treated by TESGiuseppe et
Blackwell Publishing IncMalden, USAJSMJournal of Sexual Medicine1743-6095 2006 International Society for Sexual Medicine200743702707Original ArticleWomen Affected by UI and WSD Treated by TESGiuseppe et
Nivedita Dhar M.D. Wayne State University April 25, 2013
 Female Sexual Dysfunction Nivedita Dhar M.D. Wayne State University April 25, 2013 Outline Define Sexual Health and Wellness and discuss how it is unique to each individual Discuss the current terminology
Female Sexual Dysfunction Nivedita Dhar M.D. Wayne State University April 25, 2013 Outline Define Sexual Health and Wellness and discuss how it is unique to each individual Discuss the current terminology
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
AAPI S NUTRITION GUIDE TO OPTIMAL HEALTH: USING PRINCIPLES OF FUNCTIONAL MEDICINE AND NUTRITIONAL GENOMICS PART 2
 33 Pelvicology: A Neuro Muscular Skeletal Approach to the Treatment of Pelvic Conditions Marilyn Freedman, PT, DPT, CAPP, BCB- PMB TM Riva Preil, MS, PT, DPT Introduction: Traditionally the care of patients
33 Pelvicology: A Neuro Muscular Skeletal Approach to the Treatment of Pelvic Conditions Marilyn Freedman, PT, DPT, CAPP, BCB- PMB TM Riva Preil, MS, PT, DPT Introduction: Traditionally the care of patients
Myofascial Pelvic Pain
 AACP MUSCULOSKELETAL ROADSHOW Myofascial Pelvic Pain Jennie Longbottom MSc BSc MCSP MBAcC Misdiagnosis is the common cause for patients to seek multiple physicians, to undergo pharmacological, psychological
AACP MUSCULOSKELETAL ROADSHOW Myofascial Pelvic Pain Jennie Longbottom MSc BSc MCSP MBAcC Misdiagnosis is the common cause for patients to seek multiple physicians, to undergo pharmacological, psychological
Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566
 Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
Education. Doctorate, Physical Therapy 2013 Pacific University, School of Physical Therapy Forest Grove, Oregon
 MJ (Mary Jane) Strauhal PT, DPT, BCB-PMD Program Lead Clinical Advancement Program- Pelvic Health Rehabilitation Services Department Providence St. Vincent Medical Center 9135 SW Barnes Road #362 Portland,
MJ (Mary Jane) Strauhal PT, DPT, BCB-PMD Program Lead Clinical Advancement Program- Pelvic Health Rehabilitation Services Department Providence St. Vincent Medical Center 9135 SW Barnes Road #362 Portland,
Why Kegels Don t Work by Christine Kent, RN
 Why Kegels Don t Work by Christine Kent, RN Please share by clicking the links below: 1 Why Kegels Don t Work by Christine Kent The concept that prolapse and incontinence can be improved by doing reps
Why Kegels Don t Work by Christine Kent, RN Please share by clicking the links below: 1 Why Kegels Don t Work by Christine Kent The concept that prolapse and incontinence can be improved by doing reps
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
The development of a questionnaire to measure the severity of symptoms and the quality of life before and after surgery for stress incontinence
 BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital
 Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
