The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (9), Page
|
|
|
- Quentin McKinney
- 5 years ago
- Views:
Transcription
1 The Egyptian Journal of Hospital Medicine (October 218) Vol. 73 (), Page Ayman Helmy Ibrahim, Abdel Wahab M. Abdel Wahab, Karim A. Abdel Rahman Ali Department of General Surgery, Faculty of Medicine, Al Azhar University Corresponding author: Ayman Helmy Ibrahim, ABSTRACT Background: laparoscopic cholecystectomy has become the procedure of choice for treatment of patients with gall stones. The routine placement of drains becomes a part of this operation for a long period of time. However, controversy has surrounded this practice in elective conventional cholecystectomies, with most surgeons departing from this approach. Aim of the Work: this study aimed to assess the value of the drain in uncomplicated laparoscopic cholecystectomy and if the insertion of a drain should be routinely done or not. Patients and Methods: this study was conducted at AL-Azhar University Hospitals in Cairo (Al Hussien and Bab Al Shaaria Hospitals), Kafr Al-Sheikh General Hospital and Biala Central Hospital on 18 patiants presented to general surgery clinic with gall stone disease. Patients were randomized into two groups and both groups underwent laparoscopic cholecystectomy, group A ( patients) received a drain in gall bladder bed and group B ( patients) receivd no drain. Postoperative mortalities and morbidities shuch as pain, nausea, vomiting, fever, abdominal collection, wound infection, need for analgesics and time of discharge from hospital were assessed. Statistical analysis was performed. Mean and standard deviation were estimated for each continuous variable. Results: there was no mortality in either groups and no statistically significant difference in postoperative pain, nausea, vomiting, wound infection or abdominal collection between the two groups. However, hospital stay was longer in the drain group than in group without drain. Conclusion: our study suggested that insertion of drain should not be routinely done in elective laproscopic cholecystectomy as it has no significant effect on postoperative morbidity, moreover, it delays hospital discharge. Keywords: drain, laparoscopic cholecystectomy. INTRODUCTION Laparoscopic cholecystectomy (LC), after its advent in 187, was rapidly established itself as the gold standard treatment of gallstones. Arguments of drainage from open era continue into the laparoscopic era, with another factor, that is, pneumoperitoneum being questioned (1). Laparoscopic cholecystectomy provides a safe and effective treatment for patients with gallstones as it reduces post operative pain with almost inadvisable scar, short hospital stay and earlier return to work (2).On the other side, patiants complain of abdominal pain, shoulder tip pain and nausea/vomiting post-opetatively (3).High pressure pneumoperitoneum using carbon dioxide gas was accused for those complications, thus a drain tube is inserted (4).The value of surgical drainage in open cholecystectomy is an issue that is not resolved till now (5). The same occurs in laparoscopic cholecystectomy, where the lack of evidence on usefulness of drain is present. Again surgeons keep being divided among those placing a drain selectively and those who never place a drain, based on their personal experience, beliefs or bias (6).Routine drain use after laparoscopic cholecystectomy is still debatable. The main indication for drain use after laparoscopic cholecystectomy is to prevent a biloma or hematoma. According to the Cochrane Database Systemic Review, randomized clinical studies show no benefit of a drain. Some studies even claim that drains are harmful. The tendency of surgeons to use or not use drains seems to be a matter of habit and experience (6). AIM OF THE WORK This study aimed to assess the value of the drain in uncomplicated laparoscopic cholecystectomy and if insertion of adrain should be routinely done or not. PATIENTS AND METHODS This work was conducted at AL Azhar University Hospitals in Cairo (Al Hussien and Bab Al Shaaria Hospitals), Kafr Al-Sheikh General Hospital and Biala Central Hospital. The study included 18 patiants presented to general surgery clinic with gall stone disease from May 215 to July 218. Type of study: this study was a prospective clinical study. Inclusion criteria: 1. Patients who would not had acute cholecystitis, cholangitis or pancreatitis. 2. Patients who would not had any contraindication for laparoscopic approach. 3. Patients who would not required common bile duct exploration or any other additional procedure. Exclusion criteria: 1. Patients who refused to enter the study. 2. Patients who have chronic liver diseases or bleeding tendency Received://218 Accepted:28//
2 3. Patients with previous episode(s) of acute cholecystitis, cholangitis, or pancreatitis in their history had not been included. MATERIALS AND METHODS 18 patients were simply randomized blindly before surgical procedure into two groups and both groups underwent laparoscopic cholecystictomy.group A of patients received a gravity drain in gall bladder bed and group B ( patients) receivd no drain.although entrance into the trial was decided before surgery, the randomization arm had only been notified to the operating team after the completion of the cholecystectomy and just before closure of the wound. Informed consent had been obtained from all patiants and they had been told that there was a possibility to converted to open surgery (if there is a difficulty in laparoscopic procedure) and the trial protocol had been approved by the institutional ethics committee.the procedure was performed by the same team of surgeons. All patients were given a single use of antibiotic prophylaxis (cefuroxime 75 mg) intravenously and postoperative analgesia (Diclofenac sodium 75 mg) intramuscularly. Postoperative pain assessment was performed using a visual analog scale (VAS) with which each patient noted the severity of pain, using a linear scale between zero (no pain) and 1 (strongest conceivable pain). Abdominal drainage was assessed in terms of quantity and quality of drainage. Abdominal ultrasonography was done only to patients suspected to have collection (if they had persistent shoulder pain, fever, elevated leucocytic count and/or persistent vomiting).statistical analysis was performed. Mean and standard deviation were estimated for each continuous variable. Independent t-test was used for detection of difference between the two means. Differences were considered significant when P >.5. RESULTS Statistical analysis of the data Data were fed to the computer using IBM SPSS software package version 2.. Qualitative data were described using number and percent. Comparison between different groups regarding categorical variables was tested using Chi-square test. Quantitative data were described by using mean and standard deviation for normally distributed data while abnormally distributed data was expressed using median, minimum and maximum. For normally distributed data, comparison between two independent population were done using independent t-test while, more than two population were analyzed F-test (ANOVA) to be used.significance test results were quoted as twotailed probabilities. RESULTS Table 1 showed that there was no statistical significant difference between the two studied groups regarding gall bladder conditions (P >.5). Table 1: comparison between the two studied groups regarding gall bladder conditions Gall bladder wall Mild increase Thick wall Gall bladder Stones Multiple tiny stone Solitary mobile stone Large solitary stone Table 2 showed that there was no statistical significant difference between the two studied groups regarding liver status, history of previous attack of acute cholicystitis, positive Murphy's sign and bile leakage (P >.5). 7616
3 Ayman Ibrahim et al. Table 2: comparison between the two studied groups regarding liver status, history of previous attack of acute cholicystitis, positive Murphy's sign and bile leakage Liver status Fatty Cirrhotic History of previous attack of acute cholicystitis Positive Murphy's sign Table 3 showed that there was no statistical significant difference between the two studied groups regarding time of procedure, dull aching pain in the right hypochondrium, fatty dyspepsia following meals, recurrent attacks of biliary colic and patient with calcular obstructive jaundice (P >.5). Table 3: comparison between the two studied groups regarding time of procedure, dull aching pain in the right hypochondrium, fatty dyspepsia following meals, recurrent attacks of biliary colic and patient with calcular obstructive jaundice Dull aching pain in the right.88 hypochondrium Fatty dyspepsia following meals Recurrent attacks of biliary colic Patient with calcular obstructive jaundice.. Table 4 showed that there was statistical significant difference between the two studied groups regarding analgesia and shoulder pain. Table 4: comparison between the two studied groups regarding analgesia and shoulder pain Analgesia 1-2 Multiple Shoulder pain No Yes *.1* Table 5 showed that there was no statistical significant difference between the two studied groups regarding hemodynamic data (P >.5). Table 5: comparison between the two studied groups regarding hemodynamic data Pulse Tachycardia Temp. Mild fever TLC Abnormal
4 Table 6 showed distribution of group A regarding the drain characteristics Table 6: distribution of group A regarding the drain characteristics Drain amount Significant Not significant Drain nature Serosanguinos Bloody Group A No. % Table 7 showed that there was no statistical significant difference between the two studied groups regarding postoperative radiological findings (P >.5). Table 7: comparison between the two studied groups regarding postoperative radiological findings Abdominal U/S No collection Rim of Free fluid X-ray Not done No sub phrenic air Table 8 showed that there was statistical significant difference regarding to stay at hospital (P <.5) while there was no statistical significant difference regarding postoperative wound infection (P >.5). Table 8: comparison between the two studied groups regarding postoperative wound infection and stay at hospital Postoperative wound infection No Yes Stay at hospital (days) Range Mean S.D * DISCUSSION Laparoscopic cholecystectomy was the procedure of choice for treatment of patients with gall stones (6).When Langenebuch performed the first cholecystectomy in 1882, he placed a peritoneal drain as a part of the procedure. The routine placement of drains becomes a part of this operation for a long period of time. However, controversy has surrounded this practice in elective conventional cholecystectomies, with most surgeons departing from this approach (8).Since laparoscopic cholecystectomy was introduced as an alternative to the conventional removal of the gallbladder, the issue of routine drainage needed reevaluation (2). In a study conducted by Hawasli and Brown () on 48 patients underwent laparoscopic cholecystectomy with placement of routine closed suction drain in the gallbladder bed in all patients, bile leakage was encountered in five patients and bleeding in three patients. None of the patients with bile drainage developed bile peritonitis or required reoperation; one patient with bleeding required an operation to control the oozing from the liver bed. Two of the patients had bile drainage secondary to cystic duct leak treated by endoscopic retrograde cholangiography (ERCP), two patients had 7618
5 Ayman Ibrahim et al. moderate bile drainage that ceased in 3 and 4 days and the fifth patient was discharged home in 23 h with the drain then drainage stopped in 2 days. No source of this drainage was established. All these drains were removed in the office after 3 weeks. Three patients had blood in the drain, one an unsuspected cirrhotic patient who required reoperation the next day due to continuous oozing from the liver bed. The second patient, who had chronic renal failure, was treated conservatively. The third patient with bleeding was monitored. He was discharged 3 days later. Hawasli and Brown () concluded that using a closed suction drainage after laparoscopic cholecystectomy results in no postoperative morbidity and prevens definite exploratory laparotomy in patients with cystic duct leak. In addition, use of closed suction drainage helped in early diagnosis of postoperative bleeding in three patients (). In our study, significant postoperative drainage occurred in patient, no patient required re-exploration for bleeding. In those operations the available diathermy was cutting only, however there was nothing obviously abnormal during the operation. One of those patients developed mild dyspnea, fever 38 and tachycardia 1, TLC was 8,, drain amount only 1cc.Next day abdominal U/S and Hb% were done for the patient and revealed that: Hb% was 1.2 gm%, and abdominal U/S revealed: - A small rim of collection in the hepatorenal pouch. - Minimal Fluid collection in the pelvis. The patient admitted under observation and to follow up vital signs Two days later abdominal U/S revealed no collection. In our study, in group A only three patients had small rim of free fluid in the abdomen and in group B five patients had a small rim of free fluid, in four of them the small rim disappeared after two days in the abdominal ultrasound but in the fifth patient the rim of free fluid still present and we made ultrasound guided fluid aspiration from th abdomen and the next abdominal ultrasound was free.there was no mortality in any group and no statistically significant difference in postoperative pain, nausea and vomiting, wound infection or abdominal collection between the two groups. However, hospital stay was longer in the drain group than in group without drain and it is appearing that the use of drain delays hospital discharge (1). In a study conducted by Hawasli and Brown () on 1 patients underwent elective laparoscopic cholecystectomy and they were categorized into 2 groups; group 1 patients (n=5) had a drain placed through the epigastric trocar site. Group 2 patients (n=5) did not have a drain. There was no wound infection or postoperative fever in every group. In another study carried out by Panzera et al. (11) on 8 patients, they had 12 cases (1.2%) of infection of the umbilical wound (11). In a study conducted by Champault et al. (12) on 112 patients, they had only one patient (.%) who had developed an umbilical abscess 7 days after the operation and was drained spontaneously (12).In our study, no wound infection occurred in any patient. In our study, nine patients of group A and nine patients of group B had mild postoperative fever; one of them was the case that had significant post operative drainage. Hawasli and Brown () in their study they found that there were minor with no statistically significant differences between group 1 and group 2 in postoperative severity and duration of abdominal pain shoulder pain and nausea. Likewise, Lewis et al. (5) found no increased morbidity in a prospective controlled randomized study of the short-term placement of a drain in simple cholecystectomy.in our study; all patients in group A needed multiple doses of analgesics for the first day but all patients of group B needed one or two doses of analgesics. In those patients with multiple doses the postoperative ultrasound revealed small rim of free fluid in hepatorenal pouch. With the advent of laparoscopic cholecystectomy, the incidence of bile duct injuries and hence, bile collections in the abdomen, has increased (13). Lee (13) found that most patients with bile collections did not present with peritonitis; instead, they had bile ascitis, with mild, relatively non-specific symptoms. Among the series of his patients, the correct diagnosis was missed initially in 77% of patients. The important points of this study are that once a bile collection has been drained, the major potential for immediate serious illness has usually been eliminated. This allows the injury to be fully delineated and treatment to be planned and carried out in an unhurried manner.in another study conducted by Albasini et al. (14) on a series of 5 laparoscopic cholecystectomies, in which both operative cholangiography and drainage of the gallbladder bed were routine, bile leakage was identified in ten patients (2%). There was no bile duct injury. Nine of the ten patients presented with bile in the drain within 24 h. of operation and one patient presented 1 week after operation with a subphrenic collection. Of the ten patients, five settled spontaneously. Of the five remaining patients, two needed laparotomy- one for a subphrenic collection not responding to percutaneous drainage and one for biliary peritonitis. One patient was treated by relaparoscopy and suture of a duct of Luschka and one patient had successful percutaneous drainage of an infected collection; the fifth patient who 761
6 presented with a late subphrenic collection of bile was shown at endoscopic retrograde cholangiopancreatography (ERCP) to have a cystic duct stump leak and was treated with an endoscopic stent.albasini et al. (14) believed that use of routine gallbladder bed drainage was justified for this reason alone. In a retrospective analysis of personnel experience of Panzera et al. (11) with laparoscopic cholecystectomy, compared to the literature on the subject, he presented the data of 8 laparoscopic cholecystectomies they had performed. They had 3 cases with injury of the biliary tracts, which did not occur during the training period, contrary to what quoted in the literature. Also there were 2 cases of postoperative bleeding (1 from cystic artery and 1 from the umbilical wound). They suggested the use of a systematic sub hepatic drainage during the first 24 postoperative hours, since it can be useful to reveal possible bleeding (11). In our study, there were no cases with injury of the biliary tracts. No bile was encountered in the drain or detected in postoperative abdominal U/S. During laparoscopic cholecystectomy the gallbladder was inadvertently entered and stones were spilled. Although this complication is not unique to LC, spillage of stones is probably more common than during open surgery. Spillage of the stones from the gallbladder can occur during mobilization of the gallbladder from gallbladder bed, during manipulation of the cystic duct in preparation for intra operative cholangiogram, or during removal of the gallbladder through the abdominal wall (7). In case report of Zamir et al. (7) they described four patients who presented with complications associated with dropped gallstones. In their study they confirmed the potential danger of spilled gall stones. Spilled gall stones not only caused intraperitoneal adhesions but also resulted in abscess formation. The infective complications described can be divided into two major categories. The first was the formation of trocar site abscess with late discharge of a stone either spontaneously or during subsequent wound exploration.the second category of complications was the formation of intraperitoneal abscesses. These abscesses usually formed in the sub hepatic or subphrenic spaces.these complications can become manifest at a very late stage after surgery ranging from 1 to 14 months postoperative.in another case report study by Bandyopadhyay (15) reported a case of late and recurrent subphrenic abscess following LC in a 65-year-old gentleman who underwent LC in 11. He presented 3 years and even 1 years after the operation with subphrenic abscess. Bandyopadhyay recommended surgical open drainage as opposed to percutaneous drainage. The author also stressed on taking precautions to avoid spillage of stones (15).Also another case report study of Papasavas et al. (16) they treated a 77-year-old woman who underwent laparoscopic cholecystectomy. Subsequently, a right flank abscess developed. During the cholecystectomy, the gallbladder was perforated and stones were spilled. After a failed attempt to drain the abscess percutaneously, the patient required open drainage, which revealed retained gallstones in the right flank.in our study, 28 patients had intraoperative gallbladder injury with spilled stones in which the stones were totally extracted in 4 patients and most of the stones were extracted in the other cases. A study of Voitk (17) was conducted on 1 patients booked for elective laparoscopic cholecystectomy on an outpatient basis, 4 were successfully treated as outpatients who spent an average of less than 6 hours in hospital. Six patients required postoperative admission, four because of conversion to open operation, staying an average of 2.8 days in hospital. One patient was admitted because of persistent postoperative hypoxia due to atelectasis and one elderly lady because she failed to arrange for someone to stay with her for the first postoperative night; the last stayed 1 day each.there were two later complications: one patient was readmitted 3 weeks after surgery for percutaneous drainage of a right subphrenic abscess and one patient was readmitted 8 months postoperatively for repair of an incisional hernia at the umbilicus. None of the 2 readmissions were related to the outpatient status.this study confirmed that about % of all elective cholecystectomies can be done as outpatients, both safely and with good patient acceptance (17).In our study, all patients in group A discharged on the third or fourth day postoperative and all patients in group B discharged on the second day except for two patient there post operative ultrasound shows small rim of free fluid in the hepatorenal pouch they discharged at the fourth day. CONCLUSION From the results of our study we can come to a conclusion that there was no mortality in either group and no statistically significant difference in postoperative pain, nausea and vomiting, wound infection or abdominal collection between the two groups. However, hospital stay was longer in the drain group than in group without drain and it is appearing that the use of drain delays hospital discharge, also use of analgesia was more in the drained group than in group without drain, also th pain (specialy shoulder pain) was more in the drained group than in the group without drain, so 762
7 Ayman Ibrahim et al. drainage could not be considered a routine use for uncomplicated cases. REFERENCES 1. Dubois F (15): Laparoscopic cholecystectomy, the French technique. In: Operative Strategies in Laparoscopic Surgery. Phillips EH, Rosenthal RJ, Berlin, Heidel-Bery and New York.pp: Louis S (11): Surgical laparoscopy.in: Laparscopic Equipment and Instrument. Talamini MA, Gadacz TR. Quality Medical Publishing Inc. London,USA.pp: Sarli L, Costi R, Sansebastiano G, Trivelli M and Roncoroni L (2): Prospective randomized trial of low-pressure pneumoperitoneum for reduction of shoulder-tip pain following laparoscopy. Br. J. Surg., 87: Abbott J, Hawe J, Srivastava P, Hunter D and Garry R (21): Intraperitoneal gas drain to reduce pain after laparoscopy. Obstet Gynecol., 8: Lewis RT, Goodall RG, Marien B, Park M, Lloyd- Smith W and Wiegand FM (1): Simple elective cholecystectomy.am. J. Surg., 15: PSanjay C, Polignano F and Tait I (25): Survey of current surgical treatment of gall stones in Queensland. Aust. NZJ Surg., 75: G. Zamir S, Lyass D and Pertsemlidis B (1): The fate of the dropped gallstones during laparoscopic cholecystectomy.surgical Endoscopy, 13: Ko S and Airan M (11): Review of 3 consecutive laparoscopic cholecystectomies: development, evolution and results. Surgical Endoscopy, 5(3): Hawasli A and Brown E (14): The effect of drains in laparoscopic cholecystectomy. J.Laparoscpic Surg., 4(6): Khan, H Jan, HK Wazir, M Salman, T Saeed and Pak J (212): Laparoscopic Cholecys- tectomy. J. Minim Access Surg., 8(3): Panzera F, Ghisio S, Grosso A, Vigezzi P, Vitale M, Cariaggi RM and Mistrangelo M (2): Laparoscopic cholecystectomy. Minerva Chirurgica, 55(7-8): Champault A, Vons C, Dagher I, Amerlinck S and Franco D (2): Low-cost laparoscopic cholecystectomy. Br. J. Surg., 87: Lee CM, Stewart L and Way LW (2): Postcholecystectomy abdominal bile collections. Arch. Surg., 135(5): Albasini JL, Aledo VS, Dexter SP, Marton J, Martin IG and McMah M (15): Bile leakage following laparoscopic cholecystectomy. Surg. Endosc., (12): Bandyopadhyay D (22): The stones. J.Surg. Endosc., 16(1): Papasavas KN, Canna F, Adaba E, Sezen A, Bissett G and Ihedioha U (217): Para-spinal abscess following gallstones spillage during laparoscopic cholecystectomy: an unusual presentation. J. Surg. Case Rep., 3: Voitk A J (16): Outpatient cholecystectomy. J. Laparoendosc. Surg., 6:
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
Study of post cholecystectomy biliary leakage and its management
 Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 )
 Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
Comparative Study of Outcomes of Early Versus Interval Laparoscopic Cholecystectomy in Acute Calculus Cholecystitis.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 68-73 www.iosrjournals.org Comparative Study of Outcomes of Early
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 68-73 www.iosrjournals.org Comparative Study of Outcomes of Early
Pre-operative prediction of difficult laparoscopic cholecystectomy
 International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study
 Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Laparoscopic Cholecystectomy: A Retrospective Study
 Bahrain Medical Bulletin, Vol. 37, No. 3, September 2015 Laparoscopic Cholecystectomy: A Retrospective Study Abdullah Al-Mitwalli, LRCPI, LRCSI* Martin Corbally, MBBCh, BAO, MCh, FRCSI, FRCSEd, FRCS**
Bahrain Medical Bulletin, Vol. 37, No. 3, September 2015 Laparoscopic Cholecystectomy: A Retrospective Study Abdullah Al-Mitwalli, LRCPI, LRCSI* Martin Corbally, MBBCh, BAO, MCh, FRCSI, FRCSEd, FRCS**
JMSCR Volume 03 Issue 05 Page May 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Comparison of 3-Port Versus 4-Port Laproscopic Cholecystectomy- A Prospective Comparative Study Authors Shekhar Gogna 1, Priya Goyal 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Comparison of 3-Port Versus 4-Port Laproscopic Cholecystectomy- A Prospective Comparative Study Authors Shekhar Gogna 1, Priya Goyal 2,
Gallstones and Cholecystectomy Information Sheet
 Gallstones and Cholecystectomy Information Sheet Gallstones & Cholecystectomy This information sheet desrcibes what they are, the treatment options, and what to expect following a operation. The following
Gallstones and Cholecystectomy Information Sheet Gallstones & Cholecystectomy This information sheet desrcibes what they are, the treatment options, and what to expect following a operation. The following
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010
 Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
ABDOMINAL WALL HAEMATOMA COMPLICATING LAPAROSCOPIC CHOLECYSTECTOMY
 HPB Surgery, 1994, Vol. 7, pp. 291-296 Reprints available directly from the publisher Photocopying permitted by license only (C) 1994 Harwood Academic Publishers GmbH Printed in the United States of America
HPB Surgery, 1994, Vol. 7, pp. 291-296 Reprints available directly from the publisher Photocopying permitted by license only (C) 1994 Harwood Academic Publishers GmbH Printed in the United States of America
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Current Perspective of Laparoscopic Cholecystectomy for Acute Cholecystitis
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (7), Page 4885-4893 Current Perspective of Laparoscopic Cholecystectomy for Acute Cholecystitis Abdelghany Mahmoud AlShamy, Karim Fahmy Abd
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (7), Page 4885-4893 Current Perspective of Laparoscopic Cholecystectomy for Acute Cholecystitis Abdelghany Mahmoud AlShamy, Karim Fahmy Abd
Laparoscopic Cholecystectomy in Acute Cholecystitis :An Experience with 100 cases
 ORIGINALARTICLE Laparoscopic Cholecystectomy in Acute Cholecystitis :An Experience with 100 cases Rajni Bhardwaj, M.R.Attri, Shahnawaz Ahangar Abstract This study was undertaken to evaluate our experience
ORIGINALARTICLE Laparoscopic Cholecystectomy in Acute Cholecystitis :An Experience with 100 cases Rajni Bhardwaj, M.R.Attri, Shahnawaz Ahangar Abstract This study was undertaken to evaluate our experience
Samir Deolekar, Bhushankumar A. Thakur*, Bhushan Jajoo, Parnika R. Shinde
 International Surgery Journal Deolekar S et al. Int Surg J. 2017 Feb;4(2):514-518 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20164793
International Surgery Journal Deolekar S et al. Int Surg J. 2017 Feb;4(2):514-518 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20164793
Evaluation of complications and conversion rate of laparoscopic cholecystectomy in Rural Medical College
 Original article Evaluation of complications and conversion rate of laparoscopic cholecystectomy in Rural Medical College Satish Kumar Bansal 1, Sandeep Kumar Goyal 1, Umesh Kumar Chhabra 1, Pawan Kumar
Original article Evaluation of complications and conversion rate of laparoscopic cholecystectomy in Rural Medical College Satish Kumar Bansal 1, Sandeep Kumar Goyal 1, Umesh Kumar Chhabra 1, Pawan Kumar
Retrieval of Gallbladder through Subxiphoid V/S Supraumbilical Port in Laparoscopic Cholecystectomy.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 8 Ver. 4 (August. 2018), PP 36-41 www.iosrjournals.org Retrieval of Gallbladder through Subxiphoid
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 8 Ver. 4 (August. 2018), PP 36-41 www.iosrjournals.org Retrieval of Gallbladder through Subxiphoid
Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study
 Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Laparoscopic cholecystectomyy
 Laparoscopic cholecystectomyy What is the gall bladder? The gallbladder is a small pear sized organ that stores bile. Bile is necessary for the digestion of fatty food. The bile duct is a tube that carries
Laparoscopic cholecystectomyy What is the gall bladder? The gallbladder is a small pear sized organ that stores bile. Bile is necessary for the digestion of fatty food. The bile duct is a tube that carries
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
Comparison between primary closure and T-tube drainage after open choledocotomy
 ISSN: 2203-1413 Vol.03 No.04 Comparison between primary closure and T-tube drainage after open choledocotomy Alireza Barband 1, Farzad Kakaei 1, Morteza Ghojazadeh 2, Abdolhamid Chavoshi Khamneh 1*, Morteza
ISSN: 2203-1413 Vol.03 No.04 Comparison between primary closure and T-tube drainage after open choledocotomy Alireza Barband 1, Farzad Kakaei 1, Morteza Ghojazadeh 2, Abdolhamid Chavoshi Khamneh 1*, Morteza
Guidelines for Laparoscopic CBD Exploration
 Guidelines for Laparoscopic CBD Exploration INDICATIONS Since the 1992 National Institutes of Health Consensus Development Conference Statement on Gallstones and Laparoscopic Cholecystectomy the indications
Guidelines for Laparoscopic CBD Exploration INDICATIONS Since the 1992 National Institutes of Health Consensus Development Conference Statement on Gallstones and Laparoscopic Cholecystectomy the indications
T-TUBE DRAINAGE VERSUS PRIMARY COMMON BILE DUCT CLOSURE AFTER OPEN CHOLEDOCHOTOMY
 T-TUBE DRAINAGE VERSUS PRIMARY COMMON BILE DUCT CLOSURE AFTER OPEN CHOLEDOCHOTOMY Khaled Ahmed El- Dabee, Abd Al-Lateif Ahmed, Mohamed Abdel Aziz Abdel Jawad, Taha Bahgat Salam, Ahmed Eisa Ahmed* and Saed
T-TUBE DRAINAGE VERSUS PRIMARY COMMON BILE DUCT CLOSURE AFTER OPEN CHOLEDOCHOTOMY Khaled Ahmed El- Dabee, Abd Al-Lateif Ahmed, Mohamed Abdel Aziz Abdel Jawad, Taha Bahgat Salam, Ahmed Eisa Ahmed* and Saed
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM
 A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
Predicting difficulty in laparoscopic cholecystectomy by clinical, hematological and radiological evaluation
 International Surgery Journal Naik CG et al. Int Surg J. 2017 Jan;4(1):189-193 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20164080
International Surgery Journal Naik CG et al. Int Surg J. 2017 Jan;4(1):189-193 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20164080
Complication of Laparoscopic Cholecystectomy
 Complication of Laparoscopic Cholecystectomy R.K.Mishra What to do if something goes wrong There is not a single laparoscopic surgeon in the world who has not damaged CBD Complications Early Common bile
Complication of Laparoscopic Cholecystectomy R.K.Mishra What to do if something goes wrong There is not a single laparoscopic surgeon in the world who has not damaged CBD Complications Early Common bile
laparoscopic cholecystectomy
 Combined percutaneous and endoscopic approach in management of dropped gallstones following laparoscopic cholecystectomy John S.F. Shum 1*, K.H. Fung 1, George P.C. Yang 2, Chung Ngai Tang 2, Michael K.W.
Combined percutaneous and endoscopic approach in management of dropped gallstones following laparoscopic cholecystectomy John S.F. Shum 1*, K.H. Fung 1, George P.C. Yang 2, Chung Ngai Tang 2, Michael K.W.
Study of the degree of gall bladder wall thickness and its impact on outcomes following laparoscopic cholecystectomy in JSS Hospital
 International Surgery Journal Chandra SBJ et al. Int Surg J. 2018 Apr;5(4):1417-1421 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20181122
International Surgery Journal Chandra SBJ et al. Int Surg J. 2018 Apr;5(4):1417-1421 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20181122
CHOLECYSTECTOMY CONSENT FORM
 1 of 6 Patient Name: I, have been asked to carefully read all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described
1 of 6 Patient Name: I, have been asked to carefully read all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described
Controversies in the management of acute pancreatitis
 Kathmandu University Medical Journal (3) Vol., No. 3, Issue 7, 3-7 Controversies in the management of acute pancreatitis Singh DR 1, Mehta A, Dangol UMS 3 1 Lecturer, Medical Officer, 3 Lecturer, Dept.
Kathmandu University Medical Journal (3) Vol., No. 3, Issue 7, 3-7 Controversies in the management of acute pancreatitis Singh DR 1, Mehta A, Dangol UMS 3 1 Lecturer, Medical Officer, 3 Lecturer, Dept.
Percutaneous cholecystostomy for the treatment of acute cholecystitis in the critically ill and elderly
 ORIGINAL ARTICLE Key words: Cholecystectomy; Cholecystostomy!!"#!" JCM Li DWH Lee CW Lai ACN Li DW Chu ACW Chan Hong Kong Med J 2004;10:389-93 North District Hospital, New Territories East Cluster, 9 Po
ORIGINAL ARTICLE Key words: Cholecystectomy; Cholecystostomy!!"#!" JCM Li DWH Lee CW Lai ACN Li DW Chu ACW Chan Hong Kong Med J 2004;10:389-93 North District Hospital, New Territories East Cluster, 9 Po
Per-operative conversion of laparoscopic cholecystectomy to open surgery: prospective study at JSS teaching hospital, Karnataka, India
 International Surgery Journal Raza M et al. Int Surg J. 2017 Jan;4(1):81-85 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163977
International Surgery Journal Raza M et al. Int Surg J. 2017 Jan;4(1):81-85 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163977
Surveillance proposal consultation document
 Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Surgical Workload, Outcome and Research Database: V1.1
 Technical Guidance for Surgical Workload, Outcome and Research Database: V1.1 Contents 1. Standard Indicators... 5 1.1. Activity Volume... 5 1.2. Average Length of Stay (Days)... 5 1.3. 2/7/30 day Re-admission
Technical Guidance for Surgical Workload, Outcome and Research Database: V1.1 Contents 1. Standard Indicators... 5 1.1. Activity Volume... 5 1.2. Average Length of Stay (Days)... 5 1.3. 2/7/30 day Re-admission
Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis
 Original Article Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis Pradhan S 1, Shah S 2, Maharjan S 2, Shah JN 3 1 2 2 3 Professor, Patan hospital Correspondence:
Original Article Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis Pradhan S 1, Shah S 2, Maharjan S 2, Shah JN 3 1 2 2 3 Professor, Patan hospital Correspondence:
Evaluation of Complications Occurring in Patients Undergoing Laparoscopic Cholecystectomy: An Institutional Based Study
 Original article: Evaluation of Complications Occurring in Patients Undergoing Laparoscopic Cholecystectomy: An Institutional Based Study Sudhir Tyagi 1, Sanjeev Kumar 2* 1 Assistant Professor, 2* Associate
Original article: Evaluation of Complications Occurring in Patients Undergoing Laparoscopic Cholecystectomy: An Institutional Based Study Sudhir Tyagi 1, Sanjeev Kumar 2* 1 Assistant Professor, 2* Associate
Kathmandu University Medical Journal (2009), Vol. 7, No. 1, Issue 25, 16-20
 Kathmandu University Medical Journal (2009), Vol. 7, No. 1, Issue 25, 16-20 Original Article A comparative study of early vs. delayed laparoscopic cholecystectomy in acute cholecystitis Yadav RP 1, Adhikary
Kathmandu University Medical Journal (2009), Vol. 7, No. 1, Issue 25, 16-20 Original Article A comparative study of early vs. delayed laparoscopic cholecystectomy in acute cholecystitis Yadav RP 1, Adhikary
Appendix A: Summary of evidence from surveillance
 Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
LAPAROSCOPIC GALLBLADDER SURGERY
 LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
Cholecystitis is defined as nonspecific inflammation of the gallbladder with or without cholelithiasis. Types: calculous and acalculous.
 Cholecystitis is defined as nonspecific inflammation of the gallbladder with or without cholelithiasis. Types: calculous and acalculous. Anatomy of the gallbladder The gallbladder, a pear-shaped reservoir
Cholecystitis is defined as nonspecific inflammation of the gallbladder with or without cholelithiasis. Types: calculous and acalculous. Anatomy of the gallbladder The gallbladder, a pear-shaped reservoir
Laparoscopic Subtotal Cholecystectomy for Difficult Acute Calculous Cholecystitis
 Journal of Surgery 2017; 5(6): 111-117 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20170506.15 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Laparoscopic Subtotal Cholecystectomy
Journal of Surgery 2017; 5(6): 111-117 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20170506.15 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Laparoscopic Subtotal Cholecystectomy
REFERRAL GUIDELINES: GALLSTONES
 REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
SAGES GUIDELINES FOR THE CLINICAL APPLICATION OF LAPAROSCOPIC BILIARY TRACT SURGERY
 Practice/Clinical Guidelines published on: 01/2010 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) SAGES GUIDELINES FOR THE CLINICAL APPLICATION OF LAPAROSCOPIC BILIARY TRACT
Practice/Clinical Guidelines published on: 01/2010 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) SAGES GUIDELINES FOR THE CLINICAL APPLICATION OF LAPAROSCOPIC BILIARY TRACT
Two-port needlescopic cholecystectomy: prospective study of 100 cases!"#$%&'()*+,-./0123
 KW Lee C Poon K Leung DWH Lee CW Ko Key words: Cholecystectomy, laparoscopic; iber optics; Laparoscopes; iniaturization; Needles!!"#$%&'(!"!! Hong Kong ed J 2005;11:30-5 Department of Surgery, Tuen un
KW Lee C Poon K Leung DWH Lee CW Ko Key words: Cholecystectomy, laparoscopic; iber optics; Laparoscopes; iniaturization; Needles!!"#$%&'(!"!! Hong Kong ed J 2005;11:30-5 Department of Surgery, Tuen un
Setting The study setting was hospital. The economic analysis was carried out in California, USA.
 Preoperative versus postoperative endoscopic retrograde cholangiopancreatography in mild to moderate gallstone pancreatitis: a prospective randomized trial Chang L, Lo S, Stabile B E, Lewis R J, Toosie
Preoperative versus postoperative endoscopic retrograde cholangiopancreatography in mild to moderate gallstone pancreatitis: a prospective randomized trial Chang L, Lo S, Stabile B E, Lewis R J, Toosie
GALL STONES RETREVIAL DURING LAPROSCOPIC CHOLECYSTECTOMY B. S. Johal 1, B. S. Sidhu 2, Swarn Lata 3
 GALL STONES RETREVIAL DURING LAPROSCOPIC CHOLECYSTECTOMY B. S. Johal 1, B. S. Sidhu 2, Swarn Lata 3 HOW TO CITE THIS ARTICLE: B. S. Johal, B. S. Sidhu, Swarn Lata. Gall Stones Retrevial during Laproscopic
GALL STONES RETREVIAL DURING LAPROSCOPIC CHOLECYSTECTOMY B. S. Johal 1, B. S. Sidhu 2, Swarn Lata 3 HOW TO CITE THIS ARTICLE: B. S. Johal, B. S. Sidhu, Swarn Lata. Gall Stones Retrevial during Laproscopic
The Present Scenario of Cholecystectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 71-75 www.iosrjournals.org The Present Scenario of Cholecystectomy
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 71-75 www.iosrjournals.org The Present Scenario of Cholecystectomy
Recurring abdominal wall wounds and cutaneous sinus tract formations secondary to spilled gallstones
 ISPUB.COM The Internet Journal of Surgery Volume 21 Number 1 Recurring abdominal wall wounds and cutaneous sinus tract formations secondary to spilled gallstones D Brown, A Wagner, M Aronis, A Isenberg
ISPUB.COM The Internet Journal of Surgery Volume 21 Number 1 Recurring abdominal wall wounds and cutaneous sinus tract formations secondary to spilled gallstones D Brown, A Wagner, M Aronis, A Isenberg
What can you expect after your ERCP?
 ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy. TEAM 1 Janix M. De Guzman, MD Presentor
 Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy TEAM 1 Janix M. De Guzman, MD Presentor Premise 40F Jaundice Abdominal pain US finding of gallstones with apparently normal common
Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy TEAM 1 Janix M. De Guzman, MD Presentor Premise 40F Jaundice Abdominal pain US finding of gallstones with apparently normal common
Laparoscopic Cholecystectomy in Patients With Previous Abdominal Surgery
 SCIENTIFIC PAPER Laparoscopic Cholecystectomy in Patients With Previous Abdominal Surgery Nusret Akyurek, MD, Bülent Salman, MD, Oktay Irkorucu, MD, Öge Tascilar, MD, Osman Yuksel, MD, Mustafa Sare, MD,
SCIENTIFIC PAPER Laparoscopic Cholecystectomy in Patients With Previous Abdominal Surgery Nusret Akyurek, MD, Bülent Salman, MD, Oktay Irkorucu, MD, Öge Tascilar, MD, Osman Yuksel, MD, Mustafa Sare, MD,
ISSN X (Print) Research Article. *Corresponding author Jitendra Singh Yadav
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon
 Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon Core Specialist Group Suite 5G, John Flynn Medical Centre 42 Inland Drive TUGUN QLD 4224 Tel: 07 5598 0955 Write questions or notes
Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon Core Specialist Group Suite 5G, John Flynn Medical Centre 42 Inland Drive TUGUN QLD 4224 Tel: 07 5598 0955 Write questions or notes
Early vs delayed laparoscopic cholecystectomy for acute cholecystitis
 Original articles Surg Endosc (2004) 18:1323 1327 DOI:10.1007/s00464-003-9230-6 Ó Springer Science+Business Media, Inc. 2004 Early vs delayed laparoscopic cholecystectomy for acute cholecystitis A prospective
Original articles Surg Endosc (2004) 18:1323 1327 DOI:10.1007/s00464-003-9230-6 Ó Springer Science+Business Media, Inc. 2004 Early vs delayed laparoscopic cholecystectomy for acute cholecystitis A prospective
Laparoscopic Cholecystectomy after Upper Abdominal Surgery : Is It Feasible Even after Gastrectomy?
 ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2017;20(1):22-28 Journal of Minimally Invasive Surgery Laparoscopic Cholecystectomy after Upper Abdominal Surgery : Is It Feasible
ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2017;20(1):22-28 Journal of Minimally Invasive Surgery Laparoscopic Cholecystectomy after Upper Abdominal Surgery : Is It Feasible
No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study
 Original article Annals of Gastroenterology (2013) 26, 1-6 No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study Rachel M. Gomes
Original article Annals of Gastroenterology (2013) 26, 1-6 No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study Rachel M. Gomes
ENDOSCOPIC TREATMENT OF A BILE DUCT
 HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
Primary Closure Versus T-tube Drainage After Open Choledochotomy
 Original Article Primary Closure Versus T-tube Drainage After Open Choledochotomy M. Ambreen, A.R. Shaikh, A. Jamal, J.N. Qureshi, A.G. Dalwani and M.M. Memon, Department of Surgery, Liaquat University
Original Article Primary Closure Versus T-tube Drainage After Open Choledochotomy M. Ambreen, A.R. Shaikh, A. Jamal, J.N. Qureshi, A.G. Dalwani and M.M. Memon, Department of Surgery, Liaquat University
Northumbria Healthcare NHS Foundation Trust. Laparoscopic Cholecystectomy. Issued by the Department of Upper Gastrointestinal Surgery
 Northumbria Healthcare NHS Foundation Trust Laparoscopic Cholecystectomy Issued by the Department of Upper Gastrointestinal Surgery Laparoscopic Cholecystectomy This leaflet explains why you have been
Northumbria Healthcare NHS Foundation Trust Laparoscopic Cholecystectomy Issued by the Department of Upper Gastrointestinal Surgery Laparoscopic Cholecystectomy This leaflet explains why you have been
DISCLAIMER. No Conflict of Interest
 DISCLAIMER No Conflict of Interest EXCLAIMER No Interest in Conflict GALLSTONES FAQs and FACTS John Dunn, FRACS Laparoscopy Auckland YOU GOTTA KNOW THIS STUFF HOW DO THEY FORM? Gallbladder Lithogenic
DISCLAIMER No Conflict of Interest EXCLAIMER No Interest in Conflict GALLSTONES FAQs and FACTS John Dunn, FRACS Laparoscopy Auckland YOU GOTTA KNOW THIS STUFF HOW DO THEY FORM? Gallbladder Lithogenic
Gallstones & Other Biliary Disorders
 Gallstones & Other Biliary Disorders Jason Smith MD DMI FRCS(Gen.Surg) Consultant General & Colorectal Surgeon Introduction Gallstones are found in 12% men and 24% women Prevalence increases with advancing
Gallstones & Other Biliary Disorders Jason Smith MD DMI FRCS(Gen.Surg) Consultant General & Colorectal Surgeon Introduction Gallstones are found in 12% men and 24% women Prevalence increases with advancing
COMPLICATIONS OF LAPAROSCOPIC CHOLECYSTECTOMY AT ISRA UNIVERSITY HOSPITAL, HYDERABAD
 Original Article COMPLICATIONS OF LAPAROSCOPIC CHOLECYSTECTOMY AT ISRA UNIVERSITY HOSPITAL, HYDERABAD Waseem Memon 1, Tariq Wahab Khanzada 2, Abdul Samad 3, M. Hussain Laghari 4 ABSTRACT Objective: The
Original Article COMPLICATIONS OF LAPAROSCOPIC CHOLECYSTECTOMY AT ISRA UNIVERSITY HOSPITAL, HYDERABAD Waseem Memon 1, Tariq Wahab Khanzada 2, Abdul Samad 3, M. Hussain Laghari 4 ABSTRACT Objective: The
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of single-incision cholecystectomy Gallstones form in the gallbladder and can cause
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of single-incision cholecystectomy Gallstones form in the gallbladder and can cause
Optimal timing of elective laparoscopic cholecystectomy after acute cholangitis and subsequent clearance of choledocholithiasis
 The American Journal of Surgery (2010) 200, 483 488 Clinical Science Optimal timing of elective laparoscopic cholecystectomy after acute cholangitis and subsequent clearance of choledocholithiasis Vicky
The American Journal of Surgery (2010) 200, 483 488 Clinical Science Optimal timing of elective laparoscopic cholecystectomy after acute cholangitis and subsequent clearance of choledocholithiasis Vicky
Kathmandu University Medical Journal (2009), Vol. 7, No. 1, Issue 25, 26-30
 Kathmandu University Medical Journal (29), Vol. 7, No. 1, Issue 25, 2-3 Original Article Evaluation of predictive factors for conversion of laparoscopic cholecystectomy Gabriel R, Kumar S, Shrestha A Department
Kathmandu University Medical Journal (29), Vol. 7, No. 1, Issue 25, 2-3 Original Article Evaluation of predictive factors for conversion of laparoscopic cholecystectomy Gabriel R, Kumar S, Shrestha A Department
Gallstones Information Leaflet THE DIGESTIVE SYSTEM. Gutscharity.org.uk
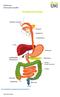 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about gallstones Gall is an old-fashioned word for bile, a liquid made in the liver and stored in the gall bladder
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about gallstones Gall is an old-fashioned word for bile, a liquid made in the liver and stored in the gall bladder
CLINICAL GUIDELINE FOR MANAGEMENT OF GALLSTONES PATHOLOGY IN ADULTS
 CLINICAL GUIDELINE FOR MANAGEMENT OF GALLSTONES PATHOLOGY IN ADULTS 1. Aim/Purpose of this Guideline This guideline is for the management of gallstones pathology in adults. It has been benchmarked against
CLINICAL GUIDELINE FOR MANAGEMENT OF GALLSTONES PATHOLOGY IN ADULTS 1. Aim/Purpose of this Guideline This guideline is for the management of gallstones pathology in adults. It has been benchmarked against
Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines
 Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines Kevin Sargen, Andrew N Kingsnorth Department of Surgery, Plymouth Postgraduate Medical School, Derriford Hospital. Plymouth.
Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines Kevin Sargen, Andrew N Kingsnorth Department of Surgery, Plymouth Postgraduate Medical School, Derriford Hospital. Plymouth.
Cholelithiasis & cholecystitis
 1 Cholelithiasis & cholecystitis Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA) Assistant Professor, Dept. of Surgery College of Medicine, Prince Sattam bin Abdulaziz University Email: surgeon.shamim@gmail.com
1 Cholelithiasis & cholecystitis Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA) Assistant Professor, Dept. of Surgery College of Medicine, Prince Sattam bin Abdulaziz University Email: surgeon.shamim@gmail.com
EAST MULTICENTER STUDY PROPOSAL
 EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES
 SAFETY AND OUTCOME OF SELECTIVE INTRA-OPERATIVE CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES Ihab Kadry, Mahmoud Reda, Hesham Ahmed and Mohamed ZaaZou. Department Of General Surgery Misr University
SAFETY AND OUTCOME OF SELECTIVE INTRA-OPERATIVE CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES Ihab Kadry, Mahmoud Reda, Hesham Ahmed and Mohamed ZaaZou. Department Of General Surgery Misr University
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 6 The Role of Ultrasound in Laprascopic Cholecystectomy Faris D. Alaswad University of Baghdad, faris alaswad@yahoo.com Copyright c 2014
World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 6 The Role of Ultrasound in Laprascopic Cholecystectomy Faris D. Alaswad University of Baghdad, faris alaswad@yahoo.com Copyright c 2014
In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo Shin Choi 2, and Seung Eun Lee 2. Departments of Surgery, Dongguk University College of Medicine 2
 Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
Abdominal Imaging. Gallbladder perforation: color Doppler findings
 Abdom Imaging 27:47 50 (2002) DOI: 10.1007/s00261-001-0048-1 Abdominal Imaging Springer-Verlag New York Inc. 2002 Gallbladder perforation: color Doppler findings K. Konno, 1 H. Ishida, 1 M. Sato, 1 H.
Abdom Imaging 27:47 50 (2002) DOI: 10.1007/s00261-001-0048-1 Abdominal Imaging Springer-Verlag New York Inc. 2002 Gallbladder perforation: color Doppler findings K. Konno, 1 H. Ishida, 1 M. Sato, 1 H.
Biomedical Research 2017; 28 (15):
 Biomedical Research 2017; 28 (15): 6671-6676 ISSN 0970-938X www.biomedres.info Single surgeon experience: intraoperative complications and conversion to open surgery in laparoscopic cholecystectomy, the
Biomedical Research 2017; 28 (15): 6671-6676 ISSN 0970-938X www.biomedres.info Single surgeon experience: intraoperative complications and conversion to open surgery in laparoscopic cholecystectomy, the
What Are Gallstones? GALLSTONES. Gallstones are pieces of hard, solid matter that form over time in. the gallbladder of some people.
 What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
Naoyuki Toyota, Tadahiro Takada, Hodaka Amano, Masahiro Yoshida, Fumihiko Miura, and Keita Wada
 J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
Risk Factors for Conversion to Open Surgery in Patients With Acute Cholecystitis Undergoing Interval Laparoscopic Cholecystectomy
 Original Article 631 Risk Factors for Conversion to Open Surgery in Patients With Acute Cholecystitis Undergoing Interval Laparoscopic Cholecystectomy Kok-Ren Lim, 1 MRCS (Edin), Salleh Ibrahim, 1 FRCS
Original Article 631 Risk Factors for Conversion to Open Surgery in Patients With Acute Cholecystitis Undergoing Interval Laparoscopic Cholecystectomy Kok-Ren Lim, 1 MRCS (Edin), Salleh Ibrahim, 1 FRCS
Downloaded from jssu.ssu.ac.ir at 13:10 IRST on Saturday October 28th 2017
 Journal of Shahid Sadoughi University of Medical Sciences Vol. 21, No. 5, Nov-Dec 2013 Pages: 675-681 1392 5 21 675-681 : 3 2* 1 1392/8/ : -1-2 -3 1391/8/24 : (). :. 1390 200 :.. SPSS (%0/5) 200 (8%) (%9/5)19
Journal of Shahid Sadoughi University of Medical Sciences Vol. 21, No. 5, Nov-Dec 2013 Pages: 675-681 1392 5 21 675-681 : 3 2* 1 1392/8/ : -1-2 -3 1391/8/24 : (). :. 1390 200 :.. SPSS (%0/5) 200 (8%) (%9/5)19
Emergency Surgery Course Graz, March ACUTE PANCREATITIS. Carlos Mesquita Coimbra
 ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018)
 Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018) Commissioning Statement Asymptomatic Gallstones Policy Exclusions (Alternative commissioning
Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018) Commissioning Statement Asymptomatic Gallstones Policy Exclusions (Alternative commissioning
SELECTED ABSTRACTS. Editor - Rohan Siriwardena. during a laparoscopic cholecystectomy in a highvolume teaching centre, was associated with a low
 SELECTED ABSTRACTS Editor - Rohan Siriwardena Impact of routine intraoperative cholangiography during laparoscopic cholecystectomy on bile duct injury Alvarez FA et. al. Br J Surg. 2014; 101(6): 677-84.
SELECTED ABSTRACTS Editor - Rohan Siriwardena Impact of routine intraoperative cholangiography during laparoscopic cholecystectomy on bile duct injury Alvarez FA et. al. Br J Surg. 2014; 101(6): 677-84.
Cholecystectomy (removal of the gallbladder) Patient Information
 Cholecystectomy (removal of the gallbladder) Patient Information Author ID: MP Leaflet Number: Surg 060 Name of Leaflet: Cholecystectomy (removal of the gallbladder) Version: 1 Date Produced: October 2017
Cholecystectomy (removal of the gallbladder) Patient Information Author ID: MP Leaflet Number: Surg 060 Name of Leaflet: Cholecystectomy (removal of the gallbladder) Version: 1 Date Produced: October 2017
Risk Factors for Development of Biliary Stricture in Patients Presenting with Bile Leak after Cholecystectomy
 Gut and Liver, Vol. 7, No. 3, May 2013, pp. 352-356 ORiginal Article Risk Factors for Development of Biliary Stricture in Patients Presenting with Bile Leak after Cholecystectomy Hosur Mayanna Lokesh,
Gut and Liver, Vol. 7, No. 3, May 2013, pp. 352-356 ORiginal Article Risk Factors for Development of Biliary Stricture in Patients Presenting with Bile Leak after Cholecystectomy Hosur Mayanna Lokesh,
General Surgery Service
 General Surgery Service Patient Care Goals and Objectives Stomach/Duodenum and Bariatric assessed for a) Obesity surgery b) Treatment of i) Adenocarcinoma of the stomach ii) GIST iii) Carcinoid 2) Optimize
General Surgery Service Patient Care Goals and Objectives Stomach/Duodenum and Bariatric assessed for a) Obesity surgery b) Treatment of i) Adenocarcinoma of the stomach ii) GIST iii) Carcinoid 2) Optimize
Diagnostic Laparoscopy patient information from your surgeon & SAGES
 Diagnostic Laparoscopy patient information from your surgeon & SAGES Diagnostic Laparoscopy 1 Diagnostic Laparoscopy About conventional colon surgery: Patients may be referred to surgeons because of an
Diagnostic Laparoscopy patient information from your surgeon & SAGES Diagnostic Laparoscopy 1 Diagnostic Laparoscopy About conventional colon surgery: Patients may be referred to surgeons because of an
Transabdominal pre peritoneal (TAPP) vs totally extraperitoneal (TEP) laparoscopic techniques for inguinal hernia repair
 Transabdominal pre peritoneal (TAPP) vs totally extraperitoneal (TEP) laparoscopic techniques for inguinal hernia repair An inguinal hernia (hernia of the groin) is a weakness in the wall of the abdominal
Transabdominal pre peritoneal (TAPP) vs totally extraperitoneal (TEP) laparoscopic techniques for inguinal hernia repair An inguinal hernia (hernia of the groin) is a weakness in the wall of the abdominal
Evaluation of Efficacy of Two versus Three Ports Technique in Patients Undergoing Laparoscopic Cholecystectomy: A Comparative Analysis
 Original article: Evaluation of Efficacy of Two versus Three Ports Technique in Patients Undergoing Laparoscopic Cholecystectomy: A Comparative Analysis Sanjeev Kumar 1, Sudhir Tyagi 2* 1 Associate Professor,
Original article: Evaluation of Efficacy of Two versus Three Ports Technique in Patients Undergoing Laparoscopic Cholecystectomy: A Comparative Analysis Sanjeev Kumar 1, Sudhir Tyagi 2* 1 Associate Professor,
Our Experience in Laparoscopic Appendectomy in Federal Teaching Hospital, Gombe
 original article Our Experience in Laparoscopic Appendectomy 10.5005/jp-journals-10007-1229 in Federal Teaching Hospital, Gombe Our Experience in Laparoscopic Appendectomy in Federal Teaching Hospital,
original article Our Experience in Laparoscopic Appendectomy 10.5005/jp-journals-10007-1229 in Federal Teaching Hospital, Gombe Our Experience in Laparoscopic Appendectomy in Federal Teaching Hospital,
Title: The impact of a percutaneous cholecystostomy catheter in situ until the time of cholecystectomy on the development of recurrent acute
 Title: The impact of a percutaneous cholecystostomy catheter in situ until the time of cholecystectomy on the development of recurrent acute cholecystitis: a historical cohort study Authors: Mustafa Hasbahceci,
Title: The impact of a percutaneous cholecystostomy catheter in situ until the time of cholecystectomy on the development of recurrent acute cholecystitis: a historical cohort study Authors: Mustafa Hasbahceci,
AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH
 AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH e-issn - 2348-2184 Print ISSN - 2348-2176 Journal homepage: www.mcmed.us/journal/ajbpr A COMPARATIVE ANALYSIS OF EARLY VERSUS DELAYED LAPAROSCOPIC
AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH e-issn - 2348-2184 Print ISSN - 2348-2176 Journal homepage: www.mcmed.us/journal/ajbpr A COMPARATIVE ANALYSIS OF EARLY VERSUS DELAYED LAPAROSCOPIC
Sharma Maneesh,Chaudhary Sanchit, Sharma Ratnakar, Mahajan Amit
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. II (October. 2016), PP 09-13 www.iosrjournals.org A Prospective Study of Complications
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. II (October. 2016), PP 09-13 www.iosrjournals.org A Prospective Study of Complications
Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary?
 Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary? Nasir Zaheer Ahmad, FRCSI SCIENTIFIC PAPER ABSTRACT Background and Objectives: Liver function
Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary? Nasir Zaheer Ahmad, FRCSI SCIENTIFIC PAPER ABSTRACT Background and Objectives: Liver function
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
JMSCR Vol 05 Issue 04 Page April 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i4.11 Post Cholecystectomy Stump Calculus Cholecystitis
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i4.11 Post Cholecystectomy Stump Calculus Cholecystitis
Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery
 SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
ERCP / PTC Surgical Laparoscopic vs open Timing and order of approach
 Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
ERCP investigation of the bile duct and pancreatic duct
 ERCP investigation of the bile duct and pancreatic duct Information for patients ERCP investigation of the bile duct and pancreatic duct 2 ERCP investigation of the bile duct and pancreatic duct 3 INTRODUCTION
ERCP investigation of the bile duct and pancreatic duct Information for patients ERCP investigation of the bile duct and pancreatic duct 2 ERCP investigation of the bile duct and pancreatic duct 3 INTRODUCTION
