Station II: Assessment of the Patient with an Intraspinal Infusion. Monitoring, Assessment and Documentation
|
|
|
- Basil Craig
- 6 years ago
- Views:
Transcription
1 The Intraspinal Pain Management training program was developed to familiarize caregivers in the Oncology Program, Palliative Care Program and in the home care setting with guidelines for care management for the patient receiving intraspinal analgesia. The training program includes 2 components including the completion of a: Resource guide for Intraspinal Analgesia 2 Hr Classroom session as outlined below Return of the post quiz Please note the resource guide should be completed in preparation for session attendance and you will be receiving additional information during the class. Introductory Lecture: Intraspinal Infusion and Drugs used Station I: Care of the Patient with an Intraspinal Infusion Infusion setup, Catheter care, and Troubleshooting Station II: Assessment of the Patient with an Intraspinal Infusion Monitoring, Assessment and Documentation 1. Describe the key anatomical structures and their functions related to Intraspinal analgesia 2. Identify the mechanism of action for the following classes of drugs: Neuraxial opioids, Local anesthetics and Naloxone 4. Identify the most common potential complications of Intraspinal analgesia and their nursing care management. 5. Describe the nursing care assessment & monitoring for patients receiving Intraspinal analgesia 6. Demonstrate, in a simulated setting and then in the clinical setting, the following : Set up of the continuous Intraspinal infusion (pump and tubings) Assessment of the patient with an Intraspinal infusion 7. Describe necessary documentation for Intraspinal analgesia 8. Discuss and demonstrate the correct nursing actions for 2 given case scenarios. Intraspinal Analgesia WRH 03/31/03 p. 1
2 Pain is a common problem for cancer patients. It is estimated that thirty to forty-five percent of patients with early to intermediate stages of cancer will experience pain, while up to seventy-five percent of patients will have advanced cancer experience pain (Bonica, 1990, Daut & Cleeland, 1982). The causes of cancer pain are multifaceted and often require frequent adjustments in pain strategy methods to achieve optimal results. The majority of cancer patients achieve relief through simple routes of administration (oral, rectal, transdermal) however two to twenty percent of patients require more invasive pain management regimes to control pain. Intraspinal catheters including intrathecal and epidural delivery methods were introduced for the treatment of cancer pain in the late 70 s. Intraspinal analgesia is indicated for patients who experience intolerable side effects or intractable pain with other administration routes. As indicated by the analgesia ladder interventional treatments such as intraspinal infusions should be considered after other measures have been utilized. The prevalence of the use of progressively more invasive therapies such as intraspinal analgesia is estimated to be 2% and 6% Interventional Nerve blocks, Spinal drug administration, surgery Strong Opioid IV, SC Strong Opioid PO, Rectal, Transdermal Mild Opioid ± Adjuvant Non-Opioid ± Adjuvant Intraspinal Analgesia WRH 03/31/03 p. 2
3 Can be used to treat somatic, visceral and neuropathic pain with fewer sides effects than systemic administered opioids Lower dosages of opioids are required to produce effective pain control with 10 times less medication needed for the epidural space and 100 times less medication needed for the intrathecal space Systemic opiods may be reduced by one half with the introduction of intraspinal administration Because all other administration routes have been found to be ineffective Because patients on epidural or intrathecal therapy may be provided with pain relief in such a way that mobility and awareness are maintained Severe hemorrhage or shock Infection at the site Bleeding tendencies or clotting abnormalities Allergy or sensitivity to local anesthetic agents Certain Neurological disorders: MS,CNS infection and Increased ICP NOTE: low dose heparin is not a contraindication provided the INR is within normal range. The potential risk of Intraspinal hematoma formation and resultant serious neurological sequela (spinal cord compression, ischemia, and subsequent paralysis) may preclude these patients as candidates. If patient is to be on subclinical anticoagulant therapy check with the prescribing physician regarding administration. Intraspinal Analgesia WRH 03/31/03 p. 3
4 The spinal cord and the brain are covered by three meningeal membranes as described in the chart below. Layer Location Description Dura mater Arachnoid mater outer layer next to bone Middle layer is a fibrous connective tissue containing many blood vessels is a delicate fibrous membrane Pia mater inner layer next to the brain is a vascular membrane containing a plexus of blood vessels-forms the choroid plexus The subarachnoid space - - is between the pia mater and the arachnoid membrane while the epidural space is a potential space between the dura mater and the vertebral canal, and extends from the cranium to the sacrum. Epidural Placement Intrathecal Placement Spinous process Ligamentum Flavuum Pia Dura Blood Vessels Spine cord Subarachnoid space Epidural Space Epidural fatty layer Intraspinal analgesia can be given by two delivery routes and is determined by the placement of the catheter. The two routes include: ❶ Epidural and ❷Intrathecal and the following table and diagram provides further explanation. Intraspinal Analgesia WRH 03/31/03 p. 4
5 Route Placement Description Epidural involves the placement of the catheter between the dura mater and the vertebral arch in the epidural space Intrathecal refers to the placement of the catheter into the subarachnoid space between the spinal cord and the dura mater. The epidural space contains fat, blood vessels and nerves. It functions as a fatty pad that surrounds the spinal cord and acts as a depot for narcotics. Drugs are administered adjacent to the spinal cord and diffuse across a fat lipid membrane called the dura and into the spinal cord. Some of the analgesia is lost into the epidural vasculature during the diffusion process, thus creating some systemic absorption This space extends from the cranium and sacrum and contains CSF. Eliminates the need for the drug to cross the dura and drug is delivered directly next to the spinal cord. This allows the analgesia to work quicker and in lower doses. Impulses from a painful stimulus enter the spinal cord through the dorsal or sensory root of a spinal nerve. The nerve terminates in the dorsal horn of the cord. A neurotransmitter known as substance P located in the dorsal horn is thought to allow the impulse of the painful stimuli to travel across and up the ascending fibre of the cord to the brain Epidural space (containing blood vessels,fatty tissue Dorsal Root (site of action for anesthetics) Vertebral body Spinous Process Subarachnoid space (intrathecal space with CSF) Dorsal horn (site of action for opiods Intraspinally administered narcotics such as morphine block the release of substance P thus interrupting the transmission of the painful stimuli. While local anesthetics act a little differently. They block the painful stimuli as it is entering the dorsal horn of the cord. The extent of block depends on the dose given but usually low concentrations are required. Intraspinal Analgesia WRH 03/31/03 p. 5
6 Intraspinal catheters include short term percutaneously inserted catheters and tunneled long term catheters. Short Term Catheter Tunneled Catheter This polyethylene catheter is used for short term pain management and is inserted as described below. It exits the spinal column and is run up the back and is looped over the shoulder. Is catheter that is tunneled under the skin to exit onto the patient s abdomen or attached to a subcutaneous reservoir/port under the skin. It is often used long term. The short term catheter will be inserted by an anesthesiologist. Verification of appropriate placement and a test dose of the anesthetic agent must be done by the MD. During the insertion the patient may be positioned on his/her side, lying in fetal position, with both knees drawn upward with head and shoulders flexed toward the chest. This extends the spine, widening the spaces between vertebrae, making insertion of the catheter easier. The patient may also be positioned in the upright position, leaning over an over-bed table. A special needle (usually a Touhey needle) is inserted through the skin, fat and fascia between the spinous processes, penetrating the ligamentum flavum then advanced into the Epidural or Subarachnoid space. Once the needle has been determined to be in the appropriate position, the catheter is threaded through the needle. The needle is then removed. A connector is then attached to the catheter. The long tunneled catheter is inserted in the OR by the Anesthesiologist. It is often made of a kink resistant material. The Touhey needle is used to place the catheter and then the catheter is tunneled from the intraspinal space under the skin and exits on the abdomen as illustrated in the accompanying diagram. A connector is attached. Illustration provided courtesy of SIMS Deltec, Inc., St. Paul, Minnesota. Intraspinal Analgesia WRH 03/31/03 p. 6
7 Intraspinal Dressing Short-term Non-Tunneled Intraspinal Catheter Tunneled Intraspinal Catheter II. Dressing Changes Q weekly and if dressing becomes wet or loose.if a gauze dressing is under the transparent dressing it must be changed q 72 hours. Occlusive transparent dressing at site on lower back Cloth/Mefix tape to be used up distal length of catheter along back The catheter adapter end is looped over the shoulder Strict aseptic technique similar to central line procedure. Glove and mask are used. Q weekly and if dressing becomes wet or loose. If a gauze dressing is under the transparent dressing it must be changed q 72 hours Occlusive transparent dressing at site on patient side or abdomen Strict aseptic technique similar to central line procedure. Glove and mask are used. Filter/ Tubing Changes Q weekly under strict aseptic techniqueoptimally is best to coordinate tubing change with the cassette/bag change. Limit opening the system as much as possible Q weekly under strict aseptic technique. optimally is best to coordinate tubing change with the cassette/bag change. Limit opening the system as much as possible Cleansing Cleanse with providone-iodine in circular fashion. Cover a diameter of 2-3 inches and allow 2-3 minutes for area to dry completely. Cleanse with providone iodine in circular fashion. Cover a diameter of 2-3 inches and allow 2-3 minutes for area to dry completely. Other This catheter may or may not be sutured; extreme caution must be taken not to dislodge catheter. Peeling the dressing toward the insertion site is recommended. Steri- strips or sutures may be used to stabilize the catheter under the transparent dressing. Steri strips must be replaced with each dressing change. Dislodgment and infection are less common with this type of catheters. The tubing and site should be labelled Intraspinal Catheter- Do not Inject. The site should be visible and covered with a transparent dressing for assessment purposes. The edges of the dressing should be window-paned to prevent rolling of the dressing. Intraspinal Analgesia WRH 03/31/03 p. 7
8 Connector Problems The catheter must be placed into a CAP connector. The design of the connector depends on the manufacture but generally HUB has two pieces: The cap and the hub. The hub itself has a freely turning ring. The catheter is inserted into the connector lumen as far it can until its in the STOP position. Then the ring is turned until fully tightened. The hub to catheter connection must be assessed routinely to ensure an intact and secure connection. If a disconnect is discovered. The infusion is stopped and the catheter should be wrapped in a sterile 4x4 and anesthesia should be notified Never use alcohol on the catheter or connectors as alcohol is neuro toxic Intraspinal Analgesia WRH 03/31/03 p. 8
9 Continuous Infusion Top Up via Syringe Intermittent /PCA Bolus via Infusion Device Delivery of medication at a constant rate using an infusion device - is a dilute solution of opioids and/or an anesthetic agent Injection of medication bolus at timed intervals or on prn basis for break through pain is more concentrated drug solution administered BYMD ONLY Injection of infusion solution as a bolus but administered via the infusion device for break through pain (local anesthetic and/or opioids). All cancer patients requiring intraspinal analgesic will be provided with medications using of a continuous infusion. The use of a continuous infusion for intraspinal medication administration to cancer patients provides long-lasting, uniform levels of analgesia. Programming the pump that allows a set rate to be infused each hour provides this. Breakthrough dosing allows the patient/family/nurse to self administer small doses of analgesic medication intraspinally. When the patient has pain or anticipates pain will be associated with an upcoming activity, the patient/family member can manually trigger the pump to inject a prescribed amount of the pain medication. The amount of medication delivered each time and the minimum interval between doses is programmed into the pump according to the physician s orders. At the Metropolitan Campus the CADD Pump is designed to administered medications into the epidural and intrathecal space. At Western Campus and in the Community, the Microject PCA pump will be used for intrathecal administration while the Microject PECA pump will be used for epidural administration of medications. ***It should be noted that infusion rates will be significantly different between intrathecal and epidural route Top up injections may performed by the MD for the following reasons: following insertion of a catheter to test catheter position. during the administration of infusion because of inadequate analgesia. Intraspinal Analgesia WRH 03/31/03 p. 9
10 Preservative free narcotics and local anesthetics are the only type of medication that can be given intraspinally. Medications used to treat cancer pain include Morphine, Hydromorphone, Fentanyl and Sufentanil and local anesthetics Bupivicaine (Marcaine) and Lidocaine (Xylocaine). Infusions can include an opioid or an opioid and local anesthetic combination. The addition of a local anesthetic helps to potentate analgesia and improves overall pain control and decrease opioid need. Neuroaxial Opiods : relieve pain by binding with opium receptors at specific sites in the brain and spine - provide effective and longer duration analgesia have a tendency to spread due to uptake in vasculature Local Anesthetics: Given Intraspinally diffuse into the spinal nerve fibres, interrupting the passage of sensory and motor impulses at the level of the injection. The number of pain impulses blocked will be determined by the concentration of the anesthetic. The aim with the lower concentrations used is to reduce pain without motor loss Intraspinal medications vary in drug solubility. This variability effects the onset of action Lipophilic drugs (ie. Fentanyl and Bupivicaine (Marcaine) cross the dura or fat layer readily and provide a more rapid onset. While hydrophilic drugs such as morphine and hydromorphone cross slower thus have a slower onset. The poor lipid solubility may result in retention of the drug in the CNS and thus prolonged analgesia. CLASS : NARCOTIC ANALGESICS DRUG EPIMORPHINE HYDROMORPHONE FENTANYL SOLUBILITY Water soluble- slower onset Lipid soluble- fast onset Lipid soluble- fast onset ONSET minutes -Peaks in 60 mins 5-15 min 5-10 minutes- Peaks in 20 min DURATION Long hours Intermediate 7-19 hours Short -3-4 hour OTHER ADVERSE REACTIONS More spread to brain Delayed Respiratory depression can occur up 8-10 hrs and up to 24 hr but can occur as early as 30 mins after dosing. May cause more sedation then fentanyl because increased spread to the brain Less spread to brain Less delayed respiratory depression (3-4 hrs. post injection). Is most likely to be used in infusions. Increased sedation, Respiratory depression, hypotension, hallucinations, vomiting, constipation, urinary retention urticaria, rash, pruritis, allergic reaction Intraspinal Analgesia WRH 03/31/03 p. 10
11 The infusion rates will have variable ranges depending on: patient condition, infusion concentrations and if epidural or intrathecal route.- however the side effects are minimized with the use of infusion Side effects will be more gradual on onset Whenever a patient is receiving Intraspinal analgesia with a narcotic agent Narcan or naloxone should be readily available on the unit- need with decreased RR and PaO2 CLASS: LOCAL ANESTHETICS BUPIVACAINE (Marcaine) LIDOCAINE(Xylocaine) ONSET 5-25 minutes 5-10 minutes DURATION Long-acting Short-acting USE Used with opioid in continuous Used for test dose or to test catheter OTHER ADVERSE REACTIONS Lower doses are used in an infusion to obtain analgesic effect, sensory blockade is not the goal of trt but may occur in some individuals. It is appropriate as long as pain is controlled. Tends to block pain first, then sensation and then motor blockade. Urinary retention, allergic reaction, decreased bp, muscle weakness, vasodilation local anesthetic toxicity/ vascular absorption (s&s:metallic taste in mouth, Numbness of fingers, Ringing in ears The infusion rates will have variable ranges depending on: patient condition, infusion concentrations and if epidural or intrathecal route. Whenever a patient is receiving, Intraspinal analgesia with a local anaesthetic Ephedrine should be readily available on the unit for the treatment of hypotension. It may also be treated with fluids too. COMPARISON OF LOCAL ANESTHETICS & NEURAXIAL OPIOIDS SIDE EFFECT NEURAXIAL OPIOID LOCAL ANESTHETIC Postural Hypotension No Yes (below T10) Respiratory depression Yes, dose dependent No, if block is too high may experience it Urinary retention Yes, parasympathetic Yes, relatively short Interferes sphincter tone Pruritis Yes No Nausea, vomiting Yes No but may occur with hypotension, or may be a sign of toxicity Sedation Yes, less frequent than with IV No Intraspinal Analgesia WRH 03/31/03 p. 11
12 Use of Intraspinal Infusion and Systemic Opioids The nurse will have a role in monitoring pain level as the ideal analgesia levels are achieved for the patient on intraspinal infusion. IV opioids will need to be reduced when initiating an intraspinal infusion. The patient can receive other sedatives and opioids while on the infusion however must be titrated carefully. During the initiation of this therapy it is important to evaluate all sedatives and analgesia that the patient is receiving. The following is a conversion table for Morphine PO Morphine IV/SC Morphine Epidural Morphine Intrathecal Morphine 200 mg 100 mg 10 mg 1 mg Volume 3-7 mls With max of mls Volume.3-.7 ml With usual max of 1 ml Intraspinal Analgesia WRH 03/31/03 p. 12
13 Assess site of catheter placement Check for signs of infection Keep occlusive, transparent dressing intact- Reinforce prn Ensure catheter is secure Label site Observe the connector that it is secure Assess pain status Use the Pain scale to evaluate patient pain Document pain status on Intraspinal flow sheet Check system for mechanical errors or check site for leakage if pain relief ineffective Notify MD if pain relief ineffective Assess sensory and motor function Ask patient if legs are numb Assess if motor function affected Assess level of sensory blockade using Dermatomes- see next page Prior to ambulation assess for postural hypotension Patient should be accompanied to ambulate and transfer Assess bladder and sphincter function- record I&O, BMs, bladder distention Assess for side effects See previous pages- CONTACT & INFORM PHYSICIAN OF ANY SIGNS OF COMPLICATIONS Have appropriate reversal agents available Drugs and Pump Double check for correct drug and dosing Check pump settings and function Have reversal agents or ephedrine readily available on the unit Intraspinal Analgesia WRH 03/31/03 p. 13
14 Pain scale Face 0 - No Pain: content, pleasant, calm Face 1- Mild Pain: hurt, lack of expression Face 2 - Discomforting: concerned, troubled, uncomfortable Face 3 - Distressing; worried, anxious, restless Face 4- Horrible: moaning, pleading Face 5 - Excruciating: tears, frightened, Clenched teeth If unable to verbalize client / care giver to choose Face that best reflects pain Level of sedation (LOC) Degree of alertness or Level of sedation (LOC) is assessed using the following 0= Alert, Easy to rouse 1= Mild, Occasionally drowsy, easy to arouse 2= Moderate, Frequently drowsy, easy to rouse 3= Severe, Somnolent, difficult to Arouse S= Sleep, Normal, Easy to arouse Remember to assess respirations first, if less than 8-10/min attempt to arouse. If sedation level is greater than 2 notify Anesthesia Remember the placement and the amount of agent can influence the level of sedation. The goal is effective analgesia NOT anesthesia. Sensory Assessment Assess the level of block to see if it is changing refer dermatome illustration next page Assess sensation q2h numbness, tingling or normal sensation using cold sensation with ice. Run the ice up from the toe and note where coldness is detected by the patient Intraspinal Analgesia WRH 03/31/03 p. 14
15 C2 C2 C3 C3 C4 C6 T3 C8 C4 C5 T1 T5 T8 C7 T1 C8 T10 C5 C6 T3 T5 T8 T10 T12 L1 C7 S2 T12 L1 S3 S3 L3 S1 L3 L2 L5 L5 S1 Anterior Dermatomes Posterior Dermatomes Note: weakness is an expected finding this finding should be correlated to the level of sensation. If sensation or motor block is above the level specified higher notify MD. Intraspinal Analgesia WRH 03/31/03 p. 15
16 References Brant, J. (1995). The Use of Access Devices in Cancer Pain Control. Seminars in Oncology Nursing. Vol. 11 (3). Pp Dunajcik, L. (1988). Controlling the dangers of epidural analgesia. RN January. P Fisher, P. (1998). Epidural Pain Management Self Directed Learning Package. London. Fulk, C., Hadley, J.C. (1990). Something for Pain: New Trends in Epidural analgesia. Journal of Post Anesthesia Nursing. Vol. 5, No 4. P Litwack, K., Lubenow, T. (1989). Practical Points in the Management of Continuous Epidural Infusions. Journal of Post Anesthesia Nursing. Vol. 4, No 5. October. P Mercadante, S. (1999). Problems of long term spinal opioid treatment in advanced Cnacer Patients. Pain 79. Naber, L, Jones, G, Halm, M. (1994). Epidural Analgesia for Effective Pain control. Critical Care Nurse. October. P Pasero, C., Vanderveer,B. (1994). Epidural Infusions: Not just for Labour Anymore. AJN. December. P Ploughe, B. (1995). Home Epidural Analgesia Infusion. Journal of Neuroscience Nursing. Vol. 27(4) p Quinn, M. (1999). Outcomes and Complication of Epidural Analgesia in Patient with Chronic Cancer Pain. Cancer 85 (1). P Rosen, H. McCutheon- Calio, M. (19 ) An Epidural analgesia program: Balancing Risks and Benfits. Critical Care Nurse. Vol. 10, No 8. P St. Marie, B. (1991). Narcotic infusions. Journal of Intravenous Nursing. Vol. 14, No 5. Sept/October. P Skobel, S. (1996). Epidural Narcotic Administration: What Nurses should know. ONF. Vol. 23, No 10.p Slowikowski, R., Flaherty, S. (2000). Epidural Analgesia for Postoperative Orthopaedic Pain. Orthopaedic Nursing. Vol. 19, No 1. Jan/Feb. p Intraspinal Analgesia WRH 03/31/03 p. 16
17 Smitt, P. (1998). Outcomes and Complication of Epidural Analgesia in Patient with Chronic Cancer Pain.Cancer Vol. 83 (9). Strathern, D. (1996). Epidural analgesia: Educating patients and nurses. Nursing Standard. Vol. 10, No 25. March. P Wild, L. Coyne, C. (1992). The Basics and Beyond: Epidural Analgesia. AJN April. P Intraspinal Analgesia WRH 03/31/03 p. 17
18 Epidural Analgesia WRH 03/31/03 p. 18
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test
 Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
VAN WERT COUNTY HOSPITAL. Policy/Procedure: Departmental No.: N 11-36A. Issue Date: 7-97 By: Nursing No. of Pages: 6
 VAN WERT COUNTY HOSPITAL Policy/Procedure: Departmental No.: N 11-36A Issue Date: 7-97 By: Nursing No. of Pages: 6 Reviewed: 9-14, 8-11, 8-10 Revised: 9-14 Distribution List: All Nursing Departments Concurrence:
VAN WERT COUNTY HOSPITAL Policy/Procedure: Departmental No.: N 11-36A Issue Date: 7-97 By: Nursing No. of Pages: 6 Reviewed: 9-14, 8-11, 8-10 Revised: 9-14 Distribution List: All Nursing Departments Concurrence:
CENTRAL IOWA HEALTHCARE Marshalltown, Iowa
 CENTRAL IOWA HEALTHCARE Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.84 Subject: Policy: Purpose: Continuous Epidural Analgesia Acute or chronic pain relief provided to a patient
CENTRAL IOWA HEALTHCARE Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.84 Subject: Policy: Purpose: Continuous Epidural Analgesia Acute or chronic pain relief provided to a patient
SURGICAL NEURAXIAL ANALGESIA/ANESTHESIA EPIDURAL/PARAVERTEBRAL/ INTRATHECAL/PERIPHERAL REGIONAL, INTERMITTENT OR CONTINUOUS
 KINGSTON GENERAL HOSPITAL SURGICAL NEURAXIAL ANALGESIA/ANESTHESIA: EPIDURAL/PARAVERTEBRAL/ INTRATHECAL/PERIPHERAL REGIONAL, INTERMITTENT OR CONTINUOUS ANALGESIA/ANESTHESIA LEARNING GUIDE Prepared by: Nursing
KINGSTON GENERAL HOSPITAL SURGICAL NEURAXIAL ANALGESIA/ANESTHESIA: EPIDURAL/PARAVERTEBRAL/ INTRATHECAL/PERIPHERAL REGIONAL, INTERMITTENT OR CONTINUOUS ANALGESIA/ANESTHESIA LEARNING GUIDE Prepared by: Nursing
Pain Management Class Post-Test
 Name: Date: Unit: Pain Management Class Post-Test 1. Contraindications to regional anesthesia include (circle all that apply): a. Allergy to medication b. Clotting disorders or anticoagulation therapy
Name: Date: Unit: Pain Management Class Post-Test 1. Contraindications to regional anesthesia include (circle all that apply): a. Allergy to medication b. Clotting disorders or anticoagulation therapy
Regional Anesthesia. Fatiş Altındaş Dept. of Anesthesiology
 Regional Anesthesia Fatiş Altındaş Dept. of Anesthesiology Regional anesthesia - Definition Renders a specific area of the body, e.g. foot, arm, lower extremities insensating to stimulus of surgery or
Regional Anesthesia Fatiş Altındaş Dept. of Anesthesiology Regional anesthesia - Definition Renders a specific area of the body, e.g. foot, arm, lower extremities insensating to stimulus of surgery or
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs
 Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
PATIENT CARE MANUAL POLICY
 PATIENT CARE MANUAL POLICY NUMBER VII-A-15 PAGE 1 OF 3 APPROVED BY: CATEGORY: Vice President and Senior Operating Officer; Rural Health Services & Professional Practice Lead Body Systems; Central Nervous
PATIENT CARE MANUAL POLICY NUMBER VII-A-15 PAGE 1 OF 3 APPROVED BY: CATEGORY: Vice President and Senior Operating Officer; Rural Health Services & Professional Practice Lead Body Systems; Central Nervous
A Patient s Guide to Pain Management: Pain Pumps
 A Patient s Guide to Pain Management: Pain Pumps 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Pain Management: Pain Pumps 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
Pain Relief Options for Labor. Providing you with quality care, information and support
 Pain Relief Options for Labor Providing you with quality care, information and support What can I expect during my labor and delivery? As a patient in the Labor and Delivery suite at Lucile Packard Children
Pain Relief Options for Labor Providing you with quality care, information and support What can I expect during my labor and delivery? As a patient in the Labor and Delivery suite at Lucile Packard Children
Better Post-Op Pain Control Starts Here
 Better Post-Op Pain Control Starts Here POST-OP PAIN CONTROL PUMP It s Easy to Get Started About the ACCUFUSER Pump Thank you for considering the This brochure makes it easy for For complete information
Better Post-Op Pain Control Starts Here POST-OP PAIN CONTROL PUMP It s Easy to Get Started About the ACCUFUSER Pump Thank you for considering the This brochure makes it easy for For complete information
Sarah Reece-Stremtan M.D. Peripheral Nerve Blockade Neuraxial Blocks
 Neuraxial Anesthesia Sarah Reece-Stremtan M.D. Regional Anesthesia Peripheral Nerve Blockade Neuraxial Blocks Placed in the OR under general anesthesia by members of the regional anesthesia team 1 Sensory
Neuraxial Anesthesia Sarah Reece-Stremtan M.D. Regional Anesthesia Peripheral Nerve Blockade Neuraxial Blocks Placed in the OR under general anesthesia by members of the regional anesthesia team 1 Sensory
Epidural Analgesia in Labor - Whats s New
 Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
How and why to do an epidural in dogs and cats? Which Indications and which drugs?
 AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
Overview of Essentials of Pain Management. Updated 11/2016
 0 Overview of Essentials of Pain Management Updated 11/2016 1 Overview of Essentials of Pain Management 1. Assess pain intensity on a 0 10 scale in which 0 = no pain at all and 10 = the worst pain imaginable.
0 Overview of Essentials of Pain Management Updated 11/2016 1 Overview of Essentials of Pain Management 1. Assess pain intensity on a 0 10 scale in which 0 = no pain at all and 10 = the worst pain imaginable.
Obstetrical Anesthesia. Safe Pain Relief for Childbirth
 Obstetrical Anesthesia Safe Pain Relief for Childbirth Introduction Pain relief (analgesia) for labor and delivery is now safer than ever. In the United States approximately two-thirds of all women receive
Obstetrical Anesthesia Safe Pain Relief for Childbirth Introduction Pain relief (analgesia) for labor and delivery is now safer than ever. In the United States approximately two-thirds of all women receive
KINGSTON GENERAL HOSPITAL NURSING SERVICE CARE OF THE PATIENT FOLLOWING SPINAL (INTRATHECAL) ANESTHESIA/ANALGESIA LEARNING GUIDE
 1 KINGSTON GENERAL HOSPITAL NURSING SERVICE CARE OF THE PATIENT FOLLOWING SPINAL (INTRATHECAL) ANESTHESIA/ANALGESIA LEARNING GUIDE Prepared by: Nursing Education Date: 2009 March Revised: 2016 July Date
1 KINGSTON GENERAL HOSPITAL NURSING SERVICE CARE OF THE PATIENT FOLLOWING SPINAL (INTRATHECAL) ANESTHESIA/ANALGESIA LEARNING GUIDE Prepared by: Nursing Education Date: 2009 March Revised: 2016 July Date
ATI Skills Modules Checklist for Central Venous Access Devices
 For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Central Venous Access Devices Student s name Date Verify order Patient record Assess for procedure need Identify, gather,
For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Central Venous Access Devices Student s name Date Verify order Patient record Assess for procedure need Identify, gather,
Pharmacologic Pain Relief: It s Use in Labor. Linda Robinson MSN, RNC Clinical Nurse Specialist, Northwest Hospital Spring, 2016
 Pharmacologic Pain Relief: It s Use in Labor Linda Robinson MSN, RNC Clinical Nurse Specialist, Northwest Hospital Spring, 2016 Objectives Recognize common medications used in the management of labor pain
Pharmacologic Pain Relief: It s Use in Labor Linda Robinson MSN, RNC Clinical Nurse Specialist, Northwest Hospital Spring, 2016 Objectives Recognize common medications used in the management of labor pain
Epidural Analgesia in Labor
 Epidural Analgesia in Labor Epidural analgesia is one of the most advanced methods used for labor pain relief. At our maternity hospital, it is a well proven and the most frequently used method. The following
Epidural Analgesia in Labor Epidural analgesia is one of the most advanced methods used for labor pain relief. At our maternity hospital, it is a well proven and the most frequently used method. The following
INTRATHECAL ANALGESIA IN CANCER PAIN A RESOURCE FOR HEALTH PROFESSIONALS
 INTRATHECAL ANALGESIA IN CANCER PAIN A RESOURCE FOR HEALTH PROFESSIONALS Canterbury Regional Cancer and Haematology Service Palliative Care Service 2014 CONTENTS Introduction Associated Resources Nursing
INTRATHECAL ANALGESIA IN CANCER PAIN A RESOURCE FOR HEALTH PROFESSIONALS Canterbury Regional Cancer and Haematology Service Palliative Care Service 2014 CONTENTS Introduction Associated Resources Nursing
Epidural analgesia technique
 Epidural analgesia technique Martin Pearson School of Veterinary Science University of Queensland, Gatton 0254601834 Peter Best Greencross South Tamworth Animal Hospital 88Duri Road, Tamworth 02 6765 4244
Epidural analgesia technique Martin Pearson School of Veterinary Science University of Queensland, Gatton 0254601834 Peter Best Greencross South Tamworth Animal Hospital 88Duri Road, Tamworth 02 6765 4244
STANDARDIZED PROCEDURE REPROGRAMMING AND REFILLING INTRATHECAL BACLOFEN PUMPS and ACCESSING THE CATHETER ACCESS PORT (Adult,Peds)
 I. Definition The purpose of this procedure is to allow the Advanced Health Practitioner (AHP) to reprogram and refill intrathecal Baclofen pumps, as well as access the catheter access port for those AHPs
I. Definition The purpose of this procedure is to allow the Advanced Health Practitioner (AHP) to reprogram and refill intrathecal Baclofen pumps, as well as access the catheter access port for those AHPs
GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR
 GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR INTRODUCTION Regional block provides superior pain relief, compared
GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR INTRODUCTION Regional block provides superior pain relief, compared
PATIENT CONTROLLED ANALGESIA LEARNING PACKAGE
 1 PATIENT CONTROLLED ANALGESIA LEARNING PACKAGE 2 Table of Contents page# Learning Objectives 3 Concepts of Pain Relief 4 Introduction to PCA 4 Definition of terms used with IV PCA 6 Opioids used with
1 PATIENT CONTROLLED ANALGESIA LEARNING PACKAGE 2 Table of Contents page# Learning Objectives 3 Concepts of Pain Relief 4 Introduction to PCA 4 Definition of terms used with IV PCA 6 Opioids used with
Analgesia. The modern approach. Dr. Mark Haworth MB.ChB.DA.MRCA.
 Analgesia The modern approach Dr. Mark Haworth MB.ChB.DA.MRCA. What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) How is pain
Analgesia The modern approach Dr. Mark Haworth MB.ChB.DA.MRCA. What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) How is pain
CONTROLLED DOCUMENT. Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) Controlled Document Number: CG259
 Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor:
Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor:
GREY NUNS and MISERICORDIA SITES CERTIFICATION MODULE. for EPIDURAL / SPINAL ANALGESIA / ANESTHESIA
 GREY NUNS and MISERICORDIA SITES CERTIFICATION MODULE for EPIDURAL / SPINAL ANALGESIA / ANESTHESIA CERTIFICATION PROGRAM FOR THE ADMINISTRATION OF POSTOPERATIVE ANALGESICS THROUGH AN EPIDURAL CATHETER
GREY NUNS and MISERICORDIA SITES CERTIFICATION MODULE for EPIDURAL / SPINAL ANALGESIA / ANESTHESIA CERTIFICATION PROGRAM FOR THE ADMINISTRATION OF POSTOPERATIVE ANALGESICS THROUGH AN EPIDURAL CATHETER
Purpose: The goal of epidural anesthesia is to reduce or eliminate pain in the laboring patient.
 Alaska Native Medical Center: Mother Baby Unit Subject: Epidural Anesthesia/PCEA in Laboring Patients Guideline: Epidural Anesthesia in Laboring Patients REVISION DATE: March 2013 REPLACES: L&D Epidural
Alaska Native Medical Center: Mother Baby Unit Subject: Epidural Anesthesia/PCEA in Laboring Patients Guideline: Epidural Anesthesia in Laboring Patients REVISION DATE: March 2013 REPLACES: L&D Epidural
Dr P.W.Buczkowski. Consultant in Anaesthesia & Pain Medicine. Royal Derby Hospital
 Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
Perioperative Pain Management
 Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
To ensure safe administration of analgesia by the epidural/intrathecal route in the community setting
 Document reference code: CLIN:N.SS/001/2001 Title: Developed by: Document status: Ratified by: on: Date to be reviewed: Purpose: GUIDELINES FOR THE MANAGEMENT OF INTRASPINAL CATHETERS IN THE COMMUNITY
Document reference code: CLIN:N.SS/001/2001 Title: Developed by: Document status: Ratified by: on: Date to be reviewed: Purpose: GUIDELINES FOR THE MANAGEMENT OF INTRASPINAL CATHETERS IN THE COMMUNITY
Central Nervous System: Part 2
 Central Nervous System: Part 2 1. Meninges 2. CSF 3. Spinal Cord and Spinal Nerves Explain spinal cord anatomy, including gray and white matter and meninges (give the general functions of this organ).
Central Nervous System: Part 2 1. Meninges 2. CSF 3. Spinal Cord and Spinal Nerves Explain spinal cord anatomy, including gray and white matter and meninges (give the general functions of this organ).
Title: RN Specialty Practice: RN Procedure: Epidural Catheter Removal. I.D. Number: 1080
 Policies and Procedures Title: EPIDURAL CATHETER REMOVAL RN Specialty Practice: RN Procedure: Epidural Catheter Removal I.D. Number: 1080 Authorization: [X] Former SKtnHR Nursing Practice Committee Source:
Policies and Procedures Title: EPIDURAL CATHETER REMOVAL RN Specialty Practice: RN Procedure: Epidural Catheter Removal I.D. Number: 1080 Authorization: [X] Former SKtnHR Nursing Practice Committee Source:
Pharmacologic Pain Relief: It s Use in Labor
 Pharmacologic Pain Relief: It s Use in Labor Linda Robinson MSN, RNC Clinical Nurse Specialist, Northwest Hospital Fall, 2016 Objectives Recognize common medications used in the management of labor pain
Pharmacologic Pain Relief: It s Use in Labor Linda Robinson MSN, RNC Clinical Nurse Specialist, Northwest Hospital Fall, 2016 Objectives Recognize common medications used in the management of labor pain
PAEDIATRIC NERVE BLOCK / WOUND INFILTRATION
 PAEDIATRIC NERVE BLOCK / WOUND INFILTRATION Addendum to the MULTIDISCIPLINARY GUIDELINES FOR ACUTE PAIN MANAGEMENT IN CHILDREN AND YOUNG PEOPLE Policy Owner: Approved by: Ratified by: ABMU HB Pain Management
PAEDIATRIC NERVE BLOCK / WOUND INFILTRATION Addendum to the MULTIDISCIPLINARY GUIDELINES FOR ACUTE PAIN MANAGEMENT IN CHILDREN AND YOUNG PEOPLE Policy Owner: Approved by: Ratified by: ABMU HB Pain Management
Emergency clamp should always be readily available in case of accidental catheter fracture
 Note: Please see individual policies for further information. Flushing best practice: Always use a 10 diameter syringe or larger when first accessing and when flushing vascular access device (VAD) Use
Note: Please see individual policies for further information. Flushing best practice: Always use a 10 diameter syringe or larger when first accessing and when flushing vascular access device (VAD) Use
GUIDELINES AND AUDIT IMPLEMENTATION NETWORK
 GUIDELINES AND AUDIT IMPLEMENTATION NETWORK General Palliative Care Guidelines The Management of Pain at the End Of Life November 2010 Aim To provide a user friendly, evidence based guide for the management
GUIDELINES AND AUDIT IMPLEMENTATION NETWORK General Palliative Care Guidelines The Management of Pain at the End Of Life November 2010 Aim To provide a user friendly, evidence based guide for the management
8/30/2010. Structured:
 3 4 5 6 7 8 9 Unit II Biopsychosocial Concepts Related to Health Care Communication Conflict Resolution - Huber Pain Management - LeMone Chp 9 Objectives Discuss importance of communication and documentation.
3 4 5 6 7 8 9 Unit II Biopsychosocial Concepts Related to Health Care Communication Conflict Resolution - Huber Pain Management - LeMone Chp 9 Objectives Discuss importance of communication and documentation.
50a A&P: Nervous System -! Peripheral Nervous System
 50a A&P: Nervous System -! Peripheral Nervous System 50a A&P: Nervous System -! Peripheral Nervous System! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
50a A&P: Nervous System -! Peripheral Nervous System 50a A&P: Nervous System -! Peripheral Nervous System! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
Paravertebral policy. The Acute pain Management Dept, UCLH
 UCLH PARAVERTEBRAL BLOCK (ADULTS) POLICY Paravertebral policy. The Acute pain Management Dept, UCLH DEFINITION A Paravertebral block is a method of providing effective analgesia using a local anaesthetic.
UCLH PARAVERTEBRAL BLOCK (ADULTS) POLICY Paravertebral policy. The Acute pain Management Dept, UCLH DEFINITION A Paravertebral block is a method of providing effective analgesia using a local anaesthetic.
Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and
 1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
Comprehensive Centers for Pain Management. Common Injection and Implant Procedures for the Treatment of Acute and Chronic Back Pain
 Comprehensive Centers for Pain Management Common Injection and Implant Procedures for the Treatment of Acute and Chronic Back Pain There are many different treatments for back pain. Taking lots of drugs
Comprehensive Centers for Pain Management Common Injection and Implant Procedures for the Treatment of Acute and Chronic Back Pain There are many different treatments for back pain. Taking lots of drugs
ISPUB.COM. Epidural For Pain Control After Surgery. A Kowalski, O Wenker WHAT IS AN EPIDURAL? WHY SHOULD I HAVE AN EPIDURAL?
 ISPUB.COM The Internet Journal of Pain, Symptom Control and Palliative Care Volume 2 Number 1 A Kowalski, O Wenker Citation A Kowalski, O Wenker.. The Internet Journal of Pain, Symptom Control and Palliative
ISPUB.COM The Internet Journal of Pain, Symptom Control and Palliative Care Volume 2 Number 1 A Kowalski, O Wenker Citation A Kowalski, O Wenker.. The Internet Journal of Pain, Symptom Control and Palliative
Collaboration. cross sector HPC. hpcconnection.ca. Analgesia. epidural. patient centered. evidence based. Physicians. Excellence
 HPC hpcconnection.ca Neuro - axial Nursing Analgesia cross sector Collaboration Pharmacists Intractable patient centered Opioids Interventional Consensus Anesthesia Physicians epidural evidence based Intraspinal
HPC hpcconnection.ca Neuro - axial Nursing Analgesia cross sector Collaboration Pharmacists Intractable patient centered Opioids Interventional Consensus Anesthesia Physicians epidural evidence based Intraspinal
CLINICAL GUIDELINES ID TAG Continuous Peripheral Nerve Block Guideline Dr Peter Merjavy and Dr Aidan Cullen
 Title: Author: CLINICAL GUIDELINES ID TAG Continuous Peripheral Nerve Block Guideline Dr Peter Merjavy and Dr Aidan Cullen Speciality / Division: Directorate: Anaesthetics / ATICS Acute Date Uploaded:
Title: Author: CLINICAL GUIDELINES ID TAG Continuous Peripheral Nerve Block Guideline Dr Peter Merjavy and Dr Aidan Cullen Speciality / Division: Directorate: Anaesthetics / ATICS Acute Date Uploaded:
Managing Pain and Sickness after Surgery
 Managing Pain and Sickness after Surgery This pamphlet explains about pain relief after surgery. There are many effective treatments to help keep you comfortable after your operation. The different ways
Managing Pain and Sickness after Surgery This pamphlet explains about pain relief after surgery. There are many effective treatments to help keep you comfortable after your operation. The different ways
PCA PRESCRIPTION is valid for a maximum of 4 days unless ceased earlier. Date: BINDING MARGIN - NO WRITING BINDING MARGIN - NO WRITING
 Attach ADR Sticker THESE INSTRUCTIONS EXPLAIN WHEN TO MAKE A CLINICAL REVIEW OR RAPID RESPONSE CALL, YOUR LOCAL ESCALATION PROTOCOL WILL EXPLAIN HOW TO MAKE A CALL PCA ALLERGIES & ADVERSE DRUG REACTIONS
Attach ADR Sticker THESE INSTRUCTIONS EXPLAIN WHEN TO MAKE A CLINICAL REVIEW OR RAPID RESPONSE CALL, YOUR LOCAL ESCALATION PROTOCOL WILL EXPLAIN HOW TO MAKE A CALL PCA ALLERGIES & ADVERSE DRUG REACTIONS
Epidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal
 Information for patients pidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal This leaflet has been made using information from the Royal College
Information for patients pidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal This leaflet has been made using information from the Royal College
Chapter 12b. Overview
 Chapter 12b Spinal Cord Overview Spinal cord gross anatomy Spinal meninges Sectional anatomy Sensory pathways Motor pathways Spinal cord pathologies 1 The Adult Spinal Cord About 18 inches (45 cm) long
Chapter 12b Spinal Cord Overview Spinal cord gross anatomy Spinal meninges Sectional anatomy Sensory pathways Motor pathways Spinal cord pathologies 1 The Adult Spinal Cord About 18 inches (45 cm) long
Pain Management Clinic ISIC
 Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
Pain relief after major surgery
 Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Central Venous Catheter Care and Maintenance (includes catheter troubleshooting guide)
 Central Venous Catheter Care and Maintenance (includes catheter troubleshooting guide) A Guide for Patients in the Home Phone Number: Nurse/Contact: Central Venous Catheters This manual is a guide for
Central Venous Catheter Care and Maintenance (includes catheter troubleshooting guide) A Guide for Patients in the Home Phone Number: Nurse/Contact: Central Venous Catheters This manual is a guide for
IR Central Venous Access [ ] Pre Procedure
![IR Central Venous Access [ ] Pre Procedure IR Central Venous Access [ ] Pre Procedure](/thumbs/90/104119758.jpg) IR Central Venous Access [1050200001] Pre Procedure Case Request/Scheduling Procedure Enter IR Case Request if not already completed (All hospitals except Grant Medical Center) [ ] Case Request IR Lab
IR Central Venous Access [1050200001] Pre Procedure Case Request/Scheduling Procedure Enter IR Case Request if not already completed (All hospitals except Grant Medical Center) [ ] Case Request IR Lab
Pain relief that s better for every body. ON-Q* Pump with ONDEMAND* Bolus Button. myon-q.com. As determined by your doctor
 Pain relief that s better for every body. ON-Q* Pump with ONDEMAND* Bolus Button 24-Hour Product Support Hotline 800.444.2728 myon-q.com FACEBOOK.COM/ONQPAINRELIEF TWITTER.COM/ONQPAINRELIEF As determined
Pain relief that s better for every body. ON-Q* Pump with ONDEMAND* Bolus Button 24-Hour Product Support Hotline 800.444.2728 myon-q.com FACEBOOK.COM/ONQPAINRELIEF TWITTER.COM/ONQPAINRELIEF As determined
The Spinal Cord & Spinal Nerves
 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
Pain Management Strategies Webinar/Teleconference
 Pain Management Strategies Webinar/Teleconference Barry K. Baines, MD April 16, 2009 Objectives Describe the principles of pain management. Identify considerations in the use of opioids. Describe the benefits
Pain Management Strategies Webinar/Teleconference Barry K. Baines, MD April 16, 2009 Objectives Describe the principles of pain management. Identify considerations in the use of opioids. Describe the benefits
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
GUIDELINES ON THE MANAGEMENT OF PAIN DUE TO CANCER IN ADULTS
 GUIDELINES ON THE MANAGEMENT OF PAIN DUE TO CANCER IN ADULTS Bristol Palliative Care Collaborative Contact Numbers: Hospital Specialist Palliative Care Teams: North Bristol 0117 4146392 UH Bristol 0117
GUIDELINES ON THE MANAGEMENT OF PAIN DUE TO CANCER IN ADULTS Bristol Palliative Care Collaborative Contact Numbers: Hospital Specialist Palliative Care Teams: North Bristol 0117 4146392 UH Bristol 0117
Epidural Infusions for Pain Relief Including Discharge Advice
 Royal Manchester Children s Hospital Epidural Infusions for Pain Relief Including Discharge Advice Children s Pain Team- Information For Parents and Carers This leaflet aims to provide information for
Royal Manchester Children s Hospital Epidural Infusions for Pain Relief Including Discharge Advice Children s Pain Team- Information For Parents and Carers This leaflet aims to provide information for
1/21/14. Cancer Related Pain: Case-Based Pharmacology. Conflicts of Interest. Learning Objective
 Cancer Related Pain: Case-Based Pharmacology Jeannine M. Brant, PhD, APRN, AOCN Oncology Clinical Nurse Specialist Nurse Scientist Billings Clinic Conflicts of Interest Jeannine Brant has served on the
Cancer Related Pain: Case-Based Pharmacology Jeannine M. Brant, PhD, APRN, AOCN Oncology Clinical Nurse Specialist Nurse Scientist Billings Clinic Conflicts of Interest Jeannine Brant has served on the
Annual Pain Competency
 Annual Pain Competency 2016 Revised for RBMC Please call Professional Development at X4196 or X5947 if you have any questions The learner will be able to: Objectives Explain pain scales & appropriate use
Annual Pain Competency 2016 Revised for RBMC Please call Professional Development at X4196 or X5947 if you have any questions The learner will be able to: Objectives Explain pain scales & appropriate use
Optimizing Your Quality of Life During Cancer Treatment: Pain & Side Effect Management
 Optimizing Your Quality of Life During Cancer Treatment: Pain & Side Effect Management Eric Roeland, MD GI Oncology Palliative Medicine Pancreatic Cancer Patient Tool Belt Chemotherapy Surgery Pain & Symptom
Optimizing Your Quality of Life During Cancer Treatment: Pain & Side Effect Management Eric Roeland, MD GI Oncology Palliative Medicine Pancreatic Cancer Patient Tool Belt Chemotherapy Surgery Pain & Symptom
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
PAIN MANAGEMENT Patient established on oral morphine or opioid naive.
 PAIN MANAGEMENT Patient established on oral morphine or opioid naive. Important; It is the responsibility of the prescriber to ensure that guidelines are followed when prescribing opioids. Every member
PAIN MANAGEMENT Patient established on oral morphine or opioid naive. Important; It is the responsibility of the prescriber to ensure that guidelines are followed when prescribing opioids. Every member
Patient Positioning strategies and Service Manual
 Patient Positioning strategies and Service Manual Simple Becomes Simply Amazing Smart Way Old Way Patent Pending Proudly Made In The USA Patient Positioning is everything. How is an epidural given? Intravenous
Patient Positioning strategies and Service Manual Simple Becomes Simply Amazing Smart Way Old Way Patent Pending Proudly Made In The USA Patient Positioning is everything. How is an epidural given? Intravenous
Your Nerve Block & Home Pump For Knee Surgery
 Your Nerve Block & Home Pump For Knee Surgery Department of Anesthesiology and Perioperative Medicine Updated 9/12 Why? To Help Control Postoperative Pain at Home A pump connected to plastic tubing will
Your Nerve Block & Home Pump For Knee Surgery Department of Anesthesiology and Perioperative Medicine Updated 9/12 Why? To Help Control Postoperative Pain at Home A pump connected to plastic tubing will
All about your anaesthetic
 Patient information leaflet All about your anaesthetic Spinal anaesthesia and 3 associated risks For patients having a surgical procedure at a Care UK independent diagnostic and treatment centre This
Patient information leaflet All about your anaesthetic Spinal anaesthesia and 3 associated risks For patients having a surgical procedure at a Care UK independent diagnostic and treatment centre This
Chapter 13. The Spinal Cord & Spinal Nerves. Spinal Cord. Spinal Cord Protection. Meninges. Together with brain forms the CNS Functions
 Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Guideline for the Post Operative Management of Women who have received Intrathecal or Epidural Opioid Analgesia for Caesarean Section
 Guideline for the Post Operative Management of Women who have received Intrathecal or Epidural Opioid Analgesia for Caesarean Section Speciality: Maternity Approval Body: Labour Ward Forum Approval Date:
Guideline for the Post Operative Management of Women who have received Intrathecal or Epidural Opioid Analgesia for Caesarean Section Speciality: Maternity Approval Body: Labour Ward Forum Approval Date:
Acute Pain NETP: SEPTEMBER 2013 COHORT
 Acute Pain NETP: SEPTEMBER 2013 COHORT Pain & Suffering an unpleasant sensory & emotional experience associated with actual or potential tissue damage, or described in terms of such damage International
Acute Pain NETP: SEPTEMBER 2013 COHORT Pain & Suffering an unpleasant sensory & emotional experience associated with actual or potential tissue damage, or described in terms of such damage International
Epidural anaesthesia and analgesia
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Epidural anaesthesia and analgesia Author : Matthew Gurney Categories : Vets Date : June 1, 2009 Matthew Gurney discusses
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Epidural anaesthesia and analgesia Author : Matthew Gurney Categories : Vets Date : June 1, 2009 Matthew Gurney discusses
KNOWLEDGE BASE: 1. These patients will be cared for in the following nursing departments: critical care, 5ET (Neuro), PACU, Radiology or ECC.
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: LUMBAR INTRATHECAL SUBARACHNOID CEREBROSPINAL FLUID CATHETER (Set Up and Maintenance) - ADULTS (neu02) Nursing DATE: REVIEWED: PAGES: RESPONSIBILITY:
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: LUMBAR INTRATHECAL SUBARACHNOID CEREBROSPINAL FLUID CATHETER (Set Up and Maintenance) - ADULTS (neu02) Nursing DATE: REVIEWED: PAGES: RESPONSIBILITY:
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet February 2018 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used
Epidural Continuous Infusion Patient information Leaflet February 2018 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used
IV Fluids. Nursing B23. Objectives. Serum Osmolality
 IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
Gross Morphology of Spinal Cord
 Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Spinal Column. Anatomy Of The Spine
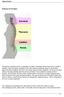 Anatomy Of The Spine The spine is a flexible column, composed of a stack of individual bones. Each bone is called a vertebra. There are seven vertebrae in the neck (cervical vertebrae) twelve in the thoracic
Anatomy Of The Spine The spine is a flexible column, composed of a stack of individual bones. Each bone is called a vertebra. There are seven vertebrae in the neck (cervical vertebrae) twelve in the thoracic
NON-OPIOID ANALGESIA & THE IMPLICATIONS OF ANESTHETIC DRUGS IN THE PERI-ANESTHETIC ARENA AMANDA AFFLECK CRNA
 NON-OPIOID ANALGESIA & THE IMPLICATIONS OF ANESTHETIC DRUGS IN THE PERI-ANESTHETIC ARENA AMANDA AFFLECK CRNA OR, ANESTHESIA, WHY DO THEY DO THAT? OUTLINE Neurotransmission of pain Arachidonic Acid pathway
NON-OPIOID ANALGESIA & THE IMPLICATIONS OF ANESTHETIC DRUGS IN THE PERI-ANESTHETIC ARENA AMANDA AFFLECK CRNA OR, ANESTHESIA, WHY DO THEY DO THAT? OUTLINE Neurotransmission of pain Arachidonic Acid pathway
WHS POSTOPERATIVE POWERPLAN CHANGES
 Medications simplified and standardized to improve safety and effectiveness in the management of pain, itching, nausea/vomiting. Management: o The Anesthesiologist will continue to manage pain in the PACU.
Medications simplified and standardized to improve safety and effectiveness in the management of pain, itching, nausea/vomiting. Management: o The Anesthesiologist will continue to manage pain in the PACU.
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Spinal Anaesthesia and Analgesia. Patient information Leaflet
 Spinal Anaesthesia and Analgesia Patient information Leaflet February 2018 Introduction For many operations, patients receive a general anaesthetic and remain asleep during the operation. A spinal anaesthetic
Spinal Anaesthesia and Analgesia Patient information Leaflet February 2018 Introduction For many operations, patients receive a general anaesthetic and remain asleep during the operation. A spinal anaesthetic
IV Fluids Nursing B23 Objectives Serum Osmolality 275 to 295 Isotonic
 1 IV Fluids Nursing B23 2 Objectives 3 Serum Osmolality Serum osmolality solute concentration of a solution Higher osmolality means greater pulling power for water Normal serum osmolality is 275 to 295
1 IV Fluids Nursing B23 2 Objectives 3 Serum Osmolality Serum osmolality solute concentration of a solution Higher osmolality means greater pulling power for water Normal serum osmolality is 275 to 295
Peripheral Nerve Blocks
 Peripheral Nerve Blocks N U R S I N G E D U C A T I O N JPS Acute Pain Service Peripheral nerve blocks are used as part of a multimodal analgesic program which provides the patient with safe and effective
Peripheral Nerve Blocks N U R S I N G E D U C A T I O N JPS Acute Pain Service Peripheral nerve blocks are used as part of a multimodal analgesic program which provides the patient with safe and effective
morphine 30 mg/ 30 ml (1 mg/ml) Opioid of choice
 PATIENT CONTROLLED ANALGESIA (PCA) PLAN Allergies: Medication Selection: morphine 30 mg/ 30 ml (1 mg/ml) Opioid of choice HYDROmorphone (Dilaudid ) 6 mg/ 30 ml (0.2 mg/ml) fentanyl 300 mcg/ 30 ml (10 mcg/ml)
PATIENT CONTROLLED ANALGESIA (PCA) PLAN Allergies: Medication Selection: morphine 30 mg/ 30 ml (1 mg/ml) Opioid of choice HYDROmorphone (Dilaudid ) 6 mg/ 30 ml (0.2 mg/ml) fentanyl 300 mcg/ 30 ml (10 mcg/ml)
2. Need for serial arterial blood gas determinations. 2. Anticipation of the initiation of thrombolytic therapy
 I. Subject: Arterial Cannulation II. Policy: Arterial cannulation will be performed upon a physician's order by Cardiopulmonary and Respiratory Therapy personnel certified in the arterial catheterization
I. Subject: Arterial Cannulation II. Policy: Arterial cannulation will be performed upon a physician's order by Cardiopulmonary and Respiratory Therapy personnel certified in the arterial catheterization
Chapter 19. Media Directory. Topical (Surface) Anesthesia. Spinal Anesthesia. Nerve-Block Anesthesia. Infiltration (Field-Block) Anesthesia
 Chapter 19 Drugs for Local and General Anesthesia Slide 18 Media Directory Lidocaine Animation Upper Saddle River, New Jersey 07458 All rights reserved. Topical (Surface) Anesthesia Creams, sprays, suppositories
Chapter 19 Drugs for Local and General Anesthesia Slide 18 Media Directory Lidocaine Animation Upper Saddle River, New Jersey 07458 All rights reserved. Topical (Surface) Anesthesia Creams, sprays, suppositories
Your Anaesthetic Explained
 Your Anaesthetic Explained Patient Information Sheet Pre Admission Assessment Clinic Tel: 4920307 What is anaesthesia? The word anaesthesia means loss of sensation. If you have ever had a dental injection
Your Anaesthetic Explained Patient Information Sheet Pre Admission Assessment Clinic Tel: 4920307 What is anaesthesia? The word anaesthesia means loss of sensation. If you have ever had a dental injection
GUIDELINE FOR THE POST OPERATIVE MANAGEMENT OF WOMEN WHO HAVE RECEIVED INTRATHECAL OR EPIDURAL OPIOID ANALGESIA FOR CAESAREAN SECTION
 GUIDELINE FOR THE POST OPERATIVE MANAGEMENT OF WOMEN WHO HAVE RECEIVED INTRATHECAL OR EPIDURAL OPIOID ANALGESIA FOR CAESAREAN SECTION Originator: Maternity Services & Anaesthetics Dept Date Approved: January
GUIDELINE FOR THE POST OPERATIVE MANAGEMENT OF WOMEN WHO HAVE RECEIVED INTRATHECAL OR EPIDURAL OPIOID ANALGESIA FOR CAESAREAN SECTION Originator: Maternity Services & Anaesthetics Dept Date Approved: January
Palliative Prescribing - Pain
 Palliative Prescribing - Pain LAURA BARNFIELD 21/2/17 Aims To understand the classes of painkillers available in palliative care To gain confidence in counselling regarding opiates To gain confidence prescribing
Palliative Prescribing - Pain LAURA BARNFIELD 21/2/17 Aims To understand the classes of painkillers available in palliative care To gain confidence in counselling regarding opiates To gain confidence prescribing
PALLIATIVE TREATMENT BY DR. KHRONGKAMOL SIHABAN MEDICAL ONCOLOGIST
 PALLIATIVE TREATMENT BY DR. KHRONGKAMOL SIHABAN MEDICAL ONCOLOGIST TREATMENT IN ONCOLOGY Main treatment : surgery Neoadjuvant treatment : RT, CMT Adjuvant treatment : Tx micrometastatic disease -CMT,Targeted
PALLIATIVE TREATMENT BY DR. KHRONGKAMOL SIHABAN MEDICAL ONCOLOGIST TREATMENT IN ONCOLOGY Main treatment : surgery Neoadjuvant treatment : RT, CMT Adjuvant treatment : Tx micrometastatic disease -CMT,Targeted
Pain Management: Epidural Steroid Injections
 A Patient s Guide to Pain Management: Epidural Steroid Injections 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Pain Management: Epidural Steroid Injections 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from
Aus Artificial Uretheral Sphincter Port System
 NORFOLK VET PRODUCTS the AUS for the long-term relief of incontinence in dogs and cats making life easier for pets Speciality Medical Devices For The Veterinary Community the Aus Artificial Uretheral Sphincter
NORFOLK VET PRODUCTS the AUS for the long-term relief of incontinence in dogs and cats making life easier for pets Speciality Medical Devices For The Veterinary Community the Aus Artificial Uretheral Sphincter
MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life
 MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life The following pages are guidelines for the management of common symptoms for a person thought to be
MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life The following pages are guidelines for the management of common symptoms for a person thought to be
Understanding your HICKMAN CATHETER
 Understanding your HICKMAN CATHETER Patient Information What is the purpose of this information sheet? This information sheet has been written by patients, members of the public and health professionals.
Understanding your HICKMAN CATHETER Patient Information What is the purpose of this information sheet? This information sheet has been written by patients, members of the public and health professionals.
Improving Pain Management: The UCSF Journey
 Improving Pain Management: The UCSF Journey April 2014 Adam Cooper, RN, MSN Clinical Nurse Educator Institute for Nursing Excellence UCSF Medical Center After this discussion, learners will be able to:
Improving Pain Management: The UCSF Journey April 2014 Adam Cooper, RN, MSN Clinical Nurse Educator Institute for Nursing Excellence UCSF Medical Center After this discussion, learners will be able to:
Pain management in Paediatric Palliative Care. Dr Jane Nakawesi 14 th August 2017
 Pain management in Paediatric Palliative Care Dr Jane Nakawesi 14 th August 2017 Content Management of pain in children Non pharmacological Pharmacological Exit level outcomes The participants will: Know
Pain management in Paediatric Palliative Care Dr Jane Nakawesi 14 th August 2017 Content Management of pain in children Non pharmacological Pharmacological Exit level outcomes The participants will: Know
Spinal Analgesia (Neuraxial analgesia in humans)
 Spinal Analgesia (Neuraxial analgesia in humans) Paul Farquhar-Smith The Royal Marsden NHS Foundation Trust And other humanoid species Neuraxial analgesia Cancer pain ADDITIONAL ANALGESIC MEASURES FINAL
Spinal Analgesia (Neuraxial analgesia in humans) Paul Farquhar-Smith The Royal Marsden NHS Foundation Trust And other humanoid species Neuraxial analgesia Cancer pain ADDITIONAL ANALGESIC MEASURES FINAL
Pain Relief During Labor
 UW MEDICINE PATIENT EDUCATION Pain Relief During Labor Common pain relief options This chapter explains common pain relief options used during labor and delivery, when and how they are used, and what the
UW MEDICINE PATIENT EDUCATION Pain Relief During Labor Common pain relief options This chapter explains common pain relief options used during labor and delivery, when and how they are used, and what the
Your Nerve Block & Home Pump For Shoulder Surgery
 Your Nerve Block & Home Pump For Shoulder Surgery Department of Anesthesiology and Perioperative Medicine www.happypatient.org Updated 10/09 Why? To Help Control Postoperative Pain at Home A pump connected
Your Nerve Block & Home Pump For Shoulder Surgery Department of Anesthesiology and Perioperative Medicine www.happypatient.org Updated 10/09 Why? To Help Control Postoperative Pain at Home A pump connected
