PAIN EDUCATION Module 4: Treatment of chronic back pain
|
|
|
- Cody Parsons
- 6 years ago
- Views:
Transcription
1 The full version of this slide deck in MS PowerPoint format (containing presentation view and expanded notes) can be downloaded on please register! PAIN EDUCATION Module 4: Treatment of chronic back pain
2 2013 Excerpta Medica BV The material presented in this teaching slide deck is for educational purposes only. If you wish to reproduce, transmit in any form or by any means, electronic, mechanical, photocopying, recording, or otherwise, any part of the material presented, you will need to obtain all the necessary permissions by writing to the publisher, the original author, or any other current copyright owner. Please cite as: PAIN EDUCATION Teaching Slides, chapter: Treatment of chronic back pain, Available from No responsibility is assumed for any injury and/or damage to persons or property as a matter of products liability, through negligence or otherwise, or from any use or operation of any methods, products, instructions, or ideas contained in the material herein. Because of rapid advances in the medical sciences, it is recommended that independent verification of diagnoses and drug dosages should be made. Produced by Excerpta Medica Radarweg NX Amsterdam Netherlands Supported by an unrestricted educational grant from Grünenthal. Produced in the Netherlands
3 Learning objectives Upon completion of this training module you should have gained an increased understanding of: The high burden of chronic back pain Back pain as a frequently under-treated condition Different chronic back pain conditions seen in practice The underlying mechanisms of back pain conditions Neuropathic pain components in chronic back pain Pharmacological and non-pharmacological treatment options for management of chronic back pain The classes of drugs used in managing back pain and the working mechanisms of various analgesic medications The rationale for combining analgesic medications in chronic pain management For additional information and further educational content related to the treatment of chronic back pain, please see Module 4 of the CME-accredited e-learning PAIN EDUCATION modules, available at
4 Chronic pain: a disease in its own right WHO recognizes pain as an important, global, public health concern Acute pain Need for improved, standardized management Chronic pain About 25% of Europeans are thought to have chronic pain conditions Chronic pain is multifaceted and involves the interaction of Physical factors Psychological factors Social factors Pain management plan development based on Good physician-patient communication Jointly agreed goals WHO = World Health Organisation. WHI European Commission
5 Inadequacy in current chronic pain management Chronic pain conditions are often poorly managed Of > 45,000 European telephone survey respondents with chronic pain > 30% experiences intolerable pain > 60% finds prescription medications inadequate 40% feels that pain is not well managed Improving these outcomes needs Understanding the effect of chronic pain on patients Appreciation of pain mechanisms The management plan must address the patient needs and the many facets of pain > 30% Intolerable pain > 60% Medications inadequate 40% Pain not well managed Breivik H, et al. Eur J Pain. 2006;10: Varrassi G, et al. Curr Med Res Opin. 2010;26:
6 Physical and psychological burden of severe pain The burden posed by severe and chronic pain is far-reaching Anxiety Reduced mobility Appetite disturbance Limited social functioning Depression Disturbed sleep Limited workplace functioning Reduced quality of life Becker N, et al. Pain. 1997;73: Breivik H, et al. Eur J Pain. 2006;10: Gore M, et al. J Pain. 2006;7: McDermott AM, et al. Eur J Pain. 2006;10:127-35, 3
7 Back problem Joint pain Neck Arthritis Surgery/medical procedure Fibromyalgia Preview for Incidence and costs of back pain Chronic back pain is the most frequently reported severe pain Incidence of back pain > 50,000 participants France, Germany, Italy, Spain, UK Severe pain: 3.5% Back pain: 66% Costs of back pain 49 billion Euros per year (Germany) > 1300 Euros per patient More than 50% attributable to indirect costs of back pain Highest indirect cost burdens of common medical illnesses ,3 Langley PC. Curr Med Res Opin. 2011;24: Kantar Health, Inc Princeton, NJ. Wenig CM, et al. Eur J Pain. 2009;13: Maniadakis N, et al. Pain. 2000;84:
8 Risk factors of back pain Physical behaviour Lack of healthy exercise Sedentary lifestyle Environmental factors Vibrations Poorly designed furniture Patient factors Age Height Physical conditions Weak trunk muscle Bad posture Psychological conditions Stress Depression Fear of movement The risk of back pain is highest during the working years, with a peak between 30 and 39 years Heliovaara M. Ann Med. 1989;21: Chou R, et al. Ann Intern Med. 2007; 147: Vlaeyen JWS, Linton SJ. Pain. 2000;85:317-32, 5
9 Localization and division of back pain Non-specific (90% of cases are non-radicular and pseudoradicular) Functional disorder through incorrect weight-bearing and wear (mechanical) Specific (10% of cases are radicular) Nerve root irritation and compression syndrome Prolonged pain (extravertebral or visceral) Intervertebral disc prolapse Metabolic (osteoporosis, fracture) Somatoform pain disorders/fibromyalgia Malignant (primary tumours/metastasis Inflammatory (rheumatic, infections) 6 Chou R, et al. Ann Intern Med. 2007; 147:
10 Natural course of back pain Back pain often starts with acute pain Acute pain is defined as pain lasting less than 4 weeks This episode may be followed by a period of subacute pain persisting for weeks to months Back pain that continues for more than 3 months is termed chronic back pain 5 10% of acute back pain cases become chronic Back pain in women tends to last longer than in men Most people experience acute back pain at least once in their lifetime Intensity and frequency can be influenced by psychological components Frank JW, et al. Spine (Phila Pa 1976). 1996;21: National Institute for Health and Clinical Excellence
11 Classification of back pain according to pain mechanisms Type of Pain Example Characteristic Nociceptive back pain Nociceptiveinflammatory pain Neuropathic back pain Dysfunctional back pain Mixed pain Osteoporosis Facet syndrome Nerve-root irritation syndrome No nervous system lesion or inflammation Pricking/burning pain sensation in response to nociceptive pain stimulus Actual or threatened damage to non-neural tissue due to inflammation Nerve damage involved Expression of maladaptive plasticity Fibromyalgia No obvious nerve damage Non-specific back pain, spinal canal stenosis No obvious nerve damage Overlapping components of nociceptive and neuropathic pain All types of pain are processed by the nervous system Deyo RA, Weinstein JN. N Engl J Med. 2001;344: Cohen SP, et al. BMJ. 2008;337:a2718. Woolf CJ, et al. Science. 2000;288: Marchand S. Rheum Dis Clin North Am. 2008;34: , 8
12 Patients (%) Preview for Neuropathic component in back pain 7,772 back pain patients: Neuropathic component likely Neuropathic component uncertain Neuropathic component unlikely 37.0% 27.7% 35.3% Neuropathic pain correlates with More intense pain More severe comorbidity Poorer quality of life n = 1,131 n = 4,254 n = 2, Freynhagen R et al. Curr Med Res Opin. 2006;22: Freynhagen R, et al. Curr Pain Headache Rep. 2009;13: Freynhagen R, et al. Curr Med Res Opin. 2006;22: Mild Moderate Severe Mainly neuropathic Unknown Mainly nociceptive
13 Central sensitization Chronification of pain May result from local tissue damage and inflammation Alteration of nociceptors by inflammatory mediators producing pain sensitization Lasting activity of damaged nerve fibres leads to neuroplastic changes in the CNS Central sensitization Reactivity nociceptive posterior horn neurons (wind up) Mechanoreceptors (Aβ-fibres) obtain contact to the nociceptive system Non-painful stimuli are recognized as painful (allodynia) CNS = central nervous system. Woolf CJ. Ann Intern Med. 2004;140: Woolf CJ, et al. Science. 2000;288: Latremoliere A, et al. J Pain. 2009;10:
14 Diagnosing back pain Red flags: Discovery of physical causes, in particular if specific or urgent treatment is required Yellow flags: Identification of risk factors for chronification of pain: assessment of psychosocial factors is a key component. Diagnostics Obtain objective evidence for physical symptoms and functional impairments to identify Non-specific back pain Back pain with radiculopathy or spinal stenosis Back pain with another potential cause Chou R, et al. Ann Intern Med. 2007;147: Savigny P, et al. BMJ. 2009;338:b1805. Rives PA, et al. J Am Board Fam Pract. 2004;17:S Cohen SP, et al. BMJ. 2008;337:a2718. Bratton RL. Am Fam Physician. 1999;60: , 11
15 Red flags and chronic pain Red flags to low back pain identified by the American college of radiology: Trauma, cumulative trauma Unexplained weight loss, insidious onset Age > 50 years, especially women, and males with osteoporosis or compression fracture Unexplained fever, history of urinary or other infection Immunosuppression, diabetes mellitus History of cancer Intravenous (IV) drug use Prolonged use of corticosteroids, osteoporosis Age > 70 Focal neurologic deficit(s) with progressive or disabling symptoms, cauda equina syndrome Duration longer than 6 weeks Prior surgery 12 Davis PC, et al. Reston (VA): American College of Radiology (ACR), 2011.
16 Yellow flags and chronic pain Yellow flags to low back pain identify psychosocial factors that increase the risk for developing or perpetuating chronic pain and long-term disability Psychosocial risk factors Inappropriate attitudes and beliefs about back pain Lifestyle habits Smoking, medicines (AT1 blockers) Poor working conditions Social class Educations Income Coexisting disease Cardio-respiratory diseases Psychiatric diseases Inappropriate pain behaviour Work-related problems or compensations issues Emotional problems 13 van Tulder M, et al. Eur Spine J. 2006;15:S
17 Back pain diagnosis The Lasegue test (straight leg raise test) The Schober test The Faber test Other simple tests Imaging The test is positive if the pain in the sciatic distribution is produced at degrees of passive inflexion of the straight leg. Lasegue s sign can be used to diagnose nerve-root irritation. This test measures the flexibility of the spine This test is frequently used to differentiate lumbar spinal problems from primary hip pathology Ask patients to walk on heels or toes Try pelvic tilts and range of motion of trunk movements Attempt finger-tofoot distance tests and chin-to-chest tests Ask patients to demonstrate chest expansion and their range of motion of the cervical spine Imaging is indicated in patients with low back pain only if they have severe progressive neurologic deficits or signs or symptoms that suggest a serious or specific underlying condition Ask patients to sit on the floor with legs stretched out Chou R, et al. Ann Intern Med. 2011;154:81. Van Tulder M, et al. Eur Spine J. 2006;15S
18 Radicular and non-radicular back pain Diagnostic indicators Radicular back pain (10% of all chronic back pain Weakened muscles Pain the the legs/buttocks Sensitivity disorders Lasegue signs Non-radicular pain (90% of all chronic back pain) Aetiology Pressure on spinal nerve roots Changes in joints (intervertebral joints, iliosacral joint) Changes of ligaments muscles Intervertrebal changes (without prolapse) Causes Slipped disc Osseous stenosis Symptoms Stabbing or shooting pain Dull, aching, difficult to locate Pain location Legs/buttocks, rather than back Unilateral or bilateral in the region of the back or buttocks Pain often intensifies when position is changed or maintained for long periods and eases on movement Chou R, et al. Ann Intern Med. 2011;154:81. Van Tulder M, et al. Eur Spine J. 2006;15S
19 Managing acute back pain Physical Stimulation to movement as soon as possible Brief bed-rest/sick leave Heat/cold application Physical therapy Pharmacological Analgesics Co-analgesics Stimulation Acupuncture Interventional/surgical treatment if other methods unsuccessful Physicians should always consider the risks for acute pain becoming chronic and persistent If there is no improvement in 2 4 weeks, the physician must order futher tests Chou R, et al. Ann Intern Med. 2007;147: Savigny P, et al. BMJ. 2009;338:b
20 Managing chronic back pain Pharmacological e.g. paracetamol, NSAIDs, weak opioids, strong opioids, muscle relaxants, TCAs, SNRIs and MOR-NRI Non-pharmacological e.g. controlled exercise therapy, relaxation measures, ergotherapy, patient education, behavioural therapy Interventional e.g. surgical Multi-modal, long term Individually oriented to the current symptoms and to the pathophysiological causes Multimodal management to Help patients to self-manage their condition Reduce pain and its impact Physical and sport therapy Active Medical training therapy Psychological pain treatment Relaxation techniques Pain coping strategies Stimulation therapy Spinal cord stimulation Pharmacotherapy Analgesics Co-analgesics Chou R, et al. Ann Intern Med. 2007;147: Grabois M. Am J Phys Med Rehabil. 2005;84:S Savigny P, et al. BMJ. 2009;338:b1805. National Institute for Health and Clinical Excellence NSAIDs = non-steroidal anti-inflammatory drugs; MOR-NRIs = µ-opioid receptornorepinephrine reuptake inhibitors; SNRIs = selective noradrenaline reuptake inhibitors; TCAs = tricyclic antidepressants; TENS = transcutaneous electrical nerve stimulation. 17
21 Non-medical, non-surgical therapy Core stability exercises Massages Chiropractic Physiotherapy Acupuncture Behavioural therapy Psychological pain coping Strength training and fitness Non-medical, Non-surgical therapy Orthotic devices Relaxation techniques Yoga The National Institute for Health and Clinical Excellence (NICE) recommends 8 supervised, physical and exercise sessions over 12 weeks that can be combined with a psychological treatment programme of management. Hayden JA, et al. Cochrane Database Syst Rev. 2005;3:CD000335, Chou R, et al. Ann Intern Med. 2007;147: Savigny P, et al. BMJ. 2009;338:b1805. National Institute for Health and Clinical Excellence
22 Exercises and chronic pain GET and pacing strategies are employed as part of a multimodel, intensive management programme GET ensures that patients take exercise that builds to allow improved flexibility and endurance, helping relieve pain and contributing to better function Pacing strategies ensure that patients with back pain learn to pace their lives, taking account of their back problems and pain GET = graded exercise therapy. 19 Hayden JA, et al. Cochrane Database Syst. Rev. 2005;3:CD
23 Pharmacological treatment of pain: a mechanism-oriented approach Pain character/symptoms Affecting the muscular and skeletal system/exertiondependent/local/tender/no signs of inflammation Affecting the muscular and skeletal system/exertiondependent/signs of inflammation/local/pressingstabbing-probing Affecting the nervous system/burning/shooting/ concomitant neurological symptoms Multi-locular/no pathological findings/hypersensitive to pain/vegetative and/or mental symptoms Morlion B. Curr Med Res Opin. 2011;27: Diagnosis examples Arthrosis/myofascial pain syndrome Activated arthrosis/arthritis Diabetic polyneuropathy/ post-zoster neuralgia Fibromyalgia syndrome Nociceptive Nociceptive/ inflammatory Neuropathic Dysfunctional Mechanisms Nociceptor activation/reduced endogenous pain inhibition Nociceptor activation and sensitization/central sensitization Forming of new channels and receptors/ectopic impulse generation (spontaneous activity) Central sensitization Forming of new channels and receptors/ectopic impulse generation (spontaneous activity) Reduced endogenous pain inhibition and changed pain processing Pain therapy with medication Nonopioids/muslce relaxants/mor- NRI Opioids NSAIDs/(glucocorticoids)/ opioids/mor-nri Anticonvulsants (Na and Ca channel blockers)/antidepressants (here above all TCA)/MOR-NRI Anti-depressants (NSRIs)/opioids/topical agents (lidocaine plaster, topical capsaicin) Anti-depressants (NSRIs) MOR-NRI = µ-opioid receptor-norepinephrine reuptake inhibitor; NSAIDs = non-steroidal anti-inflammatory drugs; SNRIs = selective noradrenaline reuptake inhibitors; TCAs = tricyclic antidepressants. 20
24 Pharmacotherapy, including combinations, for chronic back pain Pharmacological management of back pain should treat both nociceptive and neuropathic components Nociceptive pain Paracetamol, NSAIDs and COX-2 inhibitors Largely ineffective on specific neuropathic pain mechanisms E.g. ibuprofen, diclofenac, acetylsalicylic acid Topical agents E.g. ibuprofen, diclofenac ointments Opioid therapies Target nociceptive and, to a lesser extent, neuropathic pain E.g. strong opioids (morphine, oxycodone, fentanyl, buprenorphine) and weak opioids (tramadol, codeine) Neuropathic pain Anti-depressants Agents that inhibit neurotransmitter uptake E.g. TCAs, SNRIs Anticonvulsant drugs E.g. pregabalin, gabapentin Topical agents Useful in managing localized neuropathic pain E.g. lidocaine plaster, capsaicin MOR-NRI (simultaneously targeting Nociceptive and Neuropathic pain) Two mechanisms of action opioidergic activity plus noradrenaline reuptake inhibitory activity E.g. tapentadol NSAIDs = non-steroidal anti-inflammatory drugs; SNRIs = selective noradrenaline reuptake inhibitors; TCAs = tricyclic antidepressants. Morlion B. Curr Med Res Opin. 2011;27: Roelofs PD, et al. Cochrane Database Syst Rev. 2008:CD
25 Rationale for mechanism-oriented pharmacotherapy Chronic pain Often involves more than one mechanism Seldom controlled by a single pharmacological principle Combining agents with different mechanisms of action increases the probability of interrupting the pain signal (additive/synergistic effect) Use drugs with complementary pharmacokinetic profiles instead of a higher-dose single agent treatment Methods of combining drugs include use of Single, loose-drug combinations (e.g. oxycodone and pregabalin) Fixed combination preparations (formulated to contain 2 agents, e.g. paracetamol/tramadol) Use of agents with more than one mechanism of action in a single molecule (e.g. tapentadol) Warning: Certain agents are associated with risk of severe side effects Some patients have treatment-related Morlion B. Curr Med Res Opin. 2011;27: National Institute for Health and Clinical Excellence adverse side-effects Roelofs PD, et al. Cochrane Database Syst Rev. 2008;1:CD Varrassi G, et al. Curr Med Res Opin. 2010;26:
26 Summary Back pain is highly prevalent with a high socio-economic and clinical burden Chronic back pain is often non-specific in nature History and physical examination are important in distinguishing potential causes of back pain Management of back pain should be multi-modal involving programmes of exercise, relaxation, psychosocial support and pharmacological intervention tailored to patient needs and relevant to the mechanisms underlying pain 23
PAIN EDUCATION Module 1: Assessing pain & physician patient communication
 The full version of this slide deck in MS PowerPoint format (containing presentation view and expanded notes) can be downloaded on www.pain-cme.net please register! PAIN EDUCATION Module 1: Assessing pain
The full version of this slide deck in MS PowerPoint format (containing presentation view and expanded notes) can be downloaded on www.pain-cme.net please register! PAIN EDUCATION Module 1: Assessing pain
Managing Pain in the Elderly
 Managing Pain in the Elderly MILES BELGRADE, MD COMPREHENSIVE PAIN CENTER MINNEAPOLIS VA The Pain Deck is Stacked Against the Elderly Osteoporosis Fractures 1 Zoster & PHN Trigeminal Neuralgia Verne 81-year-old
Managing Pain in the Elderly MILES BELGRADE, MD COMPREHENSIVE PAIN CENTER MINNEAPOLIS VA The Pain Deck is Stacked Against the Elderly Osteoporosis Fractures 1 Zoster & PHN Trigeminal Neuralgia Verne 81-year-old
Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia
 Disclosure & Acknowledgment Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia Disclosures - None Acknowledgements Dr. Andrea Furlan Dr. Julia Alleyne Dr. Hamilton Hall
Disclosure & Acknowledgment Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia Disclosures - None Acknowledgements Dr. Andrea Furlan Dr. Julia Alleyne Dr. Hamilton Hall
CHAPTER 4 PAIN AND ITS MANAGEMENT
 CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice
 The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice David Walsh David.walsh@nottingham.ac.uk National Clinical Guideline Centre Commissioned by NICE
The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice David Walsh David.walsh@nottingham.ac.uk National Clinical Guideline Centre Commissioned by NICE
Neck Pain. Frank Thomas BSc(Hons) MBChB FANZCA FFPMANZCA
 Neck Pain Frank Thomas BSc(Hons) MBChB FANZCA FFPMANZCA Assessing Neck Pain Obtained detailed pain history Assess for red flags Assess range of neck movements Perform a neurological exam Identify psychosocial
Neck Pain Frank Thomas BSc(Hons) MBChB FANZCA FFPMANZCA Assessing Neck Pain Obtained detailed pain history Assess for red flags Assess range of neck movements Perform a neurological exam Identify psychosocial
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽
 외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
Evidence-based Clinical Practice Guidelines on Management of Pain in Older People Aza Abdulla, Margaret Bone, Nicola Adams, Alison M.
 Evidence-based Clinical Practice Guidelines on Management of Pain in Older People Aza Abdulla, Margaret Bone, Nicola Adams, Alison M. Elliott, Derek Jones, Roger Knaggs, Denis Martin, Elizabeth L. Sampson,
Evidence-based Clinical Practice Guidelines on Management of Pain in Older People Aza Abdulla, Margaret Bone, Nicola Adams, Alison M. Elliott, Derek Jones, Roger Knaggs, Denis Martin, Elizabeth L. Sampson,
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society
 Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
Are you getting the best treatment for your low back pain?
 Are you getting the best treatment for your low back pain? Dr.Rahimian Orthopedic surgon Spine fellowship resident Why are we here? To update you on the best evidence for the treatments available To give
Are you getting the best treatment for your low back pain? Dr.Rahimian Orthopedic surgon Spine fellowship resident Why are we here? To update you on the best evidence for the treatments available To give
Treatments for Common Pain Disorders. Matthew R. Kohler, MD Hudson Spine and Pain Medicine 03/01/2017
 Treatments for Common Pain Disorders Matthew R. Kohler, MD Hudson Spine and Pain Medicine 03/01/2017 Acute Disc Herniation Conservative Approach (Four to Six Weeks) Physical Therapy, exercise and gentle
Treatments for Common Pain Disorders Matthew R. Kohler, MD Hudson Spine and Pain Medicine 03/01/2017 Acute Disc Herniation Conservative Approach (Four to Six Weeks) Physical Therapy, exercise and gentle
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Neuropathic pain pharmacological management: the pharmacological management of neuropathic pain in adults in non-specialist
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Neuropathic pain pharmacological management: the pharmacological management of neuropathic pain in adults in non-specialist
3/7/2018. IASP updated definition of pain. Nociceptive Pain. Transduction. (Nociceptors) Transmission. (Peripheral nerve) Modulation
 IASP updated definition of pain The Pain of Trauma and The Trauma of Pain: The Opioid Crisis is Not What You Think. Bennet Davis, M.D. Many people report pain in the absence of tissue damage or any likely
IASP updated definition of pain The Pain of Trauma and The Trauma of Pain: The Opioid Crisis is Not What You Think. Bennet Davis, M.D. Many people report pain in the absence of tissue damage or any likely
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Spinal Cord Injury Pain. Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018
 Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
Mr. LBP: Case Presentation
 CLINICAL CASES Case: Mr. LBP Mr. LBP: Case Presentation Mr. LBP is a 35-year-old male He fell down while participating in a recreational sports activity He subsequently developed low back pain Upon arrival
CLINICAL CASES Case: Mr. LBP Mr. LBP: Case Presentation Mr. LBP is a 35-year-old male He fell down while participating in a recreational sports activity He subsequently developed low back pain Upon arrival
GUIDELINES AND AUDIT IMPLEMENTATION NETWORK
 GUIDELINES AND AUDIT IMPLEMENTATION NETWORK General Palliative Care Guidelines The Management of Pain at the End Of Life November 2010 Aim To provide a user friendly, evidence based guide for the management
GUIDELINES AND AUDIT IMPLEMENTATION NETWORK General Palliative Care Guidelines The Management of Pain at the End Of Life November 2010 Aim To provide a user friendly, evidence based guide for the management
Wendy Field Advanced Physiotherapy Practitioner June 2018
 Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
PAIN EDUCATION Module 2: Multimodal management of chronic pain
 The full version of this slide deck in MS PowerPoint format (containing presentation view and expanded notes) can be downloaded on www.pain-cme.net please register! PAIN EDUCATION Module 2: Multimodal
The full version of this slide deck in MS PowerPoint format (containing presentation view and expanded notes) can be downloaded on www.pain-cme.net please register! PAIN EDUCATION Module 2: Multimodal
CHAPTER 4 PAIN AND ITS MANAGEMENT
 CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
Management of Neuropathic pain
 Management of Neuropathic pain Ravi Parekodi Consultant in Anaesthetics and Pain Management 08/04/2014 Ref: BJA July2013, Map of Medicine2013, Pain Physician 2007, IASP 2012, Nice guideline 2013 Aims Highlight
Management of Neuropathic pain Ravi Parekodi Consultant in Anaesthetics and Pain Management 08/04/2014 Ref: BJA July2013, Map of Medicine2013, Pain Physician 2007, IASP 2012, Nice guideline 2013 Aims Highlight
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Understanding pain and mental illness Impact on management principles
 Understanding pain and mental illness Impact on management principles Chris Alderman Consultant Psychopharmacologist Pain and mental illness - context PAIN MENTAL ILLNESS OTHER FACTORS (personality, history.
Understanding pain and mental illness Impact on management principles Chris Alderman Consultant Psychopharmacologist Pain and mental illness - context PAIN MENTAL ILLNESS OTHER FACTORS (personality, history.
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acetaminophen in chronic pain management, 225 Acupuncture in chronic pain management, 251, 338 339 Ajurvedic medicine in chronic pain management,
Note: Page numbers of article titles are in boldface type. A Acetaminophen in chronic pain management, 225 Acupuncture in chronic pain management, 251, 338 339 Ajurvedic medicine in chronic pain management,
Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology
 Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
PAIN EDUCATION Module 6: The chronification of pain
 The full version of this slide deck in MS PowerPoint format (containing presentation view and expanded notes) can be downloaded on www.pain-cme.net please register! PAIN EDUCATION Module 6: The chronification
The full version of this slide deck in MS PowerPoint format (containing presentation view and expanded notes) can be downloaded on www.pain-cme.net please register! PAIN EDUCATION Module 6: The chronification
Regional Pain Syndromes: Neck and Low Back
 Regional Pain Syndromes: Neck and Low Back Srinivas Nalamachu, MD Disclosures Consultant/Independent Contractor/Honoraria: Ferring 1 Learning Objectives Identify the most common painful conditions in the
Regional Pain Syndromes: Neck and Low Back Srinivas Nalamachu, MD Disclosures Consultant/Independent Contractor/Honoraria: Ferring 1 Learning Objectives Identify the most common painful conditions in the
A Patient s Guide to Treatment Guidelines for Low Back Pain
 A Patient s Guide to Treatment Guidelines for Low Back Pain 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Treatment Guidelines for Low Back Pain 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled
Neuropathic Pain in Palliative Care
 Neuropathic Pain in Palliative Care Neuropathic Pain in Advanced Cancer Affects 40% of patients Multiple concurrent pains are common Often complex pathophysiology with mixed components Nocioceptive Neuropathic
Neuropathic Pain in Palliative Care Neuropathic Pain in Advanced Cancer Affects 40% of patients Multiple concurrent pains are common Often complex pathophysiology with mixed components Nocioceptive Neuropathic
Syllabus. Questions may appear on any of the topics below: I. Multidimensional Nature of Pain
 Questions may appear on any of the topics below: I. Multidimensional Nature of Pain Syllabus A. Epidemiology 1. Pain as a public health problem with social, ethical, legal and economic consequences 2.
Questions may appear on any of the topics below: I. Multidimensional Nature of Pain Syllabus A. Epidemiology 1. Pain as a public health problem with social, ethical, legal and economic consequences 2.
Acute Pain NETP: SEPTEMBER 2013 COHORT
 Acute Pain NETP: SEPTEMBER 2013 COHORT Pain & Suffering an unpleasant sensory & emotional experience associated with actual or potential tissue damage, or described in terms of such damage International
Acute Pain NETP: SEPTEMBER 2013 COHORT Pain & Suffering an unpleasant sensory & emotional experience associated with actual or potential tissue damage, or described in terms of such damage International
Cervical Plating BACK PAIN
 BACK PAIN Back Pain Back pain is frequent complaint. It is the commonest cause of work-related absence in the world. Although back pain may be painful and uncomfortable, it is not usually serious. Even
BACK PAIN Back Pain Back pain is frequent complaint. It is the commonest cause of work-related absence in the world. Although back pain may be painful and uncomfortable, it is not usually serious. Even
Neuropathic Pain and Pain Management Options. Mihnea Dumitrescu, MD
 Neuropathic Pain and Pain Management Options Mihnea Dumitrescu, MD www.austinppc.com International Association for the Study of Pain (IASP): Definition of Pain Pain is an unpleasant sensory and emotional
Neuropathic Pain and Pain Management Options Mihnea Dumitrescu, MD www.austinppc.com International Association for the Study of Pain (IASP): Definition of Pain Pain is an unpleasant sensory and emotional
IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY. Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group
 IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group Who Am I? Avid equestrian Trained in Physical Medicine & Rehabilitation
IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group Who Am I? Avid equestrian Trained in Physical Medicine & Rehabilitation
Hailee Gibson, CCPA Neurosurgery Physician Assistant. Windsor Neurosurgery & Spine Associates. Windsor Regional Hospital Ouellette Campus
 Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
Pain Pathways. Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH
 Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
NICE guideline Published: 30 November 2016 nice.org.uk/guidance/ng59
 Low back pain and sciatica in over 16s: assessment and management NICE guideline Published: 30 November 2016 nice.org.uk/guidance/ng59 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Low back pain and sciatica in over 16s: assessment and management NICE guideline Published: 30 November 2016 nice.org.uk/guidance/ng59 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS. Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement
 Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement 2 as 20 Experts published and leaders in their respective field 12 month lead in
Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement 2 as 20 Experts published and leaders in their respective field 12 month lead in
Pain and its Treatments. Our Goals: Understand: What is pain and what causes it? 2. What are different types of pain? 3. How do opioid drugs work?
 Pain and its Treatments Cheryl Stucky, Ph.D. Medical College of Wisconsin Our Goals: Understand: 1. What is pain and what causes it? 2. What are different types of pain? 3. How do opioid drugs work? What
Pain and its Treatments Cheryl Stucky, Ph.D. Medical College of Wisconsin Our Goals: Understand: 1. What is pain and what causes it? 2. What are different types of pain? 3. How do opioid drugs work? What
NEIGHBORHOOD HEALTH PLAN OF RHODE ISLAND
 Clinical Practice Guidelines Complementary Alternative Medicine (CAM) Ease the Pain program Section: Clinical Practice Guideline Effective: December 18, 2014 NEIGHBORHOOD HEALTH PLAN OF RHODE ISLAND Subject:
Clinical Practice Guidelines Complementary Alternative Medicine (CAM) Ease the Pain program Section: Clinical Practice Guideline Effective: December 18, 2014 NEIGHBORHOOD HEALTH PLAN OF RHODE ISLAND Subject:
Fibromyalgia: Current Trends and Concepts
 Fibromyalgia: Current Trends and Concepts Dr. Brian Kahan Fellow American Academy of Physical Medicine and Rehabilitation Diplomat American Academy of Pain Medicine American College of Rheumatology (ACR)
Fibromyalgia: Current Trends and Concepts Dr. Brian Kahan Fellow American Academy of Physical Medicine and Rehabilitation Diplomat American Academy of Pain Medicine American College of Rheumatology (ACR)
EFFECIVENESS OF THE WILLIAMS EXCERCISE IN MECHANICAL LOW BACK PAIN
 EFFECIVENESS OF THE WILLIAMS EXCERCISE IN MECHANICAL LOW BACK PAIN Dr.U.Ganapathy Sankar, Ph.D Dean I/C, SRM College of Occupational Therapy, SRMUniversity, Kattankulathur, KancheepuramDistrict, Tamil
EFFECIVENESS OF THE WILLIAMS EXCERCISE IN MECHANICAL LOW BACK PAIN Dr.U.Ganapathy Sankar, Ph.D Dean I/C, SRM College of Occupational Therapy, SRMUniversity, Kattankulathur, KancheepuramDistrict, Tamil
Back Pain Update. Steven Andersen, MD Providence Physiatry Clinic 2016
 Back Pain Update Steven Andersen, MD Providence Physiatry Clinic 2016 Back Pain is Very Common Lifetime prevalence 80% 12 month prevalence 40% Point prevalence 20% Centers for Disease Control and Prevention.
Back Pain Update Steven Andersen, MD Providence Physiatry Clinic 2016 Back Pain is Very Common Lifetime prevalence 80% 12 month prevalence 40% Point prevalence 20% Centers for Disease Control and Prevention.
UCSD DEPARTMENT OF ANESTHESIOLOGY
 UCSD DEPARTMENT OF ANESTHESIOLOGY LEARNING OBJECTIVES FOR ADVANCED PAIN MEDICINE ROTATION, UCSD MEDICAL CENTER Competencies Objective Learning Environment Instructional Method Assessment Tool Patient Care:
UCSD DEPARTMENT OF ANESTHESIOLOGY LEARNING OBJECTIVES FOR ADVANCED PAIN MEDICINE ROTATION, UCSD MEDICAL CENTER Competencies Objective Learning Environment Instructional Method Assessment Tool Patient Care:
Chiropractic Health Plan - Diagnosis of Low Back Pain
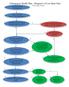 Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
Mr Chris Gregg. Dr Chris Hoffman. Dr Julie Zarifeh. 14:00-16:00 WS #12: Pain Symposium 16:30-18:30 WS #17: Pain Symposium (Repeated)
 Dr Chris Hoffman Orthopaedic Surgeon Auckland Mr Chris Gregg Physiotherapist TBI Health Wellington Dr Julie Zarifeh Senior Clinical Psychologist Professional Practise Fellow CDHB University of Otago 14:00-16:00
Dr Chris Hoffman Orthopaedic Surgeon Auckland Mr Chris Gregg Physiotherapist TBI Health Wellington Dr Julie Zarifeh Senior Clinical Psychologist Professional Practise Fellow CDHB University of Otago 14:00-16:00
HealthPartners Inspire Special Needs Basic Care Clinical Care Planning and Resource Guide CHRONIC PAIN
 The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Institute of Neurological Disorders and Stroke), Mount Sinai Beth Israel
The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Institute of Neurological Disorders and Stroke), Mount Sinai Beth Israel
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice Review consultation document Review of Clinical Guideline (CG88) Low back pain: early management of persistent non-specific
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice Review consultation document Review of Clinical Guideline (CG88) Low back pain: early management of persistent non-specific
SPINAL PAIN. Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon
 SPINAL PAIN Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon PAIN GENERATORS IN THE SPINE Ligaments: ALL,PLL Muscle Periosteum bone Outer 1/3 annulus disc Facet joints Sacro-iliac joint sinuvertebral
SPINAL PAIN Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon PAIN GENERATORS IN THE SPINE Ligaments: ALL,PLL Muscle Periosteum bone Outer 1/3 annulus disc Facet joints Sacro-iliac joint sinuvertebral
GUIDELINES ON PAIN MANAGEMENT IN UROLOGY
 GUIDELINES ON PAIN MANAGEMENT IN UROLOGY F. Francesca (chairman), P. Bader, D. Echtle, F. Giunta, J. Williams Eur Urol 2003; 44(4):383-389 Introduction Pain is defined as an unpleasant sensory and emotional
GUIDELINES ON PAIN MANAGEMENT IN UROLOGY F. Francesca (chairman), P. Bader, D. Echtle, F. Giunta, J. Williams Eur Urol 2003; 44(4):383-389 Introduction Pain is defined as an unpleasant sensory and emotional
LOTHIAN LUMBAR SPINE PATHWAYS
 LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
Gateshead Pain Guidelines for Chronic Conditions
 Gateshead Pain Guidelines for Chronic Conditions Effective Date: 13.2.2013 Review Date: 13.2.2015 Gateshead Pain Guidelines: Contents PAIN GUIDELINES Chronic Non-Malignant Pain 5 Musculoskeletal Pain 6
Gateshead Pain Guidelines for Chronic Conditions Effective Date: 13.2.2013 Review Date: 13.2.2015 Gateshead Pain Guidelines: Contents PAIN GUIDELINES Chronic Non-Malignant Pain 5 Musculoskeletal Pain 6
Malaysian Healthy Ageing Society
 Organised by: Co-Sponsored: Malaysian Healthy Ageing Society Key to back pain is alignment Michael Haneline, DC, MPH Professor, Head of Chiropractic International Medical University michael_haneline@imu.edu.my
Organised by: Co-Sponsored: Malaysian Healthy Ageing Society Key to back pain is alignment Michael Haneline, DC, MPH Professor, Head of Chiropractic International Medical University michael_haneline@imu.edu.my
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis
 Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
CLINICAL GUIDELINES. Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision
 CLINICAL GUIDELINES Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision TRIAGE At the initial visit, a focused history and physical examination is performed to assign
CLINICAL GUIDELINES Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision TRIAGE At the initial visit, a focused history and physical examination is performed to assign
Understanding your spine and how it works can help you better understand low back pain.
 Low Back Pain Almost everyone will experience low back pain at some point in their lives. This pain can vary from mild to severe. It can be short-lived or long-lasting. However it happens, low back pain
Low Back Pain Almost everyone will experience low back pain at some point in their lives. This pain can vary from mild to severe. It can be short-lived or long-lasting. However it happens, low back pain
Understanding low back pain
 Understanding low back pain UV41575 L/505/2539 Learner name: VRQ Learner number: VTCT is the specialist awarding organisation for the Hairdressing, Beauty Therapy, Complementary Therapy, Hospitality and
Understanding low back pain UV41575 L/505/2539 Learner name: VRQ Learner number: VTCT is the specialist awarding organisation for the Hairdressing, Beauty Therapy, Complementary Therapy, Hospitality and
PAIN TERMINOLOGY TABLE
 PAIN TERMINOLOGY TABLE TERM DEFINITION HOW TO USE CLINICALLY Acute Pain Pain that is usually temporary and results from something specific, such as a surgery, an injury, or an infection Addiction A chronic
PAIN TERMINOLOGY TABLE TERM DEFINITION HOW TO USE CLINICALLY Acute Pain Pain that is usually temporary and results from something specific, such as a surgery, an injury, or an infection Addiction A chronic
Spinal Trauma. General Rehabilitation of Patient with Spinal Trauma. Common Spinal Injuries. Important Anatomical Structures at each Vertebral Level
 Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain
 Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain Course: Designing Exercise Prescriptions for Normal/Special Populations Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI
Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain Course: Designing Exercise Prescriptions for Normal/Special Populations Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI
Outline. Introduction / Epidemiology. Anatomy / Pain generators. Diagnosis. Treatment. Most Important lecture!!
 Acute Low Back Pain Outline Introduction / Epidemiology. Most Important lecture!! Anatomy / Pain generators Diagnosis Treatment Course Objectives Know the RED FLAGS in history taking. Know the Pain Generators
Acute Low Back Pain Outline Introduction / Epidemiology. Most Important lecture!! Anatomy / Pain generators Diagnosis Treatment Course Objectives Know the RED FLAGS in history taking. Know the Pain Generators
What Is Back Pain? Fast Facts: An Easy-to-Read Series of Publications for the Public. Who Gets Back Pain? What Are the Causes of Back Pain?
 Back pain can range from a dull, constant ache to a sudden, sharp pain that makes it hard to move. It can start quickly if you fall or lift something too heavy, or it can get worse slowly. Who Gets Back
Back pain can range from a dull, constant ache to a sudden, sharp pain that makes it hard to move. It can start quickly if you fall or lift something too heavy, or it can get worse slowly. Who Gets Back
Refractory Central Neurogenic Pain in Spinal Cord Injury. Case Presentation
 Refractory Central Neurogenic Pain in Spinal Cord Injury Case Presentation Edwin B. George, MD, PhD Wayne State University John D. Dingell VAMC 2012 Disclosures This continuing education activity is managed
Refractory Central Neurogenic Pain in Spinal Cord Injury Case Presentation Edwin B. George, MD, PhD Wayne State University John D. Dingell VAMC 2012 Disclosures This continuing education activity is managed
Neuropathic Pain. Scott Magnuson, MD Pain Management of North Idaho, PLLC
 Neuropathic Pain Scott Magnuson, MD Pain Management of North Idaho, PLLC Pain is our friend "An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described
Neuropathic Pain Scott Magnuson, MD Pain Management of North Idaho, PLLC Pain is our friend "An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described
Pain Management. University of Illinois at Chicago College of Nursing
 Pain Management University of Illinois at Chicago College of Nursing 1 Learning Objectives Upon completion of this module, participants will be better able to: 1. Define pain management 2. Explore various
Pain Management University of Illinois at Chicago College of Nursing 1 Learning Objectives Upon completion of this module, participants will be better able to: 1. Define pain management 2. Explore various
16 year old with Disabling Chest Wall Pain after Thoracoscopic Talc Pleurodesis for Treatment of Recurrent Spontaneous Pneumothoraces
 16 year old with Disabling Chest Wall Pain after Thoracoscopic Talc Pleurodesis for Treatment of Recurrent Spontaneous Pneumothoraces Moderators: Kendra Grim, MD, Robert T. Wilder, MD, PhD Institution:
16 year old with Disabling Chest Wall Pain after Thoracoscopic Talc Pleurodesis for Treatment of Recurrent Spontaneous Pneumothoraces Moderators: Kendra Grim, MD, Robert T. Wilder, MD, PhD Institution:
Robin R. Dyer, D.O. Associate Dean for Academic Affairs Professor/Chair OMM Department Tulsa, Oklahoma. LBP Prevalence
 Robin R. Dyer, D.O. Associate Dean for Academic Affairs Professor/Chair OMM Department Tulsa, Oklahoma LBP Prevalence Approx. 80% adults sometime in their lifetime 2 nd most common pain complaint (headache
Robin R. Dyer, D.O. Associate Dean for Academic Affairs Professor/Chair OMM Department Tulsa, Oklahoma LBP Prevalence Approx. 80% adults sometime in their lifetime 2 nd most common pain complaint (headache
CERVICAL SPINE TIPS A
 CERVICAL SPINE TIPS A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of
CERVICAL SPINE TIPS A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of
8/6/18. Definitions. Disclosures. Technician Objectives. Pharmacist Objectives. Chronic Pain. Non-Opioid Alternatives for Chronic Pain Management
 Disclosures Non-Opioid Alternatives for Chronic Management Nicholas Cox, PharmD, BCACP Clinical Pharmacist, Intensive Outpatient Clinic, University of Utah Health Pharmacist, Population Health, University
Disclosures Non-Opioid Alternatives for Chronic Management Nicholas Cox, PharmD, BCACP Clinical Pharmacist, Intensive Outpatient Clinic, University of Utah Health Pharmacist, Population Health, University
405 Firemans Ave LaVale, Maryland 21502
 Dec 19, 2016 CHIEF COMPLAINT: Iris presents with a chief complaint involving her lower lumbar and sacral region, left sacroiliac region and left anterior hip and groin. ONSET OF SYMPTOMS Iris states this
Dec 19, 2016 CHIEF COMPLAINT: Iris presents with a chief complaint involving her lower lumbar and sacral region, left sacroiliac region and left anterior hip and groin. ONSET OF SYMPTOMS Iris states this
MANAGING CHRONIC PAIN
 George Hardas MANAGING CHRONIC PAIN The guide to understanding chronic pain and how to manage it. George Hardas MMed (UNSW) MScMed (Syd) MChiro (Macq) BSc (Syd) Grad Cert Pain Management (Syd) Cognitive
George Hardas MANAGING CHRONIC PAIN The guide to understanding chronic pain and how to manage it. George Hardas MMed (UNSW) MScMed (Syd) MChiro (Macq) BSc (Syd) Grad Cert Pain Management (Syd) Cognitive
WHAT IS SCIATICA? Apart from the compression of one of the nerves, there are other known causes of sciatica which include:
 WHAT IS SCIATICA? If you suffer from Sciatica, or you re close to someone who does, you already know that it is one of those conditions that can be quite overwhelming and incapacitating while causing a
WHAT IS SCIATICA? If you suffer from Sciatica, or you re close to someone who does, you already know that it is one of those conditions that can be quite overwhelming and incapacitating while causing a
Fibromyalgia , The Patient Education Institute, Inc. id Last reviewed: 03/12/2017 1
 Fibromyalgia Introduction Fibromyalgia is a common condition that causes pain and fatigue in the muscles, joints, ligaments and tendons. Fibromyalgia affects about 3 to 6% of people worldwide. Fibromyalgia
Fibromyalgia Introduction Fibromyalgia is a common condition that causes pain and fatigue in the muscles, joints, ligaments and tendons. Fibromyalgia affects about 3 to 6% of people worldwide. Fibromyalgia
SUMMARY OF ARIZONA OPIOID PRESCRIBING GUIDELINES FOR THE TREATMENT OF CHRONIC NON-TERMINAL PAIN (CNTP)
 9 SUMMARY OF ARIZONA OPIOID PRESCRIBING GUIDELINES FOR THE TREATMENT OF CHRONIC NON-TERMINAL PAIN (CNTP) SUMMARY OF ARIZONA OPIOID PRESCRIBING GUIDELINES FOR THE TREATMENT OF ACUTE PAIN NONOPIOID TREATMENTS
9 SUMMARY OF ARIZONA OPIOID PRESCRIBING GUIDELINES FOR THE TREATMENT OF CHRONIC NON-TERMINAL PAIN (CNTP) SUMMARY OF ARIZONA OPIOID PRESCRIBING GUIDELINES FOR THE TREATMENT OF ACUTE PAIN NONOPIOID TREATMENTS
Learning Objectives. Perioperative goals. Acute Pain in the Chronic Pain Patient for Ambulatory Surgery 9/8/16
 Acute Pain in the Chronic Pain Patient for Ambulatory Surgery Danielle Ludwin, MD Associate Professor of Anesthesiology Division of Regional and Orthopedic Anesthesia Columbia University Medical Center
Acute Pain in the Chronic Pain Patient for Ambulatory Surgery Danielle Ludwin, MD Associate Professor of Anesthesiology Division of Regional and Orthopedic Anesthesia Columbia University Medical Center
PAIN MANAGEMENT IN UROLOGY
 24 PAIN MANAGEMENT IN UROLOGY F. Francesca (chairman), P. Bader, D. Echtle, F. Giunta, J. Williams Eur Urol 2003; 44(4):383-389 Introduction Pain is defined as an unpleasant sensory and emotional experience
24 PAIN MANAGEMENT IN UROLOGY F. Francesca (chairman), P. Bader, D. Echtle, F. Giunta, J. Williams Eur Urol 2003; 44(4):383-389 Introduction Pain is defined as an unpleasant sensory and emotional experience
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
Spine Conditions and Treatments. Your Guide to Common
 Your Guide to Common Spine Conditions and Treatments The spine is made up of your neck and backbone. It allows your body to bend and move freely. As you get older, it is normal to have aches and pains.
Your Guide to Common Spine Conditions and Treatments The spine is made up of your neck and backbone. It allows your body to bend and move freely. As you get older, it is normal to have aches and pains.
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS North American Spine Society Public Education Series WHAT IS LUMBAR SPINAL STENOSIS? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
LUMBAR SPINAL STENOSIS North American Spine Society Public Education Series WHAT IS LUMBAR SPINAL STENOSIS? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Chronic Pain in Patients With HIV: What Clinicians Need to Know
 Chronic Pain in Patients With HIV: What Clinicians Need to Know Jessica S. Merlin, MD, MBA Assistant Professor of Medicine University of Alabama at Birmingham Birmingham, Alabama FLOWED: 11/03/2015 Learning
Chronic Pain in Patients With HIV: What Clinicians Need to Know Jessica S. Merlin, MD, MBA Assistant Professor of Medicine University of Alabama at Birmingham Birmingham, Alabama FLOWED: 11/03/2015 Learning
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
Cervical intervertebral disc disease Degenerative diseases F 04
 Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Back Pain. John W. Engstrom, MD December 16, Disclosures. A Clinical Approach to the Evaluation of Back Pain and Lumbar Radiculopathy
 Disclosures Nothing to declare --- or --- Significant ownership interests Speaker bureaus, honorarium, grants A Clinical Approach to the Evaluation of and Lumbar Radiculopathy John Engstrom, MD Acute Low
Disclosures Nothing to declare --- or --- Significant ownership interests Speaker bureaus, honorarium, grants A Clinical Approach to the Evaluation of and Lumbar Radiculopathy John Engstrom, MD Acute Low
Optimizing Non-Opioid Therapy for Chronic Pain
 Optimizing Non-Opioid Therapy for Chronic Pain Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means
Optimizing Non-Opioid Therapy for Chronic Pain Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means
UCSF Pediatric Hospital Medicine Boot Camp Pain Session 6/21/14. Cynthia Kim and Stephen Wilson
 UCSF Pediatric Hospital Medicine Boot Camp Pain Session 6/21/14 Cynthia Kim and Stephen Wilson Rules Buzz first and player answers If answer correct, then the player asks teammates if they want to keep
UCSF Pediatric Hospital Medicine Boot Camp Pain Session 6/21/14 Cynthia Kim and Stephen Wilson Rules Buzz first and player answers If answer correct, then the player asks teammates if they want to keep
Medical Affairs Policy
 Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Back Safety Healthcare #09-066
 Back Safety Healthcare Version #09-066 I. Introduction A. Scope of training This training program applies to healthcare employees whose job requires them to lift patients or other heavy objects. Lifting
Back Safety Healthcare Version #09-066 I. Introduction A. Scope of training This training program applies to healthcare employees whose job requires them to lift patients or other heavy objects. Lifting
Neuropathic pain (pain due to nerve damage)
 Neuropathic pain (pain due to nerve damage) Clinical Guideline Pain can be nociceptive, neuropathic or mixed. The neuropathic component of pain generally responds poorly to conventional analgesics. Consider
Neuropathic pain (pain due to nerve damage) Clinical Guideline Pain can be nociceptive, neuropathic or mixed. The neuropathic component of pain generally responds poorly to conventional analgesics. Consider
Practical Management Of Osteoporosis
 Practical Management Of Osteoporosis CONFERENCE 2012 Education Centre, Bournemouth.19 November The following companies have given funding towards the cost of this meeting but have no input into the agenda
Practical Management Of Osteoporosis CONFERENCE 2012 Education Centre, Bournemouth.19 November The following companies have given funding towards the cost of this meeting but have no input into the agenda
Slide 1. Slide 2. Treatment Regimens for Acute and Chronic Pain Patients: How to Progress All Injured Workers to Working Status. What is Acute Pain?
 Slide 1 Treatment Regimens for Acute and Chronic Pain Patients: How to Progress All Injured Workers to Working Status Anesco Interventional Pain Institute Slide 2 What is Acute Pain? Physiologic response
Slide 1 Treatment Regimens for Acute and Chronic Pain Patients: How to Progress All Injured Workers to Working Status Anesco Interventional Pain Institute Slide 2 What is Acute Pain? Physiologic response
The pain of it all. Rod MacLeod MNZM. Hibiscus Hospice, Auckland and University of Auckland
 The pain of it all Rod MacLeod MNZM Hibiscus Hospice, Auckland and University of Auckland Definition of PAIN An unpleasant sensory and emotional experience which we primarily associate with tissue damage
The pain of it all Rod MacLeod MNZM Hibiscus Hospice, Auckland and University of Auckland Definition of PAIN An unpleasant sensory and emotional experience which we primarily associate with tissue damage
Managing the Chronic Pain Patient. (and some stuff about opioids)
 Managing the Chronic Pain Patient. (and some stuff about opioids) C. Patrick Carroll, M.D. Assistant Professor Johns Hopkins University School of Medicine Department of Psychiatry and Behavioral Sciences
Managing the Chronic Pain Patient. (and some stuff about opioids) C. Patrick Carroll, M.D. Assistant Professor Johns Hopkins University School of Medicine Department of Psychiatry and Behavioral Sciences
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
Your guide to a healthy back. Quick and easy tips to keep your back and neck healthy.
 S A L E M H E A LT H S P I N E C E N T E R Your guide to a healthy back Quick and easy tips to keep your back and neck healthy. Taking care of neck or back pain Take it easy If you think you ve hurt your
S A L E M H E A LT H S P I N E C E N T E R Your guide to a healthy back Quick and easy tips to keep your back and neck healthy. Taking care of neck or back pain Take it easy If you think you ve hurt your
