Current Treatment of Childhood Constipation
|
|
|
- Gwendoline Lindsey
- 6 years ago
- Views:
Transcription
1 Ann Nestlé [Engl] 2007;65:73 79 DOI: / O livia Liem a, b Carlo Di Lorenzo b Jan A.J.M. Taminiau a Hayat M. Mousa b Marc A. Benninga a a Department of Pediatric Gastroenterology and Nutrition, Emma Children s Hospital, Academic Medical Center, Amsterdam, The Netherlands, and b Division of Pediatric Gastroenterology, Columbus Children s Hospital, Columbus, Ohio, USA Key Words Treatment Children Abstract Childhood constipation is a worldwide problem. It is one of the more common complaints presented to both general pediatricians and pediatric gastroenterologists. Treatment for chronic constipation is challenging and often requires long-term follow-up and medication use. Despite its high prevalence, few randomized trials have been performed to investigate the efficacy of different interventions used to treat this condition. In this review we will discuss current treatment options for childhood constipation and address some of the most frequently asked questions and misconceptions among parents and physicians. Introduction Copyright 2007 Nestec Ltd., Vevey/S. Karger AG, Basel is a common problem and affects millions of children around the world. A recent systemic review of the literature shows a prevalence of constipation ranging from 7 to 29.6% both in Western and non-west- ern countries [1]. In approximately 95% of children with constipation, no obvious anatomic, biochemical or physiologic abnormalities can be identified [2]. Many of these children have functional constipation probably resulting from stool withholding after having experienced a painful or frightening bowel movement. Long-term management is needed in most children and approximately 30% of children beyond puberty continue to struggle with symptoms of constipation, such as infrequent and painful stool evacuation and fecal incontinence [3]. Not surprisingly, the chronicity of these bowel complaints may have significant and permanent effects on the child s self-esteem and emotional growth and development. Thus, it is important to treat constipation early and effectively in order to prevent its significant morbidity [4]. The lack of randomized controlled studies in children has made the treatment of constipation largely based on clinical experience rather than on evidence-based clinical trials. Acute simple constipation is traditionally treated with a high fiber diet and sufficient fluid intake, filling out a bowel diary and toilet training. The recently updated NAPSGHAN recommendations include 4 important phases in the treatment of chronic constipation: (1) education; (2) disimpaction; (3) prevention of re-accu- Fax karger@karger.ch Nestec Ltd., Vevey/S. Karger AG, Basel /07/ $23.50/0 Accessible online at: O. Liem, MD Columbus Children s Hospital Department of Pediatric Gastroenterology and Nutrition 700 Children s Drive, Columbus, OH (USA) Tel , Fax , liemo@chi.osu.edu
2 mulation of feces, and (4) follow-up [5]. In this review all 4 steps will be discussed together with some of the most frequently asked questions and misconceptions about childhood constipation. Education and Counseling Education and support for parents and children is an important component of treatment of functional constipation. The parents need to be reassured and counseled regarding the normal range of frequency of bowel movements within the population, the etiology of constipation, and its prevalence in childhood. If fecal incontinence is present, it is important for caretakers to understand that this bothersome symptom is caused by overflow diarrhea and is not an act of willful and defiant behavior. Parents should have a non-accusatory approach and use positive reinforcement to motivate their children. Before treatment is started, parents and children should be reassured that recovery is possible with adequate, often prolonged, treatment. It should also be stressed that the time point of success of treatment is often unpredictable and 50% of treated patients experience a relapse within 1 year and the duration of maintenance therapy usually is 6 24 months [3]. Since laxatives usually constitute an important part of the treatment, it is essential to educate parents on the medications given because there are often misconceptions concerning these medications which could interfere with adherence. While medications used for the treatment of other conditions, such as gastroesophageal reflux, asthma, hypertension, and other chronic problems, are usually accepted and at times even sought by families of affected children, the prescription of laxatives usually encounters resistance by caretakers who find it disheartening that such a young child may already need laxatives! One of the most frequently asked questions by worried parents is whether the long-term use of laxatives is harmful and can give rise to lazy bowels leading to physical dependence. Each of these concerns has recently been addressed in a thorough review of the existing literature [6]. The arguments in favor of laxative-induced (especially stimulant laxatives) damage to the autonomous nervous system of the colon were derived from data gathered by poorly documented experiments, while the investigations that did not support such damage were well done and performed using a variety of techniques [6]. Osmotic laxatives do not seem to have any long-term side effects. Although a proportion of patients with chronic constipation require long-term use of laxatives to achieve normal bowel movements, no evidence exists that this is the result of prior laxative intake, nor is there any indication of rebound symptoms after stopping laxative intake. Therefore, parents should be reassured of the safety of the medications when taken in the prescribed dosage and encouraged to adhere to the treatment with medications to achieve success. D i e t Although it is a widespread concept that lack of fiber is a common cause of constipation, only a few pediatric trials have been performed to evaluate the efficacy of fiber therapy. Conflicting reports exist about constipated children having a lower, equivalent or higher intake of dietary fiber compared to non-constipated children [7 9]. The recommended minimum daily fiber intake for children older than 2 years is age in years plus 5 g [10]. Recent standardized trials in children have shown the beneficial effects of fiber supplementation in children with chronic constipation. Compared to a placebo group, Castillejo et al. [11] found a decrease in colonic transit time in children who had a basal prolonged colonic transit time and received cocoa husk. They also observed a reduction in the percentage of patients who reported hard stools. It has to be noted that these constipated children had a mean fiber intake near the recommended amount of total fiber for the specific age groups. Glucomannan supplement also led to more frequent and softer stools with an improved response to laxative treatment [12, 13]. One of the main factors that has limited the long-term efficacy of dietary fibers in children has been the poor adherence to treatment due to the fact that most fiber agents like cellulose fiber, guar gum and pectin fiber have to be consumed in large quantities to be effective and that they are unpalatable. The fibers used in the previously mentioned trials had a good acceptance rate and did not have any notable side effects. While lack of fibers is probably not the cause of chronic constipation in general, it may be a contributory factor in a subgroup. Therefore, a balanced diet containing whole grains, fruits, and vegetables is recommended as part of the treatment of constipation, without forceful implementation of fiber in the diet [5]. Increased fluid intake is another widely recommended therapy and is based on the assumption that additional oral intake of fluids leads to an increased contribution to colonic fluids, which would enhance increased stool 74 Ann Nestlé [Engl] 2007;65:73 79 Liem /Di Lorenzo /Taminiau /Mousa / Benninga
3 output. A study looking at 108 constipated children who were randomized to a control group and 2 interventional groups, where 1 group was instructed to increase their daily water intake by 50%, did not show any changes regarding stool frequency, consistency or ease of defecation [14]. The reason that the increased fluid did not result in a change in bowel habits might have to do with the large adaptive absorptive capacity of the small and large bowel in response to acute or chronic challenges [15, 16]. The solutes, not water, contribute to ileal effluents. Consequently minor modifications in liquid intake will not significantly alter stool consistency. There is no evidence that constipation can be successfully treated by increasing fluid intake; unless there is evidence of dehydration, constipated children should not be forced to drink more than normal. Disimpaction Rectal disimpaction of the usually present large fecal mass before initiation of maintenance therapy is recommended to prevent increases in abdominal pain and fecal incontinence due to overflow diarrhea once treatment has started [5]. Uncontrolled clinical trials have shown successful disimpaction by the oral route, rectal route, or a combination of the two methods [17 20]. There are no randomized controlled studies that have compared methods of disimpaction. A double-blind, different-doses, randomized trial showed polyethylene glycol (PEG) at doses of g/kg/day to be effective for disimpacting children, with good acceptance by children and parents [19 21]. No abnormalities in the serum osmolality and electrolytes or renal function tests were reported. Other agents that have been used successfully, but for which controlled trials are lacking, include magnesium hydroxide, magnesium citrate, lactulose, sorbitol, senna and bisacodyl. Rectal disimpaction is widely performed with phosphate soda enemas, saline enemas, or mineral oil enemas followed by a phosphate enema. Both ways of disimpaction, either orally or rectally, have their advantages and disadvantages, with the first method being less invasive but requiring more time than the latter. Attention should be paid to the expulsion of phosphate-containing enemas in order to prevent the absorption of excessive quantities of phosphates [22]. The choice of treatment is best determined after discussing the options with the family and child. Maintenance Therapy Once disimpaction has been accomplished, the goal is to produce soft, painless bowel movements once or twice per day. Regularity for a longer period of time is important to prevent recurrent impaction and recurrence of stool withholding behavior. This usually requires use of laxatives in combination with behavioral therapy over an extended period which may last for months or years. Despite the high prevalence and the chronicity of constipation, only a small number of randomized controlled trials have been performed to evaluate the effect of any laxative treatment in children [23 25]. Osmotic laxatives include milk of magnesia, lactulose and PEG. Their mechanism is derived either by salts of poorly absorbable cations and anions (magnesium, phosphate), molecules that are not absorbed but to some extent metabolized in the colon (lactulose), or metabolically inert compounds. Magnesium hydroxide/sulfate or milk of magnesia, as it is known in the United States, is an osmotic laxative that has a long history. Both magnesium hydroxide and magnesium sulfate are two poorly absorbed salts that act either by osmosis or by a secretory effect on prostaglandins or cholecystokinin thereby enhancing colonic motility [26, 27]. Lactulose, another widely used laxative, is a disaccharide derived from lactose and is effective in increasing defecation frequency and normalizing stool consistency [28, 29]. PEGs are synthetic, non-absorbable compounds with a high molecular mass (3,000 and higher), and are not metabolized by colonic bacteria. They exert their action by osmosis and volume expansion in the colon. PEG is available in powder form, and is colorless and odorless. It is available in combination with or without electrolytes. PEG without electrolytes has the advantage of being tasteless, a factor which can play a great role in increasing compliance with prolonged treatment in children. In two multicentered randomized controlled trials, PEG with electrolytes compared with lactulose was shown to attain a higher short-term success rate (50 vs. 29%) with better stool consistency, increased appetite, less fecal impactions, and less enema use. PEG with electrolytes had significantly fewer adverse effects, such as abdominal pain, nausea, flatulence and diarrhea, compared to lactulose but children complained about the bad taste. A randomized trial comparing PEG without electrolytes with milk of magnesia in 49 children with functional constipation and fecal incontinence demonstrated similar effectiveness after follow-up at 1, 3, 6, and 12 months: increased bowel movement frequency, decreased fecal incontinence Ann Nestlé [Engl] 2007;65:
4 episodes, and decreased abdominal pain [25]. It also revealed that PEG was more palatable and better tolerated than milk of magnesia (33% of children refused to take milk of magnesia, whereas none refused PEG). No side effects of PEG were reported. Parents should also be warned that after starting laxative treatment some leakage of feces may continue at first or, even worsen, especially if the child fears or continues to resist having a bowel movement. Stimulant laxatives, such as senna and bisacodyl, were developed decades ago and the studies investigating these drugs do not meet the current criteria for good quality therapeutic clinical trials making a review for comparison analysis not possible [30]. In contrast to previously mentioned osmotic laxatives, these stimulant laxatives are generally not encouraged for long-term daily treatment. One of their common side effects is cramping. Use of these medications may be necessary intermittently to avoid recurrence of impaction. It is still controversial whether anthraquinone-containing laxatives, such as senna, can lead to morphologic changes in the autonomous nervous system of the colon. Melanosis coli, an easily visible brown discoloration of the colon, may occur within months of regular use and can last for months after discontinuing the laxatives [31, 32]. This pigmentation is caused by the uptake of laxative-stained cell debris by the submucosal macrophages but this discoloration does not seem to have any functional consequences [33]. A reasonable regimen is to use stimulant laxatives when no spontaneous bowel movement has occurred for 48 or 72 h in combination with daily osmotic laxatives. Behavioral Therapy The combination of behavioral intervention combined with laxative treatment has the goal of lowering the level of distress associated with bowel movements and developing or restoring normal bowel habits by positive reinforcement. A commonly used practice is encouraging regular toilet training with the child being instructed to sit on the toilet for 5 10 min after each meal (to take advantage of the gastrocolonic reflex) in an attempt to defecate. The patient is stimulated to strain actively while placing his feet on a footrest. The child needs to understand that responding to the defecatory urge and not holding back is the key to success of the treatment. Another frequently used aid is to let the child keep a bowel diary to record complaints, quantify therapeutic progress and to enhance motivation. Small, age-appropriate reward systems are established for successful compliance. Behavioral modification has been studied for constipation-related fecal incontinence. A randomized controlled trial of 87 children compared three treatment modalities: intensive medical therapy; intensive medical therapy with enhanced toilet training, or intensive medical therapy with enhanced toilet training and biofeedback therapy. After 12 months, no statistically significant difference was found in the success rate among the three methods [34]. No study has yet studied the added effect of behavioral modification to medical treatment with laxatives. Psychological referral is indicated in children who fail intensive medical treatment and in those with severe emotional problems or serious family problems. B i o f e e d b a c k The role of biofeedback in the treatment of childhood constipation seems to be limited [35]. This habit training, which is based on reinforcement and is derived from a psychological learning theory, has been employed to teach children how to control their sphincter muscles using biofeedback devices, like anorectal monitoring instruments that allow the muscle tone of the external anal sphincter to be displayed on a screen or presented as sound modulations [36]. The rationale for this treatment lies in the fact that in more than 50% of children with defecation disorders the external anal sphincter and puborectalis muscles contract instead of relax during defecation (the physiologic manifestation of a withholding behavior) [37]. Biofeedback has also been thought to be useful to educate children about the sensations experienced with rectal distension. Some children are unaware that this sensation indicates the need to defecate. Small uncontrolled trials have shown that adequate contraction of the external sphincter or normalization of abnormal defecation dynamics can be achieved by biofeedback training. While a study by Loening-Baucke [38, 39] initially indicated a significant short-term effect of biofeedback, the additional benefit to laxative treatment was not seen in other controlled trials and after long-term follow-up [37, 40, 41]. Furthermore, the observed improvement in manometric parameters does not appear to translate into functional improvement as demonstrated by a large randomized controlled study of 192 constipated children in whom achievement of normal defecation dynamics was not associated with clinical success [37]. 76 Ann Nestlé [Engl] 2007;65:73 79 Liem /Di Lorenzo /Taminiau /Mousa / Benninga
5 Based on these data we conclude that there is no strong evidence to support biofeedback as a useful additional treatment for defecation disorders in the majority of children. S u r g e r y While most children with constipation are successfully treated with the conventional regimen described earlier, some children will continue to be symptomatic despite intensive therapy and optimal compliance with treatment. When these symptoms are severe enough to significantly impact the patient s quality of life, physicians might have to resort to surgery. Especially fecal incontinence, which frequently accompanies chronic constipation, can have a dramatic negative impact on the emotional and social development of the affected children [42]. Until recently, creation of a colostomy or performance of a partial colectomy were the only surgical options when nonoperative management failed. Such surgical interventions were deemed to be too invasive, were frequently irreversible, and often associated with a unpredictable clinical outcome, and are rarely utilized. Novel alternatives are now available. A continent appendicostomy or a button cecostomy can be created to provide anterograde administration of enemas aimed at cleansing the entire colon and providing predictable fecal incontinence-free intervals. Cecostomy tubes can be safely placed percutaneously by interventional radiology or endoscopy instead of surgery [43]. Regular colonic lavage results in a significant increase in defecation frequency, a reduction in fecal incontinence frequency, and consequently an improvement in quality of life [43, 44]. Success rates are high in most studies (up to 80%), probably due to careful pre-cecostomy evaluation and patient selection. Older motivated children with a normal response to colonic stimulants or the presence of propagated contractions at the time of colonic manometry testing are thought to experience more success than younger children with no response to colonic stimulants [45]. Colonic manometry is used as a predictor of cecostomy success in children with defecation disorders. Potential side effects in children receiving an appendicostomy are stenosis of the cutaneous opening (11%), painful or difficult catheterization (5%), and iatrogenic perforation of the appendicostomy [46]. Dislodged tubes (26%), leakage around the cecostomy button (42%), and granulation tissue (68%) are complications known to occur with cecostomy devices [43]. Of course, surgery should only be considered in children who have had symptoms for many years, have not responded to multiple medical treatments, and have required multiple hospitalizations for treatment of their symptoms. Comprehensive motility testing including colon manometry may help guide clinical decisions about surgery [47 49]. Follow-Up and Referral to Subspecialists The maintenance phase starts after the first steps of education and disimpaction are completed, and it may last many months to years. Van Ginkel et al. [3] found that 50% of the treated children had at least one relapse within the first 5 years after initial treatment success, and 30 50% persisted to have severe symptoms after 5 years of follow-up, even beyond the age of 18 years. These high percentages of relapse and persistence of constipation stress the importance of close and prolonged follow-up of children with constipation. Follow-up by office visits in the beginning, as often as every 3 4 weeks, to assure adherence to and the effectiveness of the treatment program is recommended. Visit intervals can be lengthened as the treatment proves to be successful, and office visits can be alternated with phone communications to keep track of progress. It might be necessary to repeat the education and demystification processes several times during treatment [50]. After success is obtained, the question arises whether to continue the medication and for how long. One common strategy is to continue treatment for at least 2 3 months after complete resolution of symptoms before attempting to taper medications, considering the high relapse rates in the first years. If the child remains symptom-free, the medication dose can be decreased with instructions to the parents to pay close attention to the child s bowel habits and stool consistency to avoid painful bowel movements that could again induce withholding behavior. If symptoms reappear, not only should medications be started again but the bowel diary should be restarted and toilet training newly emphasized. Referral or consultation with a pediatric gastroenterologist becomes necessary when therapy fails or when there is concern about an organic disease. The pediatric gastroenterologist can reevaluate the child, order specialized tests when deemed necessary and review previous therapies. Different or additional medications or higher doses of current medications are often prescribed before performing additional studies. Ann Nestlé [Engl] 2007;65:
6 Key M e s s a g e s (1) Educating children and their parents about normal bowel habits, the etiology of constipation and its treatment is an important factor to ensure adherence to the treatment program and to achieve a successful outcome. (2) There is good evidence to support the use of PEG as first-line drug in childhood constipation. (3) Close and long-term follow-up in children with chronic constipation is important considering the high prevalence of relapse and persistence of symptoms. References 1 van den Berg MM, Benninga MA, Di Lorenzo C: Epidemiology of childhood constipation: a systematic review. Am J Gastroenterol 2006; 101: Baker SS, Liptak GS, Colletti RB, et al: in infants and children: evaluation and treatment. A medical position statement of the North American Society for Pediatric Gastroenterology and Nutrition. J Pediatr Gastroenterol Nutr 1999; 29: van Ginkel R, Reitsma JB, Buller HA, et al: Childhood constipation: longitudinal follow-up beyond puberty. Gastroenterology 2003; 125: Loening-Baucke V: in early childhood: patient characteristics, treatment, and longterm follow up. Gut 1993; 34: Evaluation and treatment of constipation in infants and children: recommendations of the North American Society for Pediatric Gastroenterology, Hepatology and Nutrition. J Pediatr Gastroenterol Nutr 2006; 43: e1 e13. 6 Muller-Lissner SA, Kamm MA, Scarpignato C, Wald A: Myths and misconceptions about chronic constipation. Am J Gastroenterol 2005; 100: Roma E, Adamidis D, Nikolara R, et al: Diet and chronic constipation in children: the role of fiber. J Pediatr Gastroenterol Nutr 1999; 28: McClung HJ, Boyne L, Heitlinger L: and dietary fiber intake in children. Pediatrics 1995; 96: Morais MB, Vitolo MR, Aguirre AN, Fagundes-Neto U: Measurement of low dietary fiber intake as a risk factor for chronic constipation in children. J Pediatr Gastroenterol Nutr 1999; 29: Williams CL, Bollella M, Wynder EL: A new recommendation for dietary fiber in childhood. Pediatrics 1995; 96: Castillejo G, Bullo M, Anguera A, et al: A controlled, randomized, double-blind trial to evaluate the effect of a supplement of cocoa husk that is rich in dietary fiber on colonic transit in constipated pediatric patients. Pediatrics 2006; 118:e641 e Loening-Baucke V, Miele E, Staiano A: Fiber (glucomannan) is beneficial in the treatment of childhood constipation. Pediatrics 2004; 113:e259 e Staiano A, Simeone D, Del GE, et al: Effect of the dietary fiber glucomannan on chronic constipation in neurologically impaired children. J Pediatr 2000; 136: Young RJ, Beerman LE, Vanderhoof JA: Increasing oral fluids in chronic constipation in children. Gastroenterol Nurs 1998; 21: Schlessinger M, Fordtran JS (eds): Gastroenterology, ed 6. Philadelphia, Saunders, 1998, pp Debongnie JC, Phillips SF: Capacity of the human colon to absorb fluid. Gastroenterology 1978; 74: Tolia V: Use of a balanced lavage solution in the treatment of fecal impaction. J Pediatr Gastroenterol Nutr 1988; 7: Tolia V, Lin CH, Elitsur Y: A prospective randomized study with mineral oil and oral lavage solution for treatment of faecal impaction in children. Aliment Pharmacol Ther 1993; 7: Youssef NN, Peters JM, Henderson W, et al: Dose response of PEG 3350 for the treatment of childhood fecal impaction. J Pediatr 2002; 141: Pashankar DS, Uc A, Bishop WP: Polyethylene glycol 3350 without electrolytes: a new safe, effective, and palatable bowel preparation for colonoscopy in children. J Pediatr 2004; 144: Candy DC, Edwards D, Geraint M: Treatment of faecal impaction with polyethelene glycol plus electrolytes (PGE + E) followed by a double-blind comparison of PEG + E versus lactulose as maintenance therapy. J Pediatr Gastroenterol Nutr 2006; 43: McClung HJ, Potter C: Rational use of laxatives in children. Adv Pediatr 2004; 51: Voskuijl W, de Lorijn F, Verwijs W, et al: PEG 3350 (Transipeg) versus lactulose in the treatment of childhood functional constipation: a double blind, randomised, controlled, multicentre trial. Gut 2004; 53: Dupont C, Leluyer B, Ammar F, et al: Double-blind randomized evaluation of clinical and biological tolerance of polyethylene glycol 4000 versus lactulose in constipated children. J Pediatr Gastroenterol Nutr 2005;41: Loening-Baucke V, Pashankar DS: A randomized, prospective, comparison study of polyethylene glycol 3350 without electrolytes and milk of magnesia for children with constipation and fecal incontinence. Pediatrics 2006; 118: Donowitz M, Rood RP: Magnesium hydroxide: new insights into the mechanism of its laxative effect and the potential involvement of prostaglandin E2. J Clin Gastroenterol 1992; 14: Younoszai MK, Tolaymat N: Chronic functional constipation in infants and children; in Lebenthal E (ed): Textbook of Gastroenterology and Nutrition in Infancy. New York, Raven Press Ltd, 1989, pp Martino AM, Pesce F, Rosati U: The effects of lactitol in the treatment of intestinal stasis in childhood (in Italian). Minerva Pediatr 1992; 44: Pitzalis G, Deganello F, Mariani P, et al: Lactitol in chronic idiopathic constipation in children. Pediatr Med Chir 1995; 17: Price KJ, Elliott TM: What is the role of stimulant laxatives in the management of childhood constipation and soiling? Cochrane Database Syst Rev 2001; 3:CD Willems M, van Buuren HR, de Krijger R: Anthranoid self-medication causing rapid development of melanosis coli. Neth J Med 2003; 61: Speare GS: Melanosis coll; experimental observations on its production and elimination in twenty-three cases. Am J Surg 1951; 82: Ghadially FN, Walley VM: Melanoses of the gastrointestinal tract. Histopathology 1994; 25: Borowitz SM, Cox DJ, Sutphen JL, Kovatchev B: Treatment of childhood encopresis: a randomized trial comparing three treatment protocols. J Pediatr Gastroenterol Nutr 2002; 34: Ann Nestlé [Engl] 2007;65:73 79 Liem /Di Lorenzo /Taminiau /Mousa / Benninga
7 35 Brazzelli M, Griffiths P: Behavioural and cognitive interventions with or without other treatments for the management of faecal incontinence in children. Cochrane Database Syst Rev 2006; 2:CD Engel BT, Nikoomanesh P, Schuster MM: Operant conditioning of rectosphincteric responses in the treatment of fecal incontinence. N Engl J Med 1974; 290: van der Plas RN, Benninga MA, Buller HA, et al: Biofeedback training in treatment of childhood constipation: a randomised controlled study. Lancet 1996; 348: Loening-Baucke V: Modulation of abnormal defecation dynamics by biofeedback treatment in chronically constipated children with encopresis. J Pediatr 1990; 116: Loening-Baucke V: Biofeedback treatment for chronic constipation and encopresis in childhood: long-term outcome. Pediatrics 1995; 96: Wald A, Chandra R, Gabel S, Chiponis D: Evaluation of biofeedback in childhood encopresis. J Pediatr Gastroenterol Nutr 1987; 6: Nolan T, Catto-Smith T, Coffey C, Wells J: Randomised controlled trial of biofeedback training in persistent encopresis with anismus. Arch Dis Child 1998; 79: Youssef NN, Langseder AL, Verga BJ, Mones RL, Rosh JR: Chronic childhood constipation is associated with impaired quality of life: a case-controlled study. J Pediatr Gastroenterol Nutr 2005; 41: Mousa HM, van den Berg MM, Caniano DA, et al: Cecostomy in children with defecation disorders. Dig Dis Sci 2006; 51: Youssef NN, Barksdale JE, Griffiths JM, et al: Management of intractable constipation with antegrade enemas in neurologically intact children. J Pediatr Gastroenterol Nutr 2002; 34: van den Berg MM, Hogan M, Caniano DA, et al: Colonic manometry as predictor of cecostomy success in children with defecation disorders. J Pediatr Surg 2006; 41: Cascio S, Flett ME, De la Hunt M, et al: MACE or caecostomy button for idiopathic constipation in children: a comparison of complications and outcomes. Pediatr Surg Int 2004; 20: Youssef NN, Pensabene L, Barksdale E Jr, Di Lorenzo C: Is there a role for surgery beyond colonic aganglionosis and anorectal malformations in children with intractable constipation? J Pediatr Surg 2004; 39: Villarreal J, Sood M, Zangen T, et al: Colonic diversion for intractable constipation in children: colonic manometry helps guide clinical decisions. J Pediatr Gastroenterol Nutr 2001; 33: Pensabene L, Youssef NN, Griffiths JM, Di Lorenzo C: Colonic manometry in children with defecatory disorders. Role in diagnosis and management. Am J Gastroenterol 2003; 98: Rappaport LA, Levine MD: The prevention of constipation and encopresis: a developmental model and approach. Pediatr Clin North Am 1986; 33: Ann Nestlé [Engl] 2007;65:
Comparing the efficacy of polyethylene glycol. glycol (PEG), magnesium hydroxide, lactulose. treatment of functional constipation in children
 Original article Comparing the efficacy of polyethylene glycol (PEG), magnesium hydroxide and lactulosein treatment of functional constipation in children Hossein Saneian 1, Neda Mostofizadeh 2 1 Assistant
Original article Comparing the efficacy of polyethylene glycol (PEG), magnesium hydroxide and lactulosein treatment of functional constipation in children Hossein Saneian 1, Neda Mostofizadeh 2 1 Assistant
Constipation in childhood is characterized by a low defecation frequency in combination with either involuntary loss of
 USE OF ROME II CRITERIA IN CHILDHOOD DEFECATION DISORDERS: APPLICABILITY IN CLINICAL AND RESEARCH PRACTICE WIEGER P. VOSKUIJL, MD, JAROM HEIJMANS, HUGO S. A. HEIJMANS, MD, PHD, JAN A. J. M. TAMINIAU,MD,PHD,
USE OF ROME II CRITERIA IN CHILDHOOD DEFECATION DISORDERS: APPLICABILITY IN CLINICAL AND RESEARCH PRACTICE WIEGER P. VOSKUIJL, MD, JAROM HEIJMANS, HUGO S. A. HEIJMANS, MD, PHD, JAN A. J. M. TAMINIAU,MD,PHD,
Constipation in children
 Search date August 2003 Gregory Rubin QUESTIONS Effects of treatments...397 395 INTERVENTIONS CONSTIPATION Trade off between benefits and harms Cisapride with or without magnesium oxide*...397 Unknown
Search date August 2003 Gregory Rubin QUESTIONS Effects of treatments...397 395 INTERVENTIONS CONSTIPATION Trade off between benefits and harms Cisapride with or without magnesium oxide*...397 Unknown
Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P.
 UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
The involuntary loss of feces in the underwear after. Longitudinal Follow-up of Children With Functional Nonretentive Fecal Incontinence.
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 26;4:67 72 Longitudinal Follow-up of Children With Functional Nonretentive Fecal Incontinence WIEGER P. VOSKUIJL,* JOHANNES B. REITSMA, RIJK VAN GINKEL,* HANS A.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 26;4:67 72 Longitudinal Follow-up of Children With Functional Nonretentive Fecal Incontinence WIEGER P. VOSKUIJL,* JOHANNES B. REITSMA, RIJK VAN GINKEL,* HANS A.
Polyethylene Glycol versus Paraffin for the Treatment of Childhood Functional Constipation
 Original Article Iran J Pediatr Sep 2009; Vol 19 (No 3), Pp:255-261 Polyethylene Glycol versus Paraffin for the Treatment of Childhood Functional Constipation Hasan Karami* 1, MD; Mohammad Khademloo 2,
Original Article Iran J Pediatr Sep 2009; Vol 19 (No 3), Pp:255-261 Polyethylene Glycol versus Paraffin for the Treatment of Childhood Functional Constipation Hasan Karami* 1, MD; Mohammad Khademloo 2,
Management of Neurogenic Bowel Dysfunction. Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders
 Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Constipation in Children. Amani Al Hajeri, MD, CABFM, IBFM, MSc MG*
 1 Bahrain Medical Bulletin, Vol. 33, No. 4, December 2011 Education-Family Physician Corner Constipation in Children Amani Al Hajeri, MD, CABFM, IBFM, MSc MG* Constipation in pediatrics age group is frequently
1 Bahrain Medical Bulletin, Vol. 33, No. 4, December 2011 Education-Family Physician Corner Constipation in Children Amani Al Hajeri, MD, CABFM, IBFM, MSc MG* Constipation in pediatrics age group is frequently
Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands
 Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands Constipation 0-10% >10-20% >20-30% >30-40% Mugie SM, et al. Best Pract & Res Clin Gastroenterol
Childhood constipation, a real problem..? Marc Benninga, Emma Children s Hospital, AMC, Amsterdam, the Netherlands Constipation 0-10% >10-20% >20-30% >30-40% Mugie SM, et al. Best Pract & Res Clin Gastroenterol
Treatment of functional constipation in children: Evidence-based recommendations from ESPGHAN and NASPGHAN 2014
 Treatment of functional constipation in children: Evidence-based recommendations from ESPGHAN and NASPGHAN 2014 BS. Nguyễn Thị Kim Ngân Khoa Tiêu Hóa BV Nhi Đồng 2 Introduction Constipation is a common
Treatment of functional constipation in children: Evidence-based recommendations from ESPGHAN and NASPGHAN 2014 BS. Nguyễn Thị Kim Ngân Khoa Tiêu Hóa BV Nhi Đồng 2 Introduction Constipation is a common
Antidiarrheals Antidiarrheal
 Antidiarrheals Major factors in diarrhea Increased motility of the GI tract. Decreased absorption of fluid. Antidiarrheal drugs include: Antimotility agents. Adsorbents. Drugs that modify fluid and electrolyte
Antidiarrheals Major factors in diarrhea Increased motility of the GI tract. Decreased absorption of fluid. Antidiarrheal drugs include: Antimotility agents. Adsorbents. Drugs that modify fluid and electrolyte
BRIEF INTERVENTIONS: ENCOPRESIS
 BRIEF INTERVENTIONS: ENCOPRESIS BI-PED PROJECT (BRIEF INTERVENTIONS: PEDIATRICS) Emotional Health Committee Maryland Chapter American Academy of Pediatrics David Bromberg M.D. Overview: Encopresis is diagnosed
BRIEF INTERVENTIONS: ENCOPRESIS BI-PED PROJECT (BRIEF INTERVENTIONS: PEDIATRICS) Emotional Health Committee Maryland Chapter American Academy of Pediatrics David Bromberg M.D. Overview: Encopresis is diagnosed
Human Anatomy rectum
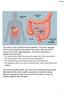 rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
Constipation is a common disorder in children,
 The Effect of Anorectal Manometry on the Outcome of Treatment in Severe Childhood Constipation: A Randomized, Controlled Trial Rijk van Ginkel, MD*; Hans A. Büller, PhD ; Guy E. Boeckxstaens, PhD ; Roos
The Effect of Anorectal Manometry on the Outcome of Treatment in Severe Childhood Constipation: A Randomized, Controlled Trial Rijk van Ginkel, MD*; Hans A. Büller, PhD ; Guy E. Boeckxstaens, PhD ; Roos
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
Chapter 31 Bowel Elimination
 Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Chronic constipation, often accompanied by encopresis. Childhood Constipation: Longitudinal Follow-up Beyond Puberty. Patients and Methods
 GASTROENTEROLOGY 2003;125:357 363 Childhood Constipation: Longitudinal Follow-up Beyond Puberty RIJK VAN GINKEL,* JOHANNES B. REITSMA, HANS A. BÜLLER, MICHIEL P. VAN WIJK,* JAN A. J. M. TAMINIAU,* and
GASTROENTEROLOGY 2003;125:357 363 Childhood Constipation: Longitudinal Follow-up Beyond Puberty RIJK VAN GINKEL,* JOHANNES B. REITSMA, HANS A. BÜLLER, MICHIEL P. VAN WIJK,* JAN A. J. M. TAMINIAU,* and
Paediatric constipation
 EARN 3 FREE CPD POINTS constipation Leader in digital CPD for Southern African healthcare professionals Best practice Paediatric constipation Diagnosis and treatment Dr Tim De Maayer Paediatric Gastroenterologist
EARN 3 FREE CPD POINTS constipation Leader in digital CPD for Southern African healthcare professionals Best practice Paediatric constipation Diagnosis and treatment Dr Tim De Maayer Paediatric Gastroenterologist
Elderly Man With Chronic Constipation
 Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Managing Defecation Disorders in Children
 A SUPPLEMENT TO Internal Medicine News Managing Defecation Disorders in Children Perspectives on Constipation and Encopresis: Current Issues and New Findings Infant Dyschezia and Functional Constipation
A SUPPLEMENT TO Internal Medicine News Managing Defecation Disorders in Children Perspectives on Constipation and Encopresis: Current Issues and New Findings Infant Dyschezia and Functional Constipation
Managing functional constipation in children
 PRACTICE POINT Managing functional constipation in children A Rowan-Legg; Canadian Paediatric Society Community Paediatrics Committee Paediatr Child Health 2011;16(10):661-5 Posted: Dec 1 2011 Reaffirmed:
PRACTICE POINT Managing functional constipation in children A Rowan-Legg; Canadian Paediatric Society Community Paediatrics Committee Paediatr Child Health 2011;16(10):661-5 Posted: Dec 1 2011 Reaffirmed:
Constipation an Old Friend. Presented by Dr. Keith Harris
 Constipation an Old Friend Presented by Dr. Keith Harris Irregularity and the Tricks of the Trade." CONSTIPATION What is constipation? INFREQUENT BOWEL MOVEMENTS DIFFICULTY DURING DEFECATION SENSATION
Constipation an Old Friend Presented by Dr. Keith Harris Irregularity and the Tricks of the Trade." CONSTIPATION What is constipation? INFREQUENT BOWEL MOVEMENTS DIFFICULTY DURING DEFECATION SENSATION
Prescribing Guidance for the Treatment of Constipation in Children
 Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
TREATMENT SOCIETY GUIDELINES FOR CONSTIPATION: WHAT IS NEW? FUNCTIONAL CONSTIPATION
 SOCIETY GUIDELINES FOR CONSTIPATION: WHAT IS NEW? Samuel Nurko MD MPH Center for Motility and Functional Gastrointestinal Disorders FUNCTIONAL CONSTIPATION One of the most common functional GI disorders
SOCIETY GUIDELINES FOR CONSTIPATION: WHAT IS NEW? Samuel Nurko MD MPH Center for Motility and Functional Gastrointestinal Disorders FUNCTIONAL CONSTIPATION One of the most common functional GI disorders
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
CONSTIPATION. Atan Baas Sinuhaji
 CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
Biofeedback for Pelvic Floor Disorders and Incontinence
 The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
Etiology and Clinical Spectrum of Constipation in Indian Children
 R E S E A R C H P A P E R Etiology and Clinical Spectrum of Constipation in Indian Children VIKRANT KHANNA*, UJJAL PODDAR AND SURENDER KUMAR YACHHA From the Departments of Pediatric Gastroenterology and
R E S E A R C H P A P E R Etiology and Clinical Spectrum of Constipation in Indian Children VIKRANT KHANNA*, UJJAL PODDAR AND SURENDER KUMAR YACHHA From the Departments of Pediatric Gastroenterology and
Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P.
 UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
Constipation. Self-study course
 Constipation Self-study course 2 Course objectives: At the end of this course you will be able to: 1. Define the term constipation 2. Explain three reasons why older adults are at greater risk for constipation
Constipation Self-study course 2 Course objectives: At the end of this course you will be able to: 1. Define the term constipation 2. Explain three reasons why older adults are at greater risk for constipation
Chronic constipation in the elderly
 Chronic constipation in the elderly 1 Dec,2011 R 2 Natta Asanaleykha Epidemiology Definition Scope The impact of chronic constipation in the elderly Pathophysiology Evaluation the elderly patient with
Chronic constipation in the elderly 1 Dec,2011 R 2 Natta Asanaleykha Epidemiology Definition Scope The impact of chronic constipation in the elderly Pathophysiology Evaluation the elderly patient with
Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate.
 NAME OF THE MEDICINE KLYX Enema Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate Sorbitol C20H37NaO7S MW: 444.56 CAS no: 577-11-7
NAME OF THE MEDICINE KLYX Enema Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate Sorbitol C20H37NaO7S MW: 444.56 CAS no: 577-11-7
Protectives and Adsorbents. Inorganic chemistry Course 1 Third year Assist. Lecturer Ahlam A. Shafeeq MSc. Pharmaceutical chemistry
 Protectives and Adsorbents Inorganic chemistry Course 1 Third year 2016-2017 Assist. Lecturer Ahlam A. Shafeeq MSc. Pharmaceutical chemistry Protectives and Adsorbents This group of gastrointestinal agents
Protectives and Adsorbents Inorganic chemistry Course 1 Third year 2016-2017 Assist. Lecturer Ahlam A. Shafeeq MSc. Pharmaceutical chemistry Protectives and Adsorbents This group of gastrointestinal agents
What Is Constipation?
 CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
Efficacy and Safety of Lubiprostone. Laura Wozniak February 23, 2010 K30 Monthly Journal Club
 Efficacy and Safety of Lubiprostone Laura Wozniak February 23, 2010 K30 Monthly Journal Club Objectives Brief overview of constipation Review of article Discussion Constipation in Children 3-5% of all
Efficacy and Safety of Lubiprostone Laura Wozniak February 23, 2010 K30 Monthly Journal Club Objectives Brief overview of constipation Review of article Discussion Constipation in Children 3-5% of all
15. Prevention of UTI and lifestyle modifications
 15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
Non-Reversed Appendicostomy for Antegrade Continence Enema in the Treatment of Encopresis
 Original Article Annals of Pediatric Surgery Vol. 6, No 3,4 July, October 2010, PP 144-149 Non-Reversed Appendicostomy for Antegrade Continence Enema in the Treatment of Encopresis Kamal Abdel-Elah, Basem
Original Article Annals of Pediatric Surgery Vol. 6, No 3,4 July, October 2010, PP 144-149 Non-Reversed Appendicostomy for Antegrade Continence Enema in the Treatment of Encopresis Kamal Abdel-Elah, Basem
A patient s guide to the. management of constipation following surgery
 A patient s guide to the management of constipation following surgery This leaflet has been designed to give you more information about using laxatives after your surgery. What is constipation? After your
A patient s guide to the management of constipation following surgery This leaflet has been designed to give you more information about using laxatives after your surgery. What is constipation? After your
Constipation in children usually is functional (ie, constipation
 Efficacy and Complications of Polyethylene Glycols for Treatment of Constipation in Children A Meta-Analysis Si-Le Chen, MD, Shi-Rong Cai, MD, PhD, Liang Deng, MD, Xin-Hua Zhang, MD, PhD, Te-Dong Luo,
Efficacy and Complications of Polyethylene Glycols for Treatment of Constipation in Children A Meta-Analysis Si-Le Chen, MD, Shi-Rong Cai, MD, PhD, Liang Deng, MD, Xin-Hua Zhang, MD, PhD, Te-Dong Luo,
C onstipation is a common problem in children, accounting
 723 ORIGINAL ARTICLE Prognosis of constipation: clinical factors and colonic transit time F de Lorijn, M P van Wijk, J B Reitsma, R van Ginkel, J A J M Taminiau, M A Benninga... See end of article for
723 ORIGINAL ARTICLE Prognosis of constipation: clinical factors and colonic transit time F de Lorijn, M P van Wijk, J B Reitsma, R van Ginkel, J A J M Taminiau, M A Benninga... See end of article for
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) Behavioral therapy for functional constipation in childhood: health-related quality of life, emotional and behavior problems & parental child-rearing attitudes van
UvA-DARE (Digital Academic Repository) Behavioral therapy for functional constipation in childhood: health-related quality of life, emotional and behavior problems & parental child-rearing attitudes van
Chronic Childhood Constipation Is Associated with Impaired Quality of Life: A Case-Controlled Study
 Journal of Pediatric Gastroenterology and Nutrition 41:56 60 Ó July 2005 Lippincott Williams & Wilkins, Philadelphia Chronic Childhood Constipation Is Associated with Impaired Quality of Life: A Case-Controlled
Journal of Pediatric Gastroenterology and Nutrition 41:56 60 Ó July 2005 Lippincott Williams & Wilkins, Philadelphia Chronic Childhood Constipation Is Associated with Impaired Quality of Life: A Case-Controlled
Management of the Neurogenic Bowel. June st National SBAA Conference Bloomington, Minnesota
 Management of the Neurogenic Bowel June 2016 41st National SBAA Conference Bloomington, Minnesota DEPARTMENT OF NURSING Rhonda Bolin, BSN, RN, CPN Spina Bifida Nurse Texas Children s Hospital Spina Bifida
Management of the Neurogenic Bowel June 2016 41st National SBAA Conference Bloomington, Minnesota DEPARTMENT OF NURSING Rhonda Bolin, BSN, RN, CPN Spina Bifida Nurse Texas Children s Hospital Spina Bifida
Randomised controlled trial of biofeedback training in persistent encopresis with anismus
 Arch Dis Child 1998;79:131 135 131 Clinical Epidemiology and Biostatistics Unit, Melbourne University Department of Paediatrics, Royal Children s Hospital, Parkville Victoria, Australia 3052 T Nolan Department
Arch Dis Child 1998;79:131 135 131 Clinical Epidemiology and Biostatistics Unit, Melbourne University Department of Paediatrics, Royal Children s Hospital, Parkville Victoria, Australia 3052 T Nolan Department
Primary Care Constipation Guidelines. Version 1 November 2016
 Primary Care Constipation Guidelines Version 1 November 2016 VERSION CONTROL Version Date Amendments made Version 1 November 2016 New guideline Contents 1. Management of constipation in adults: acute and
Primary Care Constipation Guidelines Version 1 November 2016 VERSION CONTROL Version Date Amendments made Version 1 November 2016 New guideline Contents 1. Management of constipation in adults: acute and
Understanding & Alleviating Constipation. Living (Well!) with Gastroparesis Program Warm-Up Class
 Understanding & Alleviating Constipation Living (Well!) with Gastroparesis Program Warm-Up Class Please Remember The information presented is for educational purposes only and is in no way intended as
Understanding & Alleviating Constipation Living (Well!) with Gastroparesis Program Warm-Up Class Please Remember The information presented is for educational purposes only and is in no way intended as
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) Behavioral therapy for functional constipation in childhood: health-related quality of life, emotional and behavior problems & parental child-rearing attitudes van
UvA-DARE (Digital Academic Repository) Behavioral therapy for functional constipation in childhood: health-related quality of life, emotional and behavior problems & parental child-rearing attitudes van
Constipation An Overview. Definition Physiology of GI tract Etiology Assessment Treatment
 CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
Constipation: Treatment of Chronic Constipation and Soiling
 Patient and Family Education Constipation: Treatment of Chronic Constipation and Soiling While it is normal for a child to be constipated now and then, ongoing problems are not. This handout gives a treatment
Patient and Family Education Constipation: Treatment of Chronic Constipation and Soiling While it is normal for a child to be constipated now and then, ongoing problems are not. This handout gives a treatment
Efficacy of a mixture of probiotic agents as complementary therapy for chronic functional constipation in childhood
 Russo et al. Italian Journal of Pediatrics (2017) 43:24 DOI 10.1186/s13052-017-0334-3 RESEARCH Open Access Efficacy of a mixture of probiotic agents as complementary therapy for chronic functional constipation
Russo et al. Italian Journal of Pediatrics (2017) 43:24 DOI 10.1186/s13052-017-0334-3 RESEARCH Open Access Efficacy of a mixture of probiotic agents as complementary therapy for chronic functional constipation
Drugs Affecting the Gastrointestinal System. Antidiarrheal and Laxatives
 Drugs Affecting the Gastrointestinal System Antidiarrheal and Laxatives Diarrhea Abnormal frequent passage of loose stools or Abnormal passage of stools with increased frequency, fluidity, and weight,
Drugs Affecting the Gastrointestinal System Antidiarrheal and Laxatives Diarrhea Abnormal frequent passage of loose stools or Abnormal passage of stools with increased frequency, fluidity, and weight,
Empirically Supported Treatments in Pediatric Psychology: Constipation and Encopresis
 Journal of Pediatric Psychology, Vol. 25, No. 4, 2000, pp. 225 254 Empirically Supported Treatments in Pediatric Psychology: Constipation and Encopresis Melanie L. McGrath, 1 PhD, Michael W. Mellon, 2
Journal of Pediatric Psychology, Vol. 25, No. 4, 2000, pp. 225 254 Empirically Supported Treatments in Pediatric Psychology: Constipation and Encopresis Melanie L. McGrath, 1 PhD, Michael W. Mellon, 2
Identify electrolytes that should be monitored whenever prolonged or severe diarrhea is present
 Chapter 35 Drugs Used to Treat Constipation and Diarrhea Learning Objectives State the underlying causes of constipation Explain the meaning of normal bowel habits Cite nine causes of diarrhea Describe
Chapter 35 Drugs Used to Treat Constipation and Diarrhea Learning Objectives State the underlying causes of constipation Explain the meaning of normal bowel habits Cite nine causes of diarrhea Describe
Constipation in early childhood: patient characteristics, treatment, and longterm follow up
 1400 Gut 1993; 34:1400-1404 Constipation in early childhood: patient characteristics, treatment, and longterm follow up Department of Pediatrics, University of Iowa, USA V Loening-Baucke Correspondence
1400 Gut 1993; 34:1400-1404 Constipation in early childhood: patient characteristics, treatment, and longterm follow up Department of Pediatrics, University of Iowa, USA V Loening-Baucke Correspondence
CENTENE PHARMACY AND THERAPEUTICS DRUG REVIEW 3Q17 July August
 BRAND NAME Symproic GENERIC NAME Naldemedine MANUFACTURER Shionogi Inc. DATE OF APPROVAL March 23, 2017 PRODUCT LAUNCH DATE Anticipated to launch mid-summer 2017 REVIEW TYPE Review type 1 (RT1): New Drug
BRAND NAME Symproic GENERIC NAME Naldemedine MANUFACTURER Shionogi Inc. DATE OF APPROVAL March 23, 2017 PRODUCT LAUNCH DATE Anticipated to launch mid-summer 2017 REVIEW TYPE Review type 1 (RT1): New Drug
OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA
 OMED 17 OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA 29.5 Category 1-A CME credits anticipated ACOFP / AOA s 122 nd Annual Osteopathic Medical Conference & Exposition Joint Session with ACOFP and Cleveland
OMED 17 OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA 29.5 Category 1-A CME credits anticipated ACOFP / AOA s 122 nd Annual Osteopathic Medical Conference & Exposition Joint Session with ACOFP and Cleveland
Are you aware there are many different reasons for having irregular bowels? This chart is to help you get back into balance during and post detox.
 BRISTOL POOP CHART The Bristol Poop Chart was created in the United Kingdom by a group of gastroenterologists at the University of Bristol. This chart is designed to help you determine the health of your
BRISTOL POOP CHART The Bristol Poop Chart was created in the United Kingdom by a group of gastroenterologists at the University of Bristol. This chart is designed to help you determine the health of your
IPS Childhood Constipation when we refer to Ped.Gastroenterologist? Dr.Muath Al Turaiki. Consultant of Pediatric Gastroenterology, K.S.
 Childhood Constipation when we refer to Ped.Gastroenterologist? Dr.Muath Al Turaiki Consultant of Pediatric Gastroenterology, K.S.H Dubai 22-24 Feb. 2018 Objectives: Why constipation?!!! Is it a burden
Childhood Constipation when we refer to Ped.Gastroenterologist? Dr.Muath Al Turaiki Consultant of Pediatric Gastroenterology, K.S.H Dubai 22-24 Feb. 2018 Objectives: Why constipation?!!! Is it a burden
Unraveling childhood constipation: Pathophysiology, diagnostics and treatment Mugie, S.M.
 UvA-DARE (Digital Academic Repository) Unraveling childhood constipation: Pathophysiology, diagnostics and treatment Mugie, S.M. Link to publication Citation for published version (APA): Mugie, S. M. (2014).
UvA-DARE (Digital Academic Repository) Unraveling childhood constipation: Pathophysiology, diagnostics and treatment Mugie, S.M. Link to publication Citation for published version (APA): Mugie, S. M. (2014).
SYMPROIC (naldemedine tosylate) oral capsule
 SYMPROIC (naldemedine tosylate) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
SYMPROIC (naldemedine tosylate) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
A Nursing Assessment Tool for Adults With Fecal Incontinence
 Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Diagnostic dilemmas and results of treatment for
 36 Department of Paediatrics, Free University Hospital, PO Box 757, 17 MB Amsterdam, The Netherlands CW Keuzenkamp-Jansen CJ Fijnvandraat CMF Kneepkens AC Douwes Correspondence and reprint requests to:
36 Department of Paediatrics, Free University Hospital, PO Box 757, 17 MB Amsterdam, The Netherlands CW Keuzenkamp-Jansen CJ Fijnvandraat CMF Kneepkens AC Douwes Correspondence and reprint requests to:
Common Gastrointestinal Problems in the Elderly
 Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
Xifaxan, Lotronex and Viberzi Prior Authorization and Quantity Limit Program Summary
 Xifaxan, Lotronex and Viberzi Prior Authorization and Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Lotronex (alosetron) a Indication For women with severe diarrheapredominant irritable
Xifaxan, Lotronex and Viberzi Prior Authorization and Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Lotronex (alosetron) a Indication For women with severe diarrheapredominant irritable
Authors and Disclosures
 Role of Carbon Dioxide-Releasing Suppositories in the Treatment of Chronic Functional Constipation A Double-Blind, Randomised, Placebo-Controlled Trial M. Lazzaroni; V. Casini; G. Bianchi Porro Authors
Role of Carbon Dioxide-Releasing Suppositories in the Treatment of Chronic Functional Constipation A Double-Blind, Randomised, Placebo-Controlled Trial M. Lazzaroni; V. Casini; G. Bianchi Porro Authors
MANAGING CONSTIPATION
 MANAGING CONSTIPATION INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Constipation is. The Symptoms of Constipation. How to Help Manage Constipation. WHAT IS CONSTIPATION?
MANAGING CONSTIPATION INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Constipation is. The Symptoms of Constipation. How to Help Manage Constipation. WHAT IS CONSTIPATION?
Children s Hospital of Pittsburgh Continuity Clinic Curriculum Week of April 10, Nader Shaikh, MD, MPH
 Children s Hospital of Pittsburgh Continuity Clinic Curriculum Week of April 10, 2017 Nader Shaikh, MD, MPH Topic: Toileting: Constipation and Fecal Incontinence Learning Objectives: At the end of this
Children s Hospital of Pittsburgh Continuity Clinic Curriculum Week of April 10, 2017 Nader Shaikh, MD, MPH Topic: Toileting: Constipation and Fecal Incontinence Learning Objectives: At the end of this
Continence/Constipation Workshop for RNs in Long-Term Care
 Continence/Constipation Workshop for RNs in Long-Term Care Slide Presentation Supporting Implementation of the RNAO BPGs: Promoting Continence Using Prompted Voiding and Prevention of Constipation in the
Continence/Constipation Workshop for RNs in Long-Term Care Slide Presentation Supporting Implementation of the RNAO BPGs: Promoting Continence Using Prompted Voiding and Prevention of Constipation in the
Children s Hospital of Pittsburgh Continuity Clinic Curriculum Week of April 10, Nader Shaikh, MD, MPH
 Children s Hospital of Pittsburgh Continuity Clinic Curriculum Week of April 10, 2017 Nader Shaikh, MD, MPH Topic: Toileting: Constipation and Fecal Incontinence Learning Objectives: At the end of this
Children s Hospital of Pittsburgh Continuity Clinic Curriculum Week of April 10, 2017 Nader Shaikh, MD, MPH Topic: Toileting: Constipation and Fecal Incontinence Learning Objectives: At the end of this
Constipation. Disease Review
 bowel. 1 Constipation is a symptom, not a disease. Almost everyone experiences Disease Review Constipation Introduction: Constipation is exceedingly common and is rarely associated with mortality in developed
bowel. 1 Constipation is a symptom, not a disease. Almost everyone experiences Disease Review Constipation Introduction: Constipation is exceedingly common and is rarely associated with mortality in developed
Management of childhood constipation
 J Pediatr Rev. 2013;1(1)45-51 Management of childhood constipation Hassan Karami 1 Leila Shokohi 2* 1 Department of Pediatric Gastroenterology, Faculty of Medicine, Mazandaran University of Medical Sciences,Sari,
J Pediatr Rev. 2013;1(1)45-51 Management of childhood constipation Hassan Karami 1 Leila Shokohi 2* 1 Department of Pediatric Gastroenterology, Faculty of Medicine, Mazandaran University of Medical Sciences,Sari,
Childhood constipation
 Follow the link from the online version of this article to obtain certified continuing medical education credits Childhood constipation Marcus K H Auth, Rakesh Vora, Paul Farrelly, Colin Baillie Departments
Follow the link from the online version of this article to obtain certified continuing medical education credits Childhood constipation Marcus K H Auth, Rakesh Vora, Paul Farrelly, Colin Baillie Departments
MOVICOL Junior Chocolate Flavour Powder for Solution (macrogol 3350)
 MOVICOL Junior Chocolate Flavour Powder for Solution (macrogol 3350) Product Name: MOVICOL Junior Chocolate Flavour Product Description: Each sachet of MOVICOL Junior Chocolate contains: Macrogol 3350
MOVICOL Junior Chocolate Flavour Powder for Solution (macrogol 3350) Product Name: MOVICOL Junior Chocolate Flavour Product Description: Each sachet of MOVICOL Junior Chocolate contains: Macrogol 3350
190 Index Case studies, abdominal pain, 2 Crohn s disease, 2 3, cyclic vomiting syndrome (CVS), 2 fecal incontinence (FI), 2 medical c
 Index Abdominal pain, case study, 2 Achalasia, 75 Acupuncture 108 American Academy of Pediatrics, 49 Anxiety, 8 9, 98 Autism, GI disorders and, 25 27 BASC. See Behavior Assessment System for Children (BASC)
Index Abdominal pain, case study, 2 Achalasia, 75 Acupuncture 108 American Academy of Pediatrics, 49 Anxiety, 8 9, 98 Autism, GI disorders and, 25 27 BASC. See Behavior Assessment System for Children (BASC)
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES
 OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
Is one of the most common chronic disorders. causing patients to seek medical treatment.
 ILOs After this lecture you should be able to : Define IBS Identify causes and risk factors of IBS Determine the appropriate therapeutic options for IBS Is one of the most common chronic disorders causing
ILOs After this lecture you should be able to : Define IBS Identify causes and risk factors of IBS Determine the appropriate therapeutic options for IBS Is one of the most common chronic disorders causing
Constipation Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.uk
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
Approaching Childhood Constipation Anees Siddiqui, MD Pediatric Gastroenterology. Disclosure. Learning Objectives. Epidemiology.
 Approaching Childhood Constipation p Anees Siddiqui, MD Pediatric Gastroenterology Disclosure Anees Siddiqui, MD, has no relationships with commercial companies to disclose. Specially for Children Dell
Approaching Childhood Constipation p Anees Siddiqui, MD Pediatric Gastroenterology Disclosure Anees Siddiqui, MD, has no relationships with commercial companies to disclose. Specially for Children Dell
Unraveling childhood constipation: Pathophysiology, diagnostics and treatment Mugie, S.M.
 UvA-DARE (Digital Academic Repository) Unraveling childhood constipation: Pathophysiology, diagnostics and treatment Mugie, S.M. Link to publication Citation for published version (APA): Mugie, S. M. (2014).
UvA-DARE (Digital Academic Repository) Unraveling childhood constipation: Pathophysiology, diagnostics and treatment Mugie, S.M. Link to publication Citation for published version (APA): Mugie, S. M. (2014).
Comparison of strategies and goals for treatment of chronic constipation among gastroenterologists and general practitioners
 ORIGINAL ARTICLE Annals of Gastroenterology (18) 31, 1-6 Comparison of strategies and goals for treatment of chronic constipation among gastroenterologists and general practitioners Dan Carter a,c, Eytan
ORIGINAL ARTICLE Annals of Gastroenterology (18) 31, 1-6 Comparison of strategies and goals for treatment of chronic constipation among gastroenterologists and general practitioners Dan Carter a,c, Eytan
The Digestive System or tract extends from the mouth to the anus.
 The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
UNDERSTANDING IBS AND CC Implications for diagnosis and management
 UNDERSTANDING IBS AND CC Implications for diagnosis and management J. TACK, M.D., Ph.D. Department of Gastroenterology University Hospitals, K.U. Leuven Leuven, Belgium TYPES OF GASTROINTESTINAL DISORDERS
UNDERSTANDING IBS AND CC Implications for diagnosis and management J. TACK, M.D., Ph.D. Department of Gastroenterology University Hospitals, K.U. Leuven Leuven, Belgium TYPES OF GASTROINTESTINAL DISORDERS
Functional constipation in children: which treatment is effective and safe? An evidence-based case report
 Functional constipation in children: which treatment is effective and safe? An evidence-based case report 1. Private practice, Quebec, Canada. Email: nathaelle@chirostmartin.com By Nathaëlle Martin-Marcotte,
Functional constipation in children: which treatment is effective and safe? An evidence-based case report 1. Private practice, Quebec, Canada. Email: nathaelle@chirostmartin.com By Nathaëlle Martin-Marcotte,
daily; available as 10- mg g PO
 Overview of the PRN: The Pain and Palliative Care PRN of ACCP is an organization of pharmacy practitioners, clinical scientists, pharmacy educators, and others. Its mission is to advance pain and palliative
Overview of the PRN: The Pain and Palliative Care PRN of ACCP is an organization of pharmacy practitioners, clinical scientists, pharmacy educators, and others. Its mission is to advance pain and palliative
Childhood constipation: new insights in testing, treatment and cost Liem, O.
 UvA-DARE (Digital Academic Repository) Childhood constipation: new insights in testing, treatment and cost Liem, O. Link to publication Citation for published version (APA): Liem, O. (2010). Childhood
UvA-DARE (Digital Academic Repository) Childhood constipation: new insights in testing, treatment and cost Liem, O. Link to publication Citation for published version (APA): Liem, O. (2010). Childhood
Anorectal Diagnostic Overview
 Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Short Bowel Syndrome: Medical management
 Short Bowel Syndrome: Medical management La Sindrome dell'intestino Corto in età pediatrica Brescia 18 marzo 2011 Jon A.Vanderhoof, M.D. Division of Pediatric GI Harvard Medical School Children s Hospital,
Short Bowel Syndrome: Medical management La Sindrome dell'intestino Corto in età pediatrica Brescia 18 marzo 2011 Jon A.Vanderhoof, M.D. Division of Pediatric GI Harvard Medical School Children s Hospital,
1. What evidence exists that prevention of constipation in the first year of life improves outcome of bowel management in later childhood?
 BOWEL FUNCTION AND CARE Overall Outcomes Primary Outcomes o Maintenance of social continence as appropriate for age level Secondary Outcomes o Maximization of independence with managing bowel program o
BOWEL FUNCTION AND CARE Overall Outcomes Primary Outcomes o Maintenance of social continence as appropriate for age level Secondary Outcomes o Maximization of independence with managing bowel program o
Populations Interventions Comparators Outcomes Individuals: With fecal incontinence
 Protocol Biofeedback as a Treatment of Fecal Incontinence or Constipation (20164) Medical Benefit Effective Date: 07/01/13 Next Review Date: 03/19 Preauthorization No Review Dates: 09/07, 09/08, 09/09,
Protocol Biofeedback as a Treatment of Fecal Incontinence or Constipation (20164) Medical Benefit Effective Date: 07/01/13 Next Review Date: 03/19 Preauthorization No Review Dates: 09/07, 09/08, 09/09,
Children s Hospital Of Wisconsin
 Children s Hospital Of Wisconsin Co-Management Guidelines To support collaborative care, we have developed guidelines for our community providers to utilize when referring to, and managing patients with,
Children s Hospital Of Wisconsin Co-Management Guidelines To support collaborative care, we have developed guidelines for our community providers to utilize when referring to, and managing patients with,
MOVICOL Junior Powder for Solution (macrogol 3350)
 MOVICOL Junior Powder for Solution (macrogol 3350) Product Name: MOVICOL Junior Product Description: Each sachet of MOVICOL Junior contains: Macrogol 3350 Sodium chloride Sodium bicarbonate Potassium chloride
MOVICOL Junior Powder for Solution (macrogol 3350) Product Name: MOVICOL Junior Product Description: Each sachet of MOVICOL Junior contains: Macrogol 3350 Sodium chloride Sodium bicarbonate Potassium chloride
Clinical guideline Published: 26 May 2010 nice.org.uk/guidance/cg99
 Constipation in children and young people: diagnosis and management Clinical guideline Published: 26 May 2010 nice.org.uk/guidance/cg99 NICE 2019. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Constipation in children and young people: diagnosis and management Clinical guideline Published: 26 May 2010 nice.org.uk/guidance/cg99 NICE 2019. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Chapter 19. Assisting With Bowel Elimination. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 19 Assisting With Bowel Elimination Normal Bowel Elimination Time and frequency of bowel movements (BMs) vary. To assist with bowel elimination, you need to know these terms: Defecation is the
Chapter 19 Assisting With Bowel Elimination Normal Bowel Elimination Time and frequency of bowel movements (BMs) vary. To assist with bowel elimination, you need to know these terms: Defecation is the
ACG Clinical Guideline: Management of Benign Anorectal Disorders
 ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
MOVICOL HALF PI December MOVICOL-Half. Powder for Solution (macrogol 3350) Potassium 5.4 mmol/l. Bicarbonate 17 mmol/l
 MOVICOL -Half Powder for Solution (macrogol 3350) Product Name: Product Description: MOVICOL-Half Each sachet of MOVICOL-Half contains: Macrogol 3350 6.563 g Sodium chloride 175.4 mg Sodium bicarbonate
MOVICOL -Half Powder for Solution (macrogol 3350) Product Name: Product Description: MOVICOL-Half Each sachet of MOVICOL-Half contains: Macrogol 3350 6.563 g Sodium chloride 175.4 mg Sodium bicarbonate
Chapter 5 Gastroenterology. Dose. Route. Units. Given. Dose. Route. Units. Given
 Chapter 5 Gastroenterology Georgia Woodfield TERLIPRESSIN CIPROFLOXACIN 2 initial dose 500 Every 4 hours until bleeding controlled can be reduced to 1 after initial dose if side effects develop or if patient
Chapter 5 Gastroenterology Georgia Woodfield TERLIPRESSIN CIPROFLOXACIN 2 initial dose 500 Every 4 hours until bleeding controlled can be reduced to 1 after initial dose if side effects develop or if patient
Long-Term Bowel Symptoms Following Corrective Surgery
 HIRSCHSPRUNG'S DISEASE Samuel Nurko MD MPH Center for Motility and Functional Gastrointestinal Disorders Children s Hospital Medical Center, Boston Ma Long-Term Bowel Symptoms Following Corrective Surgery
HIRSCHSPRUNG'S DISEASE Samuel Nurko MD MPH Center for Motility and Functional Gastrointestinal Disorders Children s Hospital Medical Center, Boston Ma Long-Term Bowel Symptoms Following Corrective Surgery
There are clues to help to decide if the bellyache is a medical problem:
 Bellyaches in Children Pediatric and Adolescent Gastrointestinal Motility & Pain Program Department of Pediatrics, Louisiana State University Health Sciences Center, New Orleans, Louisiana By: Paul Hyman,
Bellyaches in Children Pediatric and Adolescent Gastrointestinal Motility & Pain Program Department of Pediatrics, Louisiana State University Health Sciences Center, New Orleans, Louisiana By: Paul Hyman,
