Reliable Routes For 100% Caudal Anesthesia in Adults.
|
|
|
- Albert Claude Reynolds
- 6 years ago
- Views:
Transcription
1 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: , p-issn: Volume 13, Issue 11 Ver. IV (Nov. 2014), PP Reliable Routes For 100% Caudal Anesthesia in Adults. Radhashyam Paria Abstract: Background: The usefulness of the adult caudal anesthesia is worldwide acceptable in lower limb surgeries. Adult caudal anesthesia through the hiatus provides maximal hemodynamic stability with profound postoperative analgesia, although, anatomical distortion of the sacral hiatus in elderly persons handicapped this technique. Aims: The study is scheduled to find out ways to overcome the obstruction to get the access to sacral epidural space in adult life. Methods: 30 (thirty) elderly patients for lower limbs surgeries were recruited for the study, and it was planned to attempt all patients for caudal anesthesia firstly through the sacral hiatus, next through the sacral foramens in previously unsuccessful cases and lastly through the drilling hole on the sacral hiatus in failed cases by previous two methods. The caudal anesthesia in all cases was administered by deposition of 25 ml of 0.5% ropivacaine with help of a nerve stimulator needle after local infiltration with 6 ml of 1% injection xylocaine. Results: Only 5 cases out of 30 patients (16.6%) were successfully administered caudal anesthesia through the sacral hiatus. 20 patients out of 25 cases (80%) were successfully administered caudal anesthesia through dorsal foramen of sacrum. Lastly five patients out of 5 cases (100%) were successfully administered caudal anesthesia through drilling hole on sacral hiatus. Conclusion: Caudal anesthesia is possible in 100% elderly patients either through sacral hiatus or through its dorsal foramen of sacrum or through the drilling hole over sacral hiatus. It is exclusively one of the best techniques of anesthesia for the lower limbs surgeries. Key words: Drilling holes, sacral hiatus, dorsal foramen, nerve stimulating needle, Sacral canal I. Introduction: The motor and sensory activities of lower limbs depend on lumbosacral nerve roots of the spinal cord [L5 to S5]. The segmental block of these spinal roots [L5-S5] produces motor and sensory block of lower limbs. The sympathetic outflow, extending from tenth thoracic to second lumbar spinal segment [T10 to L2] are responsible for maintaining hemodynamic status of lower limbs. The segmental block of lumbosacral spinal nerve roots may be capable of producing the anesthesia of lower limbs for their projected surgeries from hip to toe. Introduction of caudal anesthesia in 1901 by Sicard and Cathelin1 contributed the segmental block of lumbosacral spinal nerve roots in adults with hemodynamic stability during lower limbs surgery. It became highly popular. But such popularity of caudal declined with the introduction of lumbar epidural in 1921 by Page and in 1927 by Dogliotti.[1 ]This declination was further enhanced by anatomical distortion of the sacral hiatus in adult life and absence of the sacral hiatus in 7.7% of population.2 Consequently, introduction of sacral spinal anesthesia3and sacral saddle block4 through its dorsal foramen promoted to introduce the sacral epidural5 through its dorsal foramen although, it is not appropriate to all cases with 100% success rate. Thereafter, introduction of caudal through the drilling hole on sacral hiatus with help of nerve stimulator needle6 solved all the problems in relation to adult caudal anesthesia. We designed our study to evaluate the advantages and disadvantages of caudal through its different ways like a) hiatus; b) foramen and c) drilling hole on hiatus. II. Method: We received the approval of Medical Ethical Review Board and written informed consent for procedure and study. We recruited 30(Thirty) patients, belonging to ASA class 1 and 11 for surgeries of lower limb under unilateral sacral epidural anesthesia. All participants signed their consents after full explanation about the expected benefits and results, side effects and complications of the technique of sacral epidural through its dorsal foramens. Every participant was subjected to preoperative visit to exclude the contraindication of the proposed procedure. In the O.T, peripheral infusion and non invasive monitoring were started. Anatomical landmarks were identified. We identified the spinous process of fourth lumbar vertebra (L4) and tip of coccyx. Next, we located the mid-point of above two landmarks as third sacral vertebra (S3). The first sacral vertebra (S1) was located as mid-point of L4 and S3. The second sacral vertebra (S2) was found at the mid-point between S1 and 35 Page
2 S3. The spinous processes of S1 and S2 are found approximately 2.5 cm apart, and their respective foramina lie 1.5 cm caudal and lateral to them. Similarly, S3 foramina lie 1.5 cm caudal and lateral to S3 vertebra. After identification of S1, S2 and S3 foramina, aseptic preparation was done in the lateral position of patients.the patient was kept on the surgical side downward on the operation table, and selected foramens were infiltrated with 6ml of 1% injection lignocaine. We inserted the nerve stimulator need [13] (0.8 mm x 100 mm 21G Stimuplex A100 needle/ BBraun) through any of the three dorsal foramens selected beforehand. The needle was advanced perpendicularly like sacral spinal anesthesia [14, 15] until it contracted with bone. The depth of needle was noted from grazed nerve stimulator needle..the needle was withdrawn a little and again redirected 40 degrees to the foramen until it entered the foramen and crossed the intervertebral foramen evidenced with movement of great toe on the same side. Thus, we placed the needle correctly in the sacral epidural space. This was also further confirmed by loss of resistance and absence of cerebrospinal fluid (CSF) and blood in the needle. After confirmation of needle placement in sacral epidural space, 25 ml of 0.5% Ropivacaine was injected through the needle (2.5ml / segment of the vertebra) [17]. The patient was kept on the same position for another ten minutes and after which patient was turned to the supine position. Surgeons were allowed to operate after eliciting sensory block height suitable for proposed surgery. Another leg was examined to certain the involvement. Heart rate, blood pressure, respiration, and oxygen concentration were recorded every three minutes for first ten minutes after which taken at every ten minutes interval. In the case of lower limb surgery upper level of sensory block was assessed by pinprick and motor block by modified Bromage scale which is as follows: 0 = lifting up extended leg, 1= flexed knee with full ankle movement, 2 =No knee movement, partial ankle movement, 3 = complete paralysis. We also recorded the onset time of sensory and motor block as the time gap between the epidural injection and bilateral loss of sensation and loss of motor activity of the lower limbs respectively. Similarly, we calculated the duration of the sensory and motor block and sent all collected data for statistical analysis using Graphpad Prism 5. III. Result: 30 (Thirty) patients were attempted for caudal anesthesia at first through the sacral hiatus. Only 5 (five) patients out of 30 (16.33%) were successfully administered caudal anesthesia through sacral hiatus. The rest 25 (twenty-five) patients were tried for caudal through the dorsal foramens of sacrum. 20 (twenty) patients out of 25 (twenty-five) patients (80%) were successfully administered caudal through dorsal foramens of sacrum with help of nerve stimulator needle. Last 5 (five) patients out of five patients (100%) were successfully administered caudal anesthesia through drilling hole on the sacral hiatus with help of nerve stimulator needle. All cases of caudal anesthesia were conducted with nerve stimulator needle, and a contiflex catheter kept behind in the sacral epidural space. The sensory block extended to 12th thoracic dermatome to allow the lower limbs surgeries. Motor block of both limbs developed and continued further with the help of contiplex catheter. Local anesthetic was administered through this catheter to provide postoperative analgesia. No intravenous sedative or analgesic as adjuvants was used. Thirty patients underwent orthopedic surgeries, including open reduction of hip, limb fracture, amputation and knee joint. All patients showed hemodynamic stability throughout the intraoperative period. Their hemodynamic profile is cited in table no 1. Similarly, demographic profile and nerve block profile are also placed in the table no 1. All patients were followed for three days after operation. No patient developed sacral neuralgia, postdural puncture headache and incidence of visceral perforation. IV. Discussion The motor and sensory activities of lower limbs depend on lumbosacral roots of the spinal cord extending from first lumbar spinal segment to fifth sacral spinal segments (L1 to S5). Its sympathetic supply depends on neurones in the lateral horn of the lower three thoracic (T10, T11 and T12) and upper two lumbar (L1 L2) spinal cord segments. These sympathetic outflows are responsible to control the hemodynamic status of lower limbs. The limited cephalic extension up to the twelve thoracic spinal segments in the sacral epidural provides hemodynamic stability. The segmental block of lumbosacral spinal nerve roots is capable of producing the lower limbs anesthesia for projected surgery on lower limbs. The blocking of the lumbosacral segment, extending from L1 to S5 is an essential component for lower limbs surgery. The way to block the lumbosacral spinal nerve roots is comprehensively accepted as caudal anesthesia. It is an appropriate and accurate technique of anesthesia to provide anesthesia on the lower limbs with less involvement of sympathetic outflow for the same area. Introduction of the first epidural anesthesia in 1901 by Sicard and Cathelin1 became popular as adult caudal anesthesia. Its usefulness as segmental block for lumbosacral spinal nerve roots is worldwide acceptable. But, such popularity of caudal declined with the introduction of lumbar epidural in 1921 by Page and in 1927 by 36 Page
3 Dogliotti.1]. This declination was further enhanced by anatomical distortion of the sacral hiatus in adult life and absence of the sacral hiatus in 7.7% of population.2 Successful administration of caudal anesthesia is dependent on the presence of the sacral hiatus that is the end of the sacral canal and covered by sacrococcygeal ligament. Penetration of this ligament leads to sacral epidural space and successful administration of caudal anesthesia. Easy availability of sacral epidural space is associated with lower age group, but, with the advancement of age, anatomical distortion of the sacral hiatus leads to unsuccessful caudal anesthesia. The bony overgrowth over sacral hiatus along with soft tissue is the main cause of anatomical distortion of the sacral hiatus. The calcification of sacrococcygeal ligament and also obliteration of dorsal foramens of sacrum are frequently accompanied with the disease process of Ankylosis Spondylitis. Thus, penetration of the needle through the sacral hiatus becomes impossible. Different variations of the sacral hiatus frequently mislead to detect the landmarks of the sacral hiatus and enhance the occurrences of failed caudal anesthesia. The longitudinal slit hiatus and second midline hiatus definitively offer difficulty to penetrate its posterior wall. Transverse hiatus and large hiatus without cornua make difficult to locate the position. The transverse hiatus with absent coccyx and two prominent cornua, with two proximal decoy hiatuses lateral two cornua abolishes its usual landmarks. Large midline defects in posterior sacral wall continuous with sacral hiatus and enlarged longitudinal hiatuses with overlying decoy hiatus may lead needle insertion through the ligament, but not into the sacral canal. Anyhow, any abnormal form of the sacral hiatus grossly misleads the successful penetration of the needle to sacral canal. [1] Subsequent introduction of lumbar epidural in 1921 by Page and in 1927 by Dogliotti appeared like a good alternative of caudal anesthesia. Later on, it became partially responsible for declination of initial popularity, gained by caudal just after its practical application. But, later on, lumbar epidural was criticized about its successful involvement of fifth lumbar and first sacral nerve roots. Owing to extensive cranial spread and less caudal spread [7], lumbar epidural is frequently incapable of contributing complete block of fifth lumbar (L5) and first sacral (S1) spinal segment [8] for their variable nerve size[9]. Such occurrence does not take place in caudal anesthesia, as local anesthetic, deposited in sacral epidural space, spreads only towards cephalad direction and avails enough scope to immerge the nerve roots within local anesthetic drug. Recent introduction of sacral epidural anesthesia [5] through its dorsal foramens with the help of nerve stimulator needle is capable of bye-passing the anatomical distortion of the sacral hiatus and helps to achieve caudal anesthesia. The clinical manifestations of this technique are similar to caudal. But, in fact, this technique of sacral epidural is incapable of producing anesthesia to all cases. Obliteration of foramen due to deposition of calcium salt or conversion of foramen to the smaller size for the entrance of nerve stimulator needle is the cause of failure of caudal anesthesia through the dorsal foramen. Sizes of foramen are variable individual to individual. Some foramens may be smaller, or some may be bigger in size. The foramens of bigger size are good for the insertion of the needle. Currently, surgical intervention to make access to sacral epidural space through the sacral hiatus confirms 100% success rate in administration of caudal anesthesia. With the help of an orthopedic surgeon, a hole is drilled on the sacral hiatus in cephalic direction. The sacral epidural space was identified with the help of a nerve stimulator needle, inserted through the drilling hole. Surgical drilling procedure on the posterior wall of the sacral hiatus with 2.5 mm drill bit and adjustable guard, 2.5mm apart from its tip is a simple and harmless technique. Usually, it does not cause any damage to any vital structure by an expert fellow. The sacral canal and adjustable guard prevent further progress of bit to drill the anterior wall of hiatus. The use of hand drill provides better control to stop the procedure when needed. The surgical intervention by drilling procedure on sacral hiatus is a good and harmless option to smash all obstructions offered by anatomical distortion of the sacral hiatus in the adult life. The sacral hiatus is the defect in the lower part of posterior wall of sacrum and formed by failure of fusion or absence of the laminae of the S4 and S5 in the midline. The sacral hiatus is located at the caudal end of the median crest and is surrounded by the sacral cornua which are the remnants of inferior articular processes of 5th [S5] sacral vertebrae. They are free and prominent constituting an important landmark together with adjacent coccygeal cornua. This sacral hiatus is covered posteriorly by dense sacrococcygeal ligament that is formed from the supraspinatus and interspinous ligament, as well as the ligamentum flavum. Penetration of this ligament by the needle provides the direct access to the caudal limit of the epidural space in the sacral canal. The sacral components of the sciatic nerve (S1to S3) exit through the respective intervertebral foramens bye-passing the sacral hiatus and escaping from drilling. 4th and 5th sacral spinal nerve roots, leaving dural sac at the level of S2 travel obliquely towards their respective foramens, located at 1.5 cm lateral from the midline remain uninjured at the time of drilling on the sacral hiatus. The less important structures like filum terminale and coccygeal nerve, travelling through the sacral hiatus to coccyx are on the verge of injury during drilling procedure by hand drill and such damage, if occurred at all, may be ignored causes negligible physiological alternation. 37 Page
4 Sacral epidural space (SES) is continuous upwards as lumbar epidural space and below as sacral hiatus. Thus after deposition of local anesthetic in SES, reduced height of the cephalad flow of local anesthetic is more likely due to free leakage through patent dorsal and ventral openings of sacrum and large capacity of SES. The capacious sacral epidural space helps to explain the less involvement of the spinal segments of sympathetic outflow, responsible for hemodynamic status of the body. The simplicity of the technique for perfect identification of the epidural space with the help of a nerve stimulator needle [6] is the acceptable procedure with less damage to surrounding structures. The evidence, produced by the stimulation of nerve by electric current, is an important guide to detect the epidural space in the presence of nerves. The deposition of local anesthetic in the epidural space after confirmation by nerve stimulating effect bears a better cephalad spread. Problematic situation arises in anesthetic management of elderly patients owing to their limited organ reserve and coexisting compromised cardio-respiratory status. These groups of patients are frequently associated with hepatic and renal insufficiency. Hemodynamic instability during any surgical procedure is usually unwanted. Neuraxial block has definitive benefits to control the surgical stress response with reduction of blood loss during surgery. Caudal anesthesia is the better option providing better control over hemodynamic stability, surgical stress response and reduction of blood loss during the surgical procedures of lower limbs. In this study, all participants are aged and scheduled for lower limbs surgeries. All of them were administered caudal anesthesia either through sacral hiatus (16.6%) or dorsal foramens of sacrum (80%) or drilling hole on sacral hiatus (100%).[10] In short, all were operated under caudal anesthesia with hemodynamic stability. No adverse reaction like intravenous injection, intrathecal injection and total spinal postponed the procedure. Complications of the caudal anesthesia are similar with those seen in the most of the other regional anesthesia. Meticulous attention with expertness is capable of decreasing the rate of complication. Claims of drug toxicity associated with the use of a large amount of local anesthetic failed to substantiate [11]. Nevertheless, potential danger exists with intravenous or intraossesous administration of the local anesthetic.[ 12] The chance of dural puncture is exceedingly rare as the termination of the dural sac usually occurs at the level of S2. The distance between the end of dural sac and apex of the sacral hiatus restricts the advancement of the needle not more than 1 to 2 cm.[13 ] The most frequent complications of caudal anesthesia include pain, infection and urinary retention. Among these, pain is the most common complication. It may be due to either soft tissue injury or periosteal hematoma. The periosteal pain lasts for several weeks [4] and severe in nature. Pain in soft tissue along the site of injection is usually mild in nature and of little troublesome. The chance of infection in caudal anesthesia is potentially dangerous as site of needle insertion is very closed to perineum. However, it is exceedingly rare, most probably, bacteriostatic or bacteriocidal action of local anesthetic plays an important role to contribute such low incidence of infection. No difference is observed in bacteriological comparison of skin culture or catheter culture in caudal or epidural anesthesia.[14] Like lumbar epidural and subarachnoid block caudal anesthesia is inevitably associated with some slight risky neurological complication. One permanent neurological damaged was observed by Dawkins in cases. Exact details are not available.[11] Whatever was the fact, it is obviously true that the occurrence was very small. Above all, pre-existing neurological deficit may be worsened and blamed as complication of anesthesia. In comparison with lumbar epidural, caudal epidural possesses some definitive advantages over previous one. Caudal anesthesia is more reliable than lumbar epidural with 100% involvement of L5 and S1 spinal nerve roots. Chances of dural puncture are more common in lumbar epidural than caudal procedure. Simultaneously, caudal anesthesia possesses some disadvantages over lumbar epidural. The caudal anesthesia is technically more difficult procedure than lumbar epidural. Recently, such difficulties are easily overcome with the help of nerve stimulator needle and surgical assisted procedure. But, the need of a large amount of local anesthetic for caudal anesthesia always bears a risk of drug toxicity that is the rare incident in case of lumbar epidural. The lumbar spinal anesthesia is also advantageous over caudal anesthesia. Quick onset and technical easiness make it superior to caudal anesthesia whereas low incidence of postdural puncture headache and more durable anesthesia by single dose caudal make it superior to single dose spinal anesthesia. Busoni, one of the fathers of pediatric locoregional anesthesia [15,16] introduced caudal anesthesia in pediatric through transsacral route at the level of S2 and S3 intervertebral space.[17] It was safe and easy as caudal through sacral hiatus with minimal chance of contamination from fecal soiling.[18] The needle was inserted at the angle of degrees at the level of S2-S3 intervertebral space. In fact, it was possible due to lack of ossification in pediatric patients, but it is not possible in adult life due to complete ossification. 38 Page
5 V. Conclusion Surgical assisted caudal anesthesia is a good and easily approachable device to overcome the anatomical distortion of the sacral hiatus occurred in aged persons. This surgical aided procedure makes the caudal as predictable, predominant and preferable method of anesthesia for lower limbs surgeries in aged persons. It is exclusively one of the best techniques of anesthesia for the lower limbs surgeries with devoid of hemodynamic disturbance. The surgical assisted caudal anesthesia is a stunting, but beneficial approach in the world of practicing anesthesia. References [1]. Capt STEVEN J.ZITO, CRNA, BS, USAF, NC. Adult caudal anesthesia: A reexamination of the technique. Journal of the American Association of Nurse Anesthetists. 1993; 61(2): [2]. Black MG Anatomic reasons for caudal anesthesia failure.anesth Analg. 1949;28:33. [3]. Paria R, Surroy S, Majumder M, Paria A, Paria B, Das G. Sacral spinal anesthesia. Indian J Anesth. 2014; 58(1) : 80-2 [4]. Paria R, Surroy S, Majumder M, Paria B, Sengupta S, Paria A. Sacral Saddle Block IOSR-JDMS 2014; 13(4) [5]. Paria R, Surroy S, Majumder M, Paria B, Sengupta S, Paria A. Sacral Epidural Anesthesia IOSR- JDMS 2014; 13(5) [6]. Tsui, B.C., Tarkkila, P., Gupta, S., Kearney, R. Confirmation of caudal needle placement by nerve stimulation. Anesthesiology 91: 374; [7]. Gallart L, Blanco D, Samso E, Vidal F. Clinical and radiologic evidence of the epidural plica mediana dorsalis. Anesth Analg 1990;71: [8]. Peduto VA, Tani R, Marinelli L, Pani S. Bilateral analgesia and unilateral paresis after lumbar epidural blockade. Anesth Analg 1992;74: [9]. Singh A. Unilateral epidural analgesia. Anaesthesia 1967;22: [10]. Paria RS, Caudal Anesthesia through Drilling Hole on Sacral Hiatus: A Case Report. IOSR-JDMS 2014; 13(9) [11]. DawkinsCJM An analysis of the complication of extradural and caudal block. Anesthesia 1969; 24:554. [12]. Printiss JE Cardiac arrest following caudal anesthesia.anesthesiology 1979;50:51. [13]. Chun L, Karp M,Unusual complication from placement of catheter in caudal canal in obstetrical anesthesia.anesthesiology 1966;27:96. [14]. Abouleish E,Orig T, AmortegulA Bacteriologic comparison between epidural and caudal technique.1980; 53: 511. [15]. Busoni P, Sarti A. Sacral intervertebral epidural block Anesthesiology. 1987; 67: [16]. Busoni P. Trans-sacral extradural anesthesia in pediatrics. Cah Anesthesiol. 1992; 40: [17]. Saint-maurice C, Laundais A, Othmani H, Khalloufi M. The trans-sacral route.can be the technique be sapmlified? Cah Anesthesiol. 1993; 41(3): [18]. Quinot JF, Coquelin G. Trans-sacral caudal anesthesia in ambulatory practice in infants. Our experience. Cah Anesthesiol.1993; 41(4): 347 TABLE NO 1 Showing Demographic Profile, Hemodynamic Profile, And Nerve Block Profile. DEMOGRAPHIC PROFILE Age (years) 77.27±5.49 Height (Cm) ±6.48 Weight (Kg) 58.70±5.95 Sex (M:F) 12:18 HEMODYNAMIC PROFILE. Systolic blood pressure (mm Hg) ±7.26 H Heart Rate (beats/min) 81.37±5.68 Oxygen Saturation (%) 98.93±0.9 NERVE BLOCK PROFILE. Onset time of sensory block.(min) 19.13±4.32 Onset time of motor block.(min) 25.10±4.35 Duration of sensory block. (min) ±12.41 Duration of motor block.(min) ±11.42 Cephalad extension (vertebra) T12 39 Page
Sacral Unilateral Spinal Anaesthesia With 0.25% Hypobaric Bupivacaine
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. I (Sep. 2015), PP 35-39 www.iosrjournals.org Sacral Unilateral Spinal Anaesthesia With
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. I (Sep. 2015), PP 35-39 www.iosrjournals.org Sacral Unilateral Spinal Anaesthesia With
A study of the anatomy of the caudal space using magnetic resonance imaging
 British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
Gross Morphology of Spinal Cord
 Gross Morphology of Spinal Cord Done By : Rahmeh Alsukkar ** I did my best and sorry for any mistake ** the sheet does not contain pictures, tables and some slides so please be careful and go back to slides
Gross Morphology of Spinal Cord Done By : Rahmeh Alsukkar ** I did my best and sorry for any mistake ** the sheet does not contain pictures, tables and some slides so please be careful and go back to slides
Gross Morphology of Spinal Cord
 Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
Chapter 13. The Spinal Cord & Spinal Nerves. Spinal Cord. Spinal Cord Protection. Meninges. Together with brain forms the CNS Functions
 Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
The Spinal Cord & Spinal Nerves
 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
ANATOMY OF SPINAL CORD. Khaleel Alyahya, PhD, MEd King Saud University School of
 ANATOMY OF SPINAL CORD Khaleel Alyahya, PhD, MEd King Saud University School of Medicine @khaleelya OBJECTIVES At the end of the lecture, students should be able to: Describe the external anatomy of the
ANATOMY OF SPINAL CORD Khaleel Alyahya, PhD, MEd King Saud University School of Medicine @khaleelya OBJECTIVES At the end of the lecture, students should be able to: Describe the external anatomy of the
Human Anatomy. Spinal Cord and Spinal Nerves
 Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
Anatomy of the Spine. Figure 1. (left) The spine has three natural curves that form an S-shape; strong muscles keep our spine in alignment.
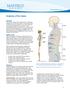 1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
Spinal Cord Protection. Chapter 13 The Spinal Cord & Spinal Nerves. External Anatomy of Spinal Cord. Structures Covering the Spinal Cord
 Spinal Cord Protection Chapter 13 The Spinal Cord & Spinal Nerves We are only going to cover Pages 420-434 and 447 Together with brain forms the CNS Functions spinal cord reflexes integration (summation
Spinal Cord Protection Chapter 13 The Spinal Cord & Spinal Nerves We are only going to cover Pages 420-434 and 447 Together with brain forms the CNS Functions spinal cord reflexes integration (summation
Epidural Analgesia in Labor - Whats s New
 Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
Anatomy of the Nervous System. Brain Components
 Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Vertebral Column. Backbone consists of 26 vertebrae. Five vertebral regions. Cervical
 Vertebral Column Backbone consists of 26 vertebrae. Five vertebral regions Cervical vertebrae (7) in the neck. Thoracic vertebrae (12) in the thorax. Lumbar vertebrae (5) in the lower back. Sacrum (5,
Vertebral Column Backbone consists of 26 vertebrae. Five vertebral regions Cervical vertebrae (7) in the neck. Thoracic vertebrae (12) in the thorax. Lumbar vertebrae (5) in the lower back. Sacrum (5,
Copyright 2010 Pearson Education, Inc.
 E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
THE VERTEBRAL COLUMN. Average adult length: In male: about 70 cms. In female: about 65 cms.
 THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
Hyperbaric 2% Lignocaine In Spinal Anaesthesia An Excellent Option For Day Care Surgeries
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 2 Ver. III. (Feb. 2014), PP 09-13 Hyperbaric 2% Lignocaine In Spinal Anaesthesia An Excellent
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 2 Ver. III. (Feb. 2014), PP 09-13 Hyperbaric 2% Lignocaine In Spinal Anaesthesia An Excellent
Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain.
 Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
Epidural anaesthesia and analgesia
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Epidural anaesthesia and analgesia Author : Matthew Gurney Categories : Vets Date : June 1, 2009 Matthew Gurney discusses
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Epidural anaesthesia and analgesia Author : Matthew Gurney Categories : Vets Date : June 1, 2009 Matthew Gurney discusses
Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for
 Chapter 13 Outline Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for what you need to know from Exhibits 13.1 13.4 I. INTRODUCTION A. The spinal cord and spinal nerves
Chapter 13 Outline Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for what you need to know from Exhibits 13.1 13.4 I. INTRODUCTION A. The spinal cord and spinal nerves
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
How and why to do an epidural in dogs and cats? Which Indications and which drugs?
 AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
NERVOUS SYSTEM ANATOMY
 INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
NERVOUS SYSTEM ANATOMY
 NTRODUCTON to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science Engineering
NTRODUCTON to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science Engineering
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Script for: Regional Anesthesia Surgery 101 Podcast Department of Surgery University of Alberta. Urooj Siddiqui Med 4 University of Alberta
 Script for: Regional Anesthesia Surgery 101 Podcast Department of Surgery University of Alberta By Urooj Siddiqui Med 4 University of Alberta Hello, and welcome back to Surgery 101. My name is Urooj Siddiqui,
Script for: Regional Anesthesia Surgery 101 Podcast Department of Surgery University of Alberta By Urooj Siddiqui Med 4 University of Alberta Hello, and welcome back to Surgery 101. My name is Urooj Siddiqui,
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Bony framework of the vertebral column Structure of the vertebral column
 5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
THE benefits of pediatric regional anesthesia are many, Ultrasound Imaging for Regional Anesthesia in Infants, Children, and Adolescents
 REVIEW ARTICLES Anesthesiology 2010; 112:719 28 Copyright 2010, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins David S. Warner, M.D., Editor Ultrasound Imaging for Regional
REVIEW ARTICLES Anesthesiology 2010; 112:719 28 Copyright 2010, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins David S. Warner, M.D., Editor Ultrasound Imaging for Regional
A Study of Sacral Hiatus in Dry Human Sacra in Southern Nigeria
 A Study of Sacral Hiatus in Dry Human Sacra in Southern Nigeria Osunwoke E.A (PhD-Corresponding author) E-mail: aeosunwoke@yahoo.com Oladipo G. S (PhD) E-mail: oladipogabriel@yahoo.com Allison T.A (MBBS)
A Study of Sacral Hiatus in Dry Human Sacra in Southern Nigeria Osunwoke E.A (PhD-Corresponding author) E-mail: aeosunwoke@yahoo.com Oladipo G. S (PhD) E-mail: oladipogabriel@yahoo.com Allison T.A (MBBS)
COMPLICATIONS AND INTERVENTIONS ASSOCIATED WITH EPIDURAL ANALGESIA FOR POSTOPERATIVE PAIN RELIEF IN A TERTIARY CARE HOSPITAL
 COMPLICATIONS AND INTERVENTIONS ASSOCIATED WITH EPIDURAL ANALGESIA FOR POSTOPERATIVE PAIN RELIEF IN A TERTIARY CARE HOSPITAL Faraz Shafiq *, Mohammad Hamid ** and Khalid Samad *** Introduction Epidural
COMPLICATIONS AND INTERVENTIONS ASSOCIATED WITH EPIDURAL ANALGESIA FOR POSTOPERATIVE PAIN RELIEF IN A TERTIARY CARE HOSPITAL Faraz Shafiq *, Mohammad Hamid ** and Khalid Samad *** Introduction Epidural
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
THEME 2. VERTEBRAE (GENERAL DATA). CERVICAL, THORACIC AND LUMBAR VERTEBRAE. SACRUM. COCCYX. THE VERTEBRAL COLUMN AS A WHOLE
 THEME 2. VERTEBRAE (GENERAL DATA). CERVICAL, THORACIC AND LUMBAR VERTEBRAE. SACRUM. COCCYX. THE VERTEBRAL COLUMN AS A WHOLE Osteology of the Vertebral Column Bone Description vertebra Notes a vertebra
THEME 2. VERTEBRAE (GENERAL DATA). CERVICAL, THORACIC AND LUMBAR VERTEBRAE. SACRUM. COCCYX. THE VERTEBRAL COLUMN AS A WHOLE Osteology of the Vertebral Column Bone Description vertebra Notes a vertebra
Regional Anesthesia. Fatiş Altındaş Dept. of Anesthesiology
 Regional Anesthesia Fatiş Altındaş Dept. of Anesthesiology Regional anesthesia - Definition Renders a specific area of the body, e.g. foot, arm, lower extremities insensating to stimulus of surgery or
Regional Anesthesia Fatiş Altındaş Dept. of Anesthesiology Regional anesthesia - Definition Renders a specific area of the body, e.g. foot, arm, lower extremities insensating to stimulus of surgery or
Chapter 7 The Skeletal System:The Axial Skeleton
 Chapter 7 The Skeletal System:The Axial Skeleton Axial Skeleton 80 bones lie along longitudinal axis skull, hyoid, vertebrae, ribs, sternum, ear ossicles Appendicular Skeleton 126 bones upper & lower limbs
Chapter 7 The Skeletal System:The Axial Skeleton Axial Skeleton 80 bones lie along longitudinal axis skull, hyoid, vertebrae, ribs, sternum, ear ossicles Appendicular Skeleton 126 bones upper & lower limbs
Spinal Column. Anatomy Of The Spine
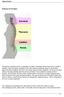 Anatomy Of The Spine The spine is a flexible column, composed of a stack of individual bones. Each bone is called a vertebra. There are seven vertebrae in the neck (cervical vertebrae) twelve in the thoracic
Anatomy Of The Spine The spine is a flexible column, composed of a stack of individual bones. Each bone is called a vertebra. There are seven vertebrae in the neck (cervical vertebrae) twelve in the thoracic
ANATOMY OF THE SPINAL CORD. Structure of the spinal cord Tracts of the spinal cord Spinal cord syndromes
 SPINAL CORD ANATOMY OF THE SPINAL CORD Structure of the spinal cord Tracts of the spinal cord Spinal cord syndromes The Nervous System Coordinates the activity of muscles, organs, senses, and actions Made
SPINAL CORD ANATOMY OF THE SPINAL CORD Structure of the spinal cord Tracts of the spinal cord Spinal cord syndromes The Nervous System Coordinates the activity of muscles, organs, senses, and actions Made
Continuous Spinal Anaesthesia
 Continuous Spinal Anaesthesia Ph. Biboulet Department of Anesthesiology and Critical Care Medicine, Lapeyronie University Hospital, Montpellier France CSA story : 1906 Dean 1944 Tuohy 1991 CSA revisited
Continuous Spinal Anaesthesia Ph. Biboulet Department of Anesthesiology and Critical Care Medicine, Lapeyronie University Hospital, Montpellier France CSA story : 1906 Dean 1944 Tuohy 1991 CSA revisited
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Eldor Epidural Kit (CSEN 68) Epidural catheter technique
 Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
Spinal Cord H. Ruth Clemo, Ph.D.
 Spinal Cord H. Ruth Clemo, Ph.D. OBJECTIVES After studying the material of this lecture, the student should be familiar with: 1. Surface anatomy of the spinal cord. 2. Internal structure and organization
Spinal Cord H. Ruth Clemo, Ph.D. OBJECTIVES After studying the material of this lecture, the student should be familiar with: 1. Surface anatomy of the spinal cord. 2. Internal structure and organization
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test
 Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
SPINAL INJECTIONS SECTION 5 SPINAL INJECTION GUIDELINES 219
 SECTION 5 SPINAL INJECTIONS SPINAL INJECTION GUIDELINES 219 Overview 219 Safety 219 Accuracy 220 Efficacy 220 Indications for spinal injection 221 Summary 222 EXAMINATION OF THE SPINE 223 CAUDAL EPIDURAL
SECTION 5 SPINAL INJECTIONS SPINAL INJECTION GUIDELINES 219 Overview 219 Safety 219 Accuracy 220 Efficacy 220 Indications for spinal injection 221 Summary 222 EXAMINATION OF THE SPINE 223 CAUDAL EPIDURAL
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology University of Washington, Seattle, WA
 ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
The sacrum is a complex anatomical structure.
 A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
Copyright 2010 Pearson Education, Inc. Copyright 2010 Pearson Education, Inc. Figure Sectioned spinous process. Interspinous.
 PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 7 The Skeleton: Part B Vertebral Column Transmits weight of trunk to lower limbs Surrounds and protects spinal cord
PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 7 The Skeleton: Part B Vertebral Column Transmits weight of trunk to lower limbs Surrounds and protects spinal cord
Pain Management: Epidural Steroid Injections
 A Patient s Guide to Pain Management: Epidural Steroid Injections 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Pain Management: Epidural Steroid Injections 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from
Lecture 14: The Spinal Cord
 Lecture 14: The Spinal Cord M/O Chapters 16 69. Describe the relationship(s) between the following structures: root, nerve, ramus, plexus, tract, nucleus, and ganglion. 70. Trace the path of information
Lecture 14: The Spinal Cord M/O Chapters 16 69. Describe the relationship(s) between the following structures: root, nerve, ramus, plexus, tract, nucleus, and ganglion. 70. Trace the path of information
Epidural puncture can be confirmed by the Queckenstedttest procedure in patients with cervical spinal canal stenosis
 Acta Anaesthesiol Scand 2008; 52: 256 261 Printed in Singapore. All rights reserved r 2007 The Authors Journal compilation r 2007 The Acta Anaesthesiologica Scandinavica Foundation ACTA ANAESTHESIOLOGICA
Acta Anaesthesiol Scand 2008; 52: 256 261 Printed in Singapore. All rights reserved r 2007 The Authors Journal compilation r 2007 The Acta Anaesthesiologica Scandinavica Foundation ACTA ANAESTHESIOLOGICA
AXIAL SKELETON FORM THE VERTICAL AXIS OF THE BODY CONSISTS OF 80 BONES INCLUDES BONES OF HEAD, VERTEBRAL COLUMN, RIBS,STERNUM
 AXIAL SKELETON FORM THE VERTICAL AXIS OF THE BODY CONSISTS OF 80 BONES INCLUDES BONES OF HEAD, VERTEBRAL COLUMN, RIBS,STERNUM APPENDICULAR SKELETON BONES OF THE FREE APPENDAGES & THEIR POINTS OF ATTACHMENTS
AXIAL SKELETON FORM THE VERTICAL AXIS OF THE BODY CONSISTS OF 80 BONES INCLUDES BONES OF HEAD, VERTEBRAL COLUMN, RIBS,STERNUM APPENDICULAR SKELETON BONES OF THE FREE APPENDAGES & THEIR POINTS OF ATTACHMENTS
THE BACK THE SPINAL CORD
 THE BACK THE SPINAL CORD The structures in the vertebral canal: the spinal cord spinal nerve roots spinal meninges the neurovascular structures THE SPINAL CORD The spinal cord occupies the superior 2/3
THE BACK THE SPINAL CORD The structures in the vertebral canal: the spinal cord spinal nerve roots spinal meninges the neurovascular structures THE SPINAL CORD The spinal cord occupies the superior 2/3
WITH ISOBARIC BUPIVACAINE (5 MG/ML)
 , 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
, 49, 2013, 3 63 (5 MG/ML) (5 MG/ML).,.,.,..,..,, SPINAL ANESTHESIA: COMPARISON OF ISOBARIC ROPIVACAINE (5 MG/ML) WITH ISOBARIC BUPIVACAINE (5 MG/ML) D. Tzoneva, Vl. Miladinov, Al. Todorov, M. P. Atanasova,
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES
 REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES 1. A 28-year-old-women presented to the hospital emergency room with intense lower back spasms in the context of coughing during an upper respiratory
REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES 1. A 28-year-old-women presented to the hospital emergency room with intense lower back spasms in the context of coughing during an upper respiratory
Interscalene brachial plexus blocks in the management of shoulder dislocations
 Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Spread of subarachnoid hyperbaric amethocaine in adolescents
 British Journal of Anaesthesia 1995; 74: 41-45 Spread of subarachnoid hyperbaric amethocaine in adolescents Y. HIRABAYASHI, R. SHIMIZU, K. SAITOH, H. FUKUDA Summary We have compared the spread of subarachnoid
British Journal of Anaesthesia 1995; 74: 41-45 Spread of subarachnoid hyperbaric amethocaine in adolescents Y. HIRABAYASHI, R. SHIMIZU, K. SAITOH, H. FUKUDA Summary We have compared the spread of subarachnoid
Anatomical study of the sacral hiatus
 Original article Anatomical study of the sacral hiatus Dr. Somanath Deepa, Dr. Rajasekar SS Department of Anatomy, Sri Manakula Vinayagar Medical College and Hospital, Puducherry (U.T.), India. Corresponding
Original article Anatomical study of the sacral hiatus Dr. Somanath Deepa, Dr. Rajasekar SS Department of Anatomy, Sri Manakula Vinayagar Medical College and Hospital, Puducherry (U.T.), India. Corresponding
Comparison of Straight Versus Flexed Back in Combined Spinal Epidural Anesthesia for Gynecological Procedure
 Comparison of Versus Flexed Back in Combined Spinal Epidural Anesthesia for Gynecological Procedure Vaishali Waindeskar, Sheetal Songir, Mahima Batra, MR Gaikwad, Munir Ahmad Khan, Anuj Dubey Department
Comparison of Versus Flexed Back in Combined Spinal Epidural Anesthesia for Gynecological Procedure Vaishali Waindeskar, Sheetal Songir, Mahima Batra, MR Gaikwad, Munir Ahmad Khan, Anuj Dubey Department
The value of Tuffier s line for neonatal neuraxial procedures. Department of Anatomy, School of Medicine, Faculty of Health Sciences,
 The value of Tuffier s line for neonatal neuraxial procedures Albert van Schoor 1, MC Bosman 1, and AT Bosenberg 2, Original article 1 Department of Anatomy, School of Medicine, Faculty of Health Sciences,
The value of Tuffier s line for neonatal neuraxial procedures Albert van Schoor 1, MC Bosman 1, and AT Bosenberg 2, Original article 1 Department of Anatomy, School of Medicine, Faculty of Health Sciences,
CHAPTER 13 LECTURE OUTLINE
 CHAPTER 13 LECTURE OUTLINE I. INTRODUCTION A. The spinal cord and spinal nerves mediate reactions to environmental changes. B. The spinal cord has several functions. 1. It processes reflexes. 2. It is
CHAPTER 13 LECTURE OUTLINE I. INTRODUCTION A. The spinal cord and spinal nerves mediate reactions to environmental changes. B. The spinal cord has several functions. 1. It processes reflexes. 2. It is
Overview. Spinal Anatomy Spaces & Meninges Spinal Cord. Anatomy of the dura. Anatomy of the arachnoid. Anatomy of the spinal meninges
 European Course in Neuroradiology Module 1 - Anatomy and Embryology Dubrovnik, October 2018 Spinal Anatomy Spaces & Meninges Spinal Cord Johan Van Goethem Overview spinal meninges & spaces spinal cord
European Course in Neuroradiology Module 1 - Anatomy and Embryology Dubrovnik, October 2018 Spinal Anatomy Spaces & Meninges Spinal Cord Johan Van Goethem Overview spinal meninges & spaces spinal cord
VERTEBRAL COLUMN VERTEBRAL COLUMN
 VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
The Spinal Cord. The Nervous System. The Spinal Cord. The Spinal Cord 1/2/2016. Continuation of CNS inferior to foramen magnum.
 The Nervous System Spinal Cord Continuation of CNS inferior to foramen magnum Simpler than the brain Conducts impulses to and from brain Two way conduction pathway Reflex actions Passes through vertebral
The Nervous System Spinal Cord Continuation of CNS inferior to foramen magnum Simpler than the brain Conducts impulses to and from brain Two way conduction pathway Reflex actions Passes through vertebral
COMPARISON OF INCREMENTAL SPINAL ANAESTHESIA USING A 32-GAUGE CATHETER WITH EXTRADURAL ANAESTHESIA FOR ELECTIVE CAESAREAN SECTION
 British Journal of Anaesthesia 1991; 66: 232-236 COMPARISON OF INCREMENTAL SPINAL ANAESTHESIA USING A 32-GAUGE CATHETER WITH EXTRADURAL ANAESTHESIA FOR ELECTIVE CAESAREAN SECTION I. G. KESTIN, A. P. MADDEN,
British Journal of Anaesthesia 1991; 66: 232-236 COMPARISON OF INCREMENTAL SPINAL ANAESTHESIA USING A 32-GAUGE CATHETER WITH EXTRADURAL ANAESTHESIA FOR ELECTIVE CAESAREAN SECTION I. G. KESTIN, A. P. MADDEN,
Assistant Professor, Anaesthesia Department, Govt. General Hospital / Guntur Medical College, Guntur, Andhra Pradesh, India.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. I (August. 2016), PP 87-91 www.iosrjournals.org A Comparative Study of 0.25% Ropivacaine
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. I (August. 2016), PP 87-91 www.iosrjournals.org A Comparative Study of 0.25% Ropivacaine
MD Bones & Joints of the Back. A/Prof Chris Briggs Department of Anatomy & Neuroscience
 MD 2017 Bones & Joints of the Back A/Prof Chris Briggs Department of Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
MD 2017 Bones & Joints of the Back A/Prof Chris Briggs Department of Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Chapter 12b. Overview
 Chapter 12b Spinal Cord Overview Spinal cord gross anatomy Spinal meninges Sectional anatomy Sensory pathways Motor pathways Spinal cord pathologies 1 The Adult Spinal Cord About 18 inches (45 cm) long
Chapter 12b Spinal Cord Overview Spinal cord gross anatomy Spinal meninges Sectional anatomy Sensory pathways Motor pathways Spinal cord pathologies 1 The Adult Spinal Cord About 18 inches (45 cm) long
Paraspinal Blocks a new paradigm in truncal analgesia
 Paraspinal Blocks a new paradigm in truncal analgesia Ki Jinn Chin, MBBS (Hons), MMed, FRCPC Associate Professor Toronto Western Hospital University of Toronto Online Resources https://youtu.be/lockhd
Paraspinal Blocks a new paradigm in truncal analgesia Ki Jinn Chin, MBBS (Hons), MMed, FRCPC Associate Professor Toronto Western Hospital University of Toronto Online Resources https://youtu.be/lockhd
Lower Extremity Ultrasound-Guided Regional Anesthesia. Stephanie Duffy, CRNA Regional Anesthesia Faculty Acute Pain Service NMCSD
 Lower Extremity Ultrasound-Guided Regional Anesthesia Stephanie Duffy, CRNA Regional Anesthesia Faculty Acute Pain Service NMCSD Objectives Review anatomy of lumbosacral plexus Lumbar plexus blocks Psoas
Lower Extremity Ultrasound-Guided Regional Anesthesia Stephanie Duffy, CRNA Regional Anesthesia Faculty Acute Pain Service NMCSD Objectives Review anatomy of lumbosacral plexus Lumbar plexus blocks Psoas
human anatomy 2015 lecture four Dr meethak ali ahmed neurosurgeon
 The Vertebral Column the vertebral columnis central pillar of the body.it serve to protect the spinal cord and support the weight of the head trunk, which it transmits to the hip bones & the lower limbs.
The Vertebral Column the vertebral columnis central pillar of the body.it serve to protect the spinal cord and support the weight of the head trunk, which it transmits to the hip bones & the lower limbs.
Continuing Education in Anaesthesia, Critical Care & Pain Advance Access published August 17, 2010
 Continuing Education in Anaesthesia, Critical Care & Pain Advance Access published August 17, 2010 Paravertebral block SQM Tighe MBBS, FRCA Michelle D Greene BMedSci, MBBS, FRCA Nirmal Rajadurai MBBS,
Continuing Education in Anaesthesia, Critical Care & Pain Advance Access published August 17, 2010 Paravertebral block SQM Tighe MBBS, FRCA Michelle D Greene BMedSci, MBBS, FRCA Nirmal Rajadurai MBBS,
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Sarah Reece-Stremtan M.D. Peripheral Nerve Blockade Neuraxial Blocks
 Neuraxial Anesthesia Sarah Reece-Stremtan M.D. Regional Anesthesia Peripheral Nerve Blockade Neuraxial Blocks Placed in the OR under general anesthesia by members of the regional anesthesia team 1 Sensory
Neuraxial Anesthesia Sarah Reece-Stremtan M.D. Regional Anesthesia Peripheral Nerve Blockade Neuraxial Blocks Placed in the OR under general anesthesia by members of the regional anesthesia team 1 Sensory
David S. Warner, M.D., Editor. Ultrasonography of the Adult Thoracic and Lumbar Spine for Central Neuraxial Blockade
 REVIEW ARTICLE David S. Warner, M.D., Editor Ultrasonography of the Adult Thoracic and Lumbar Spine for Central Neuraxial Blockade Ki Jinn Chin, F.R.C.P.C.,* Manoj Kumar Karmakar, M.D., Philip Peng, F.R.C.P.C.
REVIEW ARTICLE David S. Warner, M.D., Editor Ultrasonography of the Adult Thoracic and Lumbar Spine for Central Neuraxial Blockade Ki Jinn Chin, F.R.C.P.C.,* Manoj Kumar Karmakar, M.D., Philip Peng, F.R.C.P.C.
Intrathecal 0.75% Isobaric Ropivacaine Versus 0.5% Heavy Bupivacaine for Elective Cesarean Delivery: A Randomized Controlled Trial
 Intrathecal 0.75% Isobaric Ropivacaine Versus 0.5% Heavy Bupivacaine for Elective Cesarean Delivery: A Randomized Controlled Trial Surjeet Singh, 1 V.P. Singh, 2 Manish Jain, 3 Kumkum Gupta, 3 Bhavna Rastogi,
Intrathecal 0.75% Isobaric Ropivacaine Versus 0.5% Heavy Bupivacaine for Elective Cesarean Delivery: A Randomized Controlled Trial Surjeet Singh, 1 V.P. Singh, 2 Manish Jain, 3 Kumkum Gupta, 3 Bhavna Rastogi,
Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries and Perineal Surgeries
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/229 Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/229 Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries
Relation of Paralumbar Nerves and Conus Medullaris to the Vertebrae of Swamp Buffaloes
 Kasetsart J. (Nat. Sci.) 37 : 41-46 (2003) Relation of Paralumbar Nerves and Conus Medullaris to the Vertebrae of Swamp Buffaloes Narong Chungsamarnyart, Worawut Rerkamnuaychoke and Nati Nilnophakoon ABSTRACT
Kasetsart J. (Nat. Sci.) 37 : 41-46 (2003) Relation of Paralumbar Nerves and Conus Medullaris to the Vertebrae of Swamp Buffaloes Narong Chungsamarnyart, Worawut Rerkamnuaychoke and Nati Nilnophakoon ABSTRACT
Comparative Study of Intrathecal Ropivacaine and Levobupivacaine With Fentanyl And Magnesium As Adjuvants For Lower Abdominal Surgeries
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861. Volume 13, Issue 5 Ver. II. (May. 214), PP 39-43 Comparative Study of Intrathecal Ropivacaine and Levobupivacaine
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861. Volume 13, Issue 5 Ver. II. (May. 214), PP 39-43 Comparative Study of Intrathecal Ropivacaine and Levobupivacaine
Spinal Cord and Properties of Cerebrospinal Fluid: Options for Drug Delivery. SMA Foundation New York
 Spinal Cord and Properties of Cerebrospinal Fluid: Options for Drug Delivery New York Why Do We Need to Know about the Spinal Cord Anatomy and Properties of Cerebrospinal Fluid? SMA therapeutics need to
Spinal Cord and Properties of Cerebrospinal Fluid: Options for Drug Delivery New York Why Do We Need to Know about the Spinal Cord Anatomy and Properties of Cerebrospinal Fluid? SMA therapeutics need to
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Perioperative Pain Management
 Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Technique Guide. ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
A Case of "Foot Drop" Following Combined Spinal Epidural Anesthesia
 ISPUB.COM The Internet Journal of Anesthesiology Volume 8 Number 1 A Case of "Foot Drop" Following Combined Spinal Epidural Anesthesia H Uzunlar, E Duman, A Eroglu, B Topcu, N Erciyes Citation H Uzunlar,
ISPUB.COM The Internet Journal of Anesthesiology Volume 8 Number 1 A Case of "Foot Drop" Following Combined Spinal Epidural Anesthesia H Uzunlar, E Duman, A Eroglu, B Topcu, N Erciyes Citation H Uzunlar,
Spinal injury. Structure of the spine
 Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Human Anatomy - Problem Drill 11: The Spinal Cord and Spinal Nerves
 Human Anatomy - Problem Drill 11: The Spinal Cord and Spinal Nerves Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper as needed,
Human Anatomy - Problem Drill 11: The Spinal Cord and Spinal Nerves Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper as needed,
SPINAL CORD AND PROPERTIES OF CEREBROSPINAL FLUID: OPTIONS FOR DRUG DELIVERY
 SPINAL CORD AND PROPERTIES OF CEREBROSPINAL FLUID: OPTIONS FOR DRUG DELIVERY WHY DO WE NEED TO KNOW ABOUT THE SPINAL CORD ANATOMY AND PROPERTIES OF CEREBROSPINAL FLUID? SMA therapeutics need to reach cells
SPINAL CORD AND PROPERTIES OF CEREBROSPINAL FLUID: OPTIONS FOR DRUG DELIVERY WHY DO WE NEED TO KNOW ABOUT THE SPINAL CORD ANATOMY AND PROPERTIES OF CEREBROSPINAL FLUID? SMA therapeutics need to reach cells
SPINAL AND EPIDURAL ANESTHESIA
 Chapter 17 SPINAL AND EPIDURAL ANESTHESIA Kenneth Drasner and Merlin D. Larson COMPARISON OF SPINAL AND EPIDURAL ANESTHESIA ANATOMY Vertebral Canal Ligaments Spinal Cord Meninges Spinal Nerves Subarachnoid
Chapter 17 SPINAL AND EPIDURAL ANESTHESIA Kenneth Drasner and Merlin D. Larson COMPARISON OF SPINAL AND EPIDURAL ANESTHESIA ANATOMY Vertebral Canal Ligaments Spinal Cord Meninges Spinal Nerves Subarachnoid
MAXILLARY INJECTION TECHNIQUE. Chinthamani Laser Dental Clinic
 MAXILLARY INJECTION TECHNIQUE Chinthamani Laser Dental Clinic Introduction A number of injection techniques are available to aid in providing clinically adequate anesthesia of the teeth and soft and hard
MAXILLARY INJECTION TECHNIQUE Chinthamani Laser Dental Clinic Introduction A number of injection techniques are available to aid in providing clinically adequate anesthesia of the teeth and soft and hard
Regional Anesthesia. procedure if required. However, many patients prefer to receive sedation either during the
 1 Regional Anesthesia Regional anaesthesia (or regional anesthesia) is anesthesia affecting only a large part of the body, such as a limb or the lower half of the body. Regional anaesthetic techniques
1 Regional Anesthesia Regional anaesthesia (or regional anesthesia) is anesthesia affecting only a large part of the body, such as a limb or the lower half of the body. Regional anaesthetic techniques
The intensity of preoperative pain is directly correlated with the amount of morphine needed for postoperative analgesia
 The intensity of preoperative pain is directly correlated with the amount of morphine needed for postoperative analgesia This study has been published: The intensity of preoperative pain is directly correlated
The intensity of preoperative pain is directly correlated with the amount of morphine needed for postoperative analgesia This study has been published: The intensity of preoperative pain is directly correlated
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
