Bone ingrowth into two porous ceramics with different pore sizes : An experimental study
|
|
|
- Jonah Shaw
- 6 years ago
- Views:
Transcription
1 Acta Orthop. Belg., 2004, 70, ORIGINAL STUDY Bone ingrowth into two porous ceramics with different pore sizes : An experimental study Laurent GALOIS, Didier MAINARD From the University Hospital of Nancy, France Many properties of porous calcium phosphate ceramics have been described, but how pore size influences bony integration of various porous ceramics remains unclear. This study was performed to quantify the bony ingrowth and biodegradability of two porous calcium phosphate ceramics with four different pore size ranges (45-80 µm, µm, µm, and µm). Hydroxyapatite (HA) and b-tricalcium phosphate (TCP) cylinders were implanted into the femoral condyles of rabbits and were left in situ for up to 12 months. The percentage of bone ingrowth and the depth of ingrowth within the pores were determined. Biodegradability of the implants was also evaluated. Bone ingrowth occurred at a higher rate into the TCP than into the HA ceramics with the same pore size ranges. The amount of newly formed bone was statistically smaller (p < 0.05) into ceramics with µm pore size than with larger pore size, whatever the implantation time for HA and until four months for TCP. No statistical difference was noted between the three highest pore size ranges. No implant degradation was noted up to four months. Our results suggest that a pore size above 80 µm improves bony ingrowth in both HA and TCP ceramics. Bone formation was higher in the TCP than in the HA implants. INTRODUCTION Bone graft substitutes, especially calcium phosphate ceramics, are a useful alternative to biologic materials such as autografts (23), allografts (22) and xenografts, and natural materials such as coral (6) for filling bone defects in orthopaedic surgery (10, 12, 14). In vitro and in vivo studies (2, 3) have shown calcium phosphate ceramics to be fully biocompatible. The physical and chemical properties of these substances make them bioactive in that they are able to induce specific biologic reactions (5). In addition, calcium phosphate ceramics are osteoconductive and resorbable (9, 20) : they provide a scaffolding for new bone formation and their macroporosity allows cells to invade and bone to grow into the ceramic (1, 3, 7). The two major calcium phosphate ceramics, hydroxyapatite (HA) and b-tricalcium phosphate (b-tcp), have been investigated in animal studies (15, 17-19, 26) where they have been shown to be well tolerated and readily incorporated. However, there are fewer studies Laurent Galois, MD, Orthopaedic Surgeon. Didier Mainard, MD, Orthopaedic Surgeon, Professor of Orthopaedics. Department of Orthopaedic Surgery, University Hospital of Nancy, France. Correspondence : Didier Mainard, Department of Orthopaedic Surgery, University Hospital of Nancy, 29 avenue Maréchal de Lattre de Tassigny, C.O. n 34, F Nancy Cedex, France. lgalois@free.fr didier.mainard@ciril.fr. 2004, Acta Orthopædica Belgica.
2 BONE INGROWTH INTO TWO POROUS CERAMICS 599 describing the influence of porosity on osseointegration (1, 3, 7, 11, 24, 26). We present an experimental study concerning the osseointegration of two porous calcium phosphate ceramics (HA and b- TCP) with four different pore size ranges. This study was performed to quantitate the bone ingrowth and biodegradability of the ceramics according to their pore size. MATERIALS AND METHODS Sixty New Zealand type rabbits weighing 3 kg with controlled sanitary status were fed with standard rabbit chow pellets and tap water ad libitum. The rabbits were divided into 2 groups (HA and b-tcp) for each interval time. Rabbits were killed after 2 weeks, 1 month, 2 months, 4 months, 6 months and 12 months. Cylinders 6 10 mm of HA or b-tcp were implanted into bone defects created with a drill in the femoral condyle under general anaesthesia. After shaving the knee joint, under aseptic conditions, a parapatellar skin incision was made on the medial side of the joint. An incision on the medial side of the patellar tendon provided access to the joint space and the patella was dislocated laterally. The knee was placed in full flexion and a hole 6 mm in diameter was drilled in the femoral condyle and carefully washed clean of bone debris before being filled with a ceramic cylinder (fig 1). Postoperatively, the animals were permitted cage activity without immobilisation. The animals were closely monitored for infection and other complications. All procedures were approved by the animal welfare committee. Hydroxyapatite (Synatite ) and b-tricalcium phosphate (Biosorb ) ceramics (S.B.M., Lourdes, France) were cast in cylinder form 6 mm in diameter and 10 mm in length. The porosity was 45% +/- 5%. Four pore size ranges were studied : µm, µm, µm and µm. All implants were sterilised by gamma radiation. Rabbits were killed after 2 weeks, 1 month, 2 months, 4 months, 6 months and 12 months. After the animal was sacrificed by injection, the femoral condyle was harvested and fixed in a 4% formaldehyde solution, then dehydrated successively with graded ethanol and toluene. Nondecalcified techniques were used for bone tissue preparation (13). Nondecalcified bone specimens were embedded in polymethylmethacrylate (PMMA) obtained by mixing methylmethacrylate (Osi, Saint-Quentin Fallavier, France), benzoyle peroxide (Merck, Darmstadt, Germany) and dibutylphthalate (Merck, Darmstadt, Germany). Nondecalcified 8-mm thick sections were Fig. 1. A hole 6 mm in diameter is drilled carefully in the femoral condyle and the ceramic cylinder is implanted. made perpendicular to the long axis of the ceramic cylinder, using a Leica apparatus (Nubloch, Germany) equipped with a tungsten knife. Solochrome-cyanine R and Masson s Trichrome were then applied. Stained sections were studied under a light microscope (Olympus, Tokyo, Japan). Measurements were taken over the entire implant surface for histomorphometry. The magnification used for the measurements was 20. Three parameters were studied : the depth of bone ingrowth into the ceramic (average of ten measurements), the surface of bone ingrowth, the relative surface of bone ingrowth (bone surface in the implant section/total implant section surface) and the rate of ceramic resorption. These parameters were studied for each pore size range, each interval time and each biomaterial. In each case, three sections were analysed and the average value determined. The results are expressed as the mean +/- standard deviation. Differences between groups were assessed by the Mann-Whitney U test for two groups and by Krüskal- Wallis variance for several groups. A minimum of p < 0.05 was required for a significant difference. RESULTS No fibrosis or adverse inflammation was observed at any implantation time. No clinical problems occurred during the implantation period, except for one animal at one month, which developed an infection of the knee and was eliminated from the study. All other animals survived the observation period and did not show any signs of illness or adverse reaction to the implant material. Histological observation was performed for both biomaterials.
3 600 L. GALOIS, D. MAINARD Fig. 2. Percentage of bone ingrowth into HA implant Fig. 3. Stained section (Solochrome-cyanine R) after 12 months of implantation of the HA ceramic. The surface of the ceramic is almost completely colonised by newly formed bone. Hydroxyapatite (fig 2 and 3) After two weeks, newly formed bone was found around and in the periphery of the implants, except those with a pore size range of µm. Tissue ingrowth into pores throughout the implants was seen from µm pore size range with 39% rehabitation. There was a statistically significant difference (p < 0.05) regarding bone ingrowth between the smaller pore size range and the others. One month following implantation, bone formation seen within pores was slightly higher and trabecular bone was thicker and deeper than at two weeks, especially in ceramics with a pore size range of and µm. Morphometric analysis showed respectively 63% and 61% of bone ingrowth and a centripetal bony ingrowth of 1.12 and 1 mm in depth. Incipient bone formation was seen in implants with a pore size range of µm. In the control hole, only fibrous tissue could be seen at one month. At two months, the new bone tissue seen in the pores increased for each pore size range, except for the smallest. From µm, bone ingrowth was clearly visible. Bone ingrowth reached 77% in the implants with µm pore size. At four months, there was still a statistically higher percentage of bone ingrowth into the three highest pore size ranges compared with the smallest. Nevertheless, significant new bone tissue was formed inside the µm ceramic (76%). The depth of bone ingrowth into the cylinders was respectively 1.4 mm for the pore size and 1.59 mm for the µm pore size. After six months, new bone tissue reached the centre of the implants with the three highest pore size intervals. Degradation of the ceramic was about 5%. At 12 months, the surface of the ceramic was almost completely colonised by the newly formed bone. There was still a statistically (p < 0.05) lower bone ingrowth in the µm pore size in comparison with the others. The percentage of ceramic resorption was limited to 10%. In the control hole, fibrous tissue was still visible in its centre. b-tricalcium phosphate (fig 4 and 5) At two weeks, implants of b-tcp were already colonised by the newly formed bone, even those with the smallest pore size (21%).
4 BONE INGROWTH INTO TWO POROUS CERAMICS 601 b-tricalcium phrosphate Fig. 4. Percentage of bone ingrowth into the TCP implant Fig. 5. Stained section (Solochrome-cyanine R) after 12 months of implantation of the TCP ceramic. Note partial resorption of the TCP and bone ingrowth on the surface. One month following implantation, the percentage of bone ingrowth increased with the pore size (23%, 67%, 80% and 79% respectively). All values were significantly higher in the three highest pore size ranges compared with the smallest (p < 0.05). Nevertheless, there were no statistical differences between the , and µm pore size ranges. The evolution of the depth of new bone formation was similar to the percentages with values superior to 1 mm for the three highest pore size ranges. Fibrous tissue was present within the control cavity, without any bone formation. At two and four months, the trend was similar. Bone ingrowth reached more than 90%. At six months, no difference was noted regarding bone ingrowth for all pore size ranges. The whole surface of the implant was colonised by newly formed bone. Implant resorption was about 30%. At 12 months, the amount of newly formed bone was unchanged. No statistical difference could be noted between the various pore size ranges. The percentage of bone ingrowth was 96-98%. The degradation of the ceramic was about 60%. Comparison of HA and b-tcp The b-tcp was colonised faster and at a higher rate than the HA. Whereas a statistical difference in bone ingrowth continued to be noted for the HA implants between the µm pore size and the three higher pore sizes whatever the implantation time, no such difference could be noted beyond four months for the b-tcp. In fact, a pore size superior to 80 µm seems to promote bone and tissue ingrowth at the beginning. Data related to the depth of bone ingrowth paralleled those related to the percentage of bony ingrowth. Ceramic resorption reached 60% for b-tcp and only 10% for HA at 12 months. DISCUSSION During the past ten years there has been an increased use of bone substitutes with numerous products available in orthopaedic surgery (4). One of the most common synthetic alternatives to autologous bone graft, the gold standard, is calci-
5 602 L. GALOIS, D. MAINARD um phosphate ceramics, such as HA or b-tcp, the most widely used materials, because of their absence of toxicity, their biocompatibility, and their osteoconductivity permitting the creeping substitution process. The success of calcium phosphate ceramics depends on the formation of healing bone tissue that will bring about the incorporation of the implant. The important feature in the physical structure of a synthetic ceramic is its porosity. Pore size, volume of porosity and interconnections between the pores are three crucial parameters (8). Pore structure is of great importance for osteoconduction (9). Cell colonisation and bone ingrowth apparently occur for a minimal macropore size, not quite defined yet, and a reduction in macroporosity may have negative results for osseointegration. Many studies have shown the relationship between bone ingrowth and pore parameters, particularly the percentage of porosity, the pore size and the degree of pore interconnectivity (16, 23, 27), but these studies also report confusing data on porosity, so that optimal macroporosity parameters have not yet been defined. Cell ingrowth into porous ceramic is, in fact, not well understood. It is generally accepted that µm is the minimal pore size for osteoconduction (3, 24, 26). Nevertheless, intervals mentioned in the literature are very variable. Bobyn et al (1) have shown that a pore size of µm was recommended to provide bone ingrowth into metallic implants. Hulbert et al (16) showed optimal bone ingrowth into µm ceramic, but also demonstrated that interconnection between pores was a more crucial parameter than the pore size itself. Flautre et al (8) demonstrated the important role of both interconnection size and pore size ; the best osteoconduction in HA was obtained with a 130-µm interconnection size and a 175-to 260-µm mean pore size. Uchida et al (26) showed better osteointegration with pore size greater than 200 µm. Finally, in the literature, a pore size below 80 µm seems to be critical for osteoprogenitor cells to penetrate into the pores. Nevertheless, in our study bone ingrowth into ceramic with µm pore size was possible, but it was delayed compared to the higher pore size ranges. Another study conducted by Eggli et al (7) had already reported notable bone ingrowth for pores smaller than 100 µm. An explanation for their results was the number of interconnections, greater in small pores than in large pores. Our results indicate that a pore size above 80 µm is recommended to accelerate and to improve the bony ingrowth within the ceramic. Nevertheless, we did not find any statistical difference in osseointegration between the three higher pore size ranges : , and µm. The optimum pore size could be defined as the interval µm, according to our results. Pores of more than 500 µm diameter seem to be too large, and seem to discourage bone ingrowth (21). The nature of the ceramic also influences bone formation. We found that bony ingrowth occurred quicker and at a higher rate within b-tcp implants than within HA implants. The high resorption potential of b-tcp, compared to the poor resorption of HA, will leave larger space for the newly formed bone (20). This different resorption rate, correlated with the Ca/P ratio, can explain the difference in bony ingrowth into both ceramics. Moreover, the pore size itself also seems to play an important role in the bone ingrowth process, as demonstrated by Gauthier et al (11). Whether or not a calcium phosphate ceramic used as a bone substitute will succeed depends on the formation of healing bone tissue that will bring about the incorporation of the implant. In the biological, biochemical and physiochemical parameters involved, the pore size is a crucial parameter. The level of porosity, pore size distribution and degree of pore interconnectivity significantly influence the extent of bone ingrowth. Macroporous calcium phosphates, in particular HA and b-tcp, have achieved considerable success as bone graft substitute materials. Our findings suggest that b-tcp with an optimum pore size of µm is the most suitable ceramic for filling bone defects. REFERENCES 1. Bobyn JD, Pilliar RM, Cameron HU, Weatherly GC. The optimum pore size for the fixation of porous-surfaced metal implants by the ingrowth of bone. Clin Orthop 1980 ; 150 : Cheung HS, Haak MH. Growth of osteoblasts on porous calcium phosphate ceramic : An in vitro model for biocompatibility study. Biomaterials 1989 ; 10 :
6 BONE INGROWTH INTO TWO POROUS CERAMICS Daculsi G, Passuti N. Effect of the macroporosity for osseous substitution of calcium phosphate ceramics. Biomaterials 1990 ; 11 : Delloye C, Cnockaert N, Cornu O. Bone substitutes in 2003 : An overview. Acta Orthop Belg 2003 ; 69 : de Groot K. Effect of porosity and physicochemical properties on the stability, resorption and strength of calcium phosphate ceramics. In : Ducheyne P, Lemons J (eds). Bioceramics, New York Acad Sci, Boca Raton, 1998, pp de Peretti F, Trojani C, Cambas PM, et al. Coral as support of traumatic articular compression. A prospective study of 23 cases involving the lower limb. Rev Chir Orthop 1996 ; 82 : Eggli PS, Muller W, Schenk RK. Porous hydroxyapatite and tricalcium phosphate cylinders with two different pore size ranges implanted in the cancellous bone of rabbits. A comparative histomorphometric and histologic study of bony ingrowth and implant substitution. Clin Orthop 1988 ; 232 : Flautre B, Descamps M, Delecourt C et al. Porous HA ceramic for bone replacement : Role of the pores and interconnections : Experimental study in the rabbit. J Mat Sci Mat Med 2001 ; 12 : Frayssinet P, Mathon D, Lerch A et al. Osseointegration of composite calcium phosphate bioceramics. J Biomed Mater Res 2000 ; 50 : Galois L, Mainard D, Delagoutte JP. Beta-tricalcium phosphate ceramic as a bone substitute in orthopaedic surgery. Int Orthop 2002 ; 26 : Gauthier O, Bouler JM, Aguado E et al. Macroporous biphasic calcium phosphate ceramics : Influence of macropore diameter and macroporosity percentage on bone ingrowth. Biomaterials 1998 ; 19 : Gouin F, Delecrin J, Passuti N et al. Filling of bone defects using biphasic macroporous calcium phosphate ceramic. A propos of 23 cases. Rev Chir Orthop 1995 ; 81 : Hahn M, Vogel M, Delling G. Undecalcified preparation of bone tissue : Report of technical experience and development of new methods. Virchows Arch Pathol Anat Histopathol 1991 ; 418 : Heise U, Osborn JF, Duwe F. Hydroxyapatite ceramic as a bone substitute. Int Orthop 1990 ; 14 : Holmes RE, Bucholz RW, Mooney V. Porous hydroxyapatite as a bone-graft substitute in metaphyseal defects. A histometric study. J Bone Joint Surg 1986 ; 68-A : Hulbert SF, Young FA, Mathews RS et al. Potential of ceramic materials as permanently implantable skeletal prostheses. J Biomed Mater Res 1970 ; 4 : Johnson KD, Frierson KE, Keller TS et al. Porous ceramics as bone graft substitutes in long bone defects : A biomechanical, histological, and radiographic analysis. J Orthop Res 1996 ; 14 : Kitsugi T, Yamamuro T, Nakamura T et al. Four calcium phosphate ceramics as bone substitutes for nonweight-bearing. Biomaterials 1993 ; 14 : Klein CP, Patka P, den Hollander W. Macroporous calcium phosphate bioceramics in dog femora : A histological study of interface and biodegradation. Biomaterials 1989 ; 10 : Koerten HK, van der Meulen J. Degradation of calcium phosphate ceramics. J Biomed Mater Res 1999 ; 44 : Le Huec JC, Clément D, Lesprit E, Faber J. The use of calcium phosphates, their biological properties. Eur J Orthop Surg Traumatol 2000 ; 10 : Le Huec JC, Lesprit E, Delavigne C et al. Tri-calcium phosphate ceramics and allografts as bone substitutes for spinal fusion in idiopathic scoliosis : Comparative clinical results at four years. Acta Orthop Belg 1997 ; 63 : Schliephake H, Neukam FW, Klosa D. Influence of pore dimensions on bone ingrowth into porous hydroxylapatite blocks used as bone graft substitutes. A histometric study. Int J Oral Maxillofac Surg 1991 ; 20 : Shimazaki K, Mooney V. Comparative study of porous hydroxyapatite and tricalcium phosphate as bone substitute. J Orthop Res 1985 ; 3 : Summers BN, Eisenstein SM. Donor site pain from the ilium. A complication of lumbar spine fusion. J Bone Joint Surg 1989 ; 71-B : Uchida A, Nade S, McCartney E, Ching W. Bone ingrowth into three different porous ceramics implanted into the tibia of rats and rabbits. J Orthop Res 1985 ; 3 : van Blitterswijk CA, Grote JJ, Kuijpers W et al. Macropore tissue ingrowth : A quantitative and qualitative study on hydroxyapatite ceramic. Biomaterials 1986 ; 7 :
synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D.
 C E L L P L E X TCP synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D. TECHNICAL MONOGRAPH CELLPLEX TCP SYNTHETIC CANCELLOUS BONE CELLPLEX TCP synthetic CANCELLOUS BONE introduction
C E L L P L E X TCP synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D. TECHNICAL MONOGRAPH CELLPLEX TCP SYNTHETIC CANCELLOUS BONE CELLPLEX TCP synthetic CANCELLOUS BONE introduction
In Vivo Evaluation of BioSphere Bioactive Bone Graft Putty: Improved Bone Formation
 In Vivo Evaluation of BioSphere Bioactive Bone Graft : Improved Bone Formation ABSTRACT BioSphere is a novel bone graft product that was developed using spherical particles of bioactive glass with a narrow,
In Vivo Evaluation of BioSphere Bioactive Bone Graft : Improved Bone Formation ABSTRACT BioSphere is a novel bone graft product that was developed using spherical particles of bioactive glass with a narrow,
Biomaterials Line. MIS Corporation. All Rights Reserved.
 7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute.
 chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
BIOACTIVE SYNTHETIC GRAFT
 B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
chronos Synthetic cancellous bone graft substitute ( -tricalcium phosphate) Remodels Replaced by bone in 6 18 months Easy to use
 Synthetic cancellous bone graft substitute ( -tricalcium phosphate) Remodels Replaced by bone in 6 18 months Easy to use Granules, blocks, wedges, cylinders Safe Synthetic origin provides unsurpassed safety
Synthetic cancellous bone graft substitute ( -tricalcium phosphate) Remodels Replaced by bone in 6 18 months Easy to use Granules, blocks, wedges, cylinders Safe Synthetic origin provides unsurpassed safety
experts in bone regeneration Spine Surgery Product Line When Innovation Meets Performance
 experts in bone regeneration Spine Surgery Product Line When Innovation Meets Performance At the core of all our products: Our proprietary MBCP Technology Over 650 published studies, 30 years of clinical
experts in bone regeneration Spine Surgery Product Line When Innovation Meets Performance At the core of all our products: Our proprietary MBCP Technology Over 650 published studies, 30 years of clinical
Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study
 Journal of Orthopaedic Surgery 2010;18(1):63-7 Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study Hiroyuki Hattori, Hiroaki Matsuoka,
Journal of Orthopaedic Surgery 2010;18(1):63-7 Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study Hiroyuki Hattori, Hiroaki Matsuoka,
BONE void FILLER. Beta-tricalcium phosphate ( b-tcp) bone graft substitute. OvERvIEW BROCHURE
 chronos BONE void FILLER Beta-tricalcium phosphate ( b-tcp) bone graft substitute OvERvIEW BROCHURE chronos STRIP chronos Strip is a synthetic bone void filler manufactured from chronos Beta-Tricalcium
chronos BONE void FILLER Beta-tricalcium phosphate ( b-tcp) bone graft substitute OvERvIEW BROCHURE chronos STRIP chronos Strip is a synthetic bone void filler manufactured from chronos Beta-Tricalcium
Inion BioRestore. Bone Graft Substitute. Product Overview
 Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
easy-graft TM CRYSTAL
 1 easy-graft TM CRYSTAL Overview 2 Advantages easy-graft : principle & application Material & studies Indications easy-graft CRYSTAL & CLASSIC Advantages of easy-graft CRYSTAL 3 Easy handling: Injectable
1 easy-graft TM CRYSTAL Overview 2 Advantages easy-graft : principle & application Material & studies Indications easy-graft CRYSTAL & CLASSIC Advantages of easy-graft CRYSTAL 3 Easy handling: Injectable
Choice of spacer material for HTO! P. Landreau, MD Chief of Surgery Aspetar, Orthopaedic and Sports Medicine Hospital Doha, Qatar
 Choice of spacer material for HTO! P. Landreau, MD Chief of Surgery Aspetar, Orthopaedic and Sports Medicine Hospital Doha, Qatar High Tibial Osteotomy: HTO! Valgisation HTO Intended to transfer the mechanical
Choice of spacer material for HTO! P. Landreau, MD Chief of Surgery Aspetar, Orthopaedic and Sports Medicine Hospital Doha, Qatar High Tibial Osteotomy: HTO! Valgisation HTO Intended to transfer the mechanical
B U I L D S T R O N G B O N E F A S T
 B U I L D S T R O N G B O N E F A S T Putty MIS Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
B U I L D S T R O N G B O N E F A S T Putty MIS Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
The Outcome of Bone Substitute Wedges in Medial Opening High Tibial Osteotomy
 Send Orders for Reprints to reprints@benthamscience.net The Open Orthopaedics Journal, 2013, 7, 373-377 373 Open Access The Outcome of Bone Substitute Wedges in Medial Opening High Tibial Osteotomy N.M.
Send Orders for Reprints to reprints@benthamscience.net The Open Orthopaedics Journal, 2013, 7, 373-377 373 Open Access The Outcome of Bone Substitute Wedges in Medial Opening High Tibial Osteotomy N.M.
Properties of GENESYS TM Biocomposite Material Compared to Pure Polylactide (PLA)
 Properties of GENESYS TM Biocomposite Material Compared to Pure Polylactide (PLA) Purpose: To compare the bone in-growth of GENESYS biocomposite material (96L/4D PLA copolymer mixed with β-tcp micro-particles)
Properties of GENESYS TM Biocomposite Material Compared to Pure Polylactide (PLA) Purpose: To compare the bone in-growth of GENESYS biocomposite material (96L/4D PLA copolymer mixed with β-tcp micro-particles)
Technique Guide. chronos Strip. Osteoconductive betatricalcium phosphate ( -TCP) composite.
 Technique Guide chronos Strip. Osteoconductive betatricalcium phosphate ( -TCP) composite. Table of Contents Introduction chronos Strip 2 Indications and Contraindications 3 Surgical Technique Preparation
Technique Guide chronos Strip. Osteoconductive betatricalcium phosphate ( -TCP) composite. Table of Contents Introduction chronos Strip 2 Indications and Contraindications 3 Surgical Technique Preparation
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Calcium Phosphate Cement
 Calcium Phosphate Cement Fast-Setting Bone Graft and AutoGraft Extender. * Ossilix is a high performance next generation calcium phosphate cement indicated for filling bony defects in cancellous bone.
Calcium Phosphate Cement Fast-Setting Bone Graft and AutoGraft Extender. * Ossilix is a high performance next generation calcium phosphate cement indicated for filling bony defects in cancellous bone.
Incorporation and biodegradation of hydroxyapatite tricalcium phosphate implanted in large metaphyseal defects An animal study
 Indian Journal of Experimental Biology Vol. 46, December 008, pp. 836-841 Incorporation and biodegradation of hydroxyapatite tricalcium phosphate implanted in large metaphyseal defects An animal study
Indian Journal of Experimental Biology Vol. 46, December 008, pp. 836-841 Incorporation and biodegradation of hydroxyapatite tricalcium phosphate implanted in large metaphyseal defects An animal study
BEGO BIOMATERIALS When the result counts
 BEGO BIOMATERIALS When the result counts Partners in Progress INTRO Challenge what exists get the right answers We practise systematic thinking with a passion and we are never satisfied with the status
BEGO BIOMATERIALS When the result counts Partners in Progress INTRO Challenge what exists get the right answers We practise systematic thinking with a passion and we are never satisfied with the status
Radiology Case Reports. Bone Graft Extruded From an Intramedullary Nail Tract in the Tibia. Penelope J. Galbraith, M.D., and Felix S. Chew, M.D.
 Radiology Case Reports Volume 2, Issue 4, 2007 Bone Graft Extruded From an Intramedullary Nail Tract in the Tibia Penelope J. Galbraith, M.D., and Felix S. Chew, M.D. A 33-year-old man presented for follow
Radiology Case Reports Volume 2, Issue 4, 2007 Bone Graft Extruded From an Intramedullary Nail Tract in the Tibia Penelope J. Galbraith, M.D., and Felix S. Chew, M.D. A 33-year-old man presented for follow
Allograft Bone and Super Critical Fluid (SCF) Technology
 Allograft Bone and Super Critical Fluid (SCF) Technology Summary: 1. Supercritical Fluids (SCF) have the properties of a gas and a liquid when it is in its supercritical state; 2. SCF treatment provides
Allograft Bone and Super Critical Fluid (SCF) Technology Summary: 1. Supercritical Fluids (SCF) have the properties of a gas and a liquid when it is in its supercritical state; 2. SCF treatment provides
Electron Beam Melting EBM
 Cup Fixa Cup Fixa The uncemented cup with equatorial primary press-fit fixation is considered to be the best solution for prosthesis surgery of the acetabulum. In addition to exploiting this safe mechanical
Cup Fixa Cup Fixa The uncemented cup with equatorial primary press-fit fixation is considered to be the best solution for prosthesis surgery of the acetabulum. In addition to exploiting this safe mechanical
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH
 PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
ACL reconstruction. Osteoconductive absorbable interference screws. Unique material. Optimal design. Adapted to different surgical techniques
 ACL reconstruction Osteoconductive absorbable interference screws Unique material Optimal design Adapted to different surgical techniques + complete instrumentation set Controlled resorption Material LIGAFIX
ACL reconstruction Osteoconductive absorbable interference screws Unique material Optimal design Adapted to different surgical techniques + complete instrumentation set Controlled resorption Material LIGAFIX
Graftys. Cross-selling. Indications. Comparison. Basic Science. Graftys 415 rue Claude Nicolas Ledoux Aix en Provence Cedex 4
 2015 Graftys Cross-selling Indications Comparison Graftys 415 rue Claude Nicolas Ledoux 13854 Aix en Provence Cedex 4 www.graftys.com Basic Science Graftys QuickSet Training 1 Where to use QuickSet? Revision
2015 Graftys Cross-selling Indications Comparison Graftys 415 rue Claude Nicolas Ledoux 13854 Aix en Provence Cedex 4 www.graftys.com Basic Science Graftys QuickSet Training 1 Where to use QuickSet? Revision
chronos VIVIFY PREFORMS AND chronos GRANULES BONE VOID FILLER
 chronos VIVIFY PREFORMS AND chronos GRANULES BONE VOID FILLER Beta-Tricalcium Phosphate (ß-TCP) bone graft substitute Instruments and implants approved by the AO Foundation. This publication is not intended
chronos VIVIFY PREFORMS AND chronos GRANULES BONE VOID FILLER Beta-Tricalcium Phosphate (ß-TCP) bone graft substitute Instruments and implants approved by the AO Foundation. This publication is not intended
NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE
 NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE THE PROBLEMS Fixation failure Malunion F 83 yrs 2 Months 6 Months F 81 yrs 3 Months FIXATION AUGMENTATION TECHNIQUES (FATs) Surgical procedures aimed at increasing
NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE THE PROBLEMS Fixation failure Malunion F 83 yrs 2 Months 6 Months F 81 yrs 3 Months FIXATION AUGMENTATION TECHNIQUES (FATs) Surgical procedures aimed at increasing
Evaluation of New Biphasic Calcium Phosphate Bone Substitute: Rabbit Femur Defect Model and Preliminary Clinical Results
 J. Med. Biol. Eng. (2017) 37:85 93 DOI 10.1007/s40846-016-0203-3 ORIGINAL ARTICLE Evaluation of New Biphasic Calcium Phosphate Bone Substitute: Rabbit Femur Defect Model and Preliminary Clinical Results
J. Med. Biol. Eng. (2017) 37:85 93 DOI 10.1007/s40846-016-0203-3 ORIGINAL ARTICLE Evaluation of New Biphasic Calcium Phosphate Bone Substitute: Rabbit Femur Defect Model and Preliminary Clinical Results
BioVin Collagen Membrane
 BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
Bone Void Filler. Callos. The Next Generation in Calcium Phosphate Cement A COLSON ASSOCIATE
 Callos Bone Void Filler The Next Generation in Calcium Phosphate Cement A COLSON ASSOCIATE Callos Calcium Phosphate Cement Callos is a high performance next generation calcium phosphate cement indicated
Callos Bone Void Filler The Next Generation in Calcium Phosphate Cement A COLSON ASSOCIATE Callos Calcium Phosphate Cement Callos is a high performance next generation calcium phosphate cement indicated
CELLPLEX TCP SYNTHETIC CANCELLOUS BONE
 CELLPLEX TCP SYNTHETIC CANCELLOUS BONE 129257-9 The following languages are included in this packet: English (en) Deutsch (de) Nederlands (nl) Français (fr) Español (es) Italiano (it) Português (pt) -
CELLPLEX TCP SYNTHETIC CANCELLOUS BONE 129257-9 The following languages are included in this packet: English (en) Deutsch (de) Nederlands (nl) Français (fr) Español (es) Italiano (it) Português (pt) -
THE ESSENTIALS IN BONE GRAFTING BRIDGING MEDICAL GAPS
 THE ESSENTIALS IN BONE GRAFTING BRIDGING MEDICAL GAPS FAST FACTS Clean and sterile, free of human, animal and chemical material. Products can be custom ordered, ranging from pastes and cements to granulations
THE ESSENTIALS IN BONE GRAFTING BRIDGING MEDICAL GAPS FAST FACTS Clean and sterile, free of human, animal and chemical material. Products can be custom ordered, ranging from pastes and cements to granulations
A WIDE RANGE OF REGENERATIVE SOLUTIONS
 A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
Bone Marrow Autograft Associated to Macroporous Biphasic Calcium Phosphate for Bone Substitution in an Animal Model of Sequels of Radiotherapy
 Key Engineering Materials Online: 2005-04-15 ISSN: 1662-9795, Vols. 284-286, pp 285-288 doi:10.4028/www.scientific.net/kem.284-286.285 2005 Trans Tech Publications, Switzerland Bone Marrow Autograft Associated
Key Engineering Materials Online: 2005-04-15 ISSN: 1662-9795, Vols. 284-286, pp 285-288 doi:10.4028/www.scientific.net/kem.284-286.285 2005 Trans Tech Publications, Switzerland Bone Marrow Autograft Associated
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
Comblements osseux par céramique phosphocalcique biphasée macroporeuse A propos de 23 cas
 Revue de Chirurgie Orthopédique Masson, Paris, 1995. 1995, 81, 59-65. MÉMOIRE Comblements osseux par céramique phosphocalcique biphasée macroporeuse A propos de 23 cas Biphasic macroporous calcium phosphate
Revue de Chirurgie Orthopédique Masson, Paris, 1995. 1995, 81, 59-65. MÉMOIRE Comblements osseux par céramique phosphocalcique biphasée macroporeuse A propos de 23 cas Biphasic macroporous calcium phosphate
Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier. MEDLINEUNITE Bioactive Bone Graft
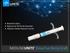 Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier Principles of Bone Healing Reparative Phase Healing Cascade 1. Cellular infiltration and migration to site (fibroblasts, macrophages,
Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier Principles of Bone Healing Reparative Phase Healing Cascade 1. Cellular infiltration and migration to site (fibroblasts, macrophages,
Comparative Animal Study of OssiMend and Healos 13,14
 Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
Versatile grafting Solutions
 Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
REASONS TO USE R.T.R.
 3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management 1 Regeneration Bone Grafting & Soft Tissue Management Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON Collagen 5 6
Regeneration Bone Grafting & Soft Tissue Management 1 Regeneration Bone Grafting & Soft Tissue Management Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON Collagen 5 6
The long term fate of the fibula when used as an intraosseous graft
 Acta Orthop. Belg., 2004, 70, 322-326 The long term fate of the fibula when used as an intraosseous graft Onkar N. NAGI, Mandeep S. DHILLON, Sameer AGGARWAL From the Post Graduate Institute of Medical
Acta Orthop. Belg., 2004, 70, 322-326 The long term fate of the fibula when used as an intraosseous graft Onkar N. NAGI, Mandeep S. DHILLON, Sameer AGGARWAL From the Post Graduate Institute of Medical
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
An Assessment of Fate of CHA Blocks Used in the Cystic Lesions of Bone.
 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 An Assessment of Fate of CHA Blocks Used in the Cystic Lesions of Bone. Pervaind Sharma 1, Asif Iqbal 2, Najmul Huda 3, Ajay Pant 4 1 Associate Professor,
Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 An Assessment of Fate of CHA Blocks Used in the Cystic Lesions of Bone. Pervaind Sharma 1, Asif Iqbal 2, Najmul Huda 3, Ajay Pant 4 1 Associate Professor,
Bone Grafting and Bone Graft Substitutes. Original Author: James Krieg, MD Revision Author: David Hak, MD Last Revision May 2010
 Bone Grafting and Bone Graft Substitutes Original Author: James Krieg, MD Revision Author: David Hak, MD Last Revision May 2010 Bone Graft Function Structural support of articular fracture Tibial plateau
Bone Grafting and Bone Graft Substitutes Original Author: James Krieg, MD Revision Author: David Hak, MD Last Revision May 2010 Bone Graft Function Structural support of articular fracture Tibial plateau
Developments in bone grafting in veterinary orthopaedics part one
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
botiss biomaterials bone & tissue regeneration collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
Examination of Porous-Coated Patellar Components and Analysis of the Reasons for Their Retrieval
 Examination of Porous-Coated Patellar Components and Analysis of the Reasons for Their Retrieval J. P. Collier,* M. B. Mayor,+ V. A. Surprenant,* H. P. Surprenant,* and R.E. Jensen* *Dartmouth Biomedical
Examination of Porous-Coated Patellar Components and Analysis of the Reasons for Their Retrieval J. P. Collier,* M. B. Mayor,+ V. A. Surprenant,* H. P. Surprenant,* and R.E. Jensen* *Dartmouth Biomedical
AttraX. Portfolio. Surface Drives Performance
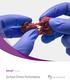 Portfolio Surface Drives Performance Advanced Biomaterial Microarchitecture Drives Bone Formation Traditional calcium phosphate materials generally do not give rise to bone formation when implanted in
Portfolio Surface Drives Performance Advanced Biomaterial Microarchitecture Drives Bone Formation Traditional calcium phosphate materials generally do not give rise to bone formation when implanted in
Bone formation and osseointegration with titanium implant using granular- and block-type porous hydroxyapatite ceramics (IP-CHA)
 Dental Materials Journal 2013; 32(5): 753 760 Bone formation and osseointegration with titanium implant using granular- and block-type porous hydroxyapatite ceramics (IP-CHA) Masahiko MINAMI, Masaaki TAKECHI,
Dental Materials Journal 2013; 32(5): 753 760 Bone formation and osseointegration with titanium implant using granular- and block-type porous hydroxyapatite ceramics (IP-CHA) Masahiko MINAMI, Masaaki TAKECHI,
Graftys R&D Team. Summary of Preclinical data for Calcium Phosphate. products: Graftys HBS and Graftys QuickSet. A Graftys preclinical studies Review
 Summary of Preclinical data for Calcium Phosphate products: HBS and QuickSet R&D Team 2011 A preclinical studies Review By Florian Boukhechba (contact: florian.boukhechba@graftys.fr) Special acknowledgment
Summary of Preclinical data for Calcium Phosphate products: HBS and QuickSet R&D Team 2011 A preclinical studies Review By Florian Boukhechba (contact: florian.boukhechba@graftys.fr) Special acknowledgment
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
THE NEXT FRONTIER OF BONE REGENERATION
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
MASTERGRAFT Putty. Technical Guide
 MASTERGRAFT Putty Technical Guide MASTERGRAFT Putty is a malleable-cohesive, osteoconductive scaffold composed of collagen that is physically mixed with resorbable ceramic granules. Mixing Process Collagen
MASTERGRAFT Putty Technical Guide MASTERGRAFT Putty is a malleable-cohesive, osteoconductive scaffold composed of collagen that is physically mixed with resorbable ceramic granules. Mixing Process Collagen
HYDROXYAPATITE IN REVISION OF TOTAL HIP REPLACEMENTS WITH MASSIVE ACETABULAR DEFECTS
 HYDROXYAPATITE IN REVISION OF TOTAL HIP REPLACEMENTS WITH MASSIVE ACETABULAR DEFECTS 4- TO 10-YEAR CLINICAL RESULTS H. OONISHI, Y. IWAKI, N. KIN, S. KUSHITANI, N. MURATA, S. WAKITANI, K. IMOTO From Osaka-Minami
HYDROXYAPATITE IN REVISION OF TOTAL HIP REPLACEMENTS WITH MASSIVE ACETABULAR DEFECTS 4- TO 10-YEAR CLINICAL RESULTS H. OONISHI, Y. IWAKI, N. KIN, S. KUSHITANI, N. MURATA, S. WAKITANI, K. IMOTO From Osaka-Minami
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
Talos -C (HA) and the PEEK-OPTIMA HA Enhanced Technology
 v Talos -C (HA) and the HA Enhanced Technology The innovative Talos -C (HA) IBF Implant made with polymer is fully integrated with the well known material Hydroxyapatite (HA). The Talos -C (HA) IBF Implant
v Talos -C (HA) and the HA Enhanced Technology The innovative Talos -C (HA) IBF Implant made with polymer is fully integrated with the well known material Hydroxyapatite (HA). The Talos -C (HA) IBF Implant
botiss dental bone & tissue regeneration biomaterials collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
chronos STRIP Bone Void Filler
 chronos STRIP Bone Void Filler Osteoconductive beta-tricalcium phosphate (b-tcp) composite This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION
chronos STRIP Bone Void Filler Osteoconductive beta-tricalcium phosphate (b-tcp) composite This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION
TRABECULAR METAL ACETABULAR RESTRICTOR AND AUGMENT. Surgical Technique
 TRABECULAR METAL ACETABULAR RESTRICTOR AND AUGMENT Surgical Technique ACETABULAR ASSESSMENT AND PREPARATION Intra-operatively, carefully assess any acetabular bone defects present. Note the location, extent,
TRABECULAR METAL ACETABULAR RESTRICTOR AND AUGMENT Surgical Technique ACETABULAR ASSESSMENT AND PREPARATION Intra-operatively, carefully assess any acetabular bone defects present. Note the location, extent,
experts in bone regeneration Osteotwin Sports Surgery Line When Innovation Meets Performance
 experts in bone regeneration Osteotwin Sports Surgery Line When Innovation Meets Performance Sports Surgery Line For more than 20 years, our philosophy has been to develop performing and safe solutions
experts in bone regeneration Osteotwin Sports Surgery Line When Innovation Meets Performance Sports Surgery Line For more than 20 years, our philosophy has been to develop performing and safe solutions
PINNACLE REVISION CUP SYSTEM
 PINNACLE REVISION CUP SYSTEM This publication is not intended for distribution in the USA. DESIGN RATIONALE FLEXIBILITY. PRECISION. CONFIDENCE. DePuy Synthes Joint Reconstruction is proud to offer the
PINNACLE REVISION CUP SYSTEM This publication is not intended for distribution in the USA. DESIGN RATIONALE FLEXIBILITY. PRECISION. CONFIDENCE. DePuy Synthes Joint Reconstruction is proud to offer the
BCP SURFACE TREATMENT
 Biocompatibility. Cleanliness. Osseointegration BCP SURFACE TREATMENT Pure like nature* 2 THE CORNERSTONE OF A SUCCESSFUL D Promoting fast and effective osseointegration through optimized surface energy!
Biocompatibility. Cleanliness. Osseointegration BCP SURFACE TREATMENT Pure like nature* 2 THE CORNERSTONE OF A SUCCESSFUL D Promoting fast and effective osseointegration through optimized surface energy!
Bone Regeneration in a Bilateral Sinus Lift
 2 A comparative pilot case study between irradiated human cancellous bone and a synthetic analogue Bone Regeneration in a Bilateral Sinus Lift Anthony McGee, BDS, Staines, and Dr J. A. Hunt, Liverpool/England
2 A comparative pilot case study between irradiated human cancellous bone and a synthetic analogue Bone Regeneration in a Bilateral Sinus Lift Anthony McGee, BDS, Staines, and Dr J. A. Hunt, Liverpool/England
ADVANCED BONE GRAFT SYSTEM OVERVIEW
 ADVANCED BONE GRAFT SYSTEM OVERVIEW NANOSS BIOACTIVE ADVANCED BONE GRAFT Table Of Contents INTRODUCTION System Overview... 1 NANOSS BIOACTIVE COMPONENTS Comparison of nanoss Bioactive and Human Bone...
ADVANCED BONE GRAFT SYSTEM OVERVIEW NANOSS BIOACTIVE ADVANCED BONE GRAFT Table Of Contents INTRODUCTION System Overview... 1 NANOSS BIOACTIVE COMPONENTS Comparison of nanoss Bioactive and Human Bone...
Over 20 Years of Proven Clinical Success. Zimmer Natural-Knee II System
 Over 20 Years of Proven Clinical Success Zimmer Natural-Knee II System CSTi Porous Coating Structurally similar to human bone CSTi porous coating combines the excellent biocompatibility of titanium with
Over 20 Years of Proven Clinical Success Zimmer Natural-Knee II System CSTi Porous Coating Structurally similar to human bone CSTi porous coating combines the excellent biocompatibility of titanium with
Case Report Use of a fully-resorbable, biomimetic composite hydroxyapatite as bone graft substitute for posterolateral spine fusion: a case report
 Int J Clin Exp Med 2016;9(11):22458-22462 www.ijcem.com /ISSN:1940-5901/IJCEM0032882 Case Report Use of a fully-resorbable, biomimetic composite hydroxyapatite as bone graft substitute for posterolateral
Int J Clin Exp Med 2016;9(11):22458-22462 www.ijcem.com /ISSN:1940-5901/IJCEM0032882 Case Report Use of a fully-resorbable, biomimetic composite hydroxyapatite as bone graft substitute for posterolateral
Cerasorb M DENTAL. O:\Zulassung\Cerasorb Dental Kanada 2013\Texte\Cerasorb M Dental final IFU docx
 Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
The use of unidirectional porous β-tricarcium phosphate in surgery for calcaneal fractures: A report of four cases
 The use of unidirectional porous β-tricarcium phosphate in surgery for calcaneal fractures: A report of four cases by Shigeo Izawa 1*, Toru Funayama 2, Masashi Iwasashi 1, Toshinori Tsukanishi 3, Hiroshi
The use of unidirectional porous β-tricarcium phosphate in surgery for calcaneal fractures: A report of four cases by Shigeo Izawa 1*, Toru Funayama 2, Masashi Iwasashi 1, Toshinori Tsukanishi 3, Hiroshi
Asymmetrical bilateral shoulder dislocation
 Asymmetrical bilateral shoulder dislocation Laurent Galois ( ), Régis Traversari, Damien Girard, Didier Mainard and Jean Pierre Delagoutte Department of Orthopaedic and Trauma Surgery, University Hospital
Asymmetrical bilateral shoulder dislocation Laurent Galois ( ), Régis Traversari, Damien Girard, Didier Mainard and Jean Pierre Delagoutte Department of Orthopaedic and Trauma Surgery, University Hospital
Research Article Evaluation of Amniotic-Derived Membrane Biomaterial as an Adjunct for Repair of Critical Sized Bone Defects
 Advances in Orthopedic Surgery, Article ID 572586, 4 pages http://dx.doi.org/10.1155/2014/572586 Research Article Evaluation of Amniotic-Derived Membrane Biomaterial as an Adjunct for Repair of Critical
Advances in Orthopedic Surgery, Article ID 572586, 4 pages http://dx.doi.org/10.1155/2014/572586 Research Article Evaluation of Amniotic-Derived Membrane Biomaterial as an Adjunct for Repair of Critical
Trabecular Metal Acetabular Restrictor and Augment
 Trabecular Metal Acetabular Restrictor and Augment Surgical Technique The Best Thing Next To Bone Trabecular Metal Acetabular Restrictor and Augment Acetabular Assessment and Preparation Intra-operatively,
Trabecular Metal Acetabular Restrictor and Augment Surgical Technique The Best Thing Next To Bone Trabecular Metal Acetabular Restrictor and Augment Acetabular Assessment and Preparation Intra-operatively,
THE NEXT FRONTIER OF BONE REGENERATION
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
Hedrocel trabecular metal monoblock acetabular cups : mid-term results
 Acta Orthop. Belg., 2006, 72, 326-331 ORIGINAL STUDY Hedrocel trabecular metal monoblock acetabular cups : mid-term results Michiel MULIER, Bart RYS, Lieven MOKE From the University Hospital Pellenberg,
Acta Orthop. Belg., 2006, 72, 326-331 ORIGINAL STUDY Hedrocel trabecular metal monoblock acetabular cups : mid-term results Michiel MULIER, Bart RYS, Lieven MOKE From the University Hospital Pellenberg,
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
THE NEXT GENERATION OF REGENERATION
 THE NEXT GENERATION OF REGENERATION Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption.
THE NEXT GENERATION OF REGENERATION Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption.
Trabecular Metal Acetabular Revision System Buttress and Shim Augments Surgical Technique
 Trabecular Metal Acetabular Revision System Buttress and Shim Augments Surgical Technique Trabecular Metal Acetabular Revision System Buttress and Shim Augments 1 Trabecular Metal Acetabular Revision
Trabecular Metal Acetabular Revision System Buttress and Shim Augments Surgical Technique Trabecular Metal Acetabular Revision System Buttress and Shim Augments 1 Trabecular Metal Acetabular Revision
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management OSTEONTMⅡ Table of Contents Bone Graft Material OSTEON TM Collagen 04 OSTEON TM Ⅱ(Sinus & Lifting) 06 OSTEON TM (Sinus & Lifting) 08 ORTHOPEDIC OSTEON
Regeneration Bone Grafting & Soft Tissue Management OSTEONTMⅡ Table of Contents Bone Graft Material OSTEON TM Collagen 04 OSTEON TM Ⅱ(Sinus & Lifting) 06 OSTEON TM (Sinus & Lifting) 08 ORTHOPEDIC OSTEON
Surgical Technique Guide. Impact & Inject Formulations
 Surgical Technique Guide Impact & Inject Formulations System Overview OsteoVation QWIK is a bone void filler consisting of a proprietary composite of calcium phosphate and calcium sulfate granules. The
Surgical Technique Guide Impact & Inject Formulations System Overview OsteoVation QWIK is a bone void filler consisting of a proprietary composite of calcium phosphate and calcium sulfate granules. The
Trabecular Metal Technology The Best Thing Next to Bone
 Trabecular Metal Technology The Best Thing Next to Bone Trabecular Metal Material resembles trabecular bone in its cellular structure and weight-bearing characteristics. By approximating the mechanical
Trabecular Metal Technology The Best Thing Next to Bone Trabecular Metal Material resembles trabecular bone in its cellular structure and weight-bearing characteristics. By approximating the mechanical
Original Article. This PDF is available for free download from a site hosted by Medknow Publications. (
 Original Article www.jpgmonline.com An injectable cement: Synthesis, physical properties and scaffold for bone repair Weitao Y, Kangmei K, Anmin J* The Second Hospital of Shantou University Medical College,
Original Article www.jpgmonline.com An injectable cement: Synthesis, physical properties and scaffold for bone repair Weitao Y, Kangmei K, Anmin J* The Second Hospital of Shantou University Medical College,
Dr. John Masonis Charlotte, NC OrthoCarolina. Dr. James Waddell Toronto, Ontario University of Toronto, St. Michael s Hospital
 Design Rationale Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the REDAPT Revision Acetabular System design team: Dr. Robert Bourne London, Ontario
Design Rationale Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the REDAPT Revision Acetabular System design team: Dr. Robert Bourne London, Ontario
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Scientific & Clinical Evidence Jason membrane
 Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Trabecular Metal Acetabular Restrictor and Augment
 Trabecular Metal Acetabular Restrictor and Augment Surgical Technique The Best Thing Next To Bone Trabecular Metal Acetabular Restrictor and Augment Acetabular Assessment and Preparation Intra-operatively,
Trabecular Metal Acetabular Restrictor and Augment Surgical Technique The Best Thing Next To Bone Trabecular Metal Acetabular Restrictor and Augment Acetabular Assessment and Preparation Intra-operatively,
Advice sheet for Surgeons and Radiologists. Radiographic appearance of CERAMENT
 Advice sheet for Surgeons and Radiologists Radiographic appearance of CERAMENT The structure and function of CERAMENT CERAMENT is an osteoconductive bone graft substitute which consists of hydroxyapatite
Advice sheet for Surgeons and Radiologists Radiographic appearance of CERAMENT The structure and function of CERAMENT CERAMENT is an osteoconductive bone graft substitute which consists of hydroxyapatite
experts in bone regeneration Osteotwin Sports Surgery Line
 experts in bone regeneration Sports Surgery Line About Biomatlante Backed by 20 years of experience in the development and manufacturing of synthetic bone substitutes, Biomatlante readily meets the challenge
experts in bone regeneration Sports Surgery Line About Biomatlante Backed by 20 years of experience in the development and manufacturing of synthetic bone substitutes, Biomatlante readily meets the challenge
Osteochondral regeneration. Getting to the core of the problem.
 Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
PEEK-OPTIMA HA Enhanced: The Latest Material Development for Interbody Fusion
 PEEK-OPTIMA HA Enhanced: The Latest Material Development for Interbody Fusion Ovine Cervical Fusion Study Finds Performance Advantages with PEEK-OPTIMA HA Enhanced Polymer. 1 Introduction For more than
PEEK-OPTIMA HA Enhanced: The Latest Material Development for Interbody Fusion Ovine Cervical Fusion Study Finds Performance Advantages with PEEK-OPTIMA HA Enhanced Polymer. 1 Introduction For more than
Spinal fusions: bone and bone substitutes
 Eur Spine J (2000) 9 :372 378 Springer-Verlag 2000 REVIEW Dante G. Marchesi Spinal fusions: bone and bone substitutes Received: 9 August 2000 Accepted: 11 August 2000 D. G. Marchesi Department of Orthopaedic
Eur Spine J (2000) 9 :372 378 Springer-Verlag 2000 REVIEW Dante G. Marchesi Spinal fusions: bone and bone substitutes Received: 9 August 2000 Accepted: 11 August 2000 D. G. Marchesi Department of Orthopaedic
CS 2.0. Product information. Intelligent innovations for a better life.
 CS 2.0 Product information Intelligent innovations for a better life. 02. 03 Syntellix AG MAGNEZIX Compression Screw 2.0 Introduction CAUTION This product description is not sufficient or adequate to allow
CS 2.0 Product information Intelligent innovations for a better life. 02. 03 Syntellix AG MAGNEZIX Compression Screw 2.0 Introduction CAUTION This product description is not sufficient or adequate to allow
BIOACTIVE BASICS. Bioactive materials elicit a controlled action and reaction in the physiological environment.
 BIOACTIVE BASICS Bioactive materials elicit a controlled action and reaction in the physiological environment. Bioglass is a glass ceramic composed of silicon dioxide (SiO 2 ), sodium oxide (Na 2 O), calcium
BIOACTIVE BASICS Bioactive materials elicit a controlled action and reaction in the physiological environment. Bioglass is a glass ceramic composed of silicon dioxide (SiO 2 ), sodium oxide (Na 2 O), calcium
chronos Inject. Synthetic Bone Substitute Injectable, Osteoconductive, Resorbable.
 chronos Inject. Synthetic Bone Substitute Injectable, Osteoconductive, Resorbable. Technique Guide The answer to bone voids Table of contents Introduction 2 Case Study 3 Indications and Contraindications
chronos Inject. Synthetic Bone Substitute Injectable, Osteoconductive, Resorbable. Technique Guide The answer to bone voids Table of contents Introduction 2 Case Study 3 Indications and Contraindications
Accelerated Neutral Atom Beam Processing Improves PEEK In Vivo Osseointegration
 Accelerated Neutral Atom Beam Processing Improves PEEK In Vivo Osseointegration Joseph Khoury, PhD 1, Cathy Tkaczyk, PhD 2, Art Kurz 1, James Bachand 1, Richard Svrluga 1, Michel Assad, PhD 2. 1 Exogenesis
Accelerated Neutral Atom Beam Processing Improves PEEK In Vivo Osseointegration Joseph Khoury, PhD 1, Cathy Tkaczyk, PhD 2, Art Kurz 1, James Bachand 1, Richard Svrluga 1, Michel Assad, PhD 2. 1 Exogenesis
Synthetic and absorbable autograft substitute with osteoinduction
 putty Synthetic and absorbable autograft substitute with osteoinduction Quality made in Germany Synthetic and absorbable autograft substitute with osteoinduction Information on the synthetic bone grafting
putty Synthetic and absorbable autograft substitute with osteoinduction Quality made in Germany Synthetic and absorbable autograft substitute with osteoinduction Information on the synthetic bone grafting
PORESORB -TCP Bone Regeneration Material. Resorbability High phase purity Osteoconductivity High stability in defect
 Bone Regeneration Material Resorbability High phase purity Osteoconductivity High stability in defect PHYSICOCHEMICAL PARAMETERS: Composition: ß - tricalciumphosphate, Ca 3 (P0 4 ) 2 Synthetic material
Bone Regeneration Material Resorbability High phase purity Osteoconductivity High stability in defect PHYSICOCHEMICAL PARAMETERS: Composition: ß - tricalciumphosphate, Ca 3 (P0 4 ) 2 Synthetic material
Zimmer Trabecular Metal Dental Implant
 Zimmer Trabecular Metal Dental Implant TRABECULAR METAL MATERIAL: Designed to Enhance Secondary Stability Through Bone Ingrowth. Artistic Rendering osseoincorporation TRABECULAR METAL MATERIAL Designed
Zimmer Trabecular Metal Dental Implant TRABECULAR METAL MATERIAL: Designed to Enhance Secondary Stability Through Bone Ingrowth. Artistic Rendering osseoincorporation TRABECULAR METAL MATERIAL Designed
"The Evaluation Nano Calcium Silicate Cements Performance for Palpation"
 "The Evaluation Nano Calcium Silicate Cements Performance for Palpation" Delaram Amini* Bachelor Student, Department of Medical Islamic Azad University Of Tehran Medical Branch Tehran,Iran Maryam Chenani
"The Evaluation Nano Calcium Silicate Cements Performance for Palpation" Delaram Amini* Bachelor Student, Department of Medical Islamic Azad University Of Tehran Medical Branch Tehran,Iran Maryam Chenani
