Asufficient quantity of bone is an essential prerequisite
|
|
|
- Lee Bradley
- 5 years ago
- Views:
Transcription
1 Clinical Evaluation of a Bilayered Collagen Membrane (Bio-Gide) Supported by Autografts in the Treatment of Bone Defects Around Implants Georges Tawil, DDS, DSc, OD 1 /Georgina El-Ghoule, DDS 2 /Muhieddine Mawla, DCD, DES 3 The aim of this study was to determine the efficacy of a bioresorbable collagen membrane (Bio-Gide) in combination with autogenous bone grafts in the treatment of peri-implant dehiscences, fenestrations, or limited vertical defects. Eighteen titanium dental implants with exposed threads placed in 17 patients were studied. Autogenous bone was used in all cases to fill the defect and maintain the space underneath the barrier. The collagen membrane was trimmed and adapted to cover the defect in a saddle configuration. The membrane absorbed the blood and easily covered and adhered to the underlying bone. It was not stabilized by any retentive means. Sixteen to 32 months postoperatively, the sites were reentered and the amount of bone regenerated was measured. The results showed significant bone gain (average 87.6%) in the treatment of peri-implant defects with Bio-Gide and autogenous bone. (INT J ORAL MAXILLOFAC IMPLANTS 2001;16: ) Key words: autologous transplantation, bioresorbable membrane, guided bone regeneration, peri-implant defect Asufficient quantity of bone is an essential prerequisite for the long-term success of implant therapy. The placement of endosseous implants in sites where the bone volume is equal to or less than the size of the implant results in part of the implant surface not being covered by bone, with possible periimplant soft tissue irritation, decreased bone-implant contact surface, and potential implant failure. 1 5 The need for bone regeneration in cases of limited dehiscences or fenestrations with machinedsurface implants has been questioned. A 5-year follow-up on implants with exposed threads at the time of placement did not show any soft tissue irritation or further bone loss when oral hygiene measures were carefully applied. 6 Large bony defects may appear when implants are placed in areas of deficient bone volume at the predetermined implant site. Sizeable reductions in 1 Professor, Department of Periodontology, and Director, Postdoctoral Studies, St Joseph University, Beirut, Lebanon. 2 Postgraduate Student, Department of Periodontology, St Joseph University, Beirut, Lebanon. 3 Assistant, Department of Periodontology, Lebanese University, Beirut, Lebanon. Reprint requests: Dr Georges Tawil, Elias Sarkis Avenue, Abou Arbib Bldg, Achrafieh, Beirut, Lebanon. Fax: gtawil@inco.com.lb the bone-implant contact area and large periimplant defects may be a more specific indication for bone regeneration. However, there are no references in the literature known to the authors concerning defect size as a definitive indication for guided bone regeneration (GBR) nor any indications for such a treatment when surfaces other than machined, commercially pure titanium are used. 6 Guided bone regeneration has been successfully applied to treat peri-implant bone defects 3,7,8 and to augment the height and the width of atrophic alveolar ridges prior to implant placement. 3,7 9 Dehiscences, fenestrations, peri-implant intrabony defects, or vertical augmentation concomitant to implant placement have been successfully managed with autogenous bone or bone substitutes as spacers and nonresorbable or resorbable barriers. 10 The barrier prevents invasion of the defect by surrounding soft tissue, offers protection and stabilization to the blood clot as well as the filling material, and gives the bone cells sufficient time to proliferate and regenerate bone. 3,11,12 Nonresorbable expanded polytetrafluoroethylene (e-ptfe) membranes (Gore-Tex, W. L. Gore and Associates, Flagstaff, AZ) have been used successfully since the 1980s. However, this material has 3 definite disadvantages. First, postoperative membrane exposure can occur and compromise the The International Journal of Oral & Maxillofacial Implants 857
2 regenerative process. 3 Second, an extensive second operation is often necessary for removal of the membrane. Finally, when the membrane is removed after 6 months, newly formed bone can react to exposure by resorption. 13 To avoid the inherent disadvantages of nonresorbable membranes, resorbable barriers have been introduced in GBR. For bone regeneration to occur, the following requisites 14 should be satisfied: bioresorbability, absence of foreign body reaction, no residues after degradation that may interact with bone regeneration, and efficient barrier function for 5 to 6 months. 15 Bio-Gide (Geistlich Biomaterials, Wolhusen, Switzerland) is a bioresorbable collagen barrier made of fiber protein, which consists of hydroxyproline with the structure of a triple helix. Collagen fibers provide structural elasticity during the crystalline phase of bone regeneration. The properties of collagen ensure optimal tissue integration and adequate wound healing. 16 The 2 disadvantages of this material are insufficient space-making ability and the possibility of antigenic reaction. 17 The problem of space creation can be solved by using bone or bone substitutes, while the development of antigenicity can be prevented by establishing excellent quality control during fabrication. The degradation rate of Bio-Gide has been tested in experimental models and varies from a few days to several weeks. 18,19 The Bio-Gide collagen membrane is simple to apply and rapidly conforms to the underlying tissues. 16 For bone regeneration to occur, membranes must be stabilized by pins or tacks to prevent any micromovement that may compromise the regenerative process. 9 The aim of the present study was to evaluate the efficacy of a collagen membrane (Bio-Gide), used in conjunction with autogenous bone grafts, for the treatment of peri-implant dehiscences, fenestrations, or limited vertical defects. Such defects were recognized at phase I surgery and resulted from implant placement at sites with insufficient bone volume; Bio-Gide membranes were placed without stabilization other than the inherent properties of collagen to adhere to the underlying tissues when adequately adapted to the defect. MATERIALS AND METHODS A total of 17 patients (10 females and 7 males, mean age 47 years, range 24 to 85 years) were included in this study. Preoperative examination consisted of periapical radiographs, a panoramic radiograph, and a clinical examination to evaluate bone volume at the proposed implant sites. No computed tomography as a diagnostic tool was used in the present series. None of the patients in the present series were smokers. All implants were screw-type with a machined surface (Nobel Biocare, Göteborg, Sweden) and were placed in a 2-stage procedure. The patients were informed of the necessity for a second surgery to evaluate the bone gain obtained after the regenerative therapy, to perform any soft tissue procedures needed to enhance esthetics, and to connect the abutment. The types of defects found are reported in Table 1 and were classified as dehiscences, fenestrations, or intrabony defects. The number of implant sites exposed was recorded (buccal/labial, mesial, distal), along with the number of walls involved (1, 2, 3, or circumferential defect) in the case of intrabony defects. Eight implants were placed in the maxilla and 10 in the mandible. After the implants were placed, during phase I surgery, a number of threads were found exposed. Twelve defects were dehiscences involving 3 sides (mesial, buccal/labial, and distal) of the implant. One defect was a fenestration, one was a combination of intrabony defect and dehiscence on the buccal, and 2 were wide circumferential intrabony defects that appeared following immediate implantation. The height and width of the defects were measured with a periodontal probe (PCP-UNC15, Hu- Friedy, Chicago, IL). The shoulder of the implant was used as a reference for height, and the bony edge of the defects at 2 distinct levels was used for the width both at the platform of the implants and at mid-distance between the top and the bottom of the defect, in cases of a V-shape type defect. The mean values for the width recorded at phase I surgery and at reentry are reported in Table 1. All measurements were made by one calibrated operator. Autogenous bone was used in all cases to fill the defect and maintain the space underneath the barrier, since the membrane has no inherent rigidity and collapses over the defect when pressed, leaving no room for the regenerating tissues. Cortical bone from adjacent sites was shaved with a rongeur. No bone from the prepared osteotomies was used for grafting. Small particles of dense cortical bone were thus harvested and gently packed over the defect (Figs 1 and 2). No cortical penetration at the site of the defect was done. The collagen barrier (Bio- Gide) was trimmed and adapted to cover the defect and extended 2 to 3 mm sideways, being laid over the implant in a saddle configuration (Fig 3). It was tucked underneath the palatal or lingual flap to cover the ridge and buccal defect, moistened, and pressed gently in place with gauze to adapt to the 858 Volume 16, Number 6, 2001
3 Table 1 Clinical Data for Pre- and Postoperative Defects Initial Second Defect Implant value (mm) value (mm) fill (mm) Time of Percent Implant length Type Mean Mean Mean second bone Clinical Patient Age Sex Location diameter (mm) of defect Height width Height width Height width operation (wk) regeneration healing 1 45 F x 3.75 DhB Exposed x 3.75 DhB membrane 2 31 F x 3.75 DhBMD Uneventful 3 49 M x 3.75 DhB Uneventful 4 35 M x 3.3 W Uneventful 5 36 M x 3.75 DhB Uneventful 6 85 F x 3.75 DhB Uneventful 7 51 M x 3.75 DhB Uneventful 8 59 M x 5 W Uneventful 9 42 F x 5 DhB Uneventful M x 3.75 DhB Uneventful F x 3.75 DhB Uneventful F x 5 (WP) FBM Uneventful F x 3.75 DhBMD Uneventful F x 3.75 DhB Exposed membrane M x 3.3 DhB Uneventful F x 3.75 DhB Uneventful F x 3.75 W Uneventful Mean SD Dh = dehiscence; B = buccal; M = mesial; D = distal; F = fenestration; W1 = intrabony defect 1 wall; W3 = intrabony defect 3 walls; Second value = value at second operation; SD = standard deviation. For difference in means between pre- and postoperative height values: t = 9.24; df = 17; P = For difference in means between pre- and postoperative width values: t = 5.53; df = 17; P = Width value represents the mean of the 2 measurements made. Implant locations (International System): 11 = maxillary right central incisor; 21 = maxillary left central incisor; 22 = maxillary left lateral incisor; 23 = maxillary left canine; 25 = maxillary left second premolar; 32 = mandibular left lateral incisor; 33 = mandibular left canine; 34 = mandibular left first premolar; 42 = mandibular right lateral incisor; 43 = mandibular right canine; 44 = mandibular right first premolar; 45 = mandibular right second premolar; 47 = mandibular right second molar. The International Journal of Oral & Maxillofacial Implants 859
4 Fig 1 Implant placed to replace the maxillary left central incisor. The dehiscence measured 4 mm on the labial side. A 1- wall vertical defect was present on the mesial and distal sides. Fig 3 The membrane was placed in a saddle configuration, covering the defect. underlying bone. The membrane absorbed the blood and easily covered and adhered to the underlying bone. It was not stabilized by any direct retentive means. The flaps were then readapted to cover the membrane and sutured without tension. In cases where the flaps remained tense during suturing, a periosteal releasing incision was made to ease handling of a tension-free flap. Nonresorbable 5.0 nylon sutures were used for suturing. Gentle compression over the defect was applied for 2 minutes, after which the patient was released. Postoperative care consisted of a 5-day course of antibiotics (amoxicillin 500 mg 3 times daily) and rinsing twice a day with a 0.12% chlorhexidine solution (Oroclense, Germiphen, Brantford, Ontario, Canada) for 2 weeks postoperatively. Sutures were removed 10 days after surgery. One patient was completely edentulous and was asked Fig 2 not to wear her prosthesis for the first 4 postoperative weeks. She was put on a liquid diet. After that, her denture was relined with a resilient liner (Coe Comfort, GC America, Alsip, IL) and was used only for esthetic purposes and eating of soft food. Checkups were done at a biweekly interval for the first month and then bimonthly until the time of abutment connection. Approximately 6 months postoperatively, the sites were reentered through a crestal incision, with vertical incisions avoided to limit the undesirable exposure of bone and potential soft tissue recession. The amount of regenerated hone was measured using the same periodontal probe and the measurements were compared to the initial values. Statistical analysis was done to evaluate the difference between the initial and the final values using the Student t test for paired samples. RESULTS Autogenous bone was gently packed into defect. The initial values and the data collected at abutment connection are reported in Table 1. Sixteen remaining sites healed without complications, and 2 membranes were exposed. In 1 patient, the membrane became exposed after 2 weeks. Mouth rinsing was continued for the following 3 weeks. The cover screw appeared and the gingiva healed around it with no visible signs of inflammation and no trace of the membrane clinically. The healing continued uneventfully until the sixth postoperative month. In the second patient, a flap dehiscence occurred 2 weeks postoperatively. Tentative resuturing of the flaps was successful. The membrane was not removed, and rather good closure of the soft tissue 860 Volume 16, Number 6, 2001
5 Fig 4 Healing at 6 months. The defect is filled with bone that has regenerated; bone has also regenerated over the cover screw. occurred, with no signs of inflammation. Four months later, a limited 1- to 2-mm fenestration of the cover screw on 1 of the patient s implants was present, without clinical evidence of inflammation. Two sites showed thin buccal osseous healing, while the newly formed tissue at all other sites showed bony consistency clinically similar to the local adjacent sound bone. Timing of the second operation varied between 16 and 32 weeks after membrane placement (mean value 23 weeks). The height of the initial defects varied between 3 and 10 mm (5.28 ± 1.93 mm). The height of the residual defect varied between 0 and 3 mm, with a mean value of 0.61 ± 1.04 mm. The vertical gain in bone varied between 1 and 10 mm, with a mean value of 4.67 ± 2.14 mm. The difference between the preand postoperative values was statistically significant (P <.001). At the time of implant placement, the width of the defect varied between 1 and 4 mm, with a mean value of 3.11 ± 1.04 mm. At the time of abutment connection, the width varied between 0 and 4 mm, with a mean value of 0.94 ± 1.63 mm. The gain in new bone mesiodistally varied between 0 and 4 mm, with a mean value of 2.17 ± 1.66 mm, and was statistically significant (P <.001). The overall percentage of bone regeneration varied between 33.3% and 100%; 13 of the 18 defects showed 100% regeneration (Figs 4 to 6). Significant bone gain (average gain 87.5%) was achieved after 16 to 32 weeks. DISCUSSION The purpose of this clinical study in humans was to evaluate the efficacy of a resorbable membrane (Bio- Fig 5 A 9-mm labial dehiscence on the implant placed in the mandibular left canine site. Fig 6 Reentry at 4 months showing bone regeneration. Gide) associated with autogenous bone chips in promoting bone regeneration around peri-implant bony defects. The overall results of the regenerative treatment of the 18 defects showed significant new bone formation, with a mean reduction in defect height and width of 87.5%. This is in accordance with other clinical studies that demonstrated similar percentages of bone fill. Simion and coworkers 20 obtained 93.38% gain in the treatment of implant dehiscences and fenestrations using polylactic acid/polyglycolic acid membranes in association with autogenous bone chips as a space-maker and stabilized with fixation screws or nails. Zitzmann and associates 21 found collagen membranes very effective in the treatment of peri-implant defects in comparison to e-ptfe. In that study, the membranes were stabilized with pins, and Bio-Oss (natural bone mineral substitute, Geistlich Biomaterials) The International Journal of Oral & Maxillofacial Implants 861
6 served as a spacer. A mean bone gain of 92% for Bio-Gide and 78% for e-ptfe was obtained. In other studies, 3,10,22 the overall reduction of periimplant defects using e-ptfe membranes ranged between 82% and 93.6%. However, when no barriers were applied over the defects, an average of 3.5% of the exposed implant surface was covered with bone, whereas 75% of the implant defect regenerated when e-ptfe membranes were used. 5 The collagen membrane itself cannot contain a cavity because it lacks the necessary stiffness to maintain enough space under the membrane to fill the defect. It is therefore desirable to use a grafting material when applying resorbable membranes. 23 Autogenous bone is the ideal material for use in regenerative therapy. 24 It is generally available adjacent to the implant site. 25 It is believed to exhibit both osteoconductive and osteoinductive properties 24,26 and can maintain adequate space under the membrane for a sufficient period of time for hard tissue regeneration and to integrate with the preexisting bone. 26 Bone substitutes have been used extensively as spacers under membranes However, in this study, autogenous bone was used exclusively for this purpose because it was readily available in the quantity needed to treat the defects. It can always be collected from adjacent sites, or if needed, from a remote site in the oral cavity or from the prepared implant site to meet the specific treatment needs. Degradation of the Bio-Gide barrier occurred without clinical signs of inflammation, even where wound dehiscence occurred postoperatively. The mean average percentage of bone fill is influenced by membrane exposure and averaged 60% in the 2 exposed sites in this series. It should be noted that membrane degradation occurs faster in case of incomplete wound closure. 30 When soft tissue dehiscence occurs, Lorenzoni and colleagues 30 found that a self-reinforced polyglycolic acid membrane (Biofix, Biocon, Tampere, Finland) was progressively resorbed, with consequent spontaneous healing of the soft tissues in 3 to 6 weeks. The absence of soft tissue coverage caused significant reduction in the quantity of bone regeneration (45% vs 75% for unexposed membranes). Removal of a resorbable barrier is not necessary in case of wound dehiscence, while exposure of an e-ptfe membrane, which occurs in 16% to 41% of sites, 3,22,26 requires its removal before 6 weeks because of contamination and potential damage to the underlying newly formed tissues. Using Bio-Gide membranes, Zitzmann and associates 21 obtained an average bone fill of 94% for sites with uncomplicated wound healing and 87% for sites with incomplete wound closure after 6 weeks. With e-ptfe membranes, the average bone fill was 98% for sites with uncomplicated wound healing and 65% for sites where membrane exposure required their early retrieval. The usefulness of bioresorbable pins to stabilize a collagen membrane may be questioned. It has been stated that absolute stability of the membrane is fundamental to the whole concept of GBR and a vital prerequisite for therapeutic success, and that the tiniest movement on the granulating tissue underneath the membrane is to be avoided. 9 In the present study, it was possible to obtain stability of the collagen membrane without additional fixation because of the inherent properties of collagen to adhere and conform to underlying tissues when gentle pressure is applied to it. However, it was not possible under the present conditions to verify whether micromovements had any deleterious effects on the percentage of regenerated bone-toimplant contact. The clinical results confirm that when handled cautiously, the soft tissues will cover the membrane and maintain it in place, with no need for further stabilization. In 2 patients, a thin layer of bone was found covering the implant threads that were underneath. This may have been caused by displacement of the autogenous bone underneath the membrane or by collapse of the membrane over the defect. CONCLUSIONS Significant bone gain was obtained in the treatment of peri-implant defects using Bio-Gide and autogenous bone. The results compared favorably to those reported in the literature with e-ptfe. The decrease in defect size was significant. This indicates that Bio-Gide has the potential to facilitate bone growth. The material possesses certain properties that facilitate clinical handling and permit uneventful healing, and it may be used without additional stabilization. However, the effect of micromovements on the percentage of regenerated bone-toimplant contact needs to be investigated. The barrier must be supported to prevent its collapse into the bone defect or onto the implant surface. REFERENCES 1. Lundgren D, Sennerby L, Falk H, Friberg B, Nyman S. The use of a new bioresorbable barrier for guided bone regeneration in connection with implant installation. Clin Oral Implants Res 1994;5: Volume 16, Number 6, 2001
7 2. Lekholm U, Adell R, Brånemark P-I. Complications. In: Brånemark P-I, Zarb GA, Albrektsson T (eds). Tissue-Integrated Prostheses: Osseointegration in Clinical Dentistry. Chicago: Quintessence, 1985: Jovanovic SA, Spiekermann H, Richter EJ. Bone regeneration around titanium dental implants in dehisced defect sites: A clinical study. Int J Oral Maxillofac Implants 1992;7: Becker W, Becker B, Handlesman M, et al. Bone formation at dehisced dental implant sites treated with implant augmentation material: A pilot study in dogs. Int J Periodontics Restorative Dent 1990;10: Dahlin C, Lekholm U, Lindhe A. Membrane-induced bone augmentation at titanium implants. A report on ten fixtures followed from 1 to 3 years after loading. Int J Periodontics Restorative Dent 1991;11: Lekholm U, Sennerby L, Ross J, Becker W. Soft tissue and marginal bone condition at osseointegrated implants that have exposed threads: A 5-year retrospective study. Int J Oral Maxillofac Implants 1996;11: Dahlin C, Lindhe A, Gottlow J. Healing of bone defects by guided tissue regeneration. Plast Reconstr Surg 1998;81: Dahlin C, Sennerby L, Lekholm U, Lindhe A, Nyman S. Generation of new bone around titanium implants using a membrane technique: An experimental study in rabbits. Int J Oral Maxillofac Implants 1989;4: Buser D, Dula K, Hirt HP, Schenk RK. Lateral ridge augmentation using autografts and barrier membranes: A clinical study with 40 partially edentulous patients. Int J Oral Maxillofac Surg 1996;54: Dahlin C, Lekholm U, Becker W, Higuchi K, Callens A. Treatment of fenestration and dehiscence bone defects around oral implants using the guided tissue regeneration technique: A prospective multicenter study. Int J Oral Maxillofac Implants 1995;10: Zitzmann N, Naef R, Schärer P. Guided bone regeneration and augmentation in implant surgery, using Bio-Oss together with the membrane technique. Dtsch Zahnärztl Z 1996;6: Stuart AK, Wisner-Lynch L, Marxer M, Lynch S. Guided bone regeneration: Integration of a resorbable membrane and a bone graft material. Pract Periodontics Aesthet Dent 1997;9: Murphy K. Postoperative healing complications associated with Gore-Tex periodontal material. Part I. Incidence and characterization. Int J Periodontics Restorative Dent 1995; 15: Gottlow J. Guided tissue regeneration using bioresorbable and non-resorbable devices: Initial healing and long-term results. J Periodontol 1993;64: Mellonig J, Triplett RG. Guided tissue regeneration and endosseous dental implants. Int J Periodontics Restorative Dent 1993;13: Hürzeler MB, Strub JR. Guided bone regeneration around exposed implants: A new bioresorbable device and bioresorbable membrane pins. Pract Periodontics Aesthet Dent 1995;7(9): Quteish D, Dolby AE. Immune responses to implanted human collagen graft in rats. J Periodontal Res 1991;26: Owens KW, Yukna RA. Collagen membrane resorption in dogs. A comparative study. Implant Dent 2001;10: Zhao J, Pinholt EM, Madsen JE, Donath K. Histological evaluation of different biodegradable and non-biodegradable membranes implanted subcutaneously in rats. J Cranio Maxillofac Surg 2000;28: Simion M, Misitano U, Gionso L, Salvato A. Treatment of dehiscences and fenestrations around dental implants using resorbable and non-resorbable membranes associated with bone autografts: A comparative clinical study. Int J Oral Maxillofac Implants 1997;12: Zitzmann N, Naef R, Schärer P. Resorbable versus nonresorbable membranes in combination with Bio-Oss for guided bone regeneration. Int J Oral Maxillofac Implants 1997;12: Becker W, Dahlin C, Becker BE, Lekholm U, van Steenberghe D, Higuchi K. The use of e-ptfe barrier membranes for bone promotion around titanium implants placed into extraction sockets: A prospective multicenter study. Int J Oral Maxillofac Implants 1994;9: Hürzeler MB, Weng D, Hutmacher D. Bone regeneration around implants: A clinical study with a new resorbable membrane. Dtsch Zahnärztl Z 1996;51: Burchardt H. The biology of bone graft repair. Clin Orthop Rel Res 1983;174: Becker W, Becker BE, Polizzi G, Bergström C. Autogenous bone grafting of bone defects adjacent to implants placed into immediate extraction sockets in patients: A prospective study. Int J Oral Maxillofac Implants 1994;9: Simion M, Dahlin C, Trisi P, Piattelli A. Qualitative and quantitative comparative study on different filling materials used in bone regeneration: A controlled clinical study. Int J Periodontics Restorative Dent 1994;14: Hammerle CH, Lang NP. Single stage surgery combining transmucosal implant placement with guided bone regeneration and bioresorbable materials. Clin Oral Implants Res 2001;12: Hockers T, Abensur D, Valentini P, Legrand R, Hämmerle C. The combined use of bioresorbable membrane and xenografts or autografts in the treatment of bone defects around implants. Clin Oral Implants Research 1999;10: Hürzeler MB, Kohal RJ, Mota LF, Naghshbandi J, Caffesse RG. Evaluation of a new bioresorbable barrier to facilitate guided bone regeneration around exposed implant threads. An experimental study in the monkey. Int J Oral Maxillofac Surg 1998;27: Lorenzoni M, Pertl C, Keil C, Wegscheider W. Treatment of peri-implant defects with guided bone regeneration: A comparative clinical study with various membranes and bone grafts. Int J Oral Maxillofac Implants 1998;13: The International Journal of Oral & Maxillofacial Implants 863
Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region
 CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Vertical and horizontal alveolar ridge augmentation
 CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
Long-term Results of Implants Treated with Guided Bone Regeneration: A 5-year Prospective Study
 Long-term Results of Implants Treated with Guided Bone Regeneration: A 5-year Prospective Study Nicola Ursula Zitzmann, Dr Med Dent 1 /Peter Schärer, Prof Dr Med Dent, MS 2 / Carlo Paolo Marinello, Prof
Long-term Results of Implants Treated with Guided Bone Regeneration: A 5-year Prospective Study Nicola Ursula Zitzmann, Dr Med Dent 1 /Peter Schärer, Prof Dr Med Dent, MS 2 / Carlo Paolo Marinello, Prof
Severe alveolar bone loss related to traumatic
 Simultaneous Implant Placement and Vertical Ridge Augmentation with a Titanium-Reinforced Membrane: A Case Report Roberto Cornelini, MD, DDS 1 /Filippo Cangini, DDS 2 /Ugo Covani, MD, DDS 3 /Sebastiano
Simultaneous Implant Placement and Vertical Ridge Augmentation with a Titanium-Reinforced Membrane: A Case Report Roberto Cornelini, MD, DDS 1 /Filippo Cangini, DDS 2 /Ugo Covani, MD, DDS 3 /Sebastiano
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Bringing you Geistlich biocompatibility with improved application and handling benefits. Your combination for success
 Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Conventional guided bone regeneration
 CLINICAL MINIMALLY INVASIVE GUIDED BONE REGENERATION Efraim Kfir, DDS; Vered Kfir, DDS; Eli Eliav, DMD, PhD; Edo Kaluski, MD Guided bone regeneration (GBR) is indicated when there is a volume deficiency
CLINICAL MINIMALLY INVASIVE GUIDED BONE REGENERATION Efraim Kfir, DDS; Vered Kfir, DDS; Eli Eliav, DMD, PhD; Edo Kaluski, MD Guided bone regeneration (GBR) is indicated when there is a volume deficiency
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report
 Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
The Sandwich Bone Augmentation Technique. Jia-Hui Fu* and Hom-Lay Wang*
 CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study
 R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
Maxillary sinus augmentation without any graft material- A case Report
 A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Many factors are known to influence the success of
 CLINICAL The Role of Two Different Collagen Membranes for Dehiscence Defect Around Implants in Humans Dong-Woon Lee, DDS, MSD 1,2 Kyeong-Taek Kim, DDS, MSD 1 Yon-Soo Joo, DDS 1 Mi-Kyung Yoo, DDS, MSD 1
CLINICAL The Role of Two Different Collagen Membranes for Dehiscence Defect Around Implants in Humans Dong-Woon Lee, DDS, MSD 1,2 Kyeong-Taek Kim, DDS, MSD 1 Yon-Soo Joo, DDS 1 Mi-Kyung Yoo, DDS, MSD 1
Vertical Augmentation
 Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up
 643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Years of research and advancement in
 Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
 227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Risk Factors for Wound Dehiscence after Guided Bone Regeneration in Dental Implant Surgery
 Maxillofac Plast Reconstr Surg 2014;36(3):116-123 http://dx.doi.org/10.14402/jkamprs.2014.36.3.116 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Original Article Risk Factors for Wound Dehiscence after
Maxillofac Plast Reconstr Surg 2014;36(3):116-123 http://dx.doi.org/10.14402/jkamprs.2014.36.3.116 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Original Article Risk Factors for Wound Dehiscence after
Posterior mandible and vertical augmentation
 CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla
 Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla Luciano Malchiodi, MD, DDS*/Antonio Scarano, DDS**/Manlio Quaranta, MD, DDS***/ Adriano
Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla Luciano Malchiodi, MD, DDS*/Antonio Scarano, DDS**/Manlio Quaranta, MD, DDS***/ Adriano
Since the report of Adell and associates, 1 well-documented
 Immediate Loading of an Implant Following Implant Site Development Using Forced Eruption: A Case Report Young-Seok Park, DDS, MSD 1 /Ki-Young Yi, DDS 2 /Seong-Cheol Moon, DDS, MSD, PhD 3 / Young-Chul Jung,
Immediate Loading of an Implant Following Implant Site Development Using Forced Eruption: A Case Report Young-Seok Park, DDS, MSD 1 /Ki-Young Yi, DDS 2 /Seong-Cheol Moon, DDS, MSD, PhD 3 / Young-Chul Jung,
Effect of GBR in Combination with Deproteinized Bovine Bone Mineral on the Healing of Calvarial Defects in Rabbits
 Original Article Effect of GBR in Combination with Deproteinized Bovine Bone Mineral on the Healing of Calvarial Defects in Rabbits AA. Khoshkhoonejad 1, A. Miremadi 2, AR. Rokn 2,3, B. Eslami 4, M. Dehghan
Original Article Effect of GBR in Combination with Deproteinized Bovine Bone Mineral on the Healing of Calvarial Defects in Rabbits AA. Khoshkhoonejad 1, A. Miremadi 2, AR. Rokn 2,3, B. Eslami 4, M. Dehghan
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
The International Journal of Periodontics & Restorative Dentistry
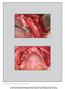 The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft
 The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
The International Journal of Periodontics & Restorative Dentistry
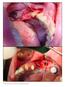 The International Journal of Periodontics & Restorative Dentistry 3 Periosteal Pocket Flap for Horizontal Bone Regeneration: A Case Series Marius Steigmann, DDS*/Maurice Salama, DDS, MS**/ Hom-Lay Wang,
The International Journal of Periodontics & Restorative Dentistry 3 Periosteal Pocket Flap for Horizontal Bone Regeneration: A Case Series Marius Steigmann, DDS*/Maurice Salama, DDS, MS**/ Hom-Lay Wang,
BOUCHLARIOTOU, Ioana, et al. Abstract
 Article Long-term stability of osseointegrated implants in bone regenerated with a collagen membrane in combination with a deproteinized bovine bone graft: 5- year follow-up of 20 implants BOUCHLARIOTOU,
Article Long-term stability of osseointegrated implants in bone regenerated with a collagen membrane in combination with a deproteinized bovine bone graft: 5- year follow-up of 20 implants BOUCHLARIOTOU,
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Guided bone regeneration
 CLINICAL REGENERATION OF THE ALVEOLAR CREST USING TITANIUM MICROMESH WITH AUTOLOGOUS BONE AND A RESORBABLE MEMBRANE Marco Degidi, MD, DDS Antonio Scarano, DDS Adriano Piattelli, MD, DDS KEY WORDS Alveolar
CLINICAL REGENERATION OF THE ALVEOLAR CREST USING TITANIUM MICROMESH WITH AUTOLOGOUS BONE AND A RESORBABLE MEMBRANE Marco Degidi, MD, DDS Antonio Scarano, DDS Adriano Piattelli, MD, DDS KEY WORDS Alveolar
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Tooth out what's next?
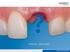 Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Ridge Augmentation. Selection of Applicable Abstracts and Posters. Using Titanium-Reinforced PTFE Membranes
 Ridge Augmentation Selection of Applicable Abstracts and Posters Using Titanium-Reinforced PTFE Membranes Gultekin BA, Cansiz E, Borahan MO. Clinical and 3-Dimensional Radiographic Evaluation of Autogenous
Ridge Augmentation Selection of Applicable Abstracts and Posters Using Titanium-Reinforced PTFE Membranes Gultekin BA, Cansiz E, Borahan MO. Clinical and 3-Dimensional Radiographic Evaluation of Autogenous
The high clinical success rate of endosseous
 Clinical Evaluation of Short, Machined-Surface Implants Followed for 12 to 92 Months Georges Tawil, DDS, DSc.Od 1 /Roland Younan, DCD, DES 2 Purpose: Bone resorption following tooth loss often limits the
Clinical Evaluation of Short, Machined-Surface Implants Followed for 12 to 92 Months Georges Tawil, DDS, DSc.Od 1 /Roland Younan, DCD, DES 2 Purpose: Bone resorption following tooth loss often limits the
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Early implant placement: 3D radiographic study on the fate of buccal wall
 Early implant placement: 3D radiographic study on the fate of buccal wall A. Lanza 1-2, F. Scognamiglio 1, G. De Marco 1, F. Di Francesco 1, F. Femiano 1-3, M. Lanza 4, A. Itro 5 1 DD-Multidisciplinary
Early implant placement: 3D radiographic study on the fate of buccal wall A. Lanza 1-2, F. Scognamiglio 1, G. De Marco 1, F. Di Francesco 1, F. Femiano 1-3, M. Lanza 4, A. Itro 5 1 DD-Multidisciplinary
The International Journal of Periodontics & Restorative Dentistry
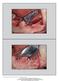 The International Journal of Periodontics & Restorative Dentistry 355 Vertical Ridge Augmentation Around Implants Using e-ptfe Titanium- Reinforced Membrane and Deproteinized Bovine Bone Mineral (Bio-Oss):
The International Journal of Periodontics & Restorative Dentistry 355 Vertical Ridge Augmentation Around Implants Using e-ptfe Titanium- Reinforced Membrane and Deproteinized Bovine Bone Mineral (Bio-Oss):
Redefining Regeneration
 Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Guided bone regeneration using two types of non-resorbable barrier membranes
 DOI:10.5125/jkaoms.2010.36.4.275 Guided bone regeneration using two types of non-resorbable barrier membranes Ji-Young Lee 1, Young-Kyun Kim 1, Pil-Young Yun 1, Ji-Su Oh 2, Su-Gwan Kim 2 1 Department of
DOI:10.5125/jkaoms.2010.36.4.275 Guided bone regeneration using two types of non-resorbable barrier membranes Ji-Young Lee 1, Young-Kyun Kim 1, Pil-Young Yun 1, Ji-Su Oh 2, Su-Gwan Kim 2 1 Department of
Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla
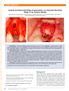 CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
Resorbable vs Non-resorbable Barriers with Immediate Implantation after Functional Loading under Overdenture
 Sahar Elkholy, Hussein Elcharkawi RESEARCH ARTICLE 10.5005/jp-journals-10029-1160 Resorbable vs Non-resorbable Barriers with Immediate Implantation after Functional Loading under Overdenture 1 Sahar Elkholy,
Sahar Elkholy, Hussein Elcharkawi RESEARCH ARTICLE 10.5005/jp-journals-10029-1160 Resorbable vs Non-resorbable Barriers with Immediate Implantation after Functional Loading under Overdenture 1 Sahar Elkholy,
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
GBR membrane for ideal regeneration
 GBR membrane for ideal regeneration 1) i-gen Lingual Extension should be considered for a large defect. Need to have at least 1mm of space above the platform of a fixture: Make this space with a pre-existing
GBR membrane for ideal regeneration 1) i-gen Lingual Extension should be considered for a large defect. Need to have at least 1mm of space above the platform of a fixture: Make this space with a pre-existing
Immediate Implant Placement:
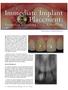 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Ridge Split Procedure
 Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A Case Series
 Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Peri-implant Augmentation
 Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Successful osseointegration of implants has been
 Therapeutic Management for Immediate Implant Placement in Sites with Periapical Deficiencies Where Coronal Bone Is Present: Technique and Case Report Cyril I. Evian, DMD 1 /Ahmed Al-Momani, BDS 2 /Edwin
Therapeutic Management for Immediate Implant Placement in Sites with Periapical Deficiencies Where Coronal Bone Is Present: Technique and Case Report Cyril I. Evian, DMD 1 /Ahmed Al-Momani, BDS 2 /Edwin
During the last 30 years, endosseous oral
 Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
The use of endosseous implants is currently a routine
 Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Case Series. Guided Bone Regeneration for Dehiscence and Fenestration Defects on Implants Using an Absorbable. polymer barriers.
 Guided Bone Regeneration for Dehiscence and Fenestration Defects on Implants Using an Absorbable Polymer Barrier Paul S. Rosen* and Mark A. Reynolds Background: Guided bone regeneration (GBR) using a non-absorbable
Guided Bone Regeneration for Dehiscence and Fenestration Defects on Implants Using an Absorbable Polymer Barrier Paul S. Rosen* and Mark A. Reynolds Background: Guided bone regeneration (GBR) using a non-absorbable
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Initially, Brånemark System (Nobel Biocare AB,
 Clinical Application of Narrow Brånemark System Implants for Single-Tooth Restorations Giovanni Polizzi, MD, DDS*/Sandro Fabbro, MD**/Marco Furri, DDS**/ Irene Herrmann, DDS***/Sergio Squarzoni, MD****
Clinical Application of Narrow Brånemark System Implants for Single-Tooth Restorations Giovanni Polizzi, MD, DDS*/Sandro Fabbro, MD**/Marco Furri, DDS**/ Irene Herrmann, DDS***/Sergio Squarzoni, MD****
Innovative Treatment Concepts IN ORAL AND MAXILLOFACIAL SURGERY
 Innovative Treatment Concepts IN ORAL AND MAXILLOFACIAL SURGERY LEADING REGENERATION CLINICAL CASES Dr. J. Aranda Onlay grafting for horizontal augmentation 8 Prof. Dr. D. Buser et al. Onlay grafting for
Innovative Treatment Concepts IN ORAL AND MAXILLOFACIAL SURGERY LEADING REGENERATION CLINICAL CASES Dr. J. Aranda Onlay grafting for horizontal augmentation 8 Prof. Dr. D. Buser et al. Onlay grafting for
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Implant Site Development Part I
 REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
Hyun-Jae Cho, Kun-Soo Jang, Ki-Hyun Jeong, Jae-Yun Jeon, Kyung-Gyun Hwang, Chang-Joo Park
 Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
GBR membrane for ideal regeneration. i-gen TM. 2mm. >2.5mm. Lingual Extension. >100 blunt angle
 REGENERATION 02/03 Design Concept GBR membrane for ideal regeneration i-gen TM Description Single A type Small IG1W4509 Single A type Regular IG1W5510 Single A type Wide IG1W6511 Single B type Small IG2W0918
REGENERATION 02/03 Design Concept GBR membrane for ideal regeneration i-gen TM Description Single A type Small IG1W4509 Single A type Regular IG1W5510 Single A type Wide IG1W6511 Single B type Small IG2W0918
Osseointegrated implants are a very reliable means
 Tridimensional Reconstruction of Knife-Edge Edentulous Maxillae by Sinus Elevation, Onlay Grafts, and Sagittal Osteotomy of the Anterior Maxilla: Preliminary Surgical and Prosthetic Results Matteo Chiapasco,
Tridimensional Reconstruction of Knife-Edge Edentulous Maxillae by Sinus Elevation, Onlay Grafts, and Sagittal Osteotomy of the Anterior Maxilla: Preliminary Surgical and Prosthetic Results Matteo Chiapasco,
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation. Sanju P. Jose
 Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
We Want to Keep You Smiling. Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
Retrospective success and survival rates of dental implants placed with simultaneous bone augmentation in partially edentulous patients
 Nima Bazrafshan Ivan Darby Retrospective success and survival rates of dental implants placed with simultaneous bone augmentation in partially edentulous patients Authors affiliations: Nima Bazrafshan,
Nima Bazrafshan Ivan Darby Retrospective success and survival rates of dental implants placed with simultaneous bone augmentation in partially edentulous patients Authors affiliations: Nima Bazrafshan,
