Case Series. Guided Bone Regeneration for Dehiscence and Fenestration Defects on Implants Using an Absorbable. polymer barriers.
|
|
|
- Kevin Palmer
- 5 years ago
- Views:
Transcription
1 Guided Bone Regeneration for Dehiscence and Fenestration Defects on Implants Using an Absorbable Polymer Barrier Paul S. Rosen* and Mark A. Reynolds Background: Guided bone regeneration (GBR) using a non-absorbable barrier has provided clinicians the ability to place implants in sites compromised by insufficient bone, including immediate extraction sites. Recent evidence suggests that successful GBR outcomes may be possible using bioabsorbable polymer barriers. Methods: This report presents a case series of 9 patients with 8 fenestration and 3 dehiscence defects on implants consecutively treated with GBR. A bioabsorbable polymer barrier of poly(dl-lactide) was used in conjunction with a composite graft of freeze-dried bone allograft (FDBA)/demineralized freeze-dried bone allograft (DFDBA) mixed in a ratio of 1 1. Secondstage surgeries were performed at 4 to 8.5 months (5.7 months average) post-placement. Biopsy material from 2 sites was obtained while exposing the implant for healing abutment connection. Results: Ten of the 11 defects (90.9%) achieved complete coverage of the osseous defects. Histologic evaluations revealed the formation of viable bone, frequently in close amalgamation with residual graft particles. Conclusion: These case reports suggest that a poly(dl-lactide) polymer can be used as a physical barrier with a composite bone replacement graft to achieve successful GBR results of dehiscence/fenestration defects when placing implants. J Periodontol 2001;72: KEY WORDS Guided bone regeneration; grafts, bone; membranes, barrier; membranes, bioabsorbable; polylactic acid/therapeutic use; follow-up studies. * Department of Periodontics, Baltimore College of Dental Surgery, University of Maryland, Baltimore, MD and private practice, Yardley, PA. Departments of Oral and Maxillofacial Pathology and Periodontics, Baltimore College of Dental Surgery. University of Maryland. Guided bone regeneration (GBR) has made the placement of implants possible in sites that were not a part of the original implant protocol. 1 GBR has expanded the predictable treatment options for clinicians to meet patients esthetic and masticatory needs. The principles of GBR date back over 30 years. 2-4 Early experimental studies, 5-8 clinical studies, 9-14 and case reports demonstrated successful outcomes for GBR in a wide variety of osseous defects, thereby facilitating the placement of implants. The vast majority of GBR reports have discussed the successful use of expanded polytetrafluoroethylene (eptfe), a non-absorbable barrier, either alone 9-14,17-19,22,25,28,33,36-39 or in combination with a bone replacement graft. 20,21,23,24,26,29-32,36,40 Because of the requirement for removal of nonabsorbable barriers, considerable interest has emerged in developing alternative absorbable materials. An absorbable barrier has been developed where a polymer of poly(dl-lactide) is dissolved in a carrier of N-methyl-2-pyrrolidone which, upon contact with water or other aqueous solution, forms a barrier of firm consistency. Originally, a partially set barrier was formed at chairside that could be trimmed to the dimensions of a periodontal defect. 42,43 Once placed, the polymer completely solidified in situ, forming an absorbable barrier for GTR. 44 A regenerative technique for periodontal defects has recently been described where this poly(dl-lactide) polymer was flowed in situ to form a custom fitting barrier directly over composite bone replacement graft, resulting in successful clinical outcomes. 45,46 Since the polymer does not significantly degrade for 5 to 6 months, 44 the same benefits of clot stability, space maintenance, and tissue exclusion might also be gained in GBR procedures with implants. Consistent with this possibility, a barrier of polylactic acid/polyglycolic acid (PLA/PGA) used in combination with an autogenous bone replacement graft was recently shown to be effective Gore-Tex, W.L. Gore & Associates, Inc., Flagstaff, AZ. Atrisorb, Block Drug, Jersey City, NJ. 250
2 in the treatment of dehiscence/fenestrations around implants. 47 The purpose of this report is to present consecutive clinical experiences with a poly(dl-lactide) polymer barrier in combination with a composite bone replacement graft for GBR of dehiscence/fenestration defects during implant placement. Implant sites requiring ostectomy for exposure of the fixture permitted histologic evaluation of the new bone formation. CASE SERIES DESCRIPTION Nine consecutively treated patients (7 male and 2 female) with an average age of 52.7 (range 32 to 81) years had a total of 11 implant fixtures L placed in combination with a GBR procedure. All of the patients were non-smokers. The implant surgeries were conducted utilizing standard protocols of the respective implant systems, notwithstanding the GBR procedure. All implant placements were done in the absence of pre-tapping the site. Photographs were taken of the implant and GBR procedure, and clinical measurements were made of the dehiscence/fenestration defects treated. All measurements were done from the most coronal aspect of the implant collar to the base of the defect. All defects received a composite graft of demineralized freeze-dried bone allograft (DFDBA) (particle size 250 to 710 µm) mixed with freeze-dried bone allograft (FDBA) (particle size 250 to 710 µm) in a 1 1 ratio. Both graft materials were obtained from a tissue bank that has demonstrated inductivity for its DFDBA material. #48 The graft was rehydrated with sterile saline prior to its placement around the implants and the defect was filled incrementally using light pressure. A method of barrier placement was used where the poly(dl-lactide) polymer was formed rapidly at chairside (M. Abou-Rass; unpublished data). Six to 10 drops of polymer were placed from the dose pack into a sterile glass dappen dish. Sterile saline was added in a ratio of one drop for every two drops of polymer. A 7A wax spatula** introduced the saline throughout the polymer and rapid mixing was performed for 8 to 10 seconds in order to drive off the N-methyl-2- pyrrolidone carrier. Care was taken to press the forming barrier against the sides of the dappen dish to begin barrier formation. Corn suture pliers** were used to remove the polymer barrier from the dappen dish to trim it to an appropriate size with suture scissors. If necessary, the barrier was handled with gloves to facilitate trimming. The barrier, which was approximately 0.5 to 1.0 mm thick, was placed at the graft site with 2 to 3 mm overlapping the adjacent osseous structure. If additional barrier was needed, the same process was repeated with the new piece overlapping the prior barrier, thereby coalescing the pieces together by physical bond. The endpoint of flap management was passive primary closure, which was achieved by using releasing incisions that extended well beyond the mucogingival junction and into the buccal turn of the vestibule. Partial thickness dissection in the apical portion of the facial flaps allowed the flaps to be passively drawn together. A monofilament suture was used of an absorbable or a non-absorbable material for flap adaptation. The antibiotic regimen was 2 g of amoxicillin at the time of implant surgery followed by 500 mg t.i.d. for 8 to 10 days. This regimen was followed by doxycycline 100 mg, 2 capsules on the first day and then 1 capsule per day for 10 days. Two patients were allergic to amoxicillin and were placed on the doxycycline regimen for a total of 14 days. Doxycyline was administered primarily for its antimicrobial property but also, in part, for its anticollagenase activity. 49 Patients were instructed to use a 0.12% chlorhexidine rinse b.i.d. for the first 30 days or during the entire healing period if the barrier became exposed. The success or failure of the GBR procedure was assessed at the second-stage surgery when flaps were reflected to place healing abutments. Clinical photographs were used to determine results of treatment. Complete success, partial success, and failure were based on previously published clinical criteria. 29 Complete success was defined as coverage of all threads or exposed implant surfaces. Partial success was deemed as incomplete coverage of most threads or exposed implant surfaces with a maximum of 2 threads or 2 mm of implant surface left uncovered. Failure was defined as no coverage beyond 2 threads or 2 mm of implant surface. The osseous defects treated included 8 dehiscence and 3 fenestration defects. Representative clinical cases and outcomes are illustrated in Figures 1 and 2. Second-stage surgeries and evaluations were performed between 4.0 and 8.5 months (5.7 months average). RESULTS Table 1 summarizes the outcomes of the GBR procedures for all sites. The length of the defects ranged L Osseotite, Implant Innovations, Inc., Palm Beach Gardens, FL. Replace, Nobel Biocare, Yorba Linda, CA. # LifeNet, Virginia Beach, VA. ** Hu-Friedy, Chicago, IL. Monocryl, Ethicon, Sommerville, NJ. J Periodontol February 2001 Rosen, Reynolds 251
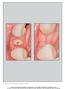
3 from 2 to 13 exposed threads with an average of 8.5 exposed threads. With the exception of one dehiscence lesion that had partial coverage, all other defects had complete coverage of the implants, representing a 90.9% success rate. Premature loss of the barrier occurred at one implant site approximately 4 weeks following clinical exposure; however, this site had complete coverage of the implant with hard tissue at stage 2 surgery. Premature loss of the barrier, based on patient report, Figure 1. A. Placement of 3.25 mm 18 mm implant at maxillary right lateral incisor site, which shows a fenestration defect exposing 13 threads in this 32-year-old male. A dehiscence of 16 exposed threads is present on a 4.0 mm 13 mm implant placed at the #8 site.teeth had been lost due to a prior accident. B. A 3.25 mm 15 mm implant placed at the #9 site, in the same patient, has a thin alveolar plate with a fenestration defect exposing 13 threads.the implant at the #10 site has a thin labial plate of bone. C.Two barriers have been rapidly formed at chairside and placed over a composite osseous graft of DFDBA/FDBA (ratio of 1 1) which covers the surfaces of the implants. D. Reentry at 6 months, with healing abutments in place, is consistent with amalgamated fibrous connective tissue and bone formed over the implant surfaces and the defects. E. Photomicrograph of tissue removed over cover screws at stage 2 procedure (original magnification 10). Evidence of amalgamation of new bone (NB) with osteoblasts (O) rimming residual graft particles is seen. 252 Guided Bone Regeneration Using Bioabsorbable Barriers
4 Figure 2. A. Placement of 4 mm 11.5 mm implant into maxillary right canine site, which shows a dehiscence defect of 8 exposed threads in this 55-yearold female. B. Composite osseous graft of DFDBA/FDBA in a ratio of 1 1 is placed over the implant and the defect. C. A barrier has been rapidly formed at chairside and placed over the site extending at least 2 mm beyond the graft and defect. D. Reentry at 6 months demonstrates that the defect and implant have been covered by hard tissue. was presumably related to physical forces during mastication causing fragmentation. The barriers were otherwise well tolerated by the tissue with no sites demonstrating untoward granulation reactions or infection. The histologic evaluation of biopsy specimens revealed the presence of viable bone and residual graft particles. Islands of viable bone were frequently observed in close amalgamation with graft particles. Notably absent in all specimens was evidence of an inflammatory cell infiltrate. DISCUSSION The clinical outcomes of this case series are consistent with the results of studies 9,13 and case reports 20,21,25,32 describing the application of nonabsorbable and bioabsorbable barriers in GBR therapy. Nevertheless, comparisons across studies remain difficult because of differences in the variety of bone defects treated, temporal sequencing of implant and GBR surgeries, and surgical outcome measures. Given the concern for the preservation of esthetics, outcome criteria were chosen based on implant coverage by either bone and/or connective tissue. 29 Removal of any dense connective tissue present might have compromised regenerated bone, which could have impacted on the soft tissue height. Preservation of tissue height was of great concern since over half of the implants were placed in the maxillary anterior region. A bone replacement graft was used in combination with the polymer barrier, in part, to avoid barrier deformation prior to its final formation. Consistent with this possibility, an absorbable barrier of PLA/PGA was previously associated with reduced regenerative outcomes, compared to eptfe due to collapse of the J Periodontol February 2001 Rosen, Reynolds 253
5 Table 1. Dehiscence/Fenestration Sites Treated With a Bioabsorbable Polymer Barrier for GBR Success Patient Age Gender Site Implant Implant Size Defect Exposed Threads Stage 2 (Months) Outcome Problem 1 49 M 13 Osseo 4 x 13 Fen 11 5 Complete 2 48 M 21 Osseo 4 x 13 Deh 6 7 Complete Exposure 3 32 M 7 Osseo 3.25 x 18 Fen 13 6 Complete 8 Osseo 4 x 13 Deh 12 6 Complete 9 Osseo 3.25 x 15 Deh 12 6 Complete 4 50 M 12 Repl 4.3 x 16 Fen Complete 5 54 F 5 Osseo 3.25 x 13 Deh 2 4 Complete 6 55 F 7 Osseo 4 x 11.5 Deh 7 6 Complete 7 61 M 11 Osseo 3.25 x 13 Deh 5 5 Partial 8 81 M 11 Osseo 4 x 15 Deh 7 4 Complete 9 44 M 9 Repl 4.3 x 10 Deh 5 5 Complete Average Osseo = Osseotite; Repl = Replace; Deh = dehiscence; Fen = fenestration. barrier. 49 In these case reports, the GBR procedure incorporated a composite graft of DFDBA/FDBA in a 1 1 ratio, which previously has been shown to support successful regenerative outcomes. 20 The concept of mixing these 2 graft materials capitalizes on combining the potential osteoinductive/osteoconductive capabilities of DFDBA 48,51 with the osteoconductive and spacemaking advantages of FDBA. 20 Allograft materials used in this case series were obtained from the same tissue bank, which routinely verifies the osteoinductive potential of its processed DFDBA in the athymic mouse model. 48 Histologic evaluation of the new bone formation was possible at 2 sites, where ostectomy had been required to expose the implant for placement of the healing abutment. In all histologic specimens, viable bone was observed in the absence of an inflammatory cell infiltrate. These histologic findings are consistent with previous reports following the use of DFDBA in regenerative therapy. 52,53 There are a number of advantages to a liquid polymer barrier. Previous reports demonstrated the clinical benefits of the poly(dl-lactide) barrier, which can be formed chairside 42,43 or in situ 45,46 for GTR procedures. This case series documents the successful application of the poly(dl-lactide) barrier with bone replacement grafts in GBR procedures involving implants. This dual capacity for GBR and GTR use simplifies the clinician s inventory of barriers since the material can be flowed or trimmed to a variety of clinical situations. This barrier material has also demonstrated an intrinsic antimicrobial property. 54 The polymer system permits repair or modification of the barrier if it is inaccurately cut or trimmed since additional material can be added to the existing barrier with the 2 coalescing. The barrier s final consistency is hard and rigid, adding to its space maintenance capabilities. It takes approximately 5 to 6 months for significant degradation of the barrier to begin, and since it is completely absorbed by 12 months, there is less concern that remaining barrier could affect the site. There are also some limitations to this barrier. The final consistency of the material is hard and firm, making it susceptible to fracture and premature loss in the presence of untoward occlusal forces. Although this occurred in a patient at one implant site, the clinical outcome was still favorable. In the presence of large defects, premature loss of the barrier might substantially compromise the regenerative outcome. A second concern is that exposure of the poly(dl-lactide) barrier may also lead to premature loss versus a non-absorbable barrier. Exposure of non-absorbable 254 Guided Bone Regeneration Using Bioabsorbable Barriers
6 barriers, which remain intact, permits bacterial colonization and potentially affects the final regenerative outcome. 55 The regenerative consequences of barrier exposure and loss are related to the maturational stage of the wound healing process. The results of this consecutive case series suggest that a poly(dl-lactide) polymer can be used as a physical barrier with a composite bone replacement graft to achieve successful GBR results at dehiscence and fenestration defects when placing implants. The compilation of case information is ongoing to determine whether similar results will be found in a larger series of patients. REFERENCES 1. Brånemark P-I, Hansson B, Adell R, et al. Osseointegrated implants in the treatment of the edentulous jaw: Experiences from a 10-year period. Scand J Plast Reconstr Surg 1977;11(Suppl.16): Murray G, Holden R, Roachleu W. Experimental and clinical study of new growth of bone in a cavity. Am J Surg 1957;96: Linghorne WJ. The sequence of events in osteogenesis as studied in polyethylene tubes. Ann NY Acad Sci 1960;85: Melcher AH, Dwyer CJ. Protection of the blood clot in the healing of circumscribed bone defects. J Bone Joint Surg (Br) 1962;48: Dahlin C, Sennerby L, Lekholm U, Linde A, Nyman S. Generation of new bone around titanium implants using a membrane technique: An experimental study in rabbits. Int J Oral Maxillofac Implants 1989;4: Seibert J, Nyman S. Localized ridge augmentation in dogs. A pilot study using membranes and hydroxyapatite. J Periodontol 1990;61: Becker W, Becker BE, Handlesman M, et al. Bone formation at dehisced dental implant sites treated with implant augmentation material: A pilot study in dogs. Int J Periodontics Restorative Dent 1990;10: Becker W, Becker B, Handlesman M, Ochsenbein C, Albrektsson T. Guided tissue regeneration for implants placed into extraction sockets. A study in dogs. J Periodontol 1991;62: Dahlin C, Andersson L, Linde A. Bone augmentation at fenestrated implants by an osteopromotive membrane technique. A controlled clinical study. Clin Oral Implants Res 1991;2: Becker W, Dahlin C, Becker BE, et al. The use of e- PTFE barrier membranes for bone promotion around titanium implants placed into extraction sockets: A prospective multicenter study. Int J Oral Maxillofac Implants 1994;9: Jovanovic SA, Spiekermann H, Richter EJ. Bone regeneration around titanium dental implants in dehisced defect sites: A clinical study. Int J Oral Maxillofac Implants 1992;7: Simion M, Baldoni M, Rossi P, Zaffe D. Comparative study of the effectiveness of GTAM membranes with and without early exposure during the healing period. Int J Periodontics Restorative Dent 1994;14: Dahlin C, Lekholm U, Becker W, et al. Treatment of fenestration and dehiscence bone defects around oral implants using the guided tissue regeneration technique: A prospective multicenter study. Int J Oral Maxillofac Implants 1995;10: Andersson B, Odman P, Widmark G, Waas A. Anterior tooth replacement with implants in patients with a narrow alveolar ridge form. A clinical study using guided tissue regeneration. Clin Oral Implants Res 1993;4: Block M, Kent J. Placement of endosseous implants into tooth extraction sites. J Oral Maxillofac Surg 1991;49: Yukna R. Clinical comparison of hydroxyapatite-coated titanium dental implants placed in fresh extraction sockets and healed sites. J Periodontol 1991;62: Augthun M, Yildirim M, Spiekermann H, Biesterfeld S. Healing of bone defects in combination with immediate implants using the membrane technique. Int J Oral Maxillofac Implants 1995;10: Lazarra R. Immediate placement into extraction sites: Surgical and restorative advantages. Int J Periodontics Restorative Dent 1989;9: Wachtel HC, Langford A, Bernimoulin JP, Reichart P. Guided bone regeneration next to osseointegrated implants in humans. Int J Oral Maxillofac Implants 1991;6: Shanaman RH. A retrospective study of 237 sites treated consecutively with guided tissue regeneration. Int J Periodontics Restorative Dent 1994;14: Fugazzotto PA, Shanaman R, Manos T, Shectman R. Guided bone regeneration around titanium implants: Report of the treatment of 1,503 sites with clinical reentries. Int J Periodontics Restorative Dent 1997;17: Becker W, Becker BE, McGuire MK. Localized ridge augmentation using absorbable pins and eptfe barrier membranes: A new surgical technique. Case reports. Int J Periodontics Restorative Dent 1994;14: Buser D, Dula K, Belser U, Hirt H-P, Berthold H. Localized ridge augmentation using guided bone regeneration. I. Surgical procedure in the maxilla. Int J Periodontics Restorative Dent 1993;13: Buser D, Bragger U, Lang NP, Nyman S. Regeneration and enlargement of jawbone using guided tissue regeneration. Clin Oral Implants Res 1990;1: Buser D, Hirt H-P, Dula K, Berthold H. GBR-technique/implant dentistry. Schweiz Monatsschr Zahnmed 1992;102: Buser D, Dula K, Belser UC, Hirt H-P, Berthold H. Localized ridge augmentation using guided bone regeneration. II. Surgical procedure in the mandible. Int J Periodontics Restorative Dent 1995;15: Callan DP, Rohrer MD. Use of bovine-derived hydroxyapatite in the treatment of edentulous ridge defects: A human clinical and histologic case report. J Periodontol 1993;64: Dahlin C, Lekholm U, Linde A. Membrane induced bone augmentation at titanium implants. Int J Periodontics Restorative Dent 1991;11: Mellonig JT, Triplett RG. Guided tissue regeneration J Periodontol February 2001 Rosen, Reynolds 255
7 and endosseous dental implants. Int J Periodontics Restorative Dent 1993;13: Nevins M, Mellonig J. Enhancement of the damaged edentulous ridge to receive dental implants: A combination of allograft and the Gore-Tex membrane. Int J Periodontics Restorative Dent 1992;12: Nevins M, Mellonig JT. The advantages of localized ridge augmentation prior to implant placement: A staged event. Int J Periodontics Restorative Dent 1994; 14: Rominger JW, Triplett RG. The use of guided tissue regeneration to improve implant osseointegration. J Oral Maxillofac Surg 1994;52: Simion M, Baldoni M, Zaffe D. Jaw bone enlargement using immediate implant placement associated with a split-crest technique and guided tissue regeneration. Int J Periodontics Restorative Dent 1992;12: Jovanovic SA, Nevins M. Bone formation utilizing titanium-reinforced barrier membranes. Int J Periodontics Restorative Dent 1995;15: Simion M, Trisi C, Piattelli A. Vertical ridge augmentation using a membrane technique associated with osseointegrated implants. Int J Periodontics Restorative Dent 1994;14: Gelb DA. Immediate implant surgery: Three-year retrospective evaluation of 50 consecutive cases. Int J Oral Maxillofac Implants 1993;8: Becker W, Becker B. Guided tissue regeneration for implants placed into extraction sockets and for implant dehiscences: Surgical techniques and case report. Int J Periodontics Restorative Dent 1990;10: Tolman D, Keller E. Endosseous implant placement immediately following dental extraction and alveoloplasty: Preliminary report with 6-year follow-up. Int J Oral Maxillofac Implants 1991;6: Wilson T Jr. Guided tissue regeneration around dental implants in immediate and recent extraction sites: Initial observations. Int J Periodontics Restorative Dent 1992;12: Watzek G, Haider R, Mensdorff-Puilly N, Haas R. Immediate and delayed implantation for complete restoration of the jaw following extraction of all residual teeth: A retrospective study comparing different types of serial immediate implantation. Int J Oral Maxillofac Implants 1995;10: Ashman A. An immediate tooth root replacement: An implant cylinder and synthetic bone combination. J Oral Implantol 1990;16: Polson AM, Southard GL, Dunn RD, Polson AP, Billen JR, Laster LL. Initial study of guided tissue regeneration in Class II furcation defects after use of a biodegradable barrier. Int J Periodontics Restorative Dent 1995;15: Polson AM, Garrett S, Stoller NH, et al. Guided tissue regeneration in human furcation defects after using a biodegradable barrier: A multi-center feasibility study. J Periodontol 1995;66: Coontz BA, Whitman SL, O Donnell M, et al. Biodegradation and biocompatibility of a guided tissue regeneration barrier formed from a liquid polymer material. J Biomed Mater Res 1998;42: Rosen PS, Reynolds MA, Bowers GM. A technique report on the in situ application of Atrisorb as a barrier for combination therapy. Int J Periodontics Restorative Dent 1998;18: Rosen PS, Reynolds MA. Polymer-assisted regenerative therapy: Case reports of 22 consecutively treated periodontal defects with a novel combined surgical approach. J Periodontol 1999;70: Simion M, Misitano U, Gionso L, Salvato A. Treatment of dehiscences and fenestrations around dental implants using resorbable and nonresorbable membranes associated with bone autografts: A comparative study. Int J Oral Maxillofac Implants 1997;12: Schwartz Z, Somers A, Mellonig JT, et al. Ability of commercial demineralized freeze-dried bone allograft to induce new bone formation is dependent on donor age but not gender. J Periodontol 1998;69: Vernillo AT, Ramamurthy NS, Golub LM, Rifkin BR. The nonantimicrobial properties of tetracycline for the treatment of periodontal disease. Curr Opin Periodontol 1994;2: Simion M, Scarano A, Gionso L, Piattelli A. Guided bone regeneration using resorbable and nonresorbable membranes: A comparative histological study in humans. Int J Oral Maxillofac Implants 1996;11: Schwartz Z, Mellonig JT, Carnes DL Jr., et al. Ability of commercial demineralized freeze dried bone allograft to induce new bone formation. J Periodontol 1996;67: Simion M, Trisi P, Piattelli A. GBR with an e-ptfe membrane associated with DFDBA: Histologic and histochemical analysis in a human implant retrieved after 4 years of loading. Int J Periodontics Restorative Dent 1996;16: Reynolds MA, Bowers GM. Fate of demineralized freeze-dried bone allografts in human intrabony defects. J Periodontol 1996;67: Botz M, Ronhold CH, Godowski KC, Dunn RD, Southard GL. Intrinsic antimicrobial properties of a bioabsorbable GTR barrier. J Dent Res 1997;76(Spec. Issue):435 (Abstr. 3375). 55. Nowzari H, Slots J. Microbiologic and clinical study of polytetrafluoroethylene membranes for guided bone regeneration around implants. Int J Oral Maxillofac Implants 1995;10: Send reprint requests to: Dr. Paul S. Rosen, 907 Floral Vale Boulevard, Yardley, PA Accepted for publication July 14, Guided Bone Regeneration Using Bioabsorbable Barriers
Years of research and advancement in
 Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report
 Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla
 Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla Luciano Malchiodi, MD, DDS*/Antonio Scarano, DDS**/Manlio Quaranta, MD, DDS***/ Adriano
Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla Luciano Malchiodi, MD, DDS*/Antonio Scarano, DDS**/Manlio Quaranta, MD, DDS***/ Adriano
Asufficient quantity of bone is an essential prerequisite
 Clinical Evaluation of a Bilayered Collagen Membrane (Bio-Gide) Supported by Autografts in the Treatment of Bone Defects Around Implants Georges Tawil, DDS, DSc, OD 1 /Georgina El-Ghoule, DDS 2 /Muhieddine
Clinical Evaluation of a Bilayered Collagen Membrane (Bio-Gide) Supported by Autografts in the Treatment of Bone Defects Around Implants Georges Tawil, DDS, DSc, OD 1 /Georgina El-Ghoule, DDS 2 /Muhieddine
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Ridge Split Procedure
 Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
Severe alveolar bone loss related to traumatic
 Simultaneous Implant Placement and Vertical Ridge Augmentation with a Titanium-Reinforced Membrane: A Case Report Roberto Cornelini, MD, DDS 1 /Filippo Cangini, DDS 2 /Ugo Covani, MD, DDS 3 /Sebastiano
Simultaneous Implant Placement and Vertical Ridge Augmentation with a Titanium-Reinforced Membrane: A Case Report Roberto Cornelini, MD, DDS 1 /Filippo Cangini, DDS 2 /Ugo Covani, MD, DDS 3 /Sebastiano
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Guided bone regeneration
 CLINICAL REGENERATION OF THE ALVEOLAR CREST USING TITANIUM MICROMESH WITH AUTOLOGOUS BONE AND A RESORBABLE MEMBRANE Marco Degidi, MD, DDS Antonio Scarano, DDS Adriano Piattelli, MD, DDS KEY WORDS Alveolar
CLINICAL REGENERATION OF THE ALVEOLAR CREST USING TITANIUM MICROMESH WITH AUTOLOGOUS BONE AND A RESORBABLE MEMBRANE Marco Degidi, MD, DDS Antonio Scarano, DDS Adriano Piattelli, MD, DDS KEY WORDS Alveolar
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
Vertical and horizontal alveolar ridge augmentation
 CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
Conventional guided bone regeneration
 CLINICAL MINIMALLY INVASIVE GUIDED BONE REGENERATION Efraim Kfir, DDS; Vered Kfir, DDS; Eli Eliav, DMD, PhD; Edo Kaluski, MD Guided bone regeneration (GBR) is indicated when there is a volume deficiency
CLINICAL MINIMALLY INVASIVE GUIDED BONE REGENERATION Efraim Kfir, DDS; Vered Kfir, DDS; Eli Eliav, DMD, PhD; Edo Kaluski, MD Guided bone regeneration (GBR) is indicated when there is a volume deficiency
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region
 CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS
 OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS DESCRIPTION OSSIX PLUS is a biodegradable and biocompatible collagen membrane intended for use during the process of guided
OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS DESCRIPTION OSSIX PLUS is a biodegradable and biocompatible collagen membrane intended for use during the process of guided
Successful osseointegration of implants has been
 Therapeutic Management for Immediate Implant Placement in Sites with Periapical Deficiencies Where Coronal Bone Is Present: Technique and Case Report Cyril I. Evian, DMD 1 /Ahmed Al-Momani, BDS 2 /Edwin
Therapeutic Management for Immediate Implant Placement in Sites with Periapical Deficiencies Where Coronal Bone Is Present: Technique and Case Report Cyril I. Evian, DMD 1 /Ahmed Al-Momani, BDS 2 /Edwin
Guided bone regeneration using two types of non-resorbable barrier membranes
 DOI:10.5125/jkaoms.2010.36.4.275 Guided bone regeneration using two types of non-resorbable barrier membranes Ji-Young Lee 1, Young-Kyun Kim 1, Pil-Young Yun 1, Ji-Su Oh 2, Su-Gwan Kim 2 1 Department of
DOI:10.5125/jkaoms.2010.36.4.275 Guided bone regeneration using two types of non-resorbable barrier membranes Ji-Young Lee 1, Young-Kyun Kim 1, Pil-Young Yun 1, Ji-Su Oh 2, Su-Gwan Kim 2 1 Department of
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
The Sandwich Bone Augmentation Technique. Jia-Hui Fu* and Hom-Lay Wang*
 CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
 227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Risk Factors for Wound Dehiscence after Guided Bone Regeneration in Dental Implant Surgery
 Maxillofac Plast Reconstr Surg 2014;36(3):116-123 http://dx.doi.org/10.14402/jkamprs.2014.36.3.116 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Original Article Risk Factors for Wound Dehiscence after
Maxillofac Plast Reconstr Surg 2014;36(3):116-123 http://dx.doi.org/10.14402/jkamprs.2014.36.3.116 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Original Article Risk Factors for Wound Dehiscence after
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26
 P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26 Please complete the speaker evaluation form in the Midwinter Meeting
P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26 Please complete the speaker evaluation form in the Midwinter Meeting
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS
 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT
 MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation. Sanju P. Jose
 Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Without intervention, alveolar
 J Periodontol July 2008 Clinical and Histologic Assessment of Lateral Alveolar Ridge Augmentation Using a Synthetic Long-Term Bioabsorbable Membrane andanallograft Nicolaas C. Geurs,* Jonathan M. Korostoff,
J Periodontol July 2008 Clinical and Histologic Assessment of Lateral Alveolar Ridge Augmentation Using a Synthetic Long-Term Bioabsorbable Membrane andanallograft Nicolaas C. Geurs,* Jonathan M. Korostoff,
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Clinical cases by Dr. Fernando Rojas-Vizcaya. botiss. dental bone & tissue regeneration. biomaterials. strictly biologic
 Clinical cases by Dr. Fernando Rojas-Vizcaya dental bone & tissue regeneration botiss biomaterials strictly biologic botiss BTR system: BONE biologic potential bovine block & granules: pure bone mineral
Clinical cases by Dr. Fernando Rojas-Vizcaya dental bone & tissue regeneration botiss biomaterials strictly biologic botiss BTR system: BONE biologic potential bovine block & granules: pure bone mineral
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Tunnel Access for Guided Bone Regeneration in the Maxillary Anterior. Thomas M. Johnson and Dmitry Baron
 Tunnel Access for Guided Bone Regeneration in the Maxillary Anterior Thomas M. Johnson and Dmitry Baron Introduction: Minimally invasive surgical techniques in periodontics, including methods for ridge
Tunnel Access for Guided Bone Regeneration in the Maxillary Anterior Thomas M. Johnson and Dmitry Baron Introduction: Minimally invasive surgical techniques in periodontics, including methods for ridge
Pre op Failed endodontic treatment with sinus involvement.
 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A Case Series
 Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Contemporary Periodontal Surgery
 Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla
 CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
Bone Grafting for Socket Preservation
 Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re. Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T
 Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Long-term success for osteointegrated
 CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants
 r s Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants richard t. kao, dds, phd; mark c. fagan, ms, dds; and gregory j. conte, ms, dmd abstract During the treatment
r s Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants richard t. kao, dds, phd; mark c. fagan, ms, dds; and gregory j. conte, ms, dmd abstract During the treatment
Immediate Implants: New Opportunities and Contraindications
 Immediate Implants: New Opportunities and Contraindications Immediate implants are becoming more common and the goal of every immediate implant is to place an implant that is just as healthy with the same
Immediate Implants: New Opportunities and Contraindications Immediate implants are becoming more common and the goal of every immediate implant is to place an implant that is just as healthy with the same
Inion GTR Biodegradable Membrane System
 Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Along with the widespread use of dental implants,
 CLINICAL Clinical Evaluation of 262 Osseointegrated Implants Placed in Sites Grafted With Calcium Phosphosilicate Putty: A Retrospective Study Charles A. Babbush, DDS, MScD 1,2 * Ali Kanawati, DDS, MBA,
CLINICAL Clinical Evaluation of 262 Osseointegrated Implants Placed in Sites Grafted With Calcium Phosphosilicate Putty: A Retrospective Study Charles A. Babbush, DDS, MScD 1,2 * Ali Kanawati, DDS, MBA,
Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report
 Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report W.P. van der Schoor*, A.R.M. van der Schoor Tooth extraction followed
Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report W.P. van der Schoor*, A.R.M. van der Schoor Tooth extraction followed
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
Localized bone regeneration with porcine bone graft: clinical and histological evidences
 Clinical Localized bone regeneration with porcine bone graft: clinical and histological evidences Luca Pagliani, 1 Stefano Volpe 2 Summary Localized bone regeneration with porcine bone graft: clinical
Clinical Localized bone regeneration with porcine bone graft: clinical and histological evidences Luca Pagliani, 1 Stefano Volpe 2 Summary Localized bone regeneration with porcine bone graft: clinical
REASONS TO USE R.T.R.
 3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
Identification of Stability Changes for Immediately Placed Dental Implants
 Identification of Stability Changes for Immediately Placed Dental Implants Jason D. West, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 Purpose: To evaluate the changes in stability of immediately placed implants
Identification of Stability Changes for Immediately Placed Dental Implants Jason D. West, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 Purpose: To evaluate the changes in stability of immediately placed implants
Evaluation of Titanium Implants Placed into Simulated Extraction Sockets: A Study in Dogs
 Evaluation of Titanium Implants Placed into Simulated Extraction Sockets: A Study in Dogs Ken Akimoto, DDS, MS*/William Becker, DDS, MS**/ Rutger Persson, DDS, Odont Dr***/David A. Baker, DDS, MS*/ Michael
Evaluation of Titanium Implants Placed into Simulated Extraction Sockets: A Study in Dogs Ken Akimoto, DDS, MS*/William Becker, DDS, MS**/ Rutger Persson, DDS, Odont Dr***/David A. Baker, DDS, MS*/ Michael
Guided Tissue and Bone Regeneration
 Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
(Images are at the end of article)
 Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Procedure Manual and Catalog
 Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up
 643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Periosteal Pocket Flap for Horizontal Bone Regeneration: A Case Series Marius Steigmann, DDS*/Maurice Salama, DDS, MS**/ Hom-Lay Wang,
The International Journal of Periodontics & Restorative Dentistry 3 Periosteal Pocket Flap for Horizontal Bone Regeneration: A Case Series Marius Steigmann, DDS*/Maurice Salama, DDS, MS**/ Hom-Lay Wang,
Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft
 The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
Since the report of Adell and associates, 1 well-documented
 Immediate Loading of an Implant Following Implant Site Development Using Forced Eruption: A Case Report Young-Seok Park, DDS, MSD 1 /Ki-Young Yi, DDS 2 /Seong-Cheol Moon, DDS, MSD, PhD 3 / Young-Chul Jung,
Immediate Loading of an Implant Following Implant Site Development Using Forced Eruption: A Case Report Young-Seok Park, DDS, MSD 1 /Ki-Young Yi, DDS 2 /Seong-Cheol Moon, DDS, MSD, PhD 3 / Young-Chul Jung,
REGENERATIONTIME. A Case Report by. Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option
 A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
Immediate Implant Placement With Ridge Split in A Siebert's Class 1 Defect - A Case Report
 Immediate Implant Placement With Ridge Split in A Siebert's Class 1 Defect - A Case Report Arjun. M. R 1, Nandini Manjunath 2 1, 2 Department of Periodontics, A. J. Institute of Dental Sciences, India
Immediate Implant Placement With Ridge Split in A Siebert's Class 1 Defect - A Case Report Arjun. M. R 1, Nandini Manjunath 2 1, 2 Department of Periodontics, A. J. Institute of Dental Sciences, India
Innovative Range of Regenerative Solutions
 TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
Redefining Regeneration
 Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Immediate Implant Placement:
 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
We Want to Keep You Smiling. Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
Enhancing implant stability with osseodensification a case report with 2-year follow-up
 Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
COPYRIGHT 2003 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY. NO PART OF THIS ARTICLE MAY BE
 The International Journal of Periodontics & Restorative Dentistry 417 Clinical Evaluation of Freeze-Dried Block Allografts for Alveolar Ridge Augmentation: A Case Series Robert H. Lyford, DDS* Michael
The International Journal of Periodontics & Restorative Dentistry 417 Clinical Evaluation of Freeze-Dried Block Allografts for Alveolar Ridge Augmentation: A Case Series Robert H. Lyford, DDS* Michael
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
