East 25th Street A- ELECTE AD-A JUL
|
|
|
- Georgina Harper
- 5 years ago
- Views:
Transcription
1 . DTIC A- ELECTE AD-A JUL HISTOLOGIC EVALUATION OF A PULYLACTIC ACID CONFLUENT SHEET IN THE TREATMENT OF OSSEOUS DEFECTS BY Charles M. Cobb, DDS, PhD * John C. Reed, DDS + Caesar E. Solano, DMD + W. Robert Hiatt, DDS + Departments of Periodontics and Oral Biology, University of Missouri-Kansas City, School of Dentistry, Kansas City, MO * Departments of Hospital Dentistry and Oral and Maxillofacial Surgery. University of Missouri-Kansas City, School of Dentistry, Kansas City, MO Acknowledgement: This project was supported, in part, by a grant from the United States Navy, Office of Naval Research, Grant No. N J ;Yltrlbutlon 13nflmited All Correspondence To: Dr. Charles M. Cobb Dept. of Periodontics School of Dentistry University of Missouri-Kansas City East 25th Street Kansas City, Missouri 64108
2 A-- i... Tor.i Statement A per telecon.ntl j*'.a David Vanmtre ONR/Code 1511 /ti Arlington, VA INTRODUCTION N 6/25/92 3 Polylactic and polyglycolic acids (alpha polyamides) or L.v±iabillyN combinations thereof are biodegradable materials commonly used in t 9pecial suture materials and surgical meshes for the temporary support of\t abdominal organs. The materials are well known in the clinical literature and have been in common usage without risk for over two decades (1-5). The polyamides are rich in polyester linkages that are degraded in aqueous environments by hydrolysis (5-7). Various investigators have shown that the pure form of polyglycolic acid (PGA) degrades over a period of 5 months whereas pure polylactic acid (PLA) takes about 6.5 months (7, 8). Copolymers of PLA/PGA have been synthesized that degrade within a few weeks to several months depending upon the ratios employed and the specific sequencing of the chemical units (7, 9). Further, the alpha polyamides show no adverse host tissue reactions when implanted in numerous animal models (10-15). As the materials are biodegradable, the rate of which can be controlled by changing the material density, we are suggesting that it may be employed as a matrix for osseous grafting, for the occlusion of large bony defects, for soft tissue contour defects, and also as a bone plating system. All of these applications are based upon the assumption that normal host fibrous and/or osseous tissues will replace the PLA and PGA materials as they undergo biologic degradation. The potential of PLA and PGA or their combination for use in osseous grafting and bone stabilization systems as not been extensively investigated. Indeed, if our assumptions prove correct, pure PLA, PGA or their combination could accomplish all - I-
3 the functions of present day surgical titanium but with the distinct advantage of not requiring a secondary surgery for removal of fixation plates. Thus, the purpose of this study is to determine the fate of a pure PLA when used as a continuous sheet within osseous defects or when placed on both sides of continuity defects in the manner of a bone plate. Further, the type and rate of host tissue replacement was determined as well as the percent fill of the defect with new bone. MATERIALS AND METHODS Animal Model: Twenty-five adult male New Zealand albino rabbits between the ages of 9 and 12 months and weighing approximately 3000 gm were obtained from a licensed commercial vendor through the Laboratory Animal Care (LAC) facility of the University of Missouri-Kansas City. All surgical procedures, postsurgery care, and animal sacrifice were performed in the LAC facility. Animals were caged individually in a standard manner and fed Purina Rabbit Chow plus water ad libitum. All animals were allowed one week of acclimation to their new environment before initiating the experimental protocol. Anesthesia: Upon completion of the acclimation period, animals were prepared for the surgical implantation of the PLA confluent sheets. Food and water were withheld for a twelve hour period prior to surgery. Anesthesia was obtained using the following, egimel,: -2-
4 (1) Preanesthetic intramuscular (IM) administration of Atropine using a dosage of mg/kg. (2) Anesthetic induction using IM administration of Xylazine 5 mg/kg plus Ketamine hydrochloride mg/kg. (3) Anesthetic maintenance was accomplished by using IM Ketamine as required. Anesthesia was confirmed by loss of reflex when pinched on the abdomen and/or loss of eye-blinking reflex. Subsequent to anesthesia, cranial hair was shaved and removed by vacuum. The resulting surgical field was then swabbed with Betadine surgical scrub solution. Surgical and Implantation Procedures: Two full-thickness semilunar flaps were raised using sharp incision and blunt dissection. each flap. The anterior border of the ears formed the base of Using a surgical steel trephine dental-implant bur in a slow-speed high-torque dental handpiece, three osseous defects, approximately 4 mm in diameter, were created in the calvaria equidistant from the mid-sagital suture and from each other. Defects penetrated the complete thickness of calvarial bone but did not violate the integrity of the dura mater. A new sterile bur was used for each animal. Further, during osseous penetration, the field was continuously irrigated with sterile saline containing penicillin (100 units/ml), streptomycin (100 )jg/ml), gentamicin (50 wg/ml), and Fungizone (2.5 yg/ml). Complete removal of all residual osseous fragments was insured by irrigation and simultaneous suctioning. This step was particularly important as osseous grindings left in defects may act as autogenous grafts and bias the experimental evaluation. -3-
5 The implant material used in this investigation consisted of a pure poly (L-lactide) *. One cranial defect in each animal was assigned by random selection and packed with a single 1 mm thick x 4 mm diameter plug of the PLA implant material (Group #1). A second defect, again selected by random assignment, was treated by placement of 1 mm thick x 4 mm diameter confluent sheets of the implant material on either side of the osseous cavity, leaving the defect unfilled (Group #2). This latter procedure required the implant material to be placed in direct contact with the osseous surface, thereby being interposed between bone and dura mater and/or bone and scalp connective tissues. The remaining defect was left untreated and serve as the control (Group #3). Scalp flaps were repositioned and held in place with polyglycolic 4-0 sutures. The scalp overlying implant and control sites was tattooed to aid identification of surgical areas for biopsy at the time of sacrifice. Post-Surgical Care: As it was reasonable to expect some post-surgical pain or distress, a regimen of 1-5 mg/kg of Diazepam administered IM was used on an "as needed basis". All animals were checked daily for the first 3-4 days post-surgery for changes in appetite, physical activity and general appearance. Sample Procurement and Analysis: Animals were randomly selected for sacrifice using Pentobarbital, mo/kg by IV administration until cessation of respiratory and cardiac Resomer L210. From Boehringer-Ingelheim Corp., Ingelheim AM Rhein, Germany -4-
6 function was apparent. Five animals were sacrificed at each of the following time intervals: 3, 7, 14, 21, and 35 days. At the specified time interval, the two implant and control surgical sites were biopsied and tissue placed in labeled bottles containing 10% buffered formalin. After fixation, specimens are demineralized in a solution of EDTA (0.003 M) and HCl acid (1.35 N) and processed for routine hematoxylin and eosin staining Sections for light microscopic examination were cut at 5-6 microns thickness and at 400 micron intervals throughout the diameter of the implant and/or control sites. Thus, each surgical site yielded a minimum of 8-9 histologic sections for data analysis. All microscopic sections at each time interval were evaluated for rate of resportion of and host response to the PLA implant material, i.e., presence, intensity and character of any inflammatory infiltrate; presence of foreign body giant cells, macrophages and osteoclastic resorption of host bone. Further, each section was analyzed for surface area of regenerated bone within the implant site as related to total surface area of the surgical defect. Thus, the percentage of new bone could be calculated and a mean value determined for all implant sites, thereby allowing for comparison of the difference between means for implant versus control sites and calculation of statistical significance using a single factor ANOVA with post hoc multiple pairwise comparisons applied using the Newman-Keuls Studentized Range Statistic assuming a significant omnibus F test. All histomorphometric measurements were accomplished with a commerically available -5-
7 computer software package (Java Video Analysis Software, Jandel Scientific, Corte Madera, CA). RESULTS All twenty-five animals survived the experimental protocol. Thus, the histologic evaluation and statistical analysis was based on a total of 5 specimens (40-45 histologic sections) from each treatment group at each time interval. Histology: At 3 days post-surgery the nontreated control defects (Group #3) exhibited a moderate degree of inflammatory cell infiltrate consisting of neutrophils, lymphocytes and a relatively few macrophages. By 7 days, the inflammatory cell population was a minor feature, having all but disappeared. Initially the intrabony defect was filled with a well formed fibrin clot with evidence of an early capillary proliferation from adjacent bone marrow spaces. Organization of the clot continued at 7 days with both capillary and fibroblastic proliferation originating from adjacent marrow spaces and periosteal and dura mater surfaces. The bony surfaces comprising the proximal walls of the defects exhibited isolated areas of osteoclastic mediated resorption that were still obvious in the 7 day specimens. One or two residual bony spicules were noted within the defect in most sections. The bony defects of 14 day post-surgery control specimens were filled with a dense fibrous connective tissue whose individual fibers exhibited a parallel orientation to one another and to the bony surfaces of the cranium. Interspersed within the -6-
8 connective tissue were randomly distributed areas of active intramembranous bone formation appearing to be trabecular in nature. In contrast, to 3 and 7 day specimens, there was no evidence of osteoclastic activity and the new bone formation made it difficult to identify the walls of the original defect. By 21 and certainly at 35 days post-surgery, the control defects were nearly filled with new trabecular bone and exhibited a well organized endosteum. Further, the periosteum appeared completely regenerated and represented a confluent and intact layer covering the original defect. The specimens in which the PLA implant material was positioned over the superior and inferior bony surfaces of the defect, thereby isolating the defect space from surrounding connective tissues (Group #2), exhibited no apparent differences when compared to controls at the corresponding 3 and 7 days postsurgery time intervals. However, specimens from 14, 21, and 35 days post-surgery appeared to lag behind controls with respect to the density of newly forming trabecular bone. Further, the periosteum regenerated as a confluent layer of fibrous connective tissue covering the superior aspect of the implant material positioned on the cranial surface. In all other respects, Group #2 and Group #3 specimens from the longer time intervals appeared very similar. Regardless of time interval, those intrabony defects in which a plug of the PLA implant material had been placed (Group #1) exhibited only a slight inflammatory reaction which appeared localized to peripheral tissue areas. As the implant -7-
9 material occupied the entire defect, there was little opportunity for capillary or fibroblastic proliferation into the defect space. Further, there was no evidence of a foreign body or giant cell reaction. Osteoclastic resorption of the intrabony defect walls was less active than that seen in controls specimens at corresponding time intervals. The 14, 21, and 35 day specimens all featured an intact layer of periosteum covering the cranial surface of the implant plug. None of the specimens from the longer time intervals showed evidence of a foreign body reaction or resorption of the implant plug or adjacent bone. Table 1 presents the results of the computerized vidio analysis of the surface area of newly formed bone within the defect as a percentage of the total surface area of the defect space. The mean percentage and standard divaiations were derived from measurements of microscopic sections from each experimental group at each time interval. In 12 of 45 microscopic sections from the 7 days postsurgery specimens there were bony spicules evident in Groups #2 and #3 which accounted for a mean percentage of bone formation of 0.50% ± 0.41 and 0.70% ± 0.62 respectively. However, the spicules did not exhibit histologic features characteristic of newly forming bone but rather appeared to be residual from the surgery. Consequently, a statistical evaluation of these specimens was not performed. Analysis of the data revealed a statistically significant increase (p = <.001) in mean percentages of bone regeneration at ---
10 14 days post-surgery in Group #2 (29.00% t 8.50) and Group #3 (34.10% ) when compared to Group #1 (0%). The difference in bony regeneration in Groups #2 and #3 was also significant (p = <.05). These same comparisons were also statistically significant at the 21 days post-surgery interval (p = <.001) when comparing Group #2 (78.30% ± 11.36) and Group #3 (84.20% 8.95) to Group #1 (0.13% ± 0.08). A comparison of the difference between the mean percentage bone increase in the control Group #3 versus that of Group #2 revealed a statistical significance at the p = <.01 level. Analysis of the 35 days post-surgery data revealed statistically significant differences in the mean percentage increase of bone (p = g.001) in Group #2 (89.60% ) and Group #3 (94.30 ± 8.32) when each was compared to Group #1 (0.44% ± 0.23). The increase in mean percentage of bone in Group #3 when compared to that of Group #2 was significant at the p = <.05 level. CONCLUSIONS When compured to control defects (Group #3), the placement of confluent sheets of polylactic acid in close apposition to the superior and inferior bony surfaces of cranial continuity defects (Group #2) resulted in delayed healing responses at 14, 21 & 35 days post-surgery. Based on a comparison of the mean percent surface area of regenerated bone, the delay in healing approximated one week. Given the advantages of avoiding a secondary surgery to remove surgical bone plates, a one week delay in healing becomes clinically insignificant. -9-
11 When compared to control defects (Group #3), the placement of polylactic acid plugs within the bony defect (Group #1) severely retarded the healing response at all time intervals. Based on a comparison of the mean percent surface area of regenerated bone, the delay in healing approximated 7-8 weeks. However, as many of the plugs showed little evidence of resorption by day 35 (termination point of study), the delay in healing response is likely to be considerably longer. Thus, it would appear that planned or inadvertent inclusion of polylactic acid materials within bony defects should be avoided. -10-
12 Table 1. Mean Percent Surface Area of Regenerated Bone Implant Material Positioned Over Defects Filled Superior & Inferior With Implant Plug Surfaces of Defect Controls (Group #1) (Group #2) (Group #3) Mean % S.D. Mean % S.D. Mean % S.D. 3 Days Days ± ± Days ± ± Days ± ± Days t ± ± 8.32 Statistical Significance: Group #1 vs. Group #2: p = <.001 at 14, 21, and 35 days. Group #1 vs. Group #3: p = <.001 at 14, 21, and 35 days. Group #2 vs. Group #3: p = <.01 at 21 days; and p = <.05 at 14 and 35 days. -11-
13 REFERENCES 1. Bostman 0, Makela EA, Tormala P, et al.: Transphyseal fracture fixation using biodegradable pins. J Bone Jt Surg (Br), 71B:706, Hirvensal E: Fracture fixation with biodegradable rods. 41 cases of severe ankle fractures. Acta Orthop Scnada, 60:601, Bostman 0, Hirvensalo E, Vainionpaa S, et al.: Degradable polyglycolide rods for the internal fixation of displaced bimalleolar fractures. Int Orthop, 14:1, Cutright DE, Hunsck EE: Tissue reaction to biodegradable polylactide acid suture. Oral Surg, 31:134, Kulkurni RK, Pani KC, Neuman C, et al.: Polylactic acid for surgical implants. Arch Surg, 93:839, Parsons JR: Restorable materials and composites. New concepts in orthopedic biomaterials. Orthopedics, 8:907, Hollinger JO, Battistone GC: Biodegradable bone repair materials: Polymers and ceramics. Clin Orthop, 207:290, Miller RA, Brady 3M, Cutright DE: Degradation rates of resorbable implants PLA/PGA. J Biomed Mater Res, 11:711, Olson RJ, Roberts DL, Osborn DB: A comparative study of polylactic acid, gel foam in surgical healing of extraction sites. Oral Surg, 53:276, Makela EA, Bainionpaa S, Vihtonek K, et al.: The effect of a penetrating biodegradable implant on the epiphyseal plate: An experimental study on growing rabbits with special regard to polyglacin 910. J Pediatr Orthop, 7:415, Bos RRM, Rozema FR, Boering G, et al.: Bone plate and screws of bioabsorbable poly-l-lactide. An animal pilot study. J Oral Maxillofac Surg (Br), 27:467, Rozema FR, Bos RRM, Pennings A, et al.: Poly-L-lactide implants in repair of defects of the orbital floor. An animal study. J Oral Maxillofac Surg, 48:1305, Bos RRM, Rozema FR, Boering G, et al.: Bio-absorbable plates and screws for the fixation of mandible fractures. A study in six dogs. Internat J Oral Maxillofac Surg, 18:365,
14 14. Suuronen R: Comparison of absorbable self-reinforced poly- L-lactide screws and metallic screws in the fixation of mandibular condyle osteotomies. J Oral Maxillofac Surg, 49:989, Hollinger J, Schmitz JP: Restoration of bone discontinunities in dogs using biodegradable implants. J Oral Maxillofac Surg, 45:594,
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Inion GTR Biodegradable Membrane System
 Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
RAPIDSORB RAPID RESORBABLE FIXATION SYSTEM. A new resorbable approach to Alveolar bone augmentation
 RAPIDSORB RAPID RESORBABLE FIXATION SYSTEM A new resorbable approach to Alveolar bone augmentation RAPIDSORB RAPID RESORBABLE FIXATION SYSTEM Bone Graft Containment The RapidSorb Rapid Resorbable Fixation
RAPIDSORB RAPID RESORBABLE FIXATION SYSTEM A new resorbable approach to Alveolar bone augmentation RAPIDSORB RAPID RESORBABLE FIXATION SYSTEM Bone Graft Containment The RapidSorb Rapid Resorbable Fixation
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
ORIGINAL ARTICLE. deformity is often made difficult because of the inherent
 ORIGINAL ARTICLE The Effects of Resorbable Plates on Rabbit Ear Cartilage Matthew D. Mingrone, MD; Jennifer P. Porter, MD; David B. Lovice, MD; Michael J. Keenan, MD; Kevin O Grady, BS; Tapan K. Bhattacharyya,
ORIGINAL ARTICLE The Effects of Resorbable Plates on Rabbit Ear Cartilage Matthew D. Mingrone, MD; Jennifer P. Porter, MD; David B. Lovice, MD; Michael J. Keenan, MD; Kevin O Grady, BS; Tapan K. Bhattacharyya,
RAPIDSORB RAPID RESORBABLE FIxATION SySTEm
 RAPIDSORB RAPID RESORBABLE FIxATION SySTEm For craniofacial reconstructionruction PRODUCT OVERVIEW RapidSorb Rapid Resorbable Fixation System Features Rapid resorbable implants maintain appropriate fixation
RAPIDSORB RAPID RESORBABLE FIxATION SySTEm For craniofacial reconstructionruction PRODUCT OVERVIEW RapidSorb Rapid Resorbable Fixation System Features Rapid resorbable implants maintain appropriate fixation
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
RapidSorb Resorbable Tacks. Resorbable Fixation System.
 RapidSorb Resorbable Tacks. Resorbable Fixation System. Fast Safe Resorbable Drill Press Fixed Table of Contents Introduction Overview 2 Indications and Contraindications 4 RapidSorb 5 Surgical Technique
RapidSorb Resorbable Tacks. Resorbable Fixation System. Fast Safe Resorbable Drill Press Fixed Table of Contents Introduction Overview 2 Indications and Contraindications 4 RapidSorb 5 Surgical Technique
Initial Fixation Strength of Bio-absorbable Magnesium Screw
 Initial Fixation Strength of Bio-absorbable Magnesium Screw Joon Kyu Lee, MD, PhD, Sahnghoon Lee, Sang Cheol Seong, Myung Chul Lee, MD, PhD. Seoul National University College of Medicine, Seoul, Korea,
Initial Fixation Strength of Bio-absorbable Magnesium Screw Joon Kyu Lee, MD, PhD, Sahnghoon Lee, Sang Cheol Seong, Myung Chul Lee, MD, PhD. Seoul National University College of Medicine, Seoul, Korea,
Bio-degradable osteosynthesis system in treatment of mandibular parasymphysis fractures
 Al Am een J Med Sci 2012; 5(4): 371-375 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G Bio-degradable osteosynthesis system in treatment of mandibular
Al Am een J Med Sci 2012; 5(4): 371-375 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G Bio-degradable osteosynthesis system in treatment of mandibular
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
ORIGINAL ARTICLE. Clinical and Histological Results of Septoplasty With a Resorbable Implant
 Clinical and Histological Results of Septoplasty With a Resorbable Implant Miriam Boenisch, MD; Antal Mink, MD, PhD ORIGINAL ARTICLE Background: The use of a resorbable implant connected with septal cartilage
Clinical and Histological Results of Septoplasty With a Resorbable Implant Miriam Boenisch, MD; Antal Mink, MD, PhD ORIGINAL ARTICLE Background: The use of a resorbable implant connected with septal cartilage
CRANIAL RECONSTRUCTION SOLUTIONS
 CRANIAL RECONSTRUCTION SOLUTIONS CRANIAL RECONSTRUCTION SOLUTIONS Your partner of CHOiCE at depuy Synthes CMF, we are dedicated to providing solutions for your individual patient needs. We do this through
CRANIAL RECONSTRUCTION SOLUTIONS CRANIAL RECONSTRUCTION SOLUTIONS Your partner of CHOiCE at depuy Synthes CMF, we are dedicated to providing solutions for your individual patient needs. We do this through
Application of a Novel Resorbable Membrane in the Treatment of Calvarial Defects in Rats
 Journal of Biomaterials Science (2010) DOI:10.1163/092050610X540477 brill.nl/jbs Application of a Novel Resorbable Membrane in the Treatment of Calvarial Defects in Rats Yanjun Ge, Hailan Feng and Lei
Journal of Biomaterials Science (2010) DOI:10.1163/092050610X540477 brill.nl/jbs Application of a Novel Resorbable Membrane in the Treatment of Calvarial Defects in Rats Yanjun Ge, Hailan Feng and Lei
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Cordis EXOSEAL Vascular Closure Device
 to receive our latest news and key activities. Cordis EXOSEAL Vascular Closure Device Polyglycolic Acid Plug (PGA) Material Absorption and Tissue Reaction Assessment 3 Days* 14 Days* 60 Days* LinkedIn
to receive our latest news and key activities. Cordis EXOSEAL Vascular Closure Device Polyglycolic Acid Plug (PGA) Material Absorption and Tissue Reaction Assessment 3 Days* 14 Days* 60 Days* LinkedIn
Bone Grafting for Socket Preservation
 Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
11/4/13. Ultrasonically Fabricated Barriers in GBR. Ultrasonically Fabricated Barriers in GBR
 Kevin G. Murphy, DDS, MS Associate Professor of Periodontics Baltimore College of Dentistry University of Maryland Private Practice, Baltimore, MD kevin@periopros.net THE USE OF ULTRASONICALLY FABRICATED
Kevin G. Murphy, DDS, MS Associate Professor of Periodontics Baltimore College of Dentistry University of Maryland Private Practice, Baltimore, MD kevin@periopros.net THE USE OF ULTRASONICALLY FABRICATED
Enhancing implant stability with osseodensification a case report with 2-year follow-up
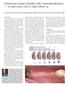 Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2, Patrick Smith, M.D. 2, and Larry S. Matthews, M.D. 2
 Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Detecting a sinus perforation.
 Extractions and the Sinus Dentistry s Black Hole. Detecting a sinus perforation. How to know when you have a small perforation? Need: Adequate light (headlight preferred) Small suction tip (2 mm diameter)
Extractions and the Sinus Dentistry s Black Hole. Detecting a sinus perforation. How to know when you have a small perforation? Need: Adequate light (headlight preferred) Small suction tip (2 mm diameter)
Two-Year Follow-up on the Use of Absorbable Mesh Plates in the Treatment of Medial Orbital Wall Fractures
 Two-Year Follow-up on the Use of Absorbable Mesh Plates in the Treatment of Medial Orbital Wall Fractures Original Article Jae-Pil You, Deok-Woo Kim, Byung-Joon Jeon, Seong-Ho Jeong, Seung-Kyu Han, Eun-Sang
Two-Year Follow-up on the Use of Absorbable Mesh Plates in the Treatment of Medial Orbital Wall Fractures Original Article Jae-Pil You, Deok-Woo Kim, Byung-Joon Jeon, Seong-Ho Jeong, Seung-Kyu Han, Eun-Sang
Procedure Manual and Catalog
 Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Pre op Failed endodontic treatment with sinus involvement.
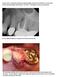 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Spontaneous Regeneration of the Mandible after Hemimandibulectomy:
 Case Report Spontaneous Regeneration of the Mandible after Hemimandibulectomy: Report of a Case A. Khodayari 1, A. Khojasteh 2, MT. Kiani 3, A. Nayebi 4, L. Mehrdad 5, M. Vahdatinia 6 1 DMD, MS. Associate
Case Report Spontaneous Regeneration of the Mandible after Hemimandibulectomy: Report of a Case A. Khodayari 1, A. Khojasteh 2, MT. Kiani 3, A. Nayebi 4, L. Mehrdad 5, M. Vahdatinia 6 1 DMD, MS. Associate
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH
 PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
4766 Research Dr. San Antonio, TX insightdentalsystems.com
 OVERVIEW OF THE INSIGHT DENTAL IMPLANT DELIVERY SYSTEM The IDS system comes in a unit dose implant system where its advantage provides sterile instrumentation in one single-use kit. It is organized to
OVERVIEW OF THE INSIGHT DENTAL IMPLANT DELIVERY SYSTEM The IDS system comes in a unit dose implant system where its advantage provides sterile instrumentation in one single-use kit. It is organized to
Rapid ResoRbable fixation system
 RapidsoRb Rapid ResoRbable fixation system Specialized implants and instruments for craniofacial reconstruction surgical Technique Table of contents Introduction RapidSorb Rapid Resorbable Fixation System
RapidsoRb Rapid ResoRbable fixation system Specialized implants and instruments for craniofacial reconstruction surgical Technique Table of contents Introduction RapidSorb Rapid Resorbable Fixation System
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
Maxillary sinus augmentation without any graft material- A case Report
 A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
Guided Tissue and Bone Regeneration
 Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Clinical Perspectives
 Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Revisions for CDT 2016
 Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Technique Guide. RapidSorb Rapid Resorbable Fixation System. A new resorbable approach to Alveolar bone augmentation.
 Technique Guide RapidSorb Rapid Resorbable Fixation System. A new resorbable approach to Alveolar bone augmentation. Table of Contents Introduction RapidSorb Rapid Resorbable Fixation System 2 RapidSorb
Technique Guide RapidSorb Rapid Resorbable Fixation System. A new resorbable approach to Alveolar bone augmentation. Table of Contents Introduction RapidSorb Rapid Resorbable Fixation System 2 RapidSorb
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
ctive Bone Bonding Bone Regeneration Osteostimulation*
 www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
Maryland AGD AE and Socket Grafting 2015
 The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
ULTRASONIC DEVICE IN BONE CUTTING
 Acta orthop. scand. 52, 5-10, 1981 ULTRASONIC DEVICE IN BONE CUTTING A Histological and Scanning Electron Microscopical Study H. ARO*, H. KALLIONIEMI**, A. J. AHO* & P. KELLOKUMPU-LEHTINEN*** *Department
Acta orthop. scand. 52, 5-10, 1981 ULTRASONIC DEVICE IN BONE CUTTING A Histological and Scanning Electron Microscopical Study H. ARO*, H. KALLIONIEMI**, A. J. AHO* & P. KELLOKUMPU-LEHTINEN*** *Department
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
Low Profile Neuro Plating System. Surgical Technique
 Low Profile Neuro Plating System Surgical Technique TABLE OF CONTENTS INTRODUCTION Low Profile Neuro Plating System 2 SURGICAL TECHNIQUE Technique 5 PRODUCT INFORMATION Low Profile Neuro Plates 10 Low
Low Profile Neuro Plating System Surgical Technique TABLE OF CONTENTS INTRODUCTION Low Profile Neuro Plating System 2 SURGICAL TECHNIQUE Technique 5 PRODUCT INFORMATION Low Profile Neuro Plates 10 Low
Technique Guide. SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction.
 Technique Guide SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction. Table of Contents Introduction SynPOR Porous Polyethylene Implants 2 Indications and Contraindications
Technique Guide SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction. Table of Contents Introduction SynPOR Porous Polyethylene Implants 2 Indications and Contraindications
Properties of GENESYS TM Biocomposite Material Compared to Pure Polylactide (PLA)
 Properties of GENESYS TM Biocomposite Material Compared to Pure Polylactide (PLA) Purpose: To compare the bone in-growth of GENESYS biocomposite material (96L/4D PLA copolymer mixed with β-tcp micro-particles)
Properties of GENESYS TM Biocomposite Material Compared to Pure Polylactide (PLA) Purpose: To compare the bone in-growth of GENESYS biocomposite material (96L/4D PLA copolymer mixed with β-tcp micro-particles)
2018 Dental Code Set For dates of service from 1/1/ /31/2018
 D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
2018 Dental Code Set
 D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
Supplementary Note 1: Anesthesia Record ANESTHESIA RECORD
 Supplementary Note 1: Anesthesia Record ANESTHESIA RECORD Date weight kg Sedation: 1.0 mg/kg Acepromazine (10mg/ml) Protocol # 37.5-52.5 mg/kg Ketamine(100mg/ml) time Pre-op analgesic: 0.02 mg/kg Buprenex
Supplementary Note 1: Anesthesia Record ANESTHESIA RECORD Date weight kg Sedation: 1.0 mg/kg Acepromazine (10mg/ml) Protocol # 37.5-52.5 mg/kg Ketamine(100mg/ml) time Pre-op analgesic: 0.02 mg/kg Buprenex
Pathophysiology of fracture healing
 Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
BIOACTIVE SYNTHETIC GRAFT
 B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
BIOH111. o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system
 BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
Years of research and advancement in
 Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Cerasorb M DENTAL. O:\Zulassung\Cerasorb Dental Kanada 2013\Texte\Cerasorb M Dental final IFU docx
 Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
THE NEXT FRONTIER OF BONE REGENERATION
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary
 SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SYNPOR POROUS POLYETHYLENE IMPLANTS. For craniofacial and orbital augmentation and reconstruction
 SYNPOR POROUS POLYETHYLENE IMPLANTS For craniofacial and orbital augmentation and reconstruction SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION SYNPOR Porous Polyethylene Implants 2 Indications and
SYNPOR POROUS POLYETHYLENE IMPLANTS For craniofacial and orbital augmentation and reconstruction SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION SYNPOR Porous Polyethylene Implants 2 Indications and
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Prosthodonticstown. Immediate Implant Placement in Fresh Extraction Sites. clinical. Table I
 Prosthodonticstown clinical Immediate Implant Placement in Fresh Extraction Sites Charles A. Babbush, DDS, MScD Table I Benefits Of Immediate Implantation Improved prosthesis fabrication and/or design
Prosthodonticstown clinical Immediate Implant Placement in Fresh Extraction Sites Charles A. Babbush, DDS, MScD Table I Benefits Of Immediate Implantation Improved prosthesis fabrication and/or design
REASONS TO USE R.T.R.
 3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
BONE GRAFTING. Product Catalog
 BONE GRAFTING Product Catalog PRODUCT LINE Titanium Mesh Surgitime Titanium Titanium Foil Surgitime Titanium Seal Polytetraflouroethylene Membrane Surgitime PTFE Bone Screws Fixation Set We innovate to
BONE GRAFTING Product Catalog PRODUCT LINE Titanium Mesh Surgitime Titanium Titanium Foil Surgitime Titanium Seal Polytetraflouroethylene Membrane Surgitime PTFE Bone Screws Fixation Set We innovate to
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
B U I L D S T R O N G B O N E F A S T
 B U I L D S T R O N G B O N E F A S T Putty MIS Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
B U I L D S T R O N G B O N E F A S T Putty MIS Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
Fig Articular cartilage. Epiphysis. Red bone marrow Epiphyseal line. Marrow cavity. Yellow bone marrow. Periosteum. Nutrient foramen Diaphysis
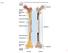 Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
low ProfIle neuro PlaTIng system
 low ProfIle neuro PlaTIng system surgical TeChnIque Table of Contents Introduction Low Profile Neuro Cranial Plating System 2 Surgical Technique Technique 5 Product Information Low Profile Neuro Plates
low ProfIle neuro PlaTIng system surgical TeChnIque Table of Contents Introduction Low Profile Neuro Cranial Plating System 2 Surgical Technique Technique 5 Product Information Low Profile Neuro Plates
PRP Usage in Today's Implantology
 Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC CHANGES
 Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
CMF. Maxillofacial portfolio
 CMF Maxillofacial portfolio Portfolio overview Through close collaboration with leading surgeons around the world, we have created a portfolio of innovative products to help you best serve your patients'
CMF Maxillofacial portfolio Portfolio overview Through close collaboration with leading surgeons around the world, we have created a portfolio of innovative products to help you best serve your patients'
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
REFERENCES for PLATELET RICH PLASMA (PRP)
 REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
easy-graft TM CRYSTAL
 1 easy-graft TM CRYSTAL Overview 2 Advantages easy-graft : principle & application Material & studies Indications easy-graft CRYSTAL & CLASSIC Advantages of easy-graft CRYSTAL 3 Easy handling: Injectable
1 easy-graft TM CRYSTAL Overview 2 Advantages easy-graft : principle & application Material & studies Indications easy-graft CRYSTAL & CLASSIC Advantages of easy-graft CRYSTAL 3 Easy handling: Injectable
Osteology. Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College
 Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Open and Endoscopic Forehead Lift. Plastic Surgery. For All Brow and Forehead Lift Procedures. Revolutionizing. Soft-Tissue Fixation
 Plastic Surgery Open and Endoscopic Forehead Lift For All Brow and Forehead Lift Procedures Revolutionizing Soft-Tissue Fixation DESIGNED FOR SIMPLICITY AND PREDICTABILITY The versatile design can be applied
Plastic Surgery Open and Endoscopic Forehead Lift For All Brow and Forehead Lift Procedures Revolutionizing Soft-Tissue Fixation DESIGNED FOR SIMPLICITY AND PREDICTABILITY The versatile design can be applied
Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla
 Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla Luciano Malchiodi, MD, DDS*/Antonio Scarano, DDS**/Manlio Quaranta, MD, DDS***/ Adriano
Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla Luciano Malchiodi, MD, DDS*/Antonio Scarano, DDS**/Manlio Quaranta, MD, DDS***/ Adriano
Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants
 Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
The body wants to heal
 58 A promising new particulate graft material: a case study The body wants to heal DR PETER J.M. FAIRBAIRN, DETROIT MERCY, MI, USA, AND LONDON, ENGLAND, AND DR MINAS LEVENTIS, ATHENS, GREECE The notion
58 A promising new particulate graft material: a case study The body wants to heal DR PETER J.M. FAIRBAIRN, DETROIT MERCY, MI, USA, AND LONDON, ENGLAND, AND DR MINAS LEVENTIS, ATHENS, GREECE The notion
Redefining Regeneration
 Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Inion OTPS TM. The Biodegradable Solution. lnion OTPS TM Plating Systems. Product description
 Inion OTPS TM 2 lnion OTPS TM Plating Systems The Biodegradable Solution Bio-advantage with Inion Technology Core Technology Inion s core technology is based on the biological and mechanical principles
Inion OTPS TM 2 lnion OTPS TM Plating Systems The Biodegradable Solution Bio-advantage with Inion Technology Core Technology Inion s core technology is based on the biological and mechanical principles
Focus on: IMPLANT TESTING ISO
 Focus on: IMPLANT TESTING ISO 10993-6 Implantation Assess the local pathological effects on living tissue, at both the gross level and microscopic level, Sample of a material or final product that is surgically
Focus on: IMPLANT TESTING ISO 10993-6 Implantation Assess the local pathological effects on living tissue, at both the gross level and microscopic level, Sample of a material or final product that is surgically
SURGICAL PROCEDURE DESCRIPTIONS
 SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
MEDPOR. Oral maxillofacial surgery
 MEDPOR Oral maxillofacial surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
MEDPOR Oral maxillofacial surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
Unitek Temporary Anchorage Device (TAD) System
 Planning and Placement Guide Treatment Planning Panoramic or P.A. X-ray - visualize root proximity Curved explorer tip - outline roots intraorally Bone sounding - measure tissue thickness using probe with
Planning and Placement Guide Treatment Planning Panoramic or P.A. X-ray - visualize root proximity Curved explorer tip - outline roots intraorally Bone sounding - measure tissue thickness using probe with
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 413 Schneiderian Membrane Perforation Rate During Sinus Elevation Using Piezosurgery: Clinical Results of 100 Consecutive Cases Stephen
The International Journal of Periodontics & Restorative Dentistry 413 Schneiderian Membrane Perforation Rate During Sinus Elevation Using Piezosurgery: Clinical Results of 100 Consecutive Cases Stephen
Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration.
 Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration. By Linero I., Chaparro O., 2014 Suzana Tufegdzic 1 Background 2 Background Stem Cells: undifferentiated
Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration. By Linero I., Chaparro O., 2014 Suzana Tufegdzic 1 Background 2 Background Stem Cells: undifferentiated
Property Latmedical, LLC.
 Dr. Goed provides a complete and innovate product portfolio solution to the growing healthcare need within the field of non-invasive orthopedics, sports medicine, bandaging, wound care and compression
Dr. Goed provides a complete and innovate product portfolio solution to the growing healthcare need within the field of non-invasive orthopedics, sports medicine, bandaging, wound care and compression
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Mandible fracture - Management. Dr Dinesh Kumar Verma OMFS SDCRI, SGNR
 Mandible fracture - Management Dr Dinesh Kumar Verma OMFS SDCRI, SGNR MANAGEMENT OPEN! CLOSE! DIRECT! INDIRECT! IMMEDIATE (PRIMARY) 1. ABC 2. Temporary stabilization 3. Tetanus prophylaxis 4. Antibiotics
Mandible fracture - Management Dr Dinesh Kumar Verma OMFS SDCRI, SGNR MANAGEMENT OPEN! CLOSE! DIRECT! INDIRECT! IMMEDIATE (PRIMARY) 1. ABC 2. Temporary stabilization 3. Tetanus prophylaxis 4. Antibiotics
Titanium Wire With Barb and Needle
 For Canthal Tendon Procedures Titanium Wire With Barb and Needle Surgical Technique Table of Contents Introduction Titanium Wire With Barb and Needle 2 Indications 2 Surgical Technique Preoperative Planning
For Canthal Tendon Procedures Titanium Wire With Barb and Needle Surgical Technique Table of Contents Introduction Titanium Wire With Barb and Needle 2 Indications 2 Surgical Technique Preoperative Planning
Compression Screw 3.2 Bioabsorbable. Product information
 Compression Screw 3.2 Bioabsorbable Product information Caution The current product description is not sufficient for the immediate application of instruments and implants. Instructional training by an
Compression Screw 3.2 Bioabsorbable Product information Caution The current product description is not sufficient for the immediate application of instruments and implants. Instructional training by an
New innovations in craniomaxillofacial fixation: the 2.0 lock system
 LECTURE New innovations in craniomaxillofacial fixation: the 2.0 lock system Brian Alpert, Rolf Gutwald1 and Rainer Schmelzeisen1 Departments of Oral & Maxillofacial Surgery and Surgical & Hospital Dentistry,
LECTURE New innovations in craniomaxillofacial fixation: the 2.0 lock system Brian Alpert, Rolf Gutwald1 and Rainer Schmelzeisen1 Departments of Oral & Maxillofacial Surgery and Surgical & Hospital Dentistry,
CHAPTER 6 LECTURE OUTLINE
 CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
