Lisa M. DiFrancesco, M.D., Mark A. Codner, M.D., and Clinton D. McCord, M.D.
|
|
|
- Alice Parrish
- 5 years ago
- Views:
Transcription
1 CME Upper Eyelid Reconstruction Lisa M. DiFrancesco, M.D., Mark A. Codner, M.D., and Clinton D. McCord, M.D. Atlanta, Ga. Learning Objectives: After studying this article, the participant should be able to: 1. Understand upper eyelid anatomy and function. 2. Analyze upper eyelid defects. 3. Understand an algorithm of upper eyelid reconstruction. 4. Have a basic understanding of techniques for upper eyelid reconstruction. There are several options available for upper eyelid reconstruction that depend on the extent of involvement of the anterior and posterior lamella. Knowledge of the anatomy will ensure that in addition to the creation of an aesthetically acceptable eyelid reconstruction, a functional upper lid will be restored. The purpose of this article is to outline the anatomy of the eyelid, to analyze the components of eyelid defects, and to provide options for lid reconstruction. (Plast. Reconstr. Surg. 114: 98e, 2004.) Any reconstructive procedure attempts to optimally restore form and function. Specifically, the eyelid is critical in protection of the eye and preservation of vision. To ensure an optimal outcome, it is necessary to understand the specialized anatomic structures and function of the orbit, eyelid, and globe. Once basic anatomy and function are understood, analysis of eyelid defects can be simplified when broken down into separate components. The workhorses of reconstruction, such as skin and muscle flaps, are described, as well as their techniques. Even the most complex eyelid problems can be addressed. This article will outline the various techniques available for eyelid reconstruction. ANATOMY Superficial skin anatomy includes the brow, upper eyelid, lower eyelid, and midface. The upper eyelid rests 2 mm below the superior limbus on forward gaze, whereas the lower eyelid is positioned at the inferior limbus. The supratarsal crease in the Occidental eyelid is generally 8 mm from the lid margin in men and 10 mm in women. The upper eyelid crease is formed by the dermal insertion of the levator aponeurosis to the orbital septum. In the Asian eyelid, this distance is only 2 to 3 mm from the lid margin as a result of fusion of the levator aponeurosis extensions with the orbital septum. The pretarsal space is the area superior to the eyelid margin where the skin is adherent to the tarsal plate. The orbital sulcus is defined by the space between the superior orbital rim and the upper eyelid crease. Loss of the orbital sulcus is seen with relaxation of the upper septum or herniation of the preaponeurotic orbital fat pads (Fig. 1). The eyelid is divided into two main layers. The anterior lamella consists of skin and muscle, and the posterior lamella is formed by the tarsal plate and conjunctiva. The medial and lateral canthi are important support structures in normal eyelid function and bony fixation. They represent the confluence of the orbicularis muscle, tarsal plate, eyelid retractors, orbital septum, and cheek ligaments. At the medial canthus this complex anatomic interplay provides the mechanism for the lacrimal pump. The lateral canthus inserts posterior on the lateral orbital rim, pulling the eyelid against the globe. The lateral canthus allows for bony stabilization of the eyelid during eyelid movement. Analysis of an acquired defect should include evaluation of the anterior lamella, posterior lamella, and medial and lateral canthi to facilitate reconstruction. The eyelid skin is the thinnest in the body, particularly on the medial aspect of the upper eyelid. At the eyelid margin the tarsal plates are From Paces Plastic Surgery. Received for publication January 15, 2003; revised April 24, DOI: /01.PRS e
2 Vol. 114, No. 7 / UPPER EYELID RECONSTRUCTION 99e FIG. 1. Anatomy of the preaponeurotic space demonstrating the structures encountered during eyelid reconstruction. tightly adherent to the skin. The tarsal plate is a fibrous structure that provides the skeletal support for the eyelid. In the upper eyelid, it measures 25 mm in length, is 1 mm thick, and has a maximal central height of 10 mm. The tarsal plate is centralized over the midpupillary line in childhood and migrates laterally with aging. Along with the conjunctiva, the tarsal plates form the posterior lamella. The orbicularis muscle is divided into pretarsal, preseptal, and orbital components. The pretarsal and preseptal orbicularis are each divided into a deep layer and a superficial layer, both medially and laterally. The medial canthal tendon is composed of superficial pretarsal and preseptal fibers. The deep pretarsal and preseptal fibers intersect posterior to the lacrimal sac and function as the lacrimal pump. The deep pretarsal and deep preseptal orbicularis insert on Whitnall s tubercle laterally within the orbital rim. Riolan s muscle represents a strip of pretarsal muscle and forms the gray line of the eyelid, which is important for alignment of full-thickness defects. 1 The orbital septum is posterior to the orbicularis muscle and forms the anterior barrier to the orbital contents. In the upper lid, the septum inserts on the levator aponeurosis approximately 10 mm above the eyelid margin just superior to the tarsal plate. The orbital septum attaches to the orbital rim at the arcus marginalis. The preaponeurotic fat pads (postseptal) are anterior extensions of orbital fat and are divided into nasal and medial compartments. The trochlea divides the nasal and medial fat pads. The lacrimal gland is located lateral to the fat pads. The eyelid retractor muscles include the levator palpebrae superioris and Müller s muscle, which are responsible for eyelid elevation. The levator palpebrae superioris originates along the lesser wing of the sphenoid and is innervated by cranial nerve III. The levator muscle extends anteriorly approximately 40 mm to Whitnall s ligament. Whitnall s ligament attaches superiorly to the levator muscle and changes the direction of levator muscle pull to a superior-inferior direction. The levator muscle extends inferiorly and transitions into a dense aponeurosis approximately 10 mm inferior to Whitnall s ligament. The levator aponeurosis inserts on the anterior surface of the tarsal plate. Müller s muscle is a smooth muscle that is innervated by the sympathetic nervous system. It originates at the level of Whitnall s ligament posterior to the levator aponeurosis and inserts on the superior tarsal plate. 2 The medial canthus represents a fixed-point fulcrum that is necessary for eyelid function. The medial canthus is a complex structure that consists of an anterior and posterior reflection of the medial canthal tendon that envelops the lacrimal sac. The tendons insert on the anterior and posterior lacrimal crest, respectively. The lateral canthal tendon is approximately 5 mm to 7 mm in length and provides dynamic support by connecting the tarsal plates to Whitnall s tubercle along the lateral orbital rim. The lateral canthus also consists of anterior
3 100e PLASTIC AND RECONSTRUCTIVE SURGERY, December 2004 and posterior fibrous attachments of the tarsal plate and fibers of the pretarsal orbicularis. 1 Eisler s fat pad can be found anterior to the lateral canthal tendon and is a useful anatomic landmark (Fig. 2). The arterial supply to the upper eyelid is primarily from branches of the ophthalmic artery that form two main arcades. The peripheral arcade is located between Müller s muscle and the levator aponeurosis on the upper border of the tarsus; the marginal arcade is in the pretarsal space 2 to 3 mm above the eyelid margin (Fig. 3). The superior palpebral vein courses parallel to the eyelid margin with an anastomosis between the angular vein and the supraorbital vein. The lymphatic drainage of the upper eyelid is to the preauricular nodes, whereas the lymphatic drainage of the lateral canthus is to the submandibular nodes. Evaluation of the appropriate lymphatic basin is important for treatment of cancers such as squamous cell carcinoma, melanoma, and sebaceous carcinoma. Sensory innervation of the upper eyelid is divided between the supratrochlear nerve medially and a combination of the supraorbital nerve and the lacrimal nerve laterally. The facial nerve cranial nerve VII supplies the motor innervation to the eyelid through the zygomatic and buccal branches. 2 Recent data collected by the authors, however, suggest that the buccal branches have a more significant contribution to motor function. RECONSTRUCTION Understanding the complex anatomy of the upper eyelid enables the surgeon to accurately analyze upper eyelid defects. The division of the eyelid into its component structures facilitates the approach to reconstruction. DIRECT REPAIR Benign lesions or biopsy defects often create small defects amenable to direct repair. This is possible with defects of up to 30 percent of the eyelid in younger patients and up to 40 percent of the eyelid in patients with eyelid skin laxity. Full-thickness incisions should be made perpendicular to the eyelid margin and extend to the superior tarsal margin to prevent notching (Figs. 4 and 5). Superior to the tarsal plate the incision is connected to a horizontal suture line hidden in the eyelid crease. Tension on the upper eyelid closure can result in mechanical ptosis; a lateral cantholysis may be performed to reduce closure under tension. It is critical that the eyelid margin, gray line, and lash line are approximated exactly to prevent eyelid inversion, which can cause corneal irritation. Next, the repair is completed in layers. The conjunctival sutures are placed with the knot buried away from the conjunctival surface. Finally, the anterior lamella is repaired. Any remaining excess tissue may be removed by two Burrow s triangles. Postoperative care consists of ophthalmic antibiotic ointment and suture removal at 7 days. 3 SKIN GRAFT A full-thickness graft can adequately reconstruct small superficial anterior lamellar defects. The skin graft may also be used as a vertically shortened eyelid with a split level with FIG. 2. Cross-section anatomy of the eyelid and orbit demonstrating the posterior insertion of the medial and lateral canthus.
4 Vol. 114, No. 7 / UPPER EYELID RECONSTRUCTION 101e FIG. 3. Arterial supply to the upper lid. a posterior lamellar graft. 2 Upper eyelid skin is the best donor site because of the match in color and thickness. Excess skin from the contralateral upper lid can be used but may only be available in limited quantities. Alternative harvest sites for skin include the supraclavicular skin, preauricular skin, and the lateral cervical skin. An elliptical incision is made in the eyelid, and using iris scissors, the skin is separated from the muscle. The donor site is closed primarily. The skin graft is inset and a bolster dressing is placed. The medial eyelid skin is avoided as a donor site to prevent lagophthalmos. There are limited indications for a splitthickness skin graft; an example would be burns or other eyelid trauma involving extensive loss of upper and lower eyelid skin. When designing a split-thickness skin graft, 50 to 70 percent overcorrection should be incorporated to allow for secondary contraction. In the upper lid, separate grafts are placed in the pretarsal area and the orbital sulcus, with the suture line hidden in the eyelid crease. 1 POSTERIOR LAMELLA Sliding Tarsoconjunctival Flap The sliding tarsoconjunctival flap (tarsal extension flap) is a transposition flap based on small adjacent conjunctival defects involving the medial or lateral upper eyelid. 3 The upper lid is everted over a Desmarres retractor. An incision is made in the adjacent conjunctiva 4 mm superior to the eyelid margin to avoid potential margin eversion. The incision is extended parallel to the lid margin with the flap length in a 1:1 ratio with the defect. Finally, the incision is carried superiorly to the edge of the tarsal plate. The blood supply is from the superior peripheral arcade, which is included in the base of the flap. Westcott scissors are used to dissect the tarsal flap from the levator aponeurosis and Müller s muscle of the remaining eyelid, and the flap is transposed into position (Fig. 6). Suture fixation secures the flap to the periosteum of the orbital rim. The tarsal plate is aligned with 6-0 silk. The conjunctiva is repaired with 6-0 plain catgut inverted sutures. The remaining anterior lamellar defect is repaired with a skin/muscle flap or a full-thickness skin graft. The transposition graft provides a highly vascularized bed for the skin graft. The eye is sutured closed and a bolster dressing is left in place for 1 week postoperatively. Free Tarsoconjunctival Flap If the ipsilateral eyelid skin is not available for reconstruction, then the contralateral upper eyelid can be used as a free tarsoconjunctival flap. An incision is made 4 mm from the lid margin to preserve the integrity of the eyelid with length equal to the defect length. Parallel vertical incisions are made and extended to the superior margin of the tarsal plate. The
5 102e PLASTIC AND RECONSTRUCTIVE SURGERY, December 2004 FIG. 4. Upper lid marginal tumors require full-thickness skin parallel excision of the lid and tarsal plate to avoid postoperative notching. FIG. 5.(Left) Outline of upper lid resection. (Right) Parallel full-thickness excision through tarsal plate. flap is dissected free from the levator aponeurosis and Müller s muscle, and the donor site is left to reepithelialize. The free graft is inset with 6-0 plain catgut sutures. 2 Other Autologous Options Oral mucosal grafts from the upper lip, lower lip, or buccal mucosa may be used as a conjunctival lining. Although oral mucosa does
6 Vol. 114, No. 7 / UPPER EYELID RECONSTRUCTION FIG. 6. Sliding tarsoconjunctival flap. The upper border of the tarsal plate is used to reconstruct posterior lamellar defects based on the lateral superior arcade. not have sufficient integrity for tarsal replacement, the smooth, nonkeratinizied epithelium is important to avoid irritation to the cornea during blinking after reconstruction of central upper eyelid defects. Ear cartilage should not be exposed directly to the cornea because of the risk of abrasion and irritation. ANTERIOR LAMELLA Semicircular Rotation Flap Tenzel and Stewart described the semicircular rotation flap for defects of 40 to 60 percent 103e of the eyelid. 4,5 The tarsal edges of the defect must be parallel for reconstruction. The flap is designed as a superiorly based musculocutaneous flap starting at the lateral canthus and extending in a semicircle with a diameter of at least 3 cm (Fig. 7). The plane of dissection is deep to the orbicularis muscle. Once the flap is dissected, a selective lateral canthotomy is performed on the upper lateral canthal tendon, preserving the anterior tendon. The flap is advanced into the defect and the tarsal plate is reapproximated first with 7-0 silk. The lateral canthus is reconstructed with a lateral canthoplasty, with the skin/muscle flap sutured to the periosteum at the point the flap overlaps the orbital rim with 4-0 Prolene. The anterior and posterior components of the lateral canthus require reconstruction by suturing the tarsal plate to the inner aspect of the orbital rim and the skin/muscle flap to the anterior aspect of the orbital rim. The conjunctiva is closed with inverted 6-0 plain catgut sutures, and the skin/ muscle flap is closed with 6-0 nylon. The donor site is closed, and removal of a Burrow s triangle may be necessary for a residual dog-ear. The Tenzel flap lateralizes the defect to create a continuous eyelash line for eye protection. Bridge Flap The Cutler-Beard 6 or bridge flap 7 is a fullthickness lower lid bridge flap designed for broad, shallow upper eyelid defects, including FIG. 7. The semicircular rotation or Tenzel flap is used for defects of 40 to 60 percent of the upper eyelid. Lateral canthotomy is required to rotate the flap and lateral remaining lid margin.
7 104e PLASTIC AND RECONSTRUCTIVE SURGERY, December 2004 total eyelid reconstruction (Fig. 8). An incision is made 5 mm inferior to the lower eyelid margin to preserve lid margin vascularity. The width of the flap corresponds to the eyelid defect. Vertical incisions are made inferiorly to the fornix and the inferior orbital rim for the skin/muscle flap. The flap is maximally mobilized for superior placement. Relaxing incisions in the capsulopalpebral fascia are made to allow passage of the flap under the eyelid margin bridge to the upper eyelid. The conjunctival layer is sutured with inverted 6-0 plain catgut sutures. Because the flap lacks tarsal support, the ear cartilage graft is harvested from the flat scaphoid donor site rather then the conchal cartilage. The cartilage is placed anterior to the conjunctiva to avoid corneal irritation and sutured with 7-0 silk along the lateral and medial borders (Figs. 9 and 10). The superior edge of the cartilage graft is sutured to the levator aponeurosis to maintain lid function. Finally, the skin/muscle flap is sutured with 7-0 silk to the cutaneous border of the defect. Division of the flap traditionally occurs at 6 weeks. The flap is transected 2 mm below the optimal position for the upper eyelid. A 1- to 2-mm section of skin and muscle is resected, leaving a conjunctival border that is rotated anteriorly and secured to the skin. This prevents corneal irritation from exposure to the keratinized skin. The donor site is repaired by insetting the residual skin bridge with deepithelialization. The edges are reapproximated and the conjunctival surface is allowed to reepithelialize. Lateral canthoplasty of the lower lid is required to avoid lower lid malposition or ectropion at the donor site. PEDICLED LOWER LID SHARING Originally described by Mustardé, 8 broad, shallow, full-thickness defects of the upper lid margin may be addressed with a pedicled flap from the lower eyelid (Fig. 11). The flap is based in the central portion of the lower lid and is the only flap that allows for primary lower lid closure. A full-thickness, 5-mm vertical incision is then made at the lateral limbus. Because a selective lateral canthotomy of the inferior tendon is made, the blood supply is preserved from the medial inferior marginal arcade. The inferior incision is then made parallel to the lid margin below the marginal artery until adequate mobilization is achieved to reach the upper lid defect. The flap is rotated FIG. 8. The bridge flap or Cutler-Beard flap is used for total upper lid reconstruction. The flap is a biplanar flap passed under the lower lid margin.
8 Vol. 114, No. 7 / UPPER EYELID RECONSTRUCTION 105e FIG. 9.Left, total upper eyelid defect following resection of squamous cell cancer. Right, outline of Cutler-Beard flap inferior to lower lid marginal blood supply. FIG. 10. Left, ear cartilage is used in the biplanar flap for tarsal plate replacement. Right, final result after division of flap. FIG. 11. Lid sharing or Mustardé lid flap utilizes a two-stage transposition of the lower lid margin, including lashes. superiorly and the lateral lower lid tarsal plate is sutured to the medial upper eyelid tarsal plate. Care must be taken to align the grey line and the lash line. Traditional flap division occurs in 6 weeks, although earlier flap division can be performed successfully. An angled incision is made and the remainder of the flap is rotated into the upper eyelid defect. The lateral margin of the defect gray line and lash line is aligned with the flap. The donor site is repaired by allowing lateral advancement of the lower lid margin and reapproximation of the lid margin. If there is concern for excess tension or lower lid malposition, a lateral canthotomy and canthoplasty should be performed.
9 106e PLASTIC AND RECONSTRUCTIVE SURGERY, December 2004 Periorbital Donor Sites The periorbital donor sites are an option for large-volume tissue loss or when adequate eyelid tissue is not available. The surrounding periorbital skin, however, is of a different quality and thickness. Temporal Forehead Flap The temporal forehead flap was first described by Fricke 9 (Fig. 12). The temporal forehead is used as a transposition flap for fullthickness eyelid defects. The scar can be hidden in the brow margin. This is a skin/ muscle flap, and conjunctival reconstruction might be necessary in conjunction with this flap. Forehead Flap The forehead flap first described by Kazanjian and Roopenian 10 can also be used for large defects in upper eyelid reconstruction. The blood supply is based on the supratrochlear or supraorbital artery and the flap is elevated in the subgaleal plane (Fig. 13). Generally, 2 weeks are required before division of the flap. The forehead flap is generally a last resort, as it requires a two-stage procedure and is a very thick flap when used for lid reconstruction. Glabellar Flap Medial canthal defects can be reconstructed from redundant glabellar tissue. 1 An inverted V-shaped incision is made and the skin flap is rotated into the defect. The donor site is closed primarily. The broad base of this flap allows it to be safely thinned to contour the defect. Quilting sutures must be used to help the flap conform to the local tissue architecture at the defect site. The glabellar flap generally requires a second procedure to thin and inset the flap. COMPLICATIONS As with any surgical procedure, the best way to handle a complication is with prevention. During surgery appropriate lubrication and corneal protectors should be used to avoid corneal irritation. The patient should be closely followed postoperatively to avoid the adverse sequelae of early complications. Complaints of dry eyes are evaluated with fluorescein and a slit-lamp examination. If a corneal abrasion occurs, liberal use of lubrication and temporary closure of the eye with an eye pad will alleviate the discomfort and prevent further injury. Hematoma is another early complication that requires prompt diagnosis and evacuation. Chemosis or postoperative swelling can be deterred with a Frost stitch or temporary tarsorrhaphy. Skin graft failure is avoided with the use of a bolster dressing and temporary tarsorrhaphy. The bolster dressing will also help to prevent skin graft contracture. If skin graft or flap failure should occur, the wound is débrided and treated with ointment to prevent desiccation. Late postoperative complications are often the result of anatomic problems that subsequently create functional problems with the new eyelid. It is best to wait 3 months before surgical revision, but it is often necessary to treat them earlier. Lid notching, lid malposition, flap failure, and lagophthalmos require surgical correction. Lid notching is best corrected with direct excision. Malposition, fail- FIG. 12. Temporal forehead flap or Fricke flap is a transposition flap from above the eyebrow used for total upper lid reconstruction.
10 Vol. 114, No. 7 / UPPER EYELID RECONSTRUCTION 107e FIG. 13. A forehead flap can be used for total upper lid reconstruction combined with a mucosal graft for lining against the cornea. ure, or lagophthalmos requires additional tissue recruitment for correction. In addition, corneal irritation from trichiasis seen with opposite lid flaps can be eliminated with excision or cryotherapy. CONCLUSIONS Upper eyelid reconstruction can be challenging to a surgeon, given the specialized anatomy and function of the eyelid. Successful aesthetic and functional reconstruction begins with analysis of a complex defect and division into its separate components. Next, an algorithmic approach is used to determine the optimal reconstruction. Finally, meticulous surgical technique and avoidance of complications will result in an optimal reconstruction. Mark A. Codner, M.D Downwood Circle, Suite 640 Atlanta, Ga macodner@aol.com REFERENCES 1. Codner, M. A. Reconstruction of the eyelids and orbit. In B. Achauer (Ed.), Plastic Surgery: Indications, Operations, and Outcomes, Vol. 3. St. Louis: Mosby, Pp McCord, C. D. Eyelid Surgery. Philadelphia: Lippincott- Raven, Pp McCord, C. D., and Wesley, R. Reconstruction of upper eyelid and medial canthus. In C. D. McCord and M. Tannenbaum (Eds.), Oculoplastic Surgery. New York: Raven, Pp Tenzel, R. R. Reconstruction of the central one half of an eyelid. Arch. Ophthalmol. 93: 125, Tenzel, R. R., and Stewart, W. B. Eyelid reconstruction by semi-circular flap technique. Trans. Am. Soc. Ophthalmol. Otolaryngol. 85: 1164, Culter, N., and Beard, C. A method for partial and total upper lid reconstruction. Am. J. Ophthalmol. 39: 1, Smith, B., and Obear, M. F. Bridge flap technique for reconstruction of large upper lid defects. Plast. Reconstr. Surg. 38: 45, Mustardé, J. C. Eyelid reconstruction. Orbit 1: 33, Fricke, J. C. G. Die Bildung neuer Augenlider (Blepharoplastik) nach Zerstorungen und dadurch hervorgebrachten Auswartswendungen derselben. Hamburg: Perthes and Bessler, Kazanjian, V. H., and Roopenian, A. Median forehead flaps in the repair of defects of the nose and surrounding areas. Trans. Am. Acad. Ophthalmol. Otolaryngol. 60: 557, 1956.
Chapter(2):the lid page (1) THE LID
 Chapter(2):the lid page (1) THE LID Anatomy of the lid: * Check movie anatomy of the lid model The eyelids are two movable muco-cutaneous folds which protect the eye on closure. The are joined temporary
Chapter(2):the lid page (1) THE LID Anatomy of the lid: * Check movie anatomy of the lid model The eyelids are two movable muco-cutaneous folds which protect the eye on closure. The are joined temporary
Entropion. Geoffrey J. Gladstone. Examination. Congenital Entropion-Epiblepharon. Etiology
 Entropion 2 Geoffrey J. Gladstone Entropion, or inward rotation of the eyelid margin, is an eyelid malposition commonly seen by general ophthalmologists and oculoplastic surgeons. The severe corneal irritation
Entropion 2 Geoffrey J. Gladstone Entropion, or inward rotation of the eyelid margin, is an eyelid malposition commonly seen by general ophthalmologists and oculoplastic surgeons. The severe corneal irritation
Eyelid Reconstruction December 2002
 TITLE: Eyelid Reconstruction SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: December 18, 2002 RESIDENT PHYSICIAN: Michael Underbrink, M.D. FACULTY ADVISOR: Karen Calhoun, M.D. SERIES
TITLE: Eyelid Reconstruction SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: December 18, 2002 RESIDENT PHYSICIAN: Michael Underbrink, M.D. FACULTY ADVISOR: Karen Calhoun, M.D. SERIES
with laser resurfacing, 36, 37 Cryotherapy, lower eyelid cicatricial ectropion after, 151 Cutler-Beard flap. See Fullthickness
 INDEX A Abrasion, from silicone tubing, 230 Acquired immunodeficiency syndrome, eyelid tumor with, 193 AIDS. See Acquired immunodeficiency syndrome Anatomy, eyelid, 155 156 Aneurysm, cerebral, Muller s
INDEX A Abrasion, from silicone tubing, 230 Acquired immunodeficiency syndrome, eyelid tumor with, 193 AIDS. See Acquired immunodeficiency syndrome Anatomy, eyelid, 155 156 Aneurysm, cerebral, Muller s
A ptosis repair of aponeurotic defects by the posterior approach
 British Journal of Ophthalmology, 1979, 63, 586-590 A ptosis repair of aponeurotic defects by the posterior approach J. R. 0. COLLIN From the Department of Clinical Ophthalmology, Moorfields Eye Hospital,
British Journal of Ophthalmology, 1979, 63, 586-590 A ptosis repair of aponeurotic defects by the posterior approach J. R. 0. COLLIN From the Department of Clinical Ophthalmology, Moorfields Eye Hospital,
INSERTION* SURGICAL ANATOMY OF THE LEVATOR PALPEBRAE. impossible to dissect and separate these layers. That the levator aponeurosis
 Brit. J. Ophthal. (1962) 46, 503. SURGICAL ANATOMY OF THE LEVATOR PALPEBRAE INSERTION* BY EDWARD EPSTEIN Johannesburg, Union of South Africa THE text-book description of the anatomy of the upper eyelid
Brit. J. Ophthal. (1962) 46, 503. SURGICAL ANATOMY OF THE LEVATOR PALPEBRAE INSERTION* BY EDWARD EPSTEIN Johannesburg, Union of South Africa THE text-book description of the anatomy of the upper eyelid
Management of Lid Lacerations
 Ocular Ocular Trauma Management of Lid Lacerations Nitin Vichare MS, DNB, FAICO Nitin Vichare MS, DNB,FAICO Dept. of Ophthalmology, Command Hospital, (Southern Command), Pune, Maharashtra Eyelids are not
Ocular Ocular Trauma Management of Lid Lacerations Nitin Vichare MS, DNB, FAICO Nitin Vichare MS, DNB,FAICO Dept. of Ophthalmology, Command Hospital, (Southern Command), Pune, Maharashtra Eyelids are not
Repair of Involutional Ectropion and Entropion: Transconjunctival Surgery of the Lower Lid Retractors
 Chapter Repair of Involutional Ectropion and Entropion: Transconjunctival Surgery of the Lower Lid Retractors Markus J. Pfeiffer Core Messages Vertical deviation of the orbicularis muscle plays the most
Chapter Repair of Involutional Ectropion and Entropion: Transconjunctival Surgery of the Lower Lid Retractors Markus J. Pfeiffer Core Messages Vertical deviation of the orbicularis muscle plays the most
cally, a distinct superior crease of the forehead marks this spot. The hairline and
 4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
Mc Gregor Flap for Lower Eyelid Defect
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. V (April. 2017), PP 69-74 www.iosrjournals.org Mc Gregor Flap for Lower Eyelid Defect
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. V (April. 2017), PP 69-74 www.iosrjournals.org Mc Gregor Flap for Lower Eyelid Defect
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Lower Eyelid Malposition
 Oculoplastic Surgeon s DDX for the Red Eye Geeta Belsare Been,MD The Center for Facial Plastic Surgery Barrington, IL Lower Eyelid Malposition Ectropion Involutional Cicatricial Paralytic Entropion Involutional
Oculoplastic Surgeon s DDX for the Red Eye Geeta Belsare Been,MD The Center for Facial Plastic Surgery Barrington, IL Lower Eyelid Malposition Ectropion Involutional Cicatricial Paralytic Entropion Involutional
1 Eyelids. Lacrimal Apparatus. Orbital Region. 3 The Orbit. The Eye
 1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
Principles of Facial Reconstruction After Mohs Surgery
 Objectives Principles of Facial Reconstruction After Mohs Surgery Identify important functional anatomy and aesthetic units of the face. Describe techniques used in facial reconstruction. Discuss postoperative
Objectives Principles of Facial Reconstruction After Mohs Surgery Identify important functional anatomy and aesthetic units of the face. Describe techniques used in facial reconstruction. Discuss postoperative
Face. Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face
 Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
The sebaceous glands (glands of Zeis) open directly into the eyelash follicles, ciliary glands (glands of Moll) are modified sweat glands that open
 The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
A Cadaveric Anatomical Study of the Levator Aponeurosis and Whitnall s Ligament
 접수번호 : 2008-087 Korean Journal of Ophthalmology 2009;23:183-187 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.183 A Cadaveric Anatomical Study of the Levator Aponeurosis and Whitnall s Ligament Han Woong
접수번호 : 2008-087 Korean Journal of Ophthalmology 2009;23:183-187 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.183 A Cadaveric Anatomical Study of the Levator Aponeurosis and Whitnall s Ligament Han Woong
Subciliary versus Subtarsal Approaches to Orbitozygomatic Fractures
 CME Subciliary versus Subtarsal Approaches to Orbitozygomatic Fractures Rod J. Rohrich, M.D., Jeffrey E. Janis, M.D., and William P. Adams, Jr., M.D. Dallas, Texas Learning Objectives: After studying this
CME Subciliary versus Subtarsal Approaches to Orbitozygomatic Fractures Rod J. Rohrich, M.D., Jeffrey E. Janis, M.D., and William P. Adams, Jr., M.D. Dallas, Texas Learning Objectives: After studying this
THE MANAGEMENT OF INVOLUTIONAL LOWER LID ECTROPION
 THE MANAGEMENT OF INVOLUTIONAL LOWER LID ECTROPION BYRON C. SMITH, M.D., STEPHEN L. BOSNIAK, M.D., MICHAEL E. SACHS, M.D. New York Eye & Ear Infirmary, Manhattan Eye, Ear & Throat Hospital, New York ABSTRACT
THE MANAGEMENT OF INVOLUTIONAL LOWER LID ECTROPION BYRON C. SMITH, M.D., STEPHEN L. BOSNIAK, M.D., MICHAEL E. SACHS, M.D. New York Eye & Ear Infirmary, Manhattan Eye, Ear & Throat Hospital, New York ABSTRACT
CHAPTER 17 FACIAL AESTHETIC SURGERY. Christopher C. Surek, DO and Mohammed S. Alghoul, MD. I. BROW LIFT (Figures 1 and 2)
 CHAPTER 17 FACIAL AESTHETIC SURGERY Christopher C. Surek, DO and Mohammed S. Alghoul, MD I. BROW LIFT (Figures 1 and 2) A. Open Coronal Brow Lift Technique 1. Coronal incision is made in the hair-bearing
CHAPTER 17 FACIAL AESTHETIC SURGERY Christopher C. Surek, DO and Mohammed S. Alghoul, MD I. BROW LIFT (Figures 1 and 2) A. Open Coronal Brow Lift Technique 1. Coronal incision is made in the hair-bearing
Case Report Reconstruction of Total Lower Eyelid Defects with the Temporoparietal Fascial Flap
 Volume 2012, Article ID 927260, 4 pages doi:10.1155/2012/927260 Case Report Reconstruction of Total Lower Eyelid Defects with the Temporoparietal Fascial Flap Simon R. Bababeygy, 1 Anne R. Kao, 1 Niels
Volume 2012, Article ID 927260, 4 pages doi:10.1155/2012/927260 Case Report Reconstruction of Total Lower Eyelid Defects with the Temporoparietal Fascial Flap Simon R. Bababeygy, 1 Anne R. Kao, 1 Niels
C13. Basic Principles of Eyelid Surgery. 11 June :00 11:30hrs. Room 116 HAND-OUTS
 C13 Basic Principles of Eyelid Surgery 11 June 2017 10:00 11:30hrs Room 116 HAND-OUTS SOE 2017 Barcelona ESOPRS Course Basic principles of eyelid surgery Sunday, 11.06.2017, 10.00 11.30 Set up, materials,
C13 Basic Principles of Eyelid Surgery 11 June 2017 10:00 11:30hrs Room 116 HAND-OUTS SOE 2017 Barcelona ESOPRS Course Basic principles of eyelid surgery Sunday, 11.06.2017, 10.00 11.30 Set up, materials,
PERIORBITAL ANATOMY - AN ESSENTIAL FOUNDATION FOR BLEPHAROPLASTY
 PERIORBITAL ANATOMY - AN ESSENTIAL FOUNDATION FOR BLEPHAROPLASTY William M. Ramsdell, M.D. 102 Westlake Dr, Ste 100 Austin, TX 78746 wmr@centexderm.com 512-327-7779 Private Practice ABSTRACT Background
PERIORBITAL ANATOMY - AN ESSENTIAL FOUNDATION FOR BLEPHAROPLASTY William M. Ramsdell, M.D. 102 Westlake Dr, Ste 100 Austin, TX 78746 wmr@centexderm.com 512-327-7779 Private Practice ABSTRACT Background
MULLERS MUSCLE-CONJUNCTIVAL RESECTION PTOSIS PROCEDURE
 Australian and New Zealand Journal of Ouhthalmology 1985; 13: 179-183 MULLERS MUSCLE-CONJUNCTIVAL RESECTION PTOSIS PROCEDURE ALLEN M. PUTTERMAN MD University Of lll~nois Eye and Ear Infirmary, Michael
Australian and New Zealand Journal of Ouhthalmology 1985; 13: 179-183 MULLERS MUSCLE-CONJUNCTIVAL RESECTION PTOSIS PROCEDURE ALLEN M. PUTTERMAN MD University Of lll~nois Eye and Ear Infirmary, Michael
Reconstruction of seventeen full-thickness defects of the eyelids with twenty-two Hübner tarsomarginal grafts *
 British Journal of Plastic Surgery (2005) 58, 361 365 Reconstruction of seventeen full-thickness defects of the eyelids with twenty-two Hübner tarsomarginal grafts * G. Dagregorio a, *, V. Huguier b, V.
British Journal of Plastic Surgery (2005) 58, 361 365 Reconstruction of seventeen full-thickness defects of the eyelids with twenty-two Hübner tarsomarginal grafts * G. Dagregorio a, *, V. Huguier b, V.
EYELID RECONSTRUCTION
 EYELID RECONSTRUCTION James F Thornton MD and Jeffrey M Kenkel MD ANATOMY AND PHYSIOLOGY Surgery of the eyelids requires a thorough knowledge of the periorbital anatomy. The complexity of the eyelids as
EYELID RECONSTRUCTION James F Thornton MD and Jeffrey M Kenkel MD ANATOMY AND PHYSIOLOGY Surgery of the eyelids requires a thorough knowledge of the periorbital anatomy. The complexity of the eyelids as
International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR)
 International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR) The International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubrics
International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR) The International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubrics
Eyelid Reconstruction An Oculoplastic Surgical Coding Minicourse. Riva Lee Asbell Philadelphia, PA. Part II
 INTRODUCTION Eyelid Reconstruction An Oculoplastic Surgical Coding Minicourse Riva Lee Asbell Philadelphia, PA Part II In this second part of the Minicourse on Surgical Coding for Eyelid Reconstruction
INTRODUCTION Eyelid Reconstruction An Oculoplastic Surgical Coding Minicourse Riva Lee Asbell Philadelphia, PA Part II In this second part of the Minicourse on Surgical Coding for Eyelid Reconstruction
An anatomical structure which results in puffiness of the upper eyelid and a narrow palpehral fissure in the Mongoloid eye
 British Journal of Plastic Surgery (2000), 53, 466-472 9 2000 The British Association of Plastic Surgeons DOI: 10.1054/bjps.2000.3387 BRITISH JOURNAL OF ~ PLASTIC SURGERY An anatomical structure which
British Journal of Plastic Surgery (2000), 53, 466-472 9 2000 The British Association of Plastic Surgeons DOI: 10.1054/bjps.2000.3387 BRITISH JOURNAL OF ~ PLASTIC SURGERY An anatomical structure which
ORIGINAL ARTICLE. The Precaruncular Approach to the Medial Orbit
 The Precaruncular Approach to the Medial Orbit Kris. S. Moe, MD ORIGINAL ARTICLE Background: Most approaches to the medial orbit and lower provide suboptimal access and leave visible scars. The transcaruncular
The Precaruncular Approach to the Medial Orbit Kris. S. Moe, MD ORIGINAL ARTICLE Background: Most approaches to the medial orbit and lower provide suboptimal access and leave visible scars. The transcaruncular
THIEME. Scalp and Superficial Temporal Region
 CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR)
 International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR) The International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubrics
International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR) The International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubrics
Head and Face Anatomy
 Head and Face Anatomy Epicranial region The Scalp The soft tissue that covers the vault of skull. Extends from supraorbital margin to superior nuchal line. Layers of the scalp S C A L P = skin = connective
Head and Face Anatomy Epicranial region The Scalp The soft tissue that covers the vault of skull. Extends from supraorbital margin to superior nuchal line. Layers of the scalp S C A L P = skin = connective
Usefulness of the orbicularis oculi myocutaneous flap in periorbital reconstruction
 Archives of Craniofacial Surgery Arch Craniofac Surg Vol.19 No.4, 254-259 Usefulness of the orbicularis oculi myocutaneous flap in periorbital reconstruction Original Article Geon Woo Kim 1, Yong Chan
Archives of Craniofacial Surgery Arch Craniofac Surg Vol.19 No.4, 254-259 Usefulness of the orbicularis oculi myocutaneous flap in periorbital reconstruction Original Article Geon Woo Kim 1, Yong Chan
3. The Jaw and Related Structures
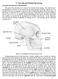 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Prevention of Lower Eyelid Ectropion Using Noninsional Suspension Sutures after Blepharoplasty
 IDE ND INNOVTION http://dx.doi.org/10.14730/.2014.20.3.173 rch esthetic Plast Surg 2014;20(3):173-177 pissn: 2234-0831 eissn: 2288-9337 Prevention Lower Eyelid Ectropion Using Noninsional Suspension Sutures
IDE ND INNOVTION http://dx.doi.org/10.14730/.2014.20.3.173 rch esthetic Plast Surg 2014;20(3):173-177 pissn: 2234-0831 eissn: 2288-9337 Prevention Lower Eyelid Ectropion Using Noninsional Suspension Sutures
Repair of Eyelid Trauma
 Repair of Eyelid Trauma Yunia Irawati, MD Plastic Reconstruction Division, Department of Ophthalmology FKUI / RSCM Introduction Eyelid trauma defined as a trauma to external surface of the lids with or
Repair of Eyelid Trauma Yunia Irawati, MD Plastic Reconstruction Division, Department of Ophthalmology FKUI / RSCM Introduction Eyelid trauma defined as a trauma to external surface of the lids with or
Surgical treatment of bilateral paralytic lagophthalmos using scapha graft in a case of lepromatous leprosy
 Lepr Rev (2009) 80, 448 452 CASE REPORT Surgical treatment of bilateral paralytic lagophthalmos using scapha graft in a case of lepromatous leprosy LAURA LAVILLA, JESÚS CASTILLO, ÁNGEL M. DOMÍNGUEZ, NELSON
Lepr Rev (2009) 80, 448 452 CASE REPORT Surgical treatment of bilateral paralytic lagophthalmos using scapha graft in a case of lepromatous leprosy LAURA LAVILLA, JESÚS CASTILLO, ÁNGEL M. DOMÍNGUEZ, NELSON
Evaluation and Management of Ectropion
 Oculoplasty Evaluation and Management of Ectropion Ruchi Goel MS, DNB, FICS, Apoorva AG MBBS, Smriti Nagpal MBBS, Sushil Kumar MD Oculoplasty Services, Gurunanak Eye Centre, Maulana Azad Medical College,
Oculoplasty Evaluation and Management of Ectropion Ruchi Goel MS, DNB, FICS, Apoorva AG MBBS, Smriti Nagpal MBBS, Sushil Kumar MD Oculoplasty Services, Gurunanak Eye Centre, Maulana Azad Medical College,
Kevin T. Kavanagh, MD
 Kevin T. Kavanagh, MD Axial Based upon a named artery. Survival length depends upon the artery not the width of the flap. Random Has random unnamed vessels supplying it. Survival length is directly proportional
Kevin T. Kavanagh, MD Axial Based upon a named artery. Survival length depends upon the artery not the width of the flap. Random Has random unnamed vessels supplying it. Survival length is directly proportional
The orbit-2. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-2 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Eyelids The eyelids (act like the curtains) protect the eye from injury and excessive light by their closure The upper eyelid
The orbit-2 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Eyelids The eyelids (act like the curtains) protect the eye from injury and excessive light by their closure The upper eyelid
3-Deep fascia: is absent (except over the parotid gland & buccopharngeal fascia covering the buccinator muscle)
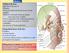 The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
Surgical repair of paralytic lagophthalmos by medial tarsal suspension of the lower lid
 708 Department of Ophthalmology, Conxo Hospital, Santiago de Compostela, Spain M Castroviejo-Bolibar Eye Bank of the Red Cross of Vizcaya, Spain A de Damborenea Ophthalmological Clinic, Oviedo, Spain A
708 Department of Ophthalmology, Conxo Hospital, Santiago de Compostela, Spain M Castroviejo-Bolibar Eye Bank of the Red Cross of Vizcaya, Spain A de Damborenea Ophthalmological Clinic, Oviedo, Spain A
Tikrit University College of Dentistry Dr.Ban I.S. head & neck anatomy 2 nd y.
 Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Surgical Treatment of Short Nose
 Surgical Treatment of Short Nose Dr. Otto YT Au MD (JEFFERSON, USA) 1957, MCPS (MANITOBA) 1963, FHKAM (SURGERY) 1995 Diplomate American Board Plastic Surgery Plastic Surgery Specialist Dr.OttoYTAu A nice
Surgical Treatment of Short Nose Dr. Otto YT Au MD (JEFFERSON, USA) 1957, MCPS (MANITOBA) 1963, FHKAM (SURGERY) 1995 Diplomate American Board Plastic Surgery Plastic Surgery Specialist Dr.OttoYTAu A nice
Senior Consultant, Plastic Surgery, Apollo Hospitals, Chennai; Prof. Emeritus Oculoplastic Surgery; Sankara Nethralaya.
 Free full text on www.ijps.org Blepharoplasty Nirmala Subramanian Senior Consultant, Plastic Surgery, Apollo Hospitals, Chennai; Prof. Emeritus Oculoplastic Surgery; Sankara Nethralaya. Chennai, India
Free full text on www.ijps.org Blepharoplasty Nirmala Subramanian Senior Consultant, Plastic Surgery, Apollo Hospitals, Chennai; Prof. Emeritus Oculoplastic Surgery; Sankara Nethralaya. Chennai, India
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
Ocular Anatomy for the Paraoptometric
 Ocular Anatomy for the Paraoptometric Minnesota Optometric Association Paraoptometric CE Friday September 30, 2016 Lindsay A. Sicks, OD, FAAO Assistant Professor, Illinois College of Optometry lsicks@ico.edu
Ocular Anatomy for the Paraoptometric Minnesota Optometric Association Paraoptometric CE Friday September 30, 2016 Lindsay A. Sicks, OD, FAAO Assistant Professor, Illinois College of Optometry lsicks@ico.edu
MAXILLA, ORBIT & PTERYGOPALATINE FOSSA. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 MAXILLA, ORBIT & PTERYGOPALATINE FOSSA Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine Maxilla MAXILLA Superior, middle, and inferior meatus Frontal
MAXILLA, ORBIT & PTERYGOPALATINE FOSSA Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine Maxilla MAXILLA Superior, middle, and inferior meatus Frontal
A CLINICAL STUDY ECTROPION AND ENTROPION
 A CLINICAL STUDY OF ECTROPION AND ENTROPION Regional Institute of Ophthalmology & Government Ophthalmic Hospital Madras Medical College Chennai Dissertation Submitted to THE TAMILNADU DR. MGR MEDICAL UNIVERSITY
A CLINICAL STUDY OF ECTROPION AND ENTROPION Regional Institute of Ophthalmology & Government Ophthalmic Hospital Madras Medical College Chennai Dissertation Submitted to THE TAMILNADU DR. MGR MEDICAL UNIVERSITY
Chapter 16. Cosmetic Concerns. Better Blood Supply and Circulation
 Chapter 16 FACIAL LACERATIONS KEY FIGURES: Tissue flap Suture bites: face vs. rest of body Lip anatomy Soft tissue loss The face has several unique properties that dictate the choice of treatment after
Chapter 16 FACIAL LACERATIONS KEY FIGURES: Tissue flap Suture bites: face vs. rest of body Lip anatomy Soft tissue loss The face has several unique properties that dictate the choice of treatment after
Protocol. Blepharoplasty
 Protocol Blepharoplasty Medical Benefit Effective Date: 01/01/13 Next Review Date: 05/19 Preauthorization No Review Dates: 09/12, 09/13, 09/14, 09/15, 09/16, 05/17, 05/18 Preauthorization is encouraged
Protocol Blepharoplasty Medical Benefit Effective Date: 01/01/13 Next Review Date: 05/19 Preauthorization No Review Dates: 09/12, 09/13, 09/14, 09/15, 09/16, 05/17, 05/18 Preauthorization is encouraged
Unit VIII Problem 8 Anatomy: Orbit and Eyeball
 Unit VIII Problem 8 Anatomy: Orbit and Eyeball - The bony orbit: it is protecting our eyeball and resembling a pyramid: With a base directed: anterolaterally. And an apex directed: posteromedially. Notes:
Unit VIII Problem 8 Anatomy: Orbit and Eyeball - The bony orbit: it is protecting our eyeball and resembling a pyramid: With a base directed: anterolaterally. And an apex directed: posteromedially. Notes:
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
Raising the suborbicularis oculi fat (SOOF): its role in chronic facial palsy
 Br J Ophthalmol 2;84:141 146 141 Western Eye Hospital, Marylebone Road, London NW1 5YE and Eye Department, Charing Cross Hospital, Fulham Palace Road, London W6 8RF, UK J M Olver Correspondence to: Western
Br J Ophthalmol 2;84:141 146 141 Western Eye Hospital, Marylebone Road, London NW1 5YE and Eye Department, Charing Cross Hospital, Fulham Palace Road, London W6 8RF, UK J M Olver Correspondence to: Western
To successfully perform any facial injection,
 INJECTABLES Newer Understanding of Specific Anatomic Targets in the Aging Face as Applied to Injectables: Facial Muscles Identifying Optimal Targets for Neuromodulators Jonathan M. Sykes, MD Patrick Trevidic,
INJECTABLES Newer Understanding of Specific Anatomic Targets in the Aging Face as Applied to Injectables: Facial Muscles Identifying Optimal Targets for Neuromodulators Jonathan M. Sykes, MD Patrick Trevidic,
Lower Eyelid Blepharoplasty. Mid-Year Seminar AOCOO-HNS Foundation September 21 st, 2013
 Lower Eyelid Blepharoplasty Mid-Year Seminar AOCOO-HNS Foundation September 21 st, 2013 The beauty of a woman must be seen from in her eyes, because that is the doorway to her heart, the place where love
Lower Eyelid Blepharoplasty Mid-Year Seminar AOCOO-HNS Foundation September 21 st, 2013 The beauty of a woman must be seen from in her eyes, because that is the doorway to her heart, the place where love
Excessive skin on the eyelids due to chronic blepharedema, which physically stretches the skin.
 Retired Date: Page 1 of 10 1. POLICY DESCRIPTION: Guideline for Blepharoplasty 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management, Pharmacy, Claim
Retired Date: Page 1 of 10 1. POLICY DESCRIPTION: Guideline for Blepharoplasty 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management, Pharmacy, Claim
Classically, the normal eyelid anatomy can
 IDEAS AND INNOVATIONS The Concept of a Glide Zone as It Relates to Upper Lid Crease, Lid Fold, and Application in Upper Blepharoplasty William Pai-Dei Chen, M.D. Los Angeles, Torrance, and Irvine, Calif.
IDEAS AND INNOVATIONS The Concept of a Glide Zone as It Relates to Upper Lid Crease, Lid Fold, and Application in Upper Blepharoplasty William Pai-Dei Chen, M.D. Los Angeles, Torrance, and Irvine, Calif.
TRADITIONAL methods of
 Superior Cantholysis for Zygomatic Fracture Repair Robert W. Dolan, MD; Daniel K. Smith, MD ORIGINAL ARTICLE Objective: To determine if performing a superior cantholysis eases the surgical exposure, reduction,
Superior Cantholysis for Zygomatic Fracture Repair Robert W. Dolan, MD; Daniel K. Smith, MD ORIGINAL ARTICLE Objective: To determine if performing a superior cantholysis eases the surgical exposure, reduction,
Maxilla, ORBIT and infratemporal fossa. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Only the Mohs Knows: Management of Periocular Skin Cancers
 Only the Mohs Knows: Management of Periocular Skin Cancers Andrew R. Harrison, M.D. Director, Oculoplastic and Orbital Surgery University of Minnesota Overview Common Eyelid Skin Cancers Management Options
Only the Mohs Knows: Management of Periocular Skin Cancers Andrew R. Harrison, M.D. Director, Oculoplastic and Orbital Surgery University of Minnesota Overview Common Eyelid Skin Cancers Management Options
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY PARAMEDIAN FOREHEAD FLAP NASAL RECONSTRUCTION SURGICAL TECHNIQUE Brian Cervenka, Travis Tollefson, Patrik Pipkorn The paramedian forehead
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY PARAMEDIAN FOREHEAD FLAP NASAL RECONSTRUCTION SURGICAL TECHNIQUE Brian Cervenka, Travis Tollefson, Patrik Pipkorn The paramedian forehead
Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A.
 UvA-DARE (Digital Academic Repository) Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A. Link to publication Citation for published
UvA-DARE (Digital Academic Repository) Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A. Link to publication Citation for published
23 Lateral Canthal Complications in Aesthetic Eyelid Surgery: Prevention and Reconstruction
 23 Lateral Canthal Complications in Aesthetic Eyelid Surgery: Prevention and Reconstruction M. Douglas Gossman 23.1 Introduction The lateral canthus is an important aesthetic facial landmark. It is formed
23 Lateral Canthal Complications in Aesthetic Eyelid Surgery: Prevention and Reconstruction M. Douglas Gossman 23.1 Introduction The lateral canthus is an important aesthetic facial landmark. It is formed
Pathogenesis and surgical correction of dynamic lower scleral show as a sign of disinsertion of the levator aponeurosis from the tarsus *
 British Journal of Plastic Surgery (2005) 58, 668 675 Pathogenesis and surgical correction of dynamic lower scleral show as a sign of disinsertion of the levator aponeurosis from the tarsus * Kiyoshi Matsuo*,
British Journal of Plastic Surgery (2005) 58, 668 675 Pathogenesis and surgical correction of dynamic lower scleral show as a sign of disinsertion of the levator aponeurosis from the tarsus * Kiyoshi Matsuo*,
Lower Eyelid Reconstruction after Basal Cell Carcinoma Removal
 Lower Eyelid Reconstruction after Basal Cell Carcinoma Removal A Decision Management Tool Pooja Sethi 1, Soroosh Behshad 1, Alejandra A. Valenzuela 1 Corresponding author address: From Department of Ophthalmology,
Lower Eyelid Reconstruction after Basal Cell Carcinoma Removal A Decision Management Tool Pooja Sethi 1, Soroosh Behshad 1, Alejandra A. Valenzuela 1 Corresponding author address: From Department of Ophthalmology,
Naso-Orbital Complex Reconstruction with Titanium Mesh and Canthopexy
 Case Report imedpub Journals http://www.imedpub.com DOI: 10.4172/2472-1905.100011 Naso-Orbital Complex Reconstruction with Titanium Mesh and Canthopexy Abstract Context: We are introducing the reconstruction
Case Report imedpub Journals http://www.imedpub.com DOI: 10.4172/2472-1905.100011 Naso-Orbital Complex Reconstruction with Titanium Mesh and Canthopexy Abstract Context: We are introducing the reconstruction
Blepharoplasty. Definitions
 Last Review Date: June 9, 2017 Number: MG.MM.SU.10eC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: June 9, 2017 Number: MG.MM.SU.10eC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
LOWER EYELID ENTROPION IS A COMMONLY ACQUIRED
 External (Subciliary) Vs Internal (Transconjunctival) Involutional Entropion Repair GUY J. BEN SIMON, MD, MARGARITA MOLINA, MD, ROBERT M. SCHWARCZ, MD, JOHN D. MCCANN, MD, PHD, AND ROBERT A. GOLDBERG,
External (Subciliary) Vs Internal (Transconjunctival) Involutional Entropion Repair GUY J. BEN SIMON, MD, MARGARITA MOLINA, MD, ROBERT M. SCHWARCZ, MD, JOHN D. MCCANN, MD, PHD, AND ROBERT A. GOLDBERG,
The Orbit. The Orbit OCULAR ANATOMY AND DISSECTION 9/25/2014. The eye is a 23 mm organ...how difficult can this be? Openings in the orbit
 The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
Our Experience with Endoscopic Brow Lifts
 Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
Technique Guide. Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures.
 Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Dynamic Diagnosis of Fishmouthing Syndrome, an Overlooked Complication of Blepharoplasty
 Oculoplastic Surgery Dynamic Diagnosis of Fishmouthing Syndrome, an Overlooked Complication of Blepharoplasty Aesthetic Surgery Journal 33(4) 497 504 2013 The American Society for Aesthetic Plastic Surgery,
Oculoplastic Surgery Dynamic Diagnosis of Fishmouthing Syndrome, an Overlooked Complication of Blepharoplasty Aesthetic Surgery Journal 33(4) 497 504 2013 The American Society for Aesthetic Plastic Surgery,
Management of the Aging Upper Face December 2001
 TITLE: Management of the Aging Upper Face SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: December 5, 2001 RESIDENT PHYSICIAN: Edward Buckingham, MD FACULTY ADVISOR: Karen Calhoun,
TITLE: Management of the Aging Upper Face SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: December 5, 2001 RESIDENT PHYSICIAN: Edward Buckingham, MD FACULTY ADVISOR: Karen Calhoun,
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
SINGLE INCISION REJUVENATION OF THE PERIORBITAL AESTHETIC UNIT
 EDITORIAL SPOTLIGHT SINGLE INCISION REJUVENATION OF THE PERIORBITAL AESTHETIC UNIT BY THOMAS J. OBERG, MD; GRANT H. MOORE, MD; KIAN EFTEKHARI, MD; MICHAEL W. WORLEY, MD; AND RICHARD L ANDERSON, MD A PARADIGM
EDITORIAL SPOTLIGHT SINGLE INCISION REJUVENATION OF THE PERIORBITAL AESTHETIC UNIT BY THOMAS J. OBERG, MD; GRANT H. MOORE, MD; KIAN EFTEKHARI, MD; MICHAEL W. WORLEY, MD; AND RICHARD L ANDERSON, MD A PARADIGM
Blepharoplasty Aging Face / Rhytidectomy Rhinoplasty Facial Resurfacing Cleft Lip/Palate Hair Transplantation
 2008 Blepharoplasty Aging Face / Rhytidectomy Rhinoplasty Facial Resurfacing Cleft Lip/Palate Hair Transplantation Dermatochalasis: laxity and redundancy of eyelid skin secondary to aging. (OLDER PATIENTS).
2008 Blepharoplasty Aging Face / Rhytidectomy Rhinoplasty Facial Resurfacing Cleft Lip/Palate Hair Transplantation Dermatochalasis: laxity and redundancy of eyelid skin secondary to aging. (OLDER PATIENTS).
PTERYGOPALATINE FOSSA
 PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
Adjustable sutures in eyelid surgery for ptosis and lid retraction
 British Journal ofophthalmology 1994; 78: 167-174 Adjustable sutures in eyelid surgery for ptosis and lid retraction J R 0 Collin, B A O'Donnell Abstract New techniques are described and illustrated for
British Journal ofophthalmology 1994; 78: 167-174 Adjustable sutures in eyelid surgery for ptosis and lid retraction J R 0 Collin, B A O'Donnell Abstract New techniques are described and illustrated for
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Aesthetic Lateral Canthoplasty
 ORIGINAL ARTICLE Mehryar Taban, M.D.*, Tanuj Nakra, M.D., Catherine Hwang, M.D.*, Jonathan A. Hoenig, M.D.*, Raymond S. Douglas, M.D., Ph.D.*, Norman Shorr, M.D.*, and Robert A. Goldberg, M.D.* *Department
ORIGINAL ARTICLE Mehryar Taban, M.D.*, Tanuj Nakra, M.D., Catherine Hwang, M.D.*, Jonathan A. Hoenig, M.D.*, Raymond S. Douglas, M.D., Ph.D.*, Norman Shorr, M.D.*, and Robert A. Goldberg, M.D.* *Department
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures.
 Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Regional nerve block of the upper eyelid in oculoplastic surg e r y
 E u ropean Journal of Ophthalmology / Vol. 16 no. 4, 2006 / pp. 5 0 9-5 1 3 Regional nerve block of the upper eyelid in oculoplastic surg e r y A.R. ISMAIL, T. ANTHONY, D.J. MORDANT, H. MacLEAN Portsmouth
E u ropean Journal of Ophthalmology / Vol. 16 no. 4, 2006 / pp. 5 0 9-5 1 3 Regional nerve block of the upper eyelid in oculoplastic surg e r y A.R. ISMAIL, T. ANTHONY, D.J. MORDANT, H. MacLEAN Portsmouth
Modified Double-Eyelid Blepharoplasty Using the Single-Knot Continuous Buried Non-Incisional Technique
 Modified Double-Eyelid Blepharoplasty Using the Single-Knot Continuous Buried Non-Incisional Technique Kyung-Chul Moon, Eul-Sik Yoon, Jun-Mun Lee Department of Plastic and Reconstructive Surgery, Korea
Modified Double-Eyelid Blepharoplasty Using the Single-Knot Continuous Buried Non-Incisional Technique Kyung-Chul Moon, Eul-Sik Yoon, Jun-Mun Lee Department of Plastic and Reconstructive Surgery, Korea
be very thin and variable. Facial nerve branches that exit the parotid gland are deep to the SMAS.
 The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
ORIGINAL ARTICLE. Reconstruction of the Nasal Columella. David A. Sherris, MD; Jon Fuerstenberg, MD; Daniel Danahey, MD, PhD; Peter A.
 ORIGINAL ARTICLE Reconstruction of the Nasal Columella David A. Sherris, MD; Jon Fuerstenberg, MD; Daniel Danahey, MD, PhD; Peter A. Hilger, MD Objective: To report techniques successful for nasal columella
ORIGINAL ARTICLE Reconstruction of the Nasal Columella David A. Sherris, MD; Jon Fuerstenberg, MD; Daniel Danahey, MD, PhD; Peter A. Hilger, MD Objective: To report techniques successful for nasal columella
5/20/2015. Mohs Surgery BCCA High risk anatomic locations. Mohs Surgery High risk anatomic locations. Mohs Surgery Histologically Aggressive BCCA
 Mohs Surgery BCCA High risk anatomic locations High risk areas H zone nasal ala, nasal septum, nasal ala groove, periorbital region, periauricual region, region around and in ear canal, ear pinna and scalp
Mohs Surgery BCCA High risk anatomic locations High risk areas H zone nasal ala, nasal septum, nasal ala groove, periorbital region, periauricual region, region around and in ear canal, ear pinna and scalp
Corporate Medical Policy
 Corporate Medical Policy Reconstructive Eyelid Surgery and Brow Lift File Name: Origination: Last CAP Review: Next CAP Review: Last Review: reconstructive_eyelid_surgery_and_brow_lift 1/2000 8/2017 8/2018
Corporate Medical Policy Reconstructive Eyelid Surgery and Brow Lift File Name: Origination: Last CAP Review: Next CAP Review: Last Review: reconstructive_eyelid_surgery_and_brow_lift 1/2000 8/2017 8/2018
Eyelid basal cell carcinoma Patient information
 Eyelid basal cell carcinoma Patient information Your procedure relates to the face, eyelids, orbit or tear drainage system that together are treated by specialist surgeons in the field of oculoplastic
Eyelid basal cell carcinoma Patient information Your procedure relates to the face, eyelids, orbit or tear drainage system that together are treated by specialist surgeons in the field of oculoplastic
Knee Disarticulation Amputation
 Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Cosmetic Lateral Canthoplasty: Preserving the Lateral Canthal Angle
 Topic Cosmetic Lateral Canthoplasty: Preserving the Lateral Canthal ngle Yeon-Jun Kim 1, Kyu Ho Lee 2, Hong Lim Choi 1, Eui Cheol Jeong 3 1 JW Plastic Surgery Center, Seoul; 2 CK Plastic Surgery Clinic,
Topic Cosmetic Lateral Canthoplasty: Preserving the Lateral Canthal ngle Yeon-Jun Kim 1, Kyu Ho Lee 2, Hong Lim Choi 1, Eui Cheol Jeong 3 1 JW Plastic Surgery Center, Seoul; 2 CK Plastic Surgery Clinic,
Case Presentation: Indications for orbital decompression in TED: Modern surgical techniques for orbital decompression in TED: Inferomedial
 Case Presentation: Jonathan W. Kim, MD Director, Oculoplastic Surgery Stanford Medical Center 61 year old man with active Graves orbitopathy Visual acuity 20/30 OD 20/50 OS Left RAPD Bilateral optic disc
Case Presentation: Jonathan W. Kim, MD Director, Oculoplastic Surgery Stanford Medical Center 61 year old man with active Graves orbitopathy Visual acuity 20/30 OD 20/50 OS Left RAPD Bilateral optic disc
RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP. By MICHAL KRAUSS. Plastic Surgery Hospital, Polanica-Zdroj, Poland
 RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP By MICHAL KRAUSS Plastic Surgery Hospital, Polanica-Zdroj, Poland RECONSTRUCTION of the nose is one of the composite procedures in
RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP By MICHAL KRAUSS Plastic Surgery Hospital, Polanica-Zdroj, Poland RECONSTRUCTION of the nose is one of the composite procedures in
Dissection of the Eyelid and Orbit with Modernised Anatomical Findings
 The Open Anatomy Journal, 2010, 2, 5-24 5 Open Access Dissection of the Eyelid and Orbit with Modernised Anatomical Findings Hirohiko Kakizaki *,1, Seah Lay-Leng 2, Ken Asamoto 3, Takashi Nakano 3, Dinesh
The Open Anatomy Journal, 2010, 2, 5-24 5 Open Access Dissection of the Eyelid and Orbit with Modernised Anatomical Findings Hirohiko Kakizaki *,1, Seah Lay-Leng 2, Ken Asamoto 3, Takashi Nakano 3, Dinesh
