Effect of thread size on the implant neck area: preliminary results at 1 year of function
|
|
|
- Imogene Daniels
- 5 years ago
- Views:
Transcription
1 Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang Moon, Department of Periodontology, Gangnam Severance Dental Hospital, College of Dentistry, Yonsei University, Seoul, Korea Kwang-Ho Park, Department of Oral and Maxillofacial Surgery, Gangnam Severance Dental Hospital, College of Dentistry, Yonsei University, Seoul, Korea Corresponding author: Prof. Ik-Sang Moon Department of Periodontology, Gangnam Severance Dental Hospital, College of Dentistry, Yonsei University Dogok-dong, Gangnam-gu, Seoul, Korea Tel.: Fax: ismoon@yuhs.ac Key words: alveolar bone loss, dental implants, microthread, prospective study, thread size Abstract Objectives: To evaluate and compare the effect of the coronal thread size on the marginal bone loss around the fixtures, when both implants were provided with threads to the top of fixture. Materials and methods: Two groups of implants, one with a macro-thread to the top of the fixture (A) and the other with a micro-thread to the top of the fixture (B), were placed adjacent to each other in the partially edentulous areas of 20 patients. Bone loss around each implant was analyzed after 1 year of functional loading. The bone losses after loading were compared using Wilcoxon s signed-rank test. Results: The mean marginal bone losses (A, ± mm; B, ± mm) were not statistically significant between the two groups (P = 0.669). Conclusions: There was no significant difference between implant with macro- and micro-neck thread in terms of marginal bone loss after 1 year of loading. *Contributed equally. Date: Accepted 3 July 2011 To cite this article: Kang Y-I, Lee D-W, Park K-H, Moon I-S. Effect of thread size on the implant neck area: preliminary results at 1 year of function. Clin. Oral Impl. Res. 00, 2011, 1 5 doi: /j x Recent clinical studies by our group regarding the effect of micro-thread on the marginal bone level showed that (i) the use of microthread on the implant neck area can preserve the peri-implant marginal bone effectively, compared with the fixtures without microthread (Lee et al. 2007), (ii) the location of the micro-thread in the neck area plays an important role in peri-implant marginal bone stabilization (Song et al. 2009) and (iii) difference in gross fixture design on the neck area did not result in significant difference of marginal bone loss (Kim et al. 2010). Naturally, the sequel question arose regarding the effect of the thread size on the neck portion of the implant. The use of certain pitch distances of the threads was known to be a favorable element in preserving the peri-implant bone (Motoyoshi et al. 2005). According to finite element analysis, very small threads with a favorable profile can affect the stress distribution in the bone as much as commonly sized threads (Hansson & Werke 2003). Adequate mechanical stimulation is an important requirement for the successful integration of load-bearing surfaces (Wiskott & Belser 1999). From a biomechanical perspective, retention elements such as the threads on the implant neck area provide the mechanical stimulation required to maintain the marginal bone level (Hansson 1999). Studies have verified the advantages of microthread on the coronal portion of fixture, compared with a smooth neck, in terms of the established bone-to-implant contact and marginal bone level maintenance (Berglundh et al. 2005; Abrahamsson & Berglundh 2006). The role of micro-threads in the neck portion has been researched in numerous studies (Hansson & Werke 2003; Berglundh et al. 2005; Abrahamsson & Berglundh 2006; Lee et al. 2007; Song et al. 2009; Kim et al. 2010). In contrast, few clinical studies have addressed the role of thread size, or thread pitch distance, on the maintenance of the peri-implant marginal bone, when the threads were positioned to the top of fixtures. Thus, the aim of this clinical investigation was to evaluate and to compare the effect of the coronal thread design on the marginal bone loss around the fixtures, when both implants were provided with threads to the top of fixture, but the size of the threads differs between the implants. Material and methods This study was approved by the Institutional Review Board of Gangnam Severance Hospital, Yonsei University. Patients were 2011 John Wiley & Sons A/S 1
2 informed of the study procedures and all provided with written informed consent. Patients Using the data from the previous publication (Lee et al. 2007), which had similar protocol with the present study, sample calculation was performed with computer software (Med- Calc for Windows, version , MedCalc Software, Mariakerke, Belgium). It revealed that 20 cases were necessary to obtain statistically significant results (the difference between the mean of groups is 0.14; SD 1 = 0.11; SD 2 = 0.19; a = 0.05; b = 0.20). At the time of inclusion to the present study, all the patients showed good general health, had been treated for existing moderate to severe chronic periodontal disease. The diagnostic criteria followed the 1999 classification for periodontal disease (Armitage 1999). All the patients received initial therapy including oral hygiene instruction, scaling and root planning, and subsequent corrective therapy including extraction and periodontal flap surgery at the Department of Periodontology at Gangnam Severance Hospital (College of Dentistry, Yonsei University, Seoul, Korea). Patients received implant surgeries from July 2007 to June In total, 40 implants in 20 patients (12 men, 8 women, mean age: 52.6 years, age range: years, Table 1) were included in the study. thread pitch from the apex to the neck area. Compared to Group A, the threads of the Group B implants (Megafix Internal, Megagen, Seoul, Korea) are smaller in both pitch and depth in the 3.0-mm neck area (Fig. 1). The depth and pitch of the Group A implants were 0.35 and 0.6 mm, respectively, and those of the Group B implant were 0.15 and 0.3 mm, respectively. Both implant types are single-threaded screws with a V-shape thread (Abuhussein et al. 2010). The thread on the neck portion of Group A is designated as a macro-thread and that of Group B is designated as a micro-thread. Both implant types are made of commercially pure titanium, surface treated with resorbable blast media, and both have the same implant abutment connection type (conical seal type with an internal slope of 11 ). Treatment procedure The treatment procedure was performed as previously described (Lee et al. 2007; Song et al. 2009; Kim et al. 2010). In brief, all surgeries were performed using a two-stage method. Implants from each group were placed adjacent to each other in the partially edentulous premolar and molar areas of each patient. The mesiodistal location of each implant was randomly determined. The diameter could not be matched on some patients (patient 1, 3, 6, 10, 11, and 19), since utmost care was taken to preserve 1 mm of bone remaining both buccally and lingually. The implants were placed at or slightly below the marginal bone level, following the manufacturer s guidelines. The location of each implant type is illustrated in Table 1. A second surgery was performed 3 or 6 months later for maxillary or mandibular implants, respectively. The prostheses were delivered 3 weeks after the second surgery. Patients were recalled every 6 months for oral hygiene evaluation, professional plaque control, and review of self-performed oral hygiene instructions. Implants The two groups of implants used in this study differ in the thread size of the implant neck area. Group A implants (EZ Plus Internal, Megagen, Seoul, Korea) have a uniform Fig. 1. Schematic presentation of the implants. (a) Macro-thread implant; (b) Micro-thread implant. Table 1. Characteristics of the subject population, position, and type of the implants Subject Age Gender Tooth no. Fixture type Subject Age Gender Tooth no. Fixture type 1 52 M 35 A M 15 A 36 B 14 B 2 55 M 26 A M 25 A 27 B 24 B 3 23 F 15 A F 36 A 14 B 37 B 4 63 M 47 A F 27 A 46 B 26 B 5 56 F 36 A M 35 A 37 B 34 B 6 65 F 25 A M 15 A 26 B 14 B 7 48 F 24 A M 26 A 25 B 25 B 8 47 M 25 A M 17 A 26 B 16 B 9 56 M 25 A * F 47 A 27 B * 46 B M 35 A F 36 A 36 B 37 B * In one patient, the implants were not placed immediately adjacent to each other and were splinted to fabricate three-unit bridges. 2 Clin. Oral Impl. Res. 0, 2011 / John Wiley & Sons A/S
3 Radiographic examination Radiographs were taken and measured as previously described (Lee et al. 2005, 2007; Song et al. 2009; Kim et al. 2010). Briefly, periapical radiographs (Kodak Insight, film speed F, Rochester, NY, USA) were taken at several time points: 1 day after implant placement, immediately after the second surgery, immediately after prosthesis delivery, and 1 year after functional loading (Fig. 2). Radiographs were taken with an XCP device (Extension cone paralleling Kit, Rinn, Elgin, IL, USA) using the parallel cone technique (70 kv, 8 ma, s). A 5.5-mm spherical metal bearing was placed for calibration. All films were developed using the same automatic processor (Periomat, Durr Dental, Bietigheim-Bissingen, Germany) following the manufacturer s instructions. Films were digitized using a digital scanner (EpsonGT , Epson, Nagano, Japan) at an input resolution of 2400 dpi with 256 gray scale values. Measurement of marginal bone level change All images were transferred to a personal computer (Processor, Intel Core2 Duo E8200, Santa Clara, CA, USA; operating system, Windows XP Professional 2002, Redmond, WA, USA). The same monitor (Flatron LX1717, LG, Seoul, Korea), set to a resolution of , was used to examine all the digitized radiographs. The room was kept dark throughout the computer-assisted radiographic measurement process. The marginal bone height was measured at three time points: at implant placement, at prosthesis delivery, and after 1 year of functional loading. The marginal bone height was measured as the distance between the reference point and the most apical point of the marginal bone level. The reference point was the border between the polished surface and the rough surface of the fixture. Calibration was performed using the known distance of the spherical metal bearing (5.5 mm). Measurements were taken to the nearest 0.01 mm using the UTHSCSA Image Tool computer software program (version 3.00, University of Texas Health Science Center in San Antonio). Bone height was measured at the mesial and distal peri-implant sites, and their average values were used. Bone loss was measured by comparing the radiographs taken immediately after prosthesis delivery to those taken 1 year after functional loading. As the interval between implant placement and baseline differed between the subjects, the marginal bone height measured at implant placement was not used for statistical analysis. All measurements were made by the same operator (Y-I K.). To test intraobserver variability, the marginal bone loss values of 20 arbitrarily selected periapical films were measured twice within a 1-week time interval. Follow-up parameters At the 1-year follow-up visit, implants were evaluated for pain, discomfort, and implantrelated infection. An implant was deemed as surviving when it was stable, functional, and asymptomatic. To rule out the possible influence of inflammatory changes of the peri-implant tissues on the surrounding marginal bone, the modified plaque index (mpi), and modified sulcus bleeding index (mbi) were measured at four aspects around each implant (Mombelli et al. 1987). The averages of the four mpi and mbi values were calculated to represent the respective values for each implant. Statistical analysis Intra-class correlation was used to test intrarater reliability. As the differences of the paired data on marginal bone loss did not show symmetric distribution (coefficient of skewness = 1.18, P = 0.025), Sign test was used to analyze the differences in periimplant marginal bone loss between the two groups. Wilcoxon s signed-rank test was used to analyze the differences in mpi and mbi. Computer software programs (MedCalc for Windows, version , MedCalc Software; SPSS, version 17, SPSS Inc, Chicago, IL, USA) were used to process the data. The values were deemed statistically significant if the P-value was <0.05. Results Clinical examination The implants of all of the patients were well maintained at the periodic follow-ups. All of the implants functioned normally during the observation period, with no sign of pain, swelling, pus discharge, or mobility. No prosthetic complications were observed. Marginal bone level changes The intra-rater reliability was high (R = 0.89) for measurements of Group A and Group B implants. A sign test indicated that marginal bone loss of Group A and Group B did not differ statistically (P = 0.803, Fig. 3, Table 2). Fig. 4 illustrates the median value of marginal bone level at different examinations. Evaluation of peri-implant soft tissue For Groups A and B, the average plaque indices were 0.35 and 0.4, respectively, and the Fig. 3. Box plot of the bone loss around the macrothread (A) and micro-threads (B) implants. (a) (b) (c) (d) Fig. 2. Intra-oral radiographs of the implants with macro-threads (A) and micro-threads (B). (a) First surgery; (b) Second surgery; (c) Prosthesis delivery; (d) 1-year follow-up. Fig. 4. Median value of marginal bone level at implant placement, baseline (prosthesis delivery) and 1 year after functional loading on macro-threads (A) and micro-threads (B) implants John Wiley & Sons A/S 3 Clin. Oral Impl. Res. 0, 2011 / 1 5
4 Table 2. Marginal bone loss (mm) around implants in Groups A and B Bone loss Subject A B Median % confidence interval for the median 95% confidence 0.04 to 0.09 interval for the median of the difference P-value average mucosal indices were 0.28 and 0.21, respectively. The mpi and mbi for each implant type are illustrated in Table 3. No significant differences in plaque accumulation (P = 0.297) or sulcus bleeding (P = 0.636) were found between Groups A and B. Discussion Placing micro-threads on the implant neck greatly increases the ability of an implant to resist axial loads, and the mechanical stimulus provided by the micro-threads helps to preserve peri-implant marginal bone (Hansson 1999). In a 3-year prospective study, we previously reported that use of micro-threads in the implant neck area can reduce periimplant marginal bone loss, although the study was performed on implants with different neck designs (Lee et al. 2007). Kim et al. (2010) found no difference in bone loss between conical- and straight-shaped implants, both of which had micro-threads. Another study found that implants with threads that began at the top showed less bone loss than otherwise-identical implants where the threads began 0.5-mm from the top (Song et al. 2009). These results indicate that the presence or absence of threads and the thread location can affect the marginal bone preservation. The thread size can be described by the thread depth (i.e. distance from the tip of the thread to the body) and thread pitch (i.e. distance from the center of the thread to the center of the next thread). A finite element Table 3. Modified plaque index (mpi) and modified sulcus bleeding index (mbi) of implants in Groups A and B mpi Subject A B A B Median % confidence interval for the median P-value mbi study comparing the effect of thread depth on marginal bone found no significant difference in the stress distribution when a thread depth of 0.1 or 0.4 mm was used, so long as the thread profile was favorable (Hansson & Werke 2003). However, the results of studies for thread pitch are controversial. In a finite element study, implants with a 0.5-mm pitch had a more favorable stress distribution than those with a pitch of 1.0 or 1.5, and the maximum effective stress gradually decreased with decreasing thread pitch (Motoyoshi et al. 2005). In another study also using finite element study, a thread pitch of mm was considered as optimal from a biomechanical point of view (Kong et al. 2008). The present study was planned to examine the effect of thread size on the marginal bone. In particular, we compared the effect of macro- and micro-threads in the implant neck area in cases where the thread location was identical. To minimize the influence of the peri-implant mucosa and plaque accumulation on bone loss, oral hygiene instructions were provided to the patients and periodic clinical examinations of the peri-implant mucosa and professional plaque control were performed. The average bone losses in Groups A and B were and mm, respectively, after 1 year of functional loading (P > 0.05). The results of this study suggest that the thread size at the implant neck area does not affect the amount of marginal bone loss during the initial first year physiologic bone remodeling period, since both groups of implants had the identical rough surface. The amount of bone loss was minor, likely because both groups of implants had internal conical seal type fixture abutment connections, which are advantageous in marginal bone preservation (Norton 1998; Hansson 2000; van Steenberghe et al. 2000; Engquist et al. 2002). It is possible that the beneficial effects of the rough surface and conical fixture abutment interface on the marginal bone-level maintenance overwhelmed the additional effects of the microthread. Alternatively, macro-threads that begin at the top of the implant neck can be assumed to distribute stress under load and to maintain the marginal bone as much as micro-threads. There are several drawbacks of the present study. One is the short-term follow up period (1 year after functional loading). As graphically demonstrated on Fig. 4, the marginal bone loss of both implant systems is not yet stabilized. However, when we analyze a previous study using similar protocol of the 4 Clin. Oral Impl. Res. 0, 2011 / John Wiley & Sons A/S
5 present study (Lee et al. 2007), the most critical period of the bone level changes occurred 1 year after loading. Stabilization around peri-implant marginal bone was observed after 1-year, which did not show statistically significant additional marginal bone resorption. It was interesting to compare the bone loss during this period, since it shows us the effect of implant design on the initial physiologic bone remodeling phase. After this phase, bone loss is mainly due to the bacterial infection (Lang & Berglundh 2011). However, whether this stabilization period would occur in this implant system is currently not known. This study is an interim report of the 5-year prospective study, and further evaluation and patient recruitment is still ongoing. The other drawback is the differences in fixture diameter, gender, age, and implant sites. These factors are possible confounding factors for the marginal bone loss and need to be stratified, if we could recruit larger numbers of patients. Within the limitations of the study, it may be concluded that macro-threads in the neck portion of an implant appear to have a similar ability to preserve the marginal bone as micro-threads. Acknowledgements: There were no financial relationships between any of the authors and the manufacturers of products involved in the study. This study was supported by a faculty research grant of Yonsei University College of Dentistry for 2010( ). Drs Kang and Lee contributed equally to the research in this study. References Abrahamsson, I. & Berglundh, T. (2006) Tissue characteristics at microthreaded implants: an experimental study in dogs. Clinical Implant Dentistry and Related Research 8: Abuhussein, H., Pagni, G., Rebaudi, A. & Wang, H. L. (2010) The effect of thread pattern upon implant osseointegration. Clinical Oral Implants Research 21: Armitage, G. (1999) Development of a classification system for periodontal disease and conditions. Annals of Periodontology 4: 1 6. Berglundh, T., Abrahamsson, I. & Lindhe, J. (2005) Bone reactions to longstanding functional load at implants: an experimental study in dogs. Journal of Clinical Periodontology 32: Engquist, B., Astrand, P., Dahlgren, S., Engquist, E., Feldmann, H. & Grondahl, K. (2002) Marginal bone reaction to oral implants: a prospective comparative study of Astra Tech and Branemark System implants. Clinical Oral Implants Research 13: Hansson, S. (1999) The implant neck: smooth or provided with retention elements. A biomechanical approach. Clinical Oral Implants Research 10: Hansson, S. (2000) Implant-abutment interface: biomechanical study of flat top versus conical. Clinical Implant Dentistry and Related Research 2: Hansson, S. & Werke, M. (2003) The implant thread as a retention element in cortical bone: the effect of thread size and thread profile: a finite element study. Journal of Biomechanics 36: Kim, J.J., Lee, D.W., Kim, C.K., Park, K.H. & Moon, I.S. (2010) Effect of conical configuration of fixture on the maintenance of marginal bone level: preliminary results at 1 year of function. Clinical Oral Implants Research 21: Kong, L., Hu, K., Li, D., Song, Y., Yang, J., Wu, Z. & Liu, B. (2008) Evaluation of the cylinder implant thread height and width: a 3-dimensional finite element analysis. International Journal of Oral and Maxillofacial Implants 23: Lang, N.P. & Berglundh, T. (2011) Periimplant diseases: where are we now? consensus of the Seventh European Workshop on Periodontology Journal of Clinical Periodontology 38 (Suppl. 11): Lee, D.W., Choi, Y.S., Park, K.H., Kim, C.S. & Moon, I.S. (2007) Effect of microthread on the maintenance of marginal bone level: a 3-year prospective study. Clinical Oral Implants Research 18: Lee, D.W., Kim, C.K., Park, K.H., Cho, K.S. & Moon, I.S. (2005) Non-invasive method to measure the length of soft tissue from the top of the papilla to the crestal bone. Journal of Periodontology 76: Mombelli, A., van Oosten, M.A., Schurch, E. Jr & Land, N.P. (1987) The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiology and Immunology 2: Motoyoshi, M., Yano, S., Tsuruoka, T. & Shimizu, N. (2005) Biomechanical effect of abutment on stability of orthodontic mini-implant. A finite element analysis. Clinical Oral Implants Research 16: Norton, M.R. (1998) Marginal bone levels at single tooth implants with a conical fixture design. The influence of surface macro- and microstructure. Clinical Oral Implants Research 9: Song, D.W., Lee, D.W., Kim, C.K., Park, K.H. & Moon, I.S. (2009) Comparative analysis of periimplant marginal bone loss based on microthread location: a 1-year prospective study after loading. Journal of Periodontology 80: van Steenberghe, D., De Mars, G., Quirynen, M., Jacobs, R. & Naert, I. (2000) A prospective splitmouth comparative study of two screw-shaped self-tapping pure titanium implant systems. Clinical Oral Implants Research 11: Wiskott, H.W. & Belser, U.C. (1999) Lack of integration of smooth titanium surfaces: a working hypothesis based on strains generated in the surrounding bone. Clinical Oral Implants Research 10: John Wiley & Sons A/S 5 Clin. Oral Impl. Res. 0, 2011 / 1 5
Effect of conical configuration of fixture on the maintenance of marginal bone level: preliminary results at 1 year of function
 Jung-Joo Kim n Dong-Won Lee n Chong-Kwan Kim Kwang-Ho Park Ik-Sang Moon Effect of conical configuration of fixture on the maintenance of marginal bone level: preliminary results at 1 year of function Authors
Jung-Joo Kim n Dong-Won Lee n Chong-Kwan Kim Kwang-Ho Park Ik-Sang Moon Effect of conical configuration of fixture on the maintenance of marginal bone level: preliminary results at 1 year of function Authors
With the establishment of evaluation
 J Periodontol December 2009 Comparative Analysis of Peri-Implant Marginal Bone Loss Based on Microthread Location: A 1-Year Prospective Study After Loading Dong-Wook Song,* Dong-Won Lee,* Chong-Kwan Kim,
J Periodontol December 2009 Comparative Analysis of Peri-Implant Marginal Bone Loss Based on Microthread Location: A 1-Year Prospective Study After Loading Dong-Wook Song,* Dong-Won Lee,* Chong-Kwan Kim,
Effect of microthread on the maintenance of marginal bone level: a 3-year prospective study
 Dong-Won Lee Young-Shill Choi Kwang-Ho Park Chang-Sung Kim Ik-Sang Moon Effect of microthread on the maintenance of marginal bone level: a 3-year prospective study Authors affiliations: Dong-Won Lee, Young-Shill
Dong-Won Lee Young-Shill Choi Kwang-Ho Park Chang-Sung Kim Ik-Sang Moon Effect of microthread on the maintenance of marginal bone level: a 3-year prospective study Authors affiliations: Dong-Won Lee, Young-Shill
Tae-Hyung Kim. The Graduate School. Yonsei University. Department of Dental Science
 Influence of early cover screw exposure on the crestal bone loss around implants: comparison between exposed and non-exposed implants in identical subjects Tae-Hyung Kim The Graduate School Yonsei University
Influence of early cover screw exposure on the crestal bone loss around implants: comparison between exposed and non-exposed implants in identical subjects Tae-Hyung Kim The Graduate School Yonsei University
To achieve esthetic success with implant restorations,
 Case Series Influence of the Tooth- and Implant-Side Marginal Bone Level on the Interproximal Papilla Dimension in a Single Implant With a Microthread, Conical Seal, and Platform-Switched Design Hee-Jun
Case Series Influence of the Tooth- and Implant-Side Marginal Bone Level on the Interproximal Papilla Dimension in a Single Implant With a Microthread, Conical Seal, and Platform-Switched Design Hee-Jun
The peri-implant mucosa has
 Influence of Early Cover Screw Exposure on Crestal Bone Loss Around Implants: Intraindividual Comparison of Bone Level at Exposed and Non-Exposed Implants Tae-Hyung Kim,* Dong-Won Lee,* Chong-Kwan Kim,
Influence of Early Cover Screw Exposure on Crestal Bone Loss Around Implants: Intraindividual Comparison of Bone Level at Exposed and Non-Exposed Implants Tae-Hyung Kim,* Dong-Won Lee,* Chong-Kwan Kim,
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis.
 Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
The effect of peri-implant bone exposure on soft tissue healing and bone loss in two adjacent implants
 Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study
 Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study Toshio Takuma, DDS 1,2 /Keiji Oishi, DDS, PhD 3 /Tomofusa Manabe, DT 2 / Satoshi Yoneda, DDS, PhD 4 /Toshihiko
Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study Toshio Takuma, DDS 1,2 /Keiji Oishi, DDS, PhD 3 /Tomofusa Manabe, DT 2 / Satoshi Yoneda, DDS, PhD 4 /Toshihiko
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Replacement of missing teeth with
 A simple surgical technique to maximise prosthetic results Timothy Kosinski presents a technique to help minimise surgical risk, as well as helping the dentist to understand anatomy and proper implant
A simple surgical technique to maximise prosthetic results Timothy Kosinski presents a technique to help minimise surgical risk, as well as helping the dentist to understand anatomy and proper implant
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
AnyRidge Internal System
 Type of Normal Thin Low Loose bone Type of and selection of fixture With the normal ridge, Standard implant is more than enough because there are enough quantity and Normal quality of bone. Type of and
Type of Normal Thin Low Loose bone Type of and selection of fixture With the normal ridge, Standard implant is more than enough because there are enough quantity and Normal quality of bone. Type of and
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Factors influencing ridge alterations following immediate implant placement into extraction sockets
 Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
S i m p l i c I t y, c o m f o r t, a e s t h e t i c s. axiom. The new dimension
 S i m p l i c I t y, c o m f o r t, a e s t h e t i c s axiom The new dimension 2 Implants by anthogyr axiom, t h e n e w g e n e r a t i o n i m p l a n t axiom characteristics represent the perfect synthesis
S i m p l i c I t y, c o m f o r t, a e s t h e t i c s axiom The new dimension 2 Implants by anthogyr axiom, t h e n e w g e n e r a t i o n i m p l a n t axiom characteristics represent the perfect synthesis
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
High Crown to Implant Ratio as Stress Factor in Short Implants Therapy
 10.1515/bjdm-2016-0015 BALKAN JOURNAL OF DENTAL MEDICINE ISSN 2335-0245 STOMATOLOGICAL SOCIETY High Crown to Implant Ratio as Stress Factor in Short Implants Therapy SUMMARY Background/Aim: The purpose
10.1515/bjdm-2016-0015 BALKAN JOURNAL OF DENTAL MEDICINE ISSN 2335-0245 STOMATOLOGICAL SOCIETY High Crown to Implant Ratio as Stress Factor in Short Implants Therapy SUMMARY Background/Aim: The purpose
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Finite Element Analysis of Dental Implant as Orthodontic Anchorage
 JCDP 10.5005/jp-journals-10024-1044 ORIGINAL RESEARCH Finite Element Analysis of Dental Implant as Orthodontic Anchorage Finite Element Analysis of Dental Implant as Orthodontic Anchorage Anirban Sarmah,
JCDP 10.5005/jp-journals-10024-1044 ORIGINAL RESEARCH Finite Element Analysis of Dental Implant as Orthodontic Anchorage Finite Element Analysis of Dental Implant as Orthodontic Anchorage Anirban Sarmah,
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
MINI System CASE REPORT. Name: Dr. Achraf Souayah Na<on: Tunisia
 MINI System SE REPORT Name: Dr. chraf Souayah Na
MINI System SE REPORT Name: Dr. chraf Souayah Na
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. To systematically appraise the impact of mechanical/technical risk factors on
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. To systematically appraise the impact of mechanical/technical risk factors on
GuidedService. The ultimate guide for precise implantations
 GuidedService The ultimate guide for precise implantations ABGuidedService The ultimate guide for precise implantations At A.B. Dental we've brought implantology into the future with a 3D digitally planned
GuidedService The ultimate guide for precise implantations ABGuidedService The ultimate guide for precise implantations At A.B. Dental we've brought implantology into the future with a 3D digitally planned
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics.
 In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
Review The effect of thread pattern upon implant osseointegration
 Heba Abuhussein Giorgio Pagni Alberto Rebaudi Hom-Lay Wang Review The effect of thread pattern upon implant osseointegration Authors affiliations: Heba Abuhussein, Giorgio Pagni, Hom-Lay Wang, Department
Heba Abuhussein Giorgio Pagni Alberto Rebaudi Hom-Lay Wang Review The effect of thread pattern upon implant osseointegration Authors affiliations: Heba Abuhussein, Giorgio Pagni, Hom-Lay Wang, Department
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial
 Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Immediate Loading of a Multi-Threaded Implant
 Immediate Loading of a Multi-Threaded Implant Dr. Jonathan Yahav, DDS (Northwestern University, Chicago, IL) Aye Myat, BS in Biological Sciences (University of Illinois at Chicago, Chicago IL) Khasim Ali
Immediate Loading of a Multi-Threaded Implant Dr. Jonathan Yahav, DDS (Northwestern University, Chicago, IL) Aye Myat, BS in Biological Sciences (University of Illinois at Chicago, Chicago IL) Khasim Ali
Dentatus ANEW Narrow Diameter Implants. Expanding Implantology with More Treatment Options
 Dentatus ANEW Narrow Diameter Implants Expanding Implantology with More Treatment Options The Versatility of Dentatus ANEW LONG-TERM RESTORATIONS INTERIM SOLUTIONS LONG-TERM RESTORATIONS Many dentists
Dentatus ANEW Narrow Diameter Implants Expanding Implantology with More Treatment Options The Versatility of Dentatus ANEW LONG-TERM RESTORATIONS INTERIM SOLUTIONS LONG-TERM RESTORATIONS Many dentists
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Keywords: Biomechanics, Biostatistics, Maxilla, Maxillary sinus, Sinus floor augmentation.
 Research Article Journal of Periodontal J Periodontal Implant Sci 2013;43:58-63 http://dx.doi.org/10.5051/jpis.2013.43.2.58 Peri-implant bone length changes and survival rates of implants penetrating the
Research Article Journal of Periodontal J Periodontal Implant Sci 2013;43:58-63 http://dx.doi.org/10.5051/jpis.2013.43.2.58 Peri-implant bone length changes and survival rates of implants penetrating the
4766 Research Dr. San Antonio, TX insightdentalsystems.com
 OVERVIEW OF THE INSIGHT DENTAL IMPLANT DELIVERY SYSTEM The IDS system comes in a unit dose implant system where its advantage provides sterile instrumentation in one single-use kit. It is organized to
OVERVIEW OF THE INSIGHT DENTAL IMPLANT DELIVERY SYSTEM The IDS system comes in a unit dose implant system where its advantage provides sterile instrumentation in one single-use kit. It is organized to
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Peri-implant health and peri-implant bone stability after immediate implant placement
 2 First report of a two-year retrospective study with a newly developed bone-level implant system Peri-implant health and peri-implant bone stability after immediate implant placement DR-MEDIC STOM. HENRIETTE
2 First report of a two-year retrospective study with a newly developed bone-level implant system Peri-implant health and peri-implant bone stability after immediate implant placement DR-MEDIC STOM. HENRIETTE
Non-osseointegrated. What type of mini-implants? 3/27/2008. Require a tight fit to be effective Stability depends on the quality and.
 Non-osseointegrated What type of mini-implants? Require a tight fit to be effective Stability depends on the quality and quantity of cortical and trabecular bone. Osseointegrated Non-osseointegrated AbsoAnchor
Non-osseointegrated What type of mini-implants? Require a tight fit to be effective Stability depends on the quality and quantity of cortical and trabecular bone. Osseointegrated Non-osseointegrated AbsoAnchor
Stress and Displacement Analysis of Dental Implant Threads Using Three-Dimensional Finite Element Analysis
 1 Research Article Stress and Displacement Analysis of Dental Implant Threads Using Three-Dimensional Finite Element Analysis Aswin Yodrux* Department of Materials Handling and Logistics for Engineering,
1 Research Article Stress and Displacement Analysis of Dental Implant Threads Using Three-Dimensional Finite Element Analysis Aswin Yodrux* Department of Materials Handling and Logistics for Engineering,
More than pure esthetics. The natural and strong solution.
 More than pure esthetics. The natural and strong solution. Expand your patient pool with an innovative solution. With the Straumann PURE Ceramic Implant, clinicians have an additional option to convince
More than pure esthetics. The natural and strong solution. Expand your patient pool with an innovative solution. With the Straumann PURE Ceramic Implant, clinicians have an additional option to convince
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES
 Braz J Periodontol - September 2014 - volume 24 - issue 03 CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES Rachel de Queiroz Ferreira Rodrigues
Braz J Periodontol - September 2014 - volume 24 - issue 03 CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES Rachel de Queiroz Ferreira Rodrigues
synocta Meso abutment for cement-retained restorations PROSTHETICS Step-by-step instructions
 synocta Meso abutment for cement-retained restorations PROSTHETICS Step-by-step instructions INTRODUCTION synocta Meso abutment for cement-retained restorations 1 The synocta Meso abutments, available
synocta Meso abutment for cement-retained restorations PROSTHETICS Step-by-step instructions INTRODUCTION synocta Meso abutment for cement-retained restorations 1 The synocta Meso abutments, available
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Astra Tech Implant System. Scientific Summary
 Astra Tech Implant System Scientific Summary Why we do what we do? Our vision of a world where everyone eats, speaks and smiles with confidence permeates and inspires everything we do. We believe in an
Astra Tech Implant System Scientific Summary Why we do what we do? Our vision of a world where everyone eats, speaks and smiles with confidence permeates and inspires everything we do. We believe in an
Screw retained implant crown restoration with digital workflow using scan body and surgical guide
 Dr. Anthony Mak W Dental Screw retained implant crown restoration with digital workflow using scan body and surgical guide Solutions featured: 3Shape TRIOS 3Shape Implant Studio 3Shape scan bodies 3Shape
Dr. Anthony Mak W Dental Screw retained implant crown restoration with digital workflow using scan body and surgical guide Solutions featured: 3Shape TRIOS 3Shape Implant Studio 3Shape scan bodies 3Shape
INTRODUCTION MATERIAL AND METHODS
 Original Research Loss of Interdental Crestal Bone Comparison Following Immediate and Delayed Loading after Delayed Placement of Dental Implants in Mandible - A Clinical Study Potharaju Santhi Priya 1,
Original Research Loss of Interdental Crestal Bone Comparison Following Immediate and Delayed Loading after Delayed Placement of Dental Implants in Mandible - A Clinical Study Potharaju Santhi Priya 1,
Clinical outcome of submerged vs. non-submerged implants placed in fresh extraction sockets
 Luca Cordaro Ferruccio Torsello Mario Roccuzzo Clinical outcome of submerged vs. non-submerged implants placed in fresh extraction sockets Author s affiliations: Luca Cordaro, Ferruccio Torsello, Eastman
Luca Cordaro Ferruccio Torsello Mario Roccuzzo Clinical outcome of submerged vs. non-submerged implants placed in fresh extraction sockets Author s affiliations: Luca Cordaro, Ferruccio Torsello, Eastman
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Complication incidence of two implant systems up to six years: a comparison between internal and external connection implants
 Complication incidence of two implant systems up to six years: a comparison between internal and external connection implants Sung-Wook Chae 1, Young-Sung Kim 1,2, Yong-Moo Lee 3, Won-Kyung Kim 1, Young-Kyoo
Complication incidence of two implant systems up to six years: a comparison between internal and external connection implants Sung-Wook Chae 1, Young-Sung Kim 1,2, Yong-Moo Lee 3, Won-Kyung Kim 1, Young-Kyoo
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH
 JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
THE PROSTHETIC VALUE OF THE TEETH ACCORDING TO THEIR PERIODONTAL ATTACHMENT LEVEL
 THE PROSTHETIC VALUE OF THE TEETH ACCORDING TO THEIR PERIODONTAL ATTACHMENT LEVEL Nicoleta Ioanid 1, Gabriela Ifteni, Irina Grădinaru 2, Silvia Mârțu 1, Oana Țănculescu 1 1 Gr. T. Popa" U.M.Ph. - Iași,
THE PROSTHETIC VALUE OF THE TEETH ACCORDING TO THEIR PERIODONTAL ATTACHMENT LEVEL Nicoleta Ioanid 1, Gabriela Ifteni, Irina Grădinaru 2, Silvia Mârțu 1, Oana Țănculescu 1 1 Gr. T. Popa" U.M.Ph. - Iași,
Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space
 Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
The 2B-3D rule for implant planning, placement and restoration
 IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
Effect of varying horizontal mismatched implants on crestal bone level and peri-implant soft tissue: An in vivo study
 2018; 4(2): 141-148 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2018; 4(2): 141-148 2018 IJADS www.oraljournal.com Received: 05-02-2018 Accepted: 09-03-2018 Dr. Renu Gupta Head of Department, Department
2018; 4(2): 141-148 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2018; 4(2): 141-148 2018 IJADS www.oraljournal.com Received: 05-02-2018 Accepted: 09-03-2018 Dr. Renu Gupta Head of Department, Department
Dental Research Journal
 Dental Research Journal Original Article The influence of thread geometry on biomechanical load transfer to bone: A finite element analysis comparing two implant thread designs Manisha G Herekar, Viraj
Dental Research Journal Original Article The influence of thread geometry on biomechanical load transfer to bone: A finite element analysis comparing two implant thread designs Manisha G Herekar, Viraj
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Comparative study of single-thread, double-thread, and triple-thread dental implant: a three-dimensional finite element analysis
 ISSN 1 746-7233, England, UK World Journal of Modelling and Simulation Vol. 3 (2007) No. 4, pp. 310-314 Comparative study of single-thread, double-thread, and triple-thread dental implant: a three-dimensional
ISSN 1 746-7233, England, UK World Journal of Modelling and Simulation Vol. 3 (2007) No. 4, pp. 310-314 Comparative study of single-thread, double-thread, and triple-thread dental implant: a three-dimensional
From planning to surgery: a totally digital working flow for Leone implants placement
 Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran
 Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
Mandibular ridge changes after adaptation. An issue of shortened dental arch to be considered from changes of soft tissues after unattended tooth loss
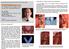 (Journal of Dental Outlook, Vol.110, Vol.6:1021~1027, Japan 2007. An issue of shortened dental arch to be considered from changes of soft tissues after unattended tooth loss Dr. Jiro Abe Abe Dental Clinic
(Journal of Dental Outlook, Vol.110, Vol.6:1021~1027, Japan 2007. An issue of shortened dental arch to be considered from changes of soft tissues after unattended tooth loss Dr. Jiro Abe Abe Dental Clinic
An osseointegrated oral implant is characterized
 Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs
 Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs Douglas Deporter, DDS, PhD 1 /Arwa Al-Sayyed, DDS, MSc 2 /Robert M. Pilliar, BSc, PhD 1 /Nancy
Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs Douglas Deporter, DDS, PhD 1 /Arwa Al-Sayyed, DDS, MSc 2 /Robert M. Pilliar, BSc, PhD 1 /Nancy
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Ankylos. Scientific Summary
 Ankylos Scientific Summary Implanting TissueCare For over 25 years, the Ankylos implant system stands for stable, long-term esthetics. The results from numerous publications and long-term clinical experience
Ankylos Scientific Summary Implanting TissueCare For over 25 years, the Ankylos implant system stands for stable, long-term esthetics. The results from numerous publications and long-term clinical experience
Paper submission. Denture repair with the application of a magnetic attachment to the inner crown of a telescopic crown: A 3-year follow-up case
 Paper submission Denture repair with the application of a magnetic attachment to the inner crown of a telescopic crown: A 3-year follow-up case A. Izumida Department of Comprehensive Dentistry, Tohoku
Paper submission Denture repair with the application of a magnetic attachment to the inner crown of a telescopic crown: A 3-year follow-up case A. Izumida Department of Comprehensive Dentistry, Tohoku
Dental Implant Treatment Planning and Restorative Considerations
 Dental Implant Treatment Planning and Restorative Considerations Aldo Leopardi, BDS, DDS, MS Practice Limited to Implant, Fixed and Removable Prosthodontics Greenwood Village, Colorado www.knowledgefactoryco.com
Dental Implant Treatment Planning and Restorative Considerations Aldo Leopardi, BDS, DDS, MS Practice Limited to Implant, Fixed and Removable Prosthodontics Greenwood Village, Colorado www.knowledgefactoryco.com
Osteoconductive S.L.A. Surface. Fantastic surface, Bioseal, and Perfect achievement of CMI f ixation.
 Fantastic surface, Bioseal, and Perfect achievement of CMI f ixation. Osteoconductive S.L.A. Surface No residual acid and cytotoxicity were observed in the surface examination. IS-II active Product Catalog
Fantastic surface, Bioseal, and Perfect achievement of CMI f ixation. Osteoconductive S.L.A. Surface No residual acid and cytotoxicity were observed in the surface examination. IS-II active Product Catalog
3D Accuitomo XYZ Slice View Tomograph. Super High-Resolution Images of Region of Interest
 3D Accuitomo XYZ Slice View Tomograph. Super High-Resolution Images of Region of Interest Thinking ahead. Focused on life. 2 Cone Beam X-Ray CT Imaging X-Ray Tube Imaging Intensifier Imaging Volume Voxel
3D Accuitomo XYZ Slice View Tomograph. Super High-Resolution Images of Region of Interest Thinking ahead. Focused on life. 2 Cone Beam X-Ray CT Imaging X-Ray Tube Imaging Intensifier Imaging Volume Voxel
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
01/05/2014. Background. Minimally invasive tooth extraction. Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry
 Background Remodelling of alveolar bone following extraction Minimally invasive tooth extraction Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry 2 weeks 4 weeks
Background Remodelling of alveolar bone following extraction Minimally invasive tooth extraction Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry 2 weeks 4 weeks
Core build-up using post systems
 Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized Balanced Occlusion
 Med. J. Cairo Univ., Vol. 83, No. 2, June: 93-97, 2015 www.medicaljournalofcairouniversity.net Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized
Med. J. Cairo Univ., Vol. 83, No. 2, June: 93-97, 2015 www.medicaljournalofcairouniversity.net Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Immediate loading in heavy smokers
 case report Immediate loading in heavy smokers Dr Dr Branislav Fatori & Dr Inge Schmitz, Germany Today, numerous implant systems and many modifications thereof are available on the market, and it may be
case report Immediate loading in heavy smokers Dr Dr Branislav Fatori & Dr Inge Schmitz, Germany Today, numerous implant systems and many modifications thereof are available on the market, and it may be
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Case Report Successful Rehabilitation of Partial Edentulous Maxilla and Mandible with New Type of Implants: Molecular Precision Implants
 Case Reports in Medicine, Article ID 307364, 8 pages http://dx.doi.org/10.1155/2014/307364 Case Report Successful Rehabilitation of Partial Edentulous Maxilla and Mandible with New Type of Implants: Molecular
Case Reports in Medicine, Article ID 307364, 8 pages http://dx.doi.org/10.1155/2014/307364 Case Report Successful Rehabilitation of Partial Edentulous Maxilla and Mandible with New Type of Implants: Molecular
T he survival of an implant involves
 KU ET AL IMPLANT DENTISTRY / VOLUME 25, NUMBER 3 2016 1 Explaining the Red Fluorescence Evident on the Surface of Failed Dental Implants: Case Reports Hye-Min Ku, RDH,* Mi-Kyoung Jun, RDH, MSD,* Jee-Hwan
KU ET AL IMPLANT DENTISTRY / VOLUME 25, NUMBER 3 2016 1 Explaining the Red Fluorescence Evident on the Surface of Failed Dental Implants: Case Reports Hye-Min Ku, RDH,* Mi-Kyoung Jun, RDH, MSD,* Jee-Hwan
Since the introduction of osseointegrated dental implants
 CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
The patient gave a history of hypertension and gastritis for which was taking Lacidipine 4mg, Omeprazole 20mg and Simvastatin 40mg.
 A.S. was referred by her general dental practitioner for assessment for possible implant placement to restore the space where her bridge replacing her maxillary central incisors had recently failed. Fig
A.S. was referred by her general dental practitioner for assessment for possible implant placement to restore the space where her bridge replacing her maxillary central incisors had recently failed. Fig
