Commissioning Statement
|
|
|
- Beverley Burns
- 5 years ago
- Views:
Transcription
1 Commissioning Statement Treatment/ device For the treatment of Commissioning position Flash Glucose Monitoring Systems (including Freestyle Libre ) Monitoring glucose levels in adults and children over 4 years of age with type 1 diabetes mellitus. Bradford district and Craven CCG commissions the use of Flash Glucose Monitoring Systems (FGS) for monitoring the level of glucose in interstitial fluid for adults and children with type 1 diabetes mellitus only in the following circumstances: Patients with Type 1 diabetes mellitus and; Aged four and above and; Under specialist care and; Using multiple daily injections of insulin, or insulin pump therapy, Whom the specialist considers the use of the device will be cost- effective and; Meets one or more of the following criteria: Meet current NICE criteria for insulin pump therapy (HbA1c 69.4 mmol/mol (8.5%) or disabling hypoglycaemia as described in NICE TA151) where a successful trial of a FGS System may avoid the need for pump therapy Recently developed impaired awareness of hypoglycaemia such that there is an inability to detect the onset of hypoglycaemia because of absence of warning symptoms. The individual must also demonstrate a willingness to engage with further education where applicable and a high level of engagement with glucose testing and management. (Note that for persistent hypoglycaemia unawareness, NICE recommends continuous glucose monitoring with alarms and FGS do not currently have this function). Two or more admissions to hospital per year with diabetic ketoacidosis or hypoglycaemia Patients or carer of a patient who have considerable difficulties in finger prick testing due to physical or mental health limitations Patients or carer of a patient with functional impairment that impacts on their ability to interpret standard finger prick testing results Reluctance to carry out finger prick testing (e.g. due to distress or inconvenience) alone is not considered to be criteria qualifying the use of FGS.
2 The FGS System will be provided initially on a 6 month trial basis. The decision to continue will be made by the diabetes specialist team only if one or more of the following are demonstrated: A demonstrable reduction in usage of blood glucose test strips. It is noted that patients will still continue to do extra tests to fulfil DVLA requirements. It is also noted that patients with smart meters and bolus calculators will continue to do regular blood glucose testing. However a demonstrable reduction in usage of strips will still be expected. (Trial data showed a reduction in blood glucose testing to an average of 0.5 times per day in patients using FreeStyle Libre ; however it is acknowledged that more frequent testing may be required in certain circumstances e.g. during periods of illness). Significant reduction in severe/non- severe hypoglycaemia frequency Reversal of impaired awareness of hypoglycaemia Significant reduction in episodes of diabetic ketoacidosis Reduction in hospital admissions Where indication is HbA1c >70 mmol/mol then treatment goal is a reduction in HbA1c depending on pre-intervention HbA1c: Pre-FlashGM HbA1c (mmol/mol) Goal HbA1c to continue FlashGM >100 reduce by at least 15 mmol/mol reduce by at least 10 mmol/mol <70 reduce by at least 5 mmol/mol FGS will be provided through the hospital specialist diabetes team only as a RED drug i.e. FreeStyle Libre ; sensors will not be prescribed by general practitioners. All patients (or carers) must be willing to undertake training in the use of FGS Systems. They must commit to regular scans of the device demonstrating evidence of FGS use in self-management, and commit to ongoing regular follow-up and monitoring. They must also agree the expected outcomes with usage and that NHS provision of FGS will be withdrawn if one or more of the above criteria are not met. The diabetes specialist team in secondary care must gain consent from the patient (or patient representative) at the point of initiation of FGS commissioned by the NHS, to permit NHS staff to undertake an audit of data from both the specialist setting and the patient's GP Practice to enable the benefit of initiation and continuation of FGS to be assessed. Secondary care specialist teams are responsible for collecting the audit data at the end of a six month trial from primary and secondary care in order for the commissioning of FGS to continue. The CCG may require data for verification that use is in line with the commissioning policy. After a six month successful trial the ongoing use of FGS in individuals should be reviewed annually by the specialist team to ensure usage continues to be in line with the commissioning criteria.
3 Treatment outcomes must be audited in all patients started on FGS by specialist teams. This audit data will be reviewed regularly by the CCGs and will inform the review of this recommendation twelve months following publication. Adjunct blood testing strips should be prescribed according to locally agreed best value guidelines with an expectation that demand/frequency of supply will be reduced. Use of FGS in patients with Type 2 diabetes mellitus is not currently licensed or commissioned. Patients who are self-funding FGS who do not meet the above criteria for initiation OR continuation will not be entitled to NHS prescriptions. Patients who are self-funding who did meet the criteria for FGS and where it can be demonstrated by their diabetes team that they achieved the criteria for continuation at 6 months will be entitled to receive FGS on an NHS prescription. A clinician can make an Individual Funding Request (IFR) for treatment when a patient does not meet the stated criteria for funding. Funding can only be approved if a case of "exceptional clinical need" has been demonstrated. See individual CCG websites for IFR policies. North Kirklees CCG/Bradford City CCG/Bradford Districts CCG/Greater Huddersfield CCG/Wakefield CCG/Calderdale CCG/Airedale Wharfedale and Craven CCG Date effective from Policy to be reviewed by (to be reviewed earlier if NICE issues guidance at an earlier date) Background information The FGS consists of a sensor worn on the upper arm that measures interstitial glucose every minute and a reader device that is scanned over the sensor to get a result. It can produce a near continuous record of measurements which can be accessed on demand. It can also indicate glucose level trends over time. The FGS is indicated for measuring interstitial fluid glucose levels in people (age 4 and older) with diabetes mellitus. The product is classified as a device and received European CE mark certification in August The sensors may also be read with an appropriate application on a Smart phone which has near-field communication. This new technology helps to reduce the burden of finger prick blood tests but there is not any evidence available as yet as to whether it reduces complications and long-term outcomes for diabetic patients. There is no NICE directive for CCGs to fund this new technology but NICE has undertaken a Medtech innovation briefing [1].
4 Summary of evidence/ rationale The main points from the evidence are from 5 studies involving 700 people [1]. This includes 2 randomised controlled trials; one that includes people with type 1 diabetes (n=241; the IMPACT study) and the other including people with type 2 diabetes (n=224; the REPLACE study) [1]. Three of the studies reported device accuracy compared with self-monitored blood glucose, with results ranging from 84% to 88% accuracy and from 99% to 100% clinical acceptability, using an error grid. One study reported device accuracy and acceptability of 97% to 99% compared with venous blood sampling [1]. Patients using FreeStyle Libre experienced less time in hypoglycaemia than patients using SMBG, averaging 1.24 hours per day (SE 0.24) or 38% less time (p<0.0001) in hypoglycaemia and 1 hour more per day in euglycaemia (p=0.0006). The number of hypoglycaemic events per day reduced by mean of 0.45 (by over 25%; p<0.0001) [1]. The limited data available suggests that using FreeStyle Libre for up to 12 months reduces time spent in hypoglycaemia compared with self-monitoring of blood glucose using finger-prick tests, and reduces the average number of finger-prick blood glucose tests needed [1] There is limited safety data available on the use of the FGS. The only published study carried out by Bailey et al reported there were no unexpected adverse device effects reported during the clinical study. Finger prick capillary blood glucose monitoring is still advised during periods of rapidly changing levels of interstitial glucose when interstitial glucose levels may not accurately reflect blood glucose levels, if hypoglycaemia or impending hypoglycaemia is reported, or the patient s symptoms do not match the system readings. Three of the studies reported device accuracy compared with self-monitored blood glucose. The investigators concluded that interstitial glucose measurements via the FreeStyle Libre system were accurate compared with capillary blood glucose reference values, and this accuracy was maintained over 14 days lifespan of the Freestyle Libre sensor.
5 Cost effectiveness / resource impact: There is currently no UK cost-effectiveness data available for FGS to be able to determine whether this new technology is cost-effective for the NHS. The resource impact depends upon the extent to which improved glucose control through the adoption of FGS translates into fewer complications (hypoglycaemia and the longer term microvascular and macrovascular complications of hyperglycaemia), reduced admissions and reduced use of blood glucose test strips. Impact upon the individual CCGs test strip expenditure will be evaluated further after 12 months. A year s cost of sensors is 910 per patient. The FGS reader is not available on prescription and will be provided free of charge by the manufacturer. Cost of Freestyle Libre (FL) sensors per annum Cost of Cost effective( 9.95 for 50) Blood Glucose Test Strip (BGTS) - 8/day Cost of more expensive( 16 for 50) BGTS 8/day If T1 patient and also using ketone strips / 10 strips If a patient is currently using more expensive strips and tests ketones once per week at 20 per box the annual cost is Therefore, FGS would be cost neutral if testing not more than once per month on ketones and no more than once per day on BGTS and could be cost effective if it reduced BGTS and Ketone strips usage further. However, for a patient using cost effective BGT strips and cost effective ketone strips once per week the cost is 631 FGS would never be cost neutral without additionality.
6 References 1.) FreeStyle Libre for glucose monitoring; Medtech innovation briefing [MIB110] Published date: July Other references used in the development of the policy Regional Medicines Optimisation Committee FreeStyle Libre Position Statement 1 st November 2018: NHS Vale of York and NHS Scarborough and Ryedale CCGs commissioned/ys-position-statement-freestyle-libre-march-2018-final pdf NHS Bath and North East Summerset CCG; NHS Swindon CCG; NHS Wiltshire CCG estyle-libre-flash-glucose-monitoring-cba.pdf Contact for this policy Head of Medicines Management
Commissioning Statement. Flash Glucose Monitoring system (FreeStyle Libre ) March 2018
 Technology Commissioning Statement Flash Glucose Monitoring system (FreeStyle Libre ) March 2018 FreeStyle Libre (Abbott) Flash Glucose Monitoring System for use in adults, young people and children. Recommendation
Technology Commissioning Statement Flash Glucose Monitoring system (FreeStyle Libre ) March 2018 FreeStyle Libre (Abbott) Flash Glucose Monitoring System for use in adults, young people and children. Recommendation
NHS GG&C Introduction of Freestyle Libre flash glucose monitoring system
 NHS GG&C Introduction of Freestyle Libre flash glucose monitoring system The Freestyle Libre flash glucose monitoring system is a sensor based, factory-calibrated system that measures interstitial fluid
NHS GG&C Introduction of Freestyle Libre flash glucose monitoring system The Freestyle Libre flash glucose monitoring system is a sensor based, factory-calibrated system that measures interstitial fluid
Placename CCG. Policies for the Commissioning of Healthcare
 Placename CCG Policies for the Commissioning of Healthcare Policy for the Provision of Continuous Glucose Monitoring and Flash Glucose Monitoring to patients with Diabetes Mellitus. This document is part
Placename CCG Policies for the Commissioning of Healthcare Policy for the Provision of Continuous Glucose Monitoring and Flash Glucose Monitoring to patients with Diabetes Mellitus. This document is part
THE SHEFFIELD AREA PRESCRIBING GROUP. Position Statement for Prescribing of Freestyle Libre In Type 1 Diabetes. Date: March 2018.
 THE SHEFFIELD AREA PRESCRIBING GROUP Position Statement for Prescribing of Freestyle Libre In Type 1 Diabetes Date: March 2018 Overview Freestyle Libre is a flash glucose sensor device that measures *interstitial
THE SHEFFIELD AREA PRESCRIBING GROUP Position Statement for Prescribing of Freestyle Libre In Type 1 Diabetes Date: March 2018 Overview Freestyle Libre is a flash glucose sensor device that measures *interstitial
NHS Leeds CCG. Policy for the Funding of Flash Glucose Monitoring (FlashGM) in Paediatrics and Adults
 NHS Leeds CCG Policy for the Funding of Flash Glucose Monitoring (FlashGM) in Paediatrics and Adults Produced by: Jo Alldred, Medicines Effectiveness Lead, NHS Leeds CCG Dr Bryan Power, Long Term Conditions
NHS Leeds CCG Policy for the Funding of Flash Glucose Monitoring (FlashGM) in Paediatrics and Adults Produced by: Jo Alldred, Medicines Effectiveness Lead, NHS Leeds CCG Dr Bryan Power, Long Term Conditions
Commissioning Policy
 Commissioning Policy Abbott FreeStyle Libre Flash Glucose Monitoring System Individual Funding Request Date Adopted: 09 September 2018 Version: 1819.1.02 Title of document: Authors job title(s): Document
Commissioning Policy Abbott FreeStyle Libre Flash Glucose Monitoring System Individual Funding Request Date Adopted: 09 September 2018 Version: 1819.1.02 Title of document: Authors job title(s): Document
FreeStyle Libre for glucose monitoring: Interim Position Statement for GPs & Patient FAQ
 North Central London Joint Formulary Committee FreeStyle Libre for glucose monitoring: Interim Position Statement for GPs & Patient FAQ GPs should not prescribe FreeStyle Libre sensors on the NHS until
North Central London Joint Formulary Committee FreeStyle Libre for glucose monitoring: Interim Position Statement for GPs & Patient FAQ GPs should not prescribe FreeStyle Libre sensors on the NHS until
Policy for the Provision of Continuous Glucose Monitoring and Flash Glucose Monitoring to patients with Diabetes Mellitus
 Policy for the Provision of Continuous Glucose Monitoring and Flash Glucose Monitoring to patients with Diabetes Mellitus Version No. Changes Made Version of 05.10.2018 V1 Policy ratified by Healthier
Policy for the Provision of Continuous Glucose Monitoring and Flash Glucose Monitoring to patients with Diabetes Mellitus Version No. Changes Made Version of 05.10.2018 V1 Policy ratified by Healthier
Implementation of Freestyle Libre prescribing guidance across the NHS in London
 Implementation of FreeStyle Libre prescribing guidance across the NHS in London Contents Section 1 Background to the document (pages 2-5) Section 2 Implementation guidance pathways 1. Recommended implementation
Implementation of FreeStyle Libre prescribing guidance across the NHS in London Contents Section 1 Background to the document (pages 2-5) Section 2 Implementation guidance pathways 1. Recommended implementation
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) JAPC Briefing FreeStyle Libre
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) JAPC Briefing FreeStyle Libre JAPC has classified Freestyle Libre as BROWN after diabetes consultant/specialist initiation within a Derbyshire diabetes
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) JAPC Briefing FreeStyle Libre JAPC has classified Freestyle Libre as BROWN after diabetes consultant/specialist initiation within a Derbyshire diabetes
In keeping with the Scottish Diabetes Group criteria, use should be restricted to those who:
 Advice Statement 009-18 July 2018 Advice Statement What is the clinical and cost effectiveness of Freestyle Libre flash glucose monitoring for patients with diabetes mellitus treated with intensive insulin
Advice Statement 009-18 July 2018 Advice Statement What is the clinical and cost effectiveness of Freestyle Libre flash glucose monitoring for patients with diabetes mellitus treated with intensive insulin
Policy for Continuous Glucose Monitoring for Type 1 Diabetic Paediatric Patients (<18 years of age)
 Policy for Continuous Glucose Monitoring for Type 1 Diabetic Paediatric Patients (
Policy for Continuous Glucose Monitoring for Type 1 Diabetic Paediatric Patients (
Flash Glucose Monitoring (Flash GM) Frequently asked questions (November 2018)
 Flash Glucose Monitoring (Flash GM) Frequently asked questions (November 2018) What is Flash Glucose Monitoring (Flash GM)? Flash glucose monitoring is a small sensor that you wear on your skin (usually
Flash Glucose Monitoring (Flash GM) Frequently asked questions (November 2018) What is Flash Glucose Monitoring (Flash GM)? Flash glucose monitoring is a small sensor that you wear on your skin (usually
medicines_management/correspondence/pathway-for-the-managed- Access-of-FreeStyle-Libre.
 Pathway for the Managed Access of FreeStyle Libre (Flash Glucose monitoring) for Adults and Children in the care of Trust Specialist Diabetes Clinics in Northern Ireland www.hscboard.hscni.net/download/publications/pharmacy_and_
Pathway for the Managed Access of FreeStyle Libre (Flash Glucose monitoring) for Adults and Children in the care of Trust Specialist Diabetes Clinics in Northern Ireland www.hscboard.hscni.net/download/publications/pharmacy_and_
Placename CCG. Policies for the Commissioning of Healthcare
 Placename CCG Policies for the Commissioning of Healthcare Policy for the funding of insulin pumps and continuous glucose monitoring devices for patients with diabetes 1 Introduction 1.1 This document
Placename CCG Policies for the Commissioning of Healthcare Policy for the funding of insulin pumps and continuous glucose monitoring devices for patients with diabetes 1 Introduction 1.1 This document
Description of the technology
 Advice Note 2017/ 001 What is the clinical effectiveness, safety and budget impact of the Freestyle Libre System compared with current glucose monitoring methods for people aged 4 years and over with diabetes
Advice Note 2017/ 001 What is the clinical effectiveness, safety and budget impact of the Freestyle Libre System compared with current glucose monitoring methods for people aged 4 years and over with diabetes
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus
 Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS)
 Type 2 Diabetes DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Clinical Guideline Self-monitoring of blood glucose (SMBG) should be considered but not be routinely offered for adults with type 2 diabetes
Type 2 Diabetes DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Clinical Guideline Self-monitoring of blood glucose (SMBG) should be considered but not be routinely offered for adults with type 2 diabetes
Healthcare professionals involved in care of children and young people with Type 1 Diabetes Mellitus. Children and young people with diabetes mellitus
 ssociation of Children s Diabetes Clinical Guideline A Practical Approach to the Management of Continuous Glucose Monitoring (CGM) / Real-Time Flash Glucose Scanning (FGS) in Type 1 Diabetes Mellitus in
ssociation of Children s Diabetes Clinical Guideline A Practical Approach to the Management of Continuous Glucose Monitoring (CGM) / Real-Time Flash Glucose Scanning (FGS) in Type 1 Diabetes Mellitus in
Healthcare professionals involved in care of children and young people with Type 1 Diabetes Mellitus
 Clinical Guideline A Practical Approach to the Management of Continuous Glucose Monitoring (CGM) / Real-Time Flash Glucose Scanning (FGS) in Type 1 Diabetes Mellitus in Children and Young People Under
Clinical Guideline A Practical Approach to the Management of Continuous Glucose Monitoring (CGM) / Real-Time Flash Glucose Scanning (FGS) in Type 1 Diabetes Mellitus in Children and Young People Under
DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS)
 DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Type 2 Diabetes Clinical Guideline Self-monitoring of blood glucose (SMBG) should be considered but not routinely offered for adults with type 2 diabetes
DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Type 2 Diabetes Clinical Guideline Self-monitoring of blood glucose (SMBG) should be considered but not routinely offered for adults with type 2 diabetes
Commissioning Policy Individual Funding Request
 Commissioning Policy Individual Funding Request Continuous Glucose Monitors Prior Approval Policy Date Adopted: 13 October 2017 Version: 1718.2 Document Control Title of document Continuous Glucose Monitors
Commissioning Policy Individual Funding Request Continuous Glucose Monitors Prior Approval Policy Date Adopted: 13 October 2017 Version: 1718.2 Document Control Title of document Continuous Glucose Monitors
Agenda Item 10 - Glucose Monitoring Device for Individuals with Diabetes
 Dorset Health Scrutiny Committee 17 October 2018 Public Participation Agenda Item 10 - Glucose Monitoring Device for Individuals with Diabetes Questions 1. Rosie and Kirsty Edwardes, Bridport Residents
Dorset Health Scrutiny Committee 17 October 2018 Public Participation Agenda Item 10 - Glucose Monitoring Device for Individuals with Diabetes Questions 1. Rosie and Kirsty Edwardes, Bridport Residents
DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS)
 Type 2 Diabetes DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Clinical Guideline Self-monitoring of blood glucose should be offered to all newly diagnosed type 2 diabetic patients as an integral part
Type 2 Diabetes DIABETES BLOOD GLUCOSE MONITORING AT HOME (ADULTS) Clinical Guideline Self-monitoring of blood glucose should be offered to all newly diagnosed type 2 diabetic patients as an integral part
Implementation of Flash Glucose Monitoring
 Equality Analysis (Health Inequalities, Human Rights, Social Value) Implementation of Flash Glucose Monitoring Before completing this equality analysis it is recommended that you: Contact your equality
Equality Analysis (Health Inequalities, Human Rights, Social Value) Implementation of Flash Glucose Monitoring Before completing this equality analysis it is recommended that you: Contact your equality
Guidance for the choice of blood glucose testing meters, strips and lancets
 Guidance for the choice of blood glucose testing meters, strips and lancets This guidance is intended to assist healthcare professionals in their selection of appropriate blood glucose meters and testing
Guidance for the choice of blood glucose testing meters, strips and lancets This guidance is intended to assist healthcare professionals in their selection of appropriate blood glucose meters and testing
Guidance on the Self-Monitoring of Blood Glucose in Adults with Diabetes
 Introduction Guidance on the Self-Monitoring of Blood Glucose in Adults with Diabetes This guideline is designed to offer guidance for primary and secondary care on the use of selfmonitoring of blood glucose
Introduction Guidance on the Self-Monitoring of Blood Glucose in Adults with Diabetes This guideline is designed to offer guidance for primary and secondary care on the use of selfmonitoring of blood glucose
Insulin Pumps and Glucose Monitors in Adults Policy
 Insulin Pumps and Glucose Monitors in Adults Policy Version: 2016-19 Ratified by: NHS Leeds West CCG Assurance Committee on; 16 November 2016 NHS Leeds North CCG Governance on Performance and Risk Committee
Insulin Pumps and Glucose Monitors in Adults Policy Version: 2016-19 Ratified by: NHS Leeds West CCG Assurance Committee on; 16 November 2016 NHS Leeds North CCG Governance on Performance and Risk Committee
COPYRIGHTED MATERIAL. Chapter 1 An Introduction to Insulin Pump Therapy WHAT IS INSULIN PUMP THERAPY?
 Chapter 1 An Introduction to Insulin Pump Therapy This chapter will provide information on what insulin pump therapy is, and how insulin pumps have developed from the early models introduced in the 1970s
Chapter 1 An Introduction to Insulin Pump Therapy This chapter will provide information on what insulin pump therapy is, and how insulin pumps have developed from the early models introduced in the 1970s
Insulin Pumps and Glucose Monitors in Adults, Children and Young People Policy
 Insulin Pumps and Glucose Monitors in Adults, Children and Young People Policy Version: 2017-20 Ratified by: NHS Leeds West CCG Assurance Committee on; 16 November 2016 NHS Leeds North CCG Governance on
Insulin Pumps and Glucose Monitors in Adults, Children and Young People Policy Version: 2017-20 Ratified by: NHS Leeds West CCG Assurance Committee on; 16 November 2016 NHS Leeds North CCG Governance on
Continuous Glucose Monitoring (CGM)/Real-Time Flash Glucose Scanning (FGS) Training for Healthcare Professionals and Patients
 ssociation of Children s Diabetes Continuous Glucose Monitoring (CGM)/Real-Time Flash Glucose Scanning (FGS) Training for Healthcare Professionals and Patients 1 ssociation of Children s Diabetes Contents
ssociation of Children s Diabetes Continuous Glucose Monitoring (CGM)/Real-Time Flash Glucose Scanning (FGS) Training for Healthcare Professionals and Patients 1 ssociation of Children s Diabetes Contents
Country Health SA Local Health Network. Title: Continuous Glucose Monitoring (CGM) and Flash Glucose Monitoring (FGM) Ambulatory Service
 Protocol (Clinical) Title: Continuous Glucose Monitoring (CGM) and Flash Glucose Monitoring (FGM) Ambulatory Service Protocol developed by: CHSALHN Diabetes Service Protocol Sponsor: CHSALHN, Executive
Protocol (Clinical) Title: Continuous Glucose Monitoring (CGM) and Flash Glucose Monitoring (FGM) Ambulatory Service Protocol developed by: CHSALHN Diabetes Service Protocol Sponsor: CHSALHN, Executive
How can I access flash glucose monitoring if I need it? Support pack. This pack will help you to find out more about flash and how you can access it.
 How can I access flash glucose monitoring if I need it? Support pack This pack will help you to find out more about flash and how you can access it. Reviewed March 2019 Introduction Following several major
How can I access flash glucose monitoring if I need it? Support pack This pack will help you to find out more about flash and how you can access it. Reviewed March 2019 Introduction Following several major
Diabetes Subcommittee of PTAC meeting held 3 March (minutes for web publishing)
 Diabetes Subcommittee of PTAC meeting held 3 March 2011 (minutes for web publishing) Diabetes Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology and Therapeutics
Diabetes Subcommittee of PTAC meeting held 3 March 2011 (minutes for web publishing) Diabetes Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology and Therapeutics
Networking for success: A burning platform in Berkshire West
 SERVICE REDESIGN CASE STUDY 1: NOVEMBER 2014 Networking for success: A burning platform in Berkshire West SUMMARY In 2012, four federated CCGs set up a network to redesign diabetes services in Berkshire
SERVICE REDESIGN CASE STUDY 1: NOVEMBER 2014 Networking for success: A burning platform in Berkshire West SUMMARY In 2012, four federated CCGs set up a network to redesign diabetes services in Berkshire
DATE RECEIVED 09/10/2017 SUBJECT Formulary PASSED TO Mary DATE PASSED 09/10/2017 RESPOND BY 27/10/2017 CATEGORY Business FoI NUMBER
 DATE RECEIVED 09/10/2017 SUBJECT Formulary PASSED TO Mary DATE PASSED 09/10/2017 RESPOND BY 27/10/2017 CATEGORY Business FoI NUMBER 2017-404 Question/s to be Answered Can you please provide the following
DATE RECEIVED 09/10/2017 SUBJECT Formulary PASSED TO Mary DATE PASSED 09/10/2017 RESPOND BY 27/10/2017 CATEGORY Business FoI NUMBER 2017-404 Question/s to be Answered Can you please provide the following
Priorities Advisory Committee
 Insulin degludec (Tresiba ) PAC - Insulin degludec (Tresiba ) 2.1 The East of England Priorities Advisory Committee A function of GUIDANCE STATEMENT PAC Recommendations 1. Insulin degludec is NOT recommended
Insulin degludec (Tresiba ) PAC - Insulin degludec (Tresiba ) 2.1 The East of England Priorities Advisory Committee A function of GUIDANCE STATEMENT PAC Recommendations 1. Insulin degludec is NOT recommended
DIABETES PATIENT STRATIFICATION AND TESTING SAVING MONEY, SAVING LIVES
 DIABETES PATIENT STRATIFICATION AND TESTING SAVING MONEY, SAVING LIVES Contents 2 The Rising Cost of Diabetes 5 Implementation 3 P atient Stratification is the Key to Saving Lives and Money 6 M eeting
DIABETES PATIENT STRATIFICATION AND TESTING SAVING MONEY, SAVING LIVES Contents 2 The Rising Cost of Diabetes 5 Implementation 3 P atient Stratification is the Key to Saving Lives and Money 6 M eeting
Diabetes UK Consensus Guideline for Flash Glucose Monitoring
 Diabetes UK Consensus Guideline for Flash Glucose Monitoring Date published Introduction Our recommendations Overview Who is flash glucose monitoring suitable for? What is the clinical evidence for flash
Diabetes UK Consensus Guideline for Flash Glucose Monitoring Date published Introduction Our recommendations Overview Who is flash glucose monitoring suitable for? What is the clinical evidence for flash
A Suite of Enhanced Services for. Prudent Structured Care for Adults with Type 2 Diabetes
 An Enhanced Service for Prudent Structured Care for Adults with Type 2 Diabetes Page 1 A Suite of Enhanced Services for Prudent Structured Care for Adults with Type 2 Diabetes 1. Introduction All practices
An Enhanced Service for Prudent Structured Care for Adults with Type 2 Diabetes Page 1 A Suite of Enhanced Services for Prudent Structured Care for Adults with Type 2 Diabetes 1. Introduction All practices
Audit support for continuous subcutaneous insulin infusion for the treatment of diabetes mellitus (review of technology appraisal guidance 57)
 Audit support for continuous subcutaneous insulin (review of technology appraisal guidance 57) Issue date: 2008 Audit support Continuous subcutaneous insulin infusion for the treatment of diabetes mellitus
Audit support for continuous subcutaneous insulin (review of technology appraisal guidance 57) Issue date: 2008 Audit support Continuous subcutaneous insulin infusion for the treatment of diabetes mellitus
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Continuous subcutaneous insulin infusion for the treatment of diabetes (review) Final scope Appraisal objective To review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Continuous subcutaneous insulin infusion for the treatment of diabetes (review) Final scope Appraisal objective To review
QOF Indicator DM013:
 QOF Indicator DM013: The percentage of patients with diabetes, on the register, who have a record of a dietary review by a suitably competent professional in the preceding 12 months Note: the bold signposts
QOF Indicator DM013: The percentage of patients with diabetes, on the register, who have a record of a dietary review by a suitably competent professional in the preceding 12 months Note: the bold signposts
Diagnostics guidance Published: 12 February 2016 nice.org.uk/guidance/dg21
 Integrated sensor-augmented pump therapy systems for managing blood glucose levels els in type 1 diabetes (the MiniMed Paradigm adigm Veo system and the Vibe and G4 PLATINUM CGM system) Diagnostics guidance
Integrated sensor-augmented pump therapy systems for managing blood glucose levels els in type 1 diabetes (the MiniMed Paradigm adigm Veo system and the Vibe and G4 PLATINUM CGM system) Diagnostics guidance
Blood Glucose monitoring during extra-corporeal renal therapy and plasmapheresis.
 Blood Glucose monitoring during extra-corporeal renal therapy and plasmapheresis. Lead Clinician: Dr. R. Diwakar Implementation date: July 2013 Last updated: August 2017 Last review date: Planned review
Blood Glucose monitoring during extra-corporeal renal therapy and plasmapheresis. Lead Clinician: Dr. R. Diwakar Implementation date: July 2013 Last updated: August 2017 Last review date: Planned review
Commissioning for Outcomes in Diabetes. Joanne Taylor Primary Care Commissioning Manager
 Commissioning for Outcomes in Diabetes Joanne Taylor Primary Care Commissioning Manager Current Diabetes Model in Dudley History and Current Diabetes Pathway Primary Care 46 2 no LIS practices Annual review
Commissioning for Outcomes in Diabetes Joanne Taylor Primary Care Commissioning Manager Current Diabetes Model in Dudley History and Current Diabetes Pathway Primary Care 46 2 no LIS practices Annual review
National Diabetes Inpatient Audit (NaDIA) 2016
 National Diabetes Inpatient Audit (NaDIA) 2016 DIABETES A summary report for people with diabetes and anyone interested in the quality of care for people with diabetes when they stay in hospital. Based
National Diabetes Inpatient Audit (NaDIA) 2016 DIABETES A summary report for people with diabetes and anyone interested in the quality of care for people with diabetes when they stay in hospital. Based
Monitoring in Type 2 Diabetes. Learning Outcomes. Type 2 Diabetes. Senga Hunter Community Diabetes Specialist Nurse
 Monitoring in Type 2 Diabetes Senga Hunter Community Diabetes Specialist Nurse Learning Outcomes Understand why blood monitoring is necessary Understand the blood tests for monitoring diabetes Understand
Monitoring in Type 2 Diabetes Senga Hunter Community Diabetes Specialist Nurse Learning Outcomes Understand why blood monitoring is necessary Understand the blood tests for monitoring diabetes Understand
Blood Glucose Level (BGL) greater than or equal to 15.0 mmol/l
 DIABETES ACTION PLAN 2019 EARLY CHILDHOOD SETTINGS Use in conjunction with Diabetes Management Plan. This plan should be reviewed every year. Twice daily injections LOW Hypoglycaemia (Hypo) Blood Glucose
DIABETES ACTION PLAN 2019 EARLY CHILDHOOD SETTINGS Use in conjunction with Diabetes Management Plan. This plan should be reviewed every year. Twice daily injections LOW Hypoglycaemia (Hypo) Blood Glucose
This Diabetes Policy should be read in conjunction with the Dealing with Medical Conditions Policy of Goulburn Region Preschool Association Inc.
 DIABETES POLICY Mandatory Quality Area 2 The content of this policy was developed for KPV by advocacy and diabetes educators at Diabetes Australia Vic and the Royal Children s Hospital Melbourne s manager
DIABETES POLICY Mandatory Quality Area 2 The content of this policy was developed for KPV by advocacy and diabetes educators at Diabetes Australia Vic and the Royal Children s Hospital Melbourne s manager
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE GUIDANCE EXECUTIVE (GE)
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE GUIDANCE EXECUTIVE (GE) Review of TA151 Continuous subcutaneous insulin infusion for the treatment of diabetes mellitus This guidance was issued in
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE GUIDANCE EXECUTIVE (GE) Review of TA151 Continuous subcutaneous insulin infusion for the treatment of diabetes mellitus This guidance was issued in
West Yorkshire & Harrogate Health and Care Partnership
 West Yorkshire & Harrogate Health and Care Partnership Engagement mapping on the communication needs for people with a sensory impairment November 2017 1.0 Introduction The purpose of the report is to
West Yorkshire & Harrogate Health and Care Partnership Engagement mapping on the communication needs for people with a sensory impairment November 2017 1.0 Introduction The purpose of the report is to
National Paediatric Diabetes Audit
 National Paediatric Diabetes Audit Parent and Carers Report 2015-16 Commissioned by the Healthcare Quality Improvement Partnership Managed by the Royal College of Paediatrics and Child Health National
National Paediatric Diabetes Audit Parent and Carers Report 2015-16 Commissioned by the Healthcare Quality Improvement Partnership Managed by the Royal College of Paediatrics and Child Health National
Quick Reference Guide
 FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the Interactive Tutorial. The Quick Reference Guide
FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the Interactive Tutorial. The Quick Reference Guide
People with type 1 diabetes and Do It Yourself (DIY) technology solutions ABOUT THIS POSITION STATEMENT
 Position Statement People with type 1 diabetes and Do It Yourself (DIY) technology solutions ABOUT THIS POSITION STATEMENT Diabetes Australia believes that people with diabetes should have choice and access
Position Statement People with type 1 diabetes and Do It Yourself (DIY) technology solutions ABOUT THIS POSITION STATEMENT Diabetes Australia believes that people with diabetes should have choice and access
APPLICATION FOR SUBSIDY BY SPECIAL AUTHORITY
 APPLICANT (stamp sticker acceptable) Page 1 Fm SA1603 Insulin Pumps INITIAL APPLICATION - permanent neonatal diabetes Applications only from a relevant specialist nurse practitioner. Approvals valid f
APPLICANT (stamp sticker acceptable) Page 1 Fm SA1603 Insulin Pumps INITIAL APPLICATION - permanent neonatal diabetes Applications only from a relevant specialist nurse practitioner. Approvals valid f
Guidance on the Self-Monitoring of Blood Glucose in Adults with Diabetes
 Introduction Guidance on the Self-Monitoring of Blood Glucose in Adults with Diabetes This guideline is designed to offer guidance for primary and secondary care on the use of selfmonitoring of blood glucose
Introduction Guidance on the Self-Monitoring of Blood Glucose in Adults with Diabetes This guideline is designed to offer guidance for primary and secondary care on the use of selfmonitoring of blood glucose
Commissioning Living with and Beyond Cancer in Yorkshire and Humber; an Overview.
 Commissioning Living with and Beyond Cancer in Yorkshire and Humber; an Overview. Document Title An Overview of Commissioning Living with and Beyond Cancer in Yorkshire and Humber Version number: 1 First
Commissioning Living with and Beyond Cancer in Yorkshire and Humber; an Overview. Document Title An Overview of Commissioning Living with and Beyond Cancer in Yorkshire and Humber Version number: 1 First
Regional Medicines Optimisation Committee (North)
 Present: Regional Medicines Optimisation Committee (North) October 26 th 2017 Minutes Quarry House, Leeds 10:00-1:00 pm Name Title Organisation Jun Oct Dr Mike Prentice (MP) Chair Michele Cossey (MC) Dr
Present: Regional Medicines Optimisation Committee (North) October 26 th 2017 Minutes Quarry House, Leeds 10:00-1:00 pm Name Title Organisation Jun Oct Dr Mike Prentice (MP) Chair Michele Cossey (MC) Dr
Community alcohol detoxification in primary care
 Community alcohol detoxification in primary care 1. Purpose The purpose of this primary care enhanced service is to improve the health and quality of life of people whose health may be compromised by their
Community alcohol detoxification in primary care 1. Purpose The purpose of this primary care enhanced service is to improve the health and quality of life of people whose health may be compromised by their
UvA-DARE (Digital Academic Repository) The artificial pancreas Kropff, J. Link to publication
 UvA-DARE (Digital Academic Repository) The artificial pancreas Kropff, J. Link to publication Citation for published version (APA): Kropff, J. (2017). The artificial pancreas: From logic to life General
UvA-DARE (Digital Academic Repository) The artificial pancreas Kropff, J. Link to publication Citation for published version (APA): Kropff, J. (2017). The artificial pancreas: From logic to life General
Outcomes of diabetes care in England and Wales. A summary of findings from the National Diabetes Audit : Complications and Mortality reports
 Outcomes of diabetes care in England and Wales A summary of findings from the National Diabetes Audit 2015 16: Complications and Mortality reports About this report This report is for people with diabetes
Outcomes of diabetes care in England and Wales A summary of findings from the National Diabetes Audit 2015 16: Complications and Mortality reports About this report This report is for people with diabetes
Quick Reference Guide
 FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the Interactive Tutorial. The Quick Reference Guide
FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the Interactive Tutorial. The Quick Reference Guide
Blood Glucose Level (BGL) greater than or equal to 15.0 mmol/l
 DIABETES ACTION PLAN 2019 SCHOOL SETTING Use in conjunction with Diabetes Management Plan. This plan should be reviewed every year. Multiple daily injections LOW Hypoglycaemia (Hypo) Blood Glucose Level
DIABETES ACTION PLAN 2019 SCHOOL SETTING Use in conjunction with Diabetes Management Plan. This plan should be reviewed every year. Multiple daily injections LOW Hypoglycaemia (Hypo) Blood Glucose Level
June 2016 Review: June 2019
 BEDFORDSHIRE & LUTON JOINT PRESCRIBING COMMITTEE June 2016 Review: June 2019 Bulletin 241 : Guidelines on self-monitoring of blood glucose (SMBG) in non-insulin treated Type 2 diabetic patients for maintaining
BEDFORDSHIRE & LUTON JOINT PRESCRIBING COMMITTEE June 2016 Review: June 2019 Bulletin 241 : Guidelines on self-monitoring of blood glucose (SMBG) in non-insulin treated Type 2 diabetic patients for maintaining
Executive Summary Management of Type 1 Diabetes Mellitus during illness in children and young people under 18 years (Sick Day Rules)
 Executive Summary Management of Type 1 Diabetes Mellitus during illness in children and young people under 18 years (Sick Day Rules) SETTING FOR STAFF PATIENTS Medical and nursing staff Children and young
Executive Summary Management of Type 1 Diabetes Mellitus during illness in children and young people under 18 years (Sick Day Rules) SETTING FOR STAFF PATIENTS Medical and nursing staff Children and young
Consultation Group: Dr Amalia Mayo, Paediatric Consultant. Review Date: March Uncontrolled when printed. Version 2. Executive Sign-Off
 Policy For The Adjustment Of Insulin Injections By Paediatric Diabetes Specialist Nurses/Community Paediatric Nurses Diabetes Working With Children Within NHS Grampian Co-ordinators: Lead Paediatric Diabetes
Policy For The Adjustment Of Insulin Injections By Paediatric Diabetes Specialist Nurses/Community Paediatric Nurses Diabetes Working With Children Within NHS Grampian Co-ordinators: Lead Paediatric Diabetes
EFFECTIVE SHARE CARE AGREEMENT. FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY
 Specialist details Patient identifier Name Tel: EFFECTIVE SHARE CARE AGREEMENT FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY The aim of Effective Shared Care Guidelines
Specialist details Patient identifier Name Tel: EFFECTIVE SHARE CARE AGREEMENT FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY The aim of Effective Shared Care Guidelines
Technology appraisal guidance Published: 27 March 2019 nice.org.uk/guidance/ta572
 Ertugliflozin as monotherapy or with metformin for treating type 2 diabetes Technology appraisal guidance Published: 27 March 2019 nice.org.uk/guidance/ta572 NICE 2019. All rights reserved. Subject to
Ertugliflozin as monotherapy or with metformin for treating type 2 diabetes Technology appraisal guidance Published: 27 March 2019 nice.org.uk/guidance/ta572 NICE 2019. All rights reserved. Subject to
New NICE guidance: Changes in practice for multidisciplinary teams. Part 1: Type 1 diabetes in children and young people
 Article New NICE guidance: Changes in practice for multidisciplinary teams. Part 1: Type 1 diabetes in children and young people Helen Thornton This is the first of two articles on the 2015 NICE NG18 guideline,
Article New NICE guidance: Changes in practice for multidisciplinary teams. Part 1: Type 1 diabetes in children and young people Helen Thornton This is the first of two articles on the 2015 NICE NG18 guideline,
GDm-Health is free to download and use. Its use may result in efficiency savings from reducing face-to-face clinic appointments.
 pat hways Health app: GDm-Health for people with gestational diabetes Medtech innovation briefing Published: 13 November 2017 nice.org.uk/guidance/mib131 Summary About this app GDm-Health is a health application
pat hways Health app: GDm-Health for people with gestational diabetes Medtech innovation briefing Published: 13 November 2017 nice.org.uk/guidance/mib131 Summary About this app GDm-Health is a health application
Type 2 Diabetes Recommended SMBG
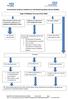 Herefordshire Diabetes Guideline for Self-Monitoring Blood Glucose (SMBG) Type 2 Diabetes Recommended SMBG Diet controlled/ metformin only/ combination of metformin and pioglitazone/dpp4/sglt2 or GLP1
Herefordshire Diabetes Guideline for Self-Monitoring Blood Glucose (SMBG) Type 2 Diabetes Recommended SMBG Diet controlled/ metformin only/ combination of metformin and pioglitazone/dpp4/sglt2 or GLP1
CONTINUOUS GLUCOSE MONITORING POLICY INDIVIDUAL FUNDING
 CONTINUOUS GLUCOSE MONITORING POLICY INDIVIDUAL FUNDING Version: 1718.v1 Recommendation by: Somerset CCG Clinical Commissioning Policy Forum (CCPF) Date Ratified: 12 July 2017 Name of Originator/Author:
CONTINUOUS GLUCOSE MONITORING POLICY INDIVIDUAL FUNDING Version: 1718.v1 Recommendation by: Somerset CCG Clinical Commissioning Policy Forum (CCPF) Date Ratified: 12 July 2017 Name of Originator/Author:
Shaping Diabetes Services in Southern Derbyshire. A vision for Diabetes Services For Southern Derbyshire CCG
 Shaping Diabetes Services in Southern Derbyshire A vision for Diabetes Services For Southern Derbyshire CCG Vanessa Vale Commissioning Manager September 2013 Contents 1. Introduction 3 2. National Guidance
Shaping Diabetes Services in Southern Derbyshire A vision for Diabetes Services For Southern Derbyshire CCG Vanessa Vale Commissioning Manager September 2013 Contents 1. Introduction 3 2. National Guidance
Glucometers Gastrostomy Tubes Nasogastric Tubes Insulin pumps Continuous Glucose monitoring system Closed Loop Smart phones/tablets
 Devices Glucometers Gastrostomy Tubes Nasogastric Tubes Insulin pumps Continuous Glucose monitoring system Closed Loop Smart phones/tablets Accuracy Glucometers The ISO (International Organization for
Devices Glucometers Gastrostomy Tubes Nasogastric Tubes Insulin pumps Continuous Glucose monitoring system Closed Loop Smart phones/tablets Accuracy Glucometers The ISO (International Organization for
Quick Reference Guide
 FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide FreeStyle LibreLink app A FreeStyle Libre product IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the
FLASH GLUCOSE MONITORING SYSTEM Quick Reference Guide FreeStyle LibreLink app A FreeStyle Libre product IMPORTANT USER INFORMATION Before you use your System, review all the product instructions and the
FLIPS FreeStyle Libre in Pregnancy Study
 FLIPS FreeStyle Libre in Pregnancy Study Evaluation of the Accuracy of the FreeStyle Libre Flash Glucose Monitoring System Use in Pregnancy Label Extension Study (CE) Section 1: PARTICIPANT INFORMATION
FLIPS FreeStyle Libre in Pregnancy Study Evaluation of the Accuracy of the FreeStyle Libre Flash Glucose Monitoring System Use in Pregnancy Label Extension Study (CE) Section 1: PARTICIPANT INFORMATION
Medicines and Technologies Programme Adoption Scoping Report MTG315 Peristeen
 Medicines and Technologies Programme Adoption Scoping Report MTG315 Peristeen SUMMARY for MTAC1 meeting Contributors questioned why NICE are writing guidance on this system alone when it is viewed and
Medicines and Technologies Programme Adoption Scoping Report MTG315 Peristeen SUMMARY for MTAC1 meeting Contributors questioned why NICE are writing guidance on this system alone when it is viewed and
GUIDELINE FOR SELF MONITORING OF BLOOD GLUCOSE IN ADULTS WITH DIABETES
 It is recognised that self- monitoring of blood glucose (SMBG) may have an important role to play for some patients with. It can allow individuals to see what impact particular behaviours, such as dietary
It is recognised that self- monitoring of blood glucose (SMBG) may have an important role to play for some patients with. It can allow individuals to see what impact particular behaviours, such as dietary
GOVERNING BOARD. Assisted Conception (IVF): Review of access criteria. Date of Meeting 21 January 2015 Agenda Item No 13. Title
 GOVERNING BOARD Date of Meeting 21 January 2015 Agenda Item No 13 Title Assisted Conception (IVF): Review of access criteria Purpose of Paper The SHIP (Southampton, Hampshire, Isle of Wight and Portsmouth)
GOVERNING BOARD Date of Meeting 21 January 2015 Agenda Item No 13 Title Assisted Conception (IVF): Review of access criteria Purpose of Paper The SHIP (Southampton, Hampshire, Isle of Wight and Portsmouth)
PROCEDURE FOR BLOOD GLUCOSE MONITORING
 PROCEDURE FOR BLOOD GLUCOSE MONITORING First Issued Issue Version Two Purpose of Issue/Description of Change Planned Review Date To promote safe and effective blood glucose monitoring using Trust equipment
PROCEDURE FOR BLOOD GLUCOSE MONITORING First Issued Issue Version Two Purpose of Issue/Description of Change Planned Review Date To promote safe and effective blood glucose monitoring using Trust equipment
requesting information regarding prescribing incentive schemes in Canterbury and Coastal Clinical Commissioning Group
 requesting information regarding prescribing incentive schemes in Canterbury and Coastal Clinical Commissioning Group Canterbury and Coastal Clinical Consortium Group Medicine Management plans 2013/14
requesting information regarding prescribing incentive schemes in Canterbury and Coastal Clinical Commissioning Group Canterbury and Coastal Clinical Consortium Group Medicine Management plans 2013/14
Corporate Medical Policy
 Corporate Medical Policy Continuous Monitoring of Glucose in the Interstitial Fluid File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_monitoring_of_glucose_in_the_interstitial_fluid
Corporate Medical Policy Continuous Monitoring of Glucose in the Interstitial Fluid File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_monitoring_of_glucose_in_the_interstitial_fluid
New Clinical Solutions in Diabetes Care
 Welcome to the Lakeside Conference Centre and the New Clinical Solutions Conference 2011 A collaboration: Worldwide 346 million people have diabetes World Health Organisation In 2010 the estimated prevalence
Welcome to the Lakeside Conference Centre and the New Clinical Solutions Conference 2011 A collaboration: Worldwide 346 million people have diabetes World Health Organisation In 2010 the estimated prevalence
DO IT TIPS & TRICKS YOU CAN WITHOUT LANCETS * with FreeStyle Libre FLASH GLUCOSE MONITORING SYSTEM
 FLASH GLUCOSE MONITORING SYSTEM YOU CAN DO IT WITHOUT LANCETS * TIPS & TRICKS with FreeStyle Libre *Scanning the sensor to obtain glucose values does not require lancets. FreeStyle Libre overview 1 The
FLASH GLUCOSE MONITORING SYSTEM YOU CAN DO IT WITHOUT LANCETS * TIPS & TRICKS with FreeStyle Libre *Scanning the sensor to obtain glucose values does not require lancets. FreeStyle Libre overview 1 The
Diabetes in England NHS Medical Directorate. Dr Rowan Hillson MBE National Clinical Director for Diabetes
 Diabetes in England 2010 Dr Rowan Hillson MBE National Clinical Director for Diabetes I strongly believe that Everyone with diabetes deserves the highest standards of personalised diabetes care, no matter
Diabetes in England 2010 Dr Rowan Hillson MBE National Clinical Director for Diabetes I strongly believe that Everyone with diabetes deserves the highest standards of personalised diabetes care, no matter
What is the role of insulin pumps in the modern day care of patients with Type 1 diabetes?
 What is the role of insulin pumps in the modern day care of patients with Type 1 diabetes? Dr. Fiona Wotherspoon Consultant in Diabetes and Endocrinology Dorset County Hospital Fiona.Wotherspoon@dchft.nhs.uk
What is the role of insulin pumps in the modern day care of patients with Type 1 diabetes? Dr. Fiona Wotherspoon Consultant in Diabetes and Endocrinology Dorset County Hospital Fiona.Wotherspoon@dchft.nhs.uk
Advances in Diabetes Care Technologies
 1979 Advances in Diabetes Care Technologies 2015 Introduction Insulin pump use: ~ 20% - 30% of patients with T1DM < 1% of insulin-treated patients with T2DM 2007 FDA estimates ~375,000 insulin pumps for
1979 Advances in Diabetes Care Technologies 2015 Introduction Insulin pump use: ~ 20% - 30% of patients with T1DM < 1% of insulin-treated patients with T2DM 2007 FDA estimates ~375,000 insulin pumps for
NEW TECHNOLOGIES FOR MANAGING DIABETES ANGELA THOMPSON DNP, FNP-C, BC-ADM, CDE, FAANP
 NEW TECHNOLOGIES FOR MANAGING DIABETES ANGELA THOMPSON DNP, FNP-C, BC-ADM, CDE, FAANP No commercial support or sponsorship was received for this project I have nothing to disclose OBJECTIVES Identify at
NEW TECHNOLOGIES FOR MANAGING DIABETES ANGELA THOMPSON DNP, FNP-C, BC-ADM, CDE, FAANP No commercial support or sponsorship was received for this project I have nothing to disclose OBJECTIVES Identify at
CONTINUOUS OR INTERMITTENT GLUCOSE MONITORING IN INTERSTITIAL FLUID
 FLUID Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
FLUID Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
NDSS Helpline
 Continuous GLUCOSE MONITORING A guide to using CGM for children and young people with type 1 diabetes NDSS Helpline 1300 136 588 ndss.com.au The National Diabetes Services Scheme is an initiative of the
Continuous GLUCOSE MONITORING A guide to using CGM for children and young people with type 1 diabetes NDSS Helpline 1300 136 588 ndss.com.au The National Diabetes Services Scheme is an initiative of the
Extract from EFFECTIVE CLINICAL COMMISSIONING POLICIES
 Extract from EFFECTIVE CLINICAL COMMISSIONING POLICIES CBA = criteria based access to treatment PA = prior approval must be obtained from the CCG prior to referral = intervention not normally funded; Individual
Extract from EFFECTIVE CLINICAL COMMISSIONING POLICIES CBA = criteria based access to treatment PA = prior approval must be obtained from the CCG prior to referral = intervention not normally funded; Individual
The management of diabetes
 MEDICINE DIGEST STATINS The management of diabetes should include efforts to prevent, or delay, the onset of cardiovascular disease. Statins have been shown to lower cardiovascular risk in diabetes and
MEDICINE DIGEST STATINS The management of diabetes should include efforts to prevent, or delay, the onset of cardiovascular disease. Statins have been shown to lower cardiovascular risk in diabetes and
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Diabetes in children and young people: diagnosis and management of type 1 and type 2 diabetes in children and young people
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Diabetes in children and young people: diagnosis and management of type 1 and type 2 diabetes in children and young people
