Neuropathy, amyloidosis, and monoclonal gammopathy
|
|
|
- Eileen Richards
- 5 years ago
- Views:
Transcription
1 Journal of Neurology, Neurosurgery, and Psychiatry, 1979, 42, Neuropathy, amyloidosis, and monoclonal gammopathy J. W. FITTING, A. BISCHOFF, F. REGLI, AND G. DE CROUSAZ From the Department of Neurology, CHUV, Lausanne, and the Department of Neurology, Berne University, Berne, Switzerland S U MM AR Y Three cases of neuropathy with monoclonal gammopathy and amyloid deposits in peripheral nerves are described. They appeared to present a benign gammopathy because of the duration of the neuropathy in the absence of any clinical or biological sign of myeloma or macroglobulinaemia. The pathological abnormality found in the sural nerves of the three patients was characterised by a marked loss of myelinated and unmyelinated nerve fibres because of active axonal degeneration with Wallerian degeneration. The most striking feature in all three cases was the finding of deposits identified as an accumulation of microfibrils. Peripheral neuropathy is often associated with malignant gammopathies, such as multiple myeloma and Waldenstrom's macroglobulinaemia. The association between neuropathy and generalised amyloidosis, in the familial or sporadic form, is also well known. We recently observed three cases of neuropathy with monoclonal gammopathy and amyloid deposits in peripheral nerve. Case reports CASE 1 (PB) In 1967, at the age of 60 years, this patient first noticed plantar paraesthesiae and slight weakness of both legs. In 1968, an examination showed distal sensory loss in both legs and arms, and moderate weakness in both legs. In 1969, a monoclonal IgM was found. In 1974, an examination showed distal sensory loss and weakness in upper and lower limbs. Sternal marrow was normal. Treatment with prednisone 60 mg/day, and later 15 mg/day was given from May 1974 and stopped in November 1974, without any clinical modification. In 1977, the patient complained of generalised weakness, pain in the legs, and tremor in action. He noticed no impotence, no orthostatic symptoms, but irregular bowel movements, and absence of perspiration in the hands and feet. Examination showed total areflexia, wasting and Address for reprint requests: Dr J. W. Fitting, Neurology, CHUV, Lausanne, Switzerland. Department of Accepted 13 July 1978 weakness of distal muscles in upper and lower limbs, and sensory loss in a glove and stocking distribution. There was postural tremor of both hands, exaggerated on movement, and ataxia of gait. The skin was dry and there was no orthostatic hypotension. Electromyography in 1976 showed a median nerve conduction velocity of 15 m/s. The lateral and medial popliteal nerves were inexcitable. All the muscles examined showed marked denervation. The ESR was 36 mm/hr, Hb 15.3 g/dl, white blood cells 5500/mm3. Serum electrolytes, glucose, urea, creatinine, uric acid, alkaline phosphatase, cholesterol, total proteins, and bilirubin were in the normal range. Electrophoresis showed a monoclonal immunoglobulin component, shown to be IgM kappa by immunoelectrophoresis. The immunoglobulin levels were: IgM 1045 mg/dl, IgG 690 mg/dl, IgA 71 mg/dl (March, 1976) and IgM 1400 mg/dl, IgG 800 mg/dl, IgA 70 mg/dl (November, 1977). Serum viscosity was CSF protein level was 0.47 g/l. The urine was normal. Sternal marrow was normal, with 23% lymphocytes. A sural nerve biopsy was performed and specimens prepared for light and electronmicroscopic examination. Segments of the nerve were also stained with Congo red, thioflavin T, and periodic acid-schiff reagent (PAS)-in the Department of Neurology, Berne University. Light microscopy on 1 jum thick transverse sections stained with methylene blue showed a 193
2 194 J. W. Fitting, A. BischofJ, F. Regli, and G. de Crousaz severe reduction in the number of the myelinated nerve fibres with virtually complete loss of myelinated nerve fibres of large diameter. The endoneurial intercellular space appeared of increased density, and around two of the endoneurial vessels a cuff of a dark amorphous substance was very striking (Fig. 1). The nerve did not react with the Congo red and thioflavine techniques. Electron microscopy showed that most of the preserved myelin sheaths had a normal lamellar structure. Some features of myelin sheath breakdown indicative of Wallerian degeneration were also present. In about 20% of the axons, including those of unmyelinated nerve fibres, axonal degeneration was obvious. Many Schwann cell processes depleted of axons showed a budded appearance. No onion bulb formation was discernible. In the extracellular space, disseminated accumulations of microfibrils, 10 nm in width, were seen. They were particularly striking in relation to endoneurial vessels, where they were condensed to a felt-like mass (Fig. 2). CASE 2 (MB) In 1969, at the age of 66 years, this patient noticed loss of sensation in his left hand and cramps and paraesthesiae in both hands. Neurological examination was normal. In 1974, he began to complain of difficulties in walking, and pain and weakness of the legs. In 1975 physical examination disclosed G Fig. 1 Case 1. Left: sural nerve from IgM gammopathy, stained with methylene blue. In the transverse section severe 0 oc loss of myelinated nerve fibres is apparent. 0 O Two intraneurial vessels show a cuff of ( an amorphous (dark) mass (arrows). C) i0 i Right: normal sural nerve. Original C magnification X r i'.- Fig. 2 Case 1. Electron micrograph of a cross-sectioned intrafascicular vessel. There is a cuff of a dense substance X around the endothelial cells representing microfibrillar masses (right) indicated by arrows. Original magnification X3900 X (right) X
3 Neuropathy, amyloidosis, and monoclonal gammopathy almost total areflexia and diffuse weakness and sensory loss in the legs. During the next two years, the patient complained of progressive weakness, with inability to walk from April He noticed constipation, impotence, and hoarseness of voice. Examination showed total areflexia and muscle wasting of both hands and legs. There was moderate weakness in upper limbs, marked weakness of the proximal muscles and almost total loss of function of the distal muscles in lower limbs. Touch and pinprick sensation were impaired in glove and stocking distribution. Temperature sensation was absent in hands and legs. Vibratory sensation was reduced in the hands and absent at the ankles. The skin was dry. There was no orthostatic hypotension on rising from supine to sitting position. Six months later, examination showed further loss of function of proximal muscles of the legs. At electromyography in 1975 conduction velocity of various nerves were: median 48 m/s, ulnar 49 m/s, right lateral popliteal 35 m/s, left lateral popliteal 38 m/s. Subacute denervation of muscles of right leg and left hand was observed. In 1977 the conduction velocities were: median nerve 32 m/s, ulnar nerve 49 m/s. Both lateral popliteal nerves were inexcitable. Subacute to chronic denervation was detected in muscles of the right leg and left hand. The ESR was 20 mm/hr, Hb 13.1 g/dl, white cells 4,500/mm3. Serum electrolytes, urea, creatinine, uric acid, alkaline phosphatase, and cholesterol were in the normal range. Fasting blood glucose level was 104 mg/dl (5.2 mmol/l). Provoked hyperglycaemia was in the normal range. Total serum proteins were 5.6 g/dl. Electrophoresis disclosed a monoclonal immunoglobulin component, shown to be IgG lambda by immunoelectrophoresis. Immunoglobulin levels were IgG 1900 mg/dl, IgA 100 mg/dl, IgM 90 mg/dl. Serum viscosity was The CSF contained 1 white cell per mm3. The level of protein was 0.94 g/l with monoclonal IgG. No Bence-Jones protein was found in the urine. Porphobilinogen was elevated, uroporphyrin absent. and coproporphyrin was in the normal range. Sternal marrow was hypocellular, with normal cells of all series; 20% were plasma cells, slightly polymorphic. Sural nerve biopsy was performed and prepared as in case 1. Histological examination showed a severe defect with almost complete loss of myelinated nerve fibres. Endoneurial vessels also showed striking changes with the presence of a poorly defined homogeneous clear substance extending from the vessel wall into the adjacent neural tissue, where the normal fascicular structure appeared more or less effaced (Fig. 3). Electron microscopy clearly displayed the severe loss of myelinated and unmyelinated nerve fibres, with a reduction in number of Schwann cell processes. Many Schwann cell processes appeared budded. Multiple deposits of a material consisting of accumulations of microfibrils typical of amyloid were recognisable within the expanded intercellular spaces (Fig. 4). CASE 3 (HF) In 1974, at the age of 47 years, this patient began to complain of paraesthesiae and dysaesthesiae in both legs. He noticed fatigue and cramps in the legs during walking. These symptoms increased progressively until He complained also of decreased sexual potency. Examination showed a depressed left ankle reflex; other reflexes were present and symmetrical. There was wasting of distal muscles of lower limbs, predominantly on the left side. Muscular function was preserved in the upper limbs but reduced in W., 195 Fig. 3 Case 2. Sural nerve from IgG gammopathy showing the almost complete loss of myelinated nerve fibres. In the centre a homogeneous clear mass.4 represents a diseased vessel (*) from which clear material is infiltrating the neural tissue. Methylene blue. Original magnification X720.
4 196 i'. t- 42t. -, >i& 3 ' 4 ~.-t:. :.@~~~~~~~~. the lower limbs, predominantly on the left side. Touch, pinprick, and temperature sensation were normal in upper and lower limbs. Vibratory sensation was reduced at both ankles, predominantly on the left side. At electromyography conduction velocities of nerves were: median 62 m/s, right lateral popliteal 59 m/s (with irregular potential, 0.5 mv), left lateral popliteal 66 m/s (with prolonged potential, 1 mv, 30 ms), left medial popliteal 48 m/s (with irregular potential, 0.5 mv). Chronic denervation was observed in muscles of the lower limbs, predominantly in the left tibialis anterior. The ESR was 6 mm/hr, Hb 16.3 g/dl, white cells 8700/mm3. Serum electrolytes, glucose, urea, creatinine, uric acid, total proteins, cholesterol, bilirubin, alkaline phosphatase, T3 and T4 were in the normal range. Electrophoresis disclosed a monoclonal immunoglobulin component, shown to be IgG kappa by immunoelectrophoresis. Immunoglobulin levels were: IgG 1200 mg/dl, IgA 210 mg/dl, IgM 110 mg/dl. Serum viscosity was The urine was normal. Sternal marrow was normal, with 20% lymphocytes and 10% well differentiated plasma cells. Sural nerve biopsy showed a virtually complete absence of myelinated nerve fibres. In a small number of nerve fascicles a loosely structured material of moderate density was accumulated circumferentially in a subperineurial location. Electron microscopic analysis revealed the preservation of only a few myelinated nerve fibres of J. W. Fitting, A. Bischoff, F. Regli, and G. de Crousaz... "..Y-...i I-. -! Fig. 4 Case 2. Electron micrograph exhibiting the complete loss of myelinated and unmyelinated axons. Schwann cell processes appear budded. There are four deposits of microfibrillar masses representing amyloid (arrows). Original magnification X5900. small calibre with a myelin sheath of normal ultrastructure (Fig. 5). Axonal degeneration was present in myelinated and unmyelinated nerve fibres. The Schwann cells were markedly reduced in number. rhe intercellular space appeared distended and filled with accumulations of microfibrils in a patchy distribution (Figs. 5 and 6). This material was collected predominantly in the subperineurial space (Fig. 7). Discussion MALIGNANT AND BENIGN MONOCLONAL GAMMOPATHIES Apart from multiple myeloma and Waldenstrom's macroglobulinaemia, production of monoclonal immunoglobulin has been described in healthy subjects and in chronic inflammatory disease. This condition was termed "benign monoclonal hyperglobulinaemia" and considered as a stable nonpremyelomatous state by Waldenstrom (1964). During recent years, malignant and benign monoclonal gammopathies have been classified under the same name as "plasma cell dyscrasias", on the basis of several observations. Monoclonal immunoglobulins of benign gammopathies may belong to any of the immunoglobulin classes, and cannot be distinguished from immunoglobulins of malignant gammopathies (Wintrobe, 1974). Several cases of apparently benign monoclonal gammopathies evolved to multiple myeloma or macroglobulinaemia after a number of years, even after
5 Neuropathy, amyloidosis, and monoclonal gammopathy A. 'i Fig. 5 Case 3 Electron micrograph of the transverse sectioned sural nerve showing a severe depletion of nerve fibres and Schwann cells In the extracellular space, a flaky infiltration by a poorly defined structure is visible Original magnification X d1r i..is ~ ~ 4 ~~~~~~~~~~~~~~~~l K~~~~~~~~~~~o X, ~.D, Fig. 6 Case 3. With high resolution there appear patchy accumulations of microfibrils consistent with amyloid. Original magnification X Fig. 7 Case 3. Electron micrograph of the subperineurial region displaying a finely dispersed infiltration by amyloid fibrils between some thin fibroblastic processes. Original magnification X
6 years of observation (Kyle and Bayrd, 1966; Wintrobe, 1974; Osserman, 1975). However, it is evident that not every benign monoclonal gammopathy progresses to a malignant gammopathy, as the incidence of these two forms is different. The yearly incidence of multiple myeloma is 0.002{0.004%, the incidence of benign monoclonal gammopathies has been estimated from % in adults, and at 3% in subjects over the age of 70 (Wintrobe, 1974; Ameis and Pruzanski, 1976). It is not known whether benign monoclonal gammopathies are precursors of myeloma, which would all progress in this direction if they had enough time, or if these conditions are distinct. For this reason Osserman (1975) does not speak of benign monoclonal gammopathy, but of "plasma cell dyscrasia of unknown significance." We are at the moment unable to predict the evolution of individual cases of benign monoclonal gammopathy. Indeed, if malignant monoclonal gammopathies differ from benign forms in a series of parameters such as a higher level of the monoclonal immunoglobulin, reduced level of other immunoglobulins, serum hyperviscosity, reduced haemoglobin level, and an increased number of plasma cells in the marrow, none of these criteria is absolute and of predictive value in an isolated case (Clauvel et al., 1971; Ritzmann et al., 1975). J. W. Fitting, A. Bischofj, F. Regli, and G. de Crousaz AMYLOID)OSIS AND MONOCLONAL GAMMOPATHIES Amyloid substance is well known for Congo red staining, polarisation birefringence, and its fibrillar aspect at electron microscopy. The different forms of amyloidosis were first classified according to the presence or absence of associated pathology, and the distribution of amyloid in the organism. In the non-familial forms, amyloidosis may be either "primary" or "secondary" to another disease, such as multiple myeloma, macroglobulinaemia, neoplasms, chronic inflammatory and autoimmune diseases. Primary amyloidoses, and those associated with a myeloma or a macroglobulinaemia, have a predominantly mesenchymatous, or "pericollagen" distribution: heart, tongue, muscles, gastrointestinal tract, nerves, skin (pattern 1). The other secondary forms have a predominantly parenchymatous, or "perireticular" distribution: liver, spleen, kidney, adrenals (pattern 2) (Wintrobe, 1974; Osserman, 1975). Biochemical studies have shown that there are at least two types of amyloid: one of immunoglobulin origin, with a pattern 1 distribution, and one of non-immunoglobulin origin with a pattern 2 distribution. Analysis of amino-acid sequences showed that pattern I amyloid is composed of immunoglobulin light chains, and particularly of their variable fragment (Wintrobe, 1974; Glenner, 1975). This amyloid appears to be the result of production of monoclonal immunoglobulin or immunoglobulin light chains for three reasons. The amino-acid sequence was found to be homogeneous in different amyloid deposits in a given individual (Wintrobe, 1974). An M component, immunoglobulin or immunoglobulin light chain, was found in serum or urine of almost all cases of pattern 1 amyloidosis (Pruzanski and Katz, 1976). In contrast to the usual predominance of kappa light chains, a predominance of lambda light chains was found in monoclonal immunoglobulins associated with amyloidosis, corresponding to a predominance of lambda-type fibrils in amyloid (Glenner, 1975; Ameis and Pruzanski, 1976). Bone marrow examination showed another analogy between "primary" amyloidosis and monoclonal gammopathies. A moderate bone marrow plasma cell infiltration was found in more than 90% of cases of "primary" amyloidosis. These plasma cells even had an immature character in some cases (Pruzanski and Katz, 1976). Thus, pattern 1 (or "primary") amyloidosis is now considered as a particular manifestation of plasma cell dyscrasias such as benign and malignant gammopathies (Wintrobe, 1974; Osserman, 1975). PERIPHERAL NEUROPATHY AND MALIGNANT MONOCLONAL GAMMOPATHIES The first case of peripheral neuropathy associated with a myeloma was described by Davison and Balser (1937). This sensorimotor neuropathy was predominant in the upper limbs, and was characterised by intense pain, hypaesthesia, and distal muscle wasting. Examination of the brachial plexuses showed swollen axons and disintegration of myelin. In the absence of nerve compression or infiltration, the neuropathy was considered to be secondary either to anaemia or to an unknown toxic factor. Many similar observations were reported, and a review of the literature mentioned a total of 44 cases of neuropathy associated with myeloma, excluding the cases with cellular infiltrate or amyloid deposits (Davis and Drachman, 1972). Among 23 cases of myeloma, Walsh (1971) found three neuropathies on clinical examination (13%), and nine on electrophysiological study (39%). The association between peripheral neuropathy and Waldenstrom's macroglobulinaemia is also well known, and more than 20 cases have been described (McLeod and Walsh, 1975). The onset of clinical manifestations is generally progressive but may be acute. This sensorimotor
7 Neuropathy, amyloidosis, and monoclonal gammopathy neuropathy begins in most cases in the lower limbs, is sometimes asymmetrical in macroglobulinaemia, and can progress to quadriplegia. Pain is a complaint frequently found in myeloma neuropathyit is mentioned in 59% of cases in a review of the literature. The signs of neuropathy generally precede the diagnosis of myeloma, sometimes for several months, but may appear either before or after the systemic manifestations of macroglobulinaemia (Davis and Drachman, 1972; McLeod and Walsh, 1975). Most studies indicate an axonal degeneration as the primary process with secondary segmental demyelination. Hesselvik (1969), on the other hand, found that demyelination was more important than axonal degeneration, and another case of diffuse demyelination without axonal degeneration, but with a plasma cell infiltration has been described (Walsh, 1971; McLeod and Walsh, 1975). Though amyloidosis is often associated with myeloma and macroglobulinaemia, deposits of amyloid in peripheral nerves were rarely found when neuropathy accompanied these conditions. In a pathological study of myeloma neuropathy Hesselvik (1969) found amyloid deposits in peripheral nerves in two cases from 17 necropsies and in none from 17 biopsies. Campbell and Halford (1964) described amyloid in the vasa nervorum in a myeloma case and Dayan et al. (1971) and Davies-Jones and Esiri (1971) reported the presence of amyloid not only in vasa nervorum but in nerve interstitium. Nevertheless, these observations remain isolated, and in most cases no amyloid has been found in peripheral nerves in myeloma neuropathy. Likewise, in macroglobulinaemia only four cases of amyloid deposits in peripheral nerves are known (McLeod and Walsh, 1975). According to a review of the literature concerning 30 cases of myeloma, the neuropathy may decrease under treatment, particularly in isolated plasmocytoma if treated with radiotherapy. Improvement of neuropathy after radiotherapy was reported in two cases of plasmocytoma with a follow-up of one and a half and 10 years. Other treatments, steroids and antimetabolites, have no effect on neuropathy (Davis and Drachman, 1972). A therapeutic effect on macroglobulinaemia neuropathy has been described in some rare cases (McLeod and Walsh, 1975). PERIPHERAL NEUROPATHY AND AMYLOIDOSIS A hereditary neuropathy associated with familial amyloidosis was first described by Andrade (1952) in Portugal. The onset consists of autonomic and sensory dysfunction and is followed by loss of B 199 motor function. The mode of transmission is autosomal dominant. Several classes of hereditary neuropathies were described with particular characters in each group. In the non-familial forms of amyloidosis, neuropathy is found only in pattern 1 amyloidosis. An M component was found in serum or urine in most cases of neuropathy associated with pattern 1 amyloidosis (Benson et al., 1973; Engel and Askanas, 1976; Trotter et al., 1977). The lower limbs are generally affected first with hypaesthesiae, paraesthesiae, or constant pain. The sensory loss is distributed in a glove and stocking pattern. Loss of pain and temperature discrimination with preservation of touch has been noted in the hereditary form and in some cases of sporadic amyloid neuropathy. Loss of motor function develops later, and frequently oedema and ulceration in the lower limbs. Autonomic dysfunction is important and is sometimes the sole manifestation in amyloid neuropathy. It is characterised by orthostatic hypotension, bowel dysfunction, loss of sweating, and impotence. The carpal tunnel syndrome is frequent, and is caused by extrinsic compression of nerve (Cohen and Benson, 1975). Cohen and Benson (1975) have described four patterns of amyloid deposits. Amyloid substance may be situated outside of the nerve and provoke a compression neuropathy, particularly a carpal tunnel syndrome. Amyloid is also intravascular and can obstruct the vasa nervorum. Lastly, it is found in the neural interstitial space, forming globular deposits and diffuse infiltration. By electron microscopy, amyloid appears as nodular masses extending tongues into the intrafascicular space. Amyloid substance is composed of microfibrils with a diameter of 100 to 150 A (Bischoff, 1973). Several authors have found a preferential loss of unmyelinated and small myelinated axons, which correlates well with the pain and temperature sensory loss and the autonomic disturbances (Thomas and King, 1974). However, one group mentioned a preferential degeneration of myelinated fibres (Coimbra and Andrade, 1971). Biopsy samples from cases of amyloid neuropathy, however, show loss of both myelinated and unmyelinated fibres. At present, no treatment is effective in amyloid neuropathy. Because of the relationship between pattern 1 amyloid and other plasma cell dyscrasias, amyloid neuropathies were treated as for myeloma with melphalan and prednisone, but without benefit (Cohen and Benson, 1975; Trotter et al., 1977).
8 W. Fitting, A. Bischofi, F. Regli, and G. de (rousaz PERIPHERAL NEUROPATHY AND BENIGN MONOCLONAL GAMMOPATHY WITHOUT AMYLOIDOSIS Apart from neuropathy associated with a malignant gammopathy, almost always without amyloid, and apart from amyloid neuropathy, mostly associated with a benign gammopathy, two cases were reported concerning a neuropathy associated with benign monoclonal gammopathy without amyloid at nerve biopsy. The patient of Forssman et al. (1973) complained of subjective sensory disturbances in the lower limbs, without sensory loss at clinical examination. A monoclonal IgM was found, whiclh was considered a benign gammopathy in the absence of other signs of Waldenstrom's macroglobulinaemia during six years. The nerve biopsy did not show amyloid, but revealed lymphocytic infiltrates, and immunofluorescence showed IgM in connection with these infiltrates. With treatment by chlorambucil, the symptoms disappeared within three weeks and a second nerve biopsy was normal six months later. The case of Contamin et al. (1976) presented a symmetrical sensorimotor neuropathy associated with a benign IgG monoclonal gammopathy. Nerve biopsy showed no amyloid deposits. These two isolated cases present unusual features for plasma cell dyscrasia neuropathiesthe absence of plasma cell infiltration of bone marrow, and the favourable effect of treatment. RELATIONSHIP BETWEEN AMYLOID NEUROPATHY ANI) NEUROPATHY ASSOCIATED WITH MALIGNANT MONOCLONAL GAMMOPATHIES There are two main classes of neuropathy associated with a monoclonal gammopathy: the neuropathy of myeloma and macroglobulinaemia, associated with a malignant monoclonal gammopathy, and amyloid neuropathy associated with a benign monoclonal gammopathy. At present, malignant and benign monoclonal gammopathies and pattern 1 amyloidosis are considered to be different manifestations of plasma cell dyscrasia. A possible common cause for the neuropathies which accompany these conditions may be invoked. The pathogenesis of nerve damage is unknown in these two types of neuropathy. In the case of amyloid neuropathy, an ischaemic process has been postulated, caused by the intravascular deposits of amyloid. However, the obstruction of vasa nervorum with amyloid is often confined to a minority of vessels and does not explain the diffuse degeneration of nerve fibres. Similarly, the hypothesis of nerve damage through amyloid nodule compression cannot be retained, because these nodular deposits are frequently absent. As electron microscopy showed dissolution of basement membrane by amyloid (Coimbra and Andrade, 1971; Bischoff, 1973), it is possible that the loss of this diffusion barrier causes damage to Schwann cells of metabolic origin. The extensive and symmetrical character of amyloid neuropathy suggested a "remote effect" of plasma cell dyscrasia through the associated M component, either immunoglobulin or immunoglobulin fragment (Engel and Askanas, 1976; Trotter et al., 1977). Thus amyloid infiltration would represent the visible manifestation of an immune mechanism by an abnormal monoclonal IgM or IgG. The hypothesis of a "remote effect" through the M component has also been applied to the neuropathy associated with myeloma and macroglobulinaemia (Dayan et al., 1971; Davis and Drachman, 1972; Trotter et al., 1977). Indeed, amyloid deposits in peripheral nerves cannot be incriminated, as they are absent in most cases. Similarly, the plasma cell or lymphocytic infiltrates are rare. Serum hyperviscosity was also invoked, particularly in macroglobulinaemia neuropathy. but this hypothesis cannot be retained because several series of macroglobulinaemia neuropathy have been described without hyperviscosity (Bigner et al., 1971). Immunofluorescence studies provide supplementary arguments for participation of M component in peripheral nerve damage. Forssman et al. (1973) described the presence of IgM in a nerve biopsy sample in a case of neuropathy associated with IgM monoclonal gammopathy. The nerve biopsy showed a lymphocytic infiltrate, but no amyloid. Chazot et al. (1976) found monoclonal immunoglobulin in nerve biopsy samples in eight of 10 cases of periplheral neuropathy associated with monoclonal gammopathy. In the two negative cases there was another possible cause for neuropathy-alcoholism and diabetes. Finally, in three cases of monoclonal gammopathy without neuropathy the nerve biopsy did not show any fluorescence. Using the serum of three cases of neuropathy with benign monoclonal gammopathy. Read et al. (1978) did not demonstrate any antibody binding to peripheral nerves. However, this observation does not eliminate an immunological origin, as these authors did not use autologous nerves, but homologous post-mortem nerves. Indeed a serum IgM M component has been demonstrated on the myelin of sural nerve in a case of macroglobulinaemia neuropathy, but this serum did not show any binding to homologous control nerve (Propp et al., 1975). It is, therefore, possible that amyloid neuropathy and neuropathy associated with malignant mono-
9 Neiuropathy, amyloidosis, and monoclonal gammopathy clonal gammopathies originate from a related or common immunological process. However, the role of the M component remains unclear, and it is not known whether the monoclonal immunoglobulin found in peripheral nerve is responsible for nerve damage, or if it is only a bystander. PRESENT CASES Our three cases presented a progressive sensorimotor neuropathy, with autonomic dysfunction (loss of sweating and irregular bowel movements in two cases, partial or total loss of potency in two cases), in association with monoclonal gammopathy (IgM kappa, IgG lambda, IgG kappa). Though no absolute criterion distinguishes the malignant from the benign forms, we think that these three cases present a benign gammopathy because of the duration of the neuropathy in the absence of any clinical or biological sign of myeloma or macroglobulinaemia (10 years in case 1, at least three years in case 2, three years in case 3). In case 1, the bone marrow was normal at the first examination and showed 23% well-differentiated lymphocytes at the second. It revealed 20% slightly polymorphic plasma cells in case 2, and 10% well differentiated plasma cells in case 3. The pathological abnormality found in the sural nerves of these three cases was characterised by a marked loss of myelinated and unmyelinated nerve fibres because of active axonal degeneration with Wallerian degeneration. The defect was particularly confined to the myelinated nerve fibres of large size in the case of IgM monoclonal gammopathy, whereas in the two cases with IgG monoclonal gammopathy it was much more pronounced, comprising also many unmyelinated nerve fibres and resulting in a remarkable decrease in Schwann cells. There was no significant evidence of primary demyelination as suggested by Propp et al. (1975), and in no case was lymphoid infiltration of the nerve fascicle observed, in contrast to the findings of Chazot et al. (1976) and Contamin et al. (1976). The most striking feature in all three cases was the finding of deposits of a material which by high resolution was identifiable as an accumulation of microfibrils. In the case of IgM gammopathy, the microfibrillar infiltration was most prominent in relation to the endoneurial blood vessels, but it was apparently unrelated to blood vessels in the third case where it gave the intercellular intrafascicular space a patchy appearance. In all three cases the microfibrils were consistent with the ultrastructural appearance of amyloid deposits. Since in the two cases with IgG gamniopathy, the severe defect of the neuiral structures is attributable to direct infiltration by amyloid, an effect of a specific antibody directed against neural tissue might be suggested. These cases appear similar to another recently described by Neundorfer et al. (1977). Their case presented a sensory, motor, and autonomic neuropathy with loss of pain discrimination and relative preservation of touch sensation. There was an IgG monoclonal gammopathy, and amyloid was discovered in a peripheral nerve biopsy. In spite of these features of amyloid neuropathy, the authors labelled this case as myeloma because of a plasma cell infiltration of bone marrow. However, in most cases of pattern 1 amyloidosis, a plasma cell infiltration is found in bone marrow, sometimes exceeding 50% and occasionally presenting atypical forms (Pruzanski and Katz, 1976). In the presence of amyloid in peripheral nerve in association with an apparently benign monoclonal gammopathy and moderate infiltration of the bone marrow with differentiated plasma cells or lymphocytes, there is a strong argument to consider these three cases as pattern 1 amyloidosis neuropathy. References 201 Ameis, A., and Pruzanski, W. (1976). M components -a review of 1,242 cases. Canadian Medical A ssociaation Journal, 114, Andrade, C. (1952). A peculiar form of peripheral neuropathy. Brain, 75, Benson, M. D., Brandt, K. D., Cathcart, E. S., and Cohen, A. S. (1973). Neuropathy, M-components and amyloid. Arthritis and Rheumatism, 16, 535. Bigner, D. D., Olson, W. H., and McFarlin, D. E. (1971). Peripheral polyneuropathy, high and low molecular weight IgM, and amyloidosis. Archives of Neurology (Chicago), 24, Bischoff, A. (1973). Ultrastructural pathology of the peripheral nervous system. Journal of Neurology, 205, Campbell, A. M. G., and Halford, M. E. H. (1964). Syndrome of diarrhoea and peripheral nerve changes due to generalised vascular disease. British Medical Journal, 2, Chazot, G., Berger, B., Carrier, H., Barbaret, C., Bady, B., Dumas, R., Creyssel, R., and Schott, B. (1976). Manifestations neurologiques des gammapathies monoclonales. Revue Neurologique, 132, Clauvel, J. P., Danon, F., and Seligmann, M. (1971). Immunoglobulines monoclonales decelees en l'absence de myelome ou de macroglobulinemie de Waldenstrom. Nouvelle Revue Fran aise d'hematologie, 11, Cohen, A. S., and Benson, M. D. (1975). Amyloid neuropathy. In Peripheral Neuropathy, vol 2, pp Edited by P. J. Dyck, P. K. Thomas, and E. H. Lambert. W. B. Saunders: Philadelphia.
10 202 Coimbra, A., and Andrade, C. (1971). Familial amyloid polyneuropathy: an electron microscope study of the peripheral nerve in five cases. I. Interstitial changes. II. Nerve fibre changes. Brain, 94, Contamin, F., Singer, B., Mignot, B., Ecoffet, M., and Kazatchkine, M. (1976). Polyneuropathie a rechutes, evoluant depuis 19 ans, associee a une gammapathie monoclonale IgG benigne. Revue Neurologique, 132, Davies-Jones, G. A. B., and Esiri, M. M. (1971). Neuropathy due to amyloid in myelomatosis. British Mediceal Journal, 2, 444. Davis, L. E., and Drachman, D. B. (1972). Myeloma neuropathy. Archives of Neurology (Chicago), 27, Davison, C., and Balser, B. H. (1937). Myeloma and its neural complications. Archives of Surgery, 35, Dayan, A. D., Urich, H., and Gardner-Thorpe, C. (1971). Peripheral neuropathy and myeloma. Journal of the Neurological Sciences, 14, Engel, W. K., and Askanas, V. (1976). Remote effects of focal cancer on the neuromuscular system. In Advances in Neurology, vol. 15, pp Edited by R. A. Thomson and J. R. Green. Raven Press: New York. Forssman, O., Bjorkman, G., Hollender, A., and Englund, N. E. (1973). IgM-producing lymphocytes in peripheral nerve in a patient with benign monoclonal gammopathy. Scandinavian Journal of Haematology, 11, Glenner, G. G. (1975). Current concepts of the formation and composition of amyloid. A nnals of Clinical and Laboratory Science, 5, Hesselvik, M. (1969). Neuropathological studies on myelomatosis. A cta Neurologica Scandinavica, 45, Kyle, R. A., and Bayrd, E. D. (1966). Benign monoclonal gammopathy: a potentially malignant condition? A merican Journal of Medicine, 40, McLeod, J. G., and Walsh, J. C. (1975). Neuropathies associated with paraproteinemias and dysproteinemias. In Peripheral Neuropathy, vol. 2, pp. J. W. Fitting, A. Bischofi, F. Regli, and G. de Crousaz Edited by P. J. Dyck, P. K. Thomas, and E. H. Lambert. W. B. Saunders: Philadelphia. Neundorfer, B., Meyer, J. G., and Volk, B. (1977). Amyloid neuropathy due to monoclonal gammopathy. Journal of Neurology, 216, Osserman, E. F. (1975). Plasma cell dyscrasias. In Textbook of Medicine, pp Edited by P. B. Beeson and W. McDermott. W. B. Saunders: Philadelphia. Propp, R. P., Means, E., Deibel, R., Sherer, G., and Barron, K. (1975). Waldenstrom's macroglobulinemia and neuropathy. Neurology (Minneapolis), 25, Pruzanski, W., and Katz, A. (1976). Clinical and laboratory findings in primary generalised and multiple-myeloma-related amyloidosis. Canadian Medical Association Journal, 114, Read, D. J., Vanhegan, R. I., and Matthews, W. B. (1978). Peripheral neuropathy and benign IgG paraproteinaemia. Journal of Neurology, Neurosurgery, and Psychiatry, 41, Ritzmann, S. E., Loukas, D., Sakai, H., Daniels, J. C., and Levin, W. C. (1975). Idiopathic (a.ymptomatic) monoclonal gammopathies. A rchives of Internal Medicine, 135, Thomas, P. K., and King, R. H. M. (1974). Peripheral nerve changes in amyloid neuropathy. Brain, 97, Trotter, J. L., Engel, W. K., and Ignaczak, T. F. (1977). Amyloidosis with plasma cell dyscrasia. An overlooked cause of adult onset sensorimotor neuropathy. Archives of Neurology (Chicago), 34, Waldenstrom, J. (1964). The occurrence of benign, essential monoclonal (M type) non-macromolecular hyperglobulinemia and its differential diagnosis. IV. Studies in the gammopathies. Acta Medica Scandinavica, 176, Walsh, J. C. (1971). The neuropathy of multiple myeloma. An electrophysiological and histological study. Archives of Neurology (Chicago), 25, Wintrobe, M. M. (1974). Plasma cell dyscrasias. Multiple myeloma. In Clinical Hematology, Seventh Edition, p Lea and Febiger: Philadelphia. J Neurol Neurosurg Psychiatry: first published as /jnnp on 1 March Downloaded from on 15 December 2018 by guest.
Significance of immunoglobulin deposition in peripheral nerve in neuropathies associated with
 Journal ofneurology, Neurosurgery, and Psychiatry, 1979, 42, 179-183 Significance of immunoglobulin deposition in peripheral nerve in neuropathies associated with paraproteinaemia M. SWASH, J. PERRIN,
Journal ofneurology, Neurosurgery, and Psychiatry, 1979, 42, 179-183 Significance of immunoglobulin deposition in peripheral nerve in neuropathies associated with paraproteinaemia M. SWASH, J. PERRIN,
Peripheral neuropathy and benign IgG
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 215-219 Peripheral neuropathy and benign IgG paraproteinaemia D. J. READ, R. I. VANHEGAN, AND W. B. MATTHEWS From the Department of Neurology,
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 215-219 Peripheral neuropathy and benign IgG paraproteinaemia D. J. READ, R. I. VANHEGAN, AND W. B. MATTHEWS From the Department of Neurology,
Jonathan Katz, MD CPMC
 Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC First, a bit of background Classic CIDP--TREATABLE MADSAM/Asymmetric Neuropathy Chronic Length Dependent Neuropathy-
Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC Jonathan Katz, MD CPMC First, a bit of background Classic CIDP--TREATABLE MADSAM/Asymmetric Neuropathy Chronic Length Dependent Neuropathy-
Distal chronic spinal muscular atrophy involving the hands
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
lymphadenopathy with dysproteinaemia
 Journal ofneurology, Neurosurgery, and Psychiatry, 1979, 42, 519-523 Peripheral neuropathy in angioimmunoblastic lymphadenopathy with dysproteinaemia GIOVANNI TREDICI, MARIO MINAZZI, AND EMILIO LAMPUGNANI
Journal ofneurology, Neurosurgery, and Psychiatry, 1979, 42, 519-523 Peripheral neuropathy in angioimmunoblastic lymphadenopathy with dysproteinaemia GIOVANNI TREDICI, MARIO MINAZZI, AND EMILIO LAMPUGNANI
CIDP + MMN - how to diagnose and treat. Dr Hadi Manji
 CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
Peripheral Nerve Amyloidosis in Sural Nerve Biopsies. A Clinicopathologic Analysis of 13 Cases
 Peripheral Nerve Amyloidosis in Sural Nerve Biopsies A Clinicopathologic Analysis of 13 Cases Bijal Rajani, MB, BS; Vakesh Rajani, MB, BS; Richard A. Prayson, MD Objective. Amyloidosis is a well-recognized
Peripheral Nerve Amyloidosis in Sural Nerve Biopsies A Clinicopathologic Analysis of 13 Cases Bijal Rajani, MB, BS; Vakesh Rajani, MB, BS; Richard A. Prayson, MD Objective. Amyloidosis is a well-recognized
A faint in the emergency department (due to primary systemic amyloidosis
 104 PRACTICAL NEUROLOGY NEUROLOGICAL RARITIES A faint in the emergency department (due to primary systemic amyloidosis Michele T. M. Hu*, Carolyn M. Gabriel*, Helen J. Lachmann, Rosalind King, Philip N.
104 PRACTICAL NEUROLOGY NEUROLOGICAL RARITIES A faint in the emergency department (due to primary systemic amyloidosis Michele T. M. Hu*, Carolyn M. Gabriel*, Helen J. Lachmann, Rosalind King, Philip N.
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Thank you to: L Magy, L Richard, N Couade, F Maquin
 «Crash course in the interpretation of peripheral nerve biopsies: which nerve to biopsy, tissue fixation: paraffin, semi thins, EM (common stains and immunos), identifying degenerating and regenerating
«Crash course in the interpretation of peripheral nerve biopsies: which nerve to biopsy, tissue fixation: paraffin, semi thins, EM (common stains and immunos), identifying degenerating and regenerating
Lec-14 د.خالد نافع. Medicine. Multiple Myeloma
 Fifth stage Lec-14 د.خالد نافع Medicine 24/4/2016 Multiple Myeloma Plasma cell myeloma Variants Non - secretory myeloma Indolent myeloma Smouldering myeloma Plasma cell leukaemia Plasmacytoma - Solitary
Fifth stage Lec-14 د.خالد نافع Medicine 24/4/2016 Multiple Myeloma Plasma cell myeloma Variants Non - secretory myeloma Indolent myeloma Smouldering myeloma Plasma cell leukaemia Plasmacytoma - Solitary
Diagnostic investigation of patients with chronic polyneuropathy: evaluation of a clinical guideline
 J Neurol Neurosurg Psychiatry 2001;71:205 209 205 Department of Neurology, Academic Medical Centre, University of Amsterdam, PO Box 22700, 1100 DE Amsterdam, The Netherlands N R Rosenberg P Portegies M
J Neurol Neurosurg Psychiatry 2001;71:205 209 205 Department of Neurology, Academic Medical Centre, University of Amsterdam, PO Box 22700, 1100 DE Amsterdam, The Netherlands N R Rosenberg P Portegies M
Clinical Aspects of Peripheral Nerve and Muscle Disease. Roy Weller Clinical Neurosciences University of Southampton School of Medicine
 Clinical Aspects of Peripheral Nerve and Muscle Disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Nerves 1. Anterior Horn Cell 2. Dorsal root ganglion cell 3.
Clinical Aspects of Peripheral Nerve and Muscle Disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Nerves 1. Anterior Horn Cell 2. Dorsal root ganglion cell 3.
M-Protien, what to do next? Ismail A Sharif MD, FRCPc Internal Medicine Day 22 nd April 2016
 + M-Protien, what to do next? Ismail A Sharif MD, FRCPc Internal Medicine Day 22 nd April 2016 + Disclosures Advisory Boards: AMGEN, Lundbeck, NOVARTIS + Subtypes of Plasma Cell Disorders Increased Plasma
+ M-Protien, what to do next? Ismail A Sharif MD, FRCPc Internal Medicine Day 22 nd April 2016 + Disclosures Advisory Boards: AMGEN, Lundbeck, NOVARTIS + Subtypes of Plasma Cell Disorders Increased Plasma
Interesting case seminar: Native kidneys Case Report:
 Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Instructions for Plasma Cell Disorders (PCD) Post-HCT Data (Form 2116 Revision 3)
 (Form 2116 Revision 3) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Plasma Cell Disorders (PCD) Post-HCT Data Form. E-mail comments regarding the
(Form 2116 Revision 3) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Plasma Cell Disorders (PCD) Post-HCT Data Form. E-mail comments regarding the
FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS
 FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS Guillermo A. Herrera MD Louisiana State University, Shreveport Fibrils in bundles 10-20 nm d Diabetic fibrillosis
FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS Guillermo A. Herrera MD Louisiana State University, Shreveport Fibrils in bundles 10-20 nm d Diabetic fibrillosis
RENAL HISTOPATHOLOGY
 RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
The near-nerve sensory nerve conduction in tarsal tunnel syndrome
 Journal of Neurology, Neurosurgery, and Psychiatry 1985;48: 999-1003 The near-nerve sensory nerve conduction in tarsal tunnel syndrome SHN J OH, HYUN S KM, BASHRUDDN K AHMAD From the Department ofneurology,
Journal of Neurology, Neurosurgery, and Psychiatry 1985;48: 999-1003 The near-nerve sensory nerve conduction in tarsal tunnel syndrome SHN J OH, HYUN S KM, BASHRUDDN K AHMAD From the Department ofneurology,
Tarek ElBaz, MD. Prof. Internal Medicine Chief, Division of Renal Medicine Al Azhar University President, ESNT
 The Kidney in Multiple Myeloma Tarek ElBaz, MD. Prof. Internal Medicine Chief, Division of Renal Medicine Al Azhar University President, ESNT Normal Cell Plasma cells produce antibodies that bind to antigens,
The Kidney in Multiple Myeloma Tarek ElBaz, MD. Prof. Internal Medicine Chief, Division of Renal Medicine Al Azhar University President, ESNT Normal Cell Plasma cells produce antibodies that bind to antigens,
NEUROPATHY IN PERIPHERAL VASCULAR DISEASE 1
 267 616.833-02:616.13-005 NEUROPATHY IN PERIPHERAL VASCULAR DISEASE 1 Its Bearing on Diabetic Neuropathy BY E. C. HUTCHINSON AND L. A. LIVERSKDGE (From the Department of Neurology, Manchester Royal Infirmary)
267 616.833-02:616.13-005 NEUROPATHY IN PERIPHERAL VASCULAR DISEASE 1 Its Bearing on Diabetic Neuropathy BY E. C. HUTCHINSON AND L. A. LIVERSKDGE (From the Department of Neurology, Manchester Royal Infirmary)
A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL
 A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL CASE HISTORY Nine year old male child Second born Born
A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL CASE HISTORY Nine year old male child Second born Born
CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME
 CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME Dr Seethalekshmy N.V., Dr.Annie Jojo, Dr Hiran K.R., Amrita institute of Medical Sciences, Kochi, Kerala Case history 34 year old gentleman Nephrotic range
CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME Dr Seethalekshmy N.V., Dr.Annie Jojo, Dr Hiran K.R., Amrita institute of Medical Sciences, Kochi, Kerala Case history 34 year old gentleman Nephrotic range
Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies
 138 Original Article Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies James M. Killian, MD,* Shane Smyth, MD,* Rudy Guerra, PhD, Ishan Adhikari, MD,* and Yadollah Harati,
138 Original Article Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies James M. Killian, MD,* Shane Smyth, MD,* Rudy Guerra, PhD, Ishan Adhikari, MD,* and Yadollah Harati,
Expanding Spectrum of Diseases Associated with Plasma Cell Dyscrasias
 Expanding Spectrum of Diseases Associated with Plasma Cell Dyscrasias Eva Honsova Institute for Clinical and Experimental Medicine Prague, Czech Republic eva.honsova@ikem.cz Plasma cell dyscrasias Plasma
Expanding Spectrum of Diseases Associated with Plasma Cell Dyscrasias Eva Honsova Institute for Clinical and Experimental Medicine Prague, Czech Republic eva.honsova@ikem.cz Plasma cell dyscrasias Plasma
Median-ulnar nerve communications and carpal tunnel syndrome
 Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 982-986 Median-ulnar nerve communications and carpal tunnel syndrome LUDWIG GUTMANN From the Department of Neurology, West Virginia University,
Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 982-986 Median-ulnar nerve communications and carpal tunnel syndrome LUDWIG GUTMANN From the Department of Neurology, West Virginia University,
Differential Diagnosis of Neuropathies and Compression. Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre
 Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
diphenylhydantoin therapy1
 Journal of Neurology, Neurosurgery, and Psychiatry, 1975, 38, 1235-1239 Motor nerve conduction study in patients on diphenylhydantoin therapy1 S. CHOKROVERTY2 AND Z. A. SAYEED3 From the Neurology Service
Journal of Neurology, Neurosurgery, and Psychiatry, 1975, 38, 1235-1239 Motor nerve conduction study in patients on diphenylhydantoin therapy1 S. CHOKROVERTY2 AND Z. A. SAYEED3 From the Neurology Service
Monoclonal Gammopathies and the Kidney. Tibor Nádasdy, MD The Ohio State University, Columbus, OH
 Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Histopathology: Glomerulonephritis and other renal pathology
 Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Glistening, Skin-Colored Nodule
 To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/436334 Medscape Dermatology Clinic Glistening, Skin-Colored Nodule
To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/436334 Medscape Dermatology Clinic Glistening, Skin-Colored Nodule
Peripheral Neuropathies
 Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
Plasma cell myeloma (multiple myeloma)
 Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Making sense of Nerve conduction & EMG
 Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
at least in part, by observing the effect of raising body temperature on the evoked potentials. upper limit of the normal value for latency of
 Journal of Neurology, Neurosurgery, and Psychiatry, 1979, 42, 250-255 Effect of raising body temperature on visual and somatosensory evoked potentials in patients with multiple sclerosis W. B. MATTHEWS,
Journal of Neurology, Neurosurgery, and Psychiatry, 1979, 42, 250-255 Effect of raising body temperature on visual and somatosensory evoked potentials in patients with multiple sclerosis W. B. MATTHEWS,
Hematology 101. Rachid Baz, M.D. 5/16/2014
 Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
Malignant Peripheral Nerve Sheath Tumor
 C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
reversing familial amyloid polyneuropathy naturally the raw vegan plant based detoxification regeneration workbook for healing patients volume 2
 DOWNLOAD OR READ : REVERSING FAMILIAL AMYLOID POLYNEUROPATHY NATURALLY THE RAW VEGAN PLANT BASED DETOXIFICATION REGENERATION WORKBOOK FOR HEALING PATIENTS VOLUME 2 PDF EBOOK EPUB MOBI Page 1 Page 2 healing
DOWNLOAD OR READ : REVERSING FAMILIAL AMYLOID POLYNEUROPATHY NATURALLY THE RAW VEGAN PLANT BASED DETOXIFICATION REGENERATION WORKBOOK FOR HEALING PATIENTS VOLUME 2 PDF EBOOK EPUB MOBI Page 1 Page 2 healing
Light-Chain Mediated Acute Tubular Interstitial Nephritis. A Poorly Recognized Pattern of Renal Disease in Patients With Plasma Cell Dyscrasia
 Light-Chain Mediated Acute Tubular Interstitial Nephritis A Poorly Recognized Pattern of Renal Disease in Patients With Plasma Cell Dyscrasia Xin Gu, MD; Guillermo A. Herrera, MD Context. Acute renal failure
Light-Chain Mediated Acute Tubular Interstitial Nephritis A Poorly Recognized Pattern of Renal Disease in Patients With Plasma Cell Dyscrasia Xin Gu, MD; Guillermo A. Herrera, MD Context. Acute renal failure
A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017
 A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017 Disclosures Research support from Cytokinetics, Inc Catalyst, Inc Editorial fees from UptoDate. Objectives Describe
A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017 Disclosures Research support from Cytokinetics, Inc Catalyst, Inc Editorial fees from UptoDate. Objectives Describe
Early View Article: Online published version of an accepted article before publication in the final form.
 Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Oncology Type of Article: Case Report Title:
Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Oncology Type of Article: Case Report Title:
Immune Mediated Neuropathies
 Immune Mediated Neuropathies Hernan Gatuslao, M.D. Assistant Professor Department of Neurology Virginia Commonwealth University School of Medicine AIDP and CIDP Acute inflammatory demyelinating polyneuropathy
Immune Mediated Neuropathies Hernan Gatuslao, M.D. Assistant Professor Department of Neurology Virginia Commonwealth University School of Medicine AIDP and CIDP Acute inflammatory demyelinating polyneuropathy
CNS third year med students Summary of midterm material H Awad
 CNS third year med students 2018 Summary of midterm material H Awad Dear All This presentation summaries the main important topics covered in the midterm material ( lectures 1-6) There will be two questions
CNS third year med students 2018 Summary of midterm material H Awad Dear All This presentation summaries the main important topics covered in the midterm material ( lectures 1-6) There will be two questions
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM. Andrzej Sladkowski
 Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Uncommon early-onset neuropathy in diabetic patients
 J Neurol (1998) 245 : 61 68 Springer-Verlag 1998 ORIGINAL COMMUNICATION G. Said A. Bigo A. Améri J.-P. Gayno F. Elgrably P. Chanson G. Slama Uncommon early-onset neuropathy in diabetic patients Received:
J Neurol (1998) 245 : 61 68 Springer-Verlag 1998 ORIGINAL COMMUNICATION G. Said A. Bigo A. Améri J.-P. Gayno F. Elgrably P. Chanson G. Slama Uncommon early-onset neuropathy in diabetic patients Received:
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases
 Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
A family study of Charcot-Marie-Tooth disease
 Joturnal of Medical Genetics, 1982, 19, 88-93 A family study of Charcot-Marie-Tooth disease A P BROOKS* AND A E H EMERY From the University Department of Human Genetics, Western General Hospital, Edinburgh
Joturnal of Medical Genetics, 1982, 19, 88-93 A family study of Charcot-Marie-Tooth disease A P BROOKS* AND A E H EMERY From the University Department of Human Genetics, Western General Hospital, Edinburgh
Burkitt lymphoma. Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8
 Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
November 16-18, 2017 Hotel Monteleone New Orleans, LA. Provided by
 November 16-18, 2017 Hotel Monteleone New Orleans, LA Provided by Diabetic Neuropathy: A Global and Growing Problem John D. England, MD Louisiana State University Health Sciences Center School of Medicine
November 16-18, 2017 Hotel Monteleone New Orleans, LA Provided by Diabetic Neuropathy: A Global and Growing Problem John D. England, MD Louisiana State University Health Sciences Center School of Medicine
Southern Derbyshire Shared Care Pathology Guidelines. MGUS (Monoclonal Gammopathy of Undetermined Significance)
 Southern Derbyshire Shared Care Pathology Guidelines MGUS (Monoclonal Gammopathy of Undetermined Significance) Purpose of guideline This guideline provides information about the risk stratification of
Southern Derbyshire Shared Care Pathology Guidelines MGUS (Monoclonal Gammopathy of Undetermined Significance) Purpose of guideline This guideline provides information about the risk stratification of
Sensory conduction of the sural nerve in polyneuropathy'
 Jourtial of Neurology, Neurosurgery, anid Psychiatry, 1974, 37, 647-652 Sensory conduction of the sural nerve in polyneuropathy' DAVID BURKE, NEVELL F. SKUSE, AND A. KEITH LETHLEAN From the Unit of Clinical
Jourtial of Neurology, Neurosurgery, anid Psychiatry, 1974, 37, 647-652 Sensory conduction of the sural nerve in polyneuropathy' DAVID BURKE, NEVELL F. SKUSE, AND A. KEITH LETHLEAN From the Unit of Clinical
The ABCs of Waldenström s Macroglobulinemia (WM)
 The ABCs of Waldenström s Macroglobulinemia (WM) Jeffrey V. Matous MD Colorado Blood Cancer Institute IWMF Ed Forum May 2017 Objectives Describe the roots underneath WM Review incidence, possible risk
The ABCs of Waldenström s Macroglobulinemia (WM) Jeffrey V. Matous MD Colorado Blood Cancer Institute IWMF Ed Forum May 2017 Objectives Describe the roots underneath WM Review incidence, possible risk
A/Professor Arun Aggarwal Balmain Hospital
 A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
Diabetic Neuropathy. Nicholas J. Silvestri, M.D.
 Diabetic Neuropathy Nicholas J. Silvestri, M.D. Types of Neuropathies Associated with Diabetes Mellitus p Chronic distal sensorimotor polyneuropathy p Focal compression neuropathies p Autonomic neuropathy
Diabetic Neuropathy Nicholas J. Silvestri, M.D. Types of Neuropathies Associated with Diabetes Mellitus p Chronic distal sensorimotor polyneuropathy p Focal compression neuropathies p Autonomic neuropathy
Doctor, I have dizzy feet! Evaluation of patients with suspected neuropathy
 Doctor, I have dizzy feet! Evaluation of patients with suspected neuropathy Causes of chronic polyneuropathy Signs and symptoms Large fiber modalities Ataxia esp. in the dark Are you ok in the shower
Doctor, I have dizzy feet! Evaluation of patients with suspected neuropathy Causes of chronic polyneuropathy Signs and symptoms Large fiber modalities Ataxia esp. in the dark Are you ok in the shower
International Journal of Basic and Applied Physiology
 A STUDY OF CARDIOVASCULAR RESPONSES TO AUTONOMIC NERVE FUNCTIONS IN RHEUMATOID ARTHRITIS Ankur *, Rampure M Dilip **, Irshad Hussain Askari *** * Associate professor, Department of Physiology, MNR Medical
A STUDY OF CARDIOVASCULAR RESPONSES TO AUTONOMIC NERVE FUNCTIONS IN RHEUMATOID ARTHRITIS Ankur *, Rampure M Dilip **, Irshad Hussain Askari *** * Associate professor, Department of Physiology, MNR Medical
Glomerular pathology in systemic disease
 Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Ordering Physician. Collected REVISED REPORT. Performed. IgG IF, Renal MCR. Lambda IF, Renal MCR. C1q IF, Renal. MCR Albumin IF, Renal MCR
 RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
Clinicopathological importance of deposits of amyloid
 J Clin Pathol 1985;38:868-872 Clinicopathological importance of deposits of amyloid in the femoral head NRB CARY From the Department ofhistopathology and Experimental Pathology, Charing Cross and Westminster
J Clin Pathol 1985;38:868-872 Clinicopathological importance of deposits of amyloid in the femoral head NRB CARY From the Department ofhistopathology and Experimental Pathology, Charing Cross and Westminster
The Internist s Approach to Neuropathy
 The Internist s Approach to Neuropathy VOLKAN GRANIT, MD, MSC ASSISTANT PROFESSOR OF NEUROLOGY NEUROMUSCU LAR DIVISION UNIVERSITY OF MIAMI, MILLER SCHOOL OF MEDICINE RELEVANT DECLARATIONS Financial disclosures:
The Internist s Approach to Neuropathy VOLKAN GRANIT, MD, MSC ASSISTANT PROFESSOR OF NEUROLOGY NEUROMUSCU LAR DIVISION UNIVERSITY OF MIAMI, MILLER SCHOOL OF MEDICINE RELEVANT DECLARATIONS Financial disclosures:
Light chain deposition disease presenting with hepatomegaly: an association with amyloid-like fibrils
 Postgraduate Medical Journal (1988) 64, 804-808 Light chain deposition disease presenting with hepatomegaly: an association with amyloid-like fibrils G. Pelletier,I M. Fabre,2 P. Attali,i A. Ladouch-Badre,2
Postgraduate Medical Journal (1988) 64, 804-808 Light chain deposition disease presenting with hepatomegaly: an association with amyloid-like fibrils G. Pelletier,I M. Fabre,2 P. Attali,i A. Ladouch-Badre,2
Hereditary quadriceps myopathy
 Journal of Neurology, Neurosurgery, and Psychiatry, 1973, 36, 1041-1045 Hereditary quadriceps myopathy MICHAEL L. E. ESPIR AND W. B. MATTHEWS' From the Department of Neurology, Derbyshire Royal Infirmary,
Journal of Neurology, Neurosurgery, and Psychiatry, 1973, 36, 1041-1045 Hereditary quadriceps myopathy MICHAEL L. E. ESPIR AND W. B. MATTHEWS' From the Department of Neurology, Derbyshire Royal Infirmary,
Pathological changes in the vagus nerve in diabetes
 Journal of Neurology, Neurosurgery, and Psychiatry 1987;50:1449-1453 Pathological changes in the vagus nerve in diabetes and chronic alcoholism Y-P GUO,* J G McLEOD, J BAVERSTOCK From the Department of
Journal of Neurology, Neurosurgery, and Psychiatry 1987;50:1449-1453 Pathological changes in the vagus nerve in diabetes and chronic alcoholism Y-P GUO,* J G McLEOD, J BAVERSTOCK From the Department of
Insulin Neuritis: an old, but still an unfamiliar and mysterious condition
 Insulin Neuritis: an old, but still an unfamiliar and mysterious condition Authors: Yun Tae Hwang 1, Gerard Davies 1 1. Department of Neurology, Royal Free Hospital, United Kingdom Corresponding author:
Insulin Neuritis: an old, but still an unfamiliar and mysterious condition Authors: Yun Tae Hwang 1, Gerard Davies 1 1. Department of Neurology, Royal Free Hospital, United Kingdom Corresponding author:
Ultrastructural studies of human cutaneous nerve
 J. clin. Path. (1965), 18, 188 Ultrastructural studies of human cutaneous nerve with special reference to lamellated cell inclusions and vacuole-containing cells MARJORE J. EVANS, J. B. FNEAN, AND A. L.
J. clin. Path. (1965), 18, 188 Ultrastructural studies of human cutaneous nerve with special reference to lamellated cell inclusions and vacuole-containing cells MARJORE J. EVANS, J. B. FNEAN, AND A. L.
Diagnosis of Amyloidosis. Maria M. Picken MD, PhD Loyola University Medical Center Chicago
 Diagnosis of Amyloidosis Maria M. Picken MD, PhD Loyola University Medical Center Chicago mpicken@lumc.edu 1 Outline Diagnosis of amyloidosis Fat pad Other 2 Amyloidoses protein folding disorders protein
Diagnosis of Amyloidosis Maria M. Picken MD, PhD Loyola University Medical Center Chicago mpicken@lumc.edu 1 Outline Diagnosis of amyloidosis Fat pad Other 2 Amyloidoses protein folding disorders protein
Familial amyloidotic polineuropathy and systemic lupus
 (2012) 21, 1455 1458 http://lup.sagepub.com CASE REPORT AC Ferreira, F Carvalho and F Nolasco Department of Nephrology, Centro Hospitalar de Lisboa Central, Hospital de Curry Cabral, Lisbon, Portugal Familial
(2012) 21, 1455 1458 http://lup.sagepub.com CASE REPORT AC Ferreira, F Carvalho and F Nolasco Department of Nephrology, Centro Hospitalar de Lisboa Central, Hospital de Curry Cabral, Lisbon, Portugal Familial
Surgical Pathology Report
 Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Michael Joffe ST6 Haematology SpR
 Michael Joffe ST6 Haematology SpR Mrs SB 71 year old female on AMU Telephone referral to haematology by medicine with Hb 102 MCV 89, normal B12, Folate, Ferritin. PMH DM General decline over several weeks
Michael Joffe ST6 Haematology SpR Mrs SB 71 year old female on AMU Telephone referral to haematology by medicine with Hb 102 MCV 89, normal B12, Folate, Ferritin. PMH DM General decline over several weeks
Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
 doi: 10.2169/internalmedicine.1723-18 http://internmed.jp CASE REPORT Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
doi: 10.2169/internalmedicine.1723-18 http://internmed.jp CASE REPORT Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
Osteosclerotic Myeloma (POEMS Syndrome)
 Osteosclerotic Myeloma (POEMS Syndrome) Osteosclerotic Myeloma (POEMS Syndrome) Synonyms Crow-Fukase syndrome Multicentric Castleman disease Takatsuki syndrome Acronym coined by Bardwick POEMS Scheinker,
Osteosclerotic Myeloma (POEMS Syndrome) Osteosclerotic Myeloma (POEMS Syndrome) Synonyms Crow-Fukase syndrome Multicentric Castleman disease Takatsuki syndrome Acronym coined by Bardwick POEMS Scheinker,
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
Peripheral neuropathy and solitary plasmacytoma
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 177-184 Peripheral neuropathy and solitary plasmacytoma DAVID RAD AND CHARLS WARLOW From the Department of Neurology, Churchill Hospital, Oxford,
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 177-184 Peripheral neuropathy and solitary plasmacytoma DAVID RAD AND CHARLS WARLOW From the Department of Neurology, Churchill Hospital, Oxford,
The Utility Of Congo Red Stain And Cytokeratin Immunostain In The Detection Of Primary Cutaneous Amyloidosis
 ISPUB.COM The Internet Journal of Pathology Volume 17 Number 1 The Utility Of Congo Red Stain And Cytokeratin Immunostain In The Detection Of Primary Cutaneous A,A Citation A, A.. The Internet Journal
ISPUB.COM The Internet Journal of Pathology Volume 17 Number 1 The Utility Of Congo Red Stain And Cytokeratin Immunostain In The Detection Of Primary Cutaneous A,A Citation A, A.. The Internet Journal
Laboratory Examination
 Todd Zimmerman, M.D. 64 year old African American male presents to establish care with PCG. Meds: Norvasc 5 mg daily PMHx: HTN x 20 years, poorly controlled SHx: No tobacco, illicit; rare EtOH ROS: Negative
Todd Zimmerman, M.D. 64 year old African American male presents to establish care with PCG. Meds: Norvasc 5 mg daily PMHx: HTN x 20 years, poorly controlled SHx: No tobacco, illicit; rare EtOH ROS: Negative
A Tale of Five Demyelinating Neuropathies
 Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
Update on Treatments for Systemic Amyloidosis
 Update on Treatments for Systemic Amyloidosis Laura M. Dember, M.D. Renal, Electrolyte and Hypertension Division University of Pennsylvania ANZSN Update Course Darwin, Australia September 2, 2017 Disclosure
Update on Treatments for Systemic Amyloidosis Laura M. Dember, M.D. Renal, Electrolyte and Hypertension Division University of Pennsylvania ANZSN Update Course Darwin, Australia September 2, 2017 Disclosure
Some observations we are making
 Some observations we are making The audience is very smart and they know how to diagnose a neuropathy. There is a standard workup that all patients seem to get: B12, folate, RPR, TSH prior to them being
Some observations we are making The audience is very smart and they know how to diagnose a neuropathy. There is a standard workup that all patients seem to get: B12, folate, RPR, TSH prior to them being
Understanding the Serum Free Light Chain Assays. Anne L Sherwood, PhD Director of Scientific Affairs The Binding Site, Inc.
 Understanding the Serum Free Light Chain Assays Anne L Sherwood, PhD Director of Scientific Affairs The Binding Site, Inc. AL Amyloidosis: abnormality of proteins from Plasma Cells in the Bone Marrow Red
Understanding the Serum Free Light Chain Assays Anne L Sherwood, PhD Director of Scientific Affairs The Binding Site, Inc. AL Amyloidosis: abnormality of proteins from Plasma Cells in the Bone Marrow Red
Motor and sensory nerve conduction studies
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
Investigating the pathological mechanisms of neuropathy in POEMS syndrome
 Dr S B Keddie- ABN Clinical Research Training Fellowship Case for Support Investigating the pathological mechanisms of neuropathy in POEMS syndrome Background and Importance POEMS syndrome (polyradiculoneuropathy,
Dr S B Keddie- ABN Clinical Research Training Fellowship Case for Support Investigating the pathological mechanisms of neuropathy in POEMS syndrome Background and Importance POEMS syndrome (polyradiculoneuropathy,
The New England Journal of Medicine
 A TRIAL OF THREE REGIMENS FOR PRIMARY AMYLOIDOSIS: COLCHICINE ALONE, MELPHALAN AND PREDNISONE, AND MELPHALAN, PREDNISONE, AND COLCHICINE ROBERT A. KYLE, M.D., MORIE A. GERTZ, M.D., PHILIP R. GREIPP, M.D.,
A TRIAL OF THREE REGIMENS FOR PRIMARY AMYLOIDOSIS: COLCHICINE ALONE, MELPHALAN AND PREDNISONE, AND MELPHALAN, PREDNISONE, AND COLCHICINE ROBERT A. KYLE, M.D., MORIE A. GERTZ, M.D., PHILIP R. GREIPP, M.D.,
Case Report Diaphragmatic Amyloidosis Causing Respiratory Failure: A Case Report and Review of Literature
 Volume 2015, Article ID 917157, 4 pages http://dx.doi.org/10.1155/2015/917157 Case Report Diaphragmatic Amyloidosis Causing Respiratory Failure: A Case Report and Review of Literature Aleksey Novikov,
Volume 2015, Article ID 917157, 4 pages http://dx.doi.org/10.1155/2015/917157 Case Report Diaphragmatic Amyloidosis Causing Respiratory Failure: A Case Report and Review of Literature Aleksey Novikov,
PRIMARY DISEASES OF MYELIN. By: Shifaa Al Qa qa
 PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
Introduction and aims of the study
 Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Balgrist Symposium zum Diabetischen Fuss. Der Charcot-Fuss Oktober diabetic neuropathies. symptoms. signs. sensory disorders.
 symptoms sensory disorders spontaneous paraesthesia tingling burning by touch, pressure dysaesthesia sign pain continuous boring cutting drawing paroxysmal lancinating neuralgiform causalgic fluctuating,
symptoms sensory disorders spontaneous paraesthesia tingling burning by touch, pressure dysaesthesia sign pain continuous boring cutting drawing paroxysmal lancinating neuralgiform causalgic fluctuating,
Compound Action Potential, CAP
 Stimulus Strength UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY INTRODUCTION TO NEUROPHYSIOLOGY Spring, 2013 Textbook of Medical Physiology by: Guyton & Hall, 12 th edition
Stimulus Strength UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY INTRODUCTION TO NEUROPHYSIOLOGY Spring, 2013 Textbook of Medical Physiology by: Guyton & Hall, 12 th edition
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL RESPONSE ASSESSMENT MYELOMA CHAPTER 11C REVISED: SEPTEMBER 2016
 MYELOMA Quantitative Markers-Myeloma Assessment Quantitative markers are biochemicals that are recorded in tests on body fluids such as serum and urine. Applicable Disease Sites The myeloma disease site
MYELOMA Quantitative Markers-Myeloma Assessment Quantitative markers are biochemicals that are recorded in tests on body fluids such as serum and urine. Applicable Disease Sites The myeloma disease site
AII-type: Select the most appropriate answer
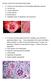 AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
Case Report A Case of Proliferative Glomerulonephritis with Monoclonal IgG Deposits That Showed Predominantly Membranous Features
 Hindawi Case Reports in Nephrology Volume 2017, Article ID 1027376, 5 pages https://doi.org/10.1155/2017/1027376 Case Report A Case of Proliferative Glomerulonephritis with Monoclonal IgG Deposits That
Hindawi Case Reports in Nephrology Volume 2017, Article ID 1027376, 5 pages https://doi.org/10.1155/2017/1027376 Case Report A Case of Proliferative Glomerulonephritis with Monoclonal IgG Deposits That
Hereditary distal spinal muscular atrophy
 Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 413-418 Hereditary distal spinal muscular atrophy with vocal cord paralysis I D YOUNG AND P S HARPER From the Section ofmedical Genetics, Department
Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 413-418 Hereditary distal spinal muscular atrophy with vocal cord paralysis I D YOUNG AND P S HARPER From the Section ofmedical Genetics, Department
Nerve pathologic features differentiate POEMS syndrome from CIDP
 Piccione et al. Acta Neuropathologica Communications (2016) 4:116 DOI 10.1186/s40478-016-0389-1 RESEARCH Nerve pathologic features differentiate POEMS syndrome from CIDP Ezequiel A. Piccione 1, Janean
Piccione et al. Acta Neuropathologica Communications (2016) 4:116 DOI 10.1186/s40478-016-0389-1 RESEARCH Nerve pathologic features differentiate POEMS syndrome from CIDP Ezequiel A. Piccione 1, Janean
Index. Note: Page numbers of article titles are in boldface type.
 Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
LIGHT CHAIN DISEASE B. DHANALAKSHMI 1 & V. HEMAVATHY 2
 TJPRC: International Journal of Nursing and Patient Safety & Care (TJPRC: IJNPSC) Vol. 1, Issue 1, Dec 2016, 21-24 TJPRC Pvt. Ltd. LIGHT CHAIN DISEASE B. DHANALAKSHMI 1 & V. HEMAVATHY 2 1 Associate Professor,
TJPRC: International Journal of Nursing and Patient Safety & Care (TJPRC: IJNPSC) Vol. 1, Issue 1, Dec 2016, 21-24 TJPRC Pvt. Ltd. LIGHT CHAIN DISEASE B. DHANALAKSHMI 1 & V. HEMAVATHY 2 1 Associate Professor,
Disclosure. Entrapment Neuropathies - Overview. Common mononeuropathy sites. Definitions. Common mononeuropathy sites. Common mononeuropathy sites
 Disclosure Entrapment Neuropathies - Overview I receive compensation from Wiley- Blackwell publishers for my work as Editor-in-Chief of Muscle & Nerve Lawrence H. Phillips, II, MD Definitions Mononeuropathy:
Disclosure Entrapment Neuropathies - Overview I receive compensation from Wiley- Blackwell publishers for my work as Editor-in-Chief of Muscle & Nerve Lawrence H. Phillips, II, MD Definitions Mononeuropathy:
Symptomatic pain treatments (carbamazepine and gabapentin) were tried and had only a transient and incomplete effect on the severe pain syndrome.
 Laurencin 1 Appendix e-1 Supplementary Material: Clinical observations Patient 1 (48-year-old man) This patient, who was without a notable medical history, presented with thoracic pain and cough, which
Laurencin 1 Appendix e-1 Supplementary Material: Clinical observations Patient 1 (48-year-old man) This patient, who was without a notable medical history, presented with thoracic pain and cough, which
INVESTIGATIVE OPHTHALMOLOGY. Corneal and conjunctival changes in dysproteinemia
 August 1969 Volume 8, Number 4 INVESTIGATIVE OPHTHALMOLOGY Corneal and conjunctival changes in dysproteinemia 7?. M. H. Pinkerton and David M. Robertson A case of dysproteinemia with corneal and conjunctival
August 1969 Volume 8, Number 4 INVESTIGATIVE OPHTHALMOLOGY Corneal and conjunctival changes in dysproteinemia 7?. M. H. Pinkerton and David M. Robertson A case of dysproteinemia with corneal and conjunctival
Patogenesi e terapia della Neuropatia Motoria Multifocale
 26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
