Acute pancreatitis in children
|
|
|
- Marcia Hodges
- 5 years ago
- Views:
Transcription
1 Original paper Acute pancreatitis in children Urszula Grzybowska-Chlebowczyk 1, Martyna Jasielska 2, Anna Flak-Wancerz 2, Sabina Więcek 2, Katarzyna Gruszczyńska 3, Wojciech Chlebowczyk 4, Halina Woś 1 1 Department of Paediatrics, School of Medicine, Medical University of Silesia, Katowice, Poland 2 Department of Gastroenterology, Upper-Silesian Child Health Care Centre, Katowice, Poland 3 Department of Diagnostic Imaging and Interventional Radiology, School of Medicine, Medical University of Silesia, Katowice, Poland 4 Department of Nursing and Social Medical Problems, School of Health Sciences, Medical University of Silesia, Katowice, Poland Gastroenterology Rev 2018; 13 (1): DOI: Key words: acute pancreatitis, children, paediatric, aetiology. Address for correspondence: Urszula Grzybowska-Chlebowczyk MD, Department of Paediatrics, Gastroenterology Unit, Upper-Silesian Child Health Care Centre, Medical University of Silesia, 16 Medyków St, Katowice, Poland, phone: , fax: , klinikapediatrii@sum.edu.pl Abstract Introduction: The acute pancreatitis is a rare disease, but it has started to be diagnosed more often in children. Aim: The aim of the study was single-centre, retrospective analysis of the incidence, aetiology, and clinical course of acute pancreatitis in children. Material and methods: We analysed the medical records of patients with acute pancreatitis hospitalised in the Gastroenterology Unit of the Paediatrics Department, Medical University of Silesia from Jan 2004 to Dec Results: There were 76 cases of acute pancreatitis among 51 children (average age: years) hospitalised in the Gastroenterology Unit between January 2004 and December The diagnosis of acute pancreatitis was performed on the basis of INSPIRE criteria and modified Atlanta classification. Patients were divided into groups: I 1 12 years old, which included 20 (39.21%) children and II years old, with 31 (60.78%) children. The idiopathic aetiology was the most common cause of acute pancreatitis, occurring in 22 (43.1%) children, and in 15 cases the aetiology of the disease was biliary (29.4%). Genetically determined causes were diagnosed in 8 (15.7%) patients, the PRSS1 mutation in four patients, mutation in SPINK1 in 1 child, and CFTR gene mutation in 1 child. Two children simultaneously had two genes mutations (CFTR, SPINK1), and during the considered period had more than one episode of acute pancreatitis. Conclusions: Acute pancreatitis of idiopathic aetiology was most common among the examined children, and this should encourage the continued search for the causes of disease, especially genetic, and with particular emphasis on younger age group. Introduction Acute pancreatitis (AP) is a disease in which there is an autolysis of this organ. Inflammatory changes in the pancreas and its surroundings are a consequence of the release of the enzymatic cascade initiated by the conversion of trypsinogen to trypsin. There are two pathological forms of AP: pancreatic oedema, with rather mild course and pancreatic or peripancreatic necrosis, with a poor prognosis, but rare in childhood (less than 1%). The aetiology, clinical course, and treatment of pancreatitis are different in children and adults. However, so far to recognise the AP and in clinical practice, the Atlanta modified guidelines were used by extrapolating them to the patient population of children under 18 years of age [1, 2]. It was not until 2012 when the group of experts published the INSPPIRE (International Study Group of Paediatric Pancreatitis: In search of a cure) guidelines, the aim of which was to establish the definition of AP, acute recurrent pancreatitis, and chronic pancreatitis in children [3]. According to INSPPIRE, AP can be recognised when there are two of the following three criteria: clinical symptoms, particularly abdominal pain, which suggests pancreatitis (abdominal pain of acute onset), nausea, vomiting, and back pain; increased levels of serum amylase and/or lipase at least three times greater than the upper limit of normal and imaging findings characteristic for AP. Acute
2 70 U. Grzybowska-Chlebowczyk, M. Jasielska, A. Flak-Wancerz, S. Więcek, K. Gruszczyńska, W. Chlebowczyk, H. Woś recurrent pancreatitis requires at least two episodes of AP separated by at least a 1-month pain-free interval or complete normalisation of serum pancreatic enzyme levels and pain-free period, irrespective of a specific time interval between AP episodes. Acute pancreatitis is a rare disease, but it has started to be diagnosed more often in children. The incidence is estimated at /100,000 per year [4, 5]. The reasons for increased incidence of AP can be different and are not fully understood, but it is considered that they may be associated with a greater awareness of the disease in the paediatric population [6 8]. Aim The aim of the study was a single-centre, retrospective analysis of the incidence, aetiology, and clinical course of AP in children. Material and methods We retrospectively analysed the medical records of patients with acute pancreatitis hospitalised in the Gastroenterology Unit of the Department of Paediatrics Medical University of Silesia within 10 years from January 2004 to December There were 76 cases of AP in 51 children. The diagnosis of AP was made based on the INSPIRE criteria and modified Atlanta criteria (two of three criteria) a threefold increase in biochemical markers (amylase or lipase), characteristic abdominal pain, and changes in imaging examinations [1 3]. The following data were analysed: the aetiology of AP, the basic values of biochemical parameters (amylase and lipase in blood serum, concentration of the alanine aminotransferase, gamma-glutamyltranspeptidase, total bilirubin, C-reactive protein, levels of leukocytes in the blood), imaging findings (ultrasonography, computed tomography and magnetic resonance imaging of the abdomen), and the length of hospitalisation. Number of episodes Time [year] Figure 1. The incidence of acute pancreatitis in subsequent years Statistical analysis The data were subjected to statistical analysis using Statistica All analyses were performed with a 95% significance interval. Due to the qualitative nature of the variables, the sample size n > 40, and the occurrence of expected size < 10, the c 2 test for qualitative variables V 2 was used. Results The incidence of acute pancreatitis Seventy-six cases of AP among 51 children (53% girls 27 children) were reported. The youngest child was 20 months old, the oldest was 18 years old, and the average age was years. Patients were divided into two age groups: I 1 12 years, which included 20 (39.21%) children and II years, with 31 (60.78%) children. In the younger age group 10 children were under 7 years of age. The incidence of AP in subsequent years is shown in Figure 1. Aetiology The most common aetiology of AP was idiopathic 43.1%. Biliary aetiology occurred in 15 (29.4%) children, among them in one child, during imaging examination, anomalies in the form of choledochal cyst were found and one patient with congenital spherocytosis with extrahepatic and intrahepatic cholestasis was reported. Genetically determined causes were diagnosed in 8 (15.7%) patients, the mutation in the trypsinogen (PRSS1) in 4 children, mutation in the gene encoding trypsin inhibitor (SPINK1) in 1 child, and mutation in the CFTR gene in 1 child. It is worth noting that 2 children simultaneously had two gene mutations (CFTR and SPINK1), and during the considered period 1 boy had 5 episodes of AP, and the second one two. Isolated cases of pancreatitis caused by separate factors were recognised as other causes of AP. This group included patients with AP due to the following reasons: iatrogenic after endoscopic retrograde cholangiopancreatography (ERCP) in 1 child; occurring with the first appearance of ulcerative colitis; alcoholic in an almost 18-yearold patient with a history of alcohol abuse directly before the onset of symptoms; and toxic in a 2-year-old patient due to consumption of the petroleum ether. In 2 children post-traumatic recurrent AP was diagnosed, among them in 1 child, 3 months earlier a classic bicycle handlebars injury occurred, after which AP occurred twice (after the second episode large cyst in the pancreatic tail) (Table I). In the younger age group the idiopathic aetiology of pancreatitis dominated (21.6%), while among older
3 Acute pancreatitis in children 71 Table I. The causes of acute pancreatitis Acute pancreatitis aetiology N (%) Biliary: 15 (29.4) Cholecystolithiasis 13 (25.4) Biliary tract anomalies 1 (2) Hereditary spherocytosis 1 (2) Genetic: 8 (15.8) PRSS1 4 (7.8) SPINK1 1 (2) CFTR 1 (2) Mutations in two genes (SPINK1, CFTR) 2 (3.9) Idiopathic 22 (43.1) Other 6 (11.7) children AP of idiopathic cause (21.6% children) and biliary cause (21.6%) occurred equally often (Figure 2). In the analysed period, 12 (23.4%) children were hospitalised more than once due to AP (Table II). Another episode of AP in the younger age group occurred in 8 (15.6%) children, and in the older group in 4 (7.8%) patients. Most frequently, disease recurrence was in cases of AP of idiopathic cause. Clinical symptoms The most frequently reported clinical symptom of AP was abdominal pain, which occurred in 73 cases of Percent Biliary Genetic Idiopathic Other Etiology Age group: 1 12 years years Figure 2. The aetiology of acute pancreatitis in different age groups disease (96%), and vomiting was observed in 40.8% of children. Fever was a rare symptom, concerning only 3.8% of patients. There was no statistically significant relationship between occurrence of symptoms and the age of patients (p > 0.05). Results of laboratory tests The increased levels of amylase enzyme activity in serum greater than three upper limits of normal were found in 63 (82.9%) cases of AP, of which 32.9% exceeded tenfold. In 28 children the serum lipase activity was investigated, in 19 children the level was least three times greater than the upper limit of normal, and in 3 patients the result was positive, with normal amylase activity in serum. The concentration of C-re- Table II. Characteristics of children with recurrent acute pancreatitis Case Gender Number of episodes during the considered period Age at the time of I episode [years] Aetiology 1 M 5 10 Idiopathic 2 M 5 6 Mutations in the SPINK1 and CFTR gene 3 F 5 4 Mutation in the PRSS1 gene 4 F 4 3 Idiopathic 5 M 4 12 Idiopathic 6 F 2 12 Mutation in the PRSS1 gene 7 F 2 15 Episodes associated with ulcerative colitis 8 M 2 4 Idiopathic 9 F 2 16 Mutation in the SPINK1 gene 10 F 2 17 Idiopathic 11 M 2 12 Mutations in the SPINK1 and CFTR gene 12 M 2 17 Idiopathic
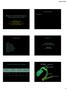
4 72 U. Grzybowska-Chlebowczyk, M. Jasielska, A. Flak-Wancerz, S. Więcek, K. Gruszczyńska, W. Chlebowczyk, H. Woś Table III. The presence of laboratory tests depending on the aetiology of acute pancreatitis Aetiology of acute pancreatitis Amylase > 3 N Leukocytosis > /µl Blood laboratory tests C-reactive protein > 10 mg/l Total bilirubin > 17 µmol/l P-value Idiopathic 13 (25.5%) 6 (11.8%) 9 (17.7%) 8 (15.6%) > 0.05 Biliary 18 (35.3%) 5 (9.8%) 7 (13.7%) 0 (0%) Genetic 6 (9.8%) 3 (5.9%) 4 (7.8%) 0 (0%) Other 5 (9.8%) 0 (0%) 1 (2%) 0 (0%) Amylase N: U/l. active protein was increased in 29 (38.1%) children, whereas leukocytosis was observed in 25 (32.9%) patients (Table III). Hiperbilirubinaemia occurred in 8 children and was observed only in children with biliary aetiology, which was statistically significant (p < 0.05). There were no statistically significant abnormalities in other laboratory studies depending on the age and aetiology of AP. The results of imaging All patients underwent abdominal ultrasound examination. In 51 (67.1%) cases of AP characteristic pancreatic parenchyma changes in the form of swelling, changes in echogenicity, or presence of peripancreatic fluid collections were shown. Imaging examinations were extended by the computed tomography (CT) scan of the abdomen in 56 cases of AP. Among performed examinations, in 60% of cases changes specific to pancreatitis occurred. The oedema pancreatitis was diagnosed in 29 patients, necrotising pancreatitis in 5 children. In 13 children cholecystitis, gallstones, or cholelithiasis biliary were diagnosed (Figure 3). Magnetic resonance imaging cholangiography was performed in 23 (45%) children; choledocholitiasis was diagnosed in 5 (9.8%) children, cholelithiasis in 4 (7.8%) children, and in one girl the biliary cysts type IV occurred. Hospitalisation The hospitalisation period ranged from 4 to 48 days (average: 13.8 days). Eight (10.5%) patients were discharged within 7 days, and hospitalisation for more than 2 weeks involved 27 (35.5%) children. The median was 13 days. In age group I (1 12 years) 21.6% of the children stayed on the ward for less than 14 days and 15.7% for more than 14 days. There was no death of a patient due to AP or its complications. The longest hospitalisation (over 14 days) occurred in children with the AP of biliary aetiology 10 (19.6%) patients, and the shortest, to 7 days, in patients with AP of unknown aetiology and AP from other causes 4 (7.8%). The statistical significance between the length of hospitalisation and the age and aetiology of AP had not been demonstrated (p > 0.05). Treatment Five children were qualified for therapeutic endoscopic retrograde cholangiopancreatography (ERCP), which took place in the Department of Gastroenterology of the Medical University of Silesia. Six (11.7%) patients were transferred to the Department of Surgery to surgical treatment: 2 children with pancreatic cysts, 2 because of cholelithiasis, and 1 child because of both cholelithiasis and pancreatic cyst. One girl (13 years old) with biliary AP was transferred because of numerous cysts of the pancreas; additionally, in the CT image thrombosis of the portal vein was visualised. The other children were treated conservatively. Discussion In recent years, many studies have drawn attention to the increasing incidence of AP in both adults and children. This phenomenon was described for the first time by Lopez in a children s hospital in Dallas (from 5 to 113 patients/years from 1993 to 1998), which has been confirmed by other researchers from various parts of the world [4, 5, 9 12]. In our 10-year study, the incidence of AP was between 3 and 13 episodes per year, the increasing trend of this disease incidence was not confirmed. On the other hand, the recurrence of AP occurred in 23.4% of children. In the literature the described frequency of relapse of AP is different: Kandula and Lowe describe 10%, Park 15%, Chen 21.3%, and Sanchez- Ramirez 34.5% [11, 13 15]. Among our patients the biliary aetiology involved nearly 30% of cases of AP, and it was also one of the dominant causes of AP among children from the older age group. It is consistent with previous studies, in which cholelithiasis was the cause of 10 30% of pancreatitis in children [11, 13, 14, 16, 17]. In other studies,
5 Acute pancreatitis in children 73 A B 2.8 cm C D Figure 3. Computed tompography in a girl with acute pancreatitis. A Enlarged pancreatic head. B Features of swelling of the pancreas tail (arrows). C Fluid in the retroperitoneal space in the vicinity of the pancreatic head (arrows). D Fluid in the retroperitoneal space in the front of the renal fascia (arrows) similar to our work, the frequency of biliary aetiology was higher among older children [11]. Acute pancreatitis of idiopathic aetiology was diagnosed in 43.1% of children, which is slightly higher than reported in the literature, where the frequency is described at the level of 8% (Werlin) to 34% (DeBanto) [4, 9, 14]. It is worth mentioning that the idiopathic aetiology most frequently involved younger children. The third leading cause of AP was genetic mutations (in the SPINK1, PRSS1, and CFTR genes) found among almost 16% of children, including 2 children with two mutations, and these children had more than one episode of pancreatitis in the analysed period. The frequency of this pancreatitis reason is described in the literature at the level of % [9, 17] In 2012, the Sultan showed a high prevalence of genetic mutations (in the SPINK, PRSS1, and CFTR genes) in patients with recurrent and chronic pancreatitis without other causes of these diseases (anatomic and metabolic) [18]. It is known that mutations in the gene PRSS1 (two types: R122H and N29I) are responsible for hereditary pancreatitis, and SPINK1 gene mutation is strongly associated (about 20% of patients) with idiopathic chronic pancreatitis in children and adolescents [19]. In recent years, some other mutations associated with the early occurrence of acute and chronic pancreatitis have been described mutations in the CPA1 gene encoding carboxypeptidase A1 (one of the pancreatic metalloproteinases) [20]. In Poland, SPINK1, PRSS1, CFTR, and AAT gene mutations were examined by Sobczyńska-Tomaszewska et al. They obtained the highest incidence of mutations in the field of SPINK1 and PRSS1 genes among patients with chronic pancreatitis and recurrent AP, and among members of the families of these patients [21]. In our
6 74 U. Grzybowska-Chlebowczyk, M. Jasielska, A. Flak-Wancerz, S. Więcek, K. Gruszczyńska, W. Chlebowczyk, H. Woś study, we examined mutations only in three genes, but it is worth noting that in 2 children with recurrent AP and a positive family history of recurrent AP the cause of the disease was not found (also a genetic mutation). It seems that in some children, who did not show the cause of AP, the mutation could occurred in other genes than in the three tested by us. Among our patients, the median hospitalisation was 13 days, and the average was 13.8 days, children from the younger age group most often were hospitalised for 7 14 days (21.6% of children), and patients from the older age group over 14 days (29.4% of patients). However, this is shorter than in other studies; the average length of hospitalisation described by Werlin et al. was 24 days, and by Sanchez-Ramirez et al. was 25.7 days. This is probably related with the overwhelming number of children without any complications in our study [12, 15]. However, the median hospitalisation of our patients was longer than described by other authors Park et al. (5 days) and Werlin et al. (8 days) [11, 12]. The most common symptoms among the studied children were the abdominal pain and vomiting (96% and 40% of children), which is confirmed by previous research [11, 12, 14]. Fever was observed in a small percentage of children (3.8%), in contrast to some other researchers. Kandula and Lowe [13] described fever in 40% of patients, Chen et al. in 33% [14], and Sanchez- Ramirez et al. in 27% [15]. Laboratory indicators of pancreatitis are the serum amylase and/or lipase activity at least three times greater than the upper limit of normal. Increased amylase activity was recorded in 83% of patients, just like in research from the UK and the US [12, 22]; a little lower (about 50% of patients) was described by Park et al. [11]. In 3 children amylase activity was within normal limits but the lipase enzyme activity was increased; these children were between the ages of 8 to 13 years. It is not rare because it is estimated that approximately 20% of patients with pancreatitis have normal amylase levels [7]. At the same time, Park and Kandula pointed out that the measurement of lipase activity might be a more sensitive indicator of AP than amylase among younger patients (100% vs %) [11, 13]. Moreover, Park et al. in their study proved that a 1.5-fold increase in lipase activity above the upper limit of normal in young children might be associated with the occurrence of AP [11]. All children had an abdominal ultrasound examination, and characteristic changes were observed in 67% of patients, slightly more than in the Werlin et al. and Sanchez-Ramirez et al. study [12, 15]. Computed tomography scan of the abdomen was performed in 73.6% of children, of which 60% visualised lesions characteristic for AP. Additionally, some researchers have shown that in the younger group of children the frequency of CT is lower (about 60%), which is related to saving children from exposure to ionising radiation and relatively low sensitivity of this test [13, 23]. According to guidelines from the Atlanta and INSPIRE group of experts, if there are two criteria of AP, i.e. characteristic abdominal pain and three times greater than the upper limit of normal pancreatic enzymes activity, there is no need to perform CT of the pancreas [1 3]. Computed tomography is not recommended, especially in the first phase of pancreatitis (oedematous); however, it is recommended when pancreatic necrosis is suspected [1, 2, 6]. The sensitivity of CT for the diagnosis of AP is estimated at 47 81% [11, 13, 14]. In recent years increasing interest in the prognostic significance of CT in children with severe AP can be seen [24 26]. In 2012 Lautz et al. assessed the predictive value of the CTSI scale (Computed Tomography Severity Index), used in adults, in a series of 64 children with AP. CTSI showed greater predictive value (sensitivity 81%, specificity 76%, PPV 62%, and NPV 90%) in predicting severe AP and serious clinical complications in relation to Ransons scale, the AP scale, and the scale of Glasgow [23]. However, so far a prospective study documenting the value of the CTSI in children with AP has not been carried out. Conclusions Acute pancreatitis of idiopathic aetiology was the most common among the examined children, and this fact should encourage researchers to continue looking for the causes of disease, especially genetic, and with particular emphasis on the younger age group. Due to the limited number of examined children in the available, current literature, it seems necessary to plan a large, prospective, multi-centre study in order to evaluate the incidence, aetiology, natural history, and evaluation of the effectiveness of available prognostic scales of AP. Conflict of interest The authors declare no conflict of interest. References 1. Bradley EL. A clinically based classification system for acute pancreatitis. Summary of the International Symposium on Acute Pancreatitis, Atlanta, Ga, September 11 through 13, Arch Surg 1993; 128: Banks PA, Bollen TL, Dervenis C, et al. Classification of acute pancreatitis--2012: revision of the Atlanta classification and definitions by international consensus. Gut 2013; 62:
7 Acute pancreatitis in children Morinville VD, Husain SZ, Bai H, et al. Definitions of pediatric pancreatitis and survey of present clinical practices. J Pediatr Gastroenterol Nutr 2012; 55: Nydegger A, Heine RG, Ranuh R, et al. Changing incidence of acute pancreatitis: 10-year experience at the Royal Children s Hospital, Melbourne. J Gastroenterol Hepatol 2007; 22: Morinville VD, Barmada MM, Lowe ME. Increasing incidence of acute pancreatitis at an American pediatric tertiary care center: is greater awareness among physicians responsible? Pancreas 2010; 39: Bai HX, Lowe ME, Husain SZ. What have we learned about acute pancreatitis in children? J Pediatr Gastroenterol Nutr 2011; 52: Abu-El-Haija M, Lin TK, Palermo J. Update to the management of pediatric acute pancreatitis: highlighting areas in need of research. J Pediatr Gastroenterol Nutr 2014; 58: Lowe ME. Pancreatitis in childhood. Curr Gastroenterol Rep 2004; 6: DeBanto JR, Goday PS, Pedroso MR, et al. Acute pancreatitis in children. Am J Gastroenterol 2002; 97: Lopez MJ. The changing incidence of acute pancreatitis in children: a single-institution perspective. J Pediatr 2002; 140: Park A, Latif SU, Shah AU, et al. Changing referral trends of acute pancreatitis in children: a 12-year single-center analysis. J Pediatr Gastroenterol Nutr 2009; 49: Werlin SL, Kugathasan S, Frautschy BC. Pancreatitis in children. J Pediatr Gastroenterol Nutr 2003; 37: Kandula L, Lowe ME. Etiology and outcome of acute pancreatitis in infants and toddlers. J Pediatr 2008; 152: , 10.e Chen CF, Kong MS, Lai MW, Wang CJ. Acute pancreatitis in children: 10-year experience in a medical center. Acta Paediatr Taiwan 2006; 47: Sánchez-Ramírez CA, Larrosa-Haro A, Flores-Martínez S, et al. Acute and recurrent pancreatitis in children: etiological factors. Acta Paediatr 2007; 96: Antunes H, Nascimento J, Mesquita A, Correia-Pinto J. Acute pancreatitis in children: a tertiary hospital report. Scand J Gastroenterol 2014; 49: Minen F, De Cunto A, Martelossi S, Ventura A. Acute and recurrent pancreatitis in children: exploring etiological factors. Scand J Gastroenterol 2012; 47: Sultan M, Werlin S, Venkatasubramani N. Genetic prevalence and characteristics in children with recurrent pancreatitis. J Pediatr Gastroenterol Nutr 2012; 54: Räty S, Piironen A, Babu M, et al. Screening for human cationic trypsinogen (PRSS1) and trypsinogen inhibitor gene (SPINK1) mutations in a Finnish family with hereditary pancreatitis. Scand J Gastroenterol 2007; 42: Witt H, Beer S, Rosendahl J, et al. Variants in CPA1 are strongly associated with early onset chronic pancreatitis. Nat Genet 2013; 45: Haddock G, Coupar G, Youngson GG, et al. Acute pancreatitis in children: a 15-year review. J Pediatr Surg 1994; 29: Sobczyńska-Tomaszewska A, Bak D, Oralewska B, et al. Analysis of CFTR, SPINK1, PRSS1 and AAT mutations in children with acute or chronic pancreatitis. J Pediatr Gastroenterol Nutr 2006; 43: Park AJ, Latif SU, Ahmad MU, et al. A comparison of presentation and management trends in acute pancreatitis between infants/toddlers and older children. J Pediatr Gastroenterol Nutr 2010; 51: Lautz TB, Turkel G, Radhakhrishnan J, et al. Utility of the computed tomography severity index (Balthazar score) in children in acute pancreatitis. J Paediatric Surg 2012; 47: Rainzer MD, Phatak UP, Baker K, et al. Acute necrotizing pancreatitis in children. J Pediatr 2013; 162: Suzuki M, Saito N, Naritaka N, et al. Scoring system for prediction of acute pancreatitis in children. Pediatr Int 2015; 57: Fabre A, Petit P, Gaudart J, et al. Severity scores in children with acute pancreatitis. J Pediatr Gastroenterol Nutr 2012; 55: Received: Accepted:
A Retrospective & Prospective Comprehensive Study of Acute Pancreatitis (Diagnosis, Course & Managment)
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. X (May. 2016), PP 15-19 www.iosrjournals.org A Retrospective & Prospective Comprehensive
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. X (May. 2016), PP 15-19 www.iosrjournals.org A Retrospective & Prospective Comprehensive
Multidetector CT evaluation of acute pancreatitis and its complications and its correlation with clinical outcome
 INTERNATIONAL JOURNAL OF CURRENT RESEARCH IN BIOLOGY AND MEDICINE ISSN: 2455-944X www.darshanpublishers.com DOI:10.22192/ijcrbm Volume 3, Issue 1-2018 Original Research Article Multidetector CT evaluation
INTERNATIONAL JOURNAL OF CURRENT RESEARCH IN BIOLOGY AND MEDICINE ISSN: 2455-944X www.darshanpublishers.com DOI:10.22192/ijcrbm Volume 3, Issue 1-2018 Original Research Article Multidetector CT evaluation
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Association of Obesity in Children with Pancreatitis in a Predominantly Hispanic Population at the US-Mexican Border: A Single Center Outpatient Study
 Health, 2016, 8, 1820-1829 http://www.scirp.org/journal/health ISSN Online: 1949-5005 ISSN Print: 1949-4998 Association of Obesity in Children with Pancreatitis in a Predominantly Hispanic Population at
Health, 2016, 8, 1820-1829 http://www.scirp.org/journal/health ISSN Online: 1949-5005 ISSN Print: 1949-4998 Association of Obesity in Children with Pancreatitis in a Predominantly Hispanic Population at
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
JMSCR Vol 05 Issue 06 Page June 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.76 A Comparative Study of Assessment of Different
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.76 A Comparative Study of Assessment of Different
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 8/27/2011 Radiology Quiz of the Week # 35 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 8/27/2011 Radiology Quiz of the Week # 35 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Anubhav Harshit Kumar* and Mahavir Singh Griwan ORIGINAL ARTICLE. Abstract. Department of Surgery, Pt. B. D. Sharma PGIMS, Rohtak, India
 Gastroenterology Report, 2017, 1 5 doi: 10.1093/gastro/gox029 Original article ORIGINAL ARTICLE A comparison of APACHE II, BISAP, Ranson s score and modified CTSI in predicting the severity of acute pancreatitis
Gastroenterology Report, 2017, 1 5 doi: 10.1093/gastro/gox029 Original article ORIGINAL ARTICLE A comparison of APACHE II, BISAP, Ranson s score and modified CTSI in predicting the severity of acute pancreatitis
IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION
 IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION Andrew T. Trout, MD @AndrewTroutMD Disclosures Grant support National Pancreas Foundation In-kind support - ChiRhoClin modified from:
IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION Andrew T. Trout, MD @AndrewTroutMD Disclosures Grant support National Pancreas Foundation In-kind support - ChiRhoClin modified from:
Comprehensive Study of Acute Pancreatitis (Diagnosis, Disease Course, and Clinical Management): A Retrospective and Prospective Study
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/449 Comprehensive Study of Acute Pancreatitis (Diagnosis, Disease Course, and Clinical Management): A Retrospective
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/449 Comprehensive Study of Acute Pancreatitis (Diagnosis, Disease Course, and Clinical Management): A Retrospective
Acute pancreatitis complications and a method to improve the outcome
 Acute pancreatitis complications and a method to improve the outcome Poster No.: C-2959 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit B. Angheloiu, A. Leandru; Brasov/RO Abdomen,
Acute pancreatitis complications and a method to improve the outcome Poster No.: C-2959 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit B. Angheloiu, A. Leandru; Brasov/RO Abdomen,
Risk Factors Associated With Biliary Pancreatitis In Children
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2012 Risk Factors Associated With Biliary Pancreatitis In
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2012 Risk Factors Associated With Biliary Pancreatitis In
Clinical profile, degree of severity and underlying factors of acute pancreatitis among a group of Bangladeshi patients
 Clinical profile, degree of severity and underlying factors of acute pancreatitis among a group of Bangladeshi patients Indrajit Kumar Datta 1, Md Nazmul Haque 1, Tareq M Bhuiyan 2 Original Article 1 Deaprtment
Clinical profile, degree of severity and underlying factors of acute pancreatitis among a group of Bangladeshi patients Indrajit Kumar Datta 1, Md Nazmul Haque 1, Tareq M Bhuiyan 2 Original Article 1 Deaprtment
Acute pancreatitis due to intragastric balloon
 www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Acute pancreatitis due to intragastric balloon Orlando Jorge Martins Torres, Jose Maria Assunção Moraes-Junior, Camila Cristina S. Torres,
www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Acute pancreatitis due to intragastric balloon Orlando Jorge Martins Torres, Jose Maria Assunção Moraes-Junior, Camila Cristina S. Torres,
ISSN X (Print) Research Article. *Corresponding author Dr. Prashant Uddhaorao Titare
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(6D):3140-3144 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(6D):3140-3144 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
THE CLINICAL course of severe
 ORIGINAL ARTICLE Improved Prediction of Outcome in Patients With Severe Acute Pancreatitis by the APACHE II Score at 48 Hours After Hospital Admission Compared With the at Admission Arif A. Khan, MD; Dilip
ORIGINAL ARTICLE Improved Prediction of Outcome in Patients With Severe Acute Pancreatitis by the APACHE II Score at 48 Hours After Hospital Admission Compared With the at Admission Arif A. Khan, MD; Dilip
Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines
 Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines Kevin Sargen, Andrew N Kingsnorth Department of Surgery, Plymouth Postgraduate Medical School, Derriford Hospital. Plymouth.
Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines Kevin Sargen, Andrew N Kingsnorth Department of Surgery, Plymouth Postgraduate Medical School, Derriford Hospital. Plymouth.
A Prospective Study of Bedside Index for Severity in Acute Pancreatitis Score in Acute Pancreatitis
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/210 A Prospective Study of Bedside Index for Severity in Acute Pancreatitis Score in Acute Pancreatitis S Kasturi Bai
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/210 A Prospective Study of Bedside Index for Severity in Acute Pancreatitis Score in Acute Pancreatitis S Kasturi Bai
Michael Wilschanski Pediatric Gastroenterology, Hadassah Medical Organization Jerusalem, Israel
 Recurrent Acute Pancreatitis in Israeli, Children Michael Wilschanski Pediatric Gastroenterology, Hadassah Medical Organization Jerusalem, Israel ISPGHAN EILAT FEBRUARY RY 2013 Etiologies of recurrent/chronic
Recurrent Acute Pancreatitis in Israeli, Children Michael Wilschanski Pediatric Gastroenterology, Hadassah Medical Organization Jerusalem, Israel ISPGHAN EILAT FEBRUARY RY 2013 Etiologies of recurrent/chronic
Pancreatitis in children has been
 An Update on Pediatric Pancreatitis Monica Shukla-Udawatta, MD; Shailender Madani, MD; and Deepak Kamat, MD, PhD, FAAP ABSTRACT There has been a rise in the incidence and number of admissions of children
An Update on Pediatric Pancreatitis Monica Shukla-Udawatta, MD; Shailender Madani, MD; and Deepak Kamat, MD, PhD, FAAP ABSTRACT There has been a rise in the incidence and number of admissions of children
Gall bladder cancer. Information for patients Hepatobiliary
 Gall bladder cancer Information for patients Hepatobiliary page 2 of 12 Who will provide my care? You will be cared for by a number of professionals who work together. These professionals will be specialist
Gall bladder cancer Information for patients Hepatobiliary page 2 of 12 Who will provide my care? You will be cared for by a number of professionals who work together. These professionals will be specialist
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE. T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar
 ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
Prognostic Indicator in Severe Acute Pancreatitis
 Open Access Journal Research Article DOI: 10.23958/ijirms/vol03-i05/10 Prognostic Indicator in Severe Acute Pancreatitis Dr. Ajay Khanolkar 1, Dr. Manish Khare *2 1 Associate Professor, 2 Assistant Professor
Open Access Journal Research Article DOI: 10.23958/ijirms/vol03-i05/10 Prognostic Indicator in Severe Acute Pancreatitis Dr. Ajay Khanolkar 1, Dr. Manish Khare *2 1 Associate Professor, 2 Assistant Professor
Corporate Medical Policy
 Corporate Medical Policy Genetic Testing for Hereditary Pancreatitis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_hereditary_pancreatits 9/2013 7/2017 7/2018
Corporate Medical Policy Genetic Testing for Hereditary Pancreatitis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_hereditary_pancreatits 9/2013 7/2017 7/2018
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
U Nordic Forum - Trauma & Emergency Radiology. Lecture Objectives. MDCT in Acute Pancreatitis. Acute Pancreatitis: Etiologies
 Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Background. RUQ Ultrasound Normal, Recommend Clinical Correlation. Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial
 RUQ Ultrasound Normal, Recommend Clinical Correlation Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial Background Incidence of pediatric gallbladder disease continues to rise U.S. Pediatric
RUQ Ultrasound Normal, Recommend Clinical Correlation Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial Background Incidence of pediatric gallbladder disease continues to rise U.S. Pediatric
Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography
 AISP - 29 th National Congress. Bologna (Italy). September 15-17, 2005. Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography Lucia Calculli 1, Raffaele Pezzilli 2, Riccardo
AISP - 29 th National Congress. Bologna (Italy). September 15-17, 2005. Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography Lucia Calculli 1, Raffaele Pezzilli 2, Riccardo
amount (per occasion): If yes: frequency: N/A / occasionally/monthly/weekly/daily
 1. Patient personal details Insurance number:.. Name:. Date of birth:... Gender: female / male Race: Asian-Indian / White / Black / N/A Admission date:.. Last day of treatment:. Date of interview: Institute:
1. Patient personal details Insurance number:.. Name:. Date of birth:... Gender: female / male Race: Asian-Indian / White / Black / N/A Admission date:.. Last day of treatment:. Date of interview: Institute:
Controversies in the management of acute pancreatitis
 Kathmandu University Medical Journal (3) Vol., No. 3, Issue 7, 3-7 Controversies in the management of acute pancreatitis Singh DR 1, Mehta A, Dangol UMS 3 1 Lecturer, Medical Officer, 3 Lecturer, Dept.
Kathmandu University Medical Journal (3) Vol., No. 3, Issue 7, 3-7 Controversies in the management of acute pancreatitis Singh DR 1, Mehta A, Dangol UMS 3 1 Lecturer, Medical Officer, 3 Lecturer, Dept.
Jaundice. Agnieszka Dobrowolska- Zachwieja, MD, PhD
 Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Comparison of Different Scoring System in Predicting the Severity and Prognosis of Acute Pancreatitis
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 3 (May. 2018), PP 56-60 www.iosrjournals.org Comparison of Different Scoring System
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 3 (May. 2018), PP 56-60 www.iosrjournals.org Comparison of Different Scoring System
Role of Imaging Methods in Diagnosis of Acute Pancreatitis. Válek V. Radiologická klinika, FN Brno a LF MU v Brně
 Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
Pathophysiology ACUTE PANCREATITIS
 Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
Correspondence should be addressed to Supot Pongprasobchai;
 Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 3525349, 7 pages https://doi.org/10.1155/2017/3525349 Research Article Severity, Treatment, and Outcome of Acute Pancreatitis in Thailand:
Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 3525349, 7 pages https://doi.org/10.1155/2017/3525349 Research Article Severity, Treatment, and Outcome of Acute Pancreatitis in Thailand:
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital
 Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
Acute Pancreatitis and its Clinical Study and Management in Amaravathi Region
 Research Article Acute Pancreatitis and its Clinical Study and Management in Amaravathi Region Satyanarayana Rao S V*, Babu Rao D, Krishna Rao S, Anvesh D Department of Surgery, Katuri Medical College
Research Article Acute Pancreatitis and its Clinical Study and Management in Amaravathi Region Satyanarayana Rao S V*, Babu Rao D, Krishna Rao S, Anvesh D Department of Surgery, Katuri Medical College
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
ACUTE PANCREATITIS IN BERGEN, NORWAY
 Scandinavian Journal of Surgery 93: 29 33, 2004 ACUTE PANCREATITIS IN BERGEN, NORWAY A study on incidence, etiology and severity H. Gislason 2, A. Horn 1, D. Hoem 1, Å. Andrén-Sandberg 1, A. K. Imsland
Scandinavian Journal of Surgery 93: 29 33, 2004 ACUTE PANCREATITIS IN BERGEN, NORWAY A study on incidence, etiology and severity H. Gislason 2, A. Horn 1, D. Hoem 1, Å. Andrén-Sandberg 1, A. K. Imsland
A Comparative Study of Different Predictive Severity Scoring Systems for Acute Pancreatitis in Relation To Outcome A Prospective Study
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 12 Ver. 2 (December. 2018), PP 01-09 www.iosrjournals.org A Comparative Study of Different
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 12 Ver. 2 (December. 2018), PP 01-09 www.iosrjournals.org A Comparative Study of Different
Setting The study setting was hospital. The economic analysis was carried out in California, USA.
 Preoperative versus postoperative endoscopic retrograde cholangiopancreatography in mild to moderate gallstone pancreatitis: a prospective randomized trial Chang L, Lo S, Stabile B E, Lewis R J, Toosie
Preoperative versus postoperative endoscopic retrograde cholangiopancreatography in mild to moderate gallstone pancreatitis: a prospective randomized trial Chang L, Lo S, Stabile B E, Lewis R J, Toosie
Case 7729 Child with choledochal cyst presenting with episodes of vomitting and jaundice
 Case 7729 Child with choledochal cyst presenting with episodes of vomitting and jaundice dos Santos R 1, Almeida J 1, Mendes PP 2, Pereira S 3, Borges C 3, Soares E 4. 1) Radiology resident, 2) Radiology
Case 7729 Child with choledochal cyst presenting with episodes of vomitting and jaundice dos Santos R 1, Almeida J 1, Mendes PP 2, Pereira S 3, Borges C 3, Soares E 4. 1) Radiology resident, 2) Radiology
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM
 A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
Chronic Pancreatitis
 Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Comparison of clinical course and outcome of acute pancreatitis according to the two main etiologies: alcohol and gallstone
 Cho et al. BMC Gastroenterology (2015) 15:87 DOI 10.1186/s12876-015-0323-1 RESEARCH ARTICLE Open Access Comparison of clinical course and outcome of acute pancreatitis according to the two main etiologies:
Cho et al. BMC Gastroenterology (2015) 15:87 DOI 10.1186/s12876-015-0323-1 RESEARCH ARTICLE Open Access Comparison of clinical course and outcome of acute pancreatitis according to the two main etiologies:
Original Article. Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome
 Tropical Gastroenterology 2015;36(1):31 35 Original Article Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome Surinder S Rana 1, Vishal Sharma 1, Deepak
Tropical Gastroenterology 2015;36(1):31 35 Original Article Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome Surinder S Rana 1, Vishal Sharma 1, Deepak
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
JMSCR Vol 04 Issue 08 Page August 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i8.08 Acute Pancreatitis with Normal Amylase
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i8.08 Acute Pancreatitis with Normal Amylase
USEFULNESS OF LIPASE / AMYLASE RATIO IN ACUTE PANCREATITIS IN SOUTH INDIAN POPULATION
 Indian Journal of Clinical Biochemistry, 2009 / 24 (4) 361-365 ORIGINAL ARTICLE USEFULNESS OF LIPASE / AMYLASE RATIO IN ACUTE PANCREATITIS IN SOUTH INDIAN POPULATION Anitha Devanath, Jaya Kumari, Jim Joe,
Indian Journal of Clinical Biochemistry, 2009 / 24 (4) 361-365 ORIGINAL ARTICLE USEFULNESS OF LIPASE / AMYLASE RATIO IN ACUTE PANCREATITIS IN SOUTH INDIAN POPULATION Anitha Devanath, Jaya Kumari, Jim Joe,
Pancreatitis. Acute Pancreatitis
 Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Prophylactic Antibiotics in Severe Acute Pancreatitis: Antibiotics are good. Karen Lo R 3 University of Colorado Oct 11, 2010
 Prophylactic Antibiotics in Severe Acute Pancreatitis: Antibiotics are good Karen Lo R 3 University of Colorado Oct 11, 2010 Overview Pancreas: The History Pancreas: The Organ The Disease Pathogenesis
Prophylactic Antibiotics in Severe Acute Pancreatitis: Antibiotics are good Karen Lo R 3 University of Colorado Oct 11, 2010 Overview Pancreas: The History Pancreas: The Organ The Disease Pathogenesis
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Acute Pancreatitis: Role of Imaging Modalities
 International Journal of Interdisciplinary and Multidisciplinary Studies (IJIMS), 2015, Vol 2, No.9,109-114. 109 Available online at http://www.ijims.com ISSN: 2348 0343 Abstract Acute Pancreatitis: Role
International Journal of Interdisciplinary and Multidisciplinary Studies (IJIMS), 2015, Vol 2, No.9,109-114. 109 Available online at http://www.ijims.com ISSN: 2348 0343 Abstract Acute Pancreatitis: Role
Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience
 Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
JMSCR Vol 05 Issue 03 Page March 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i3.177 Role of Serum Amylase and Lipase Levels
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i3.177 Role of Serum Amylase and Lipase Levels
Acute Pancreatitis: New Developments and Strategies for the Hospitalist
 REVIEWS Acute Pancreatitis: New Developments and Strategies for the Hospitalist John F. Dick, III, MD 1 *, Timothy B. Gardner, MD, MS 2, Edward J. Merrens, MD, MS 1 1 Geisel School of Medicine, Section
REVIEWS Acute Pancreatitis: New Developments and Strategies for the Hospitalist John F. Dick, III, MD 1 *, Timothy B. Gardner, MD, MS 2, Edward J. Merrens, MD, MS 1 1 Geisel School of Medicine, Section
Figure 2: Post-cholecystectomy biliary-like pain
 Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Lixin Yang, 1 Jing Liu, 2 Yun Xing, 1 Lichuan Du, 1 Jing Chen, 1 Xin Liu, 3 and Jianyu Hao Introduction. 2. Material and Method
 Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2016, Article ID 1834256, 7 pages http://dx.doi.org/10.1155/2016/1834256 Research Article Comparison of,,, and in Predicting
Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2016, Article ID 1834256, 7 pages http://dx.doi.org/10.1155/2016/1834256 Research Article Comparison of,,, and in Predicting
Acute Pancreatitis. Falk Symposium 161 Dresden
 Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
What Is Pancreatitis?
 What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
Disclosures. Overview. Case 1. Common Bile Duct Sizes 10/14/2016. General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis
 Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
A patient with an unusual congenital anomaly of the pancreaticobiliary tree
 A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
Genetic Testing for Hereditary Pancreatitis
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
Clinical Spectrum of Presentation of Obstructive Jaundice in Inflammation, Stone Disease, and Malignancy
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/326 Clinical Spectrum of Presentation of Obstructive Jaundice in Inflammation, Stone Disease, and Malignancy R Selvasekaran
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/326 Clinical Spectrum of Presentation of Obstructive Jaundice in Inflammation, Stone Disease, and Malignancy R Selvasekaran
Approach to the Patient with Liver Disease
 Approach to the Patient with Liver Disease Diagnosis of liver disease Careful history taking Physical examination Laboratory tests Radiologic examination and imaging studies Liver biopsy Liver diseases
Approach to the Patient with Liver Disease Diagnosis of liver disease Careful history taking Physical examination Laboratory tests Radiologic examination and imaging studies Liver biopsy Liver diseases
Classification of choledochal cyst with MR cholangiopancreatography in children and infants: special reference to type Ic and type IVa cyst
 Classification of choledochal cyst with MR cholangiopancreatography in children and infants: special reference to type Ic and type IVa cyst Poster No.: C-1333 Congress: ECR 2011 Type: Educational Exhibit
Classification of choledochal cyst with MR cholangiopancreatography in children and infants: special reference to type Ic and type IVa cyst Poster No.: C-1333 Congress: ECR 2011 Type: Educational Exhibit
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
Surveillance proposal consultation document
 Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Modified Computed Tomography Severity Index in Acute Pancreatitis - Its Correlation with Patient Morbidity (A Study of 40 Cases)
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/138 Modified Computed Tomography Severity Index in Acute Pancreatitis - Its Correlation with Patient Morbidity (A Study
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/138 Modified Computed Tomography Severity Index in Acute Pancreatitis - Its Correlation with Patient Morbidity (A Study
Cystic Biliary Atresia: Why Is It Important to Distinguish this from Congenital Choledochal Cyst?
 Bahrain Medical Bulletin, Vol. 36, No. 2, June 2014 Cystic Biliary Atresia: Why Is It Important to Distinguish this from Congenital Choledochal Cyst? Hussein Ahmed Mohammed Hamdy, MRCSEd, FEBPS* Hind Mustafa
Bahrain Medical Bulletin, Vol. 36, No. 2, June 2014 Cystic Biliary Atresia: Why Is It Important to Distinguish this from Congenital Choledochal Cyst? Hussein Ahmed Mohammed Hamdy, MRCSEd, FEBPS* Hind Mustafa
5.0 CLINICAL ASSESSMENT OF OED ACCURACY
 24 5.0 CLINICAL ASSESSMENT OF OED ACCURACY 5.1 Patients and methods 5.1.1 Study Design/Sampling A double-blind comparative study of OED results and clinical diagnoses, as a criterion standard, was performed
24 5.0 CLINICAL ASSESSMENT OF OED ACCURACY 5.1 Patients and methods 5.1.1 Study Design/Sampling A double-blind comparative study of OED results and clinical diagnoses, as a criterion standard, was performed
A comparative study of different predictive severity scoring system for acute pancreatitis in relation to outcome
 Research Article A comparative study of different predictive severity scoring system for acute pancreatitis in relation to outcome Sanjeeva Kumar Choudhary 1, Ved Rajan Arya 2*, Bhaskar Kumar 3, Md Sarfaraz
Research Article A comparative study of different predictive severity scoring system for acute pancreatitis in relation to outcome Sanjeeva Kumar Choudhary 1, Ved Rajan Arya 2*, Bhaskar Kumar 3, Md Sarfaraz
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010
 Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Original Article. Abstract. Introduction
 Original Article Role of Computed Tomography in Acute Pancreatitis and its Complications among Age Groups Ishtiaq Ahmed Chishty, Vaqar Bari, Sajida Pasha, Dawar Burhan, Zishan Haider, Zafar Rafique Radiology
Original Article Role of Computed Tomography in Acute Pancreatitis and its Complications among Age Groups Ishtiaq Ahmed Chishty, Vaqar Bari, Sajida Pasha, Dawar Burhan, Zishan Haider, Zafar Rafique Radiology
Peering Into the Black Box of the Complex Chronic Pancreatitis Syndrome
 PancreasFest 2017 Precision Medicine Approach For Benign Pancreatic Disease Friday, July 28, 2017 Peering Into the Black Box of the Complex Chronic Pancreatitis Syndrome David C Whitcomb MD PhD Director,
PancreasFest 2017 Precision Medicine Approach For Benign Pancreatic Disease Friday, July 28, 2017 Peering Into the Black Box of the Complex Chronic Pancreatitis Syndrome David C Whitcomb MD PhD Director,
Original Policy Date 12:2013
 MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
Acute Necrotizing Pancreatitis: Laboratory, Clinical, and Imaging Findings as Predictors of Patient Outcome
 Gastrointestinal Imaging Original Research Brand et al. Acute Necrotizing Pancreatitis Gastrointestinal Imaging Original Research Michael Brand 1 Andrea Götz 1 Florian Zeman 2 Gundula Behrens 3 Michael
Gastrointestinal Imaging Original Research Brand et al. Acute Necrotizing Pancreatitis Gastrointestinal Imaging Original Research Michael Brand 1 Andrea Götz 1 Florian Zeman 2 Gundula Behrens 3 Michael
Serum Lipase Amylase Ratio in Predicting Aetiology, Severity and Outcome of Acute Pancreatitis in a Tertiary Care Hospital
 Original Article Serum Lipase Amylase Ratio in Predicting Aetiology, Severity and Outcome of Acute Pancreatitis in a Tertiary Care Hospital Majharul Haque 1*, Golam Azam 2*, Debashis Kumar Sarkar 3, Anisur
Original Article Serum Lipase Amylase Ratio in Predicting Aetiology, Severity and Outcome of Acute Pancreatitis in a Tertiary Care Hospital Majharul Haque 1*, Golam Azam 2*, Debashis Kumar Sarkar 3, Anisur
The Bile Duct (and Pancreas) and the Physician
 The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Unresolved Issues about Post-ERCP Pancreatitis: An Overview
 Unresolved Issues about Post-ERCP Pancreatitis: An Overview Pier Alberto Testoni Division of Gastroenterology and Gastrointestinal Endoscopy, University Vita-Salute San Raffaele, IRCCS San Raffaele Hospital.
Unresolved Issues about Post-ERCP Pancreatitis: An Overview Pier Alberto Testoni Division of Gastroenterology and Gastrointestinal Endoscopy, University Vita-Salute San Raffaele, IRCCS San Raffaele Hospital.
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Appendix A: Summary of evidence from surveillance
 Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
ENDOSCOPIC TREATMENT OF A BILE DUCT
 HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Acute Pancreatitis in Pediatric Patients: Demographics, Etiology, and Diagnostic Imaging
 Pediatric Imaging Review Restrepo et al. cute Pancreatitis in Pediatric Patients Pediatric Imaging Review Ricardo Restrepo 1 Heidi E. Hagerott 2 Sakil Kulkarni 2 Mona Yasrebi 3 Edward Y. Lee 4 Restrepo
Pediatric Imaging Review Restrepo et al. cute Pancreatitis in Pediatric Patients Pediatric Imaging Review Ricardo Restrepo 1 Heidi E. Hagerott 2 Sakil Kulkarni 2 Mona Yasrebi 3 Edward Y. Lee 4 Restrepo
Is Complicated Gallstone Disease Preceded by Biliary Colic?
 J Gastrointest Surg (2009) 13:312 317 DOI 10.1007/s11605-008-0729-y ORIGINAL ARTICLE Is Complicated Gallstone Disease Preceded by Biliary Colic? Marc G. Besselink & Niels G. Venneman & Peter M. Go & Ivo
J Gastrointest Surg (2009) 13:312 317 DOI 10.1007/s11605-008-0729-y ORIGINAL ARTICLE Is Complicated Gallstone Disease Preceded by Biliary Colic? Marc G. Besselink & Niels G. Venneman & Peter M. Go & Ivo
Acute Pancreatitis:
 American College of Gastroenterology 2014 Acute Pancreatitis Scott Tenner, MD, MPH, FACG Clinical Professor of Medicine State University of New York Health Sciences Center Director, Brooklyn Gastroenterology
American College of Gastroenterology 2014 Acute Pancreatitis Scott Tenner, MD, MPH, FACG Clinical Professor of Medicine State University of New York Health Sciences Center Director, Brooklyn Gastroenterology
Cause of Acute Pancreatitis in A Case
 2008 19 531-535 Pancreas Divisum An Infrequent Cause of Acute Pancreatitis in A Case Cheuk-Kay Sun 1, Jui-Hao Chen 1, Kuo-Ching Yang 1, and Chin-Chu Wu 2 1 Division of Gastroenterology, Department of Internal
2008 19 531-535 Pancreas Divisum An Infrequent Cause of Acute Pancreatitis in A Case Cheuk-Kay Sun 1, Jui-Hao Chen 1, Kuo-Ching Yang 1, and Chin-Chu Wu 2 1 Division of Gastroenterology, Department of Internal
Patients With Severe Acute Pancreatitis Should Be More Often Treated In An Intensive Care Department
 ISPUB.COM The Internet Journal of Emergency and Intensive Care Medicine Volume 6 Number 2 Patients With Severe Acute Pancreatitis Should Be More Often Treated In An Intensive Care Department M Dinis-Ribeiro,
ISPUB.COM The Internet Journal of Emergency and Intensive Care Medicine Volume 6 Number 2 Patients With Severe Acute Pancreatitis Should Be More Often Treated In An Intensive Care Department M Dinis-Ribeiro,
A retrospective study of acute pancreatitis in patients with hemorrhagic fever with renal syndrome
 Zhu et al. BMC Gastroenterology 2013, 13:171 RESEARCH ARTICLE Open Access A retrospective study of acute pancreatitis in patients with hemorrhagic fever with renal syndrome Yin Zhu, You-Xiang Chen, Yong
Zhu et al. BMC Gastroenterology 2013, 13:171 RESEARCH ARTICLE Open Access A retrospective study of acute pancreatitis in patients with hemorrhagic fever with renal syndrome Yin Zhu, You-Xiang Chen, Yong
Provider Led Entity. CDI Quality Institute PLE Nontraumatic Abdominal Pain AUC
 Provider Led Entity CDI Quality Institute PLE Nontraumatic Abdominal Pain AUC Appropriateness of advanced imaging procedures* in patients with nontraumatic abdominal pain and the following clinical presentations
Provider Led Entity CDI Quality Institute PLE Nontraumatic Abdominal Pain AUC Appropriateness of advanced imaging procedures* in patients with nontraumatic abdominal pain and the following clinical presentations
International Journal of Medicine & Health Research. Research Article
 www.advancejournals.org Open Access Scientific Publisher Research Article A RANDOMISED CONTROL STUDY ON EFFECT OF OCTREOTIDE IN MANAGEMNT OF ACUTE PANCREATITIS WITH VARYING SEVERITIES Susnata De,Soumen
www.advancejournals.org Open Access Scientific Publisher Research Article A RANDOMISED CONTROL STUDY ON EFFECT OF OCTREOTIDE IN MANAGEMNT OF ACUTE PANCREATITIS WITH VARYING SEVERITIES Susnata De,Soumen
Updated Imaging Nomenclature for Acute Pancreatitis
 Residents Section Structured Review Murphy et al. Imaging Nomenclature for Acute Pancreatitis Residents Section Structured Review Residents inradiology Kevin P. Murphy 1,2 Owen J. O Connor 1,2 Michael
Residents Section Structured Review Murphy et al. Imaging Nomenclature for Acute Pancreatitis Residents Section Structured Review Residents inradiology Kevin P. Murphy 1,2 Owen J. O Connor 1,2 Michael
Pancreatic Diseases. Michael J. Lentze ESPGHAN goes Africa Course March Bonn. Tbilisi/Georgia
 Pancreatic Diseases Michael J. Lentze ESPGHAN goes Africa Course March 2015 Bonn Tbilisi/Georgia Bonn - Germany Georgia Georgia 4 year old Girl: Isabell 2nd child of healthy parents, pregnancy and delivery
Pancreatic Diseases Michael J. Lentze ESPGHAN goes Africa Course March 2015 Bonn Tbilisi/Georgia Bonn - Germany Georgia Georgia 4 year old Girl: Isabell 2nd child of healthy parents, pregnancy and delivery
