Teicoplanin Dosing Strategy for Treatment of Staphylococcus aureus in Korean Patients with Neutropenic Fever
|
|
|
- Arleen Ward
- 6 years ago
- Views:
Transcription
1 Original Article DOI /ymj pissn: , eissn: Yonsei Med J 52(4): , 2011 Teicoplanin Dosing Strategy for Treatment of Staphylococcus aureus in Korean Patients with Neutropenic Fever Byung-Jin Ahn, 1 Dong-Seok Yim, 2 Dong-Gun Lee, 3 Jae-Cheol Kwon, 3 Si-Hyun Kim, 3 and Su-Mi Choi 3 1 Department of Medicine, Graduate School, Dongguk University, Seoul; Departments of 2 Pharmacology, 3 Internal Medicine, College of Medicine, The Catholic University of Korea, Seoul, Korea. Received: July 7, 2010 Revised: September 20, 2010 Accepted: October 12, 2010 Corresponding author: Dr. Dong-Gun Lee, Department of Internal Medicine, College of Medicine, The Catholic University of Korea, 505 Banpo-dong, Seocho-gu, Seoul , Korea. Tel: , Fax: symonlee@catholic.ac.kr A part of this manuscript was presented at the American Society for Clinical Pharmacology and Therapeutics 2009 annual meeting held in National Harbor, MD, USA. The authors have no financial conflicts of interest. Purpose: The present study was conducted to determine and compare the target attainment rate (TAR) between microorganism-nonspecific (C trough ) and microorganism-specific (AUC 24 /MIC) targets over two weeks of teicoplanin administration according to several dose regimens for the treatment of Staphylococcus aureus in Korean patients with neutropenic fever. Materials and Methods: One thousand virtual concentrations were obtained for each dose using the population pharmacokinetic parameters of teicoplanin adopted from a published study. Simulation of 1,000 virtual MICs was performed using the MICs of 78 clinical isolates of S. aureus collected from a hospital in Korea. Thereafter, these simulated MICs were randomly allocated to 1,000 virtual patients in whom the TARs for AUC 24 /MIC >125 [or 345] and C trough >10 [or 20] mg/l were determined. The relationship of the maintenance dose with the steady-state TAR was predicted with respect to the AUC 24 /MIC >125 [or 345] using logistic analysis. Results: The standard dose regimen of teicoplanin showed TARs of about 70% [or 33%] and 70% [or 20%] at steady-state in cases with AUC 24 /MIC >125 [or 345] and C trough >10 [or 20] mg/l, respectively. Conclusion: The current standard dose regimen was predicted to be insufficient to adequately treat S. aureus in Korean patients with neutropenic fever. To assure at least an 80% TAR in this population, dose adjustment of teicoplanin should be considered. Key Words: Teicoplanin, Staphylococcus aureus, neutropenia, pharmacokinetics, pharmacodynamics INTRODUCTION Copyright: Yonsei University College of Medicine 2011 This is an Open Access article distributed under the terms of the Creative Commons Attribution Non- Commercial License ( licenses/by-nc/3.0) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Teicoplanin, one of the glycopeptide antibiotics, is primarily active against Grampositive microorganisms including Staphylococcus, Streptococcus, and Enterococcus species. During chemotherapy for hematologic malignancies, Gram-positive bacterial infections are a common cause of neutropenic fever in Korea as well as in western countries. 1,2 Teicoplanin is known to have bi- to tri-exponential distribution features and a 616 Yonsei Med J Volume 52 Number 4 July 2011
2 Teicoplanin for S. aureus in Neutropenic Fever longer elimination half-life than vancomycin, which makes its once daily administration possible. It is also generally accepted that teicoplanin with a trough concentration (C trough ) >10 mg/l is clinically effective; to ensure this trough concentration, a dose regimen of 6 mg/kg (400 mg) every 12 hours for 3 doses, then daily, are the minimal requirements for all patients with normal renal function, and a C trough of 20 mg/l should be exceeded in cases of deep-seated staphylococcal infections. 3,4 Moreover, according to Harding, et al., 5 the mean trough concentration was correlated with the clinical outcome of patients with Staphylococcus aureus septicemia. MacGowan, et al. 6 also demonstrated that the C trough >10 mg/l and C trough >20 mg/l of teicoplanin were related to favorable outcomes and curing of staphylococcal infections, respectively. Dose regimens based upon trough concentrations have not considered the microorganism-specific factors. For the appropriate use of an antimicrobial agent, physicians should be aware of microorganism-specific as well as patient-specific factors. To do this, a clear relationship between pharmacokinetic (PK) and pharmacodynamic (PD) interaction of antimicrobial agents must be elucidated. The minimum inhibitory concentration (MIC) is one of the microorganism related factors that requires consideration when determining treatment doses and durations for the best clinical outcome. 7 In the case of glycopeptides, the AUC 24 (area under the drug concentration-time curve during 24 hr) over the MIC i.e., AUC 24 /MIC that associates drug exposure with the characteristics of the microorganism has recently come into use as a surrogate marker of clinical efficacy. However, there has been some debate as to the optimal level of this target for treatment using teicoplanin. Although the AUC 24 /MIC >125 has been regarded as a PK-PD marker that can predict clinical success with vancomycin treatment, 7,8 a level of AUC 24 /MIC >345 have recently been recommended as the target to be attained. 9,10 However, the AUC 24 /MIC target values for teicoplanin treatment have not been extensively studied. Therefore, clinicians have adopted those from vancomycin with the rationale that both antibiotics belong to the same glycopeptide class. In this context, the present study was performed to assess the target attainment rate (TAR) for microorganism-nonspecific (C trough ) and microorganism-specific (AUC 24 /MIC) targets during two weeks of teicoplanin administration for the treatment of S. aureus strains in Korean patients with neutropenic fever under several dose regimens. MATERIALS AND METHODS Teicoplanin susceptibility test of S. aureus A total of 78 non-duplicate clinical isolates of S. aureus from patients with neutropenic fever at the Catholic Hematopoietic Stem Cell Transplantation (HSCT) Center were collected between 2005 and 2007 for this study. Most of these isolates were recovered from blood, wound, or purulent discharge. Specimens with possible contaminants or colonization were all excluded. Cation-adjusted Mueller-Hinton agar (Difco laboratories, Detroit, MI, USA) was used for tests of teicoplanin susceptibility. The method used for agar dilution was based on the protocol published by the Clinical Laboratory Standards Institute for the MIC. 11 The inoculation concentration was CFU/mL and the standard strain used for quality control was S. aureus ATCC The MICs at which 50% and 90% of the clinical isolates were inhibited were defined as MIC 50 and MIC 90, respectively. A frequency distribution profile was used as PD data for the clinical trial simulation. This study was approved by the Institutional Review Board of Yeouido St. Mary's Hospital, College of Medicine, The Catholic University of Korea (Protocol No. GAEUISUNG-1961, Jul/14/2003). Population PK model and simulation Population PK parameters of teicoplanin were adopted from a published study on neutropenic patients with hematological malignancies because the pharmacokinetic data of teicoplanin from Korean patients were not available. 12 From V1 (central volume of distribution), V2 (peripheral volume of distribution), Q (distribution clearance), and CL (elimination clearance) values and their distribution, 1,000 concentration-time profiles for 14 days were generated according to several dose regimens using NONMEM (Version 6.1, Icon Development Solutions, Ellicott City, MD, USA). The dose regimens to be considered for clinical application were as follows: 1) 400 mg single dose then, 200 mg once a day, by intravenous injection (iv) 2) 400 mg every 12 hr for 3 doses then, 400 mg once a day, iv (standard regimen) 3) 600 mg every 12 hr for 3 doses then, 400 mg once a day, iv 4) 800 mg every 12 hr for 3 doses then, 400 mg once a day, iv 5) 400 mg every 12 hr for 3 doses then, 400 mg twice a Yonsei Med J Volume 52 Number 4 July
3 Byung-Jin Ahn, et al. Target attainment rate under several dosing scenarios The standard dosing regimen (400 mg every 12 hr for 3 doses, then 400 mg once a day, iv) recommended by the summary in the package insert of teicoplanin for severe infections has a TAR of about 70% under steady-state (SS) conditions when C trough >10 mg/l and AUC 24 /MIC >125 were used as the therapeutic targets of teicoplanin. Howevday, iv After 1,000 virtual concentrations were obtained, for each dose scheme, the areas under the curve (AUC) were calculated from day 1 to day 14 using non-compartmental analysis with the linear trapezoidal method. Covariate effects were not considered. Simulation of MIC distribution Because we could not define appropriate distribution models for the histogram of MICs for S. aureus isolated from a single HSCT center, simple discrete proportions, as observed in the MIC test histograms, were used instead of assuming any distribution model for simulation of 1,000 virtual MICs. Thereafter, these 1,000 simulated MICs were randomly allocated to the above 1,000 simulated patients. variable because the outcome was a categorical variable. The logit (P=proportion of target attainment failure at day 7) meant the log (odds of target attainment failure) and the odds of target attainment failure was defined as P/(1-P). A logistic regression analysis was then performed using NON- MEM and the logit (P) was back-transformed with the exponential and P (proportion of target attainment failure) for each dose was calculated as follows; EXP (logit (P)) P = 1+EXP (logit (P)) With this information the dose - response (TAR) relationships could be predicted. Fig. 1 summarizes the main steps taken in the present study to elucidate the dose-response relationships of teicoplanin against Staphylococcus aureus in Korean patients with neutropenic fever. Pharmacodynamic assessment In each of the 1,000 virtual patients, attainment of microorganism-specific and nonspecific targets (AUC 24 /MIC >125 [or 345], C trough >10 [or 20] mg/l) were determined for each dosing regimen. Thereafter, we calculated the TAR (proportions of patients showing target attainment among 1,000 virtual patients) during two week dosing periods. The AUC 24 / MIC >345 and AUC 24 /MIC >125 among the above targets were chosen to determine the relationship of the maintenance dose with a steady-state TAR, after seven days of teicoplanin administration because these targets were thought to be the surrogate marker for clinical outcomes considered with microorganism specific factors. While the AUC 24 /MIC >345 [or 125] was used as a target value, the logit (P=proportion of target attainment failure at day 7) was set as an outcome variable and the log (maintenance dose) values as a predictor RESULTS MIC frequency distribution The MIC 50 and MIC 90 of teicoplanin for the S. aureus clinical isolates were 2 and 8 mg/l, respectively. Fig. 2 illustrates the frequency distribution of teicoplanin MICs for 78 clinical isolates of S. aureus. PK model & parameters from a literature MICs Data (n=78) Virtual patients with AUCs (n=1,000) Linkage Virtual MICs (n=1,000) Microorganism-specific target: AUC24/MIC >125 (or 345) Microorganism-non specific target: Ctrough >10 (or 20) mg/l Dose regimens Response: TAR Dose-response relationship Response: TAR Dose regimens Fig. 1. Summarized study flow to determine the dose-response relationship of teicoplanin against S. aureus in febrile neutropenic Korean patients. PK, pharmacokinetic; AUC, area under the curve; MIC, minimum inhibitory concentration. 618 Yonsei Med J Volume 52 Number 4 July 2011
4 Teicoplanin for S. aureus in Neutropenic Fever er, with an AUC 24 /MIC >345, only 33% of all patients with staphylococcal infection attained the target. When C trough >20 mg/l was used as a MIC-nonspecific target, less than 20% of all patients with the adopted PK parameter distributions achieved the target under SS conditions. Even though a 400 mg twice daily dose was given for maintenance, only 65% achieved a SS-TAR. Table 1 and Fig. 3 show the TARs according to several therapeutic targets with several different dosing schemes over two weeks of teicoplanin administration. Dose-response relationships According to several dosing scenarios the logistic regression models were analyzed with the following equation: Logit (AUC 24 /MIC <345)= log (maintenance dose) Logit (AUC 24 /MIC <125)= log (maintenance dose) The dose-response (TAR) relationships observed are shown in Fig. 4. For each dosing regimen, the ED 50, defined as a maintenance dose where 50% of TAR was achieved, was around 200 and 600 mg/day in the AUC 24 /MIC >125 and AUC 24 /MIC >345 targets, respectively. Since the logit (P=proportion of target attainment failure at day 7) meant the log (odds of target attainment failure) and the odds of target attainment failure was defined as P/(1-P), logit AUC 24 /MIC <345 or 125) equaled zero at the ED 50 and ED 50 for each target was thereafter calculated as follows: 0= log (ED 50 ) (for the AUC 24 /MIC >345 target) 0= log (ED 50 ) (for the AUC 24 /MIC >125 target) When the overall clinical success was arbitrarily defined as when 80% of the patients with S. aureus infections causing Frequency (n) Teicoplanin MIC (µg/ml) Fig. 2. Frequency distribution of teicoplanin MIC for 78 S. aureus isolates from patients with neutropenic fever patients at the Catholic hematopoietic stem cell transplantation center, Seoul, Korea through MIC, minimum inhibitory concentration Table 1. Rates of Therapeutic Target Attainment Under Several Dosing Scenario in a Population Having High MIC Values for Teicoplanin Dosing regimen Therapeutic target Teicoplanin administration period Ctrough >10 mg/l mg single dose Ctrough >20 mg/l then 200 mg q 24 hr AUC24/MIC > AUC24/MIC > Ctrough >10 mg/l mg q 12 hr for 3 doses Ctrough >20 mg/l then 400 mg q 24 hr AUC24/MIC > AUC24/MIC > Ctrough >10 mg/l mg q 12 hr for 3 doses Ctrough >20 mg/l then 400 mg q 24 hr AUC24/MIC > AUC24/MIC > Ctrough >10 mg/l mg q 12 hr for 3 doses Ctrough >20 mg/l then 400 mg q 24 hr AUC24/MIC > AUC24/MIC > Ctrough >10 mg/l mg q 12 hr for 3 doses Ctrough >20 mg/l then 400 mg q 12 hr AUC24/MIC > AUC24/MIC > MIC, minimum inhibitory concentration; AVC, area under the curve. Yonsei Med J Volume 52 Number 4 July
5 Byung-Jin Ahn, et al. Ctrough >10 mg/l AUC24/MIC > Time (day) Time (day) Ctrough >20 mg/l AUC24/MIC >345 Time (day) Time (day) Fig. 3. TARs according to several therapeutic targets with several dosing schemes during 2 weeks of teicoplanin administration; TAR for Ctrough >10 mg/l, Ctrough >20 mg/l, AUC24/MIC >125 and AUC24/MIC >345. TAR, target attainment rate; AUC, area under the curve; MIC, minimum inhibitory concentration mg single dose then, 200 mg q 24 hr 400 mg q 12 hr for 3 doses then, 400 mg q 24hr 600 mg q 12 hr for 3 doses then, 400 mg q 24hr 800 mg q 12 hr for 3 doses then, 400 mg q 24hr 400 mg q 12 hr for 3 doses then, 400 mg q 12hr ,000 1,100 1,200 1,300 1,400 1,500 1,600 Maintenance dose (mg) Fig. 4. Maintenance dose - response (TAR) relationships obtained from logistic regression; ED50, defined as a maintenance dose where 50% TAR was achieved; TAR for AUC24/MIC >345 (open circle) or 125 (closed rectangle). TAR, target attainment rate; AUC, area under the curve; MIC, minimum inhibitory concentration. neutropenia reached the target, the maintenance dose for overall clinical success was predicted to be about 540 and 1,000 mg/day in the AUC 24 /MIC >125 and AUC 24 /MIC >345 targets, respectively, and the maintenance dose for each target was obtained as follows: Log (0.2/(1-0.2))= log (maintenance dose) (for the AUC 24 /MIC >345 target) Log (0.2/(1-0.2))= log (maintenance dose) (for the AUC 24 /MIC >125 target) DISCUSSION According to a recent meta-analysis of 24 randomized controlled trials that compared vancomycin to teicoplanin, there were no significant differences between teicoplanin and vancomycin in terms of efficiency outcomes, such as clinical and microbiological failure rate; however, teicoplanin was associated with a lower occurrence of adverse 620 Yonsei Med J Volume 52 Number 4 July 2011
6 Teicoplanin for S. aureus in Neutropenic Fever events than vancomycin. 13 Although teicoplanin has been widely used for infections associated with hematological malignancies in Korea, due to its low rate of adverse drug reactions, a population-specific optimum dose regimen has not been established with respect to its association with the PK/PD. Therefore, the goal of this study was to determine the appropriate teicoplanin-dosing strategy for adequate treatment of S. aureus in Korean patients with neutropenic fever. To determine the effective dose regimen, validated endpoints or surrogate markers for clinical success or failure are required. In the case of teicoplanin, the trough concentration and AUC 24 /MIC are considered as microorganism-nonspecific and microorganism-specific markers, respectively. Moreover, the time to achieve a target value for the above marker must also be considered to associate the above markers with the clinical outcome. Because the loading dose could be readily determined from the maintenance dose using PK principles, for simplicity, the TAR with regard to the maintenance dose was studied. Both the trough concentration and AUC 24 /MIC are associated with the PK properties of a specific population, i.e., patients with neutropenic fever that have hematological malignancies. While the trough concentration is directly related to the dose regimen and the patient pharmacokinetics, for the AUC 24 /MIC, the MIC value for the microorganism has to be considered as well. In a study reported by Whitehouse, et al. 14 on teicoplanin PK in critically ill patients with renal impairment, the trough concentrations were not significantly different in the patients that were cured (mean mg/l) and in those that failed to respond to treatment (mean mg/l). According to Gimenez, et al., 15 eight out of 10 patients had trough concentration values below 10 mg/l at 48 hrs after a standard regimen treatment of patients with neutropenia due to underlying hematological disease. The initial inadequate concentrations during the first few days of therapy may affect the outcome of teicoplanin therapy with regard to the emergence of resistant microorganisms, and thus subtherapeutic concentrations should be avoided. 16 Especially in the critically ill patient setting, loading doses of teicoplanin (6 mg/kg every 12 hrs for at least three doses) should be considered mandatory in all patients and individually optimized dose regimens optimized. In addition, drug level monitoring is important during treatment. 17 Lothorary, et al. 12,18 reported that patients with neutropenic fever have an increased distribution and elimination clearance without significant changes in the volume of dis- tribution, as compared to healthy controls. Therefore, in this specific population, the trough concentration was associated with increased clearance and higher initial doses are required; administration of 6 mg/kg teicoplanin given every 12 hr for five doses ensured a mean trough serum concentration of 16.0 mg/l, with a trough concentration below 10 mg/l in 7% of patients, compared with 46% of patients on a regimen of teicoplanin given only four times during the first 48 h. According to Pea, et al., 19 to ensure early therapeutically effective trough concentrations (more than 10 mg/l at 24 h) in patients with acute leukemia, a high loading regimen (800 mg+400 mg 12 hr apart on day 1,600 mg +400 mg 12 hr apart on day 2) followed by a high maintenance regimen (400 mg every 12 hr from day 3 on) showed successful attainment of the initial target. It is known that glycopeptide antibiotics have a time-dependent killing pattern and moderate post-antibiotic effects. Thus, the ideal dosing regimen for a glycopeptide should be designed to maximize the amount of drug received. The AUC 24 /MIC value could be used as the surrogate parameter associated with clinical efficacy. Unfortunately, PD data and AUC 24 /MIC target value are not available for teicoplanin. Therefore, the values known for the vancomycin target value were adopted. Although past recommendations had indicated that at least an AUC 24 /MIC >125 was necessary for vancomycin, recent studies recommend an AUC 24 /MIC >345 or Rybak, et al. 24 recommended that, for complicated infections caused by S. aureus, trough vancomycin concentrations of mg/l should be obtained and the range should achieve an AUC/MIC >400 for most patients if the MIC is <1 mg/l. However, an AUC/MIC of >400 is not attainable with conventional doses when the MIC is more than 2 mg/l in patients with normal renal function. In that situation, alternative therapies should be considered. Therefore, it is predicted that if the present study chose an AUC 24 / MIC >400 as an attainable target, the TARs would show lower values than noted in the present results and larger teicoplanin doses would be needed for a favorable clinical outcome in this specific patient population with neutropenic fever. However, when the present study results were compared to clinical results from a study conducted at the same institution in which the clinical and microbiological response in febrile neutropenic patients were 53.3% and 62.5% for 200 mg/day maintenance dose regimen, the results using AUC 24 /MIC >125 target was more consistent with clinical results than those from the AUC 24 /MIC >345 target. 2 Based upon this correlation between AUC 24 /MIC >125 target and Yonsei Med J Volume 52 Number 4 July
7 Byung-Jin Ahn, et al. 1. Park SH, Choi SM, Lee DG, Choi JH, Yoo JH, Lee JW, et al. Current trends of infectious complications following hematopoietic stem cell transplantation in a single center. J Korean Med Sci 2006;21: Lee DG, Yim DS, Choi SM, Park SH, Yoo JH, Choi JH, et al. Efficacies of teicoplanin in patients with febrile neutropenia. Infect Chemother 2004;36: Wilson AP. Clinical pharmacokinetics of teicoplanin. Clin Pharmacokinet 2000;39: MacGowan AP. Pharmacodynamics, pharmacokinetics, and therapeutic drug monitoring of glycopeptides. Ther Drug Monit 1998; 20: Harding I, MacGowan AP, White LO, Darley ES, Reed V. Teicoplanin therapy for Staphylococcus aureus septicaemia: relationship between pre-dose serum concentrations and outcome. J Antimicrob Chemother 2000;45: MacGowan AP, White LO, Reeves D, Harding I. Retrospective review of serum teicoplanin concentrations in clinical trials and their relationship to clinical outcome. J Infect Chemother 1996;2: Hyatt JM, McKinnon PS, Zimmer GS, Schentag JJ. The importance of pharmacokinetic/pharmacodynamic surrogate markers to outcome. Focus on antibacterial agents. Clin Pharmacokinet 1995; 28: Korting HC, Schäfer-Korting M, The benefit/risk ratio: a handbook for the rational use of potentially hazardous drugs. Boca Raton: CRC Press; Moise PA, Forrest A, Bhavnani SM, Birmingham MC, Schentag JJ. Area under the inhibitory curve and a pneumonia scoring system for predicting outcomes of vancomycin therapy for respiratory infections by Staphylococcus aureus. Am J Health Syst Pharm 2000;57 Suppl 2:S Craig WA. Basic pharmacodynamics of antibacterials with clinical applications to the use of beta-lactams, glycopeptides, and linezolid. Infect Dis Clin North Am 2003;17: Clinical and Laboratory Standards Institute Performance standards for antimicrobial susceptibility testing. Sixteenth inforclinical results, it might be inferred that to achieve 80% TAR, about 540 mg/day of teicoplanin would be required, and a corresponding adjustment of the standard dose regimen to 400 mg/day as a maintenance dose would be considered. The MIC of teicoplanin for 90% of strains (MIC 90 ) of S. aureus was reported to be below 1 mg/l 3, while the MIC 90 for S. aureus isolated from our HSCT center in this study was about 8-fold higher. Usual practice in Korea has been limited to low doses (400 mg single dose, then 200 mg once a day for empirical therapy; or 400 mg every 12 hrs for 3 doses, then 400 mg once a day for targeted therapy) due to the reimbursement system, which may contribute to the high MIC value for S. aureus. Kuti, et al. 25 reported that a dose of 400 mg every 24 hr achieved a trough value >10 mg/l in 46.3% of the population studied. This would be similar to a 50% likelihood of a total AUC/MIC ratio >345 at an MIC of 1 mg/l. Similarly, the 800 mg dose achieved the target trough and AUC/MIC ratios in 83% and 94% of the population, respectively. In the present study, due to the high frequency of MIC >1 mg/l, the AUC 24 /MIC >345 was not associated with MIC-nonspecific targets. The results of the present study show that TARs at SS were only related to maintenance doses due to the PK properties of the PK/PD marker. With respect to the C trough >10 mg/l target, the standard recommended regimen, i.e., 400 mg q 12 hr iv for 3 doses then 400 mg once a day, showed that the current loading dose was insufficient to achieve SS- TAR during the early period of treatment in neutropenic patients. However, in the case of the AUC 24 /MIC, TAR achieved an earlier SS-TAR with the standard regimen compared to the MIC-nonspecific targets. The logistic regression analysis for TAR of AUC 24 /MIC ratio >345 with log (maintenance dose), suggested a higher dose was required than in previous reports for an adequate clinical success rate in the patient population. With respect to the emergence of resistance, the MIC breakpoint or dose regimen needs to be adjusted; however, there has been no definite consensus or guidelines established to date. 26 In conclusion, the current standard dose regimen (400 mg q 12 hr for 3 doses then, 400 mg once a day, iv) is predicted to be insufficient to treat S. aureus in Korean patients with neutropenic fever when the AUC 24 /MIC >345 was chosen as a PK/PD target to predict the clinical outcome. To assure at least an 80% TAR in this population, over 1,000 mg/ day of teicoplanin as a maintenance dose is required and dose adjustment of teicoplanin would be considered. The limitations of the present study were that PK parameters from the literature were adopted instead of being based on the values of the patients in the study and the MIC values from single hospital in Korea were used. Therefore, additional well-designed prospective PK/PD outcome studies are needed to guide the optimal dosing regimens for specific patient populations. ACKNOWLEDGEMENTS This study was supported by a grant from the Korea Health 21 R&D Project (A060093), Ministry of Health and Welfare, Republic of Korea. REFERENCES 622 Yonsei Med J Volume 52 Number 4 July 2011
8 Teicoplanin for S. aureus in Neutropenic Fever mational supplement. Approved standard M100-S16. CLSI, Wayne, PA. 12. Lortholary O, Tod M, Rizzo N, Padoin C, Biard O, Casassus P, et al. Population pharmacokinetic study of teicoplanin in severely neutropenic patients. Antimicrob Agents Chemother 1996;40: Svetitsky S, Leibovici L, Paul M. Comparative efficacy and safety of vancomycin versus teicoplanin: systematic review and metaanalysis. Antimicrob Agents Chemother 2009;53: Whitehouse T, Cepeda JA, Shulman R, Aarons L, Nalda-Molina R, Tobin C, et al. Pharmacokinetic studies of linezolid and teicoplanin in the critically ill. J Antimicrob Chemother 2005;55: Gimenez F, Leblond V, Nguyen J, Serrand P, Binet JL, Grosset J, et al. Variations of teicoplanin concentrations in neutropenic patients. J Clin Pharm Ther 1997;22: Schentag JJ. Antimicrobial management strategies for Gram-positive bacterial resistance in the intensive care unit. Crit Care Med 2001;29:N Pea F, Brollo L, Viale P, Pavan F, Furlanut M. Teicoplanin therapeutic drug monitoring in critically ill patients: a retrospective study emphasizing the importance of a loading dose. J Antimicrob Chemother 2003;51: Lortholary O, Lefort A, Tod M, Chomat AM, Darras-Joly C, Cordonnier C. Pharmacodynamics and pharmacokinetics of antibacterial drugs in the management of febrile neutropenia. Lancet Infect Dis 2008;8: Pea F, Viale P, Candoni A, Pavan F, Pagani L, Damiani D, et al. Teicoplanin in patients with acute leukaemia and febrile neutropenia: a special population benefiting from higher dosages. Clin Pharmacokinet 2004;43: Van Bambeke F. Glycopeptides in clinical development: pharmacological profile and clinical perspectives. Curr Opin Pharmacol 2004;4: McKinnon PS, Davis SL. Pharmacokinetic and pharmacodynamic issues in the treatment of bacterial infectious diseases. Eur J Clin Microbiol Infect Dis 2004;23: Moise-Broder PA, Forrest A, Birmingham MC, Schentag JJ. Pharmacodynamics of vancomycin and other antimicrobials in patients with Staphylococcus aureus lower respiratory tract infections. Clin Pharmacokinet 2004;43: Stass H, Dalhoff A. The integrated use of pharmacokinetic and pharmacodynamic models for the definition of breakpoints. Infection 2005;33 Suppl 2: Rybak MJ, Lomaestro BM, Rotschafer JC, Moellering RC, Craig WA, Billeter M, et al. Vancomycin therapeutic guidelines: a summary of consensus recommendations from the infectious diseases Society of America, the American Society of Health-System Pharmacists, and the Society of Infectious Diseases Pharmacists. Clin Infect Dis 2009;49: Kuti JL, Kiffer CR, Mendes CM, Nicolau DP. Pharmacodynamic comparison of linezolid, teicoplanin and vancomycin against clinical isolates of Staphylococcus aureus and coagulase-negative staphylococci collected from hospitals in Brazil. Clin Microbiol Infect 2008;14: Weinbren M, Struthers K. Emergence of Staphylococcus aureus (MRSA) with reduced susceptibility to teicoplanin during therapy. J Antimicrob Chemother 2002;50: Yonsei Med J Volume 52 Number 4 July
prophylaxis for endocarditis in patients at high risk prophylaxis for major surgical procedures
 1 Glycopeptides appropriate uses serious infections due to beta-lactam- resistant gram-positive microorganisms infections due to gram-positive microorganisms in patients with serious allergy to beta-lactam
1 Glycopeptides appropriate uses serious infections due to beta-lactam- resistant gram-positive microorganisms infections due to gram-positive microorganisms in patients with serious allergy to beta-lactam
Pharmacologyonline 1: (2010) ewsletter Singh and Kochbar. Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of
 Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING
 EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
MRSA Micro Scan Pos Combo 6J DADE BEHRING VCM
 PKPD MRSA 1 1 2 1 1 2 17 1 26 17 3 16 vancomycinvcm methicillin-resistant Staphylococcus aureusmrsa 31 pharmacokineticpkparameter retrospective VCM 21 10 PK parameter Mann- Whitney U-test Cmax 37.1 µ gml29.942
PKPD MRSA 1 1 2 1 1 2 17 1 26 17 3 16 vancomycinvcm methicillin-resistant Staphylococcus aureusmrsa 31 pharmacokineticpkparameter retrospective VCM 21 10 PK parameter Mann- Whitney U-test Cmax 37.1 µ gml29.942
Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients According to New Guidelines
 Original Article Clinical Chemistry Ann Lab Med 2014;34:1-6 http://dx.doi.org/10.3343/alm.2014.34.1.1 ISSN 2234-3806 eissn 2234-3814 Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients
Original Article Clinical Chemistry Ann Lab Med 2014;34:1-6 http://dx.doi.org/10.3343/alm.2014.34.1.1 ISSN 2234-3806 eissn 2234-3814 Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients
D DAVID PUBLISHING. Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within a Therapeutic Range. 1.
 Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
Evaluation of Vancomycin Continuous Infusion in Trauma Patients
 OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
%T MIC MIC. Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration time-killing-curve 1990.
 THE JAPANESE JOURNAL OF ANTIBIOTICS 58 2 159( 55 ) ( 2 15 ) %T MIC MIC 2002 30%T MIC 50%T MIC 1000 mg 3 3 /day Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration
THE JAPANESE JOURNAL OF ANTIBIOTICS 58 2 159( 55 ) ( 2 15 ) %T MIC MIC 2002 30%T MIC 50%T MIC 1000 mg 3 3 /day Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration
Lessons from recent studies. João Gonçalves Pereira UCIP DALI
 Lessons from recent studies João Gonçalves Pereira UCIP DALI 1 Patterns of Antimicrobial Activity Concentration C max Aminoglycosides Cmax/MIC>10 Metronidazol Area under the concentration curve Azithromycin
Lessons from recent studies João Gonçalves Pereira UCIP DALI 1 Patterns of Antimicrobial Activity Concentration C max Aminoglycosides Cmax/MIC>10 Metronidazol Area under the concentration curve Azithromycin
Challenges in Therapeutic Drug Monitoring:
 Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
THERAPEUTIC MONITORING OF VANCOMYCIN IN CLINICAL PRACTICE
 THERAPEUTIC MONITORING OF VANCOMYCIN IN CLINICAL PRACTICE Hana Suchánková, Martina Machačová, Tereza Herodesová Department of Pharmacology, University Hospital Olomouc Introduction and objective: Routine
THERAPEUTIC MONITORING OF VANCOMYCIN IN CLINICAL PRACTICE Hana Suchánková, Martina Machačová, Tereza Herodesová Department of Pharmacology, University Hospital Olomouc Introduction and objective: Routine
D DAVID PUBLISHING. 1. Introduction. Kathryn Koliha 1, Julie Falk 1, Rachana Patel 1 and Karen Kier 2
 Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Is the package insert correct? PK considerations
 Is the package insert correct? PK considerations Jason A Roberts B Pharm (Hons), PhD, FSHP Professor of Medicine and Pharmacy The University of Queensland, Australia Royal Brisbane and Women s Hospital,
Is the package insert correct? PK considerations Jason A Roberts B Pharm (Hons), PhD, FSHP Professor of Medicine and Pharmacy The University of Queensland, Australia Royal Brisbane and Women s Hospital,
Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics
 Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics This patient needs antibiotics. But which ones? Intensive care patient Ceftazidime,
Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics This patient needs antibiotics. But which ones? Intensive care patient Ceftazidime,
ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN
 ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN Anne Smits Fellow neonatologie UZ Leuven Use of antibiotics in neonates 50 European hospitals 23 non-european hospitals Countries n = 14 n = 9 Pediatric
ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN Anne Smits Fellow neonatologie UZ Leuven Use of antibiotics in neonates 50 European hospitals 23 non-european hospitals Countries n = 14 n = 9 Pediatric
Full title of guideline INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS. control
 Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
The CLSI Approach to Setting Breakpoints
 The CLSI Approach to Setting Breakpoints Jean B. Patel, PhD, D(ABMM) Deputy Director, Office of Antimicrobial Resistance Division of Healthcare Quality Promotion National Center for Emerging and Zoonotic
The CLSI Approach to Setting Breakpoints Jean B. Patel, PhD, D(ABMM) Deputy Director, Office of Antimicrobial Resistance Division of Healthcare Quality Promotion National Center for Emerging and Zoonotic
ICU Volume 11 - Issue 3 - Autumn Series
 ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
Voriconazole Rationale for the EUCAST clinical breakpoints, version March 2010
 Voriconazole Rationale for the EUCAST clinical breakpoints, version 2.0 20 March 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the European
Voriconazole Rationale for the EUCAST clinical breakpoints, version 2.0 20 March 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the European
Micafungin and Candida spp. Rationale for the EUCAST clinical breakpoints. Version February 2013
 Micafungin and Candida spp. Rationale for the EUCAST clinical breakpoints. Version 1.0 5 February 2013 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised
Micafungin and Candida spp. Rationale for the EUCAST clinical breakpoints. Version 1.0 5 February 2013 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised
Disclosures. Efficacy of the drug. Optimizing Dosing Based on PKPD- An overview. Dose Finding - The Past
 Disclosures Optimizing Dosing Based on PKPD- An overview Johan W. Mouton MD PhD FIDSA FAAM Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker This Patient Needs Antibiotics.
Disclosures Optimizing Dosing Based on PKPD- An overview Johan W. Mouton MD PhD FIDSA FAAM Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker This Patient Needs Antibiotics.
Pharmacodynamics: the methods
 Pharmacodynamics: the methods In vitro models Animal models Clinical studies Population studies With the support of Wallonie-Bruxelles-International 3B-1 Pharmacodynamics: the methods "un peu de tout "
Pharmacodynamics: the methods In vitro models Animal models Clinical studies Population studies With the support of Wallonie-Bruxelles-International 3B-1 Pharmacodynamics: the methods "un peu de tout "
the American Society of Health-System Pharmacists, the Infectious Diseases Society of
 1 2 3 4 Therapeutic monitoring of vancomycin: A revised consensus guideline and review of the American Society of Health-System Pharmacists, the Infectious Diseases Society of America, the Pediatric Infectious
1 2 3 4 Therapeutic monitoring of vancomycin: A revised consensus guideline and review of the American Society of Health-System Pharmacists, the Infectious Diseases Society of America, the Pediatric Infectious
Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence
 Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence Researching field Pharmacokinetics, Pharmacodynamics of antimicrobial, antifungal and antitumoral drugs
Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence Researching field Pharmacokinetics, Pharmacodynamics of antimicrobial, antifungal and antitumoral drugs
Trust Guideline for the Use of Parenteral Vancomycin and Teicoplanin in Adults
 A clinical guideline recommended for use: In: By: For: Division responsible for document: Key words: Names of document authors: Job titles of document authors: Name of document author s Line Manager: Job
A clinical guideline recommended for use: In: By: For: Division responsible for document: Key words: Names of document authors: Job titles of document authors: Name of document author s Line Manager: Job
Pharmacodynamic indices in targeting therapy of critical infections
 Pharmacodynamic indices in targeting therapy of critical infections P.M. Tulkens Cellular and Molecular Pharmacology, Catholic University of Louvain, Brussels, Belgium & International Society of Anti-infective
Pharmacodynamic indices in targeting therapy of critical infections P.M. Tulkens Cellular and Molecular Pharmacology, Catholic University of Louvain, Brussels, Belgium & International Society of Anti-infective
Clinical Guidelines for Use of Antibiotics. VANCOMYCIN (Adult)
 VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
VANCOMYCIN DOSING AND MONITORING GUIDELINES
 VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
CLINICAL USE OF GLYCOPEPTIDES. Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel
 CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Professor of Medicine Vice-Chairman, Department of Medicine SUNY at Stony Brook
 Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
SCMID Online Lecture Library. by author. Optimizing antimicrobial therapy in the elderly. Dose Finding - The Past
 Optimizing antimicrobial therapy in the elderly Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics Dosing should be such that the level of antmicrobial activity is associated
Optimizing antimicrobial therapy in the elderly Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics Dosing should be such that the level of antmicrobial activity is associated
Vancomycin Rationale for the EUCAST clinical breakpoints, version June 2010
 Vancomycin Rationale for the EUCAST clinical breakpoints, version 2.1 17 June 2010 Introduction The glycopeptides are a class of agents composed of amino acid residues and attached sugars. Glycopeptides
Vancomycin Rationale for the EUCAST clinical breakpoints, version 2.1 17 June 2010 Introduction The glycopeptides are a class of agents composed of amino acid residues and attached sugars. Glycopeptides
ESCMID Online Lecture Library. by author
 Disclosures Pk/Pd of antifungal drugs Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker Dosing should be such that the level of antmicrobial
Disclosures Pk/Pd of antifungal drugs Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker Dosing should be such that the level of antmicrobial
Cefotaxime Rationale for the EUCAST clinical breakpoints, version th September 2010
 Cefotaxime Rationale for the EUCAST clinical breakpoints, version 1.0 26 th September 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the European
Cefotaxime Rationale for the EUCAST clinical breakpoints, version 1.0 26 th September 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the European
PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS
 PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS SITI HIR HURAIZAH MD TAHIR Bpharm (UKM), MSc (Clinical Microbiology) (UoN) CLINICAL PHARMACIST HOSPITAL MELAKA WHY STUDY PHARMACOKINETICS (PK) AND PHARMACODYNAMICS
PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS SITI HIR HURAIZAH MD TAHIR Bpharm (UKM), MSc (Clinical Microbiology) (UoN) CLINICAL PHARMACIST HOSPITAL MELAKA WHY STUDY PHARMACOKINETICS (PK) AND PHARMACODYNAMICS
MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS:
 MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS: Application to Estimation of MIC Breakpoints Paul G. Ambrose, Pharm.D. Director, Division of Infectious Diseases, Cognigen Corporation; Adjunct
MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS: Application to Estimation of MIC Breakpoints Paul G. Ambrose, Pharm.D. Director, Division of Infectious Diseases, Cognigen Corporation; Adjunct
La farmacologia in aiuto
 Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
SBUH Aminoglycoside Dosing Protocol
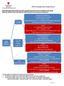 Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Estimation of In Vitro Susceptibility Breakpoints for Tigecycline Against Staphylococcus aureus
 Estimation of In Vitro Susceptibility Breakpoints for Tigecycline Against Staphylococcus aureus Alison K Meagher, PharmD Cognigen Corporation 45 th ICAAC December 17, 2005 Julie Passarell, M.A. Cognigen
Estimation of In Vitro Susceptibility Breakpoints for Tigecycline Against Staphylococcus aureus Alison K Meagher, PharmD Cognigen Corporation 45 th ICAAC December 17, 2005 Julie Passarell, M.A. Cognigen
ORIGINAL ARTICLE DOI: (e) ISSN Online: (p) ISSN Print: Anand Kumar Singh 1, Poonam Verma 2. Sciences, Dehradun
 ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
Reassessment of Recommended Imipenem Doses in Febrile Neutropenic Patients with. Haematological Malignancies ACCEPTED
 AAC Accepts, published online ahead of print on 1 December 2008 Antimicrob. Agents Chemother. doi:10.1128/aac.00891-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 1 December 2008 Antimicrob. Agents Chemother. doi:10.1128/aac.00891-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions.
Department of Pharmacy Services, Hartford Hospital, 80 Seymour Street, Hartford, CT 06102, USA; 2
 Pathogens 2015, 4, 599-605; doi:10.3390/pathogens4030599 Article OPEN ACCESS pathogens ISSN 2076-0817 www.mdpi.com/journal/pathogens Assessing the Surrogate Susceptibility of Oxacillin and Cefoxitin for
Pathogens 2015, 4, 599-605; doi:10.3390/pathogens4030599 Article OPEN ACCESS pathogens ISSN 2076-0817 www.mdpi.com/journal/pathogens Assessing the Surrogate Susceptibility of Oxacillin and Cefoxitin for
Steven D. Brown* and Maria M. Traczewski. The Clinical Microbiology Institute, 9725 SW Commerce Circle, Wilsonville, Oregon 97070
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, May 2010, p. 2063 2069 Vol. 54, No. 5 0066-4804/10/$12.00 doi:10.1128/aac.01569-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Comparative
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, May 2010, p. 2063 2069 Vol. 54, No. 5 0066-4804/10/$12.00 doi:10.1128/aac.01569-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Comparative
Department of Clinical Pharmacy, University of Michigan College of Pharmacy, Pharmacy Faculty, Siam University, Bangkok, Thailand
 1 2 Article Type: Guest Ed Mistakes We Make in Dialysis 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 We underdose antibiotics in patients on CRRT Alexander R. Shaw Weerachai Chaijamorn Bruce A. Mueller 1 Ann
1 2 Article Type: Guest Ed Mistakes We Make in Dialysis 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 We underdose antibiotics in patients on CRRT Alexander R. Shaw Weerachai Chaijamorn Bruce A. Mueller 1 Ann
Long Half-life Drugs in Infectious Diseases: Implications and Complications
 Long Half-life Drugs in Infectious Diseases: Implications and Complications In Session: Drugs That Just Won t Leave: From Stars of the Party to Unwelcome Guests Annual Meeting of the AAPS, San Diego, California
Long Half-life Drugs in Infectious Diseases: Implications and Complications In Session: Drugs That Just Won t Leave: From Stars of the Party to Unwelcome Guests Annual Meeting of the AAPS, San Diego, California
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia
 Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
NORLAND AVENUE PHARMACY PRESCRIPTION COMPOUNDING FOR GENERAL PRACTICE
 APRIL 2011 PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Methicillin-Resistant Staphylococcus 2
APRIL 2011 PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Methicillin-Resistant Staphylococcus 2
Mupirocin Rationale for the EUCAST clinical breakpoints, version th July 2010
 Mupirocin Rationale for the EUCAST clinical breakpoints, version 1.0 6 th July 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the European
Mupirocin Rationale for the EUCAST clinical breakpoints, version 1.0 6 th July 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the European
Therapeutic Dose Monitoring for Linezolid in a Patient with MRSA Pneumonia with Bacteremia in Diabetes Insipidus
 Infect Dis Ther (2016) 5:81 87 DOI 10.1007/s40121-015-0100-z CASE REPORT Therapeutic Dose Monitoring for Linezolid in a Patient with MRSA Pneumonia with Bacteremia in Diabetes Insipidus Yoshihiko Nakamura.
Infect Dis Ther (2016) 5:81 87 DOI 10.1007/s40121-015-0100-z CASE REPORT Therapeutic Dose Monitoring for Linezolid in a Patient with MRSA Pneumonia with Bacteremia in Diabetes Insipidus Yoshihiko Nakamura.
PK/PD degli antibiotici utilizzati nella sepsi
 PK/PD degli antibiotici utilizzati nella sepsi Dario Cattaneo, U.O. Farmacologia Clinica ASST Fatebenefratelli Sacco, Milano Bergamo, città alta Variability of antibiotic concentrations in critically ill
PK/PD degli antibiotici utilizzati nella sepsi Dario Cattaneo, U.O. Farmacologia Clinica ASST Fatebenefratelli Sacco, Milano Bergamo, città alta Variability of antibiotic concentrations in critically ill
Antimicrobial Reference Laboratory
 Antimicrobial Reference Laboratory GUIDELINE RANGES FOR TDM 2018 Andrew Lovering Antimicrobial Reference Laboratory North Bristol NHS Trust Southmead Hospital Bristol, BS10 5NB Guideline Ranges 2018 Aminoglycosides
Antimicrobial Reference Laboratory GUIDELINE RANGES FOR TDM 2018 Andrew Lovering Antimicrobial Reference Laboratory North Bristol NHS Trust Southmead Hospital Bristol, BS10 5NB Guideline Ranges 2018 Aminoglycosides
ASHP Therapeutic Position Statements 623
 ASHP Therapeutic Position Statements 623 Therapeutic Monitoring of Vancomycin in Adult Patients: A Consensus Review of the American Society of Health-System Pharmacists, the Infectious Diseases Society
ASHP Therapeutic Position Statements 623 Therapeutic Monitoring of Vancomycin in Adult Patients: A Consensus Review of the American Society of Health-System Pharmacists, the Infectious Diseases Society
Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects
 Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects Karolyn S. Horn, Mark H. Gotfried, Judith N. Steenbergen,
Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects Karolyn S. Horn, Mark H. Gotfried, Judith N. Steenbergen,
Optimized Use of Vancomycin
 E-Newsletter #1 Optimized Use of Vancomycin FROM THE EDITOR S DESK Methicillin-resistant Staphylococcus aureus (MRSA) is a serious concern for clinicians managing infectious diseases in the healthcare
E-Newsletter #1 Optimized Use of Vancomycin FROM THE EDITOR S DESK Methicillin-resistant Staphylococcus aureus (MRSA) is a serious concern for clinicians managing infectious diseases in the healthcare
Aminoglycosides John A. Bosso, Pharm.D.
 AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
Relationship of MIC and Bactericidal Activity to Efficacy of Vancomycin for Treatment of Methicillin-Resistant Staphylococcus aureus Bacteremia
 JOURNAL OF CLINICAL MICROBIOLOGY, June 2004, p. 2398 2402 Vol. 42, No. 6 0095-1137/04/$08.00 0 DOI: 10.1128/JCM.42.6.2398 2402.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved.
JOURNAL OF CLINICAL MICROBIOLOGY, June 2004, p. 2398 2402 Vol. 42, No. 6 0095-1137/04/$08.00 0 DOI: 10.1128/JCM.42.6.2398 2402.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved.
Doripenem: pharmacokinetics and pharmacodynamics. Paul M. Tulkens, MD, PhD Françoise Van Bambeke, PharmD, PhD
 16/04/2009 1 Doripenem: pharmacokinetics and pharmacodynamics Paul M. Tulkens, MD, PhD Françoise Van Bambeke, PharmD, PhD Unité de Pharmacologie cellulaire et moléculaire Louvain Drug Research Institute
16/04/2009 1 Doripenem: pharmacokinetics and pharmacodynamics Paul M. Tulkens, MD, PhD Françoise Van Bambeke, PharmD, PhD Unité de Pharmacologie cellulaire et moléculaire Louvain Drug Research Institute
Evaluation of Vancomycin Dosing and Corresponding Drug Concentrations in Pediatric Patients
 RESEARCH ARTICLE Evaluation of Vancomycin Dosing and Corresponding Drug Concentrations in Pediatric Patients abstract OBJECTIVE: To describe the relationships between dosing strategy, age, and vancomycin
RESEARCH ARTICLE Evaluation of Vancomycin Dosing and Corresponding Drug Concentrations in Pediatric Patients abstract OBJECTIVE: To describe the relationships between dosing strategy, age, and vancomycin
Cefuroxime iv Rationale for the EUCAST clinical breakpoints, version th September 2010
 Cefuroxime iv Rationale for the EUCAST clinical breakpoints, version 1.0 26 th September 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the
Cefuroxime iv Rationale for the EUCAST clinical breakpoints, version 1.0 26 th September 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the
Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics
 Exposure - Response Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics ACTVITY in vitro (MIC) CONCENTRATIONS in vivo (PK) DOSING regimen Other factors ANTMICROBIAL EFFICACY (Microbiological
Exposure - Response Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics ACTVITY in vitro (MIC) CONCENTRATIONS in vivo (PK) DOSING regimen Other factors ANTMICROBIAL EFFICACY (Microbiological
Daptomycin in Clinical Practice. Paolo Grossi
 Clinica delle Malattie Infettive e Tropicali Università degli Studi dell Insubria Ospedale di Circolo e Fondazione Macchi, Varese Second Opinion Infettivologica Centro Nazionale Trapianti, ISS, Roma Daptomycin
Clinica delle Malattie Infettive e Tropicali Università degli Studi dell Insubria Ospedale di Circolo e Fondazione Macchi, Varese Second Opinion Infettivologica Centro Nazionale Trapianti, ISS, Roma Daptomycin
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients
 Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
PHA Spring First Exam. 8 Aminoglycosides (5 points)
 PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
Pharmacokinetics of daptomycin in a patient with severe renal failure not under dialysis
 AAC Accepts, published online ahead of print on 1 April 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.00230-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 Pharmacokinetics
AAC Accepts, published online ahead of print on 1 April 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.00230-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 Pharmacokinetics
Severe β-lactam allergy. Alternative (use for mild-moderate β-lactam allergy) therapy
 Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
Vancomycin: Class: Antibiotic.
 Vancomycin: Class: Antibiotic. Indications: Treatment of patients with infections caused by staphylococcal species and streptococcal Species. Available dosage form in the hospital: 1G VIAL, 500MG VIAL.
Vancomycin: Class: Antibiotic. Indications: Treatment of patients with infections caused by staphylococcal species and streptococcal Species. Available dosage form in the hospital: 1G VIAL, 500MG VIAL.
Cubicin A Guide to Dosing
 Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
Joint Trust Guideline for the Use of Intravenous Vancomycin in Paediatrics
 A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
The Challenge of Managing Staphylococcus aureus Bacteremia
 The Challenge of Managing Staphylococcus aureus Bacteremia M A R G A R E T G R A Y B S P F C S H P C L I N I C A L P R A C T I C E M A N A G E R N O R T H / I D P H A R M A C I S T A L B E R T A H E A
The Challenge of Managing Staphylococcus aureus Bacteremia M A R G A R E T G R A Y B S P F C S H P C L I N I C A L P R A C T I C E M A N A G E R N O R T H / I D P H A R M A C I S T A L B E R T A H E A
Running title: Comparative Efficacy of Telavancin and Vancomycin. Key words: human simulated, vancomycin intermediate Staphylococcus aureus,
 AAC Accepts, published online ahead of print on 13 September 2010 Antimicrob. Agents Chemother. doi:10.1128/aac.00062-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 13 September 2010 Antimicrob. Agents Chemother. doi:10.1128/aac.00062-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions.
An imputation-based method to reduce bias in model parameter estimates due to non-random censoring in oncology trials
 TCP 2016;24(4):189-193 http://dx.doi.org/10.12793/tcp.2016.24.4.189 An imputation-based method to reduce bias in model parameter estimates due to non-random censoring in oncology trials Dongwoo Chae 1,2
TCP 2016;24(4):189-193 http://dx.doi.org/10.12793/tcp.2016.24.4.189 An imputation-based method to reduce bias in model parameter estimates due to non-random censoring in oncology trials Dongwoo Chae 1,2
Clinical Pharmacokinetics and Pharmacodynamics of Telavancin Compared with the Other Glycopeptides
 Clin Pharmacokinet (2018) 57:797 816 https://doi.org/10.1007/s40262-017-0623-4 REVIEW ARTICLE Clinical Pharmacokinetics and Pharmacodynamics of Telavancin Compared with the Other Glycopeptides Valentin
Clin Pharmacokinet (2018) 57:797 816 https://doi.org/10.1007/s40262-017-0623-4 REVIEW ARTICLE Clinical Pharmacokinetics and Pharmacodynamics of Telavancin Compared with the Other Glycopeptides Valentin
Received 30 March 2005; returned 16 June 2005; revised 8 September 2005; accepted 12 September 2005
 Journal of Antimicrobial Chemotherapy (2005) 56, 1047 1052 doi:10.1093/jac/dki362 Advance Access publication 20 October 2005 Evaluation of PPI-0903M (T91825), a novel cephalosporin: bactericidal activity,
Journal of Antimicrobial Chemotherapy (2005) 56, 1047 1052 doi:10.1093/jac/dki362 Advance Access publication 20 October 2005 Evaluation of PPI-0903M (T91825), a novel cephalosporin: bactericidal activity,
Development of teicoplanin dosage guidelines for patients treated within an outpatient parenteral antibiotic therapy (OPAT) programme
 Journal of Antimicrobial Chemotherapy (2009) 64, 181 187 doi:10.1093/jac/dkp147 Advance Access publication 2 May 2009 Development of teicoplanin dosage guidelines for patients treated within an outpatient
Journal of Antimicrobial Chemotherapy (2009) 64, 181 187 doi:10.1093/jac/dkp147 Advance Access publication 2 May 2009 Development of teicoplanin dosage guidelines for patients treated within an outpatient
Enhanced efficacy of single-dose versus multi-dose azithromycin regimens in preclinical infection models
 Journal of Antimicrobial Chemotherapy (25) 56, 365 37 doi:.93/jac/dki24 Advance Access publication 7 July 25 Enhanced efficacy of single-dose versus multi-dose azithromycin regimens in preclinical infection
Journal of Antimicrobial Chemotherapy (25) 56, 365 37 doi:.93/jac/dki24 Advance Access publication 7 July 25 Enhanced efficacy of single-dose versus multi-dose azithromycin regimens in preclinical infection
May 11, Ceftriaxone for MSSA. Daptomycin Dosing Weight. Candidiasis Treatment
 Diagnostics and Debates: An Update on Rapid Diagnostic Testing and Current Controversies in Infectious Diseases Nicholas Torney, PharmD, BCPS Derek Vander Horst, PharmD Munson Medical Center WMSHP Annual
Diagnostics and Debates: An Update on Rapid Diagnostic Testing and Current Controversies in Infectious Diseases Nicholas Torney, PharmD, BCPS Derek Vander Horst, PharmD Munson Medical Center WMSHP Annual
Antifungal Pharmacodynamics A Strategy to Optimize Efficacy
 Antifungal Pharmacodynamics A Strategy to Optimize Efficacy David Andes, MD Associate Professor, Department of Medicine Division of Infectious Diseases Medical Microbiology and Immunology University of
Antifungal Pharmacodynamics A Strategy to Optimize Efficacy David Andes, MD Associate Professor, Department of Medicine Division of Infectious Diseases Medical Microbiology and Immunology University of
Vancomycin Drug Class 1
 Drug Class 1 Antibiotic glycopeptide Spectrum 1 Cross Sensitivities / Allergies 1 Refer to product monograph for complete spectrum Gram positive pathogens (e.g., S. aureus, Enterococcus, S. viridans, methicillinresistant
Drug Class 1 Antibiotic glycopeptide Spectrum 1 Cross Sensitivities / Allergies 1 Refer to product monograph for complete spectrum Gram positive pathogens (e.g., S. aureus, Enterococcus, S. viridans, methicillinresistant
Towards clinical Applications of PK-PD in specific situations
 Towards clinical Applications of PK-PD in specific situations P.M. Tulkens Cellular and Molecular Pharmacology & Center for Clinical Pharmacy, Catholic University of Louvain, Brussels, Belgium with many
Towards clinical Applications of PK-PD in specific situations P.M. Tulkens Cellular and Molecular Pharmacology & Center for Clinical Pharmacy, Catholic University of Louvain, Brussels, Belgium with many
Late diagnosis of influenza in adult patients during a seasonal outbreak
 ORIGINAL ARTICLE Korean J Intern Med 2018;33:391-396 Late diagnosis of influenza in adult patients during a seasonal outbreak Seong-Ho Choi 1, Jin-Won Chung 1, Tark Kim 2, Ki-Ho Park 3, Mi Suk Lee 3, and
ORIGINAL ARTICLE Korean J Intern Med 2018;33:391-396 Late diagnosis of influenza in adult patients during a seasonal outbreak Seong-Ho Choi 1, Jin-Won Chung 1, Tark Kim 2, Ki-Ho Park 3, Mi Suk Lee 3, and
Title. Author(s)Hayakawa, Mineji; Fujita, Itaru; Iseki, Ken; Gando, CitationASAIO Journal, 55(3): Issue Date Doc URL. Rights.
 Title The Administration of Ciprofloxacin During Continuou Author(s)Hayakawa, Mineji; Fujita, Itaru; Iseki, Ken; Gando, CitationASAIO Journal, 55(3): 243-245 Issue Date 2009-05 Doc URL http://hdl.handle.net/2115/43035
Title The Administration of Ciprofloxacin During Continuou Author(s)Hayakawa, Mineji; Fujita, Itaru; Iseki, Ken; Gando, CitationASAIO Journal, 55(3): 243-245 Issue Date 2009-05 Doc URL http://hdl.handle.net/2115/43035
Consultation on the Revision of Carbapenem Breakpoints
 Consultation on the Revision of Carbapenem Breakpoints July 2018 Please send comments to the EUCAST Scientific Secretary at jturnidge@gmail.com by September 15. EUCAST revision of carbapenem breakpoints
Consultation on the Revision of Carbapenem Breakpoints July 2018 Please send comments to the EUCAST Scientific Secretary at jturnidge@gmail.com by September 15. EUCAST revision of carbapenem breakpoints
CAT. Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators. Apr. Glynis Frans Supervisor: Prof. Apr.
 CAT Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators Apr. Glynis Frans Supervisor: Prof. Apr. Katrien Lagrou 1. What are the current guidelines and recommendations on TDM for
CAT Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators Apr. Glynis Frans Supervisor: Prof. Apr. Katrien Lagrou 1. What are the current guidelines and recommendations on TDM for
INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS
 Title of guideline (must include the word Guideline (not protocol, policy, procedure etc) INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS Author: Contact Name and Job Title
Title of guideline (must include the word Guideline (not protocol, policy, procedure etc) INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS Author: Contact Name and Job Title
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Clinical Safety & Effectiveness Cohort # 10
 1 Clinical Safety & Effectiveness Cohort # 10 Improving Weight-Based Vancomycin Dosing and Monitoring DATE Educating for Quality Improvement & Patient Safety 2 Financial Disclosure lizabeth A. Walter,
1 Clinical Safety & Effectiveness Cohort # 10 Improving Weight-Based Vancomycin Dosing and Monitoring DATE Educating for Quality Improvement & Patient Safety 2 Financial Disclosure lizabeth A. Walter,
Affinity of Doripenem and Comparators to Penicillin-Binding Proteins in Escherichia coli and ACCEPTED
 AAC Accepts, published online ahead of print on February 00 Antimicrob. Agents Chemother. doi:./aac.01-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
AAC Accepts, published online ahead of print on February 00 Antimicrob. Agents Chemother. doi:./aac.01-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
SHC Vancomycin Dosing Guide
 SHC Vancomycin Dosing Guide A: Initial dosing considerations B. Pharmacodynamic Targets: goal AUC and troughs C. Loading dose D: Initial Vancomycin Maintenance Dosing and Serum Concentration Monitoring
SHC Vancomycin Dosing Guide A: Initial dosing considerations B. Pharmacodynamic Targets: goal AUC and troughs C. Loading dose D: Initial Vancomycin Maintenance Dosing and Serum Concentration Monitoring
Pharmacokinetic study of garenoxacin in severe renal failure patients
 June 2015 THE JAPANESE JOURNAL OF ANTIBIOTICS 68 3 141 1 Pharmacokinetic study of garenoxacin in severe renal failure patients YUKA YAMAGISHI 1, 2, MAO HAGIHARA 2, YUKIHIRO HAMADA 2, YUKIHIRO KIMURA 3,
June 2015 THE JAPANESE JOURNAL OF ANTIBIOTICS 68 3 141 1 Pharmacokinetic study of garenoxacin in severe renal failure patients YUKA YAMAGISHI 1, 2, MAO HAGIHARA 2, YUKIHIRO HAMADA 2, YUKIHIRO KIMURA 3,
Outpatient treatment in women with acute pyelonephritis after visiting emergency department
 LETTER TO THE EDITOR Korean J Intern Med 2017;32:369-373 Outpatient treatment in women with acute pyelonephritis after visiting emergency department Hee Kyoung Choi 1,*, Jin-Won Chung 2, Won Sup Oh 3,
LETTER TO THE EDITOR Korean J Intern Med 2017;32:369-373 Outpatient treatment in women with acute pyelonephritis after visiting emergency department Hee Kyoung Choi 1,*, Jin-Won Chung 2, Won Sup Oh 3,
Pharmacist and Physician Collaborative Practice Model Improves Vancomycin Dosing in an Intensive Care Unit
 International Journal of Clinical Medicine, 2016, 7, 675-684 http://www.scirp.org/journal/ijcm ISSN Online: 2158-2882 ISSN Print: 2158-284X Pharmacist and Physician Collaborative Practice Model Improves
International Journal of Clinical Medicine, 2016, 7, 675-684 http://www.scirp.org/journal/ijcm ISSN Online: 2158-2882 ISSN Print: 2158-284X Pharmacist and Physician Collaborative Practice Model Improves
Prediction of Cancer Incidence and Mortality in Korea, 2013
 pissn 1598-2998, eissn 256 Cancer Res Treat. 213;45(1):15-21 Special Article http://dx.doi.org/1.4143/crt.213.45.1.15 Open Access Prediction of Cancer Incidence and Mortality in Korea, 213 Kyu-Won Jung,
pissn 1598-2998, eissn 256 Cancer Res Treat. 213;45(1):15-21 Special Article http://dx.doi.org/1.4143/crt.213.45.1.15 Open Access Prediction of Cancer Incidence and Mortality in Korea, 213 Kyu-Won Jung,
Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally
 INVITED ARTICLE ANTIMICROBIAL RESISTANCE George M. Eliopoulos, Section Editor Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally George L. Drusano, Paul G. Ambrose, Sujata M.
INVITED ARTICLE ANTIMICROBIAL RESISTANCE George M. Eliopoulos, Section Editor Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally George L. Drusano, Paul G. Ambrose, Sujata M.
Sponsor/Company: sanofi-aventis Drug substance: Elitek/Fasturtec (rasburicase, SR29142)
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor/Company: sanofi-aventis Drug
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor/Company: sanofi-aventis Drug
EMA Workshop Estimating the Probability of Target Attainment
 EMA Workshop Estimating the Probability of Target Attainment G.L. Drusano, M.D. Professor and Director Institute for Therapeutic Innovation University of Florida Attainment We all tend to think problems
EMA Workshop Estimating the Probability of Target Attainment G.L. Drusano, M.D. Professor and Director Institute for Therapeutic Innovation University of Florida Attainment We all tend to think problems
Achieving pharmacokinetic/pharmacodynamic (PK/PD) targets of β-lactams in critically ill patients at first dose: Can we do it with standard dosing?
 Oral session: PK/PD-based optimized broad-spectrum beta-lactam therapy (Sunday 10 April, 11:30) Achieving pharmacokinetic/pharmacodynamic (PK/PD) targets of β-lactams in critically ill patients at first
Oral session: PK/PD-based optimized broad-spectrum beta-lactam therapy (Sunday 10 April, 11:30) Achieving pharmacokinetic/pharmacodynamic (PK/PD) targets of β-lactams in critically ill patients at first
Clinical Study Achievement of Vancomycin Therapeutic Goals in Critically Ill Patients: Early Individualization May Be Beneficial
 Critical Care Research and Practice Volume 2016, Article ID 1245815, 7 pages http://dx.doi.org/10.1155/2016/1245815 Clinical Study Achievement of Vancomycin Therapeutic Goals in Critically Ill Patients:
Critical Care Research and Practice Volume 2016, Article ID 1245815, 7 pages http://dx.doi.org/10.1155/2016/1245815 Clinical Study Achievement of Vancomycin Therapeutic Goals in Critically Ill Patients:
Prevalence and related factors for injectable vancomycin or teicoplanin-associated thrombocytopenia in a Vietnamese hospital
 Original Article Mahidol Univ J Pharm Sci 2015; 42 (4), 178-185 Prevalence and related factors for injectable vancomycin or teicoplanin-associated thrombocytopenia in a Vietnamese hospital HT. Nguyen 1,
Original Article Mahidol Univ J Pharm Sci 2015; 42 (4), 178-185 Prevalence and related factors for injectable vancomycin or teicoplanin-associated thrombocytopenia in a Vietnamese hospital HT. Nguyen 1,
ORIGINAL ARTICLE Infectious Diseases, Microbiology & Parasitology INTRODUCTION
 ORIGINAL ARTICLE Infectious Diseases, Microbiology & Parasitology http://dx.doi.org/1.3346/jkms.213.28.1.48 J Korean Med Sci 213; 28: 48-54 Serum Cystatin C Is a Major Predictor of Vancomycin Clearance
ORIGINAL ARTICLE Infectious Diseases, Microbiology & Parasitology http://dx.doi.org/1.3346/jkms.213.28.1.48 J Korean Med Sci 213; 28: 48-54 Serum Cystatin C Is a Major Predictor of Vancomycin Clearance
Clinical Study Prospective Trial of a Novel Nomogram to Achieve Updated Vancomycin Trough Concentrations
 Interdisciplinary Perspectives on Infectious Diseases Volume 2013, Article ID 839456, 8 pages http://dx.doi.org/10.1155/2013/839456 Clinical Study Prospective Trial of a Novel Nomogram to Achieve Updated
Interdisciplinary Perspectives on Infectious Diseases Volume 2013, Article ID 839456, 8 pages http://dx.doi.org/10.1155/2013/839456 Clinical Study Prospective Trial of a Novel Nomogram to Achieve Updated
