Silent kidney stones in asymptomatic primary hyperparathyroidism a comparison of multidetector computed tomography and ultrasound
|
|
|
- Rodney Howard
- 6 years ago
- Views:
Transcription
1 Langenbecks Arch Surg (2017) 402: DOI /s ORIGINAL ARTICLE Silent kidney stones in asymptomatic primary hyperparathyroidism a comparison of multidetector computed tomography and ultrasound Andreas Selberherr 1 & Marcus Hörmann 2 & Gerhard Prager 1 & Philipp Riss 1 & Christian Scheuba 1 & Bruno Niederle 1 Received: 22 April 2016 /Accepted: 2 October 2016 /Published online: 12 October 2016 # The Author(s) This article is published with open access at Springerlink.com Abstract Purpose The purpose of this study was to demonstrate the high number of kidney stones in primary hyperparathyroidism (PHPT) and the low number of in fact asymptomatic patients. Methods Forty patients with PHPT (28 female, 12 male; median age 58 (range 33 80) years; interquartile range 17 years [51 68]) without known symptoms of kidney stones prospectively underwent multidetector computed tomography (MDCT) and ultrasound (US) examinations of the urinary tract prior to parathyroid surgery. Images were evaluated for the presence and absence of stones, as well as for the number of stones and sizes in the long axis. The MDCT and US examinations were interpreted by two experienced radiologists who were blinded to all clinical and biochemical data. Statistical analysis was performed using the Wilcoxon signed-rank test. Results US revealed a total of 4 kidney stones in 4 (10 %) of 40 patients (median size 6.5 mm, interquartile range 11.5 mm). MDCT showed a total of 41 stones (median size was 3 mm, interquartile range 2.25 mm) in 15 (38 %) of 40 patients. The number of kidney stones detected with MDCT was significantly higher compared to US (p = ). This paper is not based on a previous communication to a society or a meeting. * Andreas Selberherr andreas.selberherr@meduniwien.ac.at 1 2 Section Endocrine Surgery, Division of General Surgery, Department of Surgery, Medical University, Währinger Gürtel 18-20, A-1090 Vienna, Austria Department of Radiology, Medical University, Währinger Gürtel 18-20, A-1090 Vienna, Austria Conclusions MDCT is a highly sensitive method for the detection of silent kidney stones in patients with PHPT. By widely applying this method, the number of asymptomatic courses of PHPT may be substantially reduced. MDCT should be used primarily to detect kidney stones in PHPT and to exclude asymptomatic PHPT. Keywords Asymptomatic hyperparathyroidism. Kidney stones. Primary hyperparathyroidism. PHPT Introduction Asymptomatic primary hyperparathyroidism (PHPT) is defined as biochemically verified PHPT that lacks specific symptoms or signs traditionally associated with hypercalcemia or parathyroid hormone excess [1]. Therefore, patients with PHPT and kidney stone disease are symptomatic by definition. Those patients are at a 15 to 30 % higher risk to develop kidney stones than the general population, in which an incidence of 1 % is described [2 6]. A valid detection tool for kidney stones is crucial at the initial diagnosis of PHPT especially in patients with mildly elevated laboratory findings [7, 8] and in the course of follow-up to detect patients with symptomatic disease. The only cure then is parathyroidectomy with a restoration of normocalcemia which, in the majority of patients, results in a resolution of organic manifestation [9]. Nevertheless, postoperative persistent and recurrent stone disease has been reported in up to 17 % in long-term follow-up [2, 9 11]. Calculi burden and new stone formation is important in the clinical evaluation of patients with kidney stone disease in PHPT [12]. Thus, the most sensitive method for evaluation of kidney stones has to be used to reveal persistent or recurrent (newly formed) kidney stones after successful parathyroid surgery [13 15].
2 290 Langenbecks Arch Surg (2017) 402: The current guidelines on diagnosis and treatment of asymptomatic PHPT [1] recommend evaluation of kidney stone disease and nephrocalcinosis with either abdominal x- ray, ultrasound or computed tomography as equivalent modalities to differentiate between the asymptomatic and the classically symptomatic variant. Ultrasound (US) is continuously performed in the search of kidney stones despite such limiting factors as overlying bowel gas [16]. Non-enhanced helical computed tomography (CT) is a widespread and established method in the detection of kidney stones in patients with acute flank pain [16 18]. With an increase in the use of CT intravenous pyelography, US is currently playing a secondary role in the evaluation of kidney stones [19]. We hypothesize that, in patients with PHPT CT may be more accurate in the detection of kidney stones than US [16]. The aim of the present study was to compare the value of US and CT in detecting silent kidney stones, to identify patients with symptomatic PHPT, to improve the postoperative follow-up of stone carriers and to prevent deterioration of kidney function in patients with PHPT. Materials and methods Patients In this prospective study, 40 patients (28 female, 12 male) with biochemically proven PHPT were consecutively evaluated over a 1-year period (see Table 1). AccordingtoHesch[20], all patients were classified asymptomatic clinically. The patients were neither minimally symptomatic (showing arterial hypertension, osteopenia/osteoporosis, hypercalcemic symptoms) nor symptomatic (osseous or gastrointestinal manifestation). Particularly, the study patients had no kidney stone disease, nephrocalcinosis, or impaired renal function. No patient had a pharmacological anamnesis regarding nephrotoxic or lithogenic agents. Diagnosis of PHPT was based on common laboratory tests [21]. The median age was 58 years (range 33 to 80, interquartile range 17 years [51 to 68]). Four (10 %) of the 40 patients had a history of kidney stones, two of whom underwent surgical extraction. In the remaining two subjects, the stones passed spontaneously. However, at the time of diagnosis of PHPT (including the preceding 5 years at least) none of those patients was afflicted with kidney stones. Imaging studies US and CT were performed 12 to 48 h prior to parathyroid surgery. US of the kidneys was performed by a highly experienced radiologist and with a high-end machine (ATL, HDI 5000, Seattle, USA) using a 5 or a 7-MHz curved array transducer. Documentation included multiple anatomic planes, and at least three images in the longitudinal and three in the transverse section, respectively [16]. Multidetector CT (MDCT; Volume zoom, Siemens, Forchheim, GER) of the abdomen was performed with patients in a prone position. The scanning protocol consisted of 80 kv and 100 mas low-dose scanning using a 4 1 mm collimation, 6-mm table feed, 0.5-s rotation time. Reconstruction was obtained in the axial and coronal plane with 1.5-mm slice thickness. No intravenous or oral contrast agent was administered. Imaging analysis The obtained US images were evaluated for the presence and absence of stones, as well as for the number of stones and sizes in the long axis. The stones were defined as hyperechogenicities with dorsal shadowing [16]. Table 1 Laboratory findings (mean ± standard deviation) and demographic data (median age) sca ipth 25-OH VitD 1, 25-OH VitD Crea P 24 h uca n Age Female Male Normal range > Unit mmol/l pg/ml nmol/l pg/ml mg/dl mmol/l mmol/24 h Total ± ± ± ± ± ± ± US positive 2.69 ± ± ± ± ± ± ± US negative 2.85 ± ± ± ± ± ± ± MDCT postitive 2.83 ± ± ± ± ± ± ± MDCT negative 2.83 ± ± ± ± ± ± ± sca serum calcium; albumine corrected; chemical autoanalyzer (Olympus, Hamburg, Germany), ipth intact parathyroid hormone (Elecsys 1010 Autoanalyzer (Roche, Mannheim, Germany), 25-(OH)D3 25-hydroxycholecalciferol; chemiluminescence immunoassay BLiaison 25OH-VitD- Totalassay^ (DiaSorin, Italy) or Elecsys B25OH- assay^ on COBAS E411 (Roche, Mannheim, Germany), 1,25-(OH)D3 1,25-dihydroxycholecalciferol; analyzed manually via chromatography and radioimmunosorbent assay (DiaSorin, Italy), Crea serum creatinine, P serum phosphate, 24 h uca 24-h urinary calcium excretion
3 Langenbecks Arch Surg (2017) 402: MDCT examinations were evaluated on the screen of a PACS System, again for the absence and presence of stones, as well as for the number of stones and sizes in the long axis. The stones were defined as high-attenuating opacities [16]. Two experienced radiologists evaluated the MDCT and US examinations as a team and provided interpretations in unison. Both investigators were blinded to all clinical and biochemical data. In order to prevent bias, MDCT was assessed 1 week after the evaluation of US. The location of each stone was recorded as being in either the right or the left kidney. In two patients, multiple (uncountable) stones and parenchymal calcifications were found. For size measurements, ten stones of each of those two patients were evaluated which were easily measurable. Statistical analysis Analysis was performed using a statistical software package (SPSS 11, SPSS Inc., Chicago, USA). Comparison of the number of detected stones with MDCT and US was performed with the Wilcoxon signed-rank test. Statistical significance was set at a p value of Surgery was performed on all patients and a single parathyroid adenoma was verified histopathologically. By definition, all patients were cured. Cure was documented by normocalcemia 5 years after surgery. Results Ultrasound In 4 (10 %) of 40 patients, a total of four kidney stones could be detected. The median size was 6.5 mm, quartiles ranging from 2.25 to mm (interquartile range 11.5 mm). Three females and one male were affected. In three cases, the stones were located in the left, in one case in the right kidney. Multidetector computed tomography MDCT identified a total of 41 stones in 15 (38 %) of 40 patients. The size of the stones ranged from 2 to 15 mm with a median size of 3 mm (interquartile range 2.25 mm [ mm]). Kidney stone formation affected ten females and five males. In 8 (53 %) patients, stones were revealed in both kidneys, in 2 (13 %) in the left and in 5 (33 %) in the right kidney only. Ultrasound vs multidetector computed tomography The number of detected stones was significantly higher with MDCT than with US (41 vs 4, p = ). In one patient, a kidney stone was suspected with US, but this stone failed to be detected with MDCT. In two subjects, in whom numerous calculi were seen with MDCT, only one was found to have a kidney stone with US, measuring 15 mm in diameter. The remaining calcifications in both kidneys were not seen with US (Table 2). Discussion None of the patients had clinical signs of kidney stones upon diagnosis of PHPT or other organ manifestations of classical PHPT [22] and were by definition [1] clinically asymptomatic. Following the current recommendations [23], all patients with biochemically proven PHPT who have no contraindications for a surgical intervention were presented in a multidisciplinary endocrine conference. The risks, benefits, and potential complications of surgery were discussed with the patients and all decided surgery as the treatment of choice. In this study protocol, MDCT proved significantly superior to US in the detection rate of clinically silent kidney stones in patients with initially asymptomatic PHPT. As shown in this study, a number of patients clinically classified asymptomatic may have silent organ manifestations and therefore be in fact symptomatic. In many ways, symptomatic patients profit from surgery [2, 9]. In the current guidelines [1], asymptomatic patients compose a patients group inheriting only a relative indication for surgery while in symptomatic patients early surgical intervention is recommended [23], so those patient groups need to be discriminated [24]. Therefore, the current guidelines aim to enhance the screening for oblique organ manifestations by recommending renal examinations by ultrasound, the proportion of patients identified with kidney stones might be smaller if ultrasound is used compared to MDCT and consequently, hidden symptoms might be missed. Another study concluded recently [25], that through the use of aforementioned guidelines more surgical Table 2 Kidney stones detected by ultrasound (US) and multidetector computed tomography (MDCT) Results US Total Positive Negative n % n % n % MDCT Positive Negative Total n = patients; 40 patients were evaluated prospectively
4 292 Langenbecks Arch Surg (2017) 402: candidates are identified. Nevertheless, some patients might persist who do not meet criteria for surgery if only screened with US. We assume that screening for kidney stones by MDCT could direct more patients from this uncertain group towards surgical treatment. Due to the significantly higher number of stone carriers, centers not able or unwilling to perform MDCT to definitively rule out renal involvement should apply a low threshold regarding symptomatology to indicate surgery early because of possibly overlooked kidney stones when applying US only. The superiority of MDCT in determining the size, number, and the position of kidney stones was convincing in this study, and the possibility of low-dose protocols seems to justify the use of ionizing radiation. As shown, there was a larger number of patients with clinically silent kidney stones detected by MDCT compared to US [6, 16], demonstrating the superiority of MDCT and the necessity of an adaption of the current consensus [1]. The performance of MDCT was related to the excellent contrast resolution and discrimination of different attenuation within the kidneys. The lack of acoustic shadowing that may occur with intervening tissue of different acoustic impedance can lead to a miss of stones with US [26]. This could also be the reason for the US diagnosis of kidney stones in one patient that could not be confirmed with MDCT. MDCT captures a volume that includes the entire kidney, allowing a complete evaluation of the organ. With US, due to potentially overlying bowel gas and patients varying body habitus, some areas of the kidney may be hidden [16]. Furthermore, MDCT is less operator-dependent than US which requires skillful radiological expertise [16]. As reported previously, the size of stones seems to influence the detection rate with US. Thus, the median size of stones was 6.5 mm as found with US and 3 mm as detected with MDCT [26]. Most stones missed with US were smaller than 5 mm. Kidney stones with a size of less than 5 mm may pass spontaneously, indicating the limited value of US in follow-up and identification of small stones in known stone formers [16] as well as in distinguishing recurrent from persistent silent kidney stones. Preoperative radiological assessment is crucial to determine the directions of further postoperative follow-up in patients with silent kidney stones [2, 10, 13, 22]. The study documents that MDCT is more sensitive to detect kidney stones than ultrasound. Conclusion Based on low-dose protocols and therefore a lower x-ray exposure, we propose to consider MDCT with its broad availability as the gold standard imaging technique for detecting kidney stones in patients with PHPT to identify silent stone carriers in need of surgical treatment, as by this approach patients can be cured who would otherwise develop stones during follow-up [27]. By applying this technique, the very scarce group of patients with asymptomatic PHPT may be further diminished. The current guidelines on the management of asymptomatic PHPT [1] should be adapted to this finding. If not used primarily, MDCT should particularly be considered in patients in the border zone of indication for surgery. Acknowledgments University of Vienna. Open access funding provided by Medical Authors contributions Study conception and design: B. Niederle, C. Scheuba Acquisition of data: M. Hörmann, G. Prager Analysis and interpretation of data: A. Selberherr, P. Riss Drafting of manuscript: A. Selberherr, B. Niederle Critical revision of manuscript: B. Niederle Compliance with ethical standards Funding Conflict of interest interest. There was no funding from a third party for this study. The authors declare that they have no conflict of Ethical approval All procedures performed in this study were in accordance with the ethical standards of the institutional review board (approval number: 1722/2014) and with the 1964 Helsinki declaration and its later amendments. Informed consent Informed consent was obtained from all individual participants included in the study. Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. References 1. Bilezikian JP, Brandi ML, Eastell R, Silverberg SJ, Udelsman R, Marcocci C, Potts JT Jr (2014) Guidelines for the management of asymptomatic primary hyperparathyroidism: summary statement from the Fourth International Workshop. J Clin Endocrinol Metab 99: Niederle B, Roka R, Fritsch A (1985) Long term results after surgical treatment of primary hyperparathyroidism. Prog Surg 18: Purnell DC, Heath H (1983) The dilemma of asymptomatic hypercalcaemia. Churchill Livingstone, Edinburgh 4. Bilezikian JP (1985) Surgery or no surgery for primary hyperparathyroidism. Ann Intern Med 102: Pak CY, Nicar MJ, Peterson R, Zerwekh JE, Snyder W (1981) A lack of unique pathophysiologic background for nephrolithiasis of primary hyperparathyroidism. J Clin Endocrinol Metab 53:
5 Langenbecks Arch Surg (2017) 402: Cassibba S, Pellegrino M, Gianotti L, Baffoni C, Baralis E, Attanasio R, Guarnieri A, Borretta G & Tassone F 2014 Silent renal stones in primary hyperparathyroidism: prevalence and clinical features. Endocr Pract Schneider DF, Burke JF, Ojomo KA, Clark N, Mazeh H, Sippel RS, Chen H (2013) Multigland disease and slower decline in intraoperative PTH characterize mild primary hyperparathyroidism. Ann Surg Oncol 20: Parikh PP, Allan BJ, Lew JI (2014) Surgical treatment of patients with mildly elevated parathormone and calcium levels. World J Surg 38: Niederle B, Roka R, Woloszczuk W, Klaushofer K, Kovarik J, Schernthaner G (1987) Successful parathyroidectomy in primary hyperparathyroidism: a clinical follow-up study of 212 consecutive patients. Surgery 102: Deaconson TF, Wilson SD, Lemann J Jr (1987) The effect of parathyroidectomy on the recurrence of nephrolithiasis. Surgery 102: Elkoushy MA, Yu AX, Tabah R, Payne RJ, Dragomir A, Andonian S (2014) Determinants of urolithiasis before and after parathyroidectomy in patients with primary hyperparathyroidism. Urology 84: Rejnmark L, Vestergaard P, Mosekilde L (2011) Nephrolithiasis and renal calcifications in primary hyperparathyroidism. J Clin Endocrinol Metab 96: Rowlands C, Zyada A, Zouwail S, Joshi H, Stechman MJ, Scott-Coombes DM (2013) Recurrent urolithiasis following parathyroidectomy for primary hyperparathyroidism. Ann R Coll Surg Engl 95: Walker MD, Nickolas T, Kepley A, Lee JA, Zhang C, McMahon DJ, Silverberg SJ (2014) Predictors of renal function in primary hyperparathyroidism. J Clin Endocrinol Metab 99: Starup-Linde J, Waldhauer E, Rolighed L, Mosekilde L, Vestergaard P (2012) Renal stones and calcifications in patients with primary hyperparathyroidism: associations with biochemical variables. Eur J Endocrinol 166: Fowler KA, Locken JA, Duchesne JH, Williamson MR (2002) US for detecting renal calculi with nonenhanced CT as a reference standard. Radiology 222: Vieweg J, Teh C, Freed K, Leder RA, Smith RH, Nelson RH, Preminger GM (1998) Unenhanced helical computerized tomography for the evaluation of patients with acute flank pain. J Urol 160: Hamm M, Knopfle E, Wartenberg S, Wawroschek F, Weckermann D, Harzmann R (2002) Low dose unenhanced helical computerized tomography for the evaluation of acute flank pain. J Urol 167: Yilmaz S, Sindel T, Arslan G, Ozkaynak C, Karaali K, Kabaalioglu A, Luleci E (1998) Renal colic: comparison of spiral CT, US and IVU in the detection of ureteral calculi. Eur Radiol 8: Hesch RD (1981) Die konservative Therapie des extrarenalen Hyperparathyroidismus. In: Beyer J, Krause U (eds) Therapie des Hyperparathyroidismus. Schattauer, Stuttart, pp Davies M, Fraser WD, Hosking DJ (2002) The management of primary hyperparathyroidism. Clin Endocrinol 57: Silverberg SJ, Shane E, Jacobs TP, Siris E, Bilezikian JP (1999) A 10-year prospective study of primary hyperparathyroidism with or without parathyroid surgery. N Engl J Med 341: Udelsman R, Akerstrom G, Biagini C, Duh QY, Miccoli P, Niederle B, Tonelli F (2014) The surgical management of asymptomatic primary hyperparathyroidism: proceedings of the Fourth International Workshop. J Clin Endocrinol Metab 99: Niederle B, Wemeau JL (2015) Is surgery necessary for mild or asymptomatic hyperparathyroidism? Eur J Endocrinol 173:D13 D Castellano E, Tassone F, Attanasio R, Gianotti L, Pellegrino M, Borretta G (2016) Mild primary hyperparathyroidism as defined in the Italian Society of Endocrinology s consensus statement: prevalence and clinical features. J Endocrinol Investig 39: King W 3rd, Kimme-Smith C, Winter J (1985) Renal stone shadowing: an investigation of contributing factors. Radiology 154: Hasse C, Sitter H, Bachmann S, Zielke A, Koller M, Nies C, Lorenz W, Rothmund M (2000) How asymptomatic is asymptomatic primary hyperparathyroidism? Exp Clin Endocrinol Diabetes 108:
Elena Castellano, Roberto Attanasio, Laura Gianotti, Flora Cesario, Francesco Tassone, and Giorgio Borretta
 ORIGINAL ARTICLE Forearm DXA Increases the Rate of Patients With Asymptomatic Primary Hyperparathyroidism Meeting Surgical Criteria Elena Castellano, Roberto Attanasio, Laura Gianotti, Flora Cesario, Francesco
ORIGINAL ARTICLE Forearm DXA Increases the Rate of Patients With Asymptomatic Primary Hyperparathyroidism Meeting Surgical Criteria Elena Castellano, Roberto Attanasio, Laura Gianotti, Flora Cesario, Francesco
Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand
 International Endocrinology Volume 2012, Article ID 952426, 4 pages doi:10.1155/2012/952426 Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand Poramaporn
International Endocrinology Volume 2012, Article ID 952426, 4 pages doi:10.1155/2012/952426 Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand Poramaporn
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
ORIGINAL ARTICLE. Novel Parathyroid Hormone (1-84) Assay as Basis for Parathyroid Hormone Monitoring in Renal Hyperparathyroidism
 ORIGINAL ARTICLE Novel Parathyroid Hormone (1-84) Assay as Basis for Parathyroid Hormone Monitoring in Renal Hyperparathyroidism Klaus Kaczirek, MD; Gerhard Prager, MD; Philipp Riss, MD; Gerald Wunderer,
ORIGINAL ARTICLE Novel Parathyroid Hormone (1-84) Assay as Basis for Parathyroid Hormone Monitoring in Renal Hyperparathyroidism Klaus Kaczirek, MD; Gerhard Prager, MD; Philipp Riss, MD; Gerald Wunderer,
Case Report Three-Dimensional Dual-Energy Computed Tomography for Enhancing Stone/Stent Contrasting and Stone Visualization in Urolithiasis
 Case Reports in Urology Volume 2013, Article ID 646087, 4 pages http://dx.doi.org/10.1155/2013/646087 Case Report Three-Dimensional Dual-Energy Computed Tomography for Enhancing Stone/Stent Contrasting
Case Reports in Urology Volume 2013, Article ID 646087, 4 pages http://dx.doi.org/10.1155/2013/646087 Case Report Three-Dimensional Dual-Energy Computed Tomography for Enhancing Stone/Stent Contrasting
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
4/20/2015. The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy. Learning Objectives
 The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning
The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning
PRIMARY HYPERPARATHYROIDISM PRIMARY HYPERPARATHYROIDISM. Hyperparathyroidism Etiology. Common Complex Insidious Chronic Global Only cure is surgery
 ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
Normal PTH Levels in Primary Hyperparathyroidism: Still the Same Disease?
 Ann Surg Oncol (2011) 18:3437 3442 DOI 10.1245/s10434-011-1744-x ORIGINAL ARTICLE ENDOCRINE TUMORS Normal PTH Levels in Primary Hyperparathyroidism: Still the Same Disease? Amanda L. Amin, MD, Tracy S.
Ann Surg Oncol (2011) 18:3437 3442 DOI 10.1245/s10434-011-1744-x ORIGINAL ARTICLE ENDOCRINE TUMORS Normal PTH Levels in Primary Hyperparathyroidism: Still the Same Disease? Amanda L. Amin, MD, Tracy S.
Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma
 ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 2 Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma P George, N Philip, B Pawar Citation P George,
ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 2 Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma P George, N Philip, B Pawar Citation P George,
Complementary sestamibi scintigraphy and ultrasound for primary hyperparathyroidism
 Nuclear Medicine and Biomedical Imaging Research Article Complementary sestamibi scintigraphy and ultrasound for primary hyperparathyroidism Yang Z 1,3 *, Li AY 2, Alexander G 3 and Chadha M 3 1 Department
Nuclear Medicine and Biomedical Imaging Research Article Complementary sestamibi scintigraphy and ultrasound for primary hyperparathyroidism Yang Z 1,3 *, Li AY 2, Alexander G 3 and Chadha M 3 1 Department
ORIGINAL ARTICLE. Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism
 Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism Elizabeth A. Mittendorf, MD; Christopher R. McHenry, MD ORIGINAL ARTICLE Background: Persistent
Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism Elizabeth A. Mittendorf, MD; Christopher R. McHenry, MD ORIGINAL ARTICLE Background: Persistent
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy
 "Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
Disclosure. Primary Hyperparathyroidism 4 th IW. Topic Outline. Calcium, Vitamin D, PTH Disorders. I have nothing to disclose related to this topic
 Disclosure Calcium, Vitamin D, PTH Disorders Chienying Liu MD Associate Clinical Professor Division of Endocrinology & Metabolism UCSF I have nothing to disclose related to this topic Topic Outline Calcium/Vitamin
Disclosure Calcium, Vitamin D, PTH Disorders Chienying Liu MD Associate Clinical Professor Division of Endocrinology & Metabolism UCSF I have nothing to disclose related to this topic Topic Outline Calcium/Vitamin
Coexistence of parathyroid adenoma and papillary thyroid carcinoma. Yong Sang Lee, Kee-Hyun Nam, Woong Youn Chung, Hang-Seok Chang, Cheong Soo Park
 J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from the West?
 ecommons@aku Section of Urology Department of Surgery August 1999 Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from
ecommons@aku Section of Urology Department of Surgery August 1999 Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from
Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones
 Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) 30 yr-old woman with 7 yr history
Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) 30 yr-old woman with 7 yr history
Marcin Barczynski, 1 Aleksander Konturek, 2 Alicja Hubalewska-Dydejczyk, 2. Filip Gołkowski, 1 Stanislaw Cichon, 1 Piotr Richter, 1 Wojciech Nowak
 3 rd Chair and Department of General Surgery 1 and Chair and Department of Endocrinology 2 Jagiellonian University, Medical College Head: Prof. Wojciech Nowak, MD, PhD INTRAOPERATIVE BILATERAL INTERNAL
3 rd Chair and Department of General Surgery 1 and Chair and Department of Endocrinology 2 Jagiellonian University, Medical College Head: Prof. Wojciech Nowak, MD, PhD INTRAOPERATIVE BILATERAL INTERNAL
EVALUATION OF SUSPECTED RENAL COLIC PATIENTS WITH UNENHANCED LOW-DOSE MULTI-DETECTOR COMPUTED TOMOGRAPHY
 190 EAST AFRICAN MEDICAL JOURNAL April 2009 East African Medical Journal Vol. 85 No. 4 April 2009 EVALUATION OF SUSPECTED RENAL COLIC PATIENTS WITH UNENHANCED LOW-DOSE MULTI-DETECTOR COMPUTED TOMOGRAPHY
190 EAST AFRICAN MEDICAL JOURNAL April 2009 East African Medical Journal Vol. 85 No. 4 April 2009 EVALUATION OF SUSPECTED RENAL COLIC PATIENTS WITH UNENHANCED LOW-DOSE MULTI-DETECTOR COMPUTED TOMOGRAPHY
Accuracy of ultrasonography for renal stone detection and size determination: is it good enough for management decisions?
 Upper Urinary Tract Accuracy of ultrasonography for renal stone detection and size determination: is it good enough for management decisions? Vishnu Ganesan*,, Shubha De*, Daniel Greene*, Fabio Cesar Miranda
Upper Urinary Tract Accuracy of ultrasonography for renal stone detection and size determination: is it good enough for management decisions? Vishnu Ganesan*,, Shubha De*, Daniel Greene*, Fabio Cesar Miranda
Parathyroid Imaging. A Guide to Parathyroid Surgery
 Parathyroid Imaging A Guide to Parathyroid Surgery Primary Hyperparathyroidism (PHPT) 3 rd most common endocrine disorder after diabetes and hyperthyroidism Prevalence in women 2% Often discovered in asymptomatic
Parathyroid Imaging A Guide to Parathyroid Surgery Primary Hyperparathyroidism (PHPT) 3 rd most common endocrine disorder after diabetes and hyperthyroidism Prevalence in women 2% Often discovered in asymptomatic
AUA Guidelines for Imaging Known or Suspected Ureteral Calculi. Michael Ferrandino, MD Assoc Professor of Urology Duke University Medical Center
 AUA Guidelines for Imaging Known or Suspected Ureteral Calculi Michael Ferrandino, MD Assoc Professor of Urology Duke University Medical Center Imaging for Urolithiasis Justification for the Guidelines
AUA Guidelines for Imaging Known or Suspected Ureteral Calculi Michael Ferrandino, MD Assoc Professor of Urology Duke University Medical Center Imaging for Urolithiasis Justification for the Guidelines
2016 Arizona AACE Meeting: Updated Guidelines for the Management of Primary Hyperparathyroidism (PHPT)
 2016 Arizona AACE Meeting: Updated Guidelines for the Management of Primary Hyperparathyroidism (PHPT) Scott M. Wilhelm, MD, FACS Associate Professor and Section Head Endocrine Surgery University Hospitals-Cleveland
2016 Arizona AACE Meeting: Updated Guidelines for the Management of Primary Hyperparathyroidism (PHPT) Scott M. Wilhelm, MD, FACS Associate Professor and Section Head Endocrine Surgery University Hospitals-Cleveland
Bedside Ultrasound in the Emergency Department to Detect Hydronephrosis for the Evaluation of Suspected Ureteric Colic
 Bedside Ultrasound in the Emergency Department to Detect Hydronephrosis for the Evaluation of Suspected Ureteric Colic Shrestha R, Shakya RM, Khan A ABSTRACT Background Department of Emergency Medicine
Bedside Ultrasound in the Emergency Department to Detect Hydronephrosis for the Evaluation of Suspected Ureteric Colic Shrestha R, Shakya RM, Khan A ABSTRACT Background Department of Emergency Medicine
Predictors of Renal Function in Primary Hyperparathyroidism
 ORIGINAL Endocrine ARTICLE Research Predictors of Renal Function in Primary Hyperparathyroidism Marcella D. Walker, Thomas Nickolas, Anna Kepley, James A. Lee, Chiyuan Zhang, Donald J. McMahon, and Shonni
ORIGINAL Endocrine ARTICLE Research Predictors of Renal Function in Primary Hyperparathyroidism Marcella D. Walker, Thomas Nickolas, Anna Kepley, James A. Lee, Chiyuan Zhang, Donald J. McMahon, and Shonni
RADIOGUIDED PARATHYROIDECTOMY IS SUCCESSFUL IN 98.7% OF SELECTED PATIENTS
 Original Article RADIOGUIDED PARATHYROIDECTOMY IS SUCCESSFUL IN 98.7% OF SELECTED PATIENTS Charles D. Livingston, MD, FACS ABSTRACT Objective: To examine an individualized approach to patients with primary
Original Article RADIOGUIDED PARATHYROIDECTOMY IS SUCCESSFUL IN 98.7% OF SELECTED PATIENTS Charles D. Livingston, MD, FACS ABSTRACT Objective: To examine an individualized approach to patients with primary
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Hyperparathyroidism. When to Suspect, How to Diagnose, When and How to Intervene. Johanna A. Pallotta, MD, FACP, FACE
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
Outline. Parathyroid Localization Studies. Mira Milas MD, FACS Associate Professor of Surgery Director, The Thyroid Center
 Parathyroid Localization Studies Mira Milas MD, FACS Associate Professor of Surgery Director, The Thyroid Center Outline Clinical Context of Primary Hyperparathyroidism Ultrasound, Sestamibi, and Other
Parathyroid Localization Studies Mira Milas MD, FACS Associate Professor of Surgery Director, The Thyroid Center Outline Clinical Context of Primary Hyperparathyroidism Ultrasound, Sestamibi, and Other
Preoperative Localization and Intraoperative Parathyroid Hormone Assay in Korean Patients with Primary Hyperparathyroidism
 Original Article Endocrinol Metab 2014;29:464-469 http://dx.doi.org/10.3803/enm.2014.29.4.464 pissn 2093-596X eissn 2093-5978 Preoperative Localization and Intraoperative Parathyroid Hormone Assay in Korean
Original Article Endocrinol Metab 2014;29:464-469 http://dx.doi.org/10.3803/enm.2014.29.4.464 pissn 2093-596X eissn 2093-5978 Preoperative Localization and Intraoperative Parathyroid Hormone Assay in Korean
Ultra-low dose CT of the acute abdomen: Spectrum of imaging findings
 Ultra-low dose CT of the acute abdomen: Spectrum of imaging findings Poster No.: C-1452 Congress: ECR 2010 Type: Educational Exhibit Topic: GI Tract Authors: P. A. Vlachou, C. Kloeters, S. Kandel, P. Hein,
Ultra-low dose CT of the acute abdomen: Spectrum of imaging findings Poster No.: C-1452 Congress: ECR 2010 Type: Educational Exhibit Topic: GI Tract Authors: P. A. Vlachou, C. Kloeters, S. Kandel, P. Hein,
UPDATES ON PRIMARY HYPERPARATHYROIDISM. Natalie E. Cusano, MD, MS Director, Bone Metabolism Program Lenox Hill Hospital New York, NY
 UPDATES ON PRIMARY HYPERPARATHYROIDISM Natalie E. Cusano, MD, MS Director, Bone Metabolism Program Lenox Hill Hospital New York, NY Disclosures Speaker (Honorarium): Shire Off-label use of estrogen, raloxifene
UPDATES ON PRIMARY HYPERPARATHYROIDISM Natalie E. Cusano, MD, MS Director, Bone Metabolism Program Lenox Hill Hospital New York, NY Disclosures Speaker (Honorarium): Shire Off-label use of estrogen, raloxifene
PRIMARY HYPERPARATHYROIDISM
 PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
Current Concepts in the Evaluation and Management of Abnormal Parathyroid Hormone (PTH) Levels Shireen Fatemi, M.D. April, 2012.
 Current Concepts in the Evaluation and Management of Abnormal Parathyroid Hormone (PTH) Levels Shireen Fatemi, M.D. April, 2012 Disclosures I have no financial relationships with commercial interests,
Current Concepts in the Evaluation and Management of Abnormal Parathyroid Hormone (PTH) Levels Shireen Fatemi, M.D. April, 2012 Disclosures I have no financial relationships with commercial interests,
Primary Hyperparathyroidism
 Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
Approach to a patient with hypercalcemia
 Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Parathyroid Disease Scenarios for the Practicing Clinician. Vijaya Chockalingam MD Faculty Endocrinologist Banner University Medical Center- Phoenix
 Parathyroid Disease Scenarios for the Practicing Clinician Vijaya Chockalingam MD Faculty Endocrinologist Banner University Medical Center- Phoenix Clinical Scenario-1 73 year man (BK) with hypercalcemia
Parathyroid Disease Scenarios for the Practicing Clinician Vijaya Chockalingam MD Faculty Endocrinologist Banner University Medical Center- Phoenix Clinical Scenario-1 73 year man (BK) with hypercalcemia
CALCIUM CREATININE CLEARANCE RATIO IS NOT HELPFUL IN DIFFERENTIATING PRIMARY
 ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
The 82 nd UWI/BAMP CME Conference November 18, Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist
 The 82 nd UWI/BAMP CME Conference November 18, 2017 Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist Disclosures Outline Index case Introduction Etiology Risk factors Acute stone event Conservative
The 82 nd UWI/BAMP CME Conference November 18, 2017 Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist Disclosures Outline Index case Introduction Etiology Risk factors Acute stone event Conservative
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE
 HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
Hyperparathyroidism (primary): diagnosis, assessment and initial management
 National Institute for Health and Care Excellence. Hyperparathyroidism (primary): diagnosis, assessment and initial management NICE guideline . October 2018 This guideline was developed by the
National Institute for Health and Care Excellence. Hyperparathyroidism (primary): diagnosis, assessment and initial management NICE guideline . October 2018 This guideline was developed by the
Effects of surgery on outcome of primary hyperparathyroidism
 1 Effects of surgery on outcome of primary hyperparathyroidism Peter Vestergaard Leif Mosekilde Peer Christiansen Introduction Primary hyperparathyroidism is a disease with effects on many organ systems
1 Effects of surgery on outcome of primary hyperparathyroidism Peter Vestergaard Leif Mosekilde Peer Christiansen Introduction Primary hyperparathyroidism is a disease with effects on many organ systems
Dual Energy CT: a new tool in evaluation of the urinary tract stones composition in clinical practice - initial study
 Dual Energy CT: a new tool in evaluation of the urinary tract stones composition in clinical practice - initial study Poster No.: C-2279 Congress: ECR 2013 Type: Scientific Exhibit Authors: M. Guzi#ski,
Dual Energy CT: a new tool in evaluation of the urinary tract stones composition in clinical practice - initial study Poster No.: C-2279 Congress: ECR 2013 Type: Scientific Exhibit Authors: M. Guzi#ski,
Research Article The Capabilities and Limitations of Clinical Magnetic Resonance Imaging for Detecting Kidney Stones: A Retrospective Study
 Biomedical Imaging Volume 2016, Article ID 4935656, 6 pages http://dx.doi.org/10.1155/2016/4935656 Research Article The Capabilities and Limitations of Clinical Magnetic Resonance Imaging for Detecting
Biomedical Imaging Volume 2016, Article ID 4935656, 6 pages http://dx.doi.org/10.1155/2016/4935656 Research Article The Capabilities and Limitations of Clinical Magnetic Resonance Imaging for Detecting
ORIGINAL ARTICLE. An Optimal Algorithm for Intraoperative Parathyroid Hormone Monitoring
 ORIGINAL ARTICLE An Optimal Algorithm for Intraoperative Parathyroid Hormone Monitoring Melanie L. Richards, MD; Geoffrey B. Thompson, MD; David R. Farley, MD; Clive S. Grant, MD Background: A minimally
ORIGINAL ARTICLE An Optimal Algorithm for Intraoperative Parathyroid Hormone Monitoring Melanie L. Richards, MD; Geoffrey B. Thompson, MD; David R. Farley, MD; Clive S. Grant, MD Background: A minimally
US in non-traumatic acute abdomen. Lalita, M.D. Radiologist Department of radiology Faculty of Medicine ChiangMai university
 US in non-traumatic acute abdomen Lalita, M.D. Radiologist Department of radiology Faculty of Medicine ChiangMai university Sagittal Orientation Transverse (Axial) Orientation Coronal Orientation Intercostal
US in non-traumatic acute abdomen Lalita, M.D. Radiologist Department of radiology Faculty of Medicine ChiangMai university Sagittal Orientation Transverse (Axial) Orientation Coronal Orientation Intercostal
The CaPTHUS Scoring Model revisited: Applicability from. with Primary Hyperparathyroidism
 wjoes The CaPTHUS Scoring Model revisited: Applicability from a UK Cohort 10.5005/jp-journals-10002-1199 with Primary Hyperparathyroidism Original Article The CaPTHUS Scoring Model revisited: Applicability
wjoes The CaPTHUS Scoring Model revisited: Applicability from a UK Cohort 10.5005/jp-journals-10002-1199 with Primary Hyperparathyroidism Original Article The CaPTHUS Scoring Model revisited: Applicability
PTH > 60pg/ml PRIMARY HYPERPARATHYROIDISM. Introduction Biochemical Diagnosis. Normal Parathyroid. Parathyroid Glands
 next speaker: Declan Neeson Belfast/UK SPECT/CT scanning and parathyroid surgery in Southern Trust, N. Ireland D Neeson M Korda, G Gray, C Leonard, M Fawzy, R Lambon Parathyroid Glands PRIMARY HYPERPARATHYROIDISM
next speaker: Declan Neeson Belfast/UK SPECT/CT scanning and parathyroid surgery in Southern Trust, N. Ireland D Neeson M Korda, G Gray, C Leonard, M Fawzy, R Lambon Parathyroid Glands PRIMARY HYPERPARATHYROIDISM
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Boehm BO, Rosinger S, Belyi D, Dietrich JW. The parathyroid
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Boehm BO, Rosinger S, Belyi D, Dietrich JW. The parathyroid
Acute renal colic Radiological investigation in patients with renal colic
 Acute renal colic Radiological investigation in patients with renal colic Mikael Hellström Professor Department of Radiology Sahlgrenska University Hospital Göteborg University 0.9-1.8/1.000 inhabitants
Acute renal colic Radiological investigation in patients with renal colic Mikael Hellström Professor Department of Radiology Sahlgrenska University Hospital Göteborg University 0.9-1.8/1.000 inhabitants
CT staging in sigmoid diverticulitis
 CT staging in sigmoid diverticulitis Poster No.: C-1503 Congress: ECR 2012 Type: Scientific Paper Authors: M. Buchberger, B. von Rahden, J. Schmid, W. Kenn, C.-T. Germer, D. Hahn; Würzburg/DE Keywords:
CT staging in sigmoid diverticulitis Poster No.: C-1503 Congress: ECR 2012 Type: Scientific Paper Authors: M. Buchberger, B. von Rahden, J. Schmid, W. Kenn, C.-T. Germer, D. Hahn; Würzburg/DE Keywords:
Minimally invasive parathyroidectomy with or without intraoperative parathyroid hormone for primary hyperparathyroidism
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2015.89.3.111 Annals of Surgical Treatment and Research Minimally invasive parathyroidectomy with or without intraoperative
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2015.89.3.111 Annals of Surgical Treatment and Research Minimally invasive parathyroidectomy with or without intraoperative
Peroperative PTH testing:
 07. hoofdstuk 07 23-07-2001 09:52 Pagina 69 Peroperative PTH testing: confirmation of successful surgical treatment of primary hyperparathyroidism 7 Smit PC, Thijssen JHH, Borel Rinkes IHM, van Vroonhoven
07. hoofdstuk 07 23-07-2001 09:52 Pagina 69 Peroperative PTH testing: confirmation of successful surgical treatment of primary hyperparathyroidism 7 Smit PC, Thijssen JHH, Borel Rinkes IHM, van Vroonhoven
Papers. Risk of renal stone events in primary hyperparathyroidism before and after parathyroid surgery: controlled retrospective follow up study
 Risk of renal stone events in primary hyperparathyroidism before and after parathyroid surgery: controlled retrospective follow up study Charlotte L Mollerup, Peter Vestergaard, Vibe Gedsø Frøkjær, Leif
Risk of renal stone events in primary hyperparathyroidism before and after parathyroid surgery: controlled retrospective follow up study Charlotte L Mollerup, Peter Vestergaard, Vibe Gedsø Frøkjær, Leif
Diagnosis and Management of Primary Hyperparathyroidism Clinical Practice Today CME
 Diagnosis and Management of Primary Hyperparathyroidism Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Identify patients with primary hyperparathyroidism
Diagnosis and Management of Primary Hyperparathyroidism Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Identify patients with primary hyperparathyroidism
Potential conflicts of interest: None
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene November 6, 2013 Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene November 6, 2013 Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline
Non-calculus causes of renal colic on CT KUB
 Non-calculus causes of renal colic on CT KUB Poster No.: C-1341 Congress: ECR 2010 Type: Scientific Exhibit Topic: Genitourinary Authors: A. Afaq, E. L. Leen; London/UK Keywords: renal colic, CT KUB, appendicitis
Non-calculus causes of renal colic on CT KUB Poster No.: C-1341 Congress: ECR 2010 Type: Scientific Exhibit Topic: Genitourinary Authors: A. Afaq, E. L. Leen; London/UK Keywords: renal colic, CT KUB, appendicitis
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
Normocalcemic Primary Hyperparathyroidism: A Comparison with the Hypercalcemic Form in a Tertiary Referral Population
 Pierreux Jan, Bravenboer Bert. Normocalcemic Primary Hyperparathyroidism: A Horm Metab Res 2018; 00: 00 00 Normocalcemic Primary Hyperparathyroidism: A Comparison with the Hypercalcemic Form in a Tertiary
Pierreux Jan, Bravenboer Bert. Normocalcemic Primary Hyperparathyroidism: A Horm Metab Res 2018; 00: 00 00 Normocalcemic Primary Hyperparathyroidism: A Comparison with the Hypercalcemic Form in a Tertiary
Research Article Usefulness of Nonenhanced Computed Tomography for Diagnosing Urolithiasis without Pyuria in the Emergency Department
 BioMed Research International Volume 2015, Article ID 810971, 6 pages http://dx.doi.org/10.1155/2015/810971 Research Article Usefulness of Nonenhanced Computed Tomography for Diagnosing Urolithiasis without
BioMed Research International Volume 2015, Article ID 810971, 6 pages http://dx.doi.org/10.1155/2015/810971 Research Article Usefulness of Nonenhanced Computed Tomography for Diagnosing Urolithiasis without
In highly resourced health care systems, in which serum calcium is
 The new england journal of medicine Clinical Practice Caren G. Solomon, M.D., M.P.H., Editor Primary Hyperparathyroidism Karl L. Insogna, M.D. This Journal feature begins with a case vignette highlighting
The new england journal of medicine Clinical Practice Caren G. Solomon, M.D., M.P.H., Editor Primary Hyperparathyroidism Karl L. Insogna, M.D. This Journal feature begins with a case vignette highlighting
HPI joint pain/arthritis serum calcium 11.5 PTH 147pg/ml
 HPI 45 yo female Increased calcium level during evaluation for joint pain/arthritis W/U showed serum calcium 11.5 and PTH 147pg/ml (Normal 11-67pg/ml) Otherwise asymptomatic PMH/PSH Arthritis Tonsillectomy
HPI 45 yo female Increased calcium level during evaluation for joint pain/arthritis W/U showed serum calcium 11.5 and PTH 147pg/ml (Normal 11-67pg/ml) Otherwise asymptomatic PMH/PSH Arthritis Tonsillectomy
Cases in Endocrinology
 Bones, Moans and Groans Diagnosing and Treating Primary Hyperparathyroidism By M. Usman Chaudhry, MD Table 1 Laboratory parameters Her bone density had osteopenic T-Scores of -2.3 at lumbar spine, and
Bones, Moans and Groans Diagnosing and Treating Primary Hyperparathyroidism By M. Usman Chaudhry, MD Table 1 Laboratory parameters Her bone density had osteopenic T-Scores of -2.3 at lumbar spine, and
Case 4: 27 yr-old woman with history of kidney stones and hyperparathyroidism.
 Case 4: 27 yr-old woman with history of kidney stones and hyperparathyroidism. Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) Hyperparathyroidism
Case 4: 27 yr-old woman with history of kidney stones and hyperparathyroidism. Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) Hyperparathyroidism
Perioperative parathormone assessment during surgery for primary hyperparathyroidism;
 08. hoofdstuk 08 23-07-2001 09:52 Pagina 79 Perioperative parathormone assessment during surgery for primary hyperparathyroidism; Comparison of four techniques 8 Submitted for publication as Smit PC, Borel
08. hoofdstuk 08 23-07-2001 09:52 Pagina 79 Perioperative parathormone assessment during surgery for primary hyperparathyroidism; Comparison of four techniques 8 Submitted for publication as Smit PC, Borel
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
RADIOLOGIC TECHNOLOGY (526)
 RADIOLOGIC TECHNOLOGY (526) 526-133 DMS General Procedures 2 Radiologic Technology (526) 1 526-130 Introduction to Diagnostic Medical Sonography This course introduces the student to the history of ultrasound
RADIOLOGIC TECHNOLOGY (526) 526-133 DMS General Procedures 2 Radiologic Technology (526) 1 526-130 Introduction to Diagnostic Medical Sonography This course introduces the student to the history of ultrasound
INTRALUMINAL GAS IN NON-PERFORATED ACUTE APPENDICITIS: A predictor of gangrenous appendicitis
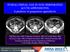 INTRALUMINAL GAS IN NON-PERFORATED ACUTE APPENDICITIS: A predictor of gangrenous appendicitis DM Plata Ariza, MD; E Martínez Chamorro, MD; D Castaño Pardo, MD; M Arroyo López, MD; E Peghini Gavilanes,
INTRALUMINAL GAS IN NON-PERFORATED ACUTE APPENDICITIS: A predictor of gangrenous appendicitis DM Plata Ariza, MD; E Martínez Chamorro, MD; D Castaño Pardo, MD; M Arroyo López, MD; E Peghini Gavilanes,
ORIGINAL ARTICLE. Severity, Clinical Significance, Relationship to Primary Hyperparathyroidism, and Response to Parathyroidectomy
 ORIGINAL ARTICLE Osteoporosis in Multiple Endocrine Neoplasia Type Severity, Clinical Significance, Relationship to Primary Hyperparathyroidism, and Response to Parathyroidectomy John R. Burgess, MD, FRACP;
ORIGINAL ARTICLE Osteoporosis in Multiple Endocrine Neoplasia Type Severity, Clinical Significance, Relationship to Primary Hyperparathyroidism, and Response to Parathyroidectomy John R. Burgess, MD, FRACP;
Dual energy computed tomography for non-invasive differentiation of renal stone composition
 Dual energy computed tomography for non-invasive differentiation of renal stone composition Poster No.: C-0079 Congress: ECR 2012 Type: Scientific Exhibit Authors: R. D. Langer, K. F. W. Neidl van Gorkom,
Dual energy computed tomography for non-invasive differentiation of renal stone composition Poster No.: C-0079 Congress: ECR 2012 Type: Scientific Exhibit Authors: R. D. Langer, K. F. W. Neidl van Gorkom,
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Case Report Spontaneous Pelvic Rupture as a Result of Renal Colic in a Patient with Klinefelter Syndrome
 Volume 2013, Article ID 374973, 4 pages http://dx.doi.org/10.1155/2013/374973 Case Report Spontaneous Pelvic Rupture as a Result of Renal Colic in a Patient with Klinefelter Syndrome Sergey Reva and Yuri
Volume 2013, Article ID 374973, 4 pages http://dx.doi.org/10.1155/2013/374973 Case Report Spontaneous Pelvic Rupture as a Result of Renal Colic in a Patient with Klinefelter Syndrome Sergey Reva and Yuri
Is Structured Reporting More Accurate Than Conventional Reporting in CT Reporting of the Abdomen and Pelvis?
 Is Structured Reporting More Accurate Than Conventional Reporting in CT Reporting of the Abdomen and Pelvis? A M Almuslim, MBBS; J G Ryan, MD; A Murtaza, MD Purpose The purpose of this research is to determine
Is Structured Reporting More Accurate Than Conventional Reporting in CT Reporting of the Abdomen and Pelvis? A M Almuslim, MBBS; J G Ryan, MD; A Murtaza, MD Purpose The purpose of this research is to determine
Hypercalcemia may be detected incidentally. Practice CMAJ. Primary hyperparathyroidism. Primer. Key points. The case. What causes hypercalcemia?
 CMAJ Practice Primer Primary hyperparathyroidism Hafsah Al-Azem HBSc, Aliya Khan MD The case A 17-year-old man presented at the clinic with thirst, lethargy and fatigue that had been ongoing for several
CMAJ Practice Primer Primary hyperparathyroidism Hafsah Al-Azem HBSc, Aliya Khan MD The case A 17-year-old man presented at the clinic with thirst, lethargy and fatigue that had been ongoing for several
Detection of Renal Stones on Portal Venous Phase CT: Comparison of Thin Axial and Coronal Maximum- Intensity-Projection Images
 Genitourinary Imaging Original Research Corwin et al. Detection of Renal Stones on Portal Venous Phase CT Genitourinary Imaging Original Research Michael T. Corwin 1 Justin S. Lee 1 Ghaneh Fananapazir
Genitourinary Imaging Original Research Corwin et al. Detection of Renal Stones on Portal Venous Phase CT Genitourinary Imaging Original Research Michael T. Corwin 1 Justin S. Lee 1 Ghaneh Fananapazir
Investigating the Impact of the Amount of Contrast Material used in Abdominal CT Examinations Regarding the Diagnosis of Appendicolith
 Research Article Investigating the Impact of the Amount of Contrast Material used in Abdominal CT Examinations Regarding the Diagnosis of Appendicolith Eleftherios Lavdas 1,2, Nadia Boci 2, Lia Sarantaenna
Research Article Investigating the Impact of the Amount of Contrast Material used in Abdominal CT Examinations Regarding the Diagnosis of Appendicolith Eleftherios Lavdas 1,2, Nadia Boci 2, Lia Sarantaenna
Iperparatiroidismo normocalcemico: vero o falso?
 Iperparatiroidismo normocalcemico: vero o falso? Bari, 7-10 novembre 2013 TERAPIA E FOLLOW-UP A. Piovesan SCDU Endocrinologia Oncologica AO Città della Salute e della Scienza Molinette Torino THE THIRD
Iperparatiroidismo normocalcemico: vero o falso? Bari, 7-10 novembre 2013 TERAPIA E FOLLOW-UP A. Piovesan SCDU Endocrinologia Oncologica AO Città della Salute e della Scienza Molinette Torino THE THIRD
Surgical treatment of primary hyperparathyroidism due to parathyroid tumor: A 15-year experience
 ONCOLOGY LETTERS 12: 1989-1993, 2016 Surgical treatment of primary hyperparathyroidism due to parathyroid tumor: A 15-year experience LU FENG, XU ZHANG and SHAN TING LIU Department of Head and Neck Surgery,
ONCOLOGY LETTERS 12: 1989-1993, 2016 Surgical treatment of primary hyperparathyroidism due to parathyroid tumor: A 15-year experience LU FENG, XU ZHANG and SHAN TING LIU Department of Head and Neck Surgery,
Length Measurements of the Aorta After Endovascular Abdominal Aortic Aneurysm Repair
 Eur J Vasc Endovasc Surg 18, 481 486 (1999) Article No. ejvs.1999.0882 Length Measurements of the Aorta After Endovascular Abdominal Aortic Aneurysm Repair J. J. Wever, J. D. Blankensteijn, I. A. M. J.
Eur J Vasc Endovasc Surg 18, 481 486 (1999) Article No. ejvs.1999.0882 Length Measurements of the Aorta After Endovascular Abdominal Aortic Aneurysm Repair J. J. Wever, J. D. Blankensteijn, I. A. M. J.
Performance of low-dose, digital X-ray scanning (LODOX) compared to conventional radiography (CR) in the diagnostics of ureteral stones
 Performance of low-dose, digital X-ray scanning (LODOX) compared to conventional radiography (CR) in the diagnostics of ureteral stones Poster No.: C-0193 Congress: ECR 2015 Type: Authors: Keywords: DOI:
Performance of low-dose, digital X-ray scanning (LODOX) compared to conventional radiography (CR) in the diagnostics of ureteral stones Poster No.: C-0193 Congress: ECR 2015 Type: Authors: Keywords: DOI:
SURGERY FOR PRIMARY HYPERPARATHYROIDISM DIAGNOSED AS ACUTE RENAL FAILURE
 CLINICAL CASE SURGERY FOR PRIMARY HYPERPARATHYROIDISM DIAGNOSED AS ACUTE RENAL FAILURE Ana Valea 1, Oana Botezan 2, Roxana Turturea 2, Mara Carsote 3, Crina Rusu 4 1 I. Hatieganu University of Medicine
CLINICAL CASE SURGERY FOR PRIMARY HYPERPARATHYROIDISM DIAGNOSED AS ACUTE RENAL FAILURE Ana Valea 1, Oana Botezan 2, Roxana Turturea 2, Mara Carsote 3, Crina Rusu 4 1 I. Hatieganu University of Medicine
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment
 Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment Poster No.: C-1753 Congress: ECR 2011 Type: Scientific Exhibit Authors: E.
Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment Poster No.: C-1753 Congress: ECR 2011 Type: Scientific Exhibit Authors: E.
Primary hyperparathyroidism. Thierry Pepersack MD PhD Medical Oncology Clinic Institut Jules Bordet Université Libre de Bruxelles (U.L.B.
 Primary hyperparathyroidism Thierry Pepersack MD PhD Medical Oncology Clinic Institut Jules Bordet Université Libre de Bruxelles (U.L.B.) Confirm hyperca: Calculator: Calcium correction in hypoalbuminemia
Primary hyperparathyroidism Thierry Pepersack MD PhD Medical Oncology Clinic Institut Jules Bordet Université Libre de Bruxelles (U.L.B.) Confirm hyperca: Calculator: Calcium correction in hypoalbuminemia
Hypercalcemia. Hypercalcemia: When to Worry, When to Treat! Mineral Metabolism : A Short Course
 Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Parathyroid Imaging: Current Concepts. Maria Gule-Monroe, M.D. Nancy Perrier, M.D.
 Parathyroid Imaging: Current Concepts Maria Gule-Monroe, M.D. Nancy Perrier, M.D. Disclosures None Objectives Ultrasound characteristics of parathyroid adenomas vs. lymph nodes 4D-CT evaluation of hyperparathyroidism
Parathyroid Imaging: Current Concepts Maria Gule-Monroe, M.D. Nancy Perrier, M.D. Disclosures None Objectives Ultrasound characteristics of parathyroid adenomas vs. lymph nodes 4D-CT evaluation of hyperparathyroidism
Role of the Radiologist
 Diagnosis and Treatment of Blunt Cerebrovascular Injuries NORDTER Consensus Conference October 22-24, 2007 Clint W. Sliker, M.D. University of Maryland Medical Center R Adams Cowley Shock Trauma Center
Diagnosis and Treatment of Blunt Cerebrovascular Injuries NORDTER Consensus Conference October 22-24, 2007 Clint W. Sliker, M.D. University of Maryland Medical Center R Adams Cowley Shock Trauma Center
Low-Dose Versus Standard-Dose CT Protocol in Patients with Clinically Suspected Renal Colic
 CT of Renal Colic Genitourinary Imaging Original Research Pierre-Alexandre Poletti 1 Alexandra Platon 1 Olivier T. Rutschmann 2 Franz R. Schmidlin 3 Christophe E. Iselin 3 Christoph D. ecker 1 Poletti
CT of Renal Colic Genitourinary Imaging Original Research Pierre-Alexandre Poletti 1 Alexandra Platon 1 Olivier T. Rutschmann 2 Franz R. Schmidlin 3 Christophe E. Iselin 3 Christoph D. ecker 1 Poletti
Case Report Rare Skeletal Complications in the Setting of Primary Hyperparathyroidism
 Case Reports in Endocrinology Volume 2015, Article ID 139751, 4 pages http://dx.doi.org/10.1155/2015/139751 Case Report Rare Skeletal Complications in the Setting of Primary Hyperparathyroidism Nikos Sabanis,
Case Reports in Endocrinology Volume 2015, Article ID 139751, 4 pages http://dx.doi.org/10.1155/2015/139751 Case Report Rare Skeletal Complications in the Setting of Primary Hyperparathyroidism Nikos Sabanis,
Case 9799 Stanford type A aortic dissection: US and CT findings
 Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
Secondary Hyperparathyroidism: Where are we now?
 Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
PARATHYROID NUCLEAR MEDICINE IMAGING REVIEW DISCLOSURES
 PARATHYROID NUCLEAR MEDICINE IMAGING REVIEW Miguel Hernandez Pampaloni, M.D., Ph.D. Chief, Nuclear Medicine Assistant Professor of Radiology UCSF Department of Radiology and Biomedical Imaging DISCLOSURES
PARATHYROID NUCLEAR MEDICINE IMAGING REVIEW Miguel Hernandez Pampaloni, M.D., Ph.D. Chief, Nuclear Medicine Assistant Professor of Radiology UCSF Department of Radiology and Biomedical Imaging DISCLOSURES
Viral N. Shah*, Chirag S. Shah, Sanjay K. Bhadada and D. Sudhakar Rao
 Clinical Endocrinology (2014) 80, 797 803 doi: 10.1111/cen.12398 ORIGINAL ARTICLE Effect of 25 (OH) D replacements in patients with primary hyperparathyroidism (PHPT) and coexistent vitamin D deficiency
Clinical Endocrinology (2014) 80, 797 803 doi: 10.1111/cen.12398 ORIGINAL ARTICLE Effect of 25 (OH) D replacements in patients with primary hyperparathyroidism (PHPT) and coexistent vitamin D deficiency
Primary hyperparathyroidism in Hong Kong: an analysis of 44 cases
 Primary hyperparathyroidism in Hong Kong: an analysis of 44 cases FKW Chan, SC Tiu, KL Choi, TK Au Yong, LF Tang Primary hyperthyroidism in Hong Kong Primary hyperparathyroidism is increasingly being diagnosed
Primary hyperparathyroidism in Hong Kong: an analysis of 44 cases FKW Chan, SC Tiu, KL Choi, TK Au Yong, LF Tang Primary hyperthyroidism in Hong Kong Primary hyperparathyroidism is increasingly being diagnosed
Since the advent of multichannel serum chemistry
 ONLINE EXCLUSIVE Padmaja Sanapureddy, MD; Vishnu Vardhan Garla, MD; Mallikarjuna Reddy Pabbidi, DVM, PhD Department of Primary Care and Medicine, G.V. (Sonny) Montgomery VA Medical Center, Jackson, Miss
ONLINE EXCLUSIVE Padmaja Sanapureddy, MD; Vishnu Vardhan Garla, MD; Mallikarjuna Reddy Pabbidi, DVM, PhD Department of Primary Care and Medicine, G.V. (Sonny) Montgomery VA Medical Center, Jackson, Miss
Clinical Policy: Cinacalcet (Sensipar) Reference Number: CP.PHAR.61 Effective Date: Last Review Date: Line of Business: Medicaid
 Clinical Policy: (Sensipar) Reference Number: CP.PHAR.61 Effective Date: 05.01.11 Last Review Date: 02.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Sensipar) Reference Number: CP.PHAR.61 Effective Date: 05.01.11 Last Review Date: 02.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Abdomen Sonography Examination Content Outline
 Abdomen Sonography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 Anatomy, Perfusion, and Function Pathology, Vascular Abnormalities, Trauma, and Postoperative Anatomy
Abdomen Sonography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 Anatomy, Perfusion, and Function Pathology, Vascular Abnormalities, Trauma, and Postoperative Anatomy
Demographic and radiologic characteristics of patients with an accessory spleen: An octennial experience
 ORIGINAL ARTICLES Demographic radiologic characteristics of patients with an accessory spleen: An octennial experience Aydin Bora 1, Alpaslan Yavuz 1, Muhammed Alpaslan 1, Güneş Açıkgöz 2, Mehmet Deniz
ORIGINAL ARTICLES Demographic radiologic characteristics of patients with an accessory spleen: An octennial experience Aydin Bora 1, Alpaslan Yavuz 1, Muhammed Alpaslan 1, Güneş Açıkgöz 2, Mehmet Deniz
Case Report Crossed Renal Ectopia without Fusion An Unusual Cause of Acute Abdominal Pain: A Case Report
 Case Reports in Urology Volume 2012, Article ID 728531, 4 pages doi:10.1155/2012/728531 Case Report Crossed Renal Ectopia without Fusion An Unusual Cause of Acute Abdominal Pain: A Case Report D. P. Ramaema,
Case Reports in Urology Volume 2012, Article ID 728531, 4 pages doi:10.1155/2012/728531 Case Report Crossed Renal Ectopia without Fusion An Unusual Cause of Acute Abdominal Pain: A Case Report D. P. Ramaema,
