Adherence and persistence with prescribed chronic medications
|
|
|
- Terence Allen
- 5 years ago
- Views:
Transcription
1 RESEARCH Impact of Appointment-Based Medication Synchronization on Existing Users of Chronic Medications David Holdford, RPh, MS, PhD, FAPhA, and Kunal Saxena, BS, MS ABSTRACT BACKGROUND: Appointment-based medication synchronization (ABMS) has been associated with greater patient adherence and persistence when patients begin taking chronic medications. It is not known whether similar results will be seen for patients who have been taking chronic medications for 6 months or more. OBJECTIVE: To compare the impact of a community pharmacy chain s ABMS program on medication adherence and persistence of existing users of chronic medications with individuals who are not enrolled in the program. METHODS: A retrospective cohort study compared patients receiving ABMS with matched comparison groups receiving usual care. ABMS consisted of synchronizing a patient s medications to be dispensed on a single appointment day every month, a call to the patient prior to the appointment day to address any prescription changes and to remind the patient, and a patient visit to the pharmacy to pick up the medications. Outcomes were 1-year adherence rates using proportion of days covered (PDC) and 1-year nonpersistence rates. Data for this study came from prescription claims records of patients taking 1 of 6 chronic medication classes during the period of December 1, 2011, to February 28, ABMS patients were matched with comparison groups according to prior adherence behavior, medication class, age, gender, and geographic region. RESULTS: Mean PDC scores ranged from 0.73 to 0.91 for ABMS patients (n = 205 to 716) and from 0.57 to 0.71 for usual care depending on the medication class. The percentage of adherent individuals (i.e., PDC 0.80) was 55% to 84% for ABMS participants and 37% to 62% for usual care. Odds of adherence was 2.3 to 3.6 times greater with ABMS. Usual care patients became nonpersistent (61% to 74%) more often than ABMS patients (33% to 44%) with hazard ratios of nonpersistence being 0.39 to 0.67 for individuals in the program. CONCLUSIONS: An ABMS program in a community pharmacy setting was associated with higher rates of adherence and persistence for patients who had been taking chronic medications for at least 6 months. Approximately 18 to 35 additional ABMS participants were adherent for every 100 patients enrolled when compared with usual care. For every 100 patients receiving usual care, 17 to 40 additional patients in the ABMS group were persistent. This study shows that ABMS programs can improve medication adherence and persistence for patients who are newly prescribed or currently taking chronic medications. J Manag Care Spec Pharm. 2015;21(8): Copyright 2015, Academy of Managed Care Pharmacy. All rights reserved. What is already known about this subject Adherence to prescribed chronic medications is a major public health concern. Medication nonadherence and nonpersistence lead to unsuccessful therapy outcomes, negative health effects, and huge economic burden. Patient-centric interventions such as appointment-based medication synchronization (ABMS) have shown significant success in improving patient adherence and persistence to chronic medications in newly enrolled patients (new medication users). What this study adds ABMS was associated with greater adherence and persistence in patients who had been taking chronic medications for at least 6 months (existing medication users). After controlling for prior adherence behavior between ABMS and non-abms patients, or the healthy adherer effect, the results still showed significant improvement in adherence and persistence in ABMS patients compared with non-abms patients. Adherence and persistence with prescribed chronic medications is a major public health concern in the United States and worldwide. Acute and chronic medication therapies are only valuable in achieving positive health outcomes if patients adhere to and persist with their therapeutic plans. 1 Failure to do so leads to negative health consequences and annual costs in the billions of dollars. 2-6 Extensive research over time has shown that adherence and persistence with prescribed plans is an intractable problem. Despite numerous interventions by health care providers in a variety of settings, patients follow prescribed plans only 25% of the time. 7 When prescribed chronic medications, patients adhere roughly 50% of the time Improving adherence to prescribed medication may have greater impact on population health than any other specific medical treatment. 12 Nonadherence to medications is a complex and multifactorial problem that is not easily resolved by simple solutions. 1,12,13 The causes of nonadherence vary depending on individual characteristics (e.g., physical impairments, cognitive problems, age-related concerns, and belief about medicines); the patient s medical condition (e.g., symptoms and comorbidities); health system limitations (e.g., disjointed care and inaccessibility); 662 Journal of Managed Care & Specialty Pharmacy JMCP August 2015 Vol. 21, No. 8
2 therapeutic regimen complexity and associated adverse effects; and socioeconomic concerns (e.g., affordability, low reading and health literacy, and weak social support). 1 This situation requires interventions that are tailored to patient needs and circumstances using various strategies that make medications convenient, provide education and reminders as needed, offer feedback on progress, and provide a therapeutic relationship. 1,12,13 Appointment-based medication synchronization (ABMS) has been promoted as an effective strategy to improve patient adherence and persistence with medication regimens. 14,15 ABMS was first implemented in 1995 by a California pharmacist, John Sykora, to standardize medication dispensing schedules to improve medication management and adherence. ABMS is increasingly being offered by pharmacies as part of the patient-centric and medication synchronization models and as specific programs such as Sync Your Meds and Simplify My Meds. Specific details often vary between programs but the basic ABMS process consists of 3 key features: Pharmacists working with patients to synchronize medication refills to come due on a single day of the month. 2. A regular call (e.g., monthly) from the pharmacy to the patient or designated care provider to identify which medications to fill. This call typically occurs 5 to 7 days prior to the scheduled pharmacy visit and consists of an opportunity to clarify changes in therapy, address managed care issues such as prior authorizations, and engage in mutual problem solving regarding nonadherence issues. This call differs from automatic refill programs, which refill prescriptions on a scheduled basis and notify patients when the prescriptions are ready. With automatic refills, contact with the pharmacy is minimized, leaving little opportunity to proactively address adherence issues. 3. An appointment date where patients are scheduled to pick up medications or have them delivered. On this date, the medications can simply be dispensed or they can be accompanied by medication therapy management, disease management, or other more intensive pharmacist-delivered services. A study of an ABMS program in rural pharmacies in the midwestern United States indicated that the program was associated with greater patient adherence and persistence when patients first start their chronic medications. 15 Patients enrolled in ABMS who received medications in 6 different chronic disease categories had 3.4 to 6.1 times greater odds of adherence over a 1-year period than matched comparisons. Individuals who were not enrolled were at least 50% more likely to stop taking their chronic medications over 1 year. To date, it is not known whether similar results would be seen for patients who have been taking chronic medications over time. The objective of this analysis was to compare the effect on medication adherence and persistence of an ABMS program in community pharmacies with standard of care. Dispensing records were obtained for patients receiving medications from at least 1 of 6 medication categories: angiotensin-converting enzyme inhibitors or angiotensin receptor blockers, beta blockers, dihydropyridine calcium channel blockers, thiazide diuretics, metformin, and statins. These records were compared between ABMS and matched comparisons. The medication categories in this study were chosen because of their widespread use, history of nonadherence and persistence in patients, and importance in achieving therapeutic outcomes when taken as directed. 2,3,9 It was hypothesized that existing medication users who enrolled in the ABMS program would have higher adherence and persistence than patients who were not in the ABMS (matched comparison) group. Methods Study Design This retrospective cohort study was conducted on patients served by Discount Drug Mart, Inc., an Ohio-based drugstore chain of 71 pharmacies in 20 Ohio counties. Data for this study came from prescription claims records of commercially insured individuals collected from December 1, 2011, to February 28, All ABMS patients received 2 or more consecutive fills for 1 of 6 chronic medication classes after enrollment and were followed for 1 year. ABMS patients were matched with comparison patients receiving usual care according to their histories of prior adherence behavior (PAB), medication class, age, gender, and geographic region. Individuals in the matched comparison group included individuals who opted out of the program or were never asked to enroll. The study was approved by the Institutional Review Board of Virginia Commonwealth University. Enrollment Individuals opted in to ABMS after being informed about the availability and details of the program by a clerk, technician, or pharmacist. Although any patient could enroll, patients with multiple, ongoing monthly prescriptions for chronic disease conditions were targeted, especially if gaps in refill patterns were noticed. All enrolled individuals were required to read, understand, and sign an ABMS Patient Agreement Form that reviewed the features of the program and patient requirements to (a) accept a monthly phone call from the pharmacy to discuss prescription refills, (b) have ABMS prescriptions filled with a 1-month supply, (c) pick up medications on a mutually agreed upon assigned appointment date, (d) pay any additional copays needed to synchronize all refills to be due on the same day, (e) have an open dialogue with the pharmacist about physician appointments, hospital/urgent care visits, and changes in health status, and (f) give permission for the pharmacist Vol. 21, No. 8 August 2015 JMCP Journal of Managed Care & Specialty Pharmacy 663
3 to discuss details of the program with the patient s caregiver. Patients who did not consent to the ABMS agreement were excluded from the program. Intervention After patient consent and enrollment, 3 actions occurred in ABMS: synchronization of medications, a monthly call to the patient or family caregiver, and a scheduled appointment to pick up medication at the pharmacy and speak with the pharmacist as needed. In the synchronization phase, the patient and pharmacist chose a monthly appointment day to pick up prescriptions. This one-time synchronization typically consisted of the pharmacist reviewing the patient s medication profile, identifying an anchor prescription to which all other prescriptions would be synchronized, and determining the quantity needed for all other prescriptions to be refilled with the anchor prescription. Another part of synchronization was a contact to the patient s physician to explain ABMS and ask for a one-time prescription for the quantity required for each medication to be synchronized to the anchor. After synchronization, a call was made approximately 7 days prior to the appointment day. During this call, the pharmacist reviewed the patient s medication list, asked about any new or changed prescriptions, and confirmed which prescriptions needed to be filled. Discussions also occurred about physician and hospital visits and any issues with the patient s medications. If necessary, the physician was contacted to resolve any discrepancies. On the date of the appointment visit to the pharmacy, an automated outbound phone call was made to inform the patient that the medications were ready to be picked up. The medications were typically filled 3 days prior to the appointment to give time for the pharmacist to troubleshoot any problems with insurance, inventory shortages, or other issues. When the patient arrived to pick up the medications, the medications were dispensed like any other prescription, or the appointment might be combined with some other medication therapy management service, such as a comprehensive medication review. Measures The outcomes used to assess ABMS were adherence and nonpersistence over a 1-year period. Adherence was measured using proportion of days covered (PDC), and patients were considered adherent with a PDC of at least Nonpersistence was calculated by identifying the date at which a patient stopped taking a medication within the chronic medication category for 30 days or more. At that point, they were labeled nonpersistent. Data Analysis The analysis period for this study was from March 1, 2013, to February 28, 2014 (Figure 1). All prescription claims were limited to a 30-day supply. Since all ABMS synchronized patients were already using the medications at the time of enrollment (i.e., no new users), a 6-month pre-enrollment period for each study patient was used to assess PAB. This 6-month period varied for each patient, depending on when the patient enrolled in the program. Only patients who started the program sometime between December 1, 2011, and the start of the 1-year analysis period, March 1, 2013, were analyzed because 6 months of data prior to that period were not available. Data availability also prevented analysis of any differences in how long patients had been taking their medications. PAB in comparison patients was calculated from data collected in the same time periods. Measures for the ABMS program were compared with usual care. Up to 3 comparison patients per study patient were used to match on PAB, medication class, age, gender, and geographic region using a 2-stage process. Patients were first categorized according to medication class, so patients taking multiple medications could fall into more than 1 class. Patients were then matched within each medication class on age, gender, geographical region, and PAB score. This allowed comparisons of adherence and persistence according to medication use classes. Neither pill burden nor medication use outside of the 6 medication classes were examined in the study. The number of patients in the comparison group who were offered but refused enrollment into the program was not measured. In the original design, sulfonylureas were included in the data analysis, but because of low sample sizes after matching (n = 31 in usual care; n = 35 among ABMS patients), this medication class was excluded from the final analysis. PAB scores were calculated to compare differences in history of medication use between ABMS patients and usual care. 17,18 These scores were constructed using 10 levels based upon patients PDC scores for the 6-month pre-enrollment period (< 0.10, , , , , , , , , and > 0.90). ABMS and comparison patients were assigned PAB scores, which were used in matching. Descriptive statistics and statistical comparisons of adherence and nonpersistence were conducted. Statistical comparisons of PDC between groups used the Friedman test to account for the paired nature of the matched comparisons and the non-normality of the PDC. Comparisons of the proportion of adherent patients in groups were assessed with a univariate conditional logistic regression, which provided the odds of adherence by study and comparison group. Because no dropout date was provided, patients who dropped out could not be censored. Hence, using the intention-to-treat principle, patients who dropped out were assumed to continue with the program as a conservative measure, and time of medication discontinuation was analyzed with a univariate conditional Cox proportional hazards regression. A P value of < 0.05 was considered statistically significant. The data analysis was conducted using SAS software, version 9.4 (SAS Institute Inc., Cary, NC). 664 Journal of Managed Care & Specialty Pharmacy JMCP August 2015 Vol. 21, No. 8
4 FIGURE 1 Sample Selection Flowchart Total claims containing ABMS and non-abms prescriptions n = 3,218,238 ABMS prescriptions (study) n = 164,019 Non-ABMS prescriptions (control) n = 3,054,219 N = 74,334 excluded N = 1,785,522 excluded Prescriptions with enrollment date before March 1, 2013 n = 89,685) N = 51,509 excluded Prescriptions with date of first fill at least 6 months before the enrollment date n = 38,176 N = 325,314 excluded Prescriptions with date of first fill on or before September 1, 2012 n = 1,268,697 Prescriptions with only 30 days of supply n = 943,383 N = 327,612 excluded Prescriptions with first fill post-abms enrollment within 30 days n = 21,791 N = 2,298 excluded Prescriptions with only 30 days of supply n = 19,493 Final sample of ABMS and non-abms prescription claims n = 962,876 ABMS = appointment-based medication synchronization. Results Descriptive information about patients and their PAB is presented in Table 1 and Figure 2, respectively. The average patient was female, between aged 59 and 66 years, and had some form of prescription insurance coverage. Because of matching, ABMS and usual care were similar in PAB, medication class, age, gender, and geographic region. There was little difference between the groups in plan type. Final sample sizes for ABMS and comparison patients ranged from 140 to 1,133 (Table 2). Medication adherence differed between ABMS and usual care prior to the start of the study (Figure 2). This finding was anticipated based upon an expectation that patients who were predisposed to be adherent would be more likely to enroll in adherence programs. This appeared to be the case because the percentage of adherent patients as measured by PAB scores was more than 17 points higher for ABMS patients for all medication categories before enrolling in the program. Nevertheless, mean PDC scores for ABMS patients in all drug classes were significantly greater than those for usual care after 1 year even after matching for PAB. Mean PDCs for the comparison group ranged from 0.57 to 0.71, while those for patients in the ABMS program ranged from 0.73 to Vol. 21, No. 8 August 2015 JMCP Journal of Managed Care & Specialty Pharmacy 665
5 TABLE 1 Description of Patients (ABMS and Usual Care) Eligible for and Enrolled in ABMS Program Prior to Matching Variable ACEIs/ARBs Beta Blockers DCCBs Thiazide Diuretics Metformin Statins Total 37,189 27,251 15,427 23,801 7,373 33,754 Age (years), mean (SD) 62.6 (14.8) 64.2 (16.2) 66.1 (15.7) 64.6 (16.4) 59.2 (14.7) 63.7 (13.2) Female (%) Number of ABMS patients Number of controls 36,486 26,707 15,101 23,302 7,168 33,038 Plan type (%) Cash Third party ABMS = appointment-based medication synchronization; ACEI = angiotensin-converting enzyme inhibitor; ARB = angiotensin receptor blocker; DCCB = dihydropyridine calcium channel blocker; SD = standard deviation. Percentage of Patients with PAB Scores over 0.80 FIGURE ACEIs/ARBs Prior Adherence Behavior of ABMS and Usual Care Before Matching 39.8 Beta blockers 42.3 DCCBs Metformin Statins Thiazides The percentage of adherent patients (i.e., PDC 0.80) was significantly greater for ABMS patients compared with usual care (Table 3). In the comparison group, approximately 37% to 62% were found to be adherent depending on the drug class. In contrast, the percentage of adherent patients in the ABMS program ranged from 55% to 84%. When comparing differences between groups, approximately 18 to 35 additional individuals were adherent in the ABMS group for every 100 patients depending on drug class. When evaluating the odds of adherence, patients enrolled in the program had 2.3 to 3.6 times greater odds of adherence (depending on drug class) compared with usual care Study Control ABMS = appointment-based medication synchronization; ACEI = angiotensin-converting enzyme inhibitor; ARB = angiotensin receptor blocker; DCCB = dihydropyridine calcium channel blocker; PAB = prior adherence behavior TABLE 2 Drug Class Proportion of Days Covered by Drug Class Usual Care ABMS Patients Mean Mean n PDC SD n PDC SD P Value ACEIs/ARBs 1, < Beta blockers < DCCBs < Thiazide diuretics Metformin Statins 1, < ABMS = appointment-based medication synchronization; ACEI = angiotensinconverting enzyme inhibitor; ARB = angiotensin receptor blocker; DCCB = dihydropyridine calcium channel blocker; PDC = proportion of days covered; SD = standard deviation. The percentage considered nonpersistent according to group and hazard ratios are displayed in Table 4. In the comparison group, approximately 61% to 74% became nonpersistent within 1 year after starting, while 33% to 44% became nonpersistent in the ABMS group. When comparing persistence between groups for every 100 individuals, approximately 17 to 40 additional individuals remained persistent for 1 year in the ABMS group. Compared with usual care, ABMS patients had a 33% to 61% lower likelihood of nonpersistence, depending on the drug class. Discussion This study provides evidence for the effectiveness of ABMS programs in community pharmacy settings for improving adherence and persistence with chronic medications. Patients enrolled in ABMS programs were significantly more adherent and persistent with medicines compared with the standard of care when controlling for PAB, medication class, age, gender, and geographic region. The findings were consistent across all 6 drug classes studied. 666 Journal of Managed Care & Specialty Pharmacy JMCP August 2015 Vol. 21, No. 8
6 TABLE 3 Drug Class Percentage of Patients Adherent and Odds Ratios from Univariate Logistic Regression Adherent (%) a Usual Care ABMS Increase in % Adherent with ABMS OR (95% CI) P Value ACEIs/ARBs < Beta blockers < DCCBs < Thiazide diuretics < Metformin Statins < a Percentage of individuals with PDC > 80%. ABMS =appointment-based medication synchronization; ACEI = angiotensinconverting enzyme inhibitor; ARB = angiotensin receptor blocker; CI = confidence interval; DCCB = dihydropyridine calcium channel blocker; OR = odds ratio; PDC = proportion of days covered. This study makes an important contribution in the area of medication adherence and persistence by examining the impact of medication synchronization on a different population than past research. In contrast to other research, which looked at the effect of ABMS on patients who were first starting chronic medications, this study examined patients who had been taking chronic medications for at least 6 months. 14,15 This patient population is significant because nonadherence is more likely to occur in patients who fill new prescriptions, with approximately 50% discontinuing therapy in the first 6 months. 5,9,12 Excluding these relatively nonadherent patients from the analysis makes the overall study population more adherent and thereby more difficult to improve upon. In other words, marginal improvements in adherence are harder with adherent populations. This study showed that ABMS works on these patients, too. Another contribution of this study was controlling for previous adherence behavior between ABMS patients and usual care. Only a few previous studies have controlled for the healthy adherer effect, a situation in which patients who are predisposed to take medicines more consistently will be more likely to enroll in adherence programs This study matched groups using PAB scores to control for the healthy adherer effect. Figure 2 demonstrates potential evidence for the healthy adherer effect in the studied population. Patients who enrolled in the ABMS program were much more adherent at the beginning of the study than comparison groups more than 17 percentage points in all 6 groups. When this effect was reduced by matching according to PAB scores, patients in the ABMS program still showed significantly higher adherence and persistence than the comparison groups. The ABMS program may be effective because it is a complex intervention consisting of a variety of opportunities to TABLE 4 Drug Class Rates of Nonpersistence and Hazard Ratios Nonpersistence (%) Usual Care ABMS Difference in Nonpersistence with ABMS HR (95% CI) P Value ACEIs/ARBs < Beta blockers < DCCBs < Thiazide diuretics < Metformin Statins < ABMS = appointment-based medication synchronization; ACEI = angiotensinconverting enzyme inhibitor; ARB = angiotensin receptor blocker; CI = confidence interval; DCCB = dihydropyridine calcium channel blocker; HR = hazard ratio. influence how patients take their medications. The first is the enrollment process, which requires each patient to commit to actively participating in medication therapy. The commitment to enroll can increase the likelihood that patients will take their medications. 20 The ABMS program also provides regular opportunities for the pharmacist, patient, and physician to communicate and solve problems, which are key activities for improving medication adherence and persistence. 21,22 Finally, ABMS reminds patients to pick up their prescriptions and simplifies the physical acquisition of medications. It is not clear if the findings of this study would be duplicated for programs that do not have all of the elements of ABMS. Similar to a medication, a minor change in the content of the ABMS program may alter its overall effectiveness in patients. In addition to the clinical benefits of ABMS, the findings of this research have important financial implications for health plans and pharmacies. Significant improvements in adherence can help Medicare Advantage plans improve their Medicare star ratings, which may make them eligible for performance bonuses and rebates. Medication adherence of plan members is an important factor in star ratings, and improving adherence for the medications in this research diabetic medications, statin therapies, and hypertension drugs can increase compensation. Pharmacies can benefit from ABMS in a variety of ways. On the revenue side, ABMS can reduce lost sales due to nonadherence and help pharmacies make a strong case for having access to patients in preferred pharmacy networks. Pharmacies that show the ability to drive patient medication adherence and persistence will be able to demonstrate their value to health plan administrators. On the cost side, ABMS can help pharmacists manage inventory, improve workflow, and manage personnel costs better. No evidence is currently available about the real financial benefits of ABMS, but the economic logic is persuasive. Vol. 21, No. 8 August 2015 JMCP Journal of Managed Care & Specialty Pharmacy 667
7 Limitations There are some limitations associated with the findings of this study. The findings of the current work may not be duplicated in other settings, although research indicates external validity for the results. A study examining the ABMS program on a different patient population located in another geographic setting showed consistent results with our study. 3 In addition, a white paper summarizing other medication synchronization programs also indicated support for the effectiveness of ABMS in a broad range of geographic and community settings. 4 This analysis did not control for all factors affecting adherence to medications. Factors not addressed in the study design included patient insurance status, complexity of medication regimens, severity of conditions, and level of patient motivation and engagement in health care. It also used pharmacy prescription fill data, which may not reflect how patients actually take their medications. In addition, the adherence and persistence measures in this study do not indicate whether the patients actually take the medications they pick up or take them as directed. It is possible that some patients simply stock pile their medications or take them inappropriately. The possibility of self-selection bias is another limitation. The people who sign up for an ABMS program might be inherently different from those who do not (e.g., level of engagement or interest in health care). Also, some patients labeled as nonpersistent may have simply switched pharmacies. These limitations were not addressed in the design of this study. Conclusions This is the first study to assess the impact of ABMS on community pharmacy patients who have been taking their chronic medications for at least 6 months. The ABMS program is associated with improved patient adherence and reduced likelihood of nonpersistence. One might expect further improvements in results over time, since this is a study of a new program in which pharmacists are just learning how to integrate it into their systems. As methods become more standardized and best practices are learned and implemented through continuous quality improvement, the impact of ABMS may improve as experience is gained. Authors DAVID HOLDFORD, RPh, MS, PhD, FAPhA, is Professor of Pharmacoeconomics and Health Outcomes, and KUNAL SAXENA, BS, MS, is a PhD Candidate, Department of Pharmacotherapy & Outcomes Science, Virginia Commonwealth University School of Pharmacy, Richmond, Virginia. AUTHOR CORRESPONDENCE: David Holdford, RPh, MS, PhD, FAPhA, McGuire Hall, Rm. 213, P.O. Box , 1112 E. Clay St., Richmond, VA Tel.: ; Fax: ; daholdfo@vcu.edu. DISCLOSURES Funding for this study was contributed by Pfizer. The authors had complete control over preparation, writing, revision, and approval of this manuscript. The authors declare no conflict of interest. Study concept and design were primarily contributed by Holdford, along with Saxena. Saxena was primarily responsible for data collection and interpretation, along with Holdford. Manuscript writing and revision was performed primarily by Holdford, along with Saxena. REFERENCES 1. Sabate E, ed. Adherence to long-term therapy: evidence for action. World Health Organization Available at: Accessed June 24, Wong MC, Tam WW, Cheung CS, et al. Drug adherence and the incidence of coronary heart disease- and stroke-specific mortality among 218,047 patients newly prescribed an antihypertensive medication: a fiveyear cohort study. Int J Cardiol. 2013;168(2): Rasmussen JN, Chong A, Alter DA. Relationship between adherence to evidence-based pharmacotherapy and long-term mortality after acute myocardial infarction. JAMA. 2007;297(2): Sokol MC, McGuigan KA, Verbrugge RR, Epstein RS. Impact of medication adherence on hospitalization risk and healthcare cost. Med Care. 2005;43(6): Osterberg L, Blaschke T. Adherence to medication. N Engl J Med. 2005;353(5): Cutler DM, Everett W. Thinking outside the pillbox medication adherence as a priority for health care reform. N Engl J Med. 2010;362(17): Dimatteo MR. Variations in patients adherence to medical recommendations: a quantitative review of 50 years of research. Med Care. 2004;42(3): Benner JS, Glynn RJ, Mogun H, Neumann PJ, Weinstein MC, Avorn J. Long-term persistence in use of statin therapy in elderly patients. JAMA. 2002;288(4): Cramer JA, Benedict A, Muszbek N, Keskinaslan A, Khan ZM. The significance of compliance and persistence in the treatment of diabetes, hypertension and dyslipidaemia: a review. Int J Clin Pract. 2008;62(1): Avorn J, Monette J, Lacour A, et al. Persistence of use of lipid-lowering medications: a cross-national study. JAMA. 1998;279(18): Briesacher BA, Andrade SE, Fouayzi H, Chan KA. Comparison of drug adherence rates among patients with seven different medical conditions. Pharmacotherapy. 2008;28(4): Haynes RB, Ackloo E, Sahota N, McDonald HP, Yao X. Interventions for enhancing medication adherence. Cochrane Database Syst Rev. 2008;(2):CD Viswanathan M, Golin CE, Jones CD, et al. Interventions to improve adherence to self-administered medications for chronic diseases in the United States: a systematic review. Ann Intern Med. 2012;157(11): American Pharmacists Association Foundation. Pharmacy s appointment based model: a prescription synchronization program that improves adherence. APhA Foundation White Paper. August 30, Available at: FINAL (3).pdf. Accessed June 24, Holdford DA, Inocencio TJ. Adherence and persistence associated with an appointment-based medication synchronization program. J Am Pharm Assoc (2003). 2013;53(6): Pharmacy Quality Alliance. PQA performance measures. Updated May Available at: Accessed June 24, Journal of Managed Care & Specialty Pharmacy JMCP August 2015 Vol. 21, No. 8
8 17. Iyengar R, Henderson R, Visaria J, Glave FS. Dispensing channel and medication adherence: evidence across 3 therapy classes. Am J Manag Care. 2013;19(10): Iyengar RN, Balagere DS, Henderson RR, LeFrancois AL, Rabbitt RM, Frazee SG. Association between dispensing channel and medication adherence among medicare beneficiaries taking medications to treat diabetes, high blood pressure, or high blood cholesterol. J Manag Care Spec Pharm. 2014;20(8): Available at: August/18390/1033.html. 19. Patrick AR, Shrank WH, Glynn RJ, et al. The association between statin use and outcomes potentially attributable to an unhealthy lifestyle in older adults. Value Health. 2011;14(4): Putnam DE, Finney JW, Barkley PL, Bonner MJ. Enhancing commitment improves adherence to a medical regimen. J Consult Clin Psychol. 1994;62(1): Haskard Zolnierek KB, DiMatteo MR. Physician communication and patient adherence to treatment: a meta-analysis. Med Care. 2009;47(8): Brunton SA. Improving medication adherence in chronic disease management. J Fam Pract. 2011;60(4 Suppl Improving):S1-S8. Vol. 21, No. 8 August 2015 JMCP Journal of Managed Care & Specialty Pharmacy 669
Leverage Healthcare Technology Applications to Improve Primary Nonadherence.
 Leverage Healthcare Technology Applications to Improve Primary Nonadherence. Page 2 Medication adherence starts with assessing a patient s opportunity for having positive outcomes on a specific therapy.
Leverage Healthcare Technology Applications to Improve Primary Nonadherence. Page 2 Medication adherence starts with assessing a patient s opportunity for having positive outcomes on a specific therapy.
9/25/15. Pharmacy Quality Measures: Financial Support. Learning Objectives. Speaker Disclosure. Access to Preferred Networks and Clinical Performance
 Pharmacy Quality Measures: Action Steps for Improvement Financial Support Financial support was provided for this activity through an unrestricted grant from Health Mart Systems, Inc. Christine Jacobson
Pharmacy Quality Measures: Action Steps for Improvement Financial Support Financial support was provided for this activity through an unrestricted grant from Health Mart Systems, Inc. Christine Jacobson
Disclosure. Learning Objectives 6/4/2014. Medication Adherence: Challenges and Opportunities
 Medication Adherence: Challenges and Opportunities Jessica W. Skelley, Pharm D., BCACP Assistant Professor of Pharmacy Practice McWhorter School of Pharmacy, Samford University jmwhalen@samford.edu Disclosure
Medication Adherence: Challenges and Opportunities Jessica W. Skelley, Pharm D., BCACP Assistant Professor of Pharmacy Practice McWhorter School of Pharmacy, Samford University jmwhalen@samford.edu Disclosure
The University of Mississippi School of Pharmacy
 LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
Medication nonadherence is a major barrier to the provision
 MANAGERIAL Cost-Benefit of Appointment-Based Medication Synchronization in Community Pharmacies Julie A. Patterson, BS; David A. Holdford, PhD, MS, BSPharm; and Kunal Saxena, PhD, MS Medication nonadherence
MANAGERIAL Cost-Benefit of Appointment-Based Medication Synchronization in Community Pharmacies Julie A. Patterson, BS; David A. Holdford, PhD, MS, BSPharm; and Kunal Saxena, PhD, MS Medication nonadherence
Improving Adherence to Chronic Medications: The Physicians Role and How 340b Can Help
 Improving Adherence to Chronic Medications: The Physicians Role and How 340b Can Help William Shrank MD MSHS Division of Pharmacoepidemiology & Pharmacoeconomics Harvard Medical School wshrank@partners.org
Improving Adherence to Chronic Medications: The Physicians Role and How 340b Can Help William Shrank MD MSHS Division of Pharmacoepidemiology & Pharmacoeconomics Harvard Medical School wshrank@partners.org
Improving Medication Adherence through Collaboration between Colleges of Pharmacy and Community Pharmacies
 Improving Medication Adherence through Collaboration between Colleges of Pharmacy and Community Pharmacies Megan Willson, PharmD, BCPS; Catrina Schwartz, PharmD, BS; Jennifer Robinson, PharmD Spokane,
Improving Medication Adherence through Collaboration between Colleges of Pharmacy and Community Pharmacies Megan Willson, PharmD, BCPS; Catrina Schwartz, PharmD, BS; Jennifer Robinson, PharmD Spokane,
ADHERTENCE AND COMPLIANCE TO TREATMENTS
 ADHERTENCE AND COMPLIANCE TO TREATMENTS Sobhi DADA, MD, FACC, FESC Consultant cardiology Hammoud Hospital- University medical center Saida, Lebanon Adherence Mosby s Medical Dictionary defines adherence
ADHERTENCE AND COMPLIANCE TO TREATMENTS Sobhi DADA, MD, FACC, FESC Consultant cardiology Hammoud Hospital- University medical center Saida, Lebanon Adherence Mosby s Medical Dictionary defines adherence
Nonadherence to chronic medications contributes to
 BRIEF REPORT Pharmacy-based Interventions to Reduce Primary Medication Nonadherence to Cardiovascular Medications Michael A. Fischer, MD, MS,* Niteesh K. Choudhry, MD, PhD,* Katsiaryna Bykov, PharmD, MS,*
BRIEF REPORT Pharmacy-based Interventions to Reduce Primary Medication Nonadherence to Cardiovascular Medications Michael A. Fischer, MD, MS,* Niteesh K. Choudhry, MD, PhD,* Katsiaryna Bykov, PharmD, MS,*
High blood pressure (BP) significantly. After the Diagnosis: Adherence and Persistence With Hypertension Therapy REPORTS
 After the Diagnosis: Adherence and Persistence With Hypertension Therapy Abstract Poor adherence to therapy is a major reason that a large percentage of patients with hypertension fail to achieve good
After the Diagnosis: Adherence and Persistence With Hypertension Therapy Abstract Poor adherence to therapy is a major reason that a large percentage of patients with hypertension fail to achieve good
Payers continue to search for effective ways to control
 At a Glance Practical Implications p 218 Author Information p 221 Full text and PDF www.ajpblive.com Value-Based Benefit Design and Healthcare Utilization in Asthma, Hypertension, and Diabetes Benefit
At a Glance Practical Implications p 218 Author Information p 221 Full text and PDF www.ajpblive.com Value-Based Benefit Design and Healthcare Utilization in Asthma, Hypertension, and Diabetes Benefit
Rethink. Adherence. David D. Pope, PharmD, CDE Editor-in-Chief, CreativePharmacist.com Brands
 Rethink. Adherence. David D. Pope, PharmD, CDE Editor-in-Chief, CreativePharmacist.com Brands Objectives Identify patient barriers to medication adherence. Describe the clinical and economic impact of
Rethink. Adherence. David D. Pope, PharmD, CDE Editor-in-Chief, CreativePharmacist.com Brands Objectives Identify patient barriers to medication adherence. Describe the clinical and economic impact of
Trends in adherence to secondary prevention medications in elderly post-myocardial infarction patients y
 pharmacoepidemiology and drug safety 2008; 17: 1189 1196 Published online 27 October 2008 in Wiley InterScience (www.interscience.wiley.com).1671 ORIGINAL REPORT Trends in adherence to secondary prevention
pharmacoepidemiology and drug safety 2008; 17: 1189 1196 Published online 27 October 2008 in Wiley InterScience (www.interscience.wiley.com).1671 ORIGINAL REPORT Trends in adherence to secondary prevention
Modernized Reference Drug Program
 Modernized Reference Drug Program Monitoring Report For the period ending May 31, 2017 Issued: November 2017 Published by: Pharmaceutical Services Division and Health Sector Information, Analysis and Reporting
Modernized Reference Drug Program Monitoring Report For the period ending May 31, 2017 Issued: November 2017 Published by: Pharmaceutical Services Division and Health Sector Information, Analysis and Reporting
Digital Technologies: The Solutions to Poor Medication Adherence?
 Digital Technologies: The Solutions to Poor Medication Adherence? Jeffrey Mesaros, PharmD Annual Meeting & Exposition Seattle, Washington March 22-25 1 Disclosures The views and opinions expressed in the
Digital Technologies: The Solutions to Poor Medication Adherence? Jeffrey Mesaros, PharmD Annual Meeting & Exposition Seattle, Washington March 22-25 1 Disclosures The views and opinions expressed in the
Κώστας Τσιούφης Iπποκράτειο Γ.Ν.Α
 Χρόνιες παθήσεις, παράλληλη φαρμακευτική αγωγή και συμμόρφωση στη θεραπεία σε ασθενείς με συννοσηρότητα Ο ρόλος της πολυφαρμακίας και των πολλαπλών θεραπειών. H συμμόρφωση στη θεραπεία του ασθενή με συννοσηρότητες.
Χρόνιες παθήσεις, παράλληλη φαρμακευτική αγωγή και συμμόρφωση στη θεραπεία σε ασθενείς με συννοσηρότητα Ο ρόλος της πολυφαρμακίας και των πολλαπλών θεραπειών. H συμμόρφωση στη θεραπεία του ασθενή με συννοσηρότητες.
The practice of using multiple medications occurs in many
 RESEARCH Adherence to Multiple Medications Prescribed for a Chronic Disease: A Methodological Investigation Ramsankar Basak, PhD; David J. McCaffrey, III, RPh, PhD; John P. Bentley, PhD; Sarahmona M. Przybyla,
RESEARCH Adherence to Multiple Medications Prescribed for a Chronic Disease: A Methodological Investigation Ramsankar Basak, PhD; David J. McCaffrey, III, RPh, PhD; John P. Bentley, PhD; Sarahmona M. Przybyla,
Getting Hypertension Under Control
 Getting Hypertension Under Control Learning Objectives EXPLAIN the factors involved in patient medication non-adherence. OUTLINE the results of studies focusing on medication adherence issues in patients
Getting Hypertension Under Control Learning Objectives EXPLAIN the factors involved in patient medication non-adherence. OUTLINE the results of studies focusing on medication adherence issues in patients
2015 Annual Convention
 2015 Annual Convention Date: Tuesday, October 13, 2015 Time: 8:00 am 9:30 am Location: Gaylord National Harbor Resort and Convention Center, National Harbor 2 Title: Activity Type: Speaker: Benefit from
2015 Annual Convention Date: Tuesday, October 13, 2015 Time: 8:00 am 9:30 am Location: Gaylord National Harbor Resort and Convention Center, National Harbor 2 Title: Activity Type: Speaker: Benefit from
REDUCING COSTS AND IMPROVING HYPERTENSION MANAGEMENT
 REDUCING COSTS AND IMPROVING HYPERTENSION MANAGEMENT Vida Stankus 1, Brenda Hemmelgarn 2, Norm RC Campbell 2, Guanmin Chen 2, Finlay A McAlister 1, Ross T Tsuyuki 1 1 EPICORE Centre, Department of Medicine,
REDUCING COSTS AND IMPROVING HYPERTENSION MANAGEMENT Vida Stankus 1, Brenda Hemmelgarn 2, Norm RC Campbell 2, Guanmin Chen 2, Finlay A McAlister 1, Ross T Tsuyuki 1 1 EPICORE Centre, Department of Medicine,
outcome measures were adherence, medication possession ratio (MPR), persistence, prescription count, and duration of therapy.
 ORIGINAL RESEARCH Patient Adherence with HMG Reductase Inhibitor Therapy among Users of Two Types of Prescription Services by T. Jeffrey White, Pharm.D., M.S., Eunice Chang, Ph.D., Scott Leslie, M.P.H.,
ORIGINAL RESEARCH Patient Adherence with HMG Reductase Inhibitor Therapy among Users of Two Types of Prescription Services by T. Jeffrey White, Pharm.D., M.S., Eunice Chang, Ph.D., Scott Leslie, M.P.H.,
How pharmacy and retail health can support health and wellness. Nancy Gagliano Chief Medical Officer, MC September, 2014
 How pharmacy and retail health can support health and wellness Nancy Gagliano Chief Medical Officer, MC September, 2014 2 An important decision for public health Current Health Care Challenges The State
How pharmacy and retail health can support health and wellness Nancy Gagliano Chief Medical Officer, MC September, 2014 2 An important decision for public health Current Health Care Challenges The State
Medication adherence, defined as taking medications as
 Dispensing Channel and Medication Adherence: Evidence Across 3 Therapy Classes Reethi Iyengar, PhD, MBA, MHM; Rochelle Henderson, PhD, MPA; Jay Visaria, PhD, MPH; and Sharon Glave Frazee, PhD, MPH Objectives:
Dispensing Channel and Medication Adherence: Evidence Across 3 Therapy Classes Reethi Iyengar, PhD, MBA, MHM; Rochelle Henderson, PhD, MPA; Jay Visaria, PhD, MPH; and Sharon Glave Frazee, PhD, MPH Objectives:
Improve the Adherence, Save the Life
 Improve the Adherence, Save the Life Park, Chang Gyu Korea University Guro Hospital Cardiovascular Center Seoul, Korea Modifiable CVD Risk Factors Obesity BMI Hypertension Cholesterol LDL HDL Diabetes
Improve the Adherence, Save the Life Park, Chang Gyu Korea University Guro Hospital Cardiovascular Center Seoul, Korea Modifiable CVD Risk Factors Obesity BMI Hypertension Cholesterol LDL HDL Diabetes
Hypertension and diabetes treatments and risk of adverse outcomes among breast cancer patients. Lu Chen
 Hypertension and diabetes treatments and risk of adverse outcomes among breast cancer patients Lu Chen A dissertation submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy
Hypertension and diabetes treatments and risk of adverse outcomes among breast cancer patients Lu Chen A dissertation submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy
Prescription Pattern of Anti-Hypertensive Drugs in Adherence to JNC- 7 Guidelines
 American Journal of Pharmacology and Toxicology Original Research Paper Prescription Pattern of Anti-Hypertensive Drugs in Adherence to JNC- 7 Guidelines 1 Krishna Murti, 1 M. Arif Khan, 1 Akalanka Dey,
American Journal of Pharmacology and Toxicology Original Research Paper Prescription Pattern of Anti-Hypertensive Drugs in Adherence to JNC- 7 Guidelines 1 Krishna Murti, 1 M. Arif Khan, 1 Akalanka Dey,
Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star
 Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star HEALTH ALLIANCE PLAN Presented by Vanita K. Pindolia, Pharm.D. VP, Ambulatory Clinical Pharmacy Programs_PCM Medicare 5-Star Rating
Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star HEALTH ALLIANCE PLAN Presented by Vanita K. Pindolia, Pharm.D. VP, Ambulatory Clinical Pharmacy Programs_PCM Medicare 5-Star Rating
By 2030, the number of seniors in the United States
 Patient Characteristics and Medication Burden Affect Adherence Among Seniors Drug Trends R. Scott Leslie, MPH; Sara C. Erickson, PharmD; and Bimal V. Patel, PharmD, MS By 2030, the number of seniors in
Patient Characteristics and Medication Burden Affect Adherence Among Seniors Drug Trends R. Scott Leslie, MPH; Sara C. Erickson, PharmD; and Bimal V. Patel, PharmD, MS By 2030, the number of seniors in
To Take or Not To Take?
 To Take or Not To Take? Assessment Question How do the terms adherence & compliance differ? 1. The terms are synonymous 2.Adherence assumes collaboration between patient & provider while compliance suggests
To Take or Not To Take? Assessment Question How do the terms adherence & compliance differ? 1. The terms are synonymous 2.Adherence assumes collaboration between patient & provider while compliance suggests
Intervention to improve adherence to Type 2 Diabetes mellitus subjects in rural teaching hospital
 Available online at wwwscholarsresearchlibrarycom Scholars Research Library Der Pharmacia Lettre, 2016, 8 (1):361-367 (http://scholarsresearchlibrarycom/archivehtml) ISSN 0975-5071 USA CODEN: DPLEB4 Intervention
Available online at wwwscholarsresearchlibrarycom Scholars Research Library Der Pharmacia Lettre, 2016, 8 (1):361-367 (http://scholarsresearchlibrarycom/archivehtml) ISSN 0975-5071 USA CODEN: DPLEB4 Intervention
Long-Term Care Updates
 Long-Term Care Updates August 2015 By Darren Hein, PharmD Hypertension is a clinical condition in which the force of blood pushing on the arteries is higher than normal. This increases the risk for heart
Long-Term Care Updates August 2015 By Darren Hein, PharmD Hypertension is a clinical condition in which the force of blood pushing on the arteries is higher than normal. This increases the risk for heart
Study Exposures, Outcomes:
 GSK Medicine: Coreg IR, Coreg CR, and InnoPran Study No.: WWE111944/WEUSRTP3149 Title: A nested case-control study of the association between Coreg IR and Coreg CR and hypersensitivity reactions: anaphylactic
GSK Medicine: Coreg IR, Coreg CR, and InnoPran Study No.: WWE111944/WEUSRTP3149 Title: A nested case-control study of the association between Coreg IR and Coreg CR and hypersensitivity reactions: anaphylactic
Re: Docket No. FDA-2009-N-0294 Regulation of Tobacco Products; Request for Comments
 VIA Electronic Submission to http://www.regulations.gov September 29, 2009 Division of Dockets Management (HFA-305) Food and Drug Administration 5630 Fishers Lane, rm. 1061 Rockville, MD 20852 Re: Docket
VIA Electronic Submission to http://www.regulations.gov September 29, 2009 Division of Dockets Management (HFA-305) Food and Drug Administration 5630 Fishers Lane, rm. 1061 Rockville, MD 20852 Re: Docket
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis.
 COMMUNITY PHARMACY V1.1 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. # NAME DESCRIPTION NUMERATOR DENOMINATOR
COMMUNITY PHARMACY V1.1 MANDATORY S Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. # NAME DESCRIPTION NUMERATOR DENOMINATOR
Medication Therapy Management Solution
 Medication Therapy Management Solution A Medicaid Case Report It s often challenging to include evidencebased clinical programs that offer financial benefits. However, pharmacotherapy is central to the
Medication Therapy Management Solution A Medicaid Case Report It s often challenging to include evidencebased clinical programs that offer financial benefits. However, pharmacotherapy is central to the
Medication Adherence
 Medication Adherence 1-30-15 Presented by: Alexander Luong, Pharm.D. Candidate 2015 University of the Pacific Preceptor: Dr. Craig Stern Pharm.D., MBA President Pro Pharma Pharmaceutical Consultants, Inc
Medication Adherence 1-30-15 Presented by: Alexander Luong, Pharm.D. Candidate 2015 University of the Pacific Preceptor: Dr. Craig Stern Pharm.D., MBA President Pro Pharma Pharmaceutical Consultants, Inc
Patient persistence with antihypertensive drugs in France, Germany and the UK
 Patient persistence with antihypertensive drugs in France, Germany and the UK B. Ehlken (1), K. Kostev (1), A. Sandberg (2), B. Holz (1), A. M. S. Oberdiek (2) (1) IMS Health Frankfurt / Munich, Germany
Patient persistence with antihypertensive drugs in France, Germany and the UK B. Ehlken (1), K. Kostev (1), A. Sandberg (2), B. Holz (1), A. M. S. Oberdiek (2) (1) IMS Health Frankfurt / Munich, Germany
Pharmacy Benefit Management
 Benefit Management Measures At A Glance Updated: 10/8/2015 Page 1 of 7 Benefit Management Mandatory Measures (6) Note: Mandatory measures are those measures that are a requirement of accreditation and
Benefit Management Measures At A Glance Updated: 10/8/2015 Page 1 of 7 Benefit Management Mandatory Measures (6) Note: Mandatory measures are those measures that are a requirement of accreditation and
16 th Annual IHA Stakeholders Meeting Session 2C
 16 th Annual IHA Stakeholders Meeting Session 2C September 19, 2017 Hilton Los Angeles Airport Thank you to our Content Partner: Medication Adherence AppleCare Pharmacy Programs Confidential and proprietary.
16 th Annual IHA Stakeholders Meeting Session 2C September 19, 2017 Hilton Los Angeles Airport Thank you to our Content Partner: Medication Adherence AppleCare Pharmacy Programs Confidential and proprietary.
ENSURING EXCELLENCE IN PRESCRIBING FOR OLDER ADULTS
 ENSURING EXCELLENCE IN PRESCRIBING FOR OLDER ADULTS Philip J. Schneider, MS, FASHP The University of Arizona College of Pharmacy Learning Objectives: Describe the medication-use system and all interdependent
ENSURING EXCELLENCE IN PRESCRIBING FOR OLDER ADULTS Philip J. Schneider, MS, FASHP The University of Arizona College of Pharmacy Learning Objectives: Describe the medication-use system and all interdependent
DISCLOSURE PHARMACIST OBJECTIVES 9/30/2014 JNC 8: A REVIEW OF THE LONG-AWAITED/MUCH-ANTICIPATED HYPERTENSION GUIDELINES. I have nothing to disclose.
 JNC 8: A REVIEW OF THE LONG-AWAITED/MUCH-ANTICIPATED HYPERTENSION GUIDELINES Tiffany Dickey, PharmD Assistant Professor, UAMS COP Clinical Pharmacy Specialist, Mercy Hospital Northwest AR DISCLOSURE I
JNC 8: A REVIEW OF THE LONG-AWAITED/MUCH-ANTICIPATED HYPERTENSION GUIDELINES Tiffany Dickey, PharmD Assistant Professor, UAMS COP Clinical Pharmacy Specialist, Mercy Hospital Northwest AR DISCLOSURE I
A COMPREHENSIVE APPROACH TO MANAGING DIABETES
 A COMPREHENSIVE APPROACH TO MANAGING DIABETES Programs and services to help individuals avoid costly complications and improve outcomes 2 0 1 8 ENTER Supporting each member with targeted guidance and services.
A COMPREHENSIVE APPROACH TO MANAGING DIABETES Programs and services to help individuals avoid costly complications and improve outcomes 2 0 1 8 ENTER Supporting each member with targeted guidance and services.
MEDICATION ADHERENCE: WE DIDN T ASK & THEY DIDN T TELL
 MEDICATION ADHERENCE: WE DIDN T ASK & THEY DIDN T TELL JENNIFER BUSSELL MD FACP INSTITUTE FOR HEALTHCARE IMPROVEMENT 15 TH ANNUAL INTERNATIONAL SUMMIT ON IMPROVING PATIENT CARE IN THE OFFICE PRACTICE AND
MEDICATION ADHERENCE: WE DIDN T ASK & THEY DIDN T TELL JENNIFER BUSSELL MD FACP INSTITUTE FOR HEALTHCARE IMPROVEMENT 15 TH ANNUAL INTERNATIONAL SUMMIT ON IMPROVING PATIENT CARE IN THE OFFICE PRACTICE AND
Prevention of Heart Failure: What s New with Hypertension
 Prevention of Heart Failure: What s New with Hypertension Ali AlMasood Prince Sultan Cardiac Center Riyadh 3ed Saudi Heart Failure conference, Jeddah, 13 December 2014 Background 20-30% of Saudi adults
Prevention of Heart Failure: What s New with Hypertension Ali AlMasood Prince Sultan Cardiac Center Riyadh 3ed Saudi Heart Failure conference, Jeddah, 13 December 2014 Background 20-30% of Saudi adults
Alabama Medicaid Pharmacy Override
 Alabama Medicaid Pharmacy Override Therapeutic Duplication, Early Refill, Maximum Unit, Prescription Limit Switchover, Dispense as Written, Accumulation Edit, Maintenance Supply Opt Out, and Maximum Cost
Alabama Medicaid Pharmacy Override Therapeutic Duplication, Early Refill, Maximum Unit, Prescription Limit Switchover, Dispense as Written, Accumulation Edit, Maintenance Supply Opt Out, and Maximum Cost
CLINICAL. Determinants of Compliance With Statin Therapy and Low-Density Lipoprotein Cholesterol Goal Attainment in a Managed Care Population
 Determinants of Compliance With Statin Therapy and Low-Density Lipoprotein Cholesterol Goal Attainment in a Managed Care Population Jennifer S. Schultz, PhD; John C. O Donnell, PhD; Ken L. McDonough, MD;
Determinants of Compliance With Statin Therapy and Low-Density Lipoprotein Cholesterol Goal Attainment in a Managed Care Population Jennifer S. Schultz, PhD; John C. O Donnell, PhD; Ken L. McDonough, MD;
Objectives. Chronic Disease Management: The Role of a Diabetes Case Manager
 Chronic Disease Management: The Role of a Diabetes Case Manager Palomar Health Diabetes Symposium November 12, 2015 Irma A Moore, MS, RN, CNS, CDE Diabetes Disease Manager Sharp Rees-Stealy Medical Centers
Chronic Disease Management: The Role of a Diabetes Case Manager Palomar Health Diabetes Symposium November 12, 2015 Irma A Moore, MS, RN, CNS, CDE Diabetes Disease Manager Sharp Rees-Stealy Medical Centers
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis.
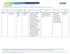 Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DESCRIPTION NUMERATOR DENOMINATOR DM2012-12 Portion of Days Covered
Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual basis. DESCRIPTION NUMERATOR DENOMINATOR DM2012-12 Portion of Days Covered
Hypertension and the Challenge of Adherence. Geneva Clark Briggs, Pharm.D., BCPS
 Hypertension and the Challenge of Adherence Geneva Clark Briggs, Pharm.D., BCPS Outline Brief overview of HTN and pharmacologic therapies Role of pharmacists in collaboration with patients and physicians
Hypertension and the Challenge of Adherence Geneva Clark Briggs, Pharm.D., BCPS Outline Brief overview of HTN and pharmacologic therapies Role of pharmacists in collaboration with patients and physicians
Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE
 Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE ORIGINAL ARTICLE Mohammed Arifulla 1, Lisha Jenny John 1, Jayadevan Sreedharan 2, Jayakumary Muttappallymyalil 3, Jenny
Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE ORIGINAL ARTICLE Mohammed Arifulla 1, Lisha Jenny John 1, Jayadevan Sreedharan 2, Jayakumary Muttappallymyalil 3, Jenny
Efforts to redesign the healthcare system are increasingly focused
 A Blueprint for Pharmacy Benefit Managers to Increase Value William H. Shrank, MD, MSHS; Michael E. Porter, PhD, MBA; Sachin H. Jain, MD, MBA; and Niteesh K. Choudhry, MD, PhD Managed Care & ealthcare
A Blueprint for Pharmacy Benefit Managers to Increase Value William H. Shrank, MD, MSHS; Michael E. Porter, PhD, MBA; Sachin H. Jain, MD, MBA; and Niteesh K. Choudhry, MD, PhD Managed Care & ealthcare
CLINICAL. The Effect of Switching on Compliance and Persistence: The Case of Statin Treatment
 The Effect of Switching on Compliance and Persistence: The Case of Statin Treatment Patrick Thiebaud, PhD; Bimal V. Patel, PharmD; Michael B. Nichol, PhD; and David M. Berenbeim, MD Objective: To determine
The Effect of Switching on Compliance and Persistence: The Case of Statin Treatment Patrick Thiebaud, PhD; Bimal V. Patel, PharmD; Michael B. Nichol, PhD; and David M. Berenbeim, MD Objective: To determine
Statins ARE Enough For The Prevention of CVD! Professor Kausik Ray Imperial College London, UK
 1 Disclosures Advisory boards PCSK9- Sanofi/ Regeneron, Amgen, Pfizer, Roche, MSD NLI/ SC member for Odyssey- (Sanofi/ Regeneron), Roche Investigator initiated research grant support (Sanofi/Regeneron/
1 Disclosures Advisory boards PCSK9- Sanofi/ Regeneron, Amgen, Pfizer, Roche, MSD NLI/ SC member for Odyssey- (Sanofi/ Regeneron), Roche Investigator initiated research grant support (Sanofi/Regeneron/
GSK Medicine: Study Number: Title: Rationale: Study Period: Objectives: Indication: Study Investigators/Centers: Research Methods: Data Source
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Presenter Disclosure Information
 Presenter Disclosure Information Soko Setoguchi, MD DrPH Prescription Drug Data: Advantages, Availability, and Access FINANCIAL DISCLOSURE: Grants/Research Support: NIH, AHRQ UNLABELED/UNAPPROVED USES
Presenter Disclosure Information Soko Setoguchi, MD DrPH Prescription Drug Data: Advantages, Availability, and Access FINANCIAL DISCLOSURE: Grants/Research Support: NIH, AHRQ UNLABELED/UNAPPROVED USES
Blue Shield Participation
 9 th Annual Right Care Initiative Summit Blue Shield Participation Scott Flinn, MD Regional Medical Director Blue Shield of California 1 Care Worthy of our Family and Friends 2 Bottom Line Up Front Blue
9 th Annual Right Care Initiative Summit Blue Shield Participation Scott Flinn, MD Regional Medical Director Blue Shield of California 1 Care Worthy of our Family and Friends 2 Bottom Line Up Front Blue
SPECIAL ISSUE. Medicaid Prescription Drug Access Restrictions: Exploring the Effect on Patient Persistence With Hypertension Medications
 Medicaid Prescription Drug Access Restrictions: Exploring the Effect on Patient Persistence With Hypertension Medications Jerome Wilson, PhD; Kirsten Axelsen, MS; and Simon Tang, MPH Objective: To compare
Medicaid Prescription Drug Access Restrictions: Exploring the Effect on Patient Persistence With Hypertension Medications Jerome Wilson, PhD; Kirsten Axelsen, MS; and Simon Tang, MPH Objective: To compare
Original Research PRACTICE-BASED RESEARCH
 The Effect of a Novel Proactive First Day Prescription Counseling Program on Adherence to Select Cardiovascular Medications Jamie L. McConaha, Pharm.D., CGP and Kevin Lynch, Pharm.D., BCPS, MBA Conflicts
The Effect of a Novel Proactive First Day Prescription Counseling Program on Adherence to Select Cardiovascular Medications Jamie L. McConaha, Pharm.D., CGP and Kevin Lynch, Pharm.D., BCPS, MBA Conflicts
Medicare Star Ratings and the Shift to Quality- Based Payment Models. David Nau, RPh, PhD, FAPhA PQS President
 Medicare Star Ratings and the Shift to Quality- Based Payment Models David Nau, RPh, PhD, FAPhA PQS President The shift to Value-Driven Healthcare The U.S. health care system is rapidly moving to value-based
Medicare Star Ratings and the Shift to Quality- Based Payment Models David Nau, RPh, PhD, FAPhA PQS President The shift to Value-Driven Healthcare The U.S. health care system is rapidly moving to value-based
Assessing Medication Adherence
 Assessing Medication Adherence Dr. Lauren Hanna and Dr. Delbert Robinson Northwell Health National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental
Assessing Medication Adherence Dr. Lauren Hanna and Dr. Delbert Robinson Northwell Health National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental
PATIENT-IMPACT SCORECARD
 UNDERSTANDING THE GSC PATIENT-IMPACT SCORECARD What is the GSC Patient-Impact Scorecard? The GSC Patient-Impact Scorecard shows pharmacy performance scores for GSC patients during the period indicated.
UNDERSTANDING THE GSC PATIENT-IMPACT SCORECARD What is the GSC Patient-Impact Scorecard? The GSC Patient-Impact Scorecard shows pharmacy performance scores for GSC patients during the period indicated.
Healthcare Implications of Achieving JNC 7 Blood Pressure Goals in Clinical Practice
 CONTINUING EDUCATION Healthcare Implications of Achieving JNC 7 Blood Pressure Goals in Clinical Practice GOAL To provide participants with current information about current blood pressure goals and effective
CONTINUING EDUCATION Healthcare Implications of Achieving JNC 7 Blood Pressure Goals in Clinical Practice GOAL To provide participants with current information about current blood pressure goals and effective
Antihypertensive Trial Design ALLHAT
 1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
Approximately 73.6 million adults in the United States have
 n clinical n Hypertension Treatment and Control Within an Independent Nurse Practitioner Setting Wendy L. Wright, MS; Joan E. Romboli, MSN; Margaret A. DiTulio, MS, MBA; Jenifer Wogen, MS; and Daniel A.
n clinical n Hypertension Treatment and Control Within an Independent Nurse Practitioner Setting Wendy L. Wright, MS; Joan E. Romboli, MSN; Margaret A. DiTulio, MS, MBA; Jenifer Wogen, MS; and Daniel A.
Understanding and Addressing Problematic Medication Adherence
 Understanding and Addressing Problematic Medication Adherence William H. Polonsky PhD, CDE November 10, 2017 whp@behavioraldiabetes.org RATES OF VERY POOR GLYCEMIC CONTROL HEDIS data from >1000 health
Understanding and Addressing Problematic Medication Adherence William H. Polonsky PhD, CDE November 10, 2017 whp@behavioraldiabetes.org RATES OF VERY POOR GLYCEMIC CONTROL HEDIS data from >1000 health
Concordance of Pharmacist Assessment of Medication Nonadherence With a Self-Report Medication Adherence Scale
 Chapman University Chapman University Digital Commons Pharmacy Faculty Articles and Research School of Pharmacy 10-13-2014 Concordance of Pharmacist Assessment of Medication Nonadherence With a Self-Report
Chapman University Chapman University Digital Commons Pharmacy Faculty Articles and Research School of Pharmacy 10-13-2014 Concordance of Pharmacist Assessment of Medication Nonadherence With a Self-Report
Measure Up/Pressure Down Medical Group Success
 Measure Up/Pressure Down Medical Group Success Deborah A. Molina, MPA, MBA Manager, Quality Jamie L. Reedy, MD, MPH Medical Director, Population Health Laura Balsamini, Pharm D, BCPS Director, Pharmacy
Measure Up/Pressure Down Medical Group Success Deborah A. Molina, MPA, MBA Manager, Quality Jamie L. Reedy, MD, MPH Medical Director, Population Health Laura Balsamini, Pharm D, BCPS Director, Pharmacy
Statement Of. The National Association of Chain Drug Stores. For. U.S. Senate Finance Committee. Hearing on:
 Statement Of The National Association of Chain Drug Stores For U.S. Senate Finance Committee Hearing on: 10:30 a.m. 215 Dirksen Senate Office Building National Association of Chain Drug Stores (NACDS)
Statement Of The National Association of Chain Drug Stores For U.S. Senate Finance Committee Hearing on: 10:30 a.m. 215 Dirksen Senate Office Building National Association of Chain Drug Stores (NACDS)
3/6/2017. Grassroots Strategies for Improving Adherence. Learning Objectives
 Grassroots Strategies for Improving Adherence Amy Knight, PhD Director of Rehabilitation Psychology Department of Physical Medicine & Rehabilitation University of Alabama Birmingham Nothing to Disclose
Grassroots Strategies for Improving Adherence Amy Knight, PhD Director of Rehabilitation Psychology Department of Physical Medicine & Rehabilitation University of Alabama Birmingham Nothing to Disclose
JNC Evidence-Based Guidelines for the Management of High Blood Pressure in Adults
 JNC 8 2014 Evidence-Based Guidelines for the Management of High Blood Pressure in Adults Table of Contents Why Do We Treat Hypertension? Blood Pressure Treatment Goals Initial Therapy Strength of Recommendation
JNC 8 2014 Evidence-Based Guidelines for the Management of High Blood Pressure in Adults Table of Contents Why Do We Treat Hypertension? Blood Pressure Treatment Goals Initial Therapy Strength of Recommendation
Apurba Chakraborty MBBS, MPH Dima M. Qato PharmD, MPH, PhD Professor Mark S. Dworkin MD, MPHTM The University of Illinois at Chicago
 Less is More: The Impact of Lower Pill Burden on Adherence to Antiretroviral Therapy among Treatment-Naive Patients with HIV Infection in the United States Apurba Chakraborty MBBS, MPH Dima M. Qato PharmD,
Less is More: The Impact of Lower Pill Burden on Adherence to Antiretroviral Therapy among Treatment-Naive Patients with HIV Infection in the United States Apurba Chakraborty MBBS, MPH Dima M. Qato PharmD,
Quit rates among smokers who received pharmacist-provided pharmacotherapy and quitline services versus those who received only quitline services.
 Quit rates among smokers who received pharmacist-provided pharmacotherapy and quitline services versus those who received only quitline services. Jill Augustine, PharmD, MPH 1 ; Ryan Seltzer, PhD 2 ; Martin
Quit rates among smokers who received pharmacist-provided pharmacotherapy and quitline services versus those who received only quitline services. Jill Augustine, PharmD, MPH 1 ; Ryan Seltzer, PhD 2 ; Martin
Non-Adherence: How to Improve the Therapeutic Relationship with Difficult Patients
 Non-Adherence: How to Improve the Therapeutic Relationship with Difficult Patients Bradford Strijack MD MHSc FRCPC Clinical Assistant Professor University of British Columbia October 7, 2016 None Disclosures
Non-Adherence: How to Improve the Therapeutic Relationship with Difficult Patients Bradford Strijack MD MHSc FRCPC Clinical Assistant Professor University of British Columbia October 7, 2016 None Disclosures
Improving Medical Statistics and Interpretation of Clinical Trials
 Improving Medical Statistics and Interpretation of Clinical Trials 1 ALLHAT Trial & ALLHAT Meta-Analysis Critique Table of Contents ALLHAT Trial Critique- Overview p 2-4 Critique Of The Flawed Meta-Analysis
Improving Medical Statistics and Interpretation of Clinical Trials 1 ALLHAT Trial & ALLHAT Meta-Analysis Critique Table of Contents ALLHAT Trial Critique- Overview p 2-4 Critique Of The Flawed Meta-Analysis
Walgreens (WAG) Analyst: Juan Fabres Fall 2014
 Recommendation: Buy Target Price August 31, 2016: $77.57 1. Reasons for the Recommendation With the acquisition of Alliance Boots in Europe, Walgreens will be the first US pharmacy to operate retail stores
Recommendation: Buy Target Price August 31, 2016: $77.57 1. Reasons for the Recommendation With the acquisition of Alliance Boots in Europe, Walgreens will be the first US pharmacy to operate retail stores
Mail Service Pharmacy
 Mail Service s At A Glance Disclaimer: reserves the right to update its measures and measure sets to maintain measure relevancy and to remedy any unintended consequences that may arise during implementation.
Mail Service s At A Glance Disclaimer: reserves the right to update its measures and measure sets to maintain measure relevancy and to remedy any unintended consequences that may arise during implementation.
How Low Do We Go? Update on Hypertension
 How Low Do We Go? Update on Beth L. Abramson, MD, FRCPC, FACC As presented at the University of Toronto s Saturday at the University Session (September 2003) Arecent World Health Organization report states
How Low Do We Go? Update on Beth L. Abramson, MD, FRCPC, FACC As presented at the University of Toronto s Saturday at the University Session (September 2003) Arecent World Health Organization report states
The problem of uncontrolled hypertension
 (2002) 16, S3 S8 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh The problem of uncontrolled hypertension Department of Public Health and Clinical Medicine, Norrlands
(2002) 16, S3 S8 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh The problem of uncontrolled hypertension Department of Public Health and Clinical Medicine, Norrlands
Pharmacy Partnership to Improve Patient Outcomes
 Pharmacy Partnership to Improve Patient Outcomes Minnesota Rural Health Conference Session 2B Ryan M. Harden, MD MS Kendra Metz, Pharm D Sarah Nelson, MD June 25, 2018 Involved Partners Involved Partners
Pharmacy Partnership to Improve Patient Outcomes Minnesota Rural Health Conference Session 2B Ryan M. Harden, MD MS Kendra Metz, Pharm D Sarah Nelson, MD June 25, 2018 Involved Partners Involved Partners
Persistence With Lipid-Lowering Therapy: Influence of the Type of Lipid-Lowering Agent and Drug Benefit Plan Option in Elderly Patients
 ORIGINAL RESEARCH Persistence With Lipid-Lowering Therapy: Influence of the Type of Lipid-Lowering Agent and Drug Benefit Plan Option in Elderly Patients SUSAN M. ABUGHOSH, PhD; STEPHEN J. KOGUT, RPh,
ORIGINAL RESEARCH Persistence With Lipid-Lowering Therapy: Influence of the Type of Lipid-Lowering Agent and Drug Benefit Plan Option in Elderly Patients SUSAN M. ABUGHOSH, PhD; STEPHEN J. KOGUT, RPh,
Medication Therapy Management: Improving Health and Saving Money
 Medication Therapy Management: Improving Health and Saving Money Ed Staffa, RPh Vice President, Pharmacy Mirixa Corporation estaffa@mirixa.com July 23, 2008 MTM At A Glance The U.S. health care system
Medication Therapy Management: Improving Health and Saving Money Ed Staffa, RPh Vice President, Pharmacy Mirixa Corporation estaffa@mirixa.com July 23, 2008 MTM At A Glance The U.S. health care system
Team-Based Decision Support in Diabetes Outcomes and Costs
 Team-Based Decision Support in Diabetes Outcomes and Costs Session 89, 8:30 a.m. February 13, 2019 Gary Ozanich, Ph.D. - College of Informatics, Northern Kentucky University 1 Conflict of Interest Gary
Team-Based Decision Support in Diabetes Outcomes and Costs Session 89, 8:30 a.m. February 13, 2019 Gary Ozanich, Ph.D. - College of Informatics, Northern Kentucky University 1 Conflict of Interest Gary
Hypertension Update 2014:
 GSHTP Webinar Hypertension Update 2014: The Kaiser Permanente Northern California Experience Presented by: Marc Jaffe, MD Associate Clinical Professor of Medicine, UCSF Kaiser Permanente Northern California
GSHTP Webinar Hypertension Update 2014: The Kaiser Permanente Northern California Experience Presented by: Marc Jaffe, MD Associate Clinical Professor of Medicine, UCSF Kaiser Permanente Northern California
CONVERSATION STARTERS: ENGAGING YOUR PATIENTS AT PICK UP JULY 12, :00 2:30 PM
 CONVERSATION STARTERS: ENGAGING YOUR PATIENTS AT PICK UP JULY 12, 2017 1:00 2:30 PM ACPE UAN: 0107-9999-17-097-L04-P 0.15 CEU/1.5 hr Activity Type: Knowledge-Based Learning Objectives for Pharmacists:
CONVERSATION STARTERS: ENGAGING YOUR PATIENTS AT PICK UP JULY 12, 2017 1:00 2:30 PM ACPE UAN: 0107-9999-17-097-L04-P 0.15 CEU/1.5 hr Activity Type: Knowledge-Based Learning Objectives for Pharmacists:
Understanding Your Patient Care Opportunity Report (PCOR)
 Understanding Your Patient Care Opportunity Report (PCOR) Use your January/February 208 PCOR to help improve performance on Medicare Part D Clinical Star Ratings measures. Your January/February 208 Patient
Understanding Your Patient Care Opportunity Report (PCOR) Use your January/February 208 PCOR to help improve performance on Medicare Part D Clinical Star Ratings measures. Your January/February 208 Patient
RESEARCH. Katrina Wilcox Hagberg, 1 Hozefa A Divan, 2 Rebecca Persson, 1 J Curtis Nickel, 3 Susan S Jick 1. open access
 open access Risk of erectile dysfunction associated with use of 5-α reductase inhibitors for benign prostatic hyperplasia or alopecia: population based studies using the Clinical Practice Research Datalink
open access Risk of erectile dysfunction associated with use of 5-α reductase inhibitors for benign prostatic hyperplasia or alopecia: population based studies using the Clinical Practice Research Datalink
International Journal of Advancements in Research & Technology, Volume 2, Issue 6, June-2013 ISSN
 ISSN 2278-7763 295 Study of Prescriptive Patterns of Antihypertensive Drugs in South India Popuri Rupa Sindhu, Malladi Srinivas Reddy St. Peters Institute of Pharmaceutical Sciences, Hanamkonda, Warangal-506001,
ISSN 2278-7763 295 Study of Prescriptive Patterns of Antihypertensive Drugs in South India Popuri Rupa Sindhu, Malladi Srinivas Reddy St. Peters Institute of Pharmaceutical Sciences, Hanamkonda, Warangal-506001,
Medication nonadherence is a major public health
 RESEARCH Hiraku Kumamaru, MD, ScD; Moa P. Lee, PharmD, MPH; Niteesh K. Choudhry, MD, PhD; Yaa-Hui Dong, PhD; Alexis A. Krumme, MS, ScD; Nazleen Khan, BS, ScM; Gregory Brill, MS; Shun Kohsaka, MD, PhD;
RESEARCH Hiraku Kumamaru, MD, ScD; Moa P. Lee, PharmD, MPH; Niteesh K. Choudhry, MD, PhD; Yaa-Hui Dong, PhD; Alexis A. Krumme, MS, ScD; Nazleen Khan, BS, ScM; Gregory Brill, MS; Shun Kohsaka, MD, PhD;
Schizophrenia, a devastating chronic. Treatment Adherence Associated With Conventional and Atypical Antipsychotics in a Large State Medicaid Program
 Treatment Adherence Associated With Conventional and Atypical Antipsychotics in a Large State Medicaid Program Joseph Menzin, Ph.D. Luke Boulanger, M.A. Mark Friedman, M.D. Joan Mackell, Ph.D. John R.
Treatment Adherence Associated With Conventional and Atypical Antipsychotics in a Large State Medicaid Program Joseph Menzin, Ph.D. Luke Boulanger, M.A. Mark Friedman, M.D. Joan Mackell, Ph.D. John R.
By Alexis A. Krumme, Robert J. Glynn, Sebastian Schneeweiss, Joshua J. Gagne, J. Samantha Dougherty, Gregory Brill, and Niteesh K.
 By Alexis A. Krumme, Robert J. Glynn, Sebastian Schneeweiss, Joshua J. Gagne, J. Samantha Dougherty, Gregory Brill, and Niteesh K. Choudhry Medication Synchronization Programs Improve Adherence To Cardiovascular
By Alexis A. Krumme, Robert J. Glynn, Sebastian Schneeweiss, Joshua J. Gagne, J. Samantha Dougherty, Gregory Brill, and Niteesh K. Choudhry Medication Synchronization Programs Improve Adherence To Cardiovascular
Bob Davis, PharmD, FAPhA Professor and Chair, KPIC South Carolina Primary Health Care Association September 19, 2015
 Bob Davis, PharmD, FAPhA Professor and Chair, KPIC davisb@kennedycenter.sc.edu South Carolina Primary Health Care Association September 19, 2015 Myrtle Beach, SC Kennedy Pharmacy Innovation Center Foundation
Bob Davis, PharmD, FAPhA Professor and Chair, KPIC davisb@kennedycenter.sc.edu South Carolina Primary Health Care Association September 19, 2015 Myrtle Beach, SC Kennedy Pharmacy Innovation Center Foundation
Value of Hospice Benefit to Medicaid Programs
 One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
2015 Healthy Heart. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2015 Healthy Heart Program Evaluation Our mission is to improve the health and quality of life of our members 2015 Healthy Heart Program Evaluation Program Title: Healthy Heart Program Evaluation Period:
2015 Healthy Heart Program Evaluation Our mission is to improve the health and quality of life of our members 2015 Healthy Heart Program Evaluation Program Title: Healthy Heart Program Evaluation Period:
PCMH 2018 Enrollment and Update August 25, 2017
 PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
Role of Pharmacoepidemiology in Drug Evaluation
 Role of Pharmacoepidemiology in Drug Evaluation Martin Wong MD, MPH School of Public Health and Primary Care Faculty of Medicine Chinese University of Hog Kong Outline of Content Introduction: what is
Role of Pharmacoepidemiology in Drug Evaluation Martin Wong MD, MPH School of Public Health and Primary Care Faculty of Medicine Chinese University of Hog Kong Outline of Content Introduction: what is
ANALYSIS OF KENTUCKY MEDICAID MANAGED CARE VERSUS FEE-FOR- SERVICE SYSTEMS: MEDICATION ADHERENCE IN PATIENTS WITH PREVALENT CHRONIC DISEASES
 University of Kentucky UKnowledge Theses and Dissertations--Pharmacy College of Pharmacy 2016 ANALYSIS OF KENTUCKY MEDICAID MANAGED CARE VERSUS FEE-FOR- SERVICE SYSTEMS: MEDICATION ADHERENCE IN PATIENTS
University of Kentucky UKnowledge Theses and Dissertations--Pharmacy College of Pharmacy 2016 ANALYSIS OF KENTUCKY MEDICAID MANAGED CARE VERSUS FEE-FOR- SERVICE SYSTEMS: MEDICATION ADHERENCE IN PATIENTS
Comprehensive support for your patients on MYALEPT
 Comprehensive support for your patients on MYALEPT Insurance and financial assistance options (see page 3) Fulfillment support (see page 6) Co-pay assistance a,b (see page 4) Your patient Injection training
Comprehensive support for your patients on MYALEPT Insurance and financial assistance options (see page 3) Fulfillment support (see page 6) Co-pay assistance a,b (see page 4) Your patient Injection training
PDE File Medication Utilization; Medication Possession Ratio. Kyoungrae Jung, Ph.D. Assistant Professor Penn State University
 PDE File Medication Utilization; Medication Possession Ratio Kyoungrae Jung, Ph.D. Assistant Professor Penn State University Outline PDE variables related to medication utilization Measures of medication
PDE File Medication Utilization; Medication Possession Ratio Kyoungrae Jung, Ph.D. Assistant Professor Penn State University Outline PDE variables related to medication utilization Measures of medication
An estimated 23.6 million people in the United States,
 Impact of Treatment Complexity on Adherence and Glycemic Control: An Analysis of Oral Antidiabetic Agents Michael Pollack, MS, Benjamin Chastek, MS, Setareh A. Williams, PhD, and Jane Moran, MD Abstract
Impact of Treatment Complexity on Adherence and Glycemic Control: An Analysis of Oral Antidiabetic Agents Michael Pollack, MS, Benjamin Chastek, MS, Setareh A. Williams, PhD, and Jane Moran, MD Abstract
2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT
 2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT December 2017 Table of Contents Executive Summary... 1 Pharmacy Benefit Management Organization Characteristics...
2017 URAC PHARMACY BENEFIT MANAGEMENT PERFORMANCE MEASUREMENT: AGGREGATE SUMMARY PERFORMANCE REPORT December 2017 Table of Contents Executive Summary... 1 Pharmacy Benefit Management Organization Characteristics...
