OPEN ACCESS TEXTBOOK OF GENERAL SURGERY
|
|
|
- Mabel Patterson
- 5 years ago
- Views:
Transcription
1 OPEN ACCESS TEXTBOOK OF GENERAL SURGERY ACUTE AND CHRONIC PANCREATITIS S Burmeister PC Bornman JEJ Krige ANATOMY AND PHYSIOLOGY OF THE PANCREAS The pancreas lies in the epigastrium and left hypochondrium, crossing the midline at the level of L1 to L3. It is an elongated organ lying in the retroperitoneum, posterior to the stomach and anterior, from right to left, to the inferior Vena Cava; superior mesenteric, portal and splenic veins; the vertebral column; the aorta and splenic artery and the left kidney. It is comprised of a head, neck, body and tail with the head lying in the C-loop of the duodenum and the tail lying within the hilum of the spleen. A small prolongation, the uncinate process, extends from the head medially, posterior to the superior mesenteric vein. The neck is that part of the pancreas overlying the superior mesenteric and portal veins as they course towards the liver. The common bile duct lies in a groove on the postero-superior surface of pancreatic head, sometimes being embedded within it. Typically the pancreas is drained by 2 ducts, the main and accessory ducts. The main duct runs through the entire gland receiving tributaries from it and exits into the duodenum via the ampulla of Vater where it is in close relationship with the common bile duct. The accessory duct drains the head and has a separate opening into the duodenum. The pancreas has both an exocrine and endocrine function. Digestive enzymes are secreted by acinar cells into the pancreatic ducts which then drain into the intestinal lumen to facilitate digestion and absorption. Pancreatic juice is alkaline and has a high HCO3 content; this together with bile and intestinal juice which are also neutral or alkaline neutralise gastric acid. Approximately 1500 ml of pancreatic juice is produced per day, under the influence of secretin and cholecystokinin. Pancreatic juice contains trypsinogen which is converted to trypsin by the brush border enzyme enterokinase when pancreatic juice enters the duodenum. Trypsin converts proenzymes in pancreatic juice into active enzymes as well as further trypsinogen into trypsin in an autocatalytic chain reaction. Thus the release into the pancreas of even a small amount of trypsin results in a chain reaction that produces active enzymes that can digest the pancreas. Trypsin also activates phospholipase A2 which forms lysolecithin from lecithin, a normal constituent of bile. Lysolecithin damages cell membranes causing disruption of pancreatic tissue and necrosis of surrounding fat. Various hormones are produced and secreted by the islets of Langerhans in the pancreas, including insulin, glucagon, somatostatin, pancreatic polypeptide and others. The first 2 are particularly important in glucose metabolism and homeostasis. Insulin is anabolic, increasing the storage of glucose, fatty acids and amino acids; deficiency results in the development of diabetes mellitus. Glucagon mobilises glucose, fatty acids and amino acids into the bloodstream. The 2 hormones are thus reciprocal in action and reciprocally secreted. Somatostatin regulates islet cell secretion while pancreatic polypeptide regulates GI function.
2 o o o o o Drugs Anti-tuberculous Anti-biotics Anti-retrovirals Thiazide diuretics Trauma Blunt Post operative Viral infections (mumps / HIV) pregnancy (mostly associated with gallstones) Collagen disease ACUTE PANCREATITIS DEFINITION Acute pancreatitis (AP) is an acute inflammatory process of the pancreas with variable involvement of other regional tissues or remote organ systems. PATHOLOGY (INCLUDING AETIOLOGY) AND PATHOPHYSIOLOGY Alcohol and gallstones make up about 70% of the causes of AP. Of these alcohol is the predominant cause in the Western Cape while the reverse is true for other countries such as the United Kingdom. Alcohol Gallstones Idiopathic 10% Table 1 Aetiology of Pancreatitis Miscellaneous 20% o o Metabolic 70% Obstructive Post ERCP Ascariasis (children) Pancreatic Carcinoma Congenital abnormalities choledochal cyst pancreas divisum hyperparathyroidism hyperlipidaemia Aminoaciduria Porphyria The pathogenesis of AP is caused by an inappropriate activation of trypsinogen to trypsin in the pancreatic cells (normally this only occurs when trypsinogen is secreted into the duodenum).once activated these enzymes are responsible for autodigestion of pancreatic tissues which result in necrosis and in severe cases stimulate the production of inflammatory cytokines which in turn triggers an inflammatory cascade causing a systemic inflammatory response syndrome (SIRS). SIRS may develop into an acute respiratory stress syndrome (ARDS), multi-organ dysfunction syndrome (MODS) or organ failure. The mechanism by which trypsin is activated in the pancreatic acini remains uncertain. Although it is known that in gallstone pancreatitis the trigger results from a gallbladder stone passing into the bile duct causing temporary obstruction at the sphincter of Oddi, it remains uncertain whether activation of pancreatic enzymes is the result of increased pancreatic duct pressure or due to bile reflux into the pancreatic duct. The mechanisms in alcohol induced and other causes of pancreatitis are even less clear but, in principle, intracellular protective mechanisms to prevent trypsinogen activation or reduce trypsin activity are overwhelmed. Genetic predisposition, such as mutation of the cationic
3 trypsinogen gene may promote AP in the presence of alcohol. Two distinct pathological entities are recognised: 1. Acute interstitial oedematous pancreatitis (IOP) where there is diffuse or localised enlargement of the pancreas due to interstitial oedema together with peripancreatic inflammation and fluid. This type usually presents with a mild attack. 2. Acute necrotising pancreatitis (NP) where there is necrosis of the parenchyma, peripancreatic tissue or both. This type represents the more severe form of the disease. The natural history of the necrotic tissue is variable, as it may remain solid or liquefy, remain sterile or become infected and persist or disappear over time. An attack of pancreatitis may become complicated as a result of the development of either local or systemic complications. Local complications include the development of: A. Collections 1. An acute peripancreatic fluid collection (associated with IOP) o Defined as peripancreatic fluid associated with IOP without necrosis and < 4 weeks after the onset of IOP, without a defined wall. Tend to resolve spontaneously unless there is persistent pancreatic duct disruption. 2. A pancreatic pseudocyst (IOP) o Encapsulated collection of fluid with a well-defined inflammatory wall, outside the pancreas with little or no necrosis. Usually >4 weeks from the onset of IOP and associated with duct disruption. 3. An acute necrotic collection (associated with NP) o Collection containing fluid and necrotic tissue, associated with NP involving the pancreas or peri-pancreatic tissue. There is no definable encapsulating wall. Peripancreatic necrosis may extend into the mesentery of small and large bowel, retroperitoneal space, peri-renal tissues and as far as the pelvis or thorax. With time the necrotic process become liquefied and walled off, the so-called walled-off necrosis. 4. Walled off necrosis (NP) o Encapsulated collection of pancreatic / peripancreatic necrosis encapsulated by a well-defined inflammatory wall. Usually occurs >4 weeks after onset after NP. Pancreatic or peripancreatic fluid collections or necrosis may be sterile or infected, however the development of the latter is particularly important as it is associated with increased morbidity and mortality and invariably requires intervention. B. Other organ complications o Gastric outlet dysfunction o Splenic / portal vein thrombosis o Intestinal necrosis Systemic complications relate to either the development of new organ failure or exacerbation of pre-existing co-morbid disease.
4 CLINICAL PRESENTATION AND COURSE (SYMPTOMS, SIGNS, GRADING) The diagnosis of pancreatitis requires 2 of the following: 1. Abdominal pain consistent with acute pancreatitis (acute onset, epigastric, severe, often radiating to the back). 2. Serum lipase or amylase 3x normal 3. Characteristic findings on CT or MRI scan Nausea and vomiting are common. There is also a subgroup of patients where the onset is insidious, presenting with cardio-respiratory failure and non-specific abdominal signs such as unexplained ileus. This is seen after major surgery (eg, cardiac) or in immune compromised patients. Physical examination varies according to the severity of the attack; in mild cases there will be minimal signs while in severe cases, marked abdominal tenderness, distension and an ileus may be present. Ecchymosis in the flanks (Grey Turner s sign) or in the peri-umbilical region (Cullen s sign) occur in about 3% of patients and are considered signs of severe disease. It is important to identify the underlying cause of acute pancreatitis during the patient s acute admission. With alcohol induced pancreatitis, a history of heavy alcohol intake of 5-10 years is usually obtained. The attack comes on typically the "afternoon after the night before". Gallstones or carcinoma of the pancreas should be considered in the middle aged or elderly patient, particularly when there is little or no alcohol history. With gallstones, the attack typically comes on after a large meal which stimulates gallbladder contraction (by the release of cholecystokinin). This causes migration of gallstone into the bile duct with temporary obstruction at the Ampulla of Vater. Trauma must always be kept in mind in the alcoholic group as the history is often unreliable in these patients. In young patients and children conditions such as ascariasis or more rarely congenital abnormalities should be considered. Acute pancreatitis is a dynamic disease process which has 2 distinct phases with corresponding peaks in mortality. The early phase lasts 1-2 weeks and is characterised by the host s response to pancreatic injury. Inflammatory cascades are activated which manifest clinically as the systemic inflammatory response syndrome (SIRS). SIRS is defined by the presence of 2 or more of the following criteria: Heart rate > 90 beats per minute Core temperature <36 C or >38 C White blood cell count < 4000 or >12000/mm³ Respirations >20/min or PCO2 <32mmHg When SIRS is persistent there is an increased risk of developing organ failure, which may be transient or persistent depending on whether it lasts less than or longer than 48 hours. The presence and duration of organ failure determines the severity of acute pancreatitis during the early phase. The organ failure is secondary to the host s systemic inflammatory response caused by tissue injury/cytokine response. Hypovolaemic shock due to third space fluid sequestration (not bleeding), and ARDS are most commonly seen early on followed by renal failure and DIC. Renal failure is caused by a combination of factors which include shock and the development of an abdominal compartmental syndrome.
5 Organ system Respirator y (PaO2/ FiO2) Renal (creatinine umol/l) CVS (systolic BP) Organ failure is defined by the modified Marshall scoring system for organ dysfunction. Score > >90 <90, response to fluid <90, no response to fluid <90, ph < >43 9 <90, ph <7.2 Organ failure is defined as a score of 2 or more for 1 of the organ systems. If organ failure affects more than 1 organ, it is termed multiple organ failure. The late phase of pancreatitis is characterised by the persistence of systemic signs of inflammation or the presence of local complications which evolve during the late phase. Persistent organ failure is the result of the necrotising process and secondary infections. The morphological characteristics of local complications are assessed by radiological imaging, typically CT scan. The onset of acute pancreatitis is defined as the time of onset of abdominal pain. Once the diagnosis of pancreatitis has been made and an estimation made as to the time of onset, it is important to grade the severity of the attack in order to identify those who require transfer to specialist care and aggressive early treatment. Three degrees of severity are defined: 1. Mild acute pancreatitis - MAP (80% of patients) a. No organ failure b. No local or systemic complications 2. Moderately severe acute pancreatitis - MSAP a. Transient organ failure that resolves within 48 hours b. Local / systemic complications without persistent organ failure 3. Severe acute pancreatitis - SAP a. Persistent single / multiple organ failure lasting >48 hours The more severe forms of pancreatitis, in particular when associated with persistent organ failure, are associated with higher mortality rates. The addition of sepsis increases these rates further. MANAGEMENT INCLUDING INVESTIGATION AND TREATMENT Special investigations 1. Serum Amylase & Lipase: Although not specific for pancreatitis, levels of more than three times normal, is usually diagnostic. High levels can also be found in conditions such as perforated peptic ulcer and small bowel infarction but seldom reach 2-3 times the normal value. The serum amylase levels reduce or normalise within the first hours. Amylase levels may be normal in severe pancreatitis and are unreliable in patients with acute on chronic pancreatitis when there is impaired pancreatic function. Raised urine amylase levels remain high for longer periods. Serum lipase levels have a slightly higher sensitivity and specificity than amylase. Newer tests, such as urine trypsinogen activation peptide (TAP) are more specific but this is currently not widely available. 2. Blood investigations to identify other aetological causes include serum calcium and a lipid profile. Blood gases and a full biochemistry are required in patients with suspected severe pancreatitis. 3. Chest and abdominal x-rays are useful to exclude other conditions
6 but the findings in pancreatitis are often non specific. Pleural effusion, typically on the L-side, and ileus with the so-called sentinel loop and/or colon cut off sign, may be seen. Pancreatic calcifications may also point to a diagnosis of acute on chronic pancreatitis. 4. Ultrasound is currently the most useful non-invasive tests to detect gallstones, while a CT scan can differentiate severe pancreatitis from other emergency abdominal conditions and monitor the development/progression of local complications. 5. ERCP is contra-indicated in the acute setting unless used as a therapeutic procedure in patients with gallstone pancreatitis associated with jaundice and cholangitis. General Treatment In mild pancreatitis hospitalisation with supportive measures such as bed rest, nil per mouth, intravenous fluids and analgesics usually suffice. Not all patients require nasogastric suction which is only indicated when pain is severe or in the presence of an ileus. Before discharge, it is important to identify the aetiological factor. In case of alcohol, the patient needs to understand that only complete abstinence will prevent recurrent attacks. An ultrasound will usually identify gallstones. Hypertriglyceridemia and very rarely hypercalcaemia need to be excluded as these require urgent correction. Gallstone pancreatitis is best treated by initial conservative treatment as the majority of patients will settle spontaneously with the passage of the offending calculus into the bowel. Elective cholecystectomy 1-4 weeks after the acute attack is strongly recommended to pre-empt a possible second attack. Earlier intervention is sometimes required in the small group of patients with progressive jaundice with or without associated cholangitis. In this situation an ERCP/ papillotomy is indicated. In elderly patients and those with co-morbid diseases, a papillotomy will suffice to prevent recurrent attacks of pancreatitis. Early recognition of the severe forms of pancreatitis is important and supportive therapy should be commenced without delay, preferably in a high care unit. Early and easily recognised parameters indicating the development of severe pancreatitis are: 1. Haemodynamic instability. 2. Hypoxic confusion. 3. Pleural effusion and pulmonary infiltrates on chest X rays. 4. SIRS response (2 or more criteria). The management of SAP is complex and requires ICU management. Hypovolaemic shock must be treated vigorously with volume replacement. Inotrope support is often required. The early recognition and appropriate management of respiratory failure is of great importance and many patients will require ventilation. Other metabolic parameters requiring close observation and treatment are; hyperglycaemia, hypocalcaemia and renal failure. Prophylactic antibiotic therapy in the setting of sterile necrosis has been controversial however there remains scant evidence that it reduces the risk of pancreatic sepsis or mortality. There are as yet no drugs available which are effective in stopping the progression of SAP, nor reducing the mortality. Patient nutrition must not be neglected, with preference given to the enteral route if possible. This can be given via a nasogastric tube however if gastroparesis or outlet obstruction is present a nasojejunal tube may be necessary. There is no place for surgery during the early phases of severe pancreatitis, unless there is ischaemic
7 large bowel necrosis which occurs rarely during this phase. Numerous prognostic factors and scoring systems have been devised for severe pancreatitis. These include CRP, Ranson s and Imrie criteria, APACHE II and Marshall scoring systems, the latter two being used mainly in the ICU setting. From a practical point of view obesity (BMI>30), age over 60 years and multiple organ failure are more commonly associated with a poor prognosis. Treatment of local complications The diagnosis and characterisation of acute peri-pancreatic fluid collections and necrosis has been simplified by modern imaging including ultra-sound, endoscopic ultrasound, CT scanning and MRI/MRCP. Interventional procedures (percutaneous radiological, endoscopic or surgical), in particular drainage of symptomatic collections or infected necrosis, may be required for local complications. Such interventions are typically only required after two weeks of the onset of severe pancreatitis. As a general rule, interventions are reserved for patients where there is persistent organ failure particularly in the presence of sepsis. But the therapeutic effects of interventions are often limited by, unliquefied necrosis and as such requires repeated procedures. The tendency today is to follow a step up approach and start with percutaneous drainage and to follow this up with minimal access percutaneous necrosectomy using a variety of scope instruments. Surgical necrosectomy is now reserved for cases where minimal access procedures fail. Well circumscribed and encapsulated pure pancreatic fluid collections (pseudocysts) are easier to manage and intervention should be considered when these persist after 4-6 weeks, particularly when they are large and symptomatic. Other indications include obstruction (bowel or biliary) and secondary infection. Depending on the location and cyst content, these may be drained: percutaneously (generally not favoured) endoscopically o using endoscopic ultrasound, stents are placed between the stomach/duodenum to allow drainage surgery o at laparotomy, a communication is created between the cyst and enteral lumen (cystgastrostomy, cystduodenostomy, cystjejunostomy) Bleeding from a false aneurysm associated with pancreatic fluid collections is managed mostly by selective angiographic embolisation. CHRONIC PANCREATITIS DEFINITION Chronic pancreatitis (CP) is defined as a continuing inflammatory disease of the pancreas characterized by irreversible morphologic changes, often associated with pain and with the loss of exocrine and/or endocrine function which may be clinically relevant. The disease involves both the parenchyma and the ductal system of the pancreas. PATHOLOGY (INCLUDING AETIOLOGY) AND PATHOPHYSIOLOGY The aetiological factors in chronic pancreatitis vary geographically, however globally alcohol remains by far the most common cause. Tropical pancreatitis is commonly seen in Asian, African and South American countries situated within 15º of the Equator.
8 Alcohol Table 2 Aetiology of Chronic Pancreatitis Nutritional (tropical Africa & Asia) Cystic fibrosis Hereditary Idiopathic (10-30%) Autoimmune Obstructive Pancreas Divisum Duct Obstruction (eg. Carcinaoma While the inflammatory process usually involves the entire pancreas, some parts may be more severely affected. A predominant inflammatory mass in the head of the pancreas occurs in about 30% of cases. During acute exacerbations there is increased interstitial oedema, necrosis and inflammatory infiltration. Intraductal calcification is seen in advanced disease and is more common in alcohol induced and tropical pancreatitis. Although the pathophysiology of chronic pancreatitis is complex and poorly understood, in alcohol induced chronic pancreatitis the most widely accepted hypothesis is the so-called necrosis-inflammation-fibrosis sequence, mediated by the formation of fatty acid ethanol esters (FAEEs). This sequence, once established may be self-perpetuating. Smoking is an important co-factor in the pathological processes precipitated by alcohol. In addition there is formation of calcified stones believed to be the result of decreased bicarbonate and water secretion on the one hand and increased protein and calcium secretion on the other, resulting in precipitation of intraductal protein plugs which subsequently calcify. Pain is the most predominant symptom in chronic pancreatitis. Understanding of the mechanisms leading to the development of pain remain equally poorly understood but are likely multi-factorial and may vary during the course of the disease. The most predominant theories include: Inflammatory processes and calcified ductal protein plugs lead to parenchymal fibrosis and ductal epithelial damage with morphological ductal changes resulting in strictures and obstruction with consequent ductal and tissue hypertension. Ductal dilatation eventually occurs. Interaction between the products of inflammation and damaged neural structures. Toxin metabolism and the generation of excessive oxygen derived free radicals which exceed normal protective mechanisms. Parenchymal fibrosis leads to a form of compartment syndrome with microvascular ischaemia and pain Complications may develop in the setting of prolonged and persistent disease. Pancreatic destruction with endocrine and/or exocrine insufficiency are particularly clinically relevant and result in the development of diabetes mellitus and fat malabsorption, leading to significant morbidity and even mortality. Inflammation, necrosis and ductal hypertension may also lead to ductal disruption with the development of pancreatic fluid collections (pseudocysts) and pancreatic ascites. Other complications include the development of a false aneurysm with subsequent haemorrhage in relation to a pseudocyst; splenic vein thrombosis leading to segmental portal hypertension and biliary or duodenal stenosis with obstruction. Although a causal relationship has not been demonstrated it is believed that there is a higher incidence of pancreatic cancer in patients with chronic pancreatitis. To this end, any patient known with chronic pancreatitis
9 who deteriorates clinically should be actively investigated to have malignancy excluded. Patients with hereditary pancreatitis are known to be at increased risk for cancer. CLINICAL PRESENTATION (SYMPTOMS AND SIGNS) The first attack of alcohol induced pancreatitis is usually preceded by a long period (±10 years) of excessive alcohol intake. This first attack may be either in the form of a severe or mild attack. The attacks are usually induced by binge drinking and present on the afternoon after the night before. Two clinical patterns subsequently emerge; a form where intermittent attacks remain mild and the disease may even burn out and a second more severe group, where the disease follows a more progressive course with severe and persistent pain with or without the development of complications. This pattern is also seen in the idiopathic form. Once established, pain may persist despite the patient being abstinent. Metabolic complications such as diabetes and steatorrhoea usually develop after years. Pain is the most incapacitating part of the disease. The pain is typically located in the epigastrium with radiation to the back and is frequently worse after meals and may be relieved by sitting upright or leaning forward. It is often associated with nausea and vomiting. Persistent pain is often linked with cyst formation or continued alcohol abuse. Patients seek relief by lying on their side in a jack-knife position. Hot water bottles are often used to relieve the pain which frequently leads to skin burn marks (erythema ab igne). Patients may also present with a palpable mass due to a pseudocyst, ascites, obstructive jaundice due to compression of the bile duct and gastrointestinal bleeding from a false aneurysm communicating with the pancreatic duct (haemosuccus pancreaticus) or gastric varices related to segmental portal hypertension. Most patients who develop diabetes mellitus require insulin which often creates problems with sugar control due to a lack of endogenous glucagon. This contributes to a greater sensitivity to insulin which together with poor compliance, increase the risk of hypoglycaemic complications. Exocrine insufficiency with consequent fat malabsortion may result in steatorrhoea, which when clinically overt, presents with bulky, pale and offensive stools. In severe cases uncontrolled passage of oil poses a major social problem for the patient and his family. Gross fat malabsorption may lead to severe weight loss and vitamin deficiencies. Most patients with alcohol induced pancreatitis are tobacco smokers and are therefore at risk of developing lung and throat cancers as well as cardiovascular diseases. MANAGEMENT INCLUDING INVESTIGATION AND TREATMENT Special investigations 1. Blood investigations Serum amylase / lipase may be raised, especially during acute exacerbations, however peak levels may be limited by reduced production due to long term pancreatic destruction. HBA1C and random or fasting blood glucose levels are accurate screening tools for the development of diabetes mellitus. Where doubt remains, oral glucose tolerance testing may be performed. A low albumen value may be a clue to malabsorption and nutritional deficiency. Elevated liver function tests (bilirubin, ALP, GGT) may indicate impending or established biliary obstruction. 2. Pancreatic fuction tests These may be either direct or indirect; direct tests are quite
10 cumbersome and have largely fallen out of favour. Many of the indirect tests are easier to perform but to a large degree lack sensitivity and specificity. Faecal acid steatocrit and elastase are reasonably accurate measurements of the stool fat content and are inexpensive and easy to perform, however they are limited in detecting mild to moderate disease. 3. Imaging This plays a crucial role in the diagnosis and characterisation of chronic pancreatitis. CT scanning, MRI/MRCP and endoscopic ultrasound are the diagnostic modalities of choice. ERCP has a more limited role in diagnosis but has the benefit of offering therapeutic options in select circumstances. Treatment Pain control Patients with established chronic pancreatitis do not necessarily follow an intractable course and as such a majority can be managed conservatively for prolonged periods and in some indefinitely. In the group of patients with mild disease, recurrent episodes of acute exacerbations can be managed by hospitalisation to help the patient over the acute phase and to provide the patient with a pain control medication regime avoiding opiates as far as possible. A step up regime is generally employed, utilising the following: Abstinence with a low fat diet Non-narcotic analgesia (paracetomol or non-steroidal anti-inflammatory drugs) Trial of high dose pancreatic enzymes together with acid suppression Narcotic analgesics, progressing in potency as necessary Consideration of anti-depressant medication to alleviate coexistent depression, ameliorate pain and potentiate opiates. When opiates are required, it is advisable to avoid those which are highly addictive such as pethidine. To this end, morphine in one form or another remains the best opiate for long-term pain management. Antioxidant supplementation has also been evaluated in the management of pain in chronic pancreatitis and although there is some data in favour of this as a potential treatment, the evidence should probably still be considered insufficient to recommend this routinely. Referral to a multidisciplinary pain clinic is advisable once control of pain becomes problematic. In alcohol induced pancreatitis, patients should be encouraged to enter a rehabilitation programme with support from a social worker, particularly when there are problems with employment. Patients should also be encouraged to stop smoking as there is evidence that this is an important contributing factor in the progression of the disease. In addition, complications or alternative diagnoses which may contribute to the development of pain should be excluded; these include pseudocyst formation, biliary / duodenal obstruction, malignancy and peptic ulcer disease. There is a group of patients who continue to suffer intractable pain, despite giving up alcohol, maximal medical management and in the absence of complications such as pseudocysts. A percutaneous coeliac plexus block or division of the thoracic afferent sensory nerves with a thoracoscopic splanchnicectomy may provide temporary relief but most of these patients will eventually require some form of surgical intervention. The risk of opoid addiction in prolonged conservative management must be weighed against the operative risks, in particular that of compromised pancreatic function.
11 Various operations have been recommended in patients with intractable pain. These can be broadly divided into drainage and resectional procedures. The choice of surgery is largely governed by the morphological changes in the pancreas (in particular whether the pancreatic duct is suitable for a drainage procedure) and whether there is a suspicion of malignancy. Drainage procedures: A pancreatic duct drainage procedure only (pancreatico-jejunostomy) is usually performed when there is isolated dilatation of the pancreatic duct. When there is an associated inflammatory mass in the head, the drainage procedure is extended further, into the head of the pancreas (Frey procedure). Resection procedures: these are performed when there is concern about a malignancy or when a drainage procedure is not feasible. If a resection of the head is required, a pylorus preserving pancreaticoduodenectomy or duodenal preserving pancreatectomy is recommended to minimise nutritional disturbances. A distal pancreatectomy is performed when there is an inflammatory mass in the tail with or without an associated pseudocyst. Worsening of pancreatic endocrine and exocrine functions are common after these resectional operations thus drainage procedures are preferred where possible. Endoscopic treatment by stenting with or without extracorporeal lithotripsy (ESWL) is seldom indicated in the treatment of pain in uncomplicated chronic pancreatitis and is limited in the main to localised and dominant strictures/stones near the Ampulla of Vater Treatment of complications Diabetes mellitus requires careful control with the emphasis on keeping the blood sugar above normoglycaemic levels to avoid hypoglycaemic complications. Insulin is invariably required for these patients but must be carefully monitored to avoid the aforementioned hypoglycaemic complications. Malapsorption and Steatorrhoea can usually be controlled by pancreatic enzyme replacement therapy in the form of extracts from porcine pancreas taken with meals. Under optimal conditions approximately IU of lipase is required per meal. Enteric coated preparations are preferred in order to protect the lipase from inactivation by gastric acid. Patients who remain symptomatic may benefit from acid suppressing medication. Pseudocysts in chronic pancreatits should be treated only once they become symptomatic, either causing pain or obstruction. Size alone is not an indication to intervene. In suitable cases endoscopic treatment is the preferred treatment, the scope of which has increased when performed under endoscopic ultrasound guidance. Surgery is reserved for cases unsuitable for endoscopic drainage and failures with recurrence of pain with or without recurrence of the pseudocyst. Surgical drainage may include cyst-gastrostomy, cystduodenostomy and cystjejunostomy. Haemorrhage from false aneurysms related to a pseudocyst is best controlled by selective angiographic embolisation. Patients with pancreatic ascites and/or pleural effusions may be effectively treated by decompression of the pancreatic duct by means of a pancreatic ductal stent placed at ERCP. Patients with asymptomatic bile duct strictures should be treated conservatively with regular follow-up. Endoscopic interventions and stenting should be discouraged, as this may cause secondary infection particularly
12 when the stents occlude. Patients who present with jaundice should initially be treated conservatively, unless there is associated cholangitis when a temporary stent should be placed. If the jaundice resolves, no further intervention is required but patients will require follow-up. If jaundice persists or where a biliary stent has been placed to manage cholangitis, a biliary bypass procedure in the form of a hepatico-jejunostomy is indicated. In the setting of duodenal obstruction, surgical relief of the obstruction is invariably required. This may involve simple mobilisation of the duodenum or a bypass type procedure such as a gastro-jejunostomy, duodeno-duodenostomy or a duodeno-jejunostomy. This work is licensed under a Creative Commons Attribution 3.0 Unported License.
Prof. (DR.) MD. ISMAIL PATWARY. MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet
 Prof. (DR.) MD. ISMAIL PATWARY MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet CHRONIC PANCREATITIS Defined as a progressive inflammatory
Prof. (DR.) MD. ISMAIL PATWARY MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet CHRONIC PANCREATITIS Defined as a progressive inflammatory
Chronic Pancreatitis
 Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
16 April 2010 Resident Teaching Conference. Pancreatitis. W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D.
 16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
CLINICAL MANIFESTATIONS AND DIAGNOSIS OF ACUTE PANCREATITIS. Raed Abu Sham a, M.D
 CLINICAL MANIFESTATIONS AND DIAGNOSIS OF ACUTE PANCREATITIS Raed Abu Sham a, M.D ACUTE PANCREATITIS Acute inflammatory process of the pancreas that resolves both clinically and histologically. It is usually
CLINICAL MANIFESTATIONS AND DIAGNOSIS OF ACUTE PANCREATITIS Raed Abu Sham a, M.D ACUTE PANCREATITIS Acute inflammatory process of the pancreas that resolves both clinically and histologically. It is usually
Chronic Pancreatitis (1 of 4) i
 Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
Pancreatitis. Acute Pancreatitis
 Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland
 pancreas Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland Acute pancreatitis Inflammation of the pancreas associated with acinar cell injury Clinical features: 1-abdominal pain cardinal
pancreas Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland Acute pancreatitis Inflammation of the pancreas associated with acinar cell injury Clinical features: 1-abdominal pain cardinal
Treatment of chronic calcific pancreatitis endoscopy versus surgery
 Treatment of chronic calcific pancreatitis endoscopy versus surgery 35 - year old ladypresented to LPC Mumbai with intermittent abdominal pain. Pain was intermittent, colicky, more in epigastrium and periumbilical
Treatment of chronic calcific pancreatitis endoscopy versus surgery 35 - year old ladypresented to LPC Mumbai with intermittent abdominal pain. Pain was intermittent, colicky, more in epigastrium and periumbilical
Emergency Surgery Course Graz, March ACUTE PANCREATITIS. Carlos Mesquita Coimbra
 ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
Diseases of pancreas - Chronic pancreatitis
 Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
PATHOLOGY MCQs. The Pancreas
 PATHOLOGY MCQs The Pancreas A patient with cystic fibrosis is characteristically: A. more than 45 years of age B. subject to recurring pulmonary infections C. obese D. subject to spontaneous fractures
PATHOLOGY MCQs The Pancreas A patient with cystic fibrosis is characteristically: A. more than 45 years of age B. subject to recurring pulmonary infections C. obese D. subject to spontaneous fractures
CLASSIFICATION OF CHRONIC PANCREATITIS
 CLASSIFICATION OF CHRONIC PANCREATITIS EAGE, Podstgraduate Course, Prague, April 2010. Tomica Milosavljević School of Medicine, University of Belgrade Clinical Center of Serbia,Belgrade The phrase chronic
CLASSIFICATION OF CHRONIC PANCREATITIS EAGE, Podstgraduate Course, Prague, April 2010. Tomica Milosavljević School of Medicine, University of Belgrade Clinical Center of Serbia,Belgrade The phrase chronic
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
PANCREATIC PSEUDOCYSTS. Madhuri Rao MD PGY-5 Kings County Hospital Center
 PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
Diagnosis of chronic Pancreatitis. Christoph Beglinger, University Hospital Basel, Switzerland
 Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Nutrition in Pancreatic Disease Topic 14
 Nutrition in Pancreatic Disease Topic 14 Module 14.2 Chronic Pancreatitis Learning objectives Johann Ockenga, MD, Prof. Dep. of Gastroenterology, Endocrinology & Nutrition, Klinikum Bremen Mitte, St. Juergensstrasse
Nutrition in Pancreatic Disease Topic 14 Module 14.2 Chronic Pancreatitis Learning objectives Johann Ockenga, MD, Prof. Dep. of Gastroenterology, Endocrinology & Nutrition, Klinikum Bremen Mitte, St. Juergensstrasse
Chronic Pancreatitis. Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture
 Chronic Pancreatitis Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture What is Chronic Pancreatitis Progressive inflammatory disease Pancreatic parenchyma replaced w/fibrous tissue Destruction
Chronic Pancreatitis Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture What is Chronic Pancreatitis Progressive inflammatory disease Pancreatic parenchyma replaced w/fibrous tissue Destruction
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
Pancreatic Lesions. Valerie Jefford Pediatric Surgery Rounds June 6, 2003
 Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
Chronic Pancreatitis
 Supportive module 2: Basics of diagnosis, treatment and prevention of major gastroenterological diseases Chronic Pancreatitis LECTURE IN INTERNAL MEDICINE FOR IV COURSE STUDENTS M. Yabluchansky, L. Bogun,
Supportive module 2: Basics of diagnosis, treatment and prevention of major gastroenterological diseases Chronic Pancreatitis LECTURE IN INTERNAL MEDICINE FOR IV COURSE STUDENTS M. Yabluchansky, L. Bogun,
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Diseases of exocrine pancreas
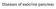 Diseases of exocrine pancreas The exocrine pancreas constitutes 80% to 85% of the organ and is composed of acinar cells that secrete enzymes needed for digestion. the accessory duct of Santorini, the main
Diseases of exocrine pancreas The exocrine pancreas constitutes 80% to 85% of the organ and is composed of acinar cells that secrete enzymes needed for digestion. the accessory duct of Santorini, the main
ESPEN Congress The Hague 2017
 ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
The Bile Duct (and Pancreas) and the Physician
 The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
The role of ERCP in chronic pancreatitis
 The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Exocrine functions: secretion of digestive enzymes (eg. lipase, amylase,
 Chapter 91 Pancreas Episode Overview: 1. List 10 differential diagnoses for acute pancreatitis 2. List 10 causes of pancreatitis. Which are most common in adults? Which one is most common in pediatrics?
Chapter 91 Pancreas Episode Overview: 1. List 10 differential diagnoses for acute pancreatitis 2. List 10 causes of pancreatitis. Which are most common in adults? Which one is most common in pediatrics?
Digestive System Module 6: Accessory Organs in Digestion: The Liver, Pancreas, and Gallbladder
 Connexions module: m49293 1 Digestive System Module 6: Accessory Organs in Digestion: The Liver, Pancreas, and Gallbladder Donna Browne Based on Accessory Organs in Digestion: The Liver, Pancreas, and
Connexions module: m49293 1 Digestive System Module 6: Accessory Organs in Digestion: The Liver, Pancreas, and Gallbladder Donna Browne Based on Accessory Organs in Digestion: The Liver, Pancreas, and
Acute Pancreatitis. What is the Pancreas? What does it do? What is acute pancreatitis? What causes acute pancreatitis? What symptoms do you get?
 In association with: Primary Care Society for Gastroenterology INFORMATION ABOUT Acute Pancreatitis www.corecharity.org.uk What is the Pancreas? What does it do? What is acute pancreatitis? What causes
In association with: Primary Care Society for Gastroenterology INFORMATION ABOUT Acute Pancreatitis www.corecharity.org.uk What is the Pancreas? What does it do? What is acute pancreatitis? What causes
Together, putting patients first
 The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine
 Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
PANCREATITIS. By April McMurray. March 14, 2013 NDFS 356
 PANCREATITIS By April McMurray March 14, 2013 NDFS 356 INTRODUCTION The pancreas is a small gland that sits behind the stomach and plays an important role in digestion (1). Its head is situated within
PANCREATITIS By April McMurray March 14, 2013 NDFS 356 INTRODUCTION The pancreas is a small gland that sits behind the stomach and plays an important role in digestion (1). Its head is situated within
Week 3 The Pancreas: Pancreatic ph buffering:
 Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Figure 2: Post-cholecystectomy biliary-like pain
 Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4)
 Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
Preview of the Medifocus Guidebook on: Chronic Pancreatitis Updated July 4, 2018
 Preview of the Medifocus Guidebook on: Chronic Pancreatitis Updated July 4, 2018 This document is only a SHORT PREVIEW of the Medifocus Guidebook on Chronic Pancreatitis. It is intended primarily to give
Preview of the Medifocus Guidebook on: Chronic Pancreatitis Updated July 4, 2018 This document is only a SHORT PREVIEW of the Medifocus Guidebook on Chronic Pancreatitis. It is intended primarily to give
This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated.
 A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
ESPEN Congress Brussels 2005
 ESPEN Congress Brussels 2005 Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition? Myriam Delhaye Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition?
ESPEN Congress Brussels 2005 Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition? Myriam Delhaye Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition?
DIGESTIVE. CHAPTER 17 Lecture: Part 1 Part 2 BIO 212: ANATOMY & PHYSIOLOGY II
 BIO 212: ANATOMY & PHYSIOLOGY II CHAPTER 17 Lecture: DIGESTIVE Part 1 Part 2 Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. SMALL INTESTINE DUODENUM > JEJUNUM
BIO 212: ANATOMY & PHYSIOLOGY II CHAPTER 17 Lecture: DIGESTIVE Part 1 Part 2 Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. SMALL INTESTINE DUODENUM > JEJUNUM
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
Evaluation of Suspected Pancreatic Cancer
 Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD
 Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD Disclosure: None In accordance with the Standards of the Wisconsin Medical Society, all those
Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD Disclosure: None In accordance with the Standards of the Wisconsin Medical Society, all those
Complex pancreatico- duodenal injuries. Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University
 Complex pancreatico- duodenal injuries Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University Pancreatic and duodenal trauma: daunting or simply confusing? 2-4% of abdominal
Complex pancreatico- duodenal injuries Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University Pancreatic and duodenal trauma: daunting or simply confusing? 2-4% of abdominal
Chapter 15 Gastrointestinal System
 Chapter 15 Gastrointestinal System Dr. LL Wang E-mail: wanglinlin@zju.edu.cn Rm 608, Block B, Research Building, School of Medicine, Zijingang Campus Pancreatic Secretion The exocrine cells in the pancreas
Chapter 15 Gastrointestinal System Dr. LL Wang E-mail: wanglinlin@zju.edu.cn Rm 608, Block B, Research Building, School of Medicine, Zijingang Campus Pancreatic Secretion The exocrine cells in the pancreas
5. Which component of the duodenal contents entering the stomach causes the most severe changes to gastric mucosa:
 Gastro-intestinal disorders 1. Which are the most common causes of chronic gastritis? 1. Toxic substances 2. Chronic stress 3. Alimentary factors 4. Endogenous noxious stimuli 5. Genetic factors 2. Chronic
Gastro-intestinal disorders 1. Which are the most common causes of chronic gastritis? 1. Toxic substances 2. Chronic stress 3. Alimentary factors 4. Endogenous noxious stimuli 5. Genetic factors 2. Chronic
د. عصام طارق. Objectives:
 GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
-12. -Renad Habahbeh. -Dr Mohammad mohtasib
 -12 -Renad Habahbeh - -Dr Mohammad mohtasib The Gallbladder -The gallbladder has a body, a fundus (a rounded end), a neck, Hartmann s pouch before the neck and a cystic duct that meets the common hepatic
-12 -Renad Habahbeh - -Dr Mohammad mohtasib The Gallbladder -The gallbladder has a body, a fundus (a rounded end), a neck, Hartmann s pouch before the neck and a cystic duct that meets the common hepatic
Causes of pancreatic insufficiency. Eugen Dumitru
 Causes of pancreatic insufficiency Eugen Dumitru Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes 3. The Consequences Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes
Causes of pancreatic insufficiency Eugen Dumitru Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes 3. The Consequences Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes
Development of the Liver and Pancreas
 Development of the Liver and Pancreas Professor Alfred Cuschieri Department of Anatomy University of Malta Three glandular buds arise from the distal end of the foregut during the fourth week Day 22 -The
Development of the Liver and Pancreas Professor Alfred Cuschieri Department of Anatomy University of Malta Three glandular buds arise from the distal end of the foregut during the fourth week Day 22 -The
BILIARY TRACT & PANCREAS, PART II
 CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
Pathophysiology ACUTE PANCREATITIS
 Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE. T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar
 ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
Anatomy of the biliary tract
 Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Gastric ulcer Duodenal ulcer Pancreatitis Ileus. Barbora Konečná
 Gastric ulcer Duodenal ulcer Pancreatitis Ileus Barbora Konečná basa.konecna@gmail.com Peptic ulcers of stomach and duodenum (PUD) Ulcers are chronic, often solitary lesions, that occur in any part of
Gastric ulcer Duodenal ulcer Pancreatitis Ileus Barbora Konečná basa.konecna@gmail.com Peptic ulcers of stomach and duodenum (PUD) Ulcers are chronic, often solitary lesions, that occur in any part of
Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram
 Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram Assistant Professor, Department of Biotechnoloy, Lady Doak College, Madurai. Acute
Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram Assistant Professor, Department of Biotechnoloy, Lady Doak College, Madurai. Acute
Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013
 Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013 Case Report 42F with h/o chronic pancreatitis due to alcohol use with chronic upper
Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013 Case Report 42F with h/o chronic pancreatitis due to alcohol use with chronic upper
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
Appendix 9: Endoscopic Ultrasound in Gastroenterology
 Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Siddharth Gosavi, Vydehi Institute of Medical Sciences & Research Centre, India Under the guidance of Gillian Lieberman, MD
 Under the guidance of Gillian Lieberman, MD March 2016 RADIOLOGICAL HALLMARKS OF NECROTIZING PANCREATITIS Siddharth Gosavi, Vydehi Institute of Medical Sciences & Research Centre, India Under the guidance
Under the guidance of Gillian Lieberman, MD March 2016 RADIOLOGICAL HALLMARKS OF NECROTIZING PANCREATITIS Siddharth Gosavi, Vydehi Institute of Medical Sciences & Research Centre, India Under the guidance
Acute pancreatitis. Information for patients Hepatobiliary
 Acute pancreatitis Information for patients Hepatobiliary What is acute pancreatitis? Acute pancreatitis is an inflammation of the pancreas gland. The main symptoms are: severe abdominal pain severe back
Acute pancreatitis Information for patients Hepatobiliary What is acute pancreatitis? Acute pancreatitis is an inflammation of the pancreas gland. The main symptoms are: severe abdominal pain severe back
Pediatric Pancreatic Lesions
 Pediatric Pancreatic Lesions Pediatric Surgery Grand Rounds 9 October 2013 Tim Weatherall, PGY2 The University of Tennessee Health Science Center Memphis, TN Disclosures No financial interests to disclose
Pediatric Pancreatic Lesions Pediatric Surgery Grand Rounds 9 October 2013 Tim Weatherall, PGY2 The University of Tennessee Health Science Center Memphis, TN Disclosures No financial interests to disclose
Pancreas and Biliary System
 Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Perforation of a Duodenal Diverticulum. Elective Student S. C.
 Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Overview. Doumit S. BouHaidar, MD ACG/VGS/ODSGNA Regional Postgraduate Course Copyright American College of Gastroenterology 1
 Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
What Is Pancreatitis?
 What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
Endoscopic Management of Acute Pancreatitis. Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018
 Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
PANCREATITIS: MEDICAL AND TRANSPLANT CONSIDERATIONS, DHIRAJ YADAV, MD 1
 DHIRAJ YADAV, MD 1 Good afternoon. This is actually an interesting time of the day to do pancreas topic since you just had lunch and this is the time when the pancreas is the most active with a lot of
DHIRAJ YADAV, MD 1 Good afternoon. This is actually an interesting time of the day to do pancreas topic since you just had lunch and this is the time when the pancreas is the most active with a lot of
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY
 OPEN ACCESS TEXTBOOK OF GENERAL SURGERY MESENTERIC ISCHAEMIA P Zwanepoel INTRODUCTION Mesenteric ischaemia results from hypoperfusion of the gut, most commonly due to occlusion, thrombosis or vasospasm.
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY MESENTERIC ISCHAEMIA P Zwanepoel INTRODUCTION Mesenteric ischaemia results from hypoperfusion of the gut, most commonly due to occlusion, thrombosis or vasospasm.
Etiology of chronic pancreatitis I. ALCOHOL Long-term alcohol abuse: Men 80g, women 40-50g/day for years Fatty food, coffee, smoking, concent
 Chronic pancreatitis Definition: Chronic pancreatitis Irreversible destruction of parenchyma Increase of the amount of connective tissue Signs of inflammation Signs of regeneration Decrease of exocrine
Chronic pancreatitis Definition: Chronic pancreatitis Irreversible destruction of parenchyma Increase of the amount of connective tissue Signs of inflammation Signs of regeneration Decrease of exocrine
Duodenum retroperitoneal
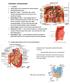 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Biliary Tree Ultrasound - In a nutshell. Pamela Parker Lead Sonographer
 Biliary Tree Ultrasound - In a nutshell Pamela Parker Lead Sonographer Aims Review what we know about the biliary system Common pathologies Pitfalls Reporting tips The Nutshell Background Biliary examinations
Biliary Tree Ultrasound - In a nutshell Pamela Parker Lead Sonographer Aims Review what we know about the biliary system Common pathologies Pitfalls Reporting tips The Nutshell Background Biliary examinations
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
SOD (Sphincter of Oddi Dysfunction)
 SOD (Sphincter of Oddi Dysfunction) SOD refers to the mechanical malfunctioning of the Sphincter of Oddi, which is the valve muscle that regulates the flow of bile and pancreatic juice into the duodenum.
SOD (Sphincter of Oddi Dysfunction) SOD refers to the mechanical malfunctioning of the Sphincter of Oddi, which is the valve muscle that regulates the flow of bile and pancreatic juice into the duodenum.
Physiology Unit 4 DIGESTIVE PHYSIOLOGY
 Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Overview. The Pancreas Pancreatitis Signs + Symptoms Investigations Grading Systems Role of Surgery Management of Chronic Pancreatitis Summary
 James Bain May 2014 1. What are the grading systems for Pancreatitis? 2. What is the role of surgery in acute pancreatitis? 3. What the principles of managing chronic pancreatitis? Overview The Pancreas
James Bain May 2014 1. What are the grading systems for Pancreatitis? 2. What is the role of surgery in acute pancreatitis? 3. What the principles of managing chronic pancreatitis? Overview The Pancreas
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
Magnetic resonance cholangiopancreatography (MRCP) is an imaging. technique that is able to non-invasively assess bile and pancreatic ducts,
 SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
Patient characteristics Intervention Comparison Length of follow-up. Endoscopic treatment. Endoscopic transampullary drainage of the pancreatic duct
 1) In patients with alcohol-related, what is the safety and efficacy of a) coeliac access block vs medical management b) thoracoscopic splanchnicectomy vs medical management c) coeliac access block vs
1) In patients with alcohol-related, what is the safety and efficacy of a) coeliac access block vs medical management b) thoracoscopic splanchnicectomy vs medical management c) coeliac access block vs
Soft palate elevates, closing off the nasopharynx. Hard palate Tongue Bolus Epiglottis. Glottis Larynx moves up and forward.
 The Cephalic Phase Chemical and mechanical digestion begins in the mouth Saliva is an exocrine secretion Salivary secretion is under autonomic control Softens and lubricates food Chemical digestion: salivary
The Cephalic Phase Chemical and mechanical digestion begins in the mouth Saliva is an exocrine secretion Salivary secretion is under autonomic control Softens and lubricates food Chemical digestion: salivary
Role of Imaging Methods in Diagnosis of Acute Pancreatitis. Válek V. Radiologická klinika, FN Brno a LF MU v Brně
 Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
U Nordic Forum - Trauma & Emergency Radiology. Lecture Objectives. MDCT in Acute Pancreatitis. Acute Pancreatitis: Etiologies
 Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Chronic Pancreatitis
 Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Safe Answers For The American Board of Surgery Certifying Exam & Recertifying Exam
 Safe Answers For The American Board of Surgery Certifying Exam & Recertifying Exam By Sarmad Aji, MD., FACS. A comprehensive review of the most commonly asked questions on the American Board of Surgery
Safe Answers For The American Board of Surgery Certifying Exam & Recertifying Exam By Sarmad Aji, MD., FACS. A comprehensive review of the most commonly asked questions on the American Board of Surgery
LIVER CIRRHOSIS. The liver extracts nutrients from the blood and processes them for later use.
 LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
Anatomy of the liver and pancreas
 Anatomy of the liver and pancreas Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk abdulameerh@yahoo.com Liver Aorta Pulm. Trunk Rt. At, Duct. Art. Lt. Ven. Rt. Ven. Internal Posterior
Anatomy of the liver and pancreas Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk abdulameerh@yahoo.com Liver Aorta Pulm. Trunk Rt. At, Duct. Art. Lt. Ven. Rt. Ven. Internal Posterior
