Gastrointestinal Hormones: Introduction and Index
|
|
|
- Myron Parks
- 5 years ago
- Views:
Transcription
1 Gastrointestinal Hormones: Introduction and Index Digesting, absorbing and assimilating a meal requires precise coordination of a huge number of physiologic processes. Control over gastrointestinal function is, as one would expect, provided by nervous and endocrine systems. The hormones most important in controlling digestive function are synthesized within the gastrointestinal tract by cells scattered in the epithelium of the stomach and small intestine. These endocrine cells and the hormones they secrete are referred to as the enteric endocrine system. Interestingly, most if not all "GI hormones" are also synthesized in the brain. The following discussions assume some familiarity with the anatomy and physiology of the digestive system. Core information on gastrointestinal endocrinology is presented in the following topics: Overview of Gastrointestinal Hormones Gastrin Cholecystokinin Secretin Ghrelin Motilin Advanced and supplemental topics related to gastrointestinal hormones: Enteroglucagon and Glucagon-Like Peptides Gastric Inhibitory Peptide Vasoactive Intestinal Peptide Overview of Gastrointestinal Hormones If you are like most people, you eat several meals and occasional snacks each day, but rarely think about the immense number of tasks that must be performed by your digestive system to break down, absorb and assimilate those nutrients. Robust control
2 systems are required to coordinate digestive processes in man and animals, and are provided by both the nervous and endocrine systems. Endocrine control over digestive functions is provided by the so-called enteric endocrine system, which is summarized elsewhere. There are a bunch of hormones, neuropeptides and neurotransmitters that affect gastrointestinal function. Interestingly, a number of the classical GI hormones are also synthesized in the brain, and sometimes referred to as "brain-gut peptides". The significance of this pattern of expression is not clear. The following table summarizes the effects and stimuli for release of the major gastrointestinal hormones, each of which is discussed in more detail on subsequent pages: Hormone Major Activities Stimuli for Release Gastrin Cholecystokinin Secretin Ghrelin Motilin Gastric inhibitory polypeptide Gastrin Stimulates gastric acid secretion and proliferation of gastric epithelium Stimulates secretion of pancreatic enzymes, and contraction and emptying of the gall bladder Stimulates secretion of water and bicarbonate from the pancreas and bile ducts Appears to be a strong stimulant for appetite and feeding; also a potent stimulator of growth hormone secretion. Apparently involved in stimulating housekeeping patterns of motility in the stomach and small intestine Inhibits gastric secretion and motility and potentiates release of insulin from beta cells in response to elevated blood glucose concentration Presence of peptides and amino acids in gastric lumen Presence of fatty acids and amino acids in the small intestine Acidic ph in the lumen of the small intestine Not clear, but secretion peaks prior to feeding and diminishes with gastric filling Not clear, but secretion is associated with fasting Presence of fat and glucose in the small intestine Gastrin is a major physiological regulator of gastric acid secretion. It also has an important trophic or growth-promoting influence on the gastric mucosa. Gastrin is
3 synthesized in G cells, which are located in gastric pits, primarily in the antrum region of the stomach and binds receptors found predominantly on parietal and enterochromaffin-like cells. Structure of Gastrin and the Gastrin Receptor Gastrin is a linear peptide that is synthesized as a preprohormone and is posttranslationally cleaved to form a family of peptides with identical carboxytermini. The predominant circulating form is gastrin-34 ("big gastrin"), but full biologic activity is present in the smallest peptide (gastrin-14 or minigastrin). Further, full bioactivity is preserved in the five C-terminal amino acids of gastrin, which is known as pentagastrin. Importantly, the five C-terminal amino acids of gastrin and cholecystokinin are identical, which explains their overlapping biological effects. The gastrin receptor is also one of the receptors that binds cholecystokinin, and is known as the CCK-B receptor. It is a member of the G protein-coupled receptor family. Binding of gastrin stimulates an increase in intracellular Ca++, activation of protein kinase C, and production of inositol phosphate. Control and Physiologic Effects of Gastrin The primary stimulus for secretion of gastrin is the presence of certain foodstuffs, especially peptides, certain amino acids and calcium, in the gastric lumen. Also, as yet unidentified compounds in coffee, wine and beer are potent stimulants for gastrin secretion. Secretion of this hormone is inhibited when the lumenal ph of the stomach becomes very low (less than about 3). Gastrin appears to have at least two major effects on gastrointestinal function: Stimulation of gastric acid secretion: Gastrin receptors are found on parietal cells, and binding of gastrin, along with histamine and acetylcholine, leads to fully-stimulated acid secretion by those cells. Canine parietal cells have roughly 44,000 gastrin receptors each, and in that species, it has been demonstrated that immunoneutralization of gastrin blocks secretion of acid in response to intragastric administration of peptides. Enterochromaffin-like (ECL) cells also bear gastrin receptors, and recent evidence indicates that this cell may be the most important target of gastrin with regard to regulating acid secretion. Stimulation of ECL cells by gastrin leads to histamine release, and histamine
4 binding to H2 receptors on parietal cells is necessary for full-blown acid secretion. Promotion of gastric mucosal growth: Gastrin clearly has the ability to stimulate many aspects of mucosal development and growth in the stomach. Treatment with gastrin stimulates DNA, RNA and protein synthesis in gastric mucosa and increases the number of parietal cellsanother observation supporting this function is that humans with hypergastrinemia (abnormally high blood levels of gastrin) consistently show gastric mucosal hypertrophy. In addition to parietal and ECL cell targets, gastrin also stimulates pancreatic acinar cells via binding to cholecystokinin receptors, and gastrin receptors have been demonstratede on certain populations of gastric smooth muscle cells, supporting pharmacologic studies that demonstrate a role for gastrin in regulating gastric motility. Disease States Excessive secretion of gastrin, or hypergastrinemia, is a well-recognized cause of a severe disease known as Zollinger-Ellison syndrome, which is seen at low frequency in man and dogs. The hallmark of this disease is gastric and duodenal ulceration due to excessive and unregulated secretion of gastric acid. Most commonly, hypergastrinemia is the result of gastrin-secreting tumors (gastrinomas), which develop in the pancreas or duodenum. Cholecystokinin Cholecystokinin plays a key role in facilitating digestion within the small intestine. It is secreted from mucosal epithelial cells in the first segment of the small intestine (duodenum), and stimulates delivery into the small intestine of digestive enzymes from the pancreas and bile from the gallbladder. Cholecystokinin is also produced by neurons in the enteric nervous system, and is widely and abundantly distributed in the brain. Structure of Cholecystokinin and Its Receptors As mentioned previously, cholecystokinin and gastrin are highly similar peptides. Like gastrin, cholecystokinin is a linear peptide that is synthesized as a preprohormone, then proteolytically cleaved to generate a family of peptides having the same carboxy ends. Full biologic activity is retained in CCK-8 (8 amino acids), but peptides of 33, 38 and 59 amino acids are also produced. In all of these CCK peptides, the tyrosine seven residues from the end is sulfated, which is necessary for activity.
5 Two receptors that bind cholecystokinin have been identified. The CCK A receptor is found abundantly on pancreatic acinar cells. The CCK B receptor, which also functions as the gastrin receptor, is the predominant form in brain and stomach. Both receptors are have seven transmembrane domains typical of G protein-coupled receptors. Control and Physiologic Effects of Cholecystokinin Foodstuffs flowing into the small intestine consist mostly of large macromolecules (proteins, polysaccharides and triglyceride) that must be digested into small molecules (amino acids, monosaccharides, fatty acids) in order to be absorbed. Digestive enzymes from the pancreas and bile salts from the liver (which are stored in the gallbladder) are critical for such digestion. Cholecystokinin is the principle stimulus for delivery of pancreatic enzymes and bile into the small intestine. The most potent stimuli for secretion of cholecystokinin are the presence of partiallydigested fats and proteins in the lumen of the duodenum (a particularly potent stimulus is pictured above). An elevation in blood concentration of cholecystokinin has two major effects that facilitate digestion: Release of digestive enzymes from the pancreas into the duodenum. Older literature refers to cholecystokinin as pancreozymin, a term coined to describe this effect. Contraction of the gallbladder to deliver bile into the duodenum. The name cholecystokinin (to "move the gallbladder") was given to describe this effect. Cholecystokinin is also known to stimulate secretion of bile salts into the biliary system. Pancreatic enzymes and bile flow through ducts into the duodenum, leading to digestion and absorption of the very molecules that stimulate cholecystokinin secretion. Thus, when absorption is completed, cholecystokinin secretion ceases. Injection of cholecystokinin into the ventricles of the brain induces satiety (lack of hunger) in laboratory animals. In view of its pattern of secretion relative to feeding, it would make physiologic sense that this hormone might participate in control of food intake. However, recent experiments suggest that cholecystokinin is at best a minor player in regulation of food intake. In addition to its synthesis in small intestinal epithelial cells, cholecystokinin has been clearly demonstrated in neurons within the wall of the intestine and in many
6 areas of the brain. It seems, in fact, to be the most abundant neuropeptide in the central nervous system. Secretion of cholecystokinin from neurons appears to modulate the activity of other hormones and neuropeptides, but it seems safe to say the understanding its role in function of the brain is rudimentary at best. Disease States Diseases resulting from excessive or deficient secretion of cholecystokinin are rare. Cholecystokinin deficiency has been described in humans as part of autoimmune polyglandular syndrome, and was manifest as a malabsorption syndrome clinically similar to pancreatic exocrine insufficiency. Additionally, there is mounting evidence that aberrations in expression of cholesystokinin or its receptor within the human brain may play a part in the pathogenesis of certain types of anxiety and schizophrenia. Clearly, a much better understanding of the role of cholecystokinin in brain function is required. Secretin The small intestine is periodically assaulted by a flood of acid from the stomach, and it is important to put out that fire in a hurry to avoid acid burns. Secretin functions as a type of fireman: it is released in response to acid in the small intestine, and stimulates the pancreas to release a flood of bicarbonate base, which neutralizes the acid.. Secretin is also of some historical interest, as it was the first hormone to be discovered. Structure of Secretin and Its Receptors Secretin is synthesized as a preprohormone, then proteolytically processed to yield a single 27-amino acid peptide by removal of the signal peptide plus amino and carboxy-terminal extensions. The sequence of the mature peptide is related to that of glucagon, vasoactive intestinal peptide and gastric inhibitory peptide. The secretin receptor has seven membrane-spanning domains and characteristics typical of a G protein-coupled receptor. Control and Physiologic Effects of Secretin Secretin is secreted in response to one known stimulus: acidification of the duodenum, which occurs most commonly when liquified ingesta from the stomach are released into the small intestine.
7 The principal target for secretin is the pancreas, which responds by secreting a bicarbonate-rich fluid, which flows into the first part of the intestine through the pancreatic duct. Bicarbonate ion is a base and serves to neutralize the acid, thus preventing acid burns and establishing a ph conducive to the action of other digestive enzymes. A similar, but quantitatively less important response to secretin is elicited by bile duct cells, resulting in additional bicarbonate being dumped into the small gut. As acid is neutralized by bicarbonate, the intestinal ph rises toward neutrality, and secretion of secretin is turned off. Disease States Diseases associated with excessive or deficient secretion of secretin are not recognized. Ghrelin Ghrelin was discovered as the peptide hormone that potently stimulates release of growth hormone from the anterior pituitary. It was subsequently determined that ghrelin, along with several other hormones, has significant effects on appetite and energy balance. The predominant source of ghrelin is epithelial cells in the stomach. Structure of Ghrelin and Its Receptor Ghrelin is synthesized as a preprohormone, then proteolytically processed to yield a 28-amino acid peptide. An interesting and unique modification is imposed on the hormone during synthesis in the form of an n-octanoic acid bound to one of its amino acids; this modification is necessary for biologic activity. Synthesis of ghrelin occurs predominantly in epithelial cells lining the fundus of the stomach, with smaller amounts produced in the placenta, kidney, pituitary and hypothalamus. The ghrelin receptor was known well before ghrelin was discovered. Cells within the anterior pituitary bear a receptor that, when activated, potently stimulates secretion of growth hormone - that receptor was named the growth hormone secretagoue receptor (GHS-R). The natural ligand for the GHS-R was announced in 1999 as ghrelin, and ghrelin was named for its ability to provoke growth hormone secretion (the suffix ghre means "grow"). Ghrelin receptors are present on the cells in the pituitary that secrete growth hormone,
8 and also have been identified in the hypothalamus, heart and adipose tissue. Control and Physiologic Effects of Ghrelin At least two major biologic activites have been ascribed to ghrelin: Stimulation of growth hormone secretion: Ghrelin, as the ligand for the growth hormone secretagogue receptor, potently stimulates secretion of growth hormone. The ghrelin signal is integrated with that of growth hormone releasing hormone and somatostatin to control the timing and magnitude of growth hormone secretion. Regulation of energy balance: In both rodents and humans, ghrelin functions to increase hunger though its action on hypothalamic feeding centers. This makes sense relative to increasing plasma ghrelin concentrations observed during fasting (see below). Additionally, humans injected with ghrelin reported sensations of intense hunger. Ghrelin also appears to suppress fat utilization in adipose tissue, which is somewhat paradoxical considering that growth hormone has the opposite effect. Overall, ghrelin seems to be one of several hormonal signals that communicates the state of energy balance in the body to the brain. Other effects of ghrelin include stimulating gastric emptying and having a variety of positive effects on cardiovascular function (e.g. increased cardiac output). It is not totally clear whether the cardiovascular effects are a direct effect of ghrelin or represent an indirect effect of ghrelin's ability to stimulate growth hormone secretion. Blood concentrations of ghrelin are lowest shortly after consumption of a meal, then rise during the fast just prior to the next meal. The figure to the right shows this pattern based on assays of plasma ghrelin in 10 humans during the course of a day.
9 Disease States Ghrelin concentrations in blood are reduced in obese humans compared to lean control subjects, but whether this is cause or effect is not defined. Patients with anorexia nervosa have higher than normal plasma ghrelin levels, which decrease if weight gain occurs. Prader-Willi syndrome is another disorder relevant to ghrelin science. Affected patients develop extreme obesity associated with uncontrollable and voracious appetite. The plasma ghrelin levels are exceptionally high in comparison to patients similarly obese due to other causes. Prader-Willi syndrome is clearly a complex disease with many defects; it may be that excessive ghrelin production contributes to the appetite and obesity components. Motilin Motilin is a 22 amino acid peptide secreted by endocrinocytes in the mucosa of the proximal small intestine. Based on amino acid sequence, motilin is unrelated to other hormones. Motilin participates in controlling the pattern of smooth muscle contractions in the upper gastrointestinal tract. There are two basic states of motility of the stomach and small intestine: the fed state, when foodstuffs are present, and the interdigestive state between meals. Motilin is secreted into the circulation during the fasted state at intervals of roughly 100 minutes. These bursts of motilin secretion are temporily related to the onset of "housekeeping contractions", which sweep the stomach and small intestine clear of undigested material (also called the migrating motor complex). Control of motilin secretion is largely unknown, although some studies suggest that an alkaline ph in the duodenum stimulates its release. An interesting aspect of the motilin story is that erythromycin and related antibiotics act as nonpeptide motilin agonists, and are sometimes used for their ability to stimulate gastrointestinal motility. Administration of a low dose of erythromycin will induce a migrating motor complex, which provides additional support for the conclusion that motilin secretion triggers this pattern of GI motility, rather than results from it. Enteroglucagon and Glucagon-Like
10 Peptides Glucagon is best known as a peptide hormone secreted from pancreatic islets that participates in control of glucose metabolism. Glucagon is synthesized initially as the protein proglucagon, which, in mammals, is encoded by a single gene. Within alpha cells of the pancreas, proglucagon is processed by proteolytic cleavage into glucagon itself, and several biologically inactive peptides. Interestingly, the proglucagon gene is also expressed in the terminal small intestine and large intestine, where it is cleaved into a number of peptides other than glucagon. This alternative pathway for processing of proglucagon occurs in gut endocrinocytes called L cells. Because these peptides were discovered by cross reactions with antisera against glucagon, they were originally given the name "enteroglucagon", and are sometimes referred to collectively as "proglucagon-derived peptides". The major, characterized patterns of proglucagon processing are depicted in the figure below. In both pancreas and gut, three types of products are generated: Peptides with known biological activity (yellow color): glucagon and glucagon-like peptide-1 (GLP-1) Peptides that may have biological activity, but which are poorly characterized or active only at what are considered non-physiologic concentrations (cyan color): glucagon-like peptide-2 (GLP-2) and oxyntomodulin Peptides without apparent biological activity(gray color): glicentin, glicentinrelated pancreatic peptide, major proglucagon fragment. Regardless of activity, each of these peptides is secreted into blood after ingestion of a meal containing carbohydrates or lipids.
11 Glucagon-like peptide-1 has a major effect of enhancing the release of insulin in response to a glucose stimulus, and coincidentally, suppressing secretion of glucagon. As a result, injections of this hormone lower blood glucose levels, not only in normal people, but in those having insulin-dependent and non-insulin-dependent diabetes mellitus. For this reason, GLP-1 is being investigated for its utility in the therapy of diabetes. GLP-1 has been shown to potently inhibit several aspects of digestive function, including gastric emptying, gastric secretion and pancreatic secretion. Like many gut peptides, GLP-1 is also synthesized in the brain, and may play a role in control of food intake. Glucagon-like peptide-2 is not well characterized, but some reports suggest that it stimulates proliferation of intestinal epithelial cells. Oxyntomodulin is identical to glucagon, but with an 8 amino acid extension on the C- terminus. Experimentally, it has glucagon-like activity, but this is of doubtful physiologic significance, as it binds the glucagon receptor with low affinity relative to glucagon. Other effects that have been demonstrated include inhibition of gastric secretion and motility, and inhibition of pancreatic secretion. References and Reviews Ahren B: Glucagon-like peptide-1 (GLP-1): a gut hormone of potential interest in the treatment of diabetes. Bioessays 20: , Drucker DJ: Glucagon-like peptides. Diabetes 47: , Holst JJ: Enteroglucagon. Annu Rev Physiol 59: , Enteroglucagon and Glucagon-Like Peptides Glucagon is best known as a peptide hormone secreted from pancreatic islets that participates in control of glucose metabolism. Glucagon is synthesized initially as the protein proglucagon, which, in mammals, is encoded by a single gene. Within alpha cells of the pancreas, proglucagon is processed by proteolytic cleavage into glucagon itself, and several biologically inactive peptides. Interestingly, the proglucagon gene is also expressed in the terminal small intestine and large intestine, where it is cleaved into a number of peptides other than
12 glucagon. This alternative pathway for processing of proglucagon occurs in gut endocrinocytes called L cells. Because these peptides were discovered by cross reactions with antisera against glucagon, they were originally given the name "enteroglucagon", and are sometimes referred to collectively as "proglucagon-derived peptides". The major, characterized patterns of proglucagon processing are depicted in the figure below. In both pancreas and gut, three types of products are generated: Peptides with known biological activity (yellow color): glucagon and glucagon-like peptide-1 (GLP-1) Peptides that may have biological activity, but which are poorly characterized or active only at what are considered non-physiologic concentrations (cyan color): glucagon-like peptide-2 (GLP-2) and oxyntomodulin Peptides without apparent biological activity(gray color): glicentin, glicentinrelated pancreatic peptide, major proglucagon fragment. Regardless of activity, each of these peptides is secreted into blood after ingestion of a meal containing carbohydrates or lipids. Glucagon-like peptide-1 has a major effect of enhancing the release of insulin in response to a glucose stimulus, and coincidentally, suppressing secretion of glucagon. As a result, injections of this hormone lower blood glucose levels, not only in normal people, but in those having insulin-dependent and non-insulin-dependent diabetes mellitus. For this reason, GLP-1 is being investigated for its utility in the therapy of diabetes. GLP-1 has been shown to potently inhibit several aspects of digestive function, including gastric emptying, gastric secretion and pancreatic secretion. Like many gut peptides, GLP-1 is also synthesized in the brain, and may play a role in control of food intake.
13 Glucagon-like peptide-2 is not well characterized, but some reports suggest that it stimulates proliferation of intestinal epithelial cells. Oxyntomodulin is identical to glucagon, but with an 8 amino acid extension on the C- terminus. Experimentally, it has glucagon-like activity, but this is of doubtful physiologic significance, as it binds the glucagon receptor with low affinity relative to glucagon. Other effects that have been demonstrated include inhibition of gastric secretion and motility, and inhibition of pancreatic secretion. References and Reviews Ahren B: Glucagon-like peptide-1 (GLP-1): a gut hormone of potential interest in the treatment of diabetes. Bioessays 20: , Drucker DJ: Glucagon-like peptides. Diabetes 47: , Holst JJ: Enteroglucagon. Annu Rev Physiol 59: , Gastric Inhibitory Peptide Gastric inhibitory peptide (GIP) is a member of the secretin family of hormones. It was discovered as a factor in extracts of intestine that inhibited gastric motility and secretion of acid, and initially called enterogastrone. Like secretin, it is secreted from mucosal epithelial cells in the first part of the small intestine. Another activity of GIP is its ability to enhance the release of insulin in response to infusions of glucose. For this action, it has also been referred to as glucose-dependent insulinotropic peptide. Vasoactive Intestinal Peptide VIP is a 28-amino acid peptide structurally related to secretin. It was originally isolated from intestinal extracts and shown to be a potent vasodilator. Subsequent work demonstrated that VIP is very widely distributed in the peripheral and central nervous systems, and probably should not be considered a true GI hormone.
14 A huge number of biological effects have been attributed to VIP. With respect to the digestive system, VIP seems to induce smooth muscle relaxation (lower esophageal sphincter, stomach, gallbladder), stimulate secretion of water into pancreatic juice and bile, and cause inhibition of gastric acid secretion and absorption from the intestinal lumen. Certain tumors arising from the pancreatic islets or nervous tissue (called VIPomas) secrete excessive quantities of VIP, and are associated with chronic, watery diarrhea.
Why would fatty foods aggravate the patient s RUQ pain? What effect does cholecystokinin (CCK) have on gastric emptying?
 CASE 28 A 43-year-old woman presents to the emergency department with the acute onset of abdominal pain. Her pain is located to the right upper quadrant (RUQ) and radiates to the right shoulder. She reports
CASE 28 A 43-year-old woman presents to the emergency department with the acute onset of abdominal pain. Her pain is located to the right upper quadrant (RUQ) and radiates to the right shoulder. She reports
For more information about how to cite these materials visit
 Author: John Williams, M.D., Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author: John Williams, M.D., Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Physiology Unit 4 DIGESTIVE PHYSIOLOGY
 Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
Physiology 12. Overview. The Gastrointestinal Tract. Germann Ch 19
 Physiology 12 The Gastrointestinal Tract Germann Ch 19 Overview 1 Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Physiology 12 The Gastrointestinal Tract Germann Ch 19 Overview 1 Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Chapter 20 The Digestive System Exam Study Questions
 Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Bio& 242 Unit 1 / Lecture 4
 Bio& 242 Unit 1 / Lecture 4 system: Gastric hormones GASTRIN: Secretion: By enteroendocrine (G) in gastric pits of the mucosa. Stimulus: Stomach distention and acid ph of chyme causes Gastrin. Action:
Bio& 242 Unit 1 / Lecture 4 system: Gastric hormones GASTRIN: Secretion: By enteroendocrine (G) in gastric pits of the mucosa. Stimulus: Stomach distention and acid ph of chyme causes Gastrin. Action:
Overview. Physiology 1. The Gastrointestinal Tract. Guyton section XI
 Overview Physiology 1 The Gastrointestinal Tract Guyton section XI Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Overview Physiology 1 The Gastrointestinal Tract Guyton section XI Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
The Players. Liver Thyroid Adrenals Pancreas Reproductive System Pituitary Gut Bacteria
 The Players Part I Quick Review Understanding some of the key systems and their relationship to hormones is the best place to start It will help with some of the hormone interconnections Key to understanding
The Players Part I Quick Review Understanding some of the key systems and their relationship to hormones is the best place to start It will help with some of the hormone interconnections Key to understanding
Week 3 The Pancreas: Pancreatic ph buffering:
 Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Chapter 20 The Digestive System Exam Study Questions
 Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, ,
 IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
University of Buea. Faculty of Health Sciences. Programme in Medicine
 Faculty of Health Sciences University of Buea Wednesday, 28 th January 2009 Time: 8 00-10 00 Programme in Medicine MED 303 (Gastrointestinal Physiology) EXAMS (2008-2009) Identify the letter of the choice
Faculty of Health Sciences University of Buea Wednesday, 28 th January 2009 Time: 8 00-10 00 Programme in Medicine MED 303 (Gastrointestinal Physiology) EXAMS (2008-2009) Identify the letter of the choice
INTRODUCTION TO GASTROINTESTINAL FUNCTIONS
 1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
Chapter 12. Ingestive Behavior
 Chapter 12 Ingestive Behavior Drinking a. fluid compartments b. osmometric thirst c. volumetric thirst Eating a. energy sources b. starting a meal c. stopping a meal d. eating disordersd Drinking a. fluid
Chapter 12 Ingestive Behavior Drinking a. fluid compartments b. osmometric thirst c. volumetric thirst Eating a. energy sources b. starting a meal c. stopping a meal d. eating disordersd Drinking a. fluid
Overview of Gastroenterology
 Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Overview of Gastroenterology Gastroenterology Made Really Simple! Food Waste
Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Overview of Gastroenterology Gastroenterology Made Really Simple! Food Waste
The Digestive System. What is the advantage of a one-way gut? If you swallow something, is it really inside you?
 The Digestive System What is the advantage of a one-way gut?! If you swallow something, is it really inside you? Functions and Processes of the Digestive System: Move nutrients, water, electrolytes from
The Digestive System What is the advantage of a one-way gut?! If you swallow something, is it really inside you? Functions and Processes of the Digestive System: Move nutrients, water, electrolytes from
The Small Intestine. The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine.
 The Small Intestine The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine. approximately six metres (the longest section of your digestive
The Small Intestine The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine. approximately six metres (the longest section of your digestive
Includes mouth, pharynx, esophagus, stomach, small intestine, large intestine, rectum, anus. Salivary glands, liver, gallbladder, pancreas
 Chapter 14 The Digestive System and Nutrition Digestive System Brings Nutrients Into the Body The digestive system includes Gastrointestinal (GI) tract (hollow tube) Lumen: space within this tube Includes
Chapter 14 The Digestive System and Nutrition Digestive System Brings Nutrients Into the Body The digestive system includes Gastrointestinal (GI) tract (hollow tube) Lumen: space within this tube Includes
Soft palate elevates, closing off the nasopharynx. Hard palate Tongue Bolus Epiglottis. Glottis Larynx moves up and forward.
 The Cephalic Phase Chemical and mechanical digestion begins in the mouth Saliva is an exocrine secretion Salivary secretion is under autonomic control Softens and lubricates food Chemical digestion: salivary
The Cephalic Phase Chemical and mechanical digestion begins in the mouth Saliva is an exocrine secretion Salivary secretion is under autonomic control Softens and lubricates food Chemical digestion: salivary
Growth Hormone, Somatostatin, and Prolactin 1 & 2 Mohammed Y. Kalimi, Ph.D.
 Growth Hormone, Somatostatin, and Prolactin 1 & 2 Mohammed Y. Kalimi, Ph.D. I. Growth Hormone (somatotropin): Growth hormone (GH) is a 191 amino acid single chain polypeptide (MW 22,000 daltons). Growth
Growth Hormone, Somatostatin, and Prolactin 1 & 2 Mohammed Y. Kalimi, Ph.D. I. Growth Hormone (somatotropin): Growth hormone (GH) is a 191 amino acid single chain polypeptide (MW 22,000 daltons). Growth
ENERGY FROM INGESTED NUTREINTS MAY BE USED IMMEDIATELY OR STORED
 QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM TYPES OF DIGESTIVE SYSTEMS Ingested food may be stored or first subjected to physical fragmentation Chemical digestion occurs next Hydrolysis reactions liberate the subunit molecules
THE DIGESTIVE SYSTEM TYPES OF DIGESTIVE SYSTEMS Ingested food may be stored or first subjected to physical fragmentation Chemical digestion occurs next Hydrolysis reactions liberate the subunit molecules
Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4)
 Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
History of Investigation
 Acini - Pancreatic juice (1º) (2º) Secretions- neuronal and hormonal mechanisms 1) Secretin - bicarbonate rich 2) Cholecystokinin - enzyme rich Islets of Langerhans (contain 4 cell types) Alpha cells (α)-
Acini - Pancreatic juice (1º) (2º) Secretions- neuronal and hormonal mechanisms 1) Secretin - bicarbonate rich 2) Cholecystokinin - enzyme rich Islets of Langerhans (contain 4 cell types) Alpha cells (α)-
Motility Conference Ghrelin
 Motility Conference Ghrelin Emori Bizer, M.D. Division of Gastroenterology/Hepatology November 21, 2007 Ghrelin: Basics Hormone produced by the A-like A endocrine cells in the oxyntic mucosa (stomach body
Motility Conference Ghrelin Emori Bizer, M.D. Division of Gastroenterology/Hepatology November 21, 2007 Ghrelin: Basics Hormone produced by the A-like A endocrine cells in the oxyntic mucosa (stomach body
Nutrition. Autotrophs. plants, some protists & bacteria producers
 Nutrition Autotrophs plants, some protists & bacteria producers Nutrition Heterotrophs animals, fungi, some protists & bacteria consumers Animal Nutrition Most obtain food by ingestion take in their food
Nutrition Autotrophs plants, some protists & bacteria producers Nutrition Heterotrophs animals, fungi, some protists & bacteria consumers Animal Nutrition Most obtain food by ingestion take in their food
Digestive System Module 4: The Stomach *
 OpenStax-CNX module: m49286 1 Digestive System Module 4: The * Donna Browne Based on The by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0
OpenStax-CNX module: m49286 1 Digestive System Module 4: The * Donna Browne Based on The by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0
Gastrointestinal Anatomy and Physiology. Bio 219 Napa Valley College Dr. Adam Ross
 Gastrointestinal Anatomy and Physiology Bio 219 Napa Valley College Dr. Adam Ross Functions of digestive system Digestion Breakdown of food (chemically) using enzymes, acid, and water Absorption Nutrients,
Gastrointestinal Anatomy and Physiology Bio 219 Napa Valley College Dr. Adam Ross Functions of digestive system Digestion Breakdown of food (chemically) using enzymes, acid, and water Absorption Nutrients,
Chapter 15 Gastrointestinal System
 Chapter 15 Gastrointestinal System Dr. LL Wang E-mail: wanglinlin@zju.edu.cn Rm 608, Block B, Research Building, School of Medicine, Zijingang Campus Pancreatic Secretion The exocrine cells in the pancreas
Chapter 15 Gastrointestinal System Dr. LL Wang E-mail: wanglinlin@zju.edu.cn Rm 608, Block B, Research Building, School of Medicine, Zijingang Campus Pancreatic Secretion The exocrine cells in the pancreas
Physiological processes in the GI tract:
 Gastrointestinal physiology for medical students General principal of gastrointestinal function Motility, nervous control and blood circulation Physiological processes in the GI tract: Motility Secretion
Gastrointestinal physiology for medical students General principal of gastrointestinal function Motility, nervous control and blood circulation Physiological processes in the GI tract: Motility Secretion
Digestive Lecture Test Questions Set 4
 Digestive Lecture Test Questions Set 4 1. Which of the following is not associated directly with the small intestine: a. villi b. circular folds c. microvilli d. haustrae e. secretin 2. The largest (longest)
Digestive Lecture Test Questions Set 4 1. Which of the following is not associated directly with the small intestine: a. villi b. circular folds c. microvilli d. haustrae e. secretin 2. The largest (longest)
18. PANCREATIC FUNCTION AND METABOLISM. Pancreatic secretions ISLETS OF LANGERHANS. Insulin
 18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
Gut hormones KHATTAB
 Gut hormones PROF:ABD ALHAFIZ HASSAN KHATTAB Gut as an endocrine gland The talk will cover the following : Historical background. Why this subject is chosen. Gastro-intestinal hormones and their function.
Gut hormones PROF:ABD ALHAFIZ HASSAN KHATTAB Gut as an endocrine gland The talk will cover the following : Historical background. Why this subject is chosen. Gastro-intestinal hormones and their function.
10/27/2016. Processing in the Large Intestine. The colon of the large intestine is connected to the small intestine
 The hepatic portal vein carries nutrient-rich blood from the capillaries of the villi to the liver, then to the heart The liver regulates nutrient distribution, interconverts many organic molecules, and
The hepatic portal vein carries nutrient-rich blood from the capillaries of the villi to the liver, then to the heart The liver regulates nutrient distribution, interconverts many organic molecules, and
AN ANIMAL S DIET MUST SUPPLY CHEMICAL ENERGY, ORGANIC MOLECULES, AND ESSENTIAL NUTRIENTS
 1 ANIMAL NUTRITION 2 3 4 5 6 7 Food is taken in, taken apart, and taken up in the process of animal nutrition In general, animals fall into three categories: Herbivores eat mainly plants and algae Carnivores
1 ANIMAL NUTRITION 2 3 4 5 6 7 Food is taken in, taken apart, and taken up in the process of animal nutrition In general, animals fall into three categories: Herbivores eat mainly plants and algae Carnivores
e. Undigested material is compacted and stored until the colon is full. When the colon is full, a signal to empty it is sent by sensors in the walls
 Digestive System 1. General a. Animals obtain energy by breaking food molecules into smaller pieces. b. The basic fuel molecules are amino acids, lipids and sugars c. Digestion is the chemical breakdown
Digestive System 1. General a. Animals obtain energy by breaking food molecules into smaller pieces. b. The basic fuel molecules are amino acids, lipids and sugars c. Digestion is the chemical breakdown
DIGESTIVE. CHAPTER 17 Lecture: Part 1 Part 2 BIO 212: ANATOMY & PHYSIOLOGY II
 BIO 212: ANATOMY & PHYSIOLOGY II CHAPTER 17 Lecture: DIGESTIVE Part 1 Part 2 Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. SMALL INTESTINE DUODENUM > JEJUNUM
BIO 212: ANATOMY & PHYSIOLOGY II CHAPTER 17 Lecture: DIGESTIVE Part 1 Part 2 Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. SMALL INTESTINE DUODENUM > JEJUNUM
Peptic Ulcer Disease: Zollinger-Ellison Syndrome
 GASTROINTESTINAL PHYSIOLOGY 235 Case 41 Peptic Ulcer Disease: Zollinger-Ellison Syndrome Abe Rosenfeld, who is 47 years old, owns a house painting business with his brothers. The brothers pride themselves
GASTROINTESTINAL PHYSIOLOGY 235 Case 41 Peptic Ulcer Disease: Zollinger-Ellison Syndrome Abe Rosenfeld, who is 47 years old, owns a house painting business with his brothers. The brothers pride themselves
Introduction to Human Anatomy & Physiology Chapter 35
 Biology Introduction to Human Anatomy & Physiology Chapter 35 Digestion The breakdown of complex biological molecules into their component parts. Lipids to fatty acids Proteins to individual amino acids
Biology Introduction to Human Anatomy & Physiology Chapter 35 Digestion The breakdown of complex biological molecules into their component parts. Lipids to fatty acids Proteins to individual amino acids
PHYSIOLOGY OF THE DIGESTIVE SYSTEM
 Student Name CHAPTER 26 PHYSIOLOGY OF THE DIGESTIVE SYSTEM D igestion is the process of breaking down complex nutrients into simpler units suitable for absorption. It involves two major processes: mechanical
Student Name CHAPTER 26 PHYSIOLOGY OF THE DIGESTIVE SYSTEM D igestion is the process of breaking down complex nutrients into simpler units suitable for absorption. It involves two major processes: mechanical
The gallbladder. Bile secretion:
 The gallbladder is a thin walled green muscular sac on the inferior surface of the liver. The gallbladder stores bile that is not immediately needed for digestion and concentrates it. When the muscular
The gallbladder is a thin walled green muscular sac on the inferior surface of the liver. The gallbladder stores bile that is not immediately needed for digestion and concentrates it. When the muscular
Overview of digestion or, gut reactions - to food
 Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions - to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology e-mail: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions - to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology e-mail: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
1-It is to prevent back flow of fecal content from colon into small intestine.
 Function of the ileocecal valve: 1-It is to prevent back flow of fecal content from colon into small intestine. 2-The wall of the ileum for several centimeters preceding valve has a thickened muscular
Function of the ileocecal valve: 1-It is to prevent back flow of fecal content from colon into small intestine. 2-The wall of the ileum for several centimeters preceding valve has a thickened muscular
All organisms must obtain and process essential nutrients (food) *** Exception: Venus Fly Traps undergo photosynthesis but needs source of nitrogen
 All organisms must obtain and process essential nutrients (food) AUTOTROPHS self feeder makes their own food eg. Plants do not require a digestive tract *** Exception: Venus Fly Traps undergo photosynthesis
All organisms must obtain and process essential nutrients (food) AUTOTROPHS self feeder makes their own food eg. Plants do not require a digestive tract *** Exception: Venus Fly Traps undergo photosynthesis
Summary break down long chain proteins, polysaccharides and nucleic acids into monomers recall hydrolysis (opposite of dehydration synthesis) (hydro-w
 Summary break down long chain proteins, polysaccharides and nucleic acids into monomers recall hydrolysis (opposite of dehydration synthesis) (hydro-water lysis-break apart) if not broken down, proteins
Summary break down long chain proteins, polysaccharides and nucleic acids into monomers recall hydrolysis (opposite of dehydration synthesis) (hydro-water lysis-break apart) if not broken down, proteins
Objectives. Define satiety and satiation Summarize the satiety cascade Describe potential dietary interventions aimed at improving satiety
 Foods that Fill Monica Esquivel PhD RDN Assistant Professor, Dietetics Program Director Department of Human Nutrition, Food and Animal Sciences November 8, 2017 Objectives Define satiety and satiation
Foods that Fill Monica Esquivel PhD RDN Assistant Professor, Dietetics Program Director Department of Human Nutrition, Food and Animal Sciences November 8, 2017 Objectives Define satiety and satiation
Paneth Cells. Road Map to the Finish. No Review this Friday. Today 11/29 Finish digestion/accessory organs. Wednesday 12/1 Immune System I
 Road Map to the Finish No Review this Friday Today 11/29 Finish digestion/accessory organs Wednesday 12/1 Immune System I Paneth Cells - base of intestinal glands -! large -! intense acidophilic granules
Road Map to the Finish No Review this Friday Today 11/29 Finish digestion/accessory organs Wednesday 12/1 Immune System I Paneth Cells - base of intestinal glands -! large -! intense acidophilic granules
Overview of digestion or, gut reactions - to food
 1 Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology email: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
1 Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology email: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
Ali Yaghi. Yaseen Fatayer. M.Khatatbeh
 6 Ali Yaghi Yaseen Fatayer M.Khatatbeh P a g e 1 pancreatic secretions note: The pancreas has endocrine (secretions are released toward the blood) and exocrine(secretions are released through the canalicular
6 Ali Yaghi Yaseen Fatayer M.Khatatbeh P a g e 1 pancreatic secretions note: The pancreas has endocrine (secretions are released toward the blood) and exocrine(secretions are released through the canalicular
Hormones. Prof. Dr. Volker Haucke Institut für Chemie-Biochemie Takustrasse 6
 Hormones Prof. Dr. Volker Haucke Institut für Chemie-Biochemie Takustrasse 6 Tel. 030-8385-6920 (Sekret.) 030-8385-6922 (direkt) e-mail: vhaucke@chemie.fu-berlin.de http://userpage.chemie.fu-berlin.de/biochemie/aghaucke/teaching.html
Hormones Prof. Dr. Volker Haucke Institut für Chemie-Biochemie Takustrasse 6 Tel. 030-8385-6920 (Sekret.) 030-8385-6922 (direkt) e-mail: vhaucke@chemie.fu-berlin.de http://userpage.chemie.fu-berlin.de/biochemie/aghaucke/teaching.html
Types of Digestive Systems. Types of Digestive Systems. Types of Digestive Systems. Types of Digestive Systems. The Digestive System
 The Digestive System Chapter 48 Types of Digestive Systems Heterotrophs are divided into three groups based on their food sources -Herbivores are animals that eat plants exclusively -Carnivores are animals
The Digestive System Chapter 48 Types of Digestive Systems Heterotrophs are divided into three groups based on their food sources -Herbivores are animals that eat plants exclusively -Carnivores are animals
Lipid Digestion. An Introduction to Lipid Transport and Digestion with consideration of High Density and Low Density Lipoproteins.
 Digestion An Introduction to Transport and Digestion with consideration of High Density and Low Density Lipoproteins By Noel Ways Suspension and Nutralization of Chyme ph Boli containing lipids enters
Digestion An Introduction to Transport and Digestion with consideration of High Density and Low Density Lipoproteins By Noel Ways Suspension and Nutralization of Chyme ph Boli containing lipids enters
NOTES: The Digestive System (Ch 14, part 2)
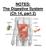 NOTES: The Digestive System (Ch 14, part 2) PANCREAS Structure of the pancreas: The pancreas produces PANCREATIC JUICE that is then secreted into a pancreatic duct. The PANCREATIC DUCT leads to the The
NOTES: The Digestive System (Ch 14, part 2) PANCREAS Structure of the pancreas: The pancreas produces PANCREATIC JUICE that is then secreted into a pancreatic duct. The PANCREATIC DUCT leads to the The
Digestion: Endocrinology of Appetite
 Digestion: Endocrinology of Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one on one relationship with a qualified health care professional
Digestion: Endocrinology of Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one on one relationship with a qualified health care professional
Figure Nutrition: omnivore, herbivore, carnivore
 Figure 41.1 Nutrition: omnivore, herbivore, carnivore Essential Nutrients: Amino acids Fatty acids Vitamins Minerals Figure 41.2 Complete vs incomplete Omnivore vs herbivore (vegetarian) Table 41.1 Table
Figure 41.1 Nutrition: omnivore, herbivore, carnivore Essential Nutrients: Amino acids Fatty acids Vitamins Minerals Figure 41.2 Complete vs incomplete Omnivore vs herbivore (vegetarian) Table 41.1 Table
GI Secretion 1: Salivary and Gastric Secretion Jack Grider, Ph.D.
 GI Secretion 1: Salivary and Gastric Secretion Jack Grider, Ph.D. OBJECTIVES: 1. List the volumes of secretion by various regions. 2. Predict the components of salivary secretion at different flow rates.
GI Secretion 1: Salivary and Gastric Secretion Jack Grider, Ph.D. OBJECTIVES: 1. List the volumes of secretion by various regions. 2. Predict the components of salivary secretion at different flow rates.
10/23/2013 ANIMAL NUTRITION ANIMAL NUTRITION ESSENTIAL NUTRIENTS AN ANIMAL S DIET MUST STUPPLY: AMINO ACIDS
 ANIMAL NUTRITION Food is taken in, taken apart, and taken up in the process of animal nutrition In general, animals fall into three categories: Herbivores Carnivores Omnivores ANIMAL NUTRITION Chapter
ANIMAL NUTRITION Food is taken in, taken apart, and taken up in the process of animal nutrition In general, animals fall into three categories: Herbivores Carnivores Omnivores ANIMAL NUTRITION Chapter
Topic 6: Human Physiology
 Topic 6: Human Physiology 6.1 Digestion and Absorption D.1 Human Nutrition D.2 Digestion Essential Understandings: The structure of the digestive system allows it to move, digest, and absorb food. A balanced
Topic 6: Human Physiology 6.1 Digestion and Absorption D.1 Human Nutrition D.2 Digestion Essential Understandings: The structure of the digestive system allows it to move, digest, and absorb food. A balanced
The Intricate Web Of Hormone Relationships Dr. Ritamarie Loscalzo
 The Intricate Web Of Hormone Relationships Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one-onone relationship with a qualified health care
The Intricate Web Of Hormone Relationships Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one-onone relationship with a qualified health care
Our gut reactions to food or, gut reactions - to food
 Key concepts in Digestion. Our gut reactions to food or, gut reactions to food Prof. Barry Campbell Cellular & Molecular Physiology email: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl Swallowing
Key concepts in Digestion. Our gut reactions to food or, gut reactions to food Prof. Barry Campbell Cellular & Molecular Physiology email: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl Swallowing
Chapter 26 The Digestive System
 Chapter 26 The Digestive System Digestive System Gastroenterology is the study of the stomach and intestine. Digestion Catabolism Absorption Anabolism The actions of the digestive system are controlled
Chapter 26 The Digestive System Digestive System Gastroenterology is the study of the stomach and intestine. Digestion Catabolism Absorption Anabolism The actions of the digestive system are controlled
Sphincters heartburn diaphragm The Stomach gastric glands pepsin, chyme The Small Intestine 1-Digestion Is Completed in the Small Intestine duodenum
 Sphincters are muscles that encircle tubes and act as valves. The tubes close when the sphincters contract and they open when the sphincters relax. When food or saliva is swallowed, the sphincter relaxes
Sphincters are muscles that encircle tubes and act as valves. The tubes close when the sphincters contract and they open when the sphincters relax. When food or saliva is swallowed, the sphincter relaxes
Digestive System. Part A Multiple Choice. 1. Which of the following is NOT a digestive enzyme? A. Pepsin. B. Ptyalin. C. Gastrin. D. Trypsin.
 Digestive System Part A Multiple Choice 1. Which of the following is NOT a digestive enzyme? A. Pepsin. B. Ptyalin. C. Gastrin. D. Trypsin. 2. The presence of large numbers of mitochondria in the cells
Digestive System Part A Multiple Choice 1. Which of the following is NOT a digestive enzyme? A. Pepsin. B. Ptyalin. C. Gastrin. D. Trypsin. 2. The presence of large numbers of mitochondria in the cells
Animal Nutrition Variations, Adaptations & Regulation
 Animal Nutrition Variations, Adaptations & Regulation This obese mouse (L) has defect in gene which normally produces leptin, an appetite-regulating protein. Many herbivores have diets deficient in mineral
Animal Nutrition Variations, Adaptations & Regulation This obese mouse (L) has defect in gene which normally produces leptin, an appetite-regulating protein. Many herbivores have diets deficient in mineral
1) Four main feeding mechanisms of animals a) Suspension feeders i) (1) Humpback whales b) Substrate feeders i)
 1 AP Biology March 2008 Digestion Chapter 41 Homeostatic mechanisms manage an animal s energy budget. 1) Four main feeding mechanisms of animals Suspension feeders (1) Humpback whales Substrate feeders
1 AP Biology March 2008 Digestion Chapter 41 Homeostatic mechanisms manage an animal s energy budget. 1) Four main feeding mechanisms of animals Suspension feeders (1) Humpback whales Substrate feeders
INTRODUCTION TO THE BIOCHEMISTRY OF HORMONES AND THEIR RECPTORS
 INTRODUCTION TO THE BIOCHEMISTRY OF HORMONES AND THEIR RECPTORS 1 Introduction to the Biochemistry of Hormones and their Receptors Lectuctre1 Sunday 17/2/ Objectives: 1. To understand the biochemical nature
INTRODUCTION TO THE BIOCHEMISTRY OF HORMONES AND THEIR RECPTORS 1 Introduction to the Biochemistry of Hormones and their Receptors Lectuctre1 Sunday 17/2/ Objectives: 1. To understand the biochemical nature
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
Chapter 14: The Digestive System
 Chapter 14: The Digestive System Digestive system consists of Muscular tube (digestive tract) alimentary canal Accessory organs teeth, tongue, glandular organs 6 essential activities 1. 2. 3. 4. 5. 6.
Chapter 14: The Digestive System Digestive system consists of Muscular tube (digestive tract) alimentary canal Accessory organs teeth, tongue, glandular organs 6 essential activities 1. 2. 3. 4. 5. 6.
What systems are involved in homeostatic regulation (give an example)?
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
Overview of digestion
 Key concepts in Digestion. Overview of digestion introduction to the GI system Prof. Barry Campbell Cellular & Molecular Physiology e-mail: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl DIGESTION
Key concepts in Digestion. Overview of digestion introduction to the GI system Prof. Barry Campbell Cellular & Molecular Physiology e-mail: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl DIGESTION
PANCREATIC BETA CELLS PRODUCE AND SECRETE
 15 March, 2018 PANCREATIC BETA CELLS PRODUCE AND SECRETE Document Filetype: PDF 374.06 KB 0 PANCREATIC BETA CELLS PRODUCE AND SECRETE Among the oldest and cheapest drugs for diabetes are the drugs that
15 March, 2018 PANCREATIC BETA CELLS PRODUCE AND SECRETE Document Filetype: PDF 374.06 KB 0 PANCREATIC BETA CELLS PRODUCE AND SECRETE Among the oldest and cheapest drugs for diabetes are the drugs that
Gastrointestinal Physiology
 Gastrointestinal Physiology Digestion and Absorption Definition Digestion: i Food dis dissolved d and broken down. Physical digestion: Propulsion and mixing of food by muscle in the alimentary tract. Chemical
Gastrointestinal Physiology Digestion and Absorption Definition Digestion: i Food dis dissolved d and broken down. Physical digestion: Propulsion and mixing of food by muscle in the alimentary tract. Chemical
The Stomach. Bởi: OpenStaxCollege
 Bởi: OpenStaxCollege Although a minimal amount of carbohydrate digestion occurs in the mouth, chemical digestion really gets underway in the stomach. An expansion of the alimentary canal that lies immediately
Bởi: OpenStaxCollege Although a minimal amount of carbohydrate digestion occurs in the mouth, chemical digestion really gets underway in the stomach. An expansion of the alimentary canal that lies immediately
Digestive System. What happens to the donut you ate for breakfast this morning?
 Digestive System What happens to the donut you ate for breakfast this morning? Free Tutoring and Extra Credit!!! Digestive System: Is the basic process of breaking down the food you eat into individual
Digestive System What happens to the donut you ate for breakfast this morning? Free Tutoring and Extra Credit!!! Digestive System: Is the basic process of breaking down the food you eat into individual
Scope. History. History. Incretins. Incretin-based Therapy and DPP-4 Inhibitors
 Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
Gastrointestinal Physiology. Secretion
 Gastrointestinal Physiology Secretion Fig. 24.26 Functions Provided by secretory glands which serve 2 functions: - Digestive enzymes. - Lubrication and protection of the mucosa. Types of secretory structures
Gastrointestinal Physiology Secretion Fig. 24.26 Functions Provided by secretory glands which serve 2 functions: - Digestive enzymes. - Lubrication and protection of the mucosa. Types of secretory structures
Digestive System Module 6: Accessory Organs in Digestion: The Liver, Pancreas, and Gallbladder
 Connexions module: m49293 1 Digestive System Module 6: Accessory Organs in Digestion: The Liver, Pancreas, and Gallbladder Donna Browne Based on Accessory Organs in Digestion: The Liver, Pancreas, and
Connexions module: m49293 1 Digestive System Module 6: Accessory Organs in Digestion: The Liver, Pancreas, and Gallbladder Donna Browne Based on Accessory Organs in Digestion: The Liver, Pancreas, and
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM
 ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM The digestive system also known as the alimentary canal or gastrointestinal tract consists of a series of hollow organs joined in a
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM The digestive system also known as the alimentary canal or gastrointestinal tract consists of a series of hollow organs joined in a
(*) (*) Ingestion, digestion, absorption, and elimination. Uptake of nutrients by body cells (intestine)
 Human Digestive System Food is pushed along the digestive tract by peristalsis the rhythmic waves of contraction of smooth muscles in the wall of the canal Accessory glands. Main stages of food processing
Human Digestive System Food is pushed along the digestive tract by peristalsis the rhythmic waves of contraction of smooth muscles in the wall of the canal Accessory glands. Main stages of food processing
Control of Glucose Metabolism
 Glucose Metabolism Control of Glucose Metabolism The pancreas is both an exocrine and endocrine gland. It secretes digestive enzymes into the duodenum (exocrine) and 3 specific hormones into the bloodstream
Glucose Metabolism Control of Glucose Metabolism The pancreas is both an exocrine and endocrine gland. It secretes digestive enzymes into the duodenum (exocrine) and 3 specific hormones into the bloodstream
(b) Stomach s function 1. Dilution of food materials 2. Acidification of food (absorption of dietary Fe in small intestine) 3. Partial chemical digest
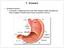 (1) General features a) Stomach is widened portion of gut-tube: between tubular and spherical; Note arranged of smooth muscle tissue in muscularis externa. 1 (b) Stomach s function 1. Dilution of food
(1) General features a) Stomach is widened portion of gut-tube: between tubular and spherical; Note arranged of smooth muscle tissue in muscularis externa. 1 (b) Stomach s function 1. Dilution of food
Causes of pancreatic insufficiency. Eugen Dumitru
 Causes of pancreatic insufficiency Eugen Dumitru Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes 3. The Consequences Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes
Causes of pancreatic insufficiency Eugen Dumitru Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes 3. The Consequences Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes
ORGANS OF THE DIGESTIVE SYSTEM
 ORGANS OF THE DIGESTIVE SYSTEM OBJECTIVES: 1. List and describe the major activities of the digestive system. 2. Identify and give the functions of the organs in and along the digestive tract. MAJOR ACTIVITIES
ORGANS OF THE DIGESTIVE SYSTEM OBJECTIVES: 1. List and describe the major activities of the digestive system. 2. Identify and give the functions of the organs in and along the digestive tract. MAJOR ACTIVITIES
Asma Karameh. -Shatha Al-Jaberi محمد خطاطبة -
 -2 Asma Karameh -Shatha Al-Jaberi محمد خطاطبة - 1 P a g e Gastrointestinal motilities Chewing: once you introduce the first bolus to the mouth you started what we call chewing reflex appears by muscle
-2 Asma Karameh -Shatha Al-Jaberi محمد خطاطبة - 1 P a g e Gastrointestinal motilities Chewing: once you introduce the first bolus to the mouth you started what we call chewing reflex appears by muscle
Ch41 Animal Nutrition
 Ch41 Animal Nutrition Digestive system Purpose = break down food into smaller nutrients to be used in the body for energy and raw materials for biosynthesis Overview of food processing Ingestion: act of
Ch41 Animal Nutrition Digestive system Purpose = break down food into smaller nutrients to be used in the body for energy and raw materials for biosynthesis Overview of food processing Ingestion: act of
Human Anatomy, First Edition. Endocrine System. Chapter 20 Lecture Outline: Endocrine System. McKinley & O'Loughlin
 Human Anatomy, First Edition McKinley & O'Loughlin Chapter 20 Lecture Outline: Endocrine System 1 Endocrine System Endocrine system and the nervous system often work together to bring about homeostasis.
Human Anatomy, First Edition McKinley & O'Loughlin Chapter 20 Lecture Outline: Endocrine System 1 Endocrine System Endocrine system and the nervous system often work together to bring about homeostasis.
HUMAN NUTRITION 08 MAY 2013
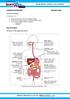 HUMAN NUTRITION 08 MAY 2013 Lesson Description In this lesson, we: Study the structure of the human digestive system Look at the processes used in the human digestive system Look at the two different types
HUMAN NUTRITION 08 MAY 2013 Lesson Description In this lesson, we: Study the structure of the human digestive system Look at the processes used in the human digestive system Look at the two different types
The Digestive System
 The Digestive System s Big Book of Handouts Digestion and nutrition Specific Learning outcomes B11-2-01: Identify major structures and functions of the human digestive system from a diagram, model, or
The Digestive System s Big Book of Handouts Digestion and nutrition Specific Learning outcomes B11-2-01: Identify major structures and functions of the human digestive system from a diagram, model, or
Digestive System. Digestive System. Digestion is the process of reducing food to small molecules that can be absorbed into the body.
 Digestive System Digestion is the process of reducing food to small molecules that can be absorbed into the body. 2 Types of Digestion Mechanical digestion physical breakdown of food into small particles
Digestive System Digestion is the process of reducing food to small molecules that can be absorbed into the body. 2 Types of Digestion Mechanical digestion physical breakdown of food into small particles
Ch 7 Nutrition in humans
 Ch 7 Nutrition in humans Think about (Ch 7, p.2) 1. The stomach churns food into smaller pieces physically. The stomach wall secretes proteases to chemically digest proteins. It also releases hydrochloric
Ch 7 Nutrition in humans Think about (Ch 7, p.2) 1. The stomach churns food into smaller pieces physically. The stomach wall secretes proteases to chemically digest proteins. It also releases hydrochloric
BIO 132 Anatomy and Physiology II Spring, 2016 Exam 1 Name: BIO 132 ID Number. Section 1 Answer questions 1 40 on the scan sheet.
 BIO 132 Anatomy and Physiology II Spring, 2016 Exam 1 Name: BIO 132 ID Number Section 1 Answer questions 1 40 on the scan sheet. 1. The homeostatic value of a particular controlled variable in the body
BIO 132 Anatomy and Physiology II Spring, 2016 Exam 1 Name: BIO 132 ID Number Section 1 Answer questions 1 40 on the scan sheet. 1. The homeostatic value of a particular controlled variable in the body
Digestive System 7/15/2015. Outline Digestive System. Digestive System
 Digestive System Biology 105 Lecture 18 Chapter 15 Outline Digestive System I. Functions II. Layers of the GI tract III. Major parts: mouth, pharynx, esophagus, stomach, small intestine, large intestine,
Digestive System Biology 105 Lecture 18 Chapter 15 Outline Digestive System I. Functions II. Layers of the GI tract III. Major parts: mouth, pharynx, esophagus, stomach, small intestine, large intestine,
LESSON 3.3 WORKBOOK. How do we decide when and how much to eat?
 Appetite The psychological desire to eat, driven by feelings of pleasure from the brain. Hunger The biological or physiological need to eat, caused by a release of hormones from the digestive tract. LESSON
Appetite The psychological desire to eat, driven by feelings of pleasure from the brain. Hunger The biological or physiological need to eat, caused by a release of hormones from the digestive tract. LESSON
ENDOCRINOLOGY. Dr.AZZA SAJID ALKINANY 2 nd STAGE
 ENDOCRINOLOGY Dr.AZZA SAJID ALKINANY 2 nd STAGE THE RELATIONSHIP AMONG THE HYPOTHALMUS,POSTERIOR PITUITARY AND TARGET TISSUES. The posterior pituitary does not produce its own hormones, but stores and
ENDOCRINOLOGY Dr.AZZA SAJID ALKINANY 2 nd STAGE THE RELATIONSHIP AMONG THE HYPOTHALMUS,POSTERIOR PITUITARY AND TARGET TISSUES. The posterior pituitary does not produce its own hormones, but stores and
The physiology of gastrointestinal system 3.
 The physiology of gastrointestinal system 3. Stomach, pancreas, bile Dr. Gabriella Kékesi The mechanism and regulation of gastric juice secretion (Lo.) 64. Secretory cells in stomach Composition and role
The physiology of gastrointestinal system 3. Stomach, pancreas, bile Dr. Gabriella Kékesi The mechanism and regulation of gastric juice secretion (Lo.) 64. Secretory cells in stomach Composition and role
KRISHNA TEJA PHARMACY COLLEGE HUMAN ANATOMY AND PHYSIOLOGY. DIGESTIVE SYSTEM Dr.B.Jyothi
 KRISHNA TEJA PHARMACY COLLEGE HUMAN ANATOMY AND PHYSIOLOGY DIGESTIVE SYSTEM Dr.B.Jyothi Prof, Dept. Of Pharmacology KTPC The Digestive System Food undergoes six major processes: 1. Ingestion : process
KRISHNA TEJA PHARMACY COLLEGE HUMAN ANATOMY AND PHYSIOLOGY DIGESTIVE SYSTEM Dr.B.Jyothi Prof, Dept. Of Pharmacology KTPC The Digestive System Food undergoes six major processes: 1. Ingestion : process
Chapter 20 Endocrine System
 Chapter 20 Endocrine System The endocrine system consists of glands and tissues that secrete Hormones are chemicals that affect other glands or tissues, many times far away from the site of hormone production
Chapter 20 Endocrine System The endocrine system consists of glands and tissues that secrete Hormones are chemicals that affect other glands or tissues, many times far away from the site of hormone production
Hypothalamic & Pituitary Hormones
 1 Hypothalamic & Pituitary Hormones Pharmacologic Applications: Drugs that mimic or block the effects of hypothalamic or pituitary hormones have the following applications: 1. Replacement therapy for hormone
1 Hypothalamic & Pituitary Hormones Pharmacologic Applications: Drugs that mimic or block the effects of hypothalamic or pituitary hormones have the following applications: 1. Replacement therapy for hormone
Chapter 3 Reading Guide Be sure to use the many figures and tables provided by the book to help answer these questions.
 Chapter 3 Reading Guide Be sure to use the many figures and tables provided by the book to help answer these questions. 1. What is digestion? What is the difference between mechanical and enzymatic digestion?
Chapter 3 Reading Guide Be sure to use the many figures and tables provided by the book to help answer these questions. 1. What is digestion? What is the difference between mechanical and enzymatic digestion?
Megan Lawless. Journal Club. January 20 th, 2011
 Megan Lawless Journal Club January 20 th, 2011 Gut-expressed gustducin and taste receptors regulate secretion of glucagon-like peptide-1 Proceedings of the National Academy of Sciences September 2007 Abstract
Megan Lawless Journal Club January 20 th, 2011 Gut-expressed gustducin and taste receptors regulate secretion of glucagon-like peptide-1 Proceedings of the National Academy of Sciences September 2007 Abstract
