The Effects of a GLP-1 Analog on Glucose Homeostasis in Type 2 Diabetes Mellitus Quantified by an Integrated Glucose Insulin Model
|
|
|
- Janice Cole
- 5 years ago
- Views:
Transcription
1 Citation: CPT Pharmacometrics Syst. Pharmacol. (2015) 4, 28 36; doi: /psp4.11 VC 2014 ASCPT All rights reserved ORIGINAL ARTICLE The Effects of a GLP-1 Analog on Glucose Homeostasis in Type 2 Diabetes Mellitus Quantified by an Integrated Glucose Insulin Model RM Røge 1,2 *, S Klim 1, SH Ingwersen 1, MC Kjellsson 2 and NR Kristensen 1 In recent years, several glucagon-like peptide-1 (GLP-1)-based therapies for the treatment of type 2 diabetes mellitus (T2DM) have been developed. The aim of this work was to extend the semimechanistic integrated glucose-insulin model to include the effects of a GLP-1 analog on glucose homeostasis in T2DM patients. Data from two trials comparing the effect of steady-state liraglutide vs. placebo on the responses of postprandial glucose and insulin in T2DM patients were used for model development. The effect of liraglutide was incorporated in the model by including a stimulatory effect on insulin secretion. Furthermore, for one of the trials an inhibitory effect on glucose absorption was included to account for a delay in gastric emptying. As other GLP-1 receptor agonists have similar modes of action, it is believed that the model can also be used to describe the effect of other receptor agonists on glucose homeostasis. CPT Pharmacometrics Syst. Pharmacol. (2015) 4, 28 36; doi: /psp4.11; published online on 30 December The incretin hormone glucagon-like peptide-1 (GLP-1), which is secreted from the small intestine following food intake, is a potent glucose-lowering agent. The glucoregulatory effects of GLP-1 are facilitated through enhanced glucose-stimulated insulin secretion, slowed gastric emptying, glucose-dependent inhibition of glucagon secretion, and improved b-cell function. 1 As the insulinotropic effect of GLP-1 is preserved in type 2 diabetes mellitus (T2DM), it has created considerable interest as an agent for the treatment of T2DM. However, since endogenous GLP-1 is rapidly degraded by the enzyme dipeptidyl peptidase-4 (DPP-4), resulting in a short half-life in humans (2 minutes) after intravenous (IV) administration, 2 the therapeutic use of endogenous GLP-1 is limited. Instead, several derivatives with a longer duration of action have been developed. 3,4 Liraglutide is a GLP-1 analog that shares 97% amino acid sequence identity with native GLP-1. 5 The analog is obtained by creating two modifications to native GLP-1: the replacement of lysine with arginine at position 34 and the attachment of a C16 fatty acid chain via a g-glutamic acid spacer to lysine at position The fatty acid chain contributes to delaying absorption and extending the plasma half-life by increased binding to plasma albumin, while the lysine replacement makes DPP-4 unable to exert its action. Clinical trials have shown that liraglutide significantly reduces fasting plasma glucose and HbA1c and does so with a low risk of hypoglycemia in T2DM. 6 The aim of this work was to evaluate the effects of a GLP-1 analog on glucose homeostasis in T2DM patients by use of the previously developed integrated glucose-insulin (IGI) model 7 10 following appropriate modification. The model was developed to describe the glucose homeostasis in nondiabetic subjects and T2DM patients during different glucose provocations, including intravenous glucose tolerance tests (IVGTTs), oral glucose tolerance tests (OGTTs), and meal tolerance tests (MTTs) The model has also been used to describe glucose homeostasis in T2DM patients treated with different antidiabetic drugs, such as a glucokinase activator 11 and an insulin analog. 12 By including drug effects in the model, it becomes a useful tool in drug development, as it may aid the selection of dosing regimen for phase II trials. 13 Thus, by extending the model with a component for liraglutide, as an example of a GLP-1 analog, it becomes useful in investigating new analogs and their effects on glucose homeostasis. RESULTS A total of 29 T2DM patients, from two trials (referred to as trial 1 and trial 2 throughout the article), were included in the pharmacokinetic-pharmacodynamic (PK-PD) analysis and detailed descriptions of the two trials are available in Flint et al. 14 and Hermansen et al. 15 PK measurements of liraglutide were available from both studies, with sparse sampling in trial 1 (4 samples per subject at each dose level) and frequent sampling in trial 2 (12 samples per subject at the highest dose level). The PD measurements, i.e., plasma glucose and serum insulin, measuring glucose homeostasis effects, as well as paracetamol, measuring gastric emptying effects, were sampled for 5 hours in trial 1 and 8 hours in trial 2 after MTTs in the presence of placebo or study drug. Treatment duration was 3 weeks in both trials. The liraglutide/placebo dose was escalated weekly in 0.6 mg increments from 0.6 mg until a daily dose of 1.8 mg was reached. In trial 1 MTTs were performed at each dose level, whereas in trial 2 MTTs were only performed at the highest dose level. In both trials standardized meals were served. In trial 2, a high-fat meal with a caloric density of 4 MJ was served, and in trial 1 the caloric density of the meal was 2 MJ. 1 Novo Nordisk A/S, Søborg, Denmark; 2 Department of Pharmaceutical Biosciences, Uppsala University, Uppsala, Sweden. *Correspondence: RM Røge (rmrg@novonordisk.com) Received 8 September 2014; accepted 4 November 2014; published online on 30 December doi: /psp4.11
2 Effects of a GLP-1 Analog on Glucose 29 pooled, and in trial 1 there are only four samples per subject which are all near C max. If data from trial 1 are omitted, no plateau is seen. Figure 1 Schematic presentation of the integrated model including glucose, insulin, and liraglutide. Full arrows indicate flows and broken arrows indicate control mechanisms. G C and G P, central and peripheral compartments for glucose; G E2, glucose effect compartment for control of insulin secretion; G A and G T, absorption (G A ) and transit (G T ) compartment for glucose absorption; I, compartment for insulin distribution; I E, insulin effect compartment for control of glucose elimination; Q, CL G, and CL GI, clearance parameters for glucose; k a, rate constant for glucose absorption; D, glucose dose; CL I, endogenous insulin clearance; k GE2, and k IE, rate constants for the delay of effect compartment concentrations; L C, compartment for liraglutide distribution; L A, depot compartment for liraglutide absorption; k al, rate constant for liraglutide absorption; CL L, liraglutide clearance. The final model is illustrated in Figure 1 and parameter estimates are given in Table 1. The model development was performed in a stepwise manner, investigating the PK of liraglutide first. For the PD model development, the PK model of liraglutide was kept fixed. Pharmacokinetics of liraglutide The PK was described by a one-compartment model with first-order absorption and first-order elimination parameterized as absorption rate constant (k al ), clearance (CL L /F), and volume of distribution (V L /F) and with between-subject variability parameters on clearance and volume. 16 Another PK model for liraglutide was also tested. 17 In this model liraglutide absorption is described by a dose-proportional zero-order process and a subsequent first-order process. However, this model did not improve the model fit judged by assessment of individual profiles, objective function value, and goodness of fit plots. Thus, it was decided to keep the simpler model with first-order absorption. In the final model clearance and volume of distribution were assumed to be proportional to weight. 17 The final parameter estimates are given in Table 1. A bootstrap with 100 samples was performed to compare the standard errors (SEs) from the bootstrap with those estimated by NON- MEM. The agreement between the SE estimates was good (Table 1). The PK model was able to describe the data well, as seen in the left panel of Figure 2, and showed reasonable predictive performance, as illustrated in a visual predictive check (VPC) in the right panel of Figure 2. The VPC, which is based on 1,000 simulations, shows that the main trend of the data is well captured by the model. However, the variability appears to be overestimated. In the figures it appears as though there is a plateau near the C max. This plateau appears because data from the two trials are Pharmacodynamics of glucose and insulin As liraglutide is known to stimulate insulin secretion in a glucose-dependent manner, the expression for insulin secretion in the IGI model was altered. In the IGI model the insulin secretion (I sec ) is governed by the product of three contributions: the basal production, the glucose stimulated production, and the endogenous incretin effect (model equations are provided in the Supplementary Material). The effect of liraglutide was incorporated by multiplying I sec with a stimulatory function F(C lira ), where C lira is the concentration of liraglutide. The function had to satisfy the conditions that F(C lira )51 for C lira 50 and F(C lira )1 for C lira 0. Different expressions for F(C lira ) were tested (linear and Emax), and in the final model a linear function was used: FðC lira Þ511p lira C lira C lira was predicted for each individual subject using the PK model for liraglutide with fixed population parameters. The parameter p lira is an estimated constant describing the linear slope between C lira and the effect on insulin secretion. This model was chosen due to its simplicity while still adequately describing the data. In both trials, 1.5 g of paracetamol was administered with the meal to assess the gastric emptying rate. Paracetamol data from trial 1 indicated a delay in gastric emptying with liraglutide during the early phase after the meal (data not shown). No delay in gastric emptying was observed in trial 2. Assuming glucose is not absorbed in the stomach but in the intestine, the glucose absorption rate, k a, reflects the gastric emptying rate. A significant model improvement was obtained by allowing k a to be reduced in trial 1 for the MTTs with liraglutide, such that two values for ka were estimated: one for the placebo data (k a,trial1,placebo ) and one for the liraglutide data (k a,trial1,liraglutide ). It was not possible to detect any liraglutide concentration-dependent reduction in k a.no model improvement was achieved by including different values for k a for the placebo and the liraglutide arm in trial 2. In trial 2 the glucagon response was significantly reduced with liraglutide vs. placebo 15 (no glucagon measurements were obtained in trial 1). Glucagon is not explicitly expressed in the IGI model; however, the IGI model for healthy subjects contains a delayed, glucose-dependent inhibition of endogenous glucose production (EGP), 7,8 which accounts for the effect of glucagon. As T2DM patients have been shown to have a malfunction in the suppression of EGP, the IGI model for T2DM patients does not contain this feedback mechanism. However, in another trial 18 the rate of EGP in the fasting state was significantly reduced in liraglutide-treated T2DM patients. Thus, it seems reasonable to assume that liraglutide has an effect on EGP. This was tested by including an inhibitory effect of C lira on EGP. Different inhibitory functions were tested (linear and Emax), but they did not improve the fit nor were they statistically significant. For each inhibitory function it was checked that, with the estimated parameters, EGP remained positive at all relevant
3 30 Effects of a GLP-1 Analog on Glucose Table 1 Final parameter estimates. Parameter estimates Description Typical value RSE, % Liraglutide V L /F [L/kg] Volume of distribution for liraglutide (14) CL L /F [L/min/kg] Liraglutide clearance (10) k al [1/min] Absorption rate for liraglutide (9) IIV V L,% Interindividual variability for V L (21) IIV CL L,% Interindividual variability for CL L (29) RESL,% Residual errors for liraglutide 14 6 (7) Glucose CL G [L/min] Insulin-independent glucose clearance CL GI [L/min/(pM)] Insulin-dependent glucose clearance V P [L] Volume of distribution peripheral compartment 8.56 V G [L] Volume of distribution central compartment 9.33 Q [L/min] Inter-compartmental clearance of glucose k GE2 [1/min] Rate constant for glucose effect compartment k a,trial 1,placebo [1/min] Glucose absorption rate constant for trial 1, placebo k a,trial 1,liraglutide [1/min] Glucose absorption rate constant for trial 1, liraglutide k a,trial 2 [1/min] Glucose absorption rate constant for trial D trial 1 [g] Glucose dose trial D trial 2 [g] Glucose dose trial G SS, trial 1 [mm] Steady-state glucose concentration for trial G SS, trial 2 [mm] Steady-state glucose concentration for trial IIV CL G, % Interindividual variability for CL G 59 IIV CL GI,% Interindividual variability for CL GI IIV CL I, % Interindividual variability for CL I 29 Insulin I SS,trial 1 [pm] Steady-state insulin concentration for trial I SS,trial 2 [pm] Steady-state insulin concentration for trial V I [L] Volume of distribution for insulin 6.09 CL I [L/min] Insulin clearance 1.22 k IE [1/min] Rate constant for insulin effect compartment IPRG Control parameter for the effect of glucose on insulin secretion 1.42 E max Maximal effect of glucose in the glucose transit compartment G T on insulin secretion ED 50 [g] Glucose amount in the glucose transit compartment G T producing 50% of E max p lira [/nm] Linear slope between liraglutide concentration and insulin secretion Residual error RESG, % Residual error for glucose 16 6 RESI, % Residual error for insulin For the liraglutide model SE estimates were obtained both from the NONMEM run and by a bootstrap with 100 samples, the estimates from the bootstrap are in parentheses. For the IGI model all SEs were obtained from a bootstrap with 50 samples. IIV%, interindividual variability as standard deviation in percentage. Estimated parameters are in bold, all other parameters are fixed to the values from Jauslin et al. 9 V G and V I are proportional to weight, which is incorporated as a covariate and normalized to 70 kg. V L and CL L are proportional to weight. RSE%, relative standard error in percentage. liraglutide concentrations. No effect of liraglutide on EGP was included in the final model. The IGI model was able to describe the glucose and insulin data well, as seen in Figures 3 and 4, in which time courses for plasma glucose and insulin concentrations for the two trials are shown together with the model fits. The MTTs with liraglutide were performed when liraglutide was at steady state. Thus, the glucose concentration at the start of the MTTs with liraglutide was less than the estimated glucose concentration at steady state G SS, which reflects the placebo steady-state concentration. In the model, all previous liraglutide doses are included to ensure that at the start of the MTTs with liraglutide the glucose concentration is less than G SS. For example, for trial 1 the estimate of G SS was 9.7 mm. At the start of the MTT with 0.6 mg liraglutide, the mean of the observed glucose concentrations was 8.1 mm, which is in accordance with the mean of the individual model predictions of 8.5 mm. At the start of the MTT with 1.2 mg liraglutide the mean observed glucose concentration was 7.6 mm and the mean of the individual CPT: Pharmacometrics & Systems Pharmacology
4 Effects of a GLP-1 Analog on Glucose 31 Figure 2 (Left) Time course for liraglutide concentration. The dots show the geometric mean and the corresponding 95% confidence interval of the data. The solid lines show the geometric mean of the individual predictions (solid line) and the geometric mean of the population predictions (dashed line). (Right) Visual predictive check for the PK model for liraglutide. Solid lines represent median concentrations and dashed lines represent 5th and 95th percentiles. The red lines represent the data and the black lines represent simulations from the model. The shaded area represents the 95% confidence intervals for the model predicted median. Time zero is the time at which the last dose of liraglutide 1.8 mg was administered. model predictions was 7.7 mm. At the start of the MTT with 1.8 mg liraglutide the mean observed glucose concentration was 7.3 mm and the mean of the individual model predictions was 7.1 mm. There seems to be a trend in the insulin concentrations that the model does not quite capture (underprediction at the low liraglutide doses and overprediction at the higher liraglutide doses). The effect of liraglutide on insulin secretion is illustrated in Figure 5, in terms of model predicted insulin secretion for trial 1 at all dose levels (left panel). The right panel of Figure 5 shows the mean baseline corrected postprandial plasma glucose at all dose levels, for comparison. As seen, liraglutide exhibited a dose-dependent stimulation of insulin secretion concurrently with a dose-dependent reduction in glucose excursions following meal intake. The predictive performance of the model was graphically evaluated by a VPC based on 1,000 simulations. The VPC is included in the Supplementary Material. The VPC shows that the main trend and the variability of glucose and insulin were well captured by the model at all dose levels. As the final model terminated with rounding errors, standard errors in the IGI model were obtained by a bootstrap. Due to long run times (18 hours), the number of bootstrap samples was limited to 50, which was deemed sufficient for the estimation of standard errors. DISCUSSION In recent years, several GLP-1-based therapies have been developed. These therapies can be divided into two groups: (i) dipeptidyl-peptidase 4 inhibitors, such as vildagliptin and sitagliptin, which increase the concentration of native GLP- 1, and (ii) GLP-1 receptor agonists, such as liraglutide and exenatide. Different models have been used to describe the effect of GLP-1-based therapies on glucose homeostasis. A mechanism-based population model of the effects of vildagliptin on GLP-1, glucose, and insulin in T2DM patients was developed by Landersdorfer et al. 19 The effect of exenatide on insulin secretion during a hyperglycemic clamp 20 as well as the effect of liraglutide on glucose and insulin homeostasis in healthy volunteers 21 have been explored using an adapted minimal model. The effects of liraglutide in the adapted minimal model were implemented as a stimulatory effect on the magnitude of the first-phase insulin secretion and an increased second-phase insulin secretion. Also, exenatide was found to increase second-phase insulin secretion. In this study the integrated glucose-insulin model was extended to describe the glucose homeostasis in T2DM patients treated with liraglutide. For this purpose data from two trials investigating the effect of steady-state liraglutide on glucose homeostasis were used. The main effect of liraglutide on glucose homeostasis was incorporated in the IGI model as a concentrationdependent stimulation of insulin secretion. This is in accordance with prior modeling of the effects of GLP-1 analogs. 20,21 No significant model improvement was achieved by including an inhibitory effect of liraglutide on the endogenous glucose production, which would mimic
5 Figure 3 Time courses for plasma glucose and insulin concentrations for trial 1. The dots show the geometric mean and the corresponding 95% confidence interval of the data. The solid lines show the geometric mean of the individual predictions (solid lines) and the geometric mean of the population predictions (dashed lines). Time zero is defined as the time of the first measurement in the MTT, which is 10 minutes before meal ingestion.
6 Effects of a GLP-1 Analog on Glucose 33 Figure 4 Time courses for plasma glucose and insulin concentrations for trial 2. The dots show the geometric mean and the corresponding 95% confidence interval of the data. The solid lines show the geometric mean of the individual predictions (solid lines) and the geometric mean of the population predictions (dashed lines). Time zero is defined as the time of the first measurement in the MTT, which is 15 minutes before meal ingestion. an effect on glucagon. Furthermore, in one of the two trials (trial 1) a significant model improvement was achieved by including an inhibitory effect of liraglutide on gastric emptying. As it was assumed that glucose is absorbed in the intestine and not in the stomach, this was modeled as a decreased glucose absorption rate for the MTTs with liraglutide. The estimated glucose absorption rate in trial 1 was nearly twice as high as in trial 2. The caloric content of a meal is known to affect the gastric emptying rate, with decreased gastric emptying rate for increased caloric density. 22 In trial 2 the caloric content of the meals was twice as large as in trial 1. Thus, it was reasonable to assume that the gastric emptying rate in trial 2 was smaller than in
7 34 Effects of a GLP-1 Analog on Glucose Figure 5 (Left) Model predicted insulin secretion for the different dose levels for trial 1. (Right) Mean baseline corrected postprandial plasma glucose profiles during the MTTs for trial 1. All placebo data was included in the calculation of the mean, i.e., each subject contributes with three placebo profiles. trial 1, which agrees with the estimated values for glucose absorption rate. The glucose equivalents of the meals were estimated instead of fixing the glucose doses based on the carbohydrate content of the meals. For trial 2, a glucose equivalent of the meal could be calculated based on the glycemic indices of the ingested food, 23 which suggested that the glucose equivalent of the meal was 25 g. If instead it is assumed that 1 kcal of carbohydrate is equivalent to 0.25 g of glucose, which has also been done in previous publications of the IGI model, 10,11 then the glucose equivalent is 46 g. Both values are lower than the estimated glucose equivalent. Assuming that 1 kcal of carbohydrate is equivalent to 0.25 g of glucose, the glucose equivalent in trial 1 is 60 g, which is in line with the estimate of 51 g. In another study investigating the effect of protein on glucose homeostasis, it was observed that the addition of protein to a glucose dose increased the insulin concentrations at least twofold compared to the ingestion of glucose alone, while little or no effect was observed for the postprandial glucose concentrations. 24 The addition of fat to a carbohydrate load also affects the glycemic response, as it slows down gastric emptying 22 and markedly alters the appearance of ingested glucose. 25 Thus, the glucose and insulin concentrations following meal ingestion are highly dependent on meal composition. The IGI model in its current form is unable to handle the effect of protein and fat on glucose homeostasis, which may result in an overestimation of the ingested glucose for mixed meals. For simulation purposes, a more mechanistic model describing the effect of the different macronutrients on glucose homeostasis would be preferable, such that other meal types can be simulated. The development of such a model, however, would require data with different meal compositions. In conclusion, we modified the IGI model for evaluating effects of GLP-1 analogs on glucose homeostasis in patients with T2DM. Our results confirm that the primary mode of action of liraglutide is via stimulated insulin secretion following a glucose challenge and that a minor effect on gastric emptying may also be present, depending on the composition of the ingested meal. No effect on endogenous glucose production could be detected using the model. In this article, data from trials with liraglutide were used for model development. However, as other GLP-1 receptor agonists have similar modes of action as liraglutide, it is believed that the model with minor alterations can also be used to describe glucose homeostasis in T2DM patients treated with other GLP-1 receptor agonists. Others are also working on implementing the effects of GLP-1 receptor agonists on glucose homeostasis in the IGI model, and have presented similar results. 26 Thus, we conclude that the IGI model is a useful tool for investigating GLP-1 receptor agonists. METHODS Data For model development data from the following two trials were used. Trial 1 Trial 1 was a single-center, randomized, placebo-controlled, double-blind, two-period, crossover trial, comparing the effect of steady-state liraglutide at three dose levels (0.6, 1.2, and 1.8 mg/day) vs. placebo on the responses of fasting plasma glucose and postprandial glucose, insulin, and gastric emptying in T2DM patients. Eighteen patients were recruited for the trial and they were randomly assigned to either treatment group A (3 weeks of once-daily liraglutide, 3 4 weeks of washout, and 3 weeks of once-daily placebo) or B (3 weeks of once-daily placebo, 3 4 weeks of washout, and 3 weeks of once-daily liraglutide). During each 3- week treatment period, the liraglutide/placebo dose was escalated weekly in 0.6-mg increments from 0.6 mg until a daily dose of 1.8 mg was reached. After 1 week of treatment at each dose level, an energy fixed MTT was performed. The patients were instructed to administer liraglutide/placebo in the evening and the MTT was performed in the morning. Along with the meal, patients also received 1.5 g paracetamol. During the MTT, plasma glucose, serum insulin, and paracetamol concentrations were measured. A baseline sample was drawn 10 minutes before the MTT and during the postprandial period nine blood samples were drawn at the following timepoints: 15, 30, 45, 60, 90, 120, 180, 240, and 300 minutes. Blood samples for assessment of liraglutide concentrations were drawn 6, 8, 10, and 12 hours after the liraglutide/placebo dosing. For more information on the trial, the reader is referred to Flint et al. 14 Trial 2 Trial 2 was a randomized, double-blind, placebo-controlled, crossover trial, comparing the effect of treatment with steady-state liraglutide 1.8 mg vs. placebo on postprandial plasma triglyceride concentrations following a standardized high-fat meal in T2DM patients. Treatment order of liraglutide 1.8 mg or placebo was determined through random assignment. Individuals randomized to liraglutide underwent weekly dose escalation, starting at 0.6 mg/day (with 0.6-mg increments to 1.8 mg). Liraglutide vehicle was used as placebo to ensure blinding. A washout period of 3 9 weeks was included between the two treatments. At the end of each 3-week period an MTT was performed. The patients CPT: Pharmacometrics & Systems Pharmacology
8 Effects of a GLP-1 Analog on Glucose 35 were instructed to administer liraglutide/placebo in the evening and the MTT was performed in the morning. Along with the meal, patients also received 1.5 g paracetamol. During the MTT, plasma glucose, serum insulin, and paracetamol concentrations were measured. A baseline sample was drawn 15 minutes before the MTT and during the postprandial period nine blood samples for glucose and insulin were drawn at the following timepoints: 15, 30, 60, 120, 180, 240, 300, 360, and 480 minutes. Blood samples for assessment of liraglutide concentrations were drawn at 15 minutes before and 4, 6, 8, 10, 12, 14, 16, 24, 36, 48, and 60 hours after the last liraglutide dose. Eighteen patients completed the trial. However, due to noncompliance with protocol requirements, meal-test endpoints for seven individuals were excluded from the analysis. For additional information on the trial, the reader is referred to Hermansen et al. 15 Model development The integrated glucose-insulin (IGI) model developed by Silber et al. 9 was used as a basis for model development. The model consists of submodels for glucose and insulin as well as homeostatic feedback mechanisms which control the insulin secretion and the elimination of glucose (the model equations are provided in the Supplementary Material). To account for the effect of liraglutide on glucose homeostasis, a PK model for liraglutide was coupled to the IGI model (Figure 1). The effect of liraglutide on glucose homeostasis was tested on relevant parts of the model (insulin secretion, endogenous glucose production, and glucose absorption rate). Glucose submodel Glucose was described by a two-compartment disposition model with both insulin-dependent and insulin-independent elimination from the central compartment and endogenous glucose production. The glucose absorption from the gut was described by a first-order process via one transit compartment. The stimulatory effect of glucose on insulin secretion was included in the model using an effect compartment. Endogenous insulin submodel Endogenous insulin kinetics were described by a onecompartment model with endogenous insulin secretion and first-order elimination. The endogenous insulin secretion was assumed to be regulated by the blood glucose concentration and the incretin effect. The incretin effect was described by a saturable function linking the amount of glucose in the glucose transit compartment to insulin secretion. Model estimation and statistical analysis Model estimation was performed using nonlinear mixed effects modeling in NONMEM 7 27 with the first-order conditional estimation (FOCE) method and the differential equation solver ADVAN13. The NONMEM code for the final model is provided in the Supplementary Material. Model selection was based on a compromise between mechanistic considerations, objective function value (OFV), plausibility of parameter estimates, and graphical assessment. A difference in the OFV of at least was used as a cutpoint value for nested models differing by one parameter, which corresponds to a significance level of a Interindividual variability. The differences between individual parameters were described using random effects, whichwereassumedtobenormallydistributedwithmean zero. The distribution of the individual parameters around the typical population value was assumed to be lognormal. Residual error model. An additive model was used to describe the residual error of the log-transformed data. The residual error was assumed to arise from a distribution with mean zero and an estimated variance. Different residual errors for glucose (RESG), insulin (RESI), and liraglutide (RESL) were estimated. Acknowledgments. The research leading to these results received support from the Innovative Medicines Initiative Joint Undertaking under grant agreement no , resources, which are composed of financial contributions from the European Union s Seventh Framework Programme (FP7/ ) and EFPIA companies in-kind contribution. The DDMoRe project is also supported by financial contributions from Academic and SME partners. This work does not necessarily represent the view of all DDMoRe partners. Author Contributions. R.M.R. wrote the article; R.M.R., S.K., S.H.I., M.C.K., and N.R.K. designed the research; R.M.R. performed the research. Conflict of Interest. R.M.R., S.K., S.H.I., and N.R.K. are employed at Novo Nordisk A/S. Study Highlights WHAT IS THE CURRENT KNOWLEDGE ON THIS TOPIC? The integrated glucose-insulin model, which was previously developed to describe the glucose homeostasis during different glucose provocations, has been used to investigate the effects of antidiabetic drugs on glucose homeostasis. WHAT QUESTION DID THIS STUDY ADDRESS? Can the integrated glucose-insulin model be extended to describe glucose homeostasis in T2DM patients treated with the GLP-1 receptor agonist liraglutide at different dose levels? WHAT THIS STUDY ADDS TO OUR KNOWLEDGE Effects of liraglutide on glucose homeostasis were included in the model, which was found suitable for clinical trial simulations.
9 36 Effects of a GLP-1 Analog on Glucose HOW THIS MIGHT CHANGE CLINICAL PHARMACOLOGY AND THERAPEUTICS As other GLP-1 receptor agonists have similar modes of action as liraglutide, the model may potentially be used to describe the glucose homeostasis in T2DM patients treated with other GLP-1 receptor agonists or possibly combination products. 1. Campbell, J.E. & Drucker, D.J. Pharmacology, physiology, and mechanisms of incretin hormone action. Cell. Metab. 17, (2013). 2. Vilsbøll, T., Agersø, H., Krarup, T. & Holst, J.J. Similar elimination rates of glucagonlike peptide-1 in obese type 2 diabetic patients and healthy subjects. J. Clin. Endocrinol. Metab. 88, (2003). 3. Garber, A.J. Novel GLP-1 receptor agonists for diabetes. Expert Opin. Investig. Drugs. 211, (2012). 4. Madsbad, S. Exenatide and liraglutide: different approaches to develop GLP-1 receptor agonists (incretin mimetics) preclinical and clinical results. Best. Pract. Res. Clin. Endocrinol. Metab. 23, (2009). 5. Russell-Jones D. Molecular, pharmacological and clinical aspects of liraglutide, a once-daily human GLP-1 analogue. Mol. Cell. Endocrinol. 297, (2009). 6. Montanya, E. & Sesti, G. A review of efficacy and safety data regarding the use of liraglutide, a once-daily human glucagon-like peptide 1 analogue, in the treatment of type 2 diabetes mellitus. Clin. Ther. 31, (2009). 7. Silber HE, Jauslin PM, Frey N, Gieschke R, Simonsson, U.S.H. & Karlsson, M.O. An integrated model for glucose and insulin regulation in healthy volunteers and type 2 diabetic patients following intravenous glucose provocations. J. Clin. Pharmacol. 47, (2007). 8. Silber, H.E., Frey, N. & Karlsson, M.O. An integrated glucose-insulin model to describe oral glucose tolerance test data in healthy volunteers. J. Clin. Pharmacol. 50, (2010). 9. Jauslin, P.M. et al. An integrated glucose-insulin model to describe oral glucose tolerance test data in type 2 diabetics. J. Clin. Pharmacol. 47, (2007). 10. Jauslin, P.M., Frey N. & Karlsson M.O. Modeling of 24-hour glucose and insulin profiles of patients with type 2 diabetes. J. Clin. Pharmacol. 51, (2011). 11. Schneck, K.B., Zhang, X., Bauer, R., Karlsson, M.O. & Sinha, V.P. Assessment of glycemic response to an oral glucokinase activator in a proof of concept study: Application of a semi-mechanistic, integrated glucose-insulin-glucagon model. J. Pharmacokinet. Pharmacodyn. 40, (2013). 12. Røge, R.M., Klim, S., Kristensen, N.R., Ingwersen, S.H. & Kjellsson, M.C. Modeling of 24-hour glucose and insulin profiles in patients with type 2 diabetes mellitus treated with biphasic insulin aspart. J. Clin. Pharmacol Zhang, X., Schneck, K., Bue-Valleskey, J., Yeo, K.P., Heathman, M. & Sinha, V. Dose selection using a semi-mechanistic integrated glucose-insulin-glucagon model: designing phase 2 trials for a novel oral glucokinase activator. J. Pharmacokinet. Pharmacodyn. 40, (2013). 14. Flint, A., Kapitza, C., Hindsberger, C. & Zdravkovic, M. The once-daily human glucagon-like peptide-1 (GLP-1) analog liraglutide improves postprandial glucose levels in type 2 diabetes patients. Adv. Ther. 28, (2011). 15. Hermansen, K. et al. Liraglutide suppresses postprandial triglyceride and apolipoprotein B48 elevations after a fat-rich meal in patients with type 2 diabetes: a randomized, double-blind, placebo-controlled, cross-over trial. Diabetes Obes. Metab. 15, (2013). 16. Ingwersen, S.H. et al. Dosing rationale for liraglutide in type 2 diabetes mellitus: a pharmacometric assessment. J. Clin. Pharmacol, 52, (2012). 17. Watson, E, Jonker, D.M., Jacobsen, L.V. & Ingwersen, S.H. Population pharmacokinetics of liraglutide, a once-daily human glucagon-like peptide-1 analog, in healthy volunteers and subjects with type 2 diabetes, and comparison to twice-daily exenatide. J. Clin. Pharmacol. 52, (2010) 18. Degn, K.B. et al. One week s treatment with the long-acting glucagon-like peptide 1 derivative liraglutide (NN2211) markedly improves 24-h glycemia and a- and b-cell function and reduces endogenous glucose release in patients with type 2 diabetes. Diabetes. 53, (2004). 19. Landersdorfer, C.B., He, Y.L. & Jusko, W.J. Mechanism-based population modelling of the effects of vildagliptin on GLP-1, glucose and insulin in patients with type 2 diabetes. Br. J. Clin. Pharmacol. 73, (2011). 20. Mager, D.E., Abernethy, D.R., Egan, J.M. & Elahi, D. Exendin-4 pharmacodynamics: insights from the hyperglycemic clamp technique. J. Pharmacol. Exp. Ther. 311, (2004). 21. Agersø, H. & Vicini, P. Pharmacodynamics of NN2211, a novel long acting GLP-1 derivative. Eur. J. Pharm. Sci. 19, (2003). 22. Calbet, J.A.L. & MacLean, D.A. Role of caloric content on gastric emptying in humans. J. Physiol. 498, (1997). 23. Jenkins, D.J.A. et al. Glycemic index of foods: A physiological basis for carbohydrate exchange. Am. J. Clin. Nutr. 34, (1981). 24. Gannon, M.C., Nuttall, F.Q., Neil, B.J. & Westphal, S.A. The insulin and glucose responses to meals of glucose plus various proteins in type II diabetic subjects. Metabolism. 37, (1988). 25. Normand, S. et al. Influence of dietary fat on postprandial glucose metabolism (exogenous and endogenous) using intrinsically 13C-enriched durum wheat. Br. J. Nutr. 86, 3 11 (2001). 26. Jauslin, P., Dubar, M., Sebastien, B., Laveille, C. & Gisleskog, P.O. Comparison of post-prandial glucose control by two GLP-1 receptor agonists (lixisenatide and liraglutide) in type 2 diabetes. Poster presented at the Population Approach Group Meeting in Alicante, Spain 2014 < abstract53042>. 27. Beal, S.L., Sheiner, L.B. & Boeckmann, A.J. Icon development solutions. NONMEM Users Guides Ellicott City, MD, Icon Development Solutions VC 2014 The Authors CPT: Pharmacometrics & Systems Pharmacology published by Wiley Periodicals, Inc. on behalf of American Society for Clinical Pharmacology and Therapeutics. This is an open access article under the terms of the Creative Commons Attribution-NonCommercial License, which permits use, distribution and reproduction in any medium, provided the original work is properly cited and is not used for commercial purposes. Supplementary information accompanies this paper on the CPT: Pharmacometrics & Systems Pharmacology website ( CPT: Pharmacometrics & Systems Pharmacology
An integrated glucose-insulin model to describe oral glucose tolerance test data in healthy volunteers
 Title: An integrated glucose-insulin model to describe oral glucose tolerance test data in healthy volunteers Authors: Hanna E. Silber 1, Nicolas Frey 2 and Mats O. Karlsson 1 Address: 1 Department of
Title: An integrated glucose-insulin model to describe oral glucose tolerance test data in healthy volunteers Authors: Hanna E. Silber 1, Nicolas Frey 2 and Mats O. Karlsson 1 Address: 1 Department of
An integrated glucose homeostasis model of glucose, insulin, C-peptide, GLP-1, GIP and glucagon in healthy subjects and patients with type 2 diabetes
 An integrated glucose homeostasis model of glucose, insulin, C-peptide, GLP-1, GIP and glucagon in healthy subjects and patients with type 2 diabetes Oskar Alskär, Jonatan Bagger, Rikke Røge, Kanji Komatsu,
An integrated glucose homeostasis model of glucose, insulin, C-peptide, GLP-1, GIP and glucagon in healthy subjects and patients with type 2 diabetes Oskar Alskär, Jonatan Bagger, Rikke Røge, Kanji Komatsu,
Pharmacometric Models of Glucose Homeostasis in Healthy Subjects and Diabetes Patients
 Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Pharmacy 212 Pharmacometric Models of Glucose Homeostasis in Healthy Subjects and Diabetes Patients RIKKE MELDGAARD RØGE ACTA
Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Pharmacy 212 Pharmacometric Models of Glucose Homeostasis in Healthy Subjects and Diabetes Patients RIKKE MELDGAARD RØGE ACTA
Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function
 Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function Background. Following meal ingestion, several hormones are released from the gastrointestinal tract. Some
Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function Background. Following meal ingestion, several hormones are released from the gastrointestinal tract. Some
Chief of Endocrinology East Orange General Hospital
 Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
GLP-1 agonists. Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK
 GLP-1 agonists Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What do GLP-1 agonists do? Physiology of postprandial glucose regulation Meal ❶ ❷ Insulin Rising plasma
GLP-1 agonists Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What do GLP-1 agonists do? Physiology of postprandial glucose regulation Meal ❶ ❷ Insulin Rising plasma
VC 2017 ASCPT All rights reserved
 Citation: CPT Pharmacometrics Syst. Pharmacol. (2017) 6, 686 694; VC 2017 ASCPT All rights reserved doi:10.1002/psp4.12214 ORIGINAL ARTICLE Implications for Drug Characterization in Glucose Tolerance Tests
Citation: CPT Pharmacometrics Syst. Pharmacol. (2017) 6, 686 694; VC 2017 ASCPT All rights reserved doi:10.1002/psp4.12214 ORIGINAL ARTICLE Implications for Drug Characterization in Glucose Tolerance Tests
Mechanism-based modelling of clinical and preclinical studies of glucose homeostasis
 Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Pharmacy 248 Mechanism-based modelling of clinical and preclinical studies of glucose homeostasis OSKAR ALSKÄR ACTA UNIVERSITATIS
Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Pharmacy 248 Mechanism-based modelling of clinical and preclinical studies of glucose homeostasis OSKAR ALSKÄR ACTA UNIVERSITATIS
Scope. History. History. Incretins. Incretin-based Therapy and DPP-4 Inhibitors
 Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
Role of incretins in the treatment of type 2 diabetes
 Role of incretins in the treatment of type 2 diabetes Jens Juul Holst Department of Medical Physiology Panum Institute University of Copenhagen Denmark Diabetes & Obesity Spanish Society of Internal Medicine
Role of incretins in the treatment of type 2 diabetes Jens Juul Holst Department of Medical Physiology Panum Institute University of Copenhagen Denmark Diabetes & Obesity Spanish Society of Internal Medicine
Drug-Disease Modeling Applied to Drug Development and Regulatory Decision Making in the Type 2 Diabetes Mellitus Arena
 Drug-Disease Modeling Applied to Drug Development and Regulatory Decision Making in the Type 2 Diabetes Mellitus Arena Tokyo, Japan, December 8, 2015 Stephan Schmidt, Ph.D. Assistant Professor Center for
Drug-Disease Modeling Applied to Drug Development and Regulatory Decision Making in the Type 2 Diabetes Mellitus Arena Tokyo, Japan, December 8, 2015 Stephan Schmidt, Ph.D. Assistant Professor Center for
The Many Faces of T2DM in Long-term Care Facilities
 The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
Model-Based Interspecies Scaling of Glucose Homeostasis
 Citation: CPT Pharmacometrics Syst. Pharmacol. (2017) 6, 778 786; VC 2017 ASCPT All rights reserved doi:10.1002/psp4.12247 ORIGINAL ARTICLE Model-Based Interspecies Scaling of Glucose Homeostasis Oskar
Citation: CPT Pharmacometrics Syst. Pharmacol. (2017) 6, 778 786; VC 2017 ASCPT All rights reserved doi:10.1002/psp4.12247 ORIGINAL ARTICLE Model-Based Interspecies Scaling of Glucose Homeostasis Oskar
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE. CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010
 Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Mechanisms and Clinical Efficacy of Lixisenatide for the Management of Type 2 Diabetes
 Adv Ther (2013) 30(2):81 101. DOI 10.1007/s12325-013-0009-4 REVIEW Mechanisms and Clinical Efficacy of Lixisenatide for the Management of Type 2 Diabetes Michael Horowitz Christopher K. Rayner Karen L.
Adv Ther (2013) 30(2):81 101. DOI 10.1007/s12325-013-0009-4 REVIEW Mechanisms and Clinical Efficacy of Lixisenatide for the Management of Type 2 Diabetes Michael Horowitz Christopher K. Rayner Karen L.
Study Design Selection in Early Clinical Anti-Hyperglycemic Drug Development: A Simulation Study of Glucose Tolerance Tests
 Citation: CPT Pharmacometrics Syst. Pharmacol. (2018) 7, 432 441; doi:10.1002/psp4.12302 ARTICLE Study Design Selection in Early Clinical Anti-Hyperglycemic Drug Development: A Simulation Study of Glucose
Citation: CPT Pharmacometrics Syst. Pharmacol. (2018) 7, 432 441; doi:10.1002/psp4.12302 ARTICLE Study Design Selection in Early Clinical Anti-Hyperglycemic Drug Development: A Simulation Study of Glucose
Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP
 Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP KEY POINTS sitagliptin (Januvia) is a DPP-4 inhibitor that blocks the breakdown of the
Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP KEY POINTS sitagliptin (Januvia) is a DPP-4 inhibitor that blocks the breakdown of the
28 Regulation of Fasting and Post-
 28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
Data from an epidemiologic analysis of
 CLINICAL TRIAL RESULTS OF GLP-1 RELATED AGENTS: THE EARLY EVIDENCE Lawrence Blonde, MD, FACP, FACE ABSTRACT Although it is well known that lowering A 1c (also known as glycated hemoglobin) is associated
CLINICAL TRIAL RESULTS OF GLP-1 RELATED AGENTS: THE EARLY EVIDENCE Lawrence Blonde, MD, FACP, FACE ABSTRACT Although it is well known that lowering A 1c (also known as glycated hemoglobin) is associated
A population pharmacokinetic model for rifampicin auto induction
 A population pharmacokinetic model for rifampicin auto induction Paolo Denti 1, Wynand Smythe 1, Ulrika SH Simonsson 2, Roxana Rustomjee 3, Philip Onyebujoh 4, Peter Smith 1, Helen McIlleron 1 1 Division
A population pharmacokinetic model for rifampicin auto induction Paolo Denti 1, Wynand Smythe 1, Ulrika SH Simonsson 2, Roxana Rustomjee 3, Philip Onyebujoh 4, Peter Smith 1, Helen McIlleron 1 1 Division
GLUCAGON LIKE PEPTIDE (GLP) 1 AGONISTS FOR THE TREATMENT OF TYPE 2 DIABETES, WEIGHT CONTROL AND CARDIOVASCULAR PROTECTION.
 GLUCAGON LIKE PEPTIDE (GLP) 1 AGONISTS FOR THE TREATMENT OF TYPE 2 DIABETES, WEIGHT CONTROL AND CARDIOVASCULAR PROTECTION. Patricia Garnica MS, ANP-BC, CDE, CDTC Inpatient Diabetes Nurse Practitioner North
GLUCAGON LIKE PEPTIDE (GLP) 1 AGONISTS FOR THE TREATMENT OF TYPE 2 DIABETES, WEIGHT CONTROL AND CARDIOVASCULAR PROTECTION. Patricia Garnica MS, ANP-BC, CDE, CDTC Inpatient Diabetes Nurse Practitioner North
New and Emerging Therapies for Type 2 DM
 Dale Clayton MHSc, MD, FRCPC Dalhousie University/Capital Health April 28, 2011 New and Emerging Therapies for Type 2 DM The science of today, is the technology of tomorrow. Edward Teller American Physicist
Dale Clayton MHSc, MD, FRCPC Dalhousie University/Capital Health April 28, 2011 New and Emerging Therapies for Type 2 DM The science of today, is the technology of tomorrow. Edward Teller American Physicist
Update on Insulin-based Agents for T2D
 Update on Insulin-based Agents for T2D Injectable Therapies for Type 2 Diabetes Mellitus (T2DM) and Obesity This presentation will: Describe established and newly available insulin therapies for treatment
Update on Insulin-based Agents for T2D Injectable Therapies for Type 2 Diabetes Mellitus (T2DM) and Obesity This presentation will: Describe established and newly available insulin therapies for treatment
Treating Type 2 Diabetes with Bariatric Surgery. Goal of Treating T2DM. Remission of T2DM with Bariatric
 Treating Type 2 Diabetes with Bariatric Surgery Number (in Millions) of Persons with Diagnosed Diabetes, United States, 198 25 The number of Americans with diabetes increased from 5.6 to 15.8 million Guilherme
Treating Type 2 Diabetes with Bariatric Surgery Number (in Millions) of Persons with Diagnosed Diabetes, United States, 198 25 The number of Americans with diabetes increased from 5.6 to 15.8 million Guilherme
Insulin Secretion and Hepatic Extraction during Euglycemic Clamp Study: Modelling of Insulin and C-peptide data
 Insulin Secretion and Hepatic Extraction during Euglycemic Clamp Study: Modelling of Insulin and C-peptide data Chantaratsamon Dansirikul Mats O Karlsson Division of Pharmacokinetics and Drug Therapy Department
Insulin Secretion and Hepatic Extraction during Euglycemic Clamp Study: Modelling of Insulin and C-peptide data Chantaratsamon Dansirikul Mats O Karlsson Division of Pharmacokinetics and Drug Therapy Department
INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES
 INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES ARSHNA SANGHRAJKA DIABETES SPECIALIST PRESCRIBING PHARMACIST OBJECTIVES EXPLORE THE TYPES OF INSULIN AND INJECTABLE DIABETES TREATMENTS AND DEVICES AVAILABLE
INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES ARSHNA SANGHRAJKA DIABETES SPECIALIST PRESCRIBING PHARMACIST OBJECTIVES EXPLORE THE TYPES OF INSULIN AND INJECTABLE DIABETES TREATMENTS AND DEVICES AVAILABLE
Type 2 DM in Adolescents: Use of GLP-1 RA. Objectives. Scope of Problem: Obesity. Background. Pathophysiology of T2DM
 Type 2 DM in Adolescents: Use of GLP-1 RA Objectives Identify patients in the pediatric population with T2DM that would potentially benefit from the use of GLP-1 RA Discuss changes in glycemic outcomes
Type 2 DM in Adolescents: Use of GLP-1 RA Objectives Identify patients in the pediatric population with T2DM that would potentially benefit from the use of GLP-1 RA Discuss changes in glycemic outcomes
MODEL-BASED DOSE INDIVIDUALIZATION APPROACHES USING BIOMARKERS
 MODEL-BASED DOSE INDIVIDUALIZATION APPROACHES USING BIOMARKERS CATHERINE M SHERWIN PAGE 27 th Meeting, Montreux, Switzerland 30 th May 2018 Division of Clinical Pharmacology, Pediatrics, School of Medicine
MODEL-BASED DOSE INDIVIDUALIZATION APPROACHES USING BIOMARKERS CATHERINE M SHERWIN PAGE 27 th Meeting, Montreux, Switzerland 30 th May 2018 Division of Clinical Pharmacology, Pediatrics, School of Medicine
Disclosure. Learning Objectives. Case. Diabetes Update: Incretin Agents in Diabetes-When to Use Them? I have no disclosures to declare
 Disclosure Diabetes Update: Incretin Agents in Diabetes-When to Use Them? I have no disclosures to declare Spring Therapeutics Update 2011 CSHP BC Branch Anar Dossa BScPharm Pharm D CDE April 20, 2011
Disclosure Diabetes Update: Incretin Agents in Diabetes-When to Use Them? I have no disclosures to declare Spring Therapeutics Update 2011 CSHP BC Branch Anar Dossa BScPharm Pharm D CDE April 20, 2011
22 Emerging Therapies for
 22 Emerging Therapies for Treatment of Type 2 Diabetes Siddharth N Shah Abstract: The prevalence of Diabetes is progressively increasing world-wide and the growth of the disease in our country is phenomenal.
22 Emerging Therapies for Treatment of Type 2 Diabetes Siddharth N Shah Abstract: The prevalence of Diabetes is progressively increasing world-wide and the growth of the disease in our country is phenomenal.
VICTOSA and Renal impairment DR.R.S.SAJAD
 VICTOSA and Renal impairment DR.R.S.SAJAD February 2019 Main effect of GLP-1 is : Stimulating glucose dependent insulin release from the pancreatic islets. Slow gastric emptying Inhibit inappropriate
VICTOSA and Renal impairment DR.R.S.SAJAD February 2019 Main effect of GLP-1 is : Stimulating glucose dependent insulin release from the pancreatic islets. Slow gastric emptying Inhibit inappropriate
Scottish Medicines Consortium
 Scottish Medicines Consortium liraglutide 6mg/mL prefilled pen for injection (3mL) (Victoza ) Novo Nordisk Ltd. No. (585/09) 06 November 2009 The Scottish Medicines Consortium (SMC) has completed its assessment
Scottish Medicines Consortium liraglutide 6mg/mL prefilled pen for injection (3mL) (Victoza ) Novo Nordisk Ltd. No. (585/09) 06 November 2009 The Scottish Medicines Consortium (SMC) has completed its assessment
Comparison of Power, Prognosis, and Extrapolation Properties of Four Population Pharmacodynamic Models of HbA1c for Type 2 Diabetes
 Citation: CPT Pharmacometrics Syst. Pharmacol. (2018) 7, 331 341; VC 2018 ASCPT All rights reserved doi:10.1002/psp4.12290 ARTICLE Comparison of Power, Prognosis, and Extrapolation Properties of Four Population
Citation: CPT Pharmacometrics Syst. Pharmacol. (2018) 7, 331 341; VC 2018 ASCPT All rights reserved doi:10.1002/psp4.12290 ARTICLE Comparison of Power, Prognosis, and Extrapolation Properties of Four Population
Management of Type 2 Diabetes
 Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
Case Report Off-Label Use of Liraglutide in the Management of a Pediatric Patient with Type 2 Diabetes Mellitus
 Case Reports in Pediatrics Volume 2013, Article ID 703925, 4 pages http://dx.doi.org/10.1155/2013/703925 Case Report Off-Label Use of Liraglutide in the Management of a Pediatric Patient with Type 2 Diabetes
Case Reports in Pediatrics Volume 2013, Article ID 703925, 4 pages http://dx.doi.org/10.1155/2013/703925 Case Report Off-Label Use of Liraglutide in the Management of a Pediatric Patient with Type 2 Diabetes
Soliqua (insulin glargine and lixisenatide), Xultophy (insulin degludec and liraglutide)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.48 Subject: Insulin GLP-1 Combinations Page: 1 of 5 Last Review Date: September 15, 2017 Insulin GLP-1
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.48 Subject: Insulin GLP-1 Combinations Page: 1 of 5 Last Review Date: September 15, 2017 Insulin GLP-1
Multiple Factors Should Be Considered When Setting a Glycemic Goal
 Multiple Facts Should Be Considered When Setting a Glycemic Goal Patient attitude and expected treatment effts Risks potentially associated with hypoglycemia, other adverse events Disease duration Me stringent
Multiple Facts Should Be Considered When Setting a Glycemic Goal Patient attitude and expected treatment effts Risks potentially associated with hypoglycemia, other adverse events Disease duration Me stringent
INJECTABLE THERAPIES IN DIABETES. Barbara Ann McKee Diabetes Specialist Nurse
 INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
Discussion & Conclusion
 Discussion & Conclusion 7. Discussion DPP-4 inhibitors augment the effects of incretin hormones by prolonging their half-life and represent a new therapeutic approach for the treatment of type 2 diabetes
Discussion & Conclusion 7. Discussion DPP-4 inhibitors augment the effects of incretin hormones by prolonging their half-life and represent a new therapeutic approach for the treatment of type 2 diabetes
Toward Better Understanding of Insulin Therapy by Translation of a PK-PD Model to Visualize Insulin and Glucose Action Profiles
 Pharmacokinetics/Pharmacodynamics Toward Better Understanding of Insulin Therapy by Translation of a PK-PD Model to Visualize Insulin and Glucose Action Profiles The Journal of Clinical Pharmacology 2019,
Pharmacokinetics/Pharmacodynamics Toward Better Understanding of Insulin Therapy by Translation of a PK-PD Model to Visualize Insulin and Glucose Action Profiles The Journal of Clinical Pharmacology 2019,
Francesca Porcellati
 XX Congresso Nazionale AMD Razionali e Benefici dell Aggiunta del GLP-1 RA Short-Acting all Insulina Basale Francesca Porcellati Dipartimento di Medicina Interna, Sezione di Medicina Interna, Endocrinologia
XX Congresso Nazionale AMD Razionali e Benefici dell Aggiunta del GLP-1 RA Short-Acting all Insulina Basale Francesca Porcellati Dipartimento di Medicina Interna, Sezione di Medicina Interna, Endocrinologia
Early treatment for patients with Type 2 Diabetes
 Israel Society of Internal Medicine Kibutz Hagoshrim, June 22, 2012 Early treatment for patients with Type 2 Diabetes Eduard Montanya Hospital Universitari Bellvitge-IDIBELL CIBERDEM University of Barcelona
Israel Society of Internal Medicine Kibutz Hagoshrim, June 22, 2012 Early treatment for patients with Type 2 Diabetes Eduard Montanya Hospital Universitari Bellvitge-IDIBELL CIBERDEM University of Barcelona
(Incretin) ( glucagon-like peptide-1 GLP-1 ) GLP-1. GLP-1 ( dipeptidyl peptidase IV DPP IV ) GLP-1 DPP IV GLP-1 exenatide liraglutide FDA 2 2 2
 007 18 189-194 (Incretin) Incretin ( ) -1 ( glucagon-like peptide-1 ) ( dipeptidyl peptidase IV ) liraglutide FDA ( Type diabetes mellitus ) -1 ( Glucagon-like peptide-1, ) ( Incretin ) ( Dipeptidyl peptidase
007 18 189-194 (Incretin) Incretin ( ) -1 ( glucagon-like peptide-1 ) ( dipeptidyl peptidase IV ) liraglutide FDA ( Type diabetes mellitus ) -1 ( Glucagon-like peptide-1, ) ( Incretin ) ( Dipeptidyl peptidase
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Single Technology Appraisal. Canagliflozin in combination therapy for treating type 2 diabetes
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Single Technology Appraisal Canagliflozin in combination therapy for Final scope Remit/appraisal objective To appraise the clinical and cost effectiveness
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Single Technology Appraisal Canagliflozin in combination therapy for Final scope Remit/appraisal objective To appraise the clinical and cost effectiveness
T2DM is a global epidemic with
 : a new option for the management of type 2 diabetes Marc Evans MRCP, MD, Consultant Diabetologist, Llandough Hospital, Cardiff Incretin-based therapies for the treatment of diabetes mellitus (T2DM) present
: a new option for the management of type 2 diabetes Marc Evans MRCP, MD, Consultant Diabetologist, Llandough Hospital, Cardiff Incretin-based therapies for the treatment of diabetes mellitus (T2DM) present
GLP-1 Receptor Agonists and SGLT-2 Inhibitors. Debbie Hicks
 GLP-1 Receptor Agonists and SGLT-2 Inhibitors Debbie Hicks Prescribing and Adverse Event reporting information is available at this meeting from the AstraZeneca representative The views expressed by the
GLP-1 Receptor Agonists and SGLT-2 Inhibitors Debbie Hicks Prescribing and Adverse Event reporting information is available at this meeting from the AstraZeneca representative The views expressed by the
The Mediterranean Diet: HOW and WHY It Works So Well for T2DM
 The Mediterranean Diet: HOW and WHY It Works So Well for T2DM Susan L. Barlow, RD, CDE. Objectives 1. Discuss the effects of meal size on GLP-1 concentrations. 2. Compare and contrast the specific effects
The Mediterranean Diet: HOW and WHY It Works So Well for T2DM Susan L. Barlow, RD, CDE. Objectives 1. Discuss the effects of meal size on GLP-1 concentrations. 2. Compare and contrast the specific effects
GLP-1 (glucagon-like peptide-1) Agonists (Byetta, Bydureon, Tanzeum, Trulicity, Victoza ) Step Therapy and Quantity Limit Criteria Program Summary
 OBJECTIVE The intent of the GLP-1 (glucagon-like peptide-1) s (Byetta/exenatide, Bydureon/ exenatide extended-release, Tanzeum/albiglutide, Trulicity/dulaglutide, and Victoza/liraglutide) Step Therapy
OBJECTIVE The intent of the GLP-1 (glucagon-like peptide-1) s (Byetta/exenatide, Bydureon/ exenatide extended-release, Tanzeum/albiglutide, Trulicity/dulaglutide, and Victoza/liraglutide) Step Therapy
Diabesity. Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs
 Diabesity Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs Abdominal obesity Low HDL, high LDL, and high triglycerides HTN High blood glucose (F>100l,
Diabesity Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs Abdominal obesity Low HDL, high LDL, and high triglycerides HTN High blood glucose (F>100l,
SYNOPSIS. The study results and synopsis are supplied for informational purposes only.
 SYNOPSIS INN : LEFLUNOMIDE Study number : HMR486/1037 et HMR486/3503 Study title : Population pharmacokinetics of A77 1726 (M1) after oral administration of leflunomide in pediatric subjects with polyarticular
SYNOPSIS INN : LEFLUNOMIDE Study number : HMR486/1037 et HMR486/3503 Study title : Population pharmacokinetics of A77 1726 (M1) after oral administration of leflunomide in pediatric subjects with polyarticular
GLP-1. GLP-1 is produced by the L-cells of the gut after food intake in two biologically active forms It is rapidly degraded by DPP-4.
 GLP-1 GLP-1 is produced by the L-cells of the gut after food intake in two biologically active forms It is rapidly degraded by DPP-4 Food intake éinsulin Gut églucose uptake Pancreas Beta cells Alpha cells
GLP-1 GLP-1 is produced by the L-cells of the gut after food intake in two biologically active forms It is rapidly degraded by DPP-4 Food intake éinsulin Gut églucose uptake Pancreas Beta cells Alpha cells
Electronic Supplementary Material to the article entitled Altered pattern of the
 Electronic Supplementary Material to the article entitled Altered pattern of the incretin effect as assessed by modelling in individuals with glucose tolerance ranging from normal to diabetic Integrated
Electronic Supplementary Material to the article entitled Altered pattern of the incretin effect as assessed by modelling in individuals with glucose tolerance ranging from normal to diabetic Integrated
Liraglutide: First Once-Daily Human GLP-1 Analogue
 DRUG PROFILE KERALA MEDICAL JOURNAL Liraglutide: First Once-Daily Human GLP-1 Analogue Sreejith N Kumar Research Cell, IMA Kerala State, K-5, Kochar Road, Sasthamangalam Thiruvananthapuram* ABSTRACT Published
DRUG PROFILE KERALA MEDICAL JOURNAL Liraglutide: First Once-Daily Human GLP-1 Analogue Sreejith N Kumar Research Cell, IMA Kerala State, K-5, Kochar Road, Sasthamangalam Thiruvananthapuram* ABSTRACT Published
Update on GLP-1 Past Present Future
 Update on GLP-1 p Past Present Future Effects of GLP-1: Glucose Metabolism and Nutritional Balance L-Cells: Glp-1 release Betacellfollowing ingestion Stress Increases satiety reduces appetite Betacell-
Update on GLP-1 p Past Present Future Effects of GLP-1: Glucose Metabolism and Nutritional Balance L-Cells: Glp-1 release Betacellfollowing ingestion Stress Increases satiety reduces appetite Betacell-
PROCEEDINGS CLINICAL RESEARCH AND EXPERIENCE WITH INCRETIN-BASED THERAPIES * Vivian A. Fonseca, MD, FRCP ABSTRACT
 CLINICAL RESEARCH AND EXPERIENCE WITH INCRETIN-BASED THERAPIES Vivian A. Fonseca, MD, FRCP ABSTRACT Despite proven lifestyle recommendations and the availability of a range of oral antidiabetic agents,
CLINICAL RESEARCH AND EXPERIENCE WITH INCRETIN-BASED THERAPIES Vivian A. Fonseca, MD, FRCP ABSTRACT Despite proven lifestyle recommendations and the availability of a range of oral antidiabetic agents,
A Population Dose Response Model for Inhaled Technosphere Insulin Administered to Healthy Subjects
 Citation: CPT Pharmacometrics Syst. Pharmacol. (2017) 6, 365 372; VC 2017 ASCPT All rights reserved doi:10.1002/psp4.12189 ORIGINAL ARTICLE A Population Dose Response Model for Inhaled Technosphere Insulin
Citation: CPT Pharmacometrics Syst. Pharmacol. (2017) 6, 365 372; VC 2017 ASCPT All rights reserved doi:10.1002/psp4.12189 ORIGINAL ARTICLE A Population Dose Response Model for Inhaled Technosphere Insulin
Diabetes: Three Core Deficits
 Diabetes: Three Core Deficits Fat Cell Dysfunction Impaired Incretin Function Impaired Appetite Suppression Obesity and Insulin Resistance in Muscle and Liver Hyperglycemia Impaired Insulin Secretion Islet
Diabetes: Three Core Deficits Fat Cell Dysfunction Impaired Incretin Function Impaired Appetite Suppression Obesity and Insulin Resistance in Muscle and Liver Hyperglycemia Impaired Insulin Secretion Islet
Update on Insulin-based Agents for T2D. Harry Jiménez MD, FACE
 Update on Insulin-based Agents for T2D Harry Jiménez MD, FACE Harry Jiménez MD, FACE Has received honorarium as Speaker and/or Consultant for the following pharmaceutical companies: Eli Lilly Merck Boehringer
Update on Insulin-based Agents for T2D Harry Jiménez MD, FACE Harry Jiménez MD, FACE Has received honorarium as Speaker and/or Consultant for the following pharmaceutical companies: Eli Lilly Merck Boehringer
GLP-1 receptor agonists for type 2 diabetes currently available in the U.S.
 GLP-1 receptor agonists for type 2 diabetes currently available in the U.S. GLP-1 agonists are a class of antidiabetic agents that mimic the actions of the glucagon-like peptide. GLP-1 is one of several
GLP-1 receptor agonists for type 2 diabetes currently available in the U.S. GLP-1 agonists are a class of antidiabetic agents that mimic the actions of the glucagon-like peptide. GLP-1 is one of several
POPULATION PHARMACOKINETICS RAYMOND MILLER, D.Sc. Daiichi Sankyo Pharma Development
 POPULATION PHARMACOKINETICS RAYMOND MILLER, D.Sc. Daiichi Sankyo Pharma Development Definition Population Pharmacokinetics Advantages/Disadvantages Objectives of Population Analyses Impact in Drug Development
POPULATION PHARMACOKINETICS RAYMOND MILLER, D.Sc. Daiichi Sankyo Pharma Development Definition Population Pharmacokinetics Advantages/Disadvantages Objectives of Population Analyses Impact in Drug Development
SELECTED ABSTRACTS AND POSTER PRESENTATIONS
 SELECTED ABSTRACTS AND POSTER PRESENTATIONS The following summaries are based on abstracts and posters presented at the American Diabetes Association s 65th Annual Scientific Sessions held in San Diego,
SELECTED ABSTRACTS AND POSTER PRESENTATIONS The following summaries are based on abstracts and posters presented at the American Diabetes Association s 65th Annual Scientific Sessions held in San Diego,
Model-Based Approach to Predict Adherence to Protocol During Antiobesity Trials
 Modeling and Simulation Model-Based Approach to Predict Adherence to Protocol During Antiobesity Trials The Journal of Clinical Pharmacology 2018, 58(2) 240 253 C 2017, The Authors. The Journal of Clinical
Modeling and Simulation Model-Based Approach to Predict Adherence to Protocol During Antiobesity Trials The Journal of Clinical Pharmacology 2018, 58(2) 240 253 C 2017, The Authors. The Journal of Clinical
(maximum effect) model described the relationship between GLP-1 concentration and insulin release. The variability in the E max
 nature publishing group articles Pharmacokinetics and Pharmacodynamics of Inhaled GLP-1 (MKC253): Proof-of-Concept Studies in Healthy Normal Volunteers and in Patients With Type 2 Diabetes MT Marino 1,
nature publishing group articles Pharmacokinetics and Pharmacodynamics of Inhaled GLP-1 (MKC253): Proof-of-Concept Studies in Healthy Normal Volunteers and in Patients With Type 2 Diabetes MT Marino 1,
A model-based analysis to describe bedaquiline s exposure-response relationship and predict the impact of drugdrug interactions
 9th International Workshop on Clinical Pharmacology of TB Drugs 24 October 2016, Liverpool, UK A model-based analysis to describe bedaquiline s exposure-response relationship and predict the impact of
9th International Workshop on Clinical Pharmacology of TB Drugs 24 October 2016, Liverpool, UK A model-based analysis to describe bedaquiline s exposure-response relationship and predict the impact of
Society for Ambulatory Anesthesia Consensus Statement on Perioperative Blood Glucose Management in Diabetic Patients Undergoing Ambulatory Surgery
 Society for Ambulatory Anesthesia Consensus Statement on Perioperative Blood Glucose Management in Diabetic Patients Undergoing Ambulatory Surgery Girish P. Joshi, MB BS, MD, FFARCSI Anesthesia & Analgesia
Society for Ambulatory Anesthesia Consensus Statement on Perioperative Blood Glucose Management in Diabetic Patients Undergoing Ambulatory Surgery Girish P. Joshi, MB BS, MD, FFARCSI Anesthesia & Analgesia
Targeting Incretins in Type 2 Diabetes: Role of GLP-1 Receptor Agonists and DPP-4 Inhibitors. Richard E. Pratley and Matthew Gilbert
 REVIEW Targeting Incretins in Type 2 Diabetes: Role of GLP-1 Receptor Agonists and DPP-4 Inhibitors Richard E. Pratley and Matthew Gilbert Diabetes and Metabolism Translational Medicine Unit, University
REVIEW Targeting Incretins in Type 2 Diabetes: Role of GLP-1 Receptor Agonists and DPP-4 Inhibitors Richard E. Pratley and Matthew Gilbert Diabetes and Metabolism Translational Medicine Unit, University
Personalized therapeutics in diabetes
 Personalized therapeutics in diabetes Leen M. t Hart Molecular Cell Biology & Molecular Epidemiology Leiden University Medical Center Epidemiology & Biostatistics VU University Medical Center Diabetes
Personalized therapeutics in diabetes Leen M. t Hart Molecular Cell Biology & Molecular Epidemiology Leiden University Medical Center Epidemiology & Biostatistics VU University Medical Center Diabetes
Diabetes 2013: Achieving Goals Through Comprehensive Treatment. Session 2: Individualizing Therapy
 Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
BARIATRIC SURGERY AND TYPE 2 DIABETES MELLITUS
 BARIATRIC SURGERY AND TYPE 2 DIABETES MELLITUS George Vl Valsamakis European Scope Fellow Obesity Visiting iti Associate Prof Warwick Medical School Diabetes is an increasing healthcare epidemic throughout
BARIATRIC SURGERY AND TYPE 2 DIABETES MELLITUS George Vl Valsamakis European Scope Fellow Obesity Visiting iti Associate Prof Warwick Medical School Diabetes is an increasing healthcare epidemic throughout
Scottish Medicines Consortium
 Scottish Medicines Consortium saxagliptin, 5mg film-coated tablet (Onglyza ) No. (603/10) Bristol-Myers Squibb Pharmaceuticals Ltd 05 February 2010 The Scottish Medicines Consortium (SMC) has completed
Scottish Medicines Consortium saxagliptin, 5mg film-coated tablet (Onglyza ) No. (603/10) Bristol-Myers Squibb Pharmaceuticals Ltd 05 February 2010 The Scottish Medicines Consortium (SMC) has completed
Insulin Initiation and Intensification. Disclosure. Objectives
 Insulin Initiation and Intensification Neil Skolnik, M.D. Associate Director Family Medicine Residency Program Abington Memorial Hospital Professor of Family and Community Medicine Temple University School
Insulin Initiation and Intensification Neil Skolnik, M.D. Associate Director Family Medicine Residency Program Abington Memorial Hospital Professor of Family and Community Medicine Temple University School
Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes
 Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes Geneva Clark Briggs, PharmD, BCPS Adjunct Professor at University of Appalachia College of Pharmacy Clinical Associate, Medical
Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes Geneva Clark Briggs, PharmD, BCPS Adjunct Professor at University of Appalachia College of Pharmacy Clinical Associate, Medical
UKPDS: Over Time, Need for Exogenous Insulin Increases
 UKPDS: Over Time, Need for Exogenous Insulin Increases Patients Requiring Additional Insulin (%) 60 40 20 Oral agents By 6 Chlorpropamide years, Glyburide more than 50% of UKPDS patients required insulin
UKPDS: Over Time, Need for Exogenous Insulin Increases Patients Requiring Additional Insulin (%) 60 40 20 Oral agents By 6 Chlorpropamide years, Glyburide more than 50% of UKPDS patients required insulin
Optimizing Treatment Strategies to Improve Patient Outcomes in the Management of Type 2 Diabetes
 Optimizing Treatment Strategies to Improve Patient Outcomes in the Management of Type 2 Diabetes Philip Raskin, MD Professor of Medicine The University of Texas, Southwestern Medical Center NAMCP Spring
Optimizing Treatment Strategies to Improve Patient Outcomes in the Management of Type 2 Diabetes Philip Raskin, MD Professor of Medicine The University of Texas, Southwestern Medical Center NAMCP Spring
Incretin-based Therapies for Type 2 Diabetes Comparisons Between Glucagon-like Peptide-1 Receptor Agonists and Dipeptidyl Peptidase-4 Inhibitors
 Incretin-based Therapies for Type 2 Diabetes Comparisons Between Glucagon-like Peptide-1 Receptor Agonists and Dipeptidyl Peptidase-4 Inhibitors Timothy Bailey, MD, FACE, CPI Director, AMCR Institute,
Incretin-based Therapies for Type 2 Diabetes Comparisons Between Glucagon-like Peptide-1 Receptor Agonists and Dipeptidyl Peptidase-4 Inhibitors Timothy Bailey, MD, FACE, CPI Director, AMCR Institute,
NOVO NORDISK v SANOFI
 CASE AUTH/2600/4/13 NOVO NORDISK v SANOFI Promotion of Lyxumia Novo Nordisk complained about claims in a leavepiece, mailer and on exhibition panels used by Sanofi to promote Lyxumia (lixisenatide). Lyxumia
CASE AUTH/2600/4/13 NOVO NORDISK v SANOFI Promotion of Lyxumia Novo Nordisk complained about claims in a leavepiece, mailer and on exhibition panels used by Sanofi to promote Lyxumia (lixisenatide). Lyxumia
Liraglutide in Type 2 Diabetes Mellitus: Clinical Pharmacokinetics and Pharmacodynamics
 Clin Pharmacokinet (2016) 55:657 672 DOI 10.1007/s40262-015-0343-6 REVIEW ARTICLE Liraglutide in Type 2 Diabetes Mellitus: Clinical Pharmacokinetics and Pharmacodynamics Lisbeth V. Jacobsen 1 Anne Flint
Clin Pharmacokinet (2016) 55:657 672 DOI 10.1007/s40262-015-0343-6 REVIEW ARTICLE Liraglutide in Type 2 Diabetes Mellitus: Clinical Pharmacokinetics and Pharmacodynamics Lisbeth V. Jacobsen 1 Anne Flint
Diabetes Care Publish Ahead of Print, published online June 1, 2009
 Diabetes Care Publish Ahead of Print, published online June 1, 2009 Biphasic insulin aspart 30/70 (BIAsp 30): pharmacokinetics (PK) and pharmacodynamics (PD) in comparison with once-daily biphasic human
Diabetes Care Publish Ahead of Print, published online June 1, 2009 Biphasic insulin aspart 30/70 (BIAsp 30): pharmacokinetics (PK) and pharmacodynamics (PD) in comparison with once-daily biphasic human
Novel Formulations to Modify Mealtime Insulin Kinetics
 Novel Formulations to Modify Mealtime Insulin Kinetics Alan Krasner, Roderike Pohl, Patrick Simms, Philip Pichotta, Robert Hauser, Errol De Souza Biodel, Inc. Danbury, CT Disclosure All authors are employees
Novel Formulations to Modify Mealtime Insulin Kinetics Alan Krasner, Roderike Pohl, Patrick Simms, Philip Pichotta, Robert Hauser, Errol De Souza Biodel, Inc. Danbury, CT Disclosure All authors are employees
1 Introduction. Trine Høyer Rose 1,2 Daniel Röshammar. Johnny T. Ottesen 2
 Drugs R D (2016) 16:165 172 DOI 10.1007/s40268-016-0126-z ORIGINAL RESEARCH ARTICLE Characterisation of Population Pharmacokinetics and Endogenous Follicle-Stimulating Hormone (FSH) Levels After Multiple
Drugs R D (2016) 16:165 172 DOI 10.1007/s40268-016-0126-z ORIGINAL RESEARCH ARTICLE Characterisation of Population Pharmacokinetics and Endogenous Follicle-Stimulating Hormone (FSH) Levels After Multiple
Determination of Plasma Concentration Reference Ranges for Risperidone and Paliperidone
 Citation: CPT Pharmacometrics Syst. Pharmacol. (), ; VC ASCPT All rights reserved doi:./psp. ORIGINAL ARTICLE Determination of Plasma Concentration Reference Ranges for Risperidone and Paliperidone J Korell,
Citation: CPT Pharmacometrics Syst. Pharmacol. (), ; VC ASCPT All rights reserved doi:./psp. ORIGINAL ARTICLE Determination of Plasma Concentration Reference Ranges for Risperidone and Paliperidone J Korell,
Case Study in Placebo Modeling and Its Effect on Drug Development
 Case Study in Placebo Modeling and Its Effect on Drug Development Modeling and Simulation Strategy for Phase 3 Dose Selection of Dasotraline in Patients With Attention-Deficit/Hyperactivity Disorder Julie
Case Study in Placebo Modeling and Its Effect on Drug Development Modeling and Simulation Strategy for Phase 3 Dose Selection of Dasotraline in Patients With Attention-Deficit/Hyperactivity Disorder Julie
Model-based quantification of the relationship between age and anti-migraine therapy
 6 Model-based quantification of the relationship between age and anti-migraine therapy HJ Maas, M Danhof, OE Della Pasqua Submitted to BMC. Clin. Pharmacol. Migraine is a neurological disease that affects
6 Model-based quantification of the relationship between age and anti-migraine therapy HJ Maas, M Danhof, OE Della Pasqua Submitted to BMC. Clin. Pharmacol. Migraine is a neurological disease that affects
Pharmacometric Approaches to Guide Dose Selection of the Novel GPR40 Agonist TAK-875 in Subjects With Type 2 Diabetes Mellitus
 ORIGINAL ARTICLE Citation: CPT: Pharmacometrics & Systems Pharmacology (2013) 2, e22; doi:.3/psp.20.23 2013 AScpt All rights reserved 213-30/ www.nature.com/psp Pharmacometric Approaches to Guide Dose
ORIGINAL ARTICLE Citation: CPT: Pharmacometrics & Systems Pharmacology (2013) 2, e22; doi:.3/psp.20.23 2013 AScpt All rights reserved 213-30/ www.nature.com/psp Pharmacometric Approaches to Guide Dose
GLP 1 agonists Winning the Losing Battle. Dr Bernard SAMIA. KCS Congress: Impact through collaboration
 GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
Changing Diabetes: The time is now!
 Midwest Cardiovascular Research Foundation Welcomes DANITA HARRISON, ARNP Ms. Harrison discloses speaking relationships with Lilly, Novo Nordisk and Pfizer. Changing Diabetes: The time is now! Danita Harrison
Midwest Cardiovascular Research Foundation Welcomes DANITA HARRISON, ARNP Ms. Harrison discloses speaking relationships with Lilly, Novo Nordisk and Pfizer. Changing Diabetes: The time is now! Danita Harrison
DPP-4 inhibitor. The new class drug for Diabetes
 DPP-4 inhibitor The new class drug for Diabetes 1 Cause of Death in Korea 1 st ; Neoplasm 2 nd ; Cardiovascular Disease 3 rd ; Cerebrovascular Disease Diabetes 2 Incidence of Fatal or Nonfatal MI During
DPP-4 inhibitor The new class drug for Diabetes 1 Cause of Death in Korea 1 st ; Neoplasm 2 nd ; Cardiovascular Disease 3 rd ; Cerebrovascular Disease Diabetes 2 Incidence of Fatal or Nonfatal MI During
Liraglutide: the therapeutic promise from animal models
 REVIEW PAPER Liraglutide: the therapeutic promise from animal models L. B. Knudsen Novo Nordisk A S, Novo Nordisk Park, DK-2760, Måløv, Denmark Correspondence to: Lotte Bjerre Knudsen, Department Biology
REVIEW PAPER Liraglutide: the therapeutic promise from animal models L. B. Knudsen Novo Nordisk A S, Novo Nordisk Park, DK-2760, Måløv, Denmark Correspondence to: Lotte Bjerre Knudsen, Department Biology
Pramlintide & Weight. Diane M Karl MD. The Endocrine Clinic & Oregon Health & Science University Portland, Oregon
 Pramlintide & Weight Diane M Karl MD The Endocrine Clinic & Oregon Health & Science University Portland, Oregon Conflict of Interest Speakers Bureau: Amylin Pharmaceuticals Consultant: sanofi-aventis Grant
Pramlintide & Weight Diane M Karl MD The Endocrine Clinic & Oregon Health & Science University Portland, Oregon Conflict of Interest Speakers Bureau: Amylin Pharmaceuticals Consultant: sanofi-aventis Grant
MOA: Long acting glucagon-like peptide 1 receptor agonist
 Alexandria Rydz MOA: Long acting glucagon-like peptide 1 receptor agonist Increases glucose dependent insulin secretion Decreases inappropriate glucagon secretion Increases β- cell growth and replication
Alexandria Rydz MOA: Long acting glucagon-like peptide 1 receptor agonist Increases glucose dependent insulin secretion Decreases inappropriate glucagon secretion Increases β- cell growth and replication
Dulaglutide (LY ) for the treatment of type 2 diabetes
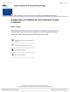 Expert Review of Clinical Pharmacology ISSN: 1751-2433 (Print) 1751-2441 (Online) Journal homepage: http://www.tandfonline.com/loi/ierj20 (LY-2189265) for the treatment of type 2 diabetes André J. Scheen
Expert Review of Clinical Pharmacology ISSN: 1751-2433 (Print) 1751-2441 (Online) Journal homepage: http://www.tandfonline.com/loi/ierj20 (LY-2189265) for the treatment of type 2 diabetes André J. Scheen
Non-insulin treatment in Type 1 DM Sang Yong Kim
 Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Abstract. Effect of sitagliptin on glycemic control in patients with type 2 diabetes. Introduction. Abbas Mahdi Rahmah
 Effect of sitagliptin on glycemic control in patients with type 2 diabetes Abbas Mahdi Rahmah Correspondence: Dr. Abbas Mahdi Rahmah Consultant Endocrinologist, FRCP (Edin) Director of Iraqi National Diabetes
Effect of sitagliptin on glycemic control in patients with type 2 diabetes Abbas Mahdi Rahmah Correspondence: Dr. Abbas Mahdi Rahmah Consultant Endocrinologist, FRCP (Edin) Director of Iraqi National Diabetes
What to Do After Basal Insulin
 BasalINSULIN What to Do After Basal Insulin 3 Treatment Strategies for Type 2 Diabetes These strategies can help you optimize glucose control in your patient with type 2 diabetes when basal insulin alone
BasalINSULIN What to Do After Basal Insulin 3 Treatment Strategies for Type 2 Diabetes These strategies can help you optimize glucose control in your patient with type 2 diabetes when basal insulin alone
Current Status of Incretin Based Therapies in Type 2 Diabetes
 Current Status of Incretin Based Therapies in Type 2 Diabetes DR.M.Mukhyaprana Prabhu Professor of Internal Medicine Kasturba Medical College, Manipal, Manipal University, India 2 nd International Endocrine
Current Status of Incretin Based Therapies in Type 2 Diabetes DR.M.Mukhyaprana Prabhu Professor of Internal Medicine Kasturba Medical College, Manipal, Manipal University, India 2 nd International Endocrine
New Treatments for Type 2 diabetes. Nandini Seevaratnam April 2016 Rushcliffe Patient Forum
 New Treatments for Type 2 diabetes Nandini Seevaratnam April 2016 Rushcliffe Patient Forum Overview Growing population of Type 2 diabetes Basic science on what goes wrong Current treatments Why there is
New Treatments for Type 2 diabetes Nandini Seevaratnam April 2016 Rushcliffe Patient Forum Overview Growing population of Type 2 diabetes Basic science on what goes wrong Current treatments Why there is
PK-PD modelling to support go/no go decisions for a novel gp120 inhibitor
 PK-PD modelling to support go/no go decisions for a novel gp120 inhibitor Phylinda LS Chan Pharmacometrics, Pfizer, UK EMA-EFPIA Modelling and Simulation Workshop BOS1 Pharmacometrics Global Clinical Pharmacology
PK-PD modelling to support go/no go decisions for a novel gp120 inhibitor Phylinda LS Chan Pharmacometrics, Pfizer, UK EMA-EFPIA Modelling and Simulation Workshop BOS1 Pharmacometrics Global Clinical Pharmacology
GLP-1 receptor agonists for type 2 diabetes A rationale drug. development. Bo Ahrén
 PROF. BO AHREN (Orcid ID : 0000-0002-9804-5340) Article type : Mini Review GLP-1 receptor agonists for type 2 diabetes A rationale drug development Bo Ahrén Department of Clinical Sciences Lund, Lund University,
PROF. BO AHREN (Orcid ID : 0000-0002-9804-5340) Article type : Mini Review GLP-1 receptor agonists for type 2 diabetes A rationale drug development Bo Ahrén Department of Clinical Sciences Lund, Lund University,
Gut hormones KHATTAB
 Gut hormones PROF:ABD ALHAFIZ HASSAN KHATTAB Gut as an endocrine gland The talk will cover the following : Historical background. Why this subject is chosen. Gastro-intestinal hormones and their function.
Gut hormones PROF:ABD ALHAFIZ HASSAN KHATTAB Gut as an endocrine gland The talk will cover the following : Historical background. Why this subject is chosen. Gastro-intestinal hormones and their function.
Ignacio Cortínez Anesthesiology Department School of Medicine, Pontificia Universidad Católica de Chile
 Recommended doses of Levobupivacaine for TAP Blocks: Development of a pharmacokinetic model and estimation of the risk of symptoms of local anesthetic systemic toxicity Ignacio Cortínez Anesthesiology
Recommended doses of Levobupivacaine for TAP Blocks: Development of a pharmacokinetic model and estimation of the risk of symptoms of local anesthetic systemic toxicity Ignacio Cortínez Anesthesiology
