An Update on the Standards of Medical Care in Diabetes 2017, With an Eye Toward 2018
|
|
|
- Bryan Richards
- 5 years ago
- Views:
Transcription
1 An Update on the Standards of Medical Care in Diabetes 2017, With an Eye Toward 2018 Erika Gebel Berg, PhD Director, Scientific and Medical Affairs Corresponding Author, ADA s Standards of Medical in Diabetes American Diabetes Association
2 Standards of Care (SOC)
3 Standards of Care Funded out of the Association s general revenues and does not use industry support. Published annually since 1989 Reviewed and approved by the Association s Board of Directors.
4 Process ADA s Professional Practice Committee (PPC) conducts annual review & revision of the SOC. Searched Medline for human studies related to each subsection and published since January 1, Recommendations revised per new evidence, for clarity, or to better match text to strength of evidence.
5 Process PPC compiles new evidence into a table including new and proposed recommendations alongside supporting research/rationale The PPC has an in-person meeting to debate the final language of the recommendations Some sections receive external review
6 2018 Watch: General Changes Standards will be ADA s sole source of Clinical Practice Recommendations The PPC will continue to update the Standards annually, but has the option to update more frequently online should the PPC determine that new evidence or regulatory changes merit immediate incorporation into the Standards ADA will begin taking proposals from the community for statements, consensus reports, scientific reviews, and clinical/research conferences Coming in February: Interactive Standards of Care App with interactive tools Professional.diabetes.org/SOC
7 Professional Practice Committee Tamara Darsow, PhD Matt Petersen William Cefalu, MD Christopher Cannon, MD Judith Fradkin, MD David Maahs, MD, PhD Medha N. Munshi, MD* Guillermo E. Umpierrez*
8
9 Updates in the SOC The following presentation will focus on specific changes in each section of the Standards of Care 2017 compared to previous years A discussion of what s been debated for 2018 The full version of the Standards of Care 2018 can be downloaded on December 8: Professional.diabetes.org/SOC
10 1. Improving Care and Promoting Health in Populations
11 Care Delivery Systems 33-49% of patients still do not meet targets for A1C, blood pressure, or lipids. 14% meet targets for all A1C, BP, lipids, and nonsmoking status. Progress in CVD risk factor control is slowing. Substantial system-level improvements are needed. Delivery system is fragmented, lacks clinical information capabilities, duplicates services & is poorly designed. American Diabetes Association Standards of Medical Care in Diabetes. Promoting Health and Reducing Disparities in Populations. Diabetes Care 2017; 40 (Suppl. 1): S6-S10
12 Strategies for System-Level Improvement Provide care that is concordant-with evidence-based guidelines Expand role of teams Track medication-taking behavior at a systems level Removing financial barriers New emphasis for 2018: Using data/ehr tools to improve processes, health outcomes, and reduce costs American Diabetes Association Standards of Medical Care in Diabetes. Promoting Health and Reducing Disparities in Populations. Diabetes Care 2017; 40 (Suppl. 1): S6-S10
13 Tailoring Treatment for Social Context Key Recommendation Providers should assess social context, including potential food insecurity, housing stability, and financial barriers, and apply that information to treatment decisions. A American Diabetes Association Standards of Medical Care in Diabetes. Promoting Health and Reducing Disparities in Populations. Diabetes Care 2017; 40 (Suppl. 1): S6-S10
14 Tailoring Treatment for Social Context Key Recommendations Patients should be referred to local community resources when available. B Patients should be provided with selfmanagement support from lay health coaches, navigators, or community health workers when available. A American Diabetes Association Standards of Medical Care in Diabetes. Promoting Health and Reducing Disparities in Populations. Diabetes Care 2017; 40 (Suppl. 1): S6-S10
15 Tailoring Treatment For Social Context Social Determinants of Health Food Insecurity Language Barriers Homelessness American Diabetes Association Standards of Medical Care in Diabetes. Promoting Health and Reducing Disparities in Populations. Diabetes Care 2017; 40 (Suppl. 1): S6-S10
16 2. Classification and Diagnosis of Diabetes
17 Nearly 1 in 4 four adults living with diabetes 7.2 million Americans didn t know they had the condition. Only 11.6 percent of adults with prediabetes knew they had it The National Diabetes Statistics Report, 2017
18 Recommendations: Screening for prediabetes/diabetes Screening with an informal assessment of risk factors or validated tools should be considered in asymptomatic adults. B Consider testing in asymptomatic adults of any age with BMI 25 kg/m 2 or 23 kg/m 2 in Asian Americans who have 1 or more add l dm risk factors. B For all patients, testing should begin at age 45 years. B If tests are normal, repeat testing carried out at a minimum of 3-year intervals is reasonable. C American Diabetes Association Standards of Medical Care in Diabetes. Classification and diagnosis of diabetes. Diabetes Care 2017; 40 (Suppl. 1): S11-S24
19 Risk factors for Prediabetes and T2D American Diabetes Association Standards of Medical Care in Diabetes. Classification and diagnosis of diabetes. Diabetes Care 2017; 40 (Suppl. 1): S11-S24
20 Recommendations: Screening for prediabetes/diabetes FPG, 2-h PG after 75-g OGTT, and the A1C are equally appropriate. B 2018 Watch: Expanded discussion on appropriate use of A1C In patients with diabetes, identify and, if appropriate, treat other CVD risk factors. B American Diabetes Association Standards of Medical Care in Diabetes. Classification and diagnosis of diabetes. Diabetes Care 2017; 40 (Suppl. 1): S11-S24
21 Criteria for Testing for T2DM in Children & Adolescents Overweight or Obesity Risk Factors Family history of type 2 diabetes in 1 st or 2 nd degree relative Race/ethnicity Signs of insulin resistance or conditions associated with insulin resistance Maternal history of diabetes or GDM Changing for 2018 based on new position statement American Diabetes Association Standards of Medical Care in Diabetes. Classification and diagnosis of diabetes. Diabetes Care 2017; 40 (Suppl. 1): S11-S24
22 3. Comprehensive Medical Evaluation and Assessment of Comorbidities
23 Patient-Centered Collaborative Care Defines a patient-centered communication style Expert Task Force convened by ADA and AADE published a paper on the use of language in diabetes care and education American Diabetes Association Standards of Medical Care in Diabetes. Comprehensive Medical Evaluation and Assessment of Comorbidities. Diabetes Care 2017; 40 (Suppl. 1): S25-S32
24 Comprehensive Medical Evaluation A complete medical evaluation should be performed at the initial visit to: Confirm & classify diagnosis B Detect complications & potential comorbid conditions E Review prior treatment & risk factor control E Begin formulation of care management plan B Develop a continuing care plan B American Diabetes Association Standards of Medical Care in Diabetes. Comprehensive Medical Evaluation and Assessment of Comorbidities. Diabetes Care 2017; 40 (Suppl. 1): S25-S32
25 Comprehensive Medical Evaluation Improved Evaluation Checklist Table for 2018 American Diabetes Association Standards of Medical Care in Diabetes. Comprehensive Medical Evaluation and Assessment of Comorbidities. Diabetes Care 2017; 40 (Suppl. 1): S25-S32
26 Common Comorbidities Autoimmune Diseases (T1D) Cancer Cognitive Impairment Dementia Fatty Liver Disease Fractures Hearing Impairment HIV Low Testosterone (Men) Obstructive Sleep Apnea Periodontal Disease Psychosocial Disorders American Diabetes Association Standards of Medical Care in Diabetes. Comprehensive Medical Evaluation and Assessment of Comorbidities. Diabetes Care 2017; 40 (Suppl. 1): S25-S32
27 Anxiety Disorders Consider screening for anxiety in people exhibiting anxiety or worries regarding diabetes complications, insulin injections or infusion, taking medications, and/or hypoglycemia that interfere with selfmanagement behaviors. Refer for treatment if anxiety is present. B Persons with hypoglycemic unawareness, which can co-occur with fear of hypoglycemia, should be treated using blood glucose awareness training (or other evidence-based similar intervention) to help re-establish awareness of hypoglycemia and reduce fear of hypoglycemia. A American Diabetes Association Standards of Medical Care in Diabetes. Comprehensive Medical Evaluation and Assessment of Comorbidities. Diabetes Care 2017; 40 (Suppl. 1): S25-S32
28 Depression Consider annual screening with age-appropriate depression screening measures. B Beginning at dx of complications or when there are significant changes in medical status, consider assessment for depression. B Referrals for treatment of depression should be made to mental health providers with experience using evidence-based treatment approaches. A American Diabetes Association Standards of Medical Care in Diabetes. Comprehensive Medical Evaluation and Assessment of Comorbidities. Diabetes Care 2017; 40 (Suppl. 1): S25-S32
29 Disordered Eating Behavior Consider reevaluating the treatment regimen in people with diabetes who present with symptoms of disordered eating. B Consider screening for disordered eating using validated screening measures when hyperglycemia and weight loss are unexplained based on self-reported behaviors. B American Diabetes Association Standards of Medical Care in Diabetes. Comprehensive Medical Evaluation and Assessment of Comorbidities. Diabetes Care 2017; 40 (Suppl. 1): S25-S32
30 Serious Mental Illness Annually screen people who are prescribed atypical antipsychotic medications for prediabetes or diabetes. B If a second-generation antipsychotic medication is prescribed, changes in weight, glycemic control, and cholesterol levels should be carefully monitored. C Incorporate monitoring of diabetes self-care activities into treatment goals in people with diabetes and serious mental illness. B American Diabetes Association Standards of Medical Care in Diabetes. Comprehensive Medical Evaluation and Assessment of Comorbidities. Diabetes Care 2017; 40 (Suppl. 1): S25-S32
31 4. Lifestyle Management
32 Recommendations: Physical Activity Children with diabetes/prediabetes: at least 60 min/day physical activity B Most adults with type 1 C and type 2 B diabetes: 150+ min/wk of moderate-to-vigorous activity over at least 3 days/week with no more than 2 consecutive days without exercise. Shorter durations (minimum 75 min/week) of vigorousintensity or interval training may be sufficient for younger and more physically fit individuals. Adults with type 1 C and type 2 B diabetes should perform resistance training in 2-3 sessions/week on nonconsecutive days American Diabetes Association Standards of Medical Care in Diabetes. Lifestyle Management. Diabetes Care 2017; 40 (Suppl. 1): S33-43
33 Recommendations: Physical Activity All adults, and particularly those with type 2 diabetes, should decrease the amount of time spent in daily sedentary behavior. B Prolonged sitting should be interrupted every 30 min for blood glucose benefits, particularly in adults with type 2 diabetes. C Flexibility training and balance training are recommended 2 3 times/week for older adults with diabetes. Yoga and tai chi may be included based on individual preferences to increase flexibility, muscular strength, and balance. C American Diabetes Association Standards of Medical Care in Diabetes. Lifestyle Management. Diabetes Care 2017; 40 (Suppl. 1): S33-43
34 Recommendations: Psychosocial Care Psychosocial care should be provided to all people with diabetes, with the goals of optimizing health outcomes and QOL. A Psychosocial screening and follow-up include: Attitudes Expectations for medical mgmt. & outcomes Affect/mood American Diabetes Association Standards of Medical Care in Diabetes. Lifestyle Management. Diabetes Care 2017; 40 (Suppl. 1): S33-43 Quality-of-life (QOL) Resources- financial, social & emotional Psychiatric history E
35 Recommendations: Psychosocial Care Providers should consider assessment for symptoms of diabetes distress, depression, anxiety, disordered eating, and cognitive capacities using patient-appropriate standardized and validated tools at the initial visit, at periodic intervals, and when there is a change in disease, treatment, or life circumstance. B Consider screening older adults (aged 65 years) with diabetes for cognitive impairment and depression. B American Diabetes Association Standards of Medical Care in Diabetes. Lifestyle Management. Diabetes Care 2017; 40 (Suppl. 1): S33-43
36 Diabetes distress Diabetes Distress Very common and distinct from other psychological disorders Negative psychological reactions related to emotional burdens of managing a demanding chronic disease Recommendation: Routinely monitor people with diabetes for diabetes distress, particularly when treatment targets are not met and/or at the onset of diabetes complications. B American Diabetes Association Standards of Medical Care in Diabetes. Lifestyle Management. Diabetes Care 2017; 40 (Suppl. 1): S33-43
37 Referral for Psychosocial Care American Diabetes Association Standards of Medical Care in Diabetes. Lifestyle Management. Diabetes Care 2017; 40 (Suppl. 1): S33-43
38 2018 Watch Emphasis on technology-based platforms for the delivery of diabetes self-management education Text updates to clarify that there IS NO ADA DIET. The Standards say that there is no ideal macronutrient distribution and that eating plans should be individualized.
39 5. Prevention or Delay of Type 2 Diabetes
40 Recommendations: Prevention or Delay of T2DM Patients with prediabetes should be referred to an intensive diet and physical activity behavioral counseling program adhering to the tenets of the DPP targeting a loss of 7% of body weight, and should increase their moderate physical activity to at least 150 min/week. A American Diabetes Association Standards of Medical Care in Diabetes. Prevention or delay of type 2 diabetes. Diabetes Care 2017; 40 (Suppl. 1): S44-S47
41 Recommendations: Prevention or Delay of T2DM Based on cost-effectiveness of diabetes prevention, such programs should be covered by third-party payers. B Metformin therapy for prevention of type 2 diabetes should be considered in those with prediabetes, especially for those with BMI >35 kg/m 2, aged < 60 years, women with prior gestational diabetes (GDM), those with rising A1C despite lifestyle intervention. A American Diabetes Association Standards of Medical Care in Diabetes. Prevention or delay of type 2 diabetes. Diabetes Care 2017; 40 (Suppl. 1): S44-S47
42 New 2017 Recommendation: Prevention or Delay of T2DM Long-term use of metformin may be associated with biochemical vitamin B12 deficiency, and periodic measurement of vitamin B12 levels should be considered in metformin-treated patients, especially in those with anemia or peripheral neuropathy. B American Diabetes Association Standards of Medical Care in Diabetes. Prevention or delay of type 2 diabetes. Diabetes Care 2017; 40 (Suppl. 1): S44-S47
43 Recommendations: Prevention or Delay of T2DM Monitor at least annually for the development of diabetes in those with prediabetes. E Screening for and treatment of modifiable risk factors for CVD is suggested. B American Diabetes Association Standards of Medical Care in Diabetes. Prevention or delay of type 2 diabetes. Diabetes Care 2017; 40 (Suppl. 1): S44-S47
44 Recommendations: Prevention or Delay of T2DM DSME and DSMS programs are appropriate for people with prediabetes to receive education and support to develop and maintain behaviors that can prevent or delay the onset of diabetes. B Technology assisted tools can be useful elements of effective lifestyle modification to prevent diabetes. B American Diabetes Association Standards of Medical Care in Diabetes. Prevention or delay of type 2 diabetes. Diabetes Care 2017; 40 (Suppl. 1): S44-S47
45 6. Glycemic Targets
46
47 CGM in the New Lots of new CGM data and regulatory changes New flash CGM approved for adults due to significant differences between flash CGM and other CGM devices, more discussion is needed on outcomes and regarding specific recommendations. SMBG requirements changed
48 Classification of Hypoglycemia American Diabetes Association Standards of Medical Care in Diabetes. Glycemic targets. Diabetes Care 2017; 40 (Suppl. 1): S48-S56
49 Recommendations: Hypoglycemia Individuals at risk for hypoglycemia should be asked about symptomatic and asymptomatic hypoglycemia at each encounter. C Glucose (15 20 g) preferred treatment for conscious individual with blood glucose < 70 mg/dl. E Glucagon should be prescribed for those at increased risk of clinically significant hypoglycemia, defined as blood glucose < 54 mg/dl, so it is available if needed. E Hypoglycemia unawareness or episodes of severe hypoglycemia should trigger treatment re-evaluation. E American Diabetes Association Standards of Medical Care in Diabetes. Glycemic targets. Diabetes Care 2017; 40 (Suppl. 1): S48-S56
50 7. Obesity Management for the Treatment of Type 2 Diabetes
51 Recommendations: Assessment At each patient encounter, BMI should be calculated and documented in the medical record. B Discuss with the patient Asian American cutpoints: Normal <23 BMI kg/m 2 Overweight kg/m 2 Obese kg/m 2 Extremely obese 37.5 kg/m 2 American Diabetes Association Standards of Medical Care in Diabetes. Obesity management for the treatment of type 2 diabetes. Diabetes Care 2017; 40 (Suppl. 1): S57-S63
52 Overweight/Obesity Treatment Body Mass Index Category (kg/m 2 ) Treatment Diet, physical activity & behavioral therapy 23.0* or * or Pharmacotherapy Metabolic surgery * Asian-American individuals Treatment may be indicated for selected, motivated patients. American Diabetes Association Standards of Medical Care in Diabetes. Obesity management for the treatment of type 2 diabetes. Diabetes Care 2017; 40 (Suppl. 1): S57-S63
53 Metabolic Surgery Evidence supports gastrointestinal operations as effective treatments for overweight T2DM patients. Randomized controlled trials with postoperative follow-up ranging from 1 to 5 years have documented sustained diabetes remission in 30 63% of patients, though erosion of remission occurs in 35-50% or more. With or without diabetes relapse, the majority of patients who undergo surgery maintain substantial improvement of glycemic control for at least 5 to 15 years American Diabetes Association Standards of Medical Care in Diabetes. Obesity management for the treatment of type 2 diabetes. Diabetes Care 2017; 40 (Suppl. 1): S57-S63
54 Recommendations: Metabolic Surgery Metabolic surgery should be recommended as an option to treat T2DM for all appropriate surgical candidates with BMIs > 40 (37.5*) and those with BMIs ( *) when hyperglycemia is inadequately controlled despite lifestyle & optimal medical therapy. A Metabolic surgery should be considered for the treatment of T2DM in adults with BMIs ( *) when hyperglycemia is inadequately controlled despite optimal medical control by either oral or injectable medications (including insulin). B Metabolic surgery should be performed in high-volume centers with multidisciplinary teams that understand and are experienced in the management of diabetes and gastrointestinal surgery. C American Diabetes Association Standards of Medical Care in Diabetes. Obesity management for the treatment of type 2 diabetes. Diabetes Care 2017; 40 (Suppl. 1): S57-S63
55 Recommendations: Metabolic Surgery Long-term lifestyle support and routine monitoring of micronutrient/nutritional status must be provided after surgery. C People presenting for metabolic surgery should receive a comprehensive mental health assessment. B Surgery should be postponed in patients with histories of alcohol or substance abuse, significant depression, suicidal ideation, or other mental health conditions until these conditions have been fully addressed. E People who undergo metabolic surgery should be evaluated to assess the need for ongoing mental health services to help them adjust to medical and psychosocial changes after surgery. C American Diabetes Association Standards of Medical Care in Diabetes. Obesity management for the treatment of type 2 diabetes. Diabetes Care 2017; 40 (Suppl. 1): S57-S63
56 Costly Adverse Effects Some associated risks Outcomes vary Patients undergoing metabolic surgery may be at higher risk for depression, substance abuse, and other psychosocial issues American Diabetes Association Standards of Medical Care in Diabetes. Obesity management for the treatment of type 2 diabetes. Diabetes Care 2017; 40 (Suppl. 1): S57-S63
57 8. Pharmacologic Approaches to Glycemic Treatment
58 Recommendations: Pharmacologic Therapy For Type 1 Diabetes Most people with T1DM should be treated with multiple daily injections of prandial insulin and basal insulin or continuous subcutaneous insulin infusion (CSII). A Individuals who have been successfully using CSII should have continued access after they turn 65 years old. E American Diabetes Association Standards of Medical Care in Diabetes. Approaches to glycemic treatment. Diabetes Care 2017; 40 (Suppl. 1): S64-S74
59 2018 Watch: Diabetes Medications and CVOT DPP-4 Inhibitors GLP-1 Receptor Agonists SGLT2 Inhibitors SAVOR-TIMI 53 (129) (n = 16,492) EXAMINE (144) (n = 5,380) TECOS (132) (n = 14,671) ELIXA (139) (n = 6,068) LEADER (137) (n = 9,340) SUSTAIN-6 (138)* (n = 3,297) EXSCEL (140) (n = 14,752) EMPA-REG OUTCOME (133) (n = 7,020) CANVAS (135) (n = 4,330) CANVAS-R (135) (n=5812) Intervention Saxagliptin/ Placebo Alogliptin/ placebo Sitagliptin/ placebo Lixisenatide/ placebo Liraglutide/ placebo Semaglutide/ placebo Exenatide QW/ placebo Empagliflozin/ placebo Canagliflozin vs. placebo Main inclusion criteria T2D/ history of or multiple risk factors for CVD T2D/ ACS within days before randomization T2D and preexisting CVD Type 2 diabetes and history of ACS (<180 days) T2D/ CVD, renal T2D/CVD at >50 disease, or HF, at years of age or >50 years of age or CV risk at >60 years of age CV risk at >60 years of age T2D/with or T2D/ preexisting CVD without known CVD or additional risk factors for CVD T2D/g CVD at >30 years of age or CV risk at >50 years of age Prior CVD/CHF (%) 78/13 100/28 74/18 100/22 81/18 59/ / / /14.4 Primary outcome 3-point MACE HR 1.00 ( ) 3-point MACE HR 0.96 (>1.16) 4-point MACE HR 0.98 ( ) 4-point MACE HR 1.02 ( ) 3-point MACE HR 0.87 ( ) 3-point MACE HR 0.74 ( ) 3-point MACE HR 0.91 ( ) (ITT) HR 0.95 ( ) 3-point MACE 3-point MACE Progression to HR 0.86 ( ) HR 0.86 (0.75 albuminuria** 0.97) HR 0.73 ( ) PP
60 New Recommendation: Pharmacologic Therapy For T2DM In patients with long-standing suboptimally controlled type 2 diabetes and established atherosclerotic cardiovascular disease, empagliflozin or liraglutide should be considered as they have been shown to reduce cardiovascular and all-cause mortality when added to standard care. Ongoing studies are investigating the cardiovascular benefits of other agents in these drug classes. B American Diabetes Association Standards of Medical Care in Diabetes. Approaches to glycemic treatment. Diabetes Care 2017; 40 (Suppl. 1): S64-S74
61 2018 Watch New type 2 diabetes treatment algorithm New table including drug effects and patient factors to help guide treatment choices as part of patient-provider shared decision making.
62
63 Recommendations: Pharmacological Therapy For T2DM If noninsulin monotherapy at maximal tolerated dose does not achieve or maintain the A1C target over 3 months, add a second oral agent, a GLP-1 receptor agonist, or basal insulin. A Use a patient-centered approach to guide choice of pharmacologic agents. E Don t delay insulin initiation in patients not achieving glycemic goals. B American Diabetes Association Standards of Medical Care in Diabetes. Approaches to glycemic treatment. Diabetes Care 2017; 40 (Suppl. 1): S64-S74
64 Recommendations: Pharmacologic Therapy For T2DM Metformin, if not contraindicated and if tolerated, is the preferred initial pharmacologic agent for T2DM. A Consider insulin therapy (with or without additional agents) in patients with newly dx d T2DM who are markedly symptomatic and/or have elevated blood glucose levels (>300 mg/dl) or A1C (>10%). E American Diabetes Association Standards of Medical Care in Diabetes. Approaches to glycemic treatment. Diabetes Care 2017; 40 (Suppl. 1): S64-S74
65 Combination Injectable Therapy in T2DM American Diabetes Association Standards of Medical Care in Diabetes. Approaches to glycemic treatment. Diabetes Care 2017; 40 (Suppl. 1): S64-S74
66
67 Average wholesale price (AWP) does not necessarily reflect discounts, rebates, or other price adjustments that may affect the actual cost incurred by the patient but highlights the importance of cost considerations.
68 There have been substantial increases in the price of insulin in the past decade, and costeffectiveness is an important consideration.
69 9. Cardiovascular Disease and Risk Management
70 Cardiovascular Disease CVD is the leading cause of morbidity & mortality for those with diabetes. Largest contributor to direct/indirect costs Common conditions coexisting with type 2 diabetes (e.g., hypertension, dyslipidemia) are clear risk factors for ASCVD. Diabetes itself confers independent risk Control individual cardiovascular risk factors to prevent/slow CVD in people with diabetes. Systematically assess all patients with diabetes for cardiovascular risk factors. American Diabetes Association Standards of Medical Care in Diabetes. Cardiovascular disease and risk management. Diabetes Care 2017; 40 (Suppl. 1): S75-S87
71 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for ASCVD & microvascular complications In T1DM, HTN often results from underlying kidney disease. In T2DM, HTN coexists with other cardiometabolic risk factors. American Diabetes Association Standards of Medical Care in Diabetes. Cardiovascular disease and risk management. Diabetes Care 2017; 40 (Suppl. 1): S75-S87
72 Hypertension
73
74 Recommendations: Hypertension/ Blood Pressure Treatment Patients with BP >120/80 should be advised on lifestyle changes to reduce BP. B Patients with confirmed BP >140/90 should, in addition to lifestyle therapy, have prompt initiation and timely subsequent titration of pharmacological therapy to achieve blood pressure goals. A American Diabetes Association Standards of Medical Care in Diabetes. Cardiovascular disease and risk management. Diabetes Care 2017; 40 (Suppl. 1): S75-S87
75 Recommendations: Hypertension/ Blood Pressure Treatment Patients with confirmed office-based blood pressure >160/100mmHg should, in addition to lifestyle therapy, have prompt initiation and timely titration of two drugs or a single pill combination of drugs demonstrated to reduce cardiovascular events in patients with diabetes. A Lifestyle intervention including: Weight loss if overweight DASH-style diet Moderation of alcohol intake Increased physical activity American Diabetes Association Standards of Medical Care in Diabetes. Cardiovascular disease and risk management. Diabetes Care 2017; 40 (Suppl. 1): S75-S87
76 Recommendations: Hypertension/ Blood Pressure Treatment Treatment for hypertension should include A ACE inhibitor Angiotensin II receptor blocker (ARB) Thiazide-like diuretic Dihydropyridine calcium channel blockers Multiple drug therapy (two or more agents at maximal doses) generally required to achieve BP targets. American Diabetes Association Standards of Medical Care in Diabetes. Cardiovascular disease and risk management. Diabetes Care 2017; 40 (Suppl. 1): S75-S87
77 Recommendations: Hypertension/ Blood Pressure Treatment An ACE inhibitor or angiotensin receptor blocker, at the maximum tolerated dose indicated for blood pressure treatment, is the recommended first-line treatment for hypertension in patients with diabetes and urinary albumin to creatinine ratio >300 mg/g creatinine (A) or mg/g creatinine (B). If one class is not tolerated, the other should be substituted. B American Diabetes Association Standards of Medical Care in Diabetes. Cardiovascular disease and risk management. Diabetes Care 2017; 40 (Suppl. 1): S75-S87
78 2018 Watch: Lipids What to do about PCSK9 Inhibitors? Simplified risk stratification scheme based on presence of two factors: Age and ASCVD American Diabetes Association Standards of Medical Care in Diabetes. Cardiovascular disease and risk management. Diabetes Care 2017; 40 (Suppl. 1): S75-S87
79 10. Microvascular Complications and Foot Care
80 Recommendations: Diabetic Retinopathy To reduce the risk or slow the progression of retinopathy Optimize glycemic control A Optimize blood pressure control A American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care 2017; 40 (Suppl. 1): S88-S98
81 Recommendations: Diabetic Retinopathy Screening: Initial dilated and comprehensive eye examination by an ophthalmologist or optometrist: Adults with type 1 diabetes, within 5 years of diabetes onset. B Patients with type 2 diabetes at the time of diabetes diagnosis. B American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care 2017; 40 (Suppl. 1): S88-S98
82 Recommendations: Diabetic Retinopathy Screening (2): If no evidence of retinopathy for one or more eye exam, exams every 2 years may be considered. B If diabetic retinopathy is present, subsequent examinations should be repeated at least annually by an ophthalmologist or optometrist. B If retinopathy is progressing or sight-threatening, more frequent exams required. B American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care 2017; 40 (Suppl. 1): S88-S98
83 2018 Watch: Diabetic Retinopathy Treatment: Ranibizumab (Anti-VEGF treatment) has a new indication for diabetic retinopathy Non-inferiority with traditional panretinal laser photocoagulation therapy Pros and Cons discussed
84 Neuropathy Early recognition & management is important because: 1. DN is a diagnosis of exclusion. 2. Numerous treatment options exist. 3. Up to 50% of DPN may be asymptomatic. 4. Recognition & treatment may improve symptoms, reduce sequelae, and improve quality-of-life. American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care 2017; 40 (Suppl. 1): S88-S98
85 Screening: Recommendations: Neuropathy Assess all patients for DPN at dx for T2DM, 5 years after dx for T1DM, and at least annually thereafter. B Assessment should include history & 10g monofilament testing, vibration sensation (large-fiber function), and temperature or pinprick (small-fiber function) B Symptoms of autonomic neuropathy should be assessed in patients with microvascular & neuropathic complications. E American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care 2017; 40 (Suppl. 1): S88-S98
86 Recommendations: Neuropathy (2) Treatment: Optimize glucose control to prevent or delay the development of neuropathy in patients with T1DM A & to slow progression in patients with T2DM. B Assess & treat patients to reduce pain related to DPN B and symptoms of autonomic neuropathy and to improve quality of life. E American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care 2017; 40 (Suppl. 1): S88-S98
87 New Recommendation: Neuropathy (3) Treatment: Either pregabalin or duloxetine are recommended as initial pharmacologic treatments for neuropathic pain in diabetes. A American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care 2017; 40 (Suppl. 1): S88-S98
88 Recommendations: Foot Care Perform a comprehensive foot evaluation annually to identify risk factors for ulcers & amputations. B All patients with diabetes should have their feet inspected at every visit. C History should contain prior hx of ulceration, amputation, Charcot foot, angioplasty or vascular surgery, cigarette smoking, retinopathy & renal disease; and should assess current symptoms of neuropathy and vascular disease. B American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care 2017; 40 (Suppl. 1): S88-S98
89 Recommendations: Foot Care Exam should include inspection of the skin, assessment of foot deformities, neurologic assessment & vascular assessment including pulses in the legs and feet. B American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care 2017; 40 (Suppl. 1): S88-S98
90 Recommendations: Foot Care To perform the 10-g monofilament test, place the device perpendicular to the skin; Apply pressure until monofilament buckles. Hold in place for 1 second & release. The monofilament test should be performed at the highlighted sites while the patient s eyes are closed. Boulton A, Armstrong D, Albert, S et. al. Comprehensive Foot Examination and Risk Assessment. Diabetes Care. 2008; 31:
91 2018 Watch: Foot Care CMS covers hyperbaric oxygen therapy (HOT) for diabetic foot ulcers in certain patients New section describes the mixed evidence regarding its use as an adjunctive treatment to enhance wound healing hyperbaric oxygen therapy in people with diabetic foot ulcers Additional evidence forthcoming
92 11. Older Adults
93 Older Adults 26% of patients aged >65 have diabetes. Older adults have higher rates of premature death, functional disability & coexisting illnesses. At greater risk for polypharmacy, cognitive impairment, urinary incontinence, injurious falls & persistent pain. Screening for complications should be individualized and periodically revisited. At higher risk for depression American Diabetes Association Standards of Medical Care in Diabetes. Older adults. Diabetes Care 2017; 40 (Suppl. 1): S99-S104
94 Recommendations: Older Adults Functional, cognitively intact older adults ( 65 years of age) with significant life expectancy should receive diabetes care using goals developed for younger adults. C Determine targets & therapeutic approaches by assessment of medical, functional, mental, and social geriatric domains for diabetes management. C American Diabetes Association Standards of Medical Care in Diabetes. Older adults. Diabetes Care 2017; 40 (Suppl. 1): S99-S104
95 Recommendations: Older Adults Glycemic goals for some older adults might be relaxed but hyperglycemia leading to symptoms or risk of acute hyperglycemic complications should be avoided in all patients. C Hypoglycemia should be avoided in older adults with diabetes. It should be screened for and managed by adjusting glycemic targets and pharmacologic interventions. B American Diabetes Association Standards of Medical Care in Diabetes. Older adults. Diabetes Care 2017; 40 (Suppl. 1): S99-S104
96 Recommendations: Older Adults Patients with DM in long-term care facilities need careful assessment to establish a glycemic goal & to make appropriate choices of glucose-lowering agents. E Other CV risk factors should be treated in older adults with consideration of the time frame of benefit and the individual patient. E Treatment of HTN is indicated in most older adults C Lipid-lowering and aspirin therapy may benefit those with life expectancy at least equal to the time frame of primary or secondary prevention trials. E American Diabetes Association Standards of Medical Care in Diabetes. Older adults. Diabetes Care 2017; 40 (Suppl. 1): S99-S104
97 Recommendations: Older Adults Screening for geriatric syndromes may be appropriate in older adults with limitations in basic and instrumental activities of daily living. C Older adults with DM should be considered a highpriority population for depression screening and treatment. B Annual screening for early detection of mild cognitive impairment or dementia is indicated for adults 65 years of age or older. B American Diabetes Association Standards of Medical Care in Diabetes. Older adults. Diabetes Care 2017; 40 (Suppl. 1): S99-S104
98 2018 Watch: Older Adults Older adults at higher risk of hyperglycemia Discussion surrounding how to lower that risk Individualizing pharmacologic therapy Avoid overtreatment Simplify complex regimens
99 12. Children & Adolescents
100 Type 1 Diabetes ¾ of all cases of T1DM are dx d in patients <18 yrs. Providers must consider many unique aspects to care & mgmt. of children & adolescents with T1DM. Attention to family dynamics, developmental stages, physiological differences is essential. Recommendations less likely to be based on clinical trial evidence. American Diabetes Association Standards of Medical Care in Diabetes. Children and adolescents. Diabetes Care 2017; 40 (Suppl. 1): S105-S113
101 Type 1 Diabetes: Psychosocial Issues At diagnosis and during routine follow-up care, assess psychosocial issues and family stresses that could impact adherence to diabetes mgmt. Provide referrals to trained mental health professionals, preferably experienced in childhood diabetes. E American Diabetes Association Standards of Medical Care in Diabetes. Children and adolescents. Diabetes Care 2017; 40 (Suppl. 1): S105-S113
102 Type 1 Diabetes: Psychosocial Issues Encourage family involvement in diabetes mgmt. tasks for children & adolescents, as premature transfer of diabetes care can result in nonadherence and deterioration in glycemic control. B Mental health professionals should be considered integral members of the pediatric diabetes multidisciplinary team. E American Diabetes Association Standards of Medical Care in Diabetes. Children and adolescents. Diabetes Care 2017; 40 (Suppl. 1): S105-S113
103 Type 1 Diabetes: Psychosocial Issues Adolescents should have the option for time by themselves with their care provider(s) starting at age 12 years. E Starting at puberty, preconception counseling should be incorporated into routine diabetes care for all girls of childbearing potential. A American Diabetes Association Standards of Medical Care in Diabetes. Children and adolescents. Diabetes Care 2017; 40 (Suppl. 1): S105-S113
104 Type 1 Diabetes: Glycemic Control Before meals Blood glucose goal range Bedtime/ overnight A1C Rationale mg/dl ( mmol/l) mg/dl ( mmol/l) <7.5% A lower goal (<7.0%) is reasonable if it can be achieved without excessive hypos 1. Goals should be individualized; lower goals may be reasonable. 2. Modify BG goals in youth w/ frequent hypos or hypoglycemia unawareness. 3. Measure postprandial BG if discrepancy between preprandial BG and A1C & to assess glycemia in basal bolus regimens. American Diabetes Association Standards of Medical Care in Diabetes. Children and adolescents. Diabetes Care 2017; 40 (Suppl. 1): S105-S113
105 Type 2 Diabetes Distinguishing between type 1 and type 2 can be challenging. Diabetes-associated autoantibodies and ketosis may be present in patients with features of type 2 such as obesity and acanthosis nigricans. Accurate diagnosis is critical. American Diabetes Association Standards of Medical Care in Diabetes. Children and adolescents. Diabetes Care 2017; 40 (Suppl. 1): S105-S113
106 2018 Watch: Youth-onset Type 2 Diabetes Position statement currently in press on the evaluation and management of youth-onset type 2 diabetes Recommendations in the Standards expanded based on this review New screening and treatment recommendations
107 13. Management of Diabetes in Pregnancy
108 Gestational Diabetes Mellitus (GDM) Lifestyle change is an essential part GDM mgmt. and may suffice for many women. Add medications if needed to achieve glycemic targets. A Insulin is the preferred medication for treating hyperglycemia in GDM, as it does not cross the placenta. Metformin and glyburide may be used but both, particularly metformin, cross the placenta. All oral agents lack long-term safety data. A American Diabetes Association. Standards of Medical Care in Diabetes Management of Diabetes in Pregnancy Diabetes Care 2017;40(Suppl. 1):S114 S119
109 Gestational Diabetes Mellitus (GDM) Metformin, when used to treat polycystic ovary syndrome and induce ovulation, need not be continued once pregnancy has been confirmed. A American Diabetes Association. Standards of Medical Care in Diabetes Management of Diabetes in Pregnancy Diabetes Care 2017;40(Suppl. 1):S114 S119
110 General Principles for Management of Diabetes in Pregnancy Potentially teratogenic medications (ACE inhibitors, statins, etc.) should be avoided in sexually active women of childbearing age who are not using reliable contraception. B Fasting and postprandial SMBG are recommended in both GDM and preexisting diabetes in pregnancy to achieve glycemic control. Some women with preexisting diabetes should also test blood glucose preprandially. B American Diabetes Association. Standards of Medical Care in Diabetes Management of Diabetes in Pregnancy Diabetes Care 2017;40(Suppl. 1):S114 S119
111 General Principles for Management of Diabetes in Pregnancy Due to increased red blood cell turnover, A1C is lower in normal pregnancy than in normal nonpregnant women. A1C target in pregnancy is 6 6.5% (42 48mmol/mol); <6% (42 mmol/mol) may be optimal if achievable without significant hypoglycemia, but the target may be relaxed to <7% (53 mmol/mol) if necessary to prevent hypoglycemia. B In pregnant patients with diabetes and hypertension, BP targets / are suggested. E American Diabetes Association. Standards of Medical Care in Diabetes Management of Diabetes in Pregnancy Diabetes Care 2017;40(Suppl. 1):S114 S119
112 Glycemic Targets in Pregnancy For women with gestational diabetes or preexisting type 1 or type 2 diabetes in pregnancy, the following targets are recommended: Fasting 95 mg/dl (5.3 mmol/l) and either One-hour postprandial 140 mg/dl (7.8 mmol/l) or Two-hour postprandial 120 mg/dl (6.7 mmol/l) American Diabetes Association. Standards of Medical Care in Diabetes Management of Diabetes in Pregnancy Diabetes Care 2017;40(Suppl. 1):S114 S119
113 2018 Watch: Pregnancy Discussion about the role of aspirin in the prevention of preeclampsia for pregnant women with type 1 or type 2 diabetes. American Diabetes Association. Standards of Medical Care in Diabetes Management of Diabetes in Pregnancy Diabetes Care 2017;40(Suppl. 1):S114 S119
114 14. Diabetes Care in the Hospital
115 Recommendations: Diabetes Care in the Hospital Basal insulin or basal + bolus correction regimen is the preferred treatment for noncritically ill patients with poor oral intake or those who are taking nothing by mouth. An insulin regimen with basal, nutritional & correction components is the preferred treatment for noncritically ill patients with good nutritional intake. A The sole use of sliding scale insulin in the inpatient hospital setting is strongly discouraged. A American Diabetes Association. Standards of Medical Care in Diabetes. Diabetes care in the hospital. Diabetes Care 2017;40(Suppl. 1):S120 S127
116 Thank you!
Standards of Medical Care in Diabetes 2018
 Standards of Medical Care in Diabetes 2018 Eric L. Johnson, M.D. Associate Professor University of North Dakota School of Medicine and Health Sciences Assistant Medical Director Altru Diabetes Center Grand
Standards of Medical Care in Diabetes 2018 Eric L. Johnson, M.D. Associate Professor University of North Dakota School of Medicine and Health Sciences Assistant Medical Director Altru Diabetes Center Grand
Standards of Medical Care In Diabetes
 Standards of Medical Care In Diabetes - 2017 Robert E. Ratner, MD, FACP, FACE Professor of Medicine Georgetown University School of Medicine Disclosed no conflict of interest Standards of Care Professional.diabetes.org/SOC
Standards of Medical Care In Diabetes - 2017 Robert E. Ratner, MD, FACP, FACE Professor of Medicine Georgetown University School of Medicine Disclosed no conflict of interest Standards of Care Professional.diabetes.org/SOC
Standards of Care in Diabetes What's New? Veronica Brady, FNP-BC, PhD, BC-ADM,CDE Karmella Thomas, RD, LD,CDE
 Standards of Care in Diabetes 2016-- What's New? Veronica Brady, FNP-BC, PhD, BC-ADM,CDE Karmella Thomas, RD, LD,CDE Terminology No longer using the term diabetic. Diabetes does not define people. People
Standards of Care in Diabetes 2016-- What's New? Veronica Brady, FNP-BC, PhD, BC-ADM,CDE Karmella Thomas, RD, LD,CDE Terminology No longer using the term diabetic. Diabetes does not define people. People
Standards of Medical Care in Diabetes 2016
 Standards of Medical Care in Diabetes 2016 Care Delivery Systems 33-49% of patients still do not meet targets for A1C, blood pressure, or lipids. 14% meet targets for all A1C, BP, lipids, and nonsmoking
Standards of Medical Care in Diabetes 2016 Care Delivery Systems 33-49% of patients still do not meet targets for A1C, blood pressure, or lipids. 14% meet targets for all A1C, BP, lipids, and nonsmoking
STATE OF THE STATE: TYPE II DIABETES
 STATE OF THE STATE: TYPE II DIABETES HENRY DRISCOLL, MD, CHIEF of ENDOCRINOLOGY MARSHALL U, CHERTOW DIABETES CENTER, HUNTINGTON VAMC HEATHER VENOY, RD, LD, CDE DIETITIAN, DIABETES EDUCATOR, CHERTOW DIABETES
STATE OF THE STATE: TYPE II DIABETES HENRY DRISCOLL, MD, CHIEF of ENDOCRINOLOGY MARSHALL U, CHERTOW DIABETES CENTER, HUNTINGTON VAMC HEATHER VENOY, RD, LD, CDE DIETITIAN, DIABETES EDUCATOR, CHERTOW DIABETES
American Diabetes Association 2018 Guidelines Important Notable Points
 American Diabetes Association 2018 Guidelines Important Notable Points The Standards of Medical Care in Diabetes-2018 by ADA include the most current evidencebased recommendations for diagnosing and treating
American Diabetes Association 2018 Guidelines Important Notable Points The Standards of Medical Care in Diabetes-2018 by ADA include the most current evidencebased recommendations for diagnosing and treating
2019 Standards of Medical Care in Diabetes: What is New and Why
 2019 Standards of Medical Care in Diabetes: What is New and Why Jane E.B. Reusch, MD ADA President of Medicine & Science Professor of Medicine, Division of Endocrinology, Metabolism and Diabetes and Associate
2019 Standards of Medical Care in Diabetes: What is New and Why Jane E.B. Reusch, MD ADA President of Medicine & Science Professor of Medicine, Division of Endocrinology, Metabolism and Diabetes and Associate
What s New in the Standards of Medical Care in Diabetes? Dr. Jason Kruse, DO Broadlawns Medical Center
 What s New in the Standards of Medical Care in Diabetes? Dr. Jason Kruse, DO Broadlawns Medical Center Learning Objectives By the end of this presentation, participants should be able to: Discuss updates
What s New in the Standards of Medical Care in Diabetes? Dr. Jason Kruse, DO Broadlawns Medical Center Learning Objectives By the end of this presentation, participants should be able to: Discuss updates
Diabetes Review Chris Paras, D.O. Assistant Prof of Medicine, NYIT & Touro COM Designated Institutional Official & Assoc. Clinical Dean, Brookdale
 Diabetes Review Chris Paras, D.O. Assistant Prof of Medicine, NYIT & Touro COM Designated Institutional Official & Assoc. Clinical Dean, Brookdale University Hospital Diabetes Care 2018 Jan; 41 Objectives
Diabetes Review Chris Paras, D.O. Assistant Prof of Medicine, NYIT & Touro COM Designated Institutional Official & Assoc. Clinical Dean, Brookdale University Hospital Diabetes Care 2018 Jan; 41 Objectives
Diabetes Summary of Medical Guidelines
 Diabetes Summary of Medical Guidelines Key concepts in setting glycemic controls: goals should be individualized; certain populations (children, pregnant women, and elderly) require special considerations;
Diabetes Summary of Medical Guidelines Key concepts in setting glycemic controls: goals should be individualized; certain populations (children, pregnant women, and elderly) require special considerations;
Vipul Lakhani, MD Oregon Medical Group Endocrinology
 Vipul Lakhani, MD Oregon Medical Group Endocrinology Disclosures None Objectives Be able to diagnose diabetes and assess control Be able to identify appropriate classes of medications for diabetes treatment
Vipul Lakhani, MD Oregon Medical Group Endocrinology Disclosures None Objectives Be able to diagnose diabetes and assess control Be able to identify appropriate classes of medications for diabetes treatment
Modified version focused on CCNC Quality Measures and Feedback Processes
 Executive Summary: Standards of Medical Care in Diabetes 2010 Modified version focused on CCNC Quality Measures and Feedback Processes See http://care.diabetesjournals.org/content/33/supplement_1/s11.full
Executive Summary: Standards of Medical Care in Diabetes 2010 Modified version focused on CCNC Quality Measures and Feedback Processes See http://care.diabetesjournals.org/content/33/supplement_1/s11.full
Standards of Medical Care in Diabetes
 Standards of Medical Care in Diabetes - 2018 1. Improving Care and Promoting Health in Populations Diabetes and Population Health: Recommendations Ensure treatment decisions are timely, rely on evidence-based
Standards of Medical Care in Diabetes - 2018 1. Improving Care and Promoting Health in Populations Diabetes and Population Health: Recommendations Ensure treatment decisions are timely, rely on evidence-based
Disclosures. Diabetes and Cardiovascular Risk Management. Learning Objectives. Atherosclerotic Cardiovascular Disease
 Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
STANDARDS OF MEDICAL CARE IN DIABETES 2014
 STANDARDS OF MEDICAL CARE IN DIABETES 2014 I. CLASSIFICATION AND DIAGNOSIS Classification of Diabetes Type 1 diabetes β-cell destruction Type 2 diabetes Progressive insulin secretory defect Other specific
STANDARDS OF MEDICAL CARE IN DIABETES 2014 I. CLASSIFICATION AND DIAGNOSIS Classification of Diabetes Type 1 diabetes β-cell destruction Type 2 diabetes Progressive insulin secretory defect Other specific
American Diabetes Association Standards of Medical Care in Diabetes 2018: Latest Updates
 American Diabetes Association Standards of Medical Care in Diabetes 2018: Latest Updates Juan Pablo Frias, MD President and CEO, National Research Institute, Los Angeles, CA Clinical Faculty, University
American Diabetes Association Standards of Medical Care in Diabetes 2018: Latest Updates Juan Pablo Frias, MD President and CEO, National Research Institute, Los Angeles, CA Clinical Faculty, University
UPDATED APRIL 26, 2018 This slide deck contains content created, reviewed, and approved by the American Diabetes Association. You are free to use the
 UPDATED APRIL 26, 2018 This slide deck contains content created, reviewed, and approved by the American Diabetes Association. You are free to use the slides in presentations without further permission
UPDATED APRIL 26, 2018 This slide deck contains content created, reviewed, and approved by the American Diabetes Association. You are free to use the slides in presentations without further permission
2018 Standard of Medical Care Diabetes and Pregnancy
 2018 Standard of Medical Care Diabetes and Pregnancy 2018 Standard of Medical Care Diabetes and Pregnancy Marjorie Cypress does not have any relevant financial relationships with any commercial interests
2018 Standard of Medical Care Diabetes and Pregnancy 2018 Standard of Medical Care Diabetes and Pregnancy Marjorie Cypress does not have any relevant financial relationships with any commercial interests
Adult Diabetes Clinician Guide NOVEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
American Diabetes Association Standards of Medical Care in Diabetes 2017: Focus on Complications
 American Diabetes Association Standards of Medical Care in Diabetes 2017: Focus on Complications Juan Pablo Frias, M.D., FACE President and CEO, National Research Institute, Los Angeles, CA Clinical Faculty,
American Diabetes Association Standards of Medical Care in Diabetes 2017: Focus on Complications Juan Pablo Frias, M.D., FACE President and CEO, National Research Institute, Los Angeles, CA Clinical Faculty,
Diabetes and Hypertension
 Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES
 Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES Objectives u At conclusion of the lecture the participant will be able to: 1. Differentiate between the classifications of diabetes
Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES Objectives u At conclusion of the lecture the participant will be able to: 1. Differentiate between the classifications of diabetes
American Diabetes Association: Standards of Medical Care in Diabetes 2015
 American Diabetes Association: Standards of Medical Care in Diabetes 2015 Synopsis of ADA standards relevant to the 11 th Scope of Work under Task B.2 ASSESSMENT OF GLYCEMIC CONTROL Recommendations: Perform
American Diabetes Association: Standards of Medical Care in Diabetes 2015 Synopsis of ADA standards relevant to the 11 th Scope of Work under Task B.2 ASSESSMENT OF GLYCEMIC CONTROL Recommendations: Perform
Executive Summary: Standards of Medical Care in Diabetes 2010
 E X E C U T I V E S U M M A R Y Executive Summary: Standards of Medical Care in Diabetes 2010 Current criteria for the diagnosis of diabetes A1C 6.5%: The test should be performed in a laboratory using
E X E C U T I V E S U M M A R Y Executive Summary: Standards of Medical Care in Diabetes 2010 Current criteria for the diagnosis of diabetes A1C 6.5%: The test should be performed in a laboratory using
Clinical Practice Guidelines for Diabetes Management
 Clinical Practice Guidelines for Diabetes Management Diabetes is a disease in which blood glucose levels are above normal. Over the years, high blood glucose damages nerves and blood vessels, which can
Clinical Practice Guidelines for Diabetes Management Diabetes is a disease in which blood glucose levels are above normal. Over the years, high blood glucose damages nerves and blood vessels, which can
Diabetes Updates. Disclosures
 Diabetes Updates Dr. Thanh D. Hoang, DO, FACP, FACE Walter Reed National Military Medical Center Associate Professor of Medicine Uniformed Services University of the Health Sciences March 2018 Disclosures
Diabetes Updates Dr. Thanh D. Hoang, DO, FACP, FACE Walter Reed National Military Medical Center Associate Professor of Medicine Uniformed Services University of the Health Sciences March 2018 Disclosures
Diabetes Mellitus: Evaluation and Care Management
 Diabetes Mellitus: Evaluation and Care Management Michael King, MD Assistant Professor Residency Program Director University of Kentucky Dept. of Family & Community Medicine Learning Objectives 1. Review
Diabetes Mellitus: Evaluation and Care Management Michael King, MD Assistant Professor Residency Program Director University of Kentucky Dept. of Family & Community Medicine Learning Objectives 1. Review
Standards of Medical Care in Diabetes 2019 Abridged for Primary Care Providers
 Standards of Medical Care in Diabetes 2019 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association s Standards of Medical Care
Standards of Medical Care in Diabetes 2019 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association s Standards of Medical Care
The Many Faces of T2DM in Long-term Care Facilities
 The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
Treating the elderly patients with type 2 diabetes mellitus
 Treating the elderly patients with type 2 diabetes mellitus Niki Katsiki MSc, PhD, MD, FRSPH IASO/EASO Scope Member EASD Diabetes & Cardiovascular Disease Group Member Member of the Executive Board of
Treating the elderly patients with type 2 diabetes mellitus Niki Katsiki MSc, PhD, MD, FRSPH IASO/EASO Scope Member EASD Diabetes & Cardiovascular Disease Group Member Member of the Executive Board of
DIABETES MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
RCHC Clinical Guidelines Type 2 Diabetes; Adults
 RCHC Clinical Guidelines Type 2 Diabetes; Adults Screening for diabetes in asymptomatic adults 1 Population: Aged > 45 years; Aged < 45 years who are overweight (BMI> 25kg/m 2 ) and have an additional
RCHC Clinical Guidelines Type 2 Diabetes; Adults Screening for diabetes in asymptomatic adults 1 Population: Aged > 45 years; Aged < 45 years who are overweight (BMI> 25kg/m 2 ) and have an additional
Diabetes Mellitus in Older Adults. Presenter Disclosure Information
 Diabetes Mellitus in Older Adults Medha Munshi, M.D. Joslin Diabetes Center Beth Israel Deaconess Medical Center Harvard Medical School Presenter Disclosure Information Medha Munshi Research grant from
Diabetes Mellitus in Older Adults Medha Munshi, M.D. Joslin Diabetes Center Beth Israel Deaconess Medical Center Harvard Medical School Presenter Disclosure Information Medha Munshi Research grant from
DM Fundamentals Class 5 Goals & Standards of Care Standards of Care Topics. CDE Coach App Download Success
 DM Fundamentals Class 5 Goals & Standards of Care 2017 Beverly Thomassian, RN, MPH, BC ADM, CDE President, Diabetes Education Services Standards of Care Topics Review the 15 Standards of Care with a focus
DM Fundamentals Class 5 Goals & Standards of Care 2017 Beverly Thomassian, RN, MPH, BC ADM, CDE President, Diabetes Education Services Standards of Care Topics Review the 15 Standards of Care with a focus
Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone
 Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Executive Summary: Standards of Medical Care in Diabetes 2009
 Executive Summary Executive Summary: Standards of Medical Care in Diabetes 2009 Current Criteria for the Diagnosis of Diabetes Fasting plasma glucose (FPG) 126 mg/dl (7.0 mmol/l). Fasting is defined as
Executive Summary Executive Summary: Standards of Medical Care in Diabetes 2009 Current Criteria for the Diagnosis of Diabetes Fasting plasma glucose (FPG) 126 mg/dl (7.0 mmol/l). Fasting is defined as
Standards of Medical Care in Diabetes 2018
 Standards of Medical Care in Diabetes 2018 William T. Cefalu, MD Chief Scientific, Medical and Mission Officer American Diabetes Association Global Prevalence of Diabetes Expected to Increase by 54% by
Standards of Medical Care in Diabetes 2018 William T. Cefalu, MD Chief Scientific, Medical and Mission Officer American Diabetes Association Global Prevalence of Diabetes Expected to Increase by 54% by
Disclosures of Interest. Publications Diabetologia Key points to emphasize
 Disclosures of Interest No conflicts or disclosures How to Use the American Diabetes Association s Type 2 Diabetes Treatment Algorithm Rashida Downing, MD, FAAFP Primary Care Physician JenCare Medical
Disclosures of Interest No conflicts or disclosures How to Use the American Diabetes Association s Type 2 Diabetes Treatment Algorithm Rashida Downing, MD, FAAFP Primary Care Physician JenCare Medical
Diabetes and Cardiovascular Risk Management Denise M. Kolanczyk, PharmD, BCPS-AQ Cardiology
 Diabetes and Cardiovascular Risk Management Denise M. Kolanczyk, PharmD, BCPS-AQ Cardiology Disclosures In compliance with the accrediting board policies, the American Diabetes Association requires the
Diabetes and Cardiovascular Risk Management Denise M. Kolanczyk, PharmD, BCPS-AQ Cardiology Disclosures In compliance with the accrediting board policies, the American Diabetes Association requires the
Diabetes Update: Diabetes Management In Primary Care. Jonathon M. Firnhaber, MD, FAAFP
 Diabetes Update: Diabetes Management In Primary Care Jonathon M. Firnhaber, MD, FAAFP Learning objectives 1. Critically evaluate the evidence emerging within diabetes research as it applies to recommendations
Diabetes Update: Diabetes Management In Primary Care Jonathon M. Firnhaber, MD, FAAFP Learning objectives 1. Critically evaluate the evidence emerging within diabetes research as it applies to recommendations
8/5/2017. Disclosure to Participants. Learning Outcomes. Terry Compton MS, APRN, CDE. Seniors with Diabetes: Why Are They Different?
 Terry Compton MS, APRN, CDE Diabetes Education Program Manager St. Tammany Parish Hospital Covington, LA Sara (Mandy) Reece PharmD, CDE, BC-ADM, FAADE Diabetes Educator Vice Chair and Associate Professor,
Terry Compton MS, APRN, CDE Diabetes Education Program Manager St. Tammany Parish Hospital Covington, LA Sara (Mandy) Reece PharmD, CDE, BC-ADM, FAADE Diabetes Educator Vice Chair and Associate Professor,
Management of DM in Older Adults: It s not all about sugar! Who needs treatment for DM? Peggy Odegard, Pharm.D., BCPS, CDE
 Management of DM in Older Adults: It s not all about sugar! Peggy Odegard, Pharm.D., BCPS, CDE Who needs treatment for DM? 87 year old, frail male with moderately severe dementia living in NH with persistent
Management of DM in Older Adults: It s not all about sugar! Peggy Odegard, Pharm.D., BCPS, CDE Who needs treatment for DM? 87 year old, frail male with moderately severe dementia living in NH with persistent
Special thanks to the EJC Foundation for their support of Sanford Center Geriatric Specialty Clinic
 Special thanks to the EJC Foundation for their support of Sanford Center Geriatric Specialty Clinic Sanford Center for Aging 775-784-4744 med.unr.edu/aging Diabetes Management Series: From Selfmanagement
Special thanks to the EJC Foundation for their support of Sanford Center Geriatric Specialty Clinic Sanford Center for Aging 775-784-4744 med.unr.edu/aging Diabetes Management Series: From Selfmanagement
Guidelines to assist General Practitioners in the Management of Type 2 Diabetes. April 2010
 Guidelines to assist General Practitioners in the Management of Type 2 Diabetes April 2010 Foreword The guidelines were devised by the Diabetes Day Centre in Beaumont Hospital in consultation with a number
Guidelines to assist General Practitioners in the Management of Type 2 Diabetes April 2010 Foreword The guidelines were devised by the Diabetes Day Centre in Beaumont Hospital in consultation with a number
Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drug Class Prior Authorization Protocol
 Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drug Class Prior Authorization Protocol Line of Business: Medicaid P&T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has
Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drug Class Prior Authorization Protocol Line of Business: Medicaid P&T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has
Harmonizing the ADA, AACE and other Guidelines in the Treatment of the Patient with Diabetes Mellitus. Angel L Comulada, MD, FACE Endocrinologist
 Harmonizing the ADA, AACE and other Guidelines in the Treatment of the Patient with Diabetes Mellitus Angel L Comulada, MD, FACE Endocrinologist 2 Disclosure Angel L Comulada, MD, FACE, CCD Has received
Harmonizing the ADA, AACE and other Guidelines in the Treatment of the Patient with Diabetes Mellitus Angel L Comulada, MD, FACE Endocrinologist 2 Disclosure Angel L Comulada, MD, FACE, CCD Has received
Quick Reference Guide
 2018 Clinical Practice Guidelines Quick Reference Guide 416569-18 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Screening and Diagnosis Assess risk ANNUALLY if: Family history (First-degree
2018 Clinical Practice Guidelines Quick Reference Guide 416569-18 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Screening and Diagnosis Assess risk ANNUALLY if: Family history (First-degree
Diabetes Mellitus II CPG
 1 Diabetes Mellitus II CPG Candidates for Screening Integrated Complex Care Patients: Check Yearly Prediabetes: Check Yearly No Diabetes Mellitus (DM) Risk Factors: Check at Age 45, Repeat Every 3 Years
1 Diabetes Mellitus II CPG Candidates for Screening Integrated Complex Care Patients: Check Yearly Prediabetes: Check Yearly No Diabetes Mellitus (DM) Risk Factors: Check at Age 45, Repeat Every 3 Years
The American Diabetes
 Standards of Medical Care in Diabetes 2016 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association Position Statement: Standards
Standards of Medical Care in Diabetes 2016 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association Position Statement: Standards
The American Diabetes
 Standards of Medical Care in Diabetes 2015 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association Position Statement: Standards
Standards of Medical Care in Diabetes 2015 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association Position Statement: Standards
A Practical Approach to the Use of Diabetes Medications
 A Practical Approach to the Use of Diabetes Medications Juan Pablo Frias, M.D., FACE President, National Research Institute, Los Angles, CA Clinical Faculty, University of California, San Diego, CA OUTLINE
A Practical Approach to the Use of Diabetes Medications Juan Pablo Frias, M.D., FACE President, National Research Institute, Los Angles, CA Clinical Faculty, University of California, San Diego, CA OUTLINE
Diabetes Complications Guideline Based Screening, Management, and Referral
 Diabetes Complications Guideline Based Screening, Management, and Referral Eric L. Johnson, M.D. Associate Professor Department of Family and Community Medicine Assistant Medical Director Altru Diabetes
Diabetes Complications Guideline Based Screening, Management, and Referral Eric L. Johnson, M.D. Associate Professor Department of Family and Community Medicine Assistant Medical Director Altru Diabetes
Physical Activity/Exercise Prescription with Diabetes
 Physical Activity/Exercise Prescription with Diabetes B R AD H I NTERMEYER C E P A C SM S A NFORD H E ALTH C A RDIAC R E H AB A N D D I ABE TES E XE RCISE The adoption and maintenance of physical activity
Physical Activity/Exercise Prescription with Diabetes B R AD H I NTERMEYER C E P A C SM S A NFORD H E ALTH C A RDIAC R E H AB A N D D I ABE TES E XE RCISE The adoption and maintenance of physical activity
Non-insulin treatment in Type 1 DM Sang Yong Kim
 Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Type 2 Diabetes: Where Do We Start with Treatment? DIABETES EDUCATION. Diabetes Mellitus: Complications and Co-Morbid Conditions
 Diabetes Mellitus: Complications and Co-Morbid Conditions ADA Guidelines for Glycemic Control: 2016 Retinopathy Between 2005-2008, 28.5% of patients with diabetes 40 years and older diagnosed with diabetic
Diabetes Mellitus: Complications and Co-Morbid Conditions ADA Guidelines for Glycemic Control: 2016 Retinopathy Between 2005-2008, 28.5% of patients with diabetes 40 years and older diagnosed with diabetic
STANDARDS OF MEDICAL CARE IN DIABETES 2012
 STANDARDS OF MEDICAL CARE IN DIABETES 2012 Section Table of Contents ADA Evidence Grading System of Clinical Recommendations Slide No. I. Classification and Diagnosis 4-11 II. Testing for Diabetes in Asymptomatic
STANDARDS OF MEDICAL CARE IN DIABETES 2012 Section Table of Contents ADA Evidence Grading System of Clinical Recommendations Slide No. I. Classification and Diagnosis 4-11 II. Testing for Diabetes in Asymptomatic
AUGUST 25-27, 2017 UPDATE & BOARD REVIEW. acofp INTENSIVE. Diabetes Review. Colleen Cagno, MD INNOVATIVE COMPREHENSIVE HANDS-ON
 acofp INTENSIVE UPDATE & BOARD REVIEW AUGUST 25-27, 2017 Loews Chicago O'Hare Hotel Rosemont, IL INNOVATIVE COMPREHENSIVE HANDS-ON Diabetes Review Colleen Cagno, MD acofp Am eric an College of Osteopathi
acofp INTENSIVE UPDATE & BOARD REVIEW AUGUST 25-27, 2017 Loews Chicago O'Hare Hotel Rosemont, IL INNOVATIVE COMPREHENSIVE HANDS-ON Diabetes Review Colleen Cagno, MD acofp Am eric an College of Osteopathi
Updates in Diabetes and Cardiovascular Disease Management: Are You Making the Link?
 Updates in Diabetes and Cardiovascular Disease Management: Are You Making the Link? Denise Kolanczyk, PharmD, BCPS AQ Cardiology 1 Erika Hellenbart, PharmD, BCPS 2 Jennifer D Souza, PharmD, CDE, BC ADM
Updates in Diabetes and Cardiovascular Disease Management: Are You Making the Link? Denise Kolanczyk, PharmD, BCPS AQ Cardiology 1 Erika Hellenbart, PharmD, BCPS 2 Jennifer D Souza, PharmD, CDE, BC ADM
Diabetes Risk Assessment and Treatment
 Diabetes Risk Assessment and Treatment Todd T. Brown, MD, PhD Professor of Medicine and Epidemiology Division of Endocrinology, Diabetes, & Metabolism Johns Hopkins University Baltimore, Maryland, USA
Diabetes Risk Assessment and Treatment Todd T. Brown, MD, PhD Professor of Medicine and Epidemiology Division of Endocrinology, Diabetes, & Metabolism Johns Hopkins University Baltimore, Maryland, USA
Diabetes and the Elderly: Medication Considerations When Determining Benefits and Risks
 Diabetes and the Elderly: Medication Considerations When Determining Benefits and Risks Gretchen M. Ray, PharmD, PhC, BCACP, CDE Associate Professor UNM College of Pharmacy September 7 th, 2018 DISCLOSURES
Diabetes and the Elderly: Medication Considerations When Determining Benefits and Risks Gretchen M. Ray, PharmD, PhC, BCACP, CDE Associate Professor UNM College of Pharmacy September 7 th, 2018 DISCLOSURES
Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead
 Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead Today s Presentation HbA1c & diagnosing Diabetes What is Impaired Glucose & IGR? Implications
Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead Today s Presentation HbA1c & diagnosing Diabetes What is Impaired Glucose & IGR? Implications
Psychosocial Issues for People with Diabetes. Richard Arakaki, M.D. Phoenix Area Diabetes Consultant June 28, 2017
 Psychosocial Issues for People with Diabetes Richard Arakaki, M.D. Phoenix Area Diabetes Consultant June 28, 2017 Objectives Provide epidemiological and interventional data of DM in AI/AN and general population
Psychosocial Issues for People with Diabetes Richard Arakaki, M.D. Phoenix Area Diabetes Consultant June 28, 2017 Objectives Provide epidemiological and interventional data of DM in AI/AN and general population
Initiation and Titration of Insulin in Diabetes Mellitus Type 2
 Initiation and Titration of Insulin in Diabetes Mellitus Type 2 Greg Doelle MD, MS April 6, 2016 Disclosure I have no actual or potential conflicts of interest in relation to the content of this lecture.
Initiation and Titration of Insulin in Diabetes Mellitus Type 2 Greg Doelle MD, MS April 6, 2016 Disclosure I have no actual or potential conflicts of interest in relation to the content of this lecture.
Vishwanath Pattan Endocrinology Wyoming Medical Center
 Vishwanath Pattan Endocrinology Wyoming Medical Center Disclosure Holdings in Tandem Non for this Training Introduction In the United States, 5 to 6 percent of pregnancies almost 250,000 women are affected
Vishwanath Pattan Endocrinology Wyoming Medical Center Disclosure Holdings in Tandem Non for this Training Introduction In the United States, 5 to 6 percent of pregnancies almost 250,000 women are affected
Clinical Practice Guidelines
 Clinical Practice Guidelines Diabetes Objective The purpose is to guide the appropriate diagnosis and management of Diabetes. This guideline is designed to assist the clinician by providing a framework
Clinical Practice Guidelines Diabetes Objective The purpose is to guide the appropriate diagnosis and management of Diabetes. This guideline is designed to assist the clinician by providing a framework
Wayne Gravois, MD August 6, 2017
 Wayne Gravois, MD August 6, 2017 Americans with Diabetes (Millions) 40 30 Source: National Diabetes Statistics Report, 2011, 2017 Millions 20 10 0 1980 2009 2015 2007 - $174 Billion 2015 - $245 Billion
Wayne Gravois, MD August 6, 2017 Americans with Diabetes (Millions) 40 30 Source: National Diabetes Statistics Report, 2011, 2017 Millions 20 10 0 1980 2009 2015 2007 - $174 Billion 2015 - $245 Billion
Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications
 Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications Nathan Woolever, Pharm.D., Resident Pharmacist Pharmacy Grand Rounds November 6 th, 2018 Franciscan Healthcare La Crosse, WI 2017
Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications Nathan Woolever, Pharm.D., Resident Pharmacist Pharmacy Grand Rounds November 6 th, 2018 Franciscan Healthcare La Crosse, WI 2017
Drug Class Monograph
 Drug Class Monograph Class: Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drugs: Farxiga (dapagliflozin), Invokamet (canagliflozin/metformin), Invokana (canagliflozin), Jardiance (empagliflozin),
Drug Class Monograph Class: Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drugs: Farxiga (dapagliflozin), Invokamet (canagliflozin/metformin), Invokana (canagliflozin), Jardiance (empagliflozin),
Chapter 37: Exercise Prescription in Patients with Diabetes
 Chapter 37: Exercise Prescription in Patients with Diabetes American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
Chapter 37: Exercise Prescription in Patients with Diabetes American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS
 IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
Individualizing Type 2 Diabetes Management. Cynthia Gerstenlauer, ANP-BC, GCNS-BC, CDE, CCD
 Individualizing Type 2 Diabetes Management Cynthia Gerstenlauer, ANP-BC, GCNS-BC, CDE, CCD Harsh Statistics 30.3 million (9.4% of population) in US had DM in 2015 The percent of population with DM increases
Individualizing Type 2 Diabetes Management Cynthia Gerstenlauer, ANP-BC, GCNS-BC, CDE, CCD Harsh Statistics 30.3 million (9.4% of population) in US had DM in 2015 The percent of population with DM increases
Quick Reference Guide
 2013 Clinical Practice Guidelines Quick Reference Guide (Updated November 2016) 416569-16 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Copyright 2016 Canadian Diabetes Association SCREENING
2013 Clinical Practice Guidelines Quick Reference Guide (Updated November 2016) 416569-16 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Copyright 2016 Canadian Diabetes Association SCREENING
2019 Update on Recent Guideline Releases for Diabetes, Hypertension, and Dyslipidemia: Can We, Please, All Just Get on the Same Page?!
 2019 Update on Recent Guideline Releases for Diabetes, Hypertension, and Dyslipidemia: Can We, Please, All Just Get on the Same Page?! Jeremy L. Johnson, PharmD, BCACP, CDE, BC-ADM Assistant Professor,
2019 Update on Recent Guideline Releases for Diabetes, Hypertension, and Dyslipidemia: Can We, Please, All Just Get on the Same Page?! Jeremy L. Johnson, PharmD, BCACP, CDE, BC-ADM Assistant Professor,
2016 Diabetes Practice Guidelines
 2016 Diabetes Practice Guidelines SOURCE(S): 1. American Diabetes Association. Standards of Medical Care in Diabetes 2016. Diabetes Care January 2016 Volume 39, Supplement 1. Diagnosis Diabetes can be
2016 Diabetes Practice Guidelines SOURCE(S): 1. American Diabetes Association. Standards of Medical Care in Diabetes 2016. Diabetes Care January 2016 Volume 39, Supplement 1. Diagnosis Diabetes can be
Standards of Medical Care for Patients With Diabetes Mellitus
 Standards of Medical Care for Patients With Diabetes Mellitus American Diabetes Association Originally approved 1988. Most recent review/revision, October 2002. Abridged from Diabetes Care 26 (Suppl. 1):S33
Standards of Medical Care for Patients With Diabetes Mellitus American Diabetes Association Originally approved 1988. Most recent review/revision, October 2002. Abridged from Diabetes Care 26 (Suppl. 1):S33
Brigham and Women s Hospital Type 2 Diabetes Management Program Physician Pharmacist Collaborative Drug Therapy Management Protocol
 Brigham and Women s Hospital Type 2 Diabetes Management Program Physician Pharmacist Collaborative Drug Therapy Management Protocol *Please note that this guideline may not be appropriate for all patients
Brigham and Women s Hospital Type 2 Diabetes Management Program Physician Pharmacist Collaborative Drug Therapy Management Protocol *Please note that this guideline may not be appropriate for all patients
Preventing Serious Health Consequences of Type 2 Diabetes
 Preventing Serious Health Consequences of Type 2 Diabetes The Evidence Hertzel C. Gerstein MD MSc FRCPC Professor and Population Health Institute Chair in Diabetes Research McMaster University and Hamilton
Preventing Serious Health Consequences of Type 2 Diabetes The Evidence Hertzel C. Gerstein MD MSc FRCPC Professor and Population Health Institute Chair in Diabetes Research McMaster University and Hamilton
Joslin Diabetes Center Joslin Diabetes Forum 2013: The Impact of Comorbidities on Glucose Control Scenario 2: Reduced Renal Function
 Scenario 2: Reduced Renal Function 62 y.o. white man with type 2 diabetes for 18 years Hypertension and hypercholesterolemia Known proliferative retinopathy Current medications: Metformin 1000 mg bid Glyburide
Scenario 2: Reduced Renal Function 62 y.o. white man with type 2 diabetes for 18 years Hypertension and hypercholesterolemia Known proliferative retinopathy Current medications: Metformin 1000 mg bid Glyburide
Dr Tahseen A. Chowdhury Royal London Hospital. New Guidelines in Diabetes: NICE or Nasty?
 Dr Tahseen A. Chowdhury Royal London Hospital New Guidelines in Diabetes: NICE or Nasty? I have no conflicts of interest I do not undertake talks / advisory bodies / research for any pharma company Consultant
Dr Tahseen A. Chowdhury Royal London Hospital New Guidelines in Diabetes: NICE or Nasty? I have no conflicts of interest I do not undertake talks / advisory bodies / research for any pharma company Consultant
Application of the Diabetes Algorithm to a Patient
 Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
Diabesity. Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs
 Diabesity Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs Abdominal obesity Low HDL, high LDL, and high triglycerides HTN High blood glucose (F>100l,
Diabesity Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs Abdominal obesity Low HDL, high LDL, and high triglycerides HTN High blood glucose (F>100l,
Management of Type 2 Diabetes Cardiovascular Outcomes Trials Tom Blevins MD Texas Diabetes and Endocrinology Austin, Texas
 Management of Type 2 Diabetes Cardiovascular Outcomes Trials 2018 Tom Blevins MD Texas Diabetes and Endocrinology Austin, Texas Speaker Disclosure Dr. Blevins has disclosed that he has received grant support
Management of Type 2 Diabetes Cardiovascular Outcomes Trials 2018 Tom Blevins MD Texas Diabetes and Endocrinology Austin, Texas Speaker Disclosure Dr. Blevins has disclosed that he has received grant support
Guideline for Management of Type 2 Diabetes Mellitus: Kingdome of Bahrain Ministry of Health 2016
 Guideline for Management of Type 2 Diabetes Mellitus: Kingdome of Bahrain Ministry of Health 2016 1. Screening and diagnosis: Detection type 2 Diabetes are usually based on a two-step approach: Step 1:
Guideline for Management of Type 2 Diabetes Mellitus: Kingdome of Bahrain Ministry of Health 2016 1. Screening and diagnosis: Detection type 2 Diabetes are usually based on a two-step approach: Step 1:
Prediabetes & Type 2 Diabetes Prevention. Jacob M. Haus, PHD
 Prediabetes & Type 2 Diabetes Prevention Jacob M. Haus, PHD Disclosures In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure to the participants:
Prediabetes & Type 2 Diabetes Prevention Jacob M. Haus, PHD Disclosures In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure to the participants:
NEW SA DIABETES GUIDELINES
 Earn 3 CPD Points online 2017 SEMDSA diabetes management guidelines The updated 2017 South African guidelines for the management of type 2 diabetes mellitus were launched on 5 May at the 52 nd congress
Earn 3 CPD Points online 2017 SEMDSA diabetes management guidelines The updated 2017 South African guidelines for the management of type 2 diabetes mellitus were launched on 5 May at the 52 nd congress
Long-Term Complications of Diabetes Mellitus Macrovascular Complication
 Long-Term Complications of Diabetes Mellitus Macrovascular Complication Sung Hee Choi MD, PhD Professor, Seoul National University College of Medicine, SNUBH, Bundang Hospital Diabetes = CVD equivalent
Long-Term Complications of Diabetes Mellitus Macrovascular Complication Sung Hee Choi MD, PhD Professor, Seoul National University College of Medicine, SNUBH, Bundang Hospital Diabetes = CVD equivalent
NEW DIABETES CARE MEDICATIONS
 NEW DIABETES CARE MEDICATIONS James Bonucchi DO, ECNU, FACE Adult Medicine and Endocrinology Specialists Disclosures Speakers bureau Sanofi AZ BI Diabetes Diabetes cost ADA 2017 data Ever increasing disorder.
NEW DIABETES CARE MEDICATIONS James Bonucchi DO, ECNU, FACE Adult Medicine and Endocrinology Specialists Disclosures Speakers bureau Sanofi AZ BI Diabetes Diabetes cost ADA 2017 data Ever increasing disorder.
Diabetes is a chronic illness that requires
 P O S I T I O N S T A T E M E N T Standards of Medical Care for Patients With Diabetes Mellitus AMERICAN DIABETES ASSOCIATION Diabetes is a chronic illness that requires continuing medical care and patient
P O S I T I O N S T A T E M E N T Standards of Medical Care for Patients With Diabetes Mellitus AMERICAN DIABETES ASSOCIATION Diabetes is a chronic illness that requires continuing medical care and patient
Standards of Care Topics
 Diabetes Boot Camp Class 2 Beverly Dyck Thomassian, RN, MPH, BC ADM, CDE President, Diabetes Education Services Standards of Care 2017 www.diabetesed.net Standards of Care Topics Review the 15 Standards
Diabetes Boot Camp Class 2 Beverly Dyck Thomassian, RN, MPH, BC ADM, CDE President, Diabetes Education Services Standards of Care 2017 www.diabetesed.net Standards of Care Topics Review the 15 Standards
Overview. Diabetes epidemiology Key elements of the VA/DoD Diabetes practice guideline How to integrate the guideline into primary care
 Overview Diabetes epidemiology Key elements of the VA/DoD Diabetes practice guideline How to integrate the guideline into primary care Diabetes Population World-wide 366 million people have diabetes 18.8
Overview Diabetes epidemiology Key elements of the VA/DoD Diabetes practice guideline How to integrate the guideline into primary care Diabetes Population World-wide 366 million people have diabetes 18.8
Diabetes: Use of Adjunctive Therapy ACEs, ARBs, ASA & STATINs --Oh My! Veronica J. Brady, PhD, FNP-BC, BC-ADM, CDE Project ECHO April 19, 2018
 Diabetes: Use of Adjunctive Therapy ACEs, ARBs, ASA & STATINs --Oh My! Veronica J. Brady, PhD, FNP-BC, BC-ADM, CDE Project ECHO April 19, 2018 Points to Ponder ASCVD is the leading cause of morbidity
Diabetes: Use of Adjunctive Therapy ACEs, ARBs, ASA & STATINs --Oh My! Veronica J. Brady, PhD, FNP-BC, BC-ADM, CDE Project ECHO April 19, 2018 Points to Ponder ASCVD is the leading cause of morbidity
RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES
 RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES Risk Factors or Complications Glycemic Control Fasting & Capillary Plasma Glucose Anti-platelet
RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES Risk Factors or Complications Glycemic Control Fasting & Capillary Plasma Glucose Anti-platelet
2018 Diabetes Update
 2018 Diabetes Update Jennifer D. Smith, PharmD, BCACP, BC-ADM, CDE Susan Cornell, PharmD, CDE, FAPhA, FAADE Midwestern University Chicago College of Pharmacy Target Audience: Pharmacists ACPE#: 0202-0000-18-043-L01-P
2018 Diabetes Update Jennifer D. Smith, PharmD, BCACP, BC-ADM, CDE Susan Cornell, PharmD, CDE, FAPhA, FAADE Midwestern University Chicago College of Pharmacy Target Audience: Pharmacists ACPE#: 0202-0000-18-043-L01-P
Overview T2DM medications. Winnie Ho
 Overview T2DM medications Winnie Ho Diabetes in Australia 1.7 million Australians with diabetes, of these 85% have T2DM 2-fold excess risk CV death in patients with diabetes Risk factor for progression
Overview T2DM medications Winnie Ho Diabetes in Australia 1.7 million Australians with diabetes, of these 85% have T2DM 2-fold excess risk CV death in patients with diabetes Risk factor for progression
Why Do We Care About Prediabetes?
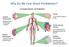 Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Chief of Endocrinology East Orange General Hospital
 Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Understanding the Diabetes Care Process Pfizer Medical Affairs
 Understanding the Diabetes Care Process Pfizer Medical Affairs Overview of Diabetes 1 Diabetes is a group of metabolic diseases characterized by hyperglycemia resulting from defects in insulin secretion,
Understanding the Diabetes Care Process Pfizer Medical Affairs Overview of Diabetes 1 Diabetes is a group of metabolic diseases characterized by hyperglycemia resulting from defects in insulin secretion,
Diabetic Retinopathy and Neuropathy: 2018 Clinical Practice Guidelines
 Diabetic Retinopathy and Neuropathy: 2018 Clinical Practice Guidelines Richard Arakaki, M.D. Phoenix Area Diabetes Consultant August 9 th 2018 Disclose no conflict of interest Complications and Co-morbidities
Diabetic Retinopathy and Neuropathy: 2018 Clinical Practice Guidelines Richard Arakaki, M.D. Phoenix Area Diabetes Consultant August 9 th 2018 Disclose no conflict of interest Complications and Co-morbidities
LOW SUGAR: CAUSES, COMPLICATIONS AND MANAGEMENT OF HYPOGLYCEMIA
 LOW SUGAR: CAUSES, COMPLICATIONS AND MANAGEMENT OF HYPOGLYCEMIA Anne Leake, PhD, APRN-Rx, BC-ADM ECHO Diabetes Learning Group 3/28/2018 Objectives 1. Identify common preventable causes of hypoglycemia
LOW SUGAR: CAUSES, COMPLICATIONS AND MANAGEMENT OF HYPOGLYCEMIA Anne Leake, PhD, APRN-Rx, BC-ADM ECHO Diabetes Learning Group 3/28/2018 Objectives 1. Identify common preventable causes of hypoglycemia
Dept of Diabetes Main Desk
 Dept of Diabetes Main Desk 01202 448060 Glucose management in Type 2 Diabetes in Adults The natural history of type 2 diabetes is for HbA1c to deteriorate with time. A stepwise approach to treatment is
Dept of Diabetes Main Desk 01202 448060 Glucose management in Type 2 Diabetes in Adults The natural history of type 2 diabetes is for HbA1c to deteriorate with time. A stepwise approach to treatment is
