Downloaded from:
|
|
|
- Stuart King
- 5 years ago
- Views:
Transcription
1 Emerging Risk Factors Collaboration (inc Fletcher, AE; ) Sarwar, N; Gao, P; Seshasai, SR; Gobin, R; Kaptoge, S; Di Angelantonio, E; Ingelsson, E; Lawlor, DA; Selvin, E; Stampfer, M; Stehouwer, CD; Lewington, S; Pennells, L; Thompson, A; Sattar, N; White, IR; Ray, KK; Danesh, J (2010) Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies. Lancet, 375 (9733). pp ISSN DOI: Downloaded from: DOI: /S (10) Usage Guidelines Please refer to usage guidelines at or alternatively contact researchonline@lshtm.ac.uk. Available under license:
2 Supplementary webappendix This webappendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: The Emerging Risk Factors Collaboration. Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies. Lancet 2010; 375:
3 Web Extra Material Diabetes mellitus, fasting glucose, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies The Emerging Risk Factors Collaboration 15 June, 2010 Correspondence: Emerging Risk Factors Collaboration Coordinating Centre Department of Public Health and Primary Care University of Cambridge Strangeways Research Laboratory Cambridge CB1 8RN UK erfc@phpc.cam.ac.uk Tel:
4 efigure 1 Flow diagram showing steps involved in study selection for the current analysis. 121 studies included in the Emerging Risk Factors Collaboration by May studies provided relevant information but were not included in the current analyses* 12 studies did not have information at baseline examination on either diabetes status or fasting blood glucose concentration 102 studies (involving participants) were included in the current analyses 97 studies (involving participants) were included in analyses of diabetes 54 studies (involving participants) were included in analyses of fasting blood glucose To be eligible for inclusion in the Emerging Risk Factors Collaboration (ERFC), prospective studies (reported variously as observational cohort studies, trials, or analyses of nested case-control or case-cohort subsets) had: (1) data available from baseline measurements of at least one of the relevant markers assessed; (2) at least 1 year of follow-up; (3) participants not selected on the basis of having previous cardiovascular diseases; and (4) information on cause-specific mortality and/or major cardiovascular morbidity collected during follow-up. Studies were prioritized for inclusion if they were known to have recorded at least person years at risk. Most eligible studies were identified in previously published meta-analyses, with additional studies identified through updated computer-assisted literature searches of databases, scanning of reference lists, hand-searching of relevant journals and correspondence with authors of relevant reports. Further details of the ERFC (including search strategies, contributing studies, data provision and management, and other characteristics) have been reported previously (Eur J Epidemiol. 2007;22: ). * None of the participants in GLOSTRUP and USPHS2 had a history of diabetes at baseline, and fasting glucose information was not provided. of the participants with relevant information in NORTH KARELIA and PREVEND had a history of diabetes, and fasting glucose information was not provided. Data from EAS, LASA and WHI-HaBPS had not been fully harmonised by the ERFC coordinating centre at the time analyses were conducted. 2
5 efigure 2 Prevalence of diabetes at the initial survey in participants in 97 studies A Age-adjusted prevalence of diabetes, by sex 20% 15% Males 10% Prevalence of diabetes (%) 5% 0 5% 10% 15% 20% Prevalence of diabetes (%) 20% 15% 10% 5% 0 Europe North America New Zealand & Australia Israel Japan Caribbean NCS3 NCS2 MRCOLD GOTO13 MONFRI86 NCS1 WHITEII BRHS MCVDRFP CAPS MONFRI89 SHHEC MORGEN WOSCOPS OSLO SPEED REYK EPICNOR TROMSØ WHITEI COPEN NPHSII FINRISK92 GOTOW MALMO GRIPS ATENA PROCAM GREPCO MOSWEGOT FINRISK97 TARFS ZUTE BUPA PRIME GOTO43 FIA MOGERAUG1 BRUN DISCO FINE_IT KIHD MOGERAUG2 BWHHS MOGERAUG3 MATISS87 MICOL ROTT MATISS93 NFR ULSAM EMOFRI MATISS83 PARIS1 HOORN FINE_FIN PROSPER GOTO33 MONFRI94 ATTICA LEADER CASTEL ESTHER ZARAGOZA DRECE AFTCAPS WHS EPESEIOW RANCHO HPFS CHARL USPHS NSHS NHANESI EPESENHA QUEBEC CHS1 EPESEBOS EPESENCA NHANESIII NHS MESA FRAMOFF ARIC HONOL CHS2 BHS DUBBO FLETCHER ISRAEL GOH HISAYAMA OSAKA IKNS PRHHP Females NCS3 MRCOLD NCS2 MONFRI86 WHITEII NCS1 AFTCAPS MONFRI89 SHHEC MCVDRFP EPICNOR MORGEN REYK COPEN TROMSØ BHS FINRISK92 MALMO PROCAM MOSWEGOT EPESEIOW FINRISK97 DUBBO TARFS FIA RANCHO BRUN FLETCHER DISCO NSHS CHARL MOGERAUG2 MOGERAUG3 ROTT MATISS87 EPESENHA MICOL NHANESI CHS1 EPESEBOS MATISS93 PROSPER EPESENCA EMOFRI HOORN MATISS83 NHANESIII MESA HISAYAMA MONFRI94 CASTEL FRAMOFF ATTICA ESTHER OSAKA ZARAGOZA ARIC CHS2 DRECE GOH IKNS GOTO13 BRHS CAPS WOSCOPS WHITEI SPEED OSLO NPHSII GRIPS ZUTE HPFS BUPA FINE_IT PRIME GOTO43 MOGERAUG1 USPHS KIHD QUEBEC ISRAEL FINE_FIN NFR ULSAM PARIS1 GOTO33 LEADER PRHHP HONOL GOTOW WHS ATENA GREPCO BWHHS NHS Study B Age- and sex-adjusted prevalence of diabetes, by study-specific definition of history of diabetes Prevalence of diabetes (%) 20% 15% 10% 5% 0 Based on self-report only Overall prevalence of diabetes: 7.0% (6.1% to 7.9%) Based on self-report and/or fasting glucose concentration GOTO13 MONFRI86 BRHS MCVDRFP MONFRI89 SHHEC AFTCAPS MORGEN WOSCOPS SPEED EPICNOR TROMSØ WHITEI COPEN NPHSII FINRISK92 WHS GRIPS ATENA PROCAM GREPCO MOSWEGOT FINRISK97 ZUTE EPESEIOW PRIME MOGERAUG1 HPFS DISCO FINE_IT CHARL USPHS FLETCHER NSHS MOGERAUG2 MOGERAUG3 MICOL NHANESI ISRAEL EPESENHA QUEBEC NFR EPESEBOS EPESENCA PROSPER GOTO33 FRAMOFF LEADER ESTHER HONOL NCS3 NCS2 MRCOLD NCS1 WHITEII CAPS OSLO REYK BHS GOTOW MALMO TARFS BUPA GOTO43 FIA DUBBO RANCHO BRUN KIHD BWHHS MATISS87 ROTT MATISS93 ULSAM EMOFRI MATISS83 CHS1 PARIS1 HOORN FINE_FIN NHANESIII MONFRI94 NHS HISAYAMA MESA ATTICA PRHHP OSAKA CASTEL ZARAGOZA DRECE ARIC GOH CHS2 IKNS Study C Age- and sex-adjusted prevalence of diabetes, by geographical region People were classified as having diabetes based on self-report or fasting glucose 7 mmol/l. Prevalence was adjusted to age 60. Two studies (ALLHAT and SHS) with adjusted prevalence of diabetes higher than 20% are not presented in this figure. Study 3
6 efigure 3 Mean fasting glucose concentration at baseline by type of blood sample Mean fasting glucose +/- 1SD (mmol/l) Serum Plasma Venous whole blood Capillary Blood Not stated 4 VITA KIHD MATISS93 VHMPP MATISS83 MATISS87 ATTICA MESA MRFIT NCS3 MONFRI94 OSAKA HISAYAMA OSLO ZARAGOZA ARIC IKNS CHS1 CHS2 ALLHAT ROTT GOTO43 WOSCOPS TARFS ULSAM DUBBO GOTO33 EMOFRI PROSPER BRUN RANCHO PARIS1 HOORN NHANESIII BWHHS CASTEL FINE_FIN SHS GOH GOTOW HBS MALMO PRHHP HELSINAG REYK BHS FIA DRECE BUPA ESTHER NCS1 NCS2 CAPS Study 4
7 efigure 4 Cross-sectional correlates of fasting glucose concentration in people without known diabetes at baseline Mean fasting glucose (95% CI), (mmol/l Age (years) Mean fasting glucose (95% CI), mmol/l BMI (kg/m 2 ) Waist/hip ratio Waist (cm) 0.19 (0.18 to 0.21) (0.17 to 0.24) (0.22 to 0.27) SBP (mmhg) DBP (mmhg) HDL-C (mmol/l) 0.17 (0.15 to 0.18) (0.11 to 0.14) (-0.12 to -0.07) Non-HDL-C (mmol/l) Log triglycerides Log CRP 0.10 (0.08 to 0.11) (0.16 to 0.18) (0.07 to 0.10) Mean for tenths of risk factor Race Smoking status Mean fasting glucose (95% CI), mmol/l White Non-White Other Current Alcohol status Physical activity Other Current Not Active Active Category of risk factor Male Female For all correlates except age, response means are adjusted to age 60. For continuous risk markers, values presented are the Pearson s correlation coefficient (95% CI) for the association between the risk marker and fasting glucose concentration in men and women combined. 5
8 efigure 5 Age- and sex-adjusted regression dilution ratios for fasting glucose measurements in people without known history of diabetes at baseline RDR (95% CI) CHS2 TARFS TARFS IKNS TARFS IKNS WOSCOPS SHS IKNS WOSCOPS WOSCOPS IKNS IKNS CHS1 PROSPER WOSCOPS WOSCOPS WOSCOPS ALLHAT KIHD MRFIT MATISS87 TARFS WOSCOPS PROSPER WOSCOPS IKNSIKNS ALLHAT IKNS BRUN BRUN IKNS IKNS IKNS BRUN IKNS MATISS83 MRFIT MRFIT MRFIT OSAKA PROSPER WOSCOPS OSAKA PROSPER TARFS SHS DRECE IKNS CASTEL IKNS BHS ALLHAT OSAKA ALLHAT IKNSIKNS MRFITMRFIT MRFIT OSAKA TARFS ALLHAT IKNS OSAKA OSAKA OSAKA OSAKA OSAKA OSAKA PRHHP OSAKA PARIS1PRHHP OSAKA OSAKA OSAKA MATISS83 ULSAM GOTOW BHS TARFS ULSAM GOTOW Pooled RDR: 0.69 (0.66, 0.72) GOTOW GOTOW GOTOW BHS BHS Time since baseline (yrs) Analyses were based on repeat (re-survey) measurements from participants with information on fasting glucose concentration from more than one survey. For each re-survey, studies with fewer than 50 participants were excluded. In people with known diabetes at baseline, the pooled RDR was 0.49 ( ). 6
9 efigure 6 Hazard ratios for coronary heart disease and ischaemic in people with diabetes at baseline compared with people without diabetes, by additional characteristics Number of participants Number of cases HR (95% CI) Interaction p-value Number of participants Number of cases HR (95% CI) Interaction p-value Geographical region North America Europe Other ( ) 2.05 ( ) 1.86 ( ) ( ) 2.54 ( ) 1.73 ( ) Race White Non-white ( ) 2.01 ( ) ( ) 2.06 ( ) Non-HDL-C (mmol/l) Bottom third Middle third Top third ( ) 2.27 ( ) 2.04 ( ) ( ) 2.39 ( ) 3.06 ( ) HDL-C (mmol/l) Bottom third Middle third Top third ( ) 2.08 ( ) 2.26 ( ) ( ) 2.42 ( ) 2.59 ( ) Log-triglyceride Bottom third Middle third Top third ( ) 2.17 ( ) 2.05 ( ) ( ) 2.28 ( ) 2.53 ( ) People were classified as having diabetes based on self-report or fasting glucose 7 mmol/l. Regression analyses were stratified, where appropriate, by sex and trial group, and adjusted for age, smoking status, BMI and systolic blood pressure. Studies with fewer than 11 cases of an outcome were excluded from the analysis of that outcome. P-values for interaction were calculated from analyses using continuous variables where appropriate. Sizes of data markers are proportional to the inverse of the variance of the hazard ratios. Non-HDL-C: Bottom, middle and top third defined as <3.83, 3.83 to <4.83, and 4.83 mmol/l with mean values of 3.17, 4.33, and 5.72 mmol/l respectively. HDL-C: Bottom, middle and top third defined as <1.14, 1.15 to <1.45, and 1.45 mmol/l with mean values of 0.96, 1.29, and 1.79 mmol/l respectively. Log-triglycerides: bottom, middle and top third defined as <0.07, 0.08 to <0.52, and 0.52 with mean values of -0.24, 0.29, and 0.91 respectively. There was no significant association between overall or sex-specific prevalence of diabetes and risk of coronary heart disease or ischaemic (linear meta-regression P>0.1 for each). 7
10 efigure 7 Hazard ratios for coronary heart disease and ischaemic by baseline fasting glucose concentration between 3.9 and 5.6 mmol/l, in participants without known diabetes at baseline A Coronary heart disease B Ischaemic HR (95% CI) Mean fasting blood glucose concentration (mmol/l) Mean fasting blood glucose concentration (mmol/l) Analyses were based on participants (9479 cases) for CHD and participants (967 cases) for ischaemic. Participants were classified into tenths of fasting glucose for CHD and fifths for ischaemic. Hazard ratios are plotted against the mean fasting glucose in each group. Reference groups are: the 8 th quantile for CHD and the 4 th quantile for (ie, the quantile that contains the overall mean). Regression analyses were stratified, where appropriate, by sex and trial group, and adjusted for age, smoking status, BMI and systolic blood pressure. Studies with fewer than 11 cases of an outcome (with fasting glucose between 3.9 and 5.6 mmol/l) were excluded from analysis of that outcome. Sizes of data markers are proportional to the inverse of the variance of the hazard ratios. 8
11 efigure 8 Hazard ratios for coronary heart disease in people with impaired fasting glucose, by individuallevel characteristics Number of participants Number of cases HR (95% CI) Interaction p-value Sex Male Female ( ) 1.15 ( ) Age at survey Age years Age years Age 70 years ( ) 1.19 ( ) 1.12 ( ) Smoking status Other Current ( ) 1.03 ( ) BMI <25 kg/m 2 25 kg/m ( ) 1.09 ( ) Systolic blood pressure <130 mmhg mmhg ( ) 1.10 ( ) Impaired fasting glucose was defined as those without known diabetes at baseline and fasting glucose values between 5.6 and 6.99 mmol/l (according to ADA criteria). HRs were calculated in reference to people with fasting glucose values below 5.6mmol/L. Regression analyses were stratified, where appropriate, by sex and trial group, and adjusted for age, smoking status, BMI and systolic blood pressure. Studies with fewer than 11 coronary heart disease cases were excluded from analysis. P-values for interaction were calculated from analyses using continuous variables where appropriate. Sizes of data markers are proportional to the inverse of the variance of the hazard ratios. Numbers of participants and cases include people with impaired fasting glucose and those in the reference group. 9
12 efigure 9 Hazard ratios for vascular outcomes in people with diabetes at baseline compared with people without diabetes, using 1-stage ( fixed-effect ) regression models Number of cases HR (95% CI) Coronary heart disease* ( ) Coronary ( ) Non-fatal myocardial infarction ( ) Cerebrovascular disease* ( ) Ischaemic ( ) Haemorrhagic ( ) Unclassified ( ) Other vascular ( ) Analyses were based on up to participants from up to 82 studies. People were classified as having diabetes based on self-report or fasting glucose 7 mmol/l. Regression analyses were stratified, where appropriate, by sex and trial group, and adjusted for age, smoking status, BMI and systolic blood pressure. Studies with fewer than 11 cases of an outcome were excluded from the analysis of that outcome. Sizes of data markers are proportional to the inverse of the variance of the hazard ratios. *Includes both fatal and non-fatal events 10
13 efigure 10 Hazard ratios for coronary heart disease by baseline fasting glucose concentration using 1-stage ( fixed effect ) and continuous regression models A In all participants 4.0 B In participants with baseline fasting glucose concentration between 3.9 and 5.6 mmol/l and no known history of diabetes at baseline 3.0 HR (95% CI) Mean fasting glucose concentration (mmol/l) Mean fasting glucose concentration (mmol/l) No known history of diabetes at baseline, HRs estimated using a 1-stage stratified Cox model Known history of diabetes at baseline, HRs estimated using a 1-stage stratified Cox model ( 95% CI) HRs estimated using a 1-stage continuous fractional polynomial model Regression analyses were stratified, where appropriate, by sex and trial group, and adjusted for age, smoking status, BMI and systolic blood pressure. Studies with fewer than 11 CHD cases and all case-control studies were excluded. Sizes of data markers are proportional to the inverse of the variance of the hazard ratios. Analyses in (a) were based on participants ( cases). Participants with fasting glucose values in the top and bottom 0.2% were excluded. Participants without known diabetes at baseline are classified into groups of fasting glucose: <4, 4-4.5, 4.5-5, 5-5.5, 5.5-6, 6-6.5, 6.5-7, and >7.5 mmol/l. The reference group is defined as those without known diabetes with glucose values between mmol/l. Analyses in (b) were based on participants (9263 cases). Participants are classified into tenths of fasting glucose. The reference group is the 7 th quantile. 11
14 efigure 11 (a) Study-specific hazard ratios for coronary heart disease in people with diabetes at baseline compared with people without diabetes Study HR (95% CI) MONFRI94 MATISS93 DRECE ATENA MOGERAUG3 QUEBEC NSHS GOTO33 GOTO43 OSAKA ZARAGOZA MATISS87 CHS2 BRUN ZUTE FINE_IT FINE_FIN ESTHER HOORN HISAYAMA MORGEN MOGERAUG1 MATISS83 MESA IKNS BWHHS NFR CASTEL LEADER MICOL MOGERAUG2 AFTCAPS FINRISK97 GOH MOSWEGOT FLETCHER PRIME GOTOW FINRISK92 HONOL BUPA TARFS NCS2 NHANESIII NPHSII MCVDRFP ROTT WHITEI PRHHP GOTO13 USPHS RANCHO NHS WHS CAPS SPEED PROSPER NCS3 DUBBO GRIPS WHITEII PARIS1 SHHEC WOSCOPS NCS1 KIHD SHS ULSAM EPICNOR PROCAM CHARL COPEN BHS FIA CHS1 TROMSØ ISRAEL NHANESI ARIC ALLHAT BRHS OSLO MALMO REYK 0.73 ( ) 1.24 ( ) 5.63 ( ) 0.60 ( ) 1.83 ( ) 6.89 ( ) 2.90 ( ) 1.49 ( ) 1.63 ( ) 2.53 ( ) 1.28 ( ) 1.16 ( ) 1.68 ( ) 0.47 ( ) 1.68 ( ) 1.91 ( ) 1.21 ( ) 1.84 ( ) 1.40 ( ) 0.95 ( ) 1.43 ( ) 2.09 ( ) 1.69 ( ) 1.37 ( ) 1.17 ( ) 1.61 ( ) 1.11 ( ) 3.53 ( ) 1.91 ( ) 2.67 ( ) 2.90 ( ) 1.34 ( ) 2.45 ( ) 1.66 ( ) 1.99 ( ) 3.06 ( ) 1.75 ( ) 7.46 ( ) 4.51 ( ) 1.43 ( ) 3.83 ( ) 0.93 ( ) 2.88 ( ) 1.90 ( ) 3.21 ( ) 1.54 ( ) 1.99 ( ) 0.99 ( ) 2.16 ( ) 3.03 ( ) 0.82 ( ) 1.86 ( ) 7.72 ( ) 4.90 ( ) 2.28 ( ) 3.31 ( ) 1.43 ( ) 2.51 ( ) 2.16 ( ) 1.37 ( ) 2.54 ( ) 1.19 ( ) 2.42 ( ) 1.51 ( ) 5.22 ( ) 2.30 ( ) 1.69 ( ) 0.91 ( ) 3.42 ( ) 2.04 ( ) 1.37 ( ) 1.76 ( ) 1.38 ( ) 2.50 ( ) 1.68 ( ) 2.08 ( ) 2.42 ( ) 2.13 ( ) 2.67 ( ) 1.48 ( ) 1.96 ( ) 2.63 ( ) 2.65 ( ) 1.88 ( ) Overall (Random-effects model) Overall (Fixed-effect model 2.00 ( ) 1.98 ( ) Regression analyses were stratified, where appropriate, by sex and trial group, and adjusted for age, smoking status, BMI and systolic blood pressure. Studies are ordered (top to bottom) by increasing number of CHD cases. Studies with fewer than 11 CHD cases were excluded from analysis. Sizes of data markers are proportional to the inverse of the variance of the hazard ratios. 12
15 efigure 11 (b) Study-specific hazard ratios for ischaemic in people with diabetes at baseline compared with people without diabetes Study HR (95% CI) HONOL MCVDRFP AFTCAPS WHITEI BRUN MATISS83 CHARL PRIME ROTT CHS2 MALMO SHHEC NPHSII LEADER PRHHP OSAKA MESA MOSWEGOT SPEED FINRISK97 DUBBO PROCAM FINRISK92 KIHD NHANESI USPHS ULSAM HISAYAMA IKNS REYK WHS TROMSØ CHS1 COPEN ARIC 1.71 ( ) ( ) 4.88 ( ) 6.35 ( ) 1.75 ( ) 1.90 ( ) 0.99 ( ) 1.40 ( ) 1.71 ( ) 1.05 ( ) 5.24 ( ) ( ) 2.30 ( ) 0.96 ( ) 2.12 ( ) 0.75 ( ) 1.88 ( ) 3.39 ( ) 1.09 ( ) 2.44 ( ) 2.61 ( ) 2.14 ( ) 4.29 ( ) 2.69 ( ) 1.83 ( ) 3.31 ( ) 1.31 ( ) 1.79 ( ) 1.69 ( ) 1.42 ( ) 3.15 ( ) 2.64 ( ) 2.14 ( ) 2.24 ( ) 3.01 ( ) Overall (Random-effects model) Overall (Fixed-effect model) 2.27 ( ) 2.33 ( ) Regression analyses were stratified, where appropriate, by sex and trial group, and adjusted for age, smoking status, BMI and systolic blood pressure. Studies are ordered (top to bottom) by increasing number of ischaemic cases. Studies with fewer than 11 ischaemic cases were excluded from analysis. Sizes of data markers are proportional to the inverse of the variance of the hazard ratios. 13
16 efigure 12 Hazard ratios for coronary heart disease and ischaemic by baseline fasting glucose concentration, ignoring known history of diabetes at baseline A Coronary heart disease B Ischaemic HR (95% CI) Mean fasting glucose concentration (mmol/l) Mean fasting glucose concentration (mmol/l) Analyses were based on participants ( cases) for CHD and participants (1754 cases) for ischaemic. Participants are classified into groups of fasting glucose (coronary heart disease: <4, 4-4.5, 4.5-5, 5-5.5, 5.5-6, 6-6.5, 6.5-7, and >7.5 mmol/l; ischaemic : <4.5, 4.5-5, 5-5.5, 5.5-6, 6-7, and >7 mmol/l). Hazard ratios are plotted against the mean fasting glucose in each group. The reference group for both outcomes is mmol/l. Regression analyses were stratified, where appropriate, by sex and trial group, and adjusted for age, smoking status, BMI and systolic blood pressure. Studies with fewer than 11 cases of an outcome were excluded from analysis of that outcome. Sizes of data markers are proportional to the inverse of the variance of the hazard ratios. 14
17 efigure 13 Hazard ratios for coronary heart disease and ischaemic by baseline fasting glucose concentration, including categories in the range 7-9 mmol/l A Coronary heart disease B Ischaemic HR (95% CI) Mean fasting glucose concentration (mmol/l) Mean fasting glucose concentration (mmol/l) No known history of diabetes at baseline survey Known history of diabetes at baseline survey Analyses were based on participants ( cases) for CHD and participants (1754 cases) for ischaemic. People were classified as having diabetes based on selfreport or fasting glucose 7 mmol/l. Participants without known diabetes at baseline are classified into groups of fasting glucose (coronary heart disease: <4, 4-4.5, 4.5-5, 5-5.5, 5.5-6, 6-6.5, 6.5-7, 7-7.5, 7.5-8, 8-8.5, and >9 mmol/l; ischaemic : <4.5, 4.5-5, 5-5.5, 5.5-6, 6-6.5, 6.5-7, 7-7.5, 7.5-8, 8-8.5, and >9 mmol/l). Hazard ratios are plotted against the mean fasting glucose in each group. The reference group for both outcomes is mmol/l. Regression analyses were stratified, where appropriate, by sex and trial group, and adjusted for age, smoking status, BMI and systolic blood pressure. Studies with fewer than 11 cases of an outcome were excluded from analysis of that outcome. Sizes of data markers are proportional to the inverse of the variance of the hazard ratios. 15
18 efigure 14 Hazard ratios for coronary heart disease and vascular death in people with diabetes compared with people without diabetes, allowing for time-dependent diabetes status A Coronary heart disease HR (95% CI) Baseline Incidence of diabetes (% per year) B Vascular death HR (95% CI) Baseline Incidence of diabetes (% per year) Analyses were based on participants ( cases) for CHD and participants ( cases) for vascular. HRs were estimated using a two-stage approach where study-specific HRs were calculated then pooled across studies by random-effects meta-analyses. In the first stage, regression analyses were stratified, where appropriate, by sex and trial group, and adjusted for age, smoking status, BMI and systolic blood pressure. In the baseline analyses (indicated by red markers) diabetes status was defined only according to the baseline measurement. In the other analyses, diabetes status was modelled as a time dependent continuous variable to represent the probability of having diabetes (range between 0 and 1). Multiple records were used for each participant when available. Up to repeat measurements from participants contributed to the analyses. Diabetes status was assessed at baseline and reassessed at each re-survey. People were classified as having diabetes based on self-report or fasting glucose 7 mmol/l. Participants classified as having diabetes kept diabetes status of 1 until time of event. For participants with no known diabetes, the probability of having diabetes was calculated according to the incident rates of diabetes (% per year) based on the cumulative exponential distribution. Case-control and studies with fewer than 11 cases of an outcome were excluded from analysis of that outcome. Sizes of data markers are proportional to the inverse of the variance of the hazard ratios. 16
19 etable 1. Characteristics of the 102 individual studies included in analyses. Study abbreviation Cohort studies Location Population source Sampling method No. of participants Mean (SD) age at survey Number (%) Male Number (%) with diabetes at baseline Mean (SD) fasting glucose (mmol/l) at baseline ARIC USA Households Random (6) 6297 (43) 1589 (11) 6.0 (2.1) ATENA Italy Volunteers Random (7) 0 (0) 118 (2) - ATTICA Greece General population Random (11) 822 (51) 147 (9) 5.3 (1.5) BHS Australia Electoral rolls Complete (16) 2940 (47) 122 (2) 5.1 (1.1) BRHS UK GP/Health service lists Random (6) 6810 (100) 77 (1) - BRUN Italy Population register Random (11) 398 (49) 44 (5) 5.5 (1.0) BUPA UK GP/Health service lists Complete (8) (100) 159 (1) 5.4 (1.1) BWHHS UK General population Random (5) 0 (0) 245 (8) 6.0 (1.4) CAPS UK Electoral rolls Random (5) 2161 (100) 30 (1) 6.3 (2.1) CASTEL Italy Screening Complete (5) 963 (38) 484 (19) 6.1 (1.7) CHARL USA Households Random (11) 866 (45) 83 (4) - CHS1 USA Medicare lists Random (5) 1483 (38) 495 (13) 6.0 (1.8) CHS2 USA Medicare lists Random (5) 178 (38) 104 (22) 6.5 (2.9) COPEN Denmark General population Random (15) 3587 (43) 247 (3) - DISCO Italy NR NR (11) 846 (44) 79 (4) - DRECE Spain General population Random (11) 1384 (48) 192 (7) 5.3 (1.4) DUBBO Australia Electoral rolls Complete (7) 866 (42) 139 (7) 5.1 (1.1) EMOFRI Italy General population Random (6) 176 (49) 24 (7) 5.4 (1.7) EPESEBOS USA General population Complete (5) 353 (34) 131 (13) - EPESEIOW USA General population Complete (5) 511 (32) 115 (7) - EPESENCA USA General population Random (5) 448 (33) 177 (13) - EPESENHA USA General population Random (6) 302 (37) 92 (11) - ESTHER Germany GP listings Complete (7) 3394 (42) 1055 (13) 5.4 (1.6) FINE_FIN Finland NR NR (5) 279 (100) 42 (15) 6.1 (2.0) FINE_IT Italy Survivors of an existing cohort Complete (5) 475 (100) 41 (9) - FINRISK92 Finland General population Random (10) 2438 (46) 96 (2) - FINRISK97 Finland General population Random (11) 3138 (50) 213 (3) - Offspring or spouse to Framingham 291 (10) FRAMOFF USA Complete (10) 1269 (44) - heart study participants GOH Israel General population Random (9) 1380 (50) 255 (9) 8.8 (3.4) GOTO13 Sweden General population Complete (0) 766 (100) 8 (1) - 17
20 Study abbreviation Location Population source Sampling method No. of participants Mean (SD) age at survey Number (%) Male Number (%) with diabetes at baseline Mean (SD) fasting glucose (mmol/l) at baseline GOTO33 Sweden General population Complete (0) 733 (100) 54 (7) 5.1 (1.9) GOTO43 Sweden General population Complete (0) 773 (100) 26 (3) 4.7 (1.3) GOTOW Sweden General population Random (7) 0 (0) 27 (2) 4.2 (1.1) GREPCO Italy NR NR (8) 0 (0) 17 (2) - GRIPS Germany Occupational Complete (5) 5786 (100) 124 (2) - HBS Finland Occupational Complete (4) 1142 (100) 19 (2) 4.9 (1.0) HELSINAG Finland Population register Random (4) 131 (25) 0 (0) 5.6 (1.9) HISAYAMA Japan General population Complete (12) 1087 (42) 295 (11) 5.8 (1.3) HONOL USA GP/Health service lists Complete (4) 2571 (100) 651 (25) - HOORN Netherlands General population Random (7) 983 (44) 207 (9) 5.7 (1.5) IKNS Japan General population Complete (10) 3300 (41) 1305 (16) 6.0 (1.3) ISRAEL Israel Occupational Occupational (7) 7838 (100) 384 (5) - KIHD Finland General population Random (5) 2068 (100) 91 (4) 4.7 (1.0) MALMO Sweden Screening Random (7) (67) 630 (2) 5.0 (1.0) MATISS83 Italy Electoral rolls Random (10) 1197 (47) 168 (7) 5.3 (1.3) MATISS87 Italy Electoral rolls Random (9) 933 (44) 101 (5) 5.3 (1.2) MATISS93 Italy Electoral rolls Random (9) 588 (49) 66 (5) 5.0 (1.4) MCVDRFP Netherlands General population Random (10) (46) 231 (1) - MESA USA General population Random (10) 3186 (47) 844 (12) 5.4 (1.7) MICOL Italy Electoral rolls NR (10) (55) 1149 (5) - MOGERAUG1 Germany General population Random (6) 874 (100) 37 (4) - MOGERAUG2 Germany General population Random (12) 1974 (49) 200 (5) - MOGERAUG3 Germany General population Random (11) 1676 (49) 183 (5) - MONFRI86 Italy NR NR (9) 556 (49) 11 (1) - MONFRI89 Italy NR NR (8) 545 (49) 14 (1) - MONFRI94 Italy Electoral rolls Random (8) 632 (49) 96 (7) 5.7 (1.4) MORGEN Netherlands General population Random (9) 8063 (45) 226 (1) - MOSWEGOT Sweden General population Random (11) 1972 (47) 99 (2) - MRCOLD UK GP/Health service lists Random (4) 3937 (37) 271 (3) - NCS1 Norway General population Complete (4) (49) 189 (1) 5.7 (1.1) NCS2 Norway General population Complete (4) 6684 (51) 76 (1) 5.7 (0.8) NCS3 Norway General population Complete (4) 5283 (52) 47 (0) 5.6 (0.7) NFR Italy NR NR (5) 3133 (100) 202 (6) - 18
21 Study abbreviation Location Population source Sampling method No. of participants Mean (SD) age at survey Number (%) Male Number (%) with diabetes at baseline Mean (SD) fasting glucose (mmol/l) at baseline NHANESI USA General population Cluster (15) 4617 (40) 631 (5) - NHANESIII USA General population Cluster (16) 5801 (46) 1226 (10) 5.8 (1.9) NPHSII UK GP/Health service lists Complete (3) 2968 (100) 74 (2) - NSHS Canada General population Random (16) 932 (48) 108 (6) - OSAKA Japan General population or occupational Complete (10) 8335 (68) 1231 (10) 5.7 (1.2) OSLO Norway General population Complete & random (6) (100) 221 (1) 5.8 (1.0) PARIS1 France Occupational Complete (2) 7079 (100) 385 (5) 5.7 (0.9) PRHHP Caribbean General population Complete (6) 6350 (100) 644 (10) 5.4 (1.7) PRIME France/NI General population Quota (3) 9582 (100) 385 (4) - PROCAM Germany Occupational Complete (10) (72) 414 (2) - QUEBEC Canada General population Random (7) 1307 (100) 90 (7) - RANCHO USA Households Complete (11) 744 (41) 133 (7) 5.5 (1.1) REYK Iceland General population Complete (9) 8060 (48) 322 (2) 4.5 (0.8) ROTT Netherlands General population Complete (8) 1824 (38) 432 (9) 8.7 (4.5) SHHEC UK GP/Health service lists Random (7) 5398 (49) 143 (1) - SHS USA General population Complete (8) 1614 (39) 2032 (49) 8.3 (4.2) SPEED UK GP/Health service lists Complete (4) 2126 (100) 41 (2) - TARFS Turkey Households Random (13) 1760 (50) 95 (3) 4.9 (1.2) TROMSØ Norway Households Complete (15) (47) 380 (2) - ULSAM Sweden General population Complete (1) 2280 (100) 122 (5) 5.0 (0.9) VHMPP Austria Health check-up Complete (13) (48) 0 (0) 5.0 (1.5) VITA Italy Census lists Random (8) 4055 (45) 0 (0) 4.6 (1.3) WHITEI UK Occupational Complete (5) 4013 (100) 191 (5) - WHITEII UK Occupational Complete (6) 6802 (67) 92 (1) 6.2 (-) WHS USA Occupational Complete (7) 0 (0) 770 (3) - ZARAGOZA Spain GP/Health service lists Complete (12) 1528 (42) 465 (13) 5.9 (1.6) ZUTE Netherlands General population Random (4) 390 (100) 30 (8) - Case-control studies USPHS USA Occupational Complete (9) 934 (100) 56 (6) - EPICNOR UK GP/Health service lists Complete (8) 966 (68) 46 (3) - FIA Sweden General population Random (7) 2116 (81) 106 (4) 5.5 (1.1) FLETCHER New Zealand Occupational, electoral rolls Complete & random (12) 405 (85) 27 (6) - HPFS USA Occupational Random (8) 736 (100) 47 (6) - 19
22 Study abbreviation Location Population source Sampling method No. of participants Mean (SD) age at survey Number (%) Male Number (%) with diabetes at baseline Mean (SD) fasting glucose (mmol/l) at baseline NHS USA Occupational Random (6) 0 (0) 77 (11) - Clinical trials AFTCAPS USA Screening Complete (7) 5587 (85) 127 (2) - USA/Canada/Puerto (43) ALLHAT General population NR (8) (49) 7.0 (3.3) Rico/US Virgin Islands LEADER UK GP listings Complete (9) 941 (100) 152 (16) - MRFIT USA Screening Complete (6) (100) 425 (3) 5.5 (0.9) Scotland/Ireland/ 477 (15) PROSPER Screening Complete (3) 1350 (42) 5.5 (1.5) Netherlands WOSCOPS UK Screening Complete (6) 6214 (100) 115 (2) 4.8 (0.7) Studies with information on history of diabetes at baseline* TOTAL (97 studies) (13) (56) (7) 5.5 (2.0) Studies with information on fasting glucose concentration TOTAL (54 studies) (12) (60) (8) 5.4 (1.8) studies TOTAL (102 studies) (13) (57) (6) 5.4 (1.8) *2 studies provided data on previous history of diabetes but were not included in the analyses of diabetes because none of the participants (MRFIT) and all of the participants with history of diabetes information (HBS) had diabetes. 3 studies (HELSINAG, VITA and VHMPP) did not provide data on previous history of diabetes. 48 studies did not provide information on fasting glucose concentration. 20
23 etable 2 Definitions of outcomes assessed in the current report Outcome ICD version ICD-9 ICD-10 Myocardial infarction 410, 412 I21, I22 Coronary heart disease I20 I25 Ischaemic 433, 434 I63 Haemorrhagic 431 I61 Unclassified * 436 I64 Other cerebrovascular disease 430, 432, 435, 437, 438 F01, I60, I62, I65-I69 Other cardiovascular outcomes 093, 391, , , , , , 458, 459, , 798 G45, I01, I05-I15, I20, I26-I28, I30- I52, I70-I82, I87,I95, I97-I99, Q20- Q28, R96 Corresponding ICD-6, 7 or 8 codes were used for studies that recorded outcomes using earlier ICD versions. *Unclassified was defined by the ICD codes stated, or as s not specified as ischaemic or haemorrhagic by study-specific codes. 21
24 etable 3 Baseline characteristics of participants with information on self-reported diabetes status (with or without supplementary information on fasting glucose) Overall summary statistics No of studies No of participants Mean (SD) or % Diabetes status Definite % Other % Non-lipid markers Age at survey (yrs) (13) Fasting glucose (mmol/l) (1.8) BMI (kg/m 2 ) (4) Waist-to-hip ratio (0.08) Waist (cm) (12) SBP (mmhg) (19) DBP (mmhg) (11) Lipid markers Total cholesterol (mmol/l) (1.10) Non-HDL-C (mmol/l) (1.12) HDL-C (mmol/l) (0.38) Log triglycerides (0.52) Apo B (g/l) (0.28) Apo AI (g/l) (0.27) Inflammatory markers Log-CRP (1.11) Fibrinogen (g/l) (0.71) Categorical variables Sex Male % Female % Race Non-white % White % Geographical region North America % Europe % Australia % New Zealand <0.5% Israel % Japan % Caribbean % Smoking status Current % Other % Alcohol status Current % Other % *2 studies provided data on history of diabetes but were not included in the analyses of diabetes because none of the participants (MRFIT) and all of the participants with history of diabetes information (HBS) had diabetes. A further participants had information on fasting glucose concentration at baseline, but no information on self-reported diabetes status. 22
25 etable 4 Summary of vascular outcomes recorded. Study No. of participants Median follow-up (5th & 95th percentiles) CVD events CVD CHD CHD MI MI (nonfatal) MI Cohort studies ARIC (5.0 to 15.7) ATENA (5.2 to 8.1) ATTICA (5.0 to 5.0) BHS (7.1 to 33.2) BRHS (4.7 to 25.4) BRUN (3.9 to 15.5) BUPA (11.3 to 26.7) BWHHS (3.1 to 8.4) CAPS (4.0 to 13.0) CASTEL (2.3 to 14.0) CHARL (3.5 to 40.0) CHS (2.0 to 12.9) CHS (1.5 to 9.5) COPEN (2.4 to 14.9) DISCO (5.5 to 9.5) DRECE (15.5 to 16.6) DUBBO (1.8 to 14.9) EMOFRI (6.5 to 7.2) EPESEBOS (6.4 to 10.9) EPESEIOW (6.8 to 11.1) EPESENCA (6.5 to 10.9) EPESENHA (6.3 to 10.8) ESTHER (2.0 to 5.9) FINE_FIN (0.9 to 10.0) FINE_IT (1.8 to 21.4) FINRISK (7.1 to 11.9) FINRISK (6.0 to 6.9) FRAMOFF (4.7 to 14.4) GOH (14.4 to 36.0) GOTO (5.0 to 30.5) GOTO (5.8 to 13.1) CBVD events Ischaem. Ischaem. Ischaem. (nonfatal) Haemorrhagic Unclassified Unclassified Unclassified (nonfatal) Other vascular -cause mortality 23
26 Study No. of participants Median follow-up (5th & 95th percentiles) CVD events CVD CHD CHD MI MI (nonfatal) MI GOTO (7.9 to 10.7) GOTOW (8.9 to 32.7) GREPCO (7.7 to 8.9) GRIPS (4.8 to 10.0) HBS (6.0 to 20.5) HELSINAG (1.7 to 11.0) HISAYAMA (3.2 to 14.0) HONOL (1.4 to 7.6) HOORN (3.7 to 9.9) IKNS (5.1 to 18.6) ISRAEL (7.9 to 23.9) KIHD (2.9 to 24.1) MALMO (7.9 to 22.6) MATISS (6.4 to 19.5) MATISS (7.0 to 16.2) MATISS (6.8 to 9.3) MCVDRFP (13.6 to 18.9) MESA (2.5 to 5.2) MICOL (4.7 to 7.1) MOGERAUG (3.6 to 13.4) MOGERAUG (2.3 to 8.4) MOGERAUG (1.8 to 3.6) MONFRI (6.2 to 16.9) MONFRI (6.7 to 13.7) MONFRI (7.0 to 8.8) MORGEN (8.5 to 13.1) MOSWEGOT (7.6 to 18.6) MRCOLD (1.1 to 11.7) NCS (14.4 to 16.7) NCS (15.5 to 17.8) NCS (12.1 to 18.8) NFR (6.1 to 11.2) NHANESI (4.7 to 21.0) NHANESIII (3.4 to 11.8) CBVD events Ischaem. Ischaem. Ischaem. (nonfatal) Haemorrhagic Unclassified Unclassified Unclassified (nonfatal) Other vascular -cause mortality 24
27 Study No. of participants Median follow-up (5th & 95th percentiles) CVD events CVD CHD CHD MI MI (nonfatal) MI NPHSII (3.4 to 10.4) NSHS (3.3 to 10.0) OSAKA (3.9 to 18.8) OSLO (10.9 to 30.5) PARIS (7.6 to 26.1) PRHHP (5.1 to 12.0) PRIME (5.0 to 7.3) PROCAM (3.9 to 18.9) QUEBEC (3.5 to 5.6) RANCHO (2.0 to 18.1) REYK (6.3 to 37.1) ROTT (3.0 to 14.2) SHHEC (6.9 to 10.0) SHS (2.0 to 14.3) SPEED (3.3 to 18.2) TARFS (4.9 to 18.0) TROMSØ (5.1 to 19.3) ULSAM (6.5 to 35.9) VHMPP (1.3 to 13.7) VITA (1.7 to 5.3) WHITEI (2.0 to 8.4) WHITEII (4.8 to 14.1) WHS (8.4 to 10.8) ZARAGOZA (4.0 to 5.1) ZUTE (1.1 to 10.1) Case-control studies USPHS EPICNOR (2.2 to 9.3) FIA (0.5 to 9.3) FLETCHER (1.8 to 6.4) HPFS (1.2 to 6.0) NHS (1.4 to 8.8) Clinical trials AFTCAPS (4.3 to 6.7) CBVD events Ischaem. Ischaem. Ischaem. (nonfatal) Haemorrhagic Unclassified Unclassified Unclassified (nonfatal) Other vascular -cause mortality 25
28 Study No. of participants Median follow-up (5th & 95th percentiles) CVD events CVD CHD CHD MI MI (nonfatal) MI ALLHAT (0.8 to 6.7) LEADER (0.8 to 6.2) MRFIT (4.4 to 7.8) PROSPER (1.1 to 3.8) WOSCOPS (2.9 to 6.0) Studies with information on history of diabetes at baseline* TOTAL (97 studies) (3.2 to 25.9) CBVD events Ischaem. Ischaem. Ischaem. (nonfatal) Haemorrhagic Unclassified Unclassified Unclassified (nonfatal) Other vascular -cause mortality Studies with information on fasting glucose concentration TOTAL (54 studies) (2.1 to 26.1) studies TOTAL (102 studies) (2.8 to 25.6) CVD indicates cardiovascular disease; CBVD cerebrovascular disease. *2 studies provided data on history of diabetes but were not included in the analyses of diabetes because none of the participants (MRFIT) and all of the participants with history of diabetes information (HBS) had diabetes. 3 studies (HELSINAG, VITA and VHMPP) did not provide data on history of diabetes. 48 studies did not provide information on fasting glucose concentration. 26
29 etable 5 Hazard ratios for coronary heart disease in people with diabetes compared with people without diabetes, progressively adjusted for baseline levels of several risk factors. (a) Adjusted for conventional risk factors. Data from studies with complete information on sex, age, smoking, BMI, SBP, HDL-C, non-hdl-c and triglycerides With adjustment for... HR (95% CI) 2 Q statistic (df) participants; cases P for heterogeneity between studies I 2 (95% CI) Age 2.06 (1.82, 2.34) (60) < (62-78) Plus smoking 2.10 (1.85, 2.39) (60) < (62-77) Plus BMI 2.00 (1.78, 2.25) (60) < (55-74) Plus SBP 1.91 (1.70, 2.14) (60) < (52-72) Plus non-hdl-c 1.93 (1.71, 2.16) (60) < (51-72) Plus HDL-C 1.87 (1.67, 2.09) (60) < (47-70) Plus log-triglycerides 1.87 (1.67, 2.09) (60) < (45-69) (b) Adjusted for conventional risk factors and apolipoproteins. Data from studies with complete information on sex, age, smoking, BMI, SBP, HDL-C, non-hdl-c and triglycerides With adjustment for... HR (95% CI) 2 Q statistic (df) P for heterogeneity between studies I 2 (95% CI) participants; 4998 Age 2.42 (1.91, 3.08) (21) < (74-88) Plus smoking 2.47 (1.95, 3.13) (21) < (72-87) Plus BMI 2.29 (1.82, 2.87) (21) < (68-86) Plus SBP 2.16 (1.73, 2.70) (21) < (66-85) Plus Apo-B 2.19 (1.77, 2.71) (21) < (61-83) Plus Apo-A (1.71, 2.61) (21) < (60-83) Plus log-triglycerides 2.08 (1.69, 2.55) (21) < (57-82) (c) Adjusted for conventional risk factors and waist-to-hip ratio (WHR). Data from studies with complete information on sex, age, smoking, BMI, SBP, HDL-C, non-hdl-c and triglycerides With adjustment for... HR (95% CI) 2 Q statistic (df) P for heterogeneity between studies I 2 (95% CI) participants; 4552 cases Age 2.07 (1.76, 2.45) (23) < (39-75) Plus smoking 2.12 (1.80, 2.51) (23) < (40-75) Plus WHR 1.99 (1.72, 2.31) (23) (18-68) Plus SBP 1.87 (1.62, 2.17) (23) (16-68) Plus non-hdl-c 1.88 (1.62, 2.18) (23) (20-69) Plus HDL-C 1.81 (1.57, 2.09) (23) (12-66) Plus log-triglycerides 1.83 (1.59, 2.12) (23) (10-66) (d) Adjusted for other vascular risk factors. With adjustment for... No. of participants No. of events HR (95% CI) Wald 2 Conventional risk factors (1.69, 2.37) 64.7 Plus fibrinogen (1.65, 2.29) 63.6 Conventional risk factors (1.61, 2.32) 50.2 Plus log-crp (1.59, 2.28) 49.4 Conventional risk factors (1.57, 2.09) 64.8 Plus egfr (1.57, 2.10) 64.4 Conventional risk factors (1.45, 1.90) 53.1 Plus fasting glucose (1.35, 1.75) 42.4 Conventional risk factors included age, smoking status, BMI, systolic blood pressure, non-hdl-c, HDL-C and log triglycerides. Studies with fewer than 11 events for an outcome were excluded from the analysis of that outcome. regression analyses were stratified, where appropriate, by sex and trial group. 27
University of Bristol - Explore Bristol Research. Peer reviewed version. Link to published version (if available): /S (18)30134-X
 Emerging Risk Factors Collaboration/EPIC-CVD/UK Biobank Alcohol Study Group (2018). Risk thresholds for alcohol consumption: combined analysis of individual-participant data on 599,912 current drinkers
Emerging Risk Factors Collaboration/EPIC-CVD/UK Biobank Alcohol Study Group (2018). Risk thresholds for alcohol consumption: combined analysis of individual-participant data on 599,912 current drinkers
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Wood AM, Kaptoge S, Butterworth AS, et al.
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Wood AM, Kaptoge S, Butterworth AS, et al.
Supplementary Online Content
 Supplementary Online Content Gregson J, Kaptoge S, Bolton T, et al; Emerging Risk Factors Collaboration. Cardiovascular risk factors associated with venous thromboembolism. JAMA Cardiol. Published online
Supplementary Online Content Gregson J, Kaptoge S, Bolton T, et al; Emerging Risk Factors Collaboration. Cardiovascular risk factors associated with venous thromboembolism. JAMA Cardiol. Published online
Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies
 Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies The Emerging Risk Factors Collaboration* Summary Background
Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies The Emerging Risk Factors Collaboration* Summary Background
C-reactive protein concentration and risk of coronary heart disease, stroke, and mortality: an individual participant meta-analysis
 C-reactive protein concentration and risk of coronary heart disease, stroke, and mortality: an individual participant meta-analysis The Emerging Risk Factors Collaboration* Lancet 2010; 375: 132 40 Published
C-reactive protein concentration and risk of coronary heart disease, stroke, and mortality: an individual participant meta-analysis The Emerging Risk Factors Collaboration* Lancet 2010; 375: 132 40 Published
University of Bristol - Explore Bristol Research
 The Global BMI Mortality Collaboration, & Bansal, N. (06). Body-mass index and all-cause mortality: individual-participant-data meta-analysis of 39 prospective studies in four continents. Lancet, 3(006),
The Global BMI Mortality Collaboration, & Bansal, N. (06). Body-mass index and all-cause mortality: individual-participant-data meta-analysis of 39 prospective studies in four continents. Lancet, 3(006),
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL A Meta-analysis of LDL-C, non-hdl-c, and apob as markers of cardiovascular risk. Slide # Contents 2 Table A1. List of candidate reports 8 Table A2. List of covariates/model adjustments
SUPPLEMENTAL MATERIAL A Meta-analysis of LDL-C, non-hdl-c, and apob as markers of cardiovascular risk. Slide # Contents 2 Table A1. List of candidate reports 8 Table A2. List of covariates/model adjustments
Advanced IPD meta-analysis methods for observational studies
 Advanced IPD meta-analysis methods for observational studies Simon Thompson University of Cambridge, UK Part 4 IBC Victoria, July 2016 1 Outline of talk Usual measures of association (e.g. hazard ratios)
Advanced IPD meta-analysis methods for observational studies Simon Thompson University of Cambridge, UK Part 4 IBC Victoria, July 2016 1 Outline of talk Usual measures of association (e.g. hazard ratios)
Articles. Funding British Heart Foundation and UK Medical Research Council.
 Separate and combined associations of body-mass index and abdominal adiposity with cardiovascular disease: collaborative analysis of 58 prospective studies The Emerging Risk Factors Collaboration* Summary
Separate and combined associations of body-mass index and abdominal adiposity with cardiovascular disease: collaborative analysis of 58 prospective studies The Emerging Risk Factors Collaboration* Summary
Supplementary Online Content
 Supplementary Online Content Åsvold BO, Vatten LJ, Bjøro T, et al; Thyroid Studies Collaboration. Thyroid function within the normal range and risk of coronary heart disease: an individual participant
Supplementary Online Content Åsvold BO, Vatten LJ, Bjøro T, et al; Thyroid Studies Collaboration. Thyroid function within the normal range and risk of coronary heart disease: an individual participant
Major Lipids, Apolipoproteins, and Risk of Vascular Disease
 Europe PMC Funders Group Author Manuscript Published in final edited form as: JAMA. 2009 November 11; 302(18): 1993 2000. doi:10.1001/jama.2009.1619. Major Lipids, Apolipoproteins, and Risk of Vascular
Europe PMC Funders Group Author Manuscript Published in final edited form as: JAMA. 2009 November 11; 302(18): 1993 2000. doi:10.1001/jama.2009.1619. Major Lipids, Apolipoproteins, and Risk of Vascular
Supplementary Online Content
 Supplementary Online Content Den Ruijter HM, Peters SA, Anderson TJ, et al. Common carotid intimamedia thickness measurements in cardiovascular risk prediction. JAMA. doi:10.1001/jama.2012.9630. etable
Supplementary Online Content Den Ruijter HM, Peters SA, Anderson TJ, et al. Common carotid intimamedia thickness measurements in cardiovascular risk prediction. JAMA. doi:10.1001/jama.2012.9630. etable
The Clinical Unmet need in the patient with Diabetes and ACS
 The Clinical Unmet need in the patient with Diabetes and ACS Professor Kausik Ray (UK) BSc(hons), MBChB, MD, MPhil, FRCP (lon), FRCP (ed), FACC, FESC, FAHA Diabetes is a global public health challenge
The Clinical Unmet need in the patient with Diabetes and ACS Professor Kausik Ray (UK) BSc(hons), MBChB, MD, MPhil, FRCP (lon), FRCP (ed), FACC, FESC, FAHA Diabetes is a global public health challenge
RELIABLE ASSESSMENT OF THE
 ORIGINAL CONTRIBUTION Major Lipids, Apolipoproteins, and Risk of Vascular Disease The Emerging Risk Factors Collaboration* Context Associations of major lipids and apolipoproteins with the risk of vascular
ORIGINAL CONTRIBUTION Major Lipids, Apolipoproteins, and Risk of Vascular Disease The Emerging Risk Factors Collaboration* Context Associations of major lipids and apolipoproteins with the risk of vascular
Prof. Renata Cífková, MD, CSc.
 Prof. Renata Cífková, MD, CSc. Head of the Department of Preventive Cardiology, Thomayer Teaching Hospital, Prague Focuses on arterial hypertension epidemiology, clinical trials, target organ damage prevention
Prof. Renata Cífková, MD, CSc. Head of the Department of Preventive Cardiology, Thomayer Teaching Hospital, Prague Focuses on arterial hypertension epidemiology, clinical trials, target organ damage prevention
Antihypertensive Trial Design ALLHAT
 1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
(n=6279). Continuous variables are reported as mean with 95% confidence interval and T1 T2 T3. Number of subjects
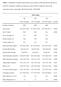 Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Supplementary webappendix
 Supplementary webappendix This webappendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Ray K K, Seshasai S R K, Wijesuriya S,
Supplementary webappendix This webappendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Ray K K, Seshasai S R K, Wijesuriya S,
CVD risk estimation in populations with high prevalence of MetS. Dilek Ural, 12 March 2017 Koç University, Istanbul
 CVD risk estimation in populations with high prevalence of MetS Dilek Ural, 12 March 2017 Koç University, Istanbul Understanding CV risk Likelihood of a person developing an atherosclerotic CV event over
CVD risk estimation in populations with high prevalence of MetS Dilek Ural, 12 March 2017 Koç University, Istanbul Understanding CV risk Likelihood of a person developing an atherosclerotic CV event over
John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam
 Latest Insights from the JUPITER Study John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam Inflammation, hscrp, and Vascular Prevention
Latest Insights from the JUPITER Study John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam Inflammation, hscrp, and Vascular Prevention
An example of a systematic review and meta-analysis
 An example of a systematic review and meta-analysis Sattar N et al. Statins and risk of incident diabetes: a collaborative meta-analysis of randomised statin trials. Lancet 2010; 375: 735-742. Search strategy
An example of a systematic review and meta-analysis Sattar N et al. Statins and risk of incident diabetes: a collaborative meta-analysis of randomised statin trials. Lancet 2010; 375: 735-742. Search strategy
Should we prescribe aspirin and statins to all subjects over 65? (Or even all over 55?) Terje R.Pedersen Oslo University Hospital Oslo, Norway
 Should we prescribe aspirin and statins to all subjects over 65? (Or even all over 55?) Terje R.Pedersen Oslo University Hospital Oslo, Norway The Polypill A strategy to reduce cardiovascular disease by
Should we prescribe aspirin and statins to all subjects over 65? (Or even all over 55?) Terje R.Pedersen Oslo University Hospital Oslo, Norway The Polypill A strategy to reduce cardiovascular disease by
Models of preventive care in clinical practice to achieve 25 by 25
 Models of preventive care in clinical practice to achieve 25 by 25 Professor David A Wood Garfield Weston Professor of Cardiovascular Medicine International Centre for Circulatory Health Imperial College
Models of preventive care in clinical practice to achieve 25 by 25 Professor David A Wood Garfield Weston Professor of Cardiovascular Medicine International Centre for Circulatory Health Imperial College
Is there a mechanism of interaction between hypertension and dyslipidaemia?
 Is there a mechanism of interaction between hypertension and dyslipidaemia? Neil R Poulter International Centre for Circulatory Health NHLI, Imperial College London Daegu, Korea April 2005 Observational
Is there a mechanism of interaction between hypertension and dyslipidaemia? Neil R Poulter International Centre for Circulatory Health NHLI, Imperial College London Daegu, Korea April 2005 Observational
STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY. Harvey D White on behalf of The STABILITY Investigators
 STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY Harvey D White on behalf of The STABILITY Investigators Lipoprotein- associated Phospholipase A 2 (Lp-PLA 2 ) activity:
STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY Harvey D White on behalf of The STABILITY Investigators Lipoprotein- associated Phospholipase A 2 (Lp-PLA 2 ) activity:
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Natriuretic Peptides Studies Collaboration.
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Natriuretic Peptides Studies Collaboration.
Supplementary Online Content
 Supplementary Online Content McEvoy JW, Chen Y, Ndumele CE, et al. Six-year change in high-sensitivity cardiac troponin T and risk of subsequent coronary heart disease, heart failure, and death. JAMA Cardiol.
Supplementary Online Content McEvoy JW, Chen Y, Ndumele CE, et al. Six-year change in high-sensitivity cardiac troponin T and risk of subsequent coronary heart disease, heart failure, and death. JAMA Cardiol.
Blood Pressure Targets in Diabetes
 Stockholm, 29 th August 2010 ESC Meeting Blood Pressure Targets in Diabetes Peter M Nilsson, MD, PhD Department of Clinical Sciences University Hospital, Malmö Sweden Studies on BP in DM2 ADVANCE RCT (Lancet
Stockholm, 29 th August 2010 ESC Meeting Blood Pressure Targets in Diabetes Peter M Nilsson, MD, PhD Department of Clinical Sciences University Hospital, Malmö Sweden Studies on BP in DM2 ADVANCE RCT (Lancet
CVD Prevention, Who to Consider
 Continuing Professional Development 3rd annual McGill CME Cruise September 20 27, 2015 CVD Prevention, Who to Consider Dr. Guy Tremblay Excellence in Health Care and Lifelong Learning Global CV risk assessment..
Continuing Professional Development 3rd annual McGill CME Cruise September 20 27, 2015 CVD Prevention, Who to Consider Dr. Guy Tremblay Excellence in Health Care and Lifelong Learning Global CV risk assessment..
The Age-Specific Quantitative Effects of Metabolic Risk Factors on Cardiovascular Diseases and Diabetes: A Pooled Analysis
 The Age-Specific Quantitative Effects of Metabolic Risk Factors on Cardiovascular Diseases and Diabetes: A Pooled Analysis The Harvard community has made this article openly available. Please share how
The Age-Specific Quantitative Effects of Metabolic Risk Factors on Cardiovascular Diseases and Diabetes: A Pooled Analysis The Harvard community has made this article openly available. Please share how
LDL cholesterol and cardiovascular outcomes?
 LDL cholesterol and cardiovascular outcomes? Prof Kausik Ray, BSc (hons), MBChB, FRCP, MD, MPhil (Cantab), FACC, FESC Professor of Cardiovascular Disease Prevention St Georges University of London Honorary
LDL cholesterol and cardiovascular outcomes? Prof Kausik Ray, BSc (hons), MBChB, FRCP, MD, MPhil (Cantab), FACC, FESC Professor of Cardiovascular Disease Prevention St Georges University of London Honorary
Ischemic Heart and Cerebrovascular Disease. Harold E. Lebovitz, MD, FACE Kathmandu November 2010
 Ischemic Heart and Cerebrovascular Disease Harold E. Lebovitz, MD, FACE Kathmandu November 2010 Relationships Between Diabetes and Ischemic Heart Disease Risk of Cardiovascular Disease in Different Categories
Ischemic Heart and Cerebrovascular Disease Harold E. Lebovitz, MD, FACE Kathmandu November 2010 Relationships Between Diabetes and Ischemic Heart Disease Risk of Cardiovascular Disease in Different Categories
Supplement materials:
 Supplement materials: Table S1: ICD-9 codes used to define prevalent comorbid conditions and incident conditions Comorbid condition ICD-9 code Hypertension 401-405 Diabetes mellitus 250.x Myocardial infarction
Supplement materials: Table S1: ICD-9 codes used to define prevalent comorbid conditions and incident conditions Comorbid condition ICD-9 code Hypertension 401-405 Diabetes mellitus 250.x Myocardial infarction
The Whitehall II study originally comprised 10,308 (3413 women) individuals who, at
 Supplementary notes on Methods The study originally comprised 10,308 (3413 women) individuals who, at recruitment in 1985/8, were London-based government employees (civil servants) aged 35 to 55 years.
Supplementary notes on Methods The study originally comprised 10,308 (3413 women) individuals who, at recruitment in 1985/8, were London-based government employees (civil servants) aged 35 to 55 years.
EuroPrevent 2010 Fatal versus total events in risk assessment models
 EuroPrevent 2010 Fatal versus total events in risk assessment models Pekka Jousilahti, MD, PhD,Research Professor National Institute for Health and Welfare, Finland Risk assessment models Estimates the
EuroPrevent 2010 Fatal versus total events in risk assessment models Pekka Jousilahti, MD, PhD,Research Professor National Institute for Health and Welfare, Finland Risk assessment models Estimates the
Atherosclerotic Cardiovascular Diseases: ischaemic heart disease and stroke
 «L Europe de la santé au service des patients» 13-14 October 2008 - Institut Pasteur Paris Atherosclerotic Cardiovascular Diseases: ischaemic heart disease and stroke Simona Giampaoli National Centre of
«L Europe de la santé au service des patients» 13-14 October 2008 - Institut Pasteur Paris Atherosclerotic Cardiovascular Diseases: ischaemic heart disease and stroke Simona Giampaoli National Centre of
Yuqing Zhang, M.D., FESC Department of Cardiology, Fu Wai Hospital. CAMS & PUMC, Beijing, China
 What Can We Learn from the Observational Studies and Clinical Trials of Prehypertension? Yuqing Zhang, M.D., FESC Department of Cardiology, Fu Wai Hospital. CAMS & PUMC, Beijing, China At ARIC visit 4
What Can We Learn from the Observational Studies and Clinical Trials of Prehypertension? Yuqing Zhang, M.D., FESC Department of Cardiology, Fu Wai Hospital. CAMS & PUMC, Beijing, China At ARIC visit 4
CENTRE FOR STATISTICAL METHODOLOGY Celebrating the first International Statistics Prize Winner, Prof Sir David Cox
 CENTRE FOR STATISTICAL METHODOLOGY Celebrating the first International Statistics Prize Winner, Prof Sir David Cox Reduce, score*, regress, repeat: using factor analysis to tackle multicollinear HDL metabolomics
CENTRE FOR STATISTICAL METHODOLOGY Celebrating the first International Statistics Prize Winner, Prof Sir David Cox Reduce, score*, regress, repeat: using factor analysis to tackle multicollinear HDL metabolomics
Supplementary Online Content
 Supplementary Online Content Clair C, Rigotti NA, Porneala B, et al. Association of smoking cessation and weight change with cardiovascular disease among people with and without diabetes. JAMA. doi:10.1001/jama.2013.1644.
Supplementary Online Content Clair C, Rigotti NA, Porneala B, et al. Association of smoking cessation and weight change with cardiovascular disease among people with and without diabetes. JAMA. doi:10.1001/jama.2013.1644.
Supplementary Online Content
 Supplementary Online Content Pedersen SB, Langsted A, Nordestgaard BG. Nonfasting mild-to-moderate hypertriglyceridemia and risk of acute pancreatitis. JAMA Intern Med. Published online November 7, 2016.
Supplementary Online Content Pedersen SB, Langsted A, Nordestgaard BG. Nonfasting mild-to-moderate hypertriglyceridemia and risk of acute pancreatitis. JAMA Intern Med. Published online November 7, 2016.
Triglyceride-mediated pathways and coronary disease: collaborative analysis of 101 studies
 Triglyceride-mediated pathways and coronary disease: collaborative analysis of 101 studies Triglyceride Coronary Disease Genetics Consortium and Emerging Risk Factors Collaboration* Lancet 2010; 375: 1634
Triglyceride-mediated pathways and coronary disease: collaborative analysis of 101 studies Triglyceride Coronary Disease Genetics Consortium and Emerging Risk Factors Collaboration* Lancet 2010; 375: 1634
Table S1. Read and ICD 10 diagnosis codes for polymyalgia rheumatica and giant cell arteritis
 SUPPLEMENTARY MATERIAL TEXT Text S1. Multiple imputation TABLES Table S1. Read and ICD 10 diagnosis codes for polymyalgia rheumatica and giant cell arteritis Table S2. List of drugs included as immunosuppressant
SUPPLEMENTARY MATERIAL TEXT Text S1. Multiple imputation TABLES Table S1. Read and ICD 10 diagnosis codes for polymyalgia rheumatica and giant cell arteritis Table S2. List of drugs included as immunosuppressant
Supplementary Online Content
 Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
ORIGINAL INVESTIGATION. Relation of Triglyceride Levels, Fasting and Nonfasting, to Fatal and Nonfatal Coronary Heart Disease
 ORIGINAL INVESTIGATION Relation of Triglyceride Levels, Fasting and Nonfasting, to Fatal and Nonfatal Coronary Heart Disease Lynn E. Eberly, PhD; Jeremiah Stamler, MD; James D. Neaton, PhD; for the Multiple
ORIGINAL INVESTIGATION Relation of Triglyceride Levels, Fasting and Nonfasting, to Fatal and Nonfatal Coronary Heart Disease Lynn E. Eberly, PhD; Jeremiah Stamler, MD; James D. Neaton, PhD; for the Multiple
Modelling Reduction of Coronary Heart Disease Risk among people with Diabetes
 Modelling Reduction of Coronary Heart Disease Risk among people with Diabetes Katherine Baldock Catherine Chittleborough Patrick Phillips Anne Taylor August 2007 Acknowledgements This project was made
Modelling Reduction of Coronary Heart Disease Risk among people with Diabetes Katherine Baldock Catherine Chittleborough Patrick Phillips Anne Taylor August 2007 Acknowledgements This project was made
Methods for meta-analysis of individual participant data from Mendelian randomization studies with binary outcomes
 Methods for meta-analysis of individual participant data from Mendelian randomization studies with binary outcomes Stephen Burgess Simon G. Thompson CRP CHD Genetics Collaboration May 24, 2012 Abstract
Methods for meta-analysis of individual participant data from Mendelian randomization studies with binary outcomes Stephen Burgess Simon G. Thompson CRP CHD Genetics Collaboration May 24, 2012 Abstract
The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009
 The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009 Learning Objectives 1. Understand the role of statin therapy in the primary and secondary prevention of stroke 2. Explain
The JUPITER trial: What does it tell us? Alice Y.Y. Cheng, MD, FRCPC January 24, 2009 Learning Objectives 1. Understand the role of statin therapy in the primary and secondary prevention of stroke 2. Explain
Biases in clinical research. Seungho Ryu, MD, PhD Kanguk Samsung Hospital, Sungkyunkwan University
 Biases in clinical research Seungho Ryu, MD, PhD Kanguk Samsung Hospital, Sungkyunkwan University Learning objectives Describe the threats to causal inferences in clinical studies Understand the role of
Biases in clinical research Seungho Ryu, MD, PhD Kanguk Samsung Hospital, Sungkyunkwan University Learning objectives Describe the threats to causal inferences in clinical studies Understand the role of
BEST PRACTICE MANAGEMENT: CARDIOVASCULAR RISKS
 BEST PRACTICE MANAGEMENT: CARDIOVASCULAR RISKS Neil R Poulter ICCH, Imperial College London BHIVA: October 10th, 2008 Background CVD is the biggest single killer in the world CVD rates are increasing High
BEST PRACTICE MANAGEMENT: CARDIOVASCULAR RISKS Neil R Poulter ICCH, Imperial College London BHIVA: October 10th, 2008 Background CVD is the biggest single killer in the world CVD rates are increasing High
Glycemic index, glycemic load, and the risk of acute myocardial infarction in middle-aged Finnish men:
 Glycemic index, glycemic load, and the risk of acute myocardial infarction in middle-aged Finnish men: The Kuopio Ischaemic Heart Disease Risk Factor Study Jaakko Mursu, Jyrki K. Virtanen, Tiina H. Rissanen,
Glycemic index, glycemic load, and the risk of acute myocardial infarction in middle-aged Finnish men: The Kuopio Ischaemic Heart Disease Risk Factor Study Jaakko Mursu, Jyrki K. Virtanen, Tiina H. Rissanen,
Diabetes Mellitus: A Cardiovascular Disease
 Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
ESC Geoffrey Rose Lecture on Population Sciences Cholesterol and risk: past, present and future
 ESC Geoffrey Rose Lecture on Population Sciences Cholesterol and risk: past, present and future Rory Collins BHF Professor of Medicine & Epidemiology Clinical Trial Service Unit & Epidemiological Studies
ESC Geoffrey Rose Lecture on Population Sciences Cholesterol and risk: past, present and future Rory Collins BHF Professor of Medicine & Epidemiology Clinical Trial Service Unit & Epidemiological Studies
Modelling diabetes Professor Alastair Gray Health Economics Research Centre University of Oxford
 Oxford Technology Showcase 2016 Big Healthcare Challenges in chronic disease Modelling diabetes Professor Alastair Gray Health Economics Research Centre University of Oxford Chronic diseases.. are long-term
Oxford Technology Showcase 2016 Big Healthcare Challenges in chronic disease Modelling diabetes Professor Alastair Gray Health Economics Research Centre University of Oxford Chronic diseases.. are long-term
Impact of Multiple Risk Factors and Preventive Interventions on Cardiovascular Diseases and Disparities
 Impact of Multiple Risk Factors and Preventive Interventions on Cardiovascular Diseases and Disparities The Harvard community has made this article openly available. Please share how this access benefits
Impact of Multiple Risk Factors and Preventive Interventions on Cardiovascular Diseases and Disparities The Harvard community has made this article openly available. Please share how this access benefits
Presented by Terje R. Pedersen Oslo Disclosure: Research grants and/or speaker- / consulting fees from Merck, MSP, Astra-Zeneca, Pfizer
 Presented by Terje R. Pedersen Oslo Disclosure: Research grants and/or speaker- / consulting fees from Merck, MSP, Astra-Zeneca, Pfizer Patients Randomized by Country 187 UK n=187 Norway n=425 Finland
Presented by Terje R. Pedersen Oslo Disclosure: Research grants and/or speaker- / consulting fees from Merck, MSP, Astra-Zeneca, Pfizer Patients Randomized by Country 187 UK n=187 Norway n=425 Finland
Targeting Glucose Metabolism to Stop Strokes IRIS: Insulin Resistance In Stroke study
 Targeting Glucose Metabolism to Stop Strokes IRIS: Insulin Resistance In Stroke study Professor Gary Ford Chief Executive Officer, Oxford Academic Health Science Network Consultant Stroke Physician, Oxford
Targeting Glucose Metabolism to Stop Strokes IRIS: Insulin Resistance In Stroke study Professor Gary Ford Chief Executive Officer, Oxford Academic Health Science Network Consultant Stroke Physician, Oxford
Table S1. Characteristics associated with frequency of nut consumption (full entire sample; Nn=4,416).
 Table S1. Characteristics associated with frequency of nut (full entire sample; Nn=4,416). Daily nut Nn= 212 Weekly nut Nn= 487 Monthly nut Nn= 1,276 Infrequent or never nut Nn= 2,441 Sex; n (%) men 52
Table S1. Characteristics associated with frequency of nut (full entire sample; Nn=4,416). Daily nut Nn= 212 Weekly nut Nn= 487 Monthly nut Nn= 1,276 Infrequent or never nut Nn= 2,441 Sex; n (%) men 52
High-sensitivity Troponin T Predicts Recurrent Cardiovascular Events in Patients with Stable Coronary Heart Disease: KAROLA Study 8 Year FU
 ESC Congress 2011 Paris, France, August 27-31 KAROLA Session: Prevention: Are biomarkers worth their money? Abstract # 84698 High-sensitivity Troponin T Predicts Recurrent Cardiovascular Events in Patients
ESC Congress 2011 Paris, France, August 27-31 KAROLA Session: Prevention: Are biomarkers worth their money? Abstract # 84698 High-sensitivity Troponin T Predicts Recurrent Cardiovascular Events in Patients
Socioeconomic status and the 25x25 risk factors as determinants of premature mortality: a multicohort study of 1.7 million men and women
 Socioeconomic status and the 25x25 risk factors as determinants of premature mortality: a multicohort study of 1.7 million men and women (Lancet. 2017 Mar 25;389(10075):1229-1237) 1 Silvia STRINGHINI Senior
Socioeconomic status and the 25x25 risk factors as determinants of premature mortality: a multicohort study of 1.7 million men and women (Lancet. 2017 Mar 25;389(10075):1229-1237) 1 Silvia STRINGHINI Senior
Supplementary Online Content
 Supplementary Online Content Schnabel RB, Aspelund T, Li G, et al. Validation of an atrial fibrillation risk algorithm in whites and African Americans. Arch Intern Med. 2010;170(21):1909-1917. eappendix.
Supplementary Online Content Schnabel RB, Aspelund T, Li G, et al. Validation of an atrial fibrillation risk algorithm in whites and African Americans. Arch Intern Med. 2010;170(21):1909-1917. eappendix.
Web Extra material. Comparison of non-laboratory-based risk scores for predicting the occurrence of type 2
 Web Extra material Comparison of non-laboratory-based risk scores for predicting the occurrence of type 2 diabetes in the general population: the EPIC-InterAct Study Outline Supplementary Figures Legend...
Web Extra material Comparison of non-laboratory-based risk scores for predicting the occurrence of type 2 diabetes in the general population: the EPIC-InterAct Study Outline Supplementary Figures Legend...
D:A:D Study Teaching Material
 D:A:D Study Teaching Material Data Collection of Adverse events of anti-hiv Drugs (D:A:D) study December 2012 - CHIP Background The D:A:D Study, is a prospective cohort study (collaboration) initiated
D:A:D Study Teaching Material Data Collection of Adverse events of anti-hiv Drugs (D:A:D) study December 2012 - CHIP Background The D:A:D Study, is a prospective cohort study (collaboration) initiated
Design and Analysis of a Cancer Prevention Trial: Plans and Results. Matthew Somerville 09 November 2009
 Design and Analysis of a Cancer Prevention Trial: Plans and Results Matthew Somerville 09 November 2009 Overview Objective: Review the planned analyses for a large prostate cancer prevention study and
Design and Analysis of a Cancer Prevention Trial: Plans and Results Matthew Somerville 09 November 2009 Overview Objective: Review the planned analyses for a large prostate cancer prevention study and
REVEAL: Randomized placebo-controlled trial of anacetrapib in 30,449 patients with atherosclerotic vascular disease
 REVEAL: Randomized placebo-controlled trial of anacetrapib in 30,449 patients with atherosclerotic vascular disease Martin Landray and Louise Bowman on behalf of the HPS 3 / TIMI 55 - REVEAL Collaborative
REVEAL: Randomized placebo-controlled trial of anacetrapib in 30,449 patients with atherosclerotic vascular disease Martin Landray and Louise Bowman on behalf of the HPS 3 / TIMI 55 - REVEAL Collaborative
Type of intervention Primary prevention; secondary prevention. Economic study type Cost-effectiveness analysis and cost utility analysis.
 A predictive model of the health benefits and cost effectiveness of celiprolol and atenolol in primary prevention of cardiovascular disease in hypertensive patients Milne R J, Hoorn S V, Jackson R T Record
A predictive model of the health benefits and cost effectiveness of celiprolol and atenolol in primary prevention of cardiovascular disease in hypertensive patients Milne R J, Hoorn S V, Jackson R T Record
Supplementary Online Content
 Supplementary Online Content Levin GP, Robinson-Cohen C, de Boer IH, Houston DK, Lohman K, Liu Y, et al. Genetic variants and associations of 25-hydroxyvitamin D concentrations with major clinical outcomes.
Supplementary Online Content Levin GP, Robinson-Cohen C, de Boer IH, Houston DK, Lohman K, Liu Y, et al. Genetic variants and associations of 25-hydroxyvitamin D concentrations with major clinical outcomes.
Assessing Cardiovascular Risk to Optimally Stratify Low- and Moderate- Risk Patients. Copyright. Not for Sale or Commercial Distribution
 CLINICAL Viewpoint Assessing Cardiovascular Risk to Optimally Stratify Low- and Moderate- Risk Patients Copyright Not for Sale or Commercial Distribution By Ruth McPherson, MD, PhD, FRCPC Unauthorised
CLINICAL Viewpoint Assessing Cardiovascular Risk to Optimally Stratify Low- and Moderate- Risk Patients Copyright Not for Sale or Commercial Distribution By Ruth McPherson, MD, PhD, FRCPC Unauthorised
DECLARATION OF CONFLICT OF INTEREST. None
 DECLARATION OF CONFLICT OF INTEREST None Dietary changes and its influence on cardiovascular diseases in Asian and European countries Problems of Eastern European countries for cardiovascular disease prevention
DECLARATION OF CONFLICT OF INTEREST None Dietary changes and its influence on cardiovascular diseases in Asian and European countries Problems of Eastern European countries for cardiovascular disease prevention
Implementing Type 2 Diabetes Prevention Programmes
 Implementing Type 2 Diabetes Prevention Programmes Jaakko Tuomilehto Department of Public Health University of Helsinki Helsinki, Finland FIN-D2D Survey 2004 Prevalence of previously diagnosed and screen-detected
Implementing Type 2 Diabetes Prevention Programmes Jaakko Tuomilehto Department of Public Health University of Helsinki Helsinki, Finland FIN-D2D Survey 2004 Prevalence of previously diagnosed and screen-detected
well-targeted primary prevention of cardiovascular disease: an underused high-value intervention?
 well-targeted primary prevention of cardiovascular disease: an underused high-value intervention? Rod Jackson University of Auckland, New Zealand October 2015 Lancet 1999; 353: 1547-57 Findings: Contribution
well-targeted primary prevention of cardiovascular disease: an underused high-value intervention? Rod Jackson University of Auckland, New Zealand October 2015 Lancet 1999; 353: 1547-57 Findings: Contribution
Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors.
 Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Appendix to: Banks E, Crouch SR, Korda RJ, et al. Absolute risk of cardiovascular
Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Appendix to: Banks E, Crouch SR, Korda RJ, et al. Absolute risk of cardiovascular
Inflammation and and Heart Heart Disease in Women Inflammation and Heart Disease
 Inflammation and Heart Disease in Women Inflammation and Heart Disease What is the link between een inflammation and atherosclerotic disease? What is the role of biomarkers in predicting cardiovascular
Inflammation and Heart Disease in Women Inflammation and Heart Disease What is the link between een inflammation and atherosclerotic disease? What is the role of biomarkers in predicting cardiovascular
Schöttker et al. BMC Medicine (2016) 14:26 DOI /s
 Schöttker et al. BMC Medicine (2016) 14:26 DOI 10.1186/s12916-016-0570-1 RESEARCH ARTICLE HbA 1c levels in non-diabetic older adults No J-shaped associations with primary cardiovascular events, cardiovascular
Schöttker et al. BMC Medicine (2016) 14:26 DOI 10.1186/s12916-016-0570-1 RESEARCH ARTICLE HbA 1c levels in non-diabetic older adults No J-shaped associations with primary cardiovascular events, cardiovascular
Low-Carbohydrate Diets and All-Cause and Cause-Specific Mortality: A Population-based Cohort Study and Pooling Prospective Studies
 Low-Carbohydrate Diets and All-Cause and Cause-Specific Mortality: A Population-based Cohort Study and Pooling Prospective Studies Mohsen Mazidi 1, Niki Katsiki 2, Dimitri P. Mikhailidis 3, Maciej Banach
Low-Carbohydrate Diets and All-Cause and Cause-Specific Mortality: A Population-based Cohort Study and Pooling Prospective Studies Mohsen Mazidi 1, Niki Katsiki 2, Dimitri P. Mikhailidis 3, Maciej Banach
Supplementary Online Content
 Supplementary Online Content Lotta LA, Stewart ID, Sharp SJ, et al. Association of genetically enhanced lipoprotein lipase mediated lipolysis and low-density lipoprotein cholesterol lowering alleles with
Supplementary Online Content Lotta LA, Stewart ID, Sharp SJ, et al. Association of genetically enhanced lipoprotein lipase mediated lipolysis and low-density lipoprotein cholesterol lowering alleles with
Coronary heart disease risk prediction in the Atherosclerosis Risk in Communities (ARIC) study
 Coronary heart disease risk prediction in the Atherosclerosis Risk in Communities (ARIC) study A. Attached below are the beta coefficients from the Cox regression models for the full models presented in
Coronary heart disease risk prediction in the Atherosclerosis Risk in Communities (ARIC) study A. Attached below are the beta coefficients from the Cox regression models for the full models presented in
Guidelines on cardiovascular risk assessment and management
 European Heart Journal Supplements (2005) 7 (Supplement L), L5 L10 doi:10.1093/eurheartj/sui079 Guidelines on cardiovascular risk assessment and management David A. Wood 1,2 * 1 Cardiovascular Medicine
European Heart Journal Supplements (2005) 7 (Supplement L), L5 L10 doi:10.1093/eurheartj/sui079 Guidelines on cardiovascular risk assessment and management David A. Wood 1,2 * 1 Cardiovascular Medicine
The CARI Guidelines Caring for Australians with Renal Impairment. Cardiovascular Risk Factors
 Cardiovascular Risk Factors ROB WALKER (Dunedin, New Zealand) Lipid-lowering therapy in patients with chronic kidney disease Date written: January 2005 Final submission: August 2005 Author: Rob Walker
Cardiovascular Risk Factors ROB WALKER (Dunedin, New Zealand) Lipid-lowering therapy in patients with chronic kidney disease Date written: January 2005 Final submission: August 2005 Author: Rob Walker
Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden
 Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden Cardiovascular Disease Prevention (CVD) Three Strategies for CVD
Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden Cardiovascular Disease Prevention (CVD) Three Strategies for CVD
The TNT Trial Is It Time to Shift Our Goals in Clinical
 The TNT Trial Is It Time to Shift Our Goals in Clinical Angioplasty Summit Luncheon Symposium Korea Assoc Prof David Colquhoun 29 April 2005 University of Queensland, Wesley Hospital, Brisbane, Australia
The TNT Trial Is It Time to Shift Our Goals in Clinical Angioplasty Summit Luncheon Symposium Korea Assoc Prof David Colquhoun 29 April 2005 University of Queensland, Wesley Hospital, Brisbane, Australia
Master Class in Preventive Cardiology. The New MI Phenotype OR. Klas Malmberg MD, PhD, FESC Karolinska Institutet, Stockholm Sweden
 Master Class in Preventive Cardiology The New MI Phenotype OR Klas Malmberg MD, PhD, FESC Karolinska Institutet, Stockholm Sweden The New MI Phenotype OR Coronary disease and glucose abnormalities Klas
Master Class in Preventive Cardiology The New MI Phenotype OR Klas Malmberg MD, PhD, FESC Karolinska Institutet, Stockholm Sweden The New MI Phenotype OR Coronary disease and glucose abnormalities Klas
T. Suithichaiyakul Cardiomed Chula
 T. Suithichaiyakul Cardiomed Chula The cardiovascular (CV) continuum: role of risk factors Endothelial Dysfunction Atherosclerosis and left ventricular hypertrophy Myocardial infarction & stroke Endothelial
T. Suithichaiyakul Cardiomed Chula The cardiovascular (CV) continuum: role of risk factors Endothelial Dysfunction Atherosclerosis and left ventricular hypertrophy Myocardial infarction & stroke Endothelial
Low-density lipoprotein as the key factor in atherogenesis too high, too long, or both
 Low-density lipoprotein as the key factor in atherogenesis too high, too long, or both Lluís Masana Vascular Medicine and Metabolism Unit. Sant Joan University Hospital. IISPV. CIBERDEM Rovira i Virgili
Low-density lipoprotein as the key factor in atherogenesis too high, too long, or both Lluís Masana Vascular Medicine and Metabolism Unit. Sant Joan University Hospital. IISPV. CIBERDEM Rovira i Virgili
ESM1 for Glucose, blood pressure and cholesterol levels and their relationships to clinical outcomes in type 2 diabetes: a retrospective cohort study
 ESM1 for Glucose, blood pressure and cholesterol levels and their relationships to clinical outcomes in type 2 diabetes: a retrospective cohort study Statistical modelling details We used Cox proportional-hazards
ESM1 for Glucose, blood pressure and cholesterol levels and their relationships to clinical outcomes in type 2 diabetes: a retrospective cohort study Statistical modelling details We used Cox proportional-hazards
Implications of The LookAHEAD Trial: Is Weight Loss Beneficial for Patients with Diabetes?
 Implications of The LookAHEAD Trial: Is Weight Loss Beneficial for Patients with Diabetes? Boston, MA November 7, 213 Edward S. Horton, MD Professor of Medicine Harvard Medical School Senior Investigator
Implications of The LookAHEAD Trial: Is Weight Loss Beneficial for Patients with Diabetes? Boston, MA November 7, 213 Edward S. Horton, MD Professor of Medicine Harvard Medical School Senior Investigator
Key causes of preventable deaths in New Zealand In a population of 10,000 New Zealanders, every year there will be about:
 Preventive care - Chronic Disease Management in primary care: a population perspective Rod Jackson University of Auckland New Zealand (22/11/8) Key causes of preventable deaths in New Zealand In a population
Preventive care - Chronic Disease Management in primary care: a population perspective Rod Jackson University of Auckland New Zealand (22/11/8) Key causes of preventable deaths in New Zealand In a population
HIGH LDL CHOLESTEROL IS NOT AN INDEPENDENT RISK FACTOR FOR HEART ATTACKS AND STROKES
 HIGH LDL CHOLESTEROL IS NOT AN INDEPENDENT RISK FACTOR FOR HEART ATTACKS AND STROKES A study published in the British Medical Journal shows that not only is high LDL cholesterol not a risk factor for all-caused
HIGH LDL CHOLESTEROL IS NOT AN INDEPENDENT RISK FACTOR FOR HEART ATTACKS AND STROKES A study published in the British Medical Journal shows that not only is high LDL cholesterol not a risk factor for all-caused
GSK Medicine: Study Number: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Update on Dyslipidemia and Recent Data on Treating the Statin Intolerant Patient
 Update on Dyslipidemia and Recent Data on Treating the Statin Intolerant Patient Steven E. Nissen MD Chairman, Department of Cardiovascular Medicine Cleveland Clinic Disclosure Consulting: Many pharmaceutical
Update on Dyslipidemia and Recent Data on Treating the Statin Intolerant Patient Steven E. Nissen MD Chairman, Department of Cardiovascular Medicine Cleveland Clinic Disclosure Consulting: Many pharmaceutical
Supplementary Online Content
 Supplementary Online Content Xu X, Qin X, Li Y, et al. Efficacy of folic acid therapy on the progression of chronic kidney disease: the Renal Substudy of the China Stroke Primary Prevention Trial. JAMA
Supplementary Online Content Xu X, Qin X, Li Y, et al. Efficacy of folic acid therapy on the progression of chronic kidney disease: the Renal Substudy of the China Stroke Primary Prevention Trial. JAMA
Supplemental Table 1. Study design and participant characteristics.
 Supplemental Table 1. Study design and participant characteristics. Study ID Study Design; Total No. of Participants Mean age at Parity Participant Selection Criteria Country; Year (PE/no PE) Index Pregnancy
Supplemental Table 1. Study design and participant characteristics. Study ID Study Design; Total No. of Participants Mean age at Parity Participant Selection Criteria Country; Year (PE/no PE) Index Pregnancy
SCIENTIFIC STUDY REPORT
 PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic
 Supplementary Information The title of the manuscript Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic stroke Xin-Wei He 1, Wei-Ling Li 1, Cai Li
Supplementary Information The title of the manuscript Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic stroke Xin-Wei He 1, Wei-Ling Li 1, Cai Li
The Diabetes Link to Heart Disease
 The Diabetes Link to Heart Disease Anthony Abe DeSantis, MD September 18, 2015 University of WA Division of Metabolism, Endocrinology and Nutrition Oswald Toosweet Case #1 68 yo M with T2DM Diagnosed DM
The Diabetes Link to Heart Disease Anthony Abe DeSantis, MD September 18, 2015 University of WA Division of Metabolism, Endocrinology and Nutrition Oswald Toosweet Case #1 68 yo M with T2DM Diagnosed DM
Secondary prevention and systems approaches: Lessons from EUROASPIRE and EUROACTION
 Secondary prevention and systems approaches: Lessons from EUROASPIRE and EUROACTION Dr Kornelia Kotseva National Heart & Lung Insitute Imperial College London, UK on behalf of all investigators participating
Secondary prevention and systems approaches: Lessons from EUROASPIRE and EUROACTION Dr Kornelia Kotseva National Heart & Lung Insitute Imperial College London, UK on behalf of all investigators participating
2013 ACC AHA LIPID GUIDELINE JAY S. FONTE, MD
 2013 ACC AHA LIPID GUIDELINE JAY S. FONTE, MD How do you interpret my blood test results? What are our targets for these tests? Before the ACC/AHA Lipid Guidelines A1c:
2013 ACC AHA LIPID GUIDELINE JAY S. FONTE, MD How do you interpret my blood test results? What are our targets for these tests? Before the ACC/AHA Lipid Guidelines A1c:
Long-term prognostic value of N-Terminal Pro-Brain Natriuretic Peptide (NT-proBNP) changes within one year in patients with coronary heart disease
 Long-term prognostic value of N-Terminal Pro-Brain Natriuretic Peptide (NT-proBNP) changes within one year in patients with coronary heart disease D. Dallmeier 1, D. Rothenbacher 2, W. Koenig 1, H. Brenner
Long-term prognostic value of N-Terminal Pro-Brain Natriuretic Peptide (NT-proBNP) changes within one year in patients with coronary heart disease D. Dallmeier 1, D. Rothenbacher 2, W. Koenig 1, H. Brenner
Beyond Framingham: Risk Assessment & Treatment for Primary Prevention
 Beyond Framingham: Risk Assessment & Treatment for Primary Prevention Ronald M. Goldenberg, MD, FRCPC, FACE Consultant Endocrinologist, North York General Hospital Medical Co-Director, LMC Endocrinology
Beyond Framingham: Risk Assessment & Treatment for Primary Prevention Ronald M. Goldenberg, MD, FRCPC, FACE Consultant Endocrinologist, North York General Hospital Medical Co-Director, LMC Endocrinology
Hypertension and Stroke: new data
 Hypertension and Stroke: new data Antonio Coca, MD, PhD, FRCP Hypertension Unit. Institute of Internal Medicine and Dermatology. Hospital Clínic (IDIBAPS). University of Barcelona, Spain WG Seminars. Hellenic
Hypertension and Stroke: new data Antonio Coca, MD, PhD, FRCP Hypertension Unit. Institute of Internal Medicine and Dermatology. Hospital Clínic (IDIBAPS). University of Barcelona, Spain WG Seminars. Hellenic
