Return to Play. Preface
|
|
|
- Linda Gibbs
- 5 years ago
- Views:
Transcription
1 Clin Sports Med 23 (2004) xv xxiii Preface Return to Play Edward G. McFarland, MD Guest Editor The topic for this issue of the Clinics in Sports Medicine was conceived after a seminar presented at the Advanced Team Physician Course (ATPC) in The ATPC is a course designed for sports medicine physicians that covers topics in more detail and covers more controversial topics than many sports meetings. It is cosponsored by the American College of Sports Medicine, the American Medical Society for Sports Medicine, and the American Orthopaedic Society for Sports Medicine. Many of the contributors to this issue were participants in that symposium, and they were chosen to contribute here because of their expertise and experience with these issues. All of them are team physicians in some capacity or deal with athletes who are referred to their practices. The topic of return to play has always been pertinent for anyone who treats athletes or active individuals. Returning a patient to an active life is not only a core concept of sports medicine but has implications for health care professionals from almost every discipline. Margo Putukian, MD, suggested that the issue of return to play has an impact on patients of any age from 5 to 85 and can apply to almost any medical condition [1]. When do you let the 5-year-old with a forearm bone fracture return to gymnastics, a college athlete with manicdepressive illness return to stressful competition, and the octogenarian with a hernia repair return to long-distance running? As practitioners, particularly as sports medicine physicians, we are faced with making these decisions and making recommendations to patients on a daily basis. There are four facets of the discussion regarding decisions to return a participant to play. The first is the medical component, and it is the one that is perhaps the least well defined of all. Although we all prefer certainty in this life, complete /04/$ see front matter D 2004 Elsevier Inc. All rights reserved. doi: /j.csm
2 xvi E.G. McFarland / Clin Sports Med 23 (2004) xv xxiii knowledge about most conditions we see in patients is rarely available. The practice of medicine is an inexact science, and this is a truism that is not always appreciated by the athlete or the other people in their lives. To make more specific recommendations, we should know the pathophysiology and natural history of the disease process, the result of both medical and surgical interventions, and when those interventions will allow the individual to return to play without further injury to themselves or to other participants. There are few conditions for which there are not gaps in our knowledge of these factors. As we begin to understand the complexity of many conditions, the decision-making often seems to become more difficult because there are many more factors to consider. This usually is a good thing, because we serve our patients better by attempting to understand all of the medical variables when evaluating return to play issues. For example, there is probably not a more controversial topic than when to return an athlete to play after a cerebral concussion, but the process of trying to develop cognitive tests for sideline use have taught us a lot about the variable presentations and recovery of athletes who sustain this injury. However, this has also generated further questions such as, What measures are the most predictive of a safe ability to return to play and are predictive of no further injury? As most medical practitioners are aware, there is so much biologic variability that it is difficult to say that guidelines to return to play will protect every individual, whether one is talking about concussions, myocardial infarctions, or stress fractures. Medical knowledge evolves, as does our understanding of most disease processes; our recommendations about return to play will change as well. When making decisions to return to play, one must try to obtain the best medical knowledge possible, make judgments about the individual patient, and hope for the best. The second variable to consider in decisions for return to play involve social and economic forces. Although sports medicine physicians are well aware of these influences, I am amazed how often these factors influence decision-making for returning patients to physical education classes or to their health club. The social influences when deciding return to play include the patient s family, their parents, their friends, the coaching staff and sometimes other medical practitioners. The pressure for an athlete to return for the big game that can be applied by these other parties can be overt or they may be more occult. They sometimes seem to make our lives as practitioners miserable, but they are an important part of understanding our patients, their goals, and their recovery from a condition or injury. Pressures should be dealt with when making decisions about diagnostic tests, treatment options, surgery, rehabilitation, or return to play. An ancillary social consideration is the economic impact of decisions to return to play, and this can occur at any level of participation. The impact of return to play upon income and endorsement benefits for professionals or Olympic-level athletes is easy to understand, but there are also economic implications of injury for collegiate athletes who are on scholarship and high school students who may be pursuing a scholarship. Unfortunately, economic benefits can be perceived by amateur athletes and their families who hope to attain fame and fortune through athletic participation. Although it is tempting to disregard unrealistic goals of
3 E.G. McFarland / Clin Sports Med 23 (2004) xv xxiii xvii economic gain when making decisions to return to play, these forces should be recognized and dealt with when counseling patients and their families. Another factor involved when making the decision to return to play is political; that is, who politically is in the position to make the decision regarding whether or not a patient returns to activity or to participation? As outlined in the consensus statement in the Appendix, there should be a system established by the physicians, trainers, and institutions to determine who makes the decision and when [2]. Disagreements between health care providers, second-opinion physicians, trainers, and therapists can create unnecessary stress. The process of making the decision regarding return to play should consider the best interest of the athlete as the primary goal, and the decision to play should not be left up to the coach or the administrator. This process should include having a chain of command, a method of communicating the decisions to the appropriate personel, a method of documentation, and a system for protecting the privacy of the player. The final facet of return to play decisions involves legal issues. Legislation sometimes dictates how health care professionals should deal with certain injuries, and these rules can be federal, statewide, local, or specific to the school. For example, there are several regulations regarding an athlete s participation in sport while taking certain medications, and the practitioner should not provide narcotics or other medications to players simply so they can play. In a larger legal sense, the physician has an obligation to put the best interest of the patient first; this relates to return to play issues, but also to eligibility decisions [3]. A physician should not allow a player to return to play when it is not believed to be medically safe, despite the desire of or pressure by the player, agent, family, or coach. Likewise, a player should not be allowed to sign a waiver when the player is not really ready to participate. It is important to recognize that the topics discussed by the authors of this issue of the Clinics of Sports Medicine are controversial. Our medical knowledge of these conditions continues to change, and this will influence how the conditions are evaluated and treated. As a result, the recommendations by the authors regarding return to play should be recognized as guidelines. The recommendations made by these authors should not be interpreted as legal standards for return to play for any of the topics presented herein. Decisions to return to play must continue to be individualized and must include recognition of the highly variable natural history of most medical conditions and the complex interaction of social, economic, political, and legal factors. Appendix. statement The team physician and return-to-play issues: a consensus Definition Return-to-play is the process of deciding when an injured or ill athlete may safely return to practice or competition.
4 xviii E.G. McFarland / Clin Sports Med 23 (2004) xv xxiii Goal The goal is to return an injured or ill athlete to practice or competition without putting the individual or others at undue risk for injury or illness. To accomplish this goal, the team physician should have knowledge and be involved with: Establishing a return-to-play process Evaluating injured or ill athletes Treating injured or ill athletes Rehabilitating injured or ill athletes Returning an injured or ill athlete to play Summary The objective of this consensus statment is to provide physicians who are responsible for the health care of teams with a decision process for determining when to return an injured or ill athlete to practice or competition. This statement is not intended as a standard of care, and should not be interpreted as such. This statement is only a guide, and as such is of a general nature consistent with the reasonable and objective practice of the health care professional. Individual decisions regarding the return of an injured or ill athlete to play will depend on the specific facts and circumstances presented to the physician. Adequate insurance should be in place to help protect the athlete, the sponsoring organization, and the physician. This statement was developed by the collaborative effort of six major professional associations concerned with clinical sports medicine issues; they have committed to forming an ongoing project-based alliance to bring together sports medicine organizations to best serve active people and athletes. The organizations are: the American Academy of Family Physicians, the American Academy of Orthopaedic Surgeons, the American College of Sports Medicine, the American Medical Society for Sports Medicine, the American Orthopaedic Society for Sports Medicine, and the American Osteopathic Academy of Sports Medicine. Expert panel Stanley A. Herring, MD, Chair, Seattle, Washington John A. Bergfeld, MD, Cleveland, Ohio Joel Boyd, MD, Edina, Minnesota Timothy Duffey, DO, Columbus, Ohio Karl B. Fields, MD, Greensboro, North Carolina William A. Grana, MD, Tucson, Arizona Peter Indelicato, MD, Gainesville, Florida W. Ben Kibler, MD, Lexington, Kentucky Robert Pallay, MD, Hillsborough, New Jersey
5 E.G. McFarland / Clin Sports Med 23 (2004) xv xxiii xix Margot Putukian, MD, University Park, Pennsylvania Robert E. Sallis, MD, Alta Loma, California Establishing a return-to-play process Establishing a process for returning an athlete to play is an essential first step in deciding when an injured or ill athlete may safely return to practice or competition. It is essential for the team physician to coordinate: Establishing a chain of command regarding decisions to return an injured or ill athlete to practice or competition Communicating the return-to-play process to players, families, certified athletic trainers, coaches, administrators, and other health care providers Establishing a system for documentation Establishing protocols to release information regarding an athlete s ability to return to practice or competition after an injury or illness It is essential that the return-to-play process address the: Safety of the athlete Potential risk to the safety of other participants Functional capabilities of the athlete Functional requirements of the athlete s sport Federal, state, local, school, and governing body regulations related to returning an injured or ill athlete to practice or competition Evaluating injured or ill athletes Evaluation of an injured or ill athlete establishes a diagnosis, directs treatment, and is the basis for deciding when an athlete may safely return to practice or competition. Repeated evaluations throughout the continuum of injury or illness management optimize medical care. It is essential that evaluation of an injured or ill athlete include: A condition-specific medical history A condition-specific physical examination Appropriate medical tests and consultations Psychosocial assessment Documentation Communication with the player, family, certified athletic trainer, coaches, and other health care providers In addition, it is desirable that: The team physician coordinate evaluation of the injured or ill athlete
6 xx E.G. McFarland / Clin Sports Med 23 (2004) xv xxiii Treating injured or ill athletes Treatment of an injured or ill athlete promotes the safe and timely return to practice or competition. It is essential that treatment of the injured or ill athlete: Begin in a timely manner (see Sideline Preparedness for the Team Physician: A Consensus Statement, 2000) Follow an individualized plan, which may include consultations and referrals Include a rehabilitation plan Include equipment modification, bracing, and orthoses as necessary Address psychosocial issues Provide a realistic prognosis as to a safe and timely return to practice or competition Include continued communication with the player, family, certified athletic trainer, coaches, and other health care providers Include documentation In addition, it is desirable that: The team physician coordinate the initial and ongoing treatment for the injured or ill athlete Rehabilitating injured or ill athletes Comprehensive treatment includes proper rehabilitation of an injured or ill athlete, thus optimizing the safe and timely return to practice or competition. The team physician should be involved in a network that integrates expertise regarding rehabilitation. This network should include certified athletic trainers, physical therapists, medical specialists, and other health care providers. It is essential that the rehabilitation network: Coordinate the development of a rehabilitation plan that is designed to: Restore function of the injured part Restore and promote musculoskeletal and cardiovascular function, as well as overall well-being of the injured or ill athlete Provide sport-specific assessment and training to serve as a basis for sportspecific conditioning (see The Team Physician and Conditioning of Athletes for Sports: A Consensus Statement, 2001) Provide for continued equipment modification, bracing, and orthoses Continue communication with the player, family, rehabilitation network, and coaches concerning the athlete s progress Include documentation
7 E.G. McFarland / Clin Sports Med 23 (2004) xv xxiii xxi In addition, it is desirable that: The team physician coordinate the rehabilitation program for the injured or ill athlete Returning an injured or ill athlete to play The decision for safe and timely return of an injured or ill athlete to practice or competition is the desired result of the process of evaluation, treatment, and rehabilitation. It is essential for return-to-play that the team physician confirm the following criteria: The status of anatomical and functional healing The status of recovery from acute illness and associated sequelae The status of chronic injury or illness That the athlete pose no undue risk to the safety of other participants Restoration of sport-specific skills Psychosocial readiness Ability to perform safely with equipment modification, bracing, and orthoses Compliance with applicable federal, state, local, school, and governing body regulations Before return-to-play, these criteria should be confirmed at a satisfactory level. Conclusion Use of the information in this document allows the team physician to make an informed decision as to whether an injured or ill athlete may safely return to practice or competition. The return-to-play process should be under the direction of the team physican whenever possible. While it is desirable that the team physician coordinate evaluating, treating, and rehabilitating the injured or ill athlete, it is essential that the the team physician ultimately be responsible for the return-toplay decision. Individual decisions regarding return of an injured or ill athlete to play will depend on the specific facts and circumstances presented to the team physician. Available resources Ongoing education pertinent to the team physician is essential. Information regarding team physician specific educational opportunities can be obtained from the six participating organizations:
8 xxii E.G. McFarland / Clin Sports Med 23 (2004) xv xxiii American Academy of Family Physicians (AAFP), Tomahawk Creek Pkwy, Leawood, KS American Academy of Orthopaedic Surgeons (AAOS), 6300 N. River Rd., Rosemont, IL AAOS. American College of Sports Medicine (ACSM), 401 W. Michigan St., Indianapolis, IN American Medical Society for Sports Medicine (AMSSM), Earnshaw, Overland Park, KS American Orthopaedic Society for Sports Medicine (AOSSM), 6300 N. River Rd., Suite 200, Rosemont, IL www. sportsmed.org. American Osteopathic Academy of Sports Medicine (AOASM), 7611 Elmwood Ave., Suite 201, Middleton, WI www. aoasm.org. From The team physician and return to play issues: a consensus statement. Med Sci Sports Exerc 2002;34:1212 4; with permisssion. References [1] Putukian M. Return to play: making the tough decisions. Phys Sportsmed 1998;26:25 7. [2] The team physician and return to play issues: a consensus statement. Med Sci Sports Exerc 2002; 34: [3] Mitten MJ. When is disqualification from sports justified? Medical judgment vs patients rights. Phys Sportsmed 1996;24:75 8. Further readings 26th Bethesda Conference: recommendations for determining eligibility for competition in athletes with cardiovascular abnormalities. January 6 7, Med Sci Sports Exerc 1994;26:S AAFP, AAP, AMSSM, AOSSM, AOASM. Preparticipation physical evaluation. In: The physician and sportsmedicine. 2nd edition. Minneapolis (MN): McGraw-Hill Healthcare; Adams BB. Transmission of cutaneous infections in athletes. Br J Sports Med 2000;34: American Academy of Pediatrics Committeee on Sports Medicine and Fitness. Cardiac dysrhythmias and sports. Pediatrics 1995;95: Cantu RC. Stingers, transient quadriplegia and cervical spinal stenosis; return-to-play criteria. Med Sci Sports Exerc 1997;29:S Goodman RA, Thacker SB, Solomon SL, Osterholm MT, Hughes JM. Infectious disease in competitive sports. JAMA 1994;271: Herring SA. Rehabilitation of muscle injuries. Med Sci Sports Exerc 1990;22: Kibler WB, Herring SA, Press JM. Functional rehabilitation of sports and muskuloskeletal injuries. Gaithersburg (MD): Aspen; 1998.
9 E.G. McFarland / Clin Sports Med 23 (2004) xv xxiii xxiii Kibler WB, Livingston BP. Closed-chain rehabilitation for upper and lower extremities. J Am Acad Orthop Surg 2001;9: Maron BJ. Cardiovascular risks to young persons on the athletic field. Ann Intern Med 1998; 129: Mellion MB, Walsh WM, Madden C, Putukian M, Shelton GL, editors. Team physician s handbook. 3rd edition. Philadelphia: Hanley & Beltus; Mitten MJ, Mitten RJ. Legal considerations in treating the injured ahtlete. J Orhtop Sports Phys Ther 1995;21: The American Medical Society for Sports Medicine (AMSSM) and the American Academy of Sports Medicine (AASM). Human immunodeficiency virus and other blood-borne pathogens in sports. Clin J Sport Med 1995;5: Edward G. McFarland, MD Division of Sports Medicine and Shoulder Surgery Department of Orthopaedic Surgery The Johns Hopkins University Falls Road, Suite 215 Lutherville, MD 21093, USA address: emcfarl@jhmi.edu
SIDELINE PREPAREDNESS FOR THE TEAM PHYSICIAN: A CONSENSUS STATEMENT
 SIDELINE PREPAREDNESS FOR THE TEAM PHYSICIAN: A CONSENSUS STATEMENT Summary The objective of the Sideline Preparedness Statement is to provide physicians who are responsible for making decisions regarding
SIDELINE PREPAREDNESS FOR THE TEAM PHYSICIAN: A CONSENSUS STATEMENT Summary The objective of the Sideline Preparedness Statement is to provide physicians who are responsible for making decisions regarding
Team Physician Consensus Conference. A project-based alliance of the six major professional associations focused on clinical sports medicine issues.
 Team Physician Consensus Conference A project-based alliance of the six major professional associations focused on clinical sports medicine issues. American Academy of Family Physicians American Academy
Team Physician Consensus Conference A project-based alliance of the six major professional associations focused on clinical sports medicine issues. American Academy of Family Physicians American Academy
Rhinelander High School Parents/coaches meeting Season
 Rhinelander High School Parents/coaches meeting 2008-2009 Season August 3, 2008 By: Kent Jason Lowry, MD Athletic Training Services & The Rhinelander High School What is sports medicine? What are we doing
Rhinelander High School Parents/coaches meeting 2008-2009 Season August 3, 2008 By: Kent Jason Lowry, MD Athletic Training Services & The Rhinelander High School What is sports medicine? What are we doing
Return to Play: A review and update of the team physician consensus statement
 Return to Play: A review and update of the team physician consensus statement John Hatzenbuehler, MD ACSM TPC February 2013 Miami Star running back RTP Football 3 wks mid fibular fracture, nondisplaced
Return to Play: A review and update of the team physician consensus statement John Hatzenbuehler, MD ACSM TPC February 2013 Miami Star running back RTP Football 3 wks mid fibular fracture, nondisplaced
Shoulder Instability: Return to Play 335 Eric C. McCarty, Paul Ritchie, Harpreet S. Gill, and Edward G. McFarland
 RETURN TO PLAY Foreword Mark D. Miller xiii Preface Edward G. McFarland xv Return to Play for Rotator Cuff Injuries and Superior Labrum Anterior Posterior (SLAP) Lesions 321 Hyung Bin Park, Sung Kai Lin,
RETURN TO PLAY Foreword Mark D. Miller xiii Preface Edward G. McFarland xv Return to Play for Rotator Cuff Injuries and Superior Labrum Anterior Posterior (SLAP) Lesions 321 Hyung Bin Park, Sung Kai Lin,
Psychological Issues Related to Injury in Athletes and the Team Physician: A Consensus Statement
 Team Physician Consensus Statement Psychological Issues Related to Injury in Athletes and the Team Physician: A Consensus Statement DEFINITION Team physicians must address the physical and psychological
Team Physician Consensus Statement Psychological Issues Related to Injury in Athletes and the Team Physician: A Consensus Statement DEFINITION Team physicians must address the physical and psychological
BASEBALL 2017 FINAL PROGRAM YOUTH TO THE BIG LEAGUES: MANAGING THE DEVELOPING PLAYER OCTOBER ROSEMONT, IL
 BASEBALL 2017 YOUTH TO THE BIG LEAGUES: MANAGING THE DEVELOPING PLAYER OCTOBER 11 13 ROSEMONT, IL FINAL PROGRAM BASEBALL 2017 YOUTH TO THE BIG LEAGUES: MANAGING THE DEVELOPING PLAYER DESCRIPTION This conference
BASEBALL 2017 YOUTH TO THE BIG LEAGUES: MANAGING THE DEVELOPING PLAYER OCTOBER 11 13 ROSEMONT, IL FINAL PROGRAM BASEBALL 2017 YOUTH TO THE BIG LEAGUES: MANAGING THE DEVELOPING PLAYER DESCRIPTION This conference
Preparticipation Physical Exam
 Preparticipation Physical Exam Angel Garcia, MD CAQ-SM Clinical Associate Professor Paul L Foster School of Medicine Department of Family and Community Medicine No Disclosures Disclosures Objectives Be
Preparticipation Physical Exam Angel Garcia, MD CAQ-SM Clinical Associate Professor Paul L Foster School of Medicine Department of Family and Community Medicine No Disclosures Disclosures Objectives Be
4. Counsel patients and families regarding athletic participation, including:
 Sports Medicine Primary Goals for this Rotation GOAL: Prevention, Counseling and Screening. Understand the pediatrician's role in preventing sports-related injuries, disorders and dysfunction in children
Sports Medicine Primary Goals for this Rotation GOAL: Prevention, Counseling and Screening. Understand the pediatrician's role in preventing sports-related injuries, disorders and dysfunction in children
Life Experience as a Team Physician. James R. Andrews, M.D.
 Life Experience as a Team Physician James R. Andrews, M.D. Goals of this presentation: 1. Discuss what has transpired in the world of sports medicine through the centuries 2. Define the responsibilities
Life Experience as a Team Physician James R. Andrews, M.D. Goals of this presentation: 1. Discuss what has transpired in the world of sports medicine through the centuries 2. Define the responsibilities
Current Concepts in Sports Concussion: Opportunities for the Physical Therapist. Concussion in Sport
 Current Concepts in Sports Concussion: Opportunities for the Physical Therapist Concussion in Sport Current Concepts in Sports Concussion: Opportunities for the Physical Therapist Concussion Management:
Current Concepts in Sports Concussion: Opportunities for the Physical Therapist Concussion in Sport Current Concepts in Sports Concussion: Opportunities for the Physical Therapist Concussion Management:
REACHING PEAK SPORTS PERFORMANCE AND PREVENTING INJURY
 The Athlete s Guide to REACHING PEAK SPORTS PERFORMANCE AND PREVENTING INJURY THE ATHLETE S GUIDE TO REACHING PEAK SPORTS PERFORMANCE AND PREVENTING INJURY Table of Contents Introduction...3 Common Sports
The Athlete s Guide to REACHING PEAK SPORTS PERFORMANCE AND PREVENTING INJURY THE ATHLETE S GUIDE TO REACHING PEAK SPORTS PERFORMANCE AND PREVENTING INJURY Table of Contents Introduction...3 Common Sports
how coaches can work with medical providers to get
 how coaches can work with medical providers to get athletes back in the game WIAA RULES 17.11.1 D. A written statement by the examiner as to the fitness of the student to undertake the proposed athletic
how coaches can work with medical providers to get athletes back in the game WIAA RULES 17.11.1 D. A written statement by the examiner as to the fitness of the student to undertake the proposed athletic
The Team Physician and Strength and Conditioning of Athletes for Sports: A Consensus Statement
 SPECIAL COMMUNICATIONS Team Physician Consensus Statement The Team Physician and Strength and Conditioning of Athletes for Sports: A Consensus Statement DEFINITION Strength and conditioning uses exercise
SPECIAL COMMUNICATIONS Team Physician Consensus Statement The Team Physician and Strength and Conditioning of Athletes for Sports: A Consensus Statement DEFINITION Strength and conditioning uses exercise
Recurrent and Chronic Elbow Instability
 Recurrent and Chronic Elbow Instability Elbow instability is a looseness in the elbow joint that may cause the joint to catch, pop, or slide out of place during certain arm movements. It most often occurs
Recurrent and Chronic Elbow Instability Elbow instability is a looseness in the elbow joint that may cause the joint to catch, pop, or slide out of place during certain arm movements. It most often occurs
SPRINGFIELD PUBLIC SCHOOLS COACH HANDBOOK INJURY MANAGEMENT PROTOCOL
 SPRINGFIELD PUBLIC SCHOOLS COACH HANDBOOK INJURY MANAGEMENT PROTOCOL The health and safety of the athletes at Springfield Public Schools is of the utmost importance. We are committed to providing a safe
SPRINGFIELD PUBLIC SCHOOLS COACH HANDBOOK INJURY MANAGEMENT PROTOCOL The health and safety of the athletes at Springfield Public Schools is of the utmost importance. We are committed to providing a safe
ASPETAR-ACSM SYMPOSIUM: NEW DEVELOPMENTS IN SPORTS MEDICINE. 22nd Sep 2016 AGENDA. In collaboration with:
 ASPETAR-ACSM SYMPOSIUM: NEW DEVELOPMENTS IN SPORTS MEDICINE 22nd Sep 2016 AGENDA In collaboration with: ASPETAR-ACSM Symposium: New developments in Sport Medicine A one-day symposium Thursday 22nd September
ASPETAR-ACSM SYMPOSIUM: NEW DEVELOPMENTS IN SPORTS MEDICINE 22nd Sep 2016 AGENDA In collaboration with: ASPETAR-ACSM Symposium: New developments in Sport Medicine A one-day symposium Thursday 22nd September
Working with Injured Athletes: Integrating Psychology into your Practice. Frances Flint, PhD, CAT(C), ATC York University Toronto, Canada
 Working with Injured Athletes: Integrating Psychology into your Practice Frances Flint, PhD, CAT(C), ATC York University Toronto, Canada But I have to play! Athletes often feel they must participate after
Working with Injured Athletes: Integrating Psychology into your Practice Frances Flint, PhD, CAT(C), ATC York University Toronto, Canada But I have to play! Athletes often feel they must participate after
SPORTS CONCUSSION SUMMIT
 2 nd Annual SPORTS CONCUSSION SUMMIT Friday, June 24 th, 2011 Lexington, KY Presented by: Cardinal Hill Rehabilitation Hospital, the Brain Injury Alliance of Kentucky; s College of Health Sciences; UK
2 nd Annual SPORTS CONCUSSION SUMMIT Friday, June 24 th, 2011 Lexington, KY Presented by: Cardinal Hill Rehabilitation Hospital, the Brain Injury Alliance of Kentucky; s College of Health Sciences; UK
SAIL CANADA CONCUSSION PROTOCOL
 SAIL CANADA CONCUSSION PROTOCOL Sail Canada has developed the Sail Canada Concussion Protocol to help guide the management of Sailing Sport Participants (athletes, coaches, instructors, officials & volunteers)
SAIL CANADA CONCUSSION PROTOCOL Sail Canada has developed the Sail Canada Concussion Protocol to help guide the management of Sailing Sport Participants (athletes, coaches, instructors, officials & volunteers)
Advocating for Your Child: 25 Tips for Parents
 Advocating for Your Child: 25 Tips for Parents Written by David Fassler, M.D. Child & Adolescent Psychiatrist According to the Surgeon General, 1 child in 5 experiences significant problems due to a psychiatric
Advocating for Your Child: 25 Tips for Parents Written by David Fassler, M.D. Child & Adolescent Psychiatrist According to the Surgeon General, 1 child in 5 experiences significant problems due to a psychiatric
Departmental Concussion Guidelines
 Concussion Plan Departmental Concussion Guidelines The following guidelines have been developed in accordance with Alabama A&M s Mission Statement and service goal of providing quality healthcare services
Concussion Plan Departmental Concussion Guidelines The following guidelines have been developed in accordance with Alabama A&M s Mission Statement and service goal of providing quality healthcare services
Pre-participation Physical Examinations
 Pre-participation Physical Examinations www.acsm.org Past Medical History History of any of the following should be made available to the healthcare provider: allergy allergies to medications asthma birth
Pre-participation Physical Examinations www.acsm.org Past Medical History History of any of the following should be made available to the healthcare provider: allergy allergies to medications asthma birth
Deciphering Chronic Pain and Pain Medicine
 Deciphering Chronic Pain and Pain Medicine Deciphering Chronic Pain and Pain Medicine Hello and welcome to Primary Care Today on ReachMD. I m your host, Dr. Brian McDonough, and I m very happy to have
Deciphering Chronic Pain and Pain Medicine Deciphering Chronic Pain and Pain Medicine Hello and welcome to Primary Care Today on ReachMD. I m your host, Dr. Brian McDonough, and I m very happy to have
Madonna University. Athletic Training Room Policies and Procedures
 Madonna University Athletic Training Room Policies and Procedures Revised June 2016 Mission Statement The sports medicine staff strives to maintain the health and wellness of MU student-athletes through
Madonna University Athletic Training Room Policies and Procedures Revised June 2016 Mission Statement The sports medicine staff strives to maintain the health and wellness of MU student-athletes through
Youth Sports and Sports Medicine
 Youth Sports and Sports Medicine Lyle J. Micheli, MD Director, Division of Sports Medicine O Donnell Family Professor of Orthopaedic Sports Medicine Children s Hospital Boston Clinical Professor of Orthopaedic
Youth Sports and Sports Medicine Lyle J. Micheli, MD Director, Division of Sports Medicine O Donnell Family Professor of Orthopaedic Sports Medicine Children s Hospital Boston Clinical Professor of Orthopaedic
LACROSSE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY
 LACROSSE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the Manitoba Lacrosse Association s Youth Concussion Protocol 1. All youth athletes (
LACROSSE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the Manitoba Lacrosse Association s Youth Concussion Protocol 1. All youth athletes (
A Patient s Guide to Burners and Stingers
 A Patient s Guide to Burners and Stingers 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Burners and Stingers 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
Concussions and the Athlete Child Neurology of Tulsa Page 1 of 5
 Page 1 of 5 The Following information has been compiled from the American Academy of Neurology: This practice parameter is based on a background paper 1 written by James P. Kelly, MD, and Jay H. Rosenberg,
Page 1 of 5 The Following information has been compiled from the American Academy of Neurology: This practice parameter is based on a background paper 1 written by James P. Kelly, MD, and Jay H. Rosenberg,
CURRICULUM VITAE RYAN A. JORDEN
 CURRICULUM VITAE RYAN A. JORDEN Work Address Department of Kinesiology 955 La Paz Road Santa Barbara, CA, 93108 (805)565-6206 rjorden@westmont.edu EDUCATIONAL BACKGROUND: Doctor of Philosophy Master of
CURRICULUM VITAE RYAN A. JORDEN Work Address Department of Kinesiology 955 La Paz Road Santa Barbara, CA, 93108 (805)565-6206 rjorden@westmont.edu EDUCATIONAL BACKGROUND: Doctor of Philosophy Master of
HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL SUMMARY
 2018-2019 HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
2018-2019 HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
Sam Houston State University Department of Athletics Concussion Management Policy
 Sam Houston State University Department of Athletics Concussion Management Policy Sam Houston State University will evaluate all student athletes who exhibit signs, symptoms or behaviors consistent with
Sam Houston State University Department of Athletics Concussion Management Policy Sam Houston State University will evaluate all student athletes who exhibit signs, symptoms or behaviors consistent with
SECTION II: DRYLAND TRAINING SUPPLEMENT
 SECTION II: DRYLAND TRAINING SUPPLEMENT Relationship to Risk Management Risk Management is the process of assessing potential variation in outcomes and then developing strategies to mange those areas where
SECTION II: DRYLAND TRAINING SUPPLEMENT Relationship to Risk Management Risk Management is the process of assessing potential variation in outcomes and then developing strategies to mange those areas where
Chiropractic Community Health Alliance. Serving America's Healthcare Safety Net. Guide To Integration
 Chiropractic Community Health Alliance Serving America's Healthcare Safety Net Guide To Integration Guide to Integration Table of Contents Integrating Chiropractic Care in FQHC P.2 Medicaid Benefits for
Chiropractic Community Health Alliance Serving America's Healthcare Safety Net Guide To Integration Guide to Integration Table of Contents Integrating Chiropractic Care in FQHC P.2 Medicaid Benefits for
C.V. EDUCATION EXPERIENCE TURNING POINT REHABILITATION CONSULTING, INC.
 C.V. EDUCATION BOSTON UNIVERSITY Post-Professional OTD Candidate, Anticipated completion May 2018 INTERNATIONAL COMMISSION ON HEALTH CARE CERTIFICATIONS Certified Life Care Planner Examination Completion,
C.V. EDUCATION BOSTON UNIVERSITY Post-Professional OTD Candidate, Anticipated completion May 2018 INTERNATIONAL COMMISSION ON HEALTH CARE CERTIFICATIONS Certified Life Care Planner Examination Completion,
The Atlantic Canada Association of Reflexology Therapists
 The Atlantic Canada Association of Reflexology Therapists Introduction to Standards for Reflexology Therapy Practice The Atlantic Canada Association of Reflexology Therapists (ACART) has developed these
The Atlantic Canada Association of Reflexology Therapists Introduction to Standards for Reflexology Therapy Practice The Atlantic Canada Association of Reflexology Therapists (ACART) has developed these
Sports Medicine Workshops For Schools
 Sports Medicine Workshops For Schools Phone: 8234 6369 Email: admin@sasma.com.au Address: 27 Valetta Road Kidman Park 5025 SA Sports Medicine Association 01 About SASMA Our Mission SA Sports Medicine Association
Sports Medicine Workshops For Schools Phone: 8234 6369 Email: admin@sasma.com.au Address: 27 Valetta Road Kidman Park 5025 SA Sports Medicine Association 01 About SASMA Our Mission SA Sports Medicine Association
Meet. Brent Adams. For more information or to schedule an appointment please call Written by Board Certified Pediatrician
 I think that a lot of orthopedic problems can be solved with medication, physical therapy, chiropractic care, injection, and other non-surgical treatment. Meet Brent Adams Written by Board Certified Pediatrician
I think that a lot of orthopedic problems can be solved with medication, physical therapy, chiropractic care, injection, and other non-surgical treatment. Meet Brent Adams Written by Board Certified Pediatrician
THE NEW BRIGHAM AND WOMEN S ORTHOPEDIC CENTER
 www.brighamandwomensfaulkner.org YOUR GUIDE TO NEW PROGRAMS AND SERVICES AT BRIGHAM AND WOMEN S FAULKNER HOSPITAL THE NEW BRIGHAM AND WOMEN S ORTHOPEDIC CENTER WORLD-CLASS ORTHOPEDIC CARE, RIGHT HERE IN
www.brighamandwomensfaulkner.org YOUR GUIDE TO NEW PROGRAMS AND SERVICES AT BRIGHAM AND WOMEN S FAULKNER HOSPITAL THE NEW BRIGHAM AND WOMEN S ORTHOPEDIC CENTER WORLD-CLASS ORTHOPEDIC CARE, RIGHT HERE IN
CONCUSSION BOARD POLICY 8604
 CONCUSSION BOARD POLICY 8604 Policy Concussion management and policy protocols are a standardized method of assessment to ensure an accurate diagnosis and the appropriate management of student-athlete
CONCUSSION BOARD POLICY 8604 Policy Concussion management and policy protocols are a standardized method of assessment to ensure an accurate diagnosis and the appropriate management of student-athlete
Adjunct Instructor School of Graduate Studies, Doctor of Physical Therapy Program Messiah College Mechanicsburg, PA 1
 Ann D. Dennison, PT, DPT, OCS, LAT, ATC Advanced Physical Therapy and Fitness 102 W. Allen St. 17055 Phone: 717-790-9994 Email: adennisonpt@gmail.com Education Bachelor of Science University of Delaware
Ann D. Dennison, PT, DPT, OCS, LAT, ATC Advanced Physical Therapy and Fitness 102 W. Allen St. 17055 Phone: 717-790-9994 Email: adennisonpt@gmail.com Education Bachelor of Science University of Delaware
Ohio Chapter Chiropractors, Concussions, and Return to Play: Myth s and Facts
 Ohio Chapter Chiropractors, Concussions, and Return to Play: Myth s and Facts Last month the Ohio House of Representatives added language to House Bill 59, the State Operating Budget, to allow chiropractors
Ohio Chapter Chiropractors, Concussions, and Return to Play: Myth s and Facts Last month the Ohio House of Representatives added language to House Bill 59, the State Operating Budget, to allow chiropractors
Introduction. Coaches should leave the training with a clear understanding of the following: How to use the Special Olympics Athletics Coaching Guide
 Introduction On behalf of Special Olympics International, THANK YOU for contributing your time and expertise. The knowledge you share with the course participants will make a significant impact on the
Introduction On behalf of Special Olympics International, THANK YOU for contributing your time and expertise. The knowledge you share with the course participants will make a significant impact on the
Rotator Cuff Tears: Surgical Treatment Options
 Rotator Cuff Tears: Surgical Treatment Options The following article provides in depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article "Rotator Cuff
Rotator Cuff Tears: Surgical Treatment Options The following article provides in depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article "Rotator Cuff
MANITOBA SOCCER ASSOCIATION YOUTH CONCUSSION PROTOCOL SUMMARY
 MANITOBA SOCCER ASSOCIATION YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the MANITOBA SOCCER ASSOCIATION (MSA) YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
MANITOBA SOCCER ASSOCIATION YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the MANITOBA SOCCER ASSOCIATION (MSA) YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
The Core Components of a Sports Physical
 Millions of American athletes - many of them teens - undergo sports physicals each year before they get into their game of choice. Also called a pre-participation examination, the sports physical may seem
Millions of American athletes - many of them teens - undergo sports physicals each year before they get into their game of choice. Also called a pre-participation examination, the sports physical may seem
SOMERVILLE SPORTS MEDICINE
 SOMERVILLE SPORTS MEDICINE Michelle Kelly, MS, ATC,LAT District Coordinator for Concussion Management Head Athletic Trainer mkelly@k12.somerville.ma.us 617-625-6600 x6160 Student-Athlete Guide Make sure
SOMERVILLE SPORTS MEDICINE Michelle Kelly, MS, ATC,LAT District Coordinator for Concussion Management Head Athletic Trainer mkelly@k12.somerville.ma.us 617-625-6600 x6160 Student-Athlete Guide Make sure
Dear Fellow U.S. Armed Services Veteran:
 Dear Fellow U.S. Armed Services Veteran: We appreciate the opportunity to share with you some important information about an issue facing many of our nation s Veterans: hearing loss. According to the Department
Dear Fellow U.S. Armed Services Veteran: We appreciate the opportunity to share with you some important information about an issue facing many of our nation s Veterans: hearing loss. According to the Department
BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY
 BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY
 RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
INTERNATIONAL RUGBY BOARD Putting players first
 The information in this Cardiac Screening Guideline is presented as guidance for Unions, Medical Practitioners and Rugby athletes. The Cardiac Screening recommendations will not be mandated for Unions
The information in this Cardiac Screening Guideline is presented as guidance for Unions, Medical Practitioners and Rugby athletes. The Cardiac Screening recommendations will not be mandated for Unions
Hip Strains. Anyone can experience a hip strain just doing everyday tasks, but strains most often occur during sports activities.
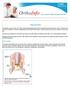 Hip Strains A hip strain occurs when one of the muscles supporting the hip joint is stretched beyond its limit or torn. Strains may be mild, moderate, or severe, depending on the extent of the injury.
Hip Strains A hip strain occurs when one of the muscles supporting the hip joint is stretched beyond its limit or torn. Strains may be mild, moderate, or severe, depending on the extent of the injury.
EMERGENCY ACTION PLAN
 WILLISTON Middle School ATHLETICS EMERGENCY ACTION PLAN Introduction Unfortunately there is an inherent risk of medical emergencies in any sport or athletic activity. It is pertinent to have an emergency
WILLISTON Middle School ATHLETICS EMERGENCY ACTION PLAN Introduction Unfortunately there is an inherent risk of medical emergencies in any sport or athletic activity. It is pertinent to have an emergency
The Heart Center and Sports Medicine. A Coach s Guide to Sudden Cardiac Arrest
 The Heart Center and Sports Medicine A Coach s Guide to Sudden Cardiac Arrest What is the purpose of the new sudden cardiac arrest (SCA) law, also known as Lindsay s Law, in Ohio? Ohio Senate Bill 252
The Heart Center and Sports Medicine A Coach s Guide to Sudden Cardiac Arrest What is the purpose of the new sudden cardiac arrest (SCA) law, also known as Lindsay s Law, in Ohio? Ohio Senate Bill 252
Treat each athlete/patient as we would treat our own family.
 Our Core Purpose To improve the lives of others through science, education and clinical skill. Our Core Values Everything you do must enhance the athlete/patient experience, thereby improving the reputation
Our Core Purpose To improve the lives of others through science, education and clinical skill. Our Core Values Everything you do must enhance the athlete/patient experience, thereby improving the reputation
Celebration Lutheran School
 Celebration Lutheran School Wisconsin Interscholastic Athletic Association Athletic History and Physical Examination Approval for TWO YEARS of Competition All students participating in interscholastic
Celebration Lutheran School Wisconsin Interscholastic Athletic Association Athletic History and Physical Examination Approval for TWO YEARS of Competition All students participating in interscholastic
City of Norwalk Recreation Department. Concussion Guidelines for Youth Athletics
 City of Norwalk Recreation Department Concussion Guidelines for Youth Athletics I. INTRODUCTION. In recognition of the dangers posed to youth athletes as a result of sports related head injuries, the City
City of Norwalk Recreation Department Concussion Guidelines for Youth Athletics I. INTRODUCTION. In recognition of the dangers posed to youth athletes as a result of sports related head injuries, the City
MEDICAL CLEARANCE AND RETURN TO PLAY
 MEDICAL CLEARANCE AND RETURN TO PLAY WIAA CONFERENCE AUGUST 1, 2014 YAKIMA, WA Presented by Raymond A. Roberts, ARM, SCLA, CPSI WWW.WSRMP.COM AGENDA What are Negligence and Liability? Return to Play Liability
MEDICAL CLEARANCE AND RETURN TO PLAY WIAA CONFERENCE AUGUST 1, 2014 YAKIMA, WA Presented by Raymond A. Roberts, ARM, SCLA, CPSI WWW.WSRMP.COM AGENDA What are Negligence and Liability? Return to Play Liability
USA GYMNASTICS 2017 NATIONAL TEAM FUNDING AND SUPPORT AGREEMENT
 USA GYMNASTICS 2017 NATIONAL TEAM FUNDING AND SUPPORT AGREEMENT This Agreement is entered into between USA GYMNASTICS (USA Gym), a not-for-profit corporation designated by the United States Olympic Committee
USA GYMNASTICS 2017 NATIONAL TEAM FUNDING AND SUPPORT AGREEMENT This Agreement is entered into between USA GYMNASTICS (USA Gym), a not-for-profit corporation designated by the United States Olympic Committee
The Spine Injured Athlete: FROM INJURY TO RETURN TO PLAY
 Marina Spine Center presents Saturday, June 9, 2018 CERTIFIED ATHLETIC TRAINER AND PHYSICAL THERAPIST CONFERENCE The Spine Injured Athlete: FROM INJURY TO RETURN TO PLAY Keynote Speakers: DOUBLETREE by
Marina Spine Center presents Saturday, June 9, 2018 CERTIFIED ATHLETIC TRAINER AND PHYSICAL THERAPIST CONFERENCE The Spine Injured Athlete: FROM INJURY TO RETURN TO PLAY Keynote Speakers: DOUBLETREE by
CDM. Coach Development Model. coach! Special Olympics
 CDM Special Olympics Coach Development Model coach! CDM_brochure_FINAL.indd 1 8/12/2014 7:22:54 PM What is the Special Olympics CDM? The Coach Development Model (CDM) provides a framework for SO Programs
CDM Special Olympics Coach Development Model coach! CDM_brochure_FINAL.indd 1 8/12/2014 7:22:54 PM What is the Special Olympics CDM? The Coach Development Model (CDM) provides a framework for SO Programs
Department of Anesthesiology. Clinical Base Year Neurosurgery Curriculum. Residency Program Director Department of Neurosurgery
 Clinical Base Year Neurosurgery Curriculum Collaborating Faculty: Julian Bailes, MD Residency Program Director Department of Neurosurgery Educational Purpose: The purpose of this rotation is for residents
Clinical Base Year Neurosurgery Curriculum Collaborating Faculty: Julian Bailes, MD Residency Program Director Department of Neurosurgery Educational Purpose: The purpose of this rotation is for residents
Welcome to the ACSM/Exercise is Medicine Professional Credential online workshop presented by Health & Exercise Connections, LLC
 Welcome to the ACSM/Exercise is Medicine Professional Credential online workshop presented by Health & Exercise Connections, LLC Objectives 1. Provide candidates with an overview of content related to
Welcome to the ACSM/Exercise is Medicine Professional Credential online workshop presented by Health & Exercise Connections, LLC Objectives 1. Provide candidates with an overview of content related to
Health Care Providers Action Guide
 Health Care Providers Action Guide Health Care Providers Action Guide How to Implement Exercise is Medicine in Your Practice This Exercise is Medicine Health Care Providers Action Guide provides simple
Health Care Providers Action Guide Health Care Providers Action Guide How to Implement Exercise is Medicine in Your Practice This Exercise is Medicine Health Care Providers Action Guide provides simple
Code of Ethics, International Federation of Sports Physical Therapists, adopted GM, Cape Town September 2013
 Code of Ethics, The following Code of Ethics of International Federations of Sports Physical Therapists (IFSPT) is based on The International Federation of Sports Medcine (FIMS) Code of Ethics (http://www.fims.org/en/general/code-of-ethics/)
Code of Ethics, The following Code of Ethics of International Federations of Sports Physical Therapists (IFSPT) is based on The International Federation of Sports Medcine (FIMS) Code of Ethics (http://www.fims.org/en/general/code-of-ethics/)
I. Introduction. II. Program Description
 Advanced Post-Graduate Athletic Training Program Division of Sports Medicine Department of Orthopaedic Surgery Department of Athletics, Physical Education and Recreation I. Introduction The Stanford University
Advanced Post-Graduate Athletic Training Program Division of Sports Medicine Department of Orthopaedic Surgery Department of Athletics, Physical Education and Recreation I. Introduction The Stanford University
Shawna D. Baker San Diego, CA (619)
 Highlights and Qualifications Shawna D. Baker San Diego, CA shawnabaker@pointloma.edu (619) 849-2914 Over 19 years of experience providing outstanding evaluation, treatment, rehabilitation, and reconditioning
Highlights and Qualifications Shawna D. Baker San Diego, CA shawnabaker@pointloma.edu (619) 849-2914 Over 19 years of experience providing outstanding evaluation, treatment, rehabilitation, and reconditioning
Suicide Prevention Strategic Plan
 Suicide Prevention Strategic Plan 2019 For more information visit dphhs.mt.gov/suicideprevention 2 Vision Zero suicide in the Big Sky State Mission Our Reduce suicide in Montana through a comprehensive,
Suicide Prevention Strategic Plan 2019 For more information visit dphhs.mt.gov/suicideprevention 2 Vision Zero suicide in the Big Sky State Mission Our Reduce suicide in Montana through a comprehensive,
Dr. Christine Pickup, Au.D. The Top 10 Things You Must Know Before Choosing Your. Audiologist. Mt. Harrison Audiology
 Dr. Christine Pickup, Au.D. The Top 10 Things You Must Know Before Choosing Your Audiologist Mt. Harrison Audiology Welcome Letter from Dr. Christine Pickup, Au.D. Dear Friend, If you are researching audiologists
Dr. Christine Pickup, Au.D. The Top 10 Things You Must Know Before Choosing Your Audiologist Mt. Harrison Audiology Welcome Letter from Dr. Christine Pickup, Au.D. Dear Friend, If you are researching audiologists
Presentation Preparation
 November 2015 TABLE OF CONTENTS page 1 CHIROPRACTORS PRESENTING CHIROPRACTIC TO OTHER HEALTH PRACTITIONERS Presentation Tips Getting Ready Presentation Day Following Up page 3 COMMON QUESTIONS AND HOW
November 2015 TABLE OF CONTENTS page 1 CHIROPRACTORS PRESENTING CHIROPRACTIC TO OTHER HEALTH PRACTITIONERS Presentation Tips Getting Ready Presentation Day Following Up page 3 COMMON QUESTIONS AND HOW
Dr. Robert "Bob" Braile brief biography
 Dr. Robert "Bob" Braile brief biography Dr. Robert "Bob" Braile has been involved in almost every aspect of chiropractic life. He has been a successful high volume practitioner. He is an author and a regular
Dr. Robert "Bob" Braile brief biography Dr. Robert "Bob" Braile has been involved in almost every aspect of chiropractic life. He has been a successful high volume practitioner. He is an author and a regular
The same ethical principles that apply to the practice of medicine shall apply to sports medicine. The main duties of a physician include:
 Fédération Internationale de Médecine Sportive (FIMS) Code of Ethics (23 September 1997) 1. Medical ethics in general: The same ethical principles that apply to the practice of medicine shall apply to
Fédération Internationale de Médecine Sportive (FIMS) Code of Ethics (23 September 1997) 1. Medical ethics in general: The same ethical principles that apply to the practice of medicine shall apply to
Curriculum Vitae. Alan W. Palmer D.C., C.C.S.T. Professional Experience
 Curriculum Vitae Alan W. Palmer D.C., C.C.S.T. Professional Experience Palmer Center for Natural Healing, Scottsdale, AZ 1990 - Present Triad Rehabilitation, Scottsdale, AZ 1990 - Present Proflex Dynamic
Curriculum Vitae Alan W. Palmer D.C., C.C.S.T. Professional Experience Palmer Center for Natural Healing, Scottsdale, AZ 1990 - Present Triad Rehabilitation, Scottsdale, AZ 1990 - Present Proflex Dynamic
CURRICULUM VITAE. Peter S. Zulia, MBA, A.T., A.T., C., P.T., S.C.S.
 CURRICULUM VITAE Peter S. Zulia, MBA, A.T., A.T., C., P.T., S.C.S. pete.zulia@oxfordpt.com Home Address Office Address 9528 Heather Ct. 7567 Central Parke Blvd. Cincinnati, Oh 45242 Mason, Ohio 45040 E
CURRICULUM VITAE Peter S. Zulia, MBA, A.T., A.T., C., P.T., S.C.S. pete.zulia@oxfordpt.com Home Address Office Address 9528 Heather Ct. 7567 Central Parke Blvd. Cincinnati, Oh 45242 Mason, Ohio 45040 E
Health and Exercise Science
 Health and Exercise Science-1 Health and Exercise Science Faculty: Hoffman, Chair; Chilakos, Faigenbaum, Farrell, Hill, Kang, Ratamess The Department of Health and Exercise Science prepares students as
Health and Exercise Science-1 Health and Exercise Science Faculty: Hoffman, Chair; Chilakos, Faigenbaum, Farrell, Hill, Kang, Ratamess The Department of Health and Exercise Science prepares students as
TRAINING COORDINATOR TRAINING
 TRAINING COORDINATOR TRAINING 1. Role of Training Coordinator: Responsible for all sports training for athletes and coaches in the local program. As a sports organization, our main focus should be to assure
TRAINING COORDINATOR TRAINING 1. Role of Training Coordinator: Responsible for all sports training for athletes and coaches in the local program. As a sports organization, our main focus should be to assure
CURRICULUM VITAE. Loyola University Medical Center
 CURRICULUM VITAE VICTOR M. ROMANO, M.D. PERSONAL INFORMATION: Born: August 16,1958 Chicago, Illinois Married: Margaret Mary Oulvey Romano, C.P.A. Children: Maria Romano McGann, DO (Born 1985) Cristina
CURRICULUM VITAE VICTOR M. ROMANO, M.D. PERSONAL INFORMATION: Born: August 16,1958 Chicago, Illinois Married: Margaret Mary Oulvey Romano, C.P.A. Children: Maria Romano McGann, DO (Born 1985) Cristina
INVESTIGATION OF MANAGEMENT MODELS
 S.K. Chen, Y.M. Cheng, Y.C. Lin, et al INVESTIGATION OF MANAGEMENT MODELS IN ELITE ATHLETE INJURIES Shen-Kai Chen, Yun-Min Cheng, Yen-Chung Lin, 1 Yu-Jue Hong, 1 Peng-Ju Huang, and Pei-Hsi Chou Department
S.K. Chen, Y.M. Cheng, Y.C. Lin, et al INVESTIGATION OF MANAGEMENT MODELS IN ELITE ATHLETE INJURIES Shen-Kai Chen, Yun-Min Cheng, Yen-Chung Lin, 1 Yu-Jue Hong, 1 Peng-Ju Huang, and Pei-Hsi Chou Department
MEDFORD SPORTS INJURY & THERAPY CENTER INC MEDFORD, OREGON CCCE CONTINUING EDUCATION AND INSTRUCTOR INFORMATION (FOUR INSTRUCTORS)
 MEDFORD SPORTS INJURY & THERAPY CENTER INC MEDFORD, OREGON 1 CCCE CONTINUING EDUCATION AND INSTRUCTOR INFORMATION (FOUR INSTRUCTORS) 1. STEVEN W. ZERKEL, Director PT, ATC, M. Ed 2780 E Barnett Road Ste
MEDFORD SPORTS INJURY & THERAPY CENTER INC MEDFORD, OREGON 1 CCCE CONTINUING EDUCATION AND INSTRUCTOR INFORMATION (FOUR INSTRUCTORS) 1. STEVEN W. ZERKEL, Director PT, ATC, M. Ed 2780 E Barnett Road Ste
Scope of Practice for the Diagnostic Ultrasound Professional
 Scope of Practice for the Diagnostic Ultrasound Professional Copyright 1993-2000 Society of Diagnostic Medical Sonographers, Dallas, Texas USA: All Rights Reserved Worldwide. Organizations which endorse
Scope of Practice for the Diagnostic Ultrasound Professional Copyright 1993-2000 Society of Diagnostic Medical Sonographers, Dallas, Texas USA: All Rights Reserved Worldwide. Organizations which endorse
MOUNT VERNON CITY SCHOOL DISTRICT ATHLETICS and HEALTH SERVICES
 STUDENT NAME SPORT DATE GRADE LEVEL COACH PARENT/GUARDIAN ATHLETIC PARTICIPATION CONSENT FORM *PLEASE RETURN THIS FORM ON THE DAY THE ATHLETE HAS HIS/HER PHYSICAL/CONFERENCE* Dear Parent or Guardian: Your
STUDENT NAME SPORT DATE GRADE LEVEL COACH PARENT/GUARDIAN ATHLETIC PARTICIPATION CONSENT FORM *PLEASE RETURN THIS FORM ON THE DAY THE ATHLETE HAS HIS/HER PHYSICAL/CONFERENCE* Dear Parent or Guardian: Your
PRT Eligibility. PRT Course Requirements. POSTURAL RESTORATION TRAINED (PRT) Application Deadline October 15, 2017 (for testing in January 2018)
 POSTURAL RESTORATION TRAINED (PRT) Application Deadline October 15, 2017 (for testing in January 2018) The Postural Restoration Institute (PRI) has implemented a credentialing process for Athletic Trainers
POSTURAL RESTORATION TRAINED (PRT) Application Deadline October 15, 2017 (for testing in January 2018) The Postural Restoration Institute (PRI) has implemented a credentialing process for Athletic Trainers
The Heart Center and Sports Medicine. A Parent s Guide to Sudden Cardiac Arrest
 The Heart Center and Sports Medicine A Parent s Guide to Sudden Cardiac Arrest What is the purpose of the new sudden cardiac arrest (SCA) law, also known as Lindsay s Law, in Ohio? Ohio Senate Bill 252
The Heart Center and Sports Medicine A Parent s Guide to Sudden Cardiac Arrest What is the purpose of the new sudden cardiac arrest (SCA) law, also known as Lindsay s Law, in Ohio? Ohio Senate Bill 252
SPORT AND PHYSICAL ACTIVITY
 2016 Suite Cambridge TECHNICALS LEVEL 3 SPORT AND PHYSICAL ACTIVITY Unit 17 Sports injuries and rehabilitation T/507/4468 Guided learning hours: 60 Version 4 - revised September 2018 *changes indicated
2016 Suite Cambridge TECHNICALS LEVEL 3 SPORT AND PHYSICAL ACTIVITY Unit 17 Sports injuries and rehabilitation T/507/4468 Guided learning hours: 60 Version 4 - revised September 2018 *changes indicated
NATA PPE POSITION STATEMENT
 NATA PPE POSITION STATEMENT Objective of the Position Statement To present athletic trainers with recommendations for the content and administration of the Pre-participation Physical Examination (PPE)
NATA PPE POSITION STATEMENT Objective of the Position Statement To present athletic trainers with recommendations for the content and administration of the Pre-participation Physical Examination (PPE)
Livingston County Community Resource Guide: Diabetes Prevention & Management
 1 Table of Contents How to use this guide... 3 Livingston County Resources... 4 Prevention... 5 Management... 8 Nearby Resources... 12 Management... 13 National and Online Resources... 19 Prevention...
1 Table of Contents How to use this guide... 3 Livingston County Resources... 4 Prevention... 5 Management... 8 Nearby Resources... 12 Management... 13 National and Online Resources... 19 Prevention...
Why Tobacco Cessation?
 Tobacco Cessation in Community Settings Introduction Hello and welcome to the Learning and Action Network event, Reaching Those in Need of Tobacco Cessation in Community Settings: Research, Recommendations
Tobacco Cessation in Community Settings Introduction Hello and welcome to the Learning and Action Network event, Reaching Those in Need of Tobacco Cessation in Community Settings: Research, Recommendations
COMPETENCIES FOR THE NEW DENTAL GRADUATE
 COMPETENCIES FOR THE NEW DENTAL GRADUATE The Competencies for the New Dental Graduate was developed by the College of Dentistry s Curriculum Committee with input from the faculty, students, and staff and
COMPETENCIES FOR THE NEW DENTAL GRADUATE The Competencies for the New Dental Graduate was developed by the College of Dentistry s Curriculum Committee with input from the faculty, students, and staff and
Dear Newport News Athletic Parent/Guardian:
 Dear Newport News Athletic Parent/Guardian: According to the Children s Hospital of the King s Daughter about one in ten local athletes in contact sports will sustain a concussion during a sports season.
Dear Newport News Athletic Parent/Guardian: According to the Children s Hospital of the King s Daughter about one in ten local athletes in contact sports will sustain a concussion during a sports season.
NEDC e-bulletin. Issue 19 February 2014
 NEDC e-bulletin Issue 19 February 2014 Introduction Welcome to the February edition of the NEDC e-bulletin. This month we are highlighting issues of relevance to athletes, coaches and other sport and fitness
NEDC e-bulletin Issue 19 February 2014 Introduction Welcome to the February edition of the NEDC e-bulletin. This month we are highlighting issues of relevance to athletes, coaches and other sport and fitness
NovaCare Rehabilitation Athletic Training Services
 NovaCare Rehabilitation Athletic Training Services Concussion Management Standards: Harrisburg Academy 10 Erford Rd Wormleysburg, PA 17043 Medical management of sports-related concussion is evolving. In
NovaCare Rehabilitation Athletic Training Services Concussion Management Standards: Harrisburg Academy 10 Erford Rd Wormleysburg, PA 17043 Medical management of sports-related concussion is evolving. In
Students With Attention Deficit Hyperactivity Disorder
 On January 29, 2018 the Arizona State Board of Education approved a list of qualified professionals for identification of educational disabilities as developed by the Arizona Department of Education. Categories
On January 29, 2018 the Arizona State Board of Education approved a list of qualified professionals for identification of educational disabilities as developed by the Arizona Department of Education. Categories
University of Notre Dame Sports Medicine Department Intercollegiate Athletics Concussion Management Plan
 ! Purpose: University of Notre Dame Sports Medicine Department Intercollegiate Athletics Concussion Management Plan Head injuries can pose a significant health risk for student-athletes competing in intercollegiate
! Purpose: University of Notre Dame Sports Medicine Department Intercollegiate Athletics Concussion Management Plan Head injuries can pose a significant health risk for student-athletes competing in intercollegiate
The Advantage of Having An Athletic Therapist on the Sidelines
 The Advantage of Having An Athletic Therapist on the Sidelines By: Wai-Ip Chung, DO(MP), NASM-Certified Personal Trainer National University of Medical Sciences MSc.AT, Class of 2015 Toronto, Canada Athletic
The Advantage of Having An Athletic Therapist on the Sidelines By: Wai-Ip Chung, DO(MP), NASM-Certified Personal Trainer National University of Medical Sciences MSc.AT, Class of 2015 Toronto, Canada Athletic
Practical Performance and Personal Exercise Programme (PEP)
 7 Practical Performance and Personal Exercise Programme (PEP) When you have worked through this chapter, you will have developed knowledge and understanding of: what is required for the practical performance
7 Practical Performance and Personal Exercise Programme (PEP) When you have worked through this chapter, you will have developed knowledge and understanding of: what is required for the practical performance
1. Improve Documentation Now
 Joseph C. Nichols, MD, Principal, Health Data Consulting, Seattle, Washington From Medscape Education Family Medicine: Transition to ICD-10: Getting Started. Posted: 06/19/2012 Target Audience: This activity
Joseph C. Nichols, MD, Principal, Health Data Consulting, Seattle, Washington From Medscape Education Family Medicine: Transition to ICD-10: Getting Started. Posted: 06/19/2012 Target Audience: This activity
Even if cleared by a physician
 ALATA Annual Meeting May 20, 2012 James B. Robinson, M.D. Head Team Physician, University of Alabama Endowed Chair of Sports Medicine, CCHS Fellowship Director Lystedt Law, Washington state Passed in 2009
ALATA Annual Meeting May 20, 2012 James B. Robinson, M.D. Head Team Physician, University of Alabama Endowed Chair of Sports Medicine, CCHS Fellowship Director Lystedt Law, Washington state Passed in 2009
CONCUSSION POLICY. Can occur even if there has been no loss of consciousness (in fact most concussions occur without a loss of consciousness).
 CONCUSSION POLICY Seven Oaks School Division places a high priority on the health, safety and overall wellness of our students and recognize that children and adolescents can be at high risk of concussion
CONCUSSION POLICY Seven Oaks School Division places a high priority on the health, safety and overall wellness of our students and recognize that children and adolescents can be at high risk of concussion
MUSCULOSKELETAL PROGRAM OF CARE
 MUSCULOSKELETAL PROGRAM OF CARE AUGUST 1, 2014 Table of contents Acknowledgements... 3 MSK POC Scope... 3 The Evidence... 3 Objectives.... 4 Target Population.... 4 Assessment of Flags and Barriers to
MUSCULOSKELETAL PROGRAM OF CARE AUGUST 1, 2014 Table of contents Acknowledgements... 3 MSK POC Scope... 3 The Evidence... 3 Objectives.... 4 Target Population.... 4 Assessment of Flags and Barriers to
When it hurts, we ll help get you moving again.
 When it hurts, we ll help get you moving again. There are nonsurgical options for you! Are you normally active but currently restricting your physical activities due to nagging pain or injury that just
When it hurts, we ll help get you moving again. There are nonsurgical options for you! Are you normally active but currently restricting your physical activities due to nagging pain or injury that just
