FEATURE. 8 EMERGENCY MEDICINE I JANUARY
|
|
|
- Rosalyn Parker
- 5 years ago
- Views:
Transcription
1 FEATURE 8 EMERGENCY MEDICINE I JANUARY
2 Pediatric ENT Complaints: An Update Melanie A. Weller, MD; Joel M. Clingenpeel, MD, MPH, MS.MEdL This review highlights the diagnosis and management of the three most common causes of pediatric otolaryngologic complaints seen in the ED. Among all of the causes of ear, nose, and throat (ENT) complaints, acute otitis media (AOM), bacterial sinusitis, and streptococcal pharyngitis (SP) are the most common infections prompting pediatric presentation to the ED. Through a series of case scenarios, along with key questions to help guide the clinician s workup, this review covers the proper evaluation and management of pediatric ENT complaints. Case Scenario 1 A 13-month-old girl presented to the ED with a 1-day history of fever and runny nose. According to her parents, the child had been continually pulling on her ears in apparent discomfort. During historytaking, the parents further informed the emergency physician (EP) that the patient started daycare 4 months earlier and had two elementary school-aged siblings. The patient s medical history was significant for otitis media, but the parents stated she had not been on antibiotics for over 4 months. On physical examination, the patient s vital signs were: blood pressure (BP), 75/50 mm Hg; temperature (T), F; slight tachycardia; and normal age-adjusted respiratory rate (RR). Oxygen saturation was 100% on room air. The lungs were clear to auscultation and heart sounds were normal and without murmur. The otolaryngologic examination revealed copious yellow discharge from both nostrils, non-erythematous posterior oropharynx, and erythema to the right tympanic membrane (TM). Questions to Guide the Work-Up: (1) What physical examination findings should be present for accurate diagnosis of otitis media? (2) Will this patient require antibiotics immediately, or is a wait-and-see approach indicated? (3) If treatment with antibiotic therapy is warranted, what are the appropriate therapeutic regimen and duration of therapy? Otitis Media Acute otitis media is one of the most common presentations in young children. Defined as the rapid onset of signs and Dr Weller is a fellow in pediatric emergency medicine, Eastern Virginia Medical School/Children s Hospital of The King s Daughters, Norfolk. Dr Clingenpeel is the fellowship director of pediatric emergency medicine; and associate professor of pediatrics, Eastern Virginia Medical School/Children s Hospital of The King s Daughters, Norfolk. Authors Disclosure Statement: The authors report no actual or potential conflict of interest in relation to this article. DOI: /emed JANUARY 2017 I EMERGENCY MEDICINE 9
3 PEDIATRIC ENT COMPLAINTS: AN UPDATE symptoms of middle ear inflammation, in conjunction with middle ear effusion (MEE), AOM can develop secondary to a viral or bacterial infection. It is estimated that more than 80% of the pediatric population will experience at least one episode of AOM by age 3 years. 1-3 Risk factors for AOM include upper respiratory infection (URI), daycare attendance, siblings, parental smoking, and formulafeeding versus breastfeeding. The patient s history may include rapid-onset otalgia, fever, irritability, anorexia, and concurrent URI symptoms, as well as other nonspecific symptoms (eg, ear rubbing and/or pulling, crying, changes in behavior and sleep patterns). 2-4 In general, otalgia and ear-rubbing in the nonverbal patient seem to have the best predictive value for AOM. 3 Signs and Symptoms A normal TM should be translucent and pearly gray, with visible landmarks of the manubrium of malleus and pars flaccida. A TM that is bulging, cloudy, and immobile is the most consistent finding in AOM, with bulging having a specificity of 97%. Redness of the tympanic membrane is not a useful predictor of AOM as this finding is noted in upward of 30% of pediatric patients on general examination but in <1% of AOM diagnoses in the absence of a bulging TM. Diagnosis Pneumatic otoscopy is the gold standard for diagnosing for MEE; however, this examination can be difficult in younger, often uncooperative, patients. A TM that does not perceptibly move with either positive or negative insufflation pressure greatly enhances the diagnostic accuracy for MEE over the use of visible eardrum characteristics alone. 2-5 Acute otitis media is a clinical diagnosis and does not require imaging studies or laboratory evaluation unless more serious processes, such as skull fracture, mastoiditis, or intracranial abscess, are being considered. 2,3 Treatment and Management Analgesia. The first step in managing patients with AOM is to provide analgesia. In most cases, acetaminophen in patients over 2 months of age, or ibuprofen in patients over 6 months of age, are adequate choices for managing pain. When either of these analgesics is administered in the clinic/ed setting, patients should be monitored to assure adequate pain relief prior to discharge. While topical agents such as combination antipyrine-benzocaine suspensions were commonly given in the past to alleviate the pain associated with AOM, there are limited data to support their effectiveness. As such, in July 2015, the US Food and Drug Administration ordered manufacturers to halt production on these unapproved prescription products. 3,4,6 There are also no randomized controlled trials (RCTs) to support the use of decongestants or antihistamines for resolution of AOM or otalgia. 3,7 Antibiotic Therapy. The most common bacteria associated with AOM are Streptococcus pneumonia, nontypeable Hemophilus influenza, and Moraxella catarrhalis. In 30% of patients, the causative etiology is viral. When the decision is made to treat AOM, high-dose amoxicillin is still considered the first-line treatment, despite ever evolving susceptibilities of bacteria. Alternate therapies include amoxicillinclavulanate, azithromycin, cefdinir, ceftriaxone, and sulfamethoxazole-trimethoprim; however, treatment with azithromycin or sulfamethoxazole-trimethoprim should be reserved for patients who have a history of anaphylactic reaction to penicillin (Table 1). When a child is noted to have been treated with amoxicillin within a 30-day period or who has concurrent conjunctivitis, amoxicillin-clavulanate is considered the first-line treatment. 2-4,7,8 The current American Academy of Pediatrics (AAP) guidelines recommend 10 days of antibiotic therapy for children younger than age 2 years, and 5 to 7 days for children older 10 EMERGENCY MEDICINE I JANUARY
4 Table 1. Recommended Antibiotic Therapy for Acute Otitis Media and Acute Bacterial Sinusitis 2-4,7,10,12 Drug Dose Maximum Dosage Notes Amoxicillin mg/kg/d, divided twice a day 2,000 mg per dose Amoxicillinclavulanate mg/kg/d (amoxicillin component divided twice a day) 2,000 mg per dose (amoxicillin component) Use 14:1 amoxicillin:clavulanate ratio (ES-600 suspension) Cefdinir 14 mg/kg/d daily or divided twice a day 600 mg/d May cause dark red stool (resembling melena), particularly in infants on iron-fortified formulas Azithromycin 10 mg/kg/d, day 1 5 mg/kg/d, days mg, day mg, days 2-5 Sulfamethoxizoletrimethoprim 8-12 mg/kg/d trimethoprim component divided twice a day 160 mg per dose trimethoprim component Ceftriaxone 50 mg/kg intramuscularly for 1,000 mg 1day, with maximum of 1,000 mg per dose * 50 mg/kg intramuscularly for 1,000 mg 3 consecutive days, with a maximum of 1,000 mg per dose^ Acute otitis media indications: *If child is unable to tolerate oral route ^For cases of oral treatment failure than age 2 years who have uncomplicated AOM. Intramuscular (IM) ceftriaxone is an acceptable first-line agent in a child who is unable to tolerate oral medications or who is suffering persistent emesis. Intramuscular ceftriaxone can be given as a single dose of 50 mg/kg, though the patient should be followed closely as studies show that a second dose may be necessary 5 to 7 days later to prevent infection recurrence. The IM dose of ceftriaxone 50 mg/kg can also be given if treatment with other antibiotics fails to resolve the AOM (failure is defined as no improvement in the patient s condition 48 to 72 hours from treatment). In such cases, ceftriaxone is given in three consecutive doses. 3,4,7 Wait-and-See Approach. Studies of patients whose AOM was confirmed via culture (19% were positive for S pneumoniae, 48% for H influenza, and 78% for M catarrhalis) showed bacterial clearance without antibiotic intervention. 4 Based on these findings, the 2013 revised AAP evidence-based clinical practice guidelines indicate an initial watching-and-waiting period combined with pain management for patients older than 6 months of age who are diagnosed with unilateral AOM in the absence of severe symptoms (ie, fever is lower than F or patient has severe otalgia). 4 A period of observation prior to treatment is also endorsed for children older than age 2 years who exhibit nonsevere symptoms even if they have bilateral disease. 4 Conversely, all patients younger than age 6 months and all children with severe symptoms should be treated with antibiotics at diagnosis. 3,4 The wait-andsee approach, recommends an observation period of 24 to 48 hours for children in the lower risk group prior to antibiotic administration. Delayed antibiotic administration can be performed by a physician JANUARY 2017 I EMERGENCY MEDICINE 11
5 PEDIATRIC ENT COMPLAINTS: AN UPDATE in an office/ed follow-up or as a safety-net antibiotic prescription (SNAP) sent home with the family on the initial ED encounter. 2-4,8,9 Case 1 Resolution Given this patient s unilateral and nonsevere symptoms (minor otalgia, fever <102.2 F), age older than 6 months, and no recent antibiotic use), she was treated with oral ibuprofen. At discharge, the parents were given a 10-day SNAP prescription of high-dose amoxicillin (90 mg/kg/d, divided into two daily doses) and instructed to fill the prescription only if the patient s otalgia did not improve in 1 or 2 days. Case Scenario 2 A 5-year-old boy was presented for evaluation by his parents, who stated that their son had been sick since he had started kindergarten in the fall. The patient had a 10-day history of cough, thick runny nose, and facial pain, and a 1-day history of new-onset fever and headache. His parents further noted that the patient had been seen by his pediatrician several times over the past week. At each of these visits, the pediatrician had informed them that their son had a virus. Vital signs on examination were: BP, 100/60 mm Hg; heart rate (HR), 112 beats/ min; normal age-adjusted RR; and T, o F. Oxygen saturation was 100% on room air. The patient did not appear toxic, his lungs were clear on auscultation, and there were no other clinical signs suggestive of meningitis. The otolaryngologic examination revealed bilateral thick mucoid drainage and visible edema and erythema of the nasal turbinates. The patient was noted to have some facial pain in the maxillary area bilaterally. Questions to Guide the Work-Up: (1) Does the patient have a prolonged URI or pediatric sinusitis, and what differentiates the two conditions? (2) What sinuses are present in a 5-year-old patient? (3) What treatment modalities are available for sinusitis? (4) Is imaging of the sinuses helpful in confirming the diagnosis? Acute Bacterial Sinusitis Rhinosinusitis is an inflammation of the mucosal lining of the nasal passages and paranasal sinuses. Most cases occur secondary to a viral URI and resolve spontaneously in 99% of the pediatric population. 10,11 Acute bacterial sinusitis (ABS) is an inflammation of the same mucosal lining of the nasal passages secondary to bacterial overgrowth that lasts more than 10 days, with complete resolution by 30 days. 12,13 When evaluating a pediatric patient for ABS, it is important to consider the sinus growth and development: If the sinus is not yet formed, it therefore cannot be the location of an ABS. 13 The ethmoid and maxillary sinuses are present at birth, aerated within 4 months of life, and are fully developed by age 12 years. The sphenoid sinuses begin development around age 3 years, are aerated by age 7 or 8 years, and are fully developed by age 18 to 20 years. The frontal sinuses begin development around age 8 years and are aerated and fully developed by age 12 to 15 years. 10,13,14 While most guidelines focus on children older than age 1 year (due to very small infantile sinuses), ABS does occur in children younger than age 1 year. 12,14 Signs and Symptoms Differentiation between a viral URI/rhinosinusitis and ABS is a challenge and can be based upon severity of symptoms as well as length of illness. Symptoms of ABS are typically present and persistent for more than 10 days, without improvement. Continuing illness and worsening of symptoms are identifying features of ABS given most viral URIs gradually resolve within a 10- day timeframe. Other common symptoms include milky/thick nasal discharge, fever, predominantly nocturnal cough, and headache. Other less common symptoms include facial pain, toothache, malodorous breath, and periorbital edema. On physical examination, erythema and edema of the turbinates, as well as reproducible pain over aerated sinuses, are suggestive of ABS EMERGENCY MEDICINE I JANUARY
6 Diagnosis In the acute care setting, diagnosis of ABS should be clinical in nature. Neither imaging nor laboratory work-up is generally required secondary to their poor diagnostic specificity for ABS. The bacteria involved in ABS are similar to those associated with AOM, with S pneumonia, nontypeable H influenza, and M catarrhalis being the predominant organisms Adjuvant Therapy. Additional therapies include nasal irrigation, decongestants, antihistamines, and intranasal steroids; however, there are only anecdotal reports of their efficacy in providing symptom relief. Therefore, there are insufficient evidencebased data to support or refute the role of these adjuvant therapies in treating pediatric patients with ABS. 9,13 Treatment and Management Treatment of ABS is generally recommended once the diagnosis is made, though this is based largely on expert opinion as there are limited RCTs available. 13 However, available studies do show a more rapid improvement in children on antibiotic therapy than those on placebo. 15,16 Antibiotic Therapy. Amoxicillin remains the antimicrobial agent of choice for firstline treatment of uncomplicated ABS forsituations in which antimicrobial resistance is not suspected. In communities with a high prevalence of nonsusceptible S pneumoniae (>10%, including intermediate- and high-level resistance), treatment may be initiated at 80 to 90 mg/kg/d in two divided doses, with a maximum of 2 g per dose. Patients presenting with moderate to severe illness, as well as those who are younger than 2 years, attend childcare, or have recently been treated with an antimicrobial, may receive high-dose amoxicillin-clavulanate as initial therapy given the elevated beta-lactamase production of the common bacteria that cause ABS. Second-line alternatives include azithromycin, cefdinir, and sulfamethoxizoletrimethoprim (Table 1). There are data to suggest higher rates of decreased susceptibility of S pneumonia and H influenza to third-generation cephalosporins, and the addition of clindamycin may be warranted when utilizing those medications. Treatment is recommended for 10 to 14 days, though improvement should be noted within 1 to 3 days ,14-17 Photographee.eu/Shutterstock JANUARY 2017 I EMERGENCY MEDICINE 13
7 PEDIATRIC ENT COMPLAINTS: AN UPDATE Case 2 Resolution The prolonged duration and severity of symptoms (high fever and headache) and the gradual worsening of the clinical course (ie, late-onset fever) in this patient all suggest ABS rather than a simple prolonged URI. The physical examination findings of inflamed turbinates and facial pain further increase the specificity for ABS. The patient was started on oral amoxicillin-clavulanate with planned treatment for 14 days. At discharge, his parents were instructed to followup with the patient s pediatrician in 3 days to ensure a degree of clinical resolution. Case Scenario 3 A 4-year-old boy was presented by his parents for evaluation of a 2-day history of a persistent and unimproved sore throat. The patient s mother indicated that the child s oral T upon returning home earlier from preschool was o F. She further noted that her 17-month-old daughter and 8-yearold son also experienced similar symptoms which had self-resolved. Triage vital signs were: T, o F, orally; BP, HR, and RR were all within normal limits. Oxygen saturation was 100% on room air. On physical examination, the child was noted to have anterior cervical lymph nodes bilaterally and an erythematous oropharynx with exudate noted on both tonsils. There were no cutaneous abnormalities, nasal edema, erythema, or drainage. Based on the clinical examination, the EP was suspicious for SP. Questions to Guide the Work-Up: (1) Is SP diagnosed based on clinical findings alone in this patient s age group? (2) At what age in the pediatric population is it appropriate to perform a rapid streptococcal antigen test? (3) Are there medications other than antibiotics that are beneficial in treating symptomatic SP? Ilike/Shutterstock 14 EMERGENCY MEDICINE I JANUARY
8 Streptococcal Pharyngitis Streptococcal pharyngitis is a clinical condition caused by group A beta-hemolytic S pyogens. This bacterium is responsible for multiple conditions, including pharyngitis, skin infections, poststreptococcal glomerulonephritis, and rheumatic fever, as well as invasive syndromes. (This case focuses solely on SP). Pharyngitis can occur secondary to a viral or bacterial infection, and SP is the most common cause of pediatric bacterial pharyngitis. It is estimated that children aged 5 to 15 years are more commonly diagnosed with SP, although approximately 24% of children younger than age 5 years with pharyngitis symptoms will be ultimately diagnosed with SP. Signs and Symptoms Typical symptoms include fever, pharyngitis, generalized abdominal pain, nausea, vomiting, headache, and absence of viral URI symptoms (eg, cough, nasal discharge). However, younger patients with SP may have clinical findings of prolonged nasal drainage and excoriated nares. Examination findings may include swollen and tender anterior cervical lymph nodes; generalized edema and erythema of the posterior pharynx; tonsillar exudates; and palatal petechiae. Diagnosis Centor Criteria. The Centor criteria were developed to assist practitioners in identifying patients with potential SP. Criteria for patients older than age 15 years include fever, absence of cough, tonsillar exudates, and tender anterior cervical lymphadenopathy. A modified Centor criteria was later established to include children older than age 5 years, with children between ages 5 and 15 years being the fifth variable in the modified score. In general, patients with a score of 4 or 5 (presence of each variable = 1 point) are most likely to test positive for SP on rapid antigen testing (RAT) or culture Swab, Rapid Antigen Testing, and Culture. Swabbing the throat and RAT and/or culture should be performed in most children with suspected SP because the clinical features alone do not reliably discriminate SP from viral pharyngitis. Rapid antigen testing is only specific for group A beta-hemolytic streptococcal species, which is the only streptococcal species that is routinely treated with antibiotics in the setting of acute pharyngitis. It is unlikely for a patient with a score of 0 or 1 to have SP, and several sources suggest neither testing nor treating this cohort, but rather to consider an alternative diagnosis Within the population of children and young adolescents, due to a RAT sensitivity of 70% to 90%, a negative result should always be backed-up by a throat culture, and treatment initiated if results of the culture are later found to be positive. As the current generation of RAT tests have a high specificity, a positive RAT does not necessitate a back-up culture, and treatment is indicated without further investigation. 19,20 Routine RAT is not recommended in children younger than age 3 years as patients in this age group are at low-risk of developing rheumatic fever. One notable exception for these very young children would be if there are siblings in the home with confirmed SP, in which case, RAT should be considered in the clinical context of SP. 21 Adolescents over age 15 years are another cohort with a low likelihood of developing rheumatic fever, though they can develop other poststreptococcal complications, such as glomerulonephritis. The US Centers for Disease Control and Prevention/American Academy of Family Practitioners (AAFP) guidelines suggest that pharyngitis in older adolescents can be approached in a similar fashion to adults, with empiric therapy for a Centor score of 3 or 4, RAT (without the need for follow-up culture) for Centor score of 2, and neither testing nor treating patients with a score of 0 or JANUARY 2017 I EMERGENCY MEDICINE 15
9 PEDIATRIC ENT COMPLAINTS: AN UPDATE Table 2. Recommended Antibiotic Therapy for Streptococcal Pharyngitis Drug Route Dose Maximum Dosage Length of Treatment Penicillin V Oral 250 mg twice a day in patients weighing <27 kg 500 mg twice a day to three times a day in patients weighing >27 kg 10 days Amoxicillin Oral 50 mg/kg/d once a day or divided twice a day 1,000 mg/d 10 days Benzathine penicillin G Intramuscular 600,000 U in patients weighing <27 kg 1,200,000 U in patients weighing >27 kg Once Cephalexin Oral 40 mg/kg/d divided twice a day 1,000 mg/d (500 mg per dose) 10 days Azithromycin Oral 12 mg/kg/d 500 mg/d 5 days (Note: Dosing strategy is different than is typical for this drug) Clindamycin Oral 21 mg/kg/d divided three times a day 900 mg/d (300 mg per dose) 10 days Treatment and Management Streptococcal pharyngitis is treated mainly to prevent the poststreptococcal complications of rheumatic fever, though it will not prevent poststreptococcal glomerulonephritis. Treatment of SP also facilitates resolution of symptoms and return to baseline activities. Antibiotic Therapy. Patients who have a positive RAT or a follow-up throat culture positive for group A streptococcus should be given antibiotics. The gold standard treatment is penicillin V orally for 10 days. Other medication choices include amoxicillin orally for 10 days or a single IM dose of benzathine penicillin G. For penicillinallergic patients, alternative regimens include oral azithromycin, cephalexin, and clindamycin (Table 2) Corticosteroid Therapy. The use of corticosteroids for symptom control of SP in pediatric patients is controversial. Although the Infectious Disease Society of America does not recommend corticosteroid therapy in the treatment of SP, several studies show such therapy (namely dexamethasone), improves pain in children and adolescents diagnosed with SP, but without significant change to the overall disease course. 21,23-26 Case 3 Resolution The patient had a modified Centor criteria score of 4, as well as siblings with similar symptoms. In following current guidelines, the EP performed a RAT and back-up culture. The RAT was negative in the ED, but the back-up culture was subsequently positive, and the child was started on a 10- day course of oral amoxicillin. 16 EMERGENCY MEDICINE I JANUARY
10 Conclusion When evaluating pediatric patients presenting with ENT signs and symptoms such as ear pain and erythema, fever, sore throat, nasal congestion and discharge, a thorough physical examination and history-taking including recent illness of any siblings along with testing when indicated, is essential to guide the diagnosis and determine appropriate treatment and management. In addition to administering antibiotic therapy when such is warranted, the EP should provide appropriate analgesia to manage the patient s pain and assure relief prior to discharge. References 1. Rosenfeld RM, Shin JJ, Schwartz SR, et al. Clinical practice guideline: otitis media with effusion (Update). Otolaryngol Head Neck Surg. 2016;154(1 Suppl):S1-S41. doi: / Acute Otitis Media Guideline Team, Cincinnati Children s Hospital Medical Center. Evidence-based care guideline for medical management of acute otitis media in children 2 months to 13 years of age. 44ae4ffe12a814f4/4eb132d744ae4ffe12a814f7.pdf. August Accessed December 29, Nesbit CE, Powers MC. An evidence-based approach to managing acute otitis media. Pediatr Emerg Med Pract. 2013;10(4):1-26; quiz Lieberthal AS, Carroll AE, Chonmaitree T, et al. The diagnosis and management of acute otitis media. Pediatrics. 2013;131(3):e964-e999. doi: / peds American Academy of Family Physicians; American Academy of Otolaryngology-Head and Neck Surgery; American Academy of Pediatrics Subcommittee on Otitis Media With Effusion. Otitis media with effusion. Pediatrics. 2004;113(5): US Food and Drug Administration Web site. FDA: Use only approved prescription ear drops. ucm htm. Updated July 10, Accessed December 15, Sack F. An evidence based approach to the management of uncomplicated acute otitis media in children. Int Pediatrics. 2005;20(1): Johnson NC, Holger JS. Pediatric acute otitis media: the case for delayed antibiotic treatment. J Emerg Med. 2007;32(3): doi: /j. jemermed Spiro DM, Tay KY, Arnold DH, Dziura JD, Baker MD, Shapiro ED. Wait-and-see prescription for the treatment of acute otitis media: a randomized controlled trial. JAMA. 2006;296(10): doi: / jama Brook I. Management of acute rhinosinusitis in pediatric patients. Pediatr Emerg Med Pract. 2012;9(5): Ferdman RM, Linzer JF Jr. The runny nose in the emergency department: rhinitis and sinusitis. Clin Pediatr Emerg Med. 2007;8(2): Acute Bacterial Sinusitis Guideline Team, Cincinnati Children s Hospital Medical Center: Evidence-based care guideline for medical management of acute bacterial sinusitis in children 1 through 18 years of age. July 7, Accessed December 29, Holt KR, Murdoch Cuenca M, Cuenca PJ, Johnston GM. acute pediatric sinusitis and the 10-day rule. Pediatr Emerg Med Pract. 2006;3(2): American Academy of Pediatrics. Subcommittee on Management of Sinusitis and Committee on Quality Improvement. Clinical practice guideline: management of sinusitis. Pediatrics. 2001;108(3): Wald ER, Nash D, Eickhoff J. Effectiveness of amoxicillin/clavulanate potassium in the treatment of acute bacterial sinusitis in children. Pediatrics. 2009;124(1):9-15. doi: /peds Arroll B, Kenealy T. Are antibiotics effective for acute purulent rhinitis? Systematic review and meta-analysis of placebo controlled randomised trials. BMJ. 2006;333(7562):279. doi: / bmj ae. 17. McQuillan L, Crane LA, Kempe A. Diagnosis and management of acute sinusitis by pediatricians. Pediatrics. 2009;123(2):e193-e Singer JI, Fontanette R. Recognizable and suspected group A beta-hemolytic streptococcal syndromes. Pediatr Emerg Med Rep. 2010;15(11): Weglowski J. An evidence-based approach to the evaluation and treatment of pharyngitis in children. Pediatr Emerg Med Pract. 2011;8(12): Gerber MA, Baltimore RS, Eaton CB, et al. Prevention of rheumatic fever and diagnosis and treatment of acute Streptococcal pharyngitis: a scientific statement from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee of the Council on Cardiovascular Disease in the Young, the Interdisciplinary Council on Functional Genomics and Translational Biology, and the Interdisciplinary Council on Quality of Care and Outcomes Research: endorsed by the American Academy of Pediatrics. Circulation. 2009;119(11): doi: /circula- TIONAHA Shulman ST, Bisno AL, Clegg HW, et al. Clinical practice guideline for the diagnosis and management of group A streptococcal pharyngitis: 2012 update by the Infectious Diseases Society of America. Clin Infect Dis. 2012;55(10): doi: /cid/ cis Clegg HW, Ryan AG, Dallas SD, et al. Treatment of streptococcal pharyngitis with once-daily compared with twice-daily amoxicillin: a noninferiority trial. Pediatr Infect Dis J. 2006;25(9): doi: /01.inf Bulloch B, Kabani A, Tenenbein M. Oral dexamethasone for the treatment of pain in children with acute pharyngitis: a randomized, double-blind, placebocontrolled trial. Ann Emerg Med. 2003;41(5): doi: /mem Niland ML, Bonsu BK, Nuss KE, Goodman DG. A pilot study of 1 versus 3 days of dexamethasone as add-on therapy in children with streptococcal pharyngitis. Pediatr Infect Dis J. 2006;25(6): doi: /01.inf f. 25. Wei JL, Kasperbauer JL, Weaver AL, Boggust AJ. Efficacy of single-dose dexamethasone as adjuvant therapy for acute pharyngitis. Laryngoscope. 2002;112(1): doi: / Hayward G, Thompson M, Heneghan C, Perera R, Del Mar C, Glasziou P. Corticosteroids for pain relief in sore throat: systematic review and meta-analysis. BMJ. 2009;339:b2976. doi: /bmj.b JANUARY 2017 I EMERGENCY MEDICINE 17
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis
 Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
UPPER RESPIRATORY TRACT INFECTIONS. IAP UG Teaching slides
 UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults
 Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
Update on Rhinosinusitis 2013 AAP Guidelines Review
 Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
Upper Respiratory Tract Infections / 42
 Upper Respiratory Tract Infections 1 Upper Respiratory Tract Infections Acute tonsillitispharyngitis Acute otitis media Acute sinusitis Common cold Acute laryngitis Otitis externa Mastoiditis Acute apiglottis
Upper Respiratory Tract Infections 1 Upper Respiratory Tract Infections Acute tonsillitispharyngitis Acute otitis media Acute sinusitis Common cold Acute laryngitis Otitis externa Mastoiditis Acute apiglottis
Choosing an appropriate antimicrobial agent. 3) the spectrum of potential pathogens
 Choosing an appropriate antimicrobial agent Consider: 1) the host 2) the site of infection 3) the spectrum of potential pathogens 4) the likelihood that these pathogens are resistant to antimicrobial agents
Choosing an appropriate antimicrobial agent Consider: 1) the host 2) the site of infection 3) the spectrum of potential pathogens 4) the likelihood that these pathogens are resistant to antimicrobial agents
Clinical Practice Guideline: Tonsillectomy in Children, Baugh et al Otolaryngology Head and Neck Surgery, 2011 J and: 144 (1 supplement) S1 30.
 Pediatric ENT Guidelines Jane Cooper, FNP, CORLN References: Clinical Practice Guideline: Tympanostomy tubes in children, Rosenfeld et al., American Academy of Otolaryngology Head and Neck Surgery Foundation
Pediatric ENT Guidelines Jane Cooper, FNP, CORLN References: Clinical Practice Guideline: Tympanostomy tubes in children, Rosenfeld et al., American Academy of Otolaryngology Head and Neck Surgery Foundation
Respiratory tract infections. Krzysztof Buczkowski
 Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Acute Otitis Media. These podcasts are designed to give medical students an overview of key topics in pediatrics. The
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Acute Otitis Media. These podcasts are designed to give medical students an overview of key topics in pediatrics. The
Definition. Otitis Media with effusion (OME)
 Otitis Media. 1 Dr,wegdan saeed ALFHAL 2 Definition Acute Otitis Media (AOM) acute onset of symptoms, evidence of a middle ear effusion, and signs or symptoms of middle ear inflammation. Otitis Media with
Otitis Media. 1 Dr,wegdan saeed ALFHAL 2 Definition Acute Otitis Media (AOM) acute onset of symptoms, evidence of a middle ear effusion, and signs or symptoms of middle ear inflammation. Otitis Media with
Evelyn A. Kluka, MD FAAP November 30, 2011
 Evelyn A. Kluka, MD FAAP November 30, 2011 > 80% of children will suffer from at least one episode of AOM by 3 years of age 40% will have > 6 recurrences by age 7 years Most common diagnosis for which
Evelyn A. Kluka, MD FAAP November 30, 2011 > 80% of children will suffer from at least one episode of AOM by 3 years of age 40% will have > 6 recurrences by age 7 years Most common diagnosis for which
PAEDIATRIC ACUTE CARE GUIDELINE. Otitis Media
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Otitis Media Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Otitis Media Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in
Upper Respiratory tract Infec1on. Gassem Gohal FAAP FRCPC
 Upper Respiratory tract Infec1on Gassem Gohal FAAP FRCPC Anatomy Contents Sinusitis Common Cold Otitis media pharyngitis Epiglottitis Croup Trachitis Sinuses Sinus development Born with ME ( Maxillary,
Upper Respiratory tract Infec1on Gassem Gohal FAAP FRCPC Anatomy Contents Sinusitis Common Cold Otitis media pharyngitis Epiglottitis Croup Trachitis Sinuses Sinus development Born with ME ( Maxillary,
Upper Respiratory Tract Infections
 Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Diagnosis and Treatment of Respiratory Illness in Children and Adults
 Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
Jimmy's Got Cooties! Common Childhood Infections and How Best to Treat Them
 Jimmy's Got Cooties! Common Childhood Infections and How Best to Treat Them Objectives:! Recognize and manage several infections commonly seen in Pediatric practice! Discuss best practices and current
Jimmy's Got Cooties! Common Childhood Infections and How Best to Treat Them Objectives:! Recognize and manage several infections commonly seen in Pediatric practice! Discuss best practices and current
CAREFUL ANTIBIOTIC USE
 Make promoting appropriate antibiotic use part of your routine clinical practice When parents ask for antibiotics to treat viral infections: PRACTICE TIPS Create an office environment to promote the reduction
Make promoting appropriate antibiotic use part of your routine clinical practice When parents ask for antibiotics to treat viral infections: PRACTICE TIPS Create an office environment to promote the reduction
USAID Health Care Improvement Project. pneumonia) respiratory infections through improved case management (amb/hosp)
 Improvement objective: : decrease morbidity and mortality due to acute upper (rhinitis, sinusitis, pharyngitis) and lower (bronchitis, pneumonia) respiratory infections through improved case management
Improvement objective: : decrease morbidity and mortality due to acute upper (rhinitis, sinusitis, pharyngitis) and lower (bronchitis, pneumonia) respiratory infections through improved case management
I have no disclosures
 Disclosures Streptococcal Pharyngitis: Update and Current Guidelines Richard A. Jacobs, MD, PhD Emeritus Professor of Medicine Division of Infectious Diseases I have no disclosures CID 2012:55;e 86-102
Disclosures Streptococcal Pharyngitis: Update and Current Guidelines Richard A. Jacobs, MD, PhD Emeritus Professor of Medicine Division of Infectious Diseases I have no disclosures CID 2012:55;e 86-102
Background. Background. AAP (2013) Guidelines. Background 4/19/2016
 Disclosure Information for: Amanda Kotowski and Laurie Newton Diagnosis & Management of Pediatric Sinusitis: A Survey of Primary Care, Otolaryngology & Urgent Care Providers Amanda Kotowski, DNP, CPNP
Disclosure Information for: Amanda Kotowski and Laurie Newton Diagnosis & Management of Pediatric Sinusitis: A Survey of Primary Care, Otolaryngology & Urgent Care Providers Amanda Kotowski, DNP, CPNP
SINUSITIS. HAVAS ENT CLINICS Excellence in otolaryngology
 JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
Prefe f rred d t e t rm: : rhi h no n s o inu n s u iti t s
 HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
Five New Clinical Guidelines in Primary Care: What we all need to know. Learning Objectives. Clinical Practice Guidelines
 Five New Clinical Guidelines in Primary Care: What we all need to know Annie Abraham, MSN, RN, FNP-BC Assistant Clinical Professor Texas Woman s University Dallas, TX Learning Objectives Discuss up-to-date
Five New Clinical Guidelines in Primary Care: What we all need to know Annie Abraham, MSN, RN, FNP-BC Assistant Clinical Professor Texas Woman s University Dallas, TX Learning Objectives Discuss up-to-date
Molina Healthcare of Washington, Inc. Guideline for the Judicious use of Antibiotics
 Molina Healthcare of Washington, Inc. Guideline for the Judicious use of Antibiotics The Washington State Clinical Practice Guidelines for the Judicious Use of Antibiotics in URI (Sinusitis, Otitis Media,
Molina Healthcare of Washington, Inc. Guideline for the Judicious use of Antibiotics The Washington State Clinical Practice Guidelines for the Judicious Use of Antibiotics in URI (Sinusitis, Otitis Media,
4/7/13 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC
 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
Diagnosis and Treatment of Respiratory Illness in Children and Adults Guideline
 Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
Streptococcal Pharyngitis
 Streptococcal Pharyngitis Guideline developed by JC Beavers, MD, in collaboration with the ANGELS Team. Last reviewed by JC Beavers, MD on November 2, 2016. Preface Streptococcal pharyngitis (ie, strep
Streptococcal Pharyngitis Guideline developed by JC Beavers, MD, in collaboration with the ANGELS Team. Last reviewed by JC Beavers, MD on November 2, 2016. Preface Streptococcal pharyngitis (ie, strep
Upper Respiratory Tract Infections Masoud Mardani. M. D. MPH, FIDSA
 Upper Respiratory Tract Infections Masoud Mardani. M. D. MPH, FIDSA Professor Of Infectious Diseases Shahid Beheshti Medical University URTI s Sinusitis Acute Otitis Media Pharyngitis Question One: What
Upper Respiratory Tract Infections Masoud Mardani. M. D. MPH, FIDSA Professor Of Infectious Diseases Shahid Beheshti Medical University URTI s Sinusitis Acute Otitis Media Pharyngitis Question One: What
Rhinosinusitis. John Ramey, MD Joseph Russell, MD
 Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Clinical Policy Title: Strep testing
 Clinical Policy Title: Strep testing Clinical Policy Number: 07.01.09 Effective Date: December 1, 2017 Initial Review Date: October 19, 2017 Most Recent Review Date: November 16, 2017 Next Review Date:
Clinical Policy Title: Strep testing Clinical Policy Number: 07.01.09 Effective Date: December 1, 2017 Initial Review Date: October 19, 2017 Most Recent Review Date: November 16, 2017 Next Review Date:
High dose amoxicillin for sinusitis
 High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
Appropriate Antibiotic Prescribing. Frank Romanelli, Pharm.D., MPH, AAHIVP Professor & Associate Dean Paul F. Parker Endowed Professor of Pharmacy
 Appropriate Antibiotic Prescribing Frank Romanelli, Pharm.D., MPH, AAHIVP Professor & Associate Dean Paul F. Parker Endowed Professor of Pharmacy Objectives Discuss CDCs Core Elements of abx stewardship.
Appropriate Antibiotic Prescribing Frank Romanelli, Pharm.D., MPH, AAHIVP Professor & Associate Dean Paul F. Parker Endowed Professor of Pharmacy Objectives Discuss CDCs Core Elements of abx stewardship.
Chronic Sinusitis. Acute Sinusitis. Sinusitis. Anatomy of the Paranasal Sinuses. Sinusitis. Medical Topics - Sinusitis
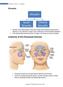 1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
Reducing Antibiotic Use in Common Infections in Family Practice
 Reducing Antibiotic Use in Common Infections in Family Practice W. Rosser Emeritus Professor Department of Family Medicine Queen s University Discussion with Honorary Teachers, University of Hong Kong
Reducing Antibiotic Use in Common Infections in Family Practice W. Rosser Emeritus Professor Department of Family Medicine Queen s University Discussion with Honorary Teachers, University of Hong Kong
Infections of the head, neck, and lower respiratory tract
 Infections of the head, neck, and lower respiratory tract Infections of the upper respiratory tract Common 25% bacteria antibiotics 75% viruses Diagnosis on clinical grounds Nonspecific infections of the
Infections of the head, neck, and lower respiratory tract Infections of the upper respiratory tract Common 25% bacteria antibiotics 75% viruses Diagnosis on clinical grounds Nonspecific infections of the
Clinical Practice Guideline for the Diagnosis and Management of Acute Bacterial Sinusitis in Children Aged 1 to 18 Years
 Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children CLINICAL PRACTICE GUIDELINE Clinical Practice Guideline for the Diagnosis and Management
Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children CLINICAL PRACTICE GUIDELINE Clinical Practice Guideline for the Diagnosis and Management
9/18/2018. Disclosures. Objectives
 Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
COMMON UPPER RESPIRATORY TRACT INFECTIONS IN CHILDREN
 ١ ٢ COMMON UPPER RESPIRATORY TRACT INFECTIONS IN CHILDREN Dr mostafavi SN Pediatric Infectious Disease Department Isfahan University of Medical Sciences Case 1 ٣ An 18 month old infant brought with high
١ ٢ COMMON UPPER RESPIRATORY TRACT INFECTIONS IN CHILDREN Dr mostafavi SN Pediatric Infectious Disease Department Isfahan University of Medical Sciences Case 1 ٣ An 18 month old infant brought with high
Research articles last 5 years- ENT
 Research articles last 5 years- ENT Throats and tonsils Tonsillectomy versus antibiotics in children for recurrent tonsillitis Randomised controlled trial (BMJ May 2007) Tonsillectomy is more beneficial
Research articles last 5 years- ENT Throats and tonsils Tonsillectomy versus antibiotics in children for recurrent tonsillitis Randomised controlled trial (BMJ May 2007) Tonsillectomy is more beneficial
Management of URTI s in Children
 Management of URTI s in Children Robin J Green PhD Antibiotics - Dilemmas for General Practitioners Antibiotic overuse = Resistance Delay in antibiotic use = Mortality Patient expectation Employer expectation
Management of URTI s in Children Robin J Green PhD Antibiotics - Dilemmas for General Practitioners Antibiotic overuse = Resistance Delay in antibiotic use = Mortality Patient expectation Employer expectation
Paediatric ENT problems
 Paediatric ENT problems Ears Otitis media Otitis media with effusion FBs Otitis externa Ruptured TM Nose FBs Allergic rhinitis Septal perforation expistaxis Throat FB Croup Stidor Tonsillitis Paediatric
Paediatric ENT problems Ears Otitis media Otitis media with effusion FBs Otitis externa Ruptured TM Nose FBs Allergic rhinitis Septal perforation expistaxis Throat FB Croup Stidor Tonsillitis Paediatric
Subspecialty Rotation: Otolaryngology
 Subspecialty Rotation: Otolaryngology Faculty: Evelyn Kluka, M.D. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's and other specialists' roles
Subspecialty Rotation: Otolaryngology Faculty: Evelyn Kluka, M.D. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's and other specialists' roles
MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE
 PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
Follow this and additional works at:
 Bond University epublications@bond Faculty of Health Sciences & Medicine Publications Faculty of Health Sciences & Medicine 5-1-2004 Chris Del Mar Bond University, chris_del_mar@bond.edu.au Paul Glasziou
Bond University epublications@bond Faculty of Health Sciences & Medicine Publications Faculty of Health Sciences & Medicine 5-1-2004 Chris Del Mar Bond University, chris_del_mar@bond.edu.au Paul Glasziou
Facilitator s Guide. Prescription Writing/Patient Safety Author: Benjamin Estrada, MD, University of South Alabama. Active Learning Module
 Facilitator s Guide Prescription Writing/Patient Safety Author: Benjamin Estrada, MD, University of South Alabama Active Learning Module Core Concepts In order to master this topic area, students must
Facilitator s Guide Prescription Writing/Patient Safety Author: Benjamin Estrada, MD, University of South Alabama Active Learning Module Core Concepts In order to master this topic area, students must
Statement on the use of delayed prescriptions of antibiotics for infants and children
 Statement on the use of delayed prescriptions of antibiotics for infants and children Endorsed by the Royal College of General Practitioners Background Delayed prescribing (also known as back up prescribing)
Statement on the use of delayed prescriptions of antibiotics for infants and children Endorsed by the Royal College of General Practitioners Background Delayed prescribing (also known as back up prescribing)
The Throat. Image source:
 The Throat Anatomy Image source: http://anatomyforlayla.blogspot.co.za/2007/04/blog-post.html The Throat consists of three parts: 1. The Nasopharynx is the upper part of the throat and it is situated behind
The Throat Anatomy Image source: http://anatomyforlayla.blogspot.co.za/2007/04/blog-post.html The Throat consists of three parts: 1. The Nasopharynx is the upper part of the throat and it is situated behind
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS
 MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
POLICY FOR TREATMENT OF UPPER RESPIRATORY TRACT INFECTIONS
 POLICY F TREATMENT OF UPPER RESPIRATY TRACT INFECTIONS Written by: Dr M Milupi, Consultant Microbiologist Date: July 2013 Approved by: The Drugs & Therapeutics Committee Date: April 2016 Implementation
POLICY F TREATMENT OF UPPER RESPIRATY TRACT INFECTIONS Written by: Dr M Milupi, Consultant Microbiologist Date: July 2013 Approved by: The Drugs & Therapeutics Committee Date: April 2016 Implementation
TENTATIVE DIAGNOSES Based on the information provided so far, what are the potential diagnoses?
 Case Study #4 PEDIATRIC CASE STUDY SCENARIO Mary Jennings has brought her son Joe to your office. Joe is a 6-year old Jordanian male. He presents with the complaint of an itchy red eye. Mary states that
Case Study #4 PEDIATRIC CASE STUDY SCENARIO Mary Jennings has brought her son Joe to your office. Joe is a 6-year old Jordanian male. He presents with the complaint of an itchy red eye. Mary states that
Disclaimer. This is a broad survey and cannot cover all differential diagnoses or each condition in thorough detail
 Objectives Pediatric Infections: Differentiating Benign from Serious Eileen Klein, MD, MPH Rashes Infectious vs non-infectious Viral vs bacterial Respiratory and GI illnesses When do you treat When do
Objectives Pediatric Infections: Differentiating Benign from Serious Eileen Klein, MD, MPH Rashes Infectious vs non-infectious Viral vs bacterial Respiratory and GI illnesses When do you treat When do
ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST
 www.manchesterchildrensent.com ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST A CHILD WITH EARACHE UNCOMPLICATED AOM ACUTE OTITIS MEDIA Acute otitis media
www.manchesterchildrensent.com ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST A CHILD WITH EARACHE UNCOMPLICATED AOM ACUTE OTITIS MEDIA Acute otitis media
AMERICAN ACADEMY OF PEDIATRICS AND AMERICAN ACADEMY OF FAMILY PHYSICIANS. Subcommittee on Management of Acute Otitis Media
 AMERICAN ACADEMY OF PEDIATRICS AND AMERICAN ACADEMY OF FAMILY PHYSICIANS CLINICAL PRACTICE GUIDELINE Subcommittee on Management of Acute Otitis Media Diagnosis and Management of Acute Otitis Media ABSTRACT.
AMERICAN ACADEMY OF PEDIATRICS AND AMERICAN ACADEMY OF FAMILY PHYSICIANS CLINICAL PRACTICE GUIDELINE Subcommittee on Management of Acute Otitis Media Diagnosis and Management of Acute Otitis Media ABSTRACT.
POLICY FOR TREATMENT OF UPPER RESPIRATORY TRACT INFECTIONS
 POLICY F TREATMENT OF UPPER RESPIRATY TRACT INFECTIONS Written by: Dr M Milupi, Consultant Microbiologist Date: June 2018 Approved by: Date: July 2018 The Drugs & Therapeutics Committee Implementation
POLICY F TREATMENT OF UPPER RESPIRATY TRACT INFECTIONS Written by: Dr M Milupi, Consultant Microbiologist Date: June 2018 Approved by: Date: July 2018 The Drugs & Therapeutics Committee Implementation
Welcome to Big Sky Country. Pediatrics Infectious disease update. Todd TwogoodMD
 Welcome to Big Sky Country Pediatrics Infectious disease update Todd TwogoodMD My kid is always sick!! We have to deal with parents Snotty nose kids Average number of colds in children from Oct to March
Welcome to Big Sky Country Pediatrics Infectious disease update Todd TwogoodMD My kid is always sick!! We have to deal with parents Snotty nose kids Average number of colds in children from Oct to March
My kid is always sick!!
 Welcome to Big Sky Country My kid is always sick!! Pediatrics Infectious disease update Todd Twogood MD We have to deal with parents Snotty nose kids Average number of colds in children from Oct to March
Welcome to Big Sky Country My kid is always sick!! Pediatrics Infectious disease update Todd Twogood MD We have to deal with parents Snotty nose kids Average number of colds in children from Oct to March
Dine & Learn - Victoria May 2015 Otolaryngology
 Dine & Learn - Victoria May 2015 Otolaryngology Allergic rhinitis Allergic rhinitis guidelines (Otolaryngology Head and Neck Surgery 2015) Diagnosis: history: allergen + either nasal congestion or runny
Dine & Learn - Victoria May 2015 Otolaryngology Allergic rhinitis Allergic rhinitis guidelines (Otolaryngology Head and Neck Surgery 2015) Diagnosis: history: allergen + either nasal congestion or runny
BIOS222 TUTORIAL ACTIVITY SESSION 1
 BIOS222 TUTORIAL ACTIVITY SESSION 1 Instructions: The Tutorial activities are designed to help you practice the concepts learned in the lecture. Read the following case studies and answer the questions
BIOS222 TUTORIAL ACTIVITY SESSION 1 Instructions: The Tutorial activities are designed to help you practice the concepts learned in the lecture. Read the following case studies and answer the questions
Journal of Pediatric Sciences
 Journal of Pediatric Sciences Buccal Cellulitis in 3 Infants Martin W Stallings Journal of Pediatric Sciences 2016;8:e252 http://dx.doi.org/10.17334/jps.78460 How to cite this article: Stallings MW. Buccal
Journal of Pediatric Sciences Buccal Cellulitis in 3 Infants Martin W Stallings Journal of Pediatric Sciences 2016;8:e252 http://dx.doi.org/10.17334/jps.78460 How to cite this article: Stallings MW. Buccal
Clarithromycin versus penicillin in the treatment of streptococcal pharyngitis
 Journal of Antimicrobial Chemotherapy (1991) 27, Suppl. A, 67-74 Clarithromycin versus penicillin in the treatment of streptococcal pharyngitis Joseph H. Levenstein* South Africa Academy of Family Practice,
Journal of Antimicrobial Chemotherapy (1991) 27, Suppl. A, 67-74 Clarithromycin versus penicillin in the treatment of streptococcal pharyngitis Joseph H. Levenstein* South Africa Academy of Family Practice,
Clindamycin strep throat dose
 Clindamycin strep throat dose User Reviews for Clindamycin. Also known as: Cleocin, Cleocin HCl, Cleocin Pediatric, Cleocin Phosphate, Cleocin Phosphate ADD-Vantage. The following information is. 1 Answer
Clindamycin strep throat dose User Reviews for Clindamycin. Also known as: Cleocin, Cleocin HCl, Cleocin Pediatric, Cleocin Phosphate, Cleocin Phosphate ADD-Vantage. The following information is. 1 Answer
Recognize the broad impact of hearing impairment on child and family, including social, psychological, educational and financial consequences.
 Otolaryngology Note: The goals and objectives described in detail below are not meant to be completed in a single one month block rotation but are meant to be cumulative, culminating in a thorough and
Otolaryngology Note: The goals and objectives described in detail below are not meant to be completed in a single one month block rotation but are meant to be cumulative, culminating in a thorough and
Acute Bacterial Sinusitis: The latest treatment recommendations. Objectives Having completed the learning activities, the participant will be able to:
 Acute Bacterial Sinusitis: The latest treatment recommendations Presented by: Monica Tombasco, MS, MSNA, FNP-BC, CRNA Senior Lecturer Fitzgerald Health Education Associates, Inc., North Andover, MA Emergency
Acute Bacterial Sinusitis: The latest treatment recommendations Presented by: Monica Tombasco, MS, MSNA, FNP-BC, CRNA Senior Lecturer Fitzgerald Health Education Associates, Inc., North Andover, MA Emergency
Supplementary Online Content
 Supplementary Online Content de la Poza Abad M, Mas Dalmau G, Moreno Bakedano M, et al; Delayed Antibiotic Prescription (DAP) Group. Prescription strategies in acute uncomplicated respiratory infections:
Supplementary Online Content de la Poza Abad M, Mas Dalmau G, Moreno Bakedano M, et al; Delayed Antibiotic Prescription (DAP) Group. Prescription strategies in acute uncomplicated respiratory infections:
Infectious diseases Dr n. med. Agnieszka Topczewska-Cabanek
 Infectious diseases Dr n. med. Agnieszka Topczewska-Cabanek Viral: Exanthema subitum (Roseaola infantum) Herpetic stomatitis Measles Rubella Chickenpox Erythema infectious (5th Disease, Slapped cheec disease)
Infectious diseases Dr n. med. Agnieszka Topczewska-Cabanek Viral: Exanthema subitum (Roseaola infantum) Herpetic stomatitis Measles Rubella Chickenpox Erythema infectious (5th Disease, Slapped cheec disease)
ANTIBIOTICS ACUTE RHINOSINUSITIS IN CHILDREN
 MARCH 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
MARCH 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
Optimizing the Management of Upper Respiratory Tract Infections.
 Optimizing the Management of Upper Respiratory Tract Infections. Tania Sih Introduction Until recently, physicians placed very high value the patient s history, and and their clinical assessment. In addition
Optimizing the Management of Upper Respiratory Tract Infections. Tania Sih Introduction Until recently, physicians placed very high value the patient s history, and and their clinical assessment. In addition
Current approaches to the treatment of URTIs in children
 Current approaches to the treatment of URTIs in children SPL Ed Clarke PhD, MRCPCH and Adam Finn MA, PhD, FRCP, FRCPCH Our series Prescribing in children gives practical advice on the management of childhood
Current approaches to the treatment of URTIs in children SPL Ed Clarke PhD, MRCPCH and Adam Finn MA, PhD, FRCP, FRCPCH Our series Prescribing in children gives practical advice on the management of childhood
Respiratory Infections
 Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
General Medical Concerns
 General Medical Concerns General Medical Concerns Fred Reifsteck MD Head Team Physician University of Georgia Missed Time: school, work, practice, games Decreased Performance Physical/ Mental stress: New
General Medical Concerns General Medical Concerns Fred Reifsteck MD Head Team Physician University of Georgia Missed Time: school, work, practice, games Decreased Performance Physical/ Mental stress: New
Should we treat strep pharyngitis with antibiotics? Paul Page Oct 10/17
 Should we treat strep pharyngitis with antibiotics? Paul Page Oct 10/17 Guidelines Uptodate: Antimicrobial therapy is warranted for patients with symptomatic pharyngitis if the presence of group A streptococci
Should we treat strep pharyngitis with antibiotics? Paul Page Oct 10/17 Guidelines Uptodate: Antimicrobial therapy is warranted for patients with symptomatic pharyngitis if the presence of group A streptococci
NECK MASS. Clinical history and examination: Document detail history of mass. Imaging: US or CT of neck
 ENT ENT Referral Referral Guidelines Guidelines Austin Health ENT Clinic holds fortnightly multidisciplinary meetings with Plastics/ Maxillary Facial and Oncology units to discuss and plan the treatment
ENT ENT Referral Referral Guidelines Guidelines Austin Health ENT Clinic holds fortnightly multidisciplinary meetings with Plastics/ Maxillary Facial and Oncology units to discuss and plan the treatment
Respiratory System Virology
 Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
Common ENT Presentations
 Common ENT Presentations MD, BScMed, FRCSC Head Section of Otolaryngology St. Boniface Hospital Winnipeg, Manitoba, Canada Assistant Professor Department of Otolaryngology University of Manitoba Winnipeg,
Common ENT Presentations MD, BScMed, FRCSC Head Section of Otolaryngology St. Boniface Hospital Winnipeg, Manitoba, Canada Assistant Professor Department of Otolaryngology University of Manitoba Winnipeg,
Comparative Efficacy and Safety Evaluation of Cefaclor VS Amoxycillin + Clavulanate in Children with Acute Otitis Media (AOM)
 Special Article Comparative Efficacy and Safety Evaluation of Cefaclor VS Amoxycillin + Clavulanate in Children with Acute Otitis Media (AOM) Mukesh Aggarwal, Ramanuj Sinha 1, M. Vasudeva Murali 2, Prita
Special Article Comparative Efficacy and Safety Evaluation of Cefaclor VS Amoxycillin + Clavulanate in Children with Acute Otitis Media (AOM) Mukesh Aggarwal, Ramanuj Sinha 1, M. Vasudeva Murali 2, Prita
Current Trend in URTI
 Current Trend in URTI Dr Chow Chun Kuen Specialist in Otorhinolaryngology Upper respiratory tract infection Nonspecific Most common cause of physician visits & sick leaves Acute infection of noes, sinuses,
Current Trend in URTI Dr Chow Chun Kuen Specialist in Otorhinolaryngology Upper respiratory tract infection Nonspecific Most common cause of physician visits & sick leaves Acute infection of noes, sinuses,
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Otolaryngology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Otolaryngology 1. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Otolaryngology 1. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's
Sinusitis in Adults UP TO DATE
 Sinusitis in Adults UP TO DATE Acute sinusitis and rhinosinusitis in adults: Treatment Authors Peter H Hwang, MD Anne Getz, MD Section Editors Daniel G Deschler, MD, FACS Stephen B Calderwood, MD Deputy
Sinusitis in Adults UP TO DATE Acute sinusitis and rhinosinusitis in adults: Treatment Authors Peter H Hwang, MD Anne Getz, MD Section Editors Daniel G Deschler, MD, FACS Stephen B Calderwood, MD Deputy
ENT Referral Guidelines
 ENT Referral Guidelines Austin Health ENT Clinic holds fortnightly multidisciplinary meetings with Plastics/ Maxillary Facial and Oncology units to discuss and plan the treatment of patients with cancerous
ENT Referral Guidelines Austin Health ENT Clinic holds fortnightly multidisciplinary meetings with Plastics/ Maxillary Facial and Oncology units to discuss and plan the treatment of patients with cancerous
ADULT ONSET ACUTE OTITIS MEDIA - A PRELIMINARY REPORT Mukta Pagrani 1, Abhinav Srivastava 2, Chander Mohan 3
 ADULT ONSET ACUTE OTITIS MEDIA - A PRELIMINARY REPORT Mukta Pagrani 1, Abhinav Srivastava 2, Chander Mohan 3 HOW TO CITE THIS ARTICLE: Mukta Pagrani, Abhinav Srivastava, Chander Mohan. Adult Onset Acute
ADULT ONSET ACUTE OTITIS MEDIA - A PRELIMINARY REPORT Mukta Pagrani 1, Abhinav Srivastava 2, Chander Mohan 3 HOW TO CITE THIS ARTICLE: Mukta Pagrani, Abhinav Srivastava, Chander Mohan. Adult Onset Acute
Alabama Medicaid Pharmacist
 Published Quarterly by Health Information Designs, LLC, Summer 2013 edition A Service of Alabama Medicaid PDL Update Effective July 1, 2013, the Alabama Medicaid Agency will update the Preferred Drug List
Published Quarterly by Health Information Designs, LLC, Summer 2013 edition A Service of Alabama Medicaid PDL Update Effective July 1, 2013, the Alabama Medicaid Agency will update the Preferred Drug List
Guideline Review. Clinical Practice Guideline on the Diagnosis and Management of Acute Otitis Media BCC LAM, YC TSAO, Y HUI.
 HK J Paediatr (new series) 2006;11:76-83 Guideline Review Clinical Practice Guideline on the Diagnosis and Management of Acute Otitis Media BCC LAM, YC TSAO, Y HUI Introduction Acute otitis media is a
HK J Paediatr (new series) 2006;11:76-83 Guideline Review Clinical Practice Guideline on the Diagnosis and Management of Acute Otitis Media BCC LAM, YC TSAO, Y HUI Introduction Acute otitis media is a
Nursing care for children with respiratory dysfunction
 Nursing care for children with respiratory dysfunction 1 Lung Development Specific Immunity to Respiratory Infection Secretory IgA in mucosal immunity IgG in systemic immunity Risk Factors Associated with
Nursing care for children with respiratory dysfunction 1 Lung Development Specific Immunity to Respiratory Infection Secretory IgA in mucosal immunity IgG in systemic immunity Risk Factors Associated with
Evidence-based Strategies to Avoid Prescribing Unnecessary Antibiotics
 Evidence-based Strategies to Avoid Prescribing Unnecessary Antibiotics Robert Redwood MD, MPH Emergency & Preventive Medicine Physician June 11, 2018. WHA Journal Club #2 Conflict of Interest Disclosure
Evidence-based Strategies to Avoid Prescribing Unnecessary Antibiotics Robert Redwood MD, MPH Emergency & Preventive Medicine Physician June 11, 2018. WHA Journal Club #2 Conflict of Interest Disclosure
Persistent Obstructive Sleep Apnea After Tonsillectomy. Learning Objectives. Mary Frances Musso, DO Pediatric Otolaryngology
 Persistent Obstructive Sleep Apnea After Tonsillectomy Mary Frances Musso, DO Pediatric Otolaryngology Learning Objectives Recognize indications for tonsillectomy List patients at risk for persistent OSA
Persistent Obstructive Sleep Apnea After Tonsillectomy Mary Frances Musso, DO Pediatric Otolaryngology Learning Objectives Recognize indications for tonsillectomy List patients at risk for persistent OSA
Rheumatic Fever And Post-streptococcal Reactive Arthritis
 www.printo.it/pediatric-rheumatology/gb/intro Rheumatic Fever And Post-streptococcal Reactive Arthritis Version of 2016 1. WHAT IS RHEUMATIC FEVER 1.1 What is it? Rheumatic fever is a disease caused by
www.printo.it/pediatric-rheumatology/gb/intro Rheumatic Fever And Post-streptococcal Reactive Arthritis Version of 2016 1. WHAT IS RHEUMATIC FEVER 1.1 What is it? Rheumatic fever is a disease caused by
Upper Respiratory Infections. Mehreen Arshad, MD Assistant Professor Pediatric Infectious Diseases Duke University
 Upper Respiratory Infections Mehreen Arshad, MD Assistant Professor Pediatric Infectious Diseases Duke University Disclosures None Objectives Know the common age- and season-specific causes of pharyngitis
Upper Respiratory Infections Mehreen Arshad, MD Assistant Professor Pediatric Infectious Diseases Duke University Disclosures None Objectives Know the common age- and season-specific causes of pharyngitis
Overview of Reviews The Cochrane Library and the Treatment of Sore Throat in Children and Adolescents: An Overview of Reviews
 EVIDENCE-BASED CHILD HEALTH: A COCHRANE REVIEW JOURNAL Evid.-Based Child Health 6: 810 823 (2011) Published online in Wiley Online Library (http://www.evidence-basedchildhealth.com). Overview of Reviews
EVIDENCE-BASED CHILD HEALTH: A COCHRANE REVIEW JOURNAL Evid.-Based Child Health 6: 810 823 (2011) Published online in Wiley Online Library (http://www.evidence-basedchildhealth.com). Overview of Reviews
Antibiotic Use in the Outpatient Setting. Ryan Bariola, MD FIDSA Visi4ng Clinical Associate Professor of Medicine
 Antibiotic Use in the Outpatient Setting Ryan Bariola, MD FIDSA Visi4ng Clinical Associate Professor of Medicine Nothing to disclose Disclosures Case 43 year old pa4ent schedules appointment for cough
Antibiotic Use in the Outpatient Setting Ryan Bariola, MD FIDSA Visi4ng Clinical Associate Professor of Medicine Nothing to disclose Disclosures Case 43 year old pa4ent schedules appointment for cough
The Diagnosis and Management of Acute Otitis Media
 Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children CLINICAL PRACTICE GUIDELINE The Diagnosis and Management of Acute Otitis Media abstract
Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children CLINICAL PRACTICE GUIDELINE The Diagnosis and Management of Acute Otitis Media abstract
Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief.
 Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
Swedish guidelines for the treatment of rhinosinusitis, pharyngotonsillitis and acute media otitis in children.
 Swedish guidelines for the treatment of rhinosinusitis, pharyngotonsillitis and acute media otitis in children. The guidelines are produced by STRAMA in collaboration with the Swedish Medical Products
Swedish guidelines for the treatment of rhinosinusitis, pharyngotonsillitis and acute media otitis in children. The guidelines are produced by STRAMA in collaboration with the Swedish Medical Products
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #331: Adult Sinusitis: Antibiotic Prescribed for Acute Viral Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #331: Adult Sinusitis: Antibiotic Prescribed for Acute Viral Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
DIFFICULT-TO-TREAT CHRONIC
 MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
UPPER RESPIRATORY TRACT INFECTION
 UPPER RESPIRATORY TRACT INFECTION OVERVIEW To learn the epidemiology and various clinical presentation of URT To identify the common etiological agents causing these syndromes To study the laboratory diagnosis
UPPER RESPIRATORY TRACT INFECTION OVERVIEW To learn the epidemiology and various clinical presentation of URT To identify the common etiological agents causing these syndromes To study the laboratory diagnosis
2019 HPN Provider Summary Guide St. Rose Parkway, Suite Smoke Ranch Road Henderson, NV Las Vegas, NV 89128
 12.5 EAR NOSE AND THROAT REFERRAL GUIDELINES Contracted Group: Ear Nose and Throat Consultants (ENTC) For Appointments: Telephone Number: (702) 792-6700 Fax: (702) 792-7198 Locations: 3195 St. Rose Parkway,
12.5 EAR NOSE AND THROAT REFERRAL GUIDELINES Contracted Group: Ear Nose and Throat Consultants (ENTC) For Appointments: Telephone Number: (702) 792-6700 Fax: (702) 792-7198 Locations: 3195 St. Rose Parkway,
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations
 White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
EDUCATIONAL COMMENTARY THROAT CULTURES LEARNING OUTCOMES. Upon completion of this exercise, the participant should be able to:
 EDUCATIONAL COMMENTARY THROAT CULTURES LEARNING OUTCOMES Upon completion of this exercise, the participant should be able to: distinguish three types of hemolysis produced by bacterial colonies. discuss
EDUCATIONAL COMMENTARY THROAT CULTURES LEARNING OUTCOMES Upon completion of this exercise, the participant should be able to: distinguish three types of hemolysis produced by bacterial colonies. discuss
