Occipital Neuromodulation: Ultrasound Guidance for Peripheral Nerve Stimulator Implantation
|
|
|
- Scott Chase
- 5 years ago
- Views:
Transcription
1 papr_ CLINICAL REPORT Occipital Neuromodulation: Ultrasound Guidance for Peripheral Nerve Stimulator Implantation Jason S. Eldrige, MD*; Jon B. Obray, MD*, ; Matthew J. Pingree, MD*; Bryan C. Hoelzer, MD* *Division of Pain Medicine, Department of Anesthesiology, Mayo Clinic, Rochester, Minnesota; Intermountain Southwest Spine and Pain Center, St. George, Utah, U.S.A. Address correspondence and reprint requests to: Bryan C. Hoelzer, MD, Division of Pain Medicine, Department of Anesthesiology, Mayo Clinic, Charlton 1-145, Rochester, MN 55905, U.S.A. hoelzer.bryan@ mayo.edu. Submitted: September 15, 2009; Revision accepted: February 13, 2010 DOI /j x 2010 The Authors Pain Practice 2010 World Institute of Pain, /10/$15.00 Pain Practice, Volume 10, Issue 6, Abstract: We report a case of chronic left-sided occipital neuralgia in a 21-year old female patient. The patient in question suffered from chronic greater occipital neuralgia for a duration of many years, which had been refractory to other conservative medical management strategies. Blockade of the greater occipital nerve with local anesthetic was consistently useful in attenuating the patient s pain, though the effects were always short lived. Consequently, a successful trial of greater occipital nerve stimulation was undertaken. Compared with spinal cord stimulation, peripheral nerve stimulation devices are often more difficult to precisely place given limited ability to visualize soft tissues with traditional fluoroscopic guidance. Additionally, there are anatomic subtleties relevant to the greater occipital nerve that potentially complicate stimulator lead placement, both from the standpoint of optimal neuromodulation efficacy and maximum safety. Ultrasound technology is a maturing imaging modality that allows soft tissue visualization and is consequently useful in addressing each of these aforementioned concerns. The specific use of high-frequency ultrasound guidance for this procedure simplified the initial device placement and allowed proper visualization of soft tissue structures, which facilitates precise device deployment. Additionally, the ability to identify relevant vascular structures may further increase the safety of stimulator lead placement. The potential advantages of ultrasoundaugmented procedural techniques, specifically as they pertain to occipital stimulator lead placement, are discussed with particular emphasis on potentially decreasing intraoperative and postoperative complications while optimizing stimulation efficacy. Key Words: occipital neuralgia, occipital nerve stimulation, neuromodulation, ultrasound guidance, peripheral nerve stimulation, neuropathic pain INTRODUCTION Chronic occipital pain, from a variety of causes, is a debilitating condition that poses significant challenges for patients. Symptomatology commonly manifests itself as pain that is lancinating in character, with paroxysmal exacerbations that are distributed from the internuchal line (between occipital protuberance and mastoid process) with radiations around the hemicranium up to the supraorbital ridge in some instances. 1 3 However, significant variability in clinical presentation
2 Occipital Neuromodulation 581 does exist. The overall incidence of occipital neuralgia is unknown, though the available data suggests that it affects men and women with equal frequency. 4 Some studies have indicated that up to 48% of patients previously diagnosed with migraine headache may, in fact, have symptoms chiefly attributable to irritation of the occipital nerve. 4 6 Conservative medical management reported in the literature includes nonsteroidal anti-inflammatory drugs, opioids, nerve membrane stabilizers, transcutaneus electrical nerve stimulation, occipital nerve block (with local 1 steroid), Botox, and acupuncture. A significant number of patients, however, prove refractory to medical management and require more invasive therapeutic intervention. Peripheral nerve stimulation, with percutaneous placement of electrodes, has been well described in case series as a promising therapy for occipital neuralgia refractory to more conservative therapies. 7 9 Several mechanisms of action have been proposed, perhaps most interesting are the physiologic interconnections of occipital nerve afferents with the trigeminal nerve via the trigeminal nucleus caudalis. 10,11 A more thorough discussion of mechanisms of action is, however, outside the scope of our intended discussion. While the precise therapeutic mechanism is yet to be determined, there is a growing body of literature supporting the clinical usefulness of occipital nerve stimulation (ONS) for refractory occipital neuralgia. Coupled with the debilitating nature of occipital neuralgia, ONS therapy is certainly a compelling emerging therapy. Traditionally, percutaneous placement for peripheral nerve stimulating devices has followed techniques that rely upon external anatomic landmarks, clinical knowledge of normal anatomy, and supplementation (where possible) with fluoroscopy. The use of ultrasound guidance for the placement of ONS is a relatively novel approach to placement, which offers several advantages over the traditional techniques. 12 Namely, ultrasound visualization allows real-time imaging of both needle and the surrounding soft tissue structures during placement. This may enable the proceduralist to avoid unnecessary stimulation and/or trauma to arterial, muscular, and fascial structures, which often leads to increased patient morbidity and/or compromises the therapeutic success of the intervention. 13,14 CASE PRESENTATION A 21-year old female suffering with chronic occipital headache pain for many years, presented to the pain clinic for further therapeutic options. Pertinent past medical history included Sydenham s chorea (movement disorder involving bilateral upper extremity tremor), remote history of migraine headaches, and left-sided occipital headache of 5-year duration. Pain intensity was described as 7 9/10, and the frequency of symptoms was continuous without obvious precipitating, exacerbating, or attenuating factors. The patient had visited numerous academic medical centers, and received several exhaustive medical workups prior to her initial presentation at our institution. Although the patient s movement disorder had been satisfactorily treated with clonazepam, the leftsided occipital headaches proved refractory to conservative medical management. Various medical therapies that included diverse traditional pharmacotherapies, physical therapy and exercise, and instruction in several biobehavioral pain management strategies (biofeedback, relaxation, stress management), were unsuccessful in ameliorating the occipital neuralgia. In addition, the patient underwent thorough radiographic imaging which did identify a left-sided arachnoid cyst behind the central sulcus. This structural feature was thought not to be a contributing factor to the patient s pain complaints, and remained stable/unchanged with serial follow-up imaging throughout her treatment regimen. Despite the aforementioned interventions, only occipital nerve block (with local anesthetic and steroid) was helpful in providing significant relief on a consistent basis, although these beneficial effects were limited in duration. Left-sided greater occipital nerve blockade, with 0.5% bupivacaine and 40 mg of triamcinolone, was consistently successful in reducing the patient s pain (near complete resolution). Initially, the duration of the effect of occipital nerve block was up to 8 months. With repeated blockade, however, the duration of the therapeutic effect became progressively shorter and eventually became much less effective over time. Ultimately, the patient was receiving only 1 2 weeks of relief from occipital nerve block. Pulsed radiofrequency of the greater occipital nerve was trialed upon one occasion without discernable benefit. After approximately 4 years of the aforementioned therapy, the patient sought medical advice regarding interventional therapies that may offer longer lasting relief. Based upon this desire, and the concern over sequelae associated with longterm steroid use, an interventional pain physician consulted with the patient. Occipital nerve stimulation trial was discussed as an option, and the patient was deemed to be an appropriate candidate (no contributing
3 582 eldrige et al. Figure 1. Ultrasound image of soft tissue structures during occipital nerve stimulator placement. Visualizing relevant tissues aid in assessment of appropriate depth of lead placement and avoidance of muscle stimulation. Note: The paracervical musculature represents the following at this cervical level: Semispinalis capitis, Rectus capitis, and Obliquus capitis in order of superficial to deep. Figure 2. Ultrasound-assisted soft tissue visualization during occipital nerve stimulator needle placement. Note that deployed electrode is positioned at the level of trapezial aponeurosis and superficial to the paracervical musculature. Though not individually identified on the ultrasound image, the paracervical musculature represents the following at this cervical level: Semispinalis capitis, Rectus capitis, and Obliquus capitis in order of superficial to deep. psychosocial issues, realistic expectations, sincere desire to fully participate in her therapy). After informed consent the patient was taken to the operative suite and was placed in the prone position. Monitored anesthesia care was initiated without difficulty. Fluoroscopy was used to identify the C1 vertebral body, which was marked with a skin maker. The skin was then cleansed and draped in a sterile fashion. Lidocaine 1% with 0.5% bupivacaine mixed in a 1:1 ratio with 1:200,000 epinephrine were used to anesthetize the skin and subcutaneous tissues. A linear 12 MHz ultrasound probe (highest frequency available on the equipment used) in a sterile sheath was used to examine the occipital and suboccipital areas. Subcutaneous tissue and paracervical muscle layers were identified (Figure 1). A 14-gauge Tuohy style needle (Boston Scientific Neuromodulation, Valencia, CA, USA) was then advanced under ultrasound guidance ensuring adequate depth without intramuscular placement (Figure 2). Next, an 8-contact electrode was advanced to the end of the Tuohy needle, and the needle subsequently removed, leaving the stimulating lead placed deep to the subcutaneous tissue but superficial to the paracervical muscles. Fluoroscopy was used to confirm lead placement over the C1 vertebral body as previously described. 5,8 (Figure 3) A pulse generator was then connected, and satisfactory impedance was confirmed. Appropriate paresthesia coverage was obtained in the suboccipital Figure 3. Postprocedural confirmation of appropriate leftsided lead placement using traditional boney landmarks under fluoroscopy. Left-sided lead is positioned just cephalad to the superior margin of the C1 arch, approximately 2 cm inferior to the nuchal line. and occipital area, in the normal anatomic distribution of the greater and lesser occipital nerves (ie, classical hemicranial pattern). Notably, this stimulation occurred without unintended muscle stimulation. The electrode
4 Occipital Neuromodulation 583 Figure 4. Occipitocervical anatomy, dissected views. The greater occipital nerve travels between the semispinalis capitis muscle and the obliquus capitis inferior, prior to penetrating the former and emerging through the trapezius muscle aponeurosis and/or semispinalis capitis fiber just inferior to the intermastoid line. Note that the pictured leads are for context only; final lead position is fully subcutaneous, overlying the trapezial aponeuronis, typically at the level of the C1 2 interface or overlying the C1 arch and oriented parallel to the intermastoid line. was consequently anchored to the skin after which fluoroscopy was used to confirm good medial to lateral electrode orientation and to serve as a reference if the trail was deemed successful. The patient experienced greater than 50% reduction in pain intensity immediately upon initiation of stimulation. The trial lasted 5 days, with the patient reporting a 60% reduction in pain intensity along with significant improvement in quality of life indicators. At 5-day postimplant follow-up, the patient related a consistent pain intensity reduction of 60% along with significant improvement in her quality of life and ability to perform daily activities. Based upon this unmitigated successful reduction in symptoms, permanent occipital nerve stimulator implantation was scheduled and performed in a similar fashion. Post-implant follow-up at 5 months
5 584 eldrige et al. continues to show consistent, significant relief of the patient s left-sided occipital neuralgia symptoms without any discernible device-related complications. DISCUSSION The greater occipital nerve (GON) is derived from contributions from the dorsal rami of the C2 and C3 spinal nerves. Its anatomic course ascends cephalad superficial to the obliquus capitis inferior and deep to the semispinalis capitis muscle. 1 3 After traversing the semispinalis capitis muscle and piercing the aponeurosis of the trapezius muscle (TMA), the GON travels parallel and slightly medial to the path of the occipital artery as it branches further to supply the occipital scalp integument (Figure 4). 1 3 Percutaneous surgical approaches for stimulation have typically relied upon external anatomic landmarks such as the occipital protuberance and the mastoid process to approximate the lie of the GON in relation to occipital artery pulsation. Based upon these external landmarks, stimulating electrodes are placed superficially in the subcutaneous plane and oriented perp endicular to the course of the nerve. Supplemental fluoroscopic visualization (PA orientation) confirms the transverse path of the needle/electrode lead relative to the underlying calvarium and C1 vertebra. 5,11,14 Limitations of this approach include an inability to see soft tissue anatomy (such as nerve, artery, muscle, and fascia), which makes precise placement (especially in regards to appropriate depth) more challenging. As demonstrated with the included ultrasound images, we were clearly able to identify the soft tissue structures of the sub-occipital regions. Subsequently, we were able to precisely place the needle in the connective tissue plane between the underlying paravertebral muscle and overlying subcutaneous fat, oriented just cephalad of the superior margin of the C1 arch and approximately 2 cm inferior to the nuchal line (Figure 5). The procedural needle tip can be clearly visualized at it traverses the subcutaneous plane immediately superficial to the trapezius muscle aponeurosis (TMA) and semispinalis capitus fibers. This enabled us to avoid traumatizing paravertebral muscle, which may have complicated the trial in terms of decrease efficacy and increased morbidity. Traditional nonguided approaches to ONS are suboptimal since they may lead to painful muscle stimulation and inefficient electrical coverage if the depth of lead implantation is inadequate. Additionally, we hypothesize that the incidence of lead tip erosion, which is partially related to depth of lead placement, will likewise decrease with ultrasonic confirmation of specific tissue planes. 15 The precise depth of implantation is immediately confirmed with ultrasonography, which may enable better optimization of stimulation parameters during programming. Ultrasound visualization allows real-time imaging of both needle and soft-tissue during placement and enables the proceduralist to avoid unnecessary stimulation and/or trauma to adjacent muscular and fascial Figure 5. Occipitocervical axial view schematic. Schematic axial representation of the relevant soft tissue structures which are reliably seen with ultrasound-guided placement of an occipital nerve stimulator lead. Note that final needle placement is superficial to or in the trapezius aponeurosis, thus, avoiding trauma to the underlying muscle.
6 Occipital Neuromodulation 585 structures. Limiting the invasiveness and potential unintended damage to surrounding structures are worthy goals for any interventional procedure. Additionally, unnecessary trauma to the muscle may lead to failed or equivocal results of occipital nerve stimulation trials. Reported cases of lead tip erosion can also likely be attenuated by intra-operative ultrasound utilization. The wide availability and relative low-cost of ultrasound technology should reduce barriers to its use in assisting with placement of occipital stimulator devices. Along with a comprehensive understanding of relevant anatomy, real-time ultrasound guidance for precise stimulation lead placement may offer significant advantages for both treatment efficacy and safety. Further study is necessary to corroborate these assertions, and to further identify areas for procedural enhancement. REFERENCES 1. Bogduk N. The anatomy of occipital neuralgia. Clin Exp Neurol. 1981;17: Loukas M, El-Sedfy A, Tubbs RS, et al. Identification of greater occipital nerve landmarks for the treatment of occipital neuralgia. Folia Morphol (Warsz). 2006;65: Natsis K, Baraliakos X, Appell HJ, Tsikaras P, Gigis I, Koebke J. The course of the greater occipital nerve in the suboccipital region: a proposal for setting landmarks for local anesthesia in patients with occipital neuralgia. Clin Anat. 2006;19: Anthony M. Headache and the greater occipital nerve. Clin Neurol Neurosurg. 1992;94: Oh MY, Ortega J, Bellotte JB, Whiting DM, Alo K. Peripheral nerve stimulation for the treatment of occipital neuralgia and transformed migraine using a C1-2-3 subcutaneous paddle style electrode: a technical report. Neuromodulation. 2004;7: Schwedt TJ, Dodick DW, Hentz J, Trentman TL, Zimmerman RS. Occipital nerve stimulation for chronic headache long-term safety and efficacy. Cephalalgia. 2007; 27: Jasper JF, Hayek SM. Implanted occipital nerve stimulators. Pain Physician. 2008;11: Weiner RL, Reed KL. Peripheral neurostimulation for control of intractable occipital neuralgia. Neuromodulation. 1999;2: Burns B, Watkins L, Goadsby PJ. Treatment of medically intractable cluster headache by occipital nerve stimulation: long-term follow-up of eight patients. Lancet. 2007;369: Schwedt TJ, Dodick DW, Trentman TL, Zimmerman RS. Response to occipital nerve block is not useful in predicting efficacy of occipital nerve stimulation. Cephalalgia. 2007;27: Trentman TL, Zimmerman RS, Nikesh S, Hentz J, Dodick DW. Stimulation ranges, usage ranges, and paresthesia mapping during occipital nerve stimulation. Neuromodulation: Technol Neural Interface. 2008;11: Narouze S. Ultrasonography in pain medicine: future direction. Tech Reg Anesth Pain Manag. 2009;13: Bianchi S, Martinoli C, Zamorani M, Valle M. Ultrasound of the Musculoskeletal System. New York: Springer; Kapural L, Mekhail N, Hayek SM, Stanton-Hicks M, Malak O. Occipital nerve electrical stimulation via the midline approach and subcutaneous surgical leads for treatment of severe occipital neuralgia: a pilot study. Anesth Analg. 2005;101: Trentman TL, Dodick DW, Zimmerman RS, Birch BD. Percutaneous occipital stimulator lead tip erosion: report of 2 cases. Pain Physician. 2008;11:
Stimulation Ranges, Usage Ranges, and. Paresthesia Mapping During Occipital Nerve Stimulation. Introduction ORIGINAL ARTICLE ABSTRACT
 NEUROMODULATION: TECHNOLOGY AT THE NEURAL INTERFACE Volume 11 Number 1 2008 http://www.blackwell-synergy.com/loi/ner ORIGINAL ARTICLE Stimulation Ranges, Usage Ranges, and Blackwell Publishing Inc Paresthesia
NEUROMODULATION: TECHNOLOGY AT THE NEURAL INTERFACE Volume 11 Number 1 2008 http://www.blackwell-synergy.com/loi/ner ORIGINAL ARTICLE Stimulation Ranges, Usage Ranges, and Blackwell Publishing Inc Paresthesia
Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache
 Pain Physician 2011; 14:435-440 ISSN 1533-3159 Case Report Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache Natalie H. Strand
Pain Physician 2011; 14:435-440 ISSN 1533-3159 Case Report Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache Natalie H. Strand
The greater and lesser occipital nerves traverse RECONSTRUCTIVE
 RECONSTRUCTIVE Anatomical Variations of the Occipital Nerves: Implications for the Treatment of Chronic Headaches Ivica Ducic, M.D., Ph.D. Maureen Moriarty, M.S., C.R.N.P. Ali Al-Attar, M.D., Ph.D. Washington,
RECONSTRUCTIVE Anatomical Variations of the Occipital Nerves: Implications for the Treatment of Chronic Headaches Ivica Ducic, M.D., Ph.D. Maureen Moriarty, M.S., C.R.N.P. Ali Al-Attar, M.D., Ph.D. Washington,
Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine:
 Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Affiliation: 1- Departments of Anesthesiology/ Pain Management and Neurology, UCSF School of Medicine 2- Thrive Clinic, LLC, Santa Rosa, CA
 Author Information Prasad Shirvalkar MD, PhD 1 Jason E. Pope MD 2 Affiliation: 1- Departments of Anesthesiology/ Pain Management and Neurology, UCSF School of Medicine 2- Thrive Clinic, LLC, Santa Rosa,
Author Information Prasad Shirvalkar MD, PhD 1 Jason E. Pope MD 2 Affiliation: 1- Departments of Anesthesiology/ Pain Management and Neurology, UCSF School of Medicine 2- Thrive Clinic, LLC, Santa Rosa,
Case Report. Ilioinguinal Peripheral Nerve Stimulation. Juan A. Ramos, MD 1, Andrew J. McNeil, DO 2, Ted F. Gingrich, MD 3
 Case Report Interventional Pain Management Reports Volume 1, Number 2, pp93-97 2017, American Society of Interventional Pain Physicians Combined Ultrasound and Fluoroscopic Guidance for Percutaneous Ilioinguinal
Case Report Interventional Pain Management Reports Volume 1, Number 2, pp93-97 2017, American Society of Interventional Pain Physicians Combined Ultrasound and Fluoroscopic Guidance for Percutaneous Ilioinguinal
A Simple Technique for Surgical Placement of Occipital Nerve Stimulators without Anchoring the Lead
 Surgical Technique A Simple Technique for Surgical Placement of Occipital Nerve Stimulators without Anchoring the Lead Mark Plazier 1 Tim Van Camp 2 Tomas Mevnosky 1 Jan Ost 2 Dirk De Ridder 3 Sven Vanneste
Surgical Technique A Simple Technique for Surgical Placement of Occipital Nerve Stimulators without Anchoring the Lead Mark Plazier 1 Tim Van Camp 2 Tomas Mevnosky 1 Jan Ost 2 Dirk De Ridder 3 Sven Vanneste
Medical Policy. Description/Scope. Position Statement. Rationale
 Subject: Document#: Current Effective Date: 06/28/2017 Status: Reviewed Last Review Date: 05/04/2017 Description/Scope This document addresses occipital nerve stimulation (ONS), which involves delivering
Subject: Document#: Current Effective Date: 06/28/2017 Status: Reviewed Last Review Date: 05/04/2017 Description/Scope This document addresses occipital nerve stimulation (ONS), which involves delivering
Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain.
 Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
Occipital Neuromodulation: A Surgical Technique with Reduced Complications
 Pain Physician 2016; 19:E1005-E1012 ISSN 2150-1149 Retrospective Analysis Occipital Neuromodulation: A Surgical Technique with Reduced Complications Thomas P Pittelkow, DO, MPH, Gabriel L Pagani-Estévez,
Pain Physician 2016; 19:E1005-E1012 ISSN 2150-1149 Retrospective Analysis Occipital Neuromodulation: A Surgical Technique with Reduced Complications Thomas P Pittelkow, DO, MPH, Gabriel L Pagani-Estévez,
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Implanted Peripheral Nerve Stimulator (PNS) for Pain Control Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS)
Implanted Peripheral Nerve Stimulator (PNS) for Pain Control Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS)
Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association
 Implanted Peripheral Nerve Stimulator (PNS) Page 1 of 6 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS) for Pain
Implanted Peripheral Nerve Stimulator (PNS) Page 1 of 6 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS) for Pain
Trigeminal and occipital peripheral nerve stimulation for craniofacial pain: a single-institution experience and review of the literature
 Neurosurg Focus 21 (6):E6, 2006 Trigeminal and occipital peripheral nerve stimulation for craniofacial pain: a single-institution experience and review of the literature KONSTANTIN V. SLAVIN, M.D., M.
Neurosurg Focus 21 (6):E6, 2006 Trigeminal and occipital peripheral nerve stimulation for craniofacial pain: a single-institution experience and review of the literature KONSTANTIN V. SLAVIN, M.D., M.
Stimulation of the Greater Occipital Nerve: Anatomical Considerations and Clinical Implications
 Pain Physician 2013; 16:E181-E189 ISSN 2150-1149 Prospective Study Stimulation of the Greater Occipital Nerve: Anatomical Considerations and Clinical Implications Oliver Mueller, MD, Vincent Hagel, MD,
Pain Physician 2013; 16:E181-E189 ISSN 2150-1149 Prospective Study Stimulation of the Greater Occipital Nerve: Anatomical Considerations and Clinical Implications Oliver Mueller, MD, Vincent Hagel, MD,
Pulsed Radiofrequency Therapy versus Greater Occipital Nerve Block in the Management of Refractory Cervicogenic Headache A Pilot Study
 Prague Medical Report / Vol. 112 (2011) No. 4, p. 279 287 279) Pulsed Radiofrequency Therapy versus Greater Occipital Nerve Block in the Management of Refractory Cervicogenic Headache A Pilot Study Gabrhelík
Prague Medical Report / Vol. 112 (2011) No. 4, p. 279 287 279) Pulsed Radiofrequency Therapy versus Greater Occipital Nerve Block in the Management of Refractory Cervicogenic Headache A Pilot Study Gabrhelík
Cervical Cooled RF Training Presentation
 Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
PERCUTANEOUS FACET JOINT DENERVATION
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Repositioning of Supraorbital Nerve Stimulation Electrode Using Retrograde Needle Insertion: A Technical Note
 Neuromodulation: Technology at the Neural Interface Received: June 7, 2010 First revision: July 24, 2010 Accepted: July 26, 2010 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2010.00315.x Repositioning
Neuromodulation: Technology at the Neural Interface Received: June 7, 2010 First revision: July 24, 2010 Accepted: July 26, 2010 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2010.00315.x Repositioning
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
National Imaging Associates, Inc. Clinical guidelines FACET JOINT INJECTIONS, MEDIAL BRANCH BLOCKS, AND FACET JOINT RADIOFREQUENCY NEUROTOMY
 National Imaging Associates, Inc. Clinical guidelines FACET JOINT INJECTIONS, MEDIAL BRANCH BLOCKS, AND FACET JOINT RADIOFREQUENCY NEUROTOMY CPT Codes: Refer to pages 5 and 6 LCD ID Number: L35936 J K
National Imaging Associates, Inc. Clinical guidelines FACET JOINT INJECTIONS, MEDIAL BRANCH BLOCKS, AND FACET JOINT RADIOFREQUENCY NEUROTOMY CPT Codes: Refer to pages 5 and 6 LCD ID Number: L35936 J K
The Role of the Neuromodulation in Management of Chronic Pain
 The Role of the Neuromodulation in Management of Chronic Pain Adnan Al-Kaisy, MB ChB, FRCA, FFPMRCA, FIPP Clinical Lead of the Pain Management & Neuromodulation Centre Guy s & St Thomas Hospital, London,
The Role of the Neuromodulation in Management of Chronic Pain Adnan Al-Kaisy, MB ChB, FRCA, FFPMRCA, FIPP Clinical Lead of the Pain Management & Neuromodulation Centre Guy s & St Thomas Hospital, London,
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Currently Recommended TON Injectate Volumes Concomitantly Block the GON: Clinical Implications for Managing Cervicogenic Headache
 Pain Physician 2016; 19:E1079-E1086 ISSN 2150-1149 Cadaver Study Currently Recommended TON Injectate Volumes Concomitantly Block the GON: Clinical Implications for Managing Cervicogenic Headache Sayed
Pain Physician 2016; 19:E1079-E1086 ISSN 2150-1149 Cadaver Study Currently Recommended TON Injectate Volumes Concomitantly Block the GON: Clinical Implications for Managing Cervicogenic Headache Sayed
Peripheral Subcutaneous Field Stimulation. Description
 Subject: Peripheral Subcutaneous Field Stimulation Page: 1 of 6 Last Review Status/Date: June 2016 Peripheral Subcutaneous Field Stimulation Description Peripheral subcutaneous field stimulation (PSFS,
Subject: Peripheral Subcutaneous Field Stimulation Page: 1 of 6 Last Review Status/Date: June 2016 Peripheral Subcutaneous Field Stimulation Description Peripheral subcutaneous field stimulation (PSFS,
ISPUB.COM. Lumbar Sympathectomy by Laser Technique. S Kantha, B Kantha METHODS AND MATERIALS
 ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
Ultrasound-guided Pulsed Radiofrequency of the Third Occipital Nerve
 Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Using Peripheral Stimulation to Reduce the Pain of C2-Mediated Occipital Headaches: A Preliminary Report
 Pain Physician 2007; 10:453-460 ISSN 1533-3159 Prospective Case Series Using Peripheral Stimulation to Reduce the Pain of C2-Mediated Occipital Headaches: A Preliminary Report Eugene A. Melvin, Jr., MD
Pain Physician 2007; 10:453-460 ISSN 1533-3159 Prospective Case Series Using Peripheral Stimulation to Reduce the Pain of C2-Mediated Occipital Headaches: A Preliminary Report Eugene A. Melvin, Jr., MD
Occipital Nerve Stimulation for Headache Disorders
 Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Occipital Nerve Stimulation for Headache Disorders Koen Paemeleire* and Thorsten Bartsch *Department of Neurology,
Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Occipital Nerve Stimulation for Headache Disorders Koen Paemeleire* and Thorsten Bartsch *Department of Neurology,
Original Policy Date
 MP 7.01.105 Occipital Nerve Stimulation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy
MP 7.01.105 Occipital Nerve Stimulation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Tikrit University College of Dentistry Dr.Ban I.S. head & neck anatomy 2 nd y.
 Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
FASCIAL PLANE BLOCKS TOM BARIBEAULT MSN, CRNA
 FASCIAL PLANE BLOCKS TOM BARIBEAULT MSN, CRNA TECHNIQUES Abdominal Wall TAP Rectus Sheath Quadratus Lumborum Erector Spinae Chest PECS I & II Erector Spinae TECHNIQUES Knee Ipack/LIA Hip Fascia Iliaca
FASCIAL PLANE BLOCKS TOM BARIBEAULT MSN, CRNA TECHNIQUES Abdominal Wall TAP Rectus Sheath Quadratus Lumborum Erector Spinae Chest PECS I & II Erector Spinae TECHNIQUES Knee Ipack/LIA Hip Fascia Iliaca
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain
 International Journal of Anesthesiology Research, 2015, 3, 37-43 37 Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain Michael Meng 1, Reid
International Journal of Anesthesiology Research, 2015, 3, 37-43 37 Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain Michael Meng 1, Reid
Technical Note NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE FLUOROSCOPIC VIEWS DURING CERVICAL RADIOFREQUENCY NEUROTOMY.
 Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
Radiofrequency Ablation 101
 Radiofrequency Ablation 101 Neuroscience Summit September 10, 2016 Chris Pratt, DO Texas Health Care Pain Management 1651 West Rosedale Street, Suite #205 Fort Worth, Texas 71604 What s in a name? Radiofrequency
Radiofrequency Ablation 101 Neuroscience Summit September 10, 2016 Chris Pratt, DO Texas Health Care Pain Management 1651 West Rosedale Street, Suite #205 Fort Worth, Texas 71604 What s in a name? Radiofrequency
1 Fatty Infiltration in the Cervical Extensor Muscles in Persistent Whiplash- Associated Disorders: A Magnetic Resonance Imaging Analysis
 1 Fatty Infiltration in the Cervical Extensor Muscles in Persistent Whiplash- Associated Disorders: A Magnetic Resonance Imaging Analysis Spine Volume 31(22) October 15, 2006 pp E847-E855 Elliott, James;
1 Fatty Infiltration in the Cervical Extensor Muscles in Persistent Whiplash- Associated Disorders: A Magnetic Resonance Imaging Analysis Spine Volume 31(22) October 15, 2006 pp E847-E855 Elliott, James;
Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
 ORIGINAL ARTICLE Year : 2015 Volume : 63 Issue : 5 Page : 707 711 Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
ORIGINAL ARTICLE Year : 2015 Volume : 63 Issue : 5 Page : 707 711 Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN
 INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN Dr John MacVicar, Medical Director Southern Rehab, Christchurch, NZ AOCPRM Nov 23 rd 2018 INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN An evidence-based
INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN Dr John MacVicar, Medical Director Southern Rehab, Christchurch, NZ AOCPRM Nov 23 rd 2018 INTERVENTIONAL TREATMENT FOR PAIN OF SPINAL ORIGIN An evidence-based
Medical Policy Manual. Topic: Peripheral Subcutaneous Field Stimulation Date of Origin: April Section: Surgery Last Reviewed Date: April 2014
 Medical Policy Manual Topic: Peripheral Subcutaneous Field Stimulation Date of Origin: April 2013 Section: Surgery Last Reviewed Date: April 2014 Policy No: 188 Effective Date: July 1, 2014 IMPORTANT REMINDER
Medical Policy Manual Topic: Peripheral Subcutaneous Field Stimulation Date of Origin: April 2013 Section: Surgery Last Reviewed Date: April 2014 Policy No: 188 Effective Date: July 1, 2014 IMPORTANT REMINDER
Pain Management Clinic ISIC
 Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
Dr Peter Gendall. Mr Steve August. Professor Nik Bogduk. Musculoskeletal Radiologist Hamilton. Physiotherapist Dunedin
 Professor Nik Bogduk Professor Pain Medicine University of Newcastle Mr Steve August Physiotherapist Dunedin Dr Peter Gendall Musculoskeletal Radiologist Hamilton 8:30-10:30 WS #5: Musculoskeletal Medicine
Professor Nik Bogduk Professor Pain Medicine University of Newcastle Mr Steve August Physiotherapist Dunedin Dr Peter Gendall Musculoskeletal Radiologist Hamilton 8:30-10:30 WS #5: Musculoskeletal Medicine
The goal of this article is to describe the. Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation.
 Pain Physician 2011; 14:45-53 ISSN 1533-3159 Technique Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation Jie Zhu, MD 1, Frank Falco, MD 1,2, C. Obi Onyewu, MD 1, Youssef
Pain Physician 2011; 14:45-53 ISSN 1533-3159 Technique Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation Jie Zhu, MD 1, Frank Falco, MD 1,2, C. Obi Onyewu, MD 1, Youssef
16 year old with Disabling Chest Wall Pain after Thoracoscopic Talc Pleurodesis for Treatment of Recurrent Spontaneous Pneumothoraces
 16 year old with Disabling Chest Wall Pain after Thoracoscopic Talc Pleurodesis for Treatment of Recurrent Spontaneous Pneumothoraces Moderators: Kendra Grim, MD, Robert T. Wilder, MD, PhD Institution:
16 year old with Disabling Chest Wall Pain after Thoracoscopic Talc Pleurodesis for Treatment of Recurrent Spontaneous Pneumothoraces Moderators: Kendra Grim, MD, Robert T. Wilder, MD, PhD Institution:
Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y
 May 10, 2018 United Healthcare Medical Policy Department 9500 Bren Road East Minnetonka, MN 55343 via Email: mpq@uhc.com Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y To Whom
May 10, 2018 United Healthcare Medical Policy Department 9500 Bren Road East Minnetonka, MN 55343 via Email: mpq@uhc.com Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y To Whom
Novel Minimally Invasive Wireless Nanotechnology Neuromodulation System in the Management of Chronic Pain Syndromes
 Novel Minimally Invasive Wireless Nanotechnology Neuromodulation System in the Management of Chronic Pain Syndromes Laura Tyler Perryman* Stimwave Technologies, Inc. 1310 Park Central Blvd South, Pompano
Novel Minimally Invasive Wireless Nanotechnology Neuromodulation System in the Management of Chronic Pain Syndromes Laura Tyler Perryman* Stimwave Technologies, Inc. 1310 Park Central Blvd South, Pompano
The Back OUTLINE. Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region
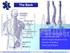 The Back OUTLINE Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region Dept. of Human Anatomy, Si Chuan University Zhou hongying eaglezhyxzy@163.com
The Back OUTLINE Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region Dept. of Human Anatomy, Si Chuan University Zhou hongying eaglezhyxzy@163.com
An Anatomical Study of the Lesser Occipital Nerve and Its Potential Compression Points: Implications for Surgical Treatment of Migraine Headaches
 RECONSTRUCTIVE An Anatomical Study of the Lesser Occipital Nerve and Its Potential Compression Points: Implications for Surgical Treatment of Migraine Headaches Michelle Lee, M.D. Matthew Brown, M.D. Kyle
RECONSTRUCTIVE An Anatomical Study of the Lesser Occipital Nerve and Its Potential Compression Points: Implications for Surgical Treatment of Migraine Headaches Michelle Lee, M.D. Matthew Brown, M.D. Kyle
Fluoroscopically-Guided Injections to Treat Kissing Spine Disease
 Pain Physician 2008; 11:549-554 ISSN 1533-3159 Case Report Fluoroscopically-Guided Injections to Treat Kissing Spine Disease Timothy J. Lamer, MD 1, Jeffrey M. Tiede, MD 2 and Douglas S. Fenton, MD 3 From:
Pain Physician 2008; 11:549-554 ISSN 1533-3159 Case Report Fluoroscopically-Guided Injections to Treat Kissing Spine Disease Timothy J. Lamer, MD 1, Jeffrey M. Tiede, MD 2 and Douglas S. Fenton, MD 3 From:
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Policy #: 411 Latest Review Date: January 2014
 Name of Policy: Occipital Nerve Stimulation Policy #: 411 Latest Review Date: January 2014 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross
Name of Policy: Occipital Nerve Stimulation Policy #: 411 Latest Review Date: January 2014 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross
Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion
 Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Occipital Nerve Stimulation Corporate Medical Policy
 Occipital Nerve Stimulation Corporate Medical Policy File Name: Occipital Nerve Stimulation File Code: UM.SPSVC.14 Origination: 2011 Last Review: 06/2018 Next Review: 06/2019 Effective Date: 10/01/2018
Occipital Nerve Stimulation Corporate Medical Policy File Name: Occipital Nerve Stimulation File Code: UM.SPSVC.14 Origination: 2011 Last Review: 06/2018 Next Review: 06/2019 Effective Date: 10/01/2018
A Standardized Protocol for Needle Placement in Suboccipital Muscles
 Clinical Anatomy 21:501 508 (2008) ORIGINAL COMMUNICATION A Standardized Protocol for Needle Placement in Suboccipital Muscles RICHARD C. HALLGREN, 1,2 * MICHAEL T. ANDARY, 2 ANDREW J. WYMAN, 3 AND JACOB
Clinical Anatomy 21:501 508 (2008) ORIGINAL COMMUNICATION A Standardized Protocol for Needle Placement in Suboccipital Muscles RICHARD C. HALLGREN, 1,2 * MICHAEL T. ANDARY, 2 ANDREW J. WYMAN, 3 AND JACOB
Radiofrequency of lumbar facet joints
 Radiofrequency treatment of lumbar spine the past, the present and the future Michael Gofeld MD, FIPP Department of Anesthesia, Sunnybrook & Women s College Health Sciences Centre University of Toronto
Radiofrequency treatment of lumbar spine the past, the present and the future Michael Gofeld MD, FIPP Department of Anesthesia, Sunnybrook & Women s College Health Sciences Centre University of Toronto
MEDICAL POLICY SUBJECT: RADIOFREQUENCY FACET DENERVATION
 MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
2016 HF10 THERAPY REIMBURSEMENT REFERENCE GUIDE
 206 HF0 THERAPY REIMBURSEMENT REFERENCE GUIDE HF0 therapy, delivered by the Nevro Senza System, is a new high-frequency spinal cord stimulation technology designed to aid in the management of chronic intractable
206 HF0 THERAPY REIMBURSEMENT REFERENCE GUIDE HF0 therapy, delivered by the Nevro Senza System, is a new high-frequency spinal cord stimulation technology designed to aid in the management of chronic intractable
Stereotactic topography of the greater and third occipital nerves and its clinical implication
 www.nature.com/scientificreports Received: 25 September 2017 Accepted: 20 December 2017 Published: xx xx xxxx OPEN Stereotactic topography of the greater and third occipital nerves and its clinical implication
www.nature.com/scientificreports Received: 25 September 2017 Accepted: 20 December 2017 Published: xx xx xxxx OPEN Stereotactic topography of the greater and third occipital nerves and its clinical implication
Basic Standards for. Fellowship Training in. Acute and Chronic Pain Management. in Anesthesiology
 Basic Standards for Fellowship Training in Acute and Chronic Pain Management in Anesthesiology American Osteopathic Association and American Osteopathic College of Anesthesiologists BOT, 7/1995 BOT, 11/2002
Basic Standards for Fellowship Training in Acute and Chronic Pain Management in Anesthesiology American Osteopathic Association and American Osteopathic College of Anesthesiologists BOT, 7/1995 BOT, 11/2002
Long-Term Outcome in Occipital Nerve Stimulation Patients With Medically Intractable Primary Headache Disorders
 Neuromodulation: Technology at the Neural Interface Received: April 12, 2012 Revised: June 15, 2012 Accepted: June 27, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2012.00490.x Long-Term Outcome
Neuromodulation: Technology at the Neural Interface Received: April 12, 2012 Revised: June 15, 2012 Accepted: June 27, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2012.00490.x Long-Term Outcome
Spinal and Trigger Point Injections
 Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Peripheral nerve stimulation for treatment of postherpetic neuralgia: A Case report
 Case report Acta Medica Academica 2011;40(2):187-191 DOI 10.5644/ama2006-124.23 Peripheral nerve stimulation for treatment of postherpetic neuralgia: A Case report Scott C. Palmer 1, Alexis A. Jimenez
Case report Acta Medica Academica 2011;40(2):187-191 DOI 10.5644/ama2006-124.23 Peripheral nerve stimulation for treatment of postherpetic neuralgia: A Case report Scott C. Palmer 1, Alexis A. Jimenez
Integra. Endoscopic Gastrocnemius Release System SURGICAL TECHNIQUE
 Integra Endoscopic Gastrocnemius Release System SURGICAL TECHNIQUE Table of Contents Indications... 2 Contraindications... 2 System Description... 2 Features and Benefits... 2 Surgical Site Preparation...3
Integra Endoscopic Gastrocnemius Release System SURGICAL TECHNIQUE Table of Contents Indications... 2 Contraindications... 2 System Description... 2 Features and Benefits... 2 Surgical Site Preparation...3
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi. E mail: a.al E. mail:
 Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Peripheral Subcutaneous Field Stimulation
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Author Information. Presenting Symptom: Burning in right foot> Chronic low back pain
 Author Information Full Names: Erica Patel, MD Kiran V. Patel, MD Presenting Symptom: Burning in right foot> Chronic low back pain Case Specific Diagnosis: Chronic low back pain and radicular pain Learning
Author Information Full Names: Erica Patel, MD Kiran V. Patel, MD Presenting Symptom: Burning in right foot> Chronic low back pain Case Specific Diagnosis: Chronic low back pain and radicular pain Learning
Nonsurgical Interventional Treatments for Spinal Pain Management
 Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
General remarks on Neurorejuvenation Spinal Cord Stimulation (SCS) Program Occipital Nerve Stimulation Gamma-knife for Trigeminal Neuralgia
 General remarks on Neurorejuvenation Spinal Cord Stimulation (SCS) Program Occipital Nerve Stimulation Gamma-knife for Trigeminal Neuralgia Deep brain Stimulation (DBS) Program Neuromodulation is a field
General remarks on Neurorejuvenation Spinal Cord Stimulation (SCS) Program Occipital Nerve Stimulation Gamma-knife for Trigeminal Neuralgia Deep brain Stimulation (DBS) Program Neuromodulation is a field
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain Goals GOALS AND OBJECTIVES The ACGME recognizes that interventional pain medicine
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain Goals GOALS AND OBJECTIVES The ACGME recognizes that interventional pain medicine
UCSD DEPARTMENT OF ANESTHESIOLOGY
 UCSD DEPARTMENT OF ANESTHESIOLOGY LEARNING OBJECTIVES FOR ADVANCED PAIN MEDICINE ROTATION, UCSD MEDICAL CENTER Competencies Objective Learning Environment Instructional Method Assessment Tool Patient Care:
UCSD DEPARTMENT OF ANESTHESIOLOGY LEARNING OBJECTIVES FOR ADVANCED PAIN MEDICINE ROTATION, UCSD MEDICAL CENTER Competencies Objective Learning Environment Instructional Method Assessment Tool Patient Care:
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 3/2018 Origination: 7/2013 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 3/2018 Origination: 7/2013 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT
 US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT www.ecografieinfiltrazioni.it Dott. Luca Di Sante LBP is a major cause of disability, the exact pathogenesis of acute LBP remains unclear The
US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT www.ecografieinfiltrazioni.it Dott. Luca Di Sante LBP is a major cause of disability, the exact pathogenesis of acute LBP remains unclear The
Review Article. The Management of the Atlanto-Occipital and Atlanto-Axial Joint Pain
 Ogoke Atlanto-Occipital and Atlanto-Axial Joint Pain 289 Pain Physician, Volume 3, Number 3, pp 289-293 2000, Association of Pain Management Anesthesiologists Review Article The Management of the Atlanto-Occipital
Ogoke Atlanto-Occipital and Atlanto-Axial Joint Pain 289 Pain Physician, Volume 3, Number 3, pp 289-293 2000, Association of Pain Management Anesthesiologists Review Article The Management of the Atlanto-Occipital
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2018 Origination: 7/2013 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2018 Origination: 7/2013 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
Epidural Steroid Injection
 Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
SURGICAL AND RADIOGRAPHIC ANATOMY of LUMBAR RADIOFREQUENCY MEDIAL BRANCH NEUROTOMY
 SURGICAL AND RADIOGRAPHIC ANATOMY of LUMBAR RADIOFREQUENCY MEDIAL BRANCH NEUROTOMY Prepared for the Spine Intervention Society by Professor Nikolai Bogduk MD, PhD, DSc University of Newcastle, Royal Newcastle
SURGICAL AND RADIOGRAPHIC ANATOMY of LUMBAR RADIOFREQUENCY MEDIAL BRANCH NEUROTOMY Prepared for the Spine Intervention Society by Professor Nikolai Bogduk MD, PhD, DSc University of Newcastle, Royal Newcastle
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Sustained Effectiveness of Occipital Nerve Stimulation in Drug-Resistant Chronic Cluster Headachehead_
 Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.01973.x Published by Wiley Periodicals, Inc. Research Submissions Sustained Effectiveness of Occipital Nerve in Drug-Resistant
Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.01973.x Published by Wiley Periodicals, Inc. Research Submissions Sustained Effectiveness of Occipital Nerve in Drug-Resistant
Yuecheng Yang, Xuehua Huang, Yinghui Fan, Yingwei Wang, and Ke Ma. 1. Introduction
 Evidence-Based Complementary and Alternative Medicine Volume 2015, Article ID 690856, 7 pages http://dx.doi.org/10.1155/2015/690856 Research Article Efficacy of Pulsed Radiofrequency on Cervical 2-3 Posterior
Evidence-Based Complementary and Alternative Medicine Volume 2015, Article ID 690856, 7 pages http://dx.doi.org/10.1155/2015/690856 Research Article Efficacy of Pulsed Radiofrequency on Cervical 2-3 Posterior
Paraspinal Blocks a new paradigm in truncal analgesia
 Paraspinal Blocks a new paradigm in truncal analgesia Ki Jinn Chin, MBBS (Hons), MMed, FRCPC Associate Professor Toronto Western Hospital University of Toronto Online Resources https://youtu.be/lockhd
Paraspinal Blocks a new paradigm in truncal analgesia Ki Jinn Chin, MBBS (Hons), MMed, FRCPC Associate Professor Toronto Western Hospital University of Toronto Online Resources https://youtu.be/lockhd
H F 1 0 T H E R A P Y R E I M B U R S E M E N T R E F E R E N C E G U I D E
 HF10 therapy, delivered by the Nevro Senza System, is the high-frequency spinal cord stimulation technology designed to aid in the management of chronic intractable pain of the trunk/limbs without paresthesia.
HF10 therapy, delivered by the Nevro Senza System, is the high-frequency spinal cord stimulation technology designed to aid in the management of chronic intractable pain of the trunk/limbs without paresthesia.
Guideline Number: NIA_CG_301 Last Revised Date: March 2018 Responsible Department: Clinical Operations
 Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Headache: Using Neuromodulation as Therapy
 Headache: Using Neuromodulation as Therapy Rashmi Halker, MD, FAHS Assistant Professor of Neurology Department of Neurology Mayo Clinic Phoenix Arizona Disclosures Nothing to disclose 2013 MFMER slide-2
Headache: Using Neuromodulation as Therapy Rashmi Halker, MD, FAHS Assistant Professor of Neurology Department of Neurology Mayo Clinic Phoenix Arizona Disclosures Nothing to disclose 2013 MFMER slide-2
Re: Treatment Modalities for Facetogenic Pain, Policy #141
 March 30, 2017 Blue Cross and Blue Shield of Alabama Attn: Health Management - Medical Policy P.O. Box 995 Birmingham, AL 35298-0001 Fax: 205-220-0878 Re: Treatment Modalities for Facetogenic Pain, Policy
March 30, 2017 Blue Cross and Blue Shield of Alabama Attn: Health Management - Medical Policy P.O. Box 995 Birmingham, AL 35298-0001 Fax: 205-220-0878 Re: Treatment Modalities for Facetogenic Pain, Policy
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Neck-2. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
MEDICAL POLICY SUBJECT: RADIOFREQUENCY JOINT ABLATION / DENERVATION
 MEDICAL POLICY SUBJECT: RADIOFREQUENCY JOINT PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including
MEDICAL POLICY SUBJECT: RADIOFREQUENCY JOINT PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including
Clinical Protocols of the Anesthesiology Department at the Dartmouth-Hitchcock Medical Center: Techniques for lower extremity nerve blocks.
 Clinical Protocols of the Anesthesiology Department at the Dartmouth-Hitchcock Medical Center: Techniques for lower extremity nerve blocks. Authors from DHMC: Brian D. Sites, MD. Assistant Professor of
Clinical Protocols of the Anesthesiology Department at the Dartmouth-Hitchcock Medical Center: Techniques for lower extremity nerve blocks. Authors from DHMC: Brian D. Sites, MD. Assistant Professor of
Disclosure. Pre-Procedural Considerations. Transducer Selection. Sterile Procedure. Sterile Procedure. Ultrasound Guided Foot and Ankle Injections
 Ultrasound Guided Foot and Ankle Injections Disclosure No relevant financial relationships exist Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012
Ultrasound Guided Foot and Ankle Injections Disclosure No relevant financial relationships exist Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012
ความส มพ นธ ทางกายว ภาคศาสตร ของเส นประสาท
 MMP35- The Anatomical Relation of The Greater Occipital Nerve to The Trapezius, Semispinalis Capitis and Obliquus Capitis Inferior Muscles ความส มพ นธ ทางกายว ภาคศาสตร ของเส นประสาท Greater occipital ก
MMP35- The Anatomical Relation of The Greater Occipital Nerve to The Trapezius, Semispinalis Capitis and Obliquus Capitis Inferior Muscles ความส มพ นธ ทางกายว ภาคศาสตร ของเส นประสาท Greater occipital ก
The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care settings,
 American Journal of Emergency Medicine (2011) xx, xxx xxx www.elsevier.com/locate/ajem Clinical Notes The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care
American Journal of Emergency Medicine (2011) xx, xxx xxx www.elsevier.com/locate/ajem Clinical Notes The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care
