Trigeminal and occipital peripheral nerve stimulation for craniofacial pain: a single-institution experience and review of the literature
|
|
|
- Samantha Houston
- 5 years ago
- Views:
Transcription
1 Neurosurg Focus 21 (6):E6, 2006 Trigeminal and occipital peripheral nerve stimulation for craniofacial pain: a single-institution experience and review of the literature KONSTANTIN V. SLAVIN, M.D., M. EFKAN COLPAN, M.D., NAUREEN MUNAWAR, M.D., CHRISTIAN WESS, M.D., AND HRACHYA NERSESYAN, M.D., PH.D. Department of Neurosurgery, University of Illinois, Chicago, Illinois Object. Treatment of chronic neuropathic pain in the region of the head and face presents a challenge for pain specialists; patients who do not respond to conventional treatment modalities usually continue to suffer from pain due to the lack of reliable medical and surgical approaches. Peripheral nerve stimulation (PNS) has been used to treat neuropathic pain for many decades, but only recently has it been applied systematically to the craniofacial region. To advance the study of this treatment option, the authors present their initial experience with this approach, summarize published data on the use of PNS in treatment of craniofacial pain, and discuss some technical details of the craniofacial PNS procedure. Methods. A review of prospectively collected data in 30 patients who underwent PNS surgery for craniofacial pain was performed. The pain location, duration, cause, and previous treatments were analyzed, along with the surgical details, initial and long-term results, complications, and repeated operations. Stimulated nerves in this group included supraorbital (seven patients), infraorbital (six), and occipital (21); in 19 patients more than one nerve was stimulated. Twenty-two patients proceeded with implantation of a permanent system after the trial. Of these, at the time of the latest evaluation (mean follow-up duration 35 months), in two patients the devices had been removed because of pain improvement over time, in three the devices were removed due to loss of effectiveness (two cases) or late infection (one), and the rest are enjoying either complete (15 patients) or partial (two patients) pain relief. Three patients underwent repeated operation due to lead erosion, infection, or migration. Conclusions. Peripheral nerve stimulation appears to be a safe and effective approach in the treatment of craniofacial neuropathic pain. The growing body of literature supports a wider acceptance of this approach in the field of pain surgery. KEY WORDS pain neuromodulation peripheral nerve stimulation occipital nerve stimulation trigeminal nerve T HE idea of using PNS to treat craniofacial pain is not new. The interest in this modality has been increasing over the last few years, but the original applications date back to the 1960s. When Wall and Sweet 19 tried to find a new approach to suppress neuropathic pain, they inserted an electrode into their own infraorbital foramina and obtained a decrease in pain perception during the entire episode of electrical stimulation. 23 Moreover, in the first article dedicated to the idea of PNS with implantable devices (even before spinal cord stimulation was introduced), 19 one of the eight patients with neuropathic pain presented with severe facial pain, and in this patient an electrode was inserted deep into the infraorbital foramen. The stimulation resulted in lasting pain suppression as long as the stimulator was on. Later, in another patient a system was applied to the temporal area, Abbreviations used in this paper: PNS = peripheral nerve stimulation. delivering stimulation aimed at the branches of the mandibular nerve. 23 At approximately the same time, Shelden 12 implanted electrodes wrapped around the mandibular nerve itself in three patients and stimulated the nerves through an implanted receiver at 14,000 Hz, thus achieving temporary pain relief. The use of PNS for craniofacial neuropathic pain was rediscovered in 1999 with the publication of an article by Weiner and Reed 22 in which they described percutaneous electrode insertion in the vicinity of the occipital nerves. Soon after publication of that pioneering paper, we began using the PNS approach in both the occipital and trigeminal regions. 13,14 Many other publications detailing the experience in many centers and describing different PNS techniques and applications have appeared over the last several years. 1 11,15 17,20,21 Patient Population Clinical Material and Methods We analyzed prospectively collected data in all patients who had undergone PNS for craniofacial pain in our insti- 1
2 K. Slavin et al. tution since The basic demographic characteristics, details of the patients conditions, surgical aspects, and follow-up observations were summarized and reviewed. The small size of the group (41 patients) and its heterogeneity did not allow statistical analysis; therefore we limited our review to clinical outcomes and complications. All 41 patients presenting with neuropathic pain in the face and/or head underwent diagnostic nerve blocks to establish participation of certain nerves in generation of the pain. Of these patients, 30 were considered candidates for PNS surgery. They were sent for routine neuropsychological testing and then underwent the stimulation trial. Demographic characteristics and pain parameters are summarized in Table 1. Surgical Technique The electrodes are inserted for the trial in a sterile fashion, either after the induction of local anesthesia or after sedation augmented by infiltration of the insertion site with local anesthetic. Because the procedure is brief and the surgical site is quite superficial, general anesthesia is almost never needed. The direction of electrode insertion may be chosen based on the surgeon s preference: we routinely insert electrodes from lateral to medial, not only in the supraorbital and infraorbital regions (where it is probably the only way to place them), 17 but also in the occipital area, 15 as opposed to some other centers in which insertion of electrodes from medial to lateral is preferred. 1,10 Standard fouror eight-contact electrodes were used (Fig. 1); the electrodes were passed in the epifascial plane under the skin but above the muscles. Our general approach is to have the electrode cross the path of the nerve chosen as a stimulation target. As long as this nerve happens to be either under one of the electrode s contacts or between two contacts, the stimulation can be steered toward it to get adequate coverage. For the trial insertion, we did not implant any deep anchors or extensions; the electrodes were sutured to the skin with plastic anchors and fine nylon, and a strain-relief loop was created around the insertion site to avoid inadvertent electrode pullout. The electrodes were inserted using fluoroscopic guidance. Standard landmarks were used for the insertion: the supraorbital groove or foramen and the supraorbital ridge for the supraorbital nerve; the infraorbital foramen and the floor of the orbit for the infraorbital nerve; and the C-1 arch and radiographic midline for the occipital nerves. In TABLE 1 Demographic characteristics of patients selected for PNS trial Characteristic Value sex female 22 male 8 age (yrs) 47.3 (range 22 97) duration of pain 4 yrs (range 8 mos 12 yrs) location of pain (no. of patients)* lt supraorbital 5 rt supraorbital 4 lt infraorbital 1 rt infraorbital 5 lt occipital 16 rt occipital 18 causative factors (no. of patients) trigeminal op 3 Chiari decompression 3 other ops 8 trauma 5 rheumatoid arthritis 1 unknown 10 duration of trial (days) 6 (range 4 7) *Pain was noted in more than one territory in 19 patients. the beginning, we tested each patient for stimulationinduced paresthesias in the operating room so that the position of the electrode could be adjusted if needed. Lately, however, we have been relying exclusively on anatomical electrode positioning due to its high reliability in getting appropriate coverage. This has resulted in significant improvement in the patient s comfort associated with the deeper sedation, which may now be used because the patient s cooperation during the procedure is not needed. The electrode is covered with sterile dressing and attached to the external stimulation system; the initial programming is performed to produce adequate paresthesias in the painful area; the patient is instructed on adjustment of the stimulator depending on activity and pain level; and antibiotics are prescribed for the duration of the trial to avoid development of superficial infection (although the need for this particular step is not supported by any clinical evidence). Once the trial is completed, the temporary system is replaced with the permanent one. We prefer to remove the temporary electrode and then insert a new permanent electrode that is connected either directly to the generator or to FIG. 1. Radiographs showing positioning of electrodes. A: Unilateral four-contact supraorbital nerve stimulation electrode. B: Unilateral eight-contact occipital nerve stimulation electrode. C: Bilateral eight-contact supraorbital nerve stimulation electrodes. 2
3 Peripheral neuromodulation for craniofacial pain an extension cable that connects to the generator. The electrodes we use are cylindrical wire types (such as Quad, Octad, Quad Plus, or Quad Compact [Medtronic, Inc.]; Qattrode, Octrode, or Axxess [Advanced Neuromodulation Systems]; and Linear [Advanced Bionics]). The electrodes or extension cables are tunneled toward the generator pocket. The tunneling step is quite painful and necessitates the use of general anesthesia. Location of the pocket is chosen based on the patient s and surgeon s preference. We routinely use the infraclavicular area for both trigeminal and occipital nerve stimulation systems, and in this way the procedure is similar to the one used for placement of deep brain stimulation generators. (According to our recent survey, 18 the patients with infraclavicular generators were found to have a very high level of satisfaction with this particular location.) The pocket should satisfy certain requirements: 1) it has to be deep enough to avoid hardware erosion; 2) it should not be too deep, thus interfering with reprogramming or, in the case of rechargeable devices, their regular charging; and 3) it should be located in a relatively immobile region because the hardware may fail if subjected to repetitive mechanical stress. Results Of 30 patients who underwent the trial stimulation, only 22 (73%) experienced more than a 50% reduction in pain intensity and went on to have a permanent system implanted. Among these patients, three had infraorbital PNS, four had supraorbital, in 13 it was occipital, and one each had a combination of infraorbital and occipital or supraorbital and occipital stimulation. Twelve patients had bilateral stimulation (10 occipital and two supraorbital). A total of 36 electrodes and 22 generators were implanted in this series. Complications directly related to the implant surgery occurred in two cases; in one patient problems were found with the connection between the generator and the extension cable, necessitating a return to the operating room and revision of the PNS system on the same day as internalization, and in another electrode migration developed that required a repeat of the operation 2 weeks later. There were no infections in the immediate postoperative period; no patient developed problems with the generator pocket site. The patients underwent periodic follow-up evaluations for a mean of 35 months after the implant (range 1 77 months; 18 patients were followed for 1 year, and 13 for 3 years). By the time of the latest follow-up visit, the systems had been removed in five patients. In two of them the reason for PNS system removal was improvement in pain intensity; both patients stopped using their stimulator at least 6 months prior to its removal. In two other patients the initial benefit of stimulation was lost after 2 years in one and 6 months in the other. Both of them continued to experience pain despite reprogramming attempts, and their devices were removed soon thereafter. In the fifth patient the system was removed because an infection developed in the generator pocket 2 years after implantation; this complication was most likely due to hematogenous spread following bacteremia. Of the 17 patients who continue to use the PNS device for pain control, three have stated that PNS improves their pain by less than 50% of its intensity (partial responders), whereas 14 have reported more than 50% improvement in pain intensity based on the visual analog scale (responders). Three patients required a repeat of the operation during the follow-up period. In one patient skin erosion developed over the electrode tip; his electrode was removed and then reimplanted 1 month later, with complete return of stimulation benefits. In another patient an infection developed over the connector between the electrode and the extension cable. This problem was solved by removing the electrode/extension cable and reinserting it 3 months later, after antibiotics were used to treat the infection. The benefits of stimulation were restored after the system was reimplanted. In the third patient, the workup for loss of the stimulation benefits revealed migration of the electrode, which was corrected in a repeated operation. Altogether, of 22 patients in whom PNS devices were implanted for craniofacial pain, 16 (73%) experienced significant ( 50%) improvement in pain intensity (14 with and two without stimulation); three patients (13.5%) reported less than 50% pain improvement; and three (13.5%) continued to experience pain after their devices were removed due to either loss of effect or infection. The percentage of successful outcomes decreases if one takes into consideration all patients who were candidates for the trial (16 [53%] of 30) or those who presented with pain and underwent nerve blocks with local anesthetic (16 [39%] of 41), even though there was some possibility of pain improvement without stimulation among those who did not undergo PNS surgery. Indications for PNS Discussion General indications for PNS are quite specific: it is usually recommended for patients with neuropathic pain of various origins as long as there is some preservation of sensation in the painful area. The four most common indications applicable to the craniofacial region that have been described in the literature are as follows: 1) postherpetic neuralgia involving the territory of the trigeminal nerve; 2) posttraumatic or postsurgical neuropathic pain that is related to an underlying dysfunction of the infraorbital, supraorbital, or occipital nerve; 3) transformed migraine presenting with occipital pain and discomfort; and 4) occipital neuralgia or cervicogenic occipital pain. In each of these situations, the patients have anatomical distribution of pain; their pain is medically intractable; they had favorable results on neuropsychological testing; the area of pain is not anesthetic (although hypesthesia and hyperesthesia are allowed); and, in the first two groups, the onset of pain is linked to a known traumatic, surgical, or infectious event. In most centers, a local anesthetic block is used to confirm involvement of the specific nerve in the generation of pain, although elimination of pain with a nerve block does not necessarily predict success of PNS. Therefore, a trial stimulation is performed to check responsiveness of the pain to the stimulation approach prior to implantation of the permanent system. Usually, a 50% improvement in pain intensity serves as a cutoff limit for considering the trial successful. The psychological evaluation is routinely performed, at 3
4 K. Slavin et al. least in our practice, where it has become a part of the evaluation of all patients who are considered for painrelieving surgery. Prior to the intervention, early detection of somatization, untreated depression, drug abuse, and drug seeking as well as various secondary gains (not necessarily financial) that may not be obvious to the surgical team helps to predict the success of surgery and address the issues that may negatively affect the outcome. The nerves that are most frequently selected for stimulation are supraorbital, infraorbital, and, less often, auriculotemporal and supratrochlear in cases of facial pain, and greater and lesser occipital nerves in cases of occipital pain. In our opinion, stimulating the nerve itself may be more effective than field stimulation, but this is debatable because the surgeons who prefer field stimulation achieve very similar clinical results in terms of improvement and overall success. Surgical Procedure We used only wire-type (percutaneous) electrodes for both trigeminal and occipital stimulation Other groups reported using plate-type (also called paddle-type) electrodes (Resume, Resume II, or Resume TL; Medtronic, Inc.) for stimulation of occipital nerves. Implantation of such electrodes can be preceded by a trial with wire-type electrodes, 5 or the trial can be done with a plate-type electrode connected to a temporary extension. 9 In all cases the electrodes are placed over the path of the peripheral nerve that supplies the painful area and may be involved in the generation of pain. The generator pocket in our series was always created in the infraclavicular region. 18 Placement of generators in the gluteal area, 5,11 abdominal wall, 3,22 or infraclavicular areas 4,9,22 has been described. Treatment Results According to our review of the literature, all published reports on the use of PNS for control of neuropathic craniofacial pain have shown significant and lasting improvement in pain intensity. What follows is a brief review of published experience based on the diagnosis of the condition being treated, although one has to keep in mind that labeling painful conditions may be difficult at times. The largest group of patients who underwent PNS suffered from occipital neuralgia and cervicogenic headaches. Pain in these patients was located primarily in the occipital region and the upper part of the neck, sometimes radiating toward the vertex or even the forehead. The participation of the occipital nerves in these pain syndromes was usually confirmed by results of local anesthetic blocks of the greater and lesser occipital nerves. Weiner and Reed 22 in 1999 reported improvement in all 13 patients with unilateral or bilateral occipital neuralgia who underwent occipital PNS implantation, and whose mean follow-up duration was 2 years. Later, the same authors reported 80% success in a group of 62 patients with intractable occipital headaches. 21 Hammer and Doleys 3 presented a report on a patient with occipital neuralgia who underwent implantation with an obliquely placed eightcontact electrode; she maintained 90% improvement in pain intensity as well as improvement in most psychological indicators. Oh et al. 9 described excellent and good outcomes at the 1-month follow-up interval in all 10 of their patients with occipital neuralgia ( 75% pain relief), and that effect persisted in eight of 10 at the 6-month follow-up visit. Rodrigo-Royo et al. 11 reported on three patients with occipital pain and headaches and one with postherpetic occipital pain; all of them improved after receiving occipital PNS, and this improvement persisted until their last follow-up visit 4 to 16 months postimplantation. In a series of patients with occipital neuralgia reported by Nörenberg and Winkenmüller, 8 three candidates proceeded with the permanent implantation after the trial, whereas two others did not benefit from stimulation, presumably due to preexisting impairment of sensation in the painful region. In a pilot study by Kapural et al., 5 six patients with occipital neuralgia who underwent implantation of paddle-type electrodes maintained significant improvement at the 3-month follow-up visit. In our current series, in a group of 18 patients with occipital neuralgia, 13 exhibited improvement of pain during the trial and underwent implantation of the permanent system. Over the mean follow-up period of 28 months, the beneficial effect of long-term occipital PNS persisted in 85% of those who significantly improved during the trial. Another indication for occipital PNS that is currently being investigated is so-called transformed migraine. Migraine is a very common affliction, and sometimes it is medically intractable. Recently, pain specialists started linking occipital neuralgia with spinally transformed migraine, sometimes using these terms interchangeably. 1 Popeney and Aló 10 reported results of occipital PNS in 25 patients with chronic disabling transformed migraine; at a mean follow-up interval of 18 months, improvement in the migraine disability assessment score was almost 90%. All 10 patients with severe chronic migraine who were evaluated using positron emission tomography studies by Matharu et al. 7 achieved excellent pain relief with suboccipital stimulators (although one patient also required bilateral supraorbital stimulation). Whereas percutaneous, wire-type electrodes were used in these two studies, Oh et al. 9 reported on 10 patients with transformed migraines who underwent implantation of paddle-type electrodes (seven of them initially had received percutaneous electrodes that migrated and were replaced with surgical leads); all 10 had more than 75% pain relief at both 1 and 6 months after the implantation. Indications for PNS of the trigeminal branches are limited primarily to trigeminal neuropathic pain and postherpetic neuralgia. In one case, supraorbital stimulation was used in addition to bilateral occipital PNS for treatment of chronic migraine. 7 Treatment of postherpetic neuralgia involving the ophthalmic nerve distribution by using the PNS technique was first described by Dunteman 2 in 2002; two patients received unilateral supraorbital PNS implants and maintained excellent pain relief for 3 years. Recently, Johnson and Burchiel 4 reported their results in four patients with postherpetic neuralgia affecting the supraorbital region; two of these patients maintained more than 50% pain relief after 2 years of follow up. In regard to posttraumatic or postsurgical neuropathic trigeminal pain, Slavin and Burchiel 13,14 reported more than 50% improvement in pain intensity in all patients who had 4
5 Peripheral neuromodulation for craniofacial pain undergone permanent implantation of a PNS system since In a group of six of these patients, one failed to improve during the trial, and the remaining five maintained significant ( 50%) improvement in pain, with a mean follow-up duration of longer than 26 months. 4 We observed somewhat similar results; nine of 12 patients proceeded with implantation of a permanent PNS system, and in three the system was subsequently removed for the following reasons: improvement of pain, the loss of efficacy, and a generator site infection (one each). Five of the remaining six patients maintained more than 50% pain improvement over a mean of 44 months of follow up. In Johnson and Burchiel s 4 experience, of six patients with nonherpetic trigeminal neuropathic pain, supraorbital and infraorbital distribution of pain was observed in three patients each. In our cohort, four patients had unilateral infraorbital pain; two each had unilateral supraorbital, bilateral supraorbital, and unilateral supraorbital and occipital pain; and of the two remaining patients, one had unilateral infra- and supraorbital and the other had unilateral infraorbital and occipital pain. The overall rate of complications in the literature and in our series was low; the majority of complications (wound breakdown, skin erosion, focal infections, discomfort due to a short extension cable, and so on) were minor, and even if additional interventions were needed, none caused any serious or lasting problem. Conclusions The number of centers using PNS for craniofacial pain is increasing, and as the experience grows one may expect better definitions of criteria predictive of lasting positive outcome. The appearance of larger clinical series will probably result in wider acceptance of this treatment approach, and its low invasiveness, testability, reversibility of effect, and the adjustability of settings may make it the preferred modality for otherwise intractable conditions. References 1. Aló KM, Holsheimer J: New trends in neuromodulation for the management of neuropathic pain. Neurosurgery 50: , Dunteman E: Peripheral nerve stimulation for unremitting ophthalmic postherpetic neuralgia. Neuromodulation 5:32 37, Hammer M, Doleys DM: Perineuromal stimulation in the treatment of occipital neuralgia: a case study. Neuromodulation 4: 47 52, Johnson MD, Burchiel KJ: Peripheral stimulation for treatment of trigeminal postherpetic neuralgia and trigeminal posttraumatic neuropathic pain: a pilot study. Neurosurgery 55: , Kapural L, Mekhail N, Hayek SM, Stanton-Hicks M, Malak O: Occipital nerve electrical stimulation via the midline approach and subcutaneous surgical leads for treatment of severe occipital neuralgia: a pilot study. Anesth Analg 101: , Lou L: Uncommon areas of electrical stimulation. Curr Rev Pain 4: , Matharu MS, Bartsch I, Ward N, Frackowiak RSJ, Weiner R, Goadsby PJ: Central neuromodulation in chronic migraine patients with suboccipital stimulators: a PET study. Brain 127: , Nörenberg E, Winkelmüller W: [The epifacial electric stimulation of the occipital nerve in cases of therapy-resistant neuralgia of the occipital nerve.] Schmerz 15: , 2001 (Ger) 9. Oh MY, Ortega J, Bellotte JB, Whiting DM, Aló K: Peripheral nerve stimulation for the treatment of occipital neuralgia and transformed migraine using a C1 2 3 subcutaneous paddle style electrode: a technical report. Neuromodulation 7: , Popeney CA, Aló KM: Peripheral neurostimulation for the treatment of chronic, disabling transformed migraine. Headache 43: , Rodrigo-Royo MD, Azcona JM, Quero J, Lorente MC, Acín P, Azcona J: Peripheral neurostimulation in the management of cervicogenic headaches: four case reports. Neuromodulation 8: , Shelden CH: Depolarization in the treatment of trigeminal neuralgia. Evaluation of compression and electrical methods; clinical concept of neurophysiological mechanism, in Knighton RS, Dumke PR (eds): Pain. Boston: Little, Brown, 1966, pp Slavin KV, Burchiel KJ: Peripheral nerve stimulation for painful nerve injuries. Contemp Neurosurg 21(19):1 6, Slavin KV, Burchiel KJ: Use of long-term nerve stimulation with implanted electrodes in the treatment of intractable craniofacial pain. J Neurosurg 92:576, 2000 (Abstract #827) 15. Slavin KV, Nersesyan H, Wess C: Peripheral neurostimulation for treatment of intractable occipital neuralgia. Neurosurgery 58: , Slavin KV, Nersesyan H, Wess C: Treatment of neuropathic craniofacial pain using peripheral nerve stimulation approach, in Meglio M, Krames ES (eds): Proceedings of 7th Meeting of International Neuromodulation Society, Rome, Italy, June 10 13, Bologna: Medimond, 2005, pp Slavin KV, Wess C: Trigeminal branch stimulation for intractable neuropathic pain: technical note. Neuromodulation 8:7 13, Syed M, Slavin KV: Infraclavicular generator placement for neurostimulation: are the patients satisfied? in Meglio M, Krames ES (eds): Proceedings of 7th Meeting of International Neuromodulation Society, Rome, Italy, June 10 13, Bologna: Medimond, 2005, pp Wall PD, Sweet WH: Temporary abolition of pain in man. Science 155: , Weiner RL: Peripheral nerve neurostimulation. Neurosurg Clin N Am 14: , Weiner RL, Aló KM, Reed KL, Fuller ML: Subcutaneous neurostimulation for intractable C-2-mediated headaches. J Neurosurg 94:398A, 2001 (Abstract) 22. Weiner RL, Reed KL: Peripheral neurostimulation for control of intractable occipital neuralgia. Neuromodulation 2: , White JC, Sweet WH: Pain and the Neurosurgeon. A Forty- Year Experience. Springfield, IL: Charles C. Thomas, 1969, pp Manuscript received September 13, Accepted in final form October 25, Address reprint requests to: Konstantin Slavin, M.D., Department of Neurosurgery, M/C 799, 912 South Wood Street, Chicago, Illinois, kslavin@uic.edu. 5
Repositioning of Supraorbital Nerve Stimulation Electrode Using Retrograde Needle Insertion: A Technical Note
 Neuromodulation: Technology at the Neural Interface Received: June 7, 2010 First revision: July 24, 2010 Accepted: July 26, 2010 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2010.00315.x Repositioning
Neuromodulation: Technology at the Neural Interface Received: June 7, 2010 First revision: July 24, 2010 Accepted: July 26, 2010 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2010.00315.x Repositioning
Stimulation Ranges, Usage Ranges, and. Paresthesia Mapping During Occipital Nerve Stimulation. Introduction ORIGINAL ARTICLE ABSTRACT
 NEUROMODULATION: TECHNOLOGY AT THE NEURAL INTERFACE Volume 11 Number 1 2008 http://www.blackwell-synergy.com/loi/ner ORIGINAL ARTICLE Stimulation Ranges, Usage Ranges, and Blackwell Publishing Inc Paresthesia
NEUROMODULATION: TECHNOLOGY AT THE NEURAL INTERFACE Volume 11 Number 1 2008 http://www.blackwell-synergy.com/loi/ner ORIGINAL ARTICLE Stimulation Ranges, Usage Ranges, and Blackwell Publishing Inc Paresthesia
Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine:
 Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Peripheral Nerve S-mula-on
 Peripheral Nerve S-mula-on Konstan-n Slavin, MD Professor, Department of Neurosurgery University of Illinois at Chicago Peripheral Nerve S-mula-on New (?) approach Neuropathic pain syndromes Off label
Peripheral Nerve S-mula-on Konstan-n Slavin, MD Professor, Department of Neurosurgery University of Illinois at Chicago Peripheral Nerve S-mula-on New (?) approach Neuropathic pain syndromes Off label
Medical Policy. Description/Scope. Position Statement. Rationale
 Subject: Document#: Current Effective Date: 06/28/2017 Status: Reviewed Last Review Date: 05/04/2017 Description/Scope This document addresses occipital nerve stimulation (ONS), which involves delivering
Subject: Document#: Current Effective Date: 06/28/2017 Status: Reviewed Last Review Date: 05/04/2017 Description/Scope This document addresses occipital nerve stimulation (ONS), which involves delivering
Peripheral Neurostimulation in Supraorbital Neuralgia Refractory to Conventional Therapy
 CLINICAL REPORT Peripheral Neurostimulation in Supraorbital Neuralgia Refractory to Conventional Therapy Juan M. Asensio-Samper, MD*; Vicente L. Villanueva, MD ; Alfonso V. Pérez, PhD ; María D. López,
CLINICAL REPORT Peripheral Neurostimulation in Supraorbital Neuralgia Refractory to Conventional Therapy Juan M. Asensio-Samper, MD*; Vicente L. Villanueva, MD ; Alfonso V. Pérez, PhD ; María D. López,
Using Peripheral Stimulation to Reduce the Pain of C2-Mediated Occipital Headaches: A Preliminary Report
 Pain Physician 2007; 10:453-460 ISSN 1533-3159 Prospective Case Series Using Peripheral Stimulation to Reduce the Pain of C2-Mediated Occipital Headaches: A Preliminary Report Eugene A. Melvin, Jr., MD
Pain Physician 2007; 10:453-460 ISSN 1533-3159 Prospective Case Series Using Peripheral Stimulation to Reduce the Pain of C2-Mediated Occipital Headaches: A Preliminary Report Eugene A. Melvin, Jr., MD
A Simple Technique for Surgical Placement of Occipital Nerve Stimulators without Anchoring the Lead
 Surgical Technique A Simple Technique for Surgical Placement of Occipital Nerve Stimulators without Anchoring the Lead Mark Plazier 1 Tim Van Camp 2 Tomas Mevnosky 1 Jan Ost 2 Dirk De Ridder 3 Sven Vanneste
Surgical Technique A Simple Technique for Surgical Placement of Occipital Nerve Stimulators without Anchoring the Lead Mark Plazier 1 Tim Van Camp 2 Tomas Mevnosky 1 Jan Ost 2 Dirk De Ridder 3 Sven Vanneste
Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association
 Implanted Peripheral Nerve Stimulator (PNS) Page 1 of 6 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS) for Pain
Implanted Peripheral Nerve Stimulator (PNS) Page 1 of 6 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS) for Pain
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Implanted Peripheral Nerve Stimulator (PNS) for Pain Control Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS)
Implanted Peripheral Nerve Stimulator (PNS) for Pain Control Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS)
Medical Policy Manual. Topic: Peripheral Subcutaneous Field Stimulation Date of Origin: April Section: Surgery Last Reviewed Date: April 2014
 Medical Policy Manual Topic: Peripheral Subcutaneous Field Stimulation Date of Origin: April 2013 Section: Surgery Last Reviewed Date: April 2014 Policy No: 188 Effective Date: July 1, 2014 IMPORTANT REMINDER
Medical Policy Manual Topic: Peripheral Subcutaneous Field Stimulation Date of Origin: April 2013 Section: Surgery Last Reviewed Date: April 2014 Policy No: 188 Effective Date: July 1, 2014 IMPORTANT REMINDER
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache
 Pain Physician 2011; 14:435-440 ISSN 1533-3159 Case Report Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache Natalie H. Strand
Pain Physician 2011; 14:435-440 ISSN 1533-3159 Case Report Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache Natalie H. Strand
Peripheral Subcutaneous Field Stimulation. Description
 Subject: Peripheral Subcutaneous Field Stimulation Page: 1 of 6 Last Review Status/Date: June 2016 Peripheral Subcutaneous Field Stimulation Description Peripheral subcutaneous field stimulation (PSFS,
Subject: Peripheral Subcutaneous Field Stimulation Page: 1 of 6 Last Review Status/Date: June 2016 Peripheral Subcutaneous Field Stimulation Description Peripheral subcutaneous field stimulation (PSFS,
General remarks on Neurorejuvenation Spinal Cord Stimulation (SCS) Program Occipital Nerve Stimulation Gamma-knife for Trigeminal Neuralgia
 General remarks on Neurorejuvenation Spinal Cord Stimulation (SCS) Program Occipital Nerve Stimulation Gamma-knife for Trigeminal Neuralgia Deep brain Stimulation (DBS) Program Neuromodulation is a field
General remarks on Neurorejuvenation Spinal Cord Stimulation (SCS) Program Occipital Nerve Stimulation Gamma-knife for Trigeminal Neuralgia Deep brain Stimulation (DBS) Program Neuromodulation is a field
The Role of the Neuromodulation in Management of Chronic Pain
 The Role of the Neuromodulation in Management of Chronic Pain Adnan Al-Kaisy, MB ChB, FRCA, FFPMRCA, FIPP Clinical Lead of the Pain Management & Neuromodulation Centre Guy s & St Thomas Hospital, London,
The Role of the Neuromodulation in Management of Chronic Pain Adnan Al-Kaisy, MB ChB, FRCA, FFPMRCA, FIPP Clinical Lead of the Pain Management & Neuromodulation Centre Guy s & St Thomas Hospital, London,
Surgical Treatment: Patient Edition
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Case Report. Ilioinguinal Peripheral Nerve Stimulation. Juan A. Ramos, MD 1, Andrew J. McNeil, DO 2, Ted F. Gingrich, MD 3
 Case Report Interventional Pain Management Reports Volume 1, Number 2, pp93-97 2017, American Society of Interventional Pain Physicians Combined Ultrasound and Fluoroscopic Guidance for Percutaneous Ilioinguinal
Case Report Interventional Pain Management Reports Volume 1, Number 2, pp93-97 2017, American Society of Interventional Pain Physicians Combined Ultrasound and Fluoroscopic Guidance for Percutaneous Ilioinguinal
Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain.
 Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
 ORIGINAL ARTICLE Year : 2015 Volume : 63 Issue : 5 Page : 707 711 Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
ORIGINAL ARTICLE Year : 2015 Volume : 63 Issue : 5 Page : 707 711 Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
Occipital Neuromodulation: Ultrasound Guidance for Peripheral Nerve Stimulator Implantation
 papr_381 580..585 CLINICAL REPORT Occipital Neuromodulation: Ultrasound Guidance for Peripheral Nerve Stimulator Implantation Jason S. Eldrige, MD*; Jon B. Obray, MD*, ; Matthew J. Pingree, MD*; Bryan
papr_381 580..585 CLINICAL REPORT Occipital Neuromodulation: Ultrasound Guidance for Peripheral Nerve Stimulator Implantation Jason S. Eldrige, MD*; Jon B. Obray, MD*, ; Matthew J. Pingree, MD*; Bryan
Novel Minimally Invasive Wireless Nanotechnology Neuromodulation System in the Management of Chronic Pain Syndromes
 Novel Minimally Invasive Wireless Nanotechnology Neuromodulation System in the Management of Chronic Pain Syndromes Laura Tyler Perryman* Stimwave Technologies, Inc. 1310 Park Central Blvd South, Pompano
Novel Minimally Invasive Wireless Nanotechnology Neuromodulation System in the Management of Chronic Pain Syndromes Laura Tyler Perryman* Stimwave Technologies, Inc. 1310 Park Central Blvd South, Pompano
Peripheral Neuromodulation and Headaches: History, Clinical Approach, and Considerations on Underlying Mechanisms
 Curr Pain Headache Rep (2013) 17:305 DOI 10.1007/s11916-012-0305-8 CHRONIC DAILY HEADACHE (SJ WANG, SECTION EDITOR) Peripheral Neuromodulation and Headaches: History, Clinical Approach, and Considerations
Curr Pain Headache Rep (2013) 17:305 DOI 10.1007/s11916-012-0305-8 CHRONIC DAILY HEADACHE (SJ WANG, SECTION EDITOR) Peripheral Neuromodulation and Headaches: History, Clinical Approach, and Considerations
Peripheral Nerve Stimulation and Percutaneous Electrical Nerve Stimulation in Pain Management: A Review and Update on Current Status -
 International Journal of Pain & Relief Review Article Peripheral Nerve Stimulation and Percutaneous Electrical Nerve Stimulation in Pain Management: A Review and Update on Current Status - Laura Tyler
International Journal of Pain & Relief Review Article Peripheral Nerve Stimulation and Percutaneous Electrical Nerve Stimulation in Pain Management: A Review and Update on Current Status - Laura Tyler
Affiliation: 1- Departments of Anesthesiology/ Pain Management and Neurology, UCSF School of Medicine 2- Thrive Clinic, LLC, Santa Rosa, CA
 Author Information Prasad Shirvalkar MD, PhD 1 Jason E. Pope MD 2 Affiliation: 1- Departments of Anesthesiology/ Pain Management and Neurology, UCSF School of Medicine 2- Thrive Clinic, LLC, Santa Rosa,
Author Information Prasad Shirvalkar MD, PhD 1 Jason E. Pope MD 2 Affiliation: 1- Departments of Anesthesiology/ Pain Management and Neurology, UCSF School of Medicine 2- Thrive Clinic, LLC, Santa Rosa,
Proven pain therapy. Stimulating results.
 Proven pain therapy. Stimulating results. Living with chronic pain can be difficult. We re here to help. We understand the physical and mental suffering associated with chronic pain. Not being able to
Proven pain therapy. Stimulating results. Living with chronic pain can be difficult. We re here to help. We understand the physical and mental suffering associated with chronic pain. Not being able to
2016 HF10 THERAPY REIMBURSEMENT REFERENCE GUIDE
 206 HF0 THERAPY REIMBURSEMENT REFERENCE GUIDE HF0 therapy, delivered by the Nevro Senza System, is a new high-frequency spinal cord stimulation technology designed to aid in the management of chronic intractable
206 HF0 THERAPY REIMBURSEMENT REFERENCE GUIDE HF0 therapy, delivered by the Nevro Senza System, is a new high-frequency spinal cord stimulation technology designed to aid in the management of chronic intractable
Original Policy Date
 MP 7.01.105 Occipital Nerve Stimulation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy
MP 7.01.105 Occipital Nerve Stimulation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy
Peripheral nerve stimulation for treatment of postherpetic neuralgia: A Case report
 Case report Acta Medica Academica 2011;40(2):187-191 DOI 10.5644/ama2006-124.23 Peripheral nerve stimulation for treatment of postherpetic neuralgia: A Case report Scott C. Palmer 1, Alexis A. Jimenez
Case report Acta Medica Academica 2011;40(2):187-191 DOI 10.5644/ama2006-124.23 Peripheral nerve stimulation for treatment of postherpetic neuralgia: A Case report Scott C. Palmer 1, Alexis A. Jimenez
The Impact of Peripheral Nerve Stimulation on Disability and Depression
 Neuromodulation: Technology at the Neural Interface Received: June 25, 2015 Revised: August 25, 2015 Accepted: September 15, 2015 (onlinelibrary.wiley.com) DOI: 10.1111/ner.12363 The Impact of Peripheral
Neuromodulation: Technology at the Neural Interface Received: June 25, 2015 Revised: August 25, 2015 Accepted: September 15, 2015 (onlinelibrary.wiley.com) DOI: 10.1111/ner.12363 The Impact of Peripheral
HF10 THERAPY 2018 Ambulatory Surgery Center Reimbursement and Coding Reference Guide
 HF10 therapy, delivered by the Nevro Senza System, is the high-frequency spinal cord stimulation technology operated at 10,000 Hz designed to aid in the management of chronic intractable pain of the trunk
HF10 therapy, delivered by the Nevro Senza System, is the high-frequency spinal cord stimulation technology operated at 10,000 Hz designed to aid in the management of chronic intractable pain of the trunk
Sacral neuromodulation (SNM), using permanent foramen S3 electrode, Early versus late treatment of voiding dysfunction with pelvic neuromodulation
 ORIGINAL RESEARCH Early versus late treatment of voiding dysfunction with pelvic neuromodulation Magdy M. Hassouna, MD, PhD; Mohamed S. Elkelini, MD See related article on page 111 Abstract Introduction:
ORIGINAL RESEARCH Early versus late treatment of voiding dysfunction with pelvic neuromodulation Magdy M. Hassouna, MD, PhD; Mohamed S. Elkelini, MD See related article on page 111 Abstract Introduction:
Long-Term Outcome in Occipital Nerve Stimulation Patients With Medically Intractable Primary Headache Disorders
 Neuromodulation: Technology at the Neural Interface Received: April 12, 2012 Revised: June 15, 2012 Accepted: June 27, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2012.00490.x Long-Term Outcome
Neuromodulation: Technology at the Neural Interface Received: April 12, 2012 Revised: June 15, 2012 Accepted: June 27, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2012.00490.x Long-Term Outcome
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
The Treatment of Medically Intractable Trigeminal Autonomic Cephalalgia With Supraorbital/Supratrochlear Stimulation: A Retrospective Case Series
 Neuromodulation: Technology at the Neural Interface Received: October 10, 2011 Revised: February 2, 2012 Accepted: March 12, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2012.00455.x The Treatment
Neuromodulation: Technology at the Neural Interface Received: October 10, 2011 Revised: February 2, 2012 Accepted: March 12, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2012.00455.x The Treatment
H F 1 0 T H E R A P Y R E I M B U R S E M E N T R E F E R E N C E G U I D E
 HF10 therapy, delivered by the Nevro Senza System, is the high-frequency spinal cord stimulation technology designed to aid in the management of chronic intractable pain of the trunk/limbs without paresthesia.
HF10 therapy, delivered by the Nevro Senza System, is the high-frequency spinal cord stimulation technology designed to aid in the management of chronic intractable pain of the trunk/limbs without paresthesia.
Nevro Reimbursement Support
 HF10 therapy, delivered by the Nevro Senza System, is the high-frequency spinal cord stimulation technology operated at 10,000 Hz designed to aid in the management of chronic intractable pain of the trunk
HF10 therapy, delivered by the Nevro Senza System, is the high-frequency spinal cord stimulation technology operated at 10,000 Hz designed to aid in the management of chronic intractable pain of the trunk
Occipital Nerve Stimulation Corporate Medical Policy
 Occipital Nerve Stimulation Corporate Medical Policy File Name: Occipital Nerve Stimulation File Code: UM.SPSVC.14 Origination: 2011 Last Review: 06/2018 Next Review: 06/2019 Effective Date: 10/01/2018
Occipital Nerve Stimulation Corporate Medical Policy File Name: Occipital Nerve Stimulation File Code: UM.SPSVC.14 Origination: 2011 Last Review: 06/2018 Next Review: 06/2019 Effective Date: 10/01/2018
Neurostimulation Systems
 Neurostimulation Systems Expanding the Array of Pain Control Solutions PROVEN EFFECTIVE FOR SIMPLE PAIN ITREL 3 SYSTEM For simple neuropathic pain Totally implantable for enhanced quality of life Easy
Neurostimulation Systems Expanding the Array of Pain Control Solutions PROVEN EFFECTIVE FOR SIMPLE PAIN ITREL 3 SYSTEM For simple neuropathic pain Totally implantable for enhanced quality of life Easy
Take control of your pain therapy. Getting started with Algovita SCS.
 Take control of your pain therapy. Getting started with Algovita SCS. The two-step approach to spinal cord stimulation therapy. You ve talked with your doctor. You ve discussed it with your family. You
Take control of your pain therapy. Getting started with Algovita SCS. The two-step approach to spinal cord stimulation therapy. You ve talked with your doctor. You ve discussed it with your family. You
Cpt code cervicogenic headaches
 P ford residence southampton, ny Cpt code cervicogenic headaches In most cases, it is really hard for sufferers to distinguish such headaches from migraine. It is so because some people with this headache
P ford residence southampton, ny Cpt code cervicogenic headaches In most cases, it is really hard for sufferers to distinguish such headaches from migraine. It is so because some people with this headache
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 3/2018 Origination: 7/2013 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 3/2018 Origination: 7/2013 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Author Information. Presenting Symptom: Burning in right foot> Chronic low back pain
 Author Information Full Names: Erica Patel, MD Kiran V. Patel, MD Presenting Symptom: Burning in right foot> Chronic low back pain Case Specific Diagnosis: Chronic low back pain and radicular pain Learning
Author Information Full Names: Erica Patel, MD Kiran V. Patel, MD Presenting Symptom: Burning in right foot> Chronic low back pain Case Specific Diagnosis: Chronic low back pain and radicular pain Learning
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2018 Origination: 7/2013 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2018 Origination: 7/2013 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Dr Patrick Schweder. Neurosurgeon Department of Neurosurgery Auckland Hospital Auckland
 Dr Patrick Schweder Neurosurgeon Department of Neurosurgery Auckland Hospital Auckland 8:30-9:25 WS #98: Management of Common Neurosurgical Problems in General Practice 9:35-10:30 WS #110: Management of
Dr Patrick Schweder Neurosurgeon Department of Neurosurgery Auckland Hospital Auckland 8:30-9:25 WS #98: Management of Common Neurosurgical Problems in General Practice 9:35-10:30 WS #110: Management of
Peripheral Subcutaneous Field Stimulation
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Spinal Cord Stimulation. OHTAC Recommendation. Spinal Cord Stimulation for the Management of Neuropathic Pain
 OHTAC Recommendation Spinal Cord Stimulation for the Management of Neuropathic Pain March 2, 2005 1 The Ontario Health Technology Advisory Committee (OHTAC) met on March 2, 2005 and reviewed the use of
OHTAC Recommendation Spinal Cord Stimulation for the Management of Neuropathic Pain March 2, 2005 1 The Ontario Health Technology Advisory Committee (OHTAC) met on March 2, 2005 and reviewed the use of
Supraorbital nerve stimulation Cefaly Device - FDA Approved for migraine prevention (also being investigated as acute therapy)
 NEUROSTIMULATION/NEUROMODULATION UPDATE Meyer and Renee Luskin Andrew Charles, M.D. Professor Luskin Chair in Migraine and Headache Studies Director, UCLA Goldberg Migraine Program David Geffen School
NEUROSTIMULATION/NEUROMODULATION UPDATE Meyer and Renee Luskin Andrew Charles, M.D. Professor Luskin Chair in Migraine and Headache Studies Director, UCLA Goldberg Migraine Program David Geffen School
Policy #: 411 Latest Review Date: January 2014
 Name of Policy: Occipital Nerve Stimulation Policy #: 411 Latest Review Date: January 2014 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross
Name of Policy: Occipital Nerve Stimulation Policy #: 411 Latest Review Date: January 2014 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross
Sacral Neuromodulation Beyond Pelvic Pain!!!
 Sacral Neuromodulation Beyond Pelvic Pain!!! Dr. Hirachand S Mutagi. Senior Consultant Pain Physician. Head -Sakra World Hospital. Director ReLeaf Pain Services. Rapid advances in neurostimulation therapy
Sacral Neuromodulation Beyond Pelvic Pain!!! Dr. Hirachand S Mutagi. Senior Consultant Pain Physician. Head -Sakra World Hospital. Director ReLeaf Pain Services. Rapid advances in neurostimulation therapy
Surgical Lead Implantation Guide
 Surgical Lead Implantation Guide Neurostimulation Therapy for Chronic Pain Innovating for life. Medtronic, PrimeAdvanced, Restore, RestoreAdvanced, RestoreUltra, and Specify are registered trademarks of
Surgical Lead Implantation Guide Neurostimulation Therapy for Chronic Pain Innovating for life. Medtronic, PrimeAdvanced, Restore, RestoreAdvanced, RestoreUltra, and Specify are registered trademarks of
2 016 HF10 THERAPY HOSPITAL OUTPATIENT DEPARTMENT AND AMBULATORY SURGERY CENTER REIMBURSEMENT REFERENCE GUIDE
 HF10 therapy, delivered by the Nevro Senza System, is a new high-frequency spinal cord stimulation technology designed to aid in the management of chronic intractable pain of the trunk/limbs, including
HF10 therapy, delivered by the Nevro Senza System, is a new high-frequency spinal cord stimulation technology designed to aid in the management of chronic intractable pain of the trunk/limbs, including
Phenotype of patients responsive to occipital nerve stimulation for refractory head pain
 Phenotype of patients responsive to occipital nerve stimulation for refractory head pain Koen Paemeleire 1*, MD, PhD, Jean-Pierre Van Buyten 2*, MD, Machteld Van Buynder 2, Dario Alicino 2, MD, Georges
Phenotype of patients responsive to occipital nerve stimulation for refractory head pain Koen Paemeleire 1*, MD, PhD, Jean-Pierre Van Buyten 2*, MD, Machteld Van Buynder 2, Dario Alicino 2, MD, Georges
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: occipital_nerve_stimulation 8/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Occipital nerve
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: occipital_nerve_stimulation 8/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Occipital nerve
Occipital Nerve Stimulation Corporate Medical Policy
 Occipital Nerve Stimulation Corporate Medical Policy File name: Occipital Nerve Stimulation File code: UM.SPSVC.14 Origination: 2011 Last Review: 11/2017 Next Review: 11/2018 Effective Date: 05/01/2018
Occipital Nerve Stimulation Corporate Medical Policy File name: Occipital Nerve Stimulation File code: UM.SPSVC.14 Origination: 2011 Last Review: 11/2017 Next Review: 11/2018 Effective Date: 05/01/2018
Face. Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face
 Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Trigeminal neuralgia (TN) is characterized by sudden, severe, brief, Peripheral neuromodulation for the treatment of refractory trigeminal neuralgia
 case report Peripheral neuromodulation for the treatment of refractory trigeminal neuralgia Naum Shaparin MD, Karina Gritsenko MD, Diego Fernandez Garcia-Roves MD, Ushma Shah MD, Todd Schultz MD, Oscar
case report Peripheral neuromodulation for the treatment of refractory trigeminal neuralgia Naum Shaparin MD, Karina Gritsenko MD, Diego Fernandez Garcia-Roves MD, Ushma Shah MD, Todd Schultz MD, Oscar
Coding for Sacral Neuromodulation
 301.273.0570 Fax 301.273.0778 Coding for Sacral Neuromodulation Sacral Neuromodulation (SNS) is a widely used technique in Female Pelvic Medicine and Reconstructive Surgery (FPMRS), with several FDA-approved
301.273.0570 Fax 301.273.0778 Coding for Sacral Neuromodulation Sacral Neuromodulation (SNS) is a widely used technique in Female Pelvic Medicine and Reconstructive Surgery (FPMRS), with several FDA-approved
Case Report WIRELESS HIGH FREQUENCY SPINAL CORD STIMULATION FOR THE TREATMENT OF POST-HERPETIC OCULAR NEURALGIA: A CASE REPORT
 Case Report Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 5, pp167-171 2018, American Society of Interventional Pain Physicians WIRELESS HIGH FREQUENCY SPINAL CORD STIMULATION
Case Report Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 5, pp167-171 2018, American Society of Interventional Pain Physicians WIRELESS HIGH FREQUENCY SPINAL CORD STIMULATION
Neurostimulation. Spinal cord stimulators use electrodes placed in the space surrounding the spinal cord (epidural space).
 Neurostimulation.305145613.pdf 1 8/11/12 11:32 PM Neurostimulation Neurostimulation, also called electrostimulation, uses low-level electrical impulses to interfere with pain signals or block them from
Neurostimulation.305145613.pdf 1 8/11/12 11:32 PM Neurostimulation Neurostimulation, also called electrostimulation, uses low-level electrical impulses to interfere with pain signals or block them from
Forward Looking Statements and Further Information
 JANUARY 2015 [ 1 ] Forward Looking Statements and Further Information SPECIAL NOTE REGARDING FORWARD-LOOKING STATEMENTS This presentation contains forward-looking statements. All statements other than
JANUARY 2015 [ 1 ] Forward Looking Statements and Further Information SPECIAL NOTE REGARDING FORWARD-LOOKING STATEMENTS This presentation contains forward-looking statements. All statements other than
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
2014 AAPM 56 th Annual Meeting
 2014 AAPM 56 th Annual Meeting SAM Diagnostic Radiology MR Safety - Deep Brain Stimulator and Other Neurostimulators Yunhong Shu, Ph.D. Mayo Clinic, Rochester, MN Outline Background of Neurostimulator
2014 AAPM 56 th Annual Meeting SAM Diagnostic Radiology MR Safety - Deep Brain Stimulator and Other Neurostimulators Yunhong Shu, Ph.D. Mayo Clinic, Rochester, MN Outline Background of Neurostimulator
B ILATERAL trigeminal neuralgia has been reported
 J Neurosurg 67:44-48, 1987 Bilateral trigeminal neuralgia RONALD BR1SMAN, M.D. Department of Neurological Surgery, The Neurological Institute of New York, Columbia University College of Physicians and
J Neurosurg 67:44-48, 1987 Bilateral trigeminal neuralgia RONALD BR1SMAN, M.D. Department of Neurological Surgery, The Neurological Institute of New York, Columbia University College of Physicians and
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_cord_stimulation 3/1980 10/2017 10/2018 10/2017 Description of Procedure or Service Spinal cord stimulation
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_cord_stimulation 3/1980 10/2017 10/2018 10/2017 Description of Procedure or Service Spinal cord stimulation
Neuromodulation techniques for treatment of refractory neuropathic pain
 Article ID: WMC004271 ISSN 2046-1690 Neuromodulation techniques for treatment of refractory neuropathic pain Corresponding Author: Prof. Angelo Lavano, Full Professor of Neurosurgery, Department of Neurosurgery,
Article ID: WMC004271 ISSN 2046-1690 Neuromodulation techniques for treatment of refractory neuropathic pain Corresponding Author: Prof. Angelo Lavano, Full Professor of Neurosurgery, Department of Neurosurgery,
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP
 INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group
 Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group This information leaflet contains information about DBS and should answer some of your questions. If
Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group This information leaflet contains information about DBS and should answer some of your questions. If
Occipital Nerve Stimulation
 Occipital Nerve Stimulation Policy Number: 7.01.125 Last Review: 5/2018 Origination: 5/2006 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
Occipital Nerve Stimulation Policy Number: 7.01.125 Last Review: 5/2018 Origination: 5/2006 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
Sustained Effectiveness of Occipital Nerve Stimulation in Drug-Resistant Chronic Cluster Headachehead_
 Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.01973.x Published by Wiley Periodicals, Inc. Research Submissions Sustained Effectiveness of Occipital Nerve in Drug-Resistant
Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.01973.x Published by Wiley Periodicals, Inc. Research Submissions Sustained Effectiveness of Occipital Nerve in Drug-Resistant
INTEROFFICE MEMORANDUM. TO: Professor K. LaGrandeur FROM: SUBJECT: Audience Analysis for project 4 DATE: 12/17/06
 INTEROFFICE MEMORANDUM TO: Professor K. LaGrandeur FROM: SUBJECT: Audience Analysis for project 4 DATE: 12/17/06 PURPOSE: The purpose of this memorandum is to present an analysis of the individuals who
INTEROFFICE MEMORANDUM TO: Professor K. LaGrandeur FROM: SUBJECT: Audience Analysis for project 4 DATE: 12/17/06 PURPOSE: The purpose of this memorandum is to present an analysis of the individuals who
MD, FA F ANS N, FA F C A S
 Advances in Neurostimulation for Pain Joshua M. Rosenow, MD, FAANS, FACS Director, Functional Neurosurgery Associate Professor, Departments of Neurosurgery, Neurology and Physical Medicine and Rehabilitation
Advances in Neurostimulation for Pain Joshua M. Rosenow, MD, FAANS, FACS Director, Functional Neurosurgery Associate Professor, Departments of Neurosurgery, Neurology and Physical Medicine and Rehabilitation
Sacral Nerve Stimulation (SNS) System Implantation
 Patient & Family Guide 2016 Sacral Nerve Stimulation (SNS) System Implantation www.nshealth.ca Sacral Nerve Stimulation (SNS) System Implantation SNS system implantation involves placing a lead ( leed,
Patient & Family Guide 2016 Sacral Nerve Stimulation (SNS) System Implantation www.nshealth.ca Sacral Nerve Stimulation (SNS) System Implantation SNS system implantation involves placing a lead ( leed,
Guidance on competencies for Spinal Cord Stimulation Reviewed
 Guidance on competencies for Spinal Cord Stimulation Reviewed 2016 Endorsed by: Contents Introduction A: Core competencies for practitioners in Pain Medicine Page 2 4 Appendix A: Curriculum 5 B: Competencies
Guidance on competencies for Spinal Cord Stimulation Reviewed 2016 Endorsed by: Contents Introduction A: Core competencies for practitioners in Pain Medicine Page 2 4 Appendix A: Curriculum 5 B: Competencies
Surgical deactivation of frontal migraine trigger RECONSTRUCTIVE
 RECONSTRUCTIVE The Anatomical Morphology of the Supraorbital Notch: Clinical Relevance to the Surgical Treatment of Migraine Headaches Michael Fallucco, M.D. Jeffrey E. Janis, M.D. Robert R. Hagan, M.D.
RECONSTRUCTIVE The Anatomical Morphology of the Supraorbital Notch: Clinical Relevance to the Surgical Treatment of Migraine Headaches Michael Fallucco, M.D. Jeffrey E. Janis, M.D. Robert R. Hagan, M.D.
Surgical Leads. Directions for Use. CAUTION: Federal law restricts this device to sale, distribution and use by or on the order of a physician.
 Surgical Leads Directions for Use CAUTION: Federal law restricts this device to sale, distribution and use by or on the order of a physician. 91078747-08 Content: 92190987 REV A Guarantees Boston Scientific
Surgical Leads Directions for Use CAUTION: Federal law restricts this device to sale, distribution and use by or on the order of a physician. 91078747-08 Content: 92190987 REV A Guarantees Boston Scientific
RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY
 RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY INFORMATION AND CONSENT FOR IMPLANT SURGERY PURPOSE OF THIS FORM: State law requires
RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY INFORMATION AND CONSENT FOR IMPLANT SURGERY PURPOSE OF THIS FORM: State law requires
Anterior Ethmoidal Nerve Overview
 Anterior Ethmoidal Nerve Overview Name Anterior Ethmoidal Nerve Latin Nervus Ethmoidalis anterior Etymology Pain Differential Diagnosis - Enrico Dellacà M.D Ph.D. Nerve from Latin nervus meaning sinew,
Anterior Ethmoidal Nerve Overview Name Anterior Ethmoidal Nerve Latin Nervus Ethmoidalis anterior Etymology Pain Differential Diagnosis - Enrico Dellacà M.D Ph.D. Nerve from Latin nervus meaning sinew,
Complex Regional Pain Syndrome: Manifestations and the Role of Neurostimulation in Its Management
 S20 Journal of Pain and Symptom Management Vol. 31 No. 4S April 2006 Special Article Complex Regional Pain Syndrome: Manifestations and the Role of Neurostimulation in Its Management Michael Stanton-Hicks
S20 Journal of Pain and Symptom Management Vol. 31 No. 4S April 2006 Special Article Complex Regional Pain Syndrome: Manifestations and the Role of Neurostimulation in Its Management Michael Stanton-Hicks
Summary of Selected Spinal Cord Stimulation Studies
 Randomized Controlled Trials Kemler, et al. Effect of for chronic complex regional pain syndrome Type I: five-year final follow-up of patients in a randomized controlled trial. Neurosurg 2008. Kemler,
Randomized Controlled Trials Kemler, et al. Effect of for chronic complex regional pain syndrome Type I: five-year final follow-up of patients in a randomized controlled trial. Neurosurg 2008. Kemler,
MEDICAL CORPORATION Asbury Rd., P.O. Box 758, Farmingdale, NJ USA Fax
 MEDICAL CORPORATION 5206 Asbury Rd., P.O. Box 758, Farmingdale, NJ 07727 USA 732-938-2266 800-323-4035 Fax 732-938-2399 MYO/WIRE Temporary Cardiac Pacing Wire System MYO/WIRE temporary cardiac pacing wires.
MEDICAL CORPORATION 5206 Asbury Rd., P.O. Box 758, Farmingdale, NJ 07727 USA 732-938-2266 800-323-4035 Fax 732-938-2399 MYO/WIRE Temporary Cardiac Pacing Wire System MYO/WIRE temporary cardiac pacing wires.
Tikrit University College of Dentistry Dr.Ban I.S. head & neck anatomy 2 nd y.
 Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Deep Brain Stimulation (DBS) For patients with tremor
 Patient Education Deep Brain Stimulation (DBS) For patients with tremor Please read this handout before reading and signing the form Special Consent for Procedural Treatment. This handout describes how
Patient Education Deep Brain Stimulation (DBS) For patients with tremor Please read this handout before reading and signing the form Special Consent for Procedural Treatment. This handout describes how
Occipital Nerve Stimulation for Headache Disorders
 Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Occipital Nerve Stimulation for Headache Disorders Koen Paemeleire* and Thorsten Bartsch *Department of Neurology,
Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Occipital Nerve Stimulation for Headache Disorders Koen Paemeleire* and Thorsten Bartsch *Department of Neurology,
DRUG-FREE PAIN MANAGEMENT THERAPY MOVE FORWARD FASTER
 DRUG-FREE PAIN MANAGEMENT THERAPY MOVE FORWARD FASTER THE SPRINT PNS SYSTEM IS A 60-DAY TREATMENT INTENDED TO HELP YOU GET BACK TO THE LIFE YOU WANT WITHOUT OPIOIDS OR PERMANENT IMPLANTS. IT USES A PULSE
DRUG-FREE PAIN MANAGEMENT THERAPY MOVE FORWARD FASTER THE SPRINT PNS SYSTEM IS A 60-DAY TREATMENT INTENDED TO HELP YOU GET BACK TO THE LIFE YOU WANT WITHOUT OPIOIDS OR PERMANENT IMPLANTS. IT USES A PULSE
Sacral Neuromodulation for Dysfunctional Voiders Workshop 1 Monday, August 23, 09:00 10:30
 Sacral Neuromodulation for Dysfunctional Voiders Workshop 1 Monday, August 23, 09:00 10:30 Time Time Topic Speaker 09:00 09:05 Introduction to the aims of the workshop and the Magdy Hassouna participants
Sacral Neuromodulation for Dysfunctional Voiders Workshop 1 Monday, August 23, 09:00 10:30 Time Time Topic Speaker 09:00 09:05 Introduction to the aims of the workshop and the Magdy Hassouna participants
Percutaneous Electrical Nerve Stimulation (PENS) and Percutaneous Neuromodulation Therapy (PNT)
 Percutaneous Electrical Nerve Stimulation (PENS) and Percutaneous Neuromodulation Therapy (PNT) Policy Number: 7.01.29 Last Review: 3/2018 Origination: 10/1988 Next Review: 3/2019 Policy Blue Cross and
Percutaneous Electrical Nerve Stimulation (PENS) and Percutaneous Neuromodulation Therapy (PNT) Policy Number: 7.01.29 Last Review: 3/2018 Origination: 10/1988 Next Review: 3/2019 Policy Blue Cross and
INFORMED-CONSENT-REDUCTION MAMMAPLASTY
 INFORMED-CONSENT-REDUCTION MAMMAPLASTY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and
INFORMED-CONSENT-REDUCTION MAMMAPLASTY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy
 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Carpal Tunnel Release
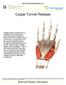 Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
Dr P.W.Buczkowski. Consultant in Anaesthesia & Pain Medicine. Royal Derby Hospital
 Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
cally, a distinct superior crease of the forehead marks this spot. The hairline and
 4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
Effective Date: 01/01/2012 Revision Date: Code(s): Application of surface (transcutaneous) neurostimulator
 ARBenefits Approval: 10/19/2011 Effective Date: 01/01/2012 Revision Date: Code(s): 64550 Application of surface (transcutaneous) neurostimulator Medical Policy Title: Electrical Stimulation, Transcutaneous
ARBenefits Approval: 10/19/2011 Effective Date: 01/01/2012 Revision Date: Code(s): 64550 Application of surface (transcutaneous) neurostimulator Medical Policy Title: Electrical Stimulation, Transcutaneous
Management Of Posttraumatic Spinal Instability (Neurosurgical Topics, No 3) READ ONLINE
 Management Of Posttraumatic Spinal Instability (Neurosurgical Topics, No 3) READ ONLINE If you are searching for a ebook Management of Posttraumatic Spinal Instability (Neurosurgical Topics, No 3) in pdf
Management Of Posttraumatic Spinal Instability (Neurosurgical Topics, No 3) READ ONLINE If you are searching for a ebook Management of Posttraumatic Spinal Instability (Neurosurgical Topics, No 3) in pdf
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
Jessica Jameson MD Post Falls, ID
 Jessica Jameson MD Post Falls, ID Discuss the history of interventiona l pain Discuss previous tools to manage chronic pain Discuss current novel therapies to manage chronic pain and indications HISTORY
Jessica Jameson MD Post Falls, ID Discuss the history of interventiona l pain Discuss previous tools to manage chronic pain Discuss current novel therapies to manage chronic pain and indications HISTORY
Peripheral Nerve Stimulation
 Peripheral Nerve Stimulation Progress in Neurological Surgery Vol. 24 Series Editor L. Dade Lunsford Pittsburgh, Pa. Peripheral Nerve Stimulation Volume Editor Konstantin V. Slavin Chicago, Ill. 59 figures,
Peripheral Nerve Stimulation Progress in Neurological Surgery Vol. 24 Series Editor L. Dade Lunsford Pittsburgh, Pa. Peripheral Nerve Stimulation Volume Editor Konstantin V. Slavin Chicago, Ill. 59 figures,
T.E.N.S (Transcutaneous Electrical Nerve Stimulation)
 You have been prescribed a T.E.N.S machine to help in the management of your pain. You should use it only for the condition for which it is prescribed. Not all pain will respond to the use of T.E.N.S and
You have been prescribed a T.E.N.S machine to help in the management of your pain. You should use it only for the condition for which it is prescribed. Not all pain will respond to the use of T.E.N.S and
OCCIPITAL NEURALGIA AND HEADACHE TREATMENT
 UnitedHealthcare Commercial Medical Policy OCCIPITAL NEURALGIA AND HEADACHE TREATMENT Policy Number: NEU027 Effective Date: April 1, 2019 Table of Contents Page COVERAGE RATIONALE... 1 DEFINITIONS... 1
UnitedHealthcare Commercial Medical Policy OCCIPITAL NEURALGIA AND HEADACHE TREATMENT Policy Number: NEU027 Effective Date: April 1, 2019 Table of Contents Page COVERAGE RATIONALE... 1 DEFINITIONS... 1
