A Simple Technique for Surgical Placement of Occipital Nerve Stimulators without Anchoring the Lead
|
|
|
- Gervais Cummings
- 5 years ago
- Views:
Transcription
1 Surgical Technique A Simple Technique for Surgical Placement of Occipital Nerve Stimulators without Anchoring the Lead Mark Plazier 1 Tim Van Camp 2 Tomas Mevnosky 1 Jan Ost 2 Dirk De Ridder 3 Sven Vanneste 4 1 Department of Neurosurgery, University Hospital Antwerp, Antwerp, Belgium 2 Department of Neurosurgery/Brai2n, St-Augustinus, Antwerp, Belgium 3 Department of Neurosurgery, University of Otago, Dunedin, New Zealand 4 Behavioral and Brain Sciences, University of Texas at Dallas, Dallas,Texas,UnitedStates Address for correspondence Sven Vanneste, PhD, Behavioral and Brain Sciences, University of Texas at Dallas, 1966 Inwood Road, Dallas, TX 75235, United States ( sven.vanneste@utdallas.edu). JNeurolSurgA Abstract Introduction Greater occipital nerve stimulation is applied in the treatment of occipital neuralgia, headache, and fibromyalgia. Multiple techniques have been described along with their subsequent complications. The most frequent complications are related to lead migration, infection, and undesired stimulation effects. Revision surgery occurs in up to 60% of the cases. Patients and Methods A total of 92 implantations, 51 trials (6 10 weeks), and 41 permanent implantations (follow-up: months) were performed in a single center using a simple technique without an anchoring device. The electrode is tunneled at a 45-degree angle to prevent migration. Complications and additional surgeries were recorded during the follow-up period. Keywords occipital nerve stimulation technique migration anchoring sharp angle Results All patients had bilateral greater occipital nerve stimulation. A total of 16 complications (17.4%) occurred. Seven patients (7.6%) underwent additional surgery. The major complication was infection; lead migration made up only 3.3% of the complications. Conclusions We present a simple technique without the use of an anchoring device that is feasible in achieving bilateral occipital nerve stimulation and decreases the complications, especially lead migration. Introduction Since Wall and Sweet came up with the concept of peripheral nerve stimulation for the treatment of pain in 1967, a lot of interest has been shown. 1 However, the publications in this field were rare in those days because of the invasive methods used to apply the technique. Peripheral nerve stimulation included the dissection of the targeted nerve, placing an electrode next to it. This demanded big exposures and certain surgical skills. Greater occipital nerve stimulation was performed in a similar way. 2 Greater occipital nerve stimulation has been applied for a variety of pain syndromes such as chronic migraine, occipital neuralgia, cluster headache, and fibromyalgia. 3 6 Since the publication of Weiner and Reed in 1999, the burden of surgery has changed. They presented a minimally invasive method that places an electrode at the greater received June 5, 2015 accepted July 3, 2015 Georg Thieme Verlag KG Stuttgart New York DOI /s ISSN
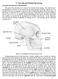
2 occipital nerve dermatome using a Tuohy needle. 7 This method shifted the focus back to the treatment of pain by stimulating the peripheral nerve. Multiple techniques have been described making use of single leads, multiple leads, cylindrical percutaneous leads, and surgical leads in multiple directions and ways. 4 Each of these methods has its own benefits and complications. However, each surgery involves complications and their management. The complications are well described for occipital nerve stimulation. The most common ones are lead migration, infection, undesired stimulation effects, and hardware failure Among them, lead migration gives rise to revision surgery rates up to 33% at 6 months after stimulation. 8,10,11 A few techniques are proposed to prevent migration. Anchoring of the lead, with or without anchoring devices, and the appliance of strain relief loops are widely used to prevent migration. 10,12,13 Anchoring can be performed in multiple ways. It can be done with a simple nonresorbable stitch (which might increase the risk of damaging the electrode) or by making use of anchoring devices, produced by most of the major neuromodulation industry companies. 10 The anchoring technique is important; however, the substance anchored to is even more critical. Solid vast tissue is needed to anchor the lead. Suitable tissue at the high cervical area may be difficult to find. The periost and the fascia are excellent tissues for this purpose. Finding these tissues and fixing the anchoring device demands particular skills in dissection and sometimes a bigger exposure. The anchoring device also demands a certain exposure of tissue. Various techniques have been described ranging from medial fixation to lateral fixation behind the ear All of these techniques have their benefits and drawbacks. In surgery the simplicity of the technical procedure limits the number of complications. We present a simple technique for occipital nerve stimulation that minimizes lead migration without the use of an anchoring device. inion is shaved, and the midline marked with a surgical marker. Subsequently a point is marked on the midline 1 cm underneath the inion. This is defined as 0 cm on the horizontal axis where the center of the electrode has to be positioned. The electrode array length of the lead (Octrode, St. Jude Medical, Plano, Texas, United States) is 5.2 cm, so 2.6 cm of the array should be positioned to the left of the marked point and 2.6 cm to the right. A line of 5.2 cm is drawn at the back of the head, just underneath the inion on an imaginary line between the two pinnae of the ears, projecting the electrode location and incision location. Subsequently a second line is drawn to project the subcutaneous tunneling trajectory. This line departs from the incision side and is in a 45-degree angle with the electrode position. This angle prevents the electrode from migrating ( Fig. 1). Depending on the side of the permanent implantable pulse generator (IPG), a knife-stab incision is made either at the left end or the right end of this line (the lead will cross the midline, so the incision is made at the opposite site of the permanent IPG). A slightly curved Tuohy needle is marked at 5.2 cm, the length of the electrode, measured from the tip. The Tuohy needle is inserted in the subcutaneous tissue just above the periost and deep enough to prevent lead tip erosion. The needle is advanced until the mark of 5.2 cm is reached. The next step is to tunnel the subcutaneous trajectory for the electrode. A sharp tunneling device is used to tunnel the electrode to the cutaneous exit site for a trial electrode or to a Methods Patients Overall, 92 implantations were performed at the University Hospital Antwerp. Patients were implanted during the period 2007 to Of these, 41 patients were implanted with a permanent system, that is, an electrode, an extension lead, and an internal pulse generator (follow-up time ranged from 36 to 76 months). Fifty-one patients were implanted with a trial lead for a period ranging between 6 and 10 weeks. All complications related to the device and the procedures were registered during the follow-up time. Surgical Procedure Patients get implanted under local anesthesia for the trial procedure and under general anesthesia for permanent implantation. Patients are positioned in the prone position with their head resting on a horseshoe headrest, creating a mild flexion of the cervical spine. The area of skin underneath the Fig. 1 A schematic overview of the trial implantation. The electrode is positioned just underneath the inion in that way that four contact points are positioned at the left side and four contact points at the right side. The electrode is tunneled at a 45-degree angle to prevent migration. The lead exits the subcutaneous tissue just underneath the hairline.
3 subcutaneous pocket at the cervical area for the permanent implantation. As soon as both the tunneling device and the Tuohy needle are in place, the stylus is removed and the lead is advanced inside the Tuohy needle until the tip of the needle is reached. The Tuohy needle is retracted making use of the hold-pull technique, and the lead is advanced through the plastic sheet of the tunneling device. The plastic sheet is removed, and the lead is pulled through just until it fits into place in the incision and lies completely in the subcutaneous tissue. If desired, the electrode can be anchored at the 45- degree angle at the incision site with a nonresorbable stitch; however, we did not perform this in the patient population described here. Concerning the trial implantation, the electrode can be tunneled to an exit point just at the hairline at the end of the tunneling trajectory. At this site, the electrode can be sutured to the skin with a nonresorbable suture or with the help of an anchoring device. For the permanent implantation, a second incision is made at the midcervical area, just 3 cm lateral to the midline in a horizontal direction. A subcutaneous pocket is created ( 1 1 cm) to provide space for a strain relief loop in the lead at this highly mobile point. After forming the strain relief loop, the electrode can be tunneled either to the IPG or to an extension lead, depending on the preferred location of the IPG. We preferred the gluteal area to implant the IPG. A horizontal incision is made, in accordance with the size of the IPG, at the gluteal area, and a subcutaneous pocket is made. At the midscapular area, a 2-cm longitudinal paravertebral incision is made. The lead of the electrode is tunneled from the cervical pocket, after creating the strain relief loop, to this pocket. A connection with an extension lead is made, and after creating another strain relief loop at this location, the extension lead is tunneled to the IPG pocket at the gluteal area to connect it with the IPG ( Fig. 2). Outcome Parameters During the follow-up periods, the following complications were recorded: 1. Hardware-related complications: lead migration, lead tip erosion, erosion of the extension connection, lead breakage 2. Biological complications: infection, allergic response to material, local irritation by material 3. Stimulation-related complications: muscle spasms, painful skin stimulation Besides these complications, all patient-reported complications were recorded as well. Treatment and especially revision surgeries or explant surgical treatments of these complications were also noted. Results Patients: Trial Implantations A total of 51 patients were implanted with trial leads (6 men and 45 women). The mean age was 47 years (mean: years). Mean duration of trial implantation Fig. 2 A schematic overview of the permanent implantation. The electrode is positioned in a similar way as shown in Fig. 1. A strain relief loop is created at the midcervical area and underneath the connection with the extension lead at the midscapular area. The extension lead is tunneled to the pocket where the internal pulse generator is positioned. was 7 weeks (mean: weeks). All patients were implanted in accordance with the technique previously described. Patients: Permanent Implantation A total of 41 patients were implanted with a permanent stimulation device (5 men and 36 women). The mean age was 49 years (mean: years). Mean duration of implantation was 45 months (mean: months). Complications and Additional Surgeries: Trial Implantation All the data of the 51 implantations were analyzed. During the trial implantation, 10 complications related to the device or procedure occurred and were registered (19.6%). Lead migration occurred in two patients (3.9%); six patients experienced infection of the subcutaneous tissue (11.8%); one patient had an allergic reaction to the material (2.0%); and one patient experienced undesirable stimulation effects that resulted in pain at the stimulation site (2.0%) ( Table 1). Four patients underwent surgery to treat the complication (9.8%). Both of the patients experiencing lead migration underwent lead revision. Infections were treated with oral
4 Table 1 Complications in the trial implantations and in the permanent implantations population Complication Trial implantations N ¼ 51 (%) Hardware related Connection extension lead erosion 0 1 (2.4) Lead tip erosion 0 1 (2.4) Lead migration 2 (3.9) 1 (2.4) Biological Infection 6 (11.8) 1 (2.4) Allergic response to implant material 1 (2) 0 Persistent pain at implant site 0 1 (2.4) Simulation related Muscle spasms 0 0 Undesirable stimulation effects (pain, anxiety) 1 (2) 1 (2.4) Total 10 (19.6) 6 (14.6) Permanent implantations N ¼ 41 (%) antibiotics and resulted in complete resolution, except for two patients whose condition required lead explantation. The patient with an allergic reaction to the material underwent surgery to explant the lead. The undesired stimulation was treated by reprogramming the stimulation parameters ( Table 2). Complications and Additional Surgeries: Permanent Implantation All the data of the 41 implantations were analyzed. During the permanent implantation with a mean follow-up of 45 months, a total of six complications related to the device and procedure occurred (14.6%). Of these six complications, five patients required revision surgery (12.2%). Lead migration occurred in one patient, leading to revision surgery (2.4%). Lead tip erosion occurred in one patient, leading to revision surgery of the tip (2.4%). One patient experienced erosion of the connection piece of the extension lead, resulting in local revision surgery (2.4%). One patient got a subcutaneous infection at the lead insertion site that was resolved by local wound debridement, leaving the electrode in place (2.4%), and one patient kept complaining of the undesirable effects of stimulation (skin fiber stimulation) that was resolved by revision of the lead tip (2.4%). Discussion We present a simple technique to perform greater occipital nerve stimulation that seems to be feasible in both achieving the desired effect (bilateral greater occipital nerve stimulation) and reducing complications related to the procedure and device. One of the advantages of the technique is that it does not require anchoring devices in the occipital area. The goal of surgery is defined as stimulation of both of the main branches of the greater occipital nerve, without undesired stimulation that results in muscle spasms and/or skin stimulation. The position of the electrode is of major importance to achieve this goal. It should be neither too superficial nor too deep, which might cause undesired stimulation effects; nor should it be too low in the cervical area. Table 2 Adverse events leading to additional surgery Additional surgery Complications Total implantations N ¼ 92 (%) Trial implantations N ¼ 51 (%) Revision surgery All 7 (7.6) 2 (3.9) 5 (12.2) Lead migration 3 (3.3) 2 (3.9) 1 (2.4) Lead tip erosion 1 (1.1) 0 1 (2.4) Extension erosion 1 (1.1) 0 1 (2.4) Infection 1 (1.1) 0 1 (2.4) Undesirable simulation 1 (1.1) 0 1 (2.4) effects Leads explanted All 3 (3.3) 3 (5.9) 0 Allergic response to 1 (1.1) 1 (2) 0 implant materials Infection 2 (2.2) 2 (3.9) 0 Permanent implantations N ¼ 41 (%)
5 Hayek et al published their findings on lead positioning in relation to neurostimulation-induced muscle spasms. They advised lead placement at the level of the nuchal line to prevent undesired stimulation effects. 16 According to an autopsy study published by Bovim et al, the main branches arise in a square area of 2 to 5 cm underneath the inion and up to 3 cm lateral of the inion. 17 This implies that placement just underneath the inion would likely result in stimulation of the main branches. Furthermore, it has the advantage of stimulating an area above the cervical muscles, preventing muscle spasms. In our experience we achieved stimulation in both branches without muscle spasms in all of our implantations, suggesting this one lead method is feasible in achieving the desired stimulation effects. One patient (2.2%) had undesired stimulation effects that stemmed from painful skin stimulation. This was caused by a superficial position of the tip of the electrode that required revision surgery. This confirms the importance of placing the electrode at the right depth. Besides achieving the desired results, prevention of complications is of major interest. With our technique we had a total of 10 complications in the group of trial implantations; 5 of them required revision surgery. Most of the complications were biological and caused by infection at the lead exit site (6 of 10). One should keep in mind that the trial period ranged from 6 to 10 weeks, which is rather long and might provoke infection. Two electrodes were removed because of extensive infection; the other was treated with oral antibiotics. Lead migration occurred in two cases requiring revision surgery. During the trial period, the electrode was sutured to the skin at the exit point. If the sutures resorbed and patients were incautious by pulling on the electrode, migration might occur. Concerning the permanent implantations, we saw a total of six complications (14.6%) five (12.2%) of which resulted in additional surgery. Lead migration occurred in one patient (2.4%) and resulted in revision surgery. This is a low number compared with the literature. The other complications arose out of erosion, infection, and undesired stimulation effects (skin stimulation). The overall number of 16 complications makes up 17.4% of the implantations, requiring 7 additional surgeries (7.6%). This is low compared with the literature, which describes a revision rate between 10% and 60%. 10 Lead migration in particular seems to be one of the major problems, and the risk seems to increase with the follow-up period. 9 In our series we saw a total of 3 lead migration in 92 implantations (3.3%); in the permanent implants we saw one migration (2.4%). The follow-up in this group ranges from 3 to > 6years. This migration occurred within 12 months after the initial implantation of the permanent electrode ( Fig. 3). In comparison with the numbers published in the review of Falowski et al, this is a very low percentage, which may imply that the presented technique is effective to prevent migration. 10 In our technique we make use of a sharp angle of 45 degrees after placing the contacts at the horizontal line underneath the occipital protuberans. This 45-degree angle might prevent migration of the lead because the lead is less bendable and flexible at the level of the contact points. Because of this, it is Fig. 3 Migration of the C2 electrode. unlikely that it will migrate in the direction of 45 degrees. One could be concerned about lead breakage because of traction at the electrode in the angle; however, we have not seen any lead breakage so far. Besides the 45-degree angle, we have created a strain relief loop at the cervical area. We did this because of the high mobility of this region. The strain relief loop provides extra movement possibilities without pulling on the lead at the level of the contact points. Our most pronounced complication was infection. A total of seven patients (7.6%) suffered from infection at the implant site. This is relatively high in comparison with published data that report infection rates between 2% and 10%. 10 However, six of these infections occurred during the trial period, which was relatively long (6 10 weeks). Four of these infections were treated with antibiotics. Two electrodes needed to be removed because of the extensiveness of the infection. Concerning the permanent trials, we noticed one infection that could be treated with antibiotics and did not require further surgery. Taking into account these facts and numbers, we conclude that the high infection rate was due to the long trial period. Two patients had erosion of the hardware, requiring additional surgery (2.2%). In one patient we noticed an erosion of the lead tip through the occipital skin; in the other patient the connection piece of the extension lead eroded through the intrascapular skin. This is caused by a overly superficial implantation of the material. This complication has been described elsewhere, as well as strategies to prevent it. 18 Both patients underwent local revision surgery in which the lead tip/extension were repositioned underneath the disinfected skin. No further inflammation or infection occurred in these two cases. One patient experienced persistent pain at the implantation site of the internal pulse generator. This was treated with pain medication, and we noticed a spontaneous resolution.
6 The neurostimulation device had to be removed in one patient (2.2%) because of a systemic allergic reaction to the stimulation device. This is a rare complication; only a few cases have been published. 19,20 After removal of the system, all symptoms resolved. One patient complained of feelings of anxiety and arousal during stimulation. We did not found any reports on that in the literature. However, by reprogramming the device, the symptoms decreased. Conclusion We presented a simple technique to perform occipital nerve stimulation with a single electrode without the use of additional anchoring devices. The technique achieves stimulation in both branches of the occipital nerves and reduces complications, more specifically lead migration. References 1 Wall PD, Sweet WH. Temporary abolition of pain in man. Science 1967;155(3758): Picaza JA, Hunter SE, Cannon BW. Pain suppression by peripheral nerve stimulation. Chronic effects of implanted devices. Appl Neurophysiol ;40(2-4): Plazier M, Dekelver I, Vanneste S, et al. Occipital nerve stimulation in fibromyalgia: a double-blind placebo-controlled pilot study with a six-month follow-up. Neuromodulation 2014;17(3): ; discussion Jasper JF, Hayek SM. Implanted occipital nerve stimulators. Pain Physician 2008;11(2): Schwedt TJ. Neurostimulation for primary headache disorders. Curr Neurol Neurosci Rep 2009;9: Bartsch T, Paemeleire K, Goadsby PJ. Neurostimulation approaches to primary headache disorders. Curr Opin Neurol 2009;22(3): Weiner RL, Reed KL. Peripheral neurostimulation for control of intractable occipital neuralgia. Neuromodulation 1999;2(3): Trentman TL, Zimmerman RS. Occipital nerve stimulation: technical and surgical aspects of implantation. Headache 2008;48(2): Schwedt TJ, Dodick DW, Hentz J, Trentman TL, Zimmerman RS. Occipital nerve stimulation for chronic headache long-term safety and efficacy. Cephalalgia 2007;27(2): Falowski S, Wang D, Sabesan A, Sharan A. Occipital nerve stimulator systems: review of complications and surgical techniques. Neuromodulation 2010;13(2): McGreevy K, Hameed H, Erdek MA. Updated perspectives on occipital nerve stimulator lead migration: case report and literature review. Clin J Pain 2012;28(9): Trentman TL, Zimmerman RS, Dodick DW. Occipital nerve stimulation: technical and surgical aspects of implantation. Prog Neurol Surg 2011;24: Franzini A, Messina G, Leone M, Broggi G. Occipital nerve stimulation (ONS). Surgical technique and prevention of late electrode migration. Acta Neurochir (Wien) 2009;151(7): ; discussion Trentman TL, Slavin KV, Freeman JA, Zimmerman RS. Occipital nerve stimulator placement via a retromastoid to infraclavicular approach: a technical report. Stereotact Funct Neurosurg 2010; 88(2): Magown P, Garcia R, Beauprie I, Mendez IM. Occipital nerve stimulation for intractable occipital neuralgia: an open surgical technique. Clin Neurosurg 2009;56: Hayek SM, Jasper JF, Deer TR, Narouze SN. Occipital neurostimulation-induced muscle spasms: implications for lead placement. Pain Physician 2009;12(5): Bovim G, Bonamico L, Fredriksen TA, Lindboe CF, Stolt-Nielsen A, Sjaastad O. Topographic variations in the peripheral course of the greater occipital nerve. Autopsy study with clinical correlations. Spine 1991;16(4): Trentman TL, Dodick DW, Zimmerman RS, Birch BD. Percutaneous occipital stimulator lead tip erosion: report of 2 cases. Pain Physician 2008;11(2): Nosbaum A, Rival-Tringali AL, Barth X, et al. Nickel-induced systemic allergic dermatitis from a sacral neurostimulator. Contact Dermat 2008;59(5): Delaplace M, Maîtred F, Dufour T, et al. Two cases of cutaneous erythema following spinal cord stimulation [in French]. Ann Dermatol Venereol 2010;137(4):
Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine:
 Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache
 Pain Physician 2011; 14:435-440 ISSN 1533-3159 Case Report Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache Natalie H. Strand
Pain Physician 2011; 14:435-440 ISSN 1533-3159 Case Report Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache Natalie H. Strand
Repositioning of Supraorbital Nerve Stimulation Electrode Using Retrograde Needle Insertion: A Technical Note
 Neuromodulation: Technology at the Neural Interface Received: June 7, 2010 First revision: July 24, 2010 Accepted: July 26, 2010 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2010.00315.x Repositioning
Neuromodulation: Technology at the Neural Interface Received: June 7, 2010 First revision: July 24, 2010 Accepted: July 26, 2010 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2010.00315.x Repositioning
Stimulation Ranges, Usage Ranges, and. Paresthesia Mapping During Occipital Nerve Stimulation. Introduction ORIGINAL ARTICLE ABSTRACT
 NEUROMODULATION: TECHNOLOGY AT THE NEURAL INTERFACE Volume 11 Number 1 2008 http://www.blackwell-synergy.com/loi/ner ORIGINAL ARTICLE Stimulation Ranges, Usage Ranges, and Blackwell Publishing Inc Paresthesia
NEUROMODULATION: TECHNOLOGY AT THE NEURAL INTERFACE Volume 11 Number 1 2008 http://www.blackwell-synergy.com/loi/ner ORIGINAL ARTICLE Stimulation Ranges, Usage Ranges, and Blackwell Publishing Inc Paresthesia
Trigeminal and occipital peripheral nerve stimulation for craniofacial pain: a single-institution experience and review of the literature
 Neurosurg Focus 21 (6):E6, 2006 Trigeminal and occipital peripheral nerve stimulation for craniofacial pain: a single-institution experience and review of the literature KONSTANTIN V. SLAVIN, M.D., M.
Neurosurg Focus 21 (6):E6, 2006 Trigeminal and occipital peripheral nerve stimulation for craniofacial pain: a single-institution experience and review of the literature KONSTANTIN V. SLAVIN, M.D., M.
Medical Policy. Description/Scope. Position Statement. Rationale
 Subject: Document#: Current Effective Date: 06/28/2017 Status: Reviewed Last Review Date: 05/04/2017 Description/Scope This document addresses occipital nerve stimulation (ONS), which involves delivering
Subject: Document#: Current Effective Date: 06/28/2017 Status: Reviewed Last Review Date: 05/04/2017 Description/Scope This document addresses occipital nerve stimulation (ONS), which involves delivering
Original Policy Date
 MP 7.01.105 Occipital Nerve Stimulation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy
MP 7.01.105 Occipital Nerve Stimulation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy
Using Peripheral Stimulation to Reduce the Pain of C2-Mediated Occipital Headaches: A Preliminary Report
 Pain Physician 2007; 10:453-460 ISSN 1533-3159 Prospective Case Series Using Peripheral Stimulation to Reduce the Pain of C2-Mediated Occipital Headaches: A Preliminary Report Eugene A. Melvin, Jr., MD
Pain Physician 2007; 10:453-460 ISSN 1533-3159 Prospective Case Series Using Peripheral Stimulation to Reduce the Pain of C2-Mediated Occipital Headaches: A Preliminary Report Eugene A. Melvin, Jr., MD
Long-Term Outcome in Occipital Nerve Stimulation Patients With Medically Intractable Primary Headache Disorders
 Neuromodulation: Technology at the Neural Interface Received: April 12, 2012 Revised: June 15, 2012 Accepted: June 27, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2012.00490.x Long-Term Outcome
Neuromodulation: Technology at the Neural Interface Received: April 12, 2012 Revised: June 15, 2012 Accepted: June 27, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2012.00490.x Long-Term Outcome
Occipital Nerve Stimulation for Headache Disorders
 Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Occipital Nerve Stimulation for Headache Disorders Koen Paemeleire* and Thorsten Bartsch *Department of Neurology,
Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Occipital Nerve Stimulation for Headache Disorders Koen Paemeleire* and Thorsten Bartsch *Department of Neurology,
Occipital Nerve Stimulation Corporate Medical Policy
 Occipital Nerve Stimulation Corporate Medical Policy File Name: Occipital Nerve Stimulation File Code: UM.SPSVC.14 Origination: 2011 Last Review: 06/2018 Next Review: 06/2019 Effective Date: 10/01/2018
Occipital Nerve Stimulation Corporate Medical Policy File Name: Occipital Nerve Stimulation File Code: UM.SPSVC.14 Origination: 2011 Last Review: 06/2018 Next Review: 06/2019 Effective Date: 10/01/2018
Medical Policy Manual. Topic: Peripheral Subcutaneous Field Stimulation Date of Origin: April Section: Surgery Last Reviewed Date: April 2014
 Medical Policy Manual Topic: Peripheral Subcutaneous Field Stimulation Date of Origin: April 2013 Section: Surgery Last Reviewed Date: April 2014 Policy No: 188 Effective Date: July 1, 2014 IMPORTANT REMINDER
Medical Policy Manual Topic: Peripheral Subcutaneous Field Stimulation Date of Origin: April 2013 Section: Surgery Last Reviewed Date: April 2014 Policy No: 188 Effective Date: July 1, 2014 IMPORTANT REMINDER
The Impact of Peripheral Nerve Stimulation on Disability and Depression
 Neuromodulation: Technology at the Neural Interface Received: June 25, 2015 Revised: August 25, 2015 Accepted: September 15, 2015 (onlinelibrary.wiley.com) DOI: 10.1111/ner.12363 The Impact of Peripheral
Neuromodulation: Technology at the Neural Interface Received: June 25, 2015 Revised: August 25, 2015 Accepted: September 15, 2015 (onlinelibrary.wiley.com) DOI: 10.1111/ner.12363 The Impact of Peripheral
Occipital Neuromodulation: A Surgical Technique with Reduced Complications
 Pain Physician 2016; 19:E1005-E1012 ISSN 2150-1149 Retrospective Analysis Occipital Neuromodulation: A Surgical Technique with Reduced Complications Thomas P Pittelkow, DO, MPH, Gabriel L Pagani-Estévez,
Pain Physician 2016; 19:E1005-E1012 ISSN 2150-1149 Retrospective Analysis Occipital Neuromodulation: A Surgical Technique with Reduced Complications Thomas P Pittelkow, DO, MPH, Gabriel L Pagani-Estévez,
Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
 ORIGINAL ARTICLE Year : 2015 Volume : 63 Issue : 5 Page : 707 711 Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
ORIGINAL ARTICLE Year : 2015 Volume : 63 Issue : 5 Page : 707 711 Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Implanted Peripheral Nerve Stimulator (PNS) for Pain Control Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS)
Implanted Peripheral Nerve Stimulator (PNS) for Pain Control Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS)
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Case Report. Ilioinguinal Peripheral Nerve Stimulation. Juan A. Ramos, MD 1, Andrew J. McNeil, DO 2, Ted F. Gingrich, MD 3
 Case Report Interventional Pain Management Reports Volume 1, Number 2, pp93-97 2017, American Society of Interventional Pain Physicians Combined Ultrasound and Fluoroscopic Guidance for Percutaneous Ilioinguinal
Case Report Interventional Pain Management Reports Volume 1, Number 2, pp93-97 2017, American Society of Interventional Pain Physicians Combined Ultrasound and Fluoroscopic Guidance for Percutaneous Ilioinguinal
Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association
 Implanted Peripheral Nerve Stimulator (PNS) Page 1 of 6 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS) for Pain
Implanted Peripheral Nerve Stimulator (PNS) Page 1 of 6 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Implanted Peripheral Nerve Stimulator (PNS) for Pain
Occipital Neuromodulation: Ultrasound Guidance for Peripheral Nerve Stimulator Implantation
 papr_381 580..585 CLINICAL REPORT Occipital Neuromodulation: Ultrasound Guidance for Peripheral Nerve Stimulator Implantation Jason S. Eldrige, MD*; Jon B. Obray, MD*, ; Matthew J. Pingree, MD*; Bryan
papr_381 580..585 CLINICAL REPORT Occipital Neuromodulation: Ultrasound Guidance for Peripheral Nerve Stimulator Implantation Jason S. Eldrige, MD*; Jon B. Obray, MD*, ; Matthew J. Pingree, MD*; Bryan
Occipital Nerve Stimulation
 Occipital Nerve Stimulation Policy Number: 7.01.125 Last Review: 5/2018 Origination: 5/2006 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
Occipital Nerve Stimulation Policy Number: 7.01.125 Last Review: 5/2018 Origination: 5/2006 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
Policy #: 411 Latest Review Date: January 2014
 Name of Policy: Occipital Nerve Stimulation Policy #: 411 Latest Review Date: January 2014 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross
Name of Policy: Occipital Nerve Stimulation Policy #: 411 Latest Review Date: January 2014 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross
Spinal cord stimulation (SCS) is a safe and effective procedure
 ORIGINAL ARTICLE A 2-center Comparative Study on Tonic Versus Burst Spinal Cord Stimulation Amount of Responders and Amount of Pain Suppression Dirk De Ridder, MD, PhD,*w Mathieu W.P.M. Lenders, MD,zy
ORIGINAL ARTICLE A 2-center Comparative Study on Tonic Versus Burst Spinal Cord Stimulation Amount of Responders and Amount of Pain Suppression Dirk De Ridder, MD, PhD,*w Mathieu W.P.M. Lenders, MD,zy
Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain.
 Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
Coding for Sacral Neuromodulation
 301.273.0570 Fax 301.273.0778 Coding for Sacral Neuromodulation Sacral Neuromodulation (SNS) is a widely used technique in Female Pelvic Medicine and Reconstructive Surgery (FPMRS), with several FDA-approved
301.273.0570 Fax 301.273.0778 Coding for Sacral Neuromodulation Sacral Neuromodulation (SNS) is a widely used technique in Female Pelvic Medicine and Reconstructive Surgery (FPMRS), with several FDA-approved
Peripheral Nerve S-mula-on
 Peripheral Nerve S-mula-on Konstan-n Slavin, MD Professor, Department of Neurosurgery University of Illinois at Chicago Peripheral Nerve S-mula-on New (?) approach Neuropathic pain syndromes Off label
Peripheral Nerve S-mula-on Konstan-n Slavin, MD Professor, Department of Neurosurgery University of Illinois at Chicago Peripheral Nerve S-mula-on New (?) approach Neuropathic pain syndromes Off label
Occipital Nerve Stimulation for the Treatment of Chronic Cluster Headache Lessons Learned from 18 Months Experience
 Original Article Occipital Nerve Stimulation for the Treatment of Chronic Cluster Headache Lessons Learned from Months Experience Authors O. M. Mueller, C. Gaul, Z. Katsarava, H. C. Diener, U. Sure, T.
Original Article Occipital Nerve Stimulation for the Treatment of Chronic Cluster Headache Lessons Learned from Months Experience Authors O. M. Mueller, C. Gaul, Z. Katsarava, H. C. Diener, U. Sure, T.
Peripheral Subcutaneous Field Stimulation. Description
 Subject: Peripheral Subcutaneous Field Stimulation Page: 1 of 6 Last Review Status/Date: June 2016 Peripheral Subcutaneous Field Stimulation Description Peripheral subcutaneous field stimulation (PSFS,
Subject: Peripheral Subcutaneous Field Stimulation Page: 1 of 6 Last Review Status/Date: June 2016 Peripheral Subcutaneous Field Stimulation Description Peripheral subcutaneous field stimulation (PSFS,
Affiliation: 1- Departments of Anesthesiology/ Pain Management and Neurology, UCSF School of Medicine 2- Thrive Clinic, LLC, Santa Rosa, CA
 Author Information Prasad Shirvalkar MD, PhD 1 Jason E. Pope MD 2 Affiliation: 1- Departments of Anesthesiology/ Pain Management and Neurology, UCSF School of Medicine 2- Thrive Clinic, LLC, Santa Rosa,
Author Information Prasad Shirvalkar MD, PhD 1 Jason E. Pope MD 2 Affiliation: 1- Departments of Anesthesiology/ Pain Management and Neurology, UCSF School of Medicine 2- Thrive Clinic, LLC, Santa Rosa,
Surgical Treatment: Patient Edition
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Peripheral nerve stimulation for treatment of postherpetic neuralgia: A Case report
 Case report Acta Medica Academica 2011;40(2):187-191 DOI 10.5644/ama2006-124.23 Peripheral nerve stimulation for treatment of postherpetic neuralgia: A Case report Scott C. Palmer 1, Alexis A. Jimenez
Case report Acta Medica Academica 2011;40(2):187-191 DOI 10.5644/ama2006-124.23 Peripheral nerve stimulation for treatment of postherpetic neuralgia: A Case report Scott C. Palmer 1, Alexis A. Jimenez
Occipital Nerve Stimulation Corporate Medical Policy
 Occipital Nerve Stimulation Corporate Medical Policy File name: Occipital Nerve Stimulation File code: UM.SPSVC.14 Origination: 2011 Last Review: 11/2017 Next Review: 11/2018 Effective Date: 05/01/2018
Occipital Nerve Stimulation Corporate Medical Policy File name: Occipital Nerve Stimulation File code: UM.SPSVC.14 Origination: 2011 Last Review: 11/2017 Next Review: 11/2018 Effective Date: 05/01/2018
Stimulation of the Greater Occipital Nerve: Anatomical Considerations and Clinical Implications
 Pain Physician 2013; 16:E181-E189 ISSN 2150-1149 Prospective Study Stimulation of the Greater Occipital Nerve: Anatomical Considerations and Clinical Implications Oliver Mueller, MD, Vincent Hagel, MD,
Pain Physician 2013; 16:E181-E189 ISSN 2150-1149 Prospective Study Stimulation of the Greater Occipital Nerve: Anatomical Considerations and Clinical Implications Oliver Mueller, MD, Vincent Hagel, MD,
Novel Minimally Invasive Wireless Nanotechnology Neuromodulation System in the Management of Chronic Pain Syndromes
 Novel Minimally Invasive Wireless Nanotechnology Neuromodulation System in the Management of Chronic Pain Syndromes Laura Tyler Perryman* Stimwave Technologies, Inc. 1310 Park Central Blvd South, Pompano
Novel Minimally Invasive Wireless Nanotechnology Neuromodulation System in the Management of Chronic Pain Syndromes Laura Tyler Perryman* Stimwave Technologies, Inc. 1310 Park Central Blvd South, Pompano
The Role of the Neuromodulation in Management of Chronic Pain
 The Role of the Neuromodulation in Management of Chronic Pain Adnan Al-Kaisy, MB ChB, FRCA, FFPMRCA, FIPP Clinical Lead of the Pain Management & Neuromodulation Centre Guy s & St Thomas Hospital, London,
The Role of the Neuromodulation in Management of Chronic Pain Adnan Al-Kaisy, MB ChB, FRCA, FFPMRCA, FIPP Clinical Lead of the Pain Management & Neuromodulation Centre Guy s & St Thomas Hospital, London,
Peripheral Nerve Stimulation and Percutaneous Electrical Nerve Stimulation in Pain Management: A Review and Update on Current Status -
 International Journal of Pain & Relief Review Article Peripheral Nerve Stimulation and Percutaneous Electrical Nerve Stimulation in Pain Management: A Review and Update on Current Status - Laura Tyler
International Journal of Pain & Relief Review Article Peripheral Nerve Stimulation and Percutaneous Electrical Nerve Stimulation in Pain Management: A Review and Update on Current Status - Laura Tyler
Peripheral Subcutaneous Field Stimulation
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
2014 AAPM 56 th Annual Meeting
 2014 AAPM 56 th Annual Meeting SAM Diagnostic Radiology MR Safety - Deep Brain Stimulator and Other Neurostimulators Yunhong Shu, Ph.D. Mayo Clinic, Rochester, MN Outline Background of Neurostimulator
2014 AAPM 56 th Annual Meeting SAM Diagnostic Radiology MR Safety - Deep Brain Stimulator and Other Neurostimulators Yunhong Shu, Ph.D. Mayo Clinic, Rochester, MN Outline Background of Neurostimulator
The greater and lesser occipital nerves traverse RECONSTRUCTIVE
 RECONSTRUCTIVE Anatomical Variations of the Occipital Nerves: Implications for the Treatment of Chronic Headaches Ivica Ducic, M.D., Ph.D. Maureen Moriarty, M.S., C.R.N.P. Ali Al-Attar, M.D., Ph.D. Washington,
RECONSTRUCTIVE Anatomical Variations of the Occipital Nerves: Implications for the Treatment of Chronic Headaches Ivica Ducic, M.D., Ph.D. Maureen Moriarty, M.S., C.R.N.P. Ali Al-Attar, M.D., Ph.D. Washington,
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 3/2018 Origination: 7/2013 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 3/2018 Origination: 7/2013 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Neuromodulation techniques for treatment of refractory neuropathic pain
 Article ID: WMC004271 ISSN 2046-1690 Neuromodulation techniques for treatment of refractory neuropathic pain Corresponding Author: Prof. Angelo Lavano, Full Professor of Neurosurgery, Department of Neurosurgery,
Article ID: WMC004271 ISSN 2046-1690 Neuromodulation techniques for treatment of refractory neuropathic pain Corresponding Author: Prof. Angelo Lavano, Full Professor of Neurosurgery, Department of Neurosurgery,
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Phenotype of patients responsive to occipital nerve stimulation for refractory head pain
 Phenotype of patients responsive to occipital nerve stimulation for refractory head pain Koen Paemeleire 1*, MD, PhD, Jean-Pierre Van Buyten 2*, MD, Machteld Van Buynder 2, Dario Alicino 2, MD, Georges
Phenotype of patients responsive to occipital nerve stimulation for refractory head pain Koen Paemeleire 1*, MD, PhD, Jean-Pierre Van Buyten 2*, MD, Machteld Van Buynder 2, Dario Alicino 2, MD, Georges
Pocket Adaptor Kit FOR SPINAL CORD STIMULATION. Tip Cards
 Pocket Adaptor Kit FOR SPINAL CORD STIMULATION Tip Cards model 74001 (1 4) model 74002 (2 4) The Pocket Adaptor Tip Cards are to be used for educational purposes only. Please refer to the Pocket Adaptor
Pocket Adaptor Kit FOR SPINAL CORD STIMULATION Tip Cards model 74001 (1 4) model 74002 (2 4) The Pocket Adaptor Tip Cards are to be used for educational purposes only. Please refer to the Pocket Adaptor
Headache: Using Neuromodulation as Therapy
 Headache: Using Neuromodulation as Therapy Rashmi Halker, MD, FAHS Assistant Professor of Neurology Department of Neurology Mayo Clinic Phoenix Arizona Disclosures Nothing to disclose 2013 MFMER slide-2
Headache: Using Neuromodulation as Therapy Rashmi Halker, MD, FAHS Assistant Professor of Neurology Department of Neurology Mayo Clinic Phoenix Arizona Disclosures Nothing to disclose 2013 MFMER slide-2
Peripheral Nerve Stimulation
 Peripheral Nerve Stimulation Progress in Neurological Surgery Vol. 24 Series Editor L. Dade Lunsford Pittsburgh, Pa. Peripheral Nerve Stimulation Volume Editor Konstantin V. Slavin Chicago, Ill. 59 figures,
Peripheral Nerve Stimulation Progress in Neurological Surgery Vol. 24 Series Editor L. Dade Lunsford Pittsburgh, Pa. Peripheral Nerve Stimulation Volume Editor Konstantin V. Slavin Chicago, Ill. 59 figures,
To you who will receive a T-Port PATIENT INFORMATION
 To you who will receive a T-Port PATIENT INFORMATION T-Port Patient information What is a T-Port? Why this booklet The purpose of this handout is to help you understand how it is to receive and live with
To you who will receive a T-Port PATIENT INFORMATION T-Port Patient information What is a T-Port? Why this booklet The purpose of this handout is to help you understand how it is to receive and live with
biowave Biowave Corporation 16 Knight Street, Norwalk, CT 06851
 biowave Biowave Corporation 16 Knight Street, Norwalk, CT 06851 1 877 BIOWAVE www.biowave.com Biowave PENS BiowavePRO System with Biowave Percutaneous Electrodes Percutaneous Neuromodulation Pain Therapy
biowave Biowave Corporation 16 Knight Street, Norwalk, CT 06851 1 877 BIOWAVE www.biowave.com Biowave PENS BiowavePRO System with Biowave Percutaneous Electrodes Percutaneous Neuromodulation Pain Therapy
Percutaneously Implanted Plate Electrodes in Failed Back Surgery Syndrome (FBSS)ner_
 Neuromodulation: Technology at the Neural Interface Received: October 4, 2010 Revised: February 13, 2011 Accepted: April 26, 2011 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2011.00368.x Percutaneously
Neuromodulation: Technology at the Neural Interface Received: October 4, 2010 Revised: February 13, 2011 Accepted: April 26, 2011 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2011.00368.x Percutaneously
Medical Review Criteria Implantable Neurostimulators
 Medical Review Criteria Implantable Neurostimulators Subject: Implantable Neurostimulators Effective Date: April 14, 2017 Authorization: Prior authorization is required for covered implantable stimulators
Medical Review Criteria Implantable Neurostimulators Subject: Implantable Neurostimulators Effective Date: April 14, 2017 Authorization: Prior authorization is required for covered implantable stimulators
Complications of Spinal Cord Stimulation and Peripheral Nerve Stimulation Techniques: A Review of the Literature
 Pain Medicine 2016; 17: 325 336 doi: 10.1093/pm/pnv025 NEUROMODULATION SECTION Review Article Complications of Spinal Cord Stimulation and Peripheral Nerve Stimulation Techniques: A Review of the Literature
Pain Medicine 2016; 17: 325 336 doi: 10.1093/pm/pnv025 NEUROMODULATION SECTION Review Article Complications of Spinal Cord Stimulation and Peripheral Nerve Stimulation Techniques: A Review of the Literature
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2018 Origination: 7/2013 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2018 Origination: 7/2013 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Procedures/Risks:central venous catheter
 Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
Procedures/Risks:central venous catheter Central Venous Catheter Placement Procedure: Placement of the central venous catheter will take place in the Interventional Radiology Department (IRD) at The Ohio
St. Jude Medical 8-Channel Adapter. Clinician's Manual
 St. Jude Medical 8-Channel Adapter Clinician's Manual CAUTION: Federal (USA) law restricts this device to sale by or on the order of a physician. For U.S. California Only: Proposition 65, a State of California
St. Jude Medical 8-Channel Adapter Clinician's Manual CAUTION: Federal (USA) law restricts this device to sale by or on the order of a physician. For U.S. California Only: Proposition 65, a State of California
NANS Conference 2017 Highlights Matthew R. Kohler, MD January 2017
 NAN Conference 2017 Highlights Matthew R. Kohler, MD January 2017 timulation timulation A dorsal root ganglion (or spinal ganglion) (also known as a posterior root ganglion), is a cluster of nerve cell
NAN Conference 2017 Highlights Matthew R. Kohler, MD January 2017 timulation timulation A dorsal root ganglion (or spinal ganglion) (also known as a posterior root ganglion), is a cluster of nerve cell
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Surgical Leads. Directions for Use. CAUTION: Federal law restricts this device to sale, distribution and use by or on the order of a physician.
 Surgical Leads Directions for Use CAUTION: Federal law restricts this device to sale, distribution and use by or on the order of a physician. 91078747-08 Content: 92190987 REV A Guarantees Boston Scientific
Surgical Leads Directions for Use CAUTION: Federal law restricts this device to sale, distribution and use by or on the order of a physician. 91078747-08 Content: 92190987 REV A Guarantees Boston Scientific
The Treatment of Medically Intractable Trigeminal Autonomic Cephalalgia With Supraorbital/Supratrochlear Stimulation: A Retrospective Case Series
 Neuromodulation: Technology at the Neural Interface Received: October 10, 2011 Revised: February 2, 2012 Accepted: March 12, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2012.00455.x The Treatment
Neuromodulation: Technology at the Neural Interface Received: October 10, 2011 Revised: February 2, 2012 Accepted: March 12, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/j.1525-1403.2012.00455.x The Treatment
Peripheral Neurostimulation in Supraorbital Neuralgia Refractory to Conventional Therapy
 CLINICAL REPORT Peripheral Neurostimulation in Supraorbital Neuralgia Refractory to Conventional Therapy Juan M. Asensio-Samper, MD*; Vicente L. Villanueva, MD ; Alfonso V. Pérez, PhD ; María D. López,
CLINICAL REPORT Peripheral Neurostimulation in Supraorbital Neuralgia Refractory to Conventional Therapy Juan M. Asensio-Samper, MD*; Vicente L. Villanueva, MD ; Alfonso V. Pérez, PhD ; María D. López,
Peripheral Neuromodulation and Headaches: History, Clinical Approach, and Considerations on Underlying Mechanisms
 Curr Pain Headache Rep (2013) 17:305 DOI 10.1007/s11916-012-0305-8 CHRONIC DAILY HEADACHE (SJ WANG, SECTION EDITOR) Peripheral Neuromodulation and Headaches: History, Clinical Approach, and Considerations
Curr Pain Headache Rep (2013) 17:305 DOI 10.1007/s11916-012-0305-8 CHRONIC DAILY HEADACHE (SJ WANG, SECTION EDITOR) Peripheral Neuromodulation and Headaches: History, Clinical Approach, and Considerations
Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y
 May 10, 2018 United Healthcare Medical Policy Department 9500 Bren Road East Minnetonka, MN 55343 via Email: mpq@uhc.com Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y To Whom
May 10, 2018 United Healthcare Medical Policy Department 9500 Bren Road East Minnetonka, MN 55343 via Email: mpq@uhc.com Re: Occipital Neuralgia and Headache Treatment, Policy Number: 2018T0080Y To Whom
Lead and Extension Insertion Tool. Model Clinician's Manual
 Lead and Extension Insertion Tool Model 1803 Clinician's Manual Unless otherwise noted, indicates that the name is a trademark of, or licensed to, St. Jude Medical or one of its subsidiaries. ST. JUDE
Lead and Extension Insertion Tool Model 1803 Clinician's Manual Unless otherwise noted, indicates that the name is a trademark of, or licensed to, St. Jude Medical or one of its subsidiaries. ST. JUDE
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY
 NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
3. The Jaw and Related Structures
 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Treatment of Intractable Hemicrania Continua by Occipital Nerve Stimulation
 Treatment of Intractable Hemicrania Continua by Occipital Nerve Stimulation 1 Sarah Miller MBBS, MRCP 2 Laurence Watkins FRCS, PhD and 1 Manjit Matharu FRCP, PhD 1 Headache Group, Institute of Neurology
Treatment of Intractable Hemicrania Continua by Occipital Nerve Stimulation 1 Sarah Miller MBBS, MRCP 2 Laurence Watkins FRCS, PhD and 1 Manjit Matharu FRCP, PhD 1 Headache Group, Institute of Neurology
Surgical Lead Implantation Guide
 Surgical Lead Implantation Guide Neurostimulation Therapy for Chronic Pain Innovating for life. Medtronic, PrimeAdvanced, Restore, RestoreAdvanced, RestoreUltra, and Specify are registered trademarks of
Surgical Lead Implantation Guide Neurostimulation Therapy for Chronic Pain Innovating for life. Medtronic, PrimeAdvanced, Restore, RestoreAdvanced, RestoreUltra, and Specify are registered trademarks of
An Anatomical Study of the Lesser Occipital Nerve and Its Potential Compression Points: Implications for Surgical Treatment of Migraine Headaches
 RECONSTRUCTIVE An Anatomical Study of the Lesser Occipital Nerve and Its Potential Compression Points: Implications for Surgical Treatment of Migraine Headaches Michelle Lee, M.D. Matthew Brown, M.D. Kyle
RECONSTRUCTIVE An Anatomical Study of the Lesser Occipital Nerve and Its Potential Compression Points: Implications for Surgical Treatment of Migraine Headaches Michelle Lee, M.D. Matthew Brown, M.D. Kyle
SURGICAL TECHNIQUE GUIDE: JONES FRACTURE USING THE PRECISION JONES FRACTURE SCREW SYSTEM
 PRODUCT DESCRIPTION The PRECISION Jones Fracture Screw System offers extensive options of Type II Anodized Titanium screws. System-specific instrumentation is designed to address procedural challenges
PRODUCT DESCRIPTION The PRECISION Jones Fracture Screw System offers extensive options of Type II Anodized Titanium screws. System-specific instrumentation is designed to address procedural challenges
Technical Note SACRAL NERVE STIMULATION (SNS) FOR PUDENDAL NEURALGIA VIA THE SACROCOCCYGEAL APPROACH: A TECHNICAL NOTE
 Technical Note Interventional Pain Management Reports Volume 1, Number 4, pp153-157 2017, American Society of Interventional Pain Physicians SACRAL NERVE STIMULATION (SNS) FOR PUDENDAL NEURALGIA VIA THE
Technical Note Interventional Pain Management Reports Volume 1, Number 4, pp153-157 2017, American Society of Interventional Pain Physicians SACRAL NERVE STIMULATION (SNS) FOR PUDENDAL NEURALGIA VIA THE
WINSTA-C. Clavicle Plating System
 Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
Supraorbital nerve stimulation Cefaly Device - FDA Approved for migraine prevention (also being investigated as acute therapy)
 NEUROSTIMULATION/NEUROMODULATION UPDATE Meyer and Renee Luskin Andrew Charles, M.D. Professor Luskin Chair in Migraine and Headache Studies Director, UCLA Goldberg Migraine Program David Geffen School
NEUROSTIMULATION/NEUROMODULATION UPDATE Meyer and Renee Luskin Andrew Charles, M.D. Professor Luskin Chair in Migraine and Headache Studies Director, UCLA Goldberg Migraine Program David Geffen School
CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE
 CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE INDICATIONS FOR USE The LATERA Absorbable Nasal Implant is indicated for supporting upper and lower lateral nasal cartilage. CAUTION: Federal law restricts
CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE INDICATIONS FOR USE The LATERA Absorbable Nasal Implant is indicated for supporting upper and lower lateral nasal cartilage. CAUTION: Federal law restricts
C ODING PAIN C LINICS. After attending this presentation, attendee will be able to: Coding Check List
 Home Town Health Take the Pain out of Coding Pain Clinics J E NAN C U S TER C P C, C C S, C D I P AH IMA A PPROVED IC D - 1 0 - C M/PC S T RAINER AND A MBASSADOR D IRECTOR OF C ODING H EALTHCARE C ODING
Home Town Health Take the Pain out of Coding Pain Clinics J E NAN C U S TER C P C, C C S, C D I P AH IMA A PPROVED IC D - 1 0 - C M/PC S T RAINER AND A MBASSADOR D IRECTOR OF C ODING H EALTHCARE C ODING
Sacral Neuromodulation for Dysfunctional Voiders Workshop 1 Monday, August 23, 09:00 10:30
 Sacral Neuromodulation for Dysfunctional Voiders Workshop 1 Monday, August 23, 09:00 10:30 Time Time Topic Speaker 09:00 09:05 Introduction to the aims of the workshop and the Magdy Hassouna participants
Sacral Neuromodulation for Dysfunctional Voiders Workshop 1 Monday, August 23, 09:00 10:30 Time Time Topic Speaker 09:00 09:05 Introduction to the aims of the workshop and the Magdy Hassouna participants
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy
 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Case Discussion: Post-implant infections & explant decision making
 Author Information Full Names: Sailesh Arulkumar, MD David Provenzano, MD Affiliation: Sailesh Arulkumar MD: Attending Pain Physician, The Orthopaedic Center, Tulsa OK David Provenzano, MD: Attending Pain
Author Information Full Names: Sailesh Arulkumar, MD David Provenzano, MD Affiliation: Sailesh Arulkumar MD: Attending Pain Physician, The Orthopaedic Center, Tulsa OK David Provenzano, MD: Attending Pain
BICEPTOR Tenodesis System
 BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
Percutaneous Lead Kit. Models 3143, 3146, 3149, 3153, 3156, 3159, 3183, 3186, Clinician's Manual
 Percutaneous Lead Kit Models 3143, 3146, 3149, 3153, 3156, 3159, 3183, 3186, 3189 Clinician's Manual Unless otherwise noted, indicates that the name is a trademark of, or licensed to, St. Jude Medical
Percutaneous Lead Kit Models 3143, 3146, 3149, 3153, 3156, 3159, 3183, 3186, 3189 Clinician's Manual Unless otherwise noted, indicates that the name is a trademark of, or licensed to, St. Jude Medical
A Patient s Guide to Transcutaneous Electrical Stimulation (TENS) for Cervical Spine Pain
 A Patient s Guide to Transcutaneous Electrical Stimulation (TENS) for Cervical Spine Pain 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information
A Patient s Guide to Transcutaneous Electrical Stimulation (TENS) for Cervical Spine Pain 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Body Contouring Implants - Calf
 Body Contouring Implants - Calf The body you were born with may or may not have the musculature you desire and it may be difficult to improve upon certain areas with exercise alone. In some cases, damage
Body Contouring Implants - Calf The body you were born with may or may not have the musculature you desire and it may be difficult to improve upon certain areas with exercise alone. In some cases, damage
Author Information. Presenting Symptom: Burning in right foot> Chronic low back pain
 Author Information Full Names: Erica Patel, MD Kiran V. Patel, MD Presenting Symptom: Burning in right foot> Chronic low back pain Case Specific Diagnosis: Chronic low back pain and radicular pain Learning
Author Information Full Names: Erica Patel, MD Kiran V. Patel, MD Presenting Symptom: Burning in right foot> Chronic low back pain Case Specific Diagnosis: Chronic low back pain and radicular pain Learning
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
Sacral Neuromodulation Beyond Pelvic Pain!!!
 Sacral Neuromodulation Beyond Pelvic Pain!!! Dr. Hirachand S Mutagi. Senior Consultant Pain Physician. Head -Sakra World Hospital. Director ReLeaf Pain Services. Rapid advances in neurostimulation therapy
Sacral Neuromodulation Beyond Pelvic Pain!!! Dr. Hirachand S Mutagi. Senior Consultant Pain Physician. Head -Sakra World Hospital. Director ReLeaf Pain Services. Rapid advances in neurostimulation therapy
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Preventive Effect of Greater Occipital Nerve Block on Severity and Frequency of Migraine Headache
 Global Journal of Health Science; Vol. 6, No. 6; 2014 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Preventive Effect of Greater Occipital Nerve Block on Severity
Global Journal of Health Science; Vol. 6, No. 6; 2014 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Preventive Effect of Greater Occipital Nerve Block on Severity
Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4)
 AO Manual of ESIN in children s fractures Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4) Title AO Manual of ESIN in children Subtitle Elastic stable intramedullary nailing (ESIN) Author
AO Manual of ESIN in children s fractures Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4) Title AO Manual of ESIN in children Subtitle Elastic stable intramedullary nailing (ESIN) Author
Spinal Cord Stimulation - Patient Information No 7
 Spinal Cord Stimulation - Patient Information No 7 DUDLEY PAIN SERVICE Patient Information Sheet No: 7 Spinal Cord Stimulation February 2009 What do we mean by this? Spinal cord stimulation is a treatment
Spinal Cord Stimulation - Patient Information No 7 DUDLEY PAIN SERVICE Patient Information Sheet No: 7 Spinal Cord Stimulation February 2009 What do we mean by this? Spinal cord stimulation is a treatment
Occipital nerve stimulation for intractable chronic cluster headache or migraine: A critical analysis of direct treatment costs and complications
 Original Article Occipital nerve stimulation for intractable chronic cluster headache or migraine: A critical analysis of direct treatment costs and complications Cephalalgia 33(16) 1283 1291! International
Original Article Occipital nerve stimulation for intractable chronic cluster headache or migraine: A critical analysis of direct treatment costs and complications Cephalalgia 33(16) 1283 1291! International
Greater Occipital Nerve stimulation: a surgical treatment for Fibromyalgia
 Greater Occipital Nerve stimulation: a surgical treatment for Fibromyalgia Nervus Occipitalis major stimulatie: een chirurgische behandeling voor Fibromyalgie Proefschrift voorgelegd tot het behalen van
Greater Occipital Nerve stimulation: a surgical treatment for Fibromyalgia Nervus Occipitalis major stimulatie: een chirurgische behandeling voor Fibromyalgie Proefschrift voorgelegd tot het behalen van
Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration.
 Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration. Recommended Surgical Tools A. Scalpel handle B. Scalpel blade (#15)
Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration. Recommended Surgical Tools A. Scalpel handle B. Scalpel blade (#15)
Sustained Effectiveness of Occipital Nerve Stimulation in Drug-Resistant Chronic Cluster Headachehead_
 Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.01973.x Published by Wiley Periodicals, Inc. Research Submissions Sustained Effectiveness of Occipital Nerve in Drug-Resistant
Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.01973.x Published by Wiley Periodicals, Inc. Research Submissions Sustained Effectiveness of Occipital Nerve in Drug-Resistant
Surgical Procedure in Guided Tissue Regeneration with the. Inion GTR Biodegradable Membrane System
 Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Technical Note NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE FLUOROSCOPIC VIEWS DURING CERVICAL RADIOFREQUENCY NEUROTOMY.
 Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion
 Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
Instead of feeling pain, the patient will experience tingling.
 Spinal Cord Stimulation or SCS is a technique involving electrical stimulation of a precise part of the spinal cord. A very low energy current is used. This essentially shuts down the pain signals from
Spinal Cord Stimulation or SCS is a technique involving electrical stimulation of a precise part of the spinal cord. A very low energy current is used. This essentially shuts down the pain signals from
INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM
 INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM WILLIAM D. MUSTAIN, PH.D., CNIM, BCS-IOM DEPARTMENT OF OTOLARYNGOLOGY AND COMMUNICATIVE
INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM WILLIAM D. MUSTAIN, PH.D., CNIM, BCS-IOM DEPARTMENT OF OTOLARYNGOLOGY AND COMMUNICATIVE
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Deep Brain Stimulation (DBS) For patients with tremor
 Patient Education Deep Brain Stimulation (DBS) For patients with tremor Please read this handout before reading and signing the form Special Consent for Procedural Treatment. This handout describes how
Patient Education Deep Brain Stimulation (DBS) For patients with tremor Please read this handout before reading and signing the form Special Consent for Procedural Treatment. This handout describes how
