PRIORITIES AND CLINICAL EFFECTIVENESS FORUM MANAGEMENT OF ADULT HEADACHE
|
|
|
- Anissa Campbell
- 6 years ago
- Views:
Transcription
1 PRIORITIES AND CLINICAL EFFECTIVENESS FORUM MANAGEMENT OF ADULT HEADACHE o This is a new guideline produced jointly by GPs and Consultant Neurologists. o The aim is to reduce referrals to Consultants for the majority of headaches that can be safely managed in Primary Care. o This will facilitate faster assessment of those headache referrals that demonstrate red flag features, requiring specialist investigation. o Diagnostic guidance and treatment schedules are provided. Page 1 of 12
2 Patient Information Adult Headache Acknowledgements History & examination Diagnostic features (no red flags) Migraine: Without aura With aura Tension-type headache Cluster headache Medication overuse Trigeminal neuralgia Treatment schedules: Migraine Tension-type (TTH) Cluster headache Medication Overuse Headache (MOH) Trigeminal Neuralgia (Prodigy notes) Diagnostic uncertainty (no red flags) (Ix) Still consider the commonest causes: Tension-type Headache Migraine Analgesic Induced Headache Cervicogenic headache in the over 60 s ESR +/- CRP Red flag features Awoken by headache at night (not awakes with a headache). Worst in the morning Worsened by changes in posture, especially bending. Coughing, sneezing, straining, or vomiting exacerbates it. Associated with: o Vomiting & drowsiness. o Progressive neurological deficit. o Cognitive changes. Papilloedema. Meningeal irritation; look specifically for neck stiffness, back pain, and Kernig's sign. New neurological deficit Refer Therapeutic trials (At least 2 treatment options at adequate dosage, esp. migraine) Review diagnosis: Any more clues? (Diary, etc) Reviews & PILs Response No response Page 2 of 12
3 Notes: Acknowledgements: The following text is taken from the Prodigy Guidelines for Headache, Migraine and Trigeminal Neuralgia. The algorithm was designed by Richard Bull (REB) with the support of Consultant Neurologists: Markus Reuber & Marios Hadjivassiliou, and the valued input of GPs on the Clinical Guidelines Group, Chesterfield CG Group, NED PCT PEC and from Peter Burrill on behalf of PACEF. Headache: This algorithm is designed to be an aid: We would encourage you to familiarise yourself with the Prodigy Guidelines themselves ( ) rather than relying on what is necessarily a brief synopsis. In 1988 The International Headache Society published its classification and operational diagnostic criteria for all headache disorders. This has now been updated with the 2004 update: Headache Classification Sub-Committee of the International Headache Society. The international classification of headache disorders. Cephalalgia 2004;24(suppl 1): This update is now the gold standard and can be viewed and saved (but not printed) at It s also worth checking out but note these guidelines have not yet been updated in line with the new 2004 HIS guidelines History: The history is the most important diagnostic factor in the majority of people with headache. Although the examination, as guided by the history, must not be omitted, it rarely reveals any positive diagnostic features. Investigations are not helpful for most people with headache as there are no diagnostic tests for the most common causes. A headache diary is a particularly useful tool to aid diagnosis. Migraine is usually easily diagnosed from the history. Common and classic migraine account for 99% of cases. Migraine without aura This is an idiopathic, recurring disorder involving attacks that last 4-72 hours. Page 3 of 12
4 The headache is typically unilateral, pulsating, of moderate or severe intensity, and is aggravated by normal physical activity. It is associated with nausea, vomiting, photophobia, and phonophobia. Five or more attacks are required to make the diagnosis. Seventy-five per cent of sufferers have this form. Patients who consult with episodic headaches that significantly interfere with normal daily activities almost always have migraine (Dowson AJ et al. The prevalence and diagnosis of migraine in a primary care setting: Insights from the Landmark study. Headache Care2004; 1: In press). They can be given a default diagnosis of migraine (which is often confirmed at a later date). Migraine with aura This is an idiopathic, recurring disorder with attacks of neurological symptoms that arise in the cerebral cortex or the brain stem, creating the aura. The aura usually develops gradually over 5-20 minutes, lasts less than 60 minutes, and is completely reversible. Typical examples of an aura are: o Homonymous visual disturbance (the most common type), usually a fortification spectrum - a spreading, scintillating scotoma in the shape of a jagged crescent o Unilateral paraesthesia or numbness o Unilateral weakness o Dysphasia o A combination of the above The headache usually starts within 60 minutes of resolution of the aura, and lasts 4-72 hours. However, it may begin before the aura, or at the same time as the aura, or it may even be absent. The headache is typically unilateral, pulsating, of moderate or severe intensity, and is aggravated by normal physical activity. It is associated with nausea, vomiting, photophobia, and phonophobia. Two or more attacks are required to make the diagnosis. Twenty-five per cent of sufferers have this form. [Headache Classification Committee of the International Headache Society, 20004] What are the trigger factors? Trigger factors that precipitate attacks may be identified, but only in the minority of sufferers. Dietary triggers affect about 20% of people. Most attacks have no obvious trigger, and some triggers that are identified are unavoidable. Trigger factors include [BASH, 2000]: Stress (and relaxation after periods of stress) Certain foods (e.g. alcohol, cheese, citrus fruits, chocolate) Missing meals Too much or too little sleep Bright lights Loud noise Hormonal changes (menstruation and menopause) Page 4 of 12
5 Tension-type headache may be episodic or chronic. Each episode lasts between 30 minutes and 7 days, although the majority last less than 24 hours. The pain is of a pressing or tightening character, and is not pulsating. It is of mild to moderate intensity, which does not prohibit activity. It is usually bilateral. It is not aggravated by normal physical activity. There is no nausea or vomiting, although anorexia may occur. Photophobia or phonophobia are rare. Tension-type headache has no prodrome or aura. The pain can involve the frontal, temporal, occipital, or parietal regions; it may radiate to the neck or jaw; it can change location during an attack and tends to worsen across the day [Headache Classification Committee of the International Headache Society, 1988; Silberstein, 1993]. Cluster headache is unilateral and involves the eye and frontal region. Attacks may occur several times in 24 hours, and last from 15 minutes to 3 hours. Attacks occur in clusters, which usually last between 1 and 2 months; most sufferers experience one or two clusters a year. The pain is severe and associated with ipsilateral conjunctival injection, lacrimation, nasal congestion, rhinorrhoea, forehead and facial sweating, miosis, ptosis, and eyelid oedema. The character of the pain is burning, boring or piercing. It is six times more common in men than in women. The average age at onset is 30 years [Headache Classification Committee of the International Headache Society, 1988; Smetana, 2000]. Headache associated with raised cerebrospinal fluid pressure is often intermittent at first, but becomes constant and more severe as the cause of the raised pressure progresses. The pain is characteristically worse in the morning, and the person may be woken by it. It is worsened by changes in posture, particularly bending, and is improved by rest. Coughing, sneezing, straining, or vomiting exacerbates it. The headache is usually generalized. Headache is a feature in only a half of people with a cerebral tumour, and is the presenting symptom in less than 10% [Hilton-Jones, 2001]. Less than 1% of people with a non-migraine headache will have a brain tumour [DH, 2000]. Visual obscuration (episodes of blurred / cloudy vision) is associated with straining and is more likely to occur after periods of recumbancy. Medication overuse headache results from the chronic overuse of medication that is used to treat headache. It is estimated to affect 1 in 50 people. It was first recognized with ergotamine use. It is now associated with aspirin, paracetamol (especially when combined with codeine), NSAIDs, and 5HT 1 agonists (triptans). The headache varies in its quality, location, and intensity. Discontinuation of the drug worsens the headache before any improvement will occur; maximum improvement may take 6 months [Redillas and Solomon, 2000; BASH, 2000]. Trigeminal neuralgia is a painful affliction of the face. It is usually unilateral. It is characterized by brief lancinating pains limited to the distribution of one or more divisions of the trigeminal nerve. It is of unknown aetiology [Headache Classification Committee of the International Headache Society, 1988]. The diagnosis is made on the history alone. The features of the pain are characteristic. The pain occurs in paroxysms, which last from 2 seconds to 2 minutes. The frequency of the paroxysms can vary from several hundred a day to long periods of remission that can last for years [Headache Classification Committee of the International Headache Society, 1988; Zakrzewska, 2001]. Page 5 of 12
6 The pain is severe, and is described as intense, sharp, superficial, stabbing, burning, or like an electric shock. In each person the character of the pain is the same in different attacks [Headache Classification Committee of the International Headache Society, 1988; Zakrzewska, 2001]. The pain is felt in the distribution of one or more divisions of the trigeminal nerve. The most frequently affected divisions are the maxillary (35% of people) and mandibular (29%) alone; both the maxillary and mandibular divisions are affected in 19%. The ophthalmic division is the least frequently affected (4%of people). All three divisions are affected in only 1% of people. The pain occurs bilaterally in 3% of people [Katusic et al, 1990]. The pain is often triggered by trivial stimuli, e.g. touch, eating, washing, shaving, brushing the teeth, or talking [Headache Classification Committee of the International Headache Society, 1988; Zakrzewska, 2001]. Between paroxysms the person is asymptomatic. The person is usually free of pain at night. What else might it be? Dental disease (e.g. apical abscess) can cause paroxysmal as well as continuous pain. The overall features should, however, readily distinguish this from trigeminal neuralgia. Atypical facial pain causes a constant dull ache in the maxillary and cheek areas, which can extend to affect the whole side of the head and the neck. Cluster headache occurs in paroxysms, but the characteristic features readily distinguish this from trigeminal neuralgia. Cluster headache is unilateral and involves the eye and frontal region. Attacks may occur several times in 24 hours, and last from 15 minutes to 3 hours. Attacks occur in clusters, which usually last for between 1 and 2 months; most sufferers experience one or two clusters a year. The pain is severe and associated with ipsilateral conjunctival injection, lacrimation, nasal congestion, rhinorrhoea, forehead and facial sweating, miosis, ptosis, and eyelid oedema. The character of the pain is burning, boring, or piercing. Multiple sclerosis (MS) causes trigeminal neuralgia in 4% of affected people, although it is rarely a presenting feature. Trigeminal neuralgia tends to occur in younger people with MS, and may be bilateral. Postherpetic neuralgia is readily distinguished by the history of shingles in the distribution of the pain. Other cranial neuralgias (e.g. glossopharyngeal, nervus intermedius, superior laryngeal, occipital) can all cause pain that is of similar character to, but in a different site from, trigeminal neuralgia. Primary tumours of the trigeminal nerve, or compression of the nerve (e.g. by a tumour or aneurysm) can very rarely cause features of trigeminal neuralgia. They more commonly cause continuous pain or numbness, and usually there are abnormal clinical signs. Temporal Arteritis: Consider temporal arteritis in any patient over 50 presenting with new headache. Classic features include headaches with jaw claudication, enlarged, tender & non-pulsatile temporal arteries and possible visual catastrophe. ESR usually considerably raised, although if index of suspicion high and ESR low, check CRP. Page 6 of 12
7 Examination: A central nervous system (CNS) and general examination, as guided by the history, should be performed in all cases. It is likely to be normal in most people, but is essential in order to exclude serious causes of headache and to allay the person's anxiety. Of people referred to outpatients because of headache, less than 1% had an intracranial lesion; each person with an intracranial lesion had physical signs of it [BASH, 2000]. Fundoscopy and blood pressure must always be performed to exclude papilloedema and hypertension. It is often sensible to repeat fundoscopy at review appointments [BASH, 2000]. Look for meningeal irritation, specifically for neck stiffness, back pain, and Kernig's sign. Meningeal irritation may be due to infection, blood (e.g. subarachnoid haemorrhage), or neoplastic infiltration. Palpation of the face and neck, including the temporal arteries, is an important part of the examination. Investigations: Most people need no investigation. There are no diagnostic tests for the most common causes of headache. An erythrocyte sedimentation rate (ESR) measurement and possible temporal artery biopsy should be considered if the history suggests giant cell arteritis. Skull X-ray is useful following a severe head injury, but is otherwise obsolete. Neuroimaging (computed tomography, CT, or magnetic resonance imaging, MRI) is unlikely to reveal positive findings in people without a history suggestive of a serious cause of headache, or without abnormal clinical signs. A recent Cochrane review recommended that neuroimaging is not warranted in people with typical migraine; but that the role of neuroimaging in people with non-migraine headache is still unclear [Frishberg, 1994]. Red flags: Rule out serious causes of headache, particularly in the elderly (e.g. subarachnoid haemorrhage, meningitis, space-occupying lesion, giant-cell arteritis). Sinister features include headaches that are: Worst in the morning (it may wake the person from sleep). Worsened by changes in posture, especially bending. Coughing, sneezing, straining, or vomiting exacerbates it. Associated with: o Vomiting & drowsiness. o Progressive neurological deficit. o Cognitive changes. Page 7 of 12
8 Papilloedema. Hypertension, especially onset with headache. Meningeal irritation; look specifically for neck stiffness, back pain, and Kernig's sign. Urgent referral is indicated for people with the following symptoms or signs: Presentation with 'first and worst' headache, especially acute onset with associated neurological signs A new headache with subacute onset that is progressively worsening (over days or weeks) Headache with unexplained fever, nausea, or vomiting Associated focal neurological signs, papilloedema, changes in consciousness or cognition, or stiff neck The Department of Health Referral Guidelines for Suspected Brain Tumours recommend urgent referral, under the 2 week standard, for people with headache, vomiting, and papilloedema. They also recommend that urgent referral, under the 2 week standard, is considered for 'people with non-migrainous headaches of recent onset, present for at least one month, when accompanied by features suggestive of raised intracranial pressure e.g. woken by headache, vomiting, drowsiness'. However GPs should use 'their discretion to decline urgent referral if there are other known features e.g. depression, somatisation disorder, making a diagnosis of brain tumour extremely unlikely.' The Department of Health Referral Guidelines for Suspected Children's Tumours recommend urgent referral, under the 2 week standard, for children (under 15 years) with headache of recent onset with one or more of the following features: Increasing in severity and frequency Worse in the mornings or causing early morning wakening Associated with vomiting Associated with neurological signs (e.g. squint, ataxia) Associated with behavioural change or deterioration in school performance Treatment: Migraine: It is important to note that the NNT (Number Needed to Treat) for even the best migraine prophylactic therapies is 3: In other words, to get a response in one person (> 50% reduction in pain/severity or frequency vs. placebo), 3 patients have to receive the drug. Corollary: You will be less successful with two out of every three patients treated. Therefore, the basis of migraine treatment is try and try again with increasing doses of migraine prophylactic treatment until one of three end-points is achieved: Success Page 8 of 12
9 Side-effects: Reduce to previous dose (if partially effective) or move on to next prophylactic. Maximum dose: Move on to next prophylactic. The Consultant neurologists would approach migraine treatment in exactly the same fashion: This can be more appropriately conducted in primary care. Acute Treatment options (1 st line): Analgesia +/- antiemetic. Aspirin 900mg + metoclopramide 10mg or domperidone 10mg (stat.) at earliest point following onset of indication of headache (pain or aura). If aspirin not tolerated (or C/I): Substitute with paracetamol 1g or ibuprofen 400mg 600mg. Alternatives include: Diclofenac, naproxen or tolfenamic acid. The first two are not specifically licensed for migraine, but are often used and are specifically mentioned in Prodigy. Note: Soluble forms are generally recommended to speed absorption. If vomiting problematic: Try domperidone 30mg + diclofenac Na 25mg suppositories tds, reverting to oral therapy when vomiting settled. Acute Treatment options (2 nd line): Triptans. Replace analgesic with triptan, used at earliest point following onset/indication of headache (pain or aura). The North Derbyshire Formulary includes two based on efficacy and cost: - Almotriptan Rizatriptan If there is no initial response: A further dose should not be taken for the same attack (except Zolmitriptan). Revert to first line Rx. If headache recurs: Another dose can be taken provided it is >2hrs (4hrs for Naratriptan) after the initial dose was taken. Note: Use should be strictly limited to no more than 12 doses per month, as it is now recognised that triptans can cause MOH (Medication Overuse Headache). Prophylactic treatment options: Consider with: 2* attacks/month (Prodigy) * It has been suggested that >2 attacks per week should be the threshold for prophylaxis (Lancet 2004; 363:381-91), although other reviews suggest 2 attacks/month (NEJM 2002; 346: & Ann Intern Med 2002; 137:840-49) if Page 9 of 12
10 attacks are disabling. GPs should use their professional judgement to define with their patients when prophylactic treatment is justified. Less frequent but severe or prolonged attacks Frequent use of acute treatments (to reduce incidence of MOH) Note on acute Rx: May still be required as severity and frequency are usually only reduced by prophylaxis. Note on prophylactic Rx: Prophylactic drugs need to be tried for 1-3 months before the full effect is seen. It is possible that patients may need a monthly review at each dose level. Prophylactic Rx may then be continued at the most appropriate dose for 6 months before a trial off Rx (gradual withdrawal) to see whether they are still required. If required, subsequent trials can be conducted when deemed appropriate by GP and Patient. 1 st option: Betablockers (E.g. propranolol but also metoprolol or atenolol (unlicensed)) Assuming no C/I, try propranolol at 40mg bd, increasing to 120mg bd, or maximum tolerated dose, by increases of %, at no sooner than monthly intervals. 2 nd option: Amitriptylline (unlicensed): Try starting with 10mg nocte, increasing to 100mg, or maximum tolerated dose, by increases of %, at no sooner than monthly intervals. (A slow and cautious start to treatment with amitriptylline often helps avoid abandoning Rx due to S/E). 3 rd options: Valproate, Nifedipine, NSAIDs (e.g. naproxen), pizotifen & clonidine (although RCTs suggest ineffective and not recommended by BNF), verapamil, SSRIs (e.g. fluoxetine), topiramate, etc: Multiple options, but see prodigy for further details ( ) 4 th option: Acupuncture may be worth suggesting: (See BMJ 2004; 328:744-7 & 747-9) Tension-type headache (TTH): 1 st /2 nd option: Betablockers (E.g. propranolol but also metoprolol or atenolol (unlicensed)) Assuming no C/I, try propranolol at 40mg bd, increasing to 320mg, or maximum tolerated dose, by increases of %, at no sooner than monthly intervals. 1 st /2 nd option: Amitriptylline (unlicensed): Try starting with 10mg nocte, increasing to 100mg, or maximum tolerated dose, by increases of %, at no sooner than monthly intervals. (A slow and cautious start to treatment with amitriptylline often helps avoid abandoning Rx due to S/E). 3 rd option: Counselling: Those with obvious psychosocial stresses may benefit more through counselling, particularly if lifelong coping strategies are learnt. Page 10 of 12
11 4 th option: Valproate: (BMJ 2002; 325:881-6) Cluster headache: Acute attacks: Notes: Analgesics have no place in acute treatment Avoid alcohol or nitrates (if considered triggers). Try triptan injection or nasal spray. Oxygen (See BNF & BMJ 2002; 325:881-6) Prophylaxis: 1 st option: Verapamil 240 (-960)mg/day 2 nd option: Topiramate or Valproate A short course of oral steroids is often helpful whilst introducing prophylactic Rx; e.g. prednisolone 20mg/day x6 days. 3 rd options: Lithium (or Methylsergide: Only prescribed by specialist.) Medication Overuse Headache (MOH): Withdrawal of offending analgesic but beware temporary exacerbation of MOH. A six day course of prednisolone 20mg/day may be helpful in this situation. Reassess any residual headache for diagnosis and appropriate Rx if needed. Trigeminal Neuralgia: 1 st option: Carbamazepine: mg bd increasing slowly to 1.2g/day. Sometimes doses as high as 1.6-2g/day might be necessary. 2 nd option: Phenytoin: 100mg od increasing slowly to 300-(350mg) od (but beware S/E and non-linear pharmacodynamics) 3 rd option: Gabapentin: Try 300mg once daily, increasing to 300mg bd on day 2, then 300mg tds on day 3: Thereafter, dose can be increased by increments of 300mg per day, up to 1800mg/day, but is better tolerated at slower increases, e.g. bi-weekly. 4 th option: Sodium Valproate: Try 200mg bd, increasing to 2400mg, or maximum tolerated dose, by increases of 200mg, at no sooner than weekly intervals. Page 11 of 12
12 Note 1: Lamotrigine and baclofen may also be tried, and amitriptylline might prove helpful. Note 2: Tricyclic antidepressants have been shown to be effective in the treatment of neurogenic pain generally. However there are no studies of their efficacy specifically in trigeminal neuralgia, although anecdotally, they may prove helpful in some patients. Prodigy: Also see the Prodigy guidelines (hyperlinked): Migraine: Acute Rx 1 st line Acute Rx failure Prophylaxis Non-migrainous headache Trigeminal neuralgia Referrals: Temporal arteritis: Same day admission under Physician on-call. (Treatment with steroids should normally be commenced on suspicion of the diagnosis: Initial dose 40mg/day; consider 60mg/day if visual symptoms). Red flag referrals: Neurologists: 2w Urgent Undiagnosed headache or Unresponsive headaches: Neurologists (or GPSI headache clinic): Routine. Referrals must show evidence of: At least two treatment approaches at adequate dosage for diagnosed headaches, or At least two therapeutic trials at adequate dosage for undiagnosed headaches. Patient Information: Non-migraine headache: Headaches: A summary Tension-type headache Medication overuse headache Migraine: Migraine Migraine - Drugs to Prevent Attacks Migraine Action Association Migraine Trust Trigeminal neuralgia: Trigeminal neuralgia Trigeminal Neuralgia Association UK REB:19/05/2004 Page 12 of 12
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy
 HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline. Scottish intercollegiate Guidelines Network SIGN
 A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE
 Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
Adult with headache. Problem-specific video guides to diagnosing patients and helping them with management and prevention
 Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
MIGRAINE A MYSTERY HEADACHE
 MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
HEADACHE. Dr Nick Pendleton. September Headache
 HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
Management of headache
 Management of headache TJ Steiner Imperial College London Based on European principles of management of common headache disorders TJ Steiner, K Paemeleire, R Jensen, D Valade, L Savi, MJA Lainez, H-C Diener,
Management of headache TJ Steiner Imperial College London Based on European principles of management of common headache disorders TJ Steiner, K Paemeleire, R Jensen, D Valade, L Savi, MJA Lainez, H-C Diener,
25/09/2018 HEADACHE. Dr Nick Pendleton
 HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
How do we treat migraine? New SIGN Guidelines
 How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
MIGRAINE UPDATE. Objectives & Disclosures. Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment.
 MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
Primary Care Adult Headache Management Pathway (formerly North West Headache Management Guideline for Adults) Version 1.0
 Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Neuralgias tend to be sudden, brief, intermittent severe, stabbing or lightning pains or electric shock sensations.
 Neuralgia is the term used to describe pain arising from a nerve. There are many different neuralgias which have been described in the medical literature, but I will only touch upon a few more common ones.
Neuralgia is the term used to describe pain arising from a nerve. There are many different neuralgias which have been described in the medical literature, but I will only touch upon a few more common ones.
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา
 ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
Chronic Daily Headaches
 Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Headache. Section 1. Migraine headache. Clinical presentation
 Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
2) Headache - Dr. Hawar
 2) Headache - Dr. Hawar Headache is caused by traction, displacement, inflammation, vascular spasm, or distention of the painsensitive structures in the head or neck. Isolated involvement of the bony skull,
2) Headache - Dr. Hawar Headache is caused by traction, displacement, inflammation, vascular spasm, or distention of the painsensitive structures in the head or neck. Isolated involvement of the bony skull,
Index. Prim Care Clin Office Pract 31 (2004) Note: Page numbers of article titles are in boldface type.
 Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Reflections on NICE Headache Guideline. Dr Kay Kennis GPwSI in Headache, Bradford
 Reflections on NICE Headache Guideline Dr Kay Kennis GPwSI in Headache, Bradford Overview The process of guideline development illustrated with the headache guideline Reflections on the process Key recommendations
Reflections on NICE Headache Guideline Dr Kay Kennis GPwSI in Headache, Bradford Overview The process of guideline development illustrated with the headache guideline Reflections on the process Key recommendations
Headache and Facial Pain. Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology
 Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Paediatric headaches. Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services. Brevity, levity, repetition
 Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
Managing Headache in General Practice 2nd Edition
 1 Managing Headache in General Practice 2nd Edition Dr Raeburn Forbes Consultant Neurologist November 2012 Email: elaine.johnston@southerntrust.hscni.net Department of Neurology Craigavon Area Hospital
1 Managing Headache in General Practice 2nd Edition Dr Raeburn Forbes Consultant Neurologist November 2012 Email: elaine.johnston@southerntrust.hscni.net Department of Neurology Craigavon Area Hospital
Do you suffer from Headaches? - November/Dec 2011
 Do you suffer from Headaches? - November/Dec 2011 Inside this month's issue Headaches Acute single headaches Recurring Headaches: Migraine What causes Migraine? Treatments for migraine & prevention Headaches
Do you suffer from Headaches? - November/Dec 2011 Inside this month's issue Headaches Acute single headaches Recurring Headaches: Migraine What causes Migraine? Treatments for migraine & prevention Headaches
Migraine Management. Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital
 Migraine Management Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital Referral Criteria for Migraine Migraine Management Migraine Diagnosis Spot on Health Migraine pathway
Migraine Management Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital Referral Criteria for Migraine Migraine Management Migraine Diagnosis Spot on Health Migraine pathway
Headache Mary D. Hughes, MD Neuroscience Associates
 Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Classification of headaches
 Classification of headaches Primary headaches OR Idiopathic headaches Secondary headaches OR Symptomatic headaches THE HEADACHE IS ITSELF THE DISEASE NO ORGANIC LESION IN THE BEACKGROUND TREAT THE HEADACHE!
Classification of headaches Primary headaches OR Idiopathic headaches Secondary headaches OR Symptomatic headaches THE HEADACHE IS ITSELF THE DISEASE NO ORGANIC LESION IN THE BEACKGROUND TREAT THE HEADACHE!
GENERAL APPROACH AND CLASSIFICATION OF HEADACHES
 GENERAL APPROACH AND CLASSIFICATION OF HEADACHES CLASSIFICATION Headache is one of the most common medical complaints. Most of the population will have experienced headache, and over 5% will seek medical
GENERAL APPROACH AND CLASSIFICATION OF HEADACHES CLASSIFICATION Headache is one of the most common medical complaints. Most of the population will have experienced headache, and over 5% will seek medical
HEADACHES THE RED FLAGS
 HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
Migraine. What are the symptoms of a migraine attack?
 Migraine Migraine causes attacks of headaches, often with feeling sick or vomiting. Treatment options include: avoiding possible 'triggers', painkillers, antiinflammatory painkillers, anti-sickness medicines,
Migraine Migraine causes attacks of headaches, often with feeling sick or vomiting. Treatment options include: avoiding possible 'triggers', painkillers, antiinflammatory painkillers, anti-sickness medicines,
Faculty Disclosure. Karen L. Bremer, MD. Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest.
 Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
Management options for Migraine. Prof. Dr. Khwaja Nazimuddin Head Dept. of Internal Medicine BIRDEM
 Management options for Migraine Prof. Dr. Khwaja Nazimuddin Head Dept. of Internal Medicine BIRDEM Assessment The Migraine Disability Assessment Score MIDAS Complete loss of work Partial loss of work Off
Management options for Migraine Prof. Dr. Khwaja Nazimuddin Head Dept. of Internal Medicine BIRDEM Assessment The Migraine Disability Assessment Score MIDAS Complete loss of work Partial loss of work Off
Managing Headache in Acute Medicine. Ben Lovell Consultant Physician in Acute Medicine University College London Hospital
 Managing Headache in Acute Medicine Ben Lovell Consultant Physician in Acute Medicine University College London Hospital Some ED headache stats Arrive by ambulance 31% Median age 39 Worst ever headache
Managing Headache in Acute Medicine Ben Lovell Consultant Physician in Acute Medicine University College London Hospital Some ED headache stats Arrive by ambulance 31% Median age 39 Worst ever headache
Outpatient Headache Care Guideline
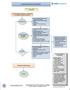 1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
PAEDIATRIC ACUTE CARE GUIDELINE. Headache. This document should be read in conjunction with this DISCLAIMER
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert
 Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Disclosures. Objectives 6/2/2017
 Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017
 Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017 SAH v benign thunderclap headaches Other pathologies not apparent on CT Severe primary headaches: management
Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017 SAH v benign thunderclap headaches Other pathologies not apparent on CT Severe primary headaches: management
Headache Management in Primary Care Dr Niranjanan Nirmalananthan Consultant Neurologist
 Headache Management in Primary Care Dr Niranjanan Nirmalananthan Consultant Neurologist Wednesday 10 th of April 2019 Summary Why does it matter? Classification and diagnosis Who to refer / scan? Serious
Headache Management in Primary Care Dr Niranjanan Nirmalananthan Consultant Neurologist Wednesday 10 th of April 2019 Summary Why does it matter? Classification and diagnosis Who to refer / scan? Serious
BOTULINUM TOXIN POLICY TO INCLUDE:
 BOTULINUM TOXIN POLICY TO INCLUDE: Blepharospasm in adults, Hemi facial spasm in adults, spasmodic torticollis (cervical dystonia), focal spasticity treatment of dynamic equinus foot deformity, focal spasticity
BOTULINUM TOXIN POLICY TO INCLUDE: Blepharospasm in adults, Hemi facial spasm in adults, spasmodic torticollis (cervical dystonia), focal spasticity treatment of dynamic equinus foot deformity, focal spasticity
July 2012 Target Population. Adult patients 18 years or older in primary care settings.
 Guideline for Primary Care Management of Headache in Adults July 2012 Target Population Adult patients 18 years or older in primary care settings. Exclusions: This guideline does not provide recommendations
Guideline for Primary Care Management of Headache in Adults July 2012 Target Population Adult patients 18 years or older in primary care settings. Exclusions: This guideline does not provide recommendations
Headache is the most common symptom in patients with Idiopathic Intracranial Hypertension (IIH). Not everybody with IIH gets headache.
 Headaches in Idiopathic Intracranial Hypertension Headache is the most common symptom in patients with Idiopathic Intracranial Hypertension (). Not everybody with gets headache. Headaches can be there
Headaches in Idiopathic Intracranial Hypertension Headache is the most common symptom in patients with Idiopathic Intracranial Hypertension (). Not everybody with gets headache. Headaches can be there
Teeth and supporting tissues, e.g. dental. Maxillary sinus, salivary gland
 MJDF Facial Pain. Patricia Thomson Always start with SOCRATES S site O onset C character R radiation A associated features T timing E exacerbating/relieving factors S severity Examine the cranial nerves
MJDF Facial Pain. Patricia Thomson Always start with SOCRATES S site O onset C character R radiation A associated features T timing E exacerbating/relieving factors S severity Examine the cranial nerves
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation.
 I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
Trigeminal Autonomic Cephalalgias. Disclosures. Objectives 6/20/2018. Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018
 Trigeminal Autonomic Cephalalgias Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018 Disclosures Honoraria from Allergan and Amgen for advisory board, Current Neurology and Neuroscience Reports
Trigeminal Autonomic Cephalalgias Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018 Disclosures Honoraria from Allergan and Amgen for advisory board, Current Neurology and Neuroscience Reports
Treatments for migraine
 Treatments for migraine Information for patients and carers Department of Neurology Aberdeen Royal Infirmary Contents Page About this leaflet Abortive medication for migraine Painkillers Antisickness medication
Treatments for migraine Information for patients and carers Department of Neurology Aberdeen Royal Infirmary Contents Page About this leaflet Abortive medication for migraine Painkillers Antisickness medication
Neuralgias T R I G E M I N A L N E U R A L G I A
 Neuralgias T R I G E M I N A L N E U R A L G I A (MEANS PAIN IN A NERVE) Definition of pain Facial pain Cranial neuralgias are commonly distinct in two groups: typical neuralgias and atypical facial pain.
Neuralgias T R I G E M I N A L N E U R A L G I A (MEANS PAIN IN A NERVE) Definition of pain Facial pain Cranial neuralgias are commonly distinct in two groups: typical neuralgias and atypical facial pain.
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, II. Management of Refractory Headaches
 Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Improving Headache Care
 Greater Manchester Neuroscience Centre Improving Headache Care (without breaking the bank) Implementation of useful referral guidelines Scale of the problem Over 10% population suffer from headache 2%
Greater Manchester Neuroscience Centre Improving Headache Care (without breaking the bank) Implementation of useful referral guidelines Scale of the problem Over 10% population suffer from headache 2%
10/31/2017 PRIMARY CARE AND HEADACHE DISCLOSURES WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Primary Care 67%
 PRIMARY CARE AND HEADACHE Sonja Potrebic MD PhD Regional Headache Specialist Kaiser LAMC 1 WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Column1 Primary Care 67% Primary Care Headache Specialty Other
PRIMARY CARE AND HEADACHE Sonja Potrebic MD PhD Regional Headache Specialist Kaiser LAMC 1 WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Column1 Primary Care 67% Primary Care Headache Specialty Other
A case of a patient with chronic headache. Focus on Migraine. None related to the presentation Grants to conduct clinical trials from: Speaker bureau:
 Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
SIGN on the pharmacological management of migraine
 GUIDELINES SIGN on the pharmacological management of migraine STEVE CHAPLIN In February 2018, the Scottish Intercollegiate Guidelines Network (SIGN) published a new guideline on the pharmacological management
GUIDELINES SIGN on the pharmacological management of migraine STEVE CHAPLIN In February 2018, the Scottish Intercollegiate Guidelines Network (SIGN) published a new guideline on the pharmacological management
Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis
 Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis Noboru Imai(Department of Neurology, Japanese Red Cross
Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis Noboru Imai(Department of Neurology, Japanese Red Cross
Chronic Migraine in Primary Care. December 11 th, 2017 Werner J. Becker University of Calgary
 Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE
 Headache in children and adolescents Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE Dept. of Psychiatry of Childhood and Adolescence Medical University of Vienna, Vienna, Austria Impact
Headache in children and adolescents Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE Dept. of Psychiatry of Childhood and Adolescence Medical University of Vienna, Vienna, Austria Impact
Headache. Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016
 Headache Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016 Contents General thoughts Primary headache Secondary headache I want to curl up in a cave and die I want to drill a
Headache Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016 Contents General thoughts Primary headache Secondary headache I want to curl up in a cave and die I want to drill a
Common Headaches. Types and Natural Treatments
 Common Headaches Types and Natural Treatments by Heidi Fritz, MA, ND Bolton Naturopathic Clinic 64 King St W, Bolton, Ontario, L7E1C7 www.boltonnaturopathic.ca Three Common Types of Headaches Headaches
Common Headaches Types and Natural Treatments by Heidi Fritz, MA, ND Bolton Naturopathic Clinic 64 King St W, Bolton, Ontario, L7E1C7 www.boltonnaturopathic.ca Three Common Types of Headaches Headaches
OH, MY ACHING HEAD! I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE MANAGING HEADACHE IN THE OUTPATIENT SETTING SECONDARY HEADACHES
 1 JUSTIN A. OSSMAN, MD CHATTANOOGA FAMILY MEDICINE UPDATE OH, MY ACHING HEAD! MANAGING HEADACHE IN THE OUTPATIENT SETTING 2 I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE OBJECTIVES International
1 JUSTIN A. OSSMAN, MD CHATTANOOGA FAMILY MEDICINE UPDATE OH, MY ACHING HEAD! MANAGING HEADACHE IN THE OUTPATIENT SETTING 2 I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE OBJECTIVES International
ADVANCES IN MIGRAINE MANAGEMENT
 ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
Case Presentation. Case Presentation. Case Presentation. Truths about Headaches (2017) Most headaches were muscle-tension headaches
 Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
Trigeminal Neuralgia Association UK. Facing pain together TRIGEMINAL NEURALGIA AN OVERVIEW
 Trigeminal Neuralgia Association UK Facing pain together TRIGEMINAL NEURALGIA AN OVERVIEW The TNA UK was established to provide support and information to people affected by trigeminal neuralgia and we
Trigeminal Neuralgia Association UK Facing pain together TRIGEMINAL NEURALGIA AN OVERVIEW The TNA UK was established to provide support and information to people affected by trigeminal neuralgia and we
By Nathan Hall Associate Editor
 By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
HEADACHE. Summary of British Association on the Study of Headaches {click to visit}
 F:M=3:1 Affects 15% adults HEADACHE Summary of British Association on the Study of Headaches {click to visit} Primary: Migraine (with aura 1/3, without aura 2/3) Tension Cluster Other Secondary Neuralgia
F:M=3:1 Affects 15% adults HEADACHE Summary of British Association on the Study of Headaches {click to visit} Primary: Migraine (with aura 1/3, without aura 2/3) Tension Cluster Other Secondary Neuralgia
HEADACHES AND MIGRAINES
 HEADACHES AND MIGRAINES CONTENT CREATED BY Learn more at www.health.harvard.edu TALK WITH YOUR DOCTOR Table of Contents Whether this is your first visit or a follow-up, answer these questions for your
HEADACHES AND MIGRAINES CONTENT CREATED BY Learn more at www.health.harvard.edu TALK WITH YOUR DOCTOR Table of Contents Whether this is your first visit or a follow-up, answer these questions for your
Subject: CGRP Inhibitors
 ARCHIVED (NOT ACTIVE RETIRED) Archived: 08/01/18 09-J2000-98 Original Effective Date: 06/15/18 Reviewed: 05/09/18 Revised: 08/01/18 Next Review: ARCHIVED (NOT ACTIVE RETIRED) Subject: CGRP Inhibitors THIS
ARCHIVED (NOT ACTIVE RETIRED) Archived: 08/01/18 09-J2000-98 Original Effective Date: 06/15/18 Reviewed: 05/09/18 Revised: 08/01/18 Next Review: ARCHIVED (NOT ACTIVE RETIRED) Subject: CGRP Inhibitors THIS
Neurological Dilemmas in Primary Care
 Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
Update on Diagnosis and Management of Migraines
 Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
Diagnosis of Primary Headache Syndromes. Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center
 Diagnosis of Primary Headache Syndromes Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center Goals Distinguish primary from secondary headaches Recognize typical histories
Diagnosis of Primary Headache Syndromes Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center Goals Distinguish primary from secondary headaches Recognize typical histories
Headaches in Children and Adolescents. Paul Shillito
 Headaches in Children and Adolescents Paul Shillito Topics For Discussion What s different about childhood migraine Chronic daily headache (CDH) Tumours and other things to worry about Management of childhood
Headaches in Children and Adolescents Paul Shillito Topics For Discussion What s different about childhood migraine Chronic daily headache (CDH) Tumours and other things to worry about Management of childhood
Cluster headache (CH): epidemiology, classification and clinical picture
 Cluster headache (CH): epidemiology, classification and clinical picture Toomas Toomsoo, M.D. Head of the Center of Neurology East Tallinn Central Hospital 1 INTRODUCTION Cluster headache - known as trigeminal
Cluster headache (CH): epidemiology, classification and clinical picture Toomas Toomsoo, M.D. Head of the Center of Neurology East Tallinn Central Hospital 1 INTRODUCTION Cluster headache - known as trigeminal
Medication For Migraine Chart: Table 1: Acute Treatment when the attack begins
 Medication For Migraine Chart: Table 1: Acute Treatment when the attack begins Page a Analgesics (painkillers) Non-steroidal antiinflammatory drugs (NSAIDs) Prescription required Brand Name Formulation
Medication For Migraine Chart: Table 1: Acute Treatment when the attack begins Page a Analgesics (painkillers) Non-steroidal antiinflammatory drugs (NSAIDs) Prescription required Brand Name Formulation
Stuart Weatherby Consultant Neurologist Derriford Hospital. Plymouth
 Stuart Weatherby Consultant Neurologist Derriford Hospital. Plymouth What is chronic headache? What are the causes? Why do people get headaches anyway? Why are there different sorts of headache? A model
Stuart Weatherby Consultant Neurologist Derriford Hospital. Plymouth What is chronic headache? What are the causes? Why do people get headaches anyway? Why are there different sorts of headache? A model
Painless, progressive weakness Could this be Motor Neurone Disease?
 APPENDIX 1 Painless, progressive weakness Could this be Motor Neurone Disease? 1. Does the patient have one or more of these? Bulbar features Limb features Respiratory features Cognitive features (rare)
APPENDIX 1 Painless, progressive weakness Could this be Motor Neurone Disease? 1. Does the patient have one or more of these? Bulbar features Limb features Respiratory features Cognitive features (rare)
FINANCIAL DISCLOSURE. No relevant financial relationships
 Sleep and Headache Paul Mathew, MD, FAHS Director of Continuing Medical Education John R. Graham Headache Center Brigham & Women s Hospital Director of Headache Medicine Cambridge Health Alliance Harvard
Sleep and Headache Paul Mathew, MD, FAHS Director of Continuing Medical Education John R. Graham Headache Center Brigham & Women s Hospital Director of Headache Medicine Cambridge Health Alliance Harvard
Current Migraine Treatment Therapy. Daniel Kassicieh, DO, FAAN
 Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
11. HEADACHE 1. Pablo Lapuerta, MD, Steven Asch, MD, MPH, and Kenneth Clark, MD, MPH
 11. HEADACHE 1 Pablo Lapuerta, MD, Steven Asch, MD, MPH, and Kenneth Clark, MD, MPH We identified articles on the evaluation and management of headache by conducting a MEDLINE search of English language
11. HEADACHE 1 Pablo Lapuerta, MD, Steven Asch, MD, MPH, and Kenneth Clark, MD, MPH We identified articles on the evaluation and management of headache by conducting a MEDLINE search of English language
Recognition and treatment of medication overuse headache
 Recognition and treatment of medication overuse headache Marcus Lewis MA, MRCGP, DRCOG, DFSRH 20 Mean weekly headache index 15 10 5 Medication overuse headache is a common condition responsible for a high
Recognition and treatment of medication overuse headache Marcus Lewis MA, MRCGP, DRCOG, DFSRH 20 Mean weekly headache index 15 10 5 Medication overuse headache is a common condition responsible for a high
INSTITUTE OF NEUROLOGY
 INSTITUTE OF NEUROLOGY HEADACHE AND FACIAL PAIN QUESTIONNAIRE Date / / SECTION 1: PERSONAL DETAILS Surname Date of Birth / / First Name Age Hospital Number Sex Male Female Handedness Right Left Ambidextrous
INSTITUTE OF NEUROLOGY HEADACHE AND FACIAL PAIN QUESTIONNAIRE Date / / SECTION 1: PERSONAL DETAILS Surname Date of Birth / / First Name Age Hospital Number Sex Male Female Handedness Right Left Ambidextrous
Brain and Central Nervous System Cancers
 Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Headache Pain Generators
 Objectives 1. Define the major categories of headache. 2. Take a history directed at characterizing a headache pattern in an individual patient and identify the cause or triggers of the headache. 3. Understand
Objectives 1. Define the major categories of headache. 2. Take a history directed at characterizing a headache pattern in an individual patient and identify the cause or triggers of the headache. 3. Understand
Diagnosing headache. The clinician should approach the diagnosis of. Secondary headache. Primary headache. Blue and red flag headaches
 Headache THEME Diagnosing headache BACKGROUND A systematic approach to the diagnosis of primary and secondary headache disorders requires the measurement of the frequency and the duration of headache.
Headache THEME Diagnosing headache BACKGROUND A systematic approach to the diagnosis of primary and secondary headache disorders requires the measurement of the frequency and the duration of headache.
HEADACHE Transient discomfort, chronic nuisance, or looming disaster?
 HEADACHE Transient discomfort, chronic nuisance, or looming disaster? Hussien H. Rizk, MD Cairo University Medical School ١ Headache Second most common o symptom (after pain) Migraine alone afflicts 12
HEADACHE Transient discomfort, chronic nuisance, or looming disaster? Hussien H. Rizk, MD Cairo University Medical School ١ Headache Second most common o symptom (after pain) Migraine alone afflicts 12
Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital
 Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital Honorarium from Current Pain and Headache Reports; Section Editor Unusual
Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital Honorarium from Current Pain and Headache Reports; Section Editor Unusual
HEADACHE HISTORY & PROFILE QUESTIONNAIRE
 1 HEADACHE HISTORY & PROFILE QUESTIONNAIRE Patient Name: On what part of the head do your headaches start? R Side L Side Either Side Both Sides Back On Top Temples Behind/AroundEyes Forehead Face Neck
1 HEADACHE HISTORY & PROFILE QUESTIONNAIRE Patient Name: On what part of the head do your headaches start? R Side L Side Either Side Both Sides Back On Top Temples Behind/AroundEyes Forehead Face Neck
Goals. Primary Headache Syndromes. One-Year Prevalence of Common Headache Disorders
 Goals One-Year Prevalence of Common Headache Disorders Impact of primary headache syndromes Non pharmacologic Rx of migraine individualized to patient triggers Complementary and alternative Rx of migraine
Goals One-Year Prevalence of Common Headache Disorders Impact of primary headache syndromes Non pharmacologic Rx of migraine individualized to patient triggers Complementary and alternative Rx of migraine
Management of chronic headache. Author. Published. Journal Title. Copyright Statement. Downloaded from. Link to published version
 Management of chronic headache Author Beran, Roy Published 2014 Journal Title Australian Family Physician Copyright Statement 2014 Australian Family Physician. Reproduced with permission. Permission to
Management of chronic headache Author Beran, Roy Published 2014 Journal Title Australian Family Physician Copyright Statement 2014 Australian Family Physician. Reproduced with permission. Permission to
NEUROPATHIC CANCER PAIN STANDARDS AND GUIDELINES
 NEUROPATHIC CANCER PAIN STANDARDS AND GUIDELINES GENERAL PRINCIPLES Neuropathic pain may be relieved in the majority of patients by multimodal management A careful history and examination are essential.
NEUROPATHIC CANCER PAIN STANDARDS AND GUIDELINES GENERAL PRINCIPLES Neuropathic pain may be relieved in the majority of patients by multimodal management A careful history and examination are essential.
PREVALENCE BY HEADACHE TYPE
 CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
HEADACHE P of o. G. G Z u Z l u iani
 HEADACHE Prof. G. Zuliani General Statistics Everyone has headaches (HA) Second most common complain after back pain in the population More than 80 million Emergency Room visits in USA per year Frequency
HEADACHE Prof. G. Zuliani General Statistics Everyone has headaches (HA) Second most common complain after back pain in the population More than 80 million Emergency Room visits in USA per year Frequency
Patient with Daily Headache NTERNATIONAL CLASSIFICATION HEADACHE DISORDERS. R. Allan Purdy, MD, FRCPC,FACP. Professor of Medicine (Neurology)
 Patient with Daily Headache NTERNATIONAL CLASSIFICATION of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) 2nd edition (ICHD-II) Learning Issues Headaches in the elderly
Patient with Daily Headache NTERNATIONAL CLASSIFICATION of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) 2nd edition (ICHD-II) Learning Issues Headaches in the elderly
Transcutaneous stimulation of the cervical branch of the vagus nerve for cluster headache and migraine
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Transcutaneous stimulation of the cervical branch of the vagus nerve for cluster headache and migraine Cluster
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Transcutaneous stimulation of the cervical branch of the vagus nerve for cluster headache and migraine Cluster
Vestibular Migraine. Information for patients and carers. Department of Neurology and Otolaryngology Aberdeen Royal Infirmary
 Vestibular Migraine Information for patients and carers Department of Neurology and Otolaryngology Aberdeen Royal Infirmary What is vestibular migraine? Migraine is a disabling headache disorder that affects
Vestibular Migraine Information for patients and carers Department of Neurology and Otolaryngology Aberdeen Royal Infirmary What is vestibular migraine? Migraine is a disabling headache disorder that affects
Migraine Management. Jane Melling Headache nurse Mater Misericordiae Hospital
 Migraine Management Jane Melling Headache nurse Mater Misericordiae Hospital Migraine facts Among the most common disorders of the nervous system 3 rd most prevalent medical disorder on the planet (lancet
Migraine Management Jane Melling Headache nurse Mater Misericordiae Hospital Migraine facts Among the most common disorders of the nervous system 3 rd most prevalent medical disorder on the planet (lancet
6/4/2018. Headache. Headaches. Headache. Migraine Headaches. Headache. Red Flag signs and symptoms. Imaging CT without contrast.
 Presented by M.D. Shepherd, M.D. OH MY ACHING HEAD! Estimated that one half of the adult population is affected by a headache disorder International Society Classification Primary : Tension s 40% of the
Presented by M.D. Shepherd, M.D. OH MY ACHING HEAD! Estimated that one half of the adult population is affected by a headache disorder International Society Classification Primary : Tension s 40% of the
continuing medical education
 In collaboration with Jeddah Primary Care CME unit This is a CME (Continuing Medical Education) article. It is presented to you in collaboration with the Middle East CME organizations. Self-test answers
In collaboration with Jeddah Primary Care CME unit This is a CME (Continuing Medical Education) article. It is presented to you in collaboration with the Middle East CME organizations. Self-test answers
MIGRAINE CLASSIFICATION
 MIGRAINE CLASSIFICATION Nada Šternić At most, only 30% of migraineurs have classic aura The same patient may have migraine headache without aura, migraine headache with aura as well as migraine aura without
MIGRAINE CLASSIFICATION Nada Šternić At most, only 30% of migraineurs have classic aura The same patient may have migraine headache without aura, migraine headache with aura as well as migraine aura without
Neuropathic Pain Treatment Guidelines
 Neuropathic Pain Treatment Guidelines Background Pain is an unpleasant sensory and emotional experience that can have a significant impact on a person s quality of life, general health, psychological health,
Neuropathic Pain Treatment Guidelines Background Pain is an unpleasant sensory and emotional experience that can have a significant impact on a person s quality of life, general health, psychological health,
Overview INTRODUCTION 3/15/2018. Headache Emergencies. Other way to differentiate between them? Is there an easy way to differentiate between them?
 Overview Headache Emergencies Primary versus Secondary headache disorder Red flags 4 cases of unusual headache emergencies Disclaimer: we will not talk about brain bleed as patients usually go the ED.
Overview Headache Emergencies Primary versus Secondary headache disorder Red flags 4 cases of unusual headache emergencies Disclaimer: we will not talk about brain bleed as patients usually go the ED.
Strategies in Migraine Care
 Strategies in Migraine Care Julie L. Roth, MD Rhode Island Hospital Assistant Professor, Neurology The Warren Alpert Medical School of Brown University March 28, 2015 Financial Disclosures None. Objectives
Strategies in Migraine Care Julie L. Roth, MD Rhode Island Hospital Assistant Professor, Neurology The Warren Alpert Medical School of Brown University March 28, 2015 Financial Disclosures None. Objectives
Understanding Migraine & other headaches
 Understanding Migraine & other headaches Dr Anne MacGregor Published by Family Doctor Publications Limited in association with the British Medical Association IMPORTANT NOTICE This book is intended not
Understanding Migraine & other headaches Dr Anne MacGregor Published by Family Doctor Publications Limited in association with the British Medical Association IMPORTANT NOTICE This book is intended not
