Hypovolemia in Shock Due to Acute Myocardial Infarction
|
|
|
- Shanna Anderson
- 5 years ago
- Views:
Transcription
1 Hypovolemia in Shock Due to Acute Myocardial Infarction By HENRY S. LOEB, M.D., RAYMOND J. PIETRAS, M.D., JoHN R. TOBIN, JR., M.D., AND ROLF M. GUNNAR, M.D. SUMMARY Twelve patients with the clinical features of shock following acute myocardial infarction were treated with low molecular weight dextran (LMWD) as a plasma volume expander. Two of the patients had elevated central venous pressures (CVP), and neither responded favorably to plasma volume expansion. The remaining 1 patients had CVPs under 7 mm Hg prior to dextran infusion; five survived. Each survivor responded favorably to dextran infusion manifested by an increase in arterial pressure and cardiac index. The average increase in CVP in these patients was 1. mm Hg per 1 ml of dextran infused. The other five patients died either without recovering from shock or in chronic cardiac failure. These patients failed to show a significant increase in arterial pressure or cardiac index after dextran infusion; CVP increased by an average of 1.9 mm Hg per 1 ml infused. Hypovolemia must be considered in all patients in whom clinical evidence of shock develops as a complication of acute myocardial infarction, and if the CVP is normal or low, plasma volume expansion should be undertaken with caution. Increase in arterial pressure and evidence of improved cardiac index with little rise in CVP indicate a good response to the infusion and excellent prognosis for survival. Downloaded from by on November 3, 218 Additional Indexing Words: Central venous pressure Pulmonary arterial pressure Cardiac index Dextran HYPOVOLEMIA is not considered to be a basic defect in shock associated with acute myocardial infarction and has seldom been recognized as an early complication. However, through routine monitoring of the CVP, we have been made aware of the frequency of this defect in patients in whom circulatory insufficiency or shock develops after acute myocardial infarction. Because hypovolemia is easily treated, some investiga- From the Department of Adult Cardiology and the Hektoen Institute for Medical Research of the Cook County Hospital; the Section of Cardiology, Department of Medicine, University of Illinois College of Medicine, Chicago, Illinois; and the Department of Medicine of the Loyola University Stritch School of Medicine, Hines, Illinois. Supported in part by Grant HE-8834, from the National Institutes of Health, U. S. Public Health Service. 653 tors have advocated plasma volume expansion of all patients in whom shock develops after myocardial infarction.' On the other hand, the potential hazards of such therapy in the presence of severe myocardial damage has caused us to attempt to establish some guidelines for using plasma volume expanders in these patients. We have conducted hemodynamic studies on 4 patients with circulatory insufficiency or shock complicating acute myocardial infarction. We report here the clinical and hemodynamic responses to low molecular weight dextran (LMWD) in 12 of these patients, 1 of whom had control CVPs of less than 7 mm Hg (1 cm H2). Methods Patients were selected for study because they presented the clinical features of shock (obtundation, weak pulses, cold extremities, and oliguria) following acute myocardial infarction. Mean
2 654 intra-arterial pressure (measured prior to vasopressor therapy) was less than 8 mm Hg in all but three patients. These three each had historical and clinical evidence of pre-existing hypertension. In addition, at the onset of clinical shock these three patients had blood pressures (obtained by the cuff method) that were significantly less than on admission. The diagnosis of acute myocardial infarction was verified by necropsy in three patients and by history, electrocardiogram, or serum enzyme changes in all. The decision to expand intravascular volume in 1 of the patients was based on the findings of a normal or low CVP (under 7 mm Hg). In two patients although the CVP was slightly elevated (1.5 and 12 mm Hg), volume expansion was attempted in the hope that a further increase in ventricular filling pressure might improve cardiac output. It should be emphasized that the majority of our patients with circulatory insufficiency or shock after acute myocardial infarction have had elevated control CVPs, and thus the question of plasma volume expansion has not arisen. Patients were studied at the bedside or in a specially equipped study unit. Arterial pressure (MAP) and CVP were measured with a transducer through catheters threaded into the central aorta and superior vena cava or right atrium after surgical exposure of the right brachial vessels. Cardiac output (CO) was measured by the indicator-dilution method by means of indocyanine green injected through the CVP catheter and sampling from the central aortic catheter. Values for CO were obtained by averaging two to five indicator-dilution curves and were corrected for body surface area (CI). We have found this method to be reproducible to + 5% when done in rapid succession on the same patient. Pressure pulses, dilution curves, and a standard electrocardiogram lead were recorded on a photographic recorder. Systemic vascular resistance (SVR) was calculated as follows: Immediately after control measurements LMWD was given in an amount averaging 58 ml (range 2 to 1,) at an average infusion rate of 7.6 ml per minute (range 4.4 to 12.). All measurements were repeated within a few minutes after completion of the LMWD infusion. Infusions of norepinephrine (in two patients) and isoproterenol (in one patient) were continued at a constant rate throughout the LMWD study period. One patient received 1 mg of morphine sulfate during the time LMWD was being given. SVR_ MAP-CVP. CO Results Two patients, one of whom was receiving LOEB ET AL. isoproterenol throughout the study period, had control CVPs over 7 mm Hg and did not respond to LMWD by significant increases in CI, urine flow, or evidence of clinical improvement. Although one patient had a modest rise in MAP (14 mm Hg) after LMWD, his ultimate recovery from shock was unrelated to plasma volume expansion, and he later died of refractory cardiac failure. The other patient failed to recover from shock. Both of these patients had massive myocardial infarction demonstrated at necropsy. The remaining 1 patients all had normal or low CVPs (less than 7 mm Hg) before infusion of LMWD and were divided into two groups on the basis of survival. Five of these patients (group A) showed marked clinical improvement and increased urine flow (average increase being 1.7 ml per minute) after receiving LMWD. These patients all survived their illness and were eventually discharged from the hospital. Four of the remaining five patients (group B) failed to show clinical improvement or significant increases in urine flow after receiving LMWD, and none of these five survived to be discharged from the hospital, although two recovered from shock only to die later of cardiac failure. Comparison is made between the two groups to determine if additional criteria could aid in the early selection of those patients in shock after acute myocardial infarction who can be expected to benefit from plasma volume expansion. Certain clinical differences between the two groups were apparent. The average age of group A patients was 48 (range 42 to 52) years, whereas group B patients averaged 69 (range 5 to 85) years. None of the group A patients were known to have had previous myocardial infarction, whereas two patients in group B had histories and electrocardiographic evidence of previous infarction. Inferior wall infarction was present in three of the five group A patients, and anterior infarction occurred in four of the five group B patients. The degree of serum enzyme elevation did not, however, differ between the groups. Although a probable cause for hypovolemia
3 HYPOVOLEMIA IN SHOCK Hemodynamic Status in Graups A and B Table Patient Group A A.F. M.G. H.S. B.M. E.G. Mean ± SD Group B-V.B. A.P. K.W. (NE) A.W. (NE) J.A. Mean ± SD LMWD Infusion volume rate Age (ml) (ml/min) i ± 2.6 MAP 13* 85t 6 89t i ± 1 Control CVP ± 2.6 After LMWD CI (L/min/m2) MAP CVP i ± 15 (NE) Received norepinephrine at constant infusion rate throughout study period. * Admission blood pressure 19/14 (cuff) fell to 1/7 (cuff) before study. t Admission blood pressure 11/8 (cuff) fell to 85/6 (cuff) before study. I Admission blood pressure 15/11 (cuff) fell to 4 systolic by palpation before study ± 3.8 CL (L/min/m2) ± ± 1.1 Downloaded from by on November 3, 218 could be found in all group A patients, in only one group B patient was it possible to establish a possible reason for hypovolemia. Group A also differed from group B in terms of hemodynamic status both before and after LMWD infusion (table 1). Before LMWD infusion hypotension was less marked in group A than in group B patients; after infusion, each group A patient showed an increase in MAP averaging 18±1 mm Hg (mean + SD), whereas only one group B patient responded to LMWD with a significant increase in MAP; the average change for group B was a fall of mm Hg. CVP increased in all patients during infusion of LMWD; however, when changes in CVP were related to the amount of LMWVD infused, group A patients increased their CVP by a mean of 1..4 mm Hg per 1 ml of LMWD infused, significantly less than the mm Hg per 1 ml for patients in group B (P<.2). Values for heart rate prior to LMWD were not significantly different between the groups and tended to be slightly lower after infusion of LMWD in most patients in both groups. Prior to LMWD, CI averaged L/min/m2 for group A and L/min/ m2 for group B. After LMWD infusion every group A patient had increased CI by at least.7 L/min/m2, with an average increase of L/min/m2. Only two patients in group B showed significant increases in CI after LMWD, and the average increase for all five patients was.1.8 L/min/m2. Left ventricular pressure was measured before infusion of LMWD in two patients, one in each group, by passing a catheter retrograde across the aortic valve. These patients are presented in some detail. Case 1 A.F., a 42-year-old Negro man with a past history of hypertension and anginal pain was admitted after 4 days of increasingly severe
4 656 anterior chest pain unrelieved by rest. On admission the patient complained of severe chest pain and required morphine. Blood pressure was 19/14, and the pulse was 8 and regular. Cardiac enlargement and a presystolic gallop were present. There was no evidence of congestive failure. The electrocardiogram showed changes typical of an acute inferior wall infarction, and serial enzymes were confirmatory. The patient was given reserpine, and his blood pressure decreased to 12/8. He continued to complain of severe chest pain and 2 days after admission atrial fibrillation with a rapid ventricular response occurred. Electrocardiographic changes suggested extension of the original infarct with involvement of the posterior basal left ventricle. Although there was no evidence of cardiac failure, digoxin was given to control the rapid ventricular rate. The patient began to complain of nausea and vomiting, which persisted. Four days after admission blood pressure by cuff was found to be 1/7 mm Hg. The pulse was weak, and the extremities were cold and clammy. Urine flow was 3 ml per hour. Hemodynamic measurements revealed a CVP of 1.5 mm Hg and a left ventricular end-diastolic pressure (LVEDP) of 4.5 mm Hg. MAP was 13 mm Hg but the pulse pressure was only 32 mm Hg. CI was 1.9 L/min/m2. The patient was given ml of LMWD, and the CVP increased by only 3 mm Hg. During this infusion MAP rose to 12 mm Hg, pulse pressure increased to 48 mm Hg, and CI to 2.6 L/min/m2. Urine flow increased to 17 ml per hour, and upon returning to the ward blood pressure by the cuff method was 14/9 mm Hg. A few days later sinus rhythm returned spontaneously. Recovery was uneventful, and upon discharge the patient was asymptomatic and did not require digitalis. Comment. In this patient circulatory insufficiency was clearly related to hypovolemia due to inadequate fluid intake, diaphoresis, and vomiting. However, until the CVP was measured, hypovolemia was unrecognized. The normal LVEDP, his rapid improvement when given volume, and his subsequent course all attest to the fact that myocardial failure following acute myocardial infarction was not the cause of the circulatory insufficiency. Case 2 A.P., a 5-year-old Negro man, was admitted for severe substernal pain. The patient had been hospitalized 3 months previously for acute myocardial infarction. For 5 years prior to this he had been treated for hypertension. He had been asymptomatic for 2 months, and this was interrupted by the onset of chest pain 2 days before admission. On admission, the patient was alert and complained of chest pain. Blood LOEB ET AL. pressure was 9/6 mm Hg, pulse 13 per minute, and temperature 11.6 F. The lungs were clear. Cardiac enlargement and a "summation" gallop were present. An electrocardiogram showed evidence of an old anterolateral and recent inferior myocardial infarction. Hemodynamic studies were initiated shortly after admission. After the catheters had been inserted, the patient developed rigors and a further elevation of temperature to 16 F. The catheters were changed, and when the rigors had subsided, measurements were made. CVP, which had been 7 mm Hg, fell to 1.5 mm Hg; however, LVEDP remained elevated at 24 mm Hg. MAP was 63 mm Hg and CI was 3.9 L/min/m2. When 7 ml of LMWD had been infused, the CVP had increased to 1.5 mm Hg, MAP had fallen to 56 mm Hg, and CI had fallen to 2.6 L/min/m2. The temperature had fallen to 11.8 F. The patient was rapidly digitalized, and this resulted in a rise in MAP and CI, while CVP and HR fell. The patient's condition stabilized; however, during the remainder of his hospital course he complained of severe dyspnea and orthopnea, which remained refractory to vigorous medical therapy until he died in cardiac failure 2 weeks after admission. Comment. The patient had severe cardiac damage from at least two myocardial infarctions. Although CVP was low after an apparent pyrogen reaction, LVEDP was markedly elevated. Plasma volume expansion was accompanied by an elevation in CVP but MAP and CI fell, indicating that hypovolemia was not responsible for the patient's circulatory insufficiency. Digitalization, which had been withheld at first because of the low CVP, clearly resulted in hemodynamic improvement. Discussion Although hypovolemia is not present in the majority of patients with acute myocardial infarction, it should be searched for in all patients in whom shock or circulatory insufficiency -develops. From our data, measurement of the CVP and, when nornal or low, CVP monitoring during a careful therapeutic trial of plasma volume expansion are safe and practical methods for identifying those patients able to respond to volume expansion. When the CVP is elevated above normal (above 7 mm Hg), volume administration alone is unlikely to result in significant hemodynamic improvement. These patients usually have severe myocardial damage and fail to increase cardiac output when given
5 HYPOVOLEMIA IN SHOCK intravenous infusions. If plasma volume expansion is to be attempted in such patients, it must be done with extreme caution. When the CVP is not elevated and yet the patient shows evidence of circulatory insufficiency or shock following acute myocardial infarction, hypovolemia must be suspected. Under these circumstances, a therapeutic trial of plasma volume expansion is indicated. A favorable response to fluid administration can be recognized by an increase in arterial pressure, pulse volume, and urine flow accompanied by clinical improvement. The CVP will remain low or increase minimally. The patients in group A (responding well to volume expansion) showed a mean rise in CVP of only 1. mm Hg per 1 ml of LMWD administered, and the highest was only 1.5 mm Hg per 1 ml infused. This response is most likely to be seen in younger patients with minimal myocardial damage and indicates an excellent prognosis. When, however, fluid administration results in a rapid increase in the CVP and shock or circulatory insufficiency persists, severe myocardial damage is probably present. The patients in group B (poor response to volume expansion) had a mean rise in the CVP of 1.9 mm Hg per 1 ml of LMWD infused, and the least rise was 1.3 mm Hg per 1 ml. These patients were elderly, had lower initial blood pressures than group A patients, and had clinical or postmortem evidence, or both, of severe myocardial damage. Although we did not measure total blood volume in our patients, others have found normal or slightly reduced blood volumes in patients with shock after acute myocardial infarction.2-4 It is likely that the hemodynamic alterations present in the shock patient prohibit the use of standard normal values for blood volume in determining the need for fluid administration.5' 6 We have used the CVP and its response to plasma volume expansion as a guide to fluid therapy. This type of therapeutic trial and monitoring has been proved to be of great value in other types of shock.a9 It should be stressed that in addition to intravascular 657 volume, the CVP is influenced by changes in venous tone and by changes in the compliance of the right ventricle. Under conditions of increased venous tone or decreased right ventricular compliance, or both, the CVP might be normal in spite of an inadequate intravascular volume.3 Since myocardial infarction usually involves the left ventricle, and since a sudden rise in LVEDP during fluid administration can precipitate acute pulmonary edema, it is important to determine the relation between the CVP and LVEDP. Increases in CVP have been shown to reflect increases in LVEDP during experimental volume overload.1 Cohn, and associates" have made simultaneous measurements of the CVP and LVEDP in nine patients with acute myocardial infarction and shock, and in none did LVEDP rise without a concomitant rise in CVP. We have made a similar observation in 23 patients with various types of shock in whom we have measured CVP and LVEDP during plasma volume expansion.12 Although in the two patients presented here LVEDP was not measured following LMWD, the rapid rise in the CVP in the patient whose initial LVEDP was elevated supports the contention that, even in acute myocardial infarction, monitoring the CVP is a safe guide for a trial of plasma volume expansion. It is possible to precipitate pulmonary edema in the presence of a normal CVP in patients with acute myocardial infarction by adding small amounts of fluid, and, therefore, measurement of LVEDP is the ideal method for monitoring this form of therapy. However, the CVP measurement can easily be made and, if used as a dynamic measurement, can reflect directional changes in LVEDP if addition of volume is the only therapeutic change being made.12 The catheter can also be used to withdraw fluid, should pulmonary edema develop. A normal SVR in spite of a reduced CI has been frequently observed in patients with shock due to acute myocardial infarction The mechanism for this absence of compensatory vasoconstriction is unclear; however, a
6 658 similar mechanism might cause a decrease in venous tone and low CVP in patients having normal or elevated blood volumes. Although our patients in groups A and B had similar values for SVR, it is possible that reduced venous tone was partly responsible for normal or low CVPs in some of our group B patients. Group A patients, however, responded well to fluid therapy, and we postulate that hypovolemia was the major cause for their low CVPs and circulatory insufficiency. The incidence of hypovolemia complicating acute myocardial infarction is probably low, and the routine administration of significant volume loads to all patients with shock does not seem justified. The use of vasodilator agents coupled with plasma volume loading has been advocated;'5 however, this form of therapy has yet to be evaluated clinically and should be reserved for those patients who although manifesting clinical signs of shock, are able to maintain adequate intra-arterial pressures in spite of vasodilator therapy. Langsjoen and associates'6 have reported a reduced mortality in patients with acute myocardial infarction treated with low molecular weight dextran. Therapy in these patients was designed to reduce intravascular sludging rather than to expand intravascular volume, and the rate of administration was significantly less than in our patients. They have postulated correction of undetected hypovolemia as contributing to improved survival in these patients. Since we did not compare our infusions with equal amounts of dextrose or saline solution infusions, it is impossible for us to know whether the dextran solution had any effect in addition to its contribution to plasma volume. Allen and others'7 reported hypovolemia to be present in 2% of patients with cardiogenic shock. Although this figure corresponds closely to our own experience, it has undoubtedly been inflated by exclusion of patients presenting with profound shock due to rapidly progressing pump failure, since such patients frequently do not survive long enough for hemodynamic measurements to be obtained. LOEB ET AL. There are many mechanisms by which hypovolemia can develop after acute myocardial infarction: 1. Inadequate fluid intake is common, and parenteral fluid administration is frequently kept at a minimum for fear of precipitating cardiac failure. 2. Excessive loss of fluids may occur because of fever and diaphoresis, the use of potent diuretics for pulmonary edema, and as a result of nausea and vomiting secondary to pain or drugs. 3. A shift of fluid from the intravascular to the extravascular compartments, or trapping of red cell aggregates in various capillary beds may result in a reduced effective circulating blood volume. This is most likely to occur in patients who remain vasoconstricted for prolonged periods, either from compensatory mechanisms or from the use of various pressor agents.'8 Also, acute acidosis following temporary circulatory arrest may result in sudden marked loss of intravascular volume. 4. In addition to the primary illness, associated illnesses such as sepsis or gastrointestinal bleeding may cause hypovolemia in patients with acute myocardial infarction and, if unrecognized, may lead to a decrease in coronary flow and extension of the myocardial damage. References 1. NIXON, P. G. F., IKROM, H., AND MORTON, S.: Cardiogenic shock treated with infusion of dextrose solution. Amer Heart J 73: 843, SMITH, W. W., WICKLER, N. S., AND Fox, A. C.: Hemodynamic studies of patients with myocardial infarction. Circulation 9: 352, FREWs, E. D., ScHNAPER, H. W., JOHNSON, R. L., AND ScHREINNm, G. E.: Hemodynamic alterations in acute myocardial infarction: I. Cardiac output, mean arterial pressure, total peripheral resistance, "central" and total blood volumes, venous pressure and average circulation time. J Clin Invest 31: 131, SHUBIN, H., BRADLEY, E. C., AND WEIL, M.: Hemodynamic and metabolic observations during the course of shock complicating myocardial infarction. (Abstr.) Circulation 36 (suppl. II): , THAL, A. P., AND KINNEY, J. M.: On the
7 HYPOVOLEMIA IN SHOCK definition and classification of shock. Progr Cardiovasc Dis 9: 527, WEIL, M. H., SHUBIN, H., A"N ROSOFF, L.: Fluid repletion in circulatory shock: Central venous pressure and other practical guides. JAMA 192: 668, JACOBSON, E. D.: A physiologic approach to shock. New Eng J Med 278: 834, WiLsON, J. N.: Rational approach to the management of clinical shock. Arch Surg 91: 92, LOEB, H. S., ET AL.: Haemodynamic studies in shock associated with infection. Brit Heart J 29: 883, HANASHIRO, P. K., Arm WEnu, M. H.: Relationship of intracardiac pressures after volume overload. (Abstr.) Clin Res 16: 18, COHN, J. N., KiAERI, I. M., AND TRISTANI, F. E.: Left and right ventricular filling pressures in clinical shock. (Abstr.) Ann Intern Med 68: 1153, LoEB, H. S., GUNNAR, R. M., PIrARAs, R. J., AND TOBIN, J. R., JR.: Relationships between central venous and left ventricular filling pressures prior to and during treatment of shock. (Abstr.) Amer J Cardiol 23: 125, KuHN, L. A.: Changing treatment of shock following acute myocardial infarction: A clinical evaluation. Amer J Cardiol 2: 757, GUNNAR, R. M., PiETRAs, R. J., STAVRAKOS, C., Loim, H. S., AND TOBIN, J. R., JR.: The physiologic basis for treatment of shock associated with myocardial infarction. Med Clin N Amer 51: 69, BLOCH, J. H., PIERCE, C. H., MANAX, W. G., AND LILLEYHEI, R. C.: Treatment of experimental cardiogenic shock. Surgery 58: 197, LANGSJOEN, P. H., FALCONER, H. S., SANCHEZ, S. A., AND LYNCH, D. J.: Observations in treatment of acute myocardial infarction with low molecular dextran. Angiology 14: 465, ALLEN, H. N., DANZIG, R., AND SWAN, H. J. C.: Incidence and significance of relative hypovolemia as a cause of shock associated with acute myocardial infarction. (Abstr.) Circulation 36: (suppl.) II): II-5, BoTTICELLI, J. T., TSAGARIS, T. J., AND LANGE, R. L.: Mechanisms of pressor amine dependence. Amer J Cardiol 16: 847, Downloaded from by on November 3, 218
FAILURE IN PATIENTS WITH MYOCARDIAL INFARCTION
 Br. J. clin. Pharmac. (1982), 14, 187S-19lS BENEFICIAL EFFECTS OF CAPTOPRIL IN LEFT VENTRICULAR FAILURE IN PATIENTS WITH MYOCARDIAL INFARCTION J.P. BOUNHOURE, J.G. KAYANAKIS, J.M. FAUVEL & J. PUEL Departments
Br. J. clin. Pharmac. (1982), 14, 187S-19lS BENEFICIAL EFFECTS OF CAPTOPRIL IN LEFT VENTRICULAR FAILURE IN PATIENTS WITH MYOCARDIAL INFARCTION J.P. BOUNHOURE, J.G. KAYANAKIS, J.M. FAUVEL & J. PUEL Departments
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Admission of patient CVICU and hemodynamic monitoring
 Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Department of Intensive Care Medicine UNDERSTANDING CIRCULATORY FAILURE IN SEPSIS
 Department of Intensive Care Medicine UNDERSTANDING CIRCULATORY FAILURE IN SEPSIS UNDERSTANDING CIRCULATORY FAILURE IN SEPSIS a mismatch between tissue perfusion and metabolic demands the heart, the vasculature
Department of Intensive Care Medicine UNDERSTANDING CIRCULATORY FAILURE IN SEPSIS UNDERSTANDING CIRCULATORY FAILURE IN SEPSIS a mismatch between tissue perfusion and metabolic demands the heart, the vasculature
Relax and Learn At the Farm 2012
 Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Complications of Acute Myocardial Infarction
 Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
Cardiac Emergencies. Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington
 Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
Hemodynamic Monitoring and Circulatory Assist Devices
 Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Topics to be Covered. Cardiac Measurements. Distribution of Blood Volume. Distribution of Pulmonary Ventilation & Blood Flow
 Topics to be Covered MODULE F HEMODYNAMIC MONITORING Cardiac Output Determinants of Stroke Volume Hemodynamic Measurements Pulmonary Artery Catheterization Control of Blood Pressure Heart Failure Cardiac
Topics to be Covered MODULE F HEMODYNAMIC MONITORING Cardiac Output Determinants of Stroke Volume Hemodynamic Measurements Pulmonary Artery Catheterization Control of Blood Pressure Heart Failure Cardiac
DESIGNER RESUSCITATION: TITRATING TO TISSUE NEEDS
 DESIGNER RESUSCITATION: TITRATING TO TISSUE NEEDS R. Phillip Dellinger MD, MSc, MCCM Professor and Chair of Medicine Cooper Medical School of Rowan University Chief of Medicine Cooper University Hospital
DESIGNER RESUSCITATION: TITRATING TO TISSUE NEEDS R. Phillip Dellinger MD, MSc, MCCM Professor and Chair of Medicine Cooper Medical School of Rowan University Chief of Medicine Cooper University Hospital
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
CATCH A WAVE.. INTRODUCTION NONINVASIVE HEMODYNAMIC MONITORING 4/12/2018
 WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
Cardiac Emergencies. A Review of Cardiac Compromise. Lawrence L. Lambert
 Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
What would be the response of the sympathetic system to this patient s decrease in arterial pressure?
 CASE 51 A 62-year-old man undergoes surgery to correct a herniated disc in his spine. The patient is thought to have an uncomplicated surgery until he complains of extreme abdominal distention and pain
CASE 51 A 62-year-old man undergoes surgery to correct a herniated disc in his spine. The patient is thought to have an uncomplicated surgery until he complains of extreme abdominal distention and pain
SHOCK. Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital
 SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
Impedance Cardiography (ICG) Method, Technology and Validity
 Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Central haemodynamics during spontaneous angina pectoris
 British Heart Journal, I974, 36, I0-I09I Central haemodynamics during spontaneous angina pectoris From the Department of Clinical Physiology, Malmo General Hospital, S-214 OI Malmo, Sweden. Central pressures
British Heart Journal, I974, 36, I0-I09I Central haemodynamics during spontaneous angina pectoris From the Department of Clinical Physiology, Malmo General Hospital, S-214 OI Malmo, Sweden. Central pressures
Titrating Critical Care Medications
 Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
constriction of the peripheral veins. The level of
 Journal of Clinical Investigation Vol. 41, No. 11, 1962 THE MECHANISM OF THE INCREASED VENOUS PRESSURE WITH EXERCISE IN CONGESTIVE HEART FAILURE * t By J. EDWIN WOOD (From the Department of Medicine and
Journal of Clinical Investigation Vol. 41, No. 11, 1962 THE MECHANISM OF THE INCREASED VENOUS PRESSURE WITH EXERCISE IN CONGESTIVE HEART FAILURE * t By J. EDWIN WOOD (From the Department of Medicine and
Medical Management of Acute Heart Failure
 Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Case year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50
 Case 1 65 year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50 Case 1 65 year old female nursing home resident with
Case 1 65 year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50 Case 1 65 year old female nursing home resident with
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United
 Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Shock Quiz! By Clare Di Bona
 Shock Quiz! By Clare Di Bona Test Question What is Mr Burns full legal name? Answer Charles Montgomery Plantagenet Schicklgruber Burns. (Season 22, episode 11) Question 1. What is the definition of shock?
Shock Quiz! By Clare Di Bona Test Question What is Mr Burns full legal name? Answer Charles Montgomery Plantagenet Schicklgruber Burns. (Season 22, episode 11) Question 1. What is the definition of shock?
Differentiation of Ventricular Tachycardia from Junctional Tachycardia with Aberrant Conduction
 Differentiation of Ventricular Tachycardia from Junctional Tachycardia with Aberrant Conduction The Use of Competitive Atrial Pacing By ROBERT M. EASLEY, JR., M.D., AND SIDNEY GOLDSTEIN, M.D. SUMMARY A
Differentiation of Ventricular Tachycardia from Junctional Tachycardia with Aberrant Conduction The Use of Competitive Atrial Pacing By ROBERT M. EASLEY, JR., M.D., AND SIDNEY GOLDSTEIN, M.D. SUMMARY A
Cardiovascular Management of Septic Shock
 Cardiovascular Management of Septic Shock R. Phillip Dellinger, MD Professor of Medicine Robert Wood Johnson Medical School/UMDNJ Director, Critical Care Medicine and Med/Surg ICU Cooper University Hospital
Cardiovascular Management of Septic Shock R. Phillip Dellinger, MD Professor of Medicine Robert Wood Johnson Medical School/UMDNJ Director, Critical Care Medicine and Med/Surg ICU Cooper University Hospital
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Management of acute decompensated heart failure and cardiogenic shock. Arintaya Phrommintikul Department of Medicine CMU
 Management of acute decompensated heart failure and cardiogenic shock Arintaya Phrommintikul Department of Medicine CMU Acute heart failure: spectrum Case 64 y/o M with Hx of non-ischemic DCM (LVEF=25-30%)
Management of acute decompensated heart failure and cardiogenic shock Arintaya Phrommintikul Department of Medicine CMU Acute heart failure: spectrum Case 64 y/o M with Hx of non-ischemic DCM (LVEF=25-30%)
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
HISTORY. Question: How do you interpret the patient s history? CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: 45-year-old man.
 HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
2.02 Understand the functions and disorders of the circulatory system
 2.02 Understand the functions and disorders of the circulatory system 2.02 Understand the functions and disorders of the circulatory system Essential questions: What are the functions of blood? What are
2.02 Understand the functions and disorders of the circulatory system 2.02 Understand the functions and disorders of the circulatory system Essential questions: What are the functions of blood? What are
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency
 Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT.
 HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
Can be felt where an artery passes near the skin surface and over a
 1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since.
 1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO)
 Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO) Michael A. Gibson, MD Assistant Professor of Medicine University of California, Irvine Division of Cardiology
Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO) Michael A. Gibson, MD Assistant Professor of Medicine University of California, Irvine Division of Cardiology
Cardiovascular Physiology
 Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Diazoxide in the Treatment CLARENCE L. GANTT, M.D. which suggest that diazoxide may be the. drug of choice in the treatment of all forms
 Intravenous Use o;f Diazoxide in the Treatment of Severe Hypertension By WILLIAM M. HAMBY, M.D., GERALD J. JANKOWSKI, M.D., J. MAURICE POUGET, M.D., GEORGE DUNEA, M.D., AND CLARENCE L. GANTT, M.D. SUMMARY
Intravenous Use o;f Diazoxide in the Treatment of Severe Hypertension By WILLIAM M. HAMBY, M.D., GERALD J. JANKOWSKI, M.D., J. MAURICE POUGET, M.D., GEORGE DUNEA, M.D., AND CLARENCE L. GANTT, M.D. SUMMARY
Cardiac Output MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
Fluid Resuscitation in Critically Ill Patients with Acute Kidney Injury (AKI)
 Fluid Resuscitation in Critically Ill Patients with Acute Kidney Injury (AKI) Robert W. Schrier, MD University of Colorado School of Medicine Denver, Colorado USA Prevalence of acute renal failure in Intensive
Fluid Resuscitation in Critically Ill Patients with Acute Kidney Injury (AKI) Robert W. Schrier, MD University of Colorado School of Medicine Denver, Colorado USA Prevalence of acute renal failure in Intensive
Effects of Propranolol on Patients with Complete Heart Block and Implanted Pacemakers
 Effects of Propranolol on Patients with Complete Heart Block and Implanted Pacemakers By EPHRAIM DONOSO, M.D., LAWRENCE J. COHN, M.D., BERTRAM J. NEWMAN, M.D., HENRY S. BLOOM, M.D., WILLIAm C. STFIN, M.D.,
Effects of Propranolol on Patients with Complete Heart Block and Implanted Pacemakers By EPHRAIM DONOSO, M.D., LAWRENCE J. COHN, M.D., BERTRAM J. NEWMAN, M.D., HENRY S. BLOOM, M.D., WILLIAm C. STFIN, M.D.,
TRANSIENT LEFT BUNDLE BRANCH BLOCK -
 Vol. 11, No. 2. June, 1970. SINGAPORE MEDICAL JOURNAL TRANSIENT LEFT BUNDLE BRANCH BLOCK - A CASE REPORT 86 By L.S. Chew (Medical Unit III, General Hospital, Singapore) INTRODUCTION It is generally believed
Vol. 11, No. 2. June, 1970. SINGAPORE MEDICAL JOURNAL TRANSIENT LEFT BUNDLE BRANCH BLOCK - A CASE REPORT 86 By L.S. Chew (Medical Unit III, General Hospital, Singapore) INTRODUCTION It is generally believed
Cardiovascular System
 Cardiovascular System angio BELLWORK Day One: Define using technology hemo/hema cardio Medical Therapeutics Standards 11) Outline the gross normal structure and function of all body systems and summarize
Cardiovascular System angio BELLWORK Day One: Define using technology hemo/hema cardio Medical Therapeutics Standards 11) Outline the gross normal structure and function of all body systems and summarize
Hemodynamic improvement upon levosimendan treatment in low cardiac output patients following coronary artery bypass graft
 Hemodynamic improvement upon levosimendan treatment in low cardiac output patients following coronary artery bypass graft M. Buerke, K. Krohe, M. Russ, C. Schneider, H. Lemm, R. Prondzinsky, I. Friedrich,
Hemodynamic improvement upon levosimendan treatment in low cardiac output patients following coronary artery bypass graft M. Buerke, K. Krohe, M. Russ, C. Schneider, H. Lemm, R. Prondzinsky, I. Friedrich,
Cardiogenic Shock. Carlos Cafri,, MD
 Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
Heart Disorders. Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8. Overview Heart Disorders Vascular Disorders
 Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8 Overview Heart Disorders Vascular Disorders Susie Turner, MD 1/7/13 Heart Disorders Coronary Artery Disease Cardiac Arrhythmias Congestive Heart
Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8 Overview Heart Disorders Vascular Disorders Susie Turner, MD 1/7/13 Heart Disorders Coronary Artery Disease Cardiac Arrhythmias Congestive Heart
Bedside assessment of fluid status
 Bedside assessment of fluid status 2nd AKI Academy October 18 th 2014 David Treacher Guy s & St Thomas NHS Trust Assessing the circulation - the 3 key questions v Is my patient adequately filled? v What
Bedside assessment of fluid status 2nd AKI Academy October 18 th 2014 David Treacher Guy s & St Thomas NHS Trust Assessing the circulation - the 3 key questions v Is my patient adequately filled? v What
Results of Ischemic Heart Disease
 Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
The right heart: the Cinderella of heart failure
 The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
Technique. Technique. Technique. Monitoring 1. Local anesthetic? Aseptic technique Hyper-extend (if radial)
 Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE
 DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
ANCE ON THE LEFT ATRIAL PRESSURE PULSE: A
 THE EFFECTS OF ACUTELY INCREASED SYSTEMIC RESIST- ANCE ON THE LEFT ATRIAL PRESSURE PULSE: A METHOD FOR THE CLINICAL DETECTION OF MITRAL INSUFFICIENCY By EUGENE BRAUNWALD, G. H. WELCH, JR., AND ANDREW G.
THE EFFECTS OF ACUTELY INCREASED SYSTEMIC RESIST- ANCE ON THE LEFT ATRIAL PRESSURE PULSE: A METHOD FOR THE CLINICAL DETECTION OF MITRAL INSUFFICIENCY By EUGENE BRAUNWALD, G. H. WELCH, JR., AND ANDREW G.
Medical Treatment for acute Decompensated Heart Failure. Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011
 Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
University of Wisconsin - Madison Cardiovascular Medicine Fellowship Program UW CICU Rotation Goals and Objectives
 Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Ostium primum defects with cleft mitral valve
 Thorax (1965), 20, 405. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Ostium primum defects are common; by 1955, 37 operated cases had been reported by
Thorax (1965), 20, 405. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Ostium primum defects are common; by 1955, 37 operated cases had been reported by
Cardiovascular Disorders. Heart Disorders. Diagnostic Tests for CV Function. Bio 375. Pathophysiology
 Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend )
 Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend ) Stephen G. Ellis, MD Section Head, Interventional Cardiology Professor of Medicine Cleveland
Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend ) Stephen G. Ellis, MD Section Head, Interventional Cardiology Professor of Medicine Cleveland
Haemodynamic effects of isoprenaline in acute myocardial infarction
 British Heart journal, I972, 34, 75-7I. Haemodynamic effects of isoprenaline in acute myocardial infarction Jonas Beregovich, Henrietta Reicher-Reiss, and Arthur Grishman From the Division of Cardiology,
British Heart journal, I972, 34, 75-7I. Haemodynamic effects of isoprenaline in acute myocardial infarction Jonas Beregovich, Henrietta Reicher-Reiss, and Arthur Grishman From the Division of Cardiology,
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
BUSINESS. Articles? Grades Midterm Review session
 BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
4. The two inferior chambers of the heart are known as the atria. the superior and inferior vena cava, which empty into the left atrium.
 Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
BOTH ATEOPINE and isoproterenol
 Effects of tropine and Isoproterenol on Cardiac Output, Central Venous Pressure, and Transit Time of Indicators Placed at Three Different Sites in the Venous System y KLPH RTEX, M.D., J. CULIE GUNXELLS,
Effects of tropine and Isoproterenol on Cardiac Output, Central Venous Pressure, and Transit Time of Indicators Placed at Three Different Sites in the Venous System y KLPH RTEX, M.D., J. CULIE GUNXELLS,
The Mammalian Circulatory System
 The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
Myocardial Infarction: Left Ventricular Failure
 CARDIOVASCULAR PHYSIOLOGY 93 Case 17 Myocardial Infarction: Left Ventricular Failure Marvin Zimmerman is a 52-year-old construction manager who is significantly overweight. Despite his physician's repeated
CARDIOVASCULAR PHYSIOLOGY 93 Case 17 Myocardial Infarction: Left Ventricular Failure Marvin Zimmerman is a 52-year-old construction manager who is significantly overweight. Despite his physician's repeated
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Means failure of heart to pump enough blood to satisfy the need of the body.
 Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
Intensive care of the patient with acute myocardial infarction
 Postgrad. med. J. (April 1967) 43, 207-211. Intensive care of the patient with acute myocardial infarction M. W. McNIcoL Central Middlesex Hospital, London, N. W.1 ACUTE myocardial infarction has an unknown
Postgrad. med. J. (April 1967) 43, 207-211. Intensive care of the patient with acute myocardial infarction M. W. McNIcoL Central Middlesex Hospital, London, N. W.1 ACUTE myocardial infarction has an unknown
Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900.
 1 2 3 4 5 6 Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900. Accounts for of every 3 deaths Cardiovascular disease
1 2 3 4 5 6 Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900. Accounts for of every 3 deaths Cardiovascular disease
Management of Advanced Systolic Heart Failure. Robert W. Hull MD FACC Associate Professor of Medicine West Virginia University
 Management of Advanced Systolic Heart Failure Robert W. Hull MD FACC Associate Professor of Medicine West Virginia University American College of Cardiology Foundation (ACCF) American Heart Association
Management of Advanced Systolic Heart Failure Robert W. Hull MD FACC Associate Professor of Medicine West Virginia University American College of Cardiology Foundation (ACCF) American Heart Association
Evaluation of pacing for heart block
 British Heart Journal, I97I, 33, 120-I24. Evaluation of pacing for heart block in myocardial infarction C. C. Watson and M. J. Goldberg From Leicester Regional Cardiothoracic Unit, Groby Road Hospital,
British Heart Journal, I97I, 33, 120-I24. Evaluation of pacing for heart block in myocardial infarction C. C. Watson and M. J. Goldberg From Leicester Regional Cardiothoracic Unit, Groby Road Hospital,
PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker
 PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg
 Rotation: or: Faculty: Coronary Care Unit (CVICU) Dr. Jeff Rottman Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg Duty Hours: Mon Fri, 7 AM to 7 PM, weekend call shared with consult
Rotation: or: Faculty: Coronary Care Unit (CVICU) Dr. Jeff Rottman Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg Duty Hours: Mon Fri, 7 AM to 7 PM, weekend call shared with consult
Role of right ventricular infarction in cardiogenic shock
 British Heart Journal, 1979, 42, 719-725 Role of right ventricular infarction in cardiogenic shock associated with inferior myocardial infarction1 HENRY GEWIRTZ,2 HERMAN K. GOLD, JOHN T. FALLON, RICHARD
British Heart Journal, 1979, 42, 719-725 Role of right ventricular infarction in cardiogenic shock associated with inferior myocardial infarction1 HENRY GEWIRTZ,2 HERMAN K. GOLD, JOHN T. FALLON, RICHARD
Copyright 2011, 2007 by Mosby, Inc., an affiliate of Elsevier Inc. Normal Cardiac Anatomy
 Mosby,, an affiliate of Elsevier Normal Cardiac Anatomy Impaired cardiac pumping Results in vasoconstriction & fluid retention Characterized by ventricular dysfunction, reduced exercise tolerance, diminished
Mosby,, an affiliate of Elsevier Normal Cardiac Anatomy Impaired cardiac pumping Results in vasoconstriction & fluid retention Characterized by ventricular dysfunction, reduced exercise tolerance, diminished
Review of Cardiac Mechanics & Pharmacology 10/23/2016. Brent Dunworth, CRNA, MSN, MBA 1. Learning Objectives
 Brent Dunworth, CRNA, MSN, MBA Associate Director of Advanced Practice Division Chief, Nurse Anesthesia Vanderbilt University Medical Center Nashville, Tennessee Learning Objectives Review the principles
Brent Dunworth, CRNA, MSN, MBA Associate Director of Advanced Practice Division Chief, Nurse Anesthesia Vanderbilt University Medical Center Nashville, Tennessee Learning Objectives Review the principles
IV Fluids. I.V. Fluid Osmolarity Composition 0.9% NaCL (Normal Saline Solution, NSS) Uses/Clinical Considerations
 IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
LV Distension and ECLS Lungs
 LV Distension and ECLS Lungs Kevin W. Hatton, MD, FCCM Interim Vice-Chair for Anesthesiology Research Division Chief, Anesthesiology Critical Care Medicine Program Director, Anesthesiology Critical Care
LV Distension and ECLS Lungs Kevin W. Hatton, MD, FCCM Interim Vice-Chair for Anesthesiology Research Division Chief, Anesthesiology Critical Care Medicine Program Director, Anesthesiology Critical Care
Index of subjects. effect on ventricular tachycardia 30 treatment with 101, 116 boosterpump 80 Brockenbrough phenomenon 55, 125
 145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12
 A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12 MONDAY TUESDAY WEDNESDAY THURSDAY FRIDAY 3/20 - B 3/21 - A 3/22 - B 3/23 - A 3/24 - B 3/27 - A Dissection Ethics Debate 3/28 - B 3/29 - A Intro to Cardiovascular
A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12 MONDAY TUESDAY WEDNESDAY THURSDAY FRIDAY 3/20 - B 3/21 - A 3/22 - B 3/23 - A 3/24 - B 3/27 - A Dissection Ethics Debate 3/28 - B 3/29 - A Intro to Cardiovascular
Cardiogenic Shock Protocol
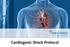 Cardiogenic Shock Protocol Impella Devices Best Practices in AMI Cardiogenic Shock Identify 1-3 SBP < 90 mmhg or on inotropes /pressors Cold, clammy, tachycardia Lactate elevated > 2 mmoi /L Stabilize
Cardiogenic Shock Protocol Impella Devices Best Practices in AMI Cardiogenic Shock Identify 1-3 SBP < 90 mmhg or on inotropes /pressors Cold, clammy, tachycardia Lactate elevated > 2 mmoi /L Stabilize
Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year
![Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year](/thumbs/76/74263761.jpg) PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
HYPOVOLEMIA AND HEMORRHAGE UPDATE ON VOLUME RESUSCITATION HEMORRHAGE AND HYPOVOLEMIA DISTRIBUTION OF BODY FLUIDS 11/7/2015
 UPDATE ON VOLUME RESUSCITATION HYPOVOLEMIA AND HEMORRHAGE HUMAN CIRCULATORY SYSTEM OPERATES WITH A SMALL VOLUME AND A VERY EFFICIENT VOLUME RESPONSIVE PUMP. HOWEVER THIS PUMP FAILS QUICKLY WITH VOLUME
UPDATE ON VOLUME RESUSCITATION HYPOVOLEMIA AND HEMORRHAGE HUMAN CIRCULATORY SYSTEM OPERATES WITH A SMALL VOLUME AND A VERY EFFICIENT VOLUME RESPONSIVE PUMP. HOWEVER THIS PUMP FAILS QUICKLY WITH VOLUME
Disclosures. Objectives 10/11/17. Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock. I have no disclosures to report
 Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock Christopher K. Gordon MSN, ACNP-BC Disclosures I have no disclosures to report 1. Pathophysiology 2. Epidemiology 3. Assessment
Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock Christopher K. Gordon MSN, ACNP-BC Disclosures I have no disclosures to report 1. Pathophysiology 2. Epidemiology 3. Assessment
On Referral to our Unit
 Case Presentation By Samah Ibrahim Abdel Meguid Idris, MD Internal Medicine & Nephrology Consultant Head of Hemodialysis Unit Ahmed Maher Hospital, Alexandria Patient Data MEA 27-year-old male patient
Case Presentation By Samah Ibrahim Abdel Meguid Idris, MD Internal Medicine & Nephrology Consultant Head of Hemodialysis Unit Ahmed Maher Hospital, Alexandria Patient Data MEA 27-year-old male patient
4/5/2018. Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY. I have no financial disclosures
 Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY I have no financial disclosures 1 Objectives Why do we care about sepsis Understanding the core measures by Centers for Medicare
Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY I have no financial disclosures 1 Objectives Why do we care about sepsis Understanding the core measures by Centers for Medicare
Blood Pressure. a change in any of these could cause a corresponding change in blood pressure
 Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Intravenous Inotropic Support an Overview
 Intravenous Inotropic Support an Overview Shaul Atar, MD Western Galilee Medical Center, Nahariya Affiliated with the Faculty of Medicine of the Galilee, Safed, Israel INOTROPES in Acute HF (not vasopressors)
Intravenous Inotropic Support an Overview Shaul Atar, MD Western Galilee Medical Center, Nahariya Affiliated with the Faculty of Medicine of the Galilee, Safed, Israel INOTROPES in Acute HF (not vasopressors)
Percutaneous Mechanical Circulatory Support Devices
 Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
Οξύ στεφανιαίο σύνδρομο και καρδιογενής καταπληξία. Επεμβατική προσέγγιση. Σωτήριος Πατσιλινάκος Κωνσταντοπούλειο Γ.Ν. Ν. Ιωνίας
 Οξύ στεφανιαίο σύνδρομο και καρδιογενής καταπληξία. Επεμβατική προσέγγιση Σωτήριος Πατσιλινάκος Κωνσταντοπούλειο Γ.Ν. Ν. Ιωνίας ACUTE HEART FAILURE AND CAD: ACS / LV ischaemic dysfunction Mechanical complications
Οξύ στεφανιαίο σύνδρομο και καρδιογενής καταπληξία. Επεμβατική προσέγγιση Σωτήριος Πατσιλινάκος Κωνσταντοπούλειο Γ.Ν. Ν. Ιωνίας ACUTE HEART FAILURE AND CAD: ACS / LV ischaemic dysfunction Mechanical complications
Swans and Pressors. Vanderbilt Surgery Summer School Ricky Shinall
 Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall Shock, Swans, Pressors in 15 minutes 4 Reasons for Shock 4 Swan numbers to know 7 Pressors =15 things to know 4 Reasons for Shock Not enough
Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall Shock, Swans, Pressors in 15 minutes 4 Reasons for Shock 4 Swan numbers to know 7 Pressors =15 things to know 4 Reasons for Shock Not enough
Swans and Pressors. Vanderbilt Surgery Summer School Ricky Shinall
 Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall SHOCK Hypotension SHOCK Hypotension SHOCK=Reduction of systemic tissue perfusion, resulting in decreased oxygen delivery to the tissues.
Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall SHOCK Hypotension SHOCK Hypotension SHOCK=Reduction of systemic tissue perfusion, resulting in decreased oxygen delivery to the tissues.
Shock Management. Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate. PDF created with pdffactory Pro trial version
 Shock Management Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate Definition of Shock The definition of shock does not involve low blood pressure, rapid pulse or cool clammy skin - these
Shock Management Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate Definition of Shock The definition of shock does not involve low blood pressure, rapid pulse or cool clammy skin - these
The Cardiovascular System. Chapter 15. Cardiovascular System FYI. Cardiology Closed systemof the heart & blood vessels. Functions
 Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Cardiac Emergencies *** CME Version *** Aaron J. Katz, AEMT-P, CIC
 Cardiac Emergencies *** CME Version *** Aaron J. Katz, AEMT-P, CIC www.es26medic.net Mechanical structure Atria Ventricles One way valves Pulmonary arteries Pulmonary veins Aorta Coronary arteries Provide
Cardiac Emergencies *** CME Version *** Aaron J. Katz, AEMT-P, CIC www.es26medic.net Mechanical structure Atria Ventricles One way valves Pulmonary arteries Pulmonary veins Aorta Coronary arteries Provide
CHF and Pulmonary Edema. Rod Hetherington
 CHF and Pulmonary Edema Rod Hetherington Objectives Given a lecture and group discussion, the paramedic will be able to: Identify and name the key anatomical structures of the heart and vessels Describe
CHF and Pulmonary Edema Rod Hetherington Objectives Given a lecture and group discussion, the paramedic will be able to: Identify and name the key anatomical structures of the heart and vessels Describe
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
